A large proportion of the body consists of water. Sodium is the major electrolyte that influences the water content and its distribution.
|
|
|
- Francine Wilson
- 5 years ago
- Views:
Transcription
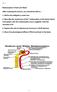
1 WATER AND SODIUM DISTURBANCES A large proportion of the body consists of water. Sodium is the major electrolyte that influences the water content and its distribution. JOCELYN NAIcKER BSc, MB ChB, MFGP (SA), FCPath (Chem) (SA), MMed (Chem Path) Principal Chemical Pathologist National Health Laboratory Services and University of the Witwatersrand Johannesburg After qualifying at the Nelson Mandela School of Medicine in Natal in 1979 Jocelyn Naicker rotated through Medicine, Surgery, Obstetrics and Gynaecology, Paediatrics and Anaesthetics departments. In 1982 she moved to Cape Town, where she practised family medicine for a number of years. She joined the Department of Chemical Pathology at the University of the Witwatersrand and the National Health Laboratory Service (joint staff) in She is currently the Principal Chemical Pathologist in charge of the chemical pathology laboratory at the Chris Hani Baragwanath Hospital. This article describes the factors that influence water and sodium homeostasis, as well as the associated clinical problems encountered when having to assess and manage a patient with these imbalances. NORMAL WATER AND ELECTROLYTE DISTRIBUTION Approximately two-thirds of the total body water is found in the intracellular fluid compartment (ICFC), and one-third in the extracellular fluid compartment (ECFC). The ECFC consists of the intravascular (1/4 ECFC) and interstitial spaces (3/4 ECFC) (Fig. 1). INTRACELLULAR FLUID COMPARTMENT (ICFC) 23 litre K + ( 110 mmol/l) Na+ (10 mmol/l) EXTRACELLULAR FLUID COMPARTMENT (ECFC) 19 litre Na : K ATPase pump Na + (135 mmol/l) K+ (4 mmol/l) Fig. 1. Water, sodium (Na + ) and potassium (K + ) distribution in the different body compartments of a young 70 kg male (total body water is 42 l). The total water content of the body differs according to age and gender this is significant when replacing fluid in dehydrated patients (Fig. 2). A 70 kg young male would have an estimated total body water content of 42 l, ICFC 23 l, ECFC 19 l (interstitial fluid 16 l and intravascular fluid 3 l). Infants 75% TBW Young males 60% TBW Young females 55% TBW Elderly males 50% TBW Elderly females 45% TBW Fig. 2. Water distribution according to age and gender expressed as a % of total body weight (TBW). Na + is the major cation of the ECFC and K + is the major cation of the ICFC (Fig. 1). The tendency for these cations to move down their individual concentration gradients is opposed by the Na + :K + ATPase pump which constantly extrudes Na + out of cells (in exchange for K + ). Under normal circumstances, the ECF [Na + ] is the main contributor of the ECFC tonicity. Mg and PO 4 ions are found predominantly intracellularly, while Cl - anions are found predominantly in the ECFC in association with Na + ions. Water, on the other hand, is freely permeable across the membranes of the ICFC and ECFC and water distribution is determined by the (osmotically active) particular content of the various compartments. At the capillary level, the oncotic pressure (osmolality due to the protein content) of plasma determines the fluid content of the interstitial space. Osmolality differences between compartments are corrected by fluid shifts. water balance A well-balanced fluid state depends upon fluid input, output and fluid shifts. A 70 kg young adult male might have an average daily balance as seen in Fig CME July 2006 Vol.24 No.7 Naicker.indd 366 7/7/06 3:39:58 PM
2 OUPUT INPUT Skin 500 ml Metabolism 400 ml Lungs 400 ml Diet ml Gut 100 ml Kidney ml ml ml Fig. 3. Input-output chart of a healthy 70 kg male. This balance can vary greatly depending on the availability of water, environmental factors (heat, humidity), physical activity, fluid losses during illness (e.g. diarrhoea/vomiting/ polyuria/sweating due to pyrexia/ respiratory loss due to tachypnoea), glomerular filtration, renal tubular concentration and dilution ability, as well the manner in which fluid is replaced. Free water clearance by the kidney (or urine dilution) is the hypothetical rate at which water is excreted in excess of that required for the renal clearance of the body s normal solute load. A normal person requires 500 ml of tubular fluid to eliminate approximately 600 mmol of solute daily. An increase in plasma osmolality or a decrease in blood volume stimulates the thirst centre in the hypothalamus. Both an increase in plasma osmolality of > 2% and a decrease in intravascular volume of > 10% stimulate the release of antidiuretic hormone (ADH) (also known as arginine vasopressin) from the posterior pituitary. ADH binds to the V2 receptors on the basolateral membrane of the renal collecting tubules. This induces the insertion of water channels called aquaporins into the luminal surface. Water is passively reabsorbed via these aquaporins down a concentration gradient created by the hyperosmolal renal medulla. Urine is thus concentrated and there is decreased free-water clearance. Normal cortisol levels are required to inhibit ADH release. In cortisoldeficient states, e.g. Addison s disease, ADH continues to be secreted and free-water clearance is impaired. Loss of ISOTONIC fluid blood small intestinal secretions e.g. fistulae, paralytic ileus, small bowel obstruction, new ileostomies Loss of HYPOTONIC fluid vomitus diarrhoeal fluid sweat, as in pyrexial patients Loss of HYPERTONIC fluid loss of hypotonic body secretions replacement with tap water has the net effect of loss of hypertonic fluid Loss of pure water loss of dilute urine in diabetes insipidus Fig. 4. Types of fluid loss. Other factors that stimulate ADH secretion are stress, nausea and drugs, e.g. morphine, barbiturates, chlorpropamide, carbamazepine. Examples of drugs that suppress ADH secretion are alcohol, phenytoin and atropine. The effect of fluid loss on the body depends on what type of fluid is lost (Fig. 4), the rapidity of the loss and the attempt at replacement (if any). SODIUM HOMEOSTASIS The average oral intake is mmol sodium/day. Major daily losses are via the kidney, although only < 1% of the mmol Na + that is filtered daily by renal glomeruli appears in the urine (fractional excretion of Na + ). Factors that regulate renal sodium include the glomerular filtration rate (GFR), the renin-angiotensinaldosterone system (RAAS) and natriuretic peptide secretion. As the GFR decreases, Na + reabsorption increases and the opposite is true for an increase in GFR. A decrease in renal blood flow (as in dehydration) causes renin secretion by the cells of the juxtaglomerular apparatus in the kidney. Renin converts angiotensinogen to angiotensin I, which in turn is converted to angiotensin II by the action of angiotensin-converting enzyme (ACE). Angiotensin II has a direct vasoconstrictor action, as well as stimulating the secretion of aldosterone from the adrenal cortex (secondary hyperaldosteronism). Aldosterone acts on the distal renal tubules and Na + is reabsorbed in exchange for H + and K +. Natriuretic peptides atrial natriuretic peptide (ANP), brain-type natriuretic peptide (BNP), C-type natriuretic peptide (CNP) are secreted in response to an increase in the intravascular volume and serve to protect against fluid overload. Cardiac atrial stretch causes release of ANP and BNP, which result in natriuresis, diuresis, kaliuresis and a reduction in blood pressure. HYPONATRAEMIA Consequences of ECF hypotonia When hypotonic hyponatraemia develops acutely, water moves from the ECFC into the ICFC along the osmotic gradient, causing swelling of cells within minutes. This response is particularly undesirable in the brain, as cerebral oedema could progress to brain-stem herniation, respiratory arrest and possibly death. There is, however, a rapid adaptation, resulting in loss of intracellular solutes, especially K +, causing the cells to decrease in size towards normal. However, if the rate of water loading is faster than this rate of adaptation then the patient will be symptomatic. Symptoms include lethargy, seizures, confusion, coma, respiratory arrest and even death. If, on the other hand, the change in the ECF hypotonicity occurs slowly, then the cells, in particular the brain cells, are able to adapt more effectively as the tonicity changes. July 2006 Vol.24 No.7 CME 367 Naicker.indd 367 7/7/06 3:39:59 PM
3 Approximately two-thirds of the total body water is found in the intracellular fluid compartment (ICFC), and one-third in the extracellular fluid compartment (ECFC). Free water clearance by the kidney (or urine dilution) is the hypothetical rate at which water is excreted in excess of that required for the renal clearance of the body s normal solute load. For this reason, in patients with the same low [Na + ], chronic hyponatraemia is better tolerated than acute hyponatraemia and lethargy and restlessness may be the only symptoms. When the serum [Na + ] is < 110 mmol/l, and the patient is symptomatic, care has to be taken not to correct the hyponatraemia too rapidly. In the adapted state, the initially swollen cells have been reduced to normal volume by loss of solute. With a rapid increase of the ECF osmolality (by the therapeutic infusion of hypertonic solutions), fluid will move out of the cells, and the ensuing rapid cell shrinkage will result in osmotic demyelination of pontine and extrapontine neurones (myelinolysis) with permanent neurological damage, coma and even death. Rapid correction may be better tolerated in acute hyponatraemia. Approach to hyponatraemia (Fig. 5) Iso-osmolal hyponatraemia (factitious) In the approach to hyponatraemia, pseudohyponatraemia should be excluded first. This term refers to a low plasma Na + measurement when the measured osmolality is normal. An aliquot of normal plasma contains about 7% solids, which include proteins and lipids. The remaining Fig. 5. Approach to the differential diagnosis of hyponatraemia. 93% of plasma consists of water (containing dissolved Na + ions). In conditions like multiple myeloma and hyperlipidaemia, where the solid fraction is increased, the water content of the plasma sample in the collection tube is markedly reduced, due to displacement of water molecules by the excessive paraproteins or lipids respectively. This reduced water phase will thus have fewer dissolved Na + molecules. The [Na + ] is expressed in terms of the total volume of plasma sampled and the factitious low reading represents an exaggerated negative analytical error. Hyperosmolal hyponatraemia Hyponatraemia in a patient with a high measured osmolality indicates the presence of increased amounts of other osmotically active solutes apart from Na + in the ECFC. This ECFC hyperosmolality causes water shift from the ICFC, diluting out the ECF Na +. The causes of hyperosmolal hyponatraemia include hyperglycaemia and the use of mannitol. Hypo-osmolal hyponatraemia (true hyponatraemia) Both the measured plasma osmolality and [Na + ] are low. Because the plasma [Na + ] is an index of the water balance, the cause of the hyponatraemia is determined by assessing ECF volume. This is accomplished by taking the patient history, measuring the body mass and assessing the state of hydration and jugular venous pressure (JVP) on physical examination. There may be: Hypovolaemia loss of water and Na + with attempted replacement using sodium-deficient fluid, e.g. tap water, 5% IV glucose. Renal losses osmotic diuresis, diuretics, aldosterone deficiency, or salt-losing nephritis. Extrarenal losses excessive sweating, vomiting, or diarrhoea. Slight hypervolaemia with no oedema. If there is pure water gain (normal total body Na + ) then there will be no oedema because the excess water will redistribute itself across both the ECFC and ICFC. Increased water intake can be the result of inappropriate salt-free IV fluids or psychogenic polydipsia (compulsive drinking of excessive quantities of water). Decreased water excretion can be caused by the syndrome of inappropriate antidiuretic hormone secretion (SIADH), cortisol deficiency, severe hypothyroidism, or drugs, e.g. oxytocin. 368 CME July 2006 Vol.24 No.7 Naicker.indd 368 7/7/06 3:40:04 PM
4 Hypervolaemia with oedema. In conditions where there is retention of both Na + and water (increased total body water and Na + ), e.g. nephrotic syndrome, cardiac failure, cirrhosis, water may be retained in the interstitial space (oedema) at the expense of the intravascular compartment. Oedematous states are often refractory to diuretic therapy and are found in hypoalbuminaemic conditions. Plasma expanders like albumin may have to be administered. SICK CELL SYNDROME Hyponatraemia is not infrequently seen in acute or chronically ill patients. The term sick cell syndrome is used in those patients where no obvious cause for the hyponatraemia can be found. The exact mechanism of the hyponatraemia has not yet been determined, although it is believed to be due to increased membrane permeability (redistribution hyponatraemia). A contributory factor may be the increase in ADH secretion that occurs in ill patients due to stress. Treatment of the underlying illness eliminates the hyponatraemia. SYNDROME OF INAPPROPRIATE ADH SECRETION (SIADH) In this syndrome, despite the hypo-osmolar hyponatraemia, ADH continues to be secreted inappropriately, resulting in a dilutional hyponatraemia. Essential diagnostic criteria for SIADH: Hypo-osmolal hyponatraemia. The urine osmolality is high relative to the serum sample collected at the same time. The spot urine [Na + ] is high (> 20 mmol/l). This is because the slight hypervolaemia due to water retention does not stimulate the RAAS and, in addition, stimulates the release of ANPs, which cause natriuresis. The patient should have no evidence of hypovolaemia or oedema. Disorders of the heart, pituitary, adrenals, kidneys and thyroid have to be excluded as they can produce similar biochemical features. The patient should not be on drugs that stimulate ADH secretion (e.g. morphine), potentiate ADH effect (e.g. indomethacin), or produce similar biochemical features (e.g. thiazide diuretics). The hyponatraemia should respond to water restriction. If the above criteria are met, then an increased ADH can be assumed. Causes of SIADH: Malignancies e.g. carcinoma of the bronchus, brain, kidney and intestine; lymphomas. Cerebral disorders infections, trauma, tumours. Pulmonary disorders pneumonia, tuberculosis, pneumothorax. Other Guillain Barré syndrome, acute intermittent porphyria. Management of water overloading Acute water overload. This is a medical emergency due to a rapidly expanded brain volume. The aim of therapy is to prevent progression, as well as to reverse this process. When the serum [Na + ] is < 110 mmol/l and the patient is symptomatic, hypertonic saline (5% NaCl) is infused until the [Na + ] is 120 mmol/l. Excessive expansion of the ECFC and the subsequent development of pulmonary oedema and cardiac failure can be prevented with the concurrent administration of furosemide. Oral fluids should be restricted. Chronic water overload. Chronic water overload may be seen in SIADH. If the patient is symptomatic the treatment will be as for acute water overload. Oral fluid restriction may suffice in the asymptomatic patient. Aggressive rapid correction can be fatal. HYPERNATRAEMIA Unlike hyponatraemia, hypernatraemia is always associated with an increase in the measured plasma osmolality. Consequences of hypernatraemia The resultant hypertonic ECF causes water to move from the ICFC into the ECFC down the osmotic gradient, thereby shrinking cells. Partial cellular recovery occurs within minutes due to solute movement (mainly Na + and Cl - ) into cells. Many cell types, particularly brain cells, have an additional slower adaptive mechanism. They are able to produce osmotically active products of cellular metabolism, known as idiogenic osmoles, which include taurine, glycine, glutamine, sorbitol and inositol. As in hyponatraemia, rapid correction of hypernatraemia, in this case with hypotonic fluids, can be dangerous, especially at the stage where cells have undergone slow osmotic adaptation. Rapid correction will result in swollen brain cells; the patient may have seizures and become comatose. The water deficit should therefore be corrected slowly over hours. Approach to hypernatraemic states (Fig. 6) With euvolaemia When there is a loss of pure water from the body, this loss is shared across both ECFC and ICFC (Fig. 7). Circulatory failure is therefore only a late feature in these cases and only when the [Na + ] is > mmol/l. Replacement should be with tap water. An example is diabetes insipidus (DI), which can be cranial or nephrogenic. In cranial (central) DI, ADH is deficient due to pituitary or hypothalamic disease, while in nephrogenic DI, despite normal ADH secretion, the kidneys are unable to respond (ADH resistance) due to either inherited or acquired causes. Both types present with polyuria and polydipsia and a fluid deprivation test has to be performed to distinguish between them. With hypovolaemia These patients develop hypernatraemia because of loss of hypotonic fluids. In this instance, although the total July 2006 Vol.24 No.7 CME 369 Naicker.indd 369 7/7/06 3:40:05 PM
5 Walmsley RN, White GH. A Guide to Diagnostic Clinical Chemistry. Oxford: Blackwell Scientific Publications, 1994: 3. Yasumasa I, Majzoub JA. Disordered water metabolism: new insights from molecular diagnosis. Curr Opin Endocrinol Diab 1999; 6: Fig. 6. Approach to the different diagnosis of hypernatraemia. Fig. 7. Effect of loss of fluid from the extracellular fluid compartment (ECFC) without replacement with oral/intravenous fluid. body Na + is depleted, the net loss of water from the ECFC is greater. Hypernatraemia is particularly evident when there is failure to respond to thirst, as in the unconscious patient who has had no replacement of the losses, or the patient who has an impaired thirst centre, e.g. the elderly, or patients with head injuries. If hypotonic fluid is considered as having isotonic and pure water components, the loss of hypotonic fluid will be seen to result in proportionally more ECFC volume depletion than would an equivalent amount of pure water. As the ECF volume decreases, there may be signs of shock and if left uncorrected, it may result in the complication of acute tubular necrosis. To prevent this, the ECFC should be rapidly expanded with isotonic fluid (normal saline) until the blood pressure and renal function are restored, and thereafter the pure water deficit can be corrected more slowly. Examples include renal loss due to osmotic diuresis and extrarenal loss due to vomiting, diarrhoea and sweating. Hypervolaemia There is a gain in both water and Na +, although in this instance, the net gain of Na + is relatively more (increased total body water and Na + ), e.g. mineralocorticoid excess as in Conn s syndrome. Patients characteristically do not have oedema and present with hypertension. The underlying cause must be treated. Conclusion Sodium homeostasis is intimately linked with water balance within the body. It is important to consider whether pure fluid losses or gains occurred in isolation or whether they occurred concurrently with salt loss or gain. The duration of the loss also has significant consequences. The patient s physical presentation together with presence of either hyper/hyponatraemia, influence the type of replacement fluid selected, as well as the replacement rate. Injudicious saline-poor or salinerich fluid administration can result in increased morbidity and mortality. Further reading Adrogue HJ, Madias NE. Hypernatraemia. N Engl J Med 2000; 342: Adrogue HJ, Madias NE. Hyponatraemia. N Engl J Med 2000; 342: Marshall WJ, Bangert SK. Clinical Chemistry. Edinburgh: Mosby, 2004: 5. Scott MG, LeGrys DA, Klutts JS. Tietz Textbook of Clinical Chemistry and Molecular Diagnostics. Missouri: Elsevier Saunders Inc, 2006: 4. Singer GG, Brenner BM. Harrison s Principles of Internal Medicine. New York: McGraw-Hill, 2005: 16. IN A NUTSHELL ECF [Na + ] is the main contributor of the ECFC tonicity. When there is pure water loss from the ECFC due to diabetes insipidus, this loss is shared across both intracellular and extracellular compartments. Dehydration is therefore only a late sign. When there is loss of both water and sodium from the ECFC, as in diarrhoea and vomiting, this loss is borne mainly by the ECFC. Dehydration is therefore an early sign. Hypernatraemia is always associated with an increase in the measured plasma osmolality. Hyponatraemia can be associated with a normal, increased or decreased measured plasma osmolality. Rapid correction of hyponatraemia or hypernatraemia after cellular adaptation has taken place can lead to irreversible demyelination of pontine and extrapontine neurones (myelinolysis). SIADH is only diagnosed after excluding cardiac, pituitary, adrenal, thyroid and renal disorders as well as the effect of drugs. Biochemical features of SIADH are true hyponatraemia, an inappropriately concentrated urine and a urine [Na + ] > 20 mmol/l (plasma and urine samples collected at the same time). 370 CME July 2006 Vol.24 No.7 Naicker.indd 370 7/7/06 3:40:16 PM
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
SODIUM BALANCE Overview
 SODIUM BALANCE Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS III Seminar VJ Temple 1 How are solute and solvent related to solution?
SODIUM BALANCE Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS III Seminar VJ Temple 1 How are solute and solvent related to solution?
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines
 Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Wales Critical Care & Trauma Network (North) Management of Hyponatraemia in Intensive Care Guidelines Author: Richard Pugh June 2015 Guideline for management of hyponatraemia in intensive care Background
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters. Dr James Ahlquist Endocrinologist Southend Hospital
 Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters Dr James Ahlquist Endocrinologist Southend Hospital Hyponatraemia: a common electrolyte disorder Electrolyte disorder Prevalence
Hyponatraemia: confident diagnosis, effective treatment and avoiding disasters Dr James Ahlquist Endocrinologist Southend Hospital Hyponatraemia: a common electrolyte disorder Electrolyte disorder Prevalence
Southern Derbyshire Shared Care Pathology Guidelines. Hyponatraemia in Adults
 Southern Derbyshire Shared Care Pathology Guidelines Hyponatraemia in Adults Purpose of Guideline The investigation and management of adult patients with newly diagnosed hyponatraemia. Hyponatraemia can
Southern Derbyshire Shared Care Pathology Guidelines Hyponatraemia in Adults Purpose of Guideline The investigation and management of adult patients with newly diagnosed hyponatraemia. Hyponatraemia can
Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are
 Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Fluid, Electrolyte, and Acid-Base Balance Body Water Content Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60%
Hyponatraemia- Principles, Investigation and Management. Sirazum Choudhury Biochemistry
 Hyponatraemia- Principles, Investigation and Management Sirazum Choudhury Biochemistry Contents Background Investigation Classification Normal Osmolality General management and SIADH Cases Background Relatively
Hyponatraemia- Principles, Investigation and Management Sirazum Choudhury Biochemistry Contents Background Investigation Classification Normal Osmolality General management and SIADH Cases Background Relatively
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Kidneys in regulation of homeostasis
 Kidneys in regulation of homeostasis Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important terms
Kidneys in regulation of homeostasis Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important terms
Abnormalities in serum sodium. David Metz Paediatric Nephrology
 Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
Abnormalities in serum sodium David Metz Paediatric Nephrology Basics Total body sodium regulated by aldosterone and ANP Mediated by intravascular volume (not sodium) RAAS and intrarenal determines Na
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Fluids and electrolytes
 Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
Body Water Content Fluids and electrolytes Infants have low body fat, low bone mass, and are 73% or more water Total water content declines throughout life Healthy males are about 60% water; healthy females
BODY FLUID. Outline. Functions of body fluid Water distribution in the body Maintenance of body fluid. Regulation of fluid homeostasis
 BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
BODY FLUID Nutritional Biochemistry Yue-Hwa Chen Dec 13, 2007 Chen 1 Outline Functions of body fluid Water distribution in the body Maintenance of body fluid Intake vs output Regulation of body fluid Fluid
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
WATER, SODIUM AND POTASSIUM
 WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
WATER, SODIUM AND POTASSIUM Attila Miseta Tamás Kőszegi Department of Laboratory Medicine, 2016 1 Average daily water intake and output of a normal adult 2 Approximate contributions to plasma osmolality
Overview. Fluid & Electrolyte Disorders. Water distribution. Introduction 5/10/2014
 Overview Fluid & Electrolyte Disorders Dr Nicola Barlow Clinical Biochemistry Department, City Hospital Introduction Fluid and electrolyte homeostasis Electrolyte disturbances Analytical parameters Methods
Overview Fluid & Electrolyte Disorders Dr Nicola Barlow Clinical Biochemistry Department, City Hospital Introduction Fluid and electrolyte homeostasis Electrolyte disturbances Analytical parameters Methods
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance
 Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 26 Fluid, Electrolyte, and Acid- Base Balance 1 Body Water Content Infants: 73% or more water (low body fat, low bone mass) Adult males: ~60% water Adult females: ~50% water (higher fat content,
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE
 Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Chapter 27: WATER, ELECTROLYTES, AND ACID-BASE BALANCE I. RELATED TOPICS Integumentary system Cerebrospinal fluid Aqueous humor Digestive juices Feces Capillary dynamics Lymph circulation Edema Osmosis
Hyponatremia. Mis-named talk? Basic Pathophysiology
 Hyponatremia Great Lakes Hospital Medicine Symposium by Brian Wolfe, MD Assistant Professor of Internal Medicine University of Colorado Denver Mis-named talk? Why do we care about Hyponatremia? concentration
Hyponatremia Great Lakes Hospital Medicine Symposium by Brian Wolfe, MD Assistant Professor of Internal Medicine University of Colorado Denver Mis-named talk? Why do we care about Hyponatremia? concentration
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Guidelines for management of. Hyponatremia
 Guidelines for management of Hyponatremia Children s Kidney Centre University Hospital of Wales Cardiff CF14 4XW DISCLAIMER: These guidelines were produced in good faith by the authors reviewing available
Guidelines for management of Hyponatremia Children s Kidney Centre University Hospital of Wales Cardiff CF14 4XW DISCLAIMER: These guidelines were produced in good faith by the authors reviewing available
Regulation of fluid and electrolytes balance
 Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
Regulation of fluid and electrolytes balance Three Compartment Fluid Compartments Intracellular = Cytoplasmic (inside cells) Extracellular compartment is subdivided into Interstitial = Intercellular +
BIOL 221 Chapter 26 Fluids & Electrolytes. 35 slides
 BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender
 BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
BIOL 221 Chapter 26 Fluids & Electrolytes 35 slides 1 Body Water Content Total Body Water is the percentage of a person s weight that is water. TBW can easily vary due to: gender males have higher TBW
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D.
 Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
Regulation of Body Fluids: Na + and Water Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. Why body sodium content determines ECF volume and the relationships
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Hormonal Control of Osmoregulatory Functions *
 OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
OpenStax-CNX module: m44828 1 Hormonal Control of Osmoregulatory Functions * OpenStax This work is produced by OpenStax-CNX and licensed under the Creative Commons Attribution License 3.0 By the end of
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Chapter 15 Fluid and Acid-Base Balance
 Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Chapter 15 Fluid and Acid-Base Balance by Dr. Jay M. Templin Brooks/Cole - Thomson Learning Fluid Balance Water constitutes ~60% of body weight. All cells and tissues are surrounded by an aqueous environment.
Body fluids. Lecture 13:
 Lecture 13: Body fluids Body fluids are distributed in compartments: A. Intracellular compartment: inside the cells of the body (two thirds) B. Extracellular compartment: (one third) it is divided into
Lecture 13: Body fluids Body fluids are distributed in compartments: A. Intracellular compartment: inside the cells of the body (two thirds) B. Extracellular compartment: (one third) it is divided into
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Basic Fluid and Electrolytes
 Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Basic Fluid and Electrolytes Chapter 22 Basic Fluid and Electrolytes Introduction Infants and young children have a greater need for water and are more vulnerable to alterations in fluid and electrolyte
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua
 Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
Water (Dysnatremia) & Sodium (Dysvolemia) Disorders Ahmad Raed Tarakji, MD, MSPH, PGCertMedEd, FRCPC, FACP, FASN, FNKF, FISQua Assistant Professor Nephrology Unit, Department of Medicine College of Medicine,
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19](/thumbs/80/80449526.jpg) 1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
8. URINE CONCENTRATION
 8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
DIURETICS-4 Dr. Shariq Syed
 DIURETICS-4 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Loop diuretics act on which transporter PKCC NKCC2 AIKTCC I Don t know AIKTC - Knowledge Resources & Relay Center 2 Pop
DIURETICS-4 Dr. Shariq Syed AIKTC - Knowledge Resources & Relay Center 1 Pop Quiz!! Loop diuretics act on which transporter PKCC NKCC2 AIKTCC I Don t know AIKTC - Knowledge Resources & Relay Center 2 Pop
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Diuretic Agents Part-2. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Diuretic Agents Part-2 Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Potassium-sparing diuretics The Ion transport pathways across the luminal and basolateral
Metabolism of water and electrolytes. 2. Special pathophysiology disturbances of intravascular volume and
 Metabolism of water and electrolytes 1. Physiology and general pathophysiology Compartments of body fluids Regulation of volume and tonicity (osmolality) Combinations of volume and osmolality disorders
Metabolism of water and electrolytes 1. Physiology and general pathophysiology Compartments of body fluids Regulation of volume and tonicity (osmolality) Combinations of volume and osmolality disorders
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Blood Pressure Regulation 2 Faisal I. Mohammed, MD,PhD 1 Objectives Outline the intermediate term and long term regulators of ABP. Describe the role of Epinephrine, Antidiuretic hormone (ADH), Renin-Angiotensin-Aldosterone
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
HYPONATRAEMIA: NUH GUIDELINE FOR INITIAL ASSESSMENT AND MANAGEMENT.
 HYPONATRAEMIA: NUH GUIDELINE FOR INITIAL ASSESSMENT AND MANAGEMENT. HYPONATRAEMIA: SODIUM < 130 MMOL/L SIGNIFICANT. Symptoms/signs usually only occur when sodium < 125 mmol/l. Acute hyponatraemia is less
HYPONATRAEMIA: NUH GUIDELINE FOR INITIAL ASSESSMENT AND MANAGEMENT. HYPONATRAEMIA: SODIUM < 130 MMOL/L SIGNIFICANT. Symptoms/signs usually only occur when sodium < 125 mmol/l. Acute hyponatraemia is less
Answers and Explanations
 Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Principles of Anatomy and Physiology
 Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Principles of Anatomy and Physiology 14 th Edition CHAPTER 27 Fluid, Electrolyte, and Acid Base Fluid Compartments and Fluid In adults, body fluids make up between 55% and 65% of total body mass. Body
Fal Fal P h y s i o l o g y 6 1 1, S a n F r a n c i s c o S t a t e U n i v e r s i t y
 Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fall 12 OSMOTIC REGULATION OF THE RENAL SYSTEM: Effects of fasting and ingestion of water, coke, or Gatorade on urine flow rate and specific gravity Dorette Franks The purpose of the physiology experiment
Fluids and electrolytes: the basics
 Fluids and electrolytes: the basics This document is based on the handout from the Surgery for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical
Fluids and electrolytes: the basics This document is based on the handout from the Surgery for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical
Disorders of sodium balance after brain injury Kate Bradshaw MBBS FRCA Martin Smith MBBS FRCA
 Disorders of sodium balance after brain injury Kate Bradshaw MBBS FRCA Martin Smith MBBS FRCA Sodium disturbances are common in patients with brain injury because of the major role that the central nervous
Disorders of sodium balance after brain injury Kate Bradshaw MBBS FRCA Martin Smith MBBS FRCA Sodium disturbances are common in patients with brain injury because of the major role that the central nervous
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Faculty version with model answers
 Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
DOWNLOAD OR READ : SYNDROME OF INAPPROPRIATE SECRETION OF ANTIDIURETIC HORMONE IN MALIGNANCY PDF EBOOK EPUB MOBI Page 1 Page 2 syndrome of inappropriate secretion of antidiuretic hormone in malignancy
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi
 Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Terminology. Terminology. Terminology. Molarity number of moles of solute / Liter of solution. a) Terminology b) Body Fluid Compartments
 Integrative Sciences: Biological Systems A Fall 2011 Body Fluids Compartments, Renal Clearance and Renal Excretion of Drugs Monday, November 21, 2011 Lisa M. Harrison-Bernard, Ph.D. Department of Physiology;
Integrative Sciences: Biological Systems A Fall 2011 Body Fluids Compartments, Renal Clearance and Renal Excretion of Drugs Monday, November 21, 2011 Lisa M. Harrison-Bernard, Ph.D. Department of Physiology;
Hyponatraemia. Dr Andy Lewington Consultant Nephrologist/Honorary Clinical Associate Professor Leeds Teaching Hospitals
 Hyponatraemia Dr Andy Lewington Consultant Nephrologist/Honorary Clinical Associate Professor Leeds Teaching Hospitals A.J.P.Lewington@leeds.ac.uk Disclosures of Interest Associate Clinical Director NIHR
Hyponatraemia Dr Andy Lewington Consultant Nephrologist/Honorary Clinical Associate Professor Leeds Teaching Hospitals A.J.P.Lewington@leeds.ac.uk Disclosures of Interest Associate Clinical Director NIHR
Blood Pressure Fox Chapter 14 part 2
 Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Vert Phys PCB3743 Blood Pressure Fox Chapter 14 part 2 T. Houpt, Ph.D. 1 Cardiac Output and Blood Pressure How to Measure Blood Pressure Contribution of vascular resistance to blood pressure Cardiovascular
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Public Assessment Report. Scientific discussion. Natriumklorid Abcur (sodium chloride) SE/H/1443/01/MR
 Public Assessment Report Scientific discussion Natriumklorid Abcur (sodium chloride) SE/H/1443/01/MR This module reflects the scientific discussion for the approval of Natriumklorid Abcur. The procedure
Public Assessment Report Scientific discussion Natriumklorid Abcur (sodium chloride) SE/H/1443/01/MR This module reflects the scientific discussion for the approval of Natriumklorid Abcur. The procedure
Physiology of the body fluids, Homeostasis
 Physiology of the body fluids, Homeostasis Tamas Banyasz The Body as an open system 1. Open system: The body exchanges material and energy with its environment 2. Homeostasis: The process through which
Physiology of the body fluids, Homeostasis Tamas Banyasz The Body as an open system 1. Open system: The body exchanges material and energy with its environment 2. Homeostasis: The process through which
IV Fluids. I.V. Fluid Osmolarity Composition 0.9% NaCL (Normal Saline Solution, NSS) Uses/Clinical Considerations
 IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
IV Fluids When administering IV fluids, the type and amount of fluid may influence patient outcomes. Make sure to understand the differences between fluid products and their effects. Crystalloids Crystalloid
Potassium secretion. E k = -61 log ([k] inside / [k] outside).
![Potassium secretion. E k = -61 log ([k] inside / [k] outside). Potassium secretion. E k = -61 log ([k] inside / [k] outside).](/thumbs/80/80478709.jpg) 1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
1 Potassium secretion In this sheet, we will continue talking about ultrafiltration in kidney but with different substance which is K+. Here are some informations that you should know about potassium;
Disclaimer. Chapter 3 Disorder of Water, Electrolyte and Acid-base Professor A. S. Alhomida. Disorder of Water and Electrolyte
 Disclaimer King Saud University College of Science Department of Biochemistry The texts, tables, figures and images contained in this course presentation (BCH 376) are not my own, they can be found on:
Disclaimer King Saud University College of Science Department of Biochemistry The texts, tables, figures and images contained in this course presentation (BCH 376) are not my own, they can be found on:
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES
 Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Amjad Bani Hani Ass.Prof. of Cardiac Surgery & Intensive Care FLUIDS AND ELECTROLYTES Body Water Content Water Balance: Normal 2500 2000 1500 1000 500 Metab Food Fluids Stool Breath Sweat Urine
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
THe Story of salty Sam
 THe Story of salty Sam Understanding fluids, urea and electrolyte balance; a quantitative approach. A self-directed learning activity. Part One. meet salty sam Salty Sam is a pretty average 70 kg bloke,
THe Story of salty Sam Understanding fluids, urea and electrolyte balance; a quantitative approach. A self-directed learning activity. Part One. meet salty sam Salty Sam is a pretty average 70 kg bloke,
ELECTROLYTES RENAL SHO TEACHING
 ELECTROLYTES RENAL SHO TEACHING Metabolic Alkalosis 2 factors are responsible for generation and maintenance of metabolic alkalosis this includes a process that raises serum bicarbonate and a process that
ELECTROLYTES RENAL SHO TEACHING Metabolic Alkalosis 2 factors are responsible for generation and maintenance of metabolic alkalosis this includes a process that raises serum bicarbonate and a process that
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Disorders of water and sodium homeostasis. Prof A. Pomeranz 2017
 Disorders of water and sodium homeostasis Prof A. Pomeranz 2017 Pediatric (Nephrology) Tool Box Disorders of water and sodium homeostasis Pediatric Nephrology Tool Box Hyponatremiaand and Hypernatremia
Disorders of water and sodium homeostasis Prof A. Pomeranz 2017 Pediatric (Nephrology) Tool Box Disorders of water and sodium homeostasis Pediatric Nephrology Tool Box Hyponatremiaand and Hypernatremia
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Correction of hypervolaemic hypernatraemia by inducing negative Na + and K + balance in excess of negative water balance: a new quantitative approach
 Nephrol Dial Transplant (2008) 23: 2223 2227 doi: 10.1093/ndt/gfm932 Advance Access publication 18 February 2008 Original Article Correction of hypervolaemic hypernatraemia by inducing negative Na + and
Nephrol Dial Transplant (2008) 23: 2223 2227 doi: 10.1093/ndt/gfm932 Advance Access publication 18 February 2008 Original Article Correction of hypervolaemic hypernatraemia by inducing negative Na + and
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
INTRAVENOUS FLUID THERAPY
 INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
INTRAVENOUS FLUID THERAPY PRINCIPLES Postnatal physiological weight loss is approximately 5 10% in first week of life Preterm neonates have more total body water and may lose 10 15% of their weight in
BASIC MEDICAL SCIENCE OF THE RENAL AND URINARY SYSTEMS
 Ch01M3428.qxd 12/5/06 6:47 M age 1 BASIC MEDICAL SCIENCE OF THE RENAL AND URINARY SYSTEMS Basic principles 3 Organization of the kidneys 13 Renal function 39 The kidneys in disease 65 The lower urinary
Ch01M3428.qxd 12/5/06 6:47 M age 1 BASIC MEDICAL SCIENCE OF THE RENAL AND URINARY SYSTEMS Basic principles 3 Organization of the kidneys 13 Renal function 39 The kidneys in disease 65 The lower urinary
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
After studying this lecture, you should be able to...
 Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Reabsorption of Salt and Water After studying this lecture, you should be able to... 1. Define the obligatory water loss. 2. Describe the mechanism of Na ++ reabsorption in the distal tubule and explain
Mechanism: 1- waterretention from the last part of the nephron which increases blood volume, venous return EDV, stroke volume and cardiac output.
 Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Blood pressure regulators: 1- Short term regulation:nervous system Occurs Within secondsof the change in BP (they are short term because after a while (2-3 days) they adapt/reset the new blood pressure
Sunday, July 17, 2011 URINARY SYSTEM
 URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
URINARY SYSTEM URINARY SYSTEM Let s take a look at the anatomy first! KIDNEYS: are complex reprocessing centers where blood is filtered through and waste products are removed. Wastes and extra water become
Regulating the Internal Environment. AP Biology
 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
Instrumental determination of electrolytes in urine. Amal Alamri
 Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Instrumental determination of electrolytes in urine Amal Alamri What is the Electrolytes? Electrolytes are positively and negatively chargedions, Found in Within body's cells extracellular fluids, including
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS
 Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
Monday, 17 April 2017 BODY FLUID HOMEOSTASIS Phenomenon: shipwrecked sailor on raft in ocean ("water, water everywhere but not a drop to drink") Why are the sailors thirsty? (What stimulated thirst?) Why
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
