Innominate artery trauma: A thirty-year experience
|
|
|
- Antonia Garrison
- 5 years ago
- Views:
Transcription
1 Innominate artery trauma: A thirty-year experience Robert H. Johnston, Jr., MD, Matthew J. Wall, Jr., MD, and Kenneth L. Mattox, MD, Houston, Texas Purpose: Injury to the innominate artery may represent a zone I cervical, thoracic outlet, or intrathoracic vascular injury and poses diagnostic, exposure, and management problems for the general, vascular, and thoracic surgeon. This complex injury often becomes a new learning experience with each infrequent encounter. Methods: Between 1960 and patients with innominate artery injuries were treated. Penetrating injuries were from gunshot wounds in 25, stab wounds in 7, and shotgun wounds in 2 patients. Blunt injuries accounted for seven of the patients. In 28 patients there were multiple injuries, including multiple vascular injuries. Median sternotomy was used in all planned operations in the later part of the study, and bilateral transsternal anterolateral thoracotomy was used in patients undergoing urgent or emergency center thoracotomy. Results: Blunt injury resulted in tears near the aortic arch with intimal disruption. Bypass grafting without hypothermia, shunts, or systemic heparinization is now used in all patients. Thirty-two patients survived to leave the hospital with no new complications related to the procedure. Postoperative neurologic complications were associated with preexisting neurologic deficits. Conclusions: Patients with innominate artery injury and stable vital signs can usually be transported without difficulty and treated without complex perioperative adjuncts. These patients can undergo revascularization with simple vascular surgical techniques and should expect an uncomplicated postoperative course unless there has been associated central nervous system injury or related injuries leading to systemic infection. Synthetic conduits have been used with success and have not required systemic heparinization or complex temporary shunting. (J VAsc StrRG 1993;17: ) Injury to the great vessels at the thoracic outlet can be one of the most challenging surgical problems that will be seen by the surgeon. These injuries can be from blunt trauma or zone I cervical, thoracic outlet, or upper thoracic penetration. The patients are frequently hypovolemic, hypothermic, and acidotic when they arrive at the emergency center. The first report of traumatic innominate artery injury was by Wheeler 1 in 1932 when ligation was the recommended treatment. Later, Langley 2 reported the case of an American airman who sustained a penetrating innominate artery injury from a shell fragment in From The Cora and Webb Mading Department of Surgery, Baylor College of Medicine, and The Ben Taub General Hospital, Houston. Presented at the Forty-sixth Annual Meeting of the Society for Vascular Surgery, Chicago, Ill., June 8-9, Reprint requests: Robert H. Johnston, Jr., MD, Clinical Professor, Department of Surgery, Baylor College of Medicine, One Baylor Plaza, Houston, TX ]6]42299 Despite 60 years of managing this injury the mortality rate has continued to remain high and this injury has continued to be associated with complications and combined injury. MATERIAL AND METHODS These data were obtained from the medical records and the surgical department's weekly activity report of the Ben Taub General Hospital. This report covers a period when one or more of the authors were participants in the surgery department at the Ben Taub General Hospital. There were 43 patients treated with innominate artery injury between 1964 and Thirty-eight were men and five were women. The average age was 38 with the age ranging from 16 to 89. The etiology was penetrating in 79.1% (34), blunt in 16.3% (7), and other causes in two patients. The penetrating injuries were secondary to gunshot wounds in 24, stab wounds in 7, and shotgun wounds in 2 (Table I) /93/$
2 Volume 17 Number 1 January 1993 Innominate artery trauma 135 Table I. Iunominate artery injury: Cause of injury No. of No. of Mortality patients deaths rate (%) Penetrating Gunshot wound Stab wound Shotgun wound Blunt trauma Other ,0 Total Associated injuries were frequently seen. Anatomic structures most commonly injured with the innominate artery were the superior vena cava, the innominate vein, and the carotid artery. These structures accounted for seven associated injuries each. Other structures injured in association with the innominate artery were the aorta, lung, and trachea. An associated condition of great significance was present in the patients who had a central nervous system deficit on presentation. There were four patients who had this problem when they were first treated, and all four died. Two patients had arteriovenous fistulas between the aorta or the innominate artery and the innominate vein. Fourteen patients had an isolated injury to the innominate artery (Table II). Shock was commonly present in these patients on admission to the emergency center. There were 17 patients who were in shock, and cardiopulmonary resuscitation was in progress on two of these on admission. Neither of these patients survived. Aortography was used in 13 of the 43 patients. Although this is the gold standard for diagnosis, shock precluded use of this test in many patients. Among the patients studied by aortography the most common wounds were by blunt trauma (six patients) and by gunshot wound (six patients). There was one study done on a patient who sustained a shotgun wound in which the only false-negative result in this series was obtained. One patient who was in shock after a gunshot wound was able to be resuscitated and underwent aortography, which demonstrated an injury to the innominate artery. The surgical approach to the management of this injury changed during the time interval under study. During the 1960s the approach was to repair this defect primarily or by inserting an interposition graft. This was accomplished through an assortment of incisions. During the 1970s there was a marked increase in the number of patients, and primary repair Table II. Innominate artery injury: Associated injury (n = 28) Associated injury No. Innominate vein 7 Superior vena cava 7 Carotid artery 7 Aorta 6 Lung 5 Trachea 4 Central nervous system 4 Subclavian artery and vein 3 Abdominal injury 3 Arteriovenous fistulas 2 Esophagus 2 Pulmonary artery and vein 1 continued to be the technique of choice. Early in the 1970s one of us (K.L.M.) began using the bypass principle for correction of this injury. The incision used was the median sternotomy, with only two patients having a "book" or "trap-door" incision and two additional patients having bilateral anterior thoracotomy. Since that time this method has become our exclusive approach to correction of this defect. Once the bypass from the ascending aorta to distal innominate artery is complete, a pledgeted suture line is placed in the aortic arch to close the origin of the innominate artery (Table III). Twenty-four patients were treated by primary arterial repair, four by interposition graft, and 13 by the insertion of a bypass graft from the ascending aorta to the distal innominate artery (Fig. 1). The bypass graft material was Dacron in nine and polytetrafluoroethylene (Gore-Tex*) in four. RESULTS The survival rate for the series was 74.4%. However, when analyzed by decade the evolution of approach is very clear. During the decade of the sixties there were four patients treated with two deaths; during the seventies 19 patients were treated for this injury and there were seven deaths. In the eighties there were 16 patients treated with two deaths, and no deaths have yet occurred in patient treated in the nineties. This calculates to a crude mortality rate of 50% during the sixties, 36.8% during the seventies, 11.8% during the eighties, and 0.0% so far during the nineties (Table IV). The clearest predictor of bad outcome was preoperative central nervous system deficit. Patients in which this was present had hemiparesis associated *Gore-Tex is a registered trademark of W.L. Gore & Associates, Flagstaff, Ariz.
3 136 Johnston, Wall, and Mattox Journal of VASCULAR SURGERY A 0 Fig. 1. Drawing depicts bypass technique used for patients with innominate artery injury. Table III. Innominate artery injury: Type of operative procedure, by decade Decade Procedure Total Bypass Primary repair Interposition Other with the injury on admission to the emergency center. Three of these patients were in shock on admission and one was normotensive but with paraplegia. All of the patients who had hemiplegia on presentation eventually died. All patients who required cardiopulmonary resuscitation before arrival at the emergency center died. Seventeen patients were in shock on admission and 59% survived (Table V). The patients who sustained innominate artery injury secondary to bltmt trauma all had proximal injury, that is, at the junction of the innominate artery and the aorta. The locations of the penetrating injuries were more distal, however, they were found throughout the length of the innominate artery. Associated injury was present in 30 of these patients (69.7%). The most common associated injury was to the innominate vein, superior vena cava, and carotid arteries. Preadmission central nervous system deficits correlated with mortality but did not correlate with carotid artery injury. There were seven carotid artery injuries present in this series. Of the patients with these injuries, one had hemiplegia on
4 Volume 17 Number 1 January 1993 Innominate artery trauma 137 Table IV. Innominate artery injury: Mortality rate and complications, by decade Decade Total No. of patients No. of complications No. of deaths Mortality rate 50.0% 36.8% 11.8% 0.0% 43 (100%) 14 (33%) 11 (25.6%) Table V. Innominate artery injury: Mortality rate, by presentation No. No. of Mortality patients deaths rate (%) Cardiopulmonary resusci tation Shock Central nervous system injury presentation and one had a seizure after operation but no residual neurologic deficit. Five patients with carotid artery injury had no neurologic deficits. When the patients with or without associated injuries are compared, 88% of the patients who were in shock on admission had associated injuries, thus a significant mortality rate of 41.2% was found. The group with the worst outcome by etiology was that with stab wounds in which three of seven died, while in the larger group of patients with gunshot wounds six of 25 died. In the group of patients with blunt trauma only one of seven patients died, and this was associated with a head injury (Table I), which caused the death. Median sternotomy was the most common incision used in this group of patients and was found to have the lowest associated mortality. This may be because of its more common use in the later part of the study and its use in combination with the bypass principle. Overall 37.2% of our patients had some complication after operation, and the overall mortality rate was 26.2% (Tables VI and VII). DISCUSSION The successful management ofvascnlar injuries of the thoracic outlet is one of the most challenging, yet rewarding feats in surgery. It has been reported that 20.1% of vascular injuries are in the chest, 3 and of that group 71% of the patients with major vascular injuries of the thoracic outlet or base of the neck die before arrival at the hospital. 4 With the development of the Emergency Medical Service system in Hous- Table VI. Innominate artery injury: Postoperative complications Complication No. Wound infection 3 Pulmonary failure : 2 Gastrointestinal bleeding 2 Mediastinitis 1 Anastomosis disruption 1 Sternal dehiscence 1 Pneumonia 1 Coagulopathy 1 Meningitis 1 Systemic air embolus 1 Sepsis 1 ton, the aggressive use of emergency center thoracotomy and arteriography, and the increase in illegal drug activities, the surgical service at Ben Taub General Hospital is seeing more patients who have sustained cardiovascular injury, s In 1991 two groups reviewed innominate artery injury and reported on a total composite of 22 patients from the literature who sustained innominate artery injury and their managementfi '6 We reviewed our experience with this injury and found that 43 patients had been treated during a 30-year period (Table VIII). Of this group the most common etiologic factor was penetrating injury, which accounted for most of the mortality. In different geographic areas there is a difference in the etiology of the penetrating wound, with some areas of the United States reporting a higher incidence of stab wound compared with the 57% of patients in this series who sustained gunshot wound. Patients with innominate vascular injury are commonly hypovolemic, hypothermic, and acidotic on arrival at the emergency center, 7 which necessitates resuscitation of the patient by surgical personnel in the emergency center before operative intervention. Emergency center thoracotomy is aggressively used in our emergency center, however, in patients with innominate artery injury only one patient was treated in this manner and did not survive. Once
5 Journal of VASCULAR 138 Johnston, Wall, and Mattox SURGERY Table VII. Innominate artery injury: Deaths Date Cause Complication Repair Presentation 4/64 Gunshot wound 9/69 Gunshot wound 5/70 Shotgun wound 12/70 Gunshot wound 10/71 Gunshot wound 12/72 Tracheostomy erosion 1/74 Gunshot wound 7/75 Blunt trattma 12/76 Shotgun wound 5/81 Shotgun wound 8/87 Gunshot wound Anastomotic breakdown Primary Unknown Pneumothorax, bronchopleural fistulas Interposition graft Shock Hypothermia, coagulopathy Primary Shock Central nervous system injury Primary Normotensive Central nervous system injury Ligation Shock Meningitis Graft interposition - Central nervous system injury Primary Unknown Central nervous system injury Bypass Shock Cardiopulmonary resuscitation Primary Shock Air embolus Bypass Shock Cardiopulmonary resuscitation Primary Shock resuscitated the patients who were in shock were transported rapidly to the operating room where definitive repair of the injury was undertaken. In the group who were stable on admission to the emergency center, aortography was done. There were 13 patients in this group who underwent aortography. In the 13 patients who underwent arteriography one false-negative result was obtained, and this was in a patient with a shotgun injury. As Richardson et al. 8 have pointed out, up to 23% of arteriograms may give false-negative results for penetrating trauma. Every effort is made to do arteriography in thoracic outlet injury. However, in a large number of patients this is precluded by the condition of the patient, which necessitates rapid mediastinal exploration. The overall mortality rate in this study was 25.6%. However, when the patient, treatment, and outcome are reviewed by decade an interesting observation is made. During a 30-year period, a fall in mortality rate from 50% to 36.8% to 11.8% is seen. During the study period there was an evolution of the incision used and the method of operative repair. Early on, all patients were treated by primary repair or graft interposition through an assortment of incisions. It was not until the seventies and eighties that the median sternotomy emerged as the incision of choice for repair of this injury, and now this is the standard approach in our trauma center. In the eighties the bypass principle became the method of choice for patients seen with this injury at the Ben Taub General Hospital. A total of 70% of our patients had associated injuries. When an associated injury existed it significantly increased the mortality rate, from 8.3% to 33.3%. As the operative management of these patients has evolved, a median sternotomy incision with a Table VIII. Innominate artery injury: McLean literature review, No. of No. Years Author Year ceases survived reviewed Lim Pate and Casini Graham Bladergroen Weaver Johnston li 30 right neck extension for better visualization of the innominate bifurcation is now preferred. Bleeding is controlled by pressure or clamp as is needed. Before this injury is dealt with a partial occluding clamp is placed on the ascending aorta and a graft is sutured in place. The innominate is then divided just before its bifilrcation and end-to-end anastomosis is accomplished. A partial occluding clamp is placed on the aorta at its junction with the innominate artery. The aorta is then closed with pledgeted sutures and fmally a second running suture line. No shunt, heparin, or cardiopulrnonary bypass is used for this repair. In the earlier bypass repairs Dacron fabric grafts were used and more recently 8 mm polytetrafluoroethylene (Gore-Tex) grafts have been the graft of choice. No problems with graft infection or thrombosis have been encountered. There were several arteriovenous fistulas present in this series. The most recent patient came to us for treatment several months after a high-velocity gunshot wound to the aortic arch-innominate junction with fismlization to the innominate vein. Symbas 9 suggests that the presence of arteriovenous fistulas may provide some protection for the patient with these injuries because the bleeding returns to the
6 Volume 17 Number 1 January 1993 Innominate artery trauma 139 vascular system. Another interesting phenomenon is that patients with a left carotid artery origin from the innominate artery seem to have more of a propensity for innominate disruption from blunt trauma.i This anomaly is present in 11% of the population, but is seen in a disproportionate number of patients who have innominate disruption when first seen (29%).I This may suggest an increased susceptibility of this anatomic variation to traumatic avulsion. The group of patients with blunt trauma tends to be more stable and transfer can be accomplished without significant fear of rupture. 11 With the exclusion of patients who are admitted in shock or have concomitant cerebral or multisystem trauma, the survival rate exceeds 90%, and in this series all survived who were not in shock or had no associated injury. The reported mortality rate of innominate artery injury approaches 30% and the reported likelihood of complications may exceed 40%.12 This current series reports a mortality rate of 25.6% and a complication rate of 37.2%, which compare favorably with the literature. Innominate artery injury is a formidable entity that requires organization and planning to achieve a desirable result for the injured patient. REFERENCES 1. Wheeler WI de C. Traumatic subclavian aneurysm. Irish J Med Sci 1942;6th s: Langley GF. Gunshot wound of the innominate artery. BM[[ 1943;Dec 4: Mattox K, Feliciano D, Butch J, Beall A, Jordan G, DeBakey M. Five thousand seven hundred sixty cardiovascular injuries in 4459 patients. Ann Surg 1989;209: Kemmerer W, Eckert W, Gathright J, et al. Patterns of thoracic injuries in fatal traffic accidents. J Trauma 1961;1: McLean TR, McManus PR. Penetrating trauma involving the innominate artery. Ann Thorac Surg 1991;51: Gubler K, Wisner D, Blaisdell FW. Multiple vessel injury to branches of the aortic arch: case report. J Trauma 1991;31: Mattox K. Symposium: new approach in vascular trauma. [1 VAsc SURG 1988;7: Richardson J, Smith M, Grover F, Arom K, Trinkle JK. Management of subclavian and innominate artery injuries. Am 1 Surg 1977;134: Symbas PN. Cardiothoracic trauma. Philadelphia: W-B Sanders; 1989: Graham J, Feliciano D, Mattox K, BeaU A. Innominate vascular injury. J Trauma 1982;22: Mattox K. Thoracic great vessel injury. Surg Clin North Am 1988;68: Submitted June 12, 1992; accepted Sept. 1, DISCUSSION Dr. Peter C. Pairolero (Rochester, Minn.). I would like to thank Dr. Johnston for an excellent presentation. Unquestionably, injuries to the great vessels at the level of the thoracic inlet have, throughout the years, been most challenging. In the past, the mortality associated with these injuries has been one of the highest for any type of arterial trauma. Fortunately, however, improvement has occurred, and the authors are to be congratulated on their excellent survival rate of nearly 90%, achieved during the past decade, for isolated innominate artery injury. Nonetheless, controversy still continues to exist regarding the best method of establishing the diagnosis of great vessel injury and of surgical management. The diagnosis of major arterial injury is obvious in the presence of bleeding, expanding hematoma, absent pulses, and circulatory collapse. But what if these are not present? In only 17 of Dr. Johnston's 42 patients was shock present. Clearly a high index of suspicion is required and, undoubtedly, this is more likely to occur if the injury is penetrating. However, approximately 15% of their patients had blunt trauma. Should great vessel injury then be suspected in all patients who have significant trauma to the anterior chest and base of the neck? As Dr. Johnston has mentioned, most surgeons would agree that if the patient is stable, arteriography is the gold standard to define the extent and location of injury. Yet arteriography is not infallible, as demonstrated in the Houston series, which had a false-negative rate of approximately 10%. If we cannot safely observe the patient with a negative arteriography result, is there any role for computed tomography after arteriography? Or, if the index of suspicion remains high, should the patient simply undergo exploratory operation? I would like Dr. Johnston to expand on the algorithm used in establishing the diagnosis of great vessel injury. The goal of surgical intervention is simple: early operation, arterial control, and vascular repair. The decision regarding exposure, however, is more complex. Is the injury in the neck, thoracic outlet, or thorax? It is probably best to consider all injuries in this region as involving the
7 140 Johnston, Wall, and Mattox Journal of VASCULAR. SURGERY thoracic outlet, and as the authors have amply demonstrated, exposure via the median sternotomy route is quite adequate. The incision can be extended into the neck or into either thorax, if indicated. Moreover, exposure of all brachiocephalic vessels, including the left subclavian, is possible, and if necessary cardiopulmonary bypass can be initiated in the patient. Finally, I agree with the authors' choice of arterial bypass when reconstruction is needed. In our experience with chronic innominate artery disease, bypass was the most successful long-term reconstructive procedure. Dr. Robert H. Johnston, Jr. Concerning our diag- nostic approach to these patients, if we are afforded the opportunity of treating a patient who is more or less stable, aortography is the gold standard for diagnosis. To explore these patients without it is like flying blind without instruments, because you do not know the extent of the injuries that could be there. Aortography is still the gold standard. However, most of the patients who are in extremis when brought to the emergency center are either operated on in the emergency center or taken directly to the operating room where exploration is undertaken.
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Penetrating wounds of the heart and great vessels
 Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
P ischemia of the brain, spinal cord, kidneys, and
 Penetrating Injuries of the Aortic Arch and Its Branches James W. Pate, MD, F. Hammond Cole, Jr, MD, William A. Walker, MD, and Timothy C. Fabian, MD Section of Cardiothoraac Surgery, University of Tennessee,
Penetrating Injuries of the Aortic Arch and Its Branches James W. Pate, MD, F. Hammond Cole, Jr, MD, William A. Walker, MD, and Timothy C. Fabian, MD Section of Cardiothoraac Surgery, University of Tennessee,
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die
 account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
Aortic Arch/ Thoracoabdominal Aortic Replacement
 Aortic Arch/ Thoracoabdominal Aortic Replacement Joseph S. Coselli, M.D. Vice Chair, Department of Surgery Professor, Chief, and Cullen Foundation Endowed Chair Division of Cardiothoracic Surgery Baylor
Aortic Arch/ Thoracoabdominal Aortic Replacement Joseph S. Coselli, M.D. Vice Chair, Department of Surgery Professor, Chief, and Cullen Foundation Endowed Chair Division of Cardiothoracic Surgery Baylor
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Blunt Partial Transection of the Innominate Artery
 Blunt Partial Transection of the Innominate Artery: Anomalous Origin of the Left Carotid Artery and Off-Pump Repair Brett E. Grizzell, M.D. 1, Gie Na Yu, M.D. 1, Phillip F. Bongiorno, M.D. 1,2, James M.
Blunt Partial Transection of the Innominate Artery: Anomalous Origin of the Left Carotid Artery and Off-Pump Repair Brett E. Grizzell, M.D. 1, Gie Na Yu, M.D. 1, Phillip F. Bongiorno, M.D. 1,2, James M.
Advances in the Treatment of Acute Type A Dissection: An Integrated Approach
 Advances in the Treatment of Acute Type A Dissection: An Integrated Approach Joseph E. Bavaria, MD, Derek R. Brinster, MD, Robert C. Gorman, MD, Y. Joseph Woo, MD, Thomas Gleason, MD, and Alberto Pochettino,
Advances in the Treatment of Acute Type A Dissection: An Integrated Approach Joseph E. Bavaria, MD, Derek R. Brinster, MD, Robert C. Gorman, MD, Y. Joseph Woo, MD, Thomas Gleason, MD, and Alberto Pochettino,
Aberrant Right Subclavian Artery Aneurysm
 Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Advances in Treatment of Traumatic Aortic Transection
 Advances in Treatment of Traumatic Aortic Transection Himanshu J. Patel MD University of Michigan Medical Center Author Disclosures Consulting fees from WL Gore Inc. There is no disease more conducive
Advances in Treatment of Traumatic Aortic Transection Himanshu J. Patel MD University of Michigan Medical Center Author Disclosures Consulting fees from WL Gore Inc. There is no disease more conducive
RESUSCITATION IN TRAUMA. Important things I have learnt
 RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
Schedule of Benefits. for Professional Fees Vascular Procedures
 Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
SELECTIVE ANTEGRADE TECHNIQUE OF CHOICE
 SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service
 Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service J Islam, 1,4 G L Laing, 2,4 J L Bruce, 2,4 G V Oosthuizen, 2,4 D L Clarke, 2,4 J V Robbs 3,4
Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service J Islam, 1,4 G L Laing, 2,4 J L Bruce, 2,4 G V Oosthuizen, 2,4 D L Clarke, 2,4 J V Robbs 3,4
TEVAR FOR! THORACIC AORTIC TRAUMA"
 10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
Thoracoabdominal aortic aneurysms by definition traverse
 Thoracoabdominal Aortic Aneurysm Repair: Open Technique Joseph Huh, MD, Scott A. LeMaire, MD, Scott A. Weldon, MA, CMI, and Joseph S. Coselli, MD Thoracoabdominal aortic aneurysms by definition traverse
Thoracoabdominal Aortic Aneurysm Repair: Open Technique Joseph Huh, MD, Scott A. LeMaire, MD, Scott A. Weldon, MA, CMI, and Joseph S. Coselli, MD Thoracoabdominal aortic aneurysms by definition traverse
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Deliberate Renal Ischemia
 Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
Deliberate Renal Ischemia A Valuable and Safe Adjunct During Operations upon the Abdominal Aorta Robert K. Brawley, M.D., R. Darryl Fisher, M.D., Tom R. DeMeester, M.D., and Ronald C. Elkins, M.D. ABSTRACT
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
Management of Penetrating Cervicomediastinal Venous Trauma
 Eur J Vasc Endovasc Surg 19, 65 69 (2000) doi:10.1053/ejvs.1999.0965, available online at http://www.idealibrary.com on Management of Penetrating Cervicomediastinal Venous Trauma R. Nair, J. V. Robbs and
Eur J Vasc Endovasc Surg 19, 65 69 (2000) doi:10.1053/ejvs.1999.0965, available online at http://www.idealibrary.com on Management of Penetrating Cervicomediastinal Venous Trauma R. Nair, J. V. Robbs and
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN
 CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Endovascular Trauma Management. Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden
 Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro.
 ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF KOMMERELL S DIVERTICULUM : AN ALTERNATIVE APPROACH. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro. Department
ABERRANT RIGHT SUBCLAVIAN ARTERY AND CALCIFIED ANEURYSM OF KOMMERELL S DIVERTICULUM : AN ALTERNATIVE APPROACH. Jose Rubio-Alvarez, Juan Sierra-Quiroga, Belen Adrio Nazar and Javier Garcia Carro. Department
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm
 Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud
 How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
DISCLOSURES ISOLATED DTA LESION? TYPE B DISSECTIONS TREATMENT OPTIONS
 Endovascular Repair of Aortic Arch Pathologies; What is available/possible in the U.S. in 2018? Kaiser Permanente Endovascular Symposium 6/2/18 Sukgu M Han, MD, MS Assistant Professor of Clinical Surgery
Endovascular Repair of Aortic Arch Pathologies; What is available/possible in the U.S. in 2018? Kaiser Permanente Endovascular Symposium 6/2/18 Sukgu M Han, MD, MS Assistant Professor of Clinical Surgery
Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report
 CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
CASE REPORTS Axillobrachial artery bypass grafting with in situ cephalic vein for axillary artery occlusion: A case report Evan S. Cohen,/VII), Robert B. Holtzman, MD, and George W. Johnson, Jr., MD, Houston,
Diagnosis & Management of Kidney Trauma. LAU - Urology Residency Program LOP Urology Residents Meeting
 Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Mechanical Bleeding Complications During Heart Surgery
 Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Mechanical Bleeding Complications During Heart Surgery Arthur C. Beall, Jr., M.D., Kenneth L. Mattox, M.D., Mary Martin, R.N., C.C.P., Bonnie Cromack, C.C.P., and Gary Cornelius, C.C.P. * Potential for
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Vascular Surgery AMPUTATION AORTA
 SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
The first report of the Society of Thoracic Surgeons
 REPORT The Society of Thoracic Surgeons National Congenital Heart Surgery Database Report: Analysis of the First Harvest (1994 1997) Constantine Mavroudis, MD, Melanie Gevitz, BA, W. Steves Ring, MD, Charles
REPORT The Society of Thoracic Surgeons National Congenital Heart Surgery Database Report: Analysis of the First Harvest (1994 1997) Constantine Mavroudis, MD, Melanie Gevitz, BA, W. Steves Ring, MD, Charles
I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical Department National Taiwan University Hospital
 Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
Comparisons of Aortic Remodeling and Outcomes after Endovascular Repair of Acute and Chronic Complicated Type B Aortic Dissections I-Hui Wu, M.D. Ph.D. Clinical Assistant Professor Cardiovascular Surgical
2 Aortic Arch Debranching UCSF Vascular Symposium /14/16. J Endovasc Ther 2002;9:suppl 2; II98 105
 How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR
 Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
Combined Endovascular and Surgical Repair of Thoracoabdominal Aortic Pathology: Hybrid TEVAR William J. Quinones-Baldrich MD Professor of Surgery Director UCLA Aortic Center UCLA Medical Center Los Angeles,
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
L cancer-related deaths in Japan. The number of patients
 Extended Resection of the Left Atrium, Great Vessels, or Both for Lung Cancer Ryosuke Tsuchiya, MD, Hisao Asamura, MD, Haruhiko Kondo, MD, Tomoyuki Goya, MD, and Tsuguo Naruke, MD Division of Thoracic
Extended Resection of the Left Atrium, Great Vessels, or Both for Lung Cancer Ryosuke Tsuchiya, MD, Hisao Asamura, MD, Haruhiko Kondo, MD, Tomoyuki Goya, MD, and Tsuguo Naruke, MD Division of Thoracic
Subclavian artery Stenting
 Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
Subclavian artery Stenting Etiology Atherosclerosis Takayasu s arteritis Fibromuscular dysplasia Giant Cell Arteritis Radiation-induced Vascular Injury Thoracic Outlet Syndrome Neurofibromatosis Incidence
May Clinical Director, Peninsula Trauma Network (Edited for PTN)
 Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND
 Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist. M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria
 Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Evidence Surgical aortic arch replacement with a Dacron
Aortic Arch Treatment Open versus Endo Evidence versus Zeitgeist M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Evidence Surgical aortic arch replacement with a Dacron
Acute Penetrating Tracheal Trauma
 Acute Penetrating Tracheal Trauma Panagiotis N. Symbas, M.D., Charles R. Hatcher, Jr., M.D., and Gerhard A. W. Boehm, M.D. ABSTRACT During the past ten years, 20 patients with acute penetrating tracheal
Acute Penetrating Tracheal Trauma Panagiotis N. Symbas, M.D., Charles R. Hatcher, Jr., M.D., and Gerhard A. W. Boehm, M.D. ABSTRACT During the past ten years, 20 patients with acute penetrating tracheal
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
3 : 37. Kirit Patel, USA CLASSIFICATION DIAGNOSIS
 3 : 37 Management of Aortic Aneurysms Clinical features and diagnosis of thoracic aortic aneurysm An aneurysm is currently defined as a localized dilatation of the aorta, 50 percent over the normal diameter,
3 : 37 Management of Aortic Aneurysms Clinical features and diagnosis of thoracic aortic aneurysm An aneurysm is currently defined as a localized dilatation of the aorta, 50 percent over the normal diameter,
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury
 TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
AORTIC DISSECTIONS Current Management. TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida
 AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
AORTIC DISSECTIONS Current Management TOMAS D. MARTIN, MD, LAT Professor, TCV Surgery Director UF Health Aortic Disease Center University of Florida DISCLOSURES Terumo Medtronic Cook Edwards Cryolife AORTIC
Table I. Associated diseases
 Thoracic and thoracoabdominal aortic aneurysm repair using cardiopulmonary bypass, profound hypothermia, and circulatory arrest via left side of the chest incision Hazim J. Safi, MD, Charles C. Miller
Thoracic and thoracoabdominal aortic aneurysm repair using cardiopulmonary bypass, profound hypothermia, and circulatory arrest via left side of the chest incision Hazim J. Safi, MD, Charles C. Miller
Management of Penetrating Neck Trauma
 Management of Penetrating Neck Trauma Shashidhar S. Reddy, MD, MPH Faculty Advisor: Shawn D. Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation
Management of Penetrating Neck Trauma Shashidhar S. Reddy, MD, MPH Faculty Advisor: Shawn D. Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Total arch replacement with separated graft technique and selective antegrade cerebral perfusion
 Masters of Cardiothoracic Surgery Total arch replacement with separated graft technique and selective antegrade cerebral perfusion Teruhisa Kazui 1,2 1 Hamamatsu University School of Medicine, Hamamatsu,
Masters of Cardiothoracic Surgery Total arch replacement with separated graft technique and selective antegrade cerebral perfusion Teruhisa Kazui 1,2 1 Hamamatsu University School of Medicine, Hamamatsu,
EAST MULTICENTER STUDY DATA DICTIONARY. Temporary Intravascular Shunt Study Data Dictionary
 EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Management of Airway Trauma I:
 Management of Airway Trauma I: Tracheobronchial Injuries James P. Kelly, M.D., Watts R. Webb, M.D., Peter V. Moulder, M.D., Charles Everson, M.D., Buford H. Burch, M.D., and Edward S. Lindsey, M.D. ABSTRACT
Management of Airway Trauma I: Tracheobronchial Injuries James P. Kelly, M.D., Watts R. Webb, M.D., Peter V. Moulder, M.D., Charles Everson, M.D., Buford H. Burch, M.D., and Edward S. Lindsey, M.D. ABSTRACT
Shock and Resuscitation: Part II. Patrick M Reilly MD FACS Professor of Surgery
 Shock and Resuscitation: Part II Patrick M Reilly MD FACS Professor of Surgery Trauma Patient 1823 / 18 Police Dropoff Torso GSW Lower Midline / Right Buttock Shock This Monday Trauma Patient 1823 / 18
Shock and Resuscitation: Part II Patrick M Reilly MD FACS Professor of Surgery Trauma Patient 1823 / 18 Police Dropoff Torso GSW Lower Midline / Right Buttock Shock This Monday Trauma Patient 1823 / 18
AORTIC DISSECTION. DISSECTING ANEURYSMS OF THE AORTA or CLASSIFICATION
 DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
DISSECTING ANEURYSMS OF THE AORTA or AORTIC DISSECTION CLASSIFICATION DeBakey classified aortic dissections into types I, II, and III :- Type I dissection the tear site originates in the ascending aorta,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection: Con
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection: Con Thomas G. Gleason, M.D. Ronald V. Pellegrini Professor and Chief Division of Cardiac Surgery University of Pittsburgh Presenter
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection: Con Thomas G. Gleason, M.D. Ronald V. Pellegrini Professor and Chief Division of Cardiac Surgery University of Pittsburgh Presenter
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Type II arch hybrid debranching procedure
 Safeguards and Pitfalls Type II arch hybrid debranching procedure Prashanth Vallabhajosyula, Wilson Y. Szeto, Nimesh Desai, Caroline Komlo, Joseph E. Bavaria Division of Cardiovascular Surgery, University
Safeguards and Pitfalls Type II arch hybrid debranching procedure Prashanth Vallabhajosyula, Wilson Y. Szeto, Nimesh Desai, Caroline Komlo, Joseph E. Bavaria Division of Cardiovascular Surgery, University
Bypass Grafting and Aneurysmorrhaphy
 ORIGINAL ARTICLES Bypass Grafting and Aneurysmorrhaphy for Aortic Arch Aneurysms Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., and Alan C. Leshnower, M.D. ABSTRACT The technique of permanent aortic
ORIGINAL ARTICLES Bypass Grafting and Aneurysmorrhaphy for Aortic Arch Aneurysms Harold C. Urschel, Jr., M.D., Maruf A. Razzuk, M.D., and Alan C. Leshnower, M.D. ABSTRACT The technique of permanent aortic
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report
 Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Occlusion of All Four Extracranial Vessels With Minimal Clinical Symptomatology. Case Report BY JIRI J. VITEK, M.D., JAMES H. HALSEY, JR., M.D., AND HOLT A. McDOWELL, M.D. Abstract: Occlusion of All Four
Acute dissections of the descending thoracic aorta (Debakey
 Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Endovascular Treatment of Acute Descending Thoracic Aortic Dissections Nimesh D. Desai, MD, PhD, and Joseph E. Bavaria, MD Acute dissections of the descending thoracic aorta (Debakey type III or Stanford
Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open techniques.
 ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
ISPUB.COM The Internet Journal of Thoracic and Cardiovascular Surgery Volume 14 Number 2 Management of the persistent sciatic artery with coexistent aortoiliac aneurysms; endovascular and open A Rodriguez-Rivera,
Anterior Spinal Artexy Syndrome with Chronic Traumatic Thoracic Aortic Aneurysm
 Anterior Spinal Artexy Syndrome with Chronic Traumatic Thoracic Aortic Aneurysm Vincent R. Conti, M.D., John Calverley, M.D., William L. Safley, M.D., Melinda Estes, M.D., and Edward H. Williams, M.D.
Anterior Spinal Artexy Syndrome with Chronic Traumatic Thoracic Aortic Aneurysm Vincent R. Conti, M.D., John Calverley, M.D., William L. Safley, M.D., Melinda Estes, M.D., and Edward H. Williams, M.D.
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery
 Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
Remodeling of the Remnant Aorta after Acute Type A Aortic Dissection Surgery Are Young Patients More Likely to Develop Adverse Aortic Remodeling of the Remnant Aorta Over Time? Suk Jung Choo¹, Jihoon Kim¹,
Experience of endovascular procedures on abdominal and thoracic aorta in CA region
 Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Disclosures: Acute Aortic Syndrome. A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO
 Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Acute Aortic Syndrome Disclosures: A. Michael Borkon, M.D. Director of CV Surgery Mid America Heart Institute Saint Luke s Hospital Kansas City, MO No financial relationships to disclose 1 Acute Aortic
Post-Op Aorta: Differentiating Normal Post-Op vs. Complications. Linda C. Chu, MD Assistant Professor of Radiology Johns Hopkins University
 Post-Op Aorta: Differentiating Normal Post-Op vs. Complications Linda C. Chu, MD Assistant Professor of Radiology Johns Hopkins University No disclosures Disclosures Goals and Objectives To review CT technique
Post-Op Aorta: Differentiating Normal Post-Op vs. Complications Linda C. Chu, MD Assistant Professor of Radiology Johns Hopkins University No disclosures Disclosures Goals and Objectives To review CT technique
LIST OF CLINICAL PRIVILEGES CARDIOTHORACIC SURGERY
 LIST OF CLINICAL PRIVILEGES CARDIOTHORACIC SURGERY AUTHORITY: Title 10, U.S.C. Chapter 55, Sections 1094 and 1102. PRINCIPAL PURPOSE: To define the scope and limits of practice for individual providers.
LIST OF CLINICAL PRIVILEGES CARDIOTHORACIC SURGERY AUTHORITY: Title 10, U.S.C. Chapter 55, Sections 1094 and 1102. PRINCIPAL PURPOSE: To define the scope and limits of practice for individual providers.
Internal Injury Documentation Guidelines
 Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Challenges. 1. Sizing. 2. Proximal landing zone 3. Distal landing zone 4. Access vessels 5. Spinal cord ischemia 6. Endoleak
 Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic, Gore Employment in industry Stockholder of a healthcare company Owner of a healthcare company Other(s)
Traumatic A-V A V Fistula
 Traumatic A-V A V Fistula PRESENT HISTORY PAST HISTORY 30 year-old, male ( XX); Denied other systemic disease before. PRESENT HISTORY A deep stabbing wound (3*1 cm) noted on 07/01/2002 over Right anterior
Traumatic A-V A V Fistula PRESENT HISTORY PAST HISTORY 30 year-old, male ( XX); Denied other systemic disease before. PRESENT HISTORY A deep stabbing wound (3*1 cm) noted on 07/01/2002 over Right anterior
Acute type A aortic dissection (Type I, proximal, ascending)
 Acute Type A Aortic Dissection R. Morton Bolman, III, MD Acute type A aortic dissection (Type I, proximal, ascending) is a true surgical emergency. It is estimated that patients suffering this calamity
Acute Type A Aortic Dissection R. Morton Bolman, III, MD Acute type A aortic dissection (Type I, proximal, ascending) is a true surgical emergency. It is estimated that patients suffering this calamity
Tracheal stenosis in infants and children is typically characterized
 Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Slide Tracheoplasty for Congenital Tracheal Stenosis Peter B. Manning, MD Tracheal stenosis in infants and children is typically characterized by the presence of complete cartilaginous tracheal rings and
Sectional Anatomy Quiz - III
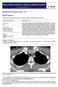 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Accepted Manuscript. Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi
 Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
Hybrid thoracic endovascular aortic repair via right anterior minithoracotomy
 Hybrid thoracic endovascular aortic repair via right anterior minithoracotomy Javier E. Anaya-Ayala, MD, a,b Zulfiqar F. Cheema, MD, PhD, a Mark G. Davies, MD, PhD, MBA, a,b Jean Bismuth, MD, a,b Basel
Hybrid thoracic endovascular aortic repair via right anterior minithoracotomy Javier E. Anaya-Ayala, MD, a,b Zulfiqar F. Cheema, MD, PhD, a Mark G. Davies, MD, PhD, MBA, a,b Jean Bismuth, MD, a,b Basel
STS/EACTS LatAm CV Conference 2017
 STS/EACTS LatAm CV Conference 2017 Joseph E. Bavaria, MD Director, Thoracic Aortic Surgery Program Roberts-Measey Professor and Vice Chair of CV Surgery University of Pennsylvania Immediate-Past President
STS/EACTS LatAm CV Conference 2017 Joseph E. Bavaria, MD Director, Thoracic Aortic Surgery Program Roberts-Measey Professor and Vice Chair of CV Surgery University of Pennsylvania Immediate-Past President
The evolution of the Fontan procedure for single ventricle
 Hemi-Fontan Procedure Thomas L. Spray, MD The evolution of the Fontan procedure for single ventricle cardiac malformations has included the development of several surgical modifications that appear to
Hemi-Fontan Procedure Thomas L. Spray, MD The evolution of the Fontan procedure for single ventricle cardiac malformations has included the development of several surgical modifications that appear to
IS POLYTETRAFLUOROETHYLENE (PTFE) THE CORRECT CHOICE TO TREAT CONTAMINATED TRAUMATIC VASCULAR INJURIES?
 IS POLYTETRAFLUOROETHYLENE (PTFE) THE CORRECT CHOICE TO TREAT CONTAMINATED TRAUMATIC VASCULAR INJURIES? Nigel Denis MD Class of 2016 University of Miami Miller School of Medicine Miami, Florida, USA Disclosures
IS POLYTETRAFLUOROETHYLENE (PTFE) THE CORRECT CHOICE TO TREAT CONTAMINATED TRAUMATIC VASCULAR INJURIES? Nigel Denis MD Class of 2016 University of Miami Miller School of Medicine Miami, Florida, USA Disclosures
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Management of the vertebral artery during thoracic endovascular aortic repair with coverage of the left subclavian artery
 Original Article Management of the vertebral artery during thoracic endovascular aortic repair with coverage of the left subclavian artery Jian Zhu*, Er-Ping Xi*, Shui-Bo Zhu, Gui-Lin Yin, Rong-Ping Wang,
Original Article Management of the vertebral artery during thoracic endovascular aortic repair with coverage of the left subclavian artery Jian Zhu*, Er-Ping Xi*, Shui-Bo Zhu, Gui-Lin Yin, Rong-Ping Wang,
Santi Trimarchi, MD, PhD Vascular Surgeon Thoracic Aortic Research Center, Director IRCCS Policlinico San Donato University of Milan
 The Gore GREAT Registry: Update about a real life data collection Santi Trimarchi, MD, PhD Vascular Surgeon Thoracic Aortic Research Center, Director IRCCS Policlinico San Donato University of Milan Disclosures
The Gore GREAT Registry: Update about a real life data collection Santi Trimarchi, MD, PhD Vascular Surgeon Thoracic Aortic Research Center, Director IRCCS Policlinico San Donato University of Milan Disclosures
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation
 Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Antegrade Thoracic Stent Grafting during Repair of Acute Debakey I Dissection: Promotes Distal Aortic Remodeling and Reduces Late Open Re-operation Vallabhajosyula, P: Szeto, W; Desai, N; Pulsipher, A;
Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine
 Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
Leonard N. Girardi, M.D. Chairman and O. Wayne Isom Professor Department of Cardiothoracic Surgery Weill Cornell Medicine New York, New York Houston Aortic Symposium Houston, Texas February 23, 2017 weill.cornell.edu
