Ren e a n l a l f un u c n t c io i n o s n Biochemistry II Lecture (J.S.) 1
|
|
|
- Basil McCoy
- 5 years ago
- Views:
Transcription
1 Renal functions Biochemistry II Lecture (J.S.) 1
2 The main functions of the kidneys Maintaining of the composition, osmolality, and volume of ECF Excretion of nitrogenous catabolites (urea, uric acid, creatinine and various hydrophilic drugs or toxins into the urine. Control of acid-base balance. An endocrine function (erythropoietin, renin, urodilatin, calcitriol). The excretory function of the kidneys includes filtration of the plasma in the glomeruli glomerular filtration, transport of water and solutes from the tubular lumen into the blood tubular resorption, and transport of substances from tubular cells to the lumen tubular secretion, The blood flow through the kidney is about l / min. 2
3 The urine Urinary excretion of selected compounds depends on the dietary intake. Approximate ranges of amounts excreted daily in adults: Inorganic ions mmol / d g / d Na K Ca Mg Cl Phosphates (P) SO (S) Nitrogenous compounds 24 h-urine: % of total nitrogen NH ~ 5 Urea ~ 84 Creatinine ~ 4 Uric acid ~ 4 Amino acids ~ 1 Other < 1 3
4 The osmolality is mostly much higher than that of blood plasma, it varies from about 80 to 1200 mmol / kg H 2 O. The osmolality of the glomerular filtrate is about 300 mmol / kg H 2 O, therefore the maximal increase in urine osmolality is approximately fourfold. There are substantial differences in the increases of particular solute concentrations. Approximate values of urine / plasma concentration ratio Na K + 10 Ca Cl 1.2 Phosphate 15 NH Urea 100 Creatinine 100 Uric acid 10 4
5 Amounts of solutes excreted into the urine during a given period The amount of a solute excreted into the urine depends on the amount that has been filtered in the glomeruli n filtered / t = c plasma V GF / t = c plasma GFR (GFR is glomerular filtration rate, l / d or ml / s) the amount reabsorbed in the tubules n abs / t, and the amount secreted from the tubular cells n secr / t. The total amount excreted during a given period equals c urine V urine / t = c plasma V GF / t + (n secr n abs ) / t From the equation can be calculated the fraction of the amount excreted into the urine from the amount that has appeared in the glomerular filtrate within a given period the fractional excretion E/F. 5
6 The clearance of substances from plasma The quantity renal clearance is commonly used to express the efficiency of the elimination of a particular solute from blood plasma into the urine, Renal clearance, simply clearance of a solute X (C x ) is the ratio of the amount of a solute X that is excreted in a unit of time into the urine (c urine V urine / t ) to its concentration in blood plasma c plasma : C x = c urine V urine t 1 / c plasma (in ml / s or l / d) x urine urine plasma Thus the clearance of a solute X may be understood as the volume of plasma that is completely cleared of that substance in a unit of time. Clearance is a very informative quantity. For example, the clearance of the compound that is completely filtered and neither reabsorbed nor secreted in the renal tubules (as inulin or, with certain limitations, endogenous creatinine) is equal to the glomerular filtration rate GFR, the volume of filtrate formed in a unit of time. 6
7 Another example: p-aminohippuric acid is an aromatic acid that is both filtered in the glomeruli and secreted by the cells of proximal renal tubules, so that the blood plasma is completely cleared of it during the sole passage through the renal vessels. If p-aminohippurate (PAH) is applied intravenously till the steady concentration is reached, concentrations of the compound can be measured in plasma and urine and the clearance C PAH calculated. Its value corresponds to the renal plasma flow in a time unit. The renal plasma flow is 8 13 ml / s ( ml / min). NH 2 CO NH CH 2 COOH p-aminohippuric acid (PAH, p-aminobenzoylglycine) 7
8 The nephron FILTRATION Obligatory isoosmotic REABSORPTION Tubular SECRETION Controlled REABSORPTION Isotonic cortex Hyperosmolal renal medulla Countercurrent mechanism of the loop of Henle and vasa recta forms a high osmolality environment in the medulla Mostly hypertonic URINE 8
9 Glomerular filtration In renal glomeruli, the blood plasma is filtered. The composition of ions and small molecules in glomerular filtrate is quite similar to that of plasma. A common statement that glomerular filtrate is a protein-free fluid is not right. Low concentrations of proteins are present (predominantly of those with M r < ), about mg per litre of filtrate, but most of proteins are reabsorbed in the tubules. The glomerular filtration barrier capillary lumen (plasma) Bowman s space (tubular fluid) fenestrated endothelial layer (about 30 % of the basement membrane not covered by the endothelial cells) the thick basement membrane ~ 300 nm the slit membrane (pore size ~ 5 nm) the processes of podocytes (visceral epithelium) and filtration slits 9
10 The basement membrane consists of type IV collagen fibres and certain amount of laminin and proteoglycans. Heparan sulfate in the membrane and sialic acid containing glycoproteins in the filtration slits have negative electrical charges. Podocytes with their interdigitating foot processes separated by filtration slits cover the basement membranes of capillary walls (scanning electron micrograph). Plasma proteins with a M r above approx are excluded by filtration. Proteins with a M r above and anionic character (albumin and transferrin) are prevented from entering the urine by an electrostatic filter, concentration of albumin in the filtrate is about 4 mg/l (0.01 % plasma concn.). Low-molecular plasma proteins (M r ) cross the filtration barrier, their concentration in glomerular filtrate can reach % concentration in plasma. 10
11 Healthy adults excrete less than 150 mg of total urinary protein per 24 h: albumin 7 11 mg / d (less than 20 mg / d), transferrin < 1 mg / d, α 1 -acid glycoprotein < 10 mg / d, α 1 -microglobulin 1 5 mg / d, retinol-binding protein < 0.5 mg / d, β 2 -microglobulin < 0.3 mg / d, etc. Proteinuria more than 300 mg of total urinary protein per 24 h. Glomerular proteinuria the normal glomerular barrier to plasma proteins is disrupted, proteins with molecular mass higher than are present in the urine (albumin , transferrin , immunoglobulins > ). Low-molecular proteins are reabsorbed in the tubules. Tubular proteinuria the cause is in incomplete proximal tubular reabsorption (in the presence of normal glomerular permeability), normally filtered low-molecular-mass plasma proteins appear in the urine in increased amounts. Tubular proteinuria can occur alone or in association with glomerular proteinuria. 11
12 Test for microalbuminuria (Micral-test ) Microalbuminuria is excretion of albumin in the range from 30 mg / d to mg /d (to obvious proteinuria). It often predicts development of nephropathy. It is important to detect microalbuminuria early, because kidney damages are minimal and are still reversible. Measurements of urinary albumin is especially important for diabetic and hypertensive patients. 12
13 Glomerular filtration rate (GFR) is the volume of glomerular filtrate formed in a unit of time. Normal range ml / s i.e ml / min ( l / d ) The ideal marker for GFR would appear endogenously in the plasma at a constant concentration, would be freely filtered at the glomerulus, would be neither reabsorbed nor secreted by the renal tubule, and would undergo no extrarenal elimination from the body. Clearance of inulin or with certain limitations also clearance of endogenous creatinine are equal to GFR. Clearance of inulin is a very exact measure of GFR, suitable more for scientific research than for routine use. Inulin is a plant (or synthetic) polyfructosan. It must be infused intravenously, about 50 mg/kg body weight. The samples of blood as well as urine cannot be taken before a steady concentration of inulin in plasma is reached. 13
14 Creatinine clearance (C creat ) serves as an routine estimate of GFR for more than 60 years, because it is a very simple test.. Creatinine is excreted predominantly through glomerular filtration. There is no tubular reabsorption, but (namely at higher plasma concentrations) the amount of creatinine secreted in the tubules increases. Clearance of creatinine depends on age and gender, timed samples of urine must be collected, and the analytical method is not quite specific. Creatinine clearances have slightly higher values when compared with inulin clearances (about 2.33 and 2.00, resp.). Calculation: Entries - c plasma (creatinine) in mmol/l (normal value about 115 µmol/l) c urine (creatinine) in mmol/l V urine / t in ml / s C creat = uncorrected GFR = c urine V urine t 1 / c plasma (ml/s) Glomerular filtration rate corrected to the standard body surface area 1.73 m 2 : GFR corr = GFR A / 1.73 (ml/s) Body surface A = h w (in m 2 ) 14
15 Estimate of GFR from cystatin C concentration in serum Cystatin C is a low-molecular protein (M r ) that acts as an inhibitor of cysteine proteinases and is released uniformly from all nuclear cells into the circulating blood. Its concentration is stable (e.g., it doesn't depend on inflammatory processes). Like other low-molecular weight proteins, cystatin C is eliminated from the plasma exclusively by glomerular filtration and decomposed in tubular cells. Cystatin C concentration in serum is indirectly related to GFR. The interindividual variability in cystatin C concentration is lower than that of creatinine, what enables the early detection of decrease in GFR. Concentration of cystatin C in serum or plasma is determined by means of an immunoturbidimetric method or ELISA. There is no need to collect urine. The estimate of GRF corrected to the standard body surface area is calculated in adults as GFR cystatin (ml / s) = 1.41 ρ (cystatin C, mg/l) 1.68, in adolescents under the age of 14 multiplied by the "praepubertal" factor Estimates of GFR corr from the clearance of creatinine are progressively substituted by GFR cystatin. 15
16 Glomerular filtration - laboratory investigations Serum creatinine concentration ~ 100 µmol/l ( µmol/l) Rough estimates of GFR from the creatinine concentration were derived in the past (e.g. the Cockcroft-Gault formula). Glomerular filtration rate ml/s estimated either from serum cystatin C concentration or as creatinine clearance corrected to body surface area 1.73 m 2. Serum urea concentration mmol/l High serum urea in any cause of impaired renal perfusion, reduced GFR, or obstruction to urine outflow. Detection of proteinuria / microalbuminuria Quantification of urinary protein excretion (albumin < 20 mg/d, total protein < 150 mg/d) Serum albumin concentration, determination of proteinuria type 16
17 The functions of renal tubules The proximal tubule Efficient reabsorption of most amino acids, nearly all glucose, unless its supply is greater than the capacity of the transfer into the cells - a threshold approximately at 10 mmol/l, most Na + (50 60 %), K +, Cl, phosphates, HCO 3, etc., driven by Na +,K + -ATPase located within the basolateral membranes. Passive reabsorption of water (70 80 %, isotonic and "obligatory", independent on ADH). Tubular secretion of organic ions, basic drugs. 17
18 Proximal tubule Tubular lumen Apical plasma membrane tight junctions Na + glucose Na + amino acids Na + Reabsorption of % water % Na + phosphate ATP Basolateral membrane K + Na + Blood plasma H 2 O solvent drag Na +, Cl GLUT2 Reabsorption of (not shown here) > 90 % K +, 85 % Cl, 90 % HCO 3, % phosphates, 65 % Ca 2+, urate, small proteins, etc. H 2 O aquaporin 1 Na + /Ca 2+ H + aquaporin 3 Tubular secretion anions of weak acids cations of organic bases amphions (e.g. EDTA) H 2 O 18
19 The loop of Henle and vasa recta form the osmotic gradient between the renal cortex and medulla. High osmolality of the medullary peritubular interstitial fluid is essential for the efficient reabsorption of water in the collecting ducts, for concentration of urine. The osmolality increases from the cortex to the medulla, and it is maintained by the countercurrent mechanism that consists of - countercurrent multiplication of the loop of Henle, and - passive countercurrent exchange of water and urea between vasa recta, the descending loop of Henle, and collecting ducts. In the thick ascending limb, which is impermeable for water, Na +,K + -ATPase drives the active ion transport out from tubules (increase in osmolality of interstitial fluid).. In the thin descending limb, water moves freely from the tubules into the hyperosmolal interstitial fluid. The medullary parts of collecting ducts are permeable for water (controlled by ADH) and urea, so that water may be efficiently reabsorbed (similarly to the thin descending limb of the loop) into the hyperosmolal interstitial fluid and drained to the cortex by vasa recta. There is also a high concentration of urea in the collecting ducts, urea freely diffuses into the interstitial fluid, into the thick ascending parts of the loop of Henle and vasa recta (urea recycling). 19
20 The thin descending limb of the loop There are numerous aquaporins in the plasma membrane (AQP 1 in the apicai part) that make the membranes freely permeable to water, which moves out of the lumen into the hyperosmolal surrounding tissue; ion transporters are absent. The thick ascending limb of the loop Apical membrane of the thick ascendent limb of the loop is impermeable for water. Na + K + Na + Na + -K + -2Cl efficient symport Na +, K +, and Cl are pumped out against the concentration gradient into the hyperosmolal interstitial fluid (the process is driven by Na +,K + -ATPase. K + ATP recirculation of K+ Cl Cl K + Cl Cl 20
21 Osmolality of the tubular and peritubular interstitial fluid renal cortex renal medulla urea recirculation of Na +, Cl, and urea 21
22 Distal tubules and collecting ducts Passive reabsorption of water into the hyperosmolal interstitium (controlled by antidiuretic hormone) the final concentration of urine. Resorption of Na + (driven by Na +,K + -ATPase) and + + tubular secretion of K + (most of K + excreted into the urine) both under the control of aldosterone or natriuretic peptides Excretion of Ca 2+ and phosphates under the control of parathyrin and calcitonin. A part of tubular secretion of H + in the form of H 2 PO 4 and NH 4+ depends on the acid-base status. 22
23 Distal tubule reabsorption driven by Na +,K + -ATPase Symport Na + Cl (no K + transport) Na + Cl K + recirculation of K + leakage of K + only at very high intracellular [K + ] The cells of distal tubules represent the sites of Ca 2+ reabsorption (about 10 % of total reabsorbed) and phosphate leakage controlled by parathyrin and to a less extent by calcitonin. 23
24 Collecting ducts The principal tubular cells Tubular lumen Aldosterone In spite of reabsorption of only about 3 % of total filtered Na + ions Na + Na + in the collecting ducts, changes in that relatively small percentage are decisive in natriuresis, elimination K + K + of Na + from the body. Both Na + and K + channels are inhibited by "potassium saving" diuretics amilorid and spironolacton. ATP aquaporin 3 H 2 O 0 aquaporin 2 Aldosterone enlarges reabsorption of Na + equally with losses of K + by exposition of Na + and K + channels and also by partial stimulation of Na +,K + -ATPase. Antidiuretic hormone (ADH, Arg-vasopressin) increases reabsorption of water. It binds onto membrane V 2 receptors and activation of proteinkinases A is a cause of exposition of aquaporin AQP-2 in the apical membrane. Blood plasma 3 Na + 2 K + H 2 O receptors V 2 for ADH Natriuretic peptides inhibit Na + and K + channels (in addition to the vasodilating effect) so that they support Na + excretion and retention of K +. The intercalated cells have their major role in excretion of H + and reabsorption of HCO 3. 24
25 Natriuresis - the renal excretion of sodium ions Diuretics are drugs that support elimination of water from the body by stimulating natriuresis through different mechanisms. Most diuretics influence the cells from the tubular fluid (the apical part of plasma membranes). proximal tubules % reabsorbed distal tubules 5 8 % of total reabsorbed Na + inhibition by thiazide diuretics (partly by "loop" diuretics, too) thick ascending limb % of total reabsorbed Na + inhibition by "loop" diuretics (e.g. furosemide) collecting ducts 2 3 % of total reabsorbed Na + (regulated by aldosterone) inhibition by potassium- saving diuretics (e.g. amiloride, spironolactone) 25
26 Tubular functions - laboratory investigation Capacity of the kidneys top concentrate the urine (formerly tested by thirsting healthy subjects up to osmolality mmol/kg H2O or density g/l) Osmolar clearance C osm should not exceed 0.05 ml/s to prevent solute losses Fractional excretion of solutes E/F osm normal values ( 3.5 %) Clearance of electrolyte-free water (EWC) C EW negative values amount of water which has to be added to the urine to become isotonic with the plasma positive values amount of water which has to be relieved from the urine to become isotonic with the plasma the usual range ± ml/s (positive values only temporarily in healthy persons after high water intake) Urinary Na + output must be proportional to the intake, about mmol/d. Fractional excretion of Na + E/F Na+ normal range ( %) Fractional excretion of K + E/F K+ normal range (4 19 %) 26
27 The endocrine function of the kidney Erythropoietin (EPO) is the primary regulatory factor of erythropoiesis (formation of red blood cells in the bone marrow). EPO is a glycoprotein (165 AA, M r ~ ), released in the kidney (about 10 % also in the liver) by splitting of the precursor protein by the action of a specific proteinase. Hypoxia and decrease in blood haemoglobin stimulate the release of EPO from the kidneys. Calcitriol (1α,25-dihydroxycalciol) originates from circulating calcidiol (25-hydroxycalciol) by hydroxylation in the renal tubular cells. The specific hydroxylating system is stimulated by parathyrine. Urodilatin is the natriuretic peptide synthesized in the kidney (4 amino acid residues more than ANP, M r ~ 3 500) being more paracrine, it is secreted into the urine. Urodilatin regulates water and sodium reabsorption in the collecting duct by inhibition of Na + channels and vasodilation. Renin is a proteinase secreted from the juxtaglomerular cells that starts the renin-angiotensin system RAS:./. 27
28 The juxtaglomerular apparatus and the renin-angiotensin system afferent arteriole and the juxtaglomerular cells distal tubule and cells of the macula densa The juxtaglomerular apparatus responds to decreased renal perfusion pressure by secreting a proteinase, renin, that uses angiotensinogen (one of the plasma glycoproteins in the α 2 -globulin fraction) as its substrate and liberates angiotensin I (a decapeptide) from angiotensinogen. Angiotensin I is transformed into a octapeptide angiotensin II (by angiotensin-converting enzyme, ACE) that stimulates the synthesis and release of a mineralocorticoid aldosterone. The macula densa also senses the tubular chloride concentration. 28
29 Control of acid-base balance by the kidneys In healthy persons, mmol H + / d (from non-volatile acids) have to be excreted. Although the urine is more acidic than blood plasma, excretion of free H + ions in this way (actual acidity) may be neglected: Only 0.01 mmol H + is excreted in one litre urine ph 5.0. Tubular cells excrete H + ions in the form of H 2 PO 4 ions (H + bound onto HPO 2 4 ), the urine so becomes slightly acidic - this titratable acidity represents approximately mmol H + / d eliminated from the body. Tubular cells excrete NH 4 + ions formed from NH 3 by binding H + ; NH 3 is released from glutamine (and glutamate). About mmol H + / d are excreted in this way. Reabsorption of HCO 3 ions from tubular fluid saves the main plasma buffer base. In alkalosis, HCO 3 ions are secreted into the urine. 29
30 Reabsorption of HCO 3 90 % HCO 3 reabsorbed in the proximal tubule (pars recta), 10 % in the collecting ducts (by intercalated cells) Reabsorption is regulated by pco 2. H + ions transported into the tubular fluid are not excreted into the urine, they give water. HCO 3 ions are secreted in alkalosis: When [HCO 3 ] in blood exceeds 28 mmol/l, Na + /H + antiport is diminished and Cl /HCO 3 antiporters are inserted into the apical membrane of separate base-secreting tubular cells by a triggered exocytosis. A steady state with a maximal HCO 3 excretion is reached in the course of several days. 30
31 Excretion of H + in the form of H 2 PO 4 Cells of straight part of proximal tubules and intercalating cells of collecting ducts H + ions bound onto hydrogen phosphate changes the ratio [HPO 4 2 ] / [H 2 PO 4 ], so that they result in only a slight decrease in ph value. The amount of H+ excreted in this way can be measured as "titratable" acidity of the urine. Tubular lumen Na + K + ATP Na + ATP H + HPO 2 4 H + proton-producing reactions H 2 CO 3 and/or increased pco 2 HCO 3 Cl H 2 PO 4 exposition of the vesicular H + -ATPase Under physiological conditions, mmol H + /d are excreted in this way. The increase of that amount is limited by the accessibility of HPO 2 4 in the tubular fluid to a maximum of about mmol/d, i.e. to the urinary ph 4.5). 31
32 The excretion of H + in the form of NH 4 + Proximal tubules, distal tubules, and intercalated cells of collecting ducts without any decrease in ph value of the urine. Tubular lumen K + NH 4 + Na + Na + instead of H + NH + 4 instead of K + in K + channel ATP glutamine glutamate oxoglutarate Na + production of glutamine in the liver preferred in acidosis transfer of NH + 4 into the blood in alkalosis (NH 4+ is the substrate for ureosynthesis that is a proton-producing process) Under physiological conditions, mmol H + /d are excreted in this way. In an extreme acidosis, the excretion of NH 4+ may reach (stepwise during 5 days) mmol/d; NH 4+ can accumulate in the renal medullary interstitium. 32
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Chapter 19 The Urinary System Fluid and Electrolyte Balance
 Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
Chapter 19 The Urinary System Fluid and Electrolyte Balance Chapter Outline The Concept of Balance Water Balance Sodium Balance Potassium Balance Calcium Balance Interactions between Fluid and Electrolyte
RENAL PHYSIOLOGY. Physiology Unit 4
 RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
RENAL PHYSIOLOGY Physiology Unit 4 Renal Functions Primary Function is to regulate the chemistry of plasma through urine formation Additional Functions Regulate concentration of waste products Regulate
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
osmoregulation mechanisms in gills, salt glands, and kidneys
 Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
Ionic & Osmotic Homeostasis osmoregulation mechanisms in gills, salt glands, and kidneys extracellular intracellular 22 23 Salt Secretion: recycle Figure in Box 26.2 Hill et al. 2004 active Down electrochemical
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Hill et al. 2004, Fig. 27.6
 Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
Lecture 25, 15 November 2005 Osmoregulation (Chapters 25-28) Vertebrate Physiology ECOL 437 (aka MCB 437, VetSci 437) University of Arizona Fall 2005 1. Osmoregulation 2. Kidney Function Text: Chapters
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX
 One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
One Minute Movies: Molecular Action at the Nephron Joy Killough / Westwood High School / Austin,TX To prepare your nephron model: ( A nephron is a tubule and the glomerulus. There are about a million of
11/05/1431. Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate
 Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
Urine Formation by the Kidneys Tubular Processing of the Glomerular Filtrate Chapter 27 pages 327 347 1 OBJECTIVES At the end of this lecture you should be able to describe: Absorptive Characteristics
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1
 BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIPN100 F15 Human Physiology (Kristan) Lecture 18: Endocrine control of renal function. p. 1 Terms you should understand by the end of this section: diuresis, antidiuresis, osmoreceptors, atrial stretch
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19
![QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19](/thumbs/80/80449526.jpg) 1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
1 QUIZ/TEST REVIEW NOTES SECTION 2 RENAL PHYSIOLOGY FILTRATION [THE KIDNEYS/URINARY SYSTEM] CHAPTER 19 Learning Objectives: Differentiate the following processes: filtration, reabsorption, secretion, excretion
Kidney Structure. Renal Lobe = renal pyramid & overlying cortex. Renal Lobule = medullary ray & surrounding cortical labryinth.
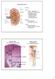 Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Kidney Structure Capsule Hilum ureter renal pelvis major and minor calyxes renal and vein segmental arteries interlobar arteries arcuate arteries interlobular arteries Medulla renal pyramids cortical/renal
Urine Formation. Urinary Physiology Urinary Section pages Urine Formation. Glomerular Filtration 4/24/2016
 Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Urine Formation Urinary Physiology Urinary Section pages 9-17 Filtrate Blood plasma minus most proteins Urine
Renal physiology D.HAMMOUDI.MD
 Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
Renal physiology D.HAMMOUDI.MD Functions Regulating blood ionic composition Regulating blood ph Regulating blood volume Regulating blood pressure Produce calcitrol and erythropoietin Regulating blood glucose
BIOH122 Human Biological Science 2
 BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
BIOH122 Human Biological Science 2 Session 18 Urinary System 3 Tubular Reabsorption and Secretion Bioscience Department Endeavour College of Natural Health endeavour.edu.au Session Plan o Principles of
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
BLOCK REVIEW Renal Physiology. May 9, 2011 Koeppen & Stanton. EXAM May 12, Tubular Epithelium
 BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
BLOCK REVIEW Renal Physiology Lisa M. HarrisonBernard, Ph.D. May 9, 2011 Koeppen & Stanton EXAM May 12, 2011 Tubular Epithelium Reabsorption Secretion 1 1. 20, 40, 60 rule for body fluid volumes 2. ECF
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate
 Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Renal physiology The kidneys Allow us to live on dry land. Body fluid volume is small (~5L (blood + serum)) Composition can change rapidly e.g. due to increase in metabolic rate Kidneys maintain composition
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
RENAL. 6. Renal acid secretion is affected by all of the following except a. pco 2 b. K c. Carbonic anhydrase d. Aldosterone e. Ca
 RENAL 1. The reabsorption of Na in the proximal tubules a. Reabsorbs 80% of the filtered sodium load b. Causes increased hypertonicity c. Is powered by N/H ATPase d. Shares a common carrier with glucose
RENAL 1. The reabsorption of Na in the proximal tubules a. Reabsorbs 80% of the filtered sodium load b. Causes increased hypertonicity c. Is powered by N/H ATPase d. Shares a common carrier with glucose
URINARY SYSTEM. Primary functions. Major organs & structures
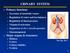 URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
URINARY SYSTEM Primary functions Excretion of metabolic wastes Regulation of water and ion balances Regulation of blood pressure Vitamin D activation Regulation of rbc s (erythropoietin) Gluconeogenesis
Renal Physiology Part II. Bio 219 Napa Valley College Dr. Adam Ross
 Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
Renal Physiology Part II Bio 219 Napa Valley College Dr. Adam Ross Fluid and Electrolyte balance As we know from our previous studies: Water and ions need to be balanced in order to maintain proper homeostatic
NORMAL POTASSIUM DISTRIBUTION AND BALANCE
 NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
Renal physiology II. Basic renal processes. Dr Alida Koorts BMS
 Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Renal physiology II Basic renal processes Dr Alida Koorts BMS 7-12 012 319 2921 akoorts@medic.up.ac.za Basic renal processes 1. filtration 2. reabsorption 3. secretion Glomerular filtration The filtration
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Renal Physiology - Lectures
 Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Renal Physiology - Lectures Physiology of Body Fluids PROBLEM SET, RESEARCH ARTICLE Structure & Function of the Kidneys Renal Clearance & Glomerular Filtration PROBLEM SET Regulation of Renal Blood Flow
Urinary System. Dr. ZHANG Xiong. Dept. of Physiology. ZJU School of Medicine. QUESTION 6
 Urinary System Dr. ZHANG Xiong Dept. of Physiology ZJU School of Medicine http://10.71.121.158 Copyright@ Xiong Zhang QUESTION 6 How is the filtrate reabsorbed in tubular system? Copyright@ Xiong Zhang
Urinary System Dr. ZHANG Xiong Dept. of Physiology ZJU School of Medicine http://10.71.121.158 Copyright@ Xiong Zhang QUESTION 6 How is the filtrate reabsorbed in tubular system? Copyright@ Xiong Zhang
Urinary System kidneys, ureters, bladder & urethra
 Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Kidney Function Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Endocrine functions regulates
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Chapter 26 The Urinary System. Overview of Kidney Functions. External Anatomy of Kidney. External Anatomy of Kidney
 Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Chapter 26 The Urinary System Kidneys, ureters, urinary bladder & urethra Urine flows from each kidney, down its ureter to the bladder and to the outside via the urethra Filter the blood and return most
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Glomerular Capillary Blood Pressure
 Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Glomerular Capillary Blood Pressure Fluid pressure exerted by blood within glomerular capillaries Depends on Contraction of the heart Resistance to blood flow offered by afferent and efferent arterioles
Fluid and electrolyte balance, imbalance
 Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Fluid and electrolyte balance, imbalance Body fluid The fluids are distributed throughout the body in various compartments. Body fluid is composed primarily of water Water is the solvent in which all solutes
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note
![Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note Running head: NEPHRON 1. The nephron the functional unit of the kidney. [Student Name] [Name of Institute] Author Note](/thumbs/77/75431210.jpg) Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
Running head: NEPHRON 1 The nephron the functional unit of the kidney [Student Name] [Name of Institute] Author Note NEPHRON 2 The nephron the functional unit of the kidney The kidney is an important excretory
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
BIOL 2402 Fluid/Electrolyte Regulation
 Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Dr. Chris Doumen Collin County Community College BIOL 2402 Fluid/Electrolyte Regulation 1 Body Water Content On average, we are 50-60 % water For a 70 kg male = 40 liters water This water is divided into
Urinary System kidneys, ureters, bladder & urethra
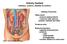 Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
Urinary System kidneys, ureters, bladder & urethra Filters blood removes waste products conserves salts, glucose, proteins, nutrients and water Produces urine Kidney Function Endocrine functions regulates
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM
 RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
RENAL PHYSIOLOGY WESTMEAD PRIMARY EXAM RENAL PHYSIOLOGY - ANATOMY Glomerulus + renal tubule Each kidney has 1.3 million nephrons Cortical nephrons (85%) have shorter Loop of Henle than Juxtamedullary nephrons
Normal Renal Function
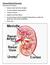 Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Renal Physiology - Lectures
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD lharris@lsuhsc.edu Renal Physiology - Lectures Physiology of Body Fluids 2. Structure & Function of the Kidneys 3. Renal Clearance & Glomerular Filtration
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Functions of the kidney
 Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Physiology of Urinary tract Kidney, Ureter, Urinary bladder Urethra Kidney function Excretion Physiology of volume regulation Functions of the kidney Excretion of dangerous substances endogenous (metabolites):
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
Collin County Community College RENAL PHYSIOLOGY
 Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Collin County Community College BIOL. 2402 Anatomy & Physiology WEEK 12 Urinary System 1 RENAL PHYSIOLOGY Glomerular Filtration Filtration process that occurs in Bowman s Capsule Blood is filtered and
Chapter 17. Lecture Outline. See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes.
 Chapter 17 Lecture Outline See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Chapter 17 Lecture Outline See separate PowerPoint slides for all figures and tables pre-inserted into PowerPoint without notes. Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
8. URINE CONCENTRATION
 8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
8. URINE CONCENTRATION The final concentration of the urine is very dependent on the amount of liquid ingested, the losses through respiration, faeces and skin, including sweating. When the intake far
5.Which part of the nephron removes water, ions and nutrients from the blood?
 Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
organs of the urinary system
 organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
organs of the urinary system Kidneys (2) bean-shaped, fist-sized organ where urine is formed. Lie on either sides of the vertebral column, in a depression beneath peritoneum and protected by lower ribs
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
RENAL FUNCTION An Overview
 RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL FUNCTION An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ. Temple 1 Kidneys
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (4) Dr. Attila Nagy 2018 Intercalated cells Intercalated cells secrete either H + (Typ A) or HCO 3- (Typ B). In intercalated cells Typ A can be observed
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Physiology (6) 2/4/2018. Rahmeh Alsukkar
 Physiology (6) 2/4/2018 Rahmeh Alsukkar **unfortunately the sheet does not involve the slides. ** the doctor repeat a lot of things from the previous lecture so this sheet will begin from slide 139 to
Physiology (6) 2/4/2018 Rahmeh Alsukkar **unfortunately the sheet does not involve the slides. ** the doctor repeat a lot of things from the previous lecture so this sheet will begin from slide 139 to
Basic Functions of the Kidneys
 Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Dr. Adelina Vlad Basic Functions of the Kidneys Eliminate plasma METABOLIC WASTE PRODUCTS and FOREIGN COMPOUNDS The kidney are the primary means for eliminating metabolic waste products (urea, creatinine,
Diagram of the inner portions of the kidney
 Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
mid ihsan (Physiology ) GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B **
 (Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
(Physiology ) mid ihsan GFR is increased when A -Renal blood flow is increased B -Sym. Ganglion activity is reduced C-A and B ** Colloid pressure in the efferent arteriole is: A- More than that leaving
Excretory System-Training Handout
 Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Excretory System-Training Handout Karen L. Lancour National Rules Committee Chairman Life Science Excretion - Excretion is the removal of the metabolic wastes of an organism. Wastes that are removed include
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
CHAPTER 27 LECTURE OUTLINE
 CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
CHAPTER 27 LECTURE OUTLINE I. INTRODUCTION A. Body fluid refers to body water and its dissolved substances. B. Regulatory mechanisms insure homeostasis of body fluids since their malfunction may seriously
Dept. of Physiology. ZJU School of Medicine.
 Urinary System Dr. ZHANG Xiong Dept. of Physiology ZJU School of Medicine Http://10.10.10.151/Able.Acc2.Web/Template/View.aspx?action =view&coursetype=0&courseid=26519 QUESTION 6 How is the filtrate reabsorbed
Urinary System Dr. ZHANG Xiong Dept. of Physiology ZJU School of Medicine Http://10.10.10.151/Able.Acc2.Web/Template/View.aspx?action =view&coursetype=0&courseid=26519 QUESTION 6 How is the filtrate reabsorbed
Regulating the Internal Environment. AP Biology
 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Therapeutics of Diuretics
 (Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
(Last Updated: 08/22/2018) Created by: Socco, Samantha Therapeutics of Diuretics Thambi, M. (2017). The Clinical Use of Diuretics. Lecture presented at PHAR 503 Lecture in UIC College of Pharmacy, Chicago.
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi
 Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Chapter 24: The Urinary System
 Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
Chapter 24: The Urinary System Overview of kidney functions n Regulation of blood ionic composition n Regulation of blood ph n Regulation of blood volume n Regulation of blood pressure n Maintenance of
הנפרון. Introduction to Physiology (Course # 72336) THE KINDEY regulation of water and inorganic ions. Adi Mizrahi
 Introduction to Physiology (Course # 72336) 1 THE KINDEY regulation of water and inorganic ions Adi Mizrahi mizrahia@cc.huji.ac.il הכליה עקרונות של תפקוד ומבנה בסיסיים 2 הנפרון הכליה רגולציית מים ויונים
Introduction to Physiology (Course # 72336) 1 THE KINDEY regulation of water and inorganic ions Adi Mizrahi mizrahia@cc.huji.ac.il הכליה עקרונות של תפקוד ומבנה בסיסיים 2 הנפרון הכליה רגולציית מים ויונים
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
