Tumours of the Central Nervous System (CNS) Histological Assessment Reporting Guide
|
|
|
- Alberta Marshall
- 5 years ago
- Views:
Transcription
1 Sponsored by Tumours of the Central Nervous System (CNS) Histological Assessment Reporting Guide Family/Last name Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory number DD MM YYYY Elements in black text are CORE. Elements in grey text are NON-CORE. SCOPE OF THIS DATASET CLINICAL INFORMATION PRIOR THERAPY (Note 1) Not administered Prior treatment not known Administered, specify RADIOLOGICAL INFORMATION TUMOUR SITE (Note 4) No macroscopically visible tumour OR select all that apply: Skull, specify precise location, if known Indeterminate RELEVANT PATIENT/FAMILY HISTORY (Note 2) Dura, specify precise location, if known Previous history of cancer, specify Not provided Leptomeninges, specify precise location, if known History of neurological tumour syndrome, specify Brain Cerebral lobes, specify precise location, if known Deep grey matter, specify Relevant familial history, specify Ventricle, specify precise location, if known Pineal, specify Other, specify Sellar/suprasellar/pituitary Brain stem, specify precise location, if known Cerebellum, specify site, if known OPERATIVE PROCEDURE (Note 3) Biopsy, specify Not provided Spine/vertebral column, specify precise location, if known Spinal cord, specify precise location, if known Resection, specify Spinal nerve root(s), specify precise location, if known Other, specify Peripheral nerve, specify site, if known Other, specify DRAFT Version 1.0 Published xxxxxx 2018 ISBN: Page 1 of 2 International Collaboration on Cancer Reporting (ICCR)
2 TUMOUR LATERALITY (Note 5) Right Left Midline Bilateral Other, specify Not specified ADEQUACY OF SPECIMEN FOR HISTOLOGICAL ASSESSMENT (Note 12) Specimen is adequate for analysis Specimen is inadequate for analysis, specify reason Crush Autolysis Cautery Necrosis Other, specify TUMOUR FOCALITY (Note 6) Unifocal Multifocal Specify number of lesions Indeterminate ADEQUACY OF SPECIMEN FOR DIAGNOSTIC PURPOSES (Note 13) Specimen is adequate for diagnostic purposes Specimen is inadequate for diagnostic purposes (e.g. not representative of likely clinic-radiological diagnosis), specify reason TUMOUR DIMENSIONS (largest/dominant lesion) (Note 7) mm x mm x mm RELATIONSHIP OF TUMOUR TO ADJACENT TISSUE (Note 8) Well demarcated Indeterminate Diffuse/infiltrative Mixed (both well-demarcated and diffuse in different areas) Peritumoral edema Absent Present HISTOLOGICAL APPEARANCE (Note 14) Describe the appearance from the WHO 2016 entities and variants based on histological appearance only Other, specify Cannot be determined HISTOLOGICAL TUMOUR GRADE (Note 15) CONTRAST ENHANCEMENT (Note 9) Non-enhancing Enhancing Diffuse/solid Patchy/heterogeneous Ring or rim Information not available WHO grade I WHO grade II WHO grade III WHO grade IV Not applicable Cannot be determined, specify INVASION (Note 16) SPECIMEN DETAILS SPECIMEN SIZE (Record for each specimen submitted) (Note 10) Cannot be assessed (e.g. only tumour is present) Not identified (i.e. tumour is well-demarcated from surrounding brain or other tissues) Present, specify type mm x mm x mm Information not available, specify SPECIMEN DESCRIPTION (Note 11) HISTOLOGICAL EVIDENCE OF PRIOR THERAPY (Note 17) No evidence of prior therapy Positive response, specify type of response Vascular changes Radiation type necrosis Reactive glial changes Inflammatory changes Granulation and/or scar tissue Foreign material (e.g. embolisation/procoagulant material) Other, specify DRAFT Version 1.0 Published xxxxxx 2018 ISBN: Page 2 of 2 International Collaboration on Cancer Reporting (ICCR)
3 Scope The dataset has been developed for the histological assessment of benign and malignant tumours of the central nervous system (CNS) and its coverings, as well as tumours from those aspects of the peripheral nervous system immediately adjacent to the CNS. This dataset applies to both biopsy and resection specimens. Tumours of the anterior pituitary gland are included. Haematological lesions that may originate in the brain are included. It is intended that this dataset should be used in conjunction with the Molecular information for CNS specimens and the Final integrated report/diagnosis for CNS specimens datasets. A full diagnosis of CNS tumours should ideally conform to the final integrated diagnoses in the 2016 World Health Organisation (WHO) Classification of Tumours of the CNS (2016 CNS WHO), which requires integration of elements from histological and ancillary analyses. Nonetheless, it is realized that some diagnoses may not fit precisely within existing diagnostic categories. 1 Note 1 Prior therapy (Non-core) Detail on prior treatment may not be available at the time of tumour diagnosis. Nonetheless, it can be helpful to know whether the patient has had specific therapies such as radiation therapy, chemotherapy, corticosteroid therapy, embolization, or radiosurgery. In particular, knowledge of such prior therapy may help to interpret changes such as necrosis, vasculature changes, cellular atypia and inflammatory cells. Note 2 - Relevant patient/family history (Non-core) Several genetic conditions (such as neurofibromatosis 1 and 2, and Turcot/Lynch, tuberous sclerosis, von-hippel- Lindau, Cowden, Li-Fraumeni and Gorlin syndromes) are known to predispose individuals to specific primary CNS tumours. Knowledge of this information may therefore help in differential diagnoses. In addition, the behavior of tumours in such syndromes may differ from those of their sporadic counterparts, and thus knowledge of a genetic condition may inform prognostic estimation. Note 3 - Operative procedure 2 (Non-core) The physical size of tissue specimens submitted for pathological assessment varies greatly depending on the operative procedure. Specimens obtained by stereotactic or, less commonly, endoscopic biopsy are typically the smallest and may be crushed during handling. Those from open biopsy are more ample and typically less damaged than those of stereotactic biopsy. Resection specimens are largest, and require careful macroscopic inspection in order to sample properly. Importantly, the size of the submitted sample does not always reflect the procedure; use of ultrasonic surgical aspirators, for example, may decrease the size of the submitted material relative to the total amount of resected material. Because the reliability of pathological diagnosis depends heavily on the representative nature and adequacy of material assessed, it is important to pay attention to any discrepancy between submitted material and clinical information, including operative procedures and imaging findings. Doing so can help to minimise the influence of sampling and/or regional heterogeneity on the rendered diagnosis. 1
4 Note 4 - Tumour site(s) (Non-core) Imaging studies are crucial in guiding neurosurgical and radiotherapeutic management of brain tumours. 3 Knowledge of the specific anatomic area in which the tumour resides can aid in the differential diagnosis and may correlate with tumour type and outcome. If known, it should be recorded whether a tumour is intra-axial (cerebrum, deep white matter, cerebellum, brain stem, spinal cord), extra-axial (dural/leptomeningeal, cerebellopontine angle, intraventricular, intra- or extradurally in the spinal canal), or located in the skull, skull base, sellar/suprasellar region, pineal gland, spine, etc. When available, the pathologist should indicate the exact location (e.g. cerebral convexity/lobe, lateral versus third or fourth ventricle, etc.). Note 5 - Tumour laterality (Non-core) Tumour laterality, as determined by imaging studies and as indicated by the surgeon, should be indicated as occurring on the right or left side of the CNS (e.g., right frontal lobe, left occipital convexity, right lateral ventricle, etc.). Midline tumours arising in the sellar, pineal, third or fourth ventricular, and spinal locations, among others, should be recorded as such. Occasionally, tumours may involve both sides of the brain and should be referred to as bilateral; a butterfly glioblastoma crossing the corpus callosum and involving both sides of the cerebrum is an example. Note 6 - Tumour focality (Non-core) While most CNS tumours are solitary (unifocal), multifocal examples exist, often representing malignant brain tumours (e.g., glioblastoma and CNS lymphoma). For tumours to be considered multifocal, they should be noncontiguous, as determined by neuroimaging studies although it is recognised that histological autopsy studies of such radiologically multifocal tumours may reveal contiguity between lesions. Gliomatosis cerebri, previously recognised as a distinct diffuse glioma entity involving multiple cerebral lobes, is now recognised as a growth pattern in the 2016 WHO Classification of CNS Tumours. 4 Note 7 Tumour dimensions (Non-core) Radiologic tumour dimensions serve as approximate guidance as to whether tumours have been sampled adequately, particularly when dealing with small biopsies. Post-surgery, they also give information regarding how much of the tumour has been resected. For example, radiologic-pathologic correlations can guard against making a diagnosis of low-grade glioma on a stereotactic biopsy sample obtained from the edge of a large, heterogeneously enhancing cerebral lesion. 2
5 Note 8 Relationship of tumour to adjacent tissue (Non-core) The interface between tumour and adjacent brain as depicted by neuroimaging (MRI, CT) provides information on the growth pattern and on the dynamics of tumour growth. Hyperintensity on fluid-attenuated inversion recovery (FLAIR) images may indicate an infiltrative tumour growth and reflect invasiveness of the tumour. This may also be reflected by diffuse or patchy contrast enhancement at the interface between tumour and normal brain (see below). Absence of peritumoural alterations on T2 and FLAIR sequences suggests a more benign nature of a lesion. The MRI patterns may also vary within one tumour with partly well-demarcated areas and partly infiltrative growth. Oedemais visualised as a hypointense signal alteration on T1-weighted sequences without contrast and, similar to infiltrative growth, as hyperintense signal on FLAIR sequences. Differentiation between infiltrative growth and oedema is often impossible, notably in gliomas. Slowly growing, more benign tumours induce relatively less oedema than fast growing, malignant tumours. Information provided by the surgeon on where the tissue specimens were collected relative to the MRI changes also aids the pathologist in interpreting the histological findings. Note 9 - Contrast enhancement (Non-core) Contrast enhancement is commonly interpreted as reflecting blood-brain barrier disturbance. Extra-axial tumours growing outside the brain parenchyma (e.g., meningiomas) commonly take up contrast vividly. For intrinsic brain tumours such as gliomas, contrast enhancement is commonly interpreted as a sign of increasing malignancy, but this correlation is far from complete. For example, it is not uncommon for non-enhancing diffuse gliomas to be deemed anaplastic on histological examination. Moreover, pilocytic astrocytomas, gangliogliomas, and others are exceptions since they take up contrast, but are assigned to WHO grade I and carry a favourable prognosis. Ring enhancement is commonly associated with extensive central necrosis and reflects a high grade of histological malignancy, but is occasionally seen in benign tumours as well. Contrast enhancement is subject to pharmacological modification (e.g., by corticosteroids) or antiangiogenic agents, (e.g., bevacizumab). Thus, pharmacotherapy may be a challenge for MRI interpretation. Changes in contrast enhancement have traditionally played a central role in response assessment in neuro-oncology, (e.g., in the Macdonald criteria), but the additional consideration of T2 and FLAIR sequences has increasingly been implemented into response assessment in recent years. Note 10 - Specimen size(s) (Core) Intrinsic tumours grow diffusely within the brain and in many instances cannot be completely removed. Clinical factors (e.g., performance status) and tumour location often determine the extent of resection, ranging from a stereotactic biopsy to a resection of a lobe. Surgical technique may result in a discrepancy of the amount of tissue resected and received in the pathology department, in particular when a surgical ultrasonic aspirator is used and the collected tissue is partly discarded. It is important to record the volume of tissue arriving in the pathology department and thus the amount of tissue available for diagnosis (and where possible for frozen tissue banking for subsequent studies). If a tumour, for example a schwannoma or meningioma, arrives in one piece, it can be measured relatively accurately. Brain tumour surgery, however, often results in tissue fragments, making an accurate assessment difficult. Where 3
6 possible, the size of large resection specimens should be recorded in three dimensions and piecemeal resections should be estimated by their aggregate size in three dimensions. Alternatively, an accurate and reproducible determination of the tissue volume may be achieved by weighing tissue fragments, compared to visual estimates in three dimensions, but this is not a common practice. Note 11 - Specimen description (Non-core) The description of resection margins is generally not applicable for intra-axial CNS tumours as surgical technique results in fragmented specimens in most instances, except when complete resection of a lobe can be achieved. Therefore, staging and assessment of resection margins is generally not possible and thus not included in published protocols. Additionally, diffusely infiltrative tumours have often invaded well beyond designated surgical margins, even when tumour cells are not evident at that margin. Extra-axial tumours, such as meningiomas, schwannomas, and other well-demarcated tumours can often be resected and submitted intact. This allows a description of the lesion itself, and adherent structures, such as meninges, nerve roots, and CNS tissue. However, when arriving in fragmented state, the report may necessarily be limited to a description of individual components, and the degree of fragmentation. When applicable, description should also include the presence of other components, such as CNS tissue, dura mater, skin, bone, blood clot and extrinsic components such as haemostatic material, metal clips, synthetic bone, mesh, shunt ducts etc. Specimens may arrive fresh or in fixative. This should be indicated when describing the colour of the specimen as it changes with fixation. Specimens may also arrive in already processed forms, such as blocks or slides. In such situations, description should be given for blocks and slides, indicating the number of blocks and/or slides. Slides may be described in greater detail, e.g. total number of glass slides, comprising number of H&E and other slides (e.g., immunohistochemistry, smears, controls), as well as other materials (e.g., EM prints, neuroimaging files). Note 12 - Adequacy of specimen for histological assessment (Non-core) The adequacy of a specimen for histological assessment can be affected by various intraoperative procedures, tissue fixation issues (duration in/volume of fixative), and technical processing issues in the histology laboratory. These include, but are not limited to, electrocautery/heat/laser treatment intraoperatively, distortion of tissue due to surgical instrumentation, delay in placing wet tissue into fixative by the surgeon/operating room technician, less than 10:1 fixative-to-tissue volume ratio, and excessive fracturing/knife chatter in tissue during cutting of the frozen tissue/paraffin block. Tiny size of a biopsy can lead to tissue exhaustion during processing. Highly necrotic, mucinous, fibrous, calcified, or ossified specimens may cause suboptimal processing/sectioning. Any of these conditions can obscure nuclear/nucleolar features, distort degree of cellularity, blur tumour margins, and or make mitotic activity impossible to assess. Prior freezing of the tissue for frozen section intraoperative diagnosis may negatively impact cytological assessment in the fixed, embedded tissues and immunohistochemistry for some antibodies. In each case, the pathologist should state which of these conditions make the tissue inadequate/suboptimal for histological assessment. 4
7 Note 13 - Adequacy of specimen for diagnostic purposes (Non-core) Many intraparenchymal brain lesions are surgically assessed by either small open excisional biopsy or stereotactic biopsy. While navigational equipment is usually employed to optimise targeting, the known ability of brain tissue to swell during an operative procedure can cause shifting of brain tissue during the procedure, which can result in biopsies that are suboptimally centred on the area(s) of interest. Examples of suboptimally centred tissues include: biopsies from diffuse infiltrating gliomas taken from the edge, not centre, of the tumour; biopsies from infections in which the necrotic/purulent centre may be submitted by the surgeon for culture(s), leaving the pathologist with reactive, but not organism-containing, edges of the process. Occasionally, tissue lost to intraoperative suctioning or lesional tissues given in overly generous amounts to brain banks can render the tissue sent to the pathologist suboptimal for diagnosis. Any of these situations can leave the pathologist with tissue that can be misleading in terms of type of tumour, grade of tumour, or inability to detect organisms, if present. The diagnosis possible on the submitted tissues may be under-representative or misrepresentative of the lesion based on the neuroimaging studies. In a few instances, more sophisticated testing (e.g., molecular) may be required for full/correct diagnosis, but the small tissue size, tissue processing issues, or suboptimal targeting of biopsy materials may make this testing impossible. The pathologist should specify any, and all, limitations of the tissue in achieving optimal diagnosis. Note 14 - Histological appearance (Non-core) In nearly all pathology reports of CNS neoplasms, the diagnosis should ideally include one of the >150 entities and variants listed in the 2016 CNS WHO 4,5 (see Table 1 below) and when additionally possible, the histological appearance should further be combined with signature molecular alterations to establish a more specific integrated diagnosis (e.g., diffuse astrocytoma, IDH-mutant; see section on Integrated Diagnosis). When using such an approach, histological impressions such as oligoastrocytoma and anaplastic oligoastrocytoma will virtually always be altered to either astrocytoma or oligodendroglioma categories based on specific molecular patterns identified. Similar modifications also apply to the RELA-fusion positive supratentorial ependymomas, diffuse midline gliomas, the solitary fibrous tumours/haemangiopericytomas, and the overarching group of embryonal neoplasms, such as medulloblastoma variants, atypical teratoid/rhabdoid tumour, and embryonal tumour with multilayered rosettes, each of which require additional molecular (or surrogate immunohistochemical biomarker) testing before a definitive diagnosis can be made. However, in the majority of entities still lacking disease-defining molecular signatures, the final diagnosis will be based on classical histopathology alone. In either approach (histological or integrated), obtaining as precise a final diagnosis as possible is critically important, as this forms the basis for all subsequent patient management decisions, accruing patients to the appropriate clinical trials, epidemiologically assessing disease trends over time, and establishing valid research conclusions. 6-9 As such, the strict application of WHO 2016 diagnostic guidelines is required to enhance both accuracy and interobserver reproducibility across the globe and it is noteworthy that for many entities, criteria have changed dramatically from the earlier 2007 WHO classification. In the remaining cases that do not neatly conform to a well-recognised entity or variant (see last category listed as Other (specify) ), a descriptive diagnosis should be rendered instead, providing as much information as possible including relevant molecular information (e.g., small round cell sarcoma of indeterminate type; low-grade neuroepithelial tumour with oligodendroglial-like histological features suggestive of dysembryoplastic neuroepithelial tumour or paediatric oligodendroglioma; high-grade glioneuronal neoplasm; poorly differentiated malignancy; etc.). Such cases can be considered Not Elsewhere Classified (NEC). 1 5
8 Table 1 Histologically Defined Diagnostic Category (based on histological appearance only, i.e., not full 2016 CNS WHO diagnoses) Diffuse glioma Diffuse astrocytoma Gemistocytic astrocytoma Anaplastic astrocytoma Glioblastoma Giant cell glioblastoma Gliosarcoma Epithelioid glioblastoma Oligodendroglioma Anaplastic oligodendroglioma Oligoastrocytoma Anaplastic oligoastrocytoma Pilocytic astrocytoma Pilomyxoid astrocytoma Subependymal giant cell astrocytoma Pleomorphic xanthoastrocytoma Anaplastic pleomorphic xanthoastrocytoma Chordoid glioma of third ventricle Angiocentric glioma Astroblastoma Subependymoma Myxopapillary ependymoma Ependymoma Papillary ependymoma Clear cell ependymoma Tanycytic ependymoma Anaplastic ependymoma Choroid plexus papilloma Atypical choroid plexus papilloma Choroid plexus carcinoma Dysembryoplastic neuroepithelial tumour 6
9 Gangliocytoma Ganglioglioma Anaplastic ganglioglioma Dysplastic gangliocytoma of cerebellum (Lhermitte-Duclos disease) Desmoplastic infantile astrocytoma or ganglioglioma (DIA or DIG) Papillary glioneuronal tumour Rosette-forming glioneuronal tumour Diffuse leptomeningeal glioneuronal tumour Central neurocytoma Extraventricular neurocytoma Cerebellar liponeurocytoma Paraganglioma Pineocytoma Pineal parenchymal tumour of intermediate differentiation Pineoblastoma Papillary tumour of the pineal region CNS Embryonal tumour CNS Embryonal tumour with rhabdoid features Medulloblastoma Medulloblastoma, classic Medulloblastoma, desmoplastic/nodular Medulloblastoma with extensive nodularity Medulloblastoma, large cell/anaplastic Embryonal tumour with multilayered rosettes Medulloepithelioma CNS Neuroblastoma CNS Ganglioneuroblastoma Schwannoma Cellular schwannoma Plexiform schwannoma Melanotic schwannoma Neurofibroma Plexiform neurofibroma Perineurioma Hybrid nerve sheath tumour 7
10 Malignant peripheral nerve sheath tumour (MPNST) Epithelioid MPNST Melanotic MPNST MPNST with mesenchymal differentiation MPNST with glandular differentiation MPNST with perineurial differentiation Meningioma Meningothelial meningioma Fibrous meningioma Transitional meningioma Psammomatous meningioma Angiomatous meningioma Microcystic meningioma Secretory meningioma Lymphoplasmacyte-rich meningioma Metaplastic meningioma Chordoid meningioma Clear cell meningioma Atypical meningioma Papillary meningioma Rhabdoid meningioma Anaplastic (malignant) meningioma Solitary fibrous tumour/haemangiopericytoma Haemangioblastoma Haemangioma Epithelioid hemangioendothelioma Angiosarcoma Kaposi sarcoma Ewing sarcoma-peripheral primitive neuroectodermal tumour Lipoma Angiolipoma Liposarcoma Desmoid-type fibromatosis Myofibroblastoma Inflammatory myofibroblastic tumour Benign fibrous histiocytoma Fibrosarcoma 8
11 Undifferentiated pleomorphic sarcoma (UPS)/malignant fibrous histiocytoma (MFH) Leiomyoma Leiomyosarcoma Rhabdomyoma Rhabdomyosarcoma Chondroma Chondrosarcoma Osteoma Osteochondroma Osteosarcoma Diffuse melanocytosis Meningeal melanocytoma Melanoma Meningeal melanomatosis Diffuse large B cell lymphoma (DLBCL) of the CNS Immunodeficiency-associated lymphoproliferative disorders of the CNS Low grade B cell lymphomas of the CNS T-cell and NK/T-cell lymphomas of the CNS Anaplastic large cell lymphoma Lymphomatoid granulomatosis Intravascular large B-cell lymphoma MALT lymphoma of the dura Langerhans cell histiocytosis Erdheim-Chester disease Rosai-Dorfman disease Juvenile xanthogranuloma Histiocytic sarcoma Germinoma Embryonal carcinoma Yolk sac tumour Choriocarcinoma Teratoma Mature teratoma Immature teratoma Teratoma with malignant transformation 9
12 Mixed germ cell tumour Craniopharyngioma Adamantinomatous craniopharyngioma Papillary craniopharyngioma Granular cell tumour Pituicytoma Spindle cell oncocytoma Pituitary adenoma Somatotroph adenoma Lactotroph adenoma Thyrotroph adenoma Corticotroph adenoma Gonadotroph adenoma Null cell adenoma Plurihormonal and double adenomas Pituitary carcinoma Pituitary blastoma Gangliocytoma and mixed gangliocytoma-adenoma Granular cell tumour Pituicytoma Spindle cell oncocytoma Metastatic carcinoma Metastatic melanoma Metastatic sarcoma Metastatic lymphoma/leukemia Note 15 - Histological tumour grade (Core) In as many pathology reports of CNS neoplasms as possible, the diagnosis should include a grade based on the WHO 2016 classification (see Table 2 below). 4,5 This scheme differs from the approaches in many other organ systems in that in most circumstances, the diagnosis dictates a given WHO grade rather than a range of grades within a diagnostic category. The scale of WHO grades from I to IV reflects the natural histories of various tumour types, rather than their shifting prognoses with changes in therapeutic practice over time. 6 Roughly speaking, a 10
13 WHO grade I tumour is considered benign and potentially curable by surgery, although in unfavourable locations, such tumours may still create significant morbidity. WHO grade II tumours typically are slowly growing malignancies that often recur and are associated with significant mortality, albeit with survival times of many years in most cases. WHO grade III tumours are rapidly growing malignancies with typical survivals of only a few years if treated with surgery alone. Nearly all such tumours are designated as anaplastic. WHO grade IV neoplasms are highly aggressive malignancies with rapid mortality (typically in less than 2 years after diagnosis) in the absence of adjuvant therapies (e.g., glioblastomas and embryonal neoplasms). Progression from lower-grade malignancy to higher-grade forms occurs in some CNS neoplasms, most commonly the diffuse gliomas (Table 3) and to a lesser extent in the meningiomas (Table 4). There are exceptions to the automatic assignment of a single WHO grade based on diagnosis, mostly in entities for which definite parameters for histological grading have not been established yet. Other bone and soft tissue neoplasms occurring within the neural axis are classified and graded using the same criteria as in other parts of the body. Lastly, it should be noted that in some cases, assigning a WHO grade is not possible or could cause more confusion than clarification for clinical colleagues (e.g., when the exact tumour subtype remains unclear). In such cases, it is preferable to omit the WHO grade from the final diagnosis. Table 2 WHO Grades Based on Histologically Defined Diagnostic Category (based on histological appearance only, i.e., not full 2016 CNS WHO diagnoses) Tumour Group Tumour Type Grade Astrocytic tumours Diffuse astrocytoma Anaplastic astrocytoma Glioblastoma (and variants) Pilocytic astrocytoma Pilomyxoid astrocytoma (grade not assigned) Subependymal giant cell astrocytoma Pleomorphic xanthoastrocytoma Anaplastic pleomorphic xanthoastrocytoma Oligodendrogliomas Oligodendroglioma Anaplastic oligodendroglioma Oligoastrocytomas Oligoastrocytoma Anaplastic oligoastrocytoma Ependymal tumours Ependymoma Anaplastic ependymoma Subependymoma Myxopapillary ependymoma Choroid plexus tumours Choroid plexus papilloma Other neuroepithelial tumours Atypical choroid plexus papilloma Choroid plexus carcinoma Chordoid glioma of the third ventricle Angiocentric glioma Neuronal-glial tumours Gangliocytoma I Grade II Grade III Grade IV 11
14 Tumour Group Tumour Type Desmoplastic infantile ganglioglioma/ astrocytoma (DIG/DIA) Dysembryoplastic neuroepithelial tumour Ganglioglioma Anaplastic ganglioglioma Central neurocytoma Extraventricular neurocytoma Cerebellar liponeurocytoma Papillary glioneuronal tumour Rosette-forming glioneuronal tumour of the fourth ventricle Paraganglioma of the spinal cord Pineal parenchymal tumours Pineocytoma Pineal parenchymal tumour of intermediate differentiation Pineoblastoma 12 Grade I Grade II Grade Papillary tumour of the pineal region Embryonal tumours Medulloblastoma CNS embryonal tumour, NOS Medulloepithelioma CNS Neuroblastoma CNS Ganglioneuroblastoma Ependymoblastoma Atypical teratoid/rhabdoid tumour Cranial and peripheral nerve tumours Schwannoma (and variants) Neurofibroma (and variants) Perineurioma Malignant peripheral nerve sheath tumours (MPNST) Meningeal tumours Meningioma (and variants) Mesenchymal tumours 10,11 Atypical meningioma Clear cell meningioma Chordoid meningioma Anaplastic meningioma Papillary meningioma Rhabdoid meningioma (Named as soft tissue counterpart) Solitary fibrous tumour / Haemangiopericytoma Tumours of uncertain histogenesis Haemangioblastoma III Grade IV
15 Tumour histology and grade are strong predictors of clinical behaviour for different CNS tumours, including diffusely infiltrating astrocytomas and meningiomas. Tables 3 and 4 list the grading criteria for these common CNS tumour types. Table 3 WHO Grading System for Diffuse, Infiltrating Astrocytomas WHO Grade WHO Designation Histologic Criteria II Diffuse astrocytoma Nuclear atypia III Anaplastic astrocytoma Nuclear atypia and mitotic figures IV Glioblastoma Nuclear atypia, mitotic figures, and microvascular proliferation and/or necrosis Table 4 WHO Grading of Meningiomas WHO grade I WHO grade II WHO grade III Benign meningioma (and variants) None of the criteria below for WHO grades II or III Atypical meningioma Mitotic figures 4/10 high-power fields (HPF) or At least 3 of 5 parameters: Sheeting architecture (loss of whorling and/or fascicles) Small cell formation Macronucleoli Hypercellularity Spontaneous necrosis or Brain invasion or Clear cell meningioma or Chordoid meningioma Anaplastic (malignant) meningioma Mitotic figures 20/10 HPF or Frank anaplasia (sarcoma, carcinoma, or melanoma-like histology) or Papillary meningioma or Rhabdoid meningioma 13
16 Note 16 Invasion (Non-core) Most neuroepithelial tumours, particularly infiltrating gliomas, demonstrate diffuse infiltration of tumour cells beyond grossly discernable margins. Isolated tumour cells are often present in grossly normal-appearing parenchyma surrounding the lesions. Involvement of leptomeninges and Virchow-Robin spaces are also common in gliomas, even in benign examples such as pilocytic astrocytoma and ganglioglioma. These invasions provide no prognostic significance beyond the given biological malignancy of each tumour. Furthermore, direct invasion into adjacent structures, such as dura and skull, is quite exceptional in gliomas. Assessment of such features therefore, has not been included as an element for the dataset for intra-axial CNS tumours. On the other hand, invasion of adjacent structures may be relevant in some non-neuroepithelial tumours, meningioma in particular, and can be assessed if the interface between the tumour and the adjacent tissue is appropriately submitted for assessment. Brain invasion is a criterion for atypical meningioma in the 2016 CNS WHO Classification 12 and is characterised by irregular, tongue-like protrusions of tumour tissue into underlying parenchyma without an intervening layer of leptomeninges; however, extension along Virchow-Robin spaces does not constitute brain invasion. Bone involvement has been associated with increased recurrence rates in the setting of atypical meningioma. 13 Note 17 Histological evidence of prior therapy 14 (Non-core) Prior therapy,including prior surgery, intravascular embolization, chemotherapy and radiotherapy may significantly alter the histological appearance of tissues and result in difficulties in tumour typing and grading. Information on prior therapy (see Note 1 Prior Therapy) is, however, not always available to the pathologist and the absence of histological evidence does not necessarily imply absence of prior therapy. Therapy-associated histological findings are often non-specific, except for iatrogenically introduced foreign materials such as embolic agents, and are not always adequately distinguished form tumour-associated findings. In this regard, WHO grades may not be readily assigned to the specimens after adjuvant therapies. Histological changes of radiation damage are particularly common in specimens from recurrent diffuse gliomas. These include large foci of coagulative necrosis with hypocellular edges and microcalcifications; hyalinised or necrotic vessels with enlarged, atypical endothelial cells; and pale, rarefied parenchyma with fibrin deposits. The presence of such changes is highly suggestive of prior radiation therapy, even if a clear clinical history of prior radiation has not been provided. 14
17 References 1 Louis DN, Wesseling P, Paulus W, Giannini C, Batchelor TT, Cairncross JG, Capper D, Figarella-Branger D, Lopes MB, Wick W and van den Bent M (2018). cimpact-now update 1: Not Otherwise Specified (NOS) and Not Elsewhere Classified (NEC). 2 Fuller GN (2009). Intraoperative consultation and optimal processing In: Practical Surgical Neuropathology, Perry A and Brat DJ (eds), Churchill Livingstone, Philadelphia, Vincentelli C, Hwang SN, Holder CA and Brat DJ (2012). The use of neuroimaging to guide the histologic diagnosis of central nervous system lesions. Adv Anat Pathol 19(2): Louis DN, Ohgaki H, Wiestler OD and Cavenee WK (eds) (2016). WHO Classification of Tumours of the Central Nervous System, Revised. Fourth Edition, IARC, Lyon. 5 Louis DN, Perry A, Reifenberger G, von Deimling A, Figarella-Branger D, Cavenee WK, Ohgaki H, Wiestler OD, Kleihues P and Ellison DW (2016). The 2016 World Health Organization Classification of Tumors of the Central Nervous System: a summary. Acta Neuropathologica 131(6): Louis DN, Perry A, Burger P, Ellison DW, Reifenberger G, von Deimling A, Aldape K, Brat D, Collins VP, Eberhart C, Figarella-Branger D, Fuller GN, Giangaspero F, Giannini C, Hawkins C, Kleihues P, Korshunov A, Kros JM, Beatriz Lopes M, Ng HK, Ohgaki H, Paulus W, Pietsch T, Rosenblum M, Rushing E, Soylemezoglu F, Wiestler O and Wesseling P (2014). International Society Of Neuropathology--Haarlem consensus guidelines for nervous system tumor classification and grading. Brain Pathol 24(5): van den Bent MJ, Weller M, Wen PY, Kros JM, Aldape K and Chang S (2017). A clinical perspective on the 2016 WHO brain tumor classification and routine molecular diagnostics. Neuro Oncol 19(5): Fuller CE, Jones DTW and Kieran MW (2017). New Classification for Central Nervous System Tumors: Implications for Diagnosis and Therapy. Am Soc Clin Oncol Educ Book 37: Perry A and Wesseling P (2016). Histologic classification of gliomas. Handb Clin Neurol 134: Perry A and Brat DJ (2010). Practical Surgical Pathology: A Diagnostic Approach. Elsevier, Philadelphia. 11 McLendon RE, Rosenblum MK and Bigner DD (eds) (2006). Russell and Rubinstein's Pathology of Tumors of the Nervous System. 7th ed, Hodder Arnold, New York. 12 Perry A (2016). Meningiomas. In: WHO Classification of Tumours of the Central Nervous System, Revised. Fourth Edition, Louis DN, Ohgaki H, Wiestler OD and Cavenee WK (eds), IARC, Lyon, Gabeau-Lacet D, Aghi M, Betensky RA, Barker FG, Loeffler JS and Louis DN (2009). Bone involvement predicts poor outcome in atypical meningioma. J Neurosurg 111(3): Perry A (2009). Therapy-associated neuropathology. In: Practical Surgical Neuropathology, Perry A and Brat DJ (eds), Churchill Livingstone, Philadelphia,
Protocol for the Examination of Specimens From Patients With Tumors of the Central Nervous System*
 Protocol for the Examination of Specimens From Patients With Tumors of the Central Nervous System* Version: Protocol Posting Date: December 2014 This protocol is NOT required for accreditation purposes
Protocol for the Examination of Specimens From Patients With Tumors of the Central Nervous System* Version: Protocol Posting Date: December 2014 This protocol is NOT required for accreditation purposes
Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS
 Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord
 Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/ spinal cord/peripheral nerve and pituitary. Metastatic
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/ spinal cord/peripheral nerve and pituitary. Metastatic
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord
 Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/spinal cord/peripheral nerve and pituitary. Metastatic
Protocol for the Examination of Specimens From Patients With Tumors of the Brain/Spinal Cord Protocol applies to all primary neoplasms of the brain/spinal cord/peripheral nerve and pituitary. Metastatic
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Histopathological Study and Categorisation of Brain Tumors
 Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Histopathological Study and Categorisation of Brain Tumors Ruchira Wadhwa 1*, Purvi Patel 2, Hansa Goswami 3 1 Third Year Resident, 2 Assistant Professor, 3 Professor and Head, Department of Pathology,
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
NERVOUS SYSTEM. Cambridge Illustrated Surgical Pathology
 NERVOUS SYSTEM Cambridge Illustrated Surgical Pathology Nervous System is the new atlas-oriented resource in nervous system pathology. As the fourth book in the Cambridge Illustrated Surgical Pathology
NERVOUS SYSTEM Cambridge Illustrated Surgical Pathology Nervous System is the new atlas-oriented resource in nervous system pathology. As the fourth book in the Cambridge Illustrated Surgical Pathology
Five Most Common Problems in Surgical Neuropathology
 Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
Five Most Common Problems in Surgical Neuropathology If the brain were so simple that we could understand it, we would be so simple that we couldn t Emerson Pugh What is your greatest difficulty in neuropathology?
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Supplementary Information
 Rise in Glioblastoma Multiforme incidence in England 1995 2015 suggests an adverse environmental or lifestyle factor Alasdair Philips, Denis L Henshaw, Graham Lamburn, Michael J O Carroll Supplementary
Rise in Glioblastoma Multiforme incidence in England 1995 2015 suggests an adverse environmental or lifestyle factor Alasdair Philips, Denis L Henshaw, Graham Lamburn, Michael J O Carroll Supplementary
INDEX. B Bailey and Cushing astrocytoma grade, 9 beta-hcg, 114 blepharoplasts, 14, brainstem glioma, 11, 33
 INDEX A abscess, 125,166-168 vs. glioblastoma multi forme, 167 acquired immunodeficiency virus (AIDS) [see also human immunodeficiency virus (HIV)], 125-127, 158, 161 acoustic neuroma (see schwanomma)
INDEX A abscess, 125,166-168 vs. glioblastoma multi forme, 167 acquired immunodeficiency virus (AIDS) [see also human immunodeficiency virus (HIV)], 125-127, 158, 161 acoustic neuroma (see schwanomma)
Childhood Brain and Spinal Cord Tumors Treatment Overview (PDQ )
 1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 8 04/03/2017 07.31 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Cerebral Parenchymal Lesions: I. Metastatic Neoplasms
 Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
Chapter 4 Cerebral Parenchymal Lesions: I. Metastatic Neoplasms After one has reasonably ruled out the possibility of a nonneoplastic diagnosis (see Chap. 3), one is left with considering a diagnosis of
Neoplasms of the Heart, Pericardium, and Great Vessels Histopathology Reporting Guide
 Neoplasms of the Heart, Pericardium, and Great Vessels Histopathology Reporting Guide Family/Last name Gender Male Female Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
Neoplasms of the Heart, Pericardium, and Great Vessels Histopathology Reporting Guide Family/Last name Gender Male Female Given name(s) Date of birth DD MM YYYY Patient identifiers Date of request Accession/Laboratory
Shared Care & Survival CTYA SSCRG (Childhood Cancer Research Group)
 Shared Care & Survival CTYA SSCRG (Childhood Cancer Research Group) January 2013 The NCIN is a UK-wide initiative, working to drive improvements in standards of cancer care and clinical outcomes by improving
Shared Care & Survival CTYA SSCRG (Childhood Cancer Research Group) January 2013 The NCIN is a UK-wide initiative, working to drive improvements in standards of cancer care and clinical outcomes by improving
Methoden / Methods inc. ICCC-3 105
 Methoden / Methods inc. ICCC-3 105 Internationale Klassifikation der Krebserkrankungen bei Kindern (ICCC-3) Zuordnung von ICD-O-3-Codes für Morphologie und Topographie zu diagnostischen Kategorien International
Methoden / Methods inc. ICCC-3 105 Internationale Klassifikation der Krebserkrankungen bei Kindern (ICCC-3) Zuordnung von ICD-O-3-Codes für Morphologie und Topographie zu diagnostischen Kategorien International
In 1988 Dumas-Duport et al. first used
 Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Copyright 2009, Barrow Neurological Institute Dysembryoplastic Neuroepithelial Tumor: A Review Mark Garrett, MD Jennifer Eschbacher, MD Peter Nakaji, MD Most DNETs are benign, low-grade lesions. However,
Childhood Brain and Spinal Cord Tumors Treatment Overview (PDQ )
 1 di 14 27/11/2016 17.42 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 14 27/11/2016 17.42 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
SUPPLEMENTARY INFORMATION
 VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
VOLUME: 1 ARTICLE NUMBER: 0027 In the format provided by the authors and unedited. Rapid intraoperative histology of unprocessed surgical specimens via fibre-laser-based stimulated Raman scattering microscopy
Protocol applies to all neoplasms of the brain/spinal cord. Excludes neoplasms of the pituitary gland.
 Brain/Spinal Cord Protocol applies to all neoplasms of the brain/spinal cord. Excludes neoplasms of the pituitary gland. Protocol revision date: January 2005 No AJCC/UICC staging system Procedures Cytology
Brain/Spinal Cord Protocol applies to all neoplasms of the brain/spinal cord. Excludes neoplasms of the pituitary gland. Protocol revision date: January 2005 No AJCC/UICC staging system Procedures Cytology
S2199 S2200. * Speaker's diagnosis 78
 98 21 2 14 13:30 * Speaker's diagnosis 78 S2199 Meningioma 48 Papillary meningioma * 30 Angiomatous meningioma 15 Ependymoma 12 Papillary ependymoma 6 Anaplastic ependymoma 2 Cellular ependymoma 1 Hemangioblastoma
98 21 2 14 13:30 * Speaker's diagnosis 78 S2199 Meningioma 48 Papillary meningioma * 30 Angiomatous meningioma 15 Ependymoma 12 Papillary ependymoma 6 Anaplastic ependymoma 2 Cellular ependymoma 1 Hemangioblastoma
Brain tumors: tumor types
 Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Effective January 1, 2018 ICD O 3 codes, behaviors and terms are site specific
 Effective January 1, 2018 codes, behaviors and terms are site specific /N 8551/3 Acinar adenocarcinoma (C34. _) Lung primaries diagnosed prior to 1/1/2018 use code 8550/3 For prostate (all years) see 8140/3
Effective January 1, 2018 codes, behaviors and terms are site specific /N 8551/3 Acinar adenocarcinoma (C34. _) Lung primaries diagnosed prior to 1/1/2018 use code 8550/3 For prostate (all years) see 8140/3
Effective January 1, 2018 ICD O 3 codes, behaviors and terms are site specific
 Effective January 1, 2018 codes, behaviors and terms are site specific Status /N 8010/3 Urachal carcinoma (C65.9, C66.9, C67. _, C68._) 8013/3 Combined large cell neuroendocrine carcinoma (C34. _, C37.9)
Effective January 1, 2018 codes, behaviors and terms are site specific Status /N 8010/3 Urachal carcinoma (C65.9, C66.9, C67. _, C68._) 8013/3 Combined large cell neuroendocrine carcinoma (C34. _, C37.9)
2018 ICD-O-3 Updates in Table Format with Annotation for Reference
 Status Histology Description (this may be preferred term or a synonym) Report Comments New term 8010 3 Urachal carcinoma (C65.9, C66.9, C67._, C68._) New term 8013 3 Combined large cell neuroendocrine
Status Histology Description (this may be preferred term or a synonym) Report Comments New term 8010 3 Urachal carcinoma (C65.9, C66.9, C67._, C68._) New term 8013 3 Combined large cell neuroendocrine
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad
 Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Anaplastic Pilocytic Astrocytoma: The fusion of good and bad Alexandrina Nikova 1, Charalampos-Chrysovalantis Chytoudis-Peroudis 2, Penelope Korkolopoulou 3 and Dimitrios Kanakis 4 Abstract 5 Pilocytic
Adult Brain and Spinal Cord Tumors
 Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
2. Subependymal giant cell astrocytoma:
 I. Astrocytomas: A. Diffusely infiltrating ( astrocytoma, anaplastic astrocytoma, GBM) B. Localised (pilocytic astrocytoma, pleomorphic xanthoastrocytoma, SGCA) *Grading: Diffuse: 1. Astrocytoma WHO grade
I. Astrocytomas: A. Diffusely infiltrating ( astrocytoma, anaplastic astrocytoma, GBM) B. Localised (pilocytic astrocytoma, pleomorphic xanthoastrocytoma, SGCA) *Grading: Diffuse: 1. Astrocytoma WHO grade
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Accuracy of intra-operative rapid diagnosis by Squash smear in CNS lesions An early institutional experience. KK Bansal,
 Accuracy of intra-operative rapid diagnosis by Squash smear in CNS lesions An early institutional experience. KK Bansal, Monika Bansal, Sanjeev Kishore, Anuradha K, Meena H, Dushyant G. Department of Neurosurgery
Accuracy of intra-operative rapid diagnosis by Squash smear in CNS lesions An early institutional experience. KK Bansal, Monika Bansal, Sanjeev Kishore, Anuradha K, Meena H, Dushyant G. Department of Neurosurgery
Q&A. Fabulous Prizes. Collecting Cancer Data:CNS 2/7/12. NAACCR Webinar Series Collecting Cancer Data Central Nervous System
 Collecting Cancer Data Central Nervous System NAACCR 2012 2013 Webinar Series 2/7/2013 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants
Collecting Cancer Data Central Nervous System NAACCR 2012 2013 Webinar Series 2/7/2013 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
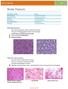 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
The new WHO 2016 classification of brain tumors what neurosurgeons need to know
 DOI 10.1007/s00701-016-3062-3 REVIEW ARTICLE - BRAIN TUMORS The new WHO 2016 classification of brain tumors what neurosurgeons need to know Rouzbeh Banan 1 & Christian Hartmann 1 Received: 8 July 2016
DOI 10.1007/s00701-016-3062-3 REVIEW ARTICLE - BRAIN TUMORS The new WHO 2016 classification of brain tumors what neurosurgeons need to know Rouzbeh Banan 1 & Christian Hartmann 1 Received: 8 July 2016
Collecting Cancer Data: Central Nervous System Prizes! Question of the Month! Tip of the Month! Q&A
 Collecting Cancer Data: Central Nervous NAACCR 2008 2009 Webinar Series April 2, 2009 Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous
Collecting Cancer Data: Central Nervous NAACCR 2008 2009 Webinar Series April 2, 2009 Prizes! Question of the Month! The participant that submits the best question of the session will receive a fbl fabulous
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas
 The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
The New WHO Classification and the Role of Integrated Molecular Profiling in the Diagnosis of Malignant Gliomas Stefan Prokop, MD Neuropathology Fellow Hospital of the University of Pennsylvania Background
Adult Central Nervous System Tumors Treatment (PDQ )
 1 di 20 28/06/2016 11.18 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
1 di 20 28/06/2016 11.18 NCBI Bookshelf. A service of the National Library of Medicine, National Institutes of Health. PDQ Cancer Information Summaries [Internet]. Bethesda (MD): National Cancer Institute
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
2 Berkeley Street, Suite 403, Toronto, Ontario M5A 2W3 Visit us at: Tel: Fax:
 E-Path A.I. Engine Knowledge Base Enhancements Version 1.0.0.29 April 1, 2018 The major enhancements in the E-Path Knowledge Base from versions 1.0.0.28 through 1.0.0.29 are as follows: 1. Addition/modification
E-Path A.I. Engine Knowledge Base Enhancements Version 1.0.0.29 April 1, 2018 The major enhancements in the E-Path Knowledge Base from versions 1.0.0.28 through 1.0.0.29 are as follows: 1. Addition/modification
Case #3. USCAP Neuropathology Evening Seminar/Companion Meeting
 Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
Case #3 USCAP Neuropathology Evening Seminar/Companion Meeting Clinical History A 71-year year-old man presented with a 4-4 week history of word finding difficulty. An initial screening head CT followed
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS JASSIN M. JOURIA, MD DR. JASSIN M. JOURIA IS A MEDICAL DOCTOR, PROFESSOR OF ACADEMIC MEDICINE, AND MEDICAL AUTHOR. HE GRADUATED FROM ROSS UNIVERSITY SCHOOL OF MEDICINE
SURGICAL MANAGEMENT OF BRAIN TUMORS JASSIN M. JOURIA, MD DR. JASSIN M. JOURIA IS A MEDICAL DOCTOR, PROFESSOR OF ACADEMIC MEDICINE, AND MEDICAL AUTHOR. HE GRADUATED FROM ROSS UNIVERSITY SCHOOL OF MEDICINE
Neuropathology Evening Session: Case 3
 Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Neuropathology Evening Session: Case 3 Christine E. Fuller, MD Cincinnati Children s Hospital Medical Center Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
H Haloes cautions, 57 neurocytomas, perinuclear, 56 Headache blue cell tumors, 147 cautions, 135, 147, 152 clinical history, 132, 144, 148
 Index A ADC. See Apparent diffusion coefficient Adult. See also Supratentorial mass, adult cerebral tumor, 1 headache and ataxia cysts, mural nodules, 118 sporadic tumors, 118 headaches and visual changes,
Index A ADC. See Apparent diffusion coefficient Adult. See also Supratentorial mass, adult cerebral tumor, 1 headache and ataxia cysts, mural nodules, 118 sporadic tumors, 118 headaches and visual changes,
Contents Part I Introduction 1 General Description 2 Natural History: Importance of Size, Site, Histopathology
 Contents Part I Introduction 1 General Description... 3 1.1 Introduction... 3 1.2 Incidence and Prevalence... 5 1.3 Predisposing and Genetic Factors... 8 References... 16 2 Natural History: Importance
Contents Part I Introduction 1 General Description... 3 1.1 Introduction... 3 1.2 Incidence and Prevalence... 5 1.3 Predisposing and Genetic Factors... 8 References... 16 2 Natural History: Importance
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
The Relevance of Cytologic Atypia in Cutaneous Neural Tumors
 The Relevance of Cytologic Atypia in Cutaneous Neural Tumors Recent Findings - New Developments New Problems Zsolt B. Argenyi, M.D. Professor of Pathology & Dermatology Director of Dermatopathology Department
The Relevance of Cytologic Atypia in Cutaneous Neural Tumors Recent Findings - New Developments New Problems Zsolt B. Argenyi, M.D. Professor of Pathology & Dermatology Director of Dermatopathology Department
Gliomas in the 2016 WHO Classification of CNS Tumors
 Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
Gliomas in the 2016 WHO Classification of CNS Tumors Hindi N Al-Hindi, MD, FCAP Consultant Neuropathologist and Head Section of Anatomic Pathology Department of Pathology and Laboratory Medicine King Faisal
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or
 monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
monotonous, stippled, round, smoothcontoured nuclei and scanty acidophilic or vacuolated cytoplasm. The cells are surrounded by a loose fibrillary stroma that is traversed by delicate capillaries. Ill
Collecting Cancer Data: CNS 1/6/2011. Collecting Cancer Data: Brain and Central Nervous System. NAACCR Webinar Series 1.
 Collecting Cancer Data: Brain and Central Nervous System January 6, 2011 NAACCR 2010-2011 Webinar Series Agenda Coding Moment Overview Multiple Primary/Histology Rules Collaborative Stage Treatment Fabulous
Collecting Cancer Data: Brain and Central Nervous System January 6, 2011 NAACCR 2010-2011 Webinar Series Agenda Coding Moment Overview Multiple Primary/Histology Rules Collaborative Stage Treatment Fabulous
2 NEUROPATHOLOGY AND MOLECULAR BIOLOGY OF INTRACRANIAL TUMORS
 2 NEUROPATHOLOGY AND MOLECULAR BIOLOGY OF INTRACRANIAL TUMORS Gregory N. Fuller and Kenneth D. Aldape Chapter Overview... 23 Introduction... 24 Cornerstones of Clinical Oncologic Neuropathology... 24 Knowledge
2 NEUROPATHOLOGY AND MOLECULAR BIOLOGY OF INTRACRANIAL TUMORS Gregory N. Fuller and Kenneth D. Aldape Chapter Overview... 23 Introduction... 24 Cornerstones of Clinical Oncologic Neuropathology... 24 Knowledge
Pleomorphic Xanthoastrocytoma
 Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Pleomorphic Xanthoastrocytoma Christine E. Fuller Keywords Pleomorphic xanthoastrocytoma; Pleomorphic xanthoastrocytoma with anaplastic features 2.1 OVERVIEW Pleomorphic xanthoastrocytoma (PXA) is an uncommon
Oligodendrogliomas & Oligoastrocytomas
 Oligodendrogliomas & Oligoastrocytomas ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit organization dedicated solely
Oligodendrogliomas & Oligoastrocytomas ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the first national nonprofit organization dedicated solely
Malignant Peripheral Nerve Sheath Tumor
 C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
C H A P T E R 120 Malignant Peripheral Nerve Sheath Tumor Currently, malignant peripheral nerve sheath tumor (MPNST) is the most commonly used generic name for the neoplasms known in the past as neurosarcoma,
SPECIAL SLIDE SEMINAR CASE 3
 SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
SPECIAL SLIDE SEMINAR CASE 3 Tihana Džombeta, MD Leo Pažanin, MD, PhD Department of Pathology, School of Medicine, University of Zagreb Department of Pathology, Clinical Hospital Centre Sestre milosrdnice
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
BAH1 - Primary Glioblastoma
 BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
BAH1 - Primary Glioblastoma R frontal tumour for frozen section. No known primary. Contrast enhancing lesion. Cholecystectomy. FROZEN SECTION REPORT Right frontal tumour: The specimen consists of multiple
DelMarVa-DC Regional Cancer Registrar s Educational Meeting. Doordan Conference Center Anne Arundel Medical Center Annapolis, MD
 DelMarVa-DC Regional Cancer Registrar s Educational Meeting Doordan Conference Center Anne Arundel Medical Center Annapolis, MD TNM Transition Updates & News from SEER Peggy Adamo, RHIT, CTR NCI SEER adamom@mail.nih.gov
DelMarVa-DC Regional Cancer Registrar s Educational Meeting Doordan Conference Center Anne Arundel Medical Center Annapolis, MD TNM Transition Updates & News from SEER Peggy Adamo, RHIT, CTR NCI SEER adamom@mail.nih.gov
Grading of Bone Tumors
 Grading of Bone Tumors Joon Hyuk Choi, M.D. Department of Pathology College of Medicine, Yeungnam University Introduction to grading system of bone tumor used at Mayo Clinic WHO Histologic Classification
Grading of Bone Tumors Joon Hyuk Choi, M.D. Department of Pathology College of Medicine, Yeungnam University Introduction to grading system of bone tumor used at Mayo Clinic WHO Histologic Classification
AMERICAN BRAIN TUMOR ASSOCIATION. Oligodendroglioma and Oligoastrocytoma
 AMERICAN BRAIN TUMOR ASSOCIATION Oligodendroglioma and Oligoastrocytoma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the
AMERICAN BRAIN TUMOR ASSOCIATION Oligodendroglioma and Oligoastrocytoma ACKNOWLEDGEMENTS ABOUT THE AMERICAN BRAIN TUMOR ASSOCIATION Founded in 1973, the American Brain Tumor Association (ABTA) was the
IAP XXVI International Congress Slide Seminar 07 (SS07)
 IAP XXVI International Congress Slide Seminar 07 (SS07) Pitfalls in Surgical Neuropathology Case 6 Richard A. Prayson, M.D. Cleveland Clinic Foundation Clinical History 64M S/P resection of pituitary adenoma
IAP XXVI International Congress Slide Seminar 07 (SS07) Pitfalls in Surgical Neuropathology Case 6 Richard A. Prayson, M.D. Cleveland Clinic Foundation Clinical History 64M S/P resection of pituitary adenoma
The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression
 The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression Alexis Roy, Harvard Medical School, Year III Our Patient AB: Clinical Presentation 53 year old female with a past
The Radiologic Evaluation of Glioblastoma (GBM) and Differentiation from Pseudoprogression Alexis Roy, Harvard Medical School, Year III Our Patient AB: Clinical Presentation 53 year old female with a past
Nonepithelial Tumors
 Nonepithelial Tumors General Definitions Mesenchymal Tumors These tumors consist of tissues that originate in the middle germ layer or mesoderm, primarily from the pluripotential supporting tissue of the
Nonepithelial Tumors General Definitions Mesenchymal Tumors These tumors consist of tissues that originate in the middle germ layer or mesoderm, primarily from the pluripotential supporting tissue of the
CASE year old male with a PET avid nodule in the left adrenal gland
 CASE 1 55 year old male with a PET avid nodule in the left adrenal gland Case 1 Adrenal gland parenchyma partly replaced by a spindle cell tumour with mild nuclear pleomorphism Atypical mitoses present
CASE 1 55 year old male with a PET avid nodule in the left adrenal gland Case 1 Adrenal gland parenchyma partly replaced by a spindle cell tumour with mild nuclear pleomorphism Atypical mitoses present
CODING TUMOUR MORPHOLOGY. Otto Visser
 CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
3/27/2017. Disclosure of Relevant Financial Relationships
 Ophthalmic Pathology Evening Specialty Conference USCAP 2017 5 th March, 2017 Mukul K. Divatia, MD Assistant Professor Department of Pathology & Genomic Medicine Weill Cornell Medical College Houston Methodist
Ophthalmic Pathology Evening Specialty Conference USCAP 2017 5 th March, 2017 Mukul K. Divatia, MD Assistant Professor Department of Pathology & Genomic Medicine Weill Cornell Medical College Houston Methodist
Epidemiology of Primary Brain and Central Nervous System Tumors in Korea
 www.jkns.or.kr 1.334/jkns.21.48.2.145 J Korean Neurosurg Soc 48 : 145-152, 21 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 21 The Korean Neurosurgical Society Clinical Article Epidemiology of Primary
www.jkns.or.kr 1.334/jkns.21.48.2.145 J Korean Neurosurg Soc 48 : 145-152, 21 Print ISSN 25-3711 On-line ISSN 1598-7876 Copyright 21 The Korean Neurosurgical Society Clinical Article Epidemiology of Primary
Histogenetic Classification of Neoplasms
 General Pathology Histogenetic Classification of Neoplasms Neuroectodermal, Mixed, Germ Cell Neoplasms, and Mesothelioma Inst. Pathol.,1 st Faculty of Medicine Charles University, Prague Neuroectodermal,
General Pathology Histogenetic Classification of Neoplasms Neuroectodermal, Mixed, Germ Cell Neoplasms, and Mesothelioma Inst. Pathol.,1 st Faculty of Medicine Charles University, Prague Neuroectodermal,
The WHO Classification of Tumors of the Nervous System
 Journal of Neuropathology and Experimental Neurology Vol. 61, No. 3 Copyright 2002 by the American Association of Neuropathologists March, 2002 pp. 215 225 The WHO Classification of Tumors of the Nervous
Journal of Neuropathology and Experimental Neurology Vol. 61, No. 3 Copyright 2002 by the American Association of Neuropathologists March, 2002 pp. 215 225 The WHO Classification of Tumors of the Nervous
Understanding general brain tumor pathology, Part I: The basics. Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky
 Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Understanding general brain tumor pathology, Part I: The basics Craig Horbinski, M.D., Ph.D. Department of Pathology University of Kentucky plan of attack what IS a pathologist, anyway? what s so special
Neoplasms of the BRAIN and CNS
 Neoplasms of the BRAIN and CNS 2015-21016 FCDS Educational Webcast Series Steven Peace, BS, CTR October 15, 2015 2015 Focus Anatomy SSS 2000 MPH Rules AJCC TNM Presentation Outline Overview Reportable
Neoplasms of the BRAIN and CNS 2015-21016 FCDS Educational Webcast Series Steven Peace, BS, CTR October 15, 2015 2015 Focus Anatomy SSS 2000 MPH Rules AJCC TNM Presentation Outline Overview Reportable
Frequency of non specific morphology codes (ICD O M) within the National Cancer Data Repository ( ) for cancer in Teenagers and Young Adults
 Frequency of non specific morphology codes (ICD O M) within the National Cancer Data Repository (2007 09) for cancer in Teenagers and Young Adults (TYA) CTYA SSCRG Data quality report on the frequency
Frequency of non specific morphology codes (ICD O M) within the National Cancer Data Repository (2007 09) for cancer in Teenagers and Young Adults (TYA) CTYA SSCRG Data quality report on the frequency
Meningiomas account for approximately 4% of all
 Intraorbital Meningiomas A Pathologic Review Using Current World Health Organization Criteria Deepali Jain, MD; Katayoon B. Ebrahimi, MD; Neil R. Miller, MD; Charles G. Eberhart, MD, PhD N Context. Meningiomas
Intraorbital Meningiomas A Pathologic Review Using Current World Health Organization Criteria Deepali Jain, MD; Katayoon B. Ebrahimi, MD; Neil R. Miller, MD; Charles G. Eberhart, MD, PhD N Context. Meningiomas
Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille
 Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
Novelties in the WHO 2016 classification of brain tumours Pr D.Figarella-Branger Service d Anatomie Pathologique et de Neuropathologie, La Timone, Marseille UMR 911 Inserm, Université d Aix-Marseille The
Update on Sarcomas of the Head and Neck. Kevin Harrington
 Update on Sarcomas of the Head and Neck Kevin Harrington Overview Classification and incidence of sarcomas Clinical presentation Challenges to treatment Management approaches Prognostic factors Radiation-induced
Update on Sarcomas of the Head and Neck Kevin Harrington Overview Classification and incidence of sarcomas Clinical presentation Challenges to treatment Management approaches Prognostic factors Radiation-induced
Rapid recurrence of a malignant meningioma: case report
 Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
Romanian Neurosurgery Volume XXXI Number 2 2017 April-June Article Rapid recurrence of a malignant meningioma: case report Oguz Baran, Sima Sayyahmeli, Taner Tanriverdi, Pamir Erdincler TURKEY DOI: 10.1515/romneu-2017-0027
FINALIZED SEER SINQ QUESTIONS
 0076 Source 1: WHO Class CNS Tumors pgs: 33 MP/H Rules/Histology--Brain and CNS: What is the histology code for a tumor originating in the cerebellum and extending into the fourth ventricle described as
0076 Source 1: WHO Class CNS Tumors pgs: 33 MP/H Rules/Histology--Brain and CNS: What is the histology code for a tumor originating in the cerebellum and extending into the fourth ventricle described as
Patients Treated with Leksell Gamma Knife
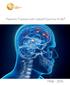 Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
Patients Treated with Leksell Gamma Knife 1968-2016 TREATMENTS REPORTED 2016 BY REGION AND INDICATION INDICATION Asia excl. Europe Latin Middle East & Africa North Grand Total Benign Tumors 12283 9778
I have no conflicts of interest in relation to this presentation. Vogel FS & Burger PC 3/28/2016
 IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
IF THIS IS NOT GLIOBLASTOMA, THEN WHAT IS IT? Murat Gokden, MD Department of Pathology/Neuropathology University of Arkansas for Medical Sciences Little Rock, AR mgokden@uams.edu I have no conflicts of
Advances In Orbital Neuropathology
 Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Neuroimaging Core Curriculum
 Neuroimaging Core Curriculum Program Content The purpose of the training program is to prepare the physician for the independent practice of neuroimaging. Neuroimaging is the subspecialty of Neurology
Neuroimaging Core Curriculum Program Content The purpose of the training program is to prepare the physician for the independent practice of neuroimaging. Neuroimaging is the subspecialty of Neurology
Histological pattern of central nervous system neoplasms
 ecommons@aku Department of Pathology and Laboratory Medicine Medical College, Pakistan April 2001 Histological pattern of central nervous system neoplasms Z. Ahmed Aga Khan University S. Muzaffar Aga Khan
ecommons@aku Department of Pathology and Laboratory Medicine Medical College, Pakistan April 2001 Histological pattern of central nervous system neoplasms Z. Ahmed Aga Khan University S. Muzaffar Aga Khan
Disclosures. An update on ancillary techniques in the diagnosis of soft tissue tumors. Ancillary techniques. Introduction
 Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
Classification of spontaneous brain tumors in rats
 Classification of spontaneous brain tumors in rats Central Nervous System Neoplasms in the Rat (Solleveld HA, et al., 1991) 1. Tumors of Neuroepithelial Tissue A. Astrocytic and oligodendroglial tumors
Classification of spontaneous brain tumors in rats Central Nervous System Neoplasms in the Rat (Solleveld HA, et al., 1991) 1. Tumors of Neuroepithelial Tissue A. Astrocytic and oligodendroglial tumors
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
WHO 2016 CNS TUMOR CLASSIFICATION UPDATE. Arie Perry, M.D. Director, Neuropathology
 WHO 2016 CNS TUMOR CLASSIFICATION UPDATE Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
WHO 2016 CNS TUMOR CLASSIFICATION UPDATE Arie Perry, M.D. Director, Neuropathology DISCLOSURES (Arie Perry, MD) I have no financial relationships to disclose. - and - I will not discuss off label use or
USCAP Neuropathology. Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC
 USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
USCAP Neuropathology Case No. 3 Elisabeth J. Rushing, MD Armed Forces Institute of Pathology Washington, DC Clinical history The patient is a 9 year-old boy who has had seizures since age 2, at which time
LOW GRADE ASTROCYTOMAS
 LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
LOW GRADE ASTROCYTOMAS This article was provided to us by David Schiff, MD, Associate Professor of Neurology, Neurosurgery, and Medicine at University of Virginia, Charlottesville. We appreciate his generous
Chapter 1 Introduction
 Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Chapter 1 Introduction Men think epilepsy divine, merely because they do not understand it. But if they called everything divine which they do not understand, why, there would be no end to divine things.
Protocol for management of patients with pineal region tumours v1
 Protocol for management of patients with pineal region tumours v1 West Midlands Cancer Alliance Coversheet for Cancer Alliance Expert Advisory Group Agreed Documentation This sheet is to accompany all
Protocol for management of patients with pineal region tumours v1 West Midlands Cancer Alliance Coversheet for Cancer Alliance Expert Advisory Group Agreed Documentation This sheet is to accompany all
TUMORS of nervous system
 TUMORS of nervous system By: Shifaa Alqa qa Done By : Ola Hijjawi CNS tumors : The annual incidence of CNS tumors ranges from 10 to 17 per 100,000 persons for intracranial tumors and 1 to 2 per 100,000
TUMORS of nervous system By: Shifaa Alqa qa Done By : Ola Hijjawi CNS tumors : The annual incidence of CNS tumors ranges from 10 to 17 per 100,000 persons for intracranial tumors and 1 to 2 per 100,000
5/10. Pathology Soft tissue tumors. Farah Bhani. Mohammed Alorjani
 5/10 Pathology Soft tissue tumors Mohammed Alorjani Farah Bhani Slides are included in this sheet. Objectives: Soft tissue tumors 1. Describe soft tissue tumors. 2. Understand the classification of soft
5/10 Pathology Soft tissue tumors Mohammed Alorjani Farah Bhani Slides are included in this sheet. Objectives: Soft tissue tumors 1. Describe soft tissue tumors. 2. Understand the classification of soft
