Blindness and severe visual impairment in facial fractures: an 11 year review
|
|
|
- Ethan Nash
- 5 years ago
- Views:
Transcription
1 British Journal of Plastic Surgery (2002), 55, The British Association of Plastic Surgeons doi: Pojps BRITISH JOURNAL OF [ ~ ] PLASTIC SURGERY Blindness and severe visual impairment in facial fractures: an 11 year review C. A. MacKinnon, D. J. David and R. D. Cooter* Australian Craniofacial Unit, Women and Children's Hospital, North Adelaide, and *Department of Plastic and Reconstructive Surgery, Royal Adelaide Hospital, Adelaide, South Australia, Australia SUMMARY. We present an 11 year review of facial fractures treated in the Australian Craniofacial Unit and the Department of Plastic and Reconstructive Surgery at the Royal Adelaide Hospital, specifically looking at those fractures in adults that resulted in blindness or severe visual impairment. During the period , a total of 2516 patients with facial fractures were treated operatively. From our facial-fracture database, 317 patients were identified as having an ophthalmological complication on presentation. Of these, 19 had severe visual impairment or blindness. The exact fracture pattern and craniofacial disruption score were recorded for each of these 19 cases using the Cooter-David facial-fracture scoring system. Laterally directed forces are implied as major causative factors in these injuries. Recommendations are made based on these findings The British Association of Plastic Surgeons Keywords: facial fracture, blindness, visual impairment. Blindness following facial fracture is rare, and its management is controversial. 13 The actual incidence of severe visual impairment is difficult to ascertain, as there are very few reports with large series of patients. 1,4 Using our database of over 2500 patients with facial fractures, we felt that it was timely to review the incidence of blindness and severe visual impairment in our series. The aim of this review was to examine the data for any correlation between fracture pattern or mechanism and visual outcome. Patients and methods All adult patients with facial fractures treated operatively by members of the Australian Craniofacial Unit and the Department of Plastic and Reconstructive Surgery at the Royal Adelaide Hospital over the 11 year period were included in the study. The details of all patients with facial fractures are encoded into a standardised database on admission, and ongoing management information is recorded perioperatively and through to long-term follow-up. The database records demographic details, history and initial examination findings, the results of radiological and other investigations, alphanumeric coding of the fracture using the Cooter-David facial-fracture scoring system (CDFSS), 5 operative findings, a detailed analysis of the operative procedure, and short, intermediate and long-term follow-up findings. The information is initially recorded by the junior surgical staff, with the operating surgeon providing the operative and follow-up details. Apart from those with minor fractures, all patients have a CT scan of the facial bones preoperatively. Included in this retrospective analysis were all adult patients managed between May 1989 and May A total of 2516 patients were identified. Using the database, 317 patients (13%) were documented as having an ophthalmological complication identified on admission. The database has fields in the history and examination sections where ophthalmological symptoms and signs can be recorded. Keyword searches were applied to other fields throughout the database to identify further ophthalmological symptoms. All of the 317 charts were manually reviewed to identify those patients with severe visual impairment or blindness. Blindness was defined as a visual acuity of 6/60 or worse, or a visual field of 10 ~ or less in the affected eye, or a destroyed globe. Severe visual impairment was defined as a visual acuity of worse than 6/18 in the affected eye. This level was chosen because it is a functionally disabling level of acuity. A useful correlate is that to obtain a new driver's licence in South Australia, one must have a visual acuity of no worse than 6/12 in either eye. For those with an existing driver's licence, one must have a visual acuity of no worse than 6/18 in the best-seeing eye. Hence, a visual acuity of less than 6/18 in one eye severely impairs the patient's ability to drive a motor vehicle, and, after discussion with our ophthalmological colleagues, we felt that this figure represented a reasonable objective measurement for severe visual impairment. All 317 patients with ophthalmological complications were assessed preoperatively and postoperatively by an ophthalmologist, and visual acuity was routinely recorded. A best postoperative visual acuity of less than 6/18 within a 6 month period was defined as severe visual loss. Other ocular disorders, such as diplopia, epiphora, conjunctival haemorrhage, etc., were recorded but not considered further in this study. Review of these 317 cases revealed 19 patients with severe visual loss or blindness (6.0%, or 0.8% of the 2516 patients with facial fractures in this study).
2 2 British Journal of Plastic Surgery The charts for these 19 patients were scrutinised, and the following information was recorded: name, identification number, gender, age, aetiology of injury, type of fracture, alphanumeric code of fracture, craniofacial disruption score, surgical treatment performed, presence or absence of associated injury, Glasgow Coma Score, CT findings, ophthalmological diagnosis, preoperative and postoperative visual acuities, and whether or not any ophthalmological treatment was performed. In addition, the CT scans of 15 out of the 19 patients were reviewed (the other four had been destroyed or reported missing), and a detailed analysis of each fractured bone was recorded for each patient. These were recorded using the minor codes of the CDFSS? The craniofacial disruption score was calculated as per the modification of the CDFSS described by O'Sullivan et al. 6 Briefly, this involves assigning a score to each bone or suture disrupted, depending on the severity of the injury, and totalling them as a percentage. All operations were carried out by consultant craniofacial or plastic surgeons, visiting craniofacial fellows, or advanced trainees in plastic and reconstructive surgery (under supervision). Our principles of operative management include early intervention, wide subperiosteal exposure of all fracture fragments, open reduction and internal fixation using low-profile titanium plates and screws, primary bone grafting where required, and avoidance of long-term intermaxillary fixation. Results Over the 11 year period, 2516 adult facial-fracture patients required surgical management. Of these, 317 (13%) had a recorded ophthalmological complication, of which 19 had severe visual impairment or blindness, as defined previously. There were 15 males and four females, giving a ratio of 3.75:1. The age range was years (mean: 39.8 years). The mean age for males was 43.0 years, and for females it was 27.8 years. Motor-vehicle accidents were the most common aetiology, accounting for nine cases. There were three assaults, three falls, one horse kick to the face, one aeroplane crash, one golf club to the face, and a tree fell on one patient. Eight of the 19 patients suffered multiple injuries in addition to their facial fractures, six suffered from other craniofacial injuries alone, and five had no other injuries (Table 1). The Glasgow Coma Scores were recorded on admission, and most patients had a score of 15 (Fig. 1). Craniofacial disruption scores ranged from 1 to 62 (mean: 15; median: 13). There were three patients with a craniofacial disruption score of 1 (Table 2). Two of these had suffered low-energy blunt injuries (one assault, one struck by a golf club), and each suffered an isolated displaced orbital-floor fracture. The third patient suffered an undisplaced fracture of the anterior wall of the left frontal sinus in a high-speed motor-vehicle accident. Unfortunately, he also had a penetrating eye injury, and, despite scleral repair, he achieved a postoperative visual acuity of only 6/36. The mean craniofacial disruption score was highest in those patients sustaining their injuries in motor-vehicle # 2 o t GC$ Figure 1---The Glasgow Coma Scores of the patients on admission. Table 1 Associated injuries Case Fracture Associated injuries 1 right orbital floor 2 naso-orbito-ethmoid, bilateral zygomas 3 right orbitozygoma, fight mandible 4 left zygoma 5 bilateral condyles, fight angle mandible 6 left orbitozygoma 7 left orbitozygoma 8 mandible 9 left fronto-orbitoethmoid 10 left frontal bone, left zygoma, left maxilla 11 right orbitozygoma, maxilla 12 frontal sinus 13 nasomaxillary, orbital rim 14 LeFort II, bilateral mandible 15 LeFort III 16 left orbital rim 17 LeFort I and III, right mandible 18 naso-orbito-ethmoid, right orbitozygoma 19 mandible, supraorbital bar fractured left tibia and bilateral fibulae, dislocated left humerus and elbow fractured fight humerus and fibula, fractured ribs and dislocated foot bilateral hearing loss and head lacerations left parietal haemorrhage and bilateral wrist fractures fractured ribs and C5, C6 and C7 penetrating facial and eye injury facial lacerations left orbital abscess skull fractures, bilateral subdural haematoma, fractured ribs and clavicles, and ear lacerations fractured C5 and facial lacerations fractured skull base and cerebral contusions fracture dislocation of the left shoulder, fractured ribs, tension pneumothorax fractured right femur, right tibia and right humerus, and cerebral contusions fractured skull base, cerebral contusion, right VIIth cranial nerve palsy, pulmonary contusion
3 Blindness and severe visual impairment in facial fractures 3 Table 2 CT findings and Craniofacial Disruption Score (CDS) Case CT findings CDS blowout fracture of the right orbital floor posteromedially, no canal fracture 1 fractures of the nasoethmoid, left lateral orbit, bilateral zygomas and anterior walls of the maxillae 28 fractures of the right zygoma, right maxilla, right orbital floor and right pterygoid plate 13 fractures of the left zygoma and posterolateral orbit, optic nerve intact, no canal fracture, anterolateral maxilla fracture on left 16 fractured medial orbital walls, bilateral fracture of the mandibular condyles, right angle and symphysis fractures 5 depressed fracture of the left antrum anterior wall, fractured nose, fracture of the left orbital floor inferomedially 3 fracture of the left zygoma and orbital floor 1 right temporal bone fracture into anterior cranial fossa, through lesser wing sphenoid, fractured right zygoma, right subcondylar and left parasymphyseal fractures 7 left frontal bone, orbital roof and ethmoid fractures, left optic canal fracture, left zygomatic arch and lateral wall antrum fractures 8 depressed frontal fracture, bilateral superior orbital rim and orbital roof fractures, left medial orbital fracture, bilateral maxillary fractures, parietal bone fracture, minimally displaced 62 multiple facial fractures, including bilateral orbital lateral walls, three walls right antrum, nasal bones, right zygomatic arch and roof of the right orbit 19 fracture of the anterior wall frontal sinus 1 fractures of the left orbital medial wall, left inferior orbital rim and left nasal bone 4 depressed left frontotemporal fracture and fractures of the right frontal bone and sinus, nasal bones, right orbital medial wall and left body of the mandible 31 naso-orbito-ethmoid fractures, bilateral midface fracture 23 fractured left zygoma, right temporal bone to petrous part including mastoids, bilateral sphenoid, lateral wall of left orbit, left pterygoid plate and multiple left zygomatic fractures 14 bilateral LeFort! and III fractures, right parasymphyseal fracture 30 fractured right orbitozygomatic complex and right frontal bone into sinus, no canal fracture 16 fractures of the floor of the anterior cranial fossa, right frontal bar, right temporal bone to external auditory canal, right clinoid, lateral wall of the right orbit, right zygomatic arch into temporomandibular joint CDS 10 0 Assault MVA Fall Other Aetiology CDS Multitrauma Craniofacial Nil Associated Injury Figure 3---The Craniofacial Disruption Scores of the patients according to the presence of associated injuries. Figure 2--The Craniofacial Disruption Scores of the patients according to aetiology. accidents, and in those who suffered multitrauma (Figs 2 and 3). In the 19 patients, there were a total of 148 fractures: 46 orbital (31%), 35 zygomatic (24%), 30 nasomaxillary (20%), 27 maxillary (18%) and 10 mandibular (7%) (Fig. 4). None of the mandibular fractures occurred in isolation. Each of the major fracture zones have been broken down into their individual minor zones, to give an indication of the numbers of individual bones fractured (Fig. 5A-E). The ophthalmological diagnoses were commonly traumatic optic neuropathy or globe rupture. The diagnoses of optic neuropathy usually received no specific Zygomatic 24% Nasomaxillary 20% Maxillary 18% Orbit Mandibular 31% 7% Figure 4~Facial fractures according to the major zones.
4 4 British Journal of Plastic Surgery Or~- - fl< 2! Inferior orbital rim 20% ial wall 3% Zygornatic arch 31% Orbital roof 9% Lateral wall A 29*. orbital rim 9% s~um B ~5~ Nasomaxillary Antedor ~hmoid Anterior wall Nasofrontal suture 13% ;e Jar bone C 37,/. exnmola 10% D 51% Pterygoid 4% plate 4% Mandibular symphysis Man~ ~dibular cor ~ody 50% 20% E Figure 5--Facial fractures according to the minor zones: (A) orbital major zone; (B) zygomatic major zone; (C) nasomaxillary major zone; (D) maxillary major zone; and (E) mandibular major zone. ophthalmological treatment. Ruptured globes underwent attempted surgical repair, enucleation or evisceration (Table 3). Follow-up lasted for 3 years postoperatively, depending on the type of fracture, complications and patient compliance. Ophthalmological follow-up OCCUlTed in conjunction with craniofacial follow-up, at a separate clinic. Discussion In presenting a study of 2516 adult facial-fracture patients, we acknowledge that a retrospective review of a database is fraught with problems: the database is totally dependent on the enthusiasm and accuracy with which it is recorded. Some patients will be unrecorded, some patients will have been lost to follow-up, or follow-up will be irregular. Various components of the database will have errors, due to inaccurate recording, inter-observer discrepancies and computer input error. Despite these acknowledged shortcomings, a sample size of 2516 patients is significant and compares well with other published series.1'4,6-8 We found that 317 out of the 2516 patients (13%) had an ocular complication. Other reports have noted an incidence ranging from 3.9% to 90.6%! 4,7-9 This extreme
5 Blindness and severe visual impairment in facial fractures Table 3 Ophthalmological findings and treatment Case Preoperative Postoperative Diagnosis Treatment visual acuity visual acuity 1 nil 5/60 retinal haemorrhage and optic nerve contusion nil 2 nil 6/24 ruptured globe scleral repair 3 nil 6/60 traumatic optic neuropathy and abducens palsy nil 4 nil nil traumatic optic neuropathy nil 5 light only 6/12, upper half traumatic optic neuropathy, 90% visual loss nil 6 6/36 6/60 traumatic macular hole nil 7 6/36 6/24 made nil 8 1/60 1/60 Purtcher's ischaemic retinopathy (traumatic optic neuropathy) nil 9 nil nil traumatic optic neuropathy secondary to optic canal fracture dexamethasone and prednisolone 10 nil nil ruptured left globe enucleation 11 count fingers nil ruptured right globe scleral repair, euucleation secondarily 12 count fingers 6/36 penetrating left eye injury scleral repair 13 nil nil retro-orbital abscess drainage of abscess 14 count fingers 1/60 left posterior pole haemorrhage, optic nerve infarct nil 15 nil nil ruptured left globe enucleation 16 nil 6/60 left optic atrophy (traumatic optic neuropathy) nil 17 nil nil ruptured left globe evisceration 18 nil 1/60 vitreoretinal haemorrhage nil 19 nil nil traumatic optic neuropathy nil range of incidence is due to the varied methods of reporting. Some prospective reports may yield a higher incidence of ocular complications, as suggested by Jabaley et al, who compared retrospective and prospective analyses of ocular injuries in orbital fractures, and showed a difference in incidence of 11% versus 29% in retrospective and prospective analyses, respectively. 1~ Other studies have been very selective in their cases. A1-Qurainy et al, who reported an incidence of 90.6%, selected mid-facial fractures only, excluding nasal-bone and mandibular fractures, and neurosurgical patients. 7 We felt that a much more useful approach would be to assess all facial fractures regardless of aetiology, site of fracture or associated injury, as this is how they present daily to a facial-trauma service. In our review, the incidence of blindness or severe visual impairment was 0.8% (19 patients of the 2516 in the study group). This compares with a previously published range of between 0.2% and 6%. t'7-9'11'12 Our male-to-female ratio was 3.5:1. This probably reflects the higher number of males involved in motor-vehicle accidents and assaultive behaviour. The mean age was higher for males (43.0 years) than for females (27.8 years); we do not have any explanation for this discrepancy. Motor-vehicle accident was the most common aetiology (47%), and 14 of the 19 patients (74%) suffered other injuries. These findings reflect the higher energies imparted to the facial skeleton in these patients, and one would expect a higher degree of damage, including an increased risk of ocular trauma. Analysis of the Glasgow Coma Scores revealed that most patients were admitted to hospital with a score of 15, implying a lack of serious brain injury in this group. This supports Le Fort's hypothesis that the process of facial fracturing absorbs energy, thereby preventing further transmission of traumatic forces to the brain. 13 The Craniofacial Disruption Scores ranged from 1 to 62, with a mean of 15. Because this study included all facial fractures, some of the patients with very low fracture scores (and therefore relatively insignificant fractures) had to be included. Two of the patients with a score of 1 had isolated displaced orbital-floor (blowout) fractures. The other patient with a score of 1 had a minimally displaced fracture of the anterior wall of the frontal sinus, but suffered a concurrent penetrating eye injury. This shows that even a relatively insignificant facial fracture can be associated with loss of vision, and the clinician must be alert to this possibility. With such a range of Craniofacial Disruption Scores represented, we were unable clinically to correlate the score with the occurrence of blindness or severe visual disturbance. The mean Craniofacial Disruption Score was highest in patients involved in motor-vehicle accidents, and in those who suffered multitrauma. Again, this would be expected due to the energy imparted to the facial skeleton and body during impact, compared with that imparted in an assault or fall. There were a total of 148 fractures in the 19 patients. This total includes sutural disruption, as per the CDFSS. 5 Sutural disruption is an integral part of this scoring system, as it allows a better quantification of the degree of force, and hence disruption, applied to the facial skeleton. Over half of the fractures (55%) were of the orbitozygomatic region. Analysis of the orbital major zone revealed the lateral orbital wall as the most frequently fractured region (29%). Along with the zygomaticomaxillary buttress, these were the most commonly fractured areas in the 19 patients (14 fractures in each zone). In the zygomatic major zone 35% of the fractures involved the zygomaticofrontal suture, and 31% were fractures of the arch. Hence, 66% of the zygomatic fractures resulted from lateral impacts, and this, combined with the high incidence of lateral-orbital-wall and zygomaticomaxillary (lateral) buttress fractures, implies a laterally directed force as a significant causative factor in these cases of blindness (Figs 6 and 7). Analysis of the maxillary major zone revealed over half (51%) of the fractures involved the zygomaticomaxillary buttress. Analysis of the nasomaxillary zone showed that 37% of the fractures involved the nasal bones. This is not surprising as the nasal bones are the most commonly
6 6 British Journal of Plastic Surgery Figure ~--Preoperative axial CT scan showing comminuted fractures of the right lateral and medial orbital walls. This is an 18-year-old woman who was involved in a motor-vehicle accident as a rear-seat passenger (case 18). She suffered multiple injuries; her visual loss was due to a posterior pole haemorrhage. No visual recovery occurred. Figure 7--Preoperative axial CT scan showing a comminuted fracture of the left lateral orbital wall and a nasoethmoidal fracture. This is an 81-year-old man who was involved in a motor-vehicle accident as a driver (case 15). He suffered LeFort III, C5 and nasoethmoidal fractures. Visual loss was due to a ruptured globe; he underwent enucleation, fractured facial bones, and cadaver studies have shown that nasal fractures occur at impact energies well below those of the other facial bones) 4 Analysis of the mandibular zone revealed that 50% of the fractures involved the condyle, although the total number of mandibular fractures was low. An association between lateral-orbital-wall fractures and blindness has been previously noted. 2,15 Jend and Jend-Rossmann reported sphenotemporal buttress fracturing in five cases, leading to amaurosis in allj 5 Their particular fracture pattern has certainly appeared in our series, and their suggestion that the radiologist and clinician pay particular attention to the presence of this fracture pattern is well noted. These findings contrast with those of Ioannides et al, who analysed 509 fractures over a 9 year period, s They had a total of 15 patients with loss of vision (2.9%), and concluded that patients with nasoethmoidoffontal fractures had a greater chance of being blinded than patients with other fractures. However, their study only assessed fractures involving the orbit. They also report a 26% incidence of ocular injury, yet exclude subconjunctival haemorrhage, corneal abrasion and retinal oedema from this group. The most frequent ophthalmological diagnosis in our series was traumatic optic neuropathy. There were seven patients with this diagnosis, five with a ruptured globe and three with retinal haemorrhage. The incidence of traumatic optic neuropathy following facial injury has been reported as 2%-3%, but it has been suggested that this incidence can be up to 15% if objective pupillary examination is undertaken. 9 Zachariades et al, in their 12 year review of 5936 patients, noted that, of their 19 blinded patients, retrobulbar haemorrhage was the most common cause of blindness. 1 In A1-Qurainy et al's series of selected mid-face fractures traumatic optic neuropathy was the cause of blindness in each instance. 7 The accuracy of the ophthalmological diagnoses will obviously differ from unit to unit and depend on the degree of initial ophthalmological input. Our findings support A1-Qurainy et al, in that traumatic neuropathy is more commonly found as the cause of blindness. Our second most common cause was ruptured globe. We had only one patient with an optic canal fracture (case 9). The patients with a diagnosis of traumatic optic neuropathy usually had no vision or worse than 6/60 visual acuity immediately after injury. In our series, the only one of these patients to be actively treated for his blindness was the patient in whom an optic canal fracture was diagnosed; he was treated with a standard course of highdose dexamethasone intravenously followed by a tapered course of prednisolone. The most common mechanisms thought to be the cause of optic neuropathy are haemorrhage into the optic-nerve sheath secondary to a shear effect, or contusion of the nerve with associated oedema and compression. This oedema would lead to secondary compromise of the microvascular supply to the nerve. 12 The use of steroid treatment is thought to decrease the microcirculatory spasm and oedema, in the hope of preventing nerve-cell compromise. However, it is felt that blindness occurring at the moment of injury has a very poor prognosis, 2 and, as it has been shown that irreversible ischaemic injury to the optic nerve may occur within 1-2h of injury, instituting a high-dose steroid regimen may well be futile unless the treatment is commenced immediately. The single case that we treated medically had an optic canal fracture (case 9). The decision at the time was not to attempt decompression of the canal, and steroid treatment was commenced to try to reduce the nerve oedema associated with the fracture. This patient's visual acuity on admission was nil, and he failed to recover any vision. With hindsight, it could be argued that a decompression procedure should have been attempted. However, the patient, aged 63 years, also had multiple facial and skull fractures, with intracerebral haemorrhage on one side,
7 Blindness and severe visual impairment in facial fractures 7 and may well not have tolerated a craniofacial procedure under general anaesthetic at the time. Five patients had a ruptured globe, and one patient (case 12) sustained a penetrating injury to the left eye. Three of these six patients underwent scleral repair by the ophthalmologist. In two of the three the visual acuity improved (cases 2 and 12); the third patient had no improvement and subsequently underwent enucleation. There is no question that an attempt should be made to salvage the damaged globe, if feasible. In this study, we have not addressed the situation where visual loss occurs after treatment of the facial fracture. Girotto et al report four cases of visual loss after operative treatment of facial fractures, and note that this is usually due to intraorbital haemorrhage, it An interesting study was published by Weymuller, who sought opinions from various experts from different specialties regarding the treatment of an acute LeFort III fracture with visual loss in one eye and a fracture involving the orbital apex on the remaining functional side) The majority of ophthalmologists and oral surgeons would not operate, the otolaryngologists were evenly split, and all of the plastic and reconstructive surgeons would operate. This implies that differing levels of training, expertise and philosophy are important factors in the management of these cases. In summary, we present an 11 year review of facial fractures causing blindness or severe visual loss. The typical patient was a male involved in a motor-vehicle accident, suffering multitrauma. The facial fractures usually involved a lateral impact to the orbitozygomatic region, with fractures involving the lateral orbital wall, zygomatic arch and zygomaticofrontal suture, and zygomaticomaxillary buttress. The cause of blindness was most commonly traumatic optic neuropathy, for which there was no specific treatment. The ruptured globe should undergo early surgical repair, if feasible. We recommend that the clinician managing these patients be alert to the possibility of ophthalmological compromise, no matter how seemingly insignificant the fracture. As shown by our results, special caution should be exercised in managing lateral impact-type fractures, and early identification of these fracture patterns by CT scan can alert the clinician to the possibility of severe visual impairment. Visual assessment is mandatory in these patients. From this series, the Craniofacial Disruption Score, calculated using the modified CDFSS, was not correlated with the occurrence of blindness or severe visual impairment. Acknowledgements The authors thank Mr M. Hammerton FRACS, FRACO, Consultant Ophthalmologist, The Australian Craniofacial Unit, for his advice in the preparation of this manuscript, and the research and secretarial staff of the Department of Plastic and Reconstructive Surgery, Royal Adelaide Hospital, for their assistance with data collection and retrieval. References 1. Zachariades N, Papavassiliou D, Christopoulos E Blindness after facial trauma. Oral Surg Oral Med Oral Pathoi 1996; 81: Lipkin AE Woodson GE, Miller RH. Visual loss due to orbital fracture: the role of early reduction. Arch Otolaryngol Head Neck Surg 1987; 113: Weymuller EA Jr. Blindness and LeFort IlI-fractures. Ann Otol Rhinol Laryngol 1984; 93: Lira LH, Lain LK, Moore MH, Trott JA, David DJ. Associated injuries in facial fractures: review of 839 patients. Br J Plast Surg 1993; 46: Cooter RD, David DJ. Computer-based coding of fractures in the craniofacial region. Br J Plast Surg 1989; 42: O'Sullivan ST, Snyder BJ, Moore MH, David DJ. Outcome measurement of the treatment of maxillary fractures: a prospective analysis of 100 consecutive cases. Br J Plast Surg 1999; 52: A1-Qurainy IA, Stassen LFA, Dutton GN, Moos KF, El-Attar A. The characteristics of midfacial fractures and the association with ocular injury: a prospective study. Br J Oral Maxillofac Surg 1991; 29: Ioannides C, Treffers W, Rutten M, Noverraz E Ocular injuries associated with fractures involving the orbit. J Craniomaxillofac Surg 1988; 16: Li KK, Teknos TN, Lauretano A, Joseph MR Traumatic optic neuropathy complicating facial fracture repair. J Craniofac Snrg 1997; 8: Jabaley ME, Lerman M, Sanders HJ. Ocular injuries in orbital fractures: a review of 119 cases. Plast Reconstr Surg 1975; 56: Girotto JA, Gamble WB, Robertson B, et al. Blindness after reduction of facial fractures. Plast Reconstr Surg 1998; 102: Manfredi SJ, Raji MR, Sprinkle PM, Weinstein GW, Minardi LM, Swanson TJ. Computerized tomographic scan findings in facial fractures associated with blindness. Plast Reconstr Surg 1981; 68: LeFort R. Etude experimentale sur les fractures de la machoire superieure. Rev Chir Paris 1901; 23: 208,360, David DJ, Simpson DA. Craniomaxillofacial Trauma. New York: Churchill Livingstone, 1995: Jend H-H, Jend-Rossmann I. Sphenotemporal buttress fracture: a report of five cases. Neuroradiology 1984; 26: The Authors Craig A. MaeKinnon MB, ChB, FRACS, Honorary Clinical Associate of the University of Hong Kong Department of Surgery, Level $3, Queen Mary Hospital, 102 Pokfulam Road, Pokfulam, Hong Kong. David J. David AC, MD, FRCS, FRACS, Head Australian Craniofacial Unit, Women and Children's Hospital, 72 King William Road, North Adelaide, South Australia 5006, Australia. Rodney D. Cooter MBBS, MD, FRACS, Head of Unit Department of Plastic and Reconstructive Surgery, Royal Adelaide Hospital, Adelaide, South Australia, Australia. Correspondence to Mr David J. David AC, MD, FRCS, FRACS. Paper received 12 January Accepted 24 September 2001, after revision.
CT of Maxillofacial Injuries
 CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
CT of Maxillofacial Injuries Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology changes the diagnosis Technologic Evolution
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
CT of Maxillofacial Fracture Patterns. CT of Maxillofacial Fracture Patterns
 CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
CT of Maxillofacial Fracture Patterns CT of Maxillofacial Fracture Patterns Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Viking 1 1976 MGS 2001 Technology
Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
 Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
Functional structure of the skull and Fractures of the skull Thickened and thinner parts of the skull = important base for understanding of the functional structure of the skull - the transmission of masticatory
MAXILLOFACIAL TRAUMA. The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital
 MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
MAXILLOFACIAL TRAUMA The on-call maxillofacial surgeons can be contacted through the switchboard at the Southern General Hospital Mandibular Injuries Mechanism of injury Assault, falls, RTA-Direct trauma
Maxillofacial Injuries Practical Tips
 Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
Saturday, October 29, 2016 Maxillofacial Injuries Practical Tips Suyash Mohan MD, PDCC THE ROOTS OF PENN RADIOLOGY RADIOLOGICAL Assistant Professor of Radiology Assistant Professor of Neurosurgery Neuroradiology
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Facial and Temporal Bone Trauma Diagnostic imaging and therapeutic challenges in emergency
 Facial and Temporal Bone Trauma Diagnostic imaging and therapeutic challenges in emergency ATTYE A, KRAINIK A Department of Neuroradiology and MRI University Hospital Grenoble / University Grenoble Alpes
Facial and Temporal Bone Trauma Diagnostic imaging and therapeutic challenges in emergency ATTYE A, KRAINIK A Department of Neuroradiology and MRI University Hospital Grenoble / University Grenoble Alpes
TRAUMA TO THE FACE AND MOUTH
 Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Dr.Yahya A. Ali 3/10/2012 F.I.C.M.S TRAUMA TO THE FACE AND MOUTH Bailey & Love s 25 th edition Injuries to the orofacial region are common, but the majority are relatively minor in nature. A few are major
Facial Trauma. Facial Trauma. Facial Trauma
 Facial Trauma Facial Trauma Brian Bast DMD, MD Department of Oral and Maxillofacial Surgery University of California, San Francisco School of Dentistry Brian Bast DMD, MD Department of Oral and Maxillofacial
Facial Trauma Facial Trauma Brian Bast DMD, MD Department of Oral and Maxillofacial Surgery University of California, San Francisco School of Dentistry Brian Bast DMD, MD Department of Oral and Maxillofacial
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
ORIGINAL ARTICLE. Facial Fracture Classification According to Skeletal Support Mechanisms
 ORIGINAL ARTICLE Facial Fracture Classification According to Skeletal Support Mechanisms Terry L. Donat, MD; Carmen Endress, MD; Robert H. Mathog, MD Objective: To construct, propose, and evaluate the
ORIGINAL ARTICLE Facial Fracture Classification According to Skeletal Support Mechanisms Terry L. Donat, MD; Carmen Endress, MD; Robert H. Mathog, MD Objective: To construct, propose, and evaluate the
Maxillofacial and Ocular Injuries
 Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Maxillofacial and Ocular Injuries Objectives At the conclusion of this presentation the participant will be able to: Identify the key anatomical structures of the face and eye and the impact of force on
Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI. Monitor the vital signs. Monitor the vital signs. Complications of Facial Traumas.
 Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Complications of Facial Traumas 1) Immediate Complications 2) Late Complications Dr. Esam Ahmad Z. Omar BDS, MSc-OMFS, FFDRCSI Assistant Professor Oral & Maxillofacial Surgeon Taibah University Monitor
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
ZYGOMATIC (MALAR) FRACTURES
 b854_chapter-12.qxd 1/31/2011 9:40 AM Page 129 ZYGOMATIC (MALAR) FRACTURES CHAPTER 12 Anatomical articulations FZ Fronto-zygomatic ZT Zygomaticotemporal ZMB Zygomatico - maxillary buttress IO Infraorbital
b854_chapter-12.qxd 1/31/2011 9:40 AM Page 129 ZYGOMATIC (MALAR) FRACTURES CHAPTER 12 Anatomical articulations FZ Fronto-zygomatic ZT Zygomaticotemporal ZMB Zygomatico - maxillary buttress IO Infraorbital
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #1 Facial Trauma The face is vital to human appearance and function. Facial injuries can impair a patient
Successful Treatment of the Traumatic Orbital Apex Syndrome due to Direct Bone Compression
 318 Case Report Successful Treatment of the Traumatic Orbital Apex Syndrome due to Direct Bone Compression Atsushi Imaizumi, MD 1 Kunihiro Ishida, MD 1 Yasunari Ishikawa, MD 2 Izuru Nakayoshi, MD 3 1 Department
318 Case Report Successful Treatment of the Traumatic Orbital Apex Syndrome due to Direct Bone Compression Atsushi Imaizumi, MD 1 Kunihiro Ishida, MD 1 Yasunari Ishikawa, MD 2 Izuru Nakayoshi, MD 3 1 Department
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line.
 Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Lesson Plans and Objectives: Review material for article Prep work for article Picture recovery Review for placement on-line. After reading the article, the staff will be able to: Define facial trauma
Maxillary and Periorbital Fractures January 2004
 TITLE: Maxillary and Periorbital Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 7, 2004 RESIDENT PHYSICIAN: Gordon Shields, MD FACULTY ADVISOR: Francis B. Quinn,
TITLE: Maxillary and Periorbital Fractures SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 7, 2004 RESIDENT PHYSICIAN: Gordon Shields, MD FACULTY ADVISOR: Francis B. Quinn,
Computed-Tomography of maxillofacial fractures: What do surgeons want to know?
 Computed-Tomography of maxillofacial fractures: What do surgeons want to know? Poster No.: C-0968 Congress: ECR 2016 Type: Educational Exhibit Authors: A. Ammar, M. Jrad, I. KASRAOUI, A. Zoubli, H. Mizouni
Computed-Tomography of maxillofacial fractures: What do surgeons want to know? Poster No.: C-0968 Congress: ECR 2016 Type: Educational Exhibit Authors: A. Ammar, M. Jrad, I. KASRAOUI, A. Zoubli, H. Mizouni
Diagnosis of Midface Fractures with CT: What the Surgeon Needs to Know 1
 Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. EDUCATION EXHIBIT
Note: This copy is for your personal non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, contact us at www.rsna.org/rsnarights. EDUCATION EXHIBIT
Orbit Fractures: Identifying Patient Factors Indicating High Risk for Ocular and Periocular Injury
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Orbit Fractures: Identifying Patient Factors Indicating High Risk for
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Orbit Fractures: Identifying Patient Factors Indicating High Risk for
Downloaded from Medico Research Chronicles Assault injury to the face with an axe- A rare case report.
 ISSN No. 2394-3971 Case Report ASSAULT INJURY TO THE FACE WITH AN AXE- A RARE CASE REPORT Dr Sandhya K 1, Dr Bobby John 2, Dr Shobitha G 3 1 Senior resident, Department of Oral and Maxillofacial Surgery,
ISSN No. 2394-3971 Case Report ASSAULT INJURY TO THE FACE WITH AN AXE- A RARE CASE REPORT Dr Sandhya K 1, Dr Bobby John 2, Dr Shobitha G 3 1 Senior resident, Department of Oral and Maxillofacial Surgery,
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S.
 THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
THE TRIPARTITE OSTEOTOMY OF THE MID-FACE FOR ORBITAL EXPANSION AND CORRECTION OF THE DEFORMITY IN CRANIOSTENOSIS By JOHN MARQUIS CONVERSE, M.D., and DAUBERT TELSEY, D.D.S. Center for Craniofacial Anomalies
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
ISSN X (Print) Research Article. *Corresponding author Ali Mortazavi,
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(4C):1760-1764 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(4C):1760-1764 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Facial Trauma ASHNR. Disclosures: Acknowledgments: None. Edward P. Quigley, III, MD PhD University of Utah
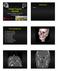 Disclosures: Facial Trauma ASHNR Edward P. Quigley, III, MD PhD University of Utah None Acknowledgments: Dr. Rebecca Cornelius Dr. Ilona M. Schmalfuss Dr. Richard Wiggins III Dr. Yoshimi Anzai Dr. Lindell
Disclosures: Facial Trauma ASHNR Edward P. Quigley, III, MD PhD University of Utah None Acknowledgments: Dr. Rebecca Cornelius Dr. Ilona M. Schmalfuss Dr. Richard Wiggins III Dr. Yoshimi Anzai Dr. Lindell
AXIAL SKELETON SKULL
 AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
Current concepts in midface fracture management
 REVIEW C URRENT OPINION Current concepts in midface fracture management AQ1 Alf L. Nastri and Ben Gurney AQ4 Purpose of review Management of midface trauma is complex and challenging and requires a clear
REVIEW C URRENT OPINION Current concepts in midface fracture management AQ1 Alf L. Nastri and Ben Gurney AQ4 Purpose of review Management of midface trauma is complex and challenging and requires a clear
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Cranium Facial bones. Sternum Rib
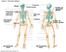 Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Major Anatomic Components of the Orbit
 Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Orbital cellulitis. Archives of Emergency Medicine, 1992, 9,
 Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Archives of Emergency Medicine, 1992, 9, 143-148 Orbital cellulitis D. P. MARTIN-HIRSCH, S. HABASHI, A. H. HINTON & B. KOTECHA University Department of ENT Surgery, Manchester Royal Infirmary, Manchester
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
MRI masterfile Part 5 WM Heme Strokes.ppt 1
 Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Ocular and Orbital Trauma Eye Trauma: Incidence 1.3 million eye injuries in the US per year. 40,000 of these injuries lead to blindness in the US. Patrick Sibony, MD March 23, 2013 Ophthalmic Emergencies
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
The diagnostic value of Computed Tomography in evaluation of maxillofacial Trauma
 The diagnostic value of Computed Tomography in evaluation of maxillofacial Trauma Qais H. Muassa FICMS College of Dentistry, Babylon University Ibrahim S. Gataa, BDS, FICMS College of Dentistry, Sulaimania
The diagnostic value of Computed Tomography in evaluation of maxillofacial Trauma Qais H. Muassa FICMS College of Dentistry, Babylon University Ibrahim S. Gataa, BDS, FICMS College of Dentistry, Sulaimania
A New Classification of Zygomatic Fracture Featuring Zygomaticofrontal Suture: Injury Mechanism and a Guide to Treatment
 IBIMA Publishing Plastic Surgery: An International Journal http://www.ibimapublishing.com/journals/psij/psij.html Vol. 2013 (2013), Article ID 383486, 6 pages DOI: 10.5171/2013.383486 Research Article
IBIMA Publishing Plastic Surgery: An International Journal http://www.ibimapublishing.com/journals/psij/psij.html Vol. 2013 (2013), Article ID 383486, 6 pages DOI: 10.5171/2013.383486 Research Article
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
APPENDICULAR SKELETON 126 AXIAL SKELETON SKELETAL SYSTEM. Cranium. Skull. Face. Skull and associated bones. Auditory ossicles. Associated bones.
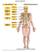 SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
Introduction to Local Anesthesia and Review of Anatomy
 5-Sep Introduction and Anatomy Review 12-Sep Neurophysiology and Pain 19-Sep Physiology and Pharmacology part 1 26-Sep Physiology and Pharmacology part 2 Introduction to Local Anesthesia and Review of
5-Sep Introduction and Anatomy Review 12-Sep Neurophysiology and Pain 19-Sep Physiology and Pharmacology part 1 26-Sep Physiology and Pharmacology part 2 Introduction to Local Anesthesia and Review of
Orbital Roof Fractures: A Clinically Based Classification and Treatment Algorithm
 198 Original Article Orbital Roof Fractures: A Clinically Based Classification and Treatment Algorithm Felicity Victoria Connon, MBBS, BMedSc 1,2 S. J. B. Austin, MBBS, BMedSc, BDSc 1 A. L. Nastri, MBBS,
198 Original Article Orbital Roof Fractures: A Clinically Based Classification and Treatment Algorithm Felicity Victoria Connon, MBBS, BMedSc 1,2 S. J. B. Austin, MBBS, BMedSc, BDSc 1 A. L. Nastri, MBBS,
External Acoustic Meatus. Mastoid Process. Zygomatic Process. Temporal Bone
 Bone lab review 1. Frontal Bone 2. Supra-Orbital Foramen 3. Orbit (Orbital Cavity) 4. Superior Orbital Fissure 5. Inferior Orbital Fissure 6. Zygomatic Bone 7. Infra-Orbital Foramen 8. Maxilla 9. Mandible
Bone lab review 1. Frontal Bone 2. Supra-Orbital Foramen 3. Orbit (Orbital Cavity) 4. Superior Orbital Fissure 5. Inferior Orbital Fissure 6. Zygomatic Bone 7. Infra-Orbital Foramen 8. Maxilla 9. Mandible
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
MRI masterfile Part 5 WM Heme Strokes.ppt 2
 Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Imaging of Orbital Trauma Corneal Abrasion CT scan is preferable to MRI Bone, Rapid, Easy to monitor patient Foreign bodies, air, hemorrhage Fractures Cost Needed for an MRI MRI Globe and intraocular injuries
Midface fractures; what the radiologist should know.
 Midface fractures; what the radiologist should know. Poster No.: C-1056 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Garcia Villanego, E.-M. Heursen, A. Rodriguez Piñero; Cadiz/ES Keywords:
Midface fractures; what the radiologist should know. Poster No.: C-1056 Congress: ECR 2013 Type: Educational Exhibit Authors: J. Garcia Villanego, E.-M. Heursen, A. Rodriguez Piñero; Cadiz/ES Keywords:
The Skull DANIL HAMMOUDI.MD
 The Skull DANIL HAMMOUDI.MD summary of bones/structures in Chapter 15 of the manual need tp be print as soon as possible http://www.mnsu.edu/emuseum/biology/humananatomy/skeletal/skul l/frontal/frontal.html
The Skull DANIL HAMMOUDI.MD summary of bones/structures in Chapter 15 of the manual need tp be print as soon as possible http://www.mnsu.edu/emuseum/biology/humananatomy/skeletal/skul l/frontal/frontal.html
Hong Kong College of Emergency Medicine OSCE July 2010
 Case 1 A 70 year old gentleman was taking warfarin for his past history of right leg deep vein thrombosis. He slipped and fell and suffered from head injury. He was sent to A&E and his GCS was 9/15 on
Case 1 A 70 year old gentleman was taking warfarin for his past history of right leg deep vein thrombosis. He slipped and fell and suffered from head injury. He was sent to A&E and his GCS was 9/15 on
Blow-in fracture of both orbital roofs caused by shear strain to the skull. Department of Neurosurgery, Kanto Teishin Hospital, Tokyo, Japan
 J Neurosurg 49:734-738, 1978 Blow-in fracture of both orbital roofs caused by shear strain to the skull Case report OSAMU SATO, M.D., HIROSHI KAMITANI, M.D., AND TAKASHI KOKUNAI, M.D. Department of Neurosurgery,
J Neurosurg 49:734-738, 1978 Blow-in fracture of both orbital roofs caused by shear strain to the skull Case report OSAMU SATO, M.D., HIROSHI KAMITANI, M.D., AND TAKASHI KOKUNAI, M.D. Department of Neurosurgery,
JMSCR Vol 05 Issue 05 Page May 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i5.134 Reconstruction of Orbital Roof Fracture
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i5.134 Reconstruction of Orbital Roof Fracture
MANAGEMENT OF ZYGOMATICO-ORBITAL FRACTURES USING RIGID INTERNAL FIXATION WITH COSMETIC SURGICAL CONSIDERATIONS - CASE REPORT
 MANAGEMENT OF ZYGOMATICO-ORBITAL FRACTURES USING RIGID INTERNAL FIXATION WITH COSMETIC SURGICAL CONSIDERATIONS - CASE REPORT Ong ARM. Management of zygomatico-orbital fracturers using rigid internal fixation
MANAGEMENT OF ZYGOMATICO-ORBITAL FRACTURES USING RIGID INTERNAL FIXATION WITH COSMETIC SURGICAL CONSIDERATIONS - CASE REPORT Ong ARM. Management of zygomatico-orbital fracturers using rigid internal fixation
Pediatric Craniofacial Injuries: Concept of Treatment
 Med. J. Cairo Univ., Vol. 83, No. 1, March: 217-224, 201 5 www.medicaljournalofcairouniversity.net Pediatric Craniofacial Injuries: Concept of Treatment FAWZY T. AL-SAYED, Ph.D.* and MOHAMAD A. SHOEIB,
Med. J. Cairo Univ., Vol. 83, No. 1, March: 217-224, 201 5 www.medicaljournalofcairouniversity.net Pediatric Craniofacial Injuries: Concept of Treatment FAWZY T. AL-SAYED, Ph.D.* and MOHAMAD A. SHOEIB,
MEDICAL CODING FOR FACIAL INJURIES & RECONSTRUCTION
 MEDICAL CODING FOR FACIAL INJURIES & RECONSTRUCTION Tirbod Fattahi, MD, DDS, FACS Chief & Associate Professor Division of Oral & Maxillofacial Surgery University of Florida Health Science Center, Jacksonville
MEDICAL CODING FOR FACIAL INJURIES & RECONSTRUCTION Tirbod Fattahi, MD, DDS, FACS Chief & Associate Professor Division of Oral & Maxillofacial Surgery University of Florida Health Science Center, Jacksonville
Research Article Factors Associated with Significant Ocular Injury in Conservatively Treated Orbital Fractures
 Hindawi Publishing Corporation Journal of Ophthalmology Volume 2014, Article ID 412397, 6 pages http://dx.doi.org/10.1155/2014/412397 Research Article Factors Associated with Significant Ocular Injury
Hindawi Publishing Corporation Journal of Ophthalmology Volume 2014, Article ID 412397, 6 pages http://dx.doi.org/10.1155/2014/412397 Research Article Factors Associated with Significant Ocular Injury
Bone Flashcards for 10a
 Bone Flashcards for 0a CLAVICLE (collar bone). Sternal extremity (end) flat end. Acromial extremity (end) rounded end. SCAPULA (shoulder blade). Right or left scapula?. Superior border (superior margin).
Bone Flashcards for 0a CLAVICLE (collar bone). Sternal extremity (end) flat end. Acromial extremity (end) rounded end. SCAPULA (shoulder blade). Right or left scapula?. Superior border (superior margin).
MDJ Zygomatic complex fractures: a 5-year retrospective study Vol.:8 No.:3 2011
 MDJ Zygomatic complex fractures: a 5-year retrospective study Dr. Thair Abdul Lateef B.D.S., H.D.D., F.I.B.M.S. * Dr.Jamal A. Mohammed B.D.S., M.Sc. * Abstract The aim of this descriptive analytic retrospective
MDJ Zygomatic complex fractures: a 5-year retrospective study Dr. Thair Abdul Lateef B.D.S., H.D.D., F.I.B.M.S. * Dr.Jamal A. Mohammed B.D.S., M.Sc. * Abstract The aim of this descriptive analytic retrospective
Facial skeletal fractures are common,
 CE This symbol indicates that there is more content in the online version of this article. Computed Tomography of Facial Fractures Bryant Furlow, BA Facial skeletal fractures are common, potentially serious,
CE This symbol indicates that there is more content in the online version of this article. Computed Tomography of Facial Fractures Bryant Furlow, BA Facial skeletal fractures are common, potentially serious,
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The upper buccal sulcus approach, an alternative for post-trauma rhinoplasty
 British Journal of Plastic Surgery (2003), 56, 218 223 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00117-6 The
British Journal of Plastic Surgery (2003), 56, 218 223 q 2003 The British Association of Plastic Surgeons. Published by Elsevier Science Ltd. All rights reserved. doi:10.1016/s0007-1226(03)00117-6 The
The impact-absorbing effects of facial fractures in closed-head injuries
 J Neurosurg66:542-547, 1987 The impact-absorbing effects of facial fractures in closed-head injuries An analysis of 2 l0 patients K. FRANCIS LEE, M.D., LOUS K. WAGNER~ PH.D., Y. EUGENIA LEE, M.D., JUNG
J Neurosurg66:542-547, 1987 The impact-absorbing effects of facial fractures in closed-head injuries An analysis of 2 l0 patients K. FRANCIS LEE, M.D., LOUS K. WAGNER~ PH.D., Y. EUGENIA LEE, M.D., JUNG
Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES
 DOI: 10.15386/cjmed-601 Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES RALUCA ROMAN 1, MIHAELA HEDEȘIU 1, FLOAREA
DOI: 10.15386/cjmed-601 Original Research THE USE OF REFORMATTED CONE BEAM CT IMAGES IN ASSESSING MID-FACE TRAUMA, WITH A FOCUS ON THE ORBITAL FLOOR FRACTURES RALUCA ROMAN 1, MIHAELA HEDEȘIU 1, FLOAREA
Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle
 Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
Case Report: Conventional radiograph verses CT for evaluation of sagittal fracture of mandibular condyle Dr Anjali Wadhwa, Dr Gaurav Shah, Dr Shweta Sharma, Dr Anand Bhatnagar, Dr Pallavi Malaviya NIMS
in compact bone, large vertical canals carrying blood vessels and nerves. in compact bone, large horizontal canals carrying blood vessels and nerves.
 Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Carl Christensen, PhD Skeletal System (Bones`) Bio. 2304 Human Anatomy 1. Identify a term for each of the following: shaft of a long bone ends of a long bone ossified remnant of the "growth plate" connective
Skeletal System -Axial System. Chapter 7 Part A
 Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
Use of Intraoperative Computed Tomography for Revisional Procedures in Patients with Complex Maxillofacial Trauma
 Use of Intraoperative Computed Tomography for Revisional Procedures in Patients with Complex Maxillofacial Trauma The Harvard community has made this article openly available. Please share how this access
Use of Intraoperative Computed Tomography for Revisional Procedures in Patients with Complex Maxillofacial Trauma The Harvard community has made this article openly available. Please share how this access
Anatomy images for MSS practical exam- 2019
 Anatomy images for MSS practical exam- 2019 Ilium Ischium Pubis Acetabulaum Iliac crest Iliac tubercle ASIS (muscle and ligament attached) AIIS (muscle attached) PSIS PIIS Ischial spine Ischial tuberosity
Anatomy images for MSS practical exam- 2019 Ilium Ischium Pubis Acetabulaum Iliac crest Iliac tubercle ASIS (muscle and ligament attached) AIIS (muscle attached) PSIS PIIS Ischial spine Ischial tuberosity
Biology 218 Human Anatomy. Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division
 Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
DR. SAAD AL-MUHAYAWI, M.D., FRCSC. ORL Head & Neck Surgery
 TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
BONE CHALLENGE DANIL HAMMOUDI.MD
 BONE CHALLENGE DANIL HAMMOUDI.MD Bone Basic functions? A. support B. protection C. movement assistance in D. RBC formation-hemopoiesis E. mineral homeostasis +importance of calcium F. energy supply -yellow
BONE CHALLENGE DANIL HAMMOUDI.MD Bone Basic functions? A. support B. protection C. movement assistance in D. RBC formation-hemopoiesis E. mineral homeostasis +importance of calcium F. energy supply -yellow
BIO 137 AXIAL SKELETON BONE STUDY THE HUMAN SKELETON
 BIO 137 THE AXIAL SKELETON MARY CATHERINE FLATH, Ph.D. THE HUMAN SKELETON AXIAL SKULL HYOID THORACIC CAGE VERTEBRAL COLUMN APPENDICULAR PECTORAL GIRDLE UPPER LIMBS PELVIC GIRDLE LOWER LIMBS AXIAL SKELETON
BIO 137 THE AXIAL SKELETON MARY CATHERINE FLATH, Ph.D. THE HUMAN SKELETON AXIAL SKULL HYOID THORACIC CAGE VERTEBRAL COLUMN APPENDICULAR PECTORAL GIRDLE UPPER LIMBS PELVIC GIRDLE LOWER LIMBS AXIAL SKELETON
Skeletal system. Prof. Abdulameer Al-Nuaimi. E. mail:
 Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
Skeletal system Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Functions of Bone and The Skeletal System Support: The skeleton serves as the structural framework
Human Anatomy - Problem Drill 06: The Skeletal System Axial Skeleton & Articualtions
 Human Anatomy - Problem Drill 06: The Skeletal System Axial Skeleton & Articualtions Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper
Human Anatomy - Problem Drill 06: The Skeletal System Axial Skeleton & Articualtions Question No. 1 of 10 Instructions: (1) Read the problem and answer choices carefully, (2) Work the problems on paper
Quantitative Determination of
 The Application of 3D Images for Quantitative Determination of Zygoma in an Asian Population Shih-Hsuan Mao, Yu-Hsuan Hsieh, Chih-Hao Chen, Chien-Tzung Chen Department of Plastic and Reconstructive Surgery,
The Application of 3D Images for Quantitative Determination of Zygoma in an Asian Population Shih-Hsuan Mao, Yu-Hsuan Hsieh, Chih-Hao Chen, Chien-Tzung Chen Department of Plastic and Reconstructive Surgery,
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. Railway accidents injured pedal cyclist
 Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Supplementary Table 1. ICD-9/-10 codes used to identify cycling injury hospitalizations. ICD Code ICD-9 E800-E807(.3) E810-E816, E818-E819(.6) E820-E825(.6) E826-E829(.1) ICD-10-CA V10-V19 (including all
Nasal Orbital Ethmoid (NOE) Fractures November, 2014
 TITLE: Nasal Orbital Ethmoid (NOE) Fractures SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch at Galveston, Department of Otolaryngology DATE: November 19, 2014 RESIDENT PHYSICIAN:
TITLE: Nasal Orbital Ethmoid (NOE) Fractures SOURCE: Grand Rounds Presentation, The University of Texas Medical Branch at Galveston, Department of Otolaryngology DATE: November 19, 2014 RESIDENT PHYSICIAN:
ISOLATED ZYGOMATIC BONE FRACTURE; MANAGEMENT BY THREE POINT FIXATION
 The Professional Medical Journal 1. BDS, FCPS 2. BDS, FCPS 3. BDS, MSc Community Dentistry 4. BDS, MSc (Trainee) 5. MBBS, FRCS Associate Professor General Surgery LUMHS, Correspondence Address: Dr. Suneel
The Professional Medical Journal 1. BDS, FCPS 2. BDS, FCPS 3. BDS, MSc Community Dentistry 4. BDS, MSc (Trainee) 5. MBBS, FRCS Associate Professor General Surgery LUMHS, Correspondence Address: Dr. Suneel
Endoscopic transnasal orbital decompression for thyrotoxic orbitopathy
 Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Key words: Endoscopes; Exophthalmos; Keratitis; Orbital diseases; Thyrotoxicosis "# " APW Yuen KYW Kwan E Chan AWC Kung KSL Lam Hong Kong Med J 2002;8:406-10 Queen Mary Hospital, 102 Pokfulam Road, Hong
Learn Connect Succeed. JCAHPO Regional Meetings 2017
 Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
Learn Connect Succeed JCAHPO Regional Meetings 2017 Financial Disclosure Evaluation and Treatment of Orbital Cellulitis Thomas E. Johnson, M.D. Bascom Palmer Eye Institute University of Miami School of
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section. REVIEW SHEET Exercise 10 Axial Skeleton
 ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
ANATOMY & PHYSIOLOGY I Laboratory Version B Name Section REVIEW SHEET Exercise 10 Axial Skeleton 1 POINT EACH. THE SKULL MULTIPLE CHOICE 1. The major components of the axial skeleton include the 7. The
Management of Craniofacial injuries
 Management of Craniofacial injuries Plastic and Reconstructive Surgery Cirujanos PlástiKos Mundi Cranio-Facial Trauma 1. Introduction Cranio-facial trauma is as old as the human race. What has changed
Management of Craniofacial injuries Plastic and Reconstructive Surgery Cirujanos PlástiKos Mundi Cranio-Facial Trauma 1. Introduction Cranio-facial trauma is as old as the human race. What has changed
UNIT 4 - SKELETAL SYSTEM LECTURE NOTES
 UNIT 4 - SKELETAL SYSTEM LECTURE NOTES 4.01 FUNCTIONS OF THE SKELETAL SYSTEM A. Support 1. Provides a framework for the body 2. Supports soft tissue 3. Serves as a point of attachment for ligaments, tendons,
UNIT 4 - SKELETAL SYSTEM LECTURE NOTES 4.01 FUNCTIONS OF THE SKELETAL SYSTEM A. Support 1. Provides a framework for the body 2. Supports soft tissue 3. Serves as a point of attachment for ligaments, tendons,
Chapter 7: Skeletal System: Gross Anatomy
 Chapter 7: Skeletal System: Gross Anatomy I. General Considerations A. How many bones in an average adult skeleton? B. Anatomic features of bones are based on II. Axial Skeleton A. Skull 1. Functionally
Chapter 7: Skeletal System: Gross Anatomy I. General Considerations A. How many bones in an average adult skeleton? B. Anatomic features of bones are based on II. Axial Skeleton A. Skull 1. Functionally
Technique Guide. Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures.
 Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Technique Guide Titanium Wire with Barb and Needle. Surgical Technique Guide for Canthal Tendon Prodecures. Indications/Features Indications The Synthes Titanium Wire with Barb and straight Needle is
Skull-2. Norma Basalis Interna. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Malignant growth Maxilla management an analysis
 ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
ISSN: 2250-0359 Volume 3 Issue 2 2013 Malignant growth Maxilla management an analysis *Balasubramanian Thiagarajan *Geetha Ramamoorthy *Stanley Medical College Abstract: Malignant tumors involving maxilla
Bones of the Skull Lateral View
 Bones of the Skull Lateral View Frontal Bone Parietal Bone Occipital Bone Temporal Bone Sphenoid Bone Pterion Sutures of the Skull Lateral View Coronal Suture Lambdoid Suture Squamous Suture Sutures of
Bones of the Skull Lateral View Frontal Bone Parietal Bone Occipital Bone Temporal Bone Sphenoid Bone Pterion Sutures of the Skull Lateral View Coronal Suture Lambdoid Suture Squamous Suture Sutures of
locomotice system Plastinated specimensⅠ: Silicone specimens Regional specimens and organs
 locomotice system Plastinated specimensⅠ: Silicone specimens Regional specimens and organs Art-No. Name Description The locomotor system SL001 Two hundred pieces of plastinated bones (without six The bones
locomotice system Plastinated specimensⅠ: Silicone specimens Regional specimens and organs Art-No. Name Description The locomotor system SL001 Two hundred pieces of plastinated bones (without six The bones
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA
 SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
University of Palestine. Midterm Exam 2013/2014 Total Grade:
 Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
Head and Neck Trauma. Disclosures: Acknowledgments: Introductory case. None
 Head and Neck Trauma None Disclosures: Edward P. Quigley III MD PhD Radiology and Imaging Sciences University of Utah Dr. Richard Wiggins III Dr. Yoshimi Anzai Dr. Lindell Gentry Dr. Blair Winegar Dr.
Head and Neck Trauma None Disclosures: Edward P. Quigley III MD PhD Radiology and Imaging Sciences University of Utah Dr. Richard Wiggins III Dr. Yoshimi Anzai Dr. Lindell Gentry Dr. Blair Winegar Dr.
Maxillary Osteotomies and Bone Grafts for. Correction of Contoural and Occlusal
 Maxillary Osteotomies and Bone Grafts for Correction of Contoural and Occlusal Deformities* M. L. LEWIN, M.D. RAVELO V. ARGAMASO, M.D. ABRAHAM I. FINGEROTH, D.D.S. Bronx, New York One of the major aims
Maxillary Osteotomies and Bone Grafts for Correction of Contoural and Occlusal Deformities* M. L. LEWIN, M.D. RAVELO V. ARGAMASO, M.D. ABRAHAM I. FINGEROTH, D.D.S. Bronx, New York One of the major aims
