CX3CR1 regulates intestinal macrophage homeostasis, bacterial translocation, and colitogenic Th17 responses in mice
|
|
|
- Alicia Henderson
- 6 years ago
- Views:
Transcription
1 Research article CX3CR1 regulates intestinal macrophage homeostasis, bacterial translocation, and colitogenic Th17 responses in mice Oscar Medina-Contreras, 1 Duke Geem, 1 Oskar Laur, 2 Ifor R. Williams, 2 Sergio A. Lira, 3 Asma Nusrat, 2 Charles A. Parkos, 2 and Timothy L. Denning 1,2 1 Department of Pediatrics and 2 Epithelial Pathobiology Research Unit, Department of Pathology and Laboratory Medicine, Emory University, Atlanta, Georgia, USA. 3 Immunology Institute, Mount Sinai School of Medicine, New York, New York, USA. The two most common forms of inflammatory bowel disease (IBD), Crohn s disease and ulcerative colitis, affect approximately 1 million people in the United States. Uncontrolled APC reactivity toward commensal bacteria is implicated in the pathogenesis of the disease. A number of functionally distinct APC populations exist in the mucosal lamina propria (LP) below the intestinal epithelium, but their relative contributions to inflammation remain unclear. Here, we demonstrate in mice important roles for the chemokine receptor CX3CR1 in maintaining LP macrophage populations, preventing translocation of commensal bacteria to mesenteric lymph nodes (mlns), and limiting colitogenic Th17 responses. CX3CR1 was found to be expressed in resident LP macrophages (defined as CD11b + F4/80 + ) but not DCs (defined as CD11c + CD103 + ). LP macrophage frequency and number were decreased in two strains of CX3CR1-knockout mice and in mice deficient in the CX3CR1 ligand CX3CL1. All these knockout strains displayed markedly increased translocation of commensal bacteria to mlns. Additionally, the severity of DSS-induced colitis was dramatically enhanced in the knockout mice as compared with controls. Disease severity could be limited by either administration of neutralizing IL-17A antibodies or transfer of CX3CR1-sufficient macrophages. Our data thus suggest key roles for the CX3CR1/CX3CL1 axis in the intestinal mucosa; further clarification of CX3CR1 function will likely direct efforts toward therapeutic intervention for mucosal inflammatory disorders such as IBD. Introduction The vertebrate immune system is poised to potently respond against invading microbes and foreign molecules while enforcing tolerance toward self antigens (1). In the intestine, however, immune reactivity toward commensal flora must be restrained to prevent pathological inflammation, such as in Crohn s disease and ulcerative colitis (2, 3). There are numerous mechanical, physical, and immunological mechanisms that play crucial roles in maintaining intestinal homeostasis (4). Of the immunological parameters, components of the innate and adaptive immune systems cooperate to promote tolerance toward commensal flora while permitting reactivity to pathogens (3, 5). Just beneath the epithelial barrier exist innate immune cells including APCs that direct appropriate B and T cell differentiation, and subsequent immunoglobulin and effector/regulatory T cell responses. Acquisition and presentation of food and bacterial antigens is believed to be carried out in large part by lamina propria (LP) DCs that migrate to the mesenteric lymph nodes (mlns) in a CCR7-dependent manner (6), where they stimulate antigen-specific B and T cells to upregulate the gut-homing molecules α 4 β 7 and CCR9. mln DCs also induce the differentiation of IgA-producing B cells and Foxp3 + regulatory T cells in the mln via retinoic acid dependent mechanisms (7 11). Thus, DCs in the LP and mln play important roles in regulating intestinal B and T cell homing and differentiation. Various different phenotypic markers have been used to identify and characterize subsets of LP DCs, and a number of conclusions Conflict of interest: The authors have declared that no conflict of interest exists. Citation for this article: J Clin Invest. 2011;121(12): doi: /jci about the function of LP DCs have been made using these markers. In particular, the chemokine receptor CX3CR1 was proposed as a marker of LP DCs that extend transepithelial dendrites to sample luminal bacteria and mediate clearance of enteroinvasive pathogens (12). While CX3CR1 is expressed on many cell types and has long been appreciated as a marker for macrophages in the central nervous system (13), it has been frequently used as a marker for specific subsets of LP DCs (14). We and others have recently reported that CX3CR1 is not highly expressed on CD103 + LP DCs (15, 16) and that CD103 + LP cells, not CX3CR1 + cells, carry out classical DCmediated functions (16). There now appears to be a consensus that CD11c + CD103 + MHC II + cells are bona fide LP DCs (14); however, controversy remains over the lineage of CX3CR1-expressing LP cells and whether they are DCs or macrophages, with many groups referring to them as DCs, others as mononuclear phagocytes, and still others as macrophages (17). Since it has become increasingly appreciated that numerous subsets of DCs and macrophages exist within the intestinal LP (14, 18), we aimed to investigate the expression of CX3CR1 on these subsets, as well as the functional consequences of interfering with the CX3CR1/CX3CL1 axis. We examined LP DC and macrophage subsets in the small and large intestines of two independent lines of CX3CR1-deficient mice as well as CX3CL1- deficient mice both in the steady state and during intestinal inflammation. In this report, we demonstrate an important role for the CX3CR1/CX3CL1 axis in regulating LP macrophage homeostasis and bacterial clearance and limiting colitogenic Th17 responses. Results Murine intestinal LP macrophage subsets preferentially express CX3CR1. In the intestine, LP DCs and macrophages play a central role in regulat- The Journal of Clinical Investigation Volume 121 Number 12 December
2 Figure 1 Murine intestinal LP macrophages express CX3CR1. (A) Flow cytometry of small (SI) and large (LI) intestine LP cells from C57BL/6 mice, stained for CD45, I-A b, CD11b, CD11c, F4/80, and CD103. Populations were defined as R1, CD11b DCs; R3, CD11c macrophages; R4, CD11b + DCs; and R5, CD11c + macrophages. (B) GFP expression in LP macrophages (MΦ; solid histograms) and DCs (open histograms) in the small and large intestine of Cx3cr1 gfp/gfp mice, assessed by flow cytometry and gated as in A. (C) qrt-pcr for Cx3cr1 mrna expression in isolated intestinal LP APCs from Cx3cr1 +/+ mice. Data are representative of 3 (B and C) or more than 3 (A) independent experiments. Error bars represent SD. *P < 0.05 versus respective controls. ing innate and adaptive immune responses as well as inflammation. These various functions are carried out by different subsets of LP DCs and macrophages. Based on the expression of CD11b, CD11c, F4/80, and CD103, we have identified 4 populations of murine intestinal LP APCs, as defined as CD45 + MHC II + cells (Figure 1A and ref. 18): CD11c + CD11b CD103 + F4/80 DCs (R1), CD11c CD11b + CD103 F4/80 + macrophages (R3), CD11c + CD11b + CD103 + F4/80 DCs (R4), and CD11c + CD11b + CD103 F4/80 + macrophages (R5). For simplicity, we refer to these populations as CD11b DCs, CD11c macrophages, CD11b + DCs, and CD11c + macrophages, respectively. It is reported that CD11b + LP DCs extend dendrites between neighboring IECs in order to sample luminal antigens in a CX3CR1-dependent manner (12, 19 21). However, CD11b + LP cells include a mixture of DC and macrophage subsets, and it is not clear which subsets express CX3CR1. Using Cx3cr1 gfp/gfp reporter mice, which have Cx3cr1 replaced with gfp in both alleles, we analyzed the CX3CR1 expression on each of the LP macrophage and DC subpopulations. As shown in Figure 1B, we observed that GFP (CX3CR1) is expressed by CD11c and CD11c + macrophages, but not by CD11b or CD11b + DCs, in both the small and large intestine. In order to rule out any possibility that GFP is not faithfully marking CX3CR1-expressing cells in this mouse model, we analyzed CX3CR1 expression in Cx3cr1 +/+ C57BL/6 mice, using anti-cx3cr1 antibodies. Our results confirmed the GFP expression pattern, with specific CX3CR1 expression by CD11c and CD11c + macrophages, but not CD11b or CD11b + DCs (Supplemental Figure 1). We also performed quantitative RT-PCR (qrt-pcr) on sorted CD11c or CD11c + macrophages, as well as CD11b or CD11b + DCs. This further confirmed highly specific expression of CX3CR1 in both macrophages populations, but not in DC subsets (Figure 1C) The Journal of Clinical Investigation Volume 121 Number 12 December 2011
3 Figure 2 Cx3cr1 gfp/gfp mice harbor a specific reduction in LP macrophages. (A) Percentage of CD45 + MHC II + macrophages and DCs in the small and large intestine of Cx3cr1 gfp/gfp or Cx3cr1 +/+ mice. (B) Total cellularity of CD45 + MHC II + macrophages and DCs in the small and large intestine of Cx3cr1 gfp/gfp or Cx3cr1 +/+ mice. (C) Percentage of bone marrow MDPs and blood monocytes of Cx3cr1 gfp/gfp or Cx3cr1 +/+ mice. Data are representative of 3 (C) or more than 3 (A and B) independent experiments. Error bars represent SEM. *P < 0.05 versus respective controls. Reduction of LP macrophages in CX3CR1- and CX3CL1-deficient mice. Having observed specific expression of CX3CR1 by LP macrophages, we performed experiments to investigate the functional role of CX3CR1 in the intestine. Interestingly, phenotypic characterization of LP APCs in Cx3cr1 gfp/gfp mice revealed a significant reduction in the frequency of CD11c and CD11c + macrophages in Cx3cr1 gfp/gfp mice when compared with Cx3cr1 +/+ mice in both the small and large intestine (Figure 2A). This reduction was specific for LP macrophage subsets, as no significant differences were observed in the frequencies of CD11b or CD11b + LP DCs between Cx3cr1 gfp/gfp mice and Cx3cr1 +/+ mice. The total cell numbers of the CD11c and CD11c + macrophage subsets were also significantly reduced in Cx3cr1 gfp/gfp mice, while DC subsets remained largely unaffected (Figure 2B). Since both LP macrophage subsets expressed high levels of GFP and were reduced in number, we wanted to verify that the observed reduction in LP macrophages was the result of CX3CR1 deficiency and not GFP-induced cytotoxicity. Therefore, we performed the same phenotypic characterization of LP DCs and macrophages in a different CX3CR1-deficient mouse line (22) that does not express GFP. Results using these Cx3cr1 / mice confirmed our observations with Cx3cr1 gfp/gfp mice, demonstrating a specific reduction in the frequency (Supplemental Figure 2A) and total cell number (Supplemental Figure 2B) of CD11c and CD11c + LP macrophages, but not CD11b or CD11b + LP DCs. These data formally exclude GFP-induced cytotoxicity as the explanation for specific LP macrophage reduction in Cx3cr1 gfp/gfp mice. Additionally, mice deficient in CX3CL1 (the ligand for CX3CR1) showed a reduction in LP macrophage subsets similar to that observed in CX3CR1-deficient mice (Supplemental Figure 3). To evaluate whether the LP macrophage reduction in Cx3cr1 gfp/gfp mice is reflective of a general defect in monocyte/macrophage development or precursor accumulation, we analyzed the frequency of monocyte-dc common precursors (MDPs) in bone marrow as well as circulating blood monocytes (Figure 2C) and did not observe any significant difference in either of these populations. The significant LP macrophage reduction in CX3CR1-deficient mice was also not likely the result of increased cell death, since transfer of CD Cx3cr1 +/+ or CD Cx3cr1 gfp/gfp bone mar- The Journal of Clinical Investigation Volume 121 Number 12 December
4 Figure 3 CX3CR1-deficient mice have increased bacterial translocation. CFU per mouse in the mlns of Cx3cr1 gfp/gfp (A) and Cx3cr1 / (B) mice. Relative abundance of phyla (C) and genera (D) among the translocated bacteria. Data are representative of 3 independent experiments, with 4 mice per group per experiment. *P < 0.05 versus respective controls. row derived macrophages (BMDMs) into CD hosts resulted in equivalent numbers of Cx3cr1 +/+ and Cx3cr1 gfp/gfp BMDMs in the spleens, but a significant reduction in Cx3cr1 gfp/gfp BMDMs in the intestines of recipient mice (data not shown). Taken together, our results demonstrate a specific reduction in LP macrophages in CX3CR1-deficient mice and suggest a role for the CX3CR1/ CX3CL1 axis in regulating LP macrophage migration and/or retention in the intestine. Interestingly, CX3CR1 deficiency also resulted in a significant reduction in macrophages in the lung and liver, but not the spleen (Supplemental Figure 4). Increased bacterial translocation in CX3CR1- and CX3CL1-deficient mice. Given the phagocytic nature of LP macrophages (23) and their significant reduction in Cx3cr1 gfp/gfp and Cx3cr1 / mice, we hypothesized that there may be a defect in the clearance of commensal bacteria that gain access to the lamina propria. To test this, we analyzed the mlns from these mice for signs of bacterial translocation. Total mln cell suspensions cultured under aerobic conditions on LB blood agar plates revealed the presence of large numbers of bacteria in Cx3cr1 gfp/gfp and Cx3cr1 / mice (Figure 3, A and B) and in Cx3cl1 / mice (Supplemental Figure 5A). In most experiments, bacteria could not be grown from mlns of Cx3cr1 +/+ mice. The increased bacteria in the mlns of CX3CR1- deficient mice was not the result of defective intestinal barrier function, since there was no difference in the uptake of orally delivered, fluorescent 4-kDa and 10-kDa dextran into the serum of Cx3cr1 +/+ and CX3CR1-deficient mice (data not shown). Additionally, Cx3cr1 +/+ and CX3CR1-deficient macrophages expressed similarly low to undetectable mrna levels for molecules involved in forming adherens junctions (E-cadherin and β-catenin) and tight junctions (ZO-1, occludin, claudin-1; data not shown); thus, unlike what has been shown for DCs (24), macrophages may not play a role in directly maintaining intestinal epithelial barrier via tight junction protein expression. To assess whether the bacteria present in the mlns of CX3CR1- deficient mice that grew under aerobic culture conditions were predominantly commensal or pathogenic bacteria, we isolated DNA from 50 individual colonies and performed PCR amplification using consensus 16S rdna primers. Sequencing of PCR amplicons revealed that the translocated bacteria were predominantly commensal bacteria corresponding to the phylum Firmicutes (Figure 3C), with Enterococcus being the predominant genus (Figure 3D). Notably, a few sequences corresponded to Shigella; therefore, we cannot exclude the possibility that pathogenic bacteria can also gain access to the LP in the absence of CX3CR1. Overall, these results suggest that CX3CR1-expressing LP macrophages play a vital role in restricting translocation of commensal bacteria to the mln during steady-state conditions. Absence of CX3CR1 or CX3CL1 leads to enhanced intestinal inflammation. It has been shown that LP macrophages are important regulators of immune responses during intestinal inflammation (25, 26). Therefore, the specific reduction in LP macrophages in CX3CR1 deficiency prompted us to analyze how these mice respond to acute colitis induced by DSS. Beginning as early as 2 days following DSS administration, Cx3cr1 gfp/gfp and Cx3cr1 / mice exhibited significantly enhanced signs of intestinal disease when compared with Cx3cr1 +/+ mice, as defined by increases in overall disease activity index (DAI), a measure of weight loss, fecal blood, and soft stool/ diarrhea (Figure 4A). Histological analysis showed greater tissue damage and inflammatory infiltrate in DSS-treated Cx3cr1 gfp/gfp and Cx3cr1 / mice when compared with Cx3cr1 +/+ mice (Figure 4B). Since mice lacking CX3CL1 also displayed a reduction in the frequency of both CD11c and CD11c + LP macrophages (Supple The Journal of Clinical Investigation Volume 121 Number 12 December 2011
5 Figure 4 Increased susceptibility to DSS-induced colitis in CX3CR1-deficient mice. (A) Severity of colitis in DSS-treated Cx3cr1 gfp/gfp and Cx3cr1 / mice or their respective Cx3cr1 +/+ age- and vendor-matched control mice, as measured by stool consistency, presence of fecal blood, and weight loss. (B) Colon histology of DSS-treated Cx3cr1 gfp/gfp, Cx3cr1 /, and Cx3cr1 +/+ mice. Original magnification, 400. Data are representative of 3 independent experiments. Error bars represent SEM. *P < mental Figure 3) and increased bacterial translocation to the mln (Supplemental Figure 5A), we investigated the response of these mice to DSS. Consistent with the increased sensitivity of Cx3cr1 gfp/gfp and Cx3cr1 / mice, Cx3cl1 / mice also displayed significantly enhanced sensitivity to DSS on days 3 5 (Supplemental Figure 5B). These data demonstrate that interfering with the CX3CR1/ CX3CL1 axis results in decreased recruitment and/or retention of macrophages to the intestinal LP, implying that there may be cells in the intestine that secrete CX3CL1 and recruit CX3CR1-expressing LP macrophages. To directly probe this possibility, we isolated RNA from intestinal epithelial cells (IECs) or total LP cells (non- IEC fraction) and performed qrt-pcr for Cx3cl1. Interestingly, we observed that both IECs and LP cells expressed robust levels of Cx3cl1 mrna (Supplemental Figure 5C). Collectively, these data suggest that regulation of CX3CL1 expression by IECs (27) or LP cells or the regulation of CX3CR1 expression by LP macrophages may have significant effects on macrophage homeostasis and intestinal inflammation. Enhanced IL-17A dependent colitis in CX3CR1-deficient mice. Since Th17 cells and Foxp3 + Tregs play important roles in regulating intestinal inflammation (3), we examined these T cell subsets in the steady state and during intestinal inflammation. Interestingly, under steady-state conditions, CX3CR1-deficient mice showed no significant differences in LP CD4 + Th17 cell or Foxp3 + Treg populations (Supplemental Figure 6) or IFN-γ producing Th1 cells (data not shown). However, upon induction of intestinal inflammation, a 3.4-fold increase in colonic IL-17 producing CD4 + T cells was observed in Cx3cr1 gfp/gfp mice, but not Cx3cr1 +/+ mice (Figure 5, A and B). Additionally, there was a trend toward reduced colonic Foxp3 + Tregs in Cx3cr1 gfp/gfp mice during DSS treatment; however, this did not reach statistical significance (Figure 5, A and B). Since innate lymphoid cells are a recently appreciated source of IL-17 that contribute to the pathogenesis of intestinal inflammation (28), we investigated whether these cells were an additional source of IL-17A in colitic Cx3cr1 gfp/gfp mice. As shown in Supplemental Figure 7, CD3 RORγt + innate lymphoid cells were not an abundant source IL-17A in Cx3cr1 gfp/gfp mice; thus, IL-17A is predominantly produced by CD4 + LP T cells in colitic CX3CR1-deficient mice. To investigate the possibility that the increased disease severity in CX3CR1-deficient mice is related to augmented IL-17A production, we induced acute colitis in Cx3cr1 gfp/gfp and Cx3cr1 +/+ mice and injected neutralizing antibody against IL-17A or isotype control IgG 1 at days 0, 2, and 4. Figure 5C shows that while IgG 1 treatment did not affect the severity of the disease in Cx3cr1 gfp/gfp and Cx3cr1 +/+ mice (when compared with Figure 4A), IL-17A neutralization significantly ameliorated the enhanced colitis symptoms in Cx3cr1 gfp/gfp mice, reducing them to levels comparable to those in Cx3cr1 +/+ mice. This neutralization also significantly ameliorated colitis symptoms in Cx3cr1 / mice (Supplemental Figure 8). Importantly, IL-17A neutralization had little to no effect in modulating colitis in Cx3cr1 +/+ mice (Figure 5C), thus emphasizing an important and unique role for IL-17A producing CD4 + T cells in enhanced colitis in CX3CR1-deficient mice. To further confirm that CD4 + T cells were involved in exacerbating colitis in CX3CR1-deficient mice, we treated Cx3cr1 gfp/gfp mice with CD4- depleting antibody and monitored disease activity. Complete depletion of CD4 + T cells in Cx3cr1 gfp/gfp mice (Supplemental Figure 9A) significantly reduced colonic inflammation as assessed by DAI (Supplemental Figure 9B). Therefore, CD4 + T cells are the major IL-17 producing cells contributing to the pathogenesis of colitis in CX3CR1-deficient mice. The Journal of Clinical Investigation Volume 121 Number 12 December
6 Figure 5 IL-17 responses contribute to enhanced colitis in Cx3cr1 gfp/gfp mice. (A) Flow cytometry of intracellular Foxp3 or IL-17A by colonic CD4 + T cells from Cx3cr1 gfp/gfp or Cx3cr1 +/+ mice. Numbers in outlined areas indicate percentage of cells in gate. (B) Percentage of IL-17A + and FoxP3 + cells in the large intestine of Cx3cr1 gfp/gfp and Cx3cr1 +/+ mice. (C) Severity of colitis in DSS-treated Cx3cr1 gfp/gfp or Cx3cr1 +/+ mice, in the presence of neutralizing IL-17A antibody or isotype control. Data are representative of 2 (C) or 3 (A and B) independent experiments. Error bars represent SEM. *P < 0.05 versus respective controls. to that afforded by IL-17A neutralization. In contrast to Cx3cr1 +/+ BMDMs, transfer of Cx3cr1 gfp/gfp BMDMs did not provide any detectable protection to Cx3cr1 gfp/gfp mice, even though Cx3cr1 gfp/gfp macrophages were equally viable as Cx3cr1 +/+ macrophages and capable of normal TNF production in response to LPS (data not shown). Additionally, transfer of either Cx3cr1 gfp/gfp or Cx3cr1 +/+ BMDMs into Cx3cr1 +/+ mice (Supplemental Figure 10) showed no detectable effect on modulating DSS-induced colitis. Collectively, these data demonstrate that the expression of CX3CR1 on transferred macrophages is required for protecting CX3CR1- deficient mice from increased sensitivity to DSS-induced colitis. Furthermore, homing of transferred macrophages to the intestine may be important for their ability to protect from colitis, since Cx3cr1 +/+ BMDMs were able to migrate to the intestine, as demonstrated by recovery of CDllb + CD11c APCs from the LP at day 5 (Supplemental Figure 11). Transfer of Cx3cr1 +/+ macrophages suppresses colitis in CX3CR1-deficient mice. In order to probe the relationship between the reduction in LP macrophages and the increased susceptibility to DSS-induced colitis, we transferred Cx3cr1 +/+ BMDMs into Cx3cr1 gfp/gfp mice 1 day prior to and 1 day after initiating DSS treatment and followed clinical signs of intestinal inflammation. Cx3cr1 +/+ BMDMs exhibited a phenotype of CD45 hi, CD11b hi, F4/80 hi, MHC II int, CX3CR1 +, CD115 +, CD135 int, CD117, indicating an intermediate phenotype between bone marrow precursors and tissue macrophages. These cells expressed low levels of CX3CR1 prior to transfer; however, CX3CR1 was upregulated after their differentiation in vivo (data not shown). This expression pattern is consistent with CX3CR1 expression increasing initially as MDPs differentiate into blood monocytes and further as blood monocytes differentiate into intestinal LP macrophages (data not shown). Beginning at 3 days following DSS administration, Cx3cr1 gfp/gfp mice that received transfer of Cx3cr1 +/+ BMDMs were significantly protected from colitis when compared with Cx3cr1 gfp/gfp mice not receiving transferred macrophages (Figure 6). The protection afforded to Cx3cr1 gfp/gfp mice by Cx3cr1 +/+ macrophages was similar Discussion Together our experiments demonstrate that murine intestinal LP macrophages, but not LP DCs, express high levels of CX3CR1 and that deletion of CX3CR1 or CX3CL1 in vivo results in a specific and significant reduction in LP macrophages. The biological consequences of CX3CR1 deficiency included increased translocation of commensal bacteria to the mln, as well as enhanced Th17 responses and exacerbated disease during acute intestinal inflammation. Importantly, transfer of CX3CR1-sufficient macrophages or neutralization of IL-17A ameliorated the increased disease severity of CX3CR1-deficient mice. These results argue that CX3CR1 is not a marker for defining LP DCs, but rather a highly specific marker for LP macrophages and a critical component in maintaining LP macrophage homeostasis. The specific expression of CX3CR1 by nearly all LP macrophages may offer insight into the findings that CX3CR1-expressing LP DCs are derived from monocyte precursors in the presence of GM-CSF (29 31). Since monocytes are well appreciated as the precursors of tissue-resident macrophages (32), it is most plausible that they are also the precursors of CX3CR1-expressing intestinal LP macrophages. Additionally, the specific expression of CX3CR1 by LP macrophages suggests that bacterial clearance and luminal sampling via extension of dendrites, previously attributed to LP DCs (12, 19 21), may indeed be performed by LP macrophage subsets extending pseudopodia under certain circumstances. This concept is consistent with the avidly phagocytic nature of LP macrophages (23) and the recent finding that CX3CR1-expressing LP cells do not possess classical DC functions (16). Our results further suggest that the absence of transepithelial dendrites by DCs in Cx3cr1 gfp/gfp mice (12, 19, 21) could be explained in part by the significant reduction in LP macrophages 4792 The Journal of Clinical Investigation Volume 121 Number 12 December 2011
7 Figure 6 LP macrophage deficiency contributes to enhanced colitis in Cx3cr1 gfp/gfp mice. Severity of colitis in DSS-treated Cx3cr1 gfp/gfp mice after adoptive transfer of Cx3cr1 gfp/gfp or Cx3cr1 +/+ BMDMs. Data are representative of 2 independent experiments. Error bars represent SEM. *P < 0.05 versus respective controls. and emphasize that data should be interpreted with caution when CX3CR1-deficient mice are used as a model system for investigating intestinal APC-dependent responses. While the α 4 β 7 and CCR9 homing receptors are important for T and B cell migration to the intestine (33 35), far less is understood about the migration and/or retention of intestinal DCs and macrophages. The specific reduction in LP macrophages in CX3CR1- and CX3CL1-deficient mice demonstrates a clear link between this chemokine/receptor axis and the presence of these cells. Additional studies are required to clarify whether CX3CR1 and CX3CL1 are important for migration and/or retention of macrophages in the intestinal LP compartment in the steady state and during inflammation. CX3CR1 and CX3CL1 interactions may be important for maintaining antiinflammatory LP macrophage homeostasis in the steady state, while CCR2/CCL2 and/or other chemokine axes may regulate the accumulation of proinflammatory macrophages in the inflamed mucosa (36). This possibility is supported by recent data demonstrating the proinflammatory function of CX3CR1 lo and CCR2 hi LP macrophages during intestinal inflammation (36, 37). Since the reduction in LP macrophages in CX3CR1- and CX3CL1-deficient mice is not complete, it is tempting to speculate that the remaining LP macrophages may be CX3CR1 lo CCR2 hi proinflammatory LP macrophages that contribute to enhanced intestinal inflammation. Our analyses of Cx3cr1 gfp/gfp reporter mice, however, revealed that these remaining LP macrophages still expressed high levels of GFP, indicating that they are not proinflammatory LP macrophages. Thus, remnant LP macrophages in CX3CR1-deficient mice may be phenotypically and functionally similar to steady-state antiinflammatory LP macrophages in wild-type mice, and it is their significant reduction in number that predisposes the host to bacterial translocation and exacerbated intestinal inflammation. It is important to note that CX3CR1 deficiency also affects macrophage abundance in the lung and liver; thus, the CX3CR1/CX3CL1 axis may play an important role in macrophage recruitment to several tissues in addition to the intestine. In addition to the antiinflammatory functions of CX3CR1- expressing LP macrophages, it has been reported that TNFproducing CX3CR1 + LP DCs contribute to the pathogenesis of colitis (30). These findings, seemingly contradictory to ours, may be explained by differences between transferred monocytes and resident LP macrophages in the duration of conditioning in situ. In particular, TNF-producing CX3CR1 + LP DCs (30) were generated following monocyte transfer in a relatively short time frame (2 weeks) compared with the long half-life of resident LP macrophages (16). Given that conditioning of LP macrophages by stromal cells may account in part for their antiinflammatory functions (23), our data suggest that resident CX3CR1 + LP macrophages are antiinflammatory, while CX3CR1 + LP macrophages derived from recently infiltrating monocytes may have proinflammatory potential (30). Recent evidence showed that CX3CR1 deficiency results in the reduction of IL-10 production by a minor subset of LP macrophages and abrogation of antigen-specific Foxp3 + Treg induction and oral tolerance, while total macrophage numbers remained unchanged (38). Interestingly, we observed that ablation of the CX3CR1/CX3CL1 axis, by using Cx3cr1 gfp/gfp, Cx3cr1 /, or Cx3cl1 / mice, resulted in a significant reduction in all MHC II + LP macrophages subsets. We (15) and others (39) have shown that these major murine LP macrophage subsets produce copious amounts of IL-10, and thus a significant reduction in these cells may at least partially influence the observed biological effects of CX3CR1 deficiency on Treg induction and oral tolerance (38). Importantly, we did not observe a reduction in CD4 + Foxp3 + Tregs in the LP of CX3CR1-deficient mice, indicating that CX3CR1-expressing LP macrophages may play a critical role in the induction (15) or maintenance (40) of Foxp3 + induced Tregs and a lesser role in maintenance of naturally existing Foxp3 + Tregs. Further experimentation is clearly required to delineate the role of CX3CR1 and specific macrophage and DC subsets in mediating intestinal tolerance to soluble oral antigens, as well as bacterial antigens. Our findings that significant amounts of commensal bacteria translocated to the mlns of CX3CR1- and CX3CL1-deficient mice are consistent with the phagocytic nature of LP macrophages (23). Since LP DC numbers are largely unaffected in the absence of CX3CR1 and CX3CL1, our data also imply that LP macrophages may be more important than LP DCs in phagocytosis and killing of commensal bacteria. In spite of commensal bacteria being present in the mlns of CX3CR1-deficient mice, we did not observe any clinical signs of intestinal inflammation or innate immune cell activation in the mln or intestinal LP; however, we did observe increases in B cells in the small and large intestine LP (data not shown). These data are consistent with increased bacteria in the mln of JAM-A deficient mice correlating with enhanced B cell follicles in the colonic LP (41). Additionally, the dramatic increase in susceptibility to DSSinduced colitis in CX3CR1-deficient mice may be related to the reduction in phagocytic macrophages, thus creating an environment where commensal bacteria freely translocate following damage to the epithelial barrier. Interestingly, a recent report (42) proposed that CX3CR1 deficiency results in suppressed DSS-induced colitis in BALB/c mice. The reason for these discrepant observations are unclear but may be related to the strains of mice used or other unappreciated factors. We emphasize, however, that we have consistently observed enhanced DSS-induced colitis using two independent lines of CX3CR1-deficient mice as well as CX3CL1- deficient mice (all on the C57BL/6 background). Beyond their phagocytic capacity, LP macrophages may limit intestinal inflammation by promoting wound healing (43), The Journal of Clinical Investigation Volume 121 Number 12 December
8 dampening proinflammatory responses to TLR ligands, and inhibiting Th17 responses (15). We have previously demonstrated that LP macrophages can inhibit the induction of Th17 cells by CD11b + LP DCs in vitro (15) and speculate that the enhanced Th17 responses during intestinal inflammation in CX3CR1-deficient mice may be the result of a loss of macrophage-mediated regulation of CD11b + LP DCs. Further, the enhanced sensitivity of CX3CR1-deficient mice to colitis could be entirely reversed by neutralization of IL-17 or transfer of CX3CR1-expressing macrophages. While there are pathogenic and protective roles for IL-17 during homeostasis and intestinal inflammation (44 46), our data highlight an important, colitogenic role for IL-17 producing CD4 + T cells in the absence of CX3CR1. Collectively, our data support a role for the CX3CR1/CX3CL1 axis in regulating LP macrophage homeostasis, bacterial translocation, and IL-17 responses during intestinal inflammation. Further clarification of the functions of CX3CR1 in the steady state and during acute and chronic (21) colitis will likely contribute to a better understanding of mucosal immune regulation and direct efforts aimed at therapeutic intervention for mucosal inflammatory disorders, such as Crohn s disease and ulcerative colitis. Methods Mice. Six- to 8-week-old male Cx3cr1 gfp/gfp mice and age-matched Cx3cr1 +/+ mice were purchased from The Jackson Laboratory. Six- to 8-week-old male Cx3cr1 / mice and age-matched Cx3cr1 +/+ mice were purchased from Taconic. Cx3cl1 / mice were provided by Sergio Lira (Mount Sinai School of Medicine, New York, New York, USA) (47). Mice were maintained under specific pathogen free conditions at Emory Division of Animal Resources facilities. All animal protocols were reviewed and approved by the Institutional Animal Care and Use Committee of Emory University. Antibodies and reagents. The following antibodies were used: CD45-PerCP (30F11; BD), CD103-PE (M290; BD), CD4-PerCP (RM4-5; BD), IL-17A (TC11-18H10; BD), CD11c-allophycocyanin (N418; ebioscience), MHC II (I-A b ) Alexa Fluor 700 (M5/ ; ebioscience), CD11b efluor 450 (M1/70; ebioscience), F4/80-PE and F4/80 PE-Cy7 (BM8; ebioscience), TCRβ-allophycocyanin (H57-597; ebioscience), and FoxP3 efluor 450 (FJK-16s; ebioscience). Anti IL-17A (17F3) and mouse IgG 1 (MOPC-21) were purchased from Bio-X-Cell. Dead cells were identified using the fixable Aqua Dead Cell Staining Kit (Invitrogen). Recombinant murine M-CSF was from Peprotech. Dextran sulfate sodium (molecular mass, kda) was from USB Corp. Isolation of LP cells. Isolation of LP cells was performed as previously described with modifications (15). Briefly, small intestines were removed and carefully cleaned of their mesentery, and Peyer s patches were excised. Small and large intestine were opened longitudinally, washed of fecal contents, cut into pieces 0.5 cm in length, and subjected to two sequential 20-minute incubations in HBSS with 5% FCS and 2 mm EDTA at 37 C with agitation to remove epithelial cells. After each incubation step, media containing epithelial cells and debris was discarded. The remaining tissue was minced and incubated for 20 minutes in HBSS with 5% FCS, 1 mg/ml collagenase IV (Sigma-Aldrich), and 40 U/ml DNase I (Roche) at 37 C in agitation. Cell suspensions were collected and passed through a 100-μm strainer and pelleted by centrifugation at 300 g. Flow cytometry. Isolated LP cells were resuspended in PBS containing 5% FBS. Live cells were identified using an Aqua Dead Cell Staining Kit accordingly to the manufacturer s instructions, and Fc receptors were blocked with the antibody anti-fcγriii/ii (2.4G2) for 15 minutes at 4 C. After incubation the cells were stained at 4 C for 30 minutes with labeled antibodies. Samples were then washed 2 times in PBS containing 5% FBS and analyzed immediately, or intracellular staining was performed using a FoxP3 fixation/permeabilization kit (ebioscience) or Cytofix/Cytoperm kit with GolgiPlug (BD). Flow cytometric analysis was performed on a LSR II (BD). Real-time PCR. Total RNA was isolated from purified LP macrophages and DCs using the QIAGEN RNeasy Mini Kit, according to the manufacturer s protocol, with on-column DNase digestion using the RNase- Free DNase set. cdna was generated using the Superscript First-Strand Synthesis System for RT-PCR and random hexamer primers (Invitrogen), according to the manufacturer s protocol. cdna was used as a template for qrt-pcr using SYBR Green Master Mix (Bio-Rad), and primers for Cx3cr1 (F, AGGACACAGCCAGACAAG; R, TCAGGGGAGAAAGCAAG) and Gapdh (F, TGGCAAAGTGGAGATTGTTGCC; R, AAGATGGTGAT- GGGCTTCCCG). PCR and analysis were performed using a MyiQ icycler (Bio-Rad), and gene expression was calculated relative to Gapdh. DSS-induced colitis. Mice were provided 3% (wt/vol) DSS dissolved in the drinking water for 5 days. Daily clinical assessment of DSS-treated animals included measurement of a validated clinical DAI ranging from 0 to 4 (41), which was calculated using the following parameters: stool consistency, presence or absence of fecal blood (Hemoccult, Beckman Coulter), and weight loss. Mice were killed at day 5, and colons were assessed for histology. Blocking of cytokine effect in vivo. CX3CR1-deficient (Cx3cr1 gfp/gfp or Cx3cr1 / ) or Cx3cr1 +/+ mice were treated with DSS as described above. Mice were i.p. injected with 200 μg of neutralizing IL-17A or isotype control antibodies at days 0, 2, and 4. Colitis was assessed as described above. Bone marrow adoptive transfer. Total bone marrow cells from Cx3cr1 gfp/gfp or Cx3cr1 +/+ mice were cultured in the presence of 10 ng/ml M-CSF. Medium was replaced every 2 days, and at day 7 adherent macrophages were harvested. BMDMs ( ) were adoptively transferred (tail vein injection) into Cx3cr1 +/+ or Cx3cr1 gfp/gfp mice at days 1 and +1 of DSS treatment. Colitis was assessed as described above. Bacterial culture. Total mln cell suspension was cultured under aerobic conditions in LB blood agar plates for 24 hours at 37 C. Total DNA was directly isolated from individual colonies and sequenced for 16S rdna gene using the following primers: F, AGAGTTTGATCACTGGCTCAG; R, CTGCTGCCTCCCGTAGGAGT. Homology alignment was performed using NCBI BLAST software. Statistics. Statistical analysis was performed with Prism software (Graph- Pad Software) using an unpaired 2-tailed Student s t test. Error bars represent SD or SEM as indicated. P values less than 0.05 were considered statistically significant. Acknowledgments We thank Aaron Rae (Emory University Department of Pediatrics and Children s Healthcare of Atlanta Flow Core) for cell sorting. This work was supported by NIH grants (AA , AI to T.L. Denning; DK to A. Nusrat; DK to I.R. Williams; DK72654 and DK79392 to C.A. Parkos), a Career Development Award from the Crohn s and Colitis Foundation of America, and an Emory Egleston Children s Research Center seed grant to T.L. Denning. Received for publication May 24, 2011, and accepted in revised form September 21, Address correspondence to: Timothy L. Denning, Emory University School of Medicine, Whitehead Biomedical Research Building, Room 105R, 615 Michael St., Atlanta, Georgia 30322, USA. Phone: ; Fax: ; tdennin@emory.edu The Journal of Clinical Investigation Volume 121 Number 12 December 2011
9 1. Janeway CA Jr, Medzhitov R. Innate immune recognition. Annu Rev Immunol. 2002;20: Duchmann R, Kaiser I, Hermann E, Mayet W, Ewe K, Meyer zum Buschenfelde KH. Tolerance exists towards resident intestinal flora but is broken in active inflammatory bowel disease (IBD). Clin Exp Immunol. 1995;102(3): Izcue A, Coombes JL, Powrie F. Regulatory lymphocytes and intestinal inflammation. Annu Rev Immunol. 2009;27: Macdonald TT, Monteleone I, Fantini MC, Monteleone G. Regulation of homeostasis and inflammation in the intestine. Gastroenterology. 2011; 140(6): Abraham C, Medzhitov R. Interactions between the host innate immune system and microbes in inflammatory bowel disease. Gastroenterology. 2011; 140(6): Jang MH, et al. CCR7 is critically important for migration of dendritic cells in intestinal lamina propria to mesenteric lymph nodes. J Immunol. 2006; 176(2): Iwata M, Hirakiyama A, Eshima Y, Kagechika H, Kato C, Song SY. Retinoic acid imprints gut-homing specificity on T cells. Immunity. 2004;21(4): Mora JR, et al. Generation of gut-homing IgAsecreting B cells by intestinal dendritic cells. Science. 2006;314(5802): Mucida D, et al. Reciprocal TH17 and regulatory T cell differentiation mediated by retinoic acid. Science. 2007;317(5835): Coombes JL, et al. A functionally specialized population of mucosal CD103+ DCs induces Foxp3+ regulatory T cells via a TGF-beta and retinoic acid-dependent mechanism. J Exp Med. 2007; 204(8): Sun CM, et al. Small intestine lamina propria dendritic cells promote de novo generation of Foxp3 T reg cells via retinoic acid. J Exp Med. 2007; 204(8): Niess JH, et al. CX3CR1-mediated dendritic cell access to the intestinal lumen and bacterial clearance. Science. 2005;307(5707): Harrison JK, et al. Role for neuronally derived fractalkine in mediating interactions between neurons and CX3CR1-expressing microglia. Proc Natl Acad Sci U S A. 1998;95(18): Rescigno M. Intestinal dendritic cells. Adv Immunol. 2010;107: Denning TL, Wang YC, Patel SR, Williams IR, Pulendran B. Lamina propria macrophages and dendritic cells differentially induce regulatory and interleukin 17-producing T cell responses. Nat Immunol. 2007; 8(10): Schulz O, et al. Intestinal CD103+, but not CX3CR1+, antigen sampling cells migrate in lymph and serve classical dendritic cell functions. J Exp Med. 2009;206(13): Pabst O, Bernhardt G. The puzzle of intestinal lamina propria dendritic cells and macrophages. Eur J Immunol. 2010;40(8): Denning TL, et al. Functional specializations of intestinal dendritic cell and macrophage subsets that control Th17 and regulatory T cell responses are dependent on the T cell/apc ratio, source of mouse strain, and regional localization. J Immunol. 2011;187(2): Vallon-Eberhard A, Landsman L, Yogev N, Verrier B, Jung S. Transepithelial pathogen uptake into the small intestinal lamina propria. J Immunol. 2006;176(4): Chieppa M, Rescigno M, Huang AY, Germain RN. Dynamic imaging of dendritic cell extension into the small bowel lumen in response to epithelial cell TLR engagement. J Exp Med. 2006;203(13): Niess JH, Adler G. Enteric flora expands gut lamina propria CX3CR1+ dendritic cells supporting inflammatory immune responses under normal and inflammatory conditions. J Immunol. 2010;184(4): Combadiere C, et al. Decreased atherosclerotic lesion formation in CX3CR1/apolipoprotein E double knockout mice. Circulation. 2003;107(7): Smythies LE, et al. Human intestinal macrophages display profound inflammatory anergy despite avid phagocytic and bacteriocidal activity. J Clin Invest. 2005;115(1): Rescigno M, et al. Dendritic cells express tight junction proteins and penetrate gut epithelial monolayers to sample bacteria. Nat Immunol. 2001; 2(4): Qualls JE, Kaplan AM, van Rooijen N, Cohen DA. Suppression of experimental colitis by intestinal mononuclear phagocytes. J Leukoc Biol. 2006; 80(4): Hunter MM, et al. In vitro-derived alternatively activated macrophages reduce colonic inflammation in mice. Gastroenterology. 2010;138(4): Muehlhoefer A, et al. Fractalkine is an epithelial and endothelial cell-derived chemoattractant for intraepithelial lymphocytes in the small intestinal mucosa. J Immunol. 2000;164(6): Buonocore S, et al. Innate lymphoid cells drive interleukin-23-dependent innate intestinal pathology. Nature. 2010;464(7293): Varol C, et al. Monocytes give rise to mucosal, but not splenic, conventional dendritic cells. J Exp Med. 2007;204(1): Varol C, et al. Intestinal lamina propria dendritic cell subsets have different origin and functions. Immunity. 2009;31(3): Bogunovic M, et al. Origin of the lamina propria dendritic cell network. Immunity. 2009;31(3): Gordon S, Taylor PR. Monocyte and macrophage heterogeneity. Nat Rev Immunol. 2005;5(12): Nakache M, Berg EL, Streeter PR, Butcher EC. The mucosal vascular addressin is a tissue-specific endothelial cell adhesion molecule for circulating lymphocytes. Nature. 1989;337(6203): Zabel BA, et al. Human G protein-coupled receptor GPR-9-6/CC chemokine receptor 9 is selectively expressed on intestinal homing T lymphocytes, mucosal lymphocytes, and thymocytes and is required for thymus-expressed chemokine-mediated chemotaxis. J Exp Med. 1999;190(9): Mora JR. Homing imprinting and immunomodulation in the gut: role of dendritic cells and retinoids. Inflamm Bowel Dis. 2008;14(2): Platt AM, Bain CC, Bordon Y, Sester DP, Mowat AM. An independent subset of TLR expressing CCR2- dependent macrophages promotes colonic inflammation. J Immunol. 2010;184(12): Weber B, Saurer L, Schenk M, Dickgreber N, Mueller C. CX3CR1 defines functionally distinct intestinal mononuclear phagocyte subsets which maintain their respective functions during homeostatic and inflammatory conditions. Eur J Immunol. 2011;41(3): Hadis U, et al. Intestinal tolerance requires gut homing and expansion of FoxP3+ regulatory T cells in the lamina propria. Immunity. 2011;34(2): Kamada N, et al. Abnormally differentiated subsets of intestinal macrophage play a key role in Th1-dominant chronic colitis through excess production of IL-12 and IL-23 in response to bacteria. J Immunol. 2005;175(10): Murai M, et al. Interleukin 10 acts on regulatory T cells to maintain expression of the transcription factor Foxp3 and suppressive function in mice with colitis. Nat Immunol. 2009;10(11): Laukoetter MG, et al. JAM-A regulates permeability and inflammation in the intestine in vivo. J Exp Med. 2007;204(13): Kostadinova FI, Baba T, Ishida Y, Kondo T, Popivanova BK, Mukaida N. Crucial involvement of the CX3CR1-CX3CL1 axis in dextran sulfate sodium-mediated acute colitis in mice. J Leukoc Biol. 2010;88(1): Pull SL, Doherty JM, Mills JC, Gordon JI, Stappenbeck TS. Activated macrophages are an adaptive element of the colonic epithelial progenitor niche necessary for regenerative responses to injury. Proc Natl Acad Sci U S A. 2005;102(1): Ogawa A, Andoh A, Araki Y, Bamba T, Fujiyama Y. Neutralization of interleukin-17 aggravates dextran sulfate sodium-induced colitis in mice. Clin Immunol. 2004;110(1): Zhang Z, Zheng M, Bindas J, Schwarzenberger P, Kolls JK. Critical role of IL-17 receptor signaling in acute TNBS-induced colitis. Inflamm Bowel Dis. 2006;12(5): O Connor W Jr, et al. A protective function for interleukin 17A in T cell-mediated intestinal inflammation. Nat Immunol. 2009;10(6): Cook DN, et al. Generation and analysis of mice lacking the chemokine fractalkine. Mol Cell Biol. 2001;21(9): The Journal of Clinical Investigation Volume 121 Number 12 December
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine
 Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Innate immune regulation of T-helper (Th) cell homeostasis in the intestine Masayuki Fukata, MD, Ph.D. Research Scientist II Division of Gastroenterology, Department of Medicine, F. Widjaja Foundation,
Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice
 Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
Genetics. Environment. You Are Only 10% Human. Pathogenesis of IBD. Advances in the Pathogenesis of IBD: Genetics Leads to Function IBD
 Advances in the Pathogenesis of IBD: Genetics Leads to Function Pathogenesis of IBD Environmental Factors Microbes Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School
Advances in the Pathogenesis of IBD: Genetics Leads to Function Pathogenesis of IBD Environmental Factors Microbes Scott Plevy, MD Associate Professor of Medicine, Microbiology & Immunology UNC School
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Supplemental Information. T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism
 Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell?
 Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Abbas Chapter 2: Sarah Spriet February 8, 2015 Question 1. Kupffer cells, microglial cells and osteoclasts are all examples of what type of immune system cell? a. Dendritic cells b. Macrophages c. Monocytes
Intestinal Microbiota in Health and Disease
 Intestinal Microbiota in Health and Disease February 27, 2015 Master s Course in Gastroenterology Prof. Kathy McCoy 1 Overview Overview of Gut Microbiota Microbiota in Health Microbiota in Disease 2 Gut
Intestinal Microbiota in Health and Disease February 27, 2015 Master s Course in Gastroenterology Prof. Kathy McCoy 1 Overview Overview of Gut Microbiota Microbiota in Health Microbiota in Disease 2 Gut
D CD8 T cell number (x10 6 )
 IFNγ Supplemental Figure 1. CD T cell number (x1 6 ) 18 15 1 9 6 3 CD CD T cells CD6L C CD5 CD T cells CD6L D CD8 T cell number (x1 6 ) 1 8 6 E CD CD8 T cells CD6L F Log(1)CFU/g Feces 1 8 6 p
IFNγ Supplemental Figure 1. CD T cell number (x1 6 ) 18 15 1 9 6 3 CD CD T cells CD6L C CD5 CD T cells CD6L D CD8 T cell number (x1 6 ) 1 8 6 E CD CD8 T cells CD6L F Log(1)CFU/g Feces 1 8 6 p
Suppl Video: Tumor cells (green) and monocytes (white) are seeded on a confluent endothelial
 Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
SUPPLEMENTARY METHODS
 SUPPLEMENTARY METHODS Histological analysis. Colonic tissues were collected from 5 parts of the middle colon on day 7 after the start of DSS treatment, and then were cut into segments, fixed with 4% paraformaldehyde,
SUPPLEMENTARY METHODS Histological analysis. Colonic tissues were collected from 5 parts of the middle colon on day 7 after the start of DSS treatment, and then were cut into segments, fixed with 4% paraformaldehyde,
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Figures
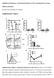 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Mononuclear Phagocytes - Origins, Fates & Functions - Dr. Steffen Jung
 1 Department of Immunology The Weizmann Institute of Science Rehovot, Israel The mononuclear phagocyte system Van Furth and Cohn (1968) Ilya (Eli) Metchnikoff (1845-1916) Nobel prize 1908 Macrophages Ralph
1 Department of Immunology The Weizmann Institute of Science Rehovot, Israel The mononuclear phagocyte system Van Furth and Cohn (1968) Ilya (Eli) Metchnikoff (1845-1916) Nobel prize 1908 Macrophages Ralph
Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces
 Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces Department of Biologic & Materials Sciences School of Dentistry University of Michigan Ann Arbor, Michigan 48109-1078 1 Image quality
Molecular and Cellular Basis of Immune Protection of Mucosal Surfaces Department of Biologic & Materials Sciences School of Dentistry University of Michigan Ann Arbor, Michigan 48109-1078 1 Image quality
SUPPLEMENTARY FIGURES
 SUPPLEMENTARY FIGURES Supplementary Figure 1: Chemokine receptor expression profiles of CCR6 + and CCR6 - CD4 + IL-17A +/ex and Treg cells. Quantitative PCR analysis of chemokine receptor transcript abundance
SUPPLEMENTARY FIGURES Supplementary Figure 1: Chemokine receptor expression profiles of CCR6 + and CCR6 - CD4 + IL-17A +/ex and Treg cells. Quantitative PCR analysis of chemokine receptor transcript abundance
PBS Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs , 27-30
 PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
PBS 803 - Class #2 Introduction to the Immune System part II Suggested reading: Abbas, pgs. 15-25, 27-30 Learning Objectives Compare and contrast the maturation of B and T lymphocytes Compare and contrast
LECTURE 12: MUCOSAL IMMUNITY GUT STRUCTURE
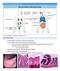 LECTURE 12: MUCOSAL IMMUNITY GUT STRUCTURE - Small intestine in humans is around 3-4 metres long - Internal surface of the small intestines are lined by villi o Villi are composed of absorptive cells (epithelial/enterocytes)
LECTURE 12: MUCOSAL IMMUNITY GUT STRUCTURE - Small intestine in humans is around 3-4 metres long - Internal surface of the small intestines are lined by villi o Villi are composed of absorptive cells (epithelial/enterocytes)
Mucosal Immunology Sophomore Dental and Optometry Microbiology Section I: Immunology. Robin Lorenz
 Mucosal Immunology Sophomore Dental and Optometry Microbiology Section I: Immunology Robin Lorenz rlorenz@uab.edu Why do we Need to Understand How the Mucosal Immune System Works? The mucosa is the major
Mucosal Immunology Sophomore Dental and Optometry Microbiology Section I: Immunology Robin Lorenz rlorenz@uab.edu Why do we Need to Understand How the Mucosal Immune System Works? The mucosa is the major
Necrotizing Enterocolitis: The Role of the Immune System
 Necrotizing Enterocolitis: The Role of the Immune System Patricia Denning, M.D. Associate Professor in Pediatrics Division of Neonatology Emory University School of Medicine What is NEC? What is NEC? Necrotizing
Necrotizing Enterocolitis: The Role of the Immune System Patricia Denning, M.D. Associate Professor in Pediatrics Division of Neonatology Emory University School of Medicine What is NEC? What is NEC? Necrotizing
Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells
 ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
ICI Basic Immunology course Effector mechanisms of cell-mediated immunity: Properties of effector, memory and regulatory T cells Abul K. Abbas, MD UCSF Stages in the development of T cell responses: induction
17 th International Conference of the Inflammation Research Association: Wednesday AM (Day 4) September 9-13, 2012
 17 th International Conference of the Inflammation Research Association: Wednesday AM (Day 4) September 9-13, 2012 The Sagamore Resort, Bolton Landing, NY, USA The following report includes highlights
17 th International Conference of the Inflammation Research Association: Wednesday AM (Day 4) September 9-13, 2012 The Sagamore Resort, Bolton Landing, NY, USA The following report includes highlights
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors Presented by Jurg Rohrer, PhD, BD Biosciences 23-10780-00 Outline Introduction Cytokines Transcription
Supplemental Table I.
 Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Effector T Cells and
 1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
1 Effector T Cells and Cytokines Andrew Lichtman, MD PhD Brigham and Women's Hospital Harvard Medical School 2 Lecture outline Cytokines Subsets of CD4+ T cells: definitions, functions, development New
Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy
 Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy Chapter 11 (pages 429-460): Dynamics of Adaptive Immunity prepared by Kelly von Elten, Walter Reed National Military Medical Center,
Review Questions: Janeway s Immunobiology 8th Edition by Kenneth Murphy Chapter 11 (pages 429-460): Dynamics of Adaptive Immunity prepared by Kelly von Elten, Walter Reed National Military Medical Center,
Control of intestinal inflammation by regulatory T cells
 Control of intestinal inflammation by regulatory T cells Fiona Powrie Sir William Dunn School of Pathology University of Oxford fiona.powrie@path.ox.ac.uk Regulatory T cells prevent immune pathology in
Control of intestinal inflammation by regulatory T cells Fiona Powrie Sir William Dunn School of Pathology University of Oxford fiona.powrie@path.ox.ac.uk Regulatory T cells prevent immune pathology in
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF
 CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
1. Overview of Adaptive Immunity
 Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
Chapter 17A: Adaptive Immunity Part I 1. Overview of Adaptive Immunity 2. T and B Cell Production 3. Antigens & Antigen Presentation 4. Helper T cells 1. Overview of Adaptive Immunity The Nature of Adaptive
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Supporting Information
 Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Accepted Manuscript. Innate immune cells regulate oncoimmunity and cancer development. Ai-Ping Bai, Yuan Guo
 Accepted Manuscript Innate immune cells regulate oncoimmunity and cancer development Ai-Ping Bai, Yuan Guo PII: S0016-5085(18)34974-6 DOI: 10.1053/j.gastro.2018.08.057 Reference: YGAST 62119 To appear
Accepted Manuscript Innate immune cells regulate oncoimmunity and cancer development Ai-Ping Bai, Yuan Guo PII: S0016-5085(18)34974-6 DOI: 10.1053/j.gastro.2018.08.057 Reference: YGAST 62119 To appear
for six pairs of mice. (b) Representative FACS analysis of absolute number of T cells (CD4 + and
 SUPPLEMENTARY DATA Supplementary Figure 1: Peripheral lymphoid organs of SMAR1 -/- mice have an effector memory phenotype. (a) Lymphocytes collected from MLNs and Peyer s patches (PPs) of WT and SMAR1
SUPPLEMENTARY DATA Supplementary Figure 1: Peripheral lymphoid organs of SMAR1 -/- mice have an effector memory phenotype. (a) Lymphocytes collected from MLNs and Peyer s patches (PPs) of WT and SMAR1
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH
 FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH ALETA A SOURCE OF 1,3-BETA GLUCANS Aleta is highly bioavailable, offering a concentration greater than 5% of 1,3-beta glucans. Aleta provides a consistent response
FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH ALETA A SOURCE OF 1,3-BETA GLUCANS Aleta is highly bioavailable, offering a concentration greater than 5% of 1,3-beta glucans. Aleta provides a consistent response
Sipper BK Experimental Animal Co. (Shanghai, China) and bred in a specific. pathogen-free environment. The animal study protocol was approved by the
 Supplementary information, Data S1 Materials and Methods Mice, Ad vectors and reagents Female C57BL/6 mice, 8-10 weeks of age, were purchased from Joint Ventures Sipper BK Experimental Animal Co. (Shanghai,
Supplementary information, Data S1 Materials and Methods Mice, Ad vectors and reagents Female C57BL/6 mice, 8-10 weeks of age, were purchased from Joint Ventures Sipper BK Experimental Animal Co. (Shanghai,
B220 CD4 CD8. Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN
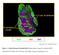 B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
B220 CD4 CD8 Natarajan et al., unpublished data Figure 1. Confocal Image of Sensitized HLN. Representative image of a sensitized HLN showing B cell follicles and T cell areas. 20 µm thick. Image of magnification
T Regulatory Cell and Body Tolerance
 Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 2017, 9 [5]:23-28 [http://scholarsresearchlibrary.com/archive.html] ISSN 0975-5071 USA CODEN: DPLEB4
Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 2017, 9 [5]:23-28 [http://scholarsresearchlibrary.com/archive.html] ISSN 0975-5071 USA CODEN: DPLEB4
General Overview of Immunology. Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center
 General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
General Overview of Immunology Kimberly S. Schluns, Ph.D. Associate Professor Department of Immunology UT MD Anderson Cancer Center Objectives Describe differences between innate and adaptive immune responses
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
Innate immunity as a therapeutic target in IBD. Elke Cario Division of Gastroenterology & Hepatology University Hospital of Essen Essen, Germany
 Innate immunity as a therapeutic target in IBD Elke Cario Division of Gastroenterology & Hepatology University Hospital of Essen Essen, Germany The intestinal mucosa must rapidly recognize luminal pathogens
Innate immunity as a therapeutic target in IBD Elke Cario Division of Gastroenterology & Hepatology University Hospital of Essen Essen, Germany The intestinal mucosa must rapidly recognize luminal pathogens
Frontiers of Science Foundation Scholar. Toby Bothwell. Freshman, University of Arkansas. final research manuscripts
 Frontiers of Science Foundation Scholar Toby Bothwell Oklahoma city, OKlahoma Freshman, University of Arkansas final research manuscripts The Effect of Estradiol and Estrogen Receptors α and β on Bone
Frontiers of Science Foundation Scholar Toby Bothwell Oklahoma city, OKlahoma Freshman, University of Arkansas final research manuscripts The Effect of Estradiol and Estrogen Receptors α and β on Bone
D2 inhibits TLR2- initiated 12p40 transcription (-) TLR2 PGN MDP. MyD88 IRAK ECSIT TRAF6 NIK. Smallest unit of PGN muramyl dipeptide IKK.
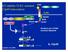 D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
D2 inhibits TLR2- initiated 12p40 transcription CARD CARD NOD2 LRR RICK/Rip2 NIK MDP TRAF6 PGN TLR2 MyD88 IRAK ECSIT (-) IKK Smallest unit of PGN muramyl dipeptide IκB NF-κB atanabe et al, 2004 NF-κB IL-12p40
Putting it Together. Stephen Canfield Secondary Lymphoid System. Tonsil Anterior Cervical LN s
 Putting it Together Stephen Canfield smc12@columbia.edu Secondary Lymphoid System Tonsil Anterior Cervical LN s Axillary LN s Mediastinal/Retroperitoneal LN s Thoracic Duct Appendix Spleen Inguinal LN
Putting it Together Stephen Canfield smc12@columbia.edu Secondary Lymphoid System Tonsil Anterior Cervical LN s Axillary LN s Mediastinal/Retroperitoneal LN s Thoracic Duct Appendix Spleen Inguinal LN
Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained
 1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
Part III Innate and Adaptive Immune Cells: General Introduction
 Innate and Adaptive Immune Cells: General Introduction Iván López-Expósito As an organ specialized in food digestion and nutrient absorption, the intestinal mucosa presents a huge surface area (almost
Innate and Adaptive Immune Cells: General Introduction Iván López-Expósito As an organ specialized in food digestion and nutrient absorption, the intestinal mucosa presents a huge surface area (almost
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Copyright 2014 The Authors. Deposited on: 19 June 2014
 Bain, Calum C., and Mowat, Allan McI. (2014) Macrophages in intestinal homeostasis and inflammation. Immunological Reviews, 260 (1). pp. 102-117. ISSN 0105-2896 Copyright 2014 The Authors http://eprints.gla.ac.uk/93404/
Bain, Calum C., and Mowat, Allan McI. (2014) Macrophages in intestinal homeostasis and inflammation. Immunological Reviews, 260 (1). pp. 102-117. ISSN 0105-2896 Copyright 2014 The Authors http://eprints.gla.ac.uk/93404/
Supplementary Material
 Supplementary Material Fig. S1. Gpa33 -/- mice do not express Gpa33 mrna or GPA33 protein. (A) The Gpa33 null allele contains a premature translational stop codon (STOP) in exon 2, and almost all of the
Supplementary Material Fig. S1. Gpa33 -/- mice do not express Gpa33 mrna or GPA33 protein. (A) The Gpa33 null allele contains a premature translational stop codon (STOP) in exon 2, and almost all of the
The Adaptive Immune Response. B-cells
 The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
The Adaptive Immune Response B-cells The innate immune system provides immediate protection. The adaptive response takes time to develop and is antigen specific. Activation of B and T lymphocytes Naive
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured
 Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
Cytokines modulate the functional activities of individual cells and tissues both under normal and pathologic conditions Interleukins,
 Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Cytokines http://highered.mcgraw-hill.com/sites/0072507470/student_view0/chapter22/animation the_immune_response.html Cytokines modulate the functional activities of individual cells and tissues both under
Immune system. Self/non-self recognition. Memory. The state of protection from infectious disease. Acceptance vs rejection
 Immune system The state of protection from infectious disease Self/non-self recognition 自我 非我 Acceptance vs rejection Memory 疫苗 2 Microbes Commensal Microbes 共生菌 Normal flora: usually confined to certain
Immune system The state of protection from infectious disease Self/non-self recognition 自我 非我 Acceptance vs rejection Memory 疫苗 2 Microbes Commensal Microbes 共生菌 Normal flora: usually confined to certain
Supplemental Figures: Supplemental Figure 1
 Supplemental Figures: Supplemental Figure 1 Suppl. Figure 1. BM-DC infection with H. pylori does not induce cytotoxicity and treatment of BM-DCs with H. pylori sonicate, but not heat-inactivated bacteria,
Supplemental Figures: Supplemental Figure 1 Suppl. Figure 1. BM-DC infection with H. pylori does not induce cytotoxicity and treatment of BM-DCs with H. pylori sonicate, but not heat-inactivated bacteria,
Newly Recognized Components of the Innate Immune System
 Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
Newly Recognized Components of the Innate Immune System NOD Proteins: Intracellular Peptidoglycan Sensors NOD-1 NOD-2 Nod Protein LRR; Ligand Recognition CARD RICK I-κB p50 p65 NF-κB Polymorphisms in Nod-2
SUPPORTING INFORMATIONS
 SUPPORTING INFORMATIONS Mice MT/ret RetCD3ε KO α-cd25 treated MT/ret Age 1 month 3 mnths 6 months 1 month 3 months 6 months 1 month 3 months 6 months 2/87 Survival 87/87 incidence of 17/87 1 ary tumor
SUPPORTING INFORMATIONS Mice MT/ret RetCD3ε KO α-cd25 treated MT/ret Age 1 month 3 mnths 6 months 1 month 3 months 6 months 1 month 3 months 6 months 2/87 Survival 87/87 incidence of 17/87 1 ary tumor
The Adaptive Immune Responses
 The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
IL-12 family members in experimental colitis. Markus F. Neurath I. Medical Clinic Johannes Gutenberg-University Mainz, Germany
 IL-12 family members in experimental colitis Markus F. Neurath I. Medical Clinic Johannes Gutenberg-University Mainz, Germany IBD - Pathogenesis Genetic Predisposition Bacterial Antigens Activation of
IL-12 family members in experimental colitis Markus F. Neurath I. Medical Clinic Johannes Gutenberg-University Mainz, Germany IBD - Pathogenesis Genetic Predisposition Bacterial Antigens Activation of
Supplemental Information. Gut Microbiota Promotes Hematopoiesis to Control Bacterial Infection. Cell Host & Microbe, Volume 15
 Cell Host & Microbe, Volume 15 Supplemental Information Gut Microbiota Promotes Hematopoiesis to Control Bacterial Infection Arya Khosravi, Alberto Yáñez, Jeremy G. Price, Andrew Chow, Miriam Merad, Helen
Cell Host & Microbe, Volume 15 Supplemental Information Gut Microbiota Promotes Hematopoiesis to Control Bacterial Infection Arya Khosravi, Alberto Yáñez, Jeremy G. Price, Andrew Chow, Miriam Merad, Helen
Chapter 3, Part A (Pages 37-45): Leukocyte Migration into Tissues
 Allergy and Immunology Review Corner: Chapter 3, Part A (pages 37-45) of Cellular and Molecular Immunology (Seventh Edition), by Abul K. Abbas, Andrew H. Lichtman and Shiv Pillai. Chapter 3, Part A (Pages
Allergy and Immunology Review Corner: Chapter 3, Part A (pages 37-45) of Cellular and Molecular Immunology (Seventh Edition), by Abul K. Abbas, Andrew H. Lichtman and Shiv Pillai. Chapter 3, Part A (Pages
The development of T cells in the thymus
 T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
T cells rearrange their receptors in the thymus whereas B cells do so in the bone marrow. The development of T cells in the thymus The lobular/cellular organization of the thymus Immature cells are called
Supplementary Information:
 Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Grup de fisiologia digestiva i adaptacions nutricionals Institut de Nutrició i Seguretat Alimentaria
 Grup de fisiologia digestiva i adaptacions nutricionals Institut de Nutrició i Seguretat Alimentaria 1 Outline Weaning and the consequences of stress Animal blood plasma Spray-drying SDP SDP in a model
Grup de fisiologia digestiva i adaptacions nutricionals Institut de Nutrició i Seguretat Alimentaria 1 Outline Weaning and the consequences of stress Animal blood plasma Spray-drying SDP SDP in a model
The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells
 1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
Targeting tumour associated macrophages in anti-cancer therapies. Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018
 Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Unique CD14 + intestinal macrophages contribute to the pathogenesis of Crohn disease via IL-23/IFN-γ axis
 Research article Unique CD14 + intestinal macrophages contribute to the pathogenesis of Crohn disease via IL-23/IFN-γ axis Nobuhiko Kamada, 1 Tadakazu Hisamatsu, 1 Susumu Okamoto, 1 Hiroshi Chinen, 1 Taku
Research article Unique CD14 + intestinal macrophages contribute to the pathogenesis of Crohn disease via IL-23/IFN-γ axis Nobuhiko Kamada, 1 Tadakazu Hisamatsu, 1 Susumu Okamoto, 1 Hiroshi Chinen, 1 Taku
Supplementary Information. Tissue-wide immunity against Leishmania. through collective production of nitric oxide
 Supplementary Information Tissue-wide immunity against Leishmania through collective production of nitric oxide Romain Olekhnovitch, Bernhard Ryffel, Andreas J. Müller and Philippe Bousso Supplementary
Supplementary Information Tissue-wide immunity against Leishmania through collective production of nitric oxide Romain Olekhnovitch, Bernhard Ryffel, Andreas J. Müller and Philippe Bousso Supplementary
Faecalibacterium prausnitzii
 Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients PNAS 105(43): 16731-16736, 2008. Speaker: Ming-Cheng Chen Advisor:
Faecalibacterium prausnitzii is an anti-inflammatory commensal bacterium identified by gut microbiota analysis of Crohn disease patients PNAS 105(43): 16731-16736, 2008. Speaker: Ming-Cheng Chen Advisor:
Supplementary Materials for
 immunology.sciencemag.org/cgi/content/full/2/16/eaan6049/dc1 Supplementary Materials for Enzymatic synthesis of core 2 O-glycans governs the tissue-trafficking potential of memory CD8 + T cells Jossef
immunology.sciencemag.org/cgi/content/full/2/16/eaan6049/dc1 Supplementary Materials for Enzymatic synthesis of core 2 O-glycans governs the tissue-trafficking potential of memory CD8 + T cells Jossef
Pathologic Stage. Lymph node Stage
 ASC ASC a c Patient ID BMI Age Gleason score Non-obese PBMC 1 22.1 81 6 (3+3) PBMC 2 21.9 6 6 (3+3) PBMC 3 22 84 8 (4+4) PBMC 4 24.6 68 7 (3+4) PBMC 24. 6 (3+3) PBMC 6 24.7 73 7 (3+4) PBMC 7 23. 67 7 (3+4)
ASC ASC a c Patient ID BMI Age Gleason score Non-obese PBMC 1 22.1 81 6 (3+3) PBMC 2 21.9 6 6 (3+3) PBMC 3 22 84 8 (4+4) PBMC 4 24.6 68 7 (3+4) PBMC 24. 6 (3+3) PBMC 6 24.7 73 7 (3+4) PBMC 7 23. 67 7 (3+4)
Mucosal immunity Reddy April Deveshni Reddy Allergy Meeting 13 April 2012
 Deveshni Reddy Allergy Meeting 13 April First recorded by Hippocrates over 2000 years ago. 1921: Prausnitz and Kustner demonstrated that substance responsible for Kustner s fish allergy was present in
Deveshni Reddy Allergy Meeting 13 April First recorded by Hippocrates over 2000 years ago. 1921: Prausnitz and Kustner demonstrated that substance responsible for Kustner s fish allergy was present in
Fig. S1 A. week 4 week 6
 Fig. S1 Trabecular Number Trabecular Thickness number/mm 3.5 3. 2.5 2. 1.5 1..5 mm.45.4.35.3.25.2.15.1.5 SKG-c SKG-A mm 1.4 1.2 1..8.6.4.2 Trabecular Spacing D. week 4 week 6 Figure S1. MicroCT analysis
Fig. S1 Trabecular Number Trabecular Thickness number/mm 3.5 3. 2.5 2. 1.5 1..5 mm.45.4.35.3.25.2.15.1.5 SKG-c SKG-A mm 1.4 1.2 1..8.6.4.2 Trabecular Spacing D. week 4 week 6 Figure S1. MicroCT analysis
Felix Yarovinsky. Department of Immunology, UT Southwestern Medical Center. Innate immune defense to Toxoplasma gondii
 Felix Yarovinsky Department of Immunology, UT Southwestern Medical Center Innate immune defense to Toxoplasma gondii Pathogen recognition by innate immune cells Pathogen Parasites Viruses Bacteria Initiator
Felix Yarovinsky Department of Immunology, UT Southwestern Medical Center Innate immune defense to Toxoplasma gondii Pathogen recognition by innate immune cells Pathogen Parasites Viruses Bacteria Initiator
A crucial role for HVEM and BTLA in preventing intestinal inflammation
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 A crucial role for HVEM and BTLA in preventing intestinal inflammation Marcos W. Steinberg La Jolla Institute
Washington University School of Medicine Digital Commons@Becker Open Access Publications 2008 A crucial role for HVEM and BTLA in preventing intestinal inflammation Marcos W. Steinberg La Jolla Institute
Optimizing Intracellular Flow Cytometry
 Optimizing Intracellular Flow Cytometry Detection of Cytokines, Transcription Factors, and Phosphoprotein by Flow Cytometry Presented by Erika O Donnell, PhD, BD Biosciences 23-14876-00 Outline Basic principles
Optimizing Intracellular Flow Cytometry Detection of Cytokines, Transcription Factors, and Phosphoprotein by Flow Cytometry Presented by Erika O Donnell, PhD, BD Biosciences 23-14876-00 Outline Basic principles
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder I Nakaya, Kousik
 SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
The Case of the Spring Break Consequences
 The Case of the Spring Break Consequences Hazel reluctantly opened her eyes when her alarm went off. Spring Break was over, and she was definitely NOT ready for the second half of the semester. However,
The Case of the Spring Break Consequences Hazel reluctantly opened her eyes when her alarm went off. Spring Break was over, and she was definitely NOT ready for the second half of the semester. However,
The Immune Response in Time and Space
 The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
The Immune Response in Time and Space Chapters 14 & 4 Sharon S. Evans, Ph.D. Department of Immunology 845-3421 sharon.evans@roswellpark.org September 18 & 23, 2014 Inflammation Inflammation Complex response
Immunology, Faculty of Medicine University of Bari, Bari (Italy) Proprietà benefiche di latte, vino e olio extra vergine di oliva
 Immunology, Faculty of Medicine University of Bari, Bari (Italy) Proprietà benefiche di latte, vino e olio extra vergine di oliva Professor Emilio Jirillo basketball court (about 400 m 2 ) mucosa-associated
Immunology, Faculty of Medicine University of Bari, Bari (Italy) Proprietà benefiche di latte, vino e olio extra vergine di oliva Professor Emilio Jirillo basketball court (about 400 m 2 ) mucosa-associated
Role of Th17 cells in the immunopathogenesis of dry eye disease
 Role of Th17 cells in the immunopathogenesis of dry eye disease The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Chauhan,
Role of Th17 cells in the immunopathogenesis of dry eye disease The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation Chauhan,
Mucosal Immunology. Cathryn Nagler University of Chicago Department of Pathology/Committee on Immunology
 Mucosal Immunology Cathryn Nagler University of Chicago Department of Pathology/Committee on Immunology cnagler@bsd.uchicago.edu Mucosal surfaces are the major portals of entry for antigen Largest area
Mucosal Immunology Cathryn Nagler University of Chicago Department of Pathology/Committee on Immunology cnagler@bsd.uchicago.edu Mucosal surfaces are the major portals of entry for antigen Largest area
SUPPLEMENTARY INFORMATION
 Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
Supplemental Figure 1. Furin is efficiently deleted in CD4 + and CD8 + T cells. a, Western blot for furin and actin proteins in CD4cre-fur f/f and fur f/f Th1 cells. Wild-type and furin-deficient CD4 +
Naive, memory and regulatory T lymphocytes populations analysis
 Naive, memory and regulatory T lymphocytes populations analysis Jaen Olivier, PhD ojaen@beckmancoulter.com Cellular Analysis application specialist Beckman Coulter France Introduction Flow cytometric analysis
Naive, memory and regulatory T lymphocytes populations analysis Jaen Olivier, PhD ojaen@beckmancoulter.com Cellular Analysis application specialist Beckman Coulter France Introduction Flow cytometric analysis
Immunology for the Rheumatologist
 Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Immunology for the Rheumatologist Rheumatologists frequently deal with the immune system gone awry, rarely studying normal immunology. This program is an overview and discussion of the function of the
Supplementary Figure 1 Chemokine and chemokine receptor expression during muscle regeneration (a) Analysis of CR3CR1 mrna expression by real time-pcr
 Supplementary Figure 1 Chemokine and chemokine receptor expression during muscle regeneration (a) Analysis of CR3CR1 mrna expression by real time-pcr at day 0, 1, 4, 10 and 21 post- muscle injury. (b)
Supplementary Figure 1 Chemokine and chemokine receptor expression during muscle regeneration (a) Analysis of CR3CR1 mrna expression by real time-pcr at day 0, 1, 4, 10 and 21 post- muscle injury. (b)
Supplementary Figure 1. mrna expression of chitinase and chitinase-like protein in splenic immune cells. Each splenic immune cell population was
 Supplementary Figure 1. mrna expression of chitinase and chitinase-like protein in splenic immune cells. Each splenic immune cell population was sorted by FACS. Surface markers for sorting were CD11c +
Supplementary Figure 1. mrna expression of chitinase and chitinase-like protein in splenic immune cells. Each splenic immune cell population was sorted by FACS. Surface markers for sorting were CD11c +
Eosinophils are required. for the maintenance of plasma cells in the bone marrow
 Eosinophils are required for the maintenance of plasma cells in the bone marrow Van Trung Chu, Anja Fröhlich, Gudrun Steinhauser, Tobias Scheel, Toralf Roch, Simon Fillatreau, James J. Lee, Max Löhning
Eosinophils are required for the maintenance of plasma cells in the bone marrow Van Trung Chu, Anja Fröhlich, Gudrun Steinhauser, Tobias Scheel, Toralf Roch, Simon Fillatreau, James J. Lee, Max Löhning
Alessandra Franco, M.D., Ph.D. UCSD School of Medicine Department of Pediatrics Division of Allergy, Immunology and Rheumatology
 Natural regulatory T cells recognize the heavy constant region (Fc) of immunoglobulins: a novel mechanism for IVIG immunotherapy in Pediatric Immune-mediated diseases Alessandra Franco, M.D., Ph.D. UCSD
Natural regulatory T cells recognize the heavy constant region (Fc) of immunoglobulins: a novel mechanism for IVIG immunotherapy in Pediatric Immune-mediated diseases Alessandra Franco, M.D., Ph.D. UCSD
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY
 ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
ACTIVATION OF T LYMPHOCYTES AND CELL MEDIATED IMMUNITY The recognition of specific antigen by naïve T cell induces its own activation and effector phases. T helper cells recognize peptide antigens through
Supplementary information CD4 T cells are required for both development and maintenance of disease in a new model of reversible colitis
 Supplementary information CD4 T cells are required for both development and maintenance of disease in a new model of reversible colitis rasseit and Steiner et al. .. Supplementary Figure 1 % of initial
Supplementary information CD4 T cells are required for both development and maintenance of disease in a new model of reversible colitis rasseit and Steiner et al. .. Supplementary Figure 1 % of initial
Advances in Cancer Immunotherapy
 Advances in Cancer Immunotherapy Immunology 101 for the Non-Immunologist Arnold H. Zea, PhD azea@lsuhsc.edu Disclosures No relevant financial relationships to disclose This presentation does not contain
Advances in Cancer Immunotherapy Immunology 101 for the Non-Immunologist Arnold H. Zea, PhD azea@lsuhsc.edu Disclosures No relevant financial relationships to disclose This presentation does not contain
Supporting Information
 Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Supporting Information Aldridge et al. 10.1073/pnas.0900655106 Fig. S1. Flow diagram of sublethal (a) and lethal (b) influenza virus infections. (a) Infection of lung epithelial cells by influenza virus
Reviewers' comments: Reviewer #1 (Remarks to the Author):
 Reviewers' comments: Reviewer #1 (Remarks to the Author): The manuscript by Sun et al., provide data showing that short-chain fatty acids produced by intestinal microbiota act through GPR43 to induced
Reviewers' comments: Reviewer #1 (Remarks to the Author): The manuscript by Sun et al., provide data showing that short-chain fatty acids produced by intestinal microbiota act through GPR43 to induced
