The Oncogenic MicroRNA mir-22 Targets the TET2 Tumor Suppressor to Promote Hematopoietic Stem Cell Self-Renewal and Transformation
|
|
|
- Matilda Floyd
- 6 years ago
- Views:
Transcription
1 Article The Oncogenic MicroRNA mir- Targets the TET Tumor Suppressor to Promote Hematopoietic Stem Cell Self-Renewal and Transformation Su Jung Song, 1,,3,4,9 Keisuke Ito, 1,,3,4,9,1 Ugo Ala, 1,,3,4 Lev Kats, 1,,3,4 Kaitlyn Webster, 1,,3,4 Su Ming Sun, 6 Mojca Jongen-Lavrencic, 6 Katia Manova-Todorova, 7 Julie Teruya-Feldstein, 8 David E. Avigan, 5 Ruud Delwel, 6 and Pier Paolo Pandolfi 1,,3,4, * 1 Cancer Genetics Program, eth Israel Deaconess Cancer Center Department of Medicine, Division of Genetics, eth Israel Deaconess Medical Center 3 Department of Pathology, eth Israel Deaconess Medical Center 4 Division of Genetics, eth Israel Deaconess Medical Center 5 Division of Hematology and Oncology, eth Israel Deaconess Medical Center Harvard Medical School, oston, MA 15, USA 6 The Institute for Hematology, Erasmus Medical Center, Rotterdam 51, Netherlands 7 Molecular Cytology 8 Department of Pathology Sloan-Kettering Institute, Memorial Sloan-Kettering Cancer Center, New York, NY 165, USA 9 These authors contributed equally to this work 1 Present address: Ruth L. and David S. Gottesman Institute for Stem Cell and Regenerative Medicine Research, Departments of Cell iology/stem Cell Institute and Medicine, Albert Einstein Cancer Center, Albert Einstein College of Medicine, ronx, NY 1461, USA *Correspondence: ppandolf@bidmc.harvard.edu SUMMARY MicroRNAs are frequently deregulated in cancer. Here we show that mir- is upregulated in myelodysplastic syndrome (MDS) and leukemia and its aberrant expression correlates with poor survival. To explore its role in hematopoietic stem cell function and malignancy, we generated transgenic mice conditionally expressing mir- in the hematopoietic compartment. These mice displayed reduced levels of global 5-hydroxymethylcytosine (5-hmC) and increased hematopoietic stem cell self-renewal accompanied by defective differentiation. Conversely, mir- inhibition blocked proliferation in both mouse and human leukemic cells. Over time, mir- transgenic mice developed MDS and hematological malignancies. We also identify TET as a key target of mir- in this context. Ectopic expression of TET suppressed the mir--induced phenotypes. Downregulation of TET protein also correlated with poor clinical outcomes and mir- overexpression in MDS patients. Our results therefore identify mir- as a potent proto-oncogene and suggest that aberrations in the mir-/tet regulatory network are common in hematopoietic malignancies. INTRODUCTION Epigenetic mechanisms such as DNA methylation and histone modification drive stable and clonally propagated changes in gene expression and have recently been shown to serve as molecular mediators of pathway dysfunction in neoplasia (Esteller, 8; Rodríguez-Paredes and Esteller, 11). Indeed, both myelodysplastic syndrome (MDS) and leukemias are characterized by frequent epigenetic abnormalities and aberrant DNA hypermethylation has been linked to poor prognosis in cases of MDS, as it is associated with more rapid progression to acute myeloid leukemia (AML) (Shen et al., 1; Shih et al., 1). Importantly, genome-wide discovery efforts in patients with myeloid malignancies have led to the identification of a number of causal genetic abnormalities that impact the epigenetic landscape. These genes include TET, IDH1, IDH, DNMT3a, and EZH, all of which affect DNA and/or histone lysine methylation (Shih et al., 1). Recent studies have examined in detail one such gene, TET (ten-eleven-translocation gene ), which is located in 4q4 and whose mutation or deletion is extremely frequent in hematological malignancies, affecting 19% of patients with MDS, 1% of patients with myeloproliferative neoplasm (MPN), and 4% of patients with secondary AML (Abdel-Wahab et al., 9; Delhommeau et al., 9; Jankowska et al., 9; Tefferi et al., 9). TET mutations are observed in CD34 + progenitor cells and are detected most frequently after MPN and MDS progression to AML (Abdel-Wahab et al., 1). TET catalyzes the oxidation of 5-methylcytosine (5-mC) to 5-hydroxymethylcytosine (5-hmC) and is known to control hematopoiesis, presumably by regulating gene expression through its effect on DNA methylation (ranco et al., 1; Ito et al., 11; Ko et al., 1; Shih et al., 1). Tet deficiency in mice impairs 5-mC hydroxylation and leads to skewed differentiation, as well as enhancement of the self-renewal and repopulating capacity of hematopoietic stem cells (HSCs). This in turn promotes malignant transformation in mice, causing Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc. 87
2 disorders resembling MDS and MPN, as well as chronic myelomonocytic leukemia (CMMoL) (Moran-Crusio et al., 11; Quivoron et al., 11). Recent studies have likewise shown that leukemia-associated Isocitrate Dehydrogenase (IDH) 1 or mutant enzymes can induce carboxylation of glutamine-derived a-ketoglutarate (a-kg), with a concomitant increase in synthesis of -hydroxyglutarate (-HG), an inhibitory metabolite of TET (Figueroa et al., 1; Sasaki et al., 1). Collectively, these studies implicate functional and mutational losses of TET as key events underlying aberrant hematopoiesis and leukemogenesis, in turn suggesting that the inactivation of TET function by additional upstream cues could play a critical role in hematological malignancies. MicroRNA (mirna) deregulation is also known to contribute to hematological malignancies, including MDS and AML (artel, 4; Chen et al., 4; Gangaraju and Lin, 9). A combined approach involving assessment of mirna expression (using microarrays) and bioinformatic prediction of mrna targets has revealed that distinct mirna signatures fine-tune each step of hematopoiesis, including the reconstitution potential of HSCs (Arnold et al., 11; Gangaraju and Lin, 9). In turn, mirnas that target critical leukemia suppressors could act as powerful proto-oncogenes in the hematopoietic compartment (Calin and Croce, 6). In this study, we demonstrate that mir- controls hematopoiesis and HSC maintenance by negatively regulating TET protein levels. Importantly, we identify mir- as an epigenetic modifier and the key oncogenic determinant for the pathogenesis of MDS and hematological malignancies in vivo, findings with prognostic and critical therapeutic implications for a large number of hematological disorders. RESULTS mir- Is Highly Expressed in Human Hematological Malignancies and Increases the Replating Ability of HSCs In order to build on the insights of mirna biology into epigenetic alterations in myeloid malignancies, we attempted to identify those mirnas playing a critical role in the pathogenesis of the stem cell disorder MDS and its progression to overt leukemia. We first analyzed a previously reported mirna microarray profiling database and found that mir- is markedly upregulated in patients with MDS (Figures S1A and S1 available online; Dostalova Merkerova et al., 11). These results prompted us to perform expression analysis by in situ hybridization in a large set of patient samples, which included bone marrow with no sign of disease (n = 37), early stage MDS (refractory anemia [RA], 5q syndrome [5q-], refractory cytopenia with multilineage dysplasia [RCMD], and RA with ringed sideroblasts [RARS]) (n = 4), and RA with excess blasts (RAE) (n = 67). Our comprehensive in situ hybridization analysis revealed that mir- is highly expressed in patients with MDS (Figure 1A and Figure S1C). We next estimated the survival rates of the sets of MDS patients by using a Kaplan-Meier analysis and applied a log-rank test to compare the survival rates of MDS patients on the basis of mir- expression levels. Remarkably, we found that aberrant expression of mir- directly correlates with poor survival rates in patients (Figure 1). It is noteworthy that the distribution of blasts into each World Health Organization (WHO) category of MDS stages was not directly associated with the expression level of mir-, but a significant correlation between mir- levels and poor survival rates was observed within each WHO classification, as well as among MDS patients harboring a normal karyotype (Figures S1D S1F). This indicates that the poorer survival expectancy linked to mir- overexpression does not simply reflect confounding factors such as blast count and cytogenetic karyotype. Taken together, these findings led us to investigate the role of mir- in the hematopoietic system and the genesis of hematological malignancies. To explore the function of mir- in hematopoiesis and leukemia, we first transduced mouse hematopoietic stem/progenitor cells (HSPCs; c-kit pos Sca-1 pos Lin neg, hereafter referred to as KSL cells) isolated from wild-type donor mice with either a retroviral vector encoding mir- and a green fluorescent protein (GFP) or a control vector encoding GFP only. The GFP-expressing KSL cells were then resorted by flow cytometry and plated in methylcellulose for an in vitro colony-forming unit (CFU) assay (Figure S1G). We observed in the first plating that the cells expressing mir- produced fewer colonies compared to control cells; however, when GFP + KSL cells were resorted and replated, mir--transduced cells produced more colonies in the second plating (Figure S1H). Strikingly, these cells also maintained this ability throughout serial replatings: whereas control cells only formed colonies in the first two platings, mir-- expressing KSL cells were able to produce colonies after being replated at least seven times (Figure S1H). Microscopic analysis of the cells from these colonies revealed a homogenous blast-like morphology (Figure S1I, top). Consistent with these results, mir--expressing KSL cells maintained their characteristics and c-kit expression (a marker of undifferentiated cells) during their replatings (Figure S1I, bottom and Figures S1J and S1K). To ensure that mir--transduced and control cells were subjected to the same experimental treatment, we also performed an in vitro competitive colony assay by mixing GFP + KSL cells expressing mir- and GFP control KSL cells (Figure S1L, top). This analysis confirmed that mir--expressing GFP +, but not GFP, KSL cells remained mostly in colonies through consecutive replatings (Figure S1L, bottom). Taken together, these data suggest that mir- can drive aberrant replating capacity of HSPCs and may contribute to malignant transformation. mir- Affects HSC iology In Vivo We next sought to examine the biological effects of mir- in vivo and generated a conditional transgenic mouse model overexpressing mir- in the hematopoietic compartment (Figure SA). mir- expression was induced by -mediated excision of a LoxP flanked transcriptional STOP cassette by administration of seven doses of polyinosine-polycytidine (pipc) over 14 days (Figures S and SC). Two weeks after pipc administration, we isolated KSL cells from mir- F/+ ; mice and littermate controls and analyzed their properties by using CFU and long-term cultureinitiating cell (LTC-IC) assays (Figures 1C 1G and Figure SD). In agreement with our previous retroviral transduction experiments, we found that KSL cells from ; transgenic mice displayed an enhanced replating potential 88 Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc.
3 A Score 1 Score Score 3 Patient pipc ; or Littermate control ( months old) Normal M M weeks, M M Sort KSL cells Colony assay LTC-IC MT r =.7 Score of mir- p =.1 x Normal RA q RCMD 4 RARS 1 RAE-1 1 RAE- 8 7 C D GEMM GM M E F G ; SSC-A gated 6.% gated 11.7% Lineage % cells in MNCs 1 5 c-kit p <.4 Sca-1 Colonies/333KSL cells % 8.5% p <.1 % CD11b pos cells in MNCs % KSL cells in Lin neg cells 4 p < p <.1 E p <. Number of colonies/plate Survival rate (%) Time (months) ; 1 p < Number of re-plating Absolute number of KSL cells % Gr-1 pos cells in MNCs p < mir- Low (n = 49) mir- High (n = 58) ***p <.5 *** p <. p <.1 p <.1 N.D p <. p <.1 N.D Figure 1. mir- Is Upregulated in MDS Patients and Leads to Increased Replating Capacity In Vitro (A) mir- is highly expressed in MDS patient samples. Expression levels of mir- in blasts in subtypes of MDS were measured by in situ hybridization analysis. Normal (n = 37), RA (n = 3), 5q- (n = 5), RCMD (n = 4), RARS (n = 1), RAE-1 (n = 3), and RAE- (n = 35) are shown. Representative images of in situ hybridization for mir- in MDS patients and normal bone marrow are also shown (left). Insets of panels show mir- staining in blasts (arrow with ) and in differentiated myeloid cells (e.g., neutrophil, arrow with M) with a high magnification. The expression levels of mir- were also scored as described in the Supplemental Experimental Procedures (right). The data were analyzed by Chi-square test. r, Pearson s r. Scale bars, 6 mm. () mir- overexpression correlates with poor survival rates of human MDS patients. MDS patients were divided into two groups; low-mir- -expressing patients group (mir- Score 1 or, n = 49, blue) and high-mir--expressing patients group (mir- Score 3, n = 58, red). Overall survival of these patients is demonstrated. p value was generated by a log-rank test. (C) Overview of the experimental design for the conditional mir- expression in the hematopoietic compartment. Two-month-old mir- F/+ ; mice or littermate controls were treated with pipc for two weeks. Two weeks after pipc administration, c-kit pos Sca-1 pos Lin neg (KSL) cells were sorted to evaluate the characteristics of mir--expressing hematopoietic stem/progenitor cells. LTC-IC, longterm culture -initiating cells; MT, bone marrow transplantation. (D) Colony-forming capacity of mir--expressing progenitor cells. Two weeks after pipc administration, sorted KSL cells from ; mice or littermate controls were cultured in semisolid medium. Counting and classification of colonies were performed in independent littermate pairs (n = 3). GEMM, Colony-forming unit-granulocyte, erythroid, macrophage, and megakaryocyte; GM, Colony-forming unit-granulocyte and macrophage; M, Colony-forming unit-macrophage; E, urst-forming unit-erythroid. (E) mir- expression retains the ability to serially replate and generate colonies. In vitro colony replating assay was performed as shown in Figure SD and colony counts in the indicated replatings were scored (n = 3). N.D., nondetectable. (F) Ectopic expression of mir- results in an increase of HSPCs in in vitro long-term culture with stromal cells. KSL cells isolated as described in (C) were cocultured with OP-9 stromal cells for weeks. Maintained Lin neg cells and KSL cells were evaluated (n = 3). Representative flow cytometry data of Lin neg and the KSL cells (left) are shown. Mean percentage ± SD of KSL cells in Lin neg cells (middle) and mean absolute numbers ± SD of KSL cells (right) are also shown. (G) mir- increases the myeloid compartment. The percentages of cells (left), CD11b pos cells (middle), or Gr-1 pos cells (right) in total mononuclear cells (MNCs) were investigated weeks after the coculture with stromal cells from (F) (n = 3). All error bars represent ± SD. See also Figures S1, SA SD, and S7. (Figures 1D and 1E). Furthermore, ectopic expression of mir- caused a robust increase in the number of both KSL and mature myeloid cells, as determined by LTC-IC assay, indicating that mir- enhances HSPC maintenance and predisposes those cells to differentiate into the myeloid lineage (Figures 1F and 1G). Next, we examined the ability of mir--overexpressing HSPCs to compete with wild-type counterparts in vivo by utilizing an in vivo competitive transplantation assay. KSL cells from ; and mice (Ly45.) were purified weeks after pipc administration, mixed with Ly45.1/Ly45. competitor bone marrow mononuclear cells (M MNCs), and transplanted into lethally irradiated Ly45.1 congenic recipient mice. The ability of donor cells to contribute to the reconstitution was then determined by flow cytometric analysis of peripheral blood stained for Ly45.1 and Ly45.. Within 3 weeks of transplantation, donor cells from ; mice exhibited a slight increase in chimerism compared to those from control animals (Figure SE). Over time this difference became more pronounced as ; KSL cells outcompeted their wild-type counterparts (Figures A C and Figure SF). At Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc. 89
4 A CD45.1 D MNCs gated C % donor-derived cells in Myeloid cells CD % 5.8% 1 5 CD % ; MNCs gated Myeloid CD45. E 94.6% 1 5 % donor-derived cells 1 5 p <.1 p <.1 p <.1 p <.1 % donor-derived cells in cells % donor-derived cells in Myeloid cells 4 ; cell p <. p <.1 % donor-derived cells in T cells % donor-derived Myeloid cells in MNCs T cell Figure. mir- Leads to an Enhanced Repopulating Capacity of HSPCs In Vivo (A and ) Ly45.1 recipient mice were transplanted with 1,5 KSL cells from ; mice (n = 15) or littermate controls (n = 1) after pipc administration together with Ly45.1/ Ly45. competitor M MNCs. Donor-derived chimerism in peripheral blood was analyzed 6 weeks after the transplantation. Representative flow data of the CD45.1/CD45. positivity (A) and the percentages of both donor-derived cells in myeloid (CD11b pos and/or Gr-1 pos ) (, left) and donor-derived myeloid cells in MNCs (, right) of recipient mice are shown. (C E) Donor contribution in hematopoiesis of recipient mice 9 weeks after the transplantation. Representative flow data of the CD45.1/CD45. positivity with the percentages of donor-derived CD45.1 neg CD45. pos cells (C, left) are shown. Mean percentages ± SD of donor-derived cells in MNCs (C, right), myeloid cells (D), cells (E, left), and T cells (E, right) are shown (n = 1 for littermate controls and n = 15 for ;). (F) c-kit pos cells are observed in peripheral blood of recipient mice transplanted with KSL cells from ; mice. Representative flow cytometry data of c-kit positivity in donor-derived cells (left) and the percentages of c-kit pos cells in donor-derived cells (right) are shown. (n = 1 for littermate controls and n = 15 for ; ). All error bars represent ± SD. See also Figures SE, SF, and S7. F SSC Donor-derived cells gated 1.38% c-kit ; Donor-derived cells gated 3.74% % c-kit pos cells in donor-derived cells 6 weeks posttransplantation, an increased chimerism was observed in all M MNCs as well as within the myeloid fraction, and by 9 weeks this effect was also evident in the c-kit pos fraction (Figures A F). Taken together, these data strongly suggest that mir- enhances the self-renewal capacity of HSPCs in vivo. mir- Triggers MDS-like Syndromes and Hematological Malignancies In Vivo To further test whether increased aberrant hematopoiesis caused by mir- overexpression ultimately progresses to malignant hematological disease, we continued to follow up primarily transplanted recipients. Notably, at 1 weeks posttransplantation, recipient mice transplanted with KSL cells from ; donors, but not from donors, developed an illness that closely resembled human MDS, as characterized by defective erythroid maturation and anemia, splenomegaly with myeloid infiltration, low white blood cell (WC) counts, and dysplastic myeloid cells in the peripheral 1 p <.1 circulation (Figure 3 and Figures SG and SH). To determine whether this disorder is transplantable, the donor-derived KSL cells resorted from primary recipient mice were subjected to a secondary transplantation using fresh competitor cells. In agreement with our earlier results, all secondary recipients developed a lethal hematological disease within 4 weeks after secondary transplantation (Figure SI). Furthermore, we also monitored disease onset and progression to malignancy in mir- transgenic mice. The development of disease similar to that found in our chimeric transplantation model was observed in ; mice but not littermate controls at 8 months after pipc administration: the hallmarks of this distress included dysplasia in many lineages including erythroid, myeloid, and platelet; splenomegaly; and an increased number of c-kit pos undifferentiated blastic cells in the peripheral blood (Figures 4A 4C). y 16 months after pipc administration, all mir- transgenic mice had developed MDS, affecting multilineage hematopoiesis. Importantly, 13% of mice succumbed to myeloid leukemia as well as T cell lymphoma by 11 months, and all mir- transgenic mice suffered from hematological abnormality by 16 months. Finally, 7% of mir- transgenic mice developed myeloid leukemia within years (Figures 4D 4G). 9 Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc.
5 A ; C CD71 R1 R R3 R4 R1 R R3 R4 Ter119 % Ter119 neg CD71 pos cells.4. Spleen % spleen weight/ body weight p < R1 p <.5 % Ter119 pos CD71 pos cells 6 4 D p <.5 ; R WC (K/mL) 3 1 Myeloid infiltration % % 76.5% 3.5% 5.9% 39.7% 35.%.5% p <.1 p =.3 1 E Plt (K/mL) 5.% 5.9% Erythroid 39.8% 1.7% 6.6% 54.1%.5% Figure 3. mir- Overexpression Develops Hematological Syndromes (A and ) mir- overexpression leads to human MDS-like phenotypes characterized by defective erythropoiesis (A) and cytopenia () in mir- transgenic mice. After pipc administration, 1,5 KSL cells from ; mice or littermate controls were transplanted into lethally irradiated Ly45.1 recipient mice with Ly45.1/ Ly45. competitor M MNCs (n = 1 for littermate controls and n = 15 for ;). Twelve weeks after transplantation, peripheral blood of recipient mice was evaluated. Representative flow data of the Ter119/CD71 positivity (A, left) and the percentages of R1 (Ter119 neg CD71 pos ) (A, middle) and R (Ter119 pos CD71 pos ) (A, right) are shown. White blood cell (WC) (, left) and platelet (Plt) counts (, right) are also shown. (C and D) SplenomegaIy and myeloid infiltration into spleen were observed in recipient mice transplanted with KSL cells from ;Mx1- Cre mice. Representative images of spleens (C, left), spleen weight (n = 3) (C, right), and representative flow data of the positivity of c-kit and CD11b and/or Gr-1 in spleen (D) are shown. (E) mir- expression leads to a differentiation defect in erythroid compartment. Representative flow data of the Ter119/CD71 positivity in spleen are shown. All error bars indicate ± SD. See also Figures SG SI. c-kit CD11b/Gr-1 CD71 Ter % We also confirmed that the disease was triggered by mir- from KSL cells sorted from mir--expressing colonies. To this end, mir--expressing cells were subjected to consecutive colony replating and at the sixth replating, the residual c-kit pos Lin neg (KL) cells were transplanted into lethally irradiated recipient mice (Figure S3A). Consistent with our in vivo mir- transgenic mice data, by 14 weeks after transplantation, recipient mice transplanted with mir--expressing cells developed myeloid leukemia, as characterized by increased myeloid blasts in the peripheral blood, defective erythroid maturation and anemia, splenomegaly with the infiltration of myeloid blasts, and increased c-kit pos blasts in bone marrow (Figures S3 S3H). Taken together, these data strongly suggest that mir- can enhance HSPC function and contribute to leukemia development in vivo. mir- Directly Targets TET and Affects the Epigenetic Landscape of the Hematopoietic Compartment In Vivo To identify relevant molecular targets of mir-, we next undertook a bioinformatic analysis using TargetScan 6. ( (Lewis et al., 5), microrna.org ( (etel et al., 8), and mirase ( (Griffiths-Jones et al., 6). Among various potential targets, we focused on ten eleven translocation (TET) as it possesses critically conserved nucleotides indicative of a legitimate target (Figure S4A). We then confirmed a direct interaction of mir- with the 3 UTR region of the TET gene by luciferase reporter assay (Figure S4 and Song et al., 13). TET is a member of the TET methylcytosine dioxygenase family, which catalyzes the conversion of 5-methylcytosine (5-mC) to 5-hydroxymethylcytosine (5-hmC). TET proteins have been implicated in epigenetic reprogramming, embryonic stem cell maintenance, and early development (Ficz et al., 11; Ito et al., 1). Importantly, recurrent TET mutations have been identified in a variety of hematological malignancies including MDS, MPN, CMMoL, and AML (Abdel- Wahab et al., 9; Delhommeau et al., 9; Jankowska et al., 9; Tefferi et al., 9). It is noteworthy that the phenotypes elicited by mir- overexpression closely phenocopy the inactivation of Tet in the hematopoietic system both in vitro and in vivo (Li et al., 11; Moran-Crusio et al., 11; Quivoron et al., 11). It has also been documented that Tet expression is increased during hematopoietic differentiation, and conversely, that mir- is highly expressed in HSPCs while its expression declines in mature cells (Figure S4C, Moran-Crusio et al., 11). We therefore tested whether mir- could act as an authentic TET-targeting mirna in the hematopoietic compartment by utilizing our conditional transgenic mouse model. To this end, we measured Tet expression in the peripheral blood and bone marrow of ; or littermate mice at 3 weeks after pipc administration. Importantly, real-time qpcr and western blot analyses revealed a marked reduction in levels of Tet mrna and protein, respectively, in ; mice compared to littermate controls (Figures 5A, 5, 5E 5G and Figure S4D). Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc. 91
6 A i ii iii iv v vi vii viii mir F/+ ; C D E ; SSC-A c-kit % c-kit pos cells in Lin neg cells p <. % Disease free survival ; **p =.59 (n = 13) ; (n = 6) 4 6 F Time (weeks) ; ** G 1.% 3.8% 3.8% 8.4% 11.5% 3.8% 9.6% 3.1% 5.% 3.8% 1.6% 9.6% 1.8% 54.% 67.8% 3.8% 8.4% Myeloid leukemia T lymphoma MPN-like MDS-like Others (Normal) 8 months 11 months 15 months 3 months Figure 4. mir- Transgenic Mice Develop Primary Hematological Diseases (A and ) mir- transgenic mice develop MDS-like hematological syndromes. Representative smears of peripheral blood of 8-month-old mice after pipc administration are shown (A). Representative images of dysplastic erythroid cells (poikilocytosis, A; polychromasia, -i, arrowhead), dysplastic platelets (giant platelet, -i, arrow, -vii), dysplastic neutrophils (hypersegmented neutrophils, -ii-iv, arrows; a pseudo-pelger-huet anomaly, -v and vi) and dysplastic blasts (-viii arrows) in mir- transgenic mice are also shown. Scale bars, 5 mm (A) and 1 mm (). (C) c-kit pos immature blasts are increased in mir- transgenic mice. Representative flow cytometry data (left) and mean percentages ± SD of c-kit pos cells in Lin neg compartment (right) are shown (n = 3). (D) Disease-free survival of ; mice (n = 6) and littermate controls (n = 13). (legend continued on next page) 9 Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc.
7 On the basis of these observations, we then sought to determine whether mir--mediated TET inactivation is sufficient to impact the global epigenetic landscape in blood cells. We therefore analyzed 5-hmC and 5-mC levels in the genomic DNA of ; mice. Immunofluorescence and dot blot analyses revealed a drastic (more than -fold) reduction in 5-hmC levels and a concomitant increase in 5-mC levels in bone marrow of these mice (Figures 5C and 5D), suggesting that changes in an important epigenetic mark (e.g., 5-hmC) may contribute to the ability of mir- to affect hematopoiesis and leukemogenesis. To further understand the consequences of repression of TET by mir- in hematopoiesis, we next examined the effects of mir- overexpression on putative targets of TET (Kallin et al., 1; Ko et al., 1; Yamazaki et al., 1). A comprehensive real-time qpcr analysis revealed that the expression levels of a substantial number of putative Tet target genes, including Aim, Hal, Igbt, and Sp14, were markedly decreased in the HSC compartment (CD15 pos CD48 neg Flt3 neg CD34 neg KSL cells) purified from ; mice (Figure 5E and Figure S4E). Interestingly, absence in myeloma (AIM) has been reported to have a role in the reduction of cell proliferation by cell cycle arrest and to also be highly methylated in MDS, especially in CMMoL patients with TET mutations (Figueroa et al., 1; Patsos et al., 1; Yamazaki et al., 1). Therefore we hypothesized that its silencing via methylation of the promoter might provide a growth advantage to cancer cells. Additionally, polymorphisms of SP14 (SP14 nuclear body protein) have been found to correlate with chronic lymphoid leukemia, and its hypermethylation has been also demonstrated in CMMoL patients with TET mutations, and hence its hypermethylation may influence the risk of leukemogenesis (Di ernardo et al., 8; Ko et al., 1; Yamazaki et al., 1). Indeed, we confirmed that the expression of Aim and Sp14 was drastically reduced at the levels of mrna and protein in the bone marrow of ; mice compared to littermate controls, and this reduction was associated with an increase in promoter methylation (Figures 5F and 5G and Figure S4F). Taken together, these results suggest that mir- represses TET expression and thereby can remodel the epigenetic landscape with global changes in 5-hmC levels and alteration in the expression of putative TET target genes including AIM and SP14. mir- Enhances Stem Cell Function and Triggers Hematological Transformation through Repression of TET Next, we explored the relevance of the crosstalk between mir- and TET in hematopoiesis and hematological malignancies. To test whether TET directly contributes to the function of mir- in the hematopoietic compartment, we first infected KSL cells isolated from wild-type mice with a retroviral vector encoding mir- and GFP. After the resorting, GFP + KSL cells were additionally infected with a TET-expressing lentiviral particle. In vitro colony replating and LTC-IC assays demonstrated that the phenotypes caused by mir- overexpression in hematopoietic compartment are potently suppressed by ectopic expression of TET (Figures S4G S4J). Notably, an in vivo transplantation assay revealed that ectopic expression of TET leads to survival advantages for recipient mice transplanted with mir--expressing KSL cells (Figure S4K). To further examine this interaction, we purified KSL cells from mir- transgenic mice and infected them with a retroviral vector encoding Cre recombinase and GFP. After the resorting of GFP + KSL cells, cells were additionally infected with a TET- expressing lentiviral particle and the resulting phenotypes were analyzed. In vitro colony replating and LTC-IC analyses demonstrated that the oncogenic function of mir- was antagonized by ectopic expression of TET (Figures 6A and 6). Notably, when KSL cells of mice were simultaneously coinfected with a Cre recombinase construct and a TET-expressing construct, ectopic expression of TET more strikingly impaired the replating potential of GFP + KSL cells (Figures S5A and S5). In line with these observations, an in vivo transplantation assay revealed significant survival advantages in recipient mice transplanted with KSL cells coinfected with Cre and TET compared to those with KSL cells coinfected with Cre and control vector (Figure 6C). Importantly, the positive survival effect drawn by ectopic expression of TET was more pronounced in secondary transplantation (Figure S5C). Finally, we purified KSL cells from mir- transgenic mice after pipc administration, infected them with a TET-expressing lentiviral particle, and evaluated the resulting phenotypes (Figure 6D). We found that all the phenotypes elicited by an elevation of mir- in vitro and in vivo in hematopoietic compartment, including repression of the expression of Aim and Sp14 in bone marrow, were also significantly suppressed by ectopic expression of TET (Figures 6E 6H and Figure S5D). Importantly, when we purified KSL cells from primary mir- transgenic mice and infected them with TET followed by in vivo transplantation together with competitor cells, ectopic expression of TET delayed the onset of hematological disorder and was accompanied by significant advantages in disease-free survival (Figure S5E). Taken together, these data suggest that TET is one of the major targets responsible for the mir- proto-oncogenic function in hematopoiesis and the development of hematological malignancies. mir- Decoying Offers Therapeutic Opportunities and Its Overexpression Correlates with the Silencing of TET Protein in MDS and AML Patients Next, we investigated whether the mir-/tet interaction may offer a therapeutic opportunity for the treatment of hematological malignancies. We therefore tested whether inhibition of mir- affects TET expression and activity, as well as the biology of (E and F) Representative lethal hematological syndromes observed in mir- transgenic mice. Representative images of spleens (E, left) and H&E staining (E, right) are shown. Scale bars, 1 mm. Representative smears of peripheral blood of mir- transgenic mice (6 months old) with increased myeloid blasts (F) are also shown. Scale bars, mm. (G) Pie charts representing the disease spectrum in ; mice at the indicated ages (n = 6). MPN, myeloproliferative neoplasm. All error bars indicate ± SD. See also Figure S3. Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc. 93
8 A mir- level (Fold increases) 6 4 p <. Peripheral lood Tet mrna level (Fold increases) p =.411 mir- level (Fold increases) 3 1 p =.3 one marrow Tet mrna level (Fold increases) p =.146 C ; 5-hmC 5-mC DAPI % cells with high intensity of 5-hmC p =.381 D 5ng gdna fold dilution ; -5-hmC E Fold expression (Log) Tet p <.1 Fold expression (Log) Aim p <.1 Fold expression (Log) Sp14 p <.1 ; ; ; Fold expression (Log) Igbt p <.1 Fold expression (Log) Hal p <.1 Fold expression (Log) Ly6c1 p =.14 F Tet mrna level (Fold increases) p =.5 p =.5 p =. Sp14 mrna level (Fold increases) ; 1.5 Aim mrna level (Fold increases) ; 1.5 G ; Tet Aim Sp14 Actin Figure 5. mir- Acts as an Epigenetic Modifier by Directly Targeting TET (A and ) A reduction in the levels of Tet mrna in mir- transgenic mice. Expression levels of mir- (left) and Tet mrna (right) in mononuclear cells from peripheral blood (A) and bone marrow (M) () of control or ; mice 3 weeks after pipc administration were determined by real-time qpcr (n = 6). (C) mir- expression results in a significant reduction in the levels of 5-hmC in the hematopoietic compartment. 5-hmC and 5-mC were evaluated by immunofluorescence analysis in M cells isolated from ; mice and littermate controls 3 weeks after pipc administration (left). Cells expressing high levels of 5-hmC show low levels of 5-mC (arrow) and conversely, cells expressing low levels of 5-hmC exhibit high levels of 5-mC (arrowhead). ar graph depicts mean percentages ± SD of cells expressing high levels of 5-hmC (n = 3) (right). Scale bars, 1 mm. (legend continued on next page) 94 Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc.
9 leukemias. To this end, we inhibited mir- in human leukemia cell lines, K56 and U937, both of which express relatively high levels of mir- (Figure S5F, Wang et al., 1), by using a mir- retroviral sponge or a custom-made locked nucleic acid (LNA; Petersen and Wengel, 3) mir- decoy as the mir- sponge. Critically, inhibition of mir- in human leukemic cells resulted in a significant reduction in cell proliferation and an elevation of the expression of TET and its targets, AIM and SP14 (Figures 6I and 6J and Figures S5G S5I). It is worth noting that the U937 cell line harbors phosphatase and tensin homolog (PTEN) mutant with premature termination of coding sequence (Liu et al., ). Hence in this setting the effects observed upon mir- decoying are not mediated by the ability of mir- to downregulate PTEN expression. In full agreement with these observations, an in vitro colony replating assay revealed that the inhibition of mir- by a mir- retroviral sponge in KSL cells purified from mir- transgenic mice led to a reduction in their colony-forming capability (Figure S5J). Taken together, these data provide a rationale for the therapeutic potential of targeting mir- with LNA mir- inhibitors in the treatment of hematological malignancies. The pathological roles of TET in myeloid malignancies have been previously highlighted as its mutations are widely observed in myeloid malignancies and MDS patients. Most of these earlier studies, however, were limited to mutation analysis and found little relationship between the progression of MDS to AML and TET expression levels, although the phenotypes of Tet knockout mice gave indications to the contrary (Moran-Crusio et al., 11; Quivoron et al., 11). Likewise, emerging evidence demonstrated no significant prognostic association between TET mutations in MDS patients and WHO subtypes, the International Prognostic Scoring System (IPSS) score, cytogenetic status, or transformation to AML (Kosmider et al., 9; Smith et al., 1). However, on the basis of our data we hypothesized that a mir- -dependent reduction in the levels of TET might have been overlooked and could play a key role in the development of myeloid malignancies. To test this hypothesis, we investigated a large cohort of patients with MDS by an immunohistochemical analysis. Strikingly, this analysis revealed that 6% of 17 MDS patients analyzed displayed a reduction in the levels of TET (36% of 17 MDS patients show Score 1 and 4% show Score ) and that this reduction was directly correlated with poor survival rates of patients (Figures 7A and 7 and Figures S6A S6D). Importantly, the percentage of blasts distributed in each WHO category of MDS stage was not directly associated with expression level of TET, but a significant correlation was found between TET expression and poor survival rates within each WHO classification, as well as among MDS patients harboring a normal karyotype, suggesting that the poorer survival expectancy linked to TET downregulation does not simply reflect confounding factors, such as blast count and cytogenetic karyotype (Figure 7C and Figures S6E and S6F). Together, these results suggest that the contribution of TET to the pathogenesis of hematological malignancies extends far beyond the initial impact of its mutations. Importantly, combined in situ hybridization and immunohistochemical analyses revealed that mir- expression was directly anticorrelated with the levels of TET in a large-cohort data set of MDS patients (n = 17) (Pearson s r =.47, p = ): 8% of MDS patients that showed the reduced levels of TET (Score 1) also exhibited high mir- levels (Score 3) (Figure 7D and Figure S6G and see also Figure 1A). Furthermore, because our in vivo analysis demonstrated that mir- triggers overt leukemia (Figure 4G), we investigated the mir-/tet interactive relationship in AML with multiple lineage dysplasia (MLD) (n = 18). Our combined analyses of in situ hybridization and immunohistochemistry revealed a clear anticorrelation between mir- expression and the levels of TET (Pearson s r =.75, p = ); in addition,.% of AML with MLD patients showing the reduced levels of TET (Score 1) displayed a high expression of mir- (Score 3) (Figure 7E). Western blot and real-time qpcr analyses also corroborated a relationship between mir- and TET in primary AML patients (Figure S6H). Finally, we confirmed these findings by analyzing the expression levels of mir- in a very large cohort of AML patients from a previously reported real-time qpcr database (Jongen-Lavrencic et al., 8). Here mir- was found highly expressed in 58.1% of 14 AML patient samples compared to normal bone marrow from healthy donors (p =.8, Figure 7F). Taken together, these data strongly suggest that aberration of the mir--tet regulatory network is one of the common events in hematopoietic malignancies. DISCUSSION The findings presented in this study point to a number of important conclusions. The first of these is that mir- is a powerful regulator of HSPC maintenance and self-renewal. These effects are so pronounced that mir--expressing HSPCs out-competed their wild-type counterparts in all the assays that we performed in vivo as well as in vitro. Importantly, in so doing mir- also skews hematopoietic differentiation, mainly toward myeloid compartment. We have also identified mir- as a key determinant of the pathogenesis of both MDS and hematological malignancies. Remarkably, mir- plays a role in the initiation of MDS as well as full-blown leukemia; hence it exerts a bona fide protooncogenic activity. MDS is a genetically heterogeneous disease and we are only now beginning to fully appreciate its diversity. (D) mir- expression leads to a significant reduction in global 5-hmC expression levels in the genome in M cells. 5-hmC levels were analyzed by quantitative dot blot assay with genomic DNA purified from M cells of ; or littermate control mice. (E) Plots depict relative expression levels of putative Tet target genes (Aim, Sp14, Igbt, and Hal) in CD15 pos CD48 neg Flt-3 neg CD34 neg KSL cells of ; mice and littermate controls 3 weeks after pipc administration (n = 4). Ly6c1 and Actb were used as a Tet unrelated gene control and an internal control, respectively. (F and G) Repression of putative downstream genes of Tet in mir- transgenic mice. Expression levels of Tet, Sp14, and Aim mrnas (F) or proteins (G)in M of ; mice or littermate controls 3 weeks after pipc administration were evaluated (n = 3). All error bars indicate ± SD. See also Figures S4A S4F. Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc. 95
10 A Colonies/5 KSL cells C 1 Disease free survival (%) F 8 4 % survival c-kit ; Mx1 Cre H * * ** Number of re-plating Time (days) ** N.D N.D N.D N.D D 1 pipc weeks EE 8 ET ; or Littermate CE control Sort KSL cells 6 ( months CT old) 4 Infection of TET Cont. + Empty vec. (n=7) Cont. + TET (n=7) ** Cre + Empty vec. (n=9) Sort KSL cells Cre+ TET (n=9) **p =.5 Colony assay, LTC-IC MT with competitor Ly45.1 MNCs Time ; Mx1 Cre CD45.1 _Cont. vec.+ Empty vec. _Cont. vec.+ TET _Cre + Empty vec. _Cre +TET (n = 3), *p <.1, **p <.1 ** Sca-1 CD45. TET 8.% 3.3% TET 7.9% 47.% TET 47.7% 9.5% TET 73.% 55.8% ** I % KSL cells in Lin neg MNCs ** Sca Cre c-kit 31.% (3.6±.7% 64.6% (67.±.6% ** + +TET ;+ ;+TET p =.3 TET AIM SP14 Actin +TET 3.9% (8.4± 4.3% Cre+TET 5.6% (48.6± 4.7% E G Colonies/5 KSL cells J Cell growth (x1 4 ) Colonies/1x1 3 KSL cells Colonies/5 KSL cells 5 _Cont. vec. + Empty vec. _Cont. vec. + TET _Cre + Empty vec. _Cre +TET (n = 3), **p <.1 1 ** ** Weeks after co-culture Cont. Sponge mir- Sponge ***p <.1 +Empty vec. +TET ;+Empty vec. ;+TET p =.18 p =. N.D 1 3 Number of re-plating + +TET ;+ ;+TET p =.7 p <.1 6 Weeks of co-culture *** p =. *** Time (days) *** Figure 6. mir-/tet Regulatory Network Affects HSC Function and Hematological Transformation (A and ) Ectopic expression of TET reduces the colony-forming capacity of mir--expressing HSPCs. The sorted KSL cells from mice were infected with Cre-GFP or GFP control vector. GFP + KSL cells were resorted and infected with empty vector or TET-expressing lentiviral particles. Cells were then incubated in semisolid medium. Colony replating assay was performed and the resulting colonies were counted at the indicated replatings (n = 3) (A). Some of TET infected cells were also subjected to LTC-IC assay. Representative flow cytometry data of the positivity of c-kit/sca-1 in Lin neg -gated cells weeks after coculture with stromal cells and mean percentages ± SD of KSL cells in Lin neg (in brackets) are shown (n = 3) (, left). Colony-forming capacities were also determined at the indicated weeks after coculture with stromal cells (n = 3) (, right). (legend continued on next page) 96 Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc.
11 This study will therefore help in the reclassification of subtypes of MDS, and possibly AML, on the basis of mir- expression. Furthermore, our comprehensive analysis of MDS patients has identified TET protein downregulation as a common event in hemopoietic malignancy (35.5% of total MDS patient samples, and.% of AML samples with MLD, with most of those patients exhibiting high expression of mir-) and a factor in poor prognosis, findings which directly impact the management and therapeutic decisions for patients with myeloid malignancies. Our findings thus imply that the contribution of TET to the pathogenesis of myeloid malignancies could be related to more than its mutations and identify the deregulation of the mir--tet pathway as one of the most frequent events in hematological malignancies. Importantly, they also provide a compelling rationale for targeted therapies that impact the mechanisms of regulation responsible for the control of TET levels (e.g., through mir- decoying). We show that mir- negatively regulates the expression of TET and that its overexpression closely phenocopies, both in vitro and in vivo, many of the characteristics observed upon inactivation of TET (Figure 7G). Extensive mouse modeling efforts support these similarities both in our current study and in other Tet-related studies (Li et al., 11; Moran-Crusio et al., 11; Quivoron et al., 11). Furthermore, our comprehensive analyses of a large cohort of MDS and AML patients likewise have demonstrated this antagonistic crosstalk. mir- also appears to exert a tumor-promoting role in other tissues, including mammary glands, through its ability to suppress the expression of other TET family members such as TET1 and TET3 (Figure S4D and Song et al., 13). Thus, mir- contributes to inactivation of TET and other TET family members in tumorigenesis, representing a tumorigeneic pathway in addition to the more familiar ones of TET and TET family mutations and deletions. We previously demonstrated that mir- also targets the PTEN tumor suppressor (Poliseno et al., 1). Pten loss has also been implicated in the pathogenesis of hematological malignancies (Yilmaz et al., 6; Zhang et al., 6). However, mir- through TET regulation can bestow to hemopoietic cells further competitive advantage as also supported by the fact that mir- decoying suppresses proliferation even in a PTEN mutant setting (Figure S5I). This may in turn explain the potent proto-oncogenic activity of mir-. Indeed, there are several intriguing phenotypical differences between Pten F/F ; and ; mouse models that could illuminate a unique and powerful role exerted by mir- in leukemogenesis. First, mir- increased the ability of HSCs to repopulate, which was then followed by leukemia development, whereas loss of Pten resulted in the exhaustion of normal HSCs. In addition, while Pten loss induces short-term expansion in HSCs through excessive cell cycle entry followed by exhaustion, no significant alteration in the stem cell compartment was observed at 3 weeks after the introduction of mir- (Figure S7). Additionally, while loss of Pten in HSCs is known to lead to MPN-like disease followed by leukemia development, hematological dysplasia with ineffective hematopoiesis is one of the main phenotypes caused by mir- expression, with bicytopenia or pancytopenia observed in mir- transgenic mice. Furthermore, although HSCs from Pten F/+ ; mice are known to be transplantable, the recipients do not develop hematopoietic syndromes (Yilmaz et al., 6). In contrast, recipient mice transplanted with HSCs purified from ; mice developed aberrant hematopoiesis followed by MDS and leukemia. Hence, the ability of mir- to concomitantly downregulate TET and PTEN provides it a unique mode of action and confers on it the ability to overcome PTEN-loss-driven stem cell exhaustion while favoring MDS development and leukemogenesis. This in turn raises the possibility that concomitant silencing of TET and PTEN by mir- could represent a powerful event underlying the pathogenesis of human cancer, as it may overcome the fail-safe mechanisms elicited by loss of PTEN (erger et al., 11). Finally, since the technology to inhibit mirnas for therapy is rapidly evolving (Elmén et al., 8; Stenvang et al., 8), this will impact treatment options for a range of diseases and disorders in the years to come. Indeed, LNA-based mirna decoying has already come of age for the treatment of hepatitis C (Lanford et al., 1) and may prove very effective for the treatment of (C) TET attenuates the hematopoietic malignancies induced by mir- overexpression. KSL cells sorted from mice were infected with Cre-GFP or GFP control vector before TET infection, and 1,5 GFP + KSL cells were transplanted into recipient mice with Ly45.1 competitor bone marrow mononuclear cells (M MNCs). Disease-free survival of recipient mice was examined by Kaplan-Meier survival curves. Log-rank test was used to generate p values. (D) Overview of the experimental design for introduction of TET into KSL cells from mir- transgenic mice. KSL cells purified from mir- transgenic mice were subjected to infection with TET-expressing vector, and their characteristics were evaluated in vivo and in vitro. (E) Colony-forming capacity of mir- transgenic progenitor cells is attenuated by ectopic expression of TET. Two weeks after pipc administration, sorted KSL cells from ; mice were infected with TET-expressing vector and resorted KSL cells were then subjected to incubation in semisolid medium. The resulting colony numbers were scored in three independent littermate pairs in the indicated platings (n = 3). N.D., nondetectable. (F and G) Ectopic expression of TET causes a reduction in LTC-IC capacity of mir- transgenic progenitor cells. TET-infected KSL cells from ;Mx1- Cre mice or littermate controls, as shown in Figure 6D, were cocultured with stromal cells for the indicated weeks. Maintained KSL cells were evaluated weeks after coculture (n = 3) (F). At the indicated times after coculture, the capacity of colony formation was also determined in semisolid medium (n = 3) (G). (H) Increased reconstitution capacity of KSL cells of mir- transgenic mice is reduced by ectopic expression of TET. The sorted KSL cells from ;Mx1- Cre mice or littermate controls were infected with TET-expressing vector KSL cells were resorted and subjected to bone marrow transplantation with competitor M MNCs. Representative flow cytometry data of the CD45.1/CD45. positivity at 6 weeks after transplantation are shown. (I) Inhibition of mir- increases the expression of TET and its putative target genes in human leukemic cells. K56 cells were infected with the vector encoding mir- sponge or control sponge, and 48 hr after the infection, cell lysates were subjected to immunoblot analysis for the indicated proteins. (J) Inhibition of mir- suppresses the proliferation of human leukemic cells. K56 cells were infected with the vector encoding mir- sponge or control sponge. Forty-eight hours after puromycin selection, cells were incubated for seven days. Optical densities of the cells were determined at the indicated times (n = 3). All error bars indicate ± SD. See also Figures S4G S4K and S5. Cell Stem Cell 13, 87 11, July 3, 13 ª13 Elsevier Inc. 97
Nature Immunology: doi: /ni Supplementary Figure 1. Huwe1 has high expression in HSCs and is necessary for quiescence.
 Supplementary Figure 1 Huwe1 has high expression in HSCs and is necessary for quiescence. (a) Heat map visualizing expression of genes with a known function in ubiquitin-mediated proteolysis (KEGG: Ubiquitin
Supplementary Figure 1 Huwe1 has high expression in HSCs and is necessary for quiescence. (a) Heat map visualizing expression of genes with a known function in ubiquitin-mediated proteolysis (KEGG: Ubiquitin
Hematology Unit Lab 2 Review Material
 Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
Objectives Hematology Unit Lab 2 Review Material - 2018 Laboratory Instructors: 1. Assist students during lab session Students: 1. Review the introductory material 2. Study the case histories provided
MicroRNA-29a Reveals Oncogenic Role on Myeloid Malignancies by Regulating DNMT3A
 MicroRNA-29a Reveals Oncogenic Role on Myeloid Malignancies by Regulating DNMT3A Heba Alkhatabi, PhD Assistant Professor Department of Medical Laboratory Collage of Applied Medical science King Abdul Aziz
MicroRNA-29a Reveals Oncogenic Role on Myeloid Malignancies by Regulating DNMT3A Heba Alkhatabi, PhD Assistant Professor Department of Medical Laboratory Collage of Applied Medical science King Abdul Aziz
September 20, Submitted electronically to: Cc: To Whom It May Concern:
 History Study (NOT-HL-12-147), p. 1 September 20, 2012 Re: Request for Information (RFI): Building a National Resource to Study Myelodysplastic Syndromes (MDS) The MDS Cohort Natural History Study (NOT-HL-12-147).
History Study (NOT-HL-12-147), p. 1 September 20, 2012 Re: Request for Information (RFI): Building a National Resource to Study Myelodysplastic Syndromes (MDS) The MDS Cohort Natural History Study (NOT-HL-12-147).
SUPPLEMENTARY INFORMATION
 a. Smo+/+ b. Smo+/+ 5.63 5.48 c. Lin- d. e. 6 5 4 3 Ter119 Mac B T Sca1 Smo+/+ 25 15 2 o BMT 2 1 5 * Supplementary Figure 1: Deletion of Smoothened does not alter the frequency of hematopoietic lineages
a. Smo+/+ b. Smo+/+ 5.63 5.48 c. Lin- d. e. 6 5 4 3 Ter119 Mac B T Sca1 Smo+/+ 25 15 2 o BMT 2 1 5 * Supplementary Figure 1: Deletion of Smoothened does not alter the frequency of hematopoietic lineages
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression
 Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Myelodysplastic Syndromes: Hematopathology. Analysis of SHIP1 as a potential biomarker of Disease Progression Carlos E. Bueso-Ramos, M.D., Ph.D Department of Hematopathology The University of Texas M.
Nature Immunology: doi: /ni.3412
 Supplementary Figure 1 Gata1 expression in heamatopoietic stem and progenitor populations. (a) Unsupervised clustering according to 100 top variable genes across single pre-gm cells. The two main cell
Supplementary Figure 1 Gata1 expression in heamatopoietic stem and progenitor populations. (a) Unsupervised clustering according to 100 top variable genes across single pre-gm cells. The two main cell
Supplementary Figure 1. Successful excision of genes from WBM lysates and
 Supplementary Information: Supplementary Figure 1. Successful excision of genes from WBM lysates and survival of mice with different genotypes. (a) The proper excision of Pten, p110α, p110α and p110δ was
Supplementary Information: Supplementary Figure 1. Successful excision of genes from WBM lysates and survival of mice with different genotypes. (a) The proper excision of Pten, p110α, p110α and p110δ was
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature12215 Supplementary Figure 1. The effects of full and dissociated GR agonists in supporting BFU-E self-renewal divisions. BFU-Es were cultured in self-renewal medium with indicated GR
doi:10.1038/nature12215 Supplementary Figure 1. The effects of full and dissociated GR agonists in supporting BFU-E self-renewal divisions. BFU-Es were cultured in self-renewal medium with indicated GR
Nature Genetics: doi: /ng Supplementary Figure 1
 Supplementary Figure 1 MSI2 interactors are associated with the riboproteome and are functionally relevant. (a) Coomassie blue staining of FLAG-MSI2 immunoprecipitated complexes. (b) GO analysis of MSI2-interacting
Supplementary Figure 1 MSI2 interactors are associated with the riboproteome and are functionally relevant. (a) Coomassie blue staining of FLAG-MSI2 immunoprecipitated complexes. (b) GO analysis of MSI2-interacting
sequences of a styx mutant reveals a T to A transversion in the donor splice site of intron 5
 sfigure 1 Styx mutant mice recapitulate the phenotype of SHIP -/- mice. (A) Analysis of the genomic sequences of a styx mutant reveals a T to A transversion in the donor splice site of intron 5 (GTAAC
sfigure 1 Styx mutant mice recapitulate the phenotype of SHIP -/- mice. (A) Analysis of the genomic sequences of a styx mutant reveals a T to A transversion in the donor splice site of intron 5 (GTAAC
Hematopoiesis. - Process of generation of mature blood cells. - Daily turnover of blood cells (70 kg human)
 Hematopoiesis - Process of generation of mature blood cells - Daily turnover of blood cells (70 kg human) 1,000,000,000,000 total cells 200,000,000,000 red blood cells 70,000,000,000 neutrophils Hematopoiesis
Hematopoiesis - Process of generation of mature blood cells - Daily turnover of blood cells (70 kg human) 1,000,000,000,000 total cells 200,000,000,000 red blood cells 70,000,000,000 neutrophils Hematopoiesis
Molecular Characterization of Leukemia Stem Cell Development. Scott A. Armstrong MD, Ph.D.
 Molecular Characterization of Leukemia Stem Cell Development Scott A. Armstrong MD, Ph.D. Normal and Leukemic Hierarchies NORMAL HSC (SRC) Myeloid progenitor LTC-IC CFU AML LSC (SL-IC) Leukemic LTC-IC
Molecular Characterization of Leukemia Stem Cell Development Scott A. Armstrong MD, Ph.D. Normal and Leukemic Hierarchies NORMAL HSC (SRC) Myeloid progenitor LTC-IC CFU AML LSC (SL-IC) Leukemic LTC-IC
Molecular Markers. Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC
 Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Molecular Markers Marcie Riches, MD, MS Associate Professor University of North Carolina Scientific Director, Infection and Immune Reconstitution WC Overview Testing methods Rationale for molecular testing
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED
 Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
Done By : WESSEN ADNAN BUTHAINAH AL-MASAEED Acute Myeloid Leukemia Firstly we ll start with this introduction then enter the title of the lecture, so be ready and let s begin by the name of Allah : We
PREPARED FOR: U.S. Army Medical Research and Materiel Command Fort Detrick, Maryland
 AD Award Number: W81XWH-13-1-0057 TITLE: Role of TIRAP in Myelodysplastic Syndromes PRINCIPAL INVESTIGATOR: Linda Ya-ting Chang CONTRACTING ORGANIZATION: British Columbia Cancer Agency Branch Vancouver,
AD Award Number: W81XWH-13-1-0057 TITLE: Role of TIRAP in Myelodysplastic Syndromes PRINCIPAL INVESTIGATOR: Linda Ya-ting Chang CONTRACTING ORGANIZATION: British Columbia Cancer Agency Branch Vancouver,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls
 Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
Myelodysplastic Syndromes: Everyday Challenges and Pitfalls Kathryn Foucar, MD kfoucar@salud.unm.edu Henry Moon lecture May 2007 Outline Definition Conceptual overview; pathophysiologic mechanisms Incidence,
University of Miami Miller School of Medicine, Miami, FL 33136, USA, 3 State Key Laboratory
 Supplementary File ASXL1 plays an important role in erythropoiesis Hui Shi 1,2,3, Shohei Yamamoto 1,2,4, Mengyao Sheng 3, Jie Bai 3, Peng Zhang 1,2, Runze Chen 1,2, Shi Chen 1,2, Lihong Shi 3, Omar Abdel-Wahab
Supplementary File ASXL1 plays an important role in erythropoiesis Hui Shi 1,2,3, Shohei Yamamoto 1,2,4, Mengyao Sheng 3, Jie Bai 3, Peng Zhang 1,2, Runze Chen 1,2, Shi Chen 1,2, Lihong Shi 3, Omar Abdel-Wahab
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms
 Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Myelodysplastic syndrome (MDS) & Myeloproliferative neoplasms Myelodysplastic syndrome (MDS) A multipotent stem cell that can differentiate into any of the myeloid lineage cells (RBCs, granulocytes, megakaryocytes)
Meeting Report. From December 8 to 11, 2012 at Atlanta, GA, U.S.A
 Meeting Report Affiliation Department of Transfusion Medicine and Cell Therapy Name Hisayuki Yao Name of the meeting Period and venue Type of your presentation Title of your presentation The 54 th Annual
Meeting Report Affiliation Department of Transfusion Medicine and Cell Therapy Name Hisayuki Yao Name of the meeting Period and venue Type of your presentation Title of your presentation The 54 th Annual
Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data
 Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Instructions for Myelodysplasia/Myeloproliferative Neoplasms (MDS/MPN) Post-HCT Data (Form 2114) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the Myelodysplasia/Myeloproliferative
Nature Genetics: doi: /ng.3812
 Nature Genetics: doi:10.1038/ng.3812 Supplementary Figure 1 Smarcd2-knockout mice die perinatally with impaired energy homeostasis. (a) Generation of the Smarcd2 conditional knockout allele. Deletion of
Nature Genetics: doi:10.1038/ng.3812 Supplementary Figure 1 Smarcd2-knockout mice die perinatally with impaired energy homeostasis. (a) Generation of the Smarcd2 conditional knockout allele. Deletion of
SUPPLEMENTARY INFORMATION GENOTOXICITY. In vitro Genotoxicity Studies
 SUPPLEMENTARY INFORMATION GENOTOXICITY In vitro Genotoxicity Studies The in vitro immortalisation (IVIM) assay relies on the induction of a survival advantage by insertional activation of cellular proto-oncogenes,
SUPPLEMENTARY INFORMATION GENOTOXICITY In vitro Genotoxicity Studies The in vitro immortalisation (IVIM) assay relies on the induction of a survival advantage by insertional activation of cellular proto-oncogenes,
Juvenile Myelomonocytic Leukemia (JMML)
 Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
Juvenile Myelomonocytic Leukemia (JMML) JMML: Definition Monoclonal hematopoietic disorder of childhood characterized by proliferation of the granulocytic and monocytic lineages Erythroid and megakaryocytic
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature11095 Supplementary Table 1. Summary of the binding between Angptls and various Igdomain containing receptors as determined by flow cytometry analysis. The results were summarized from
doi:10.1038/nature11095 Supplementary Table 1. Summary of the binding between Angptls and various Igdomain containing receptors as determined by flow cytometry analysis. The results were summarized from
Heme 9 Myeloid neoplasms
 Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
Heme 9 Myeloid neoplasms The minimum number of blasts to diagnose acute myeloid leukemia is 5% 10% 20% 50% 80% AML with the best prognosis is AML with recurrent cytogenetic abnormality AML with myelodysplasia
The role of DNMT3A and HOXA9 hypomethylation in acute myeloid leukemia (AML)
 Campbell Drohan BIOL 463 December 2016 The role of DNMT3A and HOXA9 hypomethylation in acute myeloid leukemia (AML) Introduction Epigenetic modifications of DNA and histones are key to gene regulation
Campbell Drohan BIOL 463 December 2016 The role of DNMT3A and HOXA9 hypomethylation in acute myeloid leukemia (AML) Introduction Epigenetic modifications of DNA and histones are key to gene regulation
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION Pleiotrophin Regulates the Expansion and Regeneration of Hematopoietic Stem Cells Heather A Himburg 1, Garrett G Muramoto 1 *, Pamela Daher 1*, Sarah K Meadows 1, J. Lauren Russell
SUPPLEMENTARY INFORMATION Pleiotrophin Regulates the Expansion and Regeneration of Hematopoietic Stem Cells Heather A Himburg 1, Garrett G Muramoto 1 *, Pamela Daher 1*, Sarah K Meadows 1, J. Lauren Russell
Objectives. Morphology and IHC. Flow and Cyto FISH. Testing for Heme Malignancies 3/20/2013
 Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Molecular Markers in Hematologic Malignancy: Ways to locate the needle in the haystack. Objectives Review the types of testing for hematologic malignancies Understand rationale for molecular testing Marcie
Stem cells: units of development and regeneration. Fernando D. Camargo Ph.D. Whitehead Fellow Whitehead Institute for Biomedical Research.
 Stem cells: units of development and regeneration Fernando D. Camargo Ph.D. Whitehead Fellow Whitehead Institute for Biomedical Research Concepts 1. Embryonic vs. adult stem cells 2. Hematopoietic stem
Stem cells: units of development and regeneration Fernando D. Camargo Ph.D. Whitehead Fellow Whitehead Institute for Biomedical Research Concepts 1. Embryonic vs. adult stem cells 2. Hematopoietic stem
X P. Supplementary Figure 1. Nature Medicine: doi: /nm Nilotinib LSK LT-HSC. Cytoplasm. Cytoplasm. Nucleus. Nucleus
 a b c Supplementary Figure 1 c-kit-apc-eflu780 Lin-FITC Flt3-Linc-Kit-APC-eflu780 LSK Sca-1-PE-Cy7 d e f CD48-APC LT-HSC CD150-PerCP-cy5.5 g h i j Cytoplasm RCC1 X Exp 5 mir 126 SPRED1 SPRED1 RAN P SPRED1
a b c Supplementary Figure 1 c-kit-apc-eflu780 Lin-FITC Flt3-Linc-Kit-APC-eflu780 LSK Sca-1-PE-Cy7 d e f CD48-APC LT-HSC CD150-PerCP-cy5.5 g h i j Cytoplasm RCC1 X Exp 5 mir 126 SPRED1 SPRED1 RAN P SPRED1
HEMATOLOGIC MALIGNANCIES BIOLOGY
 HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
HEMATOLOGIC MALIGNANCIES BIOLOGY Failure of terminal differentiation Failure of differentiated cells to undergo apoptosis Failure to control growth Neoplastic stem cell FAILURE OF TERMINAL DIFFERENTIATION
Supplement Material. Spleen weight (mg) LN cells (X106) Acat1-/- Acat1-/- Mouse weight (g)
 Supplement Material A Spleen weight (mg) C Mouse weight (g) 1 5 1 2 9 6 3 2 5 2 1 5 Male LN cells (X16) 4 ** ** Female B 3 2 1 Supplemental Figure I. Spleen weight (A), Inguinal lymph node (LN) cell number
Supplement Material A Spleen weight (mg) C Mouse weight (g) 1 5 1 2 9 6 3 2 5 2 1 5 Male LN cells (X16) 4 ** ** Female B 3 2 1 Supplemental Figure I. Spleen weight (A), Inguinal lymph node (LN) cell number
RUNX1 and FPD/AML Translational Research. The Leukemia and Lymphoma Society / Babich Family Foundation Partnership. September 2016
 www.lls.org www.runx1.com RUNX1 and FPD/AML Translational Research The Leukemia and Lymphoma Society / Babich Family Foundation Partnership September 2016 Prepared by L. Greenberger, PhD Chief Scientific
www.lls.org www.runx1.com RUNX1 and FPD/AML Translational Research The Leukemia and Lymphoma Society / Babich Family Foundation Partnership September 2016 Prepared by L. Greenberger, PhD Chief Scientific
CHALLENGING CASES PRESENTATION
 CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
CHALLENGING CASES PRESENTATION Michael C. Wiemann, MD, FACP Program Co-Chair and Vice President Indy Hematology Education President, Clinical St. John Providence Physician Network Detroit, Michigan 36
Haematopoietic stem cells
 Haematopoietic stem cells Neil P. Rodrigues, DPhil NIH Centre for Biomedical Research Excellence in Stem Cell Biology Boston University School of Medicine neil.rodrigues@imm.ox.ac.uk Haematopoiesis: An
Haematopoietic stem cells Neil P. Rodrigues, DPhil NIH Centre for Biomedical Research Excellence in Stem Cell Biology Boston University School of Medicine neil.rodrigues@imm.ox.ac.uk Haematopoiesis: An
MicroRNAs: the primary cause or a determinant of progression in leukemia?
 MicroRNAs: the primary cause or a determinant of progression in leukemia? The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters. Citation
MicroRNAs: the primary cause or a determinant of progression in leukemia? The MIT Faculty has made this article openly available. Please share how this access benefits you. Your story matters. Citation
IKK-dependent activation of NF-κB contributes to myeloid and lymphoid leukemogenesis by BCR-ABL1
 Supplemental Figures BLOOD/2014/547943 IKK-dependent activation of NF-κB contributes to myeloid and lymphoid leukemogenesis by BCR-ABL1 Hsieh M-Y and Van Etten RA Supplemental Figure S1. Titers of retroviral
Supplemental Figures BLOOD/2014/547943 IKK-dependent activation of NF-κB contributes to myeloid and lymphoid leukemogenesis by BCR-ABL1 Hsieh M-Y and Van Etten RA Supplemental Figure S1. Titers of retroviral
Hematology 101. Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD
 Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
Hematology 101 Blanche P Alter, MD, MPH, FAAP Clinical Genetics Branch Division of Cancer Epidemiology and Genetics Bethesda, MD Hematocrits Plasma White cells Red cells Normal, Hemorrhage, IDA, Leukemia,
SUPPLEMENTARY INFORMATION doi: /nature12026
 doi:1.138/nature1226 a 4 35 3 MCSF level (pg/ml) 25 2 15 1 5 1h3 3h 5h 7h 15h 24h b MPP (CD135 KSL) HSC (CD34 CD15 KSLF) c % 4 ** LPS 3 GFP pos cells 2 PU.1 GFP LPS 1 FSCA Ctl NI 24h LPS Sup.Fig.1 Effect
doi:1.138/nature1226 a 4 35 3 MCSF level (pg/ml) 25 2 15 1 5 1h3 3h 5h 7h 15h 24h b MPP (CD135 KSL) HSC (CD34 CD15 KSLF) c % 4 ** LPS 3 GFP pos cells 2 PU.1 GFP LPS 1 FSCA Ctl NI 24h LPS Sup.Fig.1 Effect
Myeloid neoplasms. Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories:
 Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Myeloid neoplasms Note: Early arrest in the blast cell or immature cell "we call it acute leukemia" Myoid neoplasm divided in to 3 major categories: 1. AML : Acute myeloid leukemia(stem cell with myeloid
Participants Identification No. % Evaluation. Mitotic figure Educational Erythrocyte precursor, abnormal 1 0.
 Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
Cell Identification Mitotic figure 212 99.5 Educational Erythrocyte precursor, abnormal BMD-02 The arrowed cell is a mitotic figure. It was correctly identified by 99.5% of the participants. A cell containing
Chronic variable stress activates hematopoietic stem cells
 SUPPLEMENTARY INFORMATION Chronic variable stress activates hematopoietic stem cells Timo Heidt *, Hendrik B. Sager *, Gabriel Courties, Partha Dutta, Yoshiko Iwamoto, Alex Zaltsman, Constantin von zur
SUPPLEMENTARY INFORMATION Chronic variable stress activates hematopoietic stem cells Timo Heidt *, Hendrik B. Sager *, Gabriel Courties, Partha Dutta, Yoshiko Iwamoto, Alex Zaltsman, Constantin von zur
SUPPLEMENTARY INFORMATION
 Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
Supplementary Information S1 Frequency of DNMT3A mutations in hematologic disorders and their associated clinical phenotypes. Disease Patient population Frequency (%) Associated Clinical Characteristics
New drugs in Acute Leukemia. Cristina Papayannidis, MD, PhD University of Bologna
 New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
New drugs in Acute Leukemia Cristina Papayannidis, MD, PhD University of Bologna Challenges to targeted therapy in AML Multiple subtypes based upon mutations/cytogenetic aberrations No known uniform genomic
Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome
 Molecular profiling of early MDS Hematopathology - March 2016 Article Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome Maya Thangavelu 1,*, Ryan Olson 2, Li Li 2, Wanlong
Molecular profiling of early MDS Hematopathology - March 2016 Article Molecular profiling in confirming the diagnosis of early myelodysplastic syndrome Maya Thangavelu 1,*, Ryan Olson 2, Li Li 2, Wanlong
MDS 101. What is bone marrow? Myelodysplastic Syndrome: Let s build a definition. Dysplastic? Syndrome? 5/22/2014. What does bone marrow do?
 101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
101 May 17, 2014 Myelodysplastic Syndrome: Let s build a definition Myelo bone marrow Gail J. Roboz, M.D. Director, Leukemia Program Associate Professor of Medicine What is bone marrow? What does bone
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed
 MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
MYELODYSPLASTIC SYNDROMES: A diagnosis often missed D R. EMMA W YPKEMA C O N S U LTA N T H A E M AT O L O G I S T L A N C E T L A B O R AT O R I E S THE MYELODYSPLASTIC SYNDROMES DEFINITION The Myelodysplastic
DISCOVERING ATCC IMMUNOLOGICAL CELLS - MODEL SYSTEMS TO STUDY THE IMMUNE AND CARDIOVASCULAR SYSTEMS
 DISCOVERING ATCC IMMUNOLOGICAL CELLS - MODEL SYSTEMS TO STUDY THE IMMUNE AND CARDIOVASCULAR SYSTEMS James Clinton, Ph.D. Scientist, ATCC February 19, 2015 About ATCC Founded in 1925, ATCC is a non-profit
DISCOVERING ATCC IMMUNOLOGICAL CELLS - MODEL SYSTEMS TO STUDY THE IMMUNE AND CARDIOVASCULAR SYSTEMS James Clinton, Ph.D. Scientist, ATCC February 19, 2015 About ATCC Founded in 1925, ATCC is a non-profit
CD34+ Cells: A Comparison of Stem and Progenitor Cells in Cord Blood, Peripheral Blood, and the Bone Marrow
 White Paper September 2016 CD34+ Cells: A Comparison of Stem and Progenitor Cells in Cord Blood, Peripheral Blood, and the Bone Marrow Lily C. Trajman, PhD Introduction: Hematopoietic Stem Cells (HSCs)
White Paper September 2016 CD34+ Cells: A Comparison of Stem and Progenitor Cells in Cord Blood, Peripheral Blood, and the Bone Marrow Lily C. Trajman, PhD Introduction: Hematopoietic Stem Cells (HSCs)
Myelodysplastic Syndromes Myeloproliferative Disorders
 Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
Myelodysplastic Syndromes Myeloproliferative Disorders Myelodysplastic Syndromes characterized by maturation defects that are associated with ineffective hematopoiesis and a high risk of transformation
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification
 What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
What is MDS? Epidemiology, Diagnosis, Classification & Risk Stratification Rami Komrokji, MD Clinical Director Malignant Hematology Moffitt Cancer Center Normal Blood and Bone Marrow What is MDS Myelodysplastic
Supplementary Figures
 Supplementary Figures Supplementary Figure 1. Confirmation of Dnmt1 conditional knockout out mice. a, Representative images of sorted stem (Lin - CD49f high CD24 + ), luminal (Lin - CD49f low CD24 + )
Supplementary Figures Supplementary Figure 1. Confirmation of Dnmt1 conditional knockout out mice. a, Representative images of sorted stem (Lin - CD49f high CD24 + ), luminal (Lin - CD49f low CD24 + )
When Cancer Looks Like Something Else: How Does Mutational Profiling Inform the Diagnosis of Myelodysplasia?
 Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Transcript Details This is a transcript of a continuing medical education (CME) activity accessible on the ReachMD network. Additional media formats for the activity and full activity details (including
Myelodysplastic scoring system with flow cytometry. G Detry B Husson
 Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Myelodysplastic scoring system with flow cytometry G Detry B Husson Myelodysplastic syndroms Clonal haematopoietic stem cell disease characterized by dysplasia in one or more of the myeloid cell lines
Impaired DNA replication within progenitor cell pools promotes leukemogenesis
 Impaired DNA replication within progenitor cell pools promotes leukemogenesis Ganna Bilousova, University of Colorado Andriy Marusyk, University of Colorado Christopher Porter, Emory University Robert
Impaired DNA replication within progenitor cell pools promotes leukemogenesis Ganna Bilousova, University of Colorado Andriy Marusyk, University of Colorado Christopher Porter, Emory University Robert
Control shrna#9 shrna#12. shrna#12 CD14-PE CD14-PE
 a Control shrna#9 shrna#12 c Control shrna#9 shrna#12 e Control shrna#9 shrna#12 h 14 12 CFU-E BFU-E GEMM GM b Colony number 7 6 5 4 3 2 1 6 pm A pa pc CFU-E BFU-E GEMM GM pu pgm A p pg B d f CD11b-APC
a Control shrna#9 shrna#12 c Control shrna#9 shrna#12 e Control shrna#9 shrna#12 h 14 12 CFU-E BFU-E GEMM GM b Colony number 7 6 5 4 3 2 1 6 pm A pa pc CFU-E BFU-E GEMM GM pu pgm A p pg B d f CD11b-APC
Corrigenda. WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run
 Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Corrigenda WHO Classification of Tumours of Haematopoietic and Lymphoid Tissues (revised 4th edition): corrections made in second print run In addition to corrections of minor typographical errors, corrections
Case Presentation No. 075
 Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Case Presentation No. 075 Session 4. Myelodysplastic Syndrome Cristina Montalvo, MD Baylor College of Medicine Houston, Texas 2007 Workshop of Society for Hematopathology and European Association for Haematopathology
Profiles of gene expression & diagnosis/prognosis of cancer. MCs in Advanced Genetics Ainoa Planas Riverola
 Profiles of gene expression & diagnosis/prognosis of cancer MCs in Advanced Genetics Ainoa Planas Riverola Gene expression profiles Gene expression profiling Used in molecular biology, it measures the
Profiles of gene expression & diagnosis/prognosis of cancer MCs in Advanced Genetics Ainoa Planas Riverola Gene expression profiles Gene expression profiling Used in molecular biology, it measures the
Getting to the root of Cancer
 Cancer Stem Cells: Getting to the root of Cancer Dominique Bonnet, Ph.D Senior Group Leader, Haematopoietic Stem Cell Laboratory Cancer Research UK, London Research Institute Venice, Sept 2009 Overview
Cancer Stem Cells: Getting to the root of Cancer Dominique Bonnet, Ph.D Senior Group Leader, Haematopoietic Stem Cell Laboratory Cancer Research UK, London Research Institute Venice, Sept 2009 Overview
Chronic Myelomonocytic Leukemia with molecular abnormalities SH
 Chronic Myelomonocytic Leukemia with molecular abnormalities SH2017-0351 Madhu P. Menon MD,PhD, Juan Gomez MD, Kedar V. Inamdar MD,PhD and Kristin Karner MD Madhu P Menon, MD, PhD Henry Ford Hospital Patient
Chronic Myelomonocytic Leukemia with molecular abnormalities SH2017-0351 Madhu P. Menon MD,PhD, Juan Gomez MD, Kedar V. Inamdar MD,PhD and Kristin Karner MD Madhu P Menon, MD, PhD Henry Ford Hospital Patient
SESSION 1 Reactive cytopenia and dysplasia
 SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
SESSION 1 Reactive cytopenia and dysplasia Falko Fend, Tübingen & Alexandar Tzankov, Basel 1 Disclosure of speaker s interests (Potential) conflict of interest none Potentially relevant company relationships
Acute myeloid leukemia. M. Kaźmierczak 2016
 Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
Acute myeloid leukemia M. Kaźmierczak 2016 Acute myeloid leukemia Malignant clonal disorder of immature hematopoietic cells characterized by clonal proliferation of abnormal blast cells and impaired production
mirna Dr. S Hosseini-Asl
 mirna Dr. S Hosseini-Asl 1 2 MicroRNAs (mirnas) are small noncoding RNAs which enhance the cleavage or translational repression of specific mrna with recognition site(s) in the 3 - untranslated region
mirna Dr. S Hosseini-Asl 1 2 MicroRNAs (mirnas) are small noncoding RNAs which enhance the cleavage or translational repression of specific mrna with recognition site(s) in the 3 - untranslated region
TITLE: Properties of Leukemia Stem Cells in a Novel Model of CML Progression to Lymphoid Blast Crisis
 AD Award Number: W81XWH-05-1-0608 TITLE: Properties of Leukemia Stem Cells in a Novel Model of CML Progression to Lymphoid Blast Crisis PRINCIPAL INVESTIGATOR: Craig T. Jordan, Ph.D. CONTRACTING ORGANIZATION:
AD Award Number: W81XWH-05-1-0608 TITLE: Properties of Leukemia Stem Cells in a Novel Model of CML Progression to Lymphoid Blast Crisis PRINCIPAL INVESTIGATOR: Craig T. Jordan, Ph.D. CONTRACTING ORGANIZATION:
ADx Bone Marrow Report. Patient Information Referring Physician Specimen Information
 ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
ADx Bone Marrow Report Patient Information Referring Physician Specimen Information Patient Name: Specimen: Bone Marrow Site: Left iliac Physician: Accession #: ID#: Reported: 08/19/2014 - CHRONIC MYELOGENOUS
MYELODYSPLASTIC SYNDROMES
 MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
MYELODYSPLASTIC SYNDROMES Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra university hospital, Isfahan university of medical sciences Key Features ESSENTIALS OF DIAGNOSIS Cytopenias
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure
 Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Beyond the CBC Report: Extended Laboratory Testing in the Evaluation for Hematologic Neoplasia Disclosure I am receiving an honorarium from Sysmex for today s presentation. 1 Determining the Etiology for
Innate Immunity Dysregulation in Myelodysplastic Syndromes. CONTRACTING ORGANIZATION: University of Texas MD Anderson Cancer Center Houston, TX 77030
 AWARD NUMBER: W81XWH-12-1-0221 TITLE: Innate Immunity Dysregulation in Myelodysplastic Syndromes PRINCIPAL INVESTIGATOR: Yue Wei CONTRACTING ORGANIZATION: University of Texas MD Anderson Cancer Center
AWARD NUMBER: W81XWH-12-1-0221 TITLE: Innate Immunity Dysregulation in Myelodysplastic Syndromes PRINCIPAL INVESTIGATOR: Yue Wei CONTRACTING ORGANIZATION: University of Texas MD Anderson Cancer Center
Effective Targeting of Quiescent Chronic Myelogenous
 Cancer Cell, Volume 7 Supplemental Information Effective Targeting of Quiescent Chronic Myelogenous Leukemia Stem Cells by Histone Deacetylase Inhibitors in Combination with Imatinib Mesylate Bin Zhang,
Cancer Cell, Volume 7 Supplemental Information Effective Targeting of Quiescent Chronic Myelogenous Leukemia Stem Cells by Histone Deacetylase Inhibitors in Combination with Imatinib Mesylate Bin Zhang,
Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Neoplasms. Policy Specific Section:
 Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
Medical Policy Allogeneic Hematopoietic Stem-Cell Transplantation for Myelodysplastic Syndromes and Myeloproliferative Type: Medical Necessity and Investigational / Experimental Policy Specific Section:
New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke
 University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
University of Groningen New treatment strategies in myelodysplastic syndromes and acute myeloid leukemia van der Helm, Lidia Henrieke IMPORTANT NOTE: You are advised to consult the publisher's version
Highly Efficient CRISPR/Cas9 Gene Editing and Long-Term Engraftment of Human Hematopoietic Stem and Progenitor Cells
 Highly Efficient CRISPR/Cas9 Gene Editing and Long-Term Engraftment of Human Hematopoietic Stem and Progenitor Cells J. M. Heath, A. Chalishazar, C.S. Lee, W. Selleck, C. Cotta-Ramusino, D. Bumcrot, J.L.
Highly Efficient CRISPR/Cas9 Gene Editing and Long-Term Engraftment of Human Hematopoietic Stem and Progenitor Cells J. M. Heath, A. Chalishazar, C.S. Lee, W. Selleck, C. Cotta-Ramusino, D. Bumcrot, J.L.
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
MicroRNAs Modulate Hematopoietic Lineage Differentiation
 MicroRNAs Modulate Hematopoietic Lineage Differentiation Harvey F. Lodish, Chang-Zheng Chen, David P. Bartel Whitehead Institute for Biomedical Research, Department of Biology, Massachusetts Institute
MicroRNAs Modulate Hematopoietic Lineage Differentiation Harvey F. Lodish, Chang-Zheng Chen, David P. Bartel Whitehead Institute for Biomedical Research, Department of Biology, Massachusetts Institute
SUPPLEMENTARY INFORMATION. Supp. Fig. 1. Autoimmunity. Tolerance APC APC. T cell. T cell. doi: /nature06253 ICOS ICOS TCR CD28 TCR CD28
 Supp. Fig. 1 a APC b APC ICOS ICOS TCR CD28 mir P TCR CD28 P T cell Tolerance Roquin WT SG Icos mrna T cell Autoimmunity Roquin M199R SG Icos mrna www.nature.com/nature 1 Supp. Fig. 2 CD4 + CD44 low CD4
Supp. Fig. 1 a APC b APC ICOS ICOS TCR CD28 mir P TCR CD28 P T cell Tolerance Roquin WT SG Icos mrna T cell Autoimmunity Roquin M199R SG Icos mrna www.nature.com/nature 1 Supp. Fig. 2 CD4 + CD44 low CD4
Blood 101 Introduction Blood and Marrow & Overview of Bone Marrow Failure Diseases. Dr. M. Sabloff October 16 th 2010
 Blood 101 Introduction Blood and Marrow & Overview of Bone Marrow Failure Diseases Dr. M. Sabloff October 16 th 2010 Normal Marrow knee joint white is articular cartilage Adjacent to this is the red marrow
Blood 101 Introduction Blood and Marrow & Overview of Bone Marrow Failure Diseases Dr. M. Sabloff October 16 th 2010 Normal Marrow knee joint white is articular cartilage Adjacent to this is the red marrow
SUPPLEMENTARY INFORMATION
 DOI: 1.138/ncb3355 a S1A8 + cells/ total.1.8.6.4.2 b S1A8/?-Actin c % T-cell proliferation 3 25 2 15 1 5 T cells Supplementary Figure 1 Inter-tumoral heterogeneity of MDSC accumulation in mammary tumor
DOI: 1.138/ncb3355 a S1A8 + cells/ total.1.8.6.4.2 b S1A8/?-Actin c % T-cell proliferation 3 25 2 15 1 5 T cells Supplementary Figure 1 Inter-tumoral heterogeneity of MDSC accumulation in mammary tumor
SUPPLEMENTARY INFORMATION
 DOI:.38/ncb3399 a b c d FSP DAPI 5mm mm 5mm 5mm e Correspond to melanoma in-situ Figure a DCT FSP- f MITF mm mm MlanaA melanoma in-situ DCT 5mm FSP- mm mm mm mm mm g melanoma in-situ MITF MlanaA mm mm
DOI:.38/ncb3399 a b c d FSP DAPI 5mm mm 5mm 5mm e Correspond to melanoma in-situ Figure a DCT FSP- f MITF mm mm MlanaA melanoma in-situ DCT 5mm FSP- mm mm mm mm mm g melanoma in-situ MITF MlanaA mm mm
Nature Immunology: doi: /ni Supplementary Figure 1. Cellularity of leukocytes and their progenitors in naive wild-type and Spp1 / mice.
 Supplementary Figure 1 Cellularity of leukocytes and their progenitors in naive wild-type and Spp1 / mice. (a, b) Gating strategies for differentiated cells including PMN (CD11b + Ly6G hi and CD11b + Ly6G
Supplementary Figure 1 Cellularity of leukocytes and their progenitors in naive wild-type and Spp1 / mice. (a, b) Gating strategies for differentiated cells including PMN (CD11b + Ly6G hi and CD11b + Ly6G
NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia
 Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
Case 0094 NUP214-ABL1 Fusion: A Novel Discovery in Acute Myelomonocytic Leukemia Jessica Snider, MD Medical University of South Carolina Case Report - 64 year old Caucasian Male Past Medical History Osteoarthritis
DISCLOSURE. I have the following financial relationships:
 DISCLOSURE I have the following financial relationships: Consultant for: Fate Therapeutics, GlaxoSmithKline, Bone Therapeutics, G1 Therapeutics Contracted Research for: GlaxoSmithKline Royalties from:
DISCLOSURE I have the following financial relationships: Consultant for: Fate Therapeutics, GlaxoSmithKline, Bone Therapeutics, G1 Therapeutics Contracted Research for: GlaxoSmithKline Royalties from:
Supplemental Information. Granulocyte-Monocyte Progenitors and. Monocyte-Dendritic Cell Progenitors Independently
 Immunity, Volume 47 Supplemental Information Granulocyte-Monocyte Progenitors and Monocyte-endritic ell Progenitors Independently Produce Functionally istinct Monocytes lberto Yáñez, Simon G. oetzee, ndre
Immunity, Volume 47 Supplemental Information Granulocyte-Monocyte Progenitors and Monocyte-endritic ell Progenitors Independently Produce Functionally istinct Monocytes lberto Yáñez, Simon G. oetzee, ndre
The nucleotide sugar UDP-glucose mobilizes long-term repopulating primitive hematopoietic cells
 Research article The nucleotide sugar UDP-glucose mobilizes long-term repopulating primitive hematopoietic cells Sungho Kook, 1 Joonseok Cho, 1 Sean Bong Lee, 2 and Byeong-Chel Lee 1 1 University of Pittsburgh
Research article The nucleotide sugar UDP-glucose mobilizes long-term repopulating primitive hematopoietic cells Sungho Kook, 1 Joonseok Cho, 1 Sean Bong Lee, 2 and Byeong-Chel Lee 1 1 University of Pittsburgh
Differential Connexin Function Enhances Self-Renewal in Glioblastoma
 CSU ID: 2558414 Name: Sonal Patel Differential Connexin Function Enhances Self-Renewal in Glioblastoma Cancer is one of the most common disease in the US with more than a million people affected every
CSU ID: 2558414 Name: Sonal Patel Differential Connexin Function Enhances Self-Renewal in Glioblastoma Cancer is one of the most common disease in the US with more than a million people affected every
The Hierarchical Organization of Normal and Malignant Hematopoiesis
 The Hierarchical Organization of Normal and Malignant Hematopoiesis NORMAL Hematopoie2c Stem Cell (HSC) Leukemia Stem Cells (LSC) MPP MLP CMP Leukemic Progenitors MEP GMP B/NK ETP Leukemic Blasts Erythrocytes
The Hierarchical Organization of Normal and Malignant Hematopoiesis NORMAL Hematopoie2c Stem Cell (HSC) Leukemia Stem Cells (LSC) MPP MLP CMP Leukemic Progenitors MEP GMP B/NK ETP Leukemic Blasts Erythrocytes
Classification of Hematologic Malignancies. Patricia Aoun MD MPH
 Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Classification of Hematologic Malignancies Patricia Aoun MD MPH Objectives Know the basic principles of the current classification system for hematopoietic and lymphoid malignancies Understand the differences
Normal & Leukaemic haematopoiesis. Dr. Liu Te Chih Dept of Haematology / Oncology National University Health Services Singapore
 Normal & Leukaemic haematopoiesis 2010 Dr. Liu Te Chih Dept of Haematology / Oncology National University Health Services Singapore Use of Immunophenotyping today Lineage assignment Differentiation of
Normal & Leukaemic haematopoiesis 2010 Dr. Liu Te Chih Dept of Haematology / Oncology National University Health Services Singapore Use of Immunophenotyping today Lineage assignment Differentiation of
microrna-29a induces aberrant self-renewal capacity in hematopoietic progenitors, biased myeloid development, and acute myeloid leukemia
 Published Online: 8 March, 2010 Supp Info: http://doi.org/10.1084/jem.20090831 Downloaded from jem.rupress.org on December 17, 2018 Ar ticle microrna-29a induces aberrant self-renewal capacity in hematopoietic
Published Online: 8 March, 2010 Supp Info: http://doi.org/10.1084/jem.20090831 Downloaded from jem.rupress.org on December 17, 2018 Ar ticle microrna-29a induces aberrant self-renewal capacity in hematopoietic
2013 AAIM Pathology Workshop
 2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
2013 AAIM Pathology Workshop John Schmieg, M.D., Ph.D. None Disclosures 1 Pathology Workshop Objectives Define the general philosophy of reviewing pathology reports Review the various components of Bone
Hosoya et al. TRIM28 is essential for erythroblast differentiation in the mouse (supplemental information)
 TaqMan assay Gene TRIM28 GATA-1 Applied Biosystems TaqMan assay Mm00495594_m1 Mm01352636_m1 SYBR Green assay Gene Forward primer Reverse primer Reference adult α-globin CCCGGTGCCTTGTCTGCT GTGAAATCGGCAGGGTGG
TaqMan assay Gene TRIM28 GATA-1 Applied Biosystems TaqMan assay Mm00495594_m1 Mm01352636_m1 SYBR Green assay Gene Forward primer Reverse primer Reference adult α-globin CCCGGTGCCTTGTCTGCT GTGAAATCGGCAGGGTGG
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms. Daniel A. Arber, MD Stanford University
 Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Integrated Diagnostic Approach to the Classification of Myeloid Neoplasms Daniel A. Arber, MD Stanford University What is an integrated approach? What is an integrated approach? Incorporating all diagnostic
Nature Genetics: doi: /ng Supplementary Figure 1. HOX fusions enhance self-renewal capacity.
 Supplementary Figure 1 HOX fusions enhance self-renewal capacity. Mouse bone marrow was transduced with a retrovirus carrying one of three HOX fusion genes or the empty mcherry reporter construct as described
Supplementary Figure 1 HOX fusions enhance self-renewal capacity. Mouse bone marrow was transduced with a retrovirus carrying one of three HOX fusion genes or the empty mcherry reporter construct as described
TITLE: Effects of Hematopoietic Stem Cell Age on CML Disease Progression
 AD Award Number: W81XWH-04-1-0795 TITLE: Effects of Hematopoietic Stem Cell Age on CML Disease Progression PRINCIPAL INVESTIGATOR: Kenneth Dorshkind, Ph.D. CONTRACTING ORGANIZATION: University of California,
AD Award Number: W81XWH-04-1-0795 TITLE: Effects of Hematopoietic Stem Cell Age on CML Disease Progression PRINCIPAL INVESTIGATOR: Kenneth Dorshkind, Ph.D. CONTRACTING ORGANIZATION: University of California,
Supplementary Figure 1: Comparison of acgh-based and expression-based CNA analysis of tumors from breast cancer GEMMs.
 Supplementary Figure 1: Comparison of acgh-based and expression-based CNA analysis of tumors from breast cancer GEMMs. (a) CNA analysis of expression microarray data obtained from 15 tumors in the SV40Tag
Supplementary Figure 1: Comparison of acgh-based and expression-based CNA analysis of tumors from breast cancer GEMMs. (a) CNA analysis of expression microarray data obtained from 15 tumors in the SV40Tag
Scientific report: Delineating cellular stages and regulation of human NK cell development to improve NK cell-based therapy for cancer (Dnr )
 Scientific report: Delineating cellular stages and regulation of human NK cell development to improve NK cell-based therapy for cancer (Dnr 130259) The main goal of this project focuses on establishing
Scientific report: Delineating cellular stages and regulation of human NK cell development to improve NK cell-based therapy for cancer (Dnr 130259) The main goal of this project focuses on establishing
WBCs Disorders 1. Dr. Nabila Hamdi MD, PhD
 WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
WBCs Disorders 1 Dr. Nabila Hamdi MD, PhD ILOs Compare and contrast ALL, AML, CLL, CML in terms of age distribution, cytogenetics, morphology, immunophenotyping, laboratory diagnosis clinical features
Figure S1A. Blood glucose levels in mice after glucose injection
 ## Figure S1A. Blood glucose levels in mice after glucose injection Blood glucose (mm/l) 25 2 15 1 5 # 15 3 6 3+3 Time after glucose injection (min) # Figure S1B. α-kg levels in mouse livers after glucose
## Figure S1A. Blood glucose levels in mice after glucose injection Blood glucose (mm/l) 25 2 15 1 5 # 15 3 6 3+3 Time after glucose injection (min) # Figure S1B. α-kg levels in mouse livers after glucose
TEB. Id4 p63 DAPI Merge. Id4 CK8 DAPI Merge
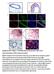 a Duct TEB b Id4 p63 DAPI Merge Id4 CK8 DAPI Merge c d e Supplementary Figure 1. Identification of Id4-positive MECs and characterization of the Comma-D model. (a) IHC analysis of ID4 expression in the
a Duct TEB b Id4 p63 DAPI Merge Id4 CK8 DAPI Merge c d e Supplementary Figure 1. Identification of Id4-positive MECs and characterization of the Comma-D model. (a) IHC analysis of ID4 expression in the
