Review Article C-Peptide Effects on Renal Physiology and Diabetes
|
|
|
- Marcus Parks
- 5 years ago
- Views:
Transcription
1 Hindawi Publishing Corporation Experimental Diabetes Research Volume 2008, Article ID , 5 pages doi: /2008/ Review Article C-Peptide Effects on Renal Physiology and Diabetes L. Rebsomen, A. Khammar, D. Raccah, and M. Tsimaratos UPRES EA 21-93, Laboratoire de Diabétologie, Faculté de Médecine de Marseille, Université de la Méditerranée, Marseille Cedex 05, France Correspondence should be addressed to M. Tsimaratos, michel.tsimaratos@mail.ap-hm.fr Received 1 November 2007; Accepted 10 April 2008 Recommended by Thomas Forst The C-peptide of proinsulin is important for the biosynthesis of insulin and has for a long time been considered to be biologically inert. Animal studies have shown that some of the renal effects of the C-peptide may in part be explained by its ability to stimulate the Na,K-ATPase activity. Precisely, the C-peptide reduces diabetes-induced glomerular hyperfiltration both in animals and humans, therefore, resulting in regression of fibrosis. The tubular function is also concerned as diabetic animals supplemented with C-peptide exhibit better renal function resulting in reduced urinary sodium waste and protein excretion together with the reduction of the diabetes-induced glomerular hyperfiltration. The tubular effectors of C-peptide were considered to be tubule transporters, but recent studies have shown that biochemical pathways involving cellular kinases and inflammatory pathways may also be important. The matter theory concerning the C-peptide effects is a metabolic one involving the effects of the C-peptide on lipidic metabolic status.this review concentrates on the most convincing data which indicate that the C-peptide is a biologically active hormone for renal physiology. Copyright 2008 L. Rebsomen et al. This is an open access article distributed under the Creative Commons Attribution License, which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited. 1. INTRODUCTION Diabetes mellitus is a chronic metabolic disorder relative to insulin deficit that induces metabolic and degenerative complications in various organs, including nerves, heart, and kidneys [1]. C-peptide, secreted in blood stream in equimolar amounts with insulin, was considered to be a reliable marker of residual beta-cell function [2 4]. During the past decade, numerous studies in both humans and animals have demonstrated that C-peptide, although not influencing blood sugar control, might play a role in preventing and potentially reversing some of the chronic complications of type 1 diabetes, especially diabetic nephropathy [5 23]. Thus C-peptide may be an active peptide with relevant physiologic effects different from and complementary to those of insulin [24]. Several theories have been raised to explain C-peptide effects on renal function during diabetes. This review focuses on the most convincing theories that are implicated in C- peptide effects on renal function. 2. C-PEPTIDE AND GLOMERULAR FUNCTION 2.1. C-peptide Effects on Renal Function have been Demonstrated in Humans Johansson et al. conducted a double blind study that measured glomerular filtration rate and proteinuria in type 1 diabetic patients with basal microalbuminuria, a marker of early stages of diabetic nephropathy. After three months of substitution by both C-peptide and insulin, patients exhibited a better glycemic control, a reduction of diabetesinduced glomerular hyperfiltration and microalbuminuria [7]. In another study, they confirmed that proteinuria was significantly reduced in the C-peptide group during the cross-over period [9]. Both studies were conducted in diabetic patients so that the effects of C-peptide could not be differentiated from an improved glycemic control. However, the same group examined the short-term effect of C-peptide infusion on renal function in insulin-treated diabetic patients and found similar results on glomerular filtration rate [5]. Altogether, these papers strongly argue for a specific C-peptide-related effect on glomerular function. Recently, Fiorina et al. observed that renal and pancreatic transplantation of diabetic patients resulted in a better renal graft outcome. They observed kidney and erythrocyte Na,K-ATPase activity, and stabilization of microalbuminuria correlated with residual pancreatic secretion [14, 15]. In chronic renal failure type 1 diabetic patients, residual pancreatic activity, restored by kidney-pancreas transplantation resulted in enhanced kidney graft survival, hypertrophy, and vascular function [25]. Furthermore, combined kidney-pancreas
2 2 Experimental Diabetes Research transplantation was associated with better high-energy phosphates metabolism than in kidney alone transplantation, suggesting that restoration of beta-cell function positively affects kidney graft metabolism [26]. All these data raised the question of C-peptide being a kidney protector [27] Similar Studies were Conducted in Animal Models In experimental conditions, several groups have shown that streptozotocin-induced diabetic rats treated with C-peptide exhibit improvement of metabolic status, renal function, and reversal of some of the morphologic changes associated with diabetic nephropathy [20, 21, 28]. Sjoquist et al. showed that perfusion of C-peptide results in significantly reduction of both proteinuria and diabetesinduced glomerular hyperfiltration which is considered to be the initial state of diabetic nephropathy in streptozotocin rats. They also showed that C-peptide also restores renal functional reserve [20]. In another study, they confirmed that 14 days of C-peptide perfusion prevented glomerular hypertrophy [21]. Theses results were confirmed by Kamikawa et al. that could demonstrate, in the same experimental model, that C- peptide suppresses diabetes-induced abnormal glomerular enos expression [29]. The mechanisms involved in glomerular effects was supposed to be an constriction of the glomerular afferent arteriols [30]. Altogether, these studies suggest that the absence of C- peptide contributes to the initial state of diabetic nephropathy. Evidence comes from specific studies that the C-terminal EVARQ fragment of the C-peptide molecule is responsible for most of the observed effects [31]. Although seducing, the glomerulocentric view of renal function during diabetes has been challenged by Thomson et al. that explored to tubuloglomerular feedback in this situation [32]. The results of their studies clearly established that a tubulocentric view of diabetes-associated nephropathy could be considered [33]. Interestingly, renal C-peptide effects were also constant with this hypothesis. 3. C-PEPTIDE AND TUBULAR FUNCTION More than twenty years ago, Wald et al. suggested that tubular Na,K-ATPase activity was related to glomerular filtration rate during diabetes [34]. Several groups have confirmed the time-dependant evolution of Na,K-ATPase activity during diabetes, and the role of Na transport (for review see [35]). Recently, Kim et al. have raised the hypothesis that uncontrolled diabetes results in increased levels of several proteins including sodium transporters such as BSC1. They suggested that the enhanced expression of sodium transporters are compensatory changes that prevent a progressive decline in urinary concentrating ability despite the continuing osmotic diuresis [36]. Thus they showed that the regulation of BSC1 was not dependant on vasopressin during streptozotocin-induced diabetes in brattelboro rats [36]. Bardoux et al. have shown that vasopressin plays a crucial role in the onset and aggravation of the renal complications of diabetes. The mechanisms involve the tubular fluid in the loop of Henle, inhibition of the tubuloglomerular feedback control of glomerular function, and alterations in glomerular hemodynamics [37]. All these data support the hypothesis that the renal tubule is involved early in the course of diabetic nephropathy. Therefore, the effects of C-peptide substitution on renal tubule during type 1 diabetes were considered The Transport Theory The Na,K-ATPase is an ubiquitous membrane-bound enzyme complex that plays fundamental role in cellular function. The basic function of the Na,K-ATPase is to maintain the high Na+ and K+ gradient across the plasma membrane of animal cells, at the expense of ATP hydrolysis (for review see [38]). Cellular C-peptide action is mediated through Na,K-ATPase activation in various organs including kidney [18, 19, 39]. Interestingly, Na+,K+-ATPase activity is increased during the first weeks after diabetes onset, and then decreased in various organs damaged by long-term diabetic degenerative complications, including kidney [40 47]. We have shown that C-peptide restores both glomerular and tubular function in diabetic rats. In vivo, C-peptide supplementation for one month improved body weight in streptozotocin-induced diabetic rats and decreased urinary sodium wasting [28]. A compensatory mechanism to conserve water and solute may involve changes in the abundance of the medullary transport proteins involved in the sodium handling. In a recent study, we observed that in vivo C-peptide supplementation for one month induced no changes in kidney abundance and transcription status of several tubular sodium transporters including the epithelial sodium channel (EnaC), and NKCC2/BSC1 cotransporter in diabetic rats. In this study, rats were made diabetic after streptozotocin injection and then were submitted to infusion with physiological doses of either insulin, homologous C- peptide, or both (unpublished data). Thus the transport theory of C-peptide s action is probably not relying on changes in amounts of renal tubule Na transporters The Biochemical Theory Even if the trigger of sodium Na transport is not dependent on changes in Na transporters, the effects on Na,K-ATPase activity and expression are permanent findings. Several groups have shown that C-peptide action was probably secondary to biochemical changes. The first argument was found in renal cells that exhibited intracellular calcium increase secondary to C-peptide exposure [18]. Then several groups showed that incubation of various cell line types with C-peptide resulted in PKC, MAPK, ERK activation (for review see [24]). Other studies have suggested that diabetes is a state of increased renal nitric oxide (NO) activity as assessed by urinary excretion of nitrites and nitrates (NOx), and that NO synthase inhibitors reverse the increased glomerular filtration rate (GFR) observed in experimental diabetes.
3 L. Rebsomen et al. 3 Interestingly, in contrast to the effects on renal haemodynamics, NO does not play an important role in the altered renal sodium handling observed in experimental diabetes [48] The Inflammatory Theory G C-peptide EVARQ fragment Adiponectin PPARγ TNF C-peptide causes multiple molecular and physiological effects, and improves renal and neuronal dysfunction in patients with diabetes. However, whether C-peptide controls the inhibitor kappab (IkappaB)/NF-kappaB-dependent transcription of genes, including inflammatory genes was unknown. Peroxisome proliferator-activated receptor gamma (PPARgamma) has key roles in the regulation of adipogenesis, inflammation, and lipid and glucose metabolism. These issues were progressively answered. In an in vitro model, both insulin and C-peptide induced a concentrationdependent stimulation of PPARgamma transcriptional activity [49]. Another step was made by Kitazawa et al. that showed that C-peptide stimulates the transcription of inflammatory genes via activation of a PKC/IkappaB/NFkappaB signaling pathway [50]. The inflammatory theory was further supported by Maezawa et al. that reported C- peptide TGF-beta surppession in STZ-model [51]. These experimental data confirm that C-peptide exerts a wide range of cellular effects (see Figure 1). Some of them may be relevant to explain renal tubular effects The metabolic theory The effects of C-peptide on lipidic metabolic status have not been documented yet. Thus the effects of C-peptide on PPAR expression triggered the curiosity on the role of the adipocyte network and its relationship with renal physiology. Preliminary results of our group showed that C-peptide infusion for one month improved lipidic status of streptozotocin rats, by reducing cholesterol and triglycerid levels, but did not influence renal PPAR gamma expression (rebsomen et al. work in progress). On the other side, C-peptide reduced the adiponectin released by human adipocytes (Khammar et al. work in progress). Thus if the mechanism of C-peptide effect on lipid metabolism remains to be elucidated, it is known that diabetes results in inhibition of several enzymatic reactions that are accessible to nutritional supplementation, and influence renal tubular physiology [52]. Although the metabolic theory stays to be documented, both the influence of the PPAR system on diabetic nephropathy and of C- peptide on PPAR are becoming obvious [53, 54]. In addition, these studies strongly suggest that both renal glomerule and tubule are a major site of C-peptide action. During type 1 diabetes, C-peptide substitution restores in part the functional properties of the renal tubule and, therefore, allows better renal function and metabolic status. 4. CONCLUSION In humans, C-peptide exerts a regulatory and physiologic influence on renal function in patients with type 1 diabetes. Successful islet transplantation has been associated with +Pi Ca 2+ PKCα Na, K-ATPase MAPK ERK PKC NO IκB/NFκB TGFβ Figure 1: Modelization of C-peptide effects on renal tubule. The EVARQ fragment of C-peptide binds to a membrane G-protein couple receptor of a tubule cell. Intracellular calcium increase results in activation of PKCa and affects Na,K-ATPase activity. Together with this effect, an increase of intracellular kinases results in either activation or inhibition of inflammatory mediators. Green indicates stimulation, red inhibition. Arrows in dash lines are suggested pathways. improvements in kidney graft survival rates and function among uremic patients with type 1 diabetes mellitus and kidney grafts. This suggests that together with the positive effects of normalization of glycometabolic control, successful islet transplantation exerts beneficial effects on kidney function, in part by restoring the C-peptide secretion, a situation closer to the endogenous pancreatic function. Although the mechanisms are not fully understood, a hormonal therapeutic role of C-peptide as an active protective factor for the diabetic kidney should be considered. REFERENCES [1] G. L. King and M. Brownlee, The cellular and molecular mechanisms of diabetic complications, Endocrinology and Metabolism Clinics of North America, vol. 25, no. 2, pp , [2] D. F. Steiner, Evidence for a precursor in the biosynthesis of insulin, Transactions of the New York Academy of Sciences, vol. 30, no. 1, pp , [3] D. F. Steiner, Proinsulin and the biosynthesis of insulin, The New England Journal of Medicine, vol. 280, no. 20, pp , [4] D. F. Steiner, Proinsulin, Triangle, vol. 11, no. 2, pp , [5] B.-L. Johansson, S. Sjoberg, and J. Wahren, The influence of human C-peptide on renal function and glucose utilization in type 1(insulin-dependent) diabetic patients, Diabetologia, vol. 35, no. 2, pp , [6] B.-L. Johansson, B. Linde, and J. Wahren, Effects of C- peptide on blood flow, capillary diffusion capacity and glucose utilization in the exercising forearm of type 1 (insulin-dependent)diabetic patients, Diabetologia, vol. 35, no. 12, pp , 1992.
4 4 Experimental Diabetes Research [7] B.-L. Johansson, A. Kernell, S. Sjoberg, and J. Wahren, Influence of combined C-peptide and insulin administration on renal function and metabolic control in diabetes type 1, Journal of Clinical Endocrinology & Metabolism, vol. 77, no. 4, pp , [8] B.-L. Johansson, K. Borg, E. Fernqvist-Forbes, T. Odergren, S. Remahl, and J. Wahren, C-peptide improves autonomic nerve function in IDDM patients, Diabetologia, vol. 39, no. 6, pp , [9] B.-L. Johansson, K. Borg, E. Fernqvist-Forbes, A. Kernell, T. Odergren, and J. Wahren, Beneficial effects of C-peptide on incipient nephropathy and neuropathy in patients with type 1 diabetes mellitus, Diabetic Medicine, vol. 17, no. 3, pp , [10] A. Djemli-Shipkolye, P. Gallice, T. Coste, et al., The effects ex vivo and in vitro of insulin and C-peptide on Na/K adenosine triphosphatase activity in red blood cell membranes of type 1 diabetic patients, Metabolism, vol. 49, no. 7, pp , [11] D. D. de La Tour, D. Raccah, M. F. Jannot, T. Coste, C. Rougerie, and P. Vague, Erythrocyte Na/K ATPase activity and diabetes: relationship with C-peptide level, Diabetologia, vol. 41, no. 9, pp , [12] A. Djemli-Shipkolye, T. Coste, D. Raccah, P. Vague, G. Pieroni, and A. Gerbi, Na,K-atpase alterations in diabetic rats: relationship with lipid metabolism and nerve physiological parameters, Cellular and Molecular Biology, vol.47,no.2,pp , [13] T. Forst, D. D. de La Tour, T. Kunt, et al., Effects of proinsulin C-peptide on nitric oxide, microvascular blood flow and erythrocyte Na +,K + -ATPase activity in diabetes mellitus type I, Clinical Science, vol. 98, no. 3, pp , [14] P. Fiorina, F. Folli, P. Maffi, et al., Islet transplantation improves vascular diabetic complications in patients with diabetes who underwent kidney transplantation: a comparison between kidney-pancreas and kidney-alone transplantation, Transplantation, vol. 75, no. 8, pp , [15] P. Fiorina, F. Folli, F. Bertuzzi, et al., Long-term beneficial effect of islet transplantation on diabetic macro- /microangiopathy in type 1 diabetic kidney-transplanted patients, Diabetes Care, vol. 26, no. 4, pp , [16] R. Rigler, A. Pramanik, P. Jonasson, et al., Specific binding of proinsulin C-peptide to human cell membranes, Proceedings of the National Academy of Sciences of the United States of America, vol. 96, no. 23, pp , [17] K. Lindström, C. Johansson, E. Johnsson, and B. Haraldsson, Acute effects of C-peptide on the microvasculature of isolated perfused skeletal muscles and kidneys in rat, Acta Physiologica Scandinavica, vol. 156, no. 1, pp , [18] Y. Ohtomo, A. Aperia, B. Sahlgren, B.-L. Johansson, and J. Wahren, C-peptide stimulates rat renal tubular Na +, K + - ATPase activity in synergism with neuropeptide Y, Diabetologia, vol. 39, no. 2, pp , [19] Y. Ohtomo, T. Bergman, B.-L. Johansson, H. Jörnvall, and J. Wahren, Differential effects of proinsulin C-peptide fragments on Na +,K + - ATPase activity of renal tubule segments, Diabetologia, vol. 41, no. 3, pp , [20] M. Sjoquist, W. Huang, and B.-L. Johansson, Effects of C- peptide on renal function at the early stage of experimental diabetes, Kidney International, vol. 54, no. 3, pp , [21] B. Samnegård, S. H. Jacobson, G. Jaremko, B.-L. Johansson, and M. Sjöquist, Effects of C-peptide on glomerular and renal size and renal function in diabetic rats, Kidney International, vol. 60, no. 4, pp , [22] A. A. F. Sima, W. Zhang, K. Sugimoto, et al., C-peptide prevents and improves chronic type I diabetic polyneuropathy in the BB/Wor rat, Diabetologia, vol. 44, no. 7, pp , [23] P. Vague, T. C. Coste, M. F. Jannot, D. Raccah, and M. Tsimaratos, C-peptide, Na +,K + -ATPase, and diabetes, Experimental Diabesity Research, vol. 5, no. 1, pp , [24] J. Wahren, J. Shafqat, J. Johansson, A. Chibalin, K. Ekberg, and H. Jörnvall, Molecular and cellular effects of C-peptide new perspectives on an old peptide, Experimental Diabesity Research, vol. 5, no. 1, pp , [25] P. Fiorina, M. Venturini, F. Folli, et al., Natural history of kidney graft survival, hypertrophy, and vascular function in end-stage renal disease type 1 diabetic kidney-transplanted patients: beneficial impact of pancreas and successful islet cotransplantation, Diabetes Care, vol. 28, no. 6, pp , [26] P. Fiorina, G. Perseghin, F. De Cobelli, et al., Altered kidney graft high-energy phosphate metabolism in kidneytransplanted end-stage renal disease type 1 diabetic patients: a cross-sectional analysis of the effect of kidney alone and kidney-pancreas transplantation, Diabetes Care, vol. 30, no. 3, pp , [27] A. M. J. Shapiro, Islet transplants and impact on secondary diabetic complications: does C-peptide protect the kidney? JournaloftheAmericanSocietyofNephrology, vol. 14, no. 8, pp , [28] L. Rebsomen, S. Pitel, F. Boubred, et al., C-peptide replacement improves weight gain and renal function in diabetic rats, Diabetes & Metabolism, vol. 32, no. 3, pp , [29] A. Kamikawa, T. Ishii, K. Shimada, et al., Proinsulin C- peptide abrogates type-1 diabetes-induced increase of renal endothelial nitric oxide synthase in rats, Diabetes/Metabolism Research and Reviews, vol. 24, no. 4, pp , [30] L. Nordquist, E. Y. Lai, M. Sjöquist, A. Patzak, and A. E. G. Persson, Proinsulin C-peptide constricts glomerular afferent arterioles in diabetic mice. A potential renoprotective mechanism, American Journal of Physiology, vol. 294, no. 3, pp. R835 R841, [31] L. Nordquist, E. Moe, and M. Sjöquist, The C-peptide fragment EVARQ reduces glomerular hyperfiltration in streptozotocin-induced diabetic rats, Diabetes/Metabolism Research and Reviews, vol. 23, no. 5, pp , [32] S. C. Thomson, A. Deng, D. Bao, J. Satriano, R. C. Blantz, and V. Vallon, Ornithine decarboxylase, kidney size, and the tubular hypothesis of glomerular hyperfiltration in experimental diabetes, Journal of Clinical Investigation, vol. 107, no. 2, pp , [33] S. C. Thomson, V. Vallon, and R. C. Blantz, Kidney function in early diabetes: the tubular hypothesis of glomerular filtration, American Journal of Physiology, vol. 286, no. 1, pp. F8 F15, [34] H. Wald and M. M. Popovtzer, The effect of streptozotocininduced diabetes mellitus on urinary excretion of sodium and renal Na + -K + -ATPase activity, Pflugers Archiv European Journal of Physiology, vol. 401, no. 1, pp , [35] M. Tsimaratos, Physiological effects of the connecting peptide, Archives de Pediatrie, vol. 12, no. 4, pp , [36] T.-H.Kwon,J.Nielsen,Y.-H.Kim,M.A.Knepper,J.Frøkiaer, and S. Nielsen, Regulation of sodium transporters in the thick ascending limb of rat kidney: response to angiotensin II,
5 L. Rebsomen et al. 5 American Journal of Physiology, vol. 285, no. 1, pp. F152 F165, [37] P. Bardoux, P. Bruneval, D. Heudes, N. Bouby, and L. Bankir, Diabetes-induced albuminuria: role of antidiuretic hormone as revealed by chronic V 2 receptor antagonism in rats, Nephrology Dialysis Transplantation, vol. 18, no. 9, pp , [38] E. Féraille and A. Doucet, Sodium-potassium-adenosinetriphosphatase-dependent sodium transport in the kidney: hormonal control, Physiological Reviews, vol. 81, no. 1, pp , [39] M. Tsimaratos, F. Roger, D. Chabardès, et al., C-peptide stimulates Na +, K + -ATPase activity via PKC alpha in rat medullary thick ascending limb, Diabetologia, vol. 46, no. 1, pp , [40] M. Tsimarato, T. C. Coste, A. Djemli-Shipkolye, et al., Evidence of time-dependent changes in renal medullary Na,K-ATPase activity and expression in diabetic rats, Cellular and Molecular Biology, vol. 47, no. 2, pp , [41] D. Raccah, M. F. Lamotte-Jannot, T. Issautier, and P. Vague, Effect of experimental diabetes on Na/K-ATPase activity in red blood cells, peripheral nerve and kidney, Diabetes & Metabolism, vol. 20, no. 3, pp , [42]D.Raccah,T.Coste,N.E.Cameron,D.Dufayet,P.Vague, and T. C. Hohman, Effect of the aldose reductase inhibitor tolrestat on nerve conduction velocity, Na/K ATPase activity, and polyols in red blood cells, sciatic nerve, kidney cortex, and kidney medulla of diabetic rats, Journal of Diabetes and Its Complications, vol. 12, no. 3, pp , [43] S. F. Leong and T. K. C. Leung, Diabetes induced by streptozotocin causes reduced Na-K ATPase in the brain, Neurochemical Research, vol. 16, no. 10, pp , [44] Y.-C. Ng, P. H. Tolerico, and C.-B. Book, Alterations in levels of Na + -K + -ATPase isoforms in heart, skeletal muscle, and kidney of diabetic rats, American Journal of Physiology, vol. 265, no. 2, part 1, pp. E243 E251, [45] P. Öner, B. Öztaş,andH.Koçak, Brain cortex Na + -K + ATPase activities in streptozotocin-diabetic and pentylenetetrazolepileptic rats, Pharmacological Research, vol. 36, no. 1, pp , [46] A. Ottlecz, C. A. Garcia, J. Eichberg, and D. A. Fox, Alterations in retinal Na +,K + -ATPase in diabetes: streptozotocin-induced and Zucker diabetic fatty rats, Current Eye Research, vol. 12, no. 12, pp , [47] T. Ohara, K. E. Sussman, and B. Draznin, Effect of diabetes on cytosolicfreeca 2+ and Na + -K + -ATPase in rat aorta, Diabetes, vol. 40, no. 11, pp , [48] R. Komers and S. Anderson, Paradoxes of nitric oxide in the diabetic kidney, American Journal of Physiology, vol. 284, no. 6, pp. F1121 F1137, [49] N. M. Al-Rasheed, R. S. Chanai, R. J. Baines, G. B. Willars, and N. J. Brunskill, Ligand-independent activation of peroxisome proliferator-activated receptor-γ by insulin and C-peptide in kidney proximal tubular cells: dependent on phosphatidylinositol 3-kinase activity, Journal of Biological Chemistry, vol. 279, no. 48, pp , [50] M. Kitazawa, Y. Shibata, S. Hashimoto, Y. Ohizumi, and T. Yamakuni, Proinsulin C-peptide stimulates a PKC/IκB/NFκB signaling pathway to activate COX-2 gene transcription in Swiss 3T3 fibroblasts, Journal of Biochemistry, vol. 139, no. 6, pp , [51] Y. Maezawa, K. Yokote, K. Sonezaki, et al., Influence of C-peptide on early glomerular changes in diabetic mice, Diabetes/Metabolism Research and Reviews, vol. 22, no. 4, pp , [52] M. Tsimaratos, T. C. Coste, A. Djemli-Shipkolye, P. Vague, G. Pieroni, and D. Raccah, γ-linolenic acid restores renal medullary thick ascending limb Na +,K + -ATPase activity in diabetic rats, Journal of Nutrition, vol. 131, no. 12, pp , [53] W. Wang, F. Liu, and N. Chen, Peroxisome proliferatoractivated receptor-γ (PPAR-γ) agonists attenuate the profibrotic response induced by TGF-β1 in renal interstitial fibroblasts, Mediators of Inflammation, vol. 2007, Article ID 62641, 7 pages, [54] M. G. Vish, P. Mangeshkar, G. Piraino, et al., Proinsulin C- peptide exerts beneficial effects in endotoxic shock in mice, Critical Care Medicine, vol. 35, no. 5, pp , 2007.
Erythrocyte Na/K ATPase activity and diabetes: relationship with C-peptide level
 Diabetologia (1998) 41: 18±184 Ó Springer-Verlag 1998 Erythrocyte Na/K ATPase activity and diabetes: relationship with C-peptide level D. Dufayet De La Tour, D. Raccah, M. F. Jannot, T. Coste, C. Rougerie,
Diabetologia (1998) 41: 18±184 Ó Springer-Verlag 1998 Erythrocyte Na/K ATPase activity and diabetes: relationship with C-peptide level D. Dufayet De La Tour, D. Raccah, M. F. Jannot, T. Coste, C. Rougerie,
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
C-peptide prevents glomerular hypertrophy and mesangial matrix expansion in diabetic rats
 NDT Advance Access published January 21, 25 Nephrol Dial Transplant (25) 1 of 7 doi:1.193/ndt/gfh683 Original Article C-peptide prevents glomerular hypertrophy and mesangial matrix expansion in diabetic
NDT Advance Access published January 21, 25 Nephrol Dial Transplant (25) 1 of 7 doi:1.193/ndt/gfh683 Original Article C-peptide prevents glomerular hypertrophy and mesangial matrix expansion in diabetic
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Proinsulin C-peptide- A Consensus Statement
 Int. Jnl. Experimental Diab. Res., Vol. 2, pp. 145-151 Reprints available directly from the publisher Photocopying permitted by license only (C) 2001 OPA (Overseas Publishers Association) N.V. Published
Int. Jnl. Experimental Diab. Res., Vol. 2, pp. 145-151 Reprints available directly from the publisher Photocopying permitted by license only (C) 2001 OPA (Overseas Publishers Association) N.V. Published
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
renoprotection therapy goals 208, 209
 Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Subject Index Aldosterone, plasminogen activator inhibitor-1 induction 163, 164, 168 Aminopeptidases angiotensin II processing 64 66, 214 diabetic expression 214, 215 Angiotensin I intrarenal compartmentalization
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
CIE Biology A-level Topic 14: Homeostasis
 CIE Biology A-level Topic 14: Homeostasis Notes Communication is essential for the survival of organism as all living organisms must be able to detect and respond to changes in both their internal and
CIE Biology A-level Topic 14: Homeostasis Notes Communication is essential for the survival of organism as all living organisms must be able to detect and respond to changes in both their internal and
Review Article Effect of C-Peptide on Diabetic Neuropathy in Patients with Type 1 Diabetes
 Hindawi Publishing Corporation Experimental Diabetes Research Volume 2008, Article ID 457912, 5 pages doi:10.1155/2008/457912 Review Article Effect of C-Peptide on Diabetic Neuropathy in Patients with
Hindawi Publishing Corporation Experimental Diabetes Research Volume 2008, Article ID 457912, 5 pages doi:10.1155/2008/457912 Review Article Effect of C-Peptide on Diabetic Neuropathy in Patients with
STEIN IN-TERM EXAM -- BIOLOGY APRIL 18, PAGE
 STEIN IN-TERM EXAM -- BIOLOGY 3058 -- APRIL 18, 2019 -- PAGE 1 of 9 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There is
STEIN IN-TERM EXAM -- BIOLOGY 3058 -- APRIL 18, 2019 -- PAGE 1 of 9 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There is
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
invited review Role of C-peptide in human physiology
 Am J Physiol Endocrinol Metab 278: E759 E768, 2000. Role of C-peptide in human physiology invited review JOHN WAHREN, 1 KARIN EKBERG, 1 JAN JOHANSSON, 2 MIKAEL HENRIKSSON, 2 ALADDIN PRAMANIK, 2 BO-LENNART
Am J Physiol Endocrinol Metab 278: E759 E768, 2000. Role of C-peptide in human physiology invited review JOHN WAHREN, 1 KARIN EKBERG, 1 JAN JOHANSSON, 2 MIKAEL HENRIKSSON, 2 ALADDIN PRAMANIK, 2 BO-LENNART
Index. A Acetylcholine, 47 Adenosine triphosphate (ATP) release, from RBCs, 18 20, 23 Advanced glycation end products (AGEs), proatherogenic
 A Acetylcholine, 47 Adenosine triphosphate (ATP) release, from RBCs, 18 20, 23 Advanced glycation end products (AGEs), proatherogenic effects, 153 Afferent and efferent arteriolar tone, 69 70 Alzheimer
A Acetylcholine, 47 Adenosine triphosphate (ATP) release, from RBCs, 18 20, 23 Advanced glycation end products (AGEs), proatherogenic effects, 153 Afferent and efferent arteriolar tone, 69 70 Alzheimer
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Diabetic neuropathy is defined by the presence of
 Amelioration of Sensory Nerve Dysfunction by C-Peptide in Patients With Type 1 Diabetes Karin Ekberg, 1 Tom Brismar, 2 Bo-Lennart Johansson, 1 Björn Jonsson, 1 Per Lindström, 3 and John Wahren 1 Studies
Amelioration of Sensory Nerve Dysfunction by C-Peptide in Patients With Type 1 Diabetes Karin Ekberg, 1 Tom Brismar, 2 Bo-Lennart Johansson, 1 Björn Jonsson, 1 Per Lindström, 3 and John Wahren 1 Studies
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
5. Maintaining the internal environment. Homeostasis
 5. Maintaining the internal environment Homeostasis Blood and tissue fluid derived from blood, flow around or close to all cells in the body. Blood and tissue fluid form the internal environment of the
5. Maintaining the internal environment Homeostasis Blood and tissue fluid derived from blood, flow around or close to all cells in the body. Blood and tissue fluid form the internal environment of the
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
ARGININE VASOPRESSIN (AVP)
 ARGININE VASOPRESSIN (AVP) AFFECTS BLOOD PRESSURE AND RENAL WATER REABSORPTION WHAT ELSE DOES IT DO? Michael F. Michelis, M.D., F.A.C.P., F.A.S.N. Director, Division of Nephrology Lenox Hill Hospital,
ARGININE VASOPRESSIN (AVP) AFFECTS BLOOD PRESSURE AND RENAL WATER REABSORPTION WHAT ELSE DOES IT DO? Michael F. Michelis, M.D., F.A.C.P., F.A.S.N. Director, Division of Nephrology Lenox Hill Hospital,
STEIN IN-TERM EXAM -- BIOLOGY APRIL 19, PAGE
 STEIN IN-TERM EXAM -- BIOLOGY 3058 -- APRIL 19, 2018 -- PAGE 1 of 9 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There is
STEIN IN-TERM EXAM -- BIOLOGY 3058 -- APRIL 19, 2018 -- PAGE 1 of 9 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There is
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
via efferent arteriole dilation and inhibition of tubular sodium reabsorption.
 Am J Physiol Renal Physiol 297: F1265 F1272, 2009. First published September 9, 2009; doi:10.1152/ajprenal.00228.2009. Proinsulin C-peptide reduces diabetes-induced glomerular hyperfiltration via efferent
Am J Physiol Renal Physiol 297: F1265 F1272, 2009. First published September 9, 2009; doi:10.1152/ajprenal.00228.2009. Proinsulin C-peptide reduces diabetes-induced glomerular hyperfiltration via efferent
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Lecture 19 Summary Gestational Diabetes and Complications of Diabetes. Gestational diabetes;
 Lecture 19 Summary Gestational Diabetes and Complications of Diabetes Gestational diabetes; - Type of diabetes that only develops during pregnancy Usually diagnosed in late pregnancy Causes high blood
Lecture 19 Summary Gestational Diabetes and Complications of Diabetes Gestational diabetes; - Type of diabetes that only develops during pregnancy Usually diagnosed in late pregnancy Causes high blood
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
Homeostatic Regulation
 Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη
 Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη Κωνσταντίνος Τζιόμαλος Επίκουρος Καθηγητής Παθολογίας Α Προπαιδευτική Παθολογική Κλινική, Νοσοκομείο
Ο ρόλος των τριγλυκεριδίων στην παθογένεια των μικροαγγειοπαθητικών επιπλοκών του σακχαρώδη διαβήτη Κωνσταντίνος Τζιόμαλος Επίκουρος Καθηγητής Παθολογίας Α Προπαιδευτική Παθολογική Κλινική, Νοσοκομείο
Urinary System. BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College
 Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary System BSC 2086 A & P 2 Professor Tcherina Duncombe Palm Beach State College Filter plasma, separate and eliminate wastes Functions Regulate blood volume and pressure Regulate osmolarity of body
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
STEIN IN-TERM EXAM -- BIOLOGY FEBRUARY 15, PAGE
 STEIN IN-TERM EXAM -- BIOLOGY 3058 -- FEBRUARY 15, 2018 -- PAGE 1 of 8 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There
STEIN IN-TERM EXAM -- BIOLOGY 3058 -- FEBRUARY 15, 2018 -- PAGE 1 of 8 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There
Basic mechanisms of Kidney function
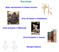 Excretion Basic mechanisms of Kidney function Urine formation in Amphibians Urine formation in Mammals Urine formation in Insects Nitrogen balance Kidneys The most fundamental function of kidneys) is to
Excretion Basic mechanisms of Kidney function Urine formation in Amphibians Urine formation in Mammals Urine formation in Insects Nitrogen balance Kidneys The most fundamental function of kidneys) is to
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
The functional unit of the kidney, the single nephron, shows
 Tubuloglomerular Feedback and the Control of Glomerular Filtration Rate Volker Vallon Institute of Pharmacology and Toxicology, University of Tübingen, D-72074 Tübingen, Germany In every nephron the glomerular
Tubuloglomerular Feedback and the Control of Glomerular Filtration Rate Volker Vallon Institute of Pharmacology and Toxicology, University of Tübingen, D-72074 Tübingen, Germany In every nephron the glomerular
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Renal Regulation of Sodium and Volume. Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM
 Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal Regulation of Sodium and Volume Dr. Dave Johnson Associate Professor Dept. Physiology UNECOM Maintaining Volume Plasma water and sodium (Na + ) are regulated independently - you are already familiar
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Principles of Renal Physiology. 4th Edition
 Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
Principles of Renal Physiology 4th Edition Principles of Renal Physiology 4th Edition Chris Lote Professor of Experimental Nephrology, University of Birmingham, UK SPRINGER SCIENCE+BUSINESS MEDIA, B.V.
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Lithium-induced Tubular Dysfunction. Jun Ki Park 11/30/10
 Lithium-induced Tubular Dysfunction Jun Ki Park 11/30/10 Use of Lithium Mid 19 th century: treatment of gout Late 19 th century: used for psychiatric disorders Early 20 th century: sodium substitute to
Lithium-induced Tubular Dysfunction Jun Ki Park 11/30/10 Use of Lithium Mid 19 th century: treatment of gout Late 19 th century: used for psychiatric disorders Early 20 th century: sodium substitute to
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Managing patients with renal disease
 Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
Managing patients with renal disease Hiddo Lambers Heerspink, MD University Medical Centre Groningen, The Netherlands Asian Cardio Diabetes Forum April 23 24, 216 Kuala Lumpur, Malaysia Prevalent cases,
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Physiology of Excretory Systems
 Physiology of Excretory Systems Fig 12-2 (a) Urea is formed by the ornithine-urea cycle in most vertebrates. Because ATP is required for the first step, nitrogen excretion in ureotelic animals is more
Physiology of Excretory Systems Fig 12-2 (a) Urea is formed by the ornithine-urea cycle in most vertebrates. Because ATP is required for the first step, nitrogen excretion in ureotelic animals is more
Anatomy/Physiology Study Guide: Unit 9 Excretory System
 Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
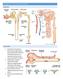 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance
 Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
Salt Sensitivity: Mechanisms, Diagnosis, and Clinical Relevance Matthew R. Weir, MD Professor and Director Division of Nephrology University of Maryland School of Medicine Overview Introduction Mechanisms
General introduction of nephrology. Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University
 General introduction of nephrology Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University Terminology Kidney,renal Nephrology Scope of nephrology Kidney diseases and
General introduction of nephrology Xiaoqiang Ding M.D., Ph.D. Department of nephrology Zhongshan Hospital, Fudan University Terminology Kidney,renal Nephrology Scope of nephrology Kidney diseases and
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
9.3 Stress Response and Blood Sugar
 9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
WJEC. BY4 Kidney Questions
 NAME: OPTION GROUP WJEC BY4 Kidney Questions Question Book 2 (Legacy Qs from Jan 2000 to June 2014) Question Number(s) Due Date & Pass Mark Homework Mark Resist Question number(s) Resist Due Date & Pass
NAME: OPTION GROUP WJEC BY4 Kidney Questions Question Book 2 (Legacy Qs from Jan 2000 to June 2014) Question Number(s) Due Date & Pass Mark Homework Mark Resist Question number(s) Resist Due Date & Pass
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1
 GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Cellular Physiology (PHSI3009) Contents:
 Cellular Physiology (PHSI3009) Contents: Cell membranes and communication 2 nd messenger systems G-coupled protein signalling Calcium signalling Small G-protein signalling o RAS o MAPK o PI3K RHO GTPases
Cellular Physiology (PHSI3009) Contents: Cell membranes and communication 2 nd messenger systems G-coupled protein signalling Calcium signalling Small G-protein signalling o RAS o MAPK o PI3K RHO GTPases
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Renal Physiology - Lectures
 Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
STEIN IN-TERM EXAM -- BIOLOGY FEBRUARY 16, PAGE
 STEIN IN-TERM EXAM -- BIOLOGY 3058 -- FEBRUARY 16, 2017 -- PAGE 1 of 9 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There
STEIN IN-TERM EXAM -- BIOLOGY 3058 -- FEBRUARY 16, 2017 -- PAGE 1 of 9 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
STEIN IN-TERM EXAM -- BIOLOGY FEBRUARY 18, PAGE
 STEIN IN-TERM EXAM -- BIOLOGY 3058 -- FEBRUARY 18, 2016 -- PAGE 1 of 8 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There
STEIN IN-TERM EXAM -- BIOLOGY 3058 -- FEBRUARY 18, 2016 -- PAGE 1 of 8 There are 25 questions in this Biology 3058 exam. All questions are "A, B, C, D, E, F, G, H" questions worth one point each. There
The ability of the kidneys to regulate extracellular fluid volume by altering sodium
 REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
REGULATION OF EXTRACELLULAR FLUID VOLUME BY INTEGRATED CONTROL OF SODIUM EXCRETION Joey P. Granger Department of Physiology and Biophysics, University of Mississippi Medical Center, Jackson, Mississippi
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
mid ihsan (Physiology ) GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B **
 (Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
(Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
1. Anatomy / Vascularisation. 2. Urine concentration. 3. Axial heterogeneity of some segments
 Lise BANKIR 1. Anatomy / Vascularisation 2. Urine concentration 3. Axial heterogeneity of some segments Rat kidney. Arterial filling with Microfil silicone rubber Alcian Blue staining Filling of arterial
Lise BANKIR 1. Anatomy / Vascularisation 2. Urine concentration 3. Axial heterogeneity of some segments Rat kidney. Arterial filling with Microfil silicone rubber Alcian Blue staining Filling of arterial
