Reprogramming of antiviral T cells prevents inactivation and restores T cell activity during persistent viral infection
|
|
|
- Clifford Manning
- 5 years ago
- Views:
Transcription
1 Research article Reprogramming of antiviral T cells prevents inactivation and restores T cell activity during persistent viral infection David G. Brooks, Dorian B. McGavern, and Michael B.A. Oldstone Viral Immunobiology Laboratory, Molecular and Integrative Neuroscience Department, and Department of Infectology, The Scripps Research Institute, La Jolla, California, USA. Failure to clear persistent viral infections results from the early loss of T cell activity. A pertinent question is whether the immune response is programmed to fail or if nonresponsive T cells can specifically be fixed to eliminate infection. Although evidence indicates that T cell expansion is permanently programmed during the initial priming events, the mechanisms that determine the acquisition of T cell function are less clear. Herein we show that in contrast to expansion, the functional programming of T cell effector and memory responses in vivo in mice is not hardwired during priming but is alterable and responsive to continuous instruction from the antigenic environment. As a direct consequence, dysfunctional T cells can be functionally reactivated during persistent infection even after an initial program of inactivation has been instituted. We also show that early therapeutic reductions in viral replication facilitate the preservation of antiviral CD4 + T cell activity, enabling the long-term control of viral replication. Thus, dysfunctional antiviral T cells can regain activity, providing a basis for future therapeutic strategies to treat persistent viral infections. Introduction It is crucial for the eradication of established persistent viral infections that the host s antiviral immune response be functionally restored. Concomitant with the establishment of viral persistence, antiviral CD4 + and CD8 + T cells become nonresponsive toward viral antigens and are either physically deleted or persist in an inactivated state (1 4). T cell inactivation is observed during a variety of different persistent viral infections, including HIV, HBV, and HCV in humans and lymphocytic choriomeningitis virus (LCMV) in rodents (1, 2, 5 11), suggesting a common mechanism influencing T cell responses. The failure to sustain T cell activity is directly associated with the inability to clear the infection, as evidenced by the fact that adoptive transfer of responsive virus-specific T cells can completely eliminate an established persistent infection (12). A relationship between T cell functionality and viral clearance is further supported by the correlation between the strength of the T cell responses and the clearance of HCV infection (7, 13) and the fact that control of HIV infection is associated with increased T cell responsiveness (14). Thus, it is important to develop strategies to boost the host s endogenous T cell responses to control infection. T cell inactivation has been recognized during persistent viral infection; however, whether it is programmed during the initial priming events and thus a predestined, irreversible outcome of infection or if instead the nonresponsive T cells can be reprogrammed and fixed to respond after priming is unknown. In response to an acute antigenic challenge, the initial priming events alone instruct a specific program of expansion, acquisition of effector functions, and memory T cell development (15 21). However, these studies focus on a single antigenic encounter (priming Nonstandard abbreviations used: Arm, Armstrong; Cl, clone; GP 61 80, glycoprotein 61 80; LCMV, lymphocytic choriomeningitis virus. Conflict of interest: The authors have declared that no conflict of interest exists. Citation for this article: J. Clin. Invest. 116: (2006). doi: /jci followed by removal from the antigenic environment) and do not separate these initial events from the later (post-priming) requirement for/effects of continuous instruction that may be important for T cell development and function. Moreover, the impact that repetitive antigenic stimulation (as encountered during chronic infections) has on the developmental program initiated during priming is not clear. Importantly, if T cell function, and specifically inactivation, is programmed during priming, then it is unlikely that therapeutic intervention employed past the priming phase of a persistent infection will rescue cell function. However, if virusspecific T cells remain functionally malleable throughout the course of a persistent infection, then they could serve as targets for therapeutic manipulation. Studies in humans illustrate that therapeutically suppressing viral replication during chronic infection causes a corresponding increase in T cell activity, particularly when therapy is initiated during the acute phase of infection (6, 10, 22 28). The ability to revive T cell responses during persistent viral infections have most thoroughly been analyzed following treatment interruption in HIV-infected patients (29 31), although similar results were observed during treatment of other persistent viral infections. Administration of antiviral therapies during acute HIV infection is associated with increased virus-specific CD8 + T cell responses (in both number and breadth) and a corresponding decrease in viremia (23, 26). However, when treatment was interrupted during the chronic phase of infection, virus was no longer well controlled. Moreover, isolation of CD8 + T cells from HIV-infected patients followed by in vitro culture in the presence of IL-2 renewed their proliferative capacity (5) and ability to produce IFN-γ (32). Thus, these studies suggested that T cell activity could be resurrected if viral replication were subdued. However, such studies, performed in human and nonhuman primates, were unable to determinate whether the resurgent T cell activity observed following therapy actually resulted from (a) the reactivation of antigen-experienced, nonresponsive T cells, (b) de novo activation of naive T cells that The Journal of Clinical Investigation Volume 116 Number 6 June
2 Figure 1 Virus-specific CD4 + and CD8 + T cells lose initially strong activity during the establishment of a persistent viral infection. (A) Spleens were isolated from LCMV Arm (open diamonds) and Cl 13 infected (filled squares) animals and titers of infectious virus determined by plaque assay. Data are expressed as plaque forming units per gram of spleen. The dashed line indicates the lower limit of detection (200 PFU/g spleen). Each time point represents the average ± 1 SD of 3 mice per group. (B and C) LCMV-specific SMARTA (TCR Tg CD4 + T cells) (B) and P14 (TCR Tg CD8 + T cells) cells (C) were cotransferred into mice that were subsequently infected with LCMV Arm or Cl 13. On days 5 (left panels) and 9 (right panels) after infection, splenocytes from individual mice were isolated and the frequency of IFN-γ, TNF-α, and IL-2 producing SMARTA and P14 cells assessed by intracellular cytokine staining. The flow plots are gated on SMARTA (B) and P14 (C) cells, and the values represent the percentage of cytokine-producing cells. The flow plots are representative of 4 independent experiments containing 4 mice per group. had not previously encountered antigen, or (c) the outgrowth and redistribution of a few functionally competent cells that thrive in situations of decreased viral replication. In this study we distinguish between these possibilities and specifically analyze whether the initial priming events specifically direct T cell nonresponsiveness and whether nonresponsive CD4 + and CD8 + T cell function can be restored during persistent infection. To address this issue, we employed LCMV infection in its natural rodent host. Here we demonstrate that T cell function is not programmed during priming but rather is an ongoing and, importantly, alterable process. The priming events during the establishment of a persistent infection are inherently productive and provide the initial instruction for the development of T cell effector and memory responses. As a result, despite prolonged periods of inactivation, CD4 + and CD8 + T cells retain the ability to recover their activity during persistent infection. Significantly, therapeutic reduction of viral loads early during persistent infection preserves CD4 + T cell function in vivo and, as a consequence, has a long-term effect on the control of viral replication. Results CD4 + and CD8 + T cells mount robust responses early during persistent viral infection. We initially analyzed CD4 + and CD8 + T cell responses in an acute, self-limited LCMV infection compared with those in a persistent infection. Before initiating infection, Thy1.1 + TCR transgenic CD4 + T cells (SMARTA cells; specific to the LCMV glycoprotein [LCMV-GP ] peptide presented in the context of I-A b ) and Thy1.1 + TCR transgenic CD8 + T cells (P14 cells; specific to LCMV-GP peptide presented in the context of H-2D b ) were cotransferred into Thy1.2 + C57BL/6 mice. These cotransfers enabled simultaneous visualization of LCMV-specific CD4 + and CD8 + T cell populations and responses separately from endogenous responses and allowed the monitoring of a single population of cells throughout the entire course of infection without contamination from new thymic emigrants. We avoided the problems associated with using large, nonphysiologic numbers of transferred transgenic T cells (33) by cotransferring 1,000 CD4 + and CD8 + T cells. Importantly, each of these transgenic T cell populations behaved similarly to their endogenous (i.e., host-derived) CD8 + and CD4 + T cell counterparts, based on MHC class I and class II tetramer analysis and intracellular cytokine staining (refs. 1 and 2 and data not shown). Two days after cell transfer, mice were infected with LCMV Armstrong (LCMV Arm) or LCMV clone (LCMV Cl) 13. The LCMV variant Cl 13 evolved during a natural infection with Arm (34) and induces immunosuppression due to a single amino acid change in its glycoprotein that enables high-affinity binding to DCs that express α-dystroglycan (35 37). LCMV Cl 13 retains CD4 + and CD8 + T cell epitopes identical to those of LCMV Arm (38) but alters the ability of DCs to activate T cells. As a result, Cl 13 caused a persistent infection lasting approximately days (Figure 1A). In contrast, LCMV Arm-infected minimal numbers 1676 The Journal of Clinical Investigation Volume 116 Number 6 June 2006
3 Figure 2 T cell function is not programmed during priming but is an ongoing process. (A) SMARTA and P14 cells were cotransferred into mice, followed 2 days later by infection with LCMV Arm or Cl 13. Five days after infection, following T cell priming, splenocytes from LCMV Arm or Cl 13 infected mice were isolated and pooled separately. B cells were depleted by positive selection, and the remaining untouched splenocytes were transferred into recipient mice infected in parallel with LCMV Arm or Cl 13 five days earlier but not given SMARTA and P14 cells. T cells from the recipient mice were analyzed at 9 and 40 days after infection. (B and C) Cotransferred SMARTA and P14 cells were primed in LCMV Arm or Cl 13 infected animals for 5 days and then transferred into mice infected in parallel with either LCMV Arm or Cl 13 four (top panels) and 35 (bottom panels) days following transfer of the primed cells (days 9 and 40 after infection, respectively). Splenocytes from each mouse were isolated, and the ability of the cotransferred SMARTA (B) and P14 cells (C) to produce IFN-γ, TNF-α, and IL-2 was analyzed by intracellular flow cytometry. The type of infection in which the cells were primed is indicated underneath each graph. Gray and black bars represent transfer into LCMV Arm and Cl 13 infected recipients, respectively. The bars represent the average ± SD of 4 mice in each group and are representative of 2 4 experiments. Note that the scales on the y axis differ for the cytokines analyzed. *Statistically significant difference (P 0.05) between cells primed in the same environment and then transferred into LCMV Arm or Cl 13 infected animals; **P The Journal of Clinical Investigation Volume 116 Number 6 June
4 Figure 3 Reversal of T cell inactivation during persistent viral infection. (A) SMARTA cells from LCMV Arm (top panels) or Cl 13 infected (bottom panels) mice were isolated 10 days after infection and pooled separately. The numbers in each flow plot indicate the frequency of SMARTA cells on day 10 after LCMV Arm or Cl 13 infection that produced IFN-γ, TNF-α, and IL-2 prior to culture. SMARTA cells isolated on day 10 or 30 after Arm or Cl 13 virus infection were analyzed directly ex vivo or were sorted and cultured for 4 days. The bars in each graph indicate the percentage of IFN-γ, TNF-α, and IL-2 producing SMARTA cells prior to the ex vivo culture and following the 4-day culture. The individual bars indicate the frequency of SMARTA cells during LCMV Cl 13 infection that produce each cytokine represented as a percentage of SMARTA cells that produced the same cytokine during LCMV Arm infection. Each group contained cells pooled (prior to sorting) from 2 3 spleens, and the data are representative of at least 2 repeat experiments. (B) The ability of P14 cells (isolated from the same animals as represented in A) to produce IFN-γ, TNF-α, and IL-2 on day 10 after LCMV Arm or Cl 13 infection is shown in the dot plots, and the graphs illustrate the pre- (gray bars) and post-culture (black bars) levels of cytokine-producing P14 cells from LCMV Cl 13 infected animals represented as a percentage of the P14 response observed during LCMV Arm infection. of DCs and stimulated the generation of a vigorous anti-lcmv T cell response that efficiently eliminated viral infection within 7 12 days (Figure 1A). Cotransfer of the SMARTA and P14 cells did not alter the kinetics of viral infection (data not shown). Five days after Arm or Cl 13 exposure, LCMV-specific CD4 + and CD8 + T cells produced similar cytokine responses (Figure 1, B and C). By day 9, LCMV Arm infection was cleared, and virus-specific CD4 + and CD8 + T cells continued to display effector functions (Figure 1, B and C). In contrast, at 9 days after Cl 13 infection, virus-specific CD4 + T cells made less IFN-γ and negligible amounts of IL-2 or TNF-α (Figure 1B). At the same time, virus-specific CD8 + T cells also lost the ability to produce TNF-α and IL-2 (Figure 1C). Thus, in spite of initially strong responses, T cells rapidly lost function during persistent infection. Functional T cell programming is altered by persistent viral infection. The progressive loss of T cell activity during persistent infection suggested that functional antiviral responses are not preset. To determine how T cells assumed function during an antiviral immune response, we transferred SMARTA and P14 cells into recipient mice that were subsequently infected with LCMV Arm or Cl 13 (Figure 2A). Five days after infection, following priming and the initial expansion (ref. 2 and data not shown), splenocytes were isolated from Arm- or Cl 13 infected animals. To avoid inclusion of antiviral antibodies, which might influence viral replication kinetics, splenocytes were depleted of B cells before transfer into infected recipients. Cell transfer from Arm- or Cl 13 infected animals did not alter the viral titers or clearance kinetics in the recipient mice (data not shown). Splenocytes from these recipients were then isolated on day 9 and day 40 after infection. SMARTA and P14 cells primed during Arm infection and subsequently transferred into Arm-infected animals efficiently produced IFN-γ, TNF-α, and IL-2 at 9 days after infection, whereas cells primed in a Cl 13 infected environment and then transferred into Cl 13 infected mice had a significantly decreased ability to produce these cytokines (Figure 2, B and C). These data illustrate that transfer itself did not alter CD4 + or CD8 + T cell function. However, when SMARTA cells were primed in Arm-infected animals and transferred into Cl 13 infected recipients, a 4-fold decrease in the frequency of IL The Journal of Clinical Investigation Volume 116 Number 6 June 2006
5 Figure 4 Decreased infection of DCs and long-term control of viral replication following early antiviral therapy. (A) Serum viral titers were determined on the indicated days from LCMV Arm or Cl 13 infected mice that were either left untreated or treated on days 1 8 with ribavirin (Rb). Data are expressed as plaque-forming units per milliliter of serum. The dashed line indicates the lower limit of detection (250 PFU/ml serum). Each circle represents a single animal. *Statistically significant difference of P < (B) Splenic DCs, B cells, and macrophages were sorted on day 9 from LCMV Cl 13 infected animals that were either left untreated (gray bars) or treated with ribavirin (black bars). The frequency of cells producing infectious virus in each sorted population was determined by an infectious center assay. Data represent 2 experiments containing pools from 4 mice per group. Tx, treatment. and TNF-α producing cells was observed (Figure 2B), equivalent to the reduced levels observed during Cl 13 infection (Figure 1B). Virus-specific CD8 + T cells primed in Arm-infected animals similarly displayed a 3- and 30-fold decrease, respectively, in IL-2 and TNF-α production following transfer into Cl 13 infected animals (Figure 2C). Of particular interest, SMARTA and P14 cells primed in Cl 13 infected animals resisted inactivation and remained functional upon transfer into Arm-infected recipients (Figure 2, B and C). Similar numbers of SMARTA and P14 cells were observed following transfer into Arm- or Cl 13 infected animals (data not shown), indicating that the functional rescue was not due to selection of a small number of cells that resisted inactivation. Thus, the functional capacity of T cells was determined by the environment into which the cells were placed, rather than where they were primed. These results indicate that priming events during the acute phase of persistent infection were intact and that functional inactivation was not predestined. We next determined when the instructive signals that potentiated T cell memory originated and how long-term generation of that memory was affected by the priming events during persistent infection. Earlier we reported the gradual selection of virus-specific CD4 + T cells that resist initial inactivation during persistent infection (2). In fact, during the chronic phase of Cl 13 infection, virus-specific CD4 + T cell responses are approximately 50 80% of those observed during Arm infection, with a more sustained decrease in TNF-α producing versus IL-2 producing cells. This is in direct opposition to CD8 + T cell responses that remain suppressed throughout infection (1). Accordingly, elevated frequencies of cytokine-producing SMARTA cells were present during the chronic phase of Cl 13 infection, and the frequency of cytokineproducing cells was not dictated by the priming environment (Figure 2B). Moreover, regardless of whether SMARTA cells were primed in an Arm- or Cl 13 infected environment, cells transferred into Arm-infected animals had increased levels of IL-7 receptor and Bcl-2 expression compared with cells transferred into Cl 13 infected animals (Supplemental Figure 1; supplemental material available online with this article; doi: /jci26856ds1), consistent with the development of a memory T cell phenotype (39, 40). In contrast to virus-specific CD4 + T cells, cytokine-producing CD8 + T cells were not selected over time in Cl 13 infected mice (Figure 2C), and despite the initial priming environment, transfer into Cl 13 infected mice resulted in long-term depression of CD8 + T cell responses (Figure 2C). Most importantly, the prolonged functional impairment of virus-specific CD8 + T cells was prevented by early transfer out of the Cl 13 environment (Figure 2C). These data indicate T cell memory development need not be instructed during priming. Restoration of T cell function during persistent infection. The transfer studies indicated that the loss of T cell function was not a preprogrammed event but instead was due to the effects of increased/ prolonged viral replication. To determine whether functionality could be restored to inactivated T cells, populations of purified CD4 + or CD8 + T cells were sorted after Arm or Cl 13 infection and cultured ex vivo. Approximately 2 4% of CD8 + and CD4 + T cells The Journal of Clinical Investigation Volume 116 Number 6 June
6 Figure 5 Therapeutically decreasing viral loads prevents CD4 + T cell inactivation but only minimally preserves CD8 + T cell function. (A and B) The ability of SMARTA (A) and P14 (B) cells from untreated (gray bars) or ribavirin-treated (black bars) animals to produce IFN-γ, TNF-α, and IL-2 was determined on day 9 after infection with either LCMV Arm (left 2 bars in each graph) or Cl 13 (right 2 bars in each graph). The top graphs of each figure represent the frequency of cytokine-producing SMARTA (A) or P14 (B) cells. The bottom graphs of each figure represent the absolute number of SMARTA (A) or P14 (B) cells and the total number of cytokine-producing SMARTA or P14 cells. The bars represent the average ± SD of 4 mice in each group in 3 independent experiments. Note that the scales on the y axis differ for the cytokines analyzed. *Statistically significant increase (P < 0.05) between the untreated and ribavirin-treated animals; **P are infected initially during Cl 13 infection (41), with a small fraction of CD4 + T cells (up to 4%) becoming persistently infected (42, 43). Furthermore, CD4 + T cells do not express MHC class II molecules (data not shown), thereby excluding the potential for LCMV antigen presentation to the virus-specific cells during the culture period. Ten days after Arm infection, a high frequency of virus-specific CD4 + and CD8 + T cells produced effector molecules, whereas the responsiveness of these cells was severely compromised during Cl 13 infection (Figure 3, A and B). After culture, the percentage of TNF-α and IL-2 producing SMARTA cells increased 6-fold, constituting nearly 80% of the optimal response observed during Arm infection (Figure 3A). Similarly, virus-specific CD8 + T cell responses from Cl 13 infected animals recovered completely, i.e., the frequency of IFN-γ, TNF-α, and IL-2 producing cells equaled the levels observed during Arm infection (Figure 3B). Reversal was not caused by proliferation of a small number of TNF-α or IL-2 producing cells, since proliferation did not occur during culture (based on CFSE dilution; data not shown). Moreover, the ratio of SMARTA and P14 cells to endogenous CD4 and CD8 populations, respectively, did not change during the culture period (data not shown), as would be expected if functional virus-specific T cells had grown selectively. To determine whether T cell responsiveness could be restored following extended periods of viral replication, CD4 + and CD8 + T cells were sorted 30 days after Cl 13 or Arm infection. Virusspecific CD4 + T cell responses during the chronic phase of Cl 13 infection are approximately 50 80% of those observed during Arm infection due to a survival advantage of the few cells that initially resist inactivation (2). Consequently, on day 30 after Arm and Cl 13 infection, SMARTA cell responses were only slightly decreased (Figure 3A), and the 4-day culture period only minimally increased the frequency of cells able to produce TNF-α and did not restore 1680 The Journal of Clinical Investigation Volume 116 Number 6 June 2006
7 Figure 6 Decreasing viral replication increases CD4 + T cell stimulation and costimulatory molecule expression by APCs. (A C) On day 9 after infection, splenocytes were isolated from mice infected with LCMV Cl 13 and either left untreated (Cl 13) or treated with ribavirin (Cl 13 + Rb). DCs (A), B cells (B), or macrophages (C) were then sorted and cultured separately with CFSE-labeled naive SMARTA, or P14 cells. No exogenous peptide was added to the cultures. Histograms show gating on SMARTA (left histograms) and P14 (right histograms) cells and illustrate CFSE dilution 3 days after culture. The number in each histogram represents the percentage of cells in each culture that divided. The MFI of the indicated costimulatory molecules on DCs (A), B cells (B), and macrophages (C) from untreated (gray bars) and ribavirin-treated (black bars) Cl 13 infected animals was determined on day 9 after infection. These data represent 2 experiments containing 4 mice per group. PD-L1, programmed death ligand; OX40L, OX40 ligand (CD134); 4-1BBL, 41BB ligand (CD137L); ICOSL, inducible costimulatory molecule ligand. *P < 0.05; **P < IL-2 production (Figure 3A). On the other hand, the percentage of virus-specific CD8 + T cells that produced TNF-α increased 3-fold following the 4-day culture (yet reached only 60% of the response observed during the Arm infection), whereas no increase in the The Journal of Clinical Investigation Volume 116 Number 6 June
8 frequency of IL-2 producing cells was observed (Figure 3B). Again, no proliferation of virus-specific cells was observed in the culture. Thus, we conclude that CD4 + and CD8 + T cells have the potential to regain responsiveness following inactivation; however, functional recovery wanes over extended periods of viral exposure. Prevention of T cell inactivation in vivo. Since T cell activity could be resurrected by removal from the persistently infected environment, we determined whether inactivation could be prevented in vivo by therapeutically decreasing viral titers. To address this issue, Armor Cl 13 infected mice were treated with the antiviral drug ribavirin beginning 1 day after infection. Compared to the viral loads during untreated Cl 13 infection, ribavirin treatment decreased viral titers by 1 log through the priming phase of Cl 13 infection (day 5 after infection) and by 1.5 logs when the infection transitioned into a persistent phase (day 9 after infection; Figure 4A). Accompanying these lower viral titers in Cl 13 infected animals treated with ribavirin was a 50 80% reduction in the percentage of infected DCs (Figure 4B), indicating that the treatment decreased the frequency of infected cells. Other APC populations (B cells and macrophages) showed only a minimal reduction in infection, although less than 0.5% of these cells were productively infected by Cl 13 (Figure 4B). Because early treatment with ribavirin had such a substantial impact on LCMV-specific T cell responses after Cl 13 infection, we next evaluated whether the immunological benefit was retained into the chronic phase of infection. Early treatment with ribavirin (on days 1 8) during Cl 13 infection had sustained antiviral effects, i.e., a 1 log decrease in serum viral titers was observed in ribavirin-treated versus untreated animals through day 28 after infection despite the discontinuation of treatment, and by day 42 infectious virus was undetectable in the treated animals (Figure 4A), indicating that early alterations in viral replication have a long-term impact on viral control. Without ribavirin treatment the frequency and number of TNF-α and IL-2 producing SMARTA and P14 cells decreased significantly during Cl 13 infection (Figure 5, A and B). In comparison, treatment of Cl 13 infected animals with ribavirin stimulated a 3-fold increase in TNF-α and 5-fold increase in IL-2 producing SMARTA cells (Figure 5A). Following ribavirin administration to Cl 13 infected animals, the frequencies of TNF-α and IL-2 producing SMARTA cells were similar to those observed during Arm infection (not significant, P > 0.1; Figure 5A), indicating that early reductions in viral infection prevented CD4 + T cell inactivation. Similar data were obtained with the endogenous (i.e., hostderived) LCMV-GP CD4 + T cell responses (data not shown). Although ribavirin treatment did not significantly increase the absolute number of SMARTA cells during Arm or Cl 13 infection, it did induce a significant 4-fold and 10-fold increase, respectively, in the absolute number of TNF-α and IL-2 producing SMARTA cells (Figure 5A), indicating that the functional recovery following ribavirin treatment is not limited to the maintenance of a small number of cells, but rather a circumvention of the normal process of CD4 + T cell inactivation. In contrast to the preserved CD4 + T cell response, decreasing viral titers during Cl 13 infection only partially prevented CD8 + T cell inactivation. Ribavirin treatment of Cl 13 infected animals did not increase the frequency of TNF-α producing P14 cells, which remained similar to that in untreated Cl 13 infected animals (Figure 5B). However, the frequency of IL-2 producing P14 cells rose a significant 2.5-fold following treatment of Cl 13 infected animals, equal to the levels observed during Arm infection (Figure 5B). Ribavirin treatment of Arm-infected animals had no impact on IFN-γ or IL-2 production by P14 cells, although it did decrease their TNF-α production (Figure 5B), suggesting that decreasing viral titers early during Arm infection may alter the functionality of CD8 + T cell responses. Ribavirin treatment did not significantly impact the absolute number of P14 cells (Figure 5B) or the absolute number of TNF-α producing P14 cells. However, there was a 1.8-fold increase in the absolute number of IL-2 producing P14 cells (P = 0.06; Figure 5B). Administration of ribavirin during the chronic phase of infection (treatment on days 20 27) had no impact on established antiviral CD4 + or CD8 + T cell responses (data not shown), in spite of significantly decreasing viral replication 6-fold ( ± PFU/ml serum in untreated mice versus ± PFU/ml serum in ribavirin-treated mice; P < 0.001). Moreover, there was no apparent change in the level of endogenous T cell responses at this time, suggesting that the induction of naive T cell responses during periods in which virus levels are therapeutically suppressed does not substantially impact the antiviral T cell pool. Overall these data indicate that it may be easier to prevent T cell inactivation during the acute phase of a persistent infection than to restore T cell functions during the chronic phase. Because high levels of antigen presentation are associated with the loss of T cell function (15, 44), we next determined whether the reduction in virus infection following ribavirin treatment decreases T cell stimulation. Three populations of APCs (DCs, B cells, and macrophages) from treated and untreated Cl 13 infected animals were isolated at day 9 after infection and incubated with naive SMARTA or P14 cells. DCs obtained from untreated Cl 13 infected animals induced nearly all the naive P14 cells to proliferate (Figure 6A). Consistent with the decreased levels of DC infection (Figure 4B), DCs from Cl 13 infected animals treated with ribavirin stimulated substantially less CD8 + T cell proliferation (Figure 6A). A decrease in the ability of B cells and macrophages to stimulate CD8 + T cells was also observed in Cl 13 infected animals treated with ribavirin, although these cells were dramatically less efficient than DCs at stimulating CD8 + T cell proliferation (Figure 6, B and C). Interestingly, despite the lower levels of DC infection (Figure 4B), DCs from Cl 13 infected, ribavirin-treated animals induced levels of CD4 + T cell proliferation similar to those induced by DCs from untreated animals (Figure 6A). Although neither B cells nor macrophages served as efficient stimulators of CD4 + T cells during Cl 13 infection (Figure 6, B and C), B cells from Cl 13 infected animals treated with ribavirin acquired the capacity to efficiently stimulate CD4 + T cell responses (Figure 6B). To demonstrate that the observed differences in T cell proliferation resulted from alterations in endogenous presentation/stimulatory capacity by the sorted APCs, not an inherent inability to stimulate T cells, we labeled the APCs with GP (SMARTA) or GP (P14) peptide. By this means the proliferation of approximately 90% of the SMARTA and P14 cells was induced (data not shown). Along with the reduced viral replication after ribavirin treatment, there was a significant increase in the expression of multiple costimulatory molecules on DCs, B cells, and macrophages (Figure 6, A C). Consistent with the newly acquired ability to stimulate T cells following ribavirin treatment, the increased costimulatory molecule expression was most notable on B cells, in which there was an approximately 2-fold increase in the expression of B7-1, B7-2, and CD40 (Figure 6B). Costimulatory molecule expression also increased on macrophages in ribavirin-treated ani The Journal of Clinical Investigation Volume 116 Number 6 June 2006
9 mals, although these cells did not efficiently stimulate naive CD4 + T cell responses (Figure 6C). This increase was not a direct result of the ribavirin per se, since identical treatment of Arm-infected animals did not enhance costimulatory molecule expression (data not shown). Moreover, not all of the costimulatory molecules analyzed were enhanced following ribavirin administration, illustrating the differential regulation/dysregulation of APCs during persistent infection. Discussion Our studies document the highly adaptable nature of T cell functions and show that CD4 + and CD8 + T cell effector and memory development are not hardwired processes but, instead, are continually modulated by signals from the environment. The discovery that T cell responses are alterable led to 4 findings. First, T cell function that is lost during persistent infection can be restored or preserved by either removing the T cells from the antigenic environment or administering antiviral therapy in vivo. Second, functional recovery is more difficult to achieve the longer CD4 + and CD8 + T cells remain in the presence of persistent viral replication. Third, the mechanisms that potentiate CD4 + T cell inactivation apparently differ from those that modulate CD8 + T cell function. That is, by decreasing viral titers in vivo, CD4 + T cell inactivation can be prevented, whereas CD8 + T cells still become largely nonresponsive. Fourth, CD4 + T cell recovery following early antiviral therapy correlates with an increased ability of APCs to costimulate T cells. Importantly, these collective findings provide what we believe to be the first insight into the mechanisms that induce T cell inactivation during persistent viral infection versus those that may maintain it (45). Virus-specific CD4 + and CD8 + T cell responses are initially robust during persistent infection; however, T cells rapidly become nonresponsive in temporal association with the viral transition into persistence. Previous studies have shown that following in vitro priming, functional effector and memory T cell development is observed (15 21). However, these studies focused on the outcome of a single antigenic encounter and did not address the role of extrinsic factors in T cell development or how the developmental program is modulated by repetitive stimulation. We show that unlike expansion and contraction, which are programmed during the initial priming interaction (15 19), CD4 + and CD8 + T cell function is not hardwired but instead can be altered after priming. Functional alterations occur rapidly in response to persisting viral antigens, as virus-specific T cells primed during an acute infection (in a manner that would otherwise yield a functional response) become inactivated 4 days following transfer into an environment with persistent antigen and fail to develop into memory T cells. In contrast, CD4 + and CD8 + T cells primed in an environment with a heavy antigenic burden can recover from the seemingly inevitable inactivation and ultimately develop into memory T cells by transfer into an environment in which the virus is cleared acutely. The ability to rapidly adjust to the antigenic environment (although apparently detrimental in the case of persistent viral infections) explains how different T cell functions can be elicited depending on the type and duration of viral infection. A fundamental problem preventing the eradication of persistent viral infections is the early loss and continued lack of effective T cell responses. During persistent viral infections of humans such as HIV, HCV, and HBV, the administration of antiviral therapy can decrease viral replication and correspondingly enhance T cell responses (6, 10, 22 28). However, it is unclear from these studies whether the increased T cell activity was due to the functional restoration of nonresponsive T cells or to the generation of new effector T cells. To specifically distinguish between these 2 possibilities, we used traceable populations of virus-specific T cells that were present and primed at the time of infection and could be distinguished from new thymic emigrants. Our studies clearly indicate that virus-specific T cells still retain potential functional capacity despite periods of inactivation and, importantly, T cell activity can be fixed in antigen-experienced, nonresponsive T cells during a persistent viral infection. Although the ability to rescue T cell responses wanes over extended periods of inactivation, indicating a progressive imprinting on these cells, components of CD4 + and CD8 + T cell function remain intact and can be restored throughout persistent infection. Our studies suggest that the early administration of therapies that decrease viral titers by as little as 1 log can have a substantial impact on the quality of the ensuing T cell responses, particularly CD4 + T cell activity, even in the face of ongoing levels of viral replication. Importantly, the early decrease in viral infection and enhanced T cell activity facilitated long-term control of viral replication well after the therapies were removed. Thus, we demonstrate that there is an optimal time for therapy during persistent viral infection. Administration of therapy late during the chronic stage of infection may not restore function to inactivated T cells, whereas, in contrast, it had a dramatic effect on sustaining function during the acute phase of infection. This finding is consistent with what is observed during HIV infection, where T cell responses are more readily restorable during the acute rather than the chronic phase of infection (23, 26, 29, 30), and suggests that an intrinsic functional defect likely accumulates in nonresponsive T cells with extended periods of inactivation. It is important to note that although therapy did not restore function during the chronic phase of infection, treatment at this time may still be beneficial when given in conjunction with agents that stimulate naive T cell activation, thereby facilitating productive stimulation of these cells. However, therapies to resurrect T cell activity appear to be most effective when administered early after the establishment of a persistent viral infection. Excessive antigen stimulation has previously been reported to induce T cell nonresponsiveness (15, 44). However, hyperstimulation appears not to play a major role in our studies, since DCs from ribavirin-treated mice retained an ability to stimulate SMARTA cells similar to that of cells from untreated mice, and B cells actually became competent stimulators of naive CD4 + T cells following ribavirin treatment. A contributing cause of CD4 + T cell inactivation may be incorrect or insufficient stimulation by APCs during the effector phase of a Cl 13 virus infection. This is supported by our data showing that ribavirin-treated mice had elevated levels of costimulatory molecules on MHC class II bearing cells. Since the signs of CD4 + T cell inactivation are not overtly manifest at day 5 after Cl 13 infection, our data further suggest that CD4 + T cells may still require costimulation during the effector phase to sustain their function. This is consistent with previous findings showing that prevention of costimulation during the chronic phase of Cl 13 infection diminishes antiviral CD8 + T cell responses and prevents control of viral replication (46). Thus, costimulation by APCs may be required at all phases of infection to sustain productive CD4 + T cell responses and prevent inactivation. However, CD8 + T cell function is not fully restored by an The Journal of Clinical Investigation Volume 116 Number 6 June
10 early decrease in viral titers, indicating that different/additional signals, distinct from those of CD4 + T cells, likely modulate CD8 + T cell inactivation. We are currently determining the precise molecules that sustain T cell responses and the cell population(s) that display them in order to facilitate the development of therapeutics to prevent inactivation and restore antiviral responses to overcome persistent viral infections. Methods Mice. C57BL/6 (H-2 b, Thy1.2 + ) mice were from the Rodent Breeding Colony at The Scripps Research Institute. CD4 / mice were bred from homozygous breeding pairs obtained from Jackson Laboratory. The LCMV-GP specific CD4 + TCR transgenic (SMARTA) mice and LCMV- GP specific CD8 + TCR transgenic (P14) mice have been described previously (47) and were gifts from Hans Hengartner and Rolf Zinkernagel (University Hospital of Zurich, Zurich, Switzerland). All mice were housed under specific pathogen free conditions. Mouse experiments conformed to the requirements of the NIH and were approved by The Scripps Research Institute Animal Research Committee. Virus. In all experiments, 6- to 8-week-old C57BL/6 mice were infected i.v. with PFU of LCMV Arm Cl 53 b or LCMV Cl 13 to generate acute or persistent infection, respectively. Stocks were prepared by a single passage on BHK-21 cells. Viral titers were determined by plaque formation on Vero cells. The frequency of productively infected splenic DCs (CD45 +, CD3, NK1.1, CD11c + ), B cells (CD45 +, CD3, NK1.1, CD11c, CD19 + ), and macrophages (CD45 +, CD3, NK1.1, CD11c, CD11b + ) was determined by sorting the individual population and performing limiting dilution plaque assays (infectious center assays) on Vero cells (48). The cells were sorted using the FACSVantage (BD). Post-sort purities for each population were at least 99%. T cell isolation and adoptive transfers. CD4 + and CD8 + T cells were purified from the spleens of naive SMARTA and P14 mice, respectively, by negative selection (StemCell Technologies), and 10 3 purified cells from each population were cotransferred into C57BL/6 mice i.v. The mice were infected 2 days later with PFU LCMV, i.v. For the transfer experiments to determine the plasticity of functional programming, spleens from Arm- or Cl 13 infected mice that had received SMARTA and P14 cells were harvested. Next, B cells were depleted (>99% removed; data not shown) from the splenocytes by positive selection with CD19 MACS beads (Miltenyi Biotec), and the remaining B cell depleted, untouched (non antibodybound) splenocytes were transferred into mice that had been infected in parallel 5 days earlier with Arm or Cl 13 but that had not initially received SMARTA or P14 cells. The absolute number of SMARTA and P14 cells in the spleen was determined by multiplying the frequency of Thy1.1 + cells (determined flow cytometrically) by the total number of splenocytes. Intracellular cytokine analysis. Total splenocytes were stimulated for 5 hours with 5 μg/ml of the MHC class II restricted LCMV-GP peptide or 2 μg/ml of the MHC class I restricted LCMV-GP peptide (both >99% pure; Synpep Corp.) in the presence of 50 U/ml recombinant murine IL-2 (R&D Systems) and 1 mg/ml brefeldin A (Sigma-Aldrich). The addition of IL-2 to the ex vivo stimulation did not alter cytokine production (data not shown). Flow cytometric analysis was performed using the Digital LSR II (BD). Forward- versus side-scatter profiles were used to define the live population, and gates were set based on antibody isotype controls and cells that stained negative for the protein of interest. T cell culture assays. To determine the restorability of T cell function, total CD4 + or CD8 + T cells were sorted flow cytometrically (>99% purity) from pooled splenocytes of 2 3 animals that had received SMARTA and P14 cells and been infected 10, 30, or 50 days earlier with either LCMV Arm or Cl 13. The sorted T cell populations were individually cultured for 4 days with 200 U/ml recombinant murine IL-2 (R&D Systems). The cells were cultured in complete medium (RPMI 1640 supplemented with 10% fetal bovine serum, 1% Na pyruvate, 10 mm HEPES, 1% nonessential amino acids, and 500 U/ml penicillin and streptomycin). To obtain APCs for the post-culture peptide stimulations, splenocytes from an Arm-infected animal (3 days after infection) were depleted of T cells using Thy1.2 MACS beads (Miltenyi Biotec). APCs were isolated 3 days after infection to allow proper maturation in an inflammatory environment. After the 4-day culture period, the T cells were incubated with the T cell depleted APCs and GP or GP peptide (for the CD4 + or CD8 + T cell stimulations, respectively) for 5 hours, followed by intracellular cytokine analysis. To evaluate the stimulatory capacity of different splenic APC populations, splenic DCs (CD45 +, CD3, NK1.1, CD11c + ), B cells (CD45 +, CD3, NK1.1, CD11c, CD19 + ), and macrophages (CD45 +, CD3, NK1.1, CD11c, CD11b + ) were sorted using the FACSVantage (BD). Post-sort purities for each population were at least 99%. The sorted APC populations were then individually mixed with CFSE-labeled naive SMARTA or P14 cells at a 2:1 ratio. The cells were cultured in complete medium supplemented with 50 μm β-mercaptoethanol for 3 days. Where indicated, the GP or GP peptide was added to the cultures. Ribavirin treatment each of SMARTA and P14 cells were cotransferred into C57BL/6 mice that were infected 2 days later with LCMV. Mice were treated with 100 mg/kg ribavirin (1-b-d-ribofuranosyl-1,2,4- triazole-3-carboxamide; Virazole, ICN Pharmaceuticals Inc.) in PBS. This dose of ribavirin maximizes the efficacy of the drug against LCMV replication, while avoiding toxicity to the host (49). In agreement with our current studies, mice treated with this dose of ribavirin failed to show toxicity. The treatment was administered once daily intraperitoneally on days 1 8 or after LCMV infection. Control mice were injected in parallel with PBS. Ribavirin has previously been shown to lower viral titers in animals persistently infected with LCMV (50) by specifically interfering with viral replication (51). In vivo cytotoxicity assays. Splenocytes from naive syngeneic mice were either left unlabeled or were labeled with 5 mg/ml of the MHC class I restricted peptides GP or NP These target cell populations were then differentially labeled with CFSE (2.5 μg/ml, 1 μg/ml, or 0.2 μg/ml) and transferred i.v. ( cells of each population) into mice previously infected with LCMV. Fifteen hours after transfer, splenocytes were isolated from the recipient mice and analyzed for CFSE expression by flow cytometry. Percent lysis was calculated as [1 (r naive/r sample) 100], in which r represents the ratio of the peptide-unlabeled peak versus the peptide-labeled peak for each sample. Statistics. One-tailed Student s t tests were performed using SigmaStat 2.0 software (Systat Software Inc.) to determine statistical significance (P 0.05). Acknowledgments This is publication number NP from the Viral Immunobiology Laboratory, Department of Molecular and Integrative Neuroscience, The Scripps Research Institute. We thank Dae Young, P. Truong, A. Tishon, and H. Lewicki for technical assistance. This work was supported by NIH grants AI09484 (to M.B.A. Oldstone) and NS (to D.B. McGavern), a Dana Foundation grant (to D.B. McGavern), and NIH training grant AI (to D.G. Brooks). Received for publication September 17, 2005, and accepted in revised form April 4, Address correspondence to: David G. Brooks, North Torrey Pines Road, La Jolla, California 92037, USA. Phone: (858) ; Fax: (858) ; dbrooks@scripps.edu The Journal of Clinical Investigation Volume 116 Number 6 June 2006
11 1. Wherry, E.J., Blattman, J.N., Murali-Krishna, K., van der Most, R., and Ahmed, R Viral persistence alters CD8 T-cell immunodominance and tissue distribution and results in distinct stages of functional impairment. J. Virol. 77: Brooks, D.G., Teyton, L., Oldstone, M.B., and McGavern, D.B Intrinsic functional dysregulation of CD4 T cells occurs rapidly following persistent viral infection. J. Virol. 79: Ciurea, A., Hunziker, L., Klenerman, P., Hengartner, H., and Zinkernagel, R.M Impairment of CD4(+) T cell responses during chronic virus infection prevents neutralizing antibody responses against virus escape mutants. J. Exp. Med. 193: Zajac, A.J., et al Viral immune evasion due to persistence of activated T cells without effector function. J. Exp. Med. 188: Lichterfeld, M., et al Loss of HIV-1-specific CD8+ T cell proliferation after acute HIV-1 infection and restoration by vaccine-induced HIV-1-specific CD4+ T cells. J. Exp. Med. 200: Rosenberg, E.S., et al Vigorous HIV-1-specific CD4+ T cell responses associated with control of viremia. Science. 278: Thimme, R., et al Determinants of viral clearance and persistence during acute hepatitis C virus infection. J. Exp. Med. 194: Reignat, S., et al Escaping high viral load exhaustion: CD8 cells with altered tetramer binding in chronic hepatitis B virus infection. J. Exp. Med. 195: Lechner, F., et al CD8+ T lymphocyte responses are induced during acute hepatitis C virus infection but are not sustained. Eur. J. Immunol. 30: Boni, C., et al Lamivudine treatment can restore T cell responsiveness in chronic hepatitis B. J. Clin. Invest. 102: Cox, A.L., et al Comprehensive analyses of CD8+ T cell responses during longitudinal study of acute human hepatitis C. Hepatology. 42: Volkert, M Studies on immunological tolerance to LCM virus. A preliminary report on adoptive immunization of virus carrier mice. Acta Pathol. Microbiol. Scand. 56: Lechner, F., et al Analysis of successful immune responses in persons infected with hepatitis C virus. J. Exp. Med. 191: McMichael, A HIV vaccines. Annu. Rev. Immunol. 24: Iezzi, G., Karjalainen, K., and Lanzavecchia, A The duration of antigenic stimulation determines the fate of naive and effector T cells. Immunity. 8: Iezzi, G., Scotet, E., Scheidegger, D., and Lanzavecchia, A The interplay between the duration of TCR and cytokine signaling determines T cell polarization. Eur. J. Immunol. 29: Van Stipdonk, M.J., Lemmens, E.E., and Schoenberger, S.P Naive CTLs require a single brief period of antigenic stimulation for clonal expansion and differentiation. Nat. Immunol. 2: Kaech, S.M., and Ahmed, R Memory CD8+ T cell differentiation: initial antigen encounter triggers a developmental program in naive cells. Nat. Immunol. 2: Kaech, S.M., Hemby, S., Kersh, E., and Ahmed, R Molecular and functional profiling of memory CD8 T cell differentiation. Cell. 111: Mercado, R., et al Early programming of T cell populations responding to bacterial infection. J. Immunol. 165: Williams, M.A., and Bevan, M.J Shortening the infectious period does not alter expansion of CD8 T cells but diminishes their capacity to differentiate into memory cells. J. Immunol. 173: Autran, B., et al Positive effects of combined antiretroviral therapy on CD4+ T cell homeostasis and function in advanced HIV disease. Science. 277: Altfeld, M., et al Cellular immune responses and viral diversity in individuals treated during acute and early HIV-1 infection. J. Exp. Med. 193: Kamal, S.M., et al Pegylated interferon alpha therapy in acute hepatitis C: relation to hepatitis C virus-specific T cell response kinetics. Hepatology. 39: Oxenius, A., et al Early highly active antiretroviral therapy for acute HIV-1 infection preserves immune function of CD8+ and CD4+ T lymphocytes. Proc. Natl. Acad. Sci. U. S. A. 97: Rosenberg, E.S., et al Immune control of HIV-1 after early treatment of acute infection. Nature. 407: Lauer, G.M., et al Full-breadth analysis of CD8+ T-cell responses in acute hepatitis C virus infection and early therapy. J. Virol. 79: Barnes, E., et al The dynamics of T-lymphocyte responses during combination therapy for chronic hepatitis C virus infection. Hepatology. 36: Garcia, F., et al The virological and immunological consequences of structured treatment interruptions in chronic HIV-1 infection. Aids. 15:F29 F Ortiz, G.M., et al Structured antiretroviral treatment interruptions in chronically HIV- 1-infected subjects. Proc. Natl. Acad. Sci. U. S. A. 98: Papasavvas, E., et al Enhancement of human immunodeficiency virus type 1-specific CD4 and CD8 T cell responses in chronically infected persons after temporary treatment interruption. J. Infect. Dis. 182: Xiong, Y., et al Simian immunodeficiency virus (SIV) infection of a rhesus macaque induces SIV-specific CD8(+) T cells with a defect in effector function that is reversible on extended interleukin-2 incubation. J. Virol. 75: Marzo, A.L., et al Initial T cell frequency dictates memory CD8+ T cell lineage commitment. Nat. Immunol. 6: Ahmed, R., Salmi, A., Butler, L.D., Chiller, J.M., and Oldstone, M.B Selection of genetic variants of lymphocytic choriomeningitis virus in spleens of persistently infected mice. Role in suppression of cytotoxic T lymphocyte response and viral persistence. J. Exp. Med. 160: Salvato, M., Borrow, P., Shimomaye, E., and Oldstone, M.B Molecular basis of viral persistence: a single amino acid change in the glycoprotein of lymphocytic choriomeningitis virus is associated with suppression of the antiviral cytotoxic T-lymphocyte response and establishment of persistence. J. Virol. 65: Borrow, P., Evans, C.F., and Oldstone, M.B Virus-induced immunosuppression: immune system-mediated destruction of virus-infected dendritic cells results in generalized immune suppression. J. Virol. 69: Sevilla, N., et al Immunosuppression and resultant viral persistence by specific viral targeting of dendritic cells. J. Exp. Med. 192: Fuller, M.J., Khanolkar, A., Tebo, A.E., and Zajac, A.J Maintenance, loss, and resurgence of T cell responses during acute, protracted, and chronic viral infections. J. Immunol. 172: Homann, D., Teyton, L., and Oldstone, M.B Differential regulation of antiviral T-cell immunity results in stable CD8+ but declining CD4+ T-cell memory. Nat. Med. 7: Kaech, S.M., et al Selective expression of the interleukin 7 receptor identifies effector CD8 T cells that give rise to long-lived memory cells. Nat. Immunol. 4: Borrow, P., Tishon, A., and Oldstone, M.B Infection of lymphocytes by a virus that aborts cytotoxic T lymphocyte activity and establishes persistent infection. J. Exp. Med. 174: Ahmed, R., King, C.C., and Oldstone, M.B Virus-lymphocyte interaction: T cells of the helper subset are infected with lymphocytic choriomeningitis virus during persistent infection in vivo. J. Virol. 61: Tishon, A., Southern, P.J., and Oldstone, M.B Virus-lymphocyte interactions. II. Expression of viral sequences during the course of persistent lymphocytic choriomeningitis virus infection and their localization to the L3T4 lymphocyte subset. J. Immunol. 140: Singh, N.J., and Schwartz, R.H The strength of persistent antigenic stimulation modulates adaptive tolerance in peripheral CD4+ T cells. J. Exp. Med. 198: Barber, D.L., et al Restoring function in exhausted CD8 T cells during chronic viral infection. Nature. 439: Williams, M.A., et al Cutting edge: persistent viral infection prevents tolerance induction and escapes immune control following CD28/CD40 blockade-based regimen. J. Immunol. 169: Oxenius, A., Bachmann, M.F., Zinkernagel, R.M., and Hengartner, H Virus-specific MHCclass II-restricted TCR-transgenic mice: effects on humoral and cellular immune responses after viral infection. Eur. J. Immunol. 28: Oldstone, M.B., Salvato, M., Tishon, A., and Lewicki, H Virus-lymphocyte interactions. III. Biologic parameters of a virus variant that fails to generate CTL and establishes persistent infection in immunocompetent hosts. Virology. 164: Von Herrath, M.G., et al Vaccination to treat persistent viral infection. Virology. 268: Berger, D.P., Homann, D., and Oldstone, M.B Defining parameters for successful immunocytotherapy of persistent viral infection. Virology. 266: Gessner, A., and Lother, H Homologous interference of lymphocytic choriomeningitis virus involves a ribavirin-susceptible block in virus replication. J. Virol. 63: The Journal of Clinical Investigation Volume 116 Number 6 June
During acute infections, antigen-specific CD8 T cells are activated
 Progressive Loss of Memory T Cell Potential and Commitment to Exhaustion during Chronic Viral Infection Jill M. Angelosanto, Shawn D. Blackburn, Alison Crawford,* and E. John Wherry Department of Microbiology
Progressive Loss of Memory T Cell Potential and Commitment to Exhaustion during Chronic Viral Infection Jill M. Angelosanto, Shawn D. Blackburn, Alison Crawford,* and E. John Wherry Department of Microbiology
Supporting Online Material for
 www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
Therapeutic PD L1 and LAG 3 blockade rapidly clears established blood stage Plasmodium infection
 Supplementary Information Therapeutic PD L1 and LAG 3 blockade rapidly clears established blood stage Plasmodium infection Noah S. Butler, Jacqueline Moebius, Lecia L. Pewe, Boubacar Traore, Ogobara K.
Supplementary Information Therapeutic PD L1 and LAG 3 blockade rapidly clears established blood stage Plasmodium infection Noah S. Butler, Jacqueline Moebius, Lecia L. Pewe, Boubacar Traore, Ogobara K.
Viral Persistence Alters CD8 T-Cell Immunodominance and Tissue Distribution and Results in Distinct Stages of Functional Impairment
 JOURNAL OF VIROLOGY, Apr. 2003, p. 4911 4927 Vol. 77, No. 8 0022-538X/03/$08.00 0 DOI: 10.1128/JVI.77.8.4911 4927.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Viral Persistence
JOURNAL OF VIROLOGY, Apr. 2003, p. 4911 4927 Vol. 77, No. 8 0022-538X/03/$08.00 0 DOI: 10.1128/JVI.77.8.4911 4927.2003 Copyright 2003, American Society for Microbiology. All Rights Reserved. Viral Persistence
The Adaptive Immune Responses
 The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
The Adaptive Immune Responses The two arms of the immune responses are; 1) the cell mediated, and 2) the humoral responses. In this chapter we will discuss the two responses in detail and we will start
Critical Role for Alpha/Beta and Gamma Interferons in Persistence of Lymphocytic Choriomeningitis Virus by Clonal Exhaustion of Cytotoxic T Cells
 JOURNAL OF VIROLOGY, Sept. 2001, p. 8407 8423 Vol. 75, No. 18 0022-538X/01/$04.00 0 DOI: 10.1128/JVI.75.18.8407 8423.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Critical
JOURNAL OF VIROLOGY, Sept. 2001, p. 8407 8423 Vol. 75, No. 18 0022-538X/01/$04.00 0 DOI: 10.1128/JVI.75.18.8407 8423.2001 Copyright 2001, American Society for Microbiology. All Rights Reserved. Critical
Resolution of a chronic viral infection after interleukin-10 receptor blockade
 ARTICLE Resolution of a chronic viral infection after interleukin-10 receptor blockade Mette Ejrnaes, 1 Christophe M. Filippi, 1 Marianne M. Martinic, 1 Eleanor M. Ling, 1 Lisa M. Togher, 1 Shane Crotty,
ARTICLE Resolution of a chronic viral infection after interleukin-10 receptor blockade Mette Ejrnaes, 1 Christophe M. Filippi, 1 Marianne M. Martinic, 1 Eleanor M. Ling, 1 Lisa M. Togher, 1 Shane Crotty,
SUPPLEMENTARY INFORMATION
 Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Complete but curtailed T-cell response to very-low-affinity antigen Dietmar Zehn, Sarah Y. Lee & Michael J. Bevan Supp. Fig. 1: TCR chain usage among endogenous K b /Ova reactive T cells. C57BL/6 mice
Clearance of viral infections is dependent on functional T-cell
 IL-1 and PD-L1 operate through distinct pathways to suppress T-cell activity during persistent viral infection David G. rooks a,1, Sang-Jun Ha b, Heidi Elsaesser c, Arlene H. Sharpe d, Gordon J. Freeman
IL-1 and PD-L1 operate through distinct pathways to suppress T-cell activity during persistent viral infection David G. rooks a,1, Sang-Jun Ha b, Heidi Elsaesser c, Arlene H. Sharpe d, Gordon J. Freeman
Out-of-sequence signal 3 as a mechanism for virusinduced immune suppression of CD8 T cell responses
 University of Massachusetts Medical School escholarship@umms Open Access Articles Open Access Publications by UMMS Authors 9-25-2014 Out-of-sequence signal 3 as a mechanism for virusinduced immune suppression
University of Massachusetts Medical School escholarship@umms Open Access Articles Open Access Publications by UMMS Authors 9-25-2014 Out-of-sequence signal 3 as a mechanism for virusinduced immune suppression
Lineage relationship and protective immunity of memory CD8 T cell subsets
 23 Nature Publishing Group http://www.nature.com/natureimmunology Lineage relationship and protective immunity of memory CD8 T cell subsets E. John Wherry 1 *,Volker Teichgräber 1 *,Todd C. Becker 1,David
23 Nature Publishing Group http://www.nature.com/natureimmunology Lineage relationship and protective immunity of memory CD8 T cell subsets E. John Wherry 1 *,Volker Teichgräber 1 *,Todd C. Becker 1,David
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Absence of mouse 2B4 promotes NK cell mediated killing of activated CD8 + T cells, leading to prolonged viral persistence and altered pathogenesis
 Research article Absence of mouse 2B4 promotes NK cell mediated killing of activated CD8 + T cells, leading to prolonged viral persistence and altered pathogenesis Stephen N. Waggoner, 1 Ruth T. Taniguchi,
Research article Absence of mouse 2B4 promotes NK cell mediated killing of activated CD8 + T cells, leading to prolonged viral persistence and altered pathogenesis Stephen N. Waggoner, 1 Ruth T. Taniguchi,
Signal 3 requirement for memory CD8 1 T-cell activation is determined by the infectious pathogen
 3176 DOI 1.12/eji.21141537 Eur. J. Immunol. 211. 41: 3176 3186 Signal 3 requirement for memory CD8 1 T-cell activation is determined by the infectious pathogen Selina J. Keppler 1,2 and Peter Aichele 1
3176 DOI 1.12/eji.21141537 Eur. J. Immunol. 211. 41: 3176 3186 Signal 3 requirement for memory CD8 1 T-cell activation is determined by the infectious pathogen Selina J. Keppler 1,2 and Peter Aichele 1
Lecture 11. Immunology and disease: parasite antigenic diversity
 Lecture 11 Immunology and disease: parasite antigenic diversity RNAi interference video and tutorial (you are responsible for this material, so check it out.) http://www.pbs.org/wgbh/nova/sciencenow/3210/02.html
Lecture 11 Immunology and disease: parasite antigenic diversity RNAi interference video and tutorial (you are responsible for this material, so check it out.) http://www.pbs.org/wgbh/nova/sciencenow/3210/02.html
Adoptive immunotherapy induces CNS dendritic cell recruitment and antigen presentation during clearance of a persistent viral infection
 Published Online: 17 July, 2006 Supp Info: http://doi.org/10.1084/jem.20060039 Downloaded from jem.rupress.org on July 27, 2018 ARTICLE Adoptive immunotherapy induces CNS dendritic cell recruitment and
Published Online: 17 July, 2006 Supp Info: http://doi.org/10.1084/jem.20060039 Downloaded from jem.rupress.org on July 27, 2018 ARTICLE Adoptive immunotherapy induces CNS dendritic cell recruitment and
Comparison of Immunoprotection of Simultaneous to Individual Vaccinations in a Murine Model
 MQP-BIO-DSA-8444 Comparison of Immunoprotection of Simultaneous to Individual Vaccinations in a Murine Model A Major Qualifying Project Report Submitted to the Faculty of the WORCESTER POLYTECHNIC INSTITUTE
MQP-BIO-DSA-8444 Comparison of Immunoprotection of Simultaneous to Individual Vaccinations in a Murine Model A Major Qualifying Project Report Submitted to the Faculty of the WORCESTER POLYTECHNIC INSTITUTE
Supplemental Table I.
 Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Control of Virus-Specific CD8 T-Cell Exhaustion and Immune-Mediated Pathology by E3 Ubiquitin Ligase Cbl-b during Chronic Viral Infection
 JOURNAL OF VIROLOGY, Apr. 2008, p. 3353 3368 Vol. 82, No. 7 0022-538X/08/$08.00 0 doi:10.1128/jvi.01350-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Control of Virus-Specific
JOURNAL OF VIROLOGY, Apr. 2008, p. 3353 3368 Vol. 82, No. 7 0022-538X/08/$08.00 0 doi:10.1128/jvi.01350-07 Copyright 2008, American Society for Microbiology. All Rights Reserved. Control of Virus-Specific
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA
 AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
AD Award Number: DAMD17-01-1-0085 TITLE: MODULATION OF T CELL TOLERANCE IN A MURINE MODEL FOR IMMUNOTHERAPY OF PROSTATIC ADENOCARCINOMA PRINCIPAL INVESTIGATOR: ARTHUR A HURWITZ, Ph.d. CONTRACTING ORGANIZATION:
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
RAISON D ETRE OF THE IMMUNE SYSTEM:
 RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Acquired Immunity Innate immunity: (Antigen nonspecific) defense
Recombinant adeno-associated virus vectors induce functionally impaired transgene product specific CD8 + T cells in mice
 Recombinant adeno-associated virus vectors induce functionally impaired transgene product specific CD8 + T cells in mice Shih-Wen Lin,, Marcio O. Lasaro, Hildegund C.J. Ertl J Clin Invest. 2007;117(12):3958-3970.
Recombinant adeno-associated virus vectors induce functionally impaired transgene product specific CD8 + T cells in mice Shih-Wen Lin,, Marcio O. Lasaro, Hildegund C.J. Ertl J Clin Invest. 2007;117(12):3958-3970.
NK cell flow cytometric assay In vivo DC viability and migration assay
 NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
Shenghua Zhou, Rong Ou, Lei Huang, and Demetrius Moskophidis*
 JOURNAL OF VIROLOGY, Jan. 2002, p. 829 840 Vol. 76, No. 2 0022-538X/02/$04.00 0 DOI: 10.1128/JVI.76.2.829 840.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved. Critical Role
JOURNAL OF VIROLOGY, Jan. 2002, p. 829 840 Vol. 76, No. 2 0022-538X/02/$04.00 0 DOI: 10.1128/JVI.76.2.829 840.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved. Critical Role
NKTR-255: Accessing The Immunotherapeutic Potential Of IL-15 for NK Cell Therapies
 NKTR-255: Accessing The Immunotherapeutic Potential Of IL-15 for NK Cell Therapies Saul Kivimäe Senior Scientist, Research Biology Nektar Therapeutics NK Cell-Based Cancer Immunotherapy, September 26-27,
NKTR-255: Accessing The Immunotherapeutic Potential Of IL-15 for NK Cell Therapies Saul Kivimäe Senior Scientist, Research Biology Nektar Therapeutics NK Cell-Based Cancer Immunotherapy, September 26-27,
Micro 204. Cytotoxic T Lymphocytes (CTL) Lewis Lanier
 Micro 204 Cytotoxic T Lymphocytes (CTL) Lewis Lanier Lewis.Lanier@ucsf.edu Lymphocyte-mediated Cytotoxicity CD8 + αβ-tcr + T cells CD4 + αβ-tcr + T cells γδ-tcr + T cells Natural Killer cells CD8 + αβ-tcr
Micro 204 Cytotoxic T Lymphocytes (CTL) Lewis Lanier Lewis.Lanier@ucsf.edu Lymphocyte-mediated Cytotoxicity CD8 + αβ-tcr + T cells CD4 + αβ-tcr + T cells γδ-tcr + T cells Natural Killer cells CD8 + αβ-tcr
Supplementary Figure 1. Enhanced detection of CTLA-4 on the surface of HIV-specific
 SUPPLEMENTARY FIGURE LEGEND Supplementary Figure 1. Enhanced detection of CTLA-4 on the surface of HIV-specific CD4 + T cells correlates with intracellular CTLA-4 levels. (a) Comparative CTLA-4 levels
SUPPLEMENTARY FIGURE LEGEND Supplementary Figure 1. Enhanced detection of CTLA-4 on the surface of HIV-specific CD4 + T cells correlates with intracellular CTLA-4 levels. (a) Comparative CTLA-4 levels
Determinants of Immunogenicity and Tolerance. Abul K. Abbas, MD Department of Pathology University of California San Francisco
 Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
Determinants of Immunogenicity and Tolerance Abul K. Abbas, MD Department of Pathology University of California San Francisco EIP Symposium Feb 2016 Why do some people respond to therapeutic proteins?
T Cell Activation, Costimulation and Regulation
 1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
1 T Cell Activation, Costimulation and Regulation Abul K. Abbas, MD University of California San Francisco 2 Lecture outline T cell antigen recognition and activation Costimulation, the B7:CD28 family
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS. Choompone Sakonwasun, MD (Hons), FRCPT
 ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
ACTIVATION AND EFFECTOR FUNCTIONS OF CELL-MEDIATED IMMUNITY AND NK CELLS Choompone Sakonwasun, MD (Hons), FRCPT Types of Adaptive Immunity Types of T Cell-mediated Immune Reactions CTLs = cytotoxic T lymphocytes
Brief Definitive Report
 Published Online: 1 May, 1988 Supp Info: http://doi.org/10.1084/jem.167.5.1749 Downloaded from jem.rupress.org on January 6, 2019 Brief Definitive Report VIRUS-TRIGGERED IMMUNE SUPPRESSION IN MICE CAUSED
Published Online: 1 May, 1988 Supp Info: http://doi.org/10.1084/jem.167.5.1749 Downloaded from jem.rupress.org on January 6, 2019 Brief Definitive Report VIRUS-TRIGGERED IMMUNE SUPPRESSION IN MICE CAUSED
Supplementary Figures
 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Scott Abrams, Ph.D. Professor of Oncology, x4375 Kuby Immunology SEVENTH EDITION
 Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 13 Effector Responses: Cell- and Antibody-Mediated Immunity Copyright 2013 by W. H.
Adaptive immune responses: T cell-mediated immunity
 MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
MICR2209 Adaptive immune responses: T cell-mediated immunity Dr Allison Imrie allison.imrie@uwa.edu.au 1 Synopsis: In this lecture we will discuss the T-cell mediated immune response, how it is activated,
Naive and memory CD8 T cell responses after antigen stimulation in vivo
 University of Iowa Iowa Research Online Theses and Dissertations Summer 2011 Naive and memory CD8 T cell responses after antigen stimulation in vivo Matthew David Martin University of Iowa Copyright 2011
University of Iowa Iowa Research Online Theses and Dissertations Summer 2011 Naive and memory CD8 T cell responses after antigen stimulation in vivo Matthew David Martin University of Iowa Copyright 2011
Supporting Information
 Supporting Information lpek et al. 1.173/pnas.1121217 SI Materials and Methods Mice. cell knockout, inos / (Taconic arms), Rag1 /, INγR /, and IL-12p4 / mice (The Jackson Laboratory) were maintained and/or
Supporting Information lpek et al. 1.173/pnas.1121217 SI Materials and Methods Mice. cell knockout, inos / (Taconic arms), Rag1 /, INγR /, and IL-12p4 / mice (The Jackson Laboratory) were maintained and/or
and Nucleic Acid-Sensing TLR Pathways in Controlling a Chronic Viral Infection
 This information is current as of November 2, 2018. Supplementary Material References Subscription Permissions Email Alerts Differential Roles for RIG-I like Receptors and Nucleic Acid-Sensing TLR Pathways
This information is current as of November 2, 2018. Supplementary Material References Subscription Permissions Email Alerts Differential Roles for RIG-I like Receptors and Nucleic Acid-Sensing TLR Pathways
NK1.1 þ CD8 þ T cells escape TGF-b control and contribute to early microbial pathogen response
 Received 24 Apr 214 Accepted 5 Sep 214 Published 6 Oct 214 DOI: 1.138/ncomms615 NK1.1 þ CD8 þ T cells escape TGF-b control and contribute to early microbial pathogen response Anne L. Ruiz 1,2,3,4, Saidi
Received 24 Apr 214 Accepted 5 Sep 214 Published 6 Oct 214 DOI: 1.138/ncomms615 NK1.1 þ CD8 þ T cells escape TGF-b control and contribute to early microbial pathogen response Anne L. Ruiz 1,2,3,4, Saidi
Supplementary Figures
 Supplementary Figures Supplementary Figure 1. NKT ligand-loaded tumour antigen-presenting B cell- and monocyte-based vaccine induces NKT, NK and CD8 T cell responses. (A) The cytokine profiles of liver
Supplementary Figures Supplementary Figure 1. NKT ligand-loaded tumour antigen-presenting B cell- and monocyte-based vaccine induces NKT, NK and CD8 T cell responses. (A) The cytokine profiles of liver
Recombinant adeno-associated virus vectors induce functionally impaired transgene product specific CD8 + T cells in mice
 Research article Recombinant adeno-associated virus vectors induce functionally impaired transgene product specific CD8 + T cells in mice Shih-Wen Lin, 1,2 Scott E. Hensley, 1,2 Nia Tatsis, 2 Marcio O.
Research article Recombinant adeno-associated virus vectors induce functionally impaired transgene product specific CD8 + T cells in mice Shih-Wen Lin, 1,2 Scott E. Hensley, 1,2 Nia Tatsis, 2 Marcio O.
Scott Abrams, Ph.D. Professor of Oncology, x4375 Kuby Immunology SEVENTH EDITION
 Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 11 T-Cell Activation, Differentiation, and Memory Copyright 2013 by W. H. Freeman and
Scott Abrams, Ph.D. Professor of Oncology, x4375 scott.abrams@roswellpark.org Kuby Immunology SEVENTH EDITION CHAPTER 11 T-Cell Activation, Differentiation, and Memory Copyright 2013 by W. H. Freeman and
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Canberra, Australia). CD11c-DTR-OVA-GFP (B6.CD11c-OVA), B6.luc + and. Cancer Research Center, Germany). B6 or BALB/c.FoxP3-DTR-GFP mice were
 Supplemental Materials and Methods Mice Female C57BL/6 (B6, I-E null, H-2 b ), BALB/c (H-2 d ) + ), FVB/N (H-2 q, I-E null, CD45.1 + ), and B6D2F1 (H-2 b/d ) mice were purchased from the Animal Resources
Supplemental Materials and Methods Mice Female C57BL/6 (B6, I-E null, H-2 b ), BALB/c (H-2 d ) + ), FVB/N (H-2 q, I-E null, CD45.1 + ), and B6D2F1 (H-2 b/d ) mice were purchased from the Animal Resources
Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to
 Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Class II tetramer staining Commercially available HLA Class II tetramers (Beckman Coulter) conjugated to PE were combined with dominant HIV epitopes (DRB1*0101-DRFYKTLRAEQASQEV, DRB1*0301- PEKEVLVWKFDSRLAFHH,
Supplemental Materials for. Effects of sphingosine-1-phosphate receptor 1 phosphorylation in response to. FTY720 during neuroinflammation
 Supplemental Materials for Effects of sphingosine-1-phosphate receptor 1 phosphorylation in response to FTY7 during neuroinflammation This file includes: Supplemental Table 1. EAE clinical parameters of
Supplemental Materials for Effects of sphingosine-1-phosphate receptor 1 phosphorylation in response to FTY7 during neuroinflammation This file includes: Supplemental Table 1. EAE clinical parameters of
RAISON D ETRE OF THE IMMUNE SYSTEM:
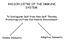 RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Adaptive Immunity Innate immunity: (Antigen - nonspecific) defense
RAISON D ETRE OF THE IMMUNE SYSTEM: To Distinguish Self from Non-Self Thereby Protecting Us From Our Hostile Environment. Innate Immunity Adaptive Immunity Innate immunity: (Antigen - nonspecific) defense
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
T Lymphocyte Activation and Costimulation. FOCiS. Lecture outline
 1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
1 T Lymphocyte Activation and Costimulation Abul K. Abbas, MD UCSF FOCiS 2 Lecture outline T cell activation Costimulation, the B7:CD28 family Inhibitory receptors of T cells Targeting costimulators for
Pathogenic virus-specific T cells cause disease during treatment with the calcineurin inhibitor FK506: implications for transplantation
 Pathogenic virus-specific T cells cause disease during treatment with the calcineurin inhibitor FK506: implications for transplantation Koichi Araki, Emory University Shivaprakash Gangappa, Emory University
Pathogenic virus-specific T cells cause disease during treatment with the calcineurin inhibitor FK506: implications for transplantation Koichi Araki, Emory University Shivaprakash Gangappa, Emory University
Immune Tolerance. Kyeong Cheon Jung. Department of Pathology Seoul National University College of Medicine
 Immune Tolerance Kyeong Cheon Jung Department of Pathology Seoul National University College of Medicine Immune tolerance Unresponsiveness to an antigen that is induced by previous exposure to that antigen
Immune Tolerance Kyeong Cheon Jung Department of Pathology Seoul National University College of Medicine Immune tolerance Unresponsiveness to an antigen that is induced by previous exposure to that antigen
Shiv Pillai Ragon Institute, Massachusetts General Hospital Harvard Medical School
 CTLs, Natural Killers and NKTs 1 Shiv Pillai Ragon Institute, Massachusetts General Hospital Harvard Medical School CTL inducing tumor apoptosis 3 Lecture outline CD8 + Cytotoxic T lymphocytes (CTL) Activation/differentiation
CTLs, Natural Killers and NKTs 1 Shiv Pillai Ragon Institute, Massachusetts General Hospital Harvard Medical School CTL inducing tumor apoptosis 3 Lecture outline CD8 + Cytotoxic T lymphocytes (CTL) Activation/differentiation
NIH Public Access Author Manuscript Nature. Author manuscript; available in PMC 2009 July 28.
 NIH Public Access Author Manuscript Published in final edited form as: Nature. 2009 January 29; 457(7229): 557 561. doi:10.1038/nature07665. Adaptive Immune Features of Natural Killer Cells Joseph C. Sun,
NIH Public Access Author Manuscript Published in final edited form as: Nature. 2009 January 29; 457(7229): 557 561. doi:10.1038/nature07665. Adaptive Immune Features of Natural Killer Cells Joseph C. Sun,
Narrowed TCR repertoire and viral escape as a consequence of heterologous immunity
 Research article Narrowed TCR repertoire and viral escape as a consequence of heterologous immunity Markus Cornberg, 1,2 Alex T. Chen, 1 Lee A. Wilkinson, 1 Michael A. Brehm, 1 Sung-Kwon Kim, 1 Claudia
Research article Narrowed TCR repertoire and viral escape as a consequence of heterologous immunity Markus Cornberg, 1,2 Alex T. Chen, 1 Lee A. Wilkinson, 1 Michael A. Brehm, 1 Sung-Kwon Kim, 1 Claudia
There are 2 major lines of defense: Non-specific (Innate Immunity) and. Specific. (Adaptive Immunity) Photo of macrophage cell
 There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
There are 2 major lines of defense: Non-specific (Innate Immunity) and Specific (Adaptive Immunity) Photo of macrophage cell Development of the Immune System ery pl neu mφ nk CD8 + CTL CD4 + thy TH1 mye
TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer
 AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
AD Award Number: W8-XWH-5-- TITLE: Development of Antigen Presenting Cells for adoptive immunotherapy in prostate cancer PRINCIPAL INVESTIGATOR: Mathias Oelke, Ph.D. CONTRACTING ORGANIZATION: Johns Hopkins
Nature Immunology: doi: /ni Supplementary Figure 1. Gene expression profile of CD4 + T cells and CTL responses in Bcl6-deficient mice.
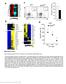 Supplementary Figure 1 Gene expression profile of CD4 + T cells and CTL responses in Bcl6-deficient mice. (a) Gene expression profile in the resting CD4 + T cells were analyzed by an Affymetrix microarray
Supplementary Figure 1 Gene expression profile of CD4 + T cells and CTL responses in Bcl6-deficient mice. (a) Gene expression profile in the resting CD4 + T cells were analyzed by an Affymetrix microarray
TCR, MHC and coreceptors
 Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
Cooperation In Immune Responses Antigen processing how peptides get into MHC Antigen processing involves the intracellular proteolytic generation of MHC binding proteins Protein antigens may be processed
IOM Immunization Safety Review 11/12/2001. Immunological Competition and the Infant Immune Response to Vaccines
 IOM Immunization Safety Review 11/12/2001 Immunological Competition and the Infant Immune Response to Vaccines Richard Insel University of Rochester Goals Neonatal and Infant Immune System Broad Effects
IOM Immunization Safety Review 11/12/2001 Immunological Competition and the Infant Immune Response to Vaccines Richard Insel University of Rochester Goals Neonatal and Infant Immune System Broad Effects
Immune Checkpoints. PD Dr med. Alessandra Curioni-Fontecedro Department of Hematology and Oncology Cancer Center Zurich University Hospital Zurich
 Immune Checkpoints PD Dr med. Alessandra Curioni-Fontecedro Department of Hematology and Oncology Cancer Center Zurich University Hospital Zurich Activation of T cells requires co-stimulation Science 3
Immune Checkpoints PD Dr med. Alessandra Curioni-Fontecedro Department of Hematology and Oncology Cancer Center Zurich University Hospital Zurich Activation of T cells requires co-stimulation Science 3
NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity
 NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity Peiwen Kuo Scientist, Research Biology Nektar Therapeutics August 31 st, 2018 Emerging
NKTR-255: Accessing IL-15 Therapeutic Potential through Robust and Sustained Engagement of Innate and Adaptive Immunity Peiwen Kuo Scientist, Research Biology Nektar Therapeutics August 31 st, 2018 Emerging
Supporting Information
 Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Eosinophils are required. for the maintenance of plasma cells in the bone marrow
 Eosinophils are required for the maintenance of plasma cells in the bone marrow Van Trung Chu, Anja Fröhlich, Gudrun Steinhauser, Tobias Scheel, Toralf Roch, Simon Fillatreau, James J. Lee, Max Löhning
Eosinophils are required for the maintenance of plasma cells in the bone marrow Van Trung Chu, Anja Fröhlich, Gudrun Steinhauser, Tobias Scheel, Toralf Roch, Simon Fillatreau, James J. Lee, Max Löhning
Supplemental Figure 1
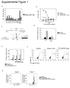 Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
Memory CD4 T Cells Enhance Primary CD8 T-Cell Responses
 INFECTION AND IMMUNITY, July 2007, p. 3556 3560 Vol. 75, No. 7 0019-9567/07/$08.00 0 doi:10.1128/iai.00086-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Memory CD4 T Cells
INFECTION AND IMMUNITY, July 2007, p. 3556 3560 Vol. 75, No. 7 0019-9567/07/$08.00 0 doi:10.1128/iai.00086-07 Copyright 2007, American Society for Microbiology. All Rights Reserved. Memory CD4 T Cells
FOCiS. Lecture outline. The immunological equilibrium: balancing lymphocyte activation and control. Immunological tolerance and immune regulation -- 1
 1 Immunological tolerance and immune regulation -- 1 Abul K. Abbas UCSF FOCiS 2 Lecture outline Principles of immune regulation Self-tolerance; mechanisms of central and peripheral tolerance Inhibitory
1 Immunological tolerance and immune regulation -- 1 Abul K. Abbas UCSF FOCiS 2 Lecture outline Principles of immune regulation Self-tolerance; mechanisms of central and peripheral tolerance Inhibitory
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases. Abul K. Abbas UCSF
 Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Tolerance, autoimmunity and the pathogenesis of immunemediated inflammatory diseases Abul K. Abbas UCSF Balancing lymphocyte activation and control Activation Effector T cells Tolerance Regulatory T cells
Examples of questions for Cellular Immunology/Cellular Biology and Immunology
 Examples of questions for Cellular Immunology/Cellular Biology and Immunology Each student gets a set of 6 questions, so that each set contains different types of questions and that the set of questions
Examples of questions for Cellular Immunology/Cellular Biology and Immunology Each student gets a set of 6 questions, so that each set contains different types of questions and that the set of questions
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
T-cell activation T cells migrate to secondary lymphoid tissues where they interact with antigen, antigen-presenting cells, and other lymphocytes:
 Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Interactions between innate immunity & adaptive immunity What happens to T cells after they leave the thymus? Naïve T cells exit the thymus and enter the bloodstream. If they remain in the bloodstream,
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured
 Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
Nature Medicine: doi: /nm.2109
 HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity
 Cell Reports Supplemental Information L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity Rebar N. Mohammed, H. Angharad Watson, Miriam Vigar,
Cell Reports Supplemental Information L-selectin Is Essential for Delivery of Activated CD8 + T Cells to Virus-Infected Organs for Protective Immunity Rebar N. Mohammed, H. Angharad Watson, Miriam Vigar,
Cytotoxicity assays. Rory D. de Vries, PhD 1. Viroscience lab, Erasmus MC, Rotterdam, the Netherlands
 Cytotoxicity assays Rory D. de Vries, PhD 1 1 Viroscience lab, Erasmus MC, Rotterdam, the Netherlands Anti-influenza immunity Humoral / CD4+ / CD8+ / NK? Function of CTL Elimination of virus-infected cells?
Cytotoxicity assays Rory D. de Vries, PhD 1 1 Viroscience lab, Erasmus MC, Rotterdam, the Netherlands Anti-influenza immunity Humoral / CD4+ / CD8+ / NK? Function of CTL Elimination of virus-infected cells?
Recombinant Vaccinia Virus-Induced T-Cell Immunity: Quantitation of the Response to the Virus Vector and the Foreign Epitope
 JOURNAL OF VIROLOGY, Apr. 2002, p. 3329 3337 Vol. 76, No. 7 0022-538X/02/$04.00 0 DOI: 10.1128/JVI.76.7.3329 3337.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved. Recombinant
JOURNAL OF VIROLOGY, Apr. 2002, p. 3329 3337 Vol. 76, No. 7 0022-538X/02/$04.00 0 DOI: 10.1128/JVI.76.7.3329 3337.2002 Copyright 2002, American Society for Microbiology. All Rights Reserved. Recombinant
Medical Virology Immunology. Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University
 Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
Medical Virology Immunology Dr. Sameer Naji, MB, BCh, PhD (UK) Head of Basic Medical Sciences Dept. Faculty of Medicine The Hashemite University Human blood cells Phases of immune responses Microbe Naïve
La risposta immune all infezione da virus ebola. Chiara Agrati, PhD
 La risposta immune all infezione da virus ebola Chiara Agrati, PhD Pathogenetic mechanisms This virus infection is able to: - disable the immune system, preventing an effective protective immune response
La risposta immune all infezione da virus ebola Chiara Agrati, PhD Pathogenetic mechanisms This virus infection is able to: - disable the immune system, preventing an effective protective immune response
Antigen Presentation and T Lymphocyte Activation. Abul K. Abbas UCSF. FOCiS
 1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
1 Antigen Presentation and T Lymphocyte Activation Abul K. Abbas UCSF FOCiS 2 Lecture outline Dendritic cells and antigen presentation The role of the MHC T cell activation Costimulation, the B7:CD28 family
Supplemental Information. CD4 + CD25 + Foxp3 + Regulatory T Cells Promote. Th17 Cells In Vitro and Enhance Host Resistance
 Immunity, Volume 34 Supplemental Information D4 + D25 + + Regulatory T ells Promote Th17 ells In Vitro and Enhance Host Resistance in Mouse andida albicans Th17 ell Infection Model Pushpa Pandiyan, Heather
Immunity, Volume 34 Supplemental Information D4 + D25 + + Regulatory T ells Promote Th17 ells In Vitro and Enhance Host Resistance in Mouse andida albicans Th17 ell Infection Model Pushpa Pandiyan, Heather
Supplementary Information. A vital role for IL-2 trans-presentation in DC-mediated T cell activation in humans as revealed by daclizumab therapy
 Supplementary Information A vital role for IL-2 trans-presentation in DC-mediated T cell activation in humans as revealed by daclizumab therapy Simone C. Wuest 1, Jehad Edwan 1, Jayne F. Martin 1, Sungpil
Supplementary Information A vital role for IL-2 trans-presentation in DC-mediated T cell activation in humans as revealed by daclizumab therapy Simone C. Wuest 1, Jehad Edwan 1, Jayne F. Martin 1, Sungpil
IMMUNOLOGICAL MEMORY. CD4 T Follicular Helper Cells. Memory CD8 T Cell Differentiation
 IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
IMMUNOLOGICAL MEMORY CD4 T Follicular Helper Cells Memory CD8 T Cell Differentiation CD4 T Cell Differentiation Bcl-6 T-bet GATA-3 ROR t Foxp3 CD4 T follicular helper (Tfh) cells FUNCTION Provide essential
Chapter 7 Conclusions
 VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
VII-1 Chapter 7 Conclusions VII-2 The development of cell-based therapies ranging from well-established practices such as bone marrow transplant to next-generation strategies such as adoptive T-cell therapy
CD8 + T-cell function and lead to significant lowering of. 1 B.M.S. and S.F.E. contributed equally to this work.
 Point mutation in the glycoprotein of lymphocytic choriomeningitis virus is necessary for receptor binding, dendritic cell infection, and long-term persistence Brian M. Sullivan a,1, Sébastien F. Emonet
Point mutation in the glycoprotein of lymphocytic choriomeningitis virus is necessary for receptor binding, dendritic cell infection, and long-term persistence Brian M. Sullivan a,1, Sébastien F. Emonet
Therapeutic Immunization with Autologous DC Pulsed with Autologous Inactivated HIV-1 Infected Apoptotic Cells
 Therapeutic Immunization with Autologous DC Pulsed with Autologous Inactivated HIV-1 Infected Apoptotic Cells Sharon A. Riddler, MD, MPH University of Pittsburgh May 2008 Slide 1 HIV and DC Vaccines During
Therapeutic Immunization with Autologous DC Pulsed with Autologous Inactivated HIV-1 Infected Apoptotic Cells Sharon A. Riddler, MD, MPH University of Pittsburgh May 2008 Slide 1 HIV and DC Vaccines During
Intron A Hepatitis B. Intron A (interferon alfa-2b) Description
 Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
Federal Employee Program 1310 G Street, N.W. Washington, D.C. 20005 202.942.1000 Fax 202.942.1125 5.01.01 Subject: Intron A Hepatitis B Page: 1 of 7 Last Review Date: November 30, 2018 Intron A Hepatitis
Washington University School of Medicine, St Louis. MO Division of Infectious
 JVI Accepts, published online ahead of print on 27 June 2012 J. Virol. doi:10.1128/jvi.00673-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 CD8 + T cells use TRAIL to restrict
JVI Accepts, published online ahead of print on 27 June 2012 J. Virol. doi:10.1128/jvi.00673-12 Copyright 2012, American Society for Microbiology. All Rights Reserved. 1 2 CD8 + T cells use TRAIL to restrict
CD4 + T cells recovered in Rag2 / recipient ( 10 5 ) Heart Lung Pancreas
 a CD4 + T cells recovered in Rag2 / recipient ( 1 5 ) Heart Lung Pancreas.5 1 2 4 6 2 4 6 Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas b Heart Lung Pancreas Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas
a CD4 + T cells recovered in Rag2 / recipient ( 1 5 ) Heart Lung Pancreas.5 1 2 4 6 2 4 6 Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas b Heart Lung Pancreas Ctla4 +/+ Ctla4 / Ctla4 / Lung Ctla4 / Pancreas
Immune Regulation and Tolerance
 Immune Regulation and Tolerance Immunoregulation: A balance between activation and suppression of effector cells to achieve an efficient immune response without damaging the host. Activation (immunity)
Immune Regulation and Tolerance Immunoregulation: A balance between activation and suppression of effector cells to achieve an efficient immune response without damaging the host. Activation (immunity)
Therapeutic efficacy of MUC1- specific CTL and CD137 costimulation. mammary cancer model. Pinku Mukherjee & Sandra Gendler
 Therapeutic efficacy of MUC1- specific CTL and CD137 costimulation in a spontaneous mammary cancer model Pinku Mukherjee & Sandra Gendler Goal of Immunotherapy Boosting the low level anti-tumor immune
Therapeutic efficacy of MUC1- specific CTL and CD137 costimulation in a spontaneous mammary cancer model Pinku Mukherjee & Sandra Gendler Goal of Immunotherapy Boosting the low level anti-tumor immune
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs
 Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
TNF-α is critical for antitumor but not antiviral T cell immunity in mice
 Research article TNF-α is critical for antitumor but not antiviral T cell immunity in mice Thomas Calzascia, Marc Pellegrini, Håkan Hall, Laurent Sabbagh, Nobuyuki Ono, Alisha R. Elford, Tak W. Mak, and
Research article TNF-α is critical for antitumor but not antiviral T cell immunity in mice Thomas Calzascia, Marc Pellegrini, Håkan Hall, Laurent Sabbagh, Nobuyuki Ono, Alisha R. Elford, Tak W. Mak, and
Manuscript: OX40 signaling is involved in the autoactivation of CD4 + CD28 - T cells and contributes to pathogenesis of autoimmune arthritis
 Manuscript: OX40 signaling is involved in the autoactivation of CD4 + CD28 - T cells and contributes to pathogenesis of autoimmune arthritis Vincent Laufer Rheumatology JC October 17 Disclosures NIH 2
Manuscript: OX40 signaling is involved in the autoactivation of CD4 + CD28 - T cells and contributes to pathogenesis of autoimmune arthritis Vincent Laufer Rheumatology JC October 17 Disclosures NIH 2
Darwinian selection and Newtonian physics wrapped up in systems biology
 Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Darwinian selection and Newtonian physics wrapped up in systems biology Concept published in 1957* by Macfarland Burnet (1960 Nobel Laureate for the theory of induced immune tolerance, leading to solid
Supplementary Information. Tissue-wide immunity against Leishmania. through collective production of nitric oxide
 Supplementary Information Tissue-wide immunity against Leishmania through collective production of nitric oxide Romain Olekhnovitch, Bernhard Ryffel, Andreas J. Müller and Philippe Bousso Supplementary
Supplementary Information Tissue-wide immunity against Leishmania through collective production of nitric oxide Romain Olekhnovitch, Bernhard Ryffel, Andreas J. Müller and Philippe Bousso Supplementary
The Immune System. These are classified as the Innate and Adaptive Immune Responses. Innate Immunity
 The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
The Immune System Biological mechanisms that defend an organism must be 1. triggered by a stimulus upon injury or pathogen attack 2. able to counteract the injury or invasion 3. able to recognise foreign
PD-L1 has distinct functions in hematopoietic and nonhematopoietic cells in regulating T cell responses during chronic infection in mice
 Research article PD-L1 has distinct functions in hematopoietic and nonhematopoietic cells in regulating T cell responses during chronic infection in mice Scott N. Mueller, 1 Vijay K. Vanguri, 2 Sang-Jun
Research article PD-L1 has distinct functions in hematopoietic and nonhematopoietic cells in regulating T cell responses during chronic infection in mice Scott N. Mueller, 1 Vijay K. Vanguri, 2 Sang-Jun
Lecture outline. Immunological tolerance and immune regulation. Central and peripheral tolerance. Inhibitory receptors of T cells. Regulatory T cells
 1 Immunological tolerance and immune regulation Abul K. Abbas UCSF 2 Lecture outline Central and peripheral tolerance Inhibitory receptors of T cells Regulatory T cells 1 The immunological equilibrium:
1 Immunological tolerance and immune regulation Abul K. Abbas UCSF 2 Lecture outline Central and peripheral tolerance Inhibitory receptors of T cells Regulatory T cells 1 The immunological equilibrium:
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16
 COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
COURSE: Medical Microbiology, PAMB 650/720 - Fall 2008 Lecture 16 Tumor Immunology M. Nagarkatti Teaching Objectives: Introduction to Cancer Immunology Know the antigens expressed by cancer cells Understand
Supplementary Figure 1
 Supplementary Figure 1 Identification of IFN-γ-producing CD8 + and CD4 + T cells with naive phenotype by alternative gating and sample-processing strategies. a. Contour 5% probability plots show definition
Supplementary Figure 1 Identification of IFN-γ-producing CD8 + and CD4 + T cells with naive phenotype by alternative gating and sample-processing strategies. a. Contour 5% probability plots show definition
