Management of Penetrating Cervicomediastinal Venous Trauma
|
|
|
- Jasmin Bruce
- 5 years ago
- Views:
Transcription
1 Eur J Vasc Endovasc Surg 19, (2000) doi: /ejvs , available online at on Management of Penetrating Cervicomediastinal Venous Trauma R. Nair, J. V. Robbs and D. J. Muckart Metropolitan Vascular Service and Department of Surgery, University of Natal, Durban, South Africa Objectives: to evaluate the results of management of penetrating cervicomediastinal venous trauma. Design: retrospective study. Materials: forty-nine consecutive patients with cervical and thoracic venous injuries treated at a tertiary hospital between 1991 and Method: patients identified from a computerised database and data extracted from case records. Results: forty-five patients were male and the mean age was 25.3 years. Forty injuries were due to stabs and 9 to gunshots. 22 patients were shocked, 25 actively bleeding and 31 were anaemic. Veins injured were internal jugular in 25, subclavian in 15, brachiocephalic in 6, and superior vena cava in 3. Injured veins were ligated in 25 cases and repaired by lateral suture in 22. No complex repairs were performed. There were 8 perioperative deaths and 5 cases of transient postoperative oedema. Venous ligation was not associated with increased risk of postoperative oedema. Conclusions: ligation is an acceptable form of treatment of cervicomediastinal venous injuries in the presence of haemodynamic instability, or where complex methods of repair would otherwise be necessary. Key Words: Cervicomediastinal venous trauma; Penetrating; Ligation. Introduction Patients and Methods The management of penetrating cervicomediastinal Consecutive patients with documented cervical and arterial trauma has been extensively debated in the thoracic venous injuries, treated at the King Edward surgical literature, particularly the need for in- VIII Hospital, Durban, between January 1991 and vestigation and exploratory surgery. Although the December 1997, were identified by a search of a management of visceral, arterial, cardiac and pul- prospectively accumulated computerised database. monary injuries is now fairly uniform, less attention Information was extracted from inpatient records and has been paid to venous injuries and their man- a vascular surgical database. Forty-nine patients were agement. Military surgeons have favoured venous repair identified. Those with injuries to the external jugular or reconstruction, 1 whereas those in civilian or minor muscular veins were excluded. Neck practice have concluded that ligation has a role. 2 4 wounds were classified into Zones I III as outlined by Attempts to restore patients to normal anatomy in Carducci. 5 Fisher s exact test was used to test for the face of complex injuries or gross haemodynamic association between risk factors and outcome, and type instability may compromise chances of survival. The of treatment. A p value less than 0.05 was considered authors service has previously evaluated management statistically significant. options in penetrating cervicomediastinal venous trauma, 2 and advocated a low threshold for ligation of complex injuries. We review our recent experience to evaluate this policy, and to identify factors predicting poor outcome in patients with major cervicomediastinal venous injuries. Please address all correspondence to: R. Nair, Department of Surgery, Faculty of Medicine, University of Natal, Private Bag 7, Congella 4013, Natal, South Africa. Clinical presentation Forty-five male and 4 female patients were identified. The mean age was 25.3 years (range 13 42). Forty patients sustained stab wounds, and nine, gunshot wounds. Apart from one shotgun injury, all gunshot wounds were of the low-velocity type. Entrance wounds were in the neck in 40 patients and the chest /00/ $35.00/ Harcourt Publishers Ltd.
2 66 R. Nair et al. Table 1. Location of external wound and mortality. Management n Mortality Operative management comprised ligation in 25 Zone I 15 2 (13) (51.0%) patients and lateral venorrhaphy in 22 (44.9%). Zone II 18 2 (11) Zone III 7 No patients were submitted to complex venous repair, Chest 9 4 (44) e.g. interposition grafting or patch angioplasty. Two Total 49 8 (16) patients had no definitive management performed: a 25-year-old patient had an unsuccessful resuscitative Percentages to nearest whole figure within parentheses. thoracotomy at which a 4 cm wound in the superior vena cava was clamped; and a 36-year-old patient, paraplegic from a spinal cord injury, whose angiogram in 9 (Table 1). Thirty-four injuries were on the left, revealed an internal jugular vein common carotid arand 15 on the right. One patient with bilateral stabs tery arteriovenous fistula following a transcervical had a left internal jugular vein injury. Twenty-two gunshot injury. He developed a dense hemiplegia, patients were shocked on admission (systolic blood presumably on the basis of embolisation via the injured pressure below 100 mmhg). Twenty-five patients carotid artery, was treated conservatively, and died. were actively bleeding on admission. Nine patients Twenty-one (95%) of the veins sutured had lateral were in extremis, with active bleeding and profound tears, compared with 14 (56%) of those ligated. This hypotension unresponsive to external compression difference was statistically significant (p=0.0057). Anand resuscitation. The average haemoglobin was 8.8 aemia was significantly more frequent in those treated (range ) g/dl, and was 10 g/dl or less in 31 by ligation (Table 4). Ligation was more likely to be patients. performed in patients who were actively bleeding Circumstances permitted chest radiography in only or shocked, although this did not reach statistical 31 patients. Twenty-two radiographs were normal, significance. 5 demonstrated haemopneumothoraces, 3, haemo- The choice of incision was based on established thoraces, one a widened mediastinum and fractured practice. 6,7 Twenty-three patients with zone II and III ribs. Neck radiographs were of limited use, only being wounds were explored via an incision over the anterior contributory in a patient with retained shotgun pellets, border of the sternocleidomastoid muscle. Twelve a second with a fractured mandible, and a paraplegic sternotomies were performed, 9 for zone I injuries (4 patient with a fractured sixth cervical vertebra fol- subclavian vein, 1 proximal internal jugular vein, 4 lowing a transcervical gunshot. Tracheal deviation due innominate vein; 1 superior vena cava) and three for to soft-tissue swelling from haematoma was evident left chest wounds with injuries to the subclavian vein. in 2 cases. Injuries to the internal jugular vein (IJV), Supraclavicular exposure was necessary in 12 patients. subclavian vein, brachiocephalic vein and superior Eight had zone I injuries, two of whom also needed vena cava (SVC) were encountered. The location and sternotomies, three had chest wounds, and the last types of injury are outlined in Table 2. There were 46 had a zone II stab which injured the subclavian vein. concomitant injuries in 24 patients (Table 3). Identi- Three patients had resuscitative left anterolateral fiable risk factors, namely shock, active haemorrhage, thoracotomies, two of whom were exsanguinated, and haemoglobin and transfusion requirement, are listed one who succumbed to multiple organ failure four on Table 4. days later. Table 2. Vein injured, surgical treatment and associated mortality rate. Vein n Management Mortality Ligated Repaired Internal jugular vein (8) Subclavian vein (20) Brachiocephalic vein (17) Superior vena cava (66) Total (16) Percentage to nearest whole number within parentheses. One patient not operated on. Clamped only in one patient.
3 Cervicomediastinal Venous Trauma 67 Table 3. Associated injuries (Total 38 patients). Arterial: Common carotid 16 Internal carotid 1 Subclavian 12 Vertebral 2 Occipital 1 Other: Brachial plexus 5 Spinal cord 2 Lung 3 Heart (right atrium) 1 Mandible 1 Remote (stab abdomen) 2 Results Eight patients died (26.7%), all of whom were shocked on admission. Four of the nine patients who were Fig. 1. Bilateral upper limb venogram following occlusion of repair admitted in profound shock died on the operating of superior vena cava demonstrating extensive network of venous collaterals draining arms and head. table from exsanguinating haemorrhage. Three had anterolateral thoracotomies, and one a median sternveins was subjected to venorrhaphy, narrowing the otomy. Two had stab wounds to the superior vena lumen of the SVC to 25% of its normal calibre. Postcava. One was ligated and one clamped only, with the operatively, he developed massive oedema of the arms, patient suffering cardiac arrest immediately thereafter. head and neck. Chest-wall collaterals were not no- The other two had left subclavian vein injury, ligated ticeable. Venography showed occlusion of the superior in one and sutured in one. Three patients died in the vena cava, with retrograde thrombosis involving both intensive care unit from multiple organ dysfunction subclavian and the left internal jugular veins. Extensive syndrome. Their injuries were gunshot internal jugular venous collaterals (intercostal and azygous) were demvein which was ligated in one; stabbed left subclavian onstrated (Fig. 1). The oedema progressively devein ligated via left thoracotomy in one; and stabbed creased, and resolved fully by day 30. None of the 9 left subclavian vein ligated via median sternotomy in patients who had internal jugular vein ligation perthe last. The paraplegic patient who developed a stroke formed had any oedema or venous congestion. At was treated conservatively. The mortality rates for follow-up, which ranged from 1 week to 1 year (mean injuries to specific veins are listed in Table 2. Patients 9 months), no patient was noted to be oedematous, with IJV injuries had the most favourable outcome and none had upper limb or cervicofacial venous (mortality rate 11.8%). hypertension. Only 5 patients had clinically apparent oedema postoperatively. Four had injuries to the left subclavian vein, 3 of which were treated by lateral repair, and 1 by ligation. Arm oedema was treated by elevation and Discussion settled fully within 5, 5, 19 and 20 days respectively. One patient with an extensive laceration to the superior Major venous trauma is justifiably viewed with trepidation by many surgeons. Circumferential control vena cava at the confluence of the brachiocephalic of Table 4. Comparison of risk factors, operating time and outcome between patients treated by repair or by ligation. Total Repair (n=22) Ligation (n=25) p Value Haemoglobin <10 g/dl (45) 19 (76) 0.03 Active bleeding 25 8 (36) 16 (64) 0.05 Shock 22 7 (32) 14 (56) 0.08 Transfusion >2 units 21 8 (36) 13 (52) 0.21 Operating time (minutes) Mortality 8 2 (9) 4 (10) 0.35 Oedema 5 4 (18) 1 (4) 0.14 Hospital stay (days) Percentages to nearest whole figure within parentheses.
4 68 R. Nair et al. veins, by loops or clamps, is more difficult to achieve Cook 11 reported two cases of fatal pulmonary embolism than that of arteries, and injudicious attempts to do originating from injured subclavian veins, and so may add to the complexity of the injury by iatrogenic advocated intentional routine ligation of the sub- damage to venous tributaries. The high flow rate clavian vein for all injuries of the subclavian artery through major cervical and thoracic veins may rapidly and/or vein. There were no cases of clinically obvious lead to hypovolaemic shock from uncontrolled haemviewpoint. pulmonary emboli in this series to support this orrhage. Although basic principles aim for restoration Similarly, the occasionally reported com- of normal anatomy, ill-advised attempts at venous plication of thrombophlebitis following venous repair preservation or reconstruction may reduce the posreports was not seen. While the literature is replete with sibility of survival. of late chronic venous insufficiency following While the management of venous injuries continues lower limb venous injury, we could find no similar to evoke discussion in the literature, most reports reports documenting this after cervicomediastinal ven- relate to lower-limb venous trauma. Rich, 8,9 amongst ous injury, nor did we encounter the problem in any others, has shown popliteal and femoral vein ligation of our patients. to be associated with high rates of amputation, posta Due to the sometimes-incomplete documentation as operative oedema and post-phlebitic syndrome. Mulof result of the urgency at presentation, the accuracy a comparison of severity of injury in patients whose lins et al., 10 Timberlake et al. 3 and Meyer et al., 4 however, showed no increase in amputation rates when ligation injuries were ligated and those who were subjected to was performed, or vein repairs thrombosed. Although repair is questionable. However, based on univariate limb oedema has been documented in up to 51% 1 of analysis of initial haemoglobin, shock, active bleeding patients with lower limb venous injuries managed by on presentation, and transfusion requirements, it ligation, it is usually transient. In one of the largest would appear that those treated by ligation had more published series of venous injuries, permanent oedema severe injuries (Table 4). The similar time taken for occurred in 2% of patients, and developed regardless repair and ligation is thought to be a consequence of of vein ligation or repair. 1 A further problem that the greater complexity of injuries that needed ligation. As a result of the retrospective nature of this analysis, bedevils reports of outcome of lower-limb venous application of any of the available trauma-scoring repair is the inaccuracy of clinical and non-invasive systems was not possible. Factors associated with an assessment of patency after venous repair. In one of increased risk of mortality were shock, haemoglobin the few papers where outcome was quantified by less than 10 g/dl, chest wounds, and the need for venography in all cases, the thrombosis rate varied thoracotomy or sternotomy. Injuries to veins other than from 21% (local repair) to 59% (complex repair). the IJV were also associated with increased mortality. Significant discrepancies between clinical and non- There was no significant difference in mortality beinvasive assessment and venography were demtween patients treated by venous repair or those onstrated in 33% and 47% of cases respectively. 4 treated by ligation. Little has been written about cervicomediastinal The present study validates the authors published venous injury. In our experience, the sequelae of major policy regarding cervicomediastinal venous trauma. 2 venous ligation have been few and short-lived. Oed- Repair should be undertaken in stable patients, where ema was as likely to follow either ligation or repair, the injury is amenable to local venorrhaphy. When and was most frequently associated with subclavian complex techniques are necessary (interposition graftvein injuries. In all cases, the oedema was self-limiting ing, patch angioplasty, resection and re-anastomosis) and resolved fully. None of the patients subjected to or in the presence of haemodynamic instability, ligunilateral internal jugular vein ligation demonstrated ation is the preferred option and may be undertaken oedema or any other sign of venous hypertension. It would appear that the extensive network of venous without fear of morbidity from persistent oedema. anastomoses allows the development of adequate collaterals, sufficient to compensate for even major venous ligation. It has not been our policy to routinely monitor References continued patency of venous repairs. Venography was 1Rich NM. Principles and indications for primary venous repair. done in the case of a patient who developed massive, Surgery 1982; 91: albeit transient, upper-extremity oedema following 2Robbs JV, Reddy E. Management options for penetrating injuries repair of a SVC injury, and showed thrombosis of the to the great veins of the neck and superior mediastinum. Surg Gyn Obs 1987; 165: SVC at the site of the injury with extension into both 3 Timberlake GA, Kerstein MD. Venous injury: to repair or ligate, innominate veins and the right IJV. the dilemma revisited. Am Surg 1995; 61:
5 Cervicomediastinal Venous Trauma 69 4Meyer J, Walsh J, Schuler J et al. The early fate of venous lower extremity venous trauma: A more aggressive approach repair after civilian vascular trauma. Ann Surg 1987; 206: required. J Trauma 1974; 14: Carducci B, Lowe RA, Dalsey W. Penetrating Neck Trauma: 10 Mullins RJ, Lucas CE, Ledgerwood AM. The natural history Consensus and controversies. Ann Emerg Med 1986; 15: following venous ligation for civilian injuries. J Trauma 1980; 20: 6 Robbs JV, Baker LW, Human RR et al. Cervicomediastinal arterial injuries. Arch Surg 1981; 116: Cook FW, Haller JA. Penetrating injuries of the subclavian 7Robbs JV, Baker LW. Cardiovascular trauma. Curr Probl Surg vessels with associated venous complications. Ann Surg 1962; 1984; 21: : Rich NM, Baugh JH, Hughes CW. Acute arterial injuries in Vietnam: 1000 cases. J Trauma 1970; 10: Rich NM, Hobson RW II, Wright CB, Fedde CW. Repair of Accepted 17 August 1999
Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service
 Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service J Islam, 1,4 G L Laing, 2,4 J L Bruce, 2,4 G V Oosthuizen, 2,4 D L Clarke, 2,4 J V Robbs 3,4
Outcomes for cervicomediastinal vascular trauma managed by a vascular subspecialistled vascular trauma service J Islam, 1,4 G L Laing, 2,4 J L Bruce, 2,4 G V Oosthuizen, 2,4 D L Clarke, 2,4 J V Robbs 3,4
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Emergency Approach to the Subclavian and Innominate Vessels
 Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Emergency Approach to the Subclavian and Innominate Vessels Joseph J. Amato, M.D., Robert M. Vanecko, M.D., See Tao Yao, M.D., and Milton Weinberg, Jr., M.D. T he operative approach to an acutely injured
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Large veins of the thorax Brachiocephalic veins
 Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
Large veins of the thorax Brachiocephalic veins Right brachiocephalic vein: formed at the root of the neck by the union of the right subclavian & the right internal jugular veins. Left brachiocephalic
10/14/2018 Dr. Shatarat
 2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
2018 Objectives To discuss mediastina and its boundaries To discuss and explain the contents of the superior mediastinum To describe the great veins of the superior mediastinum To describe the Arch of
Combat Extremity Vascular Trauma
 Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Combat Extremity Vascular Trauma Training teams to be a TEAM Chatt A. Johnson LTC, MC, USA 08 March 2010 US Army Trauma Training Center Core Discussion Series Outline: Combat Vascular Injury Physiologic
Innominate artery trauma: A thirty-year experience
 Innominate artery trauma: A thirty-year experience Robert H. Johnston, Jr., MD, Matthew J. Wall, Jr., MD, and Kenneth L. Mattox, MD, Houston, Texas Purpose: Injury to the innominate artery may represent
Innominate artery trauma: A thirty-year experience Robert H. Johnston, Jr., MD, Matthew J. Wall, Jr., MD, and Kenneth L. Mattox, MD, Houston, Texas Purpose: Injury to the innominate artery may represent
AV ACESS COMPLICATIONS. Ass. Prof. Dr. Habas
 AV ACESS COMPLICATIONS Ass. Prof. Dr. Habas COMPLICATION AVF IS CONSIDERED A MINOR PROCEDURE INCIDENCE OF COMPLICATION- 20-27% MANY A COMPLICATION LEADS TO FAILURE OF FISTULA LOSS OF SITE AND VEIN FOR
AV ACESS COMPLICATIONS Ass. Prof. Dr. Habas COMPLICATION AVF IS CONSIDERED A MINOR PROCEDURE INCIDENCE OF COMPLICATION- 20-27% MANY A COMPLICATION LEADS TO FAILURE OF FISTULA LOSS OF SITE AND VEIN FOR
Review of Surgical Treatment of Popliteal Artery Injury: Outcomes of Open vs Endovascular Repair
 Review of Surgical Treatment of Popliteal Artery Injury: Outcomes of Open vs Endovascular Repair Tze-Woei Tan, MD; Francesca D. Armstrong, MD; Wayne W. Zhang, MD From Louisiana State University Health,
Review of Surgical Treatment of Popliteal Artery Injury: Outcomes of Open vs Endovascular Repair Tze-Woei Tan, MD; Francesca D. Armstrong, MD; Wayne W. Zhang, MD From Louisiana State University Health,
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
Upper Extremity Venous Duplex. Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016
 Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
Upper Extremity Venous Duplex Michigan Sonographers Society Fall Ultrasound Symposium October 15, 2016 Patricia A. (Tish) Poe, BA RVT FSVU Director of Quality Assurance Navix Diagnostix Patricia A. Poe
RESUSCITATION IN TRAUMA. Important things I have learnt
 RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
Subclavian and Axillary Artery Aneurysms
 Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
Subclavian and Axillary Artery Aneurysms April 2008 Francesco A Aiello, M.D. Assistant Professor of Surgery Division of Vascular Endovascular Surgery University of Massachusetts Medical School None DISCLOSURES
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
EAST MULTICENTER STUDY DATA DICTIONARY. Temporary Intravascular Shunt Study Data Dictionary
 EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
2 Aortic Arch Debranching UCSF Vascular Symposium /14/16. J Endovasc Ther 2002;9:suppl 2; II98 105
 How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
How I Do It: Aortic Arch Debranching Exposures, Tunnels and Techniques Warren Gasper MD Assistant Professor of Surgery UCSF Vascular Surgery No disclosures 2 Aortic Arch Debranching UCSF Vascular Symposium
SELECTIVE ANTEGRADE TECHNIQUE OF CHOICE
 SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
SELECTIVE ANTEGRADE CEREBRAL PERFUSION IS THE TECHNIQUE OF CHOICE MARKO TURINA University of Zurich Zurich, Switzerland What is so special about the operation on the aortic arch? Disease process is usually
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS
 Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
Popliteal Aneurysm: When is surgical therapy indicated? PROF. GRZEGORZ OSZKINIS Asymptomatic mass - 38-40%will develop symptoms at a rate of 14%/yr Intermittent claudic ation (chronic ischemia) - 25%-40%
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Morbidity Audit and Logbook Tool SNOMED Board Reporting Terms for SET and IMG Vascular Surgery AMPUTATION AORTA
 SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
SNOMED s for SET and IMG Vascular Surgery AMPUTATION Amputation above-knee Amputation of leg through tibia and fibula Amputation of the foot Amputation of toe Through knee amputation Ray amputation of
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Descending aorta replacement through median sternotomy
 Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Descending aorta replacement through median sternotomy Mitrev Z, Anguseva T, Belostotckij V, Hristov N. Special hospital for surgery Filip Vtori Skopje - Makedonija June, 2010 Cardiosurgery - Skopje 1
Thoracic Outlet Syndrome
 Disclosures None relevant to this discussion The Management of Thoracic Outlet Syndrome: Acute Charles Eichler MD Professor, Department of Surgery Division of Vascular and Endovascular Surgery University
Disclosures None relevant to this discussion The Management of Thoracic Outlet Syndrome: Acute Charles Eichler MD Professor, Department of Surgery Division of Vascular and Endovascular Surgery University
Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Ultrasound-enhanced, catheter-directed thrombolysis for pulmonary embolism A pulmonary embolism (PE) is
Lung cancer or primary malignant tumors of the mediastinum
 Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Technique of Superior Vena Cava Resection for Lung Carcinomas David R. Jones, MD Division of Thoracic and Cardiovascular Surgery, Department of Surgery, University of Virginia School of Medicine, Charlottesville,
Steal Syndrome: The Role of the Vascular Lab
 Steal Syndrome: The Role of the Vascular Lab Eighth Overlook Noninvasive Vascular Lab Symposium Larry A. Scher, M.D. Professor of Surgery Division of Vascular Surgery Montefiore Medical Center Albert Einstein
Steal Syndrome: The Role of the Vascular Lab Eighth Overlook Noninvasive Vascular Lab Symposium Larry A. Scher, M.D. Professor of Surgery Division of Vascular Surgery Montefiore Medical Center Albert Einstein
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm
 Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Hybrid Repair of a Complex Thoracoabdominal Aortic Aneurysm Virendra I. Patel MD MPH Assistant Professor of Surgery Massachusetts General Hospital Division of Vascular and Endovascular Surgery Disclosure
Predictors of outcome in patients requiring surgery for liver trauma
 Injury, Int. J. Care Injured (2007) 38, 65 70 www.elsevier.com/locate/injury Predictors of outcome in patients requiring surgery for liver trauma W.L. Sikhondze, T.E. Madiba *, N.M. Naidoo, D.J.J. Muckart
Injury, Int. J. Care Injured (2007) 38, 65 70 www.elsevier.com/locate/injury Predictors of outcome in patients requiring surgery for liver trauma W.L. Sikhondze, T.E. Madiba *, N.M. Naidoo, D.J.J. Muckart
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
May Clinical Director, Peninsula Trauma Network (Edited for PTN)
 Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
Network Policy Traumatic vascular injuries Guidelines Purpose Date May 2015 Version Following the national introduction of Regional Trauma Networks, Major Trauma Networks (MTN s) are required to have a
Case #1. Case #1- Possible codes. Unraveling the -59 modifier. Principles of Interventional. CASE 1: Simple angioplasty
 Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Unraveling the -59 modifier Principles of Interventional Coding Donald Schon, MD, FACP Debra Lawson, CPC, PCS Distinct or independent from other services performed on the same day Normally not reported
Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally
 Volume 2 Issue 3 Article 3 2016 Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally Farzad Amiri, MD; Zachary Sanford; and Constantinous Constantinou, MD Follow
Volume 2 Issue 3 Article 3 2016 Traumatic Posterior Tibial Pseudoaneursym: A rare late complication repaired conventionally Farzad Amiri, MD; Zachary Sanford; and Constantinous Constantinou, MD Follow
Surgical Privileges Form: Vascular Surgery
 Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
Surgical Form: Vascular Surgery Clinical Request Applicant s Name:. License No. (If Any):... Date:... Scope of Practice:. Facility:.. Place of Work:. CATEGORY I: GENERAL PRIVILEGES 1. Admitting privileges
Saphenous Vein Autograft Replacement
 Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
Saphenous Vein Autograft Replacement of Severe Segmental Coronary Artery Occlusion Operative Technique Rene G. Favaloro, M.D. D irect operation on the coronary artery has been performed in 180 patients
THE popliteal artery is the second most common site of aneurysm. The
 POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
POPLITEAL ANEURYSM Treatment by Vein Graft: Case Report A. W. HUMPHRIES, M.D. Department of Orthopedic Surgery F. A. LeFEVRE, M.D. and V. G. dewolfe, M.D. Department of Cardiovascular Disease THE popliteal
Copy Right- Hongqi ZHANG-Department of Anatomy-Fudan University. Systematic Anatomy. Angiology Part 4. Veins. Dr.Hongqi Zhang ( 张红旗 )
 Systematic Anatomy Angiology Part 4 Veins Dr.Hongqi Zhang ( 张红旗 ) Email: zhanghq58@126.com 1 General introduction of the veins Vessel which return the blood back to atrium No pulsation,veneous blood, metabolic
Systematic Anatomy Angiology Part 4 Veins Dr.Hongqi Zhang ( 张红旗 ) Email: zhanghq58@126.com 1 General introduction of the veins Vessel which return the blood back to atrium No pulsation,veneous blood, metabolic
Penetrating Neck Trauma. Herve J. LeBoeuf, MD Francis B. Quinn, MD
 Penetrating Neck Trauma Herve J. LeBoeuf, MD Francis B. Quinn, MD Introduction 5-10% of all trauma Overall mortality rate as high as 11% Major vessel injury fatal in 65%, including prehospital deaths Attending
Penetrating Neck Trauma Herve J. LeBoeuf, MD Francis B. Quinn, MD Introduction 5-10% of all trauma Overall mortality rate as high as 11% Major vessel injury fatal in 65%, including prehospital deaths Attending
The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3-
 1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
1 2 The sinus venosus represent the venous end of the heart It receives 3 veins: 1- Common cardinal vein body wall 2- Umbilical vein from placenta 3- Vitelline vein from yolk sac 3 However!!!!! The left
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Introduction. Keywords: Egypt, 25th January revolution, management, vascular trauma. Original article 43
 Original article 43 Vascular trauma and its management: one and a half years after the 25th January revolution Mahsoub Murad, Ashraf Eweda, Hani Abdel-moamen, Mohamed Hussien and Mohamed Elsaghir Department
Original article 43 Vascular trauma and its management: one and a half years after the 25th January revolution Mahsoub Murad, Ashraf Eweda, Hani Abdel-moamen, Mohamed Hussien and Mohamed Elsaghir Department
Sample page. POWER UP YOUR CODING with Optum360, your trusted coding partner for 32 years. Visit optum360coding.com.
 2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
2018 Complete Guide for Interventional Radiology An in-depth guide to interventional radiology coding, billing, and reimbursement for facilities and physicians POWER UP YOUR CODING with Optum360, your
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
Arterial Map of the Thorax, Abdomen and Pelvis 2017 Edition
 Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
Arterial Map of the Thorax, Abdomen and Pelvis Angiography 75605 (-26) Aortography, thoracic 75625 (-26) Aortography, abdominal by serialography 75630 (-26) Aortography, abdominal + bilat iliofemoral 75705
Medical Review Guidelines Magnetic Resonance Angiography
 Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Endovascular Trauma Management. Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden
 Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
Endovascular Trauma Management Thomas Larzon, MD, PhD Dep of Cardiothoracic and Vascular Surgery Örebro University Hospital, Sweden Medtronic Symposium, LINC 2016 Disclosures I have the following potential
Penetrating wounds of the heart and great vessels
 Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Thorax (1973), 28, 142. Penetrating wounds of the heart and great vessels A report of 30 patients C. E. ANAGNOSTOPOULOS and C. FREDERICK KITTLE Department of Surgery, Section of Thoracic and Cardiovascular
Sectional Anatomy Quiz - III
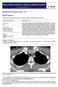 Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
Sectional Anatomy - III Rashid Hashmi * Rural Clinical School, University of New South Wales (UNSW), Wagga Wagga, NSW, Australia A R T I C L E I N F O Article type: Article history: Received: 30 Jun 2018
3 Circulatory Pathways
 40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
40 Chapter 3 Circulatory Pathways Systemic Arteries -Arteries carry blood away from the heart to the various organs of the body. -The aorta is the longest artery in the body; it branches to give rise to
P ischemia of the brain, spinal cord, kidneys, and
 Penetrating Injuries of the Aortic Arch and Its Branches James W. Pate, MD, F. Hammond Cole, Jr, MD, William A. Walker, MD, and Timothy C. Fabian, MD Section of Cardiothoraac Surgery, University of Tennessee,
Penetrating Injuries of the Aortic Arch and Its Branches James W. Pate, MD, F. Hammond Cole, Jr, MD, William A. Walker, MD, and Timothy C. Fabian, MD Section of Cardiothoraac Surgery, University of Tennessee,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection
 Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Aggressive Resection/Reconstruction of the Aortic Arch in Type A Dissection M. Grabenwoger Dept. of Cardiovascular Surgery Hospital Hietzing Vienna, Austria Disclosure Statement Consultant of Jotec, Hechingen,
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Epidemiology. 16% incidence in knee. dislocation
 Epidemiology Highest risk group: Young male between 15 and 45 years (USA) Mortality Ratio after trauma : male/female: 7/1 Peripheral vascular injuries : 70%-80% of all cases of vascular trauma : Vascular
Epidemiology Highest risk group: Young male between 15 and 45 years (USA) Mortality Ratio after trauma : male/female: 7/1 Peripheral vascular injuries : 70%-80% of all cases of vascular trauma : Vascular
Overview of CVADs. Type of device commonly used. Dwell time Flushing requirement Associated complications. lumens
 Source: Clinical Skills Management of Vascular Access Devices Pre-course handbook. Adapted with permission from NHS Lothian Employee and Education Development Team. Overview of CVADs Type of device Veins
Source: Clinical Skills Management of Vascular Access Devices Pre-course handbook. Adapted with permission from NHS Lothian Employee and Education Development Team. Overview of CVADs Type of device Veins
THE VESSELS OF BLOOD CIRCULATION
 THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
THE VESSELS OF BLOOD CIRCULATION scientistcindy.com /the-vessels-of-blood-circulation.html NOTE: You should familiarize yourself with the anatomy of the heart and have a good understanding of the flow
VESSELS: GROSS ANATOMY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. 2) Observe and sketch histology slide
Activity Three: Where s the Bleeding?
 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Traumatic A-V A V Fistula
 Traumatic A-V A V Fistula PRESENT HISTORY PAST HISTORY 30 year-old, male ( XX); Denied other systemic disease before. PRESENT HISTORY A deep stabbing wound (3*1 cm) noted on 07/01/2002 over Right anterior
Traumatic A-V A V Fistula PRESENT HISTORY PAST HISTORY 30 year-old, male ( XX); Denied other systemic disease before. PRESENT HISTORY A deep stabbing wound (3*1 cm) noted on 07/01/2002 over Right anterior
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2)
 Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Surgery Rotation Objectives for Junior Residents (PGY-1 and 2) Definition Vascular surgery is the specialty concerned with the diagnosis and management of congenital and acquired diseases of the
Vascular Trauma in Penang and Kuala Lumpur Hospitals
 Vascular Trauma in Penang and Kuala Lumpur Hospitals M N Lakhwani*, B H Gooi**, C D J Barras*** 'Penang Adventist Hospital, Penang, "Department of Surgery, Penang Hospital, 10990 Penang, "'St.Vincent's
Vascular Trauma in Penang and Kuala Lumpur Hospitals M N Lakhwani*, B H Gooi**, C D J Barras*** 'Penang Adventist Hospital, Penang, "Department of Surgery, Penang Hospital, 10990 Penang, "'St.Vincent's
In the Last Three Lectures We Already Discussed the Importance of the Thoracic Cage.
 -This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
-This Lecture Will Revise what we took in the last three lectures and will introduce the concept of the chest cavity ( Thoracic Cavity ) In the Last Three Lectures We Already Discussed the Importance of
Vertebral Artery Pseudoaneurysm
 Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
Vertebral Artery Pseudoaneurysm T. W. Khanzada,K. R. Makhdoomi ( Department of Vascular Surgery, Liaquat National Postgraduate Medical Centre, Karachi. ) Vertebral artery (VA) pseudoaneurysms are exceedingly
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques
 Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Complex Thoracic and Abdominal Aortic Repair Using Hybrid Techniques Tariq Almerey MD, January Moore BA, Houssam Farres MD, Richard Agnew MD, W. Andrew Oldenburg MD, Albert Hakaim MD Department of Vascular
Tips & Techniques in Operative Surgery II: Neck Exploration
 Tips & Techniques in Operative Surgery II: Neck Exploration ศ.ดร.นพ. พรช ย โอเจร ญร ตน สาขาว ชาศ ลยศาสตร ศ รษะ-คอ และเต านม ภาคว ชาศ ลยศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล Indications to Explore a Neck Removing
Tips & Techniques in Operative Surgery II: Neck Exploration ศ.ดร.นพ. พรช ย โอเจร ญร ตน สาขาว ชาศ ลยศาสตร ศ รษะ-คอ และเต านม ภาคว ชาศ ลยศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล Indications to Explore a Neck Removing
Delineation Of Privileges Vascular Surgery Privileges
 CATEGORY 1 - VASCULAR SURGERY PRIVILEGES Criteria: New Applicants must meet one of the following: a) Board Certification or qualified for certification by the American Board of Vascular Surgery; b) Completion
CATEGORY 1 - VASCULAR SURGERY PRIVILEGES Criteria: New Applicants must meet one of the following: a) Board Certification or qualified for certification by the American Board of Vascular Surgery; b) Completion
Subclavian-axillary vascular trauma
 Subclavian-axillary vascular trauma Robert A. McCready, M.D., C. Daniel Procter, M.D., ~ and Gordon L Hyde, M.D., Lexington, Ky. Traumatic vascular injuries to the subdavian and axillary vessels are often
Subclavian-axillary vascular trauma Robert A. McCready, M.D., C. Daniel Procter, M.D., ~ and Gordon L Hyde, M.D., Lexington, Ky. Traumatic vascular injuries to the subdavian and axillary vessels are often
SAMPLE CHAPTERS UNESCO-EOLSS MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGET-SCHROETTER SYNDROME
 MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGETSCHROETTER SYNDROME J. Ernesto Molina University of Minnesota, Minneapolis, Minnesota, U.S.A. Keywords: Thoracic outlet, Venous disease Contents 1.
MANAGEMENT OF SUBCLAVIAN VEIN THROMBOSIS KNOWN AS PAGETSCHROETTER SYNDROME J. Ernesto Molina University of Minnesota, Minneapolis, Minnesota, U.S.A. Keywords: Thoracic outlet, Venous disease Contents 1.
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1
 Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Tasopoulou KM 1, Argyriou C 1, Mantatzis M 2, Kantartzi K 3, Passadakis P 3, Georgiadis GS 1 1 Department of Vascular Surgery, 2 Department of Radiology/Interventional Radiology Unit and 3 Department of
Endovascular treatment of carotid-jugular fistula after gunshot wound
 Endovascular treatment of carotid-jugular fistula after gunshot wound Instituto Dante Pazzanese de Cardiologia São Paulo, Brazil Carrijo, LBS; Tannus, MM; Cano, MN; Izukawa, NM; Moreira, SM; Kambara, AM
Endovascular treatment of carotid-jugular fistula after gunshot wound Instituto Dante Pazzanese de Cardiologia São Paulo, Brazil Carrijo, LBS; Tannus, MM; Cano, MN; Izukawa, NM; Moreira, SM; Kambara, AM
Internal Injury Documentation Guidelines
 Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Partial anomalous pulmonary venous connection to superior
 Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Cavo-Atrial Anastomosis Technique for Partial Anomalous Pulmonary Venous Connection to the Superior Vena Cava The Warden Procedure Robert A. Gustafson, MD Partial anomalous pulmonary venous connection
Extracranial to intracranial bypass for intracranial atherosclerosis
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Extracranial to intracranial bypass for intracranial atherosclerosis In cerebrovascular disease, blood vessels
Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein
 Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein Ahmed Afifi, Ahmed ElGuindy, Mahmoud Farouk, Magdi H Yacoub* * m.yacoub@imperial.ac.uk DOI: http://dx.doi.org/10.5339/gcsp.2012.13 ISSN:
Endo- aneurysmorrhaphy of a giant aneurysm of the subclavian vein Ahmed Afifi, Ahmed ElGuindy, Mahmoud Farouk, Magdi H Yacoub* * m.yacoub@imperial.ac.uk DOI: http://dx.doi.org/10.5339/gcsp.2012.13 ISSN:
Arthroplasty after previous surgery: previous vascular problems
 Arthroplasty after previous surgery: previous vascular problems Jacques Menetrey & Victoria B. Duthon Centre de médecine de l appareil locomoteur et du sport Swiss Olympic medical Center Unité d Orthopédie
Arthroplasty after previous surgery: previous vascular problems Jacques Menetrey & Victoria B. Duthon Centre de médecine de l appareil locomoteur et du sport Swiss Olympic medical Center Unité d Orthopédie
Paraplegia in endovascular repair of TAA and in TEVAR: Incidence, prevention and therapy. Johannes Lammer Medical University Vienna, Austria
 Paraplegia in endovascular repair of TAA and in TEVAR: Incidence, prevention and therapy Johannes Lammer Medical University Vienna, Austria Conflict of interests: none 68y, male, PAU in coral reef aorta,
Paraplegia in endovascular repair of TAA and in TEVAR: Incidence, prevention and therapy Johannes Lammer Medical University Vienna, Austria Conflict of interests: none 68y, male, PAU in coral reef aorta,
c) What is the name of RBC (erythrocyte) formation? Where do blood cells form?
 UNIT 6: CARDIOVASCULAR SYSTEM 1) List the three general functions of BLOOD. REVIEW QUESTIONS Blood 2) a) What are the three formed elements /cellular elements in blood? b) Describe the composition of the
UNIT 6: CARDIOVASCULAR SYSTEM 1) List the three general functions of BLOOD. REVIEW QUESTIONS Blood 2) a) What are the three formed elements /cellular elements in blood? b) Describe the composition of the
How to manage the left subclavian and left vertebral artery during TEVAR
 How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
How to manage the left subclavian and left vertebral artery during TEVAR Jürg Schmidli Chief of Vascular Surgery Inselspital Hamburg 2017 Dept Cardiovascular Surgery, Bern, Switzerland Disclosure No Disclosures
LIVER INJURIES PROFF. S.FLORET
 LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
How to Determine Tolerance for Branch Vessel Coverage
 How to Determine Tolerance for Branch Vessel Coverage Venita Chandra, MD Clinical Assistant Professor of Surgery Division of Stanford Medical School, Stanford, CA PNEC May 25 th, 2017 DISCLOSURES Venita
How to Determine Tolerance for Branch Vessel Coverage Venita Chandra, MD Clinical Assistant Professor of Surgery Division of Stanford Medical School, Stanford, CA PNEC May 25 th, 2017 DISCLOSURES Venita
Neurological Complications of TEVAR. Frank J Criado, MD. Union Memorial-MedStar Health Baltimore, MD USA
 ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
ISES Online Neurological Complications of Frank J Criado, MD TEVAR Union Memorial-MedStar Health Baltimore, MD USA frank.criado@medstar.net Paraplegia Incidence is 0-4% after surgical Rx of TAAs confined
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis. Prof. Ralf R.Kolvenbach MD,PhD,FEBVS
 Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Catheter-based thrombolysis Local administration of lytic agent Higher local
Innovative Endovascular Approach to Pulmonary Embolism by Ultrasound Enhanced Thrombolysis Prof. Ralf R.Kolvenbach MD,PhD,FEBVS Catheter-based thrombolysis Local administration of lytic agent Higher local
Surgical Options in Thrombectomy for Non-Surgeons
 Surgical Options in Thrombectomy for Non-Surgeons Shouwen Wang, MD, PhD, FASDIN AKDHC Ambulatory Surgery Center Arizona Kidney Disease and Hypertension Center Phoenix, Arizona Disclosure No relevant financial
Surgical Options in Thrombectomy for Non-Surgeons Shouwen Wang, MD, PhD, FASDIN AKDHC Ambulatory Surgery Center Arizona Kidney Disease and Hypertension Center Phoenix, Arizona Disclosure No relevant financial
YOU MUST BRING GLOVES FOR THIS ACTIVITY
 ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
ACTIVITY 10: VESSELS AND CIRCULATION OBJECTIVES: 1) How to get ready: Read Chapter 23, McKinley et al., Human Anatomy, 5e. All text references are for this textbook. 2) Observe and sketch histology slide
Endovascular repair of inadvertent subclavian artery injury during attempted internal jugular vein catheterization: A case report
 ISPUB.COM The Internet Journal of Endovascular Medicine Volume 1 Number 2 Endovascular repair of inadvertent subclavian artery injury during attempted internal jugular vein catheterization: A case report
ISPUB.COM The Internet Journal of Endovascular Medicine Volume 1 Number 2 Endovascular repair of inadvertent subclavian artery injury during attempted internal jugular vein catheterization: A case report
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Popliteal Artery Aneurysms: Diagnosis and Repair Options
 Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
Deepak N. Deshmukh DO April 27, 2018 Popliteal Artery Aneurysms: Diagnosis and Repair Options No Disclosures Popliteal Artery Aneurysms (PAAs) Male Predominanace Most common peripheral Aneurysm (70%) 30-50%
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
An unusual shoulder injury
 An unusual shoulder injury Authors: AJ Moss, D Valenti, SC Fraser, J Murie Location: Queen Elizabeth Hospital, Norfolk, UK Citation: Moss AJ, Valenti D, Fraser S, Murie J. An unusual shoulder injury. 2011.
An unusual shoulder injury Authors: AJ Moss, D Valenti, SC Fraser, J Murie Location: Queen Elizabeth Hospital, Norfolk, UK Citation: Moss AJ, Valenti D, Fraser S, Murie J. An unusual shoulder injury. 2011.
PEDIATRIC PENETRATING TRAUMA. Laura Boomer 11/18/15
 PEDIATRIC PENETRATING TRAUMA Laura Boomer 11/18/15 PENETRATING THORACIC TRAUMA Trauma is the major cause of morbidity and mortality in children Penetrating trauma (in general) accounts for only approximately
PEDIATRIC PENETRATING TRAUMA Laura Boomer 11/18/15 PENETRATING THORACIC TRAUMA Trauma is the major cause of morbidity and mortality in children Penetrating trauma (in general) accounts for only approximately
CARDIOVASCULAR DANIL HAMMOUDI.MD
 CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
CARDIOVASCULAR DANIL HAMMOUDI.MD 18 Systemic Circulation Figure 19.19 Pulmonary Circulation Figure 19.18b 1. Thyroid gland 2. Trachea 3. Brachiocephalic 4. Common carotid 5. Internal jugular 6. Superior
Intro: Slide 1. Slide 2. Slide 3. Basic understanding of interventional radiology. Gain knowledge of key terms and phrases
 Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
Slide 1 Intro: PRESENTED BY: Selena M. Moore, AAS, CCS, CPC HIMS Physician Liaison Coder This is a modified/updated presentation that was originally written by: Rosemary Waligorski, RHIT, CCS, RCC and
EVAR replaced standard repair in most cases. Why?
 EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
EVAR replaced standard repair in most cases. Why? Initial major steps in endograft evolution Papazoglou O. Konstantinos M.D. The story of a major breakthrough in vascular surgery 1991 Parodi introduces
Recanalization Techniques: Sharp Needle Recanalization. Recanalization Techniques: Sharp Needle Recanalization
 Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
Recanalization of Occluded Central Veins When Conventional Methods Failed: Abigail Falk, MD, FSIR American Access Care New York, NY Conventional Methods of Recanalization Directional 0.035 and 0.018 Guidewires
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Shock and Resuscitation: Part II. Patrick M Reilly MD FACS Professor of Surgery
 Shock and Resuscitation: Part II Patrick M Reilly MD FACS Professor of Surgery Trauma Patient 1823 / 18 Police Dropoff Torso GSW Lower Midline / Right Buttock Shock This Monday Trauma Patient 1823 / 18
Shock and Resuscitation: Part II Patrick M Reilly MD FACS Professor of Surgery Trauma Patient 1823 / 18 Police Dropoff Torso GSW Lower Midline / Right Buttock Shock This Monday Trauma Patient 1823 / 18
Lines and tubes. 1 Nasogastric tubes Endotracheal tubes Central lines Permanent pacemakers Chest drains...
 Lines and tubes 1 Nasogastric tubes... 15 2 Endotracheal tubes.... 19 3 Central lines... 21 4 Permanent pacemakers.... 25 5 Chest drains... 30 This page intentionally left blank 1 Nasogastric tubes Background
Lines and tubes 1 Nasogastric tubes... 15 2 Endotracheal tubes.... 19 3 Central lines... 21 4 Permanent pacemakers.... 25 5 Chest drains... 30 This page intentionally left blank 1 Nasogastric tubes Background
Accepted Manuscript. External iliac artery injury secondary to indirect pressure wave effect from gun shot wound. Eugene Ng, Andrew MTL.
 Accepted Manuscript External iliac artery injury secondary to indirect pressure wave effect from gun shot wound Eugene Ng, Andrew MTL. Choong PII: S1008-1275(16)00034-1 DOI: 10.1016/j.cjtee.2016.01.013
Accepted Manuscript External iliac artery injury secondary to indirect pressure wave effect from gun shot wound Eugene Ng, Andrew MTL. Choong PII: S1008-1275(16)00034-1 DOI: 10.1016/j.cjtee.2016.01.013
CORE STANDARDS STANDARDS USED IN TARN REPORTS
 CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
