GUYTON AND HALL. 13 TH EDITION. Reproductive System Male: P , Female: , ,
|
|
|
- Julian Byrd
- 6 years ago
- Views:
Transcription
1 GUYTON AND HALL. 13 TH EDITION Reproductive System Male: P , Female: , ,
2 Fig b
3
4 shape and motility are important
5 Fig a
6 Fig c
7 Fig
8 Fig a
9 Fig c
10 Fig. 29.T02
11
12
13 CONTROL OF TESTICULAR FUNCTION HYPOTHALAMUS GRH + ANTERIOR PITUITARY TESTES SERTOLI CELL FSH LH LEYDIG CELL SPERMATOGENESIS INHIBIN TESTOSTERONE
14 +/- +/- CNS hypothalamus neurons gonadotropin releasing hormone Hypothalamic-pituitarygonadal axis +/- +/- LH ant. pituitary FSH thecal cells androgens inhibin LH R progestins + _ granulosa cells FSH R (LH R) activin Copyright 2006 by Elsevier, Inc. estrogens + Reproductive tract
15 Male Reproductive System
16
17 HORMONES GERM CELL
18
19
20 Testis Cross Section Interstitial Cells Produce Testosterone
21
22 Fig
23 Cell Divisions During Spermatogenesis
24
25 Fig
26 Morphology of Sperm head, neck, body, tail acrosome: cap at top of sperm head, contains hyaluronidase and proteolytic enzymes, important in penetration into ovum mitochondria arranged around body & tail flagellum outgrowth of centriole two microtubules in center, nine around the outside Optimal motility: ph 6-6.5
27 Epididymis: Sperm maturation Develops capability of motility Storage? To one month in suppressed state
28 Seminal vesicle: Secretes mucoid material rich in Fructose, Citric acid, Prostaglandins, Fibrinogen. PGs i) make cervical mucus more receptive to sperm movement ii) reverse peristaltic movement in the uterus and fallopian tubes
29 Prostate gland : Secrete thin milky fluid contains electrolytes: Ca, Cl, HPO3 Clotting enzymes, LMW polypeptides, proteins ph = Slightly alkaline Each ejaculation contains approximately 2-6 ml, million sperm (< 20 million = infertile)
30 WHO semen reference values Volume 2-6 ml or more ph 7.2 or more Conc. 20x10 6 /ml or more Motility 50% (T1&T2) Morphology 15%
31 LDL ECF AcCoA cholesterol SSC pregnenolone progesterone estrone 3 -OH-steroid DH CYP19 DHEA androstenedione E1 androstenediol Stim by LH 17 -OH-steroid DH 3 -OH-steroid DH testosterone 5 -reductase 5 -reductase androsterone DHT CYP19 aromatase E2 17 SSC = side chain cleavage enzyme Copyright 2006 by Elsevier, Inc.
32 Androgen receptor: found in prostate, testis (Sertoli, Leydig and myoid cells) epididymis, seminal vesicles, neurons in CNS anterior pituitary, thyroid, skin, adrenal cortex, liver kidney tubules, bladder, cardiac and striated muscle bone, vasculature In females, also found in ovary (interstitial and granulosa cells) mammary glands, uterus
33 Functions of Testosterone fetal development: present at 2nd month of embryonic life presence or absence of testosterone determines development of genital organs and characteristics + testosterone = penis, scrotum - testosterone = clitoris and vagina also, development of prostate, seminal vesicles, vas deferens causes descent of testes into scrotum during last 2-3 months of pregnancy
34 TESTOSTERONE: BEFORE BIRTH Before birth: masculinizes reproductive tract and external genetalia Descent of testes Stops at birth & returns at puberty
35 TESTOSTERONE: AT PUBERTY Spermatogenesis Accessory sex glands enlarge and become secretory Penis and scrotum enlarge Libido
36 EFFECTS OF TESTOSTERONE ON SECONDARY SEX CHARACTERISTICS Hair growth pattern Deep voice Thick skin Male body configuration
37 OTHER EFFECTS OF TESTOSTERONE Bone growth Protein anabolic effect Eventually stops bone growth Aggressive behavior (in animals) Male menopause
38
39 CONTROL OF TESTICULAR FUNCTION HYPOTHALAMUS GRH + ANTERIOR PITUITARY TESTES SERTOLI CELL FSH LH LEYDIG CELL SPERMATOGENESIS INHIBIN TESTOSTERONE
40 Cells in Seminefrous tubules Leydig cell LH-R Gs AC blood capillaries Sertoli cell AC Gs FSH-R cholesterol testosterone EC space camp PKA synthesis enzymes camp growth hormones E2 PKA synthesis aromatase testosterone ABP spermatogonia lumen inhibins
41 Puberty: transition from quiescent reproductive endocrine system (inability to reproduce) to state of reproductive function (ability to reproduce) begins with pulsatile GnRH/LH secretion during REM sleep
42 Puberty In The Male Usually years old Endocrine,physical, and behavioral Leydig cells awake Androgens
43 Puberty Range of onset: 9-14 years of age Completion of pubertal development: yr 1st sign: enlargement of testes to greater than 2.5 cm growth due to increase in size of seminiferous tubules, Leydig cells Androgens from testes are driving force for secondary sex characteristics adrenal testosterone also plays a role
44 Female Reproductive System
45 Gametogenesis: Process through which gametes are formed Spermatogenesis: produces male gametes (sperm) occurs in the seminiferous tubules of the testes involves meiosis occurs throughout life after puberty may produce 400,000,000 per day Oogenesis: produces female gametes (oocytes) occurs in the ovaries involves meiosis occurs after puberty until menopause humans normally produce one oocyte during each ovarian cycle
46 Differences Between Spermatogenesis and Oogenesis 1. In females, mitotic proliferation of germ cells occurs prior to birth. In males, spermatogonia proliferate only after puberty. 2. In female, meiotic divisions of oocyte produces only one mature ovum. In male, meiotic divisions of primary spermatocyte produces 4 mature spermatozoa 3. In female, second meiotic division is completed only upon fertilization. In male, the products of meiosis (spermatids) undergo substantial differentiation in the maturing process.
47
48
49 Oogenesis Oogonia produced by mitotic division (max # = 7 mil), Then at 8-9 wks of gestation, prophase of 1 st meiosis starts becomes primary oocyte Number of primary oocytes decreases throughout childhood from 1-2 mil to 400,000 just before puberty surrounded by pre-granulosa cells called primordial follicle complete about 6 mos. after birth
50 Fundamental reproductive unit = single ovarian follicle, composed of one germ cell (oocyte), surrounded by endocrine cells
51 Stages in follicular growth and ovulation. Figure 81-4; Guyton & Hall
52 Cumulus and Mural Granulosa cells share a common cellular origin Primordial Germ Cell Mural Granulosa Cumulus Granulosa Primordial Follicle Primary Unilaminar Follicle Ovulation Primary Multilaminar Follicle Graafian Follicle
53 Oogonia (primordial germ cells) expand through mitosis in fetal ovary Oocytes when at birth enter meiosis Primordial Follicle surrounded by layers of granulosa Follicular Development with puberty
54 Follicular Development Recruitment Maturation
55 Recruitment Absence of tumor suppressors gene, PTEN, in oocytes prematurely induces global follicular activation in mice, depleting follicular reserve, similar to POF. Reddy et al. Science 2008; 319:
56 Maturation Bidirectional communications between germ cells (oocytes) and somatic cells (granulosa) are critical to oocyte maturation, follicle growth and ovulation. Daikoku and Dey. Nature Medicine 2008; 14:
57 190 days Gougeon, A. Endocrine Reviews 17:
58 Follicle Growth Gonadotropin dependent Only a few days for recruitment Growth Phase
59 Follicle Growth Gonadotropin Only a few days for recruitment dependent Growth Phase
60 AMH Secreted by granulosa cells of small follicles FSH independent Stable under various conditions: OCP Pregnancy Menstrual cycle
61 Fig a
62 Fig b
63 Fig
64 Granulosa & Oocyte are reciprocally regulated. Cumulus Granulosa Theca interna (vascular) Mural Granulosa ocyte Granulosa Zona Pellucida racrine signals from oocyte regulate the anulosa. GDF-9, BMP-15, BMP-6 may aintain the phenotype of cumulus. ncentration gradients may radiate twards from oocyte. Theca externa (connective tissue) Oocyte Antrum Basement membrane Granulosa Ooocyte Cytoplasmic processes maintain intimate contact. GAP junctions allow in camp, metabolites & amino acids. Also, cumulus derived factors such as kit-ligand, meiosis activating sterol and EGF like proteins.
65 Thecal cells superficial no aromatase have only LH Receptors can get cholesterol from LDL in blood Granulosa cells interior have aromatase, but no 17 -hydroxylase (17,20-desmolase) (Converts pregnenolone to 17 -hydroxyprenenolone to DHEA) get cholesterol from de novo synthesis have both LH and FSH receptors And progesterone to 17 -progesterone If androgen levels high, preferentially forms DHT from Testosterone and inhibits aromatase activity decr. estradiol, inhibit synthesis LH R
66 Negative feedback of steroids on gonadotropin release -- in child, low levels of steroid blocks release of gonadotropins -- in adult, much higher levels of steroids, same level of inhibition of release of gonadotropins Reduced sensitivity to steroids with age Age dependence of feedback sensitivity: high sensitivity in childhood; low sensitivity in adulthood
67 Ovarian Cycle: follicular phase LH surge ovulation FSH and LH in the Follicular phase LH surge lasts 48 h Inc GnRH bursts FSH LH Endometrial proliferative phase Cycle: menstrual (11 d) Copyright 2006 by Elsevier, Inc. secretory phase (12d) 28
68 Fig
69 Steroid Hormone Biosynthesis Cholesterol ACTH CH 3 C O 17 -Hydroxylase (P450 c17) CH 3 C O OH 17, 20 Lyase (P450 c17) O Pregnenolone HO HO 3 -Hydroxysteroid dehydrogenase CH 3 CH 3 17-Hydroxypregnenolone HO Dehydroepiandrosterone O C O C O OH O 21 -Hydroxylase (P450 c21) Progesterone CH 2 OH O 17-Hydroxyprogesterone CH 2 OH O Androstenedione C O C O OH O 11 -Hydroxylase (P450 c11) 11-Deoxycorticosterone CH 2 OH O 11-Deoxycortisol CH 2 OH HO C O HO C O OH O Corticosterone O Cortisol
70
71 LDL ECF mitochondria AcCoA cholesterol (RLS) SSC cytosol pregnenolone progesterone * * * DHEA androstenedione E1 * 17 -hydroxylase= 17,20-desmolase -- in SER 17 -hydroxyprogesterone estrone liver estriol E3 androstenediol testosterone E2 liver 3 -hydroxysteroid DH(in cytosol) Aromatase (in cytosol) Copyright 2006 by Elsevier, Inc. Synthesis of steroid hormones 17 -hydroxysteroid DH (in SER) SSC = side chain cleavage enzyme (in mitochondria)
72 Steroid synthesis in follicular phase thecal cell LH Gs AC blood capillaries granulosa cell AC Gs FSH LH LDL R Or: cholesterol androstenedione Copyright 2006 by Elsevier, Inc. EC space camp PKA synthesis enzymes testosterone (no aromatase) E1: estrone E2: estradiol E3: estriol E2 camp E3 androstenedione 17 -HSD testosterone aromatase LDL R PKA synthesis aromatase E2 aromatase E1 17 -HSD lumen
73 Steroid synthesis in luteal phase thecal cell LDL R cholesterol LH androstenedione testosterone (no aromatase) Copyright 2006 by Elsevier, Inc. Gs AC progesterone 17 -OH Prog blood capillaries E1: estrone E2: estradiol E3: estriol granulosa cell FSH E2 camp E3 AC Gs PKA aromatase androstenedione 17 -HSD testosterone aromatase E2 cholesterol progesterone E1 synthesis aromatase 17 -HSD (no 17 -hydroxylase or 17,20 desmolase) LH LDL R
74 Ovarian Cycle: + Luteal phase ovulation Levels of estradiol in follicular & luteal phases + _ FSH Granulosa cells activin inhibin FSH estradiol 1mens4 14 proliferative phase Endometrial Cycle: Copyright 2006 by Elsevier, Inc. secretory phase 28 inhibin
75 Ovarian Cycle: follicular phase LH surge ovulation Changes in progesterone in follicular & luteal phases. progesterone activin 1 Endometrial 4 Cycle: menstrual Copyright 2006 by Elsevier, Inc. 14 Proliferative phase (11 d) 28 Secretory phase (12d) inhibin
76 Ovarian Cycle: follicular phase ovulation Corpus luteum + _ Luteal phase Corpus albicans Changes in estradiol and progesterone in luteal phase. Produces inhib GnRH_ + progesterone estradiol 1 mens4 14 Endometrial proliferative phase Cycle: Copyright 2006 by Elsevier, Inc. secretory phase 28
77 Corpus luteum Provides necessary hormones for implantation of ovum and maintenance of zygote until placenta can take over 80% granulosa cells, 20% thecal cells If no fertilization, it will regress in about 14 d Avascular scar = corpus albicans
78 cholesterol thecal cells pregnenolone 17-OH-pregnenoloneprogesterone DHEAS 17-OH-progesterone androstenedione corpus luteum granulosa cells Estrone testosterone estradiol
79 +/- +/- CNS hypothalamus neurons gonadotropin releasing hormone Hypothalamic-pituitarygonadal axis +/- +/- LH ant. pituitary FSH thecal cells androgens inhibin LH R progestins + _ granulosa cells FSH R (LH R) activin Copyright 2006 by Elsevier, Inc. estrogens + Reproductive tract
80 Fig
81 Ovarian Cycle: follicular phase LH surge ovulation Increase in estradiol to stimulate LH surge. Then estradiol has Negative feedback on GnRH to reduce LH, FSH. estradiol FSH LH neg feedback--gnrh Proliferative phase Secretory phase (12d) Endometrial (11 d) Cycle: menstrual Copyright 2006 by Elsevier, Inc.
82 Chemical mechanics of ovulation: LH surge prostaglandin endoperoxide synthase in granulosa cells (sets up pseudoinflammatory response) FSH (some LH) stimulates release of plasminogen activator from granulosa cells (converts plasminogen to plasmin) Prostaglandins E and F release lysosomal enzymes that digest follicular wall not completely understood Stigma form on surface of follicle, balloons out, forms vesicle and ruptures oocyte expelled Process facilitated by intrafollicular pressure and contraction of smooth muscle in theca Copyright 2006 by Elsevier, Inc.
83 Figure 81-5; Guyton & Hall Postulated mechanisms responsible for ovulation
84 Ovarian cycle follicular phase avg 15 d (range, 9-23 days) ovulatory phase 1-3 d culminates with ovulation luteal phase 13 d less variable than follicular Endometrial cycle menstruation, proliferative and secretory phases Menstrual cycle controlled by gonadotropins, gonadal hormones
85 Phases of Endometrial Cycle Figure 81-7; Guyton & Hall
86 Fig
87 Fig
88 Differences Between Spermatogenesis and Oogenesis 1. In female, mitotic proliferation of oogonia occurs prior to birth. In males, spermatogonia proliferate only after puberty. 2. In female, meiotic divisions of oocyte produces only one mature ovum. In male, meiotic divisions of primary spermatocyte produces 4 mature spermatozoa 3. In female, second meiotic division is completed only upon fertilization. In male, the products of meiosis (spermatids) undergo substantial differentiation in the maturing process.
89 Estradiol nuclear receptor ( and ) genomic effects: there may be membrane receptor as well acute effects: increase IC Ca, vasodilation upregulates synthesis of ER and PR antioxidant
90 Functions of Estradiol External female sex organs: at puberty, increase in size of fallopian tubes, uterus and vagina, external genitalia deposition of fat in mons pubis change vaginal epithelia from cuboidal to stratified type endometrium: proliferation of cells and endometrial glands (important in nutrition of fertilized ovum) Breasts: fat deposition, development of stromal cells, ducts (progesterone, prolactin important in milk production) Bones: estrogen causes osteoclastic activity, so height increases after puberty, but epiphyses and shafts of bones unite early and growth stops
91 Functions of Estradiol Fat deposition: more subcutaneous fat in women than men Women: estrogens: hips and thighs fat deposition (prior to menopause) then more abdominal (Men: androgens: abdominal fat deposition) Skin: increase vascularization of skin
92 Progesterone Progesterone Nuclear receptor interacts with progesterone regulatory elements on DNA Progesterone receptor antagonist: mifepristone causes abortion and also inhibits hyperhydrocortisolism Inhibits estrogen receptor synthesis Causes endometrial proliferation during luteal phase
93 Puberty: transition from noncyclic, relatively quiescent reproductive endocrine system to state of cyclic reproductive function begins with pulsatile GnRH/LH secretion during REM sleep
94
95 Fertilization & Implantation
96
97
98
99
100
101
102 Genome activation Maternal transcripts Embryonic transcript Hours post-insemination S.I.S.ME.R. VISION 2000
103 Fig
104 a receptive endometrium a functionally normal blastocyst an adequate cross-communication
105 Endometrium: Integrin molecules, L-selectin ligands, mucin-1 Heparin-binding EGF Embryo: cytokines and growth factor interleukins; prostaglandins, VEGF receptor for endometrial signals LIF receptor,insulin-like GF and heparin-binding epidermal growth factor receptor Hoozemans et al, 2004
106 LH day +6 to +10 Phases: signaling, apposition, attachment, invasion Key associated findings: luminal epithelial pinopodes; expression of adhesion molecules and novel cytokines profile
107 Fig
108 Early invasion phase Human Conceptus upa + tpa MMP 2, 9 TI MMP PAI Endometrium
109 Late invasion phase Human Conceptus IL-4 IL-6 IL-10 TH 2 reaction Blocking antibodies NK and cytotoxic cells TH 1 reaction IL-2 IL-12 TNF- IFN Endometrium
110 T1 and T2 helper cells in implantation T1 helper cells Favours rejection IFN-γ IL-2 IL-12 TNF-α T2 helper cells Favours implantation IL-4 IL-5 IL-6 IL-9 IL-10 IL-13
111
112 Implantation failure In normal fertile women, 78 to 83 % of embryos fail to implant (Wilcox et al, 1988; Ellish et al, 1996) In infertile women, 85 % of embryos fail to implant (Edwards et al, 1995)
113
114 Fig b
115 Fig a
116 Maternal-feto-placental steroid hormone synthesis mother placenta fetus cholesterol adrenal SSC 17 -OH-ase cholesterol pregnenolone pregnenolone DHEA-S sulfate 3 -OHSDH progesterone progesterone 17,20-des Gluco/mineralocorticoids DHEA-S estradiol 17 -OH-ase estrone estriol sulfatase 17 -OH-ase DHEA estradiol estrone sulfatase 3 -OHSDH 17 -OHSDH aromatase estriol 16 -OH-DHEA 3, 17 sulfatase aromatase DHEA-S liver 16 OH-ase 16 -OH-DHEA-S
117 Lactation
118 Fig
119
120 Regulation of Prolactin secretion Stimulation Inhibition Pregnancy Estrogen Nursing-breast manipulation Sleep Stress TRH Dopamine antagonist Dopamine Dopamine agonist Somatostatin GnRH associated peptide Prolactin
121 1. Growth and development of the mammary glands - primarily 2. Milk production - requires prolactin, insulin and glucocorticoids 3. Neuroendocrine mechanisms - sucking causes prolactin and oxytocin release 4. Milk let-down reflex - necessary for the infant to obtain milk 5. Control of prolactin secretion - suckling releases prolactin, the more the infant is nursed, the more milk is produced 6. Lactation and resumption of ovarian cycles
122
123
124 Puberty: transition from quiescent reproductive endocrine system (inability to reproduce) to state of reproductive function (ability to reproduce) begins with pulsatile GnRH/LH secretion during REM sleep
125 What determines age at puberty: genetics nutrition geographic location exposure to light body composition, fat deposition exercise Menarche has been occurring earlier in past few decades in US and Europe Distance from equator, higher altitudes
126 Puberty Range of onset: 9-14 years of age Completion of pubertal development: yr 1st sign: enlargement of testes to greater than 2.5 cm growth due to increase in size of seminiferous tubules, Leydig cells Androgens from testes are driving force for secondary sex characteristics adrenal testosterone also plays a role
127 Menopause- Andropause
128 Different Stages of Male Sexual Function: Plasma Testsosterone and Sperm Production Figure 80-9; Guyton & Hall
129 Menopause Defn: obsolescence of ovaries, no estradiol production, ova only occasional secondary follicle, few primary follicles Occurs at 50 yr of age (average) Due to reduction in estrogen, low levels of inhibin, no negative feedback of LH and FSH; therefore, high levels LH and FSH Can occur naturally, due to surgery or as a result of chemotherapy
130 Ovarian Aging Physiologic Premature
131 RECRUITMENT AND MATURATION IS AFFECTED BY AGE FEMALE FERTILITY DECLINES
132 Follicle Growth Gonadotropin Only a few days for recruitment dependent Growth Phase
133 Follicle Growth Only a few days for recruitment Growth Phase
134 AMH Termellen KP et al: Australian NZ J Obstet Gynecol 2005; 45:20-24 AMH decreases with age
135 Fertility/Relative of Follicle and Oocyte Numbers Physiological Age-Related Fertility Curve (Range) and Parallel Curves Shifted towards Younger Age and Suggestive of POA Age of Physiologically Accelerated Decline in Fertility: ~25,000 Follicles Menopause < 1000 Follicles * * * 37.5 Age in Years * * * 51 Age of Premature Accelerated Decline in Fertility on Parallel Curves, Suggestive of POA ~ 13.5 Years Age of Early Menopause in Women on Parallel Curves, Suggestive of POA ~ 13.5 Years Gleicher N. Contemp Ob/gyn 2004
136
Physiology of Male Reproductive System
 Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Physiology of Male Reproductive System the anterior pituitary gland serves as the primary control of reproductive function at puberty Ant Pituitary secretes FSH & large amounts of LH (ICSH) FSH & LH cause
Reproductive physiology. About this Chapter. Case introduction. The brain directs reproduction 2010/6/29. The Male Reproductive System
 Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
Section Ⅻ Reproductive physiology Ming-jie Wang E-Mail: mjwang@shmu.edu.cn About this Chapter The reproductive organs and how they work the major endocrine functions of sexual glands actions of sex hormones
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
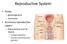 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
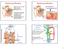 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Biology of Reproduction- Zool 346 Exam 2
 Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Biology of Reproduction- Zool 346 Exam 2 ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER. Some critical words are boldfaced. This exam is 7 pages long.
Reproductive Endocrinology. Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007
 Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
Reproductive Endocrinology Isabel Hwang Department of Physiology Faculty of Medicine University of Hong Kong Hong Kong May2007 isabelss@hkucc.hku.hk A 3-hormone chain of command controls reproduction with
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
Reproductive physiology
 Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
Reproductive physiology Sex hormones: Androgens Estrogens Gestagens Learning objectives 86 (also 90) Sex Genetic sex Gonadal sex Phenotypic sex XY - XX chromosomes testes - ovaries external features Tha
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
The reproductive lifespan
 The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
The reproductive lifespan Reproductive potential Ovarian cycles Pregnancy Lactation Male Female Puberty Menopause Age Menstruation is an external indicator of ovarian events controlled by the hypothalamicpituitary
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure.
 Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Chapter 27 Exam Due NLT Thursday, July 31, 2015 Name MULTIPLE CHOICE: match the term(s) or description with the appropriate letter of the structure. Figure 27.1 Using Figure 27.1, match the following:
Reproductive Hormones
 Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive Hormones Male gonads: testes produce male sex cells! sperm Female gonads: ovaries produce female sex cells! ovum The union of male and female sex cells during fertilization produces a zygote
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara
 Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
Reproductive System (Hormone Function) Physiology Department Medical School, University of Sumatera Utara 1 Endocrine Control: Three Levels of Integration Hormones of the hypothalamic-anterior pituitary
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Sample Provincial exam Q s: Reproduction
 Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
Sample Provincial exam Q s: Reproduction 11. Functions Testosterone Makes the male sex organs function normally, and also inhibits hypothalamus s release of GnRH and thus LH & FSH and thus testosterone
 MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
10.7 The Reproductive Hormones
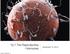 10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
10.7 The Reproductive Hormones December 10, 2013. Website survey?? QUESTION: Who is more complicated: men or women? The Female Reproductive System ovaries: produce gametes (eggs) produce estrogen (steroid
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Ch 20: Reproduction. Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition
 Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
Ch 20: Reproduction Keypoints: Human Chromosomes Gametogenesis Fertilization Early development Parturition SLOs Contrast mitosis/meiosis, haploid/diploid, autosomes/sex chromosomes. Outline the hormonal
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY
 Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
Physiology Unit 4 REPRODUCTIVE PHSYIOLOGY Gonads Gonads have 2 func7ons Gametogenesis Spermatogenesis Oogenesis Secrete steroid hormones Testosterone Estrogens (3 forms) Estradiol, produced by ovaries,
Chapter 36 Active Reading Guide Reproduction and Development
 Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
Name: AP Biology Mr. Croft Chapter 36 Active Reading Guide Reproduction and Development Section 1 1. Distinguish between sexual reproduction and asexual reproduction. 2. Which form of reproduction: a.
AP Biology Ch ANIMAL REPRODUCTION. Using only what you already know (you cannot look up anything) complete the chart below.
 AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
AP Biology Ch. 46 - ANIMAL REPRODUCTION Using only what you already know (you cannot look up anything) complete the chart below. I. Overview of Animal Reproduction A. Both asexual and sexual reproduction
Chapter 46 ~ Animal Reproduction
 Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
Chapter 46 ~ Animal Reproduction Overview Asexual (one parent) fission (parent separation) budding (corals) fragmentation & regeneration (inverts) parthenogenesis Sexual (fusion of haploid gametes) gametes
9.4 Regulating the Reproductive System
 9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
9.4 Regulating the Reproductive System The Reproductive System to unite a single reproductive cell from a female with a single reproductive cell from a male Both male and female reproductive systems include
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Hormones of brain-testicular axis
 (Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
(Hormone Function) Hormones of brain-testicular axis anterior pituitary drives changes during puberty controlled by GnRH from hypothalamus begins to secrete FSH, LH LH targets interstitial endocrinocytes
Endocrine and Reproductive Systems. Chapter 39: Biology II
 Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
Endocrine and Reproductive Systems Chapter 39: Biology II The Endocrine System Made up of glands that release their products into the bloodstream These products broadcast messages throughout the body Chemicals
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
The Reproductive System
 Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Animal Reproductive Systems. Chapter 42
 Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
Animal Reproductive Systems Chapter 42 Impacts, Issues Male or Female? Body or Genes? Body and genes don t always match male or female characteristics also depend on hormones mutations can result in intersex
1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase
 Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
Human Sexuality Exam II Review Material Gametogenesis: Oogenesis 1. Be able to characterize the menstrual cycle from the perspective of the ovary a. Follicular phase b. Luteal phase 2. Know the relative
Two important cells in female are the theca cells and the granulose cells. Granulosa cells are affected by the two gonadotropin hormones; FSH and LH.
 1 UGS physiology sheet #13 lecture 3 Dr.Saleem Khresha. Now we will start discussing the female reproductive system Ovarian Steroids Two important cells in female are the theca cells and the granulose
1 UGS physiology sheet #13 lecture 3 Dr.Saleem Khresha. Now we will start discussing the female reproductive system Ovarian Steroids Two important cells in female are the theca cells and the granulose
Synthesis of sex steroids
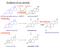 Synthesis of sex steroids CH 3 NAD(P)H NAD(P)+ Dehidroepiandroszteron Androszténdion 17- -hidroxiszteroid dehidrogenáz CH 3 dehydroepiandrosterone Dehidroepiandroszteron (DHEA) 3SDH Koleszterin CH 3 aromatase
Synthesis of sex steroids CH 3 NAD(P)H NAD(P)+ Dehidroepiandroszteron Androszténdion 17- -hidroxiszteroid dehidrogenáz CH 3 dehydroepiandrosterone Dehidroepiandroszteron (DHEA) 3SDH Koleszterin CH 3 aromatase
Chapter 27 The Reproductive System. MDufilho
 Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Chapter 27 The Reproductive System 1 Figure 27.19 Events of oogenesis. Before birth Meiotic events 2n Oogonium (stem cell) Mitosis Follicle development in ovary Follicle cells Oocyte 2n Primary oocyte
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Male Reproductive System. Figure 80-1 Copyright 2011 by Saunders, an imprint of Elsevier Inc.
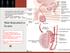 Male reprodctive system anatomy: briefly: composed of testis and external genetilia, the testis seminefrous tubules with space for spermatogenesis...the path is from the epidedimys-->vas defans-->prostatic
Male reprodctive system anatomy: briefly: composed of testis and external genetilia, the testis seminefrous tubules with space for spermatogenesis...the path is from the epidedimys-->vas defans-->prostatic
Stage 4 - Ovarian Cancer Symptoms
 WELCOME Stage 4 - Ovarian Cancer Symptoms University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad,
WELCOME Stage 4 - Ovarian Cancer Symptoms University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad,
Web Activity: Simulation Structures of the Female Reproductive System
 differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
differentiate. The epididymis is a coiled tube found along the outer edge of the testis where the sperm mature. 3. Testosterone is a male sex hormone produced in the interstitial cells of the testes. It
Female Reproductive System. Lesson 10
 Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
Female Reproductive System Lesson 10 Learning Goals 1. What are the five hormones involved in the female reproductive system? 2. Understand the four phases of the menstrual cycle. Human Reproductive System
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23
 AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
AnS 214 SI Multiple Choice Set 4 Weeks 10/14-10/23 The following multiple choice questions pertain to material covered in the last two weeks' lecture sets. Answering the following questions will aid your
The beginning of puberty is marked by the progressive increase in the production of sex hormones.
 Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
Puberty is characterized by the changes that prepare the human body for the ability to reproduce. This stage generally occurs between the ages of 10 and 14 years old. The beginning of puberty is marked
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5)
 IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
The Sex Hormones & Reproductive Systems (6)
 The Sex Hormones & Reproductive Systems (6) The Male Reproductive System The male reproductive system Lumen) Sperm Scrotum ~300 lobules Sertoli cell Leydig cell Testosterone Testes : - produce sperm cells
The Sex Hormones & Reproductive Systems (6) The Male Reproductive System The male reproductive system Lumen) Sperm Scrotum ~300 lobules Sertoli cell Leydig cell Testosterone Testes : - produce sperm cells
Ch 28 Lecture Study Guide
 Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Ch 28 Lecture Study Guide 1. List the characteristics of the reproductive system. Only organ system not essential to life Ensures continued existence of human species Produces, stores, nourishes, and transports
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
to ensure the. Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion of.
 The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
The Reproductive System Fill-In Notes Purpose of life: to ensure the. Stages of Human Development Sexual reproduction requires the (from the mother) by a (from the father). Fertilization is the fusion
The Reproductive System
 The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
Mohammad. Renad zakaria ---
 13 Mohammad Renad zakaria --- Before we start: - I didn t follow the record order, for organizing purposes. - I added extra information from our text box which is Guyton 12 th edition, pages 987-997, actually
13 Mohammad Renad zakaria --- Before we start: - I didn t follow the record order, for organizing purposes. - I added extra information from our text box which is Guyton 12 th edition, pages 987-997, actually
FEMALE REPRODUCTUVE SYSTEM
 FEMALE REPRODUCTUVE SYSTEM Female reproductive organs Figure 81-1 Internal structures of the uterus, ovary and a Fallopian tube Figure 81-2 Fundamental reproductive unit = single ovarian follicle, composed
FEMALE REPRODUCTUVE SYSTEM Female reproductive organs Figure 81-1 Internal structures of the uterus, ovary and a Fallopian tube Figure 81-2 Fundamental reproductive unit = single ovarian follicle, composed
2. Which of the following factors does not contribute to ion selectivity?
 General Biology Summer 2014 Exam II Sample Answers 1. Which of the following is TRUE about a neuron at rest? A. The cytosol is positive relative to the outside B. Na+ concentrations are higher inside C.
General Biology Summer 2014 Exam II Sample Answers 1. Which of the following is TRUE about a neuron at rest? A. The cytosol is positive relative to the outside B. Na+ concentrations are higher inside C.
CASE 41. What is the pathophysiologic cause of her amenorrhea? Which cells in the ovary secrete estrogen?
 CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
REPRODUCTIVE CYCLE OF FEMALE MAMMAL
 REPRODUCTIVE CYCLE OF FEMALE MAMMAL Fig. 8-12 Secondary follicles growing follicles increase in number of layers of granulosa cells Tertiary follicles maturing follicles antrum formation fluid filled space
REPRODUCTIVE CYCLE OF FEMALE MAMMAL Fig. 8-12 Secondary follicles growing follicles increase in number of layers of granulosa cells Tertiary follicles maturing follicles antrum formation fluid filled space
Hormonal Control of Human Reproduction
 Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
Hormonal Control of Human Reproduction Bởi: OpenStaxCollege The human male and female reproductive cycles are controlled by the interaction of hormones from the hypothalamus and anterior pituitary with
THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY
 THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY REFERENCE Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
THE MENSTRUAL CYCLE INA S. IRABON, MD, FPOGS, FPSRM, FPSGE OBSTETRICS AND GYNECOLOGY REPRODUCTIVE ENDOCRINOLOGY AND INFERTILITY REFERENCE Comprehensive Gynecology 7 th edition, 2017 (Lobo RA, Gershenson
BIOLOGY. Animal Reproduction CAMPBELL. Reece Urry Cain Wasserman Minorsky Jackson. Lecture Presentation by Nicole Tunbridge and Kathleen Fitzpatrick
 CAMPBELL BIOLOGY TENTH EDITION Reece Urry Cain Wasserman Minorsky Jackson 46 Animal Reproduction Lecture Presentation by Nicole Tunbridge and Kathleen Fitzpatrick 1. Asexual vs Sexual Reproduction Both
CAMPBELL BIOLOGY TENTH EDITION Reece Urry Cain Wasserman Minorsky Jackson 46 Animal Reproduction Lecture Presentation by Nicole Tunbridge and Kathleen Fitzpatrick 1. Asexual vs Sexual Reproduction Both
Mohammad Sha ban. Basheq Jehad. Hamzah Nakhleh
 11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
11 Mohammad Sha ban Basheq Jehad Hamzah Nakhleh Physiology of the reproductive system In physiology, we are concerned with the mechanisms in which the system functions, and how the system responds to different
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal
 What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
What are the main functions of the male reproductive system? 1. Produce sperm 2. Deposit sperm into the female 3. Provide a pathway for the removal of urine Where is sperm produced? -In the 2 testes What
Male reproductive system The physiology of sexual act
 Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
Animal Reproduction Chapter 46. Fission. Budding. Parthenogenesis. Fragmentation 11/27/2017
 Animal Reproduction Chapter 46 Both asexual and sexual reproduction occur in the animal kingdom Sexual reproduction is the creation of an offspring by fusion of a male gamete (sperm) and female gamete
Animal Reproduction Chapter 46 Both asexual and sexual reproduction occur in the animal kingdom Sexual reproduction is the creation of an offspring by fusion of a male gamete (sperm) and female gamete
Dr. Garrett Thursday! Dr. Kaplan following Tuesday! Hooray!!...
 Dr. Garrett Thursday! Dr. Kaplan following Tuesday! Hooray!!... Lecture 12 I. Quiz 4 CV physiology 8:15 next T < class Presentations. Q? For Quiz, 12 n section go to 112 WIL with Nelson @ ~ 8:15! II. Endocrinology
Dr. Garrett Thursday! Dr. Kaplan following Tuesday! Hooray!!... Lecture 12 I. Quiz 4 CV physiology 8:15 next T < class Presentations. Q? For Quiz, 12 n section go to 112 WIL with Nelson @ ~ 8:15! II. Endocrinology
DATE: NAME: CLASS: Chapter 14 Test
 Multiple Choice Questions Decide which of the choices best completes the statement or answers the question. Locate that question number on the separate answer sheet provided. Use the procedure described
Multiple Choice Questions Decide which of the choices best completes the statement or answers the question. Locate that question number on the separate answer sheet provided. Use the procedure described
Module J ENDOCRINE SYSTEM. Learning Outcome
 Module J ENDOCRINE SYSTEM Topic from HAPS Guidelines General functions of the endocrine system Chemical classification of hormones & mechanism of hormone actions at receptors. Control of hormone secretion
Module J ENDOCRINE SYSTEM Topic from HAPS Guidelines General functions of the endocrine system Chemical classification of hormones & mechanism of hormone actions at receptors. Control of hormone secretion
Reproduction Lecture Spring 2009
 Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
Reproduction Lecture Spring 2009 Slide #2: The term gonads refer to the sex organs. In the male, these are the testes, and the in the female, the ovary. The produce sex cells, or gametes. The male gamete
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Animal Science 434! Tonic and Preovulatory Surge of GnRH! Tonic and Preovulatory Surge of GnRH! Lecture 11: The Follicular Phase of the Estrous Cycle!
 Tonic and Preovulatory Surge of GnRH! Animal Science 434! Lecture 11: The Follicular Phase of the Estrous Cycle!! (-)! Hypothalamus! GnRH! Estradiol! (-)! Tonic and Preovulatory Surge of GnRH! Anterior!
Tonic and Preovulatory Surge of GnRH! Animal Science 434! Lecture 11: The Follicular Phase of the Estrous Cycle!! (-)! Hypothalamus! GnRH! Estradiol! (-)! Tonic and Preovulatory Surge of GnRH! Anterior!
The Reproductive System
 A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
A+ NURSING TEAM The Reproductive System Chapter 28 Page1129-1181 2012 A PLUS TEAM ~ فريقك األكاديمي في كليتك التمريض ~. *`'. A+ team. *`'. ما هى إال وسيلة لتفعيل دور كل واحد منا في تيسير المعرفة بطريقة
Embryology Lecture # 4
 1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
1 Quick Review: Oogenesis : - Oogonia start appear in the ovary when the age of the fetus 1 is th (5 week). - Then the Oogonia transformed into 1ry Oocyte. - 1ry Oocyte is surrounded by a follicle (cover).
Fig Chapter 46. Animal Reproduction
 Fig. 46-1 Chapter 46 Animal Reproduction Overview: Pairing Up for Sexual Reproduction Each earthworm produces sperm and eggs; Aspects of animal form and function can be viewed broadly as adaptations contributing
Fig. 46-1 Chapter 46 Animal Reproduction Overview: Pairing Up for Sexual Reproduction Each earthworm produces sperm and eggs; Aspects of animal form and function can be viewed broadly as adaptations contributing
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
Section 39 1 The Endocrine System (pages )
 Chapter 39 Endocrine and Reproductive Systems Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system? How does the endocrine system maintain homeostasis?
Chapter 39 Endocrine and Reproductive Systems Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system? How does the endocrine system maintain homeostasis?
Reproductive Systems. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Section 39 1 The Endocrine System (pages )
 Chapter 39 Endocrine and Reproductive Systems 11 What is the function of the parathyroid glands? Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system?
Chapter 39 Endocrine and Reproductive Systems 11 What is the function of the parathyroid glands? Section 39 1 The Endocrine System (pages 997 1002) Key Concepts What is the function of the endocrine system?
2 - male hormones/ female system
 2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
2 - male hormones/ female system May 7, 2012 5:08 PM I) Testosterone: main androgen (male sex hormone) A) Intro to Testosterone: -steroid hormone produced by interstitial cells in testes -produced in response
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
Special Parts: Gender. Why Have Sex?
 Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
BIOL 2402 Reproductive Systems!
 Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
Dr. Chris Doumen! Female Reproductive Anatomy BIOL 2402 Reproductive Systems! Establishing the Ovarian Cycle During childhood, until puberty Ovaries grow and secrete small amounts of estrogens Estrogen
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Female Reproductive Physiology. Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF
 Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
Female Reproductive Physiology Dr Raelia Lew CREI, FRANZCOG, PhD, MMed, MBBS Fertility Specialist, Melbourne IVF REFERENCE Lew, R, Natural History of ovarian function including assessment of ovarian reserve
