Congenital Nasal Neuroglial Heterotopia and Encephaloceles: An Update on Current Evaluation and Management
|
|
|
- Emil White
- 5 years ago
- Views:
Transcription
1 The Laryngoscope VC 2016 The American Laryngological, Rhinological and Otological Society, Inc. Congenital Nasal Neuroglial Heterotopia and Encephaloceles: An Update on Current Evaluation and Management Eelam Adil, MD, MBA; Caroline Robson, MB, ChB; Antonio Perez-Atayde, MD; Colleen Heffernan, MB, BAO, Bch; Ethan Moritz, BS; Liliana Goumnerova, MD; Reza Rahbar, DMD, MD Objectives/Hypothesis: To describe our experience and current management approach for congenital nasal neuroglial heterotopia (NGH) and encephaloceles. Study Design: Retrospective chart review at a tertiary pediatric hospital from 1970 to Methods: Thirty patients met inclusion criteria: 21 NGH and nine encephaloceles. Data including demographics, pathology, imaging modality, surgical approach, resection extent, outcomes, and complications were analyzed. Results: Fourteen NGH patients (67%) presented with an internal nasal mass and nasal obstruction. Three patients (14%) presented with an external nasal mass and four (19%) had a mixed lesion. Median age at surgery was 0.51 years (interquartile range 1.32 years). Thirteen (62%) had an intranasal endoscopic approach. Median operative time was 1.6 hours (interquartile range 1.2 hours), and there were no major complications. Nine patients with encephalocele were identified: six (67%) presented with transethmoidal encephaloceles, two (22%) presented with nasoethmoidal encephaloceles, and one (11%) presented with a nasofrontal lesion. The median age at surgery was 1.25 years (interquartile range 1.4 years). All patients required a craniotomy for intracranial extension. Median operative time was 5 hours (interquartile range 1.9 hours), and eight patients (88%) had a total resection. Length of stay ranged from 3 to 14 days. Conclusion: Nasal neuroglial heterotopia and encephaloceles are very rare lesions that require multidisciplinary evaluation and management. At our institution, there has been a shift to magnetic resonance imaging alone for the evaluation of NGH to avoid radiation exposure. Endoscopic extracranial resection is feasible for most intranasal and mixed NGH without an increase in operative time, residual disease, or complications. Key Words: Nasal glioma, neuroglial heterotopia, encephalocele, congenital nasal lesion. Level of Evidence: 4. Laryngoscope, 126: , 2016 INTRODUCTION Congenital frontonasal masses are a group of very rare benign lesions that occur in one out of every 20,000 to 40,000 live births. 1 Neuroglial heterotopia (NGH; previously known as nasal glioma) and encephaloceles are included in this group and often discussed together given their similar neural origins. There are several theories regarding their pathogenesis. Neuroglial heterotopia or sequestration during cribriform plate fusion are two theories that may explain nasal NGH development but not frontonasal encephaloceles. A defect of anterior From the Department of Otolaryngology and Communication Enhancement (E.A., E.M., R.R.); the Department of Radiology (C.R.); the Department of Pathology (A.P-A.); the Department of Neurosurgery (L.G.), Boston Children s Hospital; the Harvard Medical School (E.A., C.R., A.P-A., R.R.), Boston, Massachusetts, U.S.A.; and the Department of Ear, Nose, Throat, Head and Neck Surgery, Galway University Hospital (C.H.), Galway, Ireland. Editor s Note: This Manuscript was accepted for publication December 15, Presented at the Triological Society Combined Sections Meeting, Coronado, California, U.S.A., January 23, The authors have no funding, financial relationships, or conflicts of interest to disclose. Send correspondence to Reza Rahbar, MD, Department of Otolaryngology and Communication Enhancement, Boston Children s Hospital, 300 Longwood Avenue, LO-367, Boston, MA reza.rahbar@ childrens.harvard.edu DOI: /lary neuropore closure during embryogenesis, resulting in herniation or sequestration of tissue through the fonticulus frontalis or foramen cecum, is a more widely accepted theory. 2 Due to their central nervous system origin, both pathologies can have intracranial extension. Given the rarity of these lesions and the changes in evaluation and management of these tumors over the past decade, we sought to update our previously reported experience with NGH and encephaloceles. 3 Over the past 20 years, there has been a trend toward endoscopic management of nasal masses. There are several unique challenges with approaching the skull base in pediatric patients when compared to their adult counterparts. The relatively smaller size of the nose is an obvious obstacle to endoscopic approaches. A smaller orifice inhibits both the size and maneuverability of endoscopic instruments. There are also potential effects of both open and endoscopic approaches on the developing craniofacial skeleton. Finally, variation in the location of anatomic landmarks in the developing basicranium is an issue in pediatric skull base surgery. However, advances in image guidance have helped dramatically with this concern. In addition to shifting to endoscopic management, the imaging evaluation of nasal masses has evolved because of concerns regarding cancer risk in pediatric patients exposed to ionizing radiation. It is generally 2161
2 accepted that pediatric computerized tomography (CT) has the potential for a significantly increased lifetime radiation risk over adult CT due to increased patient dose per milliampere-second (mas) and increased lifetime risk per unit dose. 4 Because of these concerns, the Society for Pediatric Radiology has developed the Image Gently campaign advocating for radiation dose reduction strategies. Lower mas can be used while preserving the diagnostic quality of CT exams in order to decrease patient radiation dose. Alternatively replacing CT exams with magnetic resonance imaging (MRI) avoids radiation exposure altogether. The purpose of this study is to review the presentation, lesion characteristics, and management strategy of our patients with nasal NGH and encephaloceles with a focus on what has changed since the publication of our initial manuscript 12 years ago. MATERIALS AND METHODS The Boston Children s Hospital Institutional Review Board approved this study, and its guidelines were followed. A retrospective chart review was performed on all patients under age 18 diagnosed with nasal NGH or encephalocele based on final pathology results at Boston Children s Hospital from 1970 to Patients with traumatic or iatrogenic nasal encephaloceles were excluded. Encephaloceles without a nasal component were excluded (ie., occipital, nasoorbital, sphenoethmoidal, transsphenoidal, and sphenomaxillary) because of the heterogeneity of these lesions. A total of 21 patients with NGH and nine patients with congenital nasal encephaloceles met inclusion criteria. Patient records and imaging were reviewed to identify patient demographics, lesion location, imaging strategy, surgical approach, reconstruction technique, and postoperative course. RESULTS Neuroglial Heterotopia Data regarding the 21 pediatric patients with NGH is summarized in Table I (note that the 10 NGH patients reported in our previous case series are indicated in bold). There was a male:female ratio of 2:1. Fourteen patients (67%) presented with an internal nasal mass and symptoms of nasal obstruction. In the youngest patient (0.02 years), nasal obstruction led to respiratory distress that required urgent surgical intervention. Three patients (14%) presented with an external nasal mass, and four (19%) had a mixed lesion. Four patients had their initial resection at outside institutions and presented to our facility with recurrences. All patients underwent imaging prior to surgery (Figs. 1 and 2). Five (24%) patients had a CT scan, 10 (48%) underwent MRI, and six (29%) had both. In our original report, three patients (30%) with NGH had a MRI alone, whereas seven (64%) were evaluated solely with MRI in our most recent experience. 3 The median age at the time of surgery was 0.51 years (interquartile range 1.32 years). Thirteen (62%) patients had an intranasal endoscopic approach, five (24%) had an external approach, and two (10%) had an intranasal. One (5%) patient had a cleft palate and the lesion was excised transorally. Median operative time was 1.6 hours (interquartile 2162 range 1.2 hours) and there were no major hemorrhages. Length of stay ranged from 0 to 3 days. All patients had a total resection. There were no early or late major complications. One patient developed erythema of the nasal vestibule, likely secondary to pressure from the endoscope, and this resolved within 8 days. There were no reported recurrences during the follow-up period. Encephaloceles A total of nine patients with congenital nasal encephaloceles were identified during the study period (Table II; note that the 6 encephalocele patients from our original article are highlighted in bold). There was a female to male ratio of 2:1. Six patients (67%) presented with transethmoidal encephaloceles. Most of these patients presented with symptoms of nasal obstruction, and one presented with meningitis. Two patients (22%) presented with nasoethmoidal encephaloceles, and one (11%) presented with a nasofrontal lesion. The median age at surgery was 1.25 years (interquartile range 1.4 years). All lesions were found to have intracranial extension, and all underwent a craniotomy. The nasal portion of the lesion was approached endoscopically in three patients (33%), through the craniotomy incision in three patients (33%), transnasally in two patients (22%), and through a lateral rhinotomy in one patient (11%). The median operative time was 5 hours (interquartile range 1.9 hours), and blood loss was 50 cc (interquartile range 70cc). Eight patients (88%) had a total resection of their lesion. There were three (33%) postoperative complications: epiphora, cerebrospinal fluid (CSF) leak, and hydrocephalus. Length of stay ranged from 3 to 14 days. DISCUSSION Patient and Tumor Demographics Similar to prior studies, we found that NGH and congenital nasal encephaloceles are extremely rare. In the 43-year span of this study, only 21 NGH and nine nasal encephaloceles that met our inclusion criteria were identified. This makes conclusions about demographics very difficult. Previous reports indicate that NGH occur in a male to female ratio of 3:2 and encephaloceles are evenly distributed. 5 Similarly, NGH was more common in males (2:1) in our series. Nasal encephaloceles were more common in females (2:1) in our series, but we excluded traumatic, iatrogenic, and any encephaloceles without a nasal component that may explain the discrepancy. It has also been reported that most NGH are extranasal (60%), 30% are intranasal, and 10% are mixed. 6,7 During our total study period, most patients (67%) had intranasal lesions. Nine of 11 patients over the past 10 years had intranasal lesions. It is difficult to know whether this is a true trend or based on our referral pattern. Only one patient in our series (5%) had intracranial extension, which is lower than the 10% to 25% reported in the literature. 2
3 TABLE I. Characteristics of 21 Pediatric Nasal Neuroglial Heterotopia Patients. Age at Surgery (years) Gender Presenting Symptoms Tumor Site Recurrence on Presentation Initial Surgical Approach Time to Recurrence (years) Imaging Intracranial Extension Surgical Approach Operative Time (hours) Length of Stay (days) Length of Follow-up (years) 0.51 Male Nasal mass, nasal Anterior nasal cavity No CT No Intranasal Male Nasal mass, nasal Anterior nasal cavity No CT/MRI No Intranasal endoscopic Male Nasal mass Nasal dorsum No MRI No Lateral rhinotomy Male Recurrent nasal mass, Glabella Yes Craniotomy 2.5 CT/MRI No Lateral rhinotomy nasal swelling 0.07 Female Nasal mass, nasal Anterior nasal cavity No CT/MRI Intranasal endoscopic Male Nasal mass, recurrent disease Septum, upper lateral cartilage Yes Intranasal 0.83 MRI No External rhinoplasty Male Nasal mass Glabella/nasal dorsum No CT/MRI No Median rhinotomy Female Nasal mass, nasal, growth of mass Nasal dorsum, lateral nasal wall No MRI No External rhinoplasty Female Nasal mass Posterior nasal cavity No CT No Transoral (cleft palate) Male Nasal mass, Anterior nasal cavity No CT No Intranasal Male Nasal mass Anterio nasal cavity No CT No Intranasal endoscopic Female Growth of residual disease noted Posterior nasal cavity Yes Craniotomy, intranasal 2 CT/MRI Yes Frontotemporal craniotomy, intranasal endoscopic Male Nasal mass Nasoethmoid No CT No Intranasal endoscopic Male Nasal obstruction, Anterior nasal cavity No MRI No Intranasal endoscopic nasal 0.42 Female Nasal mass, snoring Anterior nasal cavity No MRI No Intranasal endoscopic Male Nasal Anterior nasal cavity No MRI No Intranasal endoscopic Female Periorbital edema, Anterior nasal cavity No CT/MRI No Intranasal endoscopic rhinorrhea 0.1 Male Nasal obstruction, Anterior nasal cavity No MRI No Intranasal endoscopic rhinorrhea 7.48 Male Nasal mass, residual disease 0.02 Female Nasal mass, respiratory distress, difficulty feeding Anterior nasal cavity Yes Intranasal Skull base, lateral nasal wall 0.51 Male Nasal mass Skull base, lateral nasal wall 5 MRI No Intranasal endoscopic No MRI No Intranasal endoscopic No MRI No Intranasal endoscopic Patients in bold are those that were reported in our previous article. 3 CT 5 computed tomography; MRI 5 magnetic resonance imaging.
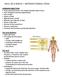
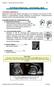
4 Fig. 1. A 41-day-old male with a left intranasal NGH. (A) Coronal T2-weighted MRI demonstrating a partially cystic intranasal mass protruding superomedial to the left inferior turbinate (long arrow). The nasal septum is bowed to the right (short arrow). The anterior cranial fossa appears intact. (B) High-resolution, thin-section axial-t2 and (C) axial T1-weighted MRI show the partially cystic, anterior nasal cavity mass with a solid component that is isointense with cortex. (D) Fat-suppressed axial T1-weighted MR reveals only peripheral enhancement (arrowhead). The location superomedial to the inferior turbinate and solid component distinguishes this lesion from a nasolacrimal duct cyst. The absence of intracranial connection excludes an encephalocele. The absence of enhancement differentiates NGH from an intranasal tumor or venous malformation. MRI 5 magnetic resonance imaging; NGH 5 nasal neuroglial heterotopia Evaluation As noted in our prior publication, these lesions require a thorough multidisciplinary approach, which includes otolaryngology, neuroradiology, neurosurgery, and possibly a reconstructive team. 3 Evaluation begins with a thorough history and physical exam. On examination, it is important to note the location of the lesion and whether or not it is pulsatile. Expansion of the nasal lesion with compression of the internal jugular vein (Furstenberg s sign) can indicate an intracranial connection. If a NGH or encephalocele is suspected, biopsy should be avoided and imaging pursued instead. There has been a shift at our institution toward MRI imaging alone for NGH, given the improved soft tissue characterization when compared to CT imaging and the presumed increased risk of carcinogenesis with ionizing radiation in the pediatric age group. Three patients in our recent experience had CT scans because they were initially evaluated at outside institutions, and one had a CT scan because of intracranial extension. No patients in our series of NGH evaluated with MRI alone had a subtotal resection or unexpected intracranial extension, which indicates that MRI alone is an adequate imaging study for NGH without intracranial extension. Therefore, the authors recommend MRI alone for patients with NGH isolated to the nasal cavity. This may not be feasible at all institutions; some institutions may not have access to MRI and/or pediatric anesthesiology, the latter being necessary for some pediatric patients who require sedation during image acquisition. In these cases, transfer to an outside facility for both image acquisition and operative management can be considered. Pulse sequences should consist of high-resolution, thin-section, fat-suppressed multiplanar T2; multiplanar Fig. 2. A 77-day-old male with solid prenasal nasal neuroglial heterotopia versus encephalocele. (A) Sagittal fast-spin echo inversion recovery magnetic resonance imaging shows a prenasal mass that is isointense with gray matter connected via a small stalk (arrow) to the anterior cranial fossa. Absence of continuity with the frontal lobes distinguishes this from an encephalocele in spite of the presence of the small stalk. (B) Helical axial computed tomography delineates the bony defect (arrow) prior to surgical resection.
5 TABLE II. Characteristics of Congenital Nasal Encephalocele Patients. Age at Surgery (years) Gender Laterality Presenting symptoms Type Imaging Type of Craniotomy ORL Approach Reconstruction Extent of Resection Operative time (hours) Estimated blood loss (cc) Complications Time to Resolution of complication (days) Length of Stay (days) Length of follow-up (years) 0.58 Female Left Respiratory distress, rhinorrhea, nasal obstruction 2 Female Left Nasal obstruction, rhinorrhea 1.9 Female Right Nasal mass Transethmoidal Skull X-ray Male Left Respiratory distress, rhinorrhea, nasal obstruction Transethmoidal MRI Bifrontal Intranasal endoscopic Transethmoidal CT Bifrontal Lateral rhinotomy Transethmoidal Skull X-ray Bifrontal Intranasal Bifrontal Intranasal Fascia graft from left temporal to dura, Pericranial Pericranial Pericranial 0.58 Female Bilateral Nasal mass Nasoethmoidal CT/MRI Subcranial None Pericranial 6 Female Left Nasal mass Nasoethmoidal CT/MRI Bifrontal None Pericranial 0.6 Female Right Nasal obstruction Transethmoidal CT/MRI Bifrontal Intranasal endoscopic Bone tiseel, 1.25 Male Bilateral Nasal mass Nasofrontal CT/MRI Bifrontal None Bilateral frontoorbital advancement. Calvarial bone graft nasal reconstruction 13 Male Right Meningitis Transethmoidal CT/MRI Bifrontal Intranasal endoscopic Mucoperiosteal graft Total None N/A 3 3 Subtotal 5 80 Epiphora Total CSF leak Total None N/A 4 3 Total None N/A Total None N/A 4 5 Total 5 30 None N/A Total Hydrocephalus Total None N/A Patients in bold are those that were reported in our previous article. 3 CSF 5 cerebral spinal fluid; CT 5 computed tomography; MRI 5 magnetic resonance imaging; N/A 5 not applicable.
6 Fig. 3. Light microscopy of nasal glioma: (A) Bundles of neuroglial tissue with hypertrophic astrocytes are separated by vascular, collagenous septa. (B) Bundles of neuroglial tissue are diffusely and strongly immunoreactive (brown color) for glial fibrillary acidic protein. Light microscopy of encephalocele: (C) Neuroglial tissue with hypertrophic astrocytes (arrowheads) and scattered neurons (arrows). (D) Choroid plexus component. [Color figure can be viewed in the online issue, which is available at high resolution T1; and nonecho planar diffusionweighted images (Figs. 1 and 2). Gadolinium-enhanced fat-suppressed T1-weighted images should also be obtained if a mass other than encephalocele is demonstrated. Every attempt is made to obtain the exam while the patient is naturally asleep in order to avoid sedation or general anesthetic. This may require obtaining intravenous access ahead of the infant falling asleep. For patients in whom an intracranial connection is found on MRI, a limited sinus CT scan is then indicated for assessment of the calvarium and for use with image guidance systems. Because the soft tissue characteristics of the lesion are well characterized by MR, when required, CT is obtained for assessment of bony detail alone and consists of helical axial images utilizing a lowdose technique, with multiplanar reformatted images. The MR exam provides a guide as to whether contrast is required for CT. For assessment of nasofrontal encephaloceles, contrast is not required. However if there is a question regarding the integrity of the anterior cranial fossa (the anterior cranial fossa is incompletely ossified in an infant under the age of 2 years), contrast will be required in order to demonstrate the integrity of the unossified enhancing cartilage in this region. Management In our original series, five out of 10 patients had an external approach to their NGH. Since that time, we have been able to resect all of our NGH through an endonasal endoscopic approach. The median operative time was lower for our transnasal endoscopic cases (0.75 hours; interquartile range hours) when compared to cases that required a facial incision (2.55 hours; interquartile range hours). Only one patient 2166 had transient nasal alar erythema in the transnasal endoscopic group. This occurred in a 3-month-old infant and was secondary to stretch of the nasal ala from the transnasal instrumentation during resection. This resolved spontaneously in 8 days without any permanent sequelae. Similarly, we have been able to achieve total resection for all of our recent nasal encephaloceles using a transnasal endoscopic approach and/or transcranial endoscopic approach (i.e., accessing the intranasal component of the encephalocele through the craniotomy and skull base defect created by the lesion). Therefore, the authors advocate for avoiding all facial incisions for all sinonasal pathology if technically feasible. For all patients with intracranial extension, the use of image guidance as an adjunct is also recommended. In particular, when accessing intranasal components of tumors through limited craniotomy defects, the use of image guidance has been quite useful for ensuring complete resection. Reconstruction of skull base defects in patients with intracranial extension has been accomplished through the use of an anteriorly based pericranial flap in all patients. Most recently, we have been augmenting the pericranial flap with a free inferior turbinate mucoperiosteal graft. No recent patients have developed a complication such as meningitis or CSF leak. Given the anterior location and relatively small residual skull base defect following of lesions with intracranial extension, a nasoseptal flap has not been utilized for skull base reconstruction. Length of stay (LOS) ranged from 0 to 3 days for most NGH patients. One patient had a prolonged stay (45 days) because of congenital heart disease that required management. The LOS of encephalocele
7 patients ranged from 3 to 14 days. In general, LOS was longer for younger patients, those travelling from outside of the region for resection, and those in need of a craniotomy. Pathology It can be difficult to distinguish NGH and encephaloceles based on histopathology. Nasal neuroglial heterotopia is characterized by fibroconnective tissue with focal infiltration by bundles of glial tissue (Fig. 3). This is typically immunoreactive for glial fibrillary acid protein, S-100, synaptophysin, and epithelial membrane antigen. Encephaloceles can also contain variable amounts of glial tissue. The presence of leptomeninges helps distinguish encephalocele from NGH. If no ependymal tissue is present, then the diagnosis is based on clinicopathological and imaging findings. Since our original publication, no new staining or imaging techniques have improved our ability to detect these lesions. CONCLUSION Nasal neuroglial heterotopia and encephaloceles are very rare lesions that must be considered in the differential of congenital nasal masses. Magnetic resonance imaging alone is adequate for imaging evaluation of lesions limited to the nasal cavity. Low dose sinus CT imaging is necessary for both bony evaluation and image guidance for patients with intracranial extension. Most tumors can be completely resected without the use of any facial incisions through the use of a transnasal endoscopic approach and/or endoscopic transcraniotomy approach. Operative time is shorter with endoscopic approaches without compromising tumor resection or increasing complications. BIBLIOGRAPHY 1. Hughes GB, Sharpino G, Hunt W, Tucker HM. Management of the congenital midline nasal masses: a review. Head Neck Surg 1980;2: Patterson K, Kapur S, Chandra RS. Nasal glial heterotopias and related brain heterotopias: a pathologist s perspective. Pediatr Pathol 1986;5: Rahbar R, Resto VA, Robson CD, et al. Nasal glial heterotopia and encephalocele: diagnosis and management. Laryngoscope 2003;113: Brenner DJ, Elliston CD. Estimated radiation risks potentially associated with full-body CT screening. Radiology 2004;232: Rouev P, Dimov P, Shomov G. A case of nasal glial heterotopia in newborn infant. Int J Pediatr Otorhinolaryngol 2001;58: Jaffe BF. Classification and management of anomalies of the nose. Otolaryngol Clin North Am 1981;14: Pensler JM, Ivescu AS, Ciletti SJ, et al. Craniofacial gliomas. Plas Reconstr Surg 1996;98:
Endoscopic Assisted resection for congenital Midline Nasal Mass
 Endoscopic Assisted resection for congenital Midline Nasal Mass Ahmed Aly Ibrahim A.prof ORL Department Alexandria University Emad. A Magdy prof ORL Department Alexandria University Haytham Morsi,MD Mohammad
Endoscopic Assisted resection for congenital Midline Nasal Mass Ahmed Aly Ibrahim A.prof ORL Department Alexandria University Emad. A Magdy prof ORL Department Alexandria University Haytham Morsi,MD Mohammad
Case Report A Case of Nasal Glial Heterotopia in an Adult
 Case Reports in Otolaryngology, Article ID 354672, 4 pages http://dx.doi.org/10.1155/2014/354672 Case Report A Case of Nasal Glial Heterotopia in an Adult Akira Hagiwara, 1,2 Noriko Nagai, 1 Yasuo Ogawa,
Case Reports in Otolaryngology, Article ID 354672, 4 pages http://dx.doi.org/10.1155/2014/354672 Case Report A Case of Nasal Glial Heterotopia in an Adult Akira Hagiwara, 1,2 Noriko Nagai, 1 Yasuo Ogawa,
Nasal Glioma: Prenatal Diagnosis and Multidisciplinary Surgical Approach
 Nasal Glioma: Prenatal Diagnosis and Multidisciplinary Surgical Approach The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation
Nasal Glioma: Prenatal Diagnosis and Multidisciplinary Surgical Approach The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters Citation
MANAGEMENT OF CSF. Steven D. Schaefer, MD, FACS. Department of Otolaryngology New York Eye and Ear Infirmary
 MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
MANAGEMENT OF CSF RHINORRHEA, MENIGIOCELES, Steven D. Schaefer, MD, FACS Professor and Chair Department of Otolaryngology New York Eye and Ear Infirmary New York Medical College Anatomy and Physiology
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
Rare Combination of Frontonasal and Bilateral Naso-orbital Encephaloceles
 Rare Combination of Frontonasal and Bilateral Naso-orbital Encephaloceles Alan A. Alexander 1*, Megan R. Saettele 2, Daniel L'Heureux 1, Paras A. Shah 3, Kristin A. Fickenscher 4 1. Department of Radiology,
Rare Combination of Frontonasal and Bilateral Naso-orbital Encephaloceles Alan A. Alexander 1*, Megan R. Saettele 2, Daniel L'Heureux 1, Paras A. Shah 3, Kristin A. Fickenscher 4 1. Department of Radiology,
Biological Early Detection of Nasal Dermoid Cyst Using CT/ MRI Scan - A Review
 Biological Early Detection of Nasal Dermoid Cyst Using CT/ MRI Scan - A Review Neeraj Singla 1, Sugandha Sharma 2 M.Tech Student, Dept. of CSE, CGC, Gharuan, Punjab, India 1 Assistant Professor, Dept.
Biological Early Detection of Nasal Dermoid Cyst Using CT/ MRI Scan - A Review Neeraj Singla 1, Sugandha Sharma 2 M.Tech Student, Dept. of CSE, CGC, Gharuan, Punjab, India 1 Assistant Professor, Dept.
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Management of Nasal Dermoid Sinus Cyst by Modified
 AIJCR CASE REPORT Management of Nasal Dermoid Sinus Cyst by Modified Bipedicle 10.5005/jp-journals-10013-1247 Advancement Flap Technique Management of Nasal Dermoid Sinus Cyst by Modified Bipedicle Advancement
AIJCR CASE REPORT Management of Nasal Dermoid Sinus Cyst by Modified Bipedicle 10.5005/jp-journals-10013-1247 Advancement Flap Technique Management of Nasal Dermoid Sinus Cyst by Modified Bipedicle Advancement
An important indication for imaging the anterior skull base
 ORIGINAL RESEARCH D.C. Hughes M.J. Kaduthodil D.J.A. Connolly P.D. Griffiths Dimensions and Ossification of the Normal Anterior Cranial Fossa in Children BACKGROUND AND PURPOSE: Interpretation of CT of
ORIGINAL RESEARCH D.C. Hughes M.J. Kaduthodil D.J.A. Connolly P.D. Griffiths Dimensions and Ossification of the Normal Anterior Cranial Fossa in Children BACKGROUND AND PURPOSE: Interpretation of CT of
CASE REPORT-NASO-ETHMOIDAL ENCEPHALOCELE Shrishail Patil 1, Tanvi Choubey 2
 -NASO-ETHMOIDAL ENCEPHALOCELE Shrishail Patil 1, Tanvi Choubey 2 HOW TO CITE THIS ARTICLE: Shrishail Patil, Tanvi Choubey. Case Report-_Naso-ethmoidal Encephalocele. Journal of Evolution of Medical and
-NASO-ETHMOIDAL ENCEPHALOCELE Shrishail Patil 1, Tanvi Choubey 2 HOW TO CITE THIS ARTICLE: Shrishail Patil, Tanvi Choubey. Case Report-_Naso-ethmoidal Encephalocele. Journal of Evolution of Medical and
Endoscopic Approach a Rare Adult Nasal Glioma and Review of the Literature
 International Archives of Medical Research Volume5, No. 2, pp.15-21, 2013. CASE REPORT Endoscopic Approach a Rare Adult Nasal Glioma and Review of the Literature Mehmet Akdag 1, Ulaş Alabalik 2, Abdurrahim
International Archives of Medical Research Volume5, No. 2, pp.15-21, 2013. CASE REPORT Endoscopic Approach a Rare Adult Nasal Glioma and Review of the Literature Mehmet Akdag 1, Ulaş Alabalik 2, Abdurrahim
Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features
 The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features Yin-Ping
The Laryngoscope VC 2014 The American Laryngological, Rhinological and Otological Society, Inc. Extranodal Natural Killer/T-Cell Lymphoma Nasal Type: Detection by Computed Tomography Features Yin-Ping
CSF Leaks. Abnormal communication between the subarachnoid space and the tympanomastoid space or nasal cavity. Presenting symptoms:
 CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
CSF Leaks Steven Wright, M.D. Faculty Advisor: Matthew Ryan, M.D. The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January 5, 2005 CSF Leaks Abnormal communication
RADIOLOGY TEACHING CONFERENCE
 RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
RADIOLOGY TEACHING CONFERENCE John Athas, MD Monica Tadros, MD Columbia University, College of Physicians & Surgeons Department of Otolaryngology- Head & Neck Surgery September 27, 2007 CT SCAN IMAGING
Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Transnasal Endoscopic Medial Maxillary Sinus Wall Transposition With Preservation of Structures Alice Z.
Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
 Case Reports in Medicine Volume 2012, Article ID 763259, 4 pages doi:10.1155/2012/763259 Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
Case Reports in Medicine Volume 2012, Article ID 763259, 4 pages doi:10.1155/2012/763259 Case Report Gigant Transethmoidal Meningoencephalocele Operated by Full Endonasal Endoscopic Approach: Case Report
Complex Hydrocephalus
 2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
2012 Hydrocephalus Association Conference Washington, DC - June 27-July1, 2012 Complex Hydrocephalus Marion L. Walker, MD Professor of Neurosurgery & Pediatrics Primary Children s Medical Center University
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA
 SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
SKULL AS A WHOLE + ANTERIOR CRANIAL FOSSA LEARNING OBJECTIVES At the end of this lecture, the student should be able to know: Parts of skeleton (axial and appendicular) Parts of skull Sutures of skull
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA
 ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
ENDOSCOPIC-ASSISTED CRANIONASAL RESECTION OF OLFACTORY NEUROBLASTOMA Anthony Po-Wing Yuen, FRCS, 1 Yiu Wah Fan, FRCS, 2 Ching Fai Fung, FRCS, 2 Kwan Ngai Hung, FRCS 2 1 Division of Otorhinolaryngology,
The management of midline transcranial nasal dermoid sinus cysts *
 British Journal of Plastic Surgery (2005) 58, 1043 1050 The management of midline transcranial nasal dermoid sinus cysts * M. Hanikeri*, N. Waterhouse, N. Kirkpatrick, D. Peterson, I. Macleod Department
British Journal of Plastic Surgery (2005) 58, 1043 1050 The management of midline transcranial nasal dermoid sinus cysts * M. Hanikeri*, N. Waterhouse, N. Kirkpatrick, D. Peterson, I. Macleod Department
intracranial anomalies
 Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Chapter 5: Fetal Central Nervous System 84 intracranial anomalies Hydrocephaly Dilatation of ventricular system secondary to an increase in the amount of CSF. Effects of hydrocephalus include flattening
Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series
 CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
CASE REPORT Spontaneous Cerebrospinal Fluid Rhinorrhea as the Presenting Symptom of Idiopathic Intracranial Hypertension: A Case Series Hossein Ghalaenovi 1, Maziar Azar 1, Morteza Taheri 1, Mahdi Safdarian
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Mucocele of paranasal sinuses
 From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
From the SelectedWorks of Balasubramanian Thiagarajan March 7, 2012 Mucocele of paranasal sinuses Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/57/ Mucoceles of paranasal
Skull base defects that result in dural tears and CSF leaks can
 ORIGINAL RESEARCH V. La Fata N. McLean S.K. Wise J.M. DelGaudio P.A. Hudgins CSF Leaks: Correlation of High-Resolution CT and Multiplanar Reformations with Intraoperative Endoscopic Findings BACKGROUND
ORIGINAL RESEARCH V. La Fata N. McLean S.K. Wise J.M. DelGaudio P.A. Hudgins CSF Leaks: Correlation of High-Resolution CT and Multiplanar Reformations with Intraoperative Endoscopic Findings BACKGROUND
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488
 National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
National Imaging Associates, Inc. Clinical guidelines/considerations SINUS & MAXILLOFACIAL AREA CT 70486, 70487, 70488 Date: September 1997 Page 1 of 5 LIMITED OR LOCALIZED FOLLOW UP - SINUS CT 76380 Guideline
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Juvenile Angiofibroma
 Juvenile Angiofibroma Disclaimer The pictures used in this presentation have been obtained from a number of sources. Their use is purely for academic and teaching purposes. The contents of this presentation
Juvenile Angiofibroma Disclaimer The pictures used in this presentation have been obtained from a number of sources. Their use is purely for academic and teaching purposes. The contents of this presentation
DR. ASEEL DOUBI R5 ORL HNS SPONTANEOUS CSF LEAKS
 DR. ASEEL DOUBI R5 ORL HNS SPONTANEOUS CSF LEAKS OUTLINE: Physiology of CSF Types of CSF rhinorrhea Spontaneous CSF leak approach and diagnosis Operative options and postoperative care Lumbar drains current
DR. ASEEL DOUBI R5 ORL HNS SPONTANEOUS CSF LEAKS OUTLINE: Physiology of CSF Types of CSF rhinorrhea Spontaneous CSF leak approach and diagnosis Operative options and postoperative care Lumbar drains current
Department of Neurosurgery. Differentiating Craniosynostosis from Positional Plagiocephaly
 Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Department of Neurosurgery Differentiating Craniosynostosis from Positional Plagiocephaly The number of infants with head shape deformities has risen over the past several years, likely due to increased
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
NASAL SEPTUM ADENOID CYSTIC CARCINOMA: A CASE REPORT
 NASAL SEPTUM ADENOID CYSTIC CARCINOMA: A CASE REPORT Shu-Yu Tai, 1 Chen-Yu Chien, 2 Chih-Feng Tai, 2,4 Wen-Rei Kuo, 2,4 Wan-Ting Huang, 3 and Ling-Feng Wang 2,4 Departments of 1 Family Medicine, 2 Otolaryngology
NASAL SEPTUM ADENOID CYSTIC CARCINOMA: A CASE REPORT Shu-Yu Tai, 1 Chen-Yu Chien, 2 Chih-Feng Tai, 2,4 Wen-Rei Kuo, 2,4 Wan-Ting Huang, 3 and Ling-Feng Wang 2,4 Departments of 1 Family Medicine, 2 Otolaryngology
A Case of Naso-Ethmoidal Meningoencephalocele
 A Case of Naso-Ethmoidal Meningoencephalocele Divyanshu Dubey, Sonjjay Pande, Pradeep Dubey, Anshudha Sawhney Vol. 3 No. 8 (August 2011) International Journal of Collaborative Research on Internal Medicine
A Case of Naso-Ethmoidal Meningoencephalocele Divyanshu Dubey, Sonjjay Pande, Pradeep Dubey, Anshudha Sawhney Vol. 3 No. 8 (August 2011) International Journal of Collaborative Research on Internal Medicine
ORIGINAL ARTICLE. Temporal Lobe Injury in Temporal Bone Fractures. imaging (MRI) to evaluate lesions of the temporal
 ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
ACUTE MASTOIDITIS IN CHILDREN: SUSCEPTIBILITY FACTORS AND MANAGEMENT
 & ACUTE MASTOIDITIS IN CHILDREN: SUSCEPTIBILITY FACTORS AND MANAGEMENT Slobodan Spremo*, Biljana Udovčić Clinic for Otorhinolaryngology, Clinic Center in Banja Luka, Zdrave Korde 1, 78000 Banja Luka, Bosnia
& ACUTE MASTOIDITIS IN CHILDREN: SUSCEPTIBILITY FACTORS AND MANAGEMENT Slobodan Spremo*, Biljana Udovčić Clinic for Otorhinolaryngology, Clinic Center in Banja Luka, Zdrave Korde 1, 78000 Banja Luka, Bosnia
Spontaneous Cerebrospinal Fluid Rhinorrhea: A clinical and anatomical study
 The Laryngoscope VC 2010 The American Laryngological, Rhinological and Otological Society, Inc. Spontaneous Cerebrospinal Fluid Rhinorrhea: A clinical and anatomical study Miklós Tóth, MD, PhD; Oxana Selivanova,
The Laryngoscope VC 2010 The American Laryngological, Rhinological and Otological Society, Inc. Spontaneous Cerebrospinal Fluid Rhinorrhea: A clinical and anatomical study Miklós Tóth, MD, PhD; Oxana Selivanova,
RECURRENT INTRA NASAL GLIOMA: A CASE REPORT D. Ranganath Swamy 1, K. Nagaraju 2, E. Yugandhar 3, B. Kathyayani 4, T. Shankar 5
 RECURRENT INTRA NASAL GLIOMA: A D. Ranganath Swamy 1, K. Nagaraju 2, E. Yugandhar 3, B. Kathyayani 4, T. Shankar 5 HOW TO CITE THIS ARTICLE: D. Ranganath Swamy, K. Nagaraju, E. Yugandhar, B. Kathyayani,
RECURRENT INTRA NASAL GLIOMA: A D. Ranganath Swamy 1, K. Nagaraju 2, E. Yugandhar 3, B. Kathyayani 4, T. Shankar 5 HOW TO CITE THIS ARTICLE: D. Ranganath Swamy, K. Nagaraju, E. Yugandhar, B. Kathyayani,
NEUROCRANIUM VISCEROCRANIUM VISCEROCRANIUM VISCEROCRANIUM
 LECTURE 4 SKULL NEUROCRANIUM VISCEROCRANIUM VISCEROCRANIUM VISCEROCRANIUM CRANIUM NEUROCRANIUM (protective case around brain) VISCEROCRANIUM (skeleton of face) NASOMAXILLARY COMPLEX MANDIBLE (DESMOCRANIUM)
LECTURE 4 SKULL NEUROCRANIUM VISCEROCRANIUM VISCEROCRANIUM VISCEROCRANIUM CRANIUM NEUROCRANIUM (protective case around brain) VISCEROCRANIUM (skeleton of face) NASOMAXILLARY COMPLEX MANDIBLE (DESMOCRANIUM)
Intranasal location of lacrimal sac in Thai cadavers
 Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Asian Biomedicine Vol. 4 No. 2 April 2010; 323-327 Clinical report Napas Tanamai a, Teeraporn Ratanaanekchai a, Sanguansak Thanaviratananich a, Kowit Chaisiwamongkol b, Thanarat Chantaumpalee b a Department
Combined transnasal and transoral endoscopic approach to a transsphenoidal encephalocele in an infant
 DOI 10.1007/s00381-015-2667-9 TECHNICAL NOTE Combined transnasal and transoral endoscopic approach to a transsphenoidal encephalocele in an infant Sien Hui Tan & Kein Seong Mun & Patricia Ann Chandran
DOI 10.1007/s00381-015-2667-9 TECHNICAL NOTE Combined transnasal and transoral endoscopic approach to a transsphenoidal encephalocele in an infant Sien Hui Tan & Kein Seong Mun & Patricia Ann Chandran
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K.
 05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
05 Tips and Tricks in Ventral Skull Base Dissection Narayanan Janakiram, Dharambir S. Sethi, Onkar K. Deshmukh, and Arvindh K. Gananathan Introduction...75 General Principles...76 Tips and Tricks in Ventral
FOR CMS (MEDICARE) MEMBERS ONLY NATIONAL COVERAGE DETERMINATION (NCD) FOR MAGNETIC RESONANCE IMAGING:
 National Imaging Associates, Inc. Clinical guidelines SINUS MRI Original Date: November 2007 Page 1 of 5 CPT Codes: 70540, 70542, 70543 Last Review Date: July 2014 NCD 220.2 MRI Last Effective Date: July
National Imaging Associates, Inc. Clinical guidelines SINUS MRI Original Date: November 2007 Page 1 of 5 CPT Codes: 70540, 70542, 70543 Last Review Date: July 2014 NCD 220.2 MRI Last Effective Date: July
Nasal Encephalocele: Endoscopic excision with anesthetic consideration
 Nasal Encephalocele: Endoscopic excision with anesthetic consideration Introduction An encephalocele is a herniation of cranial contents through a defect in the skull. It may include meninges only, termed
Nasal Encephalocele: Endoscopic excision with anesthetic consideration Introduction An encephalocele is a herniation of cranial contents through a defect in the skull. It may include meninges only, termed
T HERE is an unusual and interesting variety of craniosynostosis in
 SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
SURGICAL TREATMENT OF CONGENITAL ANOMALIES OF THE CORONAL AND METOPIC SUTURES TECHNICAL NOTE DONALD D. MATSON, M.D. Neurosurgical Service, The Children's Medical Center, and Deparlment of Surgery, Itarvard
Remember from the first year embryology Trilaminar disc has 3 layers: ectoderm, mesoderm, and endoderm
 Development of face Remember from the first year embryology Trilaminar disc has 3 layers: ectoderm, mesoderm, and endoderm The ectoderm forms the neural groove, then tube The neural tube lies in the mesoderm
Development of face Remember from the first year embryology Trilaminar disc has 3 layers: ectoderm, mesoderm, and endoderm The ectoderm forms the neural groove, then tube The neural tube lies in the mesoderm
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within the Paranasal Sinuses
 ISRN Minimally Invasive Surgery Volume 2013, Article ID 129780, 5 pages http://dx.doi.org/10.1155/2013/129780 Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within
ISRN Minimally Invasive Surgery Volume 2013, Article ID 129780, 5 pages http://dx.doi.org/10.1155/2013/129780 Research Article Expanded Endoscopic Endonasal Treatment of Primary Intracranial Tumors within
Case Report Endoscopic Endonasal Approach of Congenital Meningoencephalocele Surgery: First Reported Case in Lithuania
 Case Reports in Otolaryngology Volume 2015, Article ID 728561, 5 pages http://dx.doi.org/10.1155/2015/728561 Case Report Endoscopic Endonasal Approach of Congenital Meningoencephalocele Surgery: First
Case Reports in Otolaryngology Volume 2015, Article ID 728561, 5 pages http://dx.doi.org/10.1155/2015/728561 Case Report Endoscopic Endonasal Approach of Congenital Meningoencephalocele Surgery: First
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Craniosynostosis and Plagiocephaly
 Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
Craniosynostosis and Plagiocephaly Andrew Jea MD MHA FAAP Professor and Chief Section of Pediatric Neurosurgery Riley Hospital for Children Department of Neurosurgery Indiana University School of Medicine
CEREBRO SPINAL FLUID ANALYSIS IN BRAIN TUMOUR
 CEREBRO SPINAL FLUID ANALYSIS IN BRAIN TUMOUR Sankar K 1, Shankar N 2, Anushya 3, ShymalaDevi 4, Purvaja 5 3,4,5 III Biomedical Student, Alpha college of Engineering, Chennai. kssankar10@yahoo.co.in 1,
CEREBRO SPINAL FLUID ANALYSIS IN BRAIN TUMOUR Sankar K 1, Shankar N 2, Anushya 3, ShymalaDevi 4, Purvaja 5 3,4,5 III Biomedical Student, Alpha college of Engineering, Chennai. kssankar10@yahoo.co.in 1,
Two-Stage Management of Mega Occipito Encephalocele
 Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Two-Stage Management of Mega Occipito Encephalocele CASE REPORT A I Mardzuki*, J Abdullah**, G Ghazaime*, A R Ariff!'*, M Ghazali* *Department of Neurosciences, **Department of Radiology, Hospital Universiti
Disclosures. The Thin Red Line Between Neuropathology and Head & Neck Pathology. Introduction CASE 1. Current Issues Tihan
 Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Frontal sinus disease continues to be one of the great
 Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Unilateral transnasal endoscopic approach to frontal sinuses: Draf IIc Mohammed K. Al Komser, M.D., M.A.S. and Andrew N. Goldberg, M.D., M.S.C.E. ABSTRACT For chronic sinusitis surgery, the Draf III approach
Fetal Medicine. Case Presentations. Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital. October 2003
 Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
Case Presentations Dr Ermos Nicolaou Fetal Medicine Unit Chris Hani Baragwanath Hospital October 2003 Case 1 Ms A M 22year old P0 G1 Referred from Sebokeng Hospital at 36w for polyhydramnios On Ultrasound:
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Nasal region. cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?
 Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
Nasal region skull bones: nasal and frontal processes of maxilla cartilages: septal cartilage (l); lateral nasal cartilage (2); greater alar cartilages (2); lesser alar cartilages (?) 1 Nasal cavity Roof
OBSTRUCTIVE NASAL AND NASOPHARYNGEAL AIRWAY MASSES IN CHILDREN AND ADOLESCENTS
 OBSTRUCTIVE NASAL AND NASOPHARYNGEAL AIRWAY MASSES IN CHILDREN AND ADOLESCENTS Michael J. Cunningham MD Department of Otolaryngology and Communication Enhancement Children s Hospital Boston Nasal Airway
OBSTRUCTIVE NASAL AND NASOPHARYNGEAL AIRWAY MASSES IN CHILDREN AND ADOLESCENTS Michael J. Cunningham MD Department of Otolaryngology and Communication Enhancement Children s Hospital Boston Nasal Airway
The surgical approach to the sphenoid sinus continues to
 A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
A comparison of two sphenoidotomy approaches using a novel computerized tomography grading system Heitham Gheriani, F.R.C.S.C., F.R.C.S.I., David Flamer, B.Sc., Trent Orton, M.D., Brad Mechor, F.R.C.S.C.,
Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p
 Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Title Radiological conference. Frontal sinus osteoma complicated by pneumocephalus Author(s) Fung, WT; Peh, WCG Citation Hong Kong Practitioner, 1996, v. 18 n. 12, p. 658-662 Issued Date 1996 URL http://hdl.handle.net/10722/44655
Congenital Neck Masses C. Stefan Kénel-Pierre, MD
 Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal suture
 IJAE Vol. 119, n. 3: 263-267, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal
IJAE Vol. 119, n. 3: 263-267, 2014 ITALIAN JOURNAL OF ANATOMY AND EMBRYOLOGY Research Article Human Anatomy Case Report Bathrocephaly: a case report of a head shape associated with a persistent mendosal
Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma
 Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
Open Access Case Report DOI: 10.7759/cureus.2217 Temporal Lobe Cystic Collection and Associated Oedema: A Rare Complication of Translabyrinthine Resection of Vestibular Schwannoma Abdurrahman Raeiq 1 1.
A Clicking Larynx: Diagnostic and Therapeutic Challenges
 The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. Case Report A Clicking Larynx: Diagnostic and Therapeutic Challenges Derrek A. Heuveling, MD, PhD ; Maarten
The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. Case Report A Clicking Larynx: Diagnostic and Therapeutic Challenges Derrek A. Heuveling, MD, PhD ; Maarten
Utility of Preoperative Computed Tomography and Magnetic Resonance Imaging in Adult and Pediatric Cochlear Implant Candidates
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Utility of Preoperative Computed Tomography and Magnetic Resonance Imaging in Adult and Pediatric Cochlear
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Utility of Preoperative Computed Tomography and Magnetic Resonance Imaging in Adult and Pediatric Cochlear
Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience
 80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
80 Original Article THIEME Management Strategies for Communited Fractures of Frontal Skull Base: An Institutional Experience V. Velho 1 Hrushikesh U. Kharosekar 1 Jasmeet S. Thukral 1 Shonali Valsangkar
Leptomeningeal Cyst of the Orbital Roof in an Adult: Case Report and Literature Review
 CASE REPORT Leptomeningeal Cyst of the Orbital Roof in an Adult: Case Report and Literature Review Jeremy D. Meier, M.D., 1 Arthur B. Dublin, M.D., M.B.A., F.A.C.R., 2 and E. Bradley Strong, M.D. 1 ABSTRACT
CASE REPORT Leptomeningeal Cyst of the Orbital Roof in an Adult: Case Report and Literature Review Jeremy D. Meier, M.D., 1 Arthur B. Dublin, M.D., M.B.A., F.A.C.R., 2 and E. Bradley Strong, M.D. 1 ABSTRACT
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY
 Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS
Measure #334: Adult Sinusitis: More than One Computerized Tomography (CT) Scan Within 90 Days for Chronic Sinusitis (Overuse) National Quality Strategy Domain: Efficiency and Cost Reduction 2016 PQRS OPTIONS
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery FACIAL FRACTURES
 Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Core Curriculum Syllabus Emergencies in Otolaryngology-Head and Neck Surgery A. General Considerations FACIAL FRACTURES Look for other fractures like skull and/or cervical spine fractures Test function
Nasopharyngeal Masses Arising from Embryologic Remnants of the Clivus: A Case Series
 THIEME Case Report e253 Nasopharyngeal Masses Arising from Embryologic Remnants of the Clivus: A Case Series Mirabelle Sajisevi 1 Jenny K. Hoang 2 Rose Eapen 1 David W. Jang 1 1 Division of Head and Neck
THIEME Case Report e253 Nasopharyngeal Masses Arising from Embryologic Remnants of the Clivus: A Case Series Mirabelle Sajisevi 1 Jenny K. Hoang 2 Rose Eapen 1 David W. Jang 1 1 Division of Head and Neck
Chiari III Joseph Junewick, MD FACR
 Chiari III Joseph Junewick, MD FACR 07/02/2010 History Newborn with suboccipital mass. Diagnosis Chiari III Additional Clinical Surgery-Skin covered suboccipital cystic mass confined by the dura. Pathology-Leptomeningeal
Chiari III Joseph Junewick, MD FACR 07/02/2010 History Newborn with suboccipital mass. Diagnosis Chiari III Additional Clinical Surgery-Skin covered suboccipital cystic mass confined by the dura. Pathology-Leptomeningeal
Case MDCT 3D reconstructed features of posterior urethral valve
 Case 12688 MDCT 3D reconstructed features of posterior urethral valve Hidayatullah Hamidi Third year Resident of Radiology French medical institute for children Radiology Department; Kabul, Afghanistan;
Case 12688 MDCT 3D reconstructed features of posterior urethral valve Hidayatullah Hamidi Third year Resident of Radiology French medical institute for children Radiology Department; Kabul, Afghanistan;
Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma
 AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
AJNR Am J Neuroradiol 23:243 247, February 2002 Case Report Astroblastoma: Radiologic-Pathologic Correlation and Distinction from Ependymoma John D. Port, Daniel J. Brat, Peter C. Burger, and Martin G.
Imaging Orbit/Periorbital Injury
 Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Imaging Orbit/Periorbital Injury 9 th Nordic Trauma Radiology Course 2016 Stuart E. Mirvis, M.D., FACR Department of Radiology University of Maryland School of Medicine Fireworks Topics to Cover Struts
Endoscopic Endonasal Surgery for Subdiaphragmatic Type Craniopharyngiomas
 Original Article doi: 10.2176/nmc.oa.2018-0028 Neurol Med Chir (Tokyo) 58, 260 265, 2018 Endoscopic Endonasal Surgery for Subdiaphragmatic Type Craniopharyngiomas Hiroshi NISHIOKA, 1,2 Yuichi NAGATA, 1
Original Article doi: 10.2176/nmc.oa.2018-0028 Neurol Med Chir (Tokyo) 58, 260 265, 2018 Endoscopic Endonasal Surgery for Subdiaphragmatic Type Craniopharyngiomas Hiroshi NISHIOKA, 1,2 Yuichi NAGATA, 1
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery
 The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
The View through the Nose: ENT considerations for Pituitary/Skull Base Surgery Edsel Kim, M.D. Otolaryngology-Head and Neck Surgery The Oregon Clinic Providence Brain and Spine Institute Pituitary, Thyroid
Practical CT and MRI Anthony J. Fischetti, DVM, MS, DACVR Department Head of Diagnostic Imaging The Animal Medical Center, New York OBJECTIVE:
 Practical CT and MRI Anthony J. Fischetti, DVM, MS, DACVR Department Head of Diagnostic Imaging The Animal Medical Center, New York OBJECTIVE: This lecture describes the most common indications for referred
Practical CT and MRI Anthony J. Fischetti, DVM, MS, DACVR Department Head of Diagnostic Imaging The Animal Medical Center, New York OBJECTIVE: This lecture describes the most common indications for referred
Epidemiology 3002). Epidemiology and Pathophysiology
 Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Epidemiology Maxillofacial trauma or injuries are commonly encountered in the practice of emergency medicine and are presenting one of the most challenging problems to the attending surgeons or physicians
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study
 Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Relationship of the Optic Nerve to the Posterior Paranasal Sinuses: A CT Anatomic Study Mark C. DeLano, F. Y. Fun, and S. James Zinreich PURPOSE: To delineate the relationship between the optic nerves
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
MedStar Health considers Septoplasty-Rhinoplasty medically necessary for the following indications:
 MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.038.MH Septoplasty-Rhinoplasty This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
MedStar Health, Inc. POLICY AND PROCEDURE MANUAL MP.038.MH Septoplasty-Rhinoplasty This policy applies to the following lines of business: MedStar Employee (Select) MedStar MA DSNP CSNP MedStar CareFirst
CT assessment of acute coalescent mastoiditis.
 CT assessment of acute coalescent mastoiditis. Poster No.: C-1794 Congress: ECR 2010 Type: Educational Exhibit Topic: Head and Neck Authors: A. Thomson, S. J. Thomas, A. Hutchings, E. Tilley; Portsmouth/UK
CT assessment of acute coalescent mastoiditis. Poster No.: C-1794 Congress: ECR 2010 Type: Educational Exhibit Topic: Head and Neck Authors: A. Thomson, S. J. Thomas, A. Hutchings, E. Tilley; Portsmouth/UK
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Fracture frontal bone and its management
 From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
From the SelectedWorks of Balasubramanian Thiagarajan March 1, 2013 Fracture frontal bone and its management Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/14/ ISSN: 2250-0359
Attenuation value in HU From -500 To HU From -10 To HU From 60 To 90 HU. From 200 HU and above
 Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Brain Imaging Common CT attenuation values Structure Air Fat Water Brain tissue Recent hematoma Calcifications Bone Brain edema and infarction Normal liver parenchyma Attenuation value in HU From -500
Proboscis lateralis: report of two cases
 The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
The British Association of Plastic Surgeons (2003) 56, 704 708 CASE REPORT Proboscis lateralis: report of two cases Lütfi Eroğlu a, *, Osman Ata Uysal b a Faculty of Medicine, Department of Plastic and
Dr.ALI AL BAZZAZ PLASTIC SURGON CLEFT LIP AND PALATE
 Dr.ALI AL BAZZAZ PLASTIC SURGON CLEFT LIP AND PALATE Cleft lip (cheiloschisis) and cleft palate (palatoschisis), which can also occur together as cleft lip and palate, are variations of a type of clefting
Dr.ALI AL BAZZAZ PLASTIC SURGON CLEFT LIP AND PALATE Cleft lip (cheiloschisis) and cleft palate (palatoschisis), which can also occur together as cleft lip and palate, are variations of a type of clefting
What Is an Arteriovenous malformation (AVM)?
 American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
American Society of Neuroradiology What Is an Arteriovenous malformation (AVM)? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall
Endoscopic Management Of A Giant Ethmoid Mucocele
 ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
ISPUB.COM The Internet Journal of Otorhinolaryngology Volume 6 Number 1 S Ceylan, F Bora Citation S Ceylan, F Bora.. The Internet Journal of Otorhinolaryngology. 2006 Volume 6 Number 1. Abstract We present
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Congenital Nasal Pyriform Aperture Stenosis Is There a Role for Nasal Dilation?
 Research Original Investigation Is There a Role for Nasal Dilation? Todd M. Wine, MD; Kavita Dedhia, MD; David H. Chi, MD IMPORTANCE Congenital nasal pyriform aperture stenosis (CNPAS) may require sublabial
Research Original Investigation Is There a Role for Nasal Dilation? Todd M. Wine, MD; Kavita Dedhia, MD; David H. Chi, MD IMPORTANCE Congenital nasal pyriform aperture stenosis (CNPAS) may require sublabial
Comprehensive Techniques in CSF Leak Repair and Skull Base Reconstruction
 Comprehensive Techniques in CSF Leak Repair and Skull Base Reconstruction Advances in Oto-Rhino-Laryngology Vol. 74 Series Editors G. Randolph Boston, Mass. Comprehensive Techniques in CSF Leak Repair
Comprehensive Techniques in CSF Leak Repair and Skull Base Reconstruction Advances in Oto-Rhino-Laryngology Vol. 74 Series Editors G. Randolph Boston, Mass. Comprehensive Techniques in CSF Leak Repair
1. BRIEF DESCRIPTION OF TRAINING
 RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
RHINOLOGY 1. BRIEF DESCRIPTION OF TRAINING Exposure to clinical rhinology is provided in each of the four ORL years over the course of several rotations in a graduated approach. MEE General Otolaryngology
Surgical Treatment of Nasal Obstruction
 Surgical Treatment of Nasal Obstruction P. Daniel Knott, MD FACS Director, Division of Facial Plastic and Reconstructive Surgery Department of Otolaryngology/Head and Neck Surgery UCSF Medical Center Nothing
Surgical Treatment of Nasal Obstruction P. Daniel Knott, MD FACS Director, Division of Facial Plastic and Reconstructive Surgery Department of Otolaryngology/Head and Neck Surgery UCSF Medical Center Nothing
