Peroneal Neuropathy after Tibio-Fibular Fracture Ye Chan Kim, M.D. 1, Tae Du Jung, M.D. 1,2
|
|
|
- Barrie Newman
- 6 years ago
- Views:
Transcription
1 Original Article Ann Rehabil Med 2011; 35: pissn: eissn: Annals of Rehabilitation Medicine Peroneal Neuropathy after Tibio-Fibular Fracture Ye Chan Kim, M.D. 1, Tae Du Jung, M.D. 1,2 Department of Rehabilitation Medicine, 1 Kyung-pook National University College of Medicine, 2 Kyung-pook National University Medical Center, Daegu , Korea Objective To investigate the injury mechanism in patients who had peroneal neuropathy after a tibio-fibular fracture and the correlation between tibio-fibular fracture location and the severity of the peroneal neuropathy by using electrodiagnosis. Method Thirty-four patients with peroneal neuropathy after a tibio-fibular fracture were recruited for this study. Their medical records, radiologic and electrodiagnostic findings were investigated retrospectively. They were divided into 2 groups according to the existence of a fibular head fracture. The group of patients without the fibular head fracture was further classified according to the criteria of Orthopedic Trauma Association (OTA) classification. The differences between the two groups in the severity of the neuropathy and electrodiagnostic findings were evaluated. Results Nine cases (26.5%) had tibio-fibular fractures with a coexisting fibular-head fracture and 25 cases (73.5%) had tibio-fibular fractures without fractures in the fibular-head area. There was no statistical significance in the correlation between the existence of the fibular head fracture and the severity of the electrodiagnostic findings. Neither was there any statistically significant relationship between the site of the tibio-fibular fracture and the severity of the peroneal neuropathy (p>0.05). Conclusion This study showed there were numerous cases with common peroneal neuropathy after tibiofibular fracture without a coexisting fibular-head fracture, which shows the importance of indirect nerve injury mechanisms as well as that of direct nerve injury as a cause of peroneal neuropathy. In addition, this study showed that there was no statistically significant correlation between the site of tibio-fibular fracture and the severity of peroneal neuropathy. Key Words Peroneal neuropathy, Tibial fracture Received January 17, 2011; Accepted July 1, 2011 Corresponding author: Tae Du Jung Deparment of Rehabilitation Medicine, Kyung-pook National University Medical Center, 474, Hakjeong-dong, Buk-gu, Daegu , Korea Tel: , Fax: , teeed0522@naver. com This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( creativecommons.org/licenses/by-nc/3.0) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright 2011 by Korean Academy of Rehabilitation Medicine INTRODUCTION It is well known that peroneal neuropathy is the most common mononeuropathy in the lower limb 1,2 and it is vulnerable to damage around the fibular head because of the anatomical position between the peroneal nerve and fibula when it winds around the fibular head. 3,4 However, the peroneal nerve can be injured anywhere along its course of the leg such as the calf, ankle or foot. 5
2 Peroneal Neuropathy after Tibio-Fibular Fracture Clinically, peroneal neuropathy can be suspected when patients complain of foot drop or sensory change of dorsum of their foot, but the differential diagnosis is needed to rule out L4, 5 radiculopathies caused by the herniated nucleus pulposus of the lumbar spine, lumbosacral plexopathy or sciatic neuropathy in which a peroneal division is predominantly damaged. 6,7 However, limitations always exists in differential diagnosis by means of only clinical symptoms and physical findings. It is very difficult when a patient complains of atypical symptoms. Therefore, an electrodiagnostic study is used to make the diagnosis. 6 These electrodiagnostic findings are closely related with the degree of damage and prognosis, and those resulted by stimulating distal portion of the lesion are different according to the duration from the onset of the nerve damage. 8 According to electodiagnostic findings, types of peroneal neuropathy are reported as conduction block, axonal loss or mixed axonal loss/conduction block and the axonal loss type is the most common, reaching 60% of the entire peroneal neuropathies. 8 Generally, traumatic tibio-fubular fracture can be suspected as one of the common causes of peroneal neuropathy, but the mechanism of injury is not clearly identified 9 and further investigation is required. In this case, there is a strong likelihood that direct laceration and compression were the causes of peroneal neuropathy. However, we consider there can be indirect mechanisms because there have been patients that complained of foot drop after the sole diaphyseal fracture not located closely with the course of the peroneal nerve. If peroneal neuropathy after tibio-fibular fracture can be caused by indirect and direct mechanisms, further analysis will be needed. Therefore, we searched patients diagnosed as peroneal neuropathy by the electrodiagnostic studies and confirmed the existence of tibio-fibular fracture. We investigated fracture site, fracture type and electrodiagnostic findings by their medical records and radiologic findings retrospectively. They were classified into two groups according to the existence of the fracture around the fibular head, 10 known as the most vulnerable site of peroneal nerve, 9 to find out the injury mechanism of peroneal neuropathy after tibio-fibular fracture. A group without the fibular head fracture was further classified according to the site of the fracture and the degree of severity of the two groups was investigated. MATERIALS AND METHODS Subjects A total of 138 patients that were suspected of peroneal neuropathy for footdrop and diagnosed with common peroneal neuropathy or deep peroneal neuropathy by electrodiagnosis at Kyung-pook National University Hospital rehabilitation center were recruited for this study from January, 2007 to August, Their medical records, X-ray, CT and MRI findings were investigated retrospectively. A total of 34 patients with traumatic tibio-fibular fractures confirmed by radiologic findings were included. Patients that showed normal findings in electrodiagnosis within 2 weeks from the onset of symptoms were excluded even if they had peripheral nerve injury. 11 Classifications Medelec Synergy (Oxford Instruments Medical, Surrey, UK) was used for the electrodiagnostic study. Nerve conduction studies and electromyographies were performed. In nerve conduction studies, deep peroneal nerve, tibial nerve, superficial peroneal nerve and sural nerve were performed. In motor nerve conduction studies, active electrodes were placed over the motor point of the muscles and reference electrodes were placed over the tendon or the bony insertion site of the same muscle where active electrodes were placed. In sensory nerve conduction studies, active electrodes were placed over the specific site along the course of a nerve and reference electrodes were placed over a point 4 cm distally apart from the active electrodes. Active electrodes were basically placed at EDB (extensor digitorum brevis) muscle to evaluate deep peroneal nerve. However, in case CMAP (compound muscle action potential) had no response at EDB, we checked it again at the TA (tibialis anterior) muscle. CMAP and SNAP (sensory nerve action potential) were recorded in the nerve conduction studies. In CMAP, baseline to peak amplitude, distal onset latency and nerve conduction velocity were measured. In SNAP, base line to peak amplitude and distal peak latency were measured. According to electodiagnostic findings by Katirji and Willbourn 2 (Table 1), types of peroneal neuropathy are reported as conduction block, axonal loss or mixed axonal loss/conduction block. Conduction block was defined as a condition the amplitude of the 649
3 Ye Chan Kim and Tae Du Jung Table 1. Criteria for Different Pathophysiologic Processes Affecting the Peroneal Nerve I. Conduction block (presumably secondary to focal demyelination) ; The amplitude of the compound muscle action potential (CMAP), stimulating proximally, was less than 50% of the distal amplitude, recording from the extensor digitorum brevis (EDB) and/or tibialis anterior (TA) II. Axonal loss 1) The amplitude of the peroneal CMAP, while stimulating distally, recording either EDB or TA, was unelicitable, low compared with normal values for age, or relatively low (less than 50%) compared with the corresponding contralateral response 2) The amplitude of the superficial peroneal sensory nerve action potential (SNAP) was unelicitable, low compared with normal values for age, or relatively low (less than 50%) compared with the corresponding contralateral response III. Mixed conduction block and axonal loss ; The nerve conduction study results fulfilled both criteria CMAP, stimulating proximally, was less than 50% of the distal amplitude, recording from EDB and/or TA. Axonal loss was defined as a condition the amplitude of the peroneal CMAP, while stimulating distally, recording either EDB or TA, was unelicitable, low compared with normal values 12 for age, or relatively low (less than 50%) compared with the corresponding contralateral response or a condition the amplitude of the superficial peroneal SNAP was unelicitable, low compared with normal values for age, or relatively low (less than 50%) compared with the corresponding contralateral response. Mixed axonal loss/conduction block was defined as a condition that fulfilled both criteria of conduction block and axonal loss. Patients were classified into two groups by severity of peroneal neuropathy: group with complete lesion or incomplete lesion. Complete lesion was defined as a condition which CMAP and SNAP could not be observed in nerve conduction studies or MUAP (motor unit action potential) could not be observed in electromyography, and incomplete lesion was defined as a condition in which MUAP could be observed in peroneal nerveinnervated muscles in electromyography. 13 Severity was classified as complete lesion or incomplete lesion because incomplete lesions were expected to have better prognosis than complete lesions because the reinnervation of muscle fibers through axonal sprouting occurred more efficiently in incomplete lesions. 14 Needle electromyographies were performed at more than two muscles innervated by deep peroneal nerve such as EDB, EHL (extensor hallucis longus) including TA, peroneus longus innervated by superficial peroneal nerve, biceps femoris short head innervated by common peroneal division of sciatic nerve, tensor fascia lata and gluteus medius innervated by L5 nerve root and gluteus maximus and gastrocnemius innervated by S1 nerve root. Tibia/fibula fracture classification was carried out by Orthopedic Trauma Association (OTA classification). 15 OTA classification classified the tibio-fibular fracture into proximal segment, diaphyseal segment, distal segment or malleolar segment according to their site of fracture (Fig. 1). Proximal and distal segment fractures are further classified into A, B or C types; A type for the group that did not involve the joint, B type for the group that involved the joint partially, and C type for the group that involved the joint entirely. Diaphyseal segment fracture was classified into A, B or C according to fracture patterns: A for simple type, B for wedge type, C for complex type. Malleolar segment fracture was classified into A, B or C according to relative location of fracture based on syndesmosis. A type for fracture below the syndesmosis, B type for fracture at the syndesmosis, C type for fracture above the syndesmosis. Also, all patients were classified into 2 groups according to the existence of fibular head fracture, then severity and electrodiganostic findings of 2 groups were compared to find out the role of the fibular head fracture upon the peroneal nerve injury. Analysis We used the SPSS 12.0 program. Pearson s chi-square test was used to evaluate the relationship between the existence of the fibular head fracture and the electrodiagnostic findings and between the existence of the fibular head fracture and the severity of peroneal neuropathy. Additionally, among the patients without fibular head fracture, the same test was used to evaluate the relationship between the site of tibio-fibular fracture according to the OTA classification and the electrodiagnostic findings and between the site of tibiofibular fracture and the severity of peroneal neuropathy. All of the statistical significance level was set as p=
4 Peroneal Neuropathy after Tibio-Fibular Fracture Fig. 1. OTA (Orthopedic Trauma Association) classification of tibio-fibular fracture. Tibio-fibular fracture is classified as proximal, diaphyseal, distal and malleolar segment according to the anatomical site of the fracture. RESULTS Characteristics of subjects Fifty-eight patients out of a total 138 patients diagnosed as peroneal neuropathy by electrodiagnosis were confirmed to have tibio-fibular fracture with radiologic findings. Seventeen patients with co-existent femur fracture and 7 patients with coexistent pelvic bone fracture were excluded. Therefore, 34 patients without coexistent fracture were included in the study. Subjects 651
5 Ye Chan Kim and Tae Du Jung included 30 male patients (88.2%) and 4 female patients (11.8%). Mean age was 39.2 (ranging from 12 to 71). Fifth decade were the most common (9 patients, 26.4%) followed by the third and fourth decade (7 patients, 20.6%, respectively). 30 patients (87.9%) were unilateral, 17 patients were left side and 13 patients were right side. Classification ac cording to the existence of fibular head fracture and the location of fracture Among all subjects, 9 patients had fibular head fracture whereas 25 patients did not. According to OTA classification, 25 patients without fibular head fracture were classified again. Diaphyseal segment fracture were the most common (19 patients) and proximal segment fracture were 2 patients, distal segment fractures were 3 patients, malleolar segment fracture was 1 patients respectively. In minor classification, 19 patients with diphyseal segment fracture consisted of 14 type A patients, 5 type B patients and there was no type C patient in diaphyseal segment fracture. Proximal segment fracture consisted only of 2 type A patients, distal segment fracture consisted of 2 type A patients and 1 type C patient and malleolar segment fracture consisted of 1 type C patient (Table 2). Electrodiagnostic findings The total 34 patients consisted of 27 patients with common peroneal neuropathy and 7 patients with deep peroneal neuropathy. According to the severity in electrodiagnostic findings, incomplete lesions were in 32 patients, which greatly outnumbered the complete lesions (2 patients). Axonal loss lesions were the most common (30 patients), mixed axonal loss/ conduction block lesions were 4 patients and there was no conduction block lesion in our study by classification suggested by Katirji and Willbourn. 2 Analysis Nine patients with fibular head fracture were all diagnosed as common peroneal neuropathy and 25 patients without fibular head fracture consisted of 18 patients with common peroneal neuropathy and 7 patients with deep peroneal neuropathy in electrodiagnosis (Table 3). In comparison of the severity between two groups Table 2. Electrodiagnostic Findings and Types of Tibiofibular Fracture without Fracture Around the Fibular Head OTA classification Electrodiagnostic findings Conduction block Axonal loss Mixed lesion Total Proximal A Proximal B Proximal C Diaphysis A Diaphysis B Diaphysis C Distal A Distal B Distal C Malleolar A Malleolar B Malleolar C Total p>0.05 compared pathophysiologic processes with types of tibio-fibular fracture Table 3. Types of Peroneal Neuropathy Observed in the Patients Types of peroneal neuropathy Common peroneal neuropathy Deep peroneal neuropathy Group with fibular head fracture Group without fibular head fracture Total Total classified according to the existence of fibular head fracture, the group with fibular head fracture consisted of 1 patient with complete lesion and 8 patients with incomplete lesion, and the group without fibular head fracture consisted of 1 patient with complete lesion and 24 patients with incomplete lesion. There was no statistical significance in correlation between the existence of fibular head fracture and the severity of peroneal neuropathy (p=0.437, Fig. 2). In comparison of the electrodiagnostic findings between 2 groups, group with fibular head fracture consisted 652
6 Peroneal Neuropathy after Tibio-Fibular Fracture of 8 patients with axonal loss lesion and 1 patient with mixed axonal loss/conduction block lesion, and group without fibular head fracture consisted of 22 patients with axonal loss lesion and 3 patients with mixed axonal loss/conduction block lesion. There was no statistical significance in correlation between the existence of fibular head fracture and the electrodiagnostic findings (p=0.723, Fig. 3). A total of 25 patients without fibular head fracture Fig. 2. Distribution of severity according to the injury mechanism. There was one complete lesion and 8 incomplete lesions in groups with fibular head fracture, and there was one complete lesion and 24 incomplete lesions in groups without fibular head fracture. There was no statistical significance in the relationship between the injury mechanism and severity. were classified into groups according to the location of the fracture and the difference of each group in the electrodiagnostic findings, and the severity was evaluated. Proximal segment fracture consisted of 2 patients with incomplete lesion. Diaphyseal segment fracture group was 19 patients and consisted of 18 patients with incomplete lesion and 1 patient with complete lesion. Distal segment fracture group consisted of 3 patients with incomplete lesion, and malleolar segment fracture group consisted of 1 patient with incomplete lesion. There was no statistical significance in correlation between the location of fracture and the severity of peroneal neuropathy in the electrodiagnostic findings (p=0.954, Fig. 4). According to the classification suggested by Katirji and Willbourn, 2 patients with proximal segment fracture consisted of 1 patient with axonal loss lesion and 1 patient with mixed axonal loss/conduction block lesion. Nineteen patients of the diaphyseal segment fracture consisted of 17 patients with axonal loss lesion and 2 patients with mixed axonal loss/conduction block lesion. Three patients with distal segment fracture consisted of 2 patients with axonal loss lesion and 1 patient with mixed axonal loss/conduction block lesion and 1 patient with Fig. 3. Distribution of electrodiagnostic findings according to the injury mechanism. There was one mixed lesion and 8 axonal loss lesions in groups with fibular head fracture, and there were 3 mixed lesions and 22 axonal loss lesions in groups without fibular head fracture. There was no statistical significance in the relationship between the injury mechanism and the electrodiagnostic findings. Fig. 4. Distribution of severity in the electrodiagnostic findings according to fracture patterns in patients without fracture around the fibular head (Prox.: proximal segment fracture, Dia.: diaphyseal segment fracture, Dist.: distal segment fracture, Mall.: malleolar segment fracture). 1 complete lesion was found in diaphyseal segment fracture and 24 incomplete lesions were found, 2 cases in proximal segment fracture, 18 cases in diaphyseal segment fracture, 3 cases in distal segment fracture, 1 case in malleolar segment fracture. There was no statistical significance in the relationship between the anatomical site of fracture and the severity
7 Ye Chan Kim and Tae Du Jung Fig. 5. Distribution of electrodiagnostic findings according to fracture patterns in patients without fibular head fracture (Prox.: proximal segment fracture, Dia.: diaphyseal segment fracture, Dist.: distal segment fracture, Mall.: malleolar segment fracture). 4 mixed lesions were found, 1 case in proximal segment fracture, 2 cases in diaphyseasl segment fracture and 1 case in distal segment fracture. 21 axonal loss lesions were found, 1 case in proximal segment fracture, 17 cases in diaphyesal segment fracture, 2 cases in distal segment fracture and 1 case in malleolar segment fracture. There was no statistical significance in the relationship between the anatomical site of fracture and the electrodiagnostic findings. malleolar segment fracture was identified as axonal loss lesion. There was no statistical significance in correlation between the electrodiagnostic findings and the location of the fracture (p=3.91, Fig. 5). DISCUSSION There were only 9 patients out of the total 34 with fibular head fracture that were considered to have inflicted direct damage to the peroneal nerve in this study. On the other hand, there were 25 patients without fibular head fracture, which outnumbered the patients with fibular head fracture. The electrodiagnostic findings of 25 patients without fibular head fracture were investigated and there were 18 patients with peroneal neuropathy and 7 patients with deep peroneal neuropathy. Common peroneal nerve, as a lateral branch of sciatic nerve, is separated from a sciatic nerve at the distal third portion of a thigh, and descends posterior to the fibular head, winding around the neck of the fibula, running toward the anterior portion of the leg, then enters the anterior compartment penetrating through the superficial head of the peroneus longus muscle. The fiber of peroneus longus muscle at this part comprises the tendinous arch called fibular tunnel right above the common peroneal nerve, which is known as one of the causes of peroneal neuropathy. 3 After passing through the fibular tunnel, the common peroneal nerve divides in to the deep peroneal nerve and superficial peroneal nerve. Considering the course of peroneal nerve and the anatomy around fibular head, all patients without fibular head fracture should have been diagnosed as deep peroneal neuropathy. However, 18 out of 25 patients were diagnosed as common peroneal neuropathy. This study showed that among patients with peroneal neuropathy after traumatic tibio-fibular fracture, there were more patients without fibular head fracture that would have been thought to inflict direct damage on the peroneal nerve than patients with fibular head fracture, and there were more patients diagnosed as common peroneal neuropathy than patients diagnosed as deep peroneal neuropathy by electrodiagnosis. This study also showed that diaphyseal segment fracture was the most common type of tibio-fibular fracture among patients without fibular head fracture who complained of foot drop, and type A (simple type) was the most common type (14 cases) among the diaphyseal segment fracture. These results implied that peroneal neuropathy after tibio-fibular fracture was caused more frequently by indirect injury such as traction injury, compression over the fibular head after surgery or immobilization, compartment syndrome or entrapment neuropathy than by direct injury such as direct compression or dissection. In other words, direct nerve injury was not the only reason that caused peroneal neuropathy. Possible mechanisms for indirect injury of peroneal nerve are as follows. First, the limited motion toward the longitudinal direction of common peroneal nerve can be a cause of indirect injury. Berry and Richardson 3 reported that fibular tunnel limited the motion toward the longitudinal direction of common and deep peroneal nerves 0.5 cm at most and due to this, severe ankle inversion or posterior dislocation of hip joint could cause the traction force over common peroneal nerve toward the longitudinal direction Second, the fact that the traction injury can occur over the entire length of nerve as well as the maximal point of the traction supports the common peroneal neuropathy that occurs after the traction that inflict maximal damage 654
8 Peroneal Neuropathy after Tibio-Fibular Fracture on deep peroneal nerve, distal portion of common peroneal nerve. Haftek 19 reported the result that nerve fibers and endoneurial tubes were damaged at the point even except the maximal point of the damage. Third, peroneal nerve can be damaged by the swelling or hemorrhage inside the nerve at the fibular tunnel. Nobel 20 reported 2 cases of peroneal neuropathy caused by hematoma inside the peroneal nerve sheath after diaphyseal fracture of tibia and suggested the mechanism the torsional forces that occurred during the trauma transmitted the traction force along the nerve and dissected the nutritional vessels of the nerve, consequently inflicting the nerve damage. Stoff and Greene 18 suggested the hypotheses acute onset peroneal neuropathy after ankle inversion was caused by the traction force that inflicted directly on fibular head and delayed onset peroneal neuropathy after ankle inversion was caused by the hematoma within the peroneal nerve. The subjects had tibio-fibular fracture without ankle inversion in this study. However, an external force strong enough to cause the fracture could outweigh the traction force that occurred at ankle inversion. Therefore, the above two mechanisms can be applied to our subjects. Also, Whitesides and Heckman 21 reported neuropathy caused by the compartment syndrome occurred in 10% of patients with closed fracture of tibia. Fourth, compression caused by immobilization such as splint or cast and leg edema as a cause of peroneal neuropathy during treatment process can be a cause of indirect injury. Baima and Krivickas 22 reported that injury of ligament or bone could cause peroneal neuropathy, but peroneal neuropathy occurred more frequently during treatment process than during traumatic event and mentioned these. There was a general notion that nerve injury after fracture would be caused by direct trauma, but as mentioned above, there are many cases that have reported consistently about peroneal neuropathy that occurred during the treatment or healing process of fracture. In addition, there are many cases that have been reported about other peripheral neuropathies that occurred during the healing or treatment process of fracture. 23,24 Meanwhile, the fact that common peroneal neuropathy was covered only by the skin and fascia at the head and neck portion of the fibula support the hypothesis that peroneal nerve can be easily damaged by the direct contusion or laceration. In other words, peroneal nerve can be damaged by the direct injury mechanism. Nine cases in our study had fibular head fracture, and the direct damage caused by contusion or compression could be suspected as the mechanism of peroneal nerve injury. In this study, there was no statistical significance in the correlation between the existence of fibular head fracture and the severity or the electrodiagnostic findings. Neither was there any statistical significant relationship between the site of fracture and the severity or the electrodiagnostic findings in the group without fibular head fracture. Therefore we expect there would be no difference in prognosis according to the existence of fibular head fracture or the site of fracture. Also, considering the fact that there were only 2 patients with complete lesion out of the total set of 34 patients, close observation for occurrence of peroneal neuropathy during healing and treatment process will be needed and if peroneal neuropathy occurs, intensive rehabilitation and follow up of patients will be needed because there is a possibility for recovery. In our study, there were 9 patients that could be considered as cases for direct nerve injury, even though there were more patients that could be considered as patients with the indirect nerve injury, peroneal neuropathy by the direct nerve injury must not be underestimated. There are some limitations in our study. The number of subjects was relatively small. Electrodiagnostic studies were not performed by one person, because this study was performed retrospectively, we could not consider the error of inter-reliability. In addition, we could not fully estimate the relationship between the electrodiagnostic study and clinical symptoms because of poor description of medical records and it was not easy for us to check correct duration from the onset in some cases. Imaging studies such as ultrasonography were not performed in the group that was considered as the indirect nerve injury to find out structural damage of the nerve. However, it was meaningful to verify that there was no statistical significance in the correlation between the severity and incidence of peroneal neuropathy or the site of fracture. It would be beneficial in further research for mechanism of peroneal neuropathy, to perform combined imaging studies such as ultrasonography or MRI for confirmation of the structural damage and study the relation between 655
9 Ye Chan Kim and Tae Du Jung those findings with the electrodiagnostic findings. CONCLUSION There were more cases without fibular fracture than cases with fibular head fracture which were considered as direct nerve injury cases in patients with peroneal neuro - pathy after tibio-fibular fracture. In addition, among patients without fibular head fracture, cases diagnosed as common peroneal neuropathy outnumbered the cases diagnosed as deep peroneal neuropathy. These results suggested that peroneal neuropathy occurred not only by direct nerve injury but also by indirect nerve injury. We must pay attention to the patients with tibiofibular fracture that do not involve the fibular head as well as the patients with fibular head fracture who are vulnerable to peroneal nerve injury in anatomical point of view. Considering the facts that there was no statistical significance between the site of tibio-fibular fracture and the severity of peroneal neuropathy and incomplete lesions outnumbered complete lesions, more favorable prognosis can be expected, therefore intensive rehabilitation will be needed. REFERENCES 1. Clawson DK, Seddon HJ. The late consequences of sciatic nerve injury. J Bone Joint Surg Br 1960; 42: Katirji MB, Wilbourn AJ. Common peroneal mononeuropathy: a clinical and electrophysiologic study of 116 lesions. Neurology 1988; 38: Berry H, Richardson PM. Common peroneal nerve palsy: a clinical and electrophysiological review. J Neurol Neurosurg Psychiatry 1976; 39: Smith T, Trojaborg W. Clinical and electro physiological recovery from peroneal palsy. Acta Neurol Scand 1986; 74: Oh SJ, Demirci M, Dajani B, Melo AC, Claussen GC. Distal sensory nerve conduction of the superficial pero neal nerve: new method and its clinical application. Muscle Nerve 2001; 24: Marciniak C, Armon C, Wilson J, Miller R. Practice parameter: utility of electrodiagnostic techniques in evaluating patients with suspected peroneal neuropathy: an evidence-based review. Muscle Nerve 2005; 31: Ayyar R. MR imaging of the lower leg versus clinical electrophysiologic examination in the differential diagnosis of neurogenic foot drop. AJNR Am J Neuroradiol 2003; 24: Singh H, Behse F, Buchthal F. Electrophysiological study of peroneal palsy. J Neurol Neurosurg Psychiatry 1974; 37: Masakado Y, Kawakami M, Suzuki K, Abe L, Ota T, Kimura A. Clinical neurophysiology in the diagnosis of peroneal nerve palsy. Keio J Med 2008; 57: Kiechl S. Clinical and Electrodiagnostic Work-Up of Peripheral Nerve Lesions. In: Peer S, Bodner G, Editors. High resolution sonography of the peripheral nervous system, 2nd ed, Berlin, Springer, 2008, Dumitru D, Amato AA, Zwarts MJ. Peripheral nervous system's reaction to injury. In: Dumitru D, Amato AA, Zwarts MJ, Editors. Electrodiagnostic medicine, 2nd ed, Philadelphia, Hanley & Belfus, 2002, Dumitru D, Amato AA, Zwarts MJ. Nerve conduction studies. In: Dumitru D, Amato AA, Zwarts MJ, Editors. Electrodiagnostic medicine, 2nd ed, Philadelphia, Hanley & Belfus, 2002, Kim DH, Yim SK, Kwon HK, Lee HJ. Clinical and electrophysiologic review of patients with common peroneal mononeuropathy. J Korean EMG Electrodiagn Med 2000; 2: Katirji B. Peroneal neuropathy. Neurol Clin 1999; 17: Marsh JL, Slongo TF, Agel J, Broderick JS, Creevey W, DeCoster TA, Prokuski L, Sirkin MS, Ziran B, Henley B, et al. Fracture and dislocation classification compendium : Orthopaedic Trauma Association classification, database and outcomes committee. J Orthop Trauma 2007; 21: S Meals RA. Peroneal-nerve palsy complicating ankle sprain. Report of two cases and review of the literature. J Bone Joint Surg Am 1977; 59: Johnston EC, Howell SJ. Tension neuropathy of the superficial peroneal nerve: associated conditions and results of release. Foot Ankle Int 1999; 20: Stoff MD, Greene AF. Common peroneal nerve palsy following inversion ankle injury: a report of two cases. Phys Ther 1982; 62: Haftek J. Stretch injury of peripheral nerve. Acute effects of stretching on rabbit nerve. J Bone Joint Surg 656
10 Peroneal Neuropathy after Tibio-Fibular Fracture Br 1970; 52: Nobel W. Peroneal palsy due to hematoma in the common peroneal nerve sheath after distal torsional fractures and inversion ankle sprains. J Bone Joint Surg Am 1966; 48: Whitesides TE, Heckman MM. Acute Compartment Syndrome: Update on Diagnosis and Treatment. J Am Acad Orthop Surg 1996; 4: Baima J, Krivickas L. Evaluation and treatment of peroneal neuropathy. Curr Rev Musculoskelet Med 2008; 1: Vural M, Arslantas A. Delayed radial nerve palsy due to entrapment of the nerve in the callus of a distal third humerus fracture. Turk Neurosurg 2008; 18: Bodner G, Buchberger W, Schocke M, Bale R, Huber B, Harpf C, Gassner E, Jaschke W. Radial nerve palsy associated with humeral shaft fracture: evaluation with US--initial experience. Radiology 2001; 219:
Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve Action Potential in Common Peroneal Neuropathy
 J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
J Korean Med Sci 2008; 23: 117-21 ISSN 1011-8934 DOI: 10.3346/jkms.2008.23.1.117 Copyright The Korean Academy of Medical Sciences Compound Nerve Action Potential of Common Peroneal Nerve and Sural Nerve
Yoshihisa Masakado, Michiyuki Kawakami, Kanjiro Suzuki, Leon Abe, Tetsuo Ota, and Akio Kimura
 REVIEW Clinical Neurophysiology in the Diagnosis of Peroneal Nerve Palsy Yoshihisa Masakado, Michiyuki Kawakami, Kanjiro Suzuki, Leon Abe, Tetsuo Ota, and Akio Kimura Keio University Tsukigase Rehabilitation
REVIEW Clinical Neurophysiology in the Diagnosis of Peroneal Nerve Palsy Yoshihisa Masakado, Michiyuki Kawakami, Kanjiro Suzuki, Leon Abe, Tetsuo Ota, and Akio Kimura Keio University Tsukigase Rehabilitation
Department of Rehabilitation Medicine, Michuhol Rehabilitation Center, Incheon; 2
 Case Report Ann Rehabil Med 2013;37(6):886-890 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.6.886 Annals of Rehabilitation Medicine Sciatic Nerve Injury Caused by a Stretching
Case Report Ann Rehabil Med 2013;37(6):886-890 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.6.886 Annals of Rehabilitation Medicine Sciatic Nerve Injury Caused by a Stretching
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
musculoskeletal system anatomy nerves of the lower limb 2 done by: Dina sawadha & mohammad abukabeer #Sacral plexus : emerges from the ventral rami of the spinal segments L4 - S4 and provides motor and
The Lower Limb VI: The Leg. Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa
 The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
The Lower Limb VI: The Leg Anatomy RHS 241 Lecture 6 Dr. Einas Al-Eisa Muscles of the leg Posterior compartment (superficial & deep): primary plantar flexors of the foot flexors of the toes Anterior compartment:
Year 2004 Paper one: Questions supplied by Megan
 QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
QUESTION 47 A 58yo man is noted to have a right foot drop three days following a right total hip replacement. On examination there is weakness of right ankle dorsiflexion and toe extension (grade 4/5).
Lower Limb Nerves. Clinical Anatomy
 Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Lower Limb Nerves Clinical Anatomy Lumbar Plexus Ventral rami L1 L4 Supplies: Abdominal wall External genitalia Anteromedial thigh Major nerves.. Lumbar Plexus Nerves relation to psoas m. : Obturator n.
Case Example. Nerve Entrapments in the Lower limb
 Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Nerve Entrapments in the Lower limb February, 2013 William S. Pease, M.D. Ernest W. Johnson Professor of PM&R Case Example CC: Right ankle dorsiflexion weakness with minimal paresthesias HPI: 87 year-old
Clinical Characteristics of Peroneal Nerve Palsy by Posture
 www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2013.53.5.269 J Korean Neurosurg Soc 53 : 269-273, 2013 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2013 The Korean Neurosurgical Society Clinical
www.jkns.or.kr http://dx.doi.org/10.3340/jkns.2013.53.5.269 J Korean Neurosurg Soc 53 : 269-273, 2013 Print ISSN 2005-3711 On-line ISSN 1598-7876 Copyright 2013 The Korean Neurosurgical Society Clinical
Lumbar Plexus. Ventral rami L1 L4 Supplies: Major nerves.. Abdominal wall External genitalia Anteromedial thigh
 Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Lower Limb Nerves Lectures Objectives Describe the structure and relationships of the plexuses of the lower limb. Describe the course, relationships and structures supplied for the major nerves of the
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2013;37(4):577-581 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.4.577 Annals of Rehabilitation Medicine Compressive Neuropathy of the Posterior Tibial
Case Report Ann Rehabil Med 2013;37(4):577-581 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.4.577 Annals of Rehabilitation Medicine Compressive Neuropathy of the Posterior Tibial
Leg. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
Leg Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Skin of the Leg Cutaneous Nerves Medially: The saphenous nerve, a branch of the femoral nerve supplies the skin on the medial surface
A/Professor Arun Aggarwal Balmain Hospital
 A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
A/Professor Arun Aggarwal Balmain Hospital Nerve Conduction Studies Test to evaluate the function of motor / sensory nerves Evaluate Paraesthesia (numbness, tingling, burning) Weakness of arms and legs
Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature Review
 ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
ISPUB.COM The Internet Journal of Plastic Surgery Volume 2 Number 1 Tibial and Common Peroneal Nerve Compression in The Popliteal Fossa: A Case Report and Literature D Reichner, G Evans Citation D Reichner,
MUSCULOSKELETAL LOWER LIMB
 MUSCULOSKELETAL LOWER LIMB Spinal Cord Lumbar and Sacral Regions Spinal cord Dorsal root ganglion Conus medullaris Cauda equina Dorsal root ganglion of the fifth lumbar nerve End of subarachnoid space
MUSCULOSKELETAL LOWER LIMB Spinal Cord Lumbar and Sacral Regions Spinal cord Dorsal root ganglion Conus medullaris Cauda equina Dorsal root ganglion of the fifth lumbar nerve End of subarachnoid space
Human Anatomy Biology 351
 Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
Lecture 09. Popliteal Fossa. BY Dr Farooq Khan Aurakzai
 Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Lecture 09 Popliteal Fossa BY Dr Farooq Khan Aurakzai Dated: 14.02.2018 What is popliteus? Introduction Anything relating to, or near the part of the leg behind the knee. From New Latin popliteus the muscle
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2018;42(3):483-487 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2018.42.3.483 Annals of Rehabilitation Medicine Diagnosis of Pure Ulnar Sensory Neuropathy Around
Case Report Ann Rehabil Med 2018;42(3):483-487 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2018.42.3.483 Annals of Rehabilitation Medicine Diagnosis of Pure Ulnar Sensory Neuropathy Around
Case Report. Annals of Rehabilitation Medicine CASE REPORT INTRODUCTION
 Case Report Ann Rehabil Med 2017;41(4):715-719 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.4.715 Annals of Rehabilitation Medicine Common Peroneal Neuropathy With Anterior Tibial
Case Report Ann Rehabil Med 2017;41(4):715-719 pissn: 2234-0645 eissn: 2234-0653 https://doi.org/10.5535/arm.2017.41.4.715 Annals of Rehabilitation Medicine Common Peroneal Neuropathy With Anterior Tibial
Electrodiagnostics for Back & Neck Pain. Steven Andersen, MD Providence Physiatry Clinic
 Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrodiagnostics for Back & Neck Pain Steven Andersen, MD Providence Physiatry Clinic Electrodiagnostics Electromyography (EMG) Needle EMG exam (NEE) Nerve conduction studies (NCS) Motor Sensory Late
Electrophysiology of Brachial and Lumbosacral Plexopathies
 18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
18 Electrophysiology of Brachial and Lumbosacral Plexopathies Juan A. Acosta and Elizabeth M. Raynor Summary Brachial and lumbosacral plexopathies represent a heterogeneous group of disorders including
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2016;40(3):545-550 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.3.545 Annals of Rehabilitation Medicine Neurovascular Compression Caused by Popliteus
Case Report Ann Rehabil Med 2016;40(3):545-550 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.3.545 Annals of Rehabilitation Medicine Neurovascular Compression Caused by Popliteus
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2014;38(3):427-432 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.427 Annals of Rehabilitation Medicine Acetabular Paralabral Cyst as a Rare Cause
Case Report Ann Rehabil Med 2014;38(3):427-432 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.3.427 Annals of Rehabilitation Medicine Acetabular Paralabral Cyst as a Rare Cause
Human Anatomy Biology 351
 Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
Human Anatomy Biology 351 Lower Limb Please place your name on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average, between
The Lower Limb II. Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa
 The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
The Lower Limb II Anatomy RHS 241 Lecture 3 Dr. Einas Al-Eisa Tibia The larger & medial bone of the leg Functions: Attachment of muscles Transfer of weight from femur to skeleton of the foot Articulations
DISSECTION SCHEDULE. Session I - Hip (Front) & Thigh (Superficial)
 DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
DISSECTION SCHEDULE Session I - Hip (Front) & Thigh (Superficial) Surface anatomy Inguinal region Gluteal region Thigh Leg Foot bones Hip bone Femur Superficial fascia Great saphenous vein Superficial
The near-nerve sensory nerve conduction in tarsal tunnel syndrome
 Journal of Neurology, Neurosurgery, and Psychiatry 1985;48: 999-1003 The near-nerve sensory nerve conduction in tarsal tunnel syndrome SHN J OH, HYUN S KM, BASHRUDDN K AHMAD From the Department ofneurology,
Journal of Neurology, Neurosurgery, and Psychiatry 1985;48: 999-1003 The near-nerve sensory nerve conduction in tarsal tunnel syndrome SHN J OH, HYUN S KM, BASHRUDDN K AHMAD From the Department ofneurology,
Index. Note: Page numbers of article titles are in boldface type.
 Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Neurol Clin N Am 20 (2002) 605 617 Index Note: Page numbers of article titles are in boldface type. A ALS. See Amyotrophic lateral sclerosis (ALS) Amyotrophic lateral sclerosis (ALS) active denervation
Understanding Leg Anatomy and Function THE UPPER LEG
 Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Understanding Leg Anatomy and Function THE UPPER LEG The long thigh bone is the femur. It connects to the pelvis to form the hip joint and then extends down to meet the tibia (shin bone) at the knee joint.
Muscles of the lower extremities. Dr. Nabil khouri MD, MSc, Ph.D
 Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
Muscles of the lower extremities Dr. Nabil khouri MD, MSc, Ph.D Posterior leg Popliteal fossa Boundaries Biceps femoris (superior-lateral) Semitendinosis and semimembranosis (superior-medial) Gastrocnemius
Anatomy MCQs Week 13
 Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Anatomy MCQs Week 13 1. Posterior to the medial malleolus of the ankle: The neurovascular bundle lies between Tibialis Posterior and Flexor Digitorum Longus The tendon of Tibialis Posterior inserts into
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve
 Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Muscles of the Hip 1. Tensor Fasciae Latae O: iliac crest I: lateral femoral condyle Action: abducts the thigh Nerve: gluteal nerve 2. Gluteus Maximus O: ilium I: femur Action: abduct the thigh Nerve:
Where should you palpate the pulse of different arteries in the lower limb?
 Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
Where should you palpate the pulse of different arteries in the lower limb? The femoral artery In the femoral triangle, its pulse is easily felt just inferior to the inguinal ligament midway between the
VENOUS DRAINAGE OF THE LOWER LIMB
 Anatomy of the lower limb Superficial veins & nerve injuries Dr. Hayder VENOUS DRAINAGE OF THE LOWER LIMB The venous drainage of the lower limb is of huge clinical & surgical importance. Since the venous
Anatomy of the lower limb Superficial veins & nerve injuries Dr. Hayder VENOUS DRAINAGE OF THE LOWER LIMB The venous drainage of the lower limb is of huge clinical & surgical importance. Since the venous
Borderline Moderately out of normal range Severely out of normal range Technical
 Urgent Care Specialists 2200 Universal Drive, Boston, MA Phone: 761-621-5216 Fax: 761-564-0336 Report: EMG-1133-28616 Physician: Dr. John Smith Age Range: 40-59 Ref Phys: Dr. Joe Ranier Height Range cm:
Urgent Care Specialists 2200 Universal Drive, Boston, MA Phone: 761-621-5216 Fax: 761-564-0336 Report: EMG-1133-28616 Physician: Dr. John Smith Age Range: 40-59 Ref Phys: Dr. Joe Ranier Height Range cm:
The Leg. Prof. Oluwadiya KS
 The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
The Leg Prof. Oluwadiya KS www.oluwadiya.sitesled.com Compartments of the leg 4 Four Compartments: 1. Anterior compartment Deep fibular nerve Dorsiflexes the foot and toes 2. Lateral Compartment Superficial
Peripheral Nervous System: Lower Body
 Peripheral Nervous System: Lower Body MSTN121 - Neurophysiology Session 11 Department of Myotherapy Lumbar Plexus Iliohypogastric nerve (T12-L1) Motor: Transverse abdominis and internal obliques Sensory:
Peripheral Nervous System: Lower Body MSTN121 - Neurophysiology Session 11 Department of Myotherapy Lumbar Plexus Iliohypogastric nerve (T12-L1) Motor: Transverse abdominis and internal obliques Sensory:
Organization of the Lower Limb
 Organization of the Lower Limb Limb Development Lower limb develops in an aterolateral position at the level of the L2 to S3 trunk segments Great toe positioned cephalic direction with the soles of the
Organization of the Lower Limb Limb Development Lower limb develops in an aterolateral position at the level of the L2 to S3 trunk segments Great toe positioned cephalic direction with the soles of the
Saeid Khosrawi, Farnaz Dehghan Department of Physical Medicine and Rehabilitation, Isfahan University of Medical Sciences, Isfahan, Iran
 Original Article Determination of the median nerve residual latency values in the diagnosis of carpal tunnel syndrome in comparison with other electrodiagnostic parameters Saeid Khosrawi, Farnaz Dehghan
Original Article Determination of the median nerve residual latency values in the diagnosis of carpal tunnel syndrome in comparison with other electrodiagnostic parameters Saeid Khosrawi, Farnaz Dehghan
Evaluating concomitant lateral epicondylitis and cervical radiculopathy
 Evaluating concomitant lateral epicondylitis and cervical radiculopathy March 06, 2010 This article describes a study of the prevalence of lateral epicondylitis or tennis elbow among patients with neck
Evaluating concomitant lateral epicondylitis and cervical radiculopathy March 06, 2010 This article describes a study of the prevalence of lateral epicondylitis or tennis elbow among patients with neck
Contents of the Posterior Fascial Compartment of the Thigh
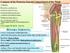 Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
Contents of the Posterior Fascial Compartment of the Thigh 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t
MRI of the Distal Biceps Femoris Muscle: Normal Anatomy, Variants, and Association with Common Peroneal Entrapment Neuropathy
 Vieira et al. MRI of the iceps Femoris Muscle Musculoskeletal Imaging Original Research 09_07_2308_Vieira.fm 7/27/07 Renata La Rocca Vieira 1 Zehava Sadka Rosenberg Kiril Kiprovski Vieira RLR, Rosenberg
Vieira et al. MRI of the iceps Femoris Muscle Musculoskeletal Imaging Original Research 09_07_2308_Vieira.fm 7/27/07 Renata La Rocca Vieira 1 Zehava Sadka Rosenberg Kiril Kiprovski Vieira RLR, Rosenberg
Lower limb summary. Anterior compartment of the thigh. Done By: Laith Qashou. Doctor_2016
 Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
Lower limb summary Done By: Laith Qashou Doctor_2016 Anterior compartment of the thigh Sartorius Anterior superior iliac spine Upper medial surface of shaft of tibia 1. Flexes, abducts, laterally rotates
The Muscular System. Chapter 10 Part D. PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College
 Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Chapter 10 Part D The Muscular System Annie Leibovitz/Contact Press Images PowerPoint Lecture Slides prepared by Karen Dunbar Kareiva Ivy Tech Community College Table 10.14: Muscles Crossing the Hip and
Disclosure. Entrapment Neuropathies - Overview. Common mononeuropathy sites. Definitions. Common mononeuropathy sites. Common mononeuropathy sites
 Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
Disclosure Entrapment Neuropathies - Overview I receive compensation from Wiley- Blackwell publishers for my work as Editor-in-Chief of Muscle & Nerve Lawrence H. Phillips, II, MD Definitions Mononeuropathy:
The Pattern of Peripheral Nerve Injuries among Iraqi Soldiers in the War by using Nerve Conductive Study
 Research Article The Pattern of Peripheral Nerve Injuries among Iraqi Soldiers in the War by using Nerve Conductive Study Qaisar A. Atea, M.B.Ch.B, D.R.M.R. Safaa H. Ali, M.B.Ch.B, Msc, Ph.D. Date Submitted:
Research Article The Pattern of Peripheral Nerve Injuries among Iraqi Soldiers in the War by using Nerve Conductive Study Qaisar A. Atea, M.B.Ch.B, D.R.M.R. Safaa H. Ali, M.B.Ch.B, Msc, Ph.D. Date Submitted:
Organization of the Lower Limb Audrone Biknevicius, Ph.D. Dept. Biomedical Sciences, OU HCOM at Dublin Clinical Anatomy Immersion 2014
 Organization of the Lower Limb Audrone Biknevicius, Ph.D. Dept. Biomedical Sciences, OU HCOM at Dublin Clinical Anatomy Immersion 2014 www.thestudio1.co.za LIMB FUNCTION choco-locate.com blog.coolibar.com
Organization of the Lower Limb Audrone Biknevicius, Ph.D. Dept. Biomedical Sciences, OU HCOM at Dublin Clinical Anatomy Immersion 2014 www.thestudio1.co.za LIMB FUNCTION choco-locate.com blog.coolibar.com
lesser trochanter of femur lesser trochanter of femur iliotibial tract (connective tissue) medial surface of proximal tibia
 LOWER LIMB MUSCLES OF THE APPENDICULAR SKELETON The muscles that act on the lower limb fall into three groups: those that move the thigh, those that move the lower leg, and those that move the ankle, foot,
LOWER LIMB MUSCLES OF THE APPENDICULAR SKELETON The muscles that act on the lower limb fall into three groups: those that move the thigh, those that move the lower leg, and those that move the ankle, foot,
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Original Articles. 198 Medicina Interna REVISTA DA SOCIEDADE PORTUGUESA DE MEDICINA INTERNA
 Original Articles Lumbosacral radiculopathy. The sensitivity of electromyographical studies compared to imaging techniques and clinical findings L. Negrão*, J. M. Santos**, J. Gonçalves***, L. Cunha****
Original Articles Lumbosacral radiculopathy. The sensitivity of electromyographical studies compared to imaging techniques and clinical findings L. Negrão*, J. M. Santos**, J. Gonçalves***, L. Cunha****
Case Presentation MATT WORONCZAK ADVANCED MUSCULOSKELETAL PHYSIOTHERAPIST DANDENONG HOSPITAL VICTORIA
 Case Presentation MATT WORONCZAK ADVANCED MUSCULOSKELETAL PHYSIOTHERAPIST DANDENONG HOSPITAL VICTORIA Scenario Supervising an intern 22 year old male playing soccer yesterday, rolled ankle and unable to
Case Presentation MATT WORONCZAK ADVANCED MUSCULOSKELETAL PHYSIOTHERAPIST DANDENONG HOSPITAL VICTORIA Scenario Supervising an intern 22 year old male playing soccer yesterday, rolled ankle and unable to
Ulnar Nerve Conduction Study of the First Dorsal Interosseous Muscle in Korean Subjects Dong Hwee Kim, M.D., Ph.D.
 Original Article Ann Rehabil Med 2011; 35: 658-663 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2011.35.5.658 Annals of Rehabilitation Medicine Ulnar Nerve Conduction Study of the First
Original Article Ann Rehabil Med 2011; 35: 658-663 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2011.35.5.658 Annals of Rehabilitation Medicine Ulnar Nerve Conduction Study of the First
MUSCLES OF THE LOWER LIMBS
 MUSCLES OF THE LOWER LIMBS Naming, location and general function Dr. Nabil khouri ROLES THAT SHOULD NOT BE FORGOTTEN Most anterior compartment muscles of the hip and thigh Flexor of the femur at the hip
MUSCLES OF THE LOWER LIMBS Naming, location and general function Dr. Nabil khouri ROLES THAT SHOULD NOT BE FORGOTTEN Most anterior compartment muscles of the hip and thigh Flexor of the femur at the hip
Prevention and Treatment of Injuries. Anatomy. Anatomy. Tibia: the second longest bone in the body
 Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES
 BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
BLUE SKY SCHOOL OF PROFESSIONAL MASSAGE AND THERAPEUTIC BODYWORK Musculoskeletal Anatomy & Kinesiology KNEE & ANKLE MUSCLES MSAK201-I Session 3 1) REVIEW a) THIGH, LEG, ANKLE & FOOT i) Tibia Medial Malleolus
~, /' ~::'~ EXTENSOR HALLUCIS LONGUS. Leg-anterolateral :.:~ / ~\,
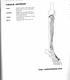 TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
TIBIALIS ANTERIOR Lateral condyle of tibia, upper half of lateral surface of tibia, interosseous membrane Medial side and plantar surface of medial cuneiform bone, and base of first metatarsal bone Dorsiflexes
موسى صالح عبد الرحمن الحنبلي أحمد سلمان
 8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
8 موسى صالح عبد الرحمن الحنبلي أحمد سلمان 1 P a g e Today we will talk about a new region, which is the leg. And as always, we will start with studying the sensory innervation of the leg. What is the importance
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2014;38(1):132-137 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.132 Annals of Rehabilitation Medicine Right Calf Claudication Revealing Leriche
Case Report Ann Rehabil Med 2014;38(1):132-137 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.132 Annals of Rehabilitation Medicine Right Calf Claudication Revealing Leriche
Wrist, Elbow Hand. Surface Recording Technique, Study from Median Thenar (MT) Muscle
 Surface ecording Technique, Study from Median Thenar (MT) Muscle Original Settings Sensitivity, duration of pulse, sweep speed, low-frequency filter, high- frequency filter, and the machine used were not
Surface ecording Technique, Study from Median Thenar (MT) Muscle Original Settings Sensitivity, duration of pulse, sweep speed, low-frequency filter, high- frequency filter, and the machine used were not
Proper Performance and Interpretation of Electrodiagnostic Studies
 Proper Performance and Interpretation of Electrodiagnostic Studies Introduction The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) has developed the following position statement
Proper Performance and Interpretation of Electrodiagnostic Studies Introduction The American Association of Neuromuscular & Electrodiagnostic Medicine (AANEM) has developed the following position statement
Organization of the Lower Limb
 Organization of the Lower Limb Most illustrations from: Thieme Atlas of Anatomy: Musculoskeletal System. M Schuenke, et al, 2006. Anatomy: A Regional Atlas of the Human Body. Carmine Clemente, 4th edition.
Organization of the Lower Limb Most illustrations from: Thieme Atlas of Anatomy: Musculoskeletal System. M Schuenke, et al, 2006. Anatomy: A Regional Atlas of the Human Body. Carmine Clemente, 4th edition.
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
Case Report Ann Rehabil Med 2014;38(1):109-115 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.1.109 Annals of Rehabilitation Medicine Sonographic Evaluation of the Peripheral Nerves
5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh:
 5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Proximal attachment Distal attachment Sartorius ASIS» Upper part of shaft tibia (middle surface)»
5.1 Identify, describe the attachments of and deduce the actions of the muscles of the thigh: Anterior group Proximal attachment Distal attachment Sartorius ASIS» Upper part of shaft tibia (middle surface)»
SURGICAL AND APPLIED ANATOMY
 Página 1 de 9 Copyright 2001 Lippincott Williams & Wilkins Bucholz, Robert W., Heckman, James D. Rockwood & Green's Fractures in Adults, 5th Edition SURGICAL AND APPLIED ANATOMY Part of "47 - ANKLE FRACTURES"
Página 1 de 9 Copyright 2001 Lippincott Williams & Wilkins Bucholz, Robert W., Heckman, James D. Rockwood & Green's Fractures in Adults, 5th Edition SURGICAL AND APPLIED ANATOMY Part of "47 - ANKLE FRACTURES"
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and
 Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
Section Three: The Leg, Ankle, and Foot Lecture: Review of Clinical Anatomy, Patterns of Dysfunction and Injury, and Treatment Implications for the Leg, Ankle, and Foot Levels I and II Demonstration and
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately
 1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
1. A worker falls from a height and lands on his feet. Radiographs reveal a fracture of the sustentaculum tali. The muscle passing immediately beneath it that would be adversely affected is the: fibularis
Application of High-resolution Ultrasonography for the Diagnosis of a Case With Sports-related Sural Neuritis
 C A S E R E P O R T Application of High-resolution Ultrasonography for the Diagnosis of a Case With Sports-related Sural Neuritis Tsung-Ching Lin 1, Hsiu-Ling Chou 2, Hong-Jen Chiou 3, Cheng-Ming Chiu
C A S E R E P O R T Application of High-resolution Ultrasonography for the Diagnosis of a Case With Sports-related Sural Neuritis Tsung-Ching Lin 1, Hsiu-Ling Chou 2, Hong-Jen Chiou 3, Cheng-Ming Chiu
Clinical and Neurophysiological Assessment of Cervical Radiculopathy
 Mohamed El-Khatib et al. Clinical and Neurophysiological Assessment of Cervical Radiculopathy Mohamed G. El-Khatib 1, Mohamed Saad 1, Seyam Saeed 2, Mohamed El-Sayed 1 Departments of Neurology, Mansoura
Mohamed El-Khatib et al. Clinical and Neurophysiological Assessment of Cervical Radiculopathy Mohamed G. El-Khatib 1, Mohamed Saad 1, Seyam Saeed 2, Mohamed El-Sayed 1 Departments of Neurology, Mansoura
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program
 Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Therapeutic Foot Care Certificate Program Part I: Online Home Study Program 1 Anatomy And Terminology Of The Lower Extremity Joan E. Edelstein, MA, PT, FISPO Associate Professor of Clinical Physical Therapy
Evaluation and treatment of peroneal neuropathy
 Curr Rev Musculoskelet Med (2008) 1:147 153 DOI 10.1007/s12178-008-9023-6 Evaluation and treatment of peroneal neuropathy Jennifer Baima Æ Lisa Krivickas Published online: 11 March 2008 Ó Humana Press
Curr Rev Musculoskelet Med (2008) 1:147 153 DOI 10.1007/s12178-008-9023-6 Evaluation and treatment of peroneal neuropathy Jennifer Baima Æ Lisa Krivickas Published online: 11 March 2008 Ó Humana Press
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer
 musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
musculoskeletal system anatomy muscles of foot sheet done by: dina sawadha & mohammad abukabeer Extensor retinaculum : A- superior extensor retinaculum (SER) : originates from the distal ends of the tibia
Department of Physical Medicine and Rehabilitation, Korea University College of Medicine, Seoul; 2
 Original Article Ann Rehabil Med 2016;40(3):457-462 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.3.457 Annals of Rehabilitation Medicine Optimal Needle Placement for Extensor
Original Article Ann Rehabil Med 2016;40(3):457-462 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2016.40.3.457 Annals of Rehabilitation Medicine Optimal Needle Placement for Extensor
Anatomy & Physiology. Muscles of the Lower Limbs.
 Anatomy & Physiology Muscles of the Lower Limbs http://www.ishapeup.com/musclecharts.html Muscles of the Lower Limbs Among the strongest muscles in the body. Because pelvic girdle is composed of heavy,
Anatomy & Physiology Muscles of the Lower Limbs http://www.ishapeup.com/musclecharts.html Muscles of the Lower Limbs Among the strongest muscles in the body. Because pelvic girdle is composed of heavy,
Copyright 2004, Yoshiyuki Shiratori. All right reserved.
 Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Ankle and Leg Evaluation 1. History Chief Complaint: A. What happened? B. Is it a sharp or dull pain? C. How long have you had the pain? D. Can you pinpoint the pain? E. Do you have any numbness or tingling?
Lower Limb Dr. Robin Paudel
 Lower Limb n What is a limb? n Skeleton n Joints n Pelvis or limb girdle n Hip/Hip Muscles n Lumber and sacral plexus getting spinal nerves out onto limb n Muscles anterior and posterior compartments n
Lower Limb n What is a limb? n Skeleton n Joints n Pelvis or limb girdle n Hip/Hip Muscles n Lumber and sacral plexus getting spinal nerves out onto limb n Muscles anterior and posterior compartments n
Mohammad Ashraf. Abdulrahman Al-Hanbali. Ahmad Salman. 1 P a g e
 - 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
- 7 Mohammad Ashraf Abdulrahman Al-Hanbali Ahmad Salman 1 P a g e Structures under the cover of Gluteus Maximus: 1-Bones: Ileum, Femur (Head, greater trochanter and gluteal tuberosity), Ischium (ischial
LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES
 Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
Neurology DOI: 10.15386/cjmed-382 LATE RESPONSES IN THE ELECTRODIAGNOSIS OF CERVICAL RADICULOPATHIES ANA MARIA GALAMB, IOAN DAN MINEA Department of Medical and Surgical Specialities, Faculty of Medicine,
1-Muscles: 2-Blood supply: Branches of the profunda femoris artery. 3-Nerve supply: Sciatic nerve
 1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
1-Muscles: B i c e p s f e m o r i s S e m i t e n d i n o s u s S e m i m e m b r a n o s u s a small part of the adductor magnus (h a m s t r i n g p a r t o r i s c h i a l p a r t ) 2-Blood supply:
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists
 Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Guide to the use of nerve conduction studies (NCS) & electromyography (EMG) for non-neurologists What is NCS/EMG? NCS examines the conduction properties of sensory and motor peripheral nerves. For both
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Human Anatomy Biology 255
 Human Anatomy Biology 255 Exam #4 Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
Human Anatomy Biology 255 Exam #4 Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics demonstrate that, on average,
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Introduction Compartment Syndromes of the Leg Related to Athletic Activity Mark M. Casillas, M.D. Consequences of a misdiagnosis persistence of a performance limitation loss of function/compartment loss
Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD
 Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
Numb Toes Jose Santiago Campos, MD and Eric L. Altschuler, MD, PhD No one involved in the planning of this CME activity have anyy relevant financial relationships to disclose. Authors/faculty have nothingg
The Usefulness of Proximal Radial Motor Conduction in Acute Compressive Radial Neuropathy
 JCN Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2015;11(2):178-182 / http://dx.doi.org/10.3988/jcn.2015.11.2.178 ORIGINAL ARTICLE The Usefulness of Proximal Radial Motor Conduction in
JCN Open Access pissn 1738-6586 / eissn 2005-5013 / J Clin Neurol 2015;11(2):178-182 / http://dx.doi.org/10.3988/jcn.2015.11.2.178 ORIGINAL ARTICLE The Usefulness of Proximal Radial Motor Conduction in
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
Motor and Sensory Peripheral Neuropathy in a Patient Came after Acute Carbon Monoxide Intoxication: a Case Report with Magnetic Resonance Image
 pissn 2384-1095 eissn 2384-1109 imri 2016;20:175-180 http://dx.doi.org/10.13104/imri.2016.20.3.175 Motor and Sensory Peripheral Neuropathy in a Patient Came after Acute Carbon Monoxide Intoxication: a
pissn 2384-1095 eissn 2384-1109 imri 2016;20:175-180 http://dx.doi.org/10.13104/imri.2016.20.3.175 Motor and Sensory Peripheral Neuropathy in a Patient Came after Acute Carbon Monoxide Intoxication: a
fig fig For the following diagrams
 fig. 1271 For the following diagrams Please draw small circles at the following points (pts in bold are main syllabus pts): Liver-1 Liver-2 Liver-3 Liver-4 Spleen-4 Spleen-5 Stomach-41 Stomach-42 Stomach-43
fig. 1271 For the following diagrams Please draw small circles at the following points (pts in bold are main syllabus pts): Liver-1 Liver-2 Liver-3 Liver-4 Spleen-4 Spleen-5 Stomach-41 Stomach-42 Stomach-43
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS
 HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
HUMAN BODY COURSE LOWER LIMB NERVES AND VESSELS October 22, 2010 D. LOWER LIMB MUSCLES 2. Lower limb compartments ANTERIOR THIGH COMPARTMENT General lfunction: Hip flexion, knee extension, other motions
The Foot. Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob:
 The Foot Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob: 0127155717 The skeleton of the foot Cutaneous innervations Sole of foot layers of muscles First layer -Abductor hallucis -Flexor
The Foot Dr. Wegdan Moh.Mustafa Medicine Faculty Assistant Professor Mob: 0127155717 The skeleton of the foot Cutaneous innervations Sole of foot layers of muscles First layer -Abductor hallucis -Flexor
Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B.
 UvA-DARE (Digital Academic Repository) Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B. Link to publication Citation for published version (APA): Kuijper, B. (2011). Cervical
UvA-DARE (Digital Academic Repository) Cervical radiculopathy: diagnostic aspects and non-surgical treatment Kuijper, B. Link to publication Citation for published version (APA): Kuijper, B. (2011). Cervical
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy. Dr Grace Ng Department of Paed PMH
 Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Neurophysiological Diagnosis of Birth Brachial Plexus Palsy Dr Grace Ng Department of Paed PMH Brachial Plexus Anatomy Brachial Plexus Cords Medial cord: motor and sensory conduction for median and ulnar
Anatomage Table Instructors Guide- Lower Limb
 The Lower Limb Anatomage Table Instructors Guide- Lower Limb Table of Contents Lower Limb 1- The Skeletal System...3 1: Hip Bone...3 2: Hip Joint and Femur...4 3: Patella and Knee Joint...7 4: Tibia, Fibula,
The Lower Limb Anatomage Table Instructors Guide- Lower Limb Table of Contents Lower Limb 1- The Skeletal System...3 1: Hip Bone...3 2: Hip Joint and Femur...4 3: Patella and Knee Joint...7 4: Tibia, Fibula,
stimulation with a magnetic coil. This approach has the great advantage of being relatively painless. We
 Journal ofneurology, Neurosurgery, and Psychiatry 1989;52:767-772 Magnetic stimulation in the diagnosis of lumbosacral radiculopathy S CHOKROVERTY, R SACHDEO, J DILULLO, R C DUVOISIN From the Department
Journal ofneurology, Neurosurgery, and Psychiatry 1989;52:767-772 Magnetic stimulation in the diagnosis of lumbosacral radiculopathy S CHOKROVERTY, R SACHDEO, J DILULLO, R C DUVOISIN From the Department
Quillen College of Medicine
 Ea s t T e n n e s s e e St a t e Un i v e r s i t y Quillen College of Medicine Failing to prepare is preparing to fail. John Wooden, UCL A Dr. Tom Kwasigroch Associate Dean Director, Medical Human Gross
Ea s t T e n n e s s e e St a t e Un i v e r s i t y Quillen College of Medicine Failing to prepare is preparing to fail. John Wooden, UCL A Dr. Tom Kwasigroch Associate Dean Director, Medical Human Gross
The Hip (Iliofemoral) Joint. Presented by: Rob, Rachel, Alina and Lisa
 The Hip (Iliofemoral) Joint Presented by: Rob, Rachel, Alina and Lisa Surface Anatomy: Posterior Surface Anatomy: Anterior Bones: Os Coxae Consists of 3 Portions: Ilium Ischium Pubis Bones: Pubis Portion
The Hip (Iliofemoral) Joint Presented by: Rob, Rachel, Alina and Lisa Surface Anatomy: Posterior Surface Anatomy: Anterior Bones: Os Coxae Consists of 3 Portions: Ilium Ischium Pubis Bones: Pubis Portion
The University Of Jordan Faculty Of Medicine THE LOWER LIMB. Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan
 The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
The University Of Jordan Faculty Of Medicine THE LOWER LIMB Dr.Ahmed Salman Assistant Prof. of Anatomy. The University Of Jordan Gluteal Region Cutaneous nerve supply of (Gluteal region) 1. Lateral cutaneous
Cavus Foot: Subtle and Not-So-Subtle AOFAS Resident Review Course September 28, 2013
 Cavus Foot: Subtle and Not-So-Subtle Course September 28, 2013 Matthew M. Roberts, MD Associate Professor of Clinical Orthopaedic Surgery Co-Chief, Foot and Ankle Service Hospital for Special Surgery Disclosure
Cavus Foot: Subtle and Not-So-Subtle Course September 28, 2013 Matthew M. Roberts, MD Associate Professor of Clinical Orthopaedic Surgery Co-Chief, Foot and Ankle Service Hospital for Special Surgery Disclosure
Introduction to Anatomy. Dr. Maher Hadidi. Laith Al-Hawajreh. Mar/25 th /2013
 Introduction to Anatomy Dr. Maher Hadidi Laith Al-Hawajreh 22 Mar/25 th /2013 Lower limb - The leg The skeleton of the leg is formed by two bones: 1) Medial: Tibia 2) Lateral: Fibula The two bones are
Introduction to Anatomy Dr. Maher Hadidi Laith Al-Hawajreh 22 Mar/25 th /2013 Lower limb - The leg The skeleton of the leg is formed by two bones: 1) Medial: Tibia 2) Lateral: Fibula The two bones are
