Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service
|
|
|
- Barrie Burns
- 5 years ago
- Views:
Transcription
1 Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service J Islam, 1,4 G L Laing, 2,4 J L Bruce, 2,4 G V Oosthuizen, 2,4 D L Clarke, 2,4 J V Robbs 3,4 VASCULAR SURGERY 1 Pietermaritzburg Metropolitan Vascular Surgery, Pietermaritzburg, South Africa 2 Pietermaritzburg Metropolitan Trauma Surgery, Pietermartizburg, South Africa 3 Private Practice, Entabeni Hospital, Durban, South Africa 4 Nelson R Mandela School of Medicine, University of KwaZulu-Natal, Pietermaritzburg, South Africa Corresponding author: J Islam (islam@telkomsa.net) Background: The management of cervicomediastinal vascular trauma is challenging. We report on our experience with the condition in a newly established vascular trauma service unit, and compare the outcomes to those reported in our parent vascular surgery department. Method: The details of patients with cervicomediastinal vascular injuries from January 2012 to June 2014 were retrieved for analysis from a prospective database. Results: Ninety-three patients were identified, 84 of whom were male (90%), with an average age of 29 years. Most were penetrating injuries (89%), and 87% of these were due to stab wounds. There were 107 vascular injuries, 88 cervical and 19 mediastinal. Of these, 87 were arterial and 20 venous injuries. The most common arterial injury involved the subclavian artery (24%), followed by the common carotid artery (22%). Management was multimodal, and included conservative (8%), stenting and embolisation (8%), referral to a higher centre (8%), vascular repair (64%) and ligation (12%). Nineteen per cent required median sternotomy or thoracotomy. Eight patients died postoperatively (9%). Seven of them presented in extremis and died within 24 hours, and one died after a week from associated abdominal injuries. Postoperative complications were 9%. There was no incidence of a stroke or limb loss despite ligation of the arteries, including ligation of four internal carotids. Conclusion: The development of endovascular techniques would allow for noninvasive management of a significant number of patients. Open surgery is still necessary, and associated with significant morbidity. Comparable results were reported in our newly established vascular trauma service unit to those obtained in our parent vascular surgery department in Durban. S Afr J Surg 2016;54(2) Cervicomediastinal vascular injuries may be caused by blunt or penetrating trauma, and collectively constitute 5 10% of all reported cases of vascular trauma. 1,2 The operative management of cervicomediastinal vascular trauma is challenging as surgical access is difficult, and loss of control can result in rapid exsanguination. High morbidity and the mortality rates, ranging from 14 25%, have been cited in both South African and international reports. 3 7 Blunt thoracic aortic injury is immediately fatal in 80 90% of cases, and if untreated, survivors have a dismal prognosis. Thirty per cent die within six hours, 40 50% within 24 hours and 90% within four months, while overall operative mortality is approximately 28%, with a systemic complication rate of 50%. 8,9 Penetrating thoracic aortic trauma is highly lethal, and the mortality rate can be as high as 80%. 10 New techniques have been introduced over the last two decades with the rapid development of endovascular surgery, and offer potential solutions to complex injuries while avoiding the risk of open surgery. 11 This makes decisionmaking more nuanced and complex. Our parent vascular surgery department in Durban pioneered the concept of a dedicated metropolitan vascular trauma service over three decades ago in response to the complex nature of these injuries and their relative rarity. 12,13 The spectrum and outcomes of cervicomediastinal vascular trauma in our newly established vascular trauma team are reviewed in this report, and a comparison made with those in Durban, while attempting to contextualise the new and emerging endovascular and imaging techniques with a more established approach. VOL. 54 NO. 2 JUNE 2016 SAJS 15
2 Setting The Pietermaritzburg Metropolitan Hospitals Complex consists of three hospitals. The Pietermaritzburg Metropolitan Trauma Service was initiated in 2006, and the aim is the delivery of trauma care across hospitals in Pietermaritzburg. The vascular surgery unit was initiated in January 2013, with a single full-time certified vascular surgeon. Vascular trauma management had been left up to individual surgeons prior to the development of these two services. Currently, vascular trauma cases are exclusively co-managed by the trauma and vascular surgery units. The unit functions in a closed fashion, and there is a separate vascular trauma roster to ensure that vascular trauma cases are exclusively managed by a dedicated core of vascular trauma surgeons. Method The details of patients with cervicomediastinal vascular injuries from January 2012 to June 2014 were retrieved for analysis from a prospectively maintained database. Cervicomediastinal vascular injuries are defined as arterial or venous injuries of the neck [carotids, subclavian (including its branches) and the proximal axillary artery], and mediastinum [ascending aorta, aortic arch (including its branches), descending aorta, the pulmonary artery and veins]. Injuries to the first part of the axillary artery were included because surgical exposure is often similar to that for the third part of the subclavian artery, and it can be difficult to distinguish between them anatomically. A supraclavicular and/or infraclavicular incision is used for subclavian and axillary artery injuries. An attempt is not made to divide the clavicle as clavicular division is associated with significant postoperative morbidity. If required, the incision can be extended up into the neck along the anterior border of the sternocleidomastoid muscle, or downwards into the chest in the form of a median sternotomy. We do not make use of lateral thoracotomy for exposure of the neck vessels. This paper was written in full compliance with ethical standards. Pietermaritzburg Metropolitan Trauma Service personnel maintain a prospective digital trauma registry. The data from this registry were interrogated retrospectively. Ethics approval to maintain this registry was obtained from the Biomedical Research Ethics Committee (Ethics Number BE207/09 and BCA221/13) of the University of KwaZulu- Natal, Durban, South Africa; and from the Research Unit of the Department of Health (HRKM 265/13), KwaZulu-Natal, South Africa. Results Ninety-three patients with cervicomediastinal vascular injuries were identified over the 30-month period, 84 of whom were male (90%), with an average age of 29 years (a range of years). The overall Injury Severity Score at presentation was 17 (a range of 4 75). The mechanisms of injury were mostly penetrating wounds (83); among them stab (72) and gunshot wounds (11), and the rest were blunt trauma (7) and iatrogenic injuries (3). Seventy-four of the patients presented within 24 hours of the injury (80%), 16 within 72 hours (17%), two after one month (2%), while one patient presented five years after the initial injury (1%). Investigations Preoperative computed tomography (CT) angiography was performed for 65 patients (70%). Injuries Table 1: Anatomical distribution of arterial injury Arterial injuries n Cervical arteries Common carotid 19 Internal carotid 8 External carotid 3 Subclavian 21 Axillary 13 Vertebral 4 Internal mammary 1 Costocervical 1 Dorsal scapular 1 Mediastinal arteries Ascending and arch of aorta 5 Descending aorta 7 Innominate artery 3 Pulmonary artery 1 Total 87 There were 107 vascular injuries in 93 patients. Fourteen patients had received combined arterial and venous injuries, and six isolated venous injuries. There were 74 cervical (80%) and 19 mediastinal injuries (20%). The anatomical distribution of arterial injury is shown in Table 1. Most of the patients who had experienced blunt trauma were involved in a motor vehicle collision (5) and sustained descending aortic injuries and blunt carotid injuries (2). Three patients presented with iatrogenic injuries, i.e. common carotid artery injury (1) from the insertion of a central venous line; subclavian artery injury (1), also from the insertion of a central venous line and a subclavian artery injury (1) from internal fixation of the fractured clavicle. The injuries according to body region were 88 cervical (71 arterial and 17 venous), and 19 mediastinal (16 arterial and 3 venous) vascular injuries. The anatomical distribution of venous injuries is listed in Table 2. The most common arterial injury was to the subclavian artery (24%), followed by the common carotid artery (22%). Of the venous injuries, internal jugular and axillary vein injuries comprised the highest number (6%), followed by subclavian vein injuries (5%). The most common associated injury was haemothorax 16 SAJS VOL. 54 NO. 2 JUNE 2016
3 or pneumothorax in 32 patients (34%), followed by brachial plexus injury in 15 (16%). The other associated injuries were cardiac injury (4), head injury (4), maxilla/mandible fracture (4), rib fracture (3), oesophageal injury (2), tracheal injury (2) and clavicle fracture (2). artery (1) and dorsal scapular artery (1). Seven patients (8%) were treated expectantly; vertebral artery (2), internal carotid artery (2) and descending aortic (3) injuries. Table 2: The anatomical distribution of venous injury Venous injuries n Cervical veins Internal jugular 6 Subclavian 5 Axillary 6 Mediastinal veins Pulmonary 2 Superior vena cava 1 Total 20 Figure 1 a: Left subclavian artery pseudoaneurysm before stenting Management Fifty-six (64%) of the arterial injuries were managed by operative repair. Median sternotomy or thoracotomy was required in 18 patients (19%); 12 for mediastinal vascular injuries and six for cervical vascular injuries. Arterial exploration was undertaken in 66 patients (76%); 56 were repaired (64%) and 10 were ligated (12%). The most common arterial repairs were to the common carotid (18%) and subclavian (18%) artery, followed by the axillary artery (15%). The other arterial repairs were internal carotid (2), ascending and arch of aorta (3), descending aorta (2), innominate artery (3) and pulmonary artery (1). Primary repair was performed for all carotid and aortic injuries. Fourteen subclavian and axillary arteries underwent primary repair (48%), and 15 were repaired with interposition vein grafts (52%). Arterial ligation was performed in external carotid (3), internal carotid (4), vertebral (2) and internal mammary arteries (1). A subclavian artery injury was repaired as part of a hybrid procedure (combined endovascular and open), in which median sternotomy was avoided. Proximal subclavian artery control was obtained by an endovascularly placed temporary balloon occlusion. The artery was then approached via a supraclavicular incision and repaired. Five arterial injuries (6%) were treated with endovascular stent grafts. These included the proximal common carotid (2), the first part of the subclavian artery (1) and the second part of the subclavian artery (2). A single patient presented five years after the initial injury with a false aneurysm, and in another patient the stent graft was inserted as a bail out procedure to avoid open surgery due to lack of blood in the blood bank. Subclavian and carotid artery stenting is shown in Figure 1 a and b, and Figure 2 a and b, respectively. One of the subclavian artery stent grafts was converted to open repair after three days due to an endoleak. Two patients (2%) were treated endovascularly with coil embolisation; costocervical Figure 1 b: Left subclavian artery pseudoaneurysm after stenting Figure 2 a: Left common carotid artery pseudoaneurysm before stenting VOL. 54 NO. 2 JUNE 2016 SAJS 17
4 Figure 2 b: Left common carotid artery pseudoaneurysm after stenting Seven patients (8%) were referred to the quaternary centre at Inkosi Albert Luthuli Central Hospital, Durban. The disciplines to which the patients were referred were cardiothoracic surgery (2) and vascular surgery (5). Aortic arch injuries (2) were repaired operatively with cardiopulmonary bypass, descending aortic injuries (2) were treated by stent graft, and common carotid (1) and subclavian artery injuries (2) were treated by open repair at the quaternary centre. Of the 20 venous injuries that were managed operatively, 5 were ligated (25%) and 15 were repaired (75%) by simple lateral suture. Ligated veins included the subclavian (2) and axillary veins (3). Thrombosed vertebral arteries (2) and internal carotid arteries (2), and type I descending aortic injuries (3) were managed conservatively. Postoperative complications were seen in 8 patients (9%); i.e. wound sepsis (2), graft thrombosis (1), graft sepsis (1), mediastinitis (1), missed injury (2) and endoleak (1). Wound sepsis and mediastinitis were treated with antibiotics with full recovery. One thrombosed graft was treated conservatively and the septic graft removed without any further complications. There was no incidence of a stroke or limb loss, despite ligation of the arteries. Eight patients died postoperatively (9%). Seven of the patients who died presented in extremis and died within 24 hours post surgery. One patient died after a week from associated abdominal injuries. Discussion As is typical in most trauma series, the patients in our series were young and 90% of them were male. 2,14 Eighty-nine per cent of them presented with penetrating injuries, and 87% of these were due to stab wounds. This is in keeping with the literature from South Africa over the last four decades, and reflects the high rate of interpersonal violence in the country. 14,15 As expected, cervical vascular injuries were more common than mediastinal vascular injuries (80% versus 20%). Arterial injuries were more common than venous injuries (81% versus 19%), and this is reflective of the fact that many venous injuries thrombosed and stopped bleeding with simple measures, such as the application of direct pressure. Patients who presented with active bleeding or haemodynamic instability were expedited to the operating room and were not investigated further. Although a policy of selective investigation of trauma patients is followed, the widespread availability of CT angiography has resulted in increased reliance on imaging. Over 90% of all injuries were managed operatively either by open or endovascular procedures, and nearly a third of these open procedures required formal median sternotomy or thoracotomy in order for proximal control to be achieved. These are daunting injuries, and most patients presented acutely and required urgent exploration in less than optimal conditions. Appropriate decision-making in this cohort is important, and the results testify to the fact that a closed system results in very good outcomes for such patients. The fact that seven of the eight patients who demised presented in an agonal state is testament to this. Six of them had an associated venous or cardiac injury, and four of them required median sternotomy. Seven of the patients who died were managed before the inception of the vascular trauma surgery unit. Only one patient died postoperatively due to associated abdominal injuries after the inception of the vascular surgery unit. The endovascular treatment of traumatic subclavian and axillary artery injuries continues to evolve. 16 Du Toit et al. 11,17 recommend that the endovascular management of penetrating carotid artery injuries is safe, and that endovascular repair should be considered the first choice of treatment in stable patients with subclavian artery injuries. We continue to have concerns about the durability of a stent graft in a young patient, and in an area with considerable movement and strain, like the subclavian artery. However, there is no doubt that an endovascular approach avoids a difficult operative approach in this instance. We have used it selectively and will continue to follow-up our cohort as best we can, hoping to further define the role of this procedure. Endovascular stent grafts helped to avoid sternotomy in three patients. Currently, endovascular stenting has replaced open surgery for the management of blunt aortic injury. This approach is associated with significantly lower morbidity and mortality in comparison to open repair, although long-term follow-up data are only beginning to emerge now. 9,18 Angio-embolisation is well established in trauma, is an important weapon in the armamentarium, and is especially useful for the management of injuries to non-essential vessels. The ligation of non-essential arteries is a useful approach, and was applied liberally in our series. However, the ligation of the internal carotid artery is controversial, and can result in a stroke in up to 18% of patients, and mortality in up to 45%. 19 Four internal carotid arteries were ligated in our series, i.e. those that were thrombosed and had no back bleeding. There is a possibility that repairing the thrombosed internal carotid artery might cause haemorrhagic infarction. Neither a stroke 18 SAJS VOL. 54 NO. 2 JUNE 2016
5 nor mortality were associated with this. Adequate blood flow via the intact circle of Willis in young patients is the most likely explanation for the lack of strokes. Five patients were referred to the Durban vascular surgery department before the inception of the vascular surgery service at Pietermaritzburg. Other patients were not referred after that. The management principle of cervicomediastinal venous injuries differs to that for arterial injuries. Ligation is an acceptable form of treatment of cervicomediastinal venous injuries in the presence of haemodynamic instability, or where complex methods of repair would otherwise be necessary. 20 Despite the ligation of 25% of the venous injuries, there weren t any postoperative complications associated with it, and thus the ligation of complex venous injuries is advocated. Non-operative management strategies are applicable to less than a tenth of patients with cervicomediastinal vascular trauma. Thrombosed vertebral arteries may be safely observed, and our experience with this injury supports the literature on this topic. 21 Two internal carotid arteries were shown to be thrombosed following blunt neck trauma, and were treated expectantly. This also supports the literature on this topic. 22 Three descending aortic injuries (type I intimal tear injury) from blunt thoracic trauma were also managed expectantly, again in accordance with evidence in the literature. 23 The mortality rate of 9% in our series of complex injuries compares favourably with the rates reported from our parent unit over a decade and a half ago. The mortality rates for penetrating mediastinal arterial injuries, axillary and subclavian artery injuries and venous injuries were 17%, 12% and 16%, respectively, in their series. 20,24,25 This reflects improved access to endovascular therapy, and is a testament to the success of our own newly established vascular trauma service. Conclusion Cervicomediastinal vascular trauma is complex and challenging. A closed system of care, delivered by a select group of specialists with an interest in vascular trauma, results in very good outcomes for patients who require an operation. The development of endovascular techniques may allow for noninvasive management of a significant number of patients. This subset of patients needs to be managed by a competent vascular and endovascular surgeon. Open surgery is still necessary, and is associated with significant morbidity. Our newly established vascular trauma service is a model which produced comparable, if not better, results, to that of our already established unit. Declaration There was no funding for this study. Conflict of interest The authors declare that there was no conflict of interest which may have inappropriately influenced them when writing this article. REFERENCES 1. Du Toit DF, Strauss DC, Blaszczyk M, et al. Endovascular treatment of penetrating thoracic outlet arterial injuries. Eur J Vasc Endovasc Surg. 2000;19(5): Thoma M, Navsaria PH, Edu S, Nicol AJ. Analysis of 203 patients with penetrating neck injuries. World J Surg. 2008;32(12): Du Toit DF, Odendaal W, Lambrechts A, Warren BL. Surgical and endovascular management of penetrating innominate artery injuries. Eur J Vasc Endovasc Surg. 2008;36(1): George SM Jr, Croce MA, Fabian TC, et al. Cervicothoracic arterial injuries: recommendations for diagnosis and management. World J Surg. 1991;15(1): Demetriades D, Skalkides J, Sofianos C, et al. Carotid artery injuries: experience with 124 cases. J Trauma. 1989;29(1): Johnston RH Jr, Wall MJ Jr, Mattox KL. Innominate artery trauma: a thirty-year experience. J Vasc Surg. 1993;17(1): Navsaria P, Omoshoro-Jones J, Nicol A. An analysis of 32 surgically managed penetrating carotid artery injuries. Eur J Vasc Endovasc Surg. 2002;24(4): Jamieson WRE, Janusz MT, Gudas VM, et al. Traumatic rupture of the thoracic aorta: third decade of experience. Am J Surg. 2002;183(5): Demetriades D, Velmahos GC, Scalea TM, et al. Operative repair or endovascular stent graft in blunt traumatic thoracic aortic injuries: results of an American Association for the Surgery of Trauma Multicenter Study. J Trauma. 2008;64(3): Demetriades D, Theodorou D, Murray J, et al. Mortality and prognostic factors in penetrating injuries of the aorta. J Trauma. 1996;40(5): Du Toit DF, Coolen D, Lambrechts A, et al. The endovascular management of penetrating carotid artery injuries: long-term follow-up. Eur J Vasc Endovasc Surg. 2009;38(3): Campbell FC, Robbs JV. Penetrating injuries of the neck: a prospective study of 108 patients. Br J Surg. 1980;67(8): Robbs JV, Baker LW, Human RR, et al. Cervicomediastinal arterial injuries: a surgical challenge. Arch Surg. 1981;116(5): Clarke DL, Quazi MA, Reddy K, Thomson SR. Emergency operation for penetrating thoracic trauma in a metropolitan surgical service in South Africa. J Thorac Cardiovasc Surg. 2011;142(3): Sobnach S, Nicol AJ, Nathire H, et al. An analysis of 50 surgically managed penetrating subclavian artery injuries. Eur J Vasc Endovasc Surg. 2010;39(2): Dubose JJ, Rajani R, Gilani R, et al. Endovascular management of axillo-subclavian arterial injury: a review of published experience. Injury. 2012;43(11): Du Toit DF, Lambrechts AV, Stark H, Warren BL. Long-term results of stent graft treatment of subclavian artery injuries: management of choice for stable patients. J Vasc Surg. 2008;47(4): Demetriades D, Velmahos GC, Scalea TM, et al. Diagnosis and treatment of blunt thoracic aortic injuries: changing VOL. 54 NO. 2 JUNE 2016 SAJS 19
6 perspectives. J Trauma. 2008;64(6): Du Toit DF, Van Schalkwyk GD, Wadee SA, Warren BL. Neurological outcome after penetrating extracranial arterial trauma. J Vasc Surg. 2003;38(2): Nair R, Robbs JV, Muckart DJ. Management of penetrating cervicomediastinal venous trauma. Eur J Vasc Endovasc Surg. 2000;19(1): Mwipatayi BP, Jeffery P, Beningfield SJ, et al. Management of extra-cranial vertebral artery injuries. Eur J Vasc Endovasc Surg. 2004;27(2): Biffl WL, Moore EE, Offner PJ, et al. Blunt carotid arterial injuries: implications of a new grading scale. J Trauma. 1999;47(5): Starnes BW, Lundgren RS, Gunn M, et al. A new classification scheme for treating blunt aortic injury. J Vasc Surg. 2012;55(1): Buchan K, Robbs JV. Surgical management of penetrating mediastinal arterial trauma. Eur J Cardiothorac Surg. 1995;9(2): McKinley AG, Carrim ATO, Robbs JV. Management of proximal axillary and subclavian artery injuries. BJS. 2000;87(1): SAJS VOL. 54 NO. 2 JUNE 2016
Bilateral blunt carotid artery injury: A case report and review of the literature
 CASE REPORT Bilateral blunt carotid artery injury: A case report and review of the literature S Cheddie, 1 MMed (Surg), FCS (SA); B Pillay, 2 FCS (SA), Cert Vascular Surgery; R Goga, 2 FCS (SA) 1 Department
CASE REPORT Bilateral blunt carotid artery injury: A case report and review of the literature S Cheddie, 1 MMed (Surg), FCS (SA); B Pillay, 2 FCS (SA), Cert Vascular Surgery; R Goga, 2 FCS (SA) 1 Department
Management of Penetrating Cervicomediastinal Venous Trauma
 Eur J Vasc Endovasc Surg 19, 65 69 (2000) doi:10.1053/ejvs.1999.0965, available online at http://www.idealibrary.com on Management of Penetrating Cervicomediastinal Venous Trauma R. Nair, J. V. Robbs and
Eur J Vasc Endovasc Surg 19, 65 69 (2000) doi:10.1053/ejvs.1999.0965, available online at http://www.idealibrary.com on Management of Penetrating Cervicomediastinal Venous Trauma R. Nair, J. V. Robbs and
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Endovascular treatment of carotid-jugular fistula after gunshot wound
 Endovascular treatment of carotid-jugular fistula after gunshot wound Instituto Dante Pazzanese de Cardiologia São Paulo, Brazil Carrijo, LBS; Tannus, MM; Cano, MN; Izukawa, NM; Moreira, SM; Kambara, AM
Endovascular treatment of carotid-jugular fistula after gunshot wound Instituto Dante Pazzanese de Cardiologia São Paulo, Brazil Carrijo, LBS; Tannus, MM; Cano, MN; Izukawa, NM; Moreira, SM; Kambara, AM
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1
 Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Haemodynamically unstable patient with chest trauma
 HR J Clinical Case - Test Yourself Interventional Haemodynamically unstable patient with chest trauma Dimitrios Tomais, Theodoros Kratimenos, Dimosthenis Farsaris Interventional Radiology Unit, Radiology
HR J Clinical Case - Test Yourself Interventional Haemodynamically unstable patient with chest trauma Dimitrios Tomais, Theodoros Kratimenos, Dimosthenis Farsaris Interventional Radiology Unit, Radiology
Subclavian and Axillary Artery Aneurysms
 Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die
 account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
account for 10% to 15% of all traffic fatalities majority fatal at the scene 50% who survive the initial injury die in the first 24 hours 90% die within the first month if aorta not repaired 30-90% overall
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND
 Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
Stent graft repair of subclavian and axillary vascular injuries: The Groote Schuur experience
 VASCULAR SURGERY Stent graft repair of subclavian and axillary vascular injuries: The Groote Schuur experience N G Naidoo, 1,2 MB ChB, FCS (SA); P Navsaria, 1,3 MB ChB, FCS (SA); S J Beningfield, 4 MB
VASCULAR SURGERY Stent graft repair of subclavian and axillary vascular injuries: The Groote Schuur experience N G Naidoo, 1,2 MB ChB, FCS (SA); P Navsaria, 1,3 MB ChB, FCS (SA); S J Beningfield, 4 MB
Experience of endovascular procedures on abdominal and thoracic aorta in CA region
 Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Experience of endovascular procedures on abdominal and thoracic aorta in CA region May 14-15, 2015, Dubai Dr. Viktor Zemlyanskiy National Research Center of Emergency Care Astana, Kazakhstan Region Characteristics
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/39153 holds various files of this Leiden University dissertation. Author: Hommes, M. Title: The injured liver : management and hepatic injuries in the traumapatient
Cover Page The handle http://hdl.handle.net/1887/39153 holds various files of this Leiden University dissertation. Author: Hommes, M. Title: The injured liver : management and hepatic injuries in the traumapatient
Advances in Treatment of Traumatic Aortic Transection
 Advances in Treatment of Traumatic Aortic Transection Himanshu J. Patel MD University of Michigan Medical Center Author Disclosures Consulting fees from WL Gore Inc. There is no disease more conducive
Advances in Treatment of Traumatic Aortic Transection Himanshu J. Patel MD University of Michigan Medical Center Author Disclosures Consulting fees from WL Gore Inc. There is no disease more conducive
Innominate artery trauma: A thirty-year experience
 Innominate artery trauma: A thirty-year experience Robert H. Johnston, Jr., MD, Matthew J. Wall, Jr., MD, and Kenneth L. Mattox, MD, Houston, Texas Purpose: Injury to the innominate artery may represent
Innominate artery trauma: A thirty-year experience Robert H. Johnston, Jr., MD, Matthew J. Wall, Jr., MD, and Kenneth L. Mattox, MD, Houston, Texas Purpose: Injury to the innominate artery may represent
Management of Acute Aortic Syndromes. M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria
 Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Management of Acute Aortic Syndromes M. Grabenwoger, MD Dept. of Cardiovascular Surgery Hospital Hietzing, Vienna, Austria I have nothing to disclose. Acute Aortic Syndromes Acute Aortic Dissection Type
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury. Conflict of Interest. Hypotensive shock 5/5/2014. none
 EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
EVAR and TEVAR: Extending Their Use for Rupture and Traumatic Injury Bruce H. Gray, DO MSVM FSCAI Professor of Surgery/Vascular Medicine USC SOM-Greenville Greenville, South Carolina none Conflict of Interest
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
TEVAR FOR! THORACIC AORTIC TRAUMA"
 10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
RESUSCITATION IN TRAUMA. Important things I have learnt
 RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN
 CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
2 Aortic Arch Debranching UCSF Vascular Symposium /14/16. J Endovasc Ther 2002;9:suppl 2; II98 105
 How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
Transluminal Stent-graft Placement endovascular surgery
 13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
13 545 551 2004 Transluminal Stent-graft Placement endovascular surgery 1 1 2 2 1 1 1 3 2 1 1996 11Transluminal Stent-graft Placement TSGP 6 82 TSGP T42 O TSGP Th10 T 26 O 5 T 3 O 23T 6 O 2 T 47 A15B17B15O
Vertebral Artery Pseudoaneurysm
 Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011
 Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Follow-up of Aortic Dissection: How, How Often, Which Consequences Euro Echo 2011 Susan E. Wiegers, MD, FASE Director of Clinical Echocardiography Hospital of the University of Pennsylvania Disclosure
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Endovascular Trauma Management. Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden
 Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Vascular Surgery AMPUTATION AORTA
 SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
Diagnosis & Management of Kidney Trauma. LAU - Urology Residency Program LOP Urology Residents Meeting
 Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
EAST MULTICENTER STUDY DATA DICTIONARY. Temporary Intravascular Shunt Study Data Dictionary
 EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
Screening and Management of Blunt Cereberovascular Injuries (BCVI)
 Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Development of a Branched LSA Endograft & Ascending Aorta Endograft
 Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
Development of a Branched LSA Endograft & Ascending Aorta Endograft Frank R. Arko III, MD Sanger Heart & Vascular Institute Carolinas Medical Center Charlotte, North Carolina, USA Disclosures Proximal
University of Florida Department of Surgery. CardioThoracic Surgery VA Learning Objectives
 University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
University of Florida Department of Surgery CardioThoracic Surgery VA Learning Objectives This service performs coronary revascularization, valve replacement and lung cancer resections. There are 2 faculty
Santi Trimarchi, MD, PhD Vascular Surgeon Thoracic Aortic Research Center, Director IRCCS Policlinico San Donato University of Milan
 The Gore GREAT Registry: Update about a real life data collection Santi Trimarchi, MD, PhD Vascular Surgeon Thoracic Aortic Research Center, Director IRCCS Policlinico San Donato University of Milan Disclosures
The Gore GREAT Registry: Update about a real life data collection Santi Trimarchi, MD, PhD Vascular Surgeon Thoracic Aortic Research Center, Director IRCCS Policlinico San Donato University of Milan Disclosures
Animesh Rathore, MD 4/22/17. The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management
 Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
Animesh Rathore, MD 4/22/17 The Great Debate 45yo Man With Uncomplicated Acute TBAD: The Case For Medical Management Disclosures Just a young vascular surgeon who would like to keep his job My opponent
Delayed Surgical Management of Traumatic Pseudoaneurysm of the Ascending Aorta in Multiple Trauma
 CASE REPORT J Trauma Inj 2018;31(1):29-33 http://doi.org/10.20408/jti.2018.31.1.29 JOURNAL OF TRAUMA AND INJURY Delayed Surgical Management of Traumatic Pseudoaneurysm of the Ascending Aorta in Multiple
CASE REPORT J Trauma Inj 2018;31(1):29-33 http://doi.org/10.20408/jti.2018.31.1.29 JOURNAL OF TRAUMA AND INJURY Delayed Surgical Management of Traumatic Pseudoaneurysm of the Ascending Aorta in Multiple
DISCLOSURES ISOLATED DTA LESION? TYPE B DISSECTIONS TREATMENT OPTIONS
 Endovascular Repair of Aortic Arch Pathologies; What is available/possible in the U.S. in 2018? Kaiser Permanente Endovascular Symposium 6/2/18 Sukgu M Han, MD, MS Assistant Professor of Clinical Surgery
Endovascular Repair of Aortic Arch Pathologies; What is available/possible in the U.S. in 2018? Kaiser Permanente Endovascular Symposium 6/2/18 Sukgu M Han, MD, MS Assistant Professor of Clinical Surgery
SELECTIVE ANTEGRADE TECHNIQUE OF CHOICE
 SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Contemporary management of brachiocephalic occlusive disease. TM Sullivan Minneapolis, MN
 Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Contemporary management of brachiocephalic occlusive disease TM Sullivan Minneapolis, MN WL Gore & Associates Disclosures Meeting organizer (SOAR) CR Bard Chair, CEC Bolster trial Veryan National PI, MIMICS
Endovascular repair of inadvertent subclavian artery injury during attempted internal jugular vein catheterization: A case report
 ISPUB.COM The Internet Journal of Endovascular Medicine Volume 1 Number 2 Endovascular repair of inadvertent subclavian artery injury during attempted internal jugular vein catheterization: A case report
ISPUB.COM The Internet Journal of Endovascular Medicine Volume 1 Number 2 Endovascular repair of inadvertent subclavian artery injury during attempted internal jugular vein catheterization: A case report
THE VESSELS OF BLOOD CIRCULATION
 THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
Schedule of Benefits. for Professional Fees Vascular Procedures
 Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
Schedule of Benefits for Professional Fees 2018 Vascular Procedures ANASTOMOSIS RULES 820 Arteriovenous anastomosis in arm 1453 Arteriovenous anastomosis, open by basilic vein transposition 1465 Splenorenal
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D.
 CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
CT of Acute Thoracic Aortic Syndromes Stuart S. Sagel, M.D. Thoracic Aortic Aneurysms Atherosclerotic Dissection Penetrating ulcer Mycotic Inflammatory (vasculitis) Traumatic Aortic Imaging Options Catheter
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA)
 The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
The Management and Treatment of Ruptured Abdominal Aortic Aneurysm (RAAA) Disclosure Speaker name: Ren Wei, Li Zhui, Li Fenghe, Zhao Yu Department of Vascular Surgery, The First Affiliated Hospital of
Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta
 02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
02-33000-29 Original Effective Date: 04/15/03 Reviewed: 07/26/18 Revised: 08/15/18 Subject: Endovascular Stent Grafts for Disorders of the Thoracic Aorta THIS MEDICAL COVERAGE GUIDELINE IS NOT AN AUTHORIZATION,
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui
 Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Endovascular Management of Thoracic Aortic Pathology Stéphan Haulon, J Sobocinski, B Maurel, T Martin-Gonzalez, R Spear, A Hertault, R Azzaoui Aortic Center, Lille University Hospital, France Disclosures
Open fenestration for complicated acute aortic B dissection
 Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Art of Operative Techniques Open fenestration for complicated acute aortic B dissection Santi Trimarchi 1, Sara Segreti 1, Viviana Grassi 1, Chiara Lomazzi 1, Marta Cova 1, Gabriele Piffaretti 2, Vincenzo
Review of Surgical Treatment of Popliteal Artery Injury: Outcomes of Open vs Endovascular Repair
 Review of Surgical Treatment of Popliteal Artery Injury: Outcomes of Open vs Endovascular Repair Tze-Woei Tan, MD; Francesca D. Armstrong, MD; Wayne W. Zhang, MD From Louisiana State University Health,
Review of Surgical Treatment of Popliteal Artery Injury: Outcomes of Open vs Endovascular Repair Tze-Woei Tan, MD; Francesca D. Armstrong, MD; Wayne W. Zhang, MD From Louisiana State University Health,
Recommendations for Follow-up After Vascular Surgery Arterial Procedures SVS Practice Guidelines
 Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Recommendations for Follow-up After Vascular Surgery Arterial Procedures 2018 SVS Practice Guidelines vsweb.org/svsguidelines About the guidelines Published in the July 2018 issue of Journal of Vascular
Ascending Aorta: Is The Endovascular Approach Realistic?
 Ascending Aorta: Is The Endovascular Approach Realistic? Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosures Research-grants, travelling, proctoring speaking-fees,
Ascending Aorta: Is The Endovascular Approach Realistic? Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Disclosures Research-grants, travelling, proctoring speaking-fees,
SAMPLE EDITION PELVIC AND LOWER EXTREMITY ARTERIES WITH ENDOVASCULAR REVASCULARIZATION. Cardiovascular Illustrations and Guidelines
 Cardiovascular Illustrations and Guidelines PELVIC AND LOWER EXTREMITY ARTERIES WITH ENDOVASCULAR REVASCULARIZATION ANGIOPLASTY INTRAVASCULAR STENT PLACEMENT ATHERECTOMY For Fem-Pop Territory Angioplasty
Cardiovascular Illustrations and Guidelines PELVIC AND LOWER EXTREMITY ARTERIES WITH ENDOVASCULAR REVASCULARIZATION ANGIOPLASTY INTRAVASCULAR STENT PLACEMENT ATHERECTOMY For Fem-Pop Territory Angioplasty
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury
 TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud
 How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
How to achieve a successful proximal sealing in TEVAR? Pr L Canaud CHU de Montpellier France Disclosure I have the following potential conflicts of interest to report: Consulting: Medtronic. Proximal neck
SANGER HEART & VASCULAR INSTITUTE
 VASCULAR SURGERY & MEDICINE PROGRAM GUIDE SANGER HEART & VASCULAR INSTITUTE Vascular Surgery & Medicine Program Guide About Us...1 Vascular Surgery & Medicine...3 Comprehensive Aortic Disease Management...5
VASCULAR SURGERY & MEDICINE PROGRAM GUIDE SANGER HEART & VASCULAR INSTITUTE Vascular Surgery & Medicine Program Guide About Us...1 Vascular Surgery & Medicine...3 Comprehensive Aortic Disease Management...5
6. Endovascular aneurysm repair
 Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Introduction The standard treatment for aortic aneurysm, open repair, involves a large abdominal incision and cross-clamping of the aorta. In recent years, a minimally invasive technique, endovascular
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Surgical Privileges Form: Vascular Surgery
 Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome
 Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
Case Report 1 Dissection of descending aorta treated by stent-graft implantation in a patient with Marfan syndrome Marat. ripov, Ildar Z. bdyldaev, Semen D. Chevgun, ektur S. Daniyarov, Dinara. Toktosunova,
Visceral aneurysm. Diagnosis and Interventions M.NEDEVSKA
 Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
Visceral aneurysm Diagnosis and Interventions M.NEDEVSKA History 1953 De Bakeyand Cooley Visceral aneurysm VAAs rare, reported incidence of 0.01 to 0.2% on routine autopsies. Clinically important Potentially
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
Blunt Partial Transection of the Innominate Artery
 Blunt Partial Transection of the Innominate Artery: Anomalous Origin of the Left Carotid Artery and Off-Pump Repair Brett E. Grizzell, M.D. 1, Gie Na Yu, M.D. 1, Phillip F. Bongiorno, M.D. 1,2, James M.
Blunt Partial Transection of the Innominate Artery: Anomalous Origin of the Left Carotid Artery and Off-Pump Repair Brett E. Grizzell, M.D. 1, Gie Na Yu, M.D. 1, Phillip F. Bongiorno, M.D. 1,2, James M.
Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally
 Volume 2 Issue 3 Article 3 2016 Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally Farzad Amiri, MD; Zachary Sanford; and Constantinous Constantinou, MD Follow
Volume 2 Issue 3 Article 3 2016 Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally Farzad Amiri, MD; Zachary Sanford; and Constantinous Constantinou, MD Follow
Accepted Manuscript. Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi
 Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
Accepted Manuscript Is A More Extensive Operation Justified for Acute Type A Dissection Repair? Dr. Leonard N. Girardi PII: S0022-5223(18)32552-2 DOI: 10.1016/j.jtcvs.2018.09.048 Reference: YMTC 13502
Primary to non-coronary IVUS
 codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
codes 2018 2018 codes Primary to non-coronary IVUS Page 2 All coding, coverage, billing and payment information provided herein by Philips is gathered from third-party sources and is subject to change.
An unusual shoulder injury
 An unusual shoulder injury Authors: AJ Moss, D Valenti, SC Fraser, J Murie Location: Queen Elizabeth Hospital, Norfolk, UK Citation: Moss AJ, Valenti D, Fraser S, Murie J. An unusual shoulder injury. 2011.
An unusual shoulder injury Authors: AJ Moss, D Valenti, SC Fraser, J Murie Location: Queen Elizabeth Hospital, Norfolk, UK Citation: Moss AJ, Valenti D, Fraser S, Murie J. An unusual shoulder injury. 2011.
Thoracic endovascular aortic repair (TEVAR) is
 Expanding the Landing Zone for TEVAR A discussion of the longevity and durability of commonly used extrathoracic debranching techniques. BY DANIEL K. HAN, MD, RPVI; CHRISTINE JOKISCH, BS; AND JAMES F.
Expanding the Landing Zone for TEVAR A discussion of the longevity and durability of commonly used extrathoracic debranching techniques. BY DANIEL K. HAN, MD, RPVI; CHRISTINE JOKISCH, BS; AND JAMES F.
Hybrid procedure to treat aortic arch aneurysm combined with aortic arch coarctation and left internal carotid artery aneurysm (Case Report)
 Zhou et al. Journal of Cardiothoracic Surgery 2014, 9:3 CASE REPORT Open Access Hybrid procedure to treat aortic arch aneurysm combined with aortic arch coarctation and left internal carotid artery aneurysm
Zhou et al. Journal of Cardiothoracic Surgery 2014, 9:3 CASE REPORT Open Access Hybrid procedure to treat aortic arch aneurysm combined with aortic arch coarctation and left internal carotid artery aneurysm
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
An urban trauma centre experience with abdominal vena cava injuries
 TRAUMA SURGERY An urban trauma centre experience with abdominal vena cava injuries M Hampton, 1,2 D Bew, 1,2 S Edu, 1,2 A Nicol, 1,2 N Naidoo, 1,2 P Navsaria 1,2 1 Trauma Centre and Vascular Surgery Unit,
TRAUMA SURGERY An urban trauma centre experience with abdominal vena cava injuries M Hampton, 1,2 D Bew, 1,2 S Edu, 1,2 A Nicol, 1,2 N Naidoo, 1,2 P Navsaria 1,2 1 Trauma Centre and Vascular Surgery Unit,
DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region.
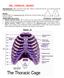 1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
1 THE THORACIC REGION DESCRIPTION: This is the part of the trunk, which is located between the root of the neck and the superior border of the abdominal region. SHAPE : T It has the shape of a truncated
Indications for stent grafts in type B aortic dissection
 expert opinion I Akin C A Nienaber Indications for stent grafts in type B aortic dissection ibrahim akin christoph a nienaber Department of Medicine, Divisions of Cardiology, Pulmology and Intensive Care
expert opinion I Akin C A Nienaber Indications for stent grafts in type B aortic dissection ibrahim akin christoph a nienaber Department of Medicine, Divisions of Cardiology, Pulmology and Intensive Care
Case Report 1. CTA head. (c) Tele3D Advantage, LLC
 Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Case Report 1 CTA head 1 History 82 YEAR OLD woman with signs and symptoms of increased intra cranial pressure in setting of SAH. CT Brain was performed followed by CT Angiography of head. 2 CT brain Extensive
Physician s Vascular Interpretation Examination Content Outline
 Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Physician s Vascular Interpretation Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 6 Cerebrovascular Abdominal Peripheral Arterial - Duplex Imaging Peripheral Arterial
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 CPT CODING CHANGES
 17 2018 CPT coding changes by Samuel Smith, MD, FACS; Megan McNally, MD, FACS; and Jan Nagle, MS, RPh JAN 2018 BULLETIN American College of Surgeons 18 Significant changes in Current Procedural Terminology
17 2018 CPT coding changes by Samuel Smith, MD, FACS; Megan McNally, MD, FACS; and Jan Nagle, MS, RPh JAN 2018 BULLETIN American College of Surgeons 18 Significant changes in Current Procedural Terminology
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely
 Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
Percutaneous Axillary Artery Access For Branch Grafting for complex TAAAs and pararenal AAAs: How to do it safely Daniela Branzan, MD, Department of Vascular Surgery University Hospital Leipzig Disclosure
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies. Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018
 Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Intravascular Ultrasound in the Treatment of Complex Aortic Pathologies Naixin Kang, M.D. Vascular Surgery Fellow April 26 th, 2018 DISCLOSURES Nothing To Disclose 2 ENDOVASCULAR AORTIC INTERVENTION Improved
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic
 Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Free Esophageal Perforation Following Hybrid Visceral Debranching and Distal Endograft Extension to Repair a Ruptured Thoracoabdominal Aortic Aneurysm History A 56-year-old gentleman, who had been referred
Alternate Vascular Access for TAVR. Gian Paolo Ussia Campus Bio-medico University, Rome Italy
 Alternate Vascular Access for TAVR Gian Paolo Ussia Campus Bio-medico University, Rome Italy g.ussia@unicampus.it REQUIRED Gian Paolo Ussia I have no relevant financial relationships Transcatheter Valves
Alternate Vascular Access for TAVR Gian Paolo Ussia Campus Bio-medico University, Rome Italy g.ussia@unicampus.it REQUIRED Gian Paolo Ussia I have no relevant financial relationships Transcatheter Valves
PERPHERAL ARTERY ANEURYSM. By Pooja Sharma and Susanna Sebastianpillai
 PERPHERAL ARTERY ANEURYSM By Pooja Sharma and Susanna Sebastianpillai Defintions True Aneurysm Involves all three layers of the vessel. Have two basic shapes; Fusiform = symmetric widening of the vessels
PERPHERAL ARTERY ANEURYSM By Pooja Sharma and Susanna Sebastianpillai Defintions True Aneurysm Involves all three layers of the vessel. Have two basic shapes; Fusiform = symmetric widening of the vessels
Management of the vertebral artery during thoracic endovascular aortic repair with coverage of the left subclavian artery
 Original Article Management of the vertebral artery during thoracic endovascular aortic repair with coverage of the left subclavian artery Jian Zhu*, Er-Ping Xi*, Shui-Bo Zhu, Gui-Lin Yin, Rong-Ping Wang,
Original Article Management of the vertebral artery during thoracic endovascular aortic repair with coverage of the left subclavian artery Jian Zhu*, Er-Ping Xi*, Shui-Bo Zhu, Gui-Lin Yin, Rong-Ping Wang,
Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry
 University of Milan Thoracic Aortic Research Center Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry Santi Trimarchi, MD, PhD Associate
University of Milan Thoracic Aortic Research Center Performance of the conformable GORE TAG device in Type B aortic dissection from the GORE GREAT real world registry Santi Trimarchi, MD, PhD Associate
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Mediastinum It is a thick movable partition between the two pleural sacs & lungs. It contains all the structures which lie
 Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Dr Jamila EL medany OBJECTIVES At the end of the lecture, students should be able to: Define the Mediastinum. Differentiate between the divisions of the mediastinum. List the boundaries and contents of
Contemporary Management of Blunt Thoracic Aortic Injury: Results of an EAST, AAST and SVS Survey by the Aortic Trauma Foundation
 Original Article Vol. 1, No. 1; 2017; pp 4 8 DOI: 10.26676/jevtm.v1i1.8 Contemporary Management of Blunt Thoracic Aortic Injury: Results of an EAST, AAST and SVS Survey by the Aortic Trauma Foundation
Original Article Vol. 1, No. 1; 2017; pp 4 8 DOI: 10.26676/jevtm.v1i1.8 Contemporary Management of Blunt Thoracic Aortic Injury: Results of an EAST, AAST and SVS Survey by the Aortic Trauma Foundation
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm
 Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Aberrant Right Subclavian Artery Aneurysm
 Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Aberrant Right Subclavian Artery William S. Stoney, M.D., William C. Alford, Jr., M.D., George R. Burrus, M.D., and Clarence S. Thomas, Jr., M.D. ABSTRACT Ten patients with aneurysm of an aberrant right
Abdominal and thoracic aneurysm repair
 Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Abdominal and thoracic aneurysm repair William A. Gray MD Director, Endovascular Intervention Cardiovascular Research Foundation Columbia University Medical Center Abdominal Aortic Aneurysm Endografts
Ascending Aorta: The Endovascular Approach
 University Heart Center Hamburg GERMAN AORTIC CENTER Ascending Aorta: The Endovascular Approach Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Gold Standard for Ascending
University Heart Center Hamburg GERMAN AORTIC CENTER Ascending Aorta: The Endovascular Approach Tilo Kölbel, MD, PhD University Heart Center Hamburg University Hospital Eppendorf Gold Standard for Ascending
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST
 CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
CORONARY ARTERY BYPASS GRAFTING (CABG) (Part 1) Mark Shikhman, MD, Ph.D., CSA Andrea Scott, CST I have constructed this lecture based on publications by leading cardiothoracic American surgeons: Timothy
Penetrating abdominal trauma clinical view. Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland
 Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
How Did We Get To The? CT Scan Granularity & Development of TAVER. Multi & Single Center Reports Getting Us Closer to Answer
 How Did We Get To The? CT Scan Granularity & Development of TAVER Multi & Single Center Reports Getting Us Closer to Answer # Patients Dying That anyone survives complete transection of this artery is
How Did We Get To The? CT Scan Granularity & Development of TAVER Multi & Single Center Reports Getting Us Closer to Answer # Patients Dying That anyone survives complete transection of this artery is
Animesh Rathore, MD 4/21/17. Penetrating atherosclerotic ulcers of aorta
 Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
Animesh Rathore, MD 4/21/17 Penetrating atherosclerotic ulcers of aorta Disclosures No financial disclosures Thank You Dr. Panneton for giving this lecture for me. I am stuck at Norfolk with an emergency
WHAT IS THE BEST OPTION FOR ARCH ANEURYSMS?
 WHAT IS THE BEST OPTION FOR ARCH ANEURYSMS? Prof. Furuzan Numan M.D Chief of Interventional Radiology Department Cerrahpasa Medical Faculty & Memorial Hospital, ISTANBUL, TURKIYE 3ad INTERNATIONAL MEETING
WHAT IS THE BEST OPTION FOR ARCH ANEURYSMS? Prof. Furuzan Numan M.D Chief of Interventional Radiology Department Cerrahpasa Medical Faculty & Memorial Hospital, ISTANBUL, TURKIYE 3ad INTERNATIONAL MEETING
Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein
 Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein Ahmed Afifi, Ahmed ElGuindy, Mahmoud Farouk, Magdi H Yacoub* * m.yacoub@imperial.ac.uk DOI: http://dx.doi.org/10.5339/gcsp.2012.13 ISSN:
Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein Ahmed Afifi, Ahmed ElGuindy, Mahmoud Farouk, Magdi H Yacoub* * m.yacoub@imperial.ac.uk DOI: http://dx.doi.org/10.5339/gcsp.2012.13 ISSN:
Predictors of outcome in patients requiring surgery for liver trauma
 Injury, Int. J. Care Injured (2007) 38, 65 70 www.elsevier.com/locate/injury Predictors of outcome in patients requiring surgery for liver trauma W.L. Sikhondze, T.E. Madiba *, N.M. Naidoo, D.J.J. Muckart
Injury, Int. J. Care Injured (2007) 38, 65 70 www.elsevier.com/locate/injury Predictors of outcome in patients requiring surgery for liver trauma W.L. Sikhondze, T.E. Madiba *, N.M. Naidoo, D.J.J. Muckart
