Retinal arterial macroaneurysm causing multilevel retinal hemorrhage
|
|
|
- Juniper Townsend
- 5 years ago
- Views:
Transcription
1 Optometry (2009) 80, Retinal arterial macroaneurysm causing multilevel retinal hemorrhage Elizabeth Kester, O.D., a and Erica Walker, O.D. b a William Chappell VA Outpatient Clinic, Daytona Beach, Florida; and b Orlando VA Healthcare Center, Orlando, Florida. KEYWORDS Retinal arterial macroaneurysm; Hypertension; Masquerade syndrome; Intravenous fluorescein angiography Abstract BACKGROUND: Retinal arterial macroaneurysms are focal dilatations of the retinal arteries that present with varying degrees of retinal hemorrhage or exudation. They are most often associated with hypertension and may masquerade as many other retinal conditions. CASE REPORT: A hypertensive 59-year-old man presented to the clinic with a sudden onset of painless vision loss in the left eye. Best-corrected visual acuities were 20/20 in the right eye and counting fingers at 3 feet with eccentric viewing in the left. Dilated fundus examination found a multilevel retinal hemorrhage involving most of the superior arcade and extending into the macular area. A diagnosis of retinal arterial macroaneurysm was given after fluorescein angiography and evaluation by a retina specialist. Hemorrhage resolved without treatment, and visual acuity returned to 20/25 by the 6-month follow-up visit. CONCLUSIONS: Optometrists should be aware of presenting signs and symptoms associated with retinal macroaneurysms as well as the many differentials and possible treatments. Given the high incidence of associated systemic disease, proper knowledge of necessary systemic workup is also critical. Optometry 2009;80: Retinal arterial macroaneurysms have been described in the literature for many years. These vascular lesions can have a multitude of findings at presentation, including multilevel retinal hemorrhages, exudates, and edema. Primary eye care providers need to be familiar with the varied presentations, differential diagnoses, and management options of retinal arterial macroaneurysms. Systemic diseases, such as hypertension, have been associated with macroaneurysms; therefore, a systemic workup may be indicated. The following case report describes a patient with a macroaneurysm, from the significant hemorrhagic presentation to eventual resolution, over 18 months of follow-up. This case also shows that a multidisciplinary approach, including primary eye provider, Corresponding author: Elizabeth Kester, O.D., William Chappell VA Outpatient Clinic, 551 National Healthcare Dr., Daytona Beach, Florida Elizabeth.kester@va.gov retina specialist, and internist/primary care provider may be necessary. Case report A 59-year-old man presented with complaints of sudden loss of vision in the left eye (O.S.) upon wakening that morning. He reported that a large, yellowish-red spot was blocking his central vision O.S., and he felt it had the appearance of blood. He denied pain O.S. or any loss of vision in the right eye (O.D.). He denied any recent symptoms of flashes or floaters in either eye. Medical history was significant for type 2 diabetes mellitus, hyperlipidemia, peripheral neuropathy, pernicious anemia, vitamin B12 deficiency, and actinic keratosis. Ocular history was unremarkable. The patient was examined approximately 9 months prior, and no ocular pathology was noted at that time. Current medications included glipizide, hydroxyzine pamoate, insulin novolin 70/30, /09/$ -see front matter -This is a U.S. government work. There are no restrictions on its use. Published by Elsevier, Inc. on behalf of the American Optometric Association. doi: /j.optm
2 426 Optometry, Vol 80, No 8, August 2009 naproxen, and propoxyphene N/APAP. Blood pressure was measured in the office at 149/89 mmhg. Best-corrected visual acuity was 20/20 O.D. and counting fingers at 3 feet with eccentric viewing O.S. Pupils were equal, round, and reactive to light without afferent pupillary defect. Ocular motility was full in both eyes (OU), and confrontation fields were full to finger counting with some difficulty O.S. Anterior-segment slit lamp examination found early nuclear sclerotic lens changes with otherwise unremarkable findings. Applanation tonometry found tensions of 16 mmhg O.D. and 14 mmhg O.S. Dilated fundus examination found vertical cup-to-disc ratios of 0.3 O.D. and 0.3 O.S. Posterior pole, macular, and peripheral examination findings were unremarkable O.D. A large retinal hemorrhage extended from the superior arcade inferiorly to the superior rim of the optic nerve and also extended through the macular area obscuring macular details (see Figure 1A). The hemorrhage was multilevel, including preretinal, intraretinal, and subretinal involvement. A possible source of the hemorrhage could be appreciated in the superior arcade, as slight vessel elevation or outpouching was noted, but obscuration by the hemorrhage made it difficult to determine. A tentative diagnosis of macroaneurysm was made, and the patient was scheduled to see a retina specialist the following day. Clinical picture and patient complaints were unchanged the following day. Intravenous fluorescien angiography (IVFA) and indocyanine green (ICG) angiography were performed but did not show any areas of active leakage or hotspots. The retina specialist felt it was a multilevel retinal hemorrhage likely caused by a macroaneurysm. No treatment was recommended at that time, and a follow-up appointment was made for 1 month. Strict blood pressure control was stressed, and the patient s primary care physician started him on lisinopril, 5 mg/day the following day. At the 1-month follow-up examination, the patient felt he may have had a minimal improvement in his vision O.S. Best-corrected visual acuity was measured at 20/20 O.D. and 20/400 O.S. Pupils, anterior segment examination, and intraocular pressures (IOPs) were unremarkable. Dilated fundus examination was unchanged O.D., and the left eye showed some resolution of the multilevel hemorrhage from presentation (see Figure 1B). Portions of the hemorrhage contained degenerating red blood cells, and this dehemoglobinization gives portions of the resolving hemorrhage a yellowish color. A small amount of exudate was visible temporal to the macula. No treatment was recommended at that time given the improvement in the clinical picture. The patient was scheduled for a re-evaluation in 1 month. The visual acuity in the left eye was still 20/400 at the 2- month follow-up but the patient felt the vision was improving. On fundus examination O.S., the hemorrhage was still resolving, with most of the hemorrhage dehemoglobinized with a yellowish appearance (see Figure 1C). No new leakage or bleeding was noted that day. The retina specialist felt that if there was no resolution in 3 to 4 weeks, a 25-gauge vitrectomy would be indicated. Blood pressure at this visit had improved to 115/68 mmhg. Three months after initial presentation, the patient s visual acuity had improved to 20/100 O.S. A preretinal Figure 1 Fundus photos of the left eye at A, Initial presentation; B, 1 month; C, 2 months; D, 4 months; and E, 6 months after presentation.
3 Kester and Walker Clinical Care 427 hemorrhage was still present extending from the optic nerve to the macula, but given the improvement in vision, no treatment was recommended at that time. Four months after the initial visit, the visual acuity was 20/150 O.S., and a small amount of preretinal hemorrhage was still present in the macular area, as well as temporal to the optic nerve and in the superior arcade (see Figure 1D). Repeat IVFA was performed, and no leakage was noted. A return visit was scheduled for 8 weeks. At the 6-month follow-up visit, visual acuity had improved to 20/25 O.S. Almost complete resolution of the macular hemorrhage was noted, with small residual areas of preretinal hemorrhage noted in the posterior pole (see Figure 1E). A small area of perivascular sclerotic tissue was present in the superior arcade at the previous source of the macroaneurysm. The patient was encouraged to continue proper blood pressure control and to return to the clinic immediately with any changes in vision. The patient returned 1 year later, with best-corrected visual acuity of 20/20 O.D. and 20/20 O.S. Vessel sclerosis was still present at the site of the previous macroaneurysm, and a very faint preretinal heme was visible temporally to the optic nerve. women affected. 7 Several studies have reported average age on presentation of 66.1 years, years, 8 and 73.7 years, 9 respectively, with increasing age elevating risk of occurrence. Systemic risk factors include hypertension, atherosclerosis, hyperlipidemia, retinal arterial emboli, 10 cerebrovascular disease, and polycythemia. 4 Hypertension is the most common association, affecting approximately 75% of patients presenting with MAs. 11 In fact, in a retrospective study of macroaneurysm patients by Lavin et al., 4 17 of the 18 patients examined by their medical clinic were found to have evidence of systemic vascular or relevant metabolic disease. Patients who present with MAs require full investigation for systemic disease with attention to hypertension, systemic vascular disease, and embolic disease. Recommended studies include complete blood count (with differential and platelets), fasting blood sugar and glycosylated hemoglobin, blood pressure, fasting lipid profile, carotid auscultation or carotid duplex ultrasonography, and cardiac evaluation. A prompt multispecialty approach may include primary eye provider, retina specialist, internal medicine physician, and cardiologist. Discussion Background Retinal arterial macroaneurysms (MAs) have been described in the literature since the nineteenth century, 1,2 though Robertson was the first to give the retinal finding a name and description in The term was applied to retinal arterial lesions with the following characteristics: (1) arterial swelling with a saccular or fusiform ( blowout or cuffed ) appearance; (2) positioned on the first 3 orders of the retinal artery tree; and (3) found mainly at arterial bifurcations. Lavin et al. 4 described MAs as local arterial dilatations with variable degrees of artery wall hyalinization and surrounding retinal exudate or hemorrhage. 4 These vessel dilatations tend to rupture before they grow large and tend to be no larger than approximately 1/3 disc diameter in size. 5,6 Symptomatic patients notice a loss of vision caused by retinal hemorrhage (on any level of the retina), exudate, or edema. Careful examination and regards to differential diagnoses are important, because MAs are often diagnosed incorrectly and are regarded as a masquerade syndrome. 7 Given strong associations with systemic disease, patients with macroaneurysms should also have prompt medical evaluation. Epidemiology and risk factors Macroaneurysms are most frequently seen in elderly persons in the sixth to eighth decade with a preponderance of Pathophysiology Histologic study of macroaneurysms confirms a true aneurysm formation including vessel wall thickening, change in hyaline, and elastotic degeneration. 12 As arterioles age, intimal collagen replaces smooth muscle fibers, and the arterial wall becomes less elastic. These vessels are more susceptible to dilatation from elevated hydrostatic pressure. 9 Hypertensive patients also experience elevated hydrostatic pressure, decreased autoregulation, and hyaline degeneration and are especially at risk. Though this setting predisposes these patients to the formation of MAs, the cause of focal arterial wall weakness is still not completely understood. 8,10 Most MAs occur at arteriovenous crossings, where the 2 vessels are in contact and share a common coat. Less structural support is present in this area and the weaker vessel walls may be prone to aneurysmal formation. 4 Macroaneurysms have a dynamic formation, followed by enlargement (which may or may not disrupt the blood retinal barrier). Most MAs then undergo a gradual thrombosis, fibrosis, and spontaneous involution. The type of vessel changes classifies MAs as saccular (blow-out) or fusiform (cuffed). 12,13 Fusiform MAs display circumferential widening of the retinal artery, whereas saccular MAs represent localized outpouchings of the retinal artery wall. The saccular type is more prone to bleed, as a thin, stretched aneurysmal sac is relatively easy to perforate in an area of high perfusion pressure. 13 After resolution of the MA, findings often include vessel kinking at the site of the resolved MA, arteriolar constriction proximal to the MA, and arterial sheathing distal to the MA Fluorescein angiographic findings
4 428 Optometry, Vol 80, No 8, August 2009 after MA resolution include widening of the capillary-free zone and intra-arterial collateral vessels. 9 Presentation Macroaneurysms most commonly are seen on the first 3 orders of the retinal artery tree and are found mainly at vessel bifurcations. They are more commonly found on superotemporal and inferotemporal vessels than nasal vessels (see Figure 2). 4 The most dominant feature of MAs is hemorrhage into the retinal and vitreous spaces and, less frequently, retinal exudate and edema. Amount of hemorrhage can be variable, from small hemorrhages involving 1 layer of the retina, to large, multilevel hemorrhages with or without vitreous extension. Exudation can be very insignificant in severity or can produce a massive exudative response. Retinal hemorrhage can involve subretinal, intraretinal, and preretinal spaces. It has been reported that approximately 50% of patients have an associated retinal hemorrhage, 40% have simultaneous subretinal and preretinal bleeding, and 10% have a vitreous hemorrhage. 17 Vitreous hemorrhage from MAs can lead to ghost cell glaucoma and has been reported to be associated with a secondary acute angle closure glaucoma. 18,19 Though some MAs that do not affect the macular area may be asymptomatic, patients most commonly present with acute, painless loss of vision. Level of vision loss depends on severity of hemorrhage or exudate. Central loss of vision is often caused by retina hemorrhage, exudate, or edema affecting the macula or a generalized loss of vision caused by vitreous hemorrhage. 4 Subretinal hemorrhage is the most damaging to sight and retinal tissue, especially in the macular area, as subretinal blood can be toxic. 9 Irreversible damage to photoreceptor and retinal pigmented epithelial cells can occur after 2 weeks of subretinal bleeding as seen in animal studies, which can lead to permanent loss of central vision. 20 Prognosis for visual recovery depends on macular pathology. Patients with vitreous hemorrhage or premacular hemorrhage have a better visual prognosis than those with macular edema, intraretinal hemorrhage, or submacular hemorrhage. 21 Differential diagnosis Clinical presentation of MAs can vary widely and is considered a masquerade syndrome. 7 They often are misdiagnosed before fluorescein angiography. One study found hemorrhagic MAs were misdiagnosed at a rate of 75% upon presentation. 4 Differential diagnoses vary depending on ocular signs upon presentation. Differential diagnosis for a vitreous hemorrhage would include proliferative diabetic retinopathy, retinal tear, branch retinal vein occlusion, and hemorrhagic macular degeneration. When presented with hemorrhage near or involving the macula, etiologies such as macular degeneration, presumed ocular histoplasmosis syndrome (POHS), high myopia, trauma, Valsalva Figure 2 patient. Presentation of a retinal arterial macroaneurysm in another retinopathy, idiopathic polypoidal choroidal vasculopathy, or choroidal neovascularization from any cause should be considered. 22 When presented with retinal hemorrhaging or exudation, differentials should include diabetic retinopathy, central or branch retinal vein occlusion, venous macroaneurysms, Coat s disease, retinal telangiectasias, radiation retinopathy, cavernous hemangioma, and retinal capillary angiomas. Leakage of blood beneath the sensory retina from MAs can appear as a dark mass that may simulate choroidal melanoma. 23 Larger retinal macroaneurysms may present with large amounts of retinal exudation and hemorrhage and can simulate metastatic intraocular tumor. 5 Because macroaneurysms can mimic many retinal conditions, fluorescein angiography often establishes the diagnosis. Fluorescein angiography of fusiform MAs shows rapid filling in early arterial phase, whereas saccular MAs showed minimal early filling, with good filling in the middle to late phases. 4 Filling in the early arterial phase may be segmental in nature due to clot formation or scarring from blockage of the lumen by thrombosis or endothelial cell formation. 24 Angiography of MAs that have self-sealed may show no leakage, as in the case discussed above. Fluorescein may also show changes in capillaries adjacent to the MAs, including dilatation, telangiectasia, and closure. In cases in which retinal hemorrhage blocks visual inspection of the aneurysm, as well as adequate imaging with fluorescein angiography, ICG has been useful. ICG s dye absorption and emission peak is in the near-infrared spectrum, and allows better penetration through dense hemorrhage, exudates, and retinal pigmented epithelial changes. 25,26 Fluorescein angiography uses blue or green light in the shorter wavelengths and does not have this ability. ICG is also 98% protein bound (compared with 60% for fluorescein), so it leaks less and provides sharper, more well-defined images, especially of the choroid and choroidal pathology. 27 ICG can pinpoint the exact location of the macroaneurysm in cases of dense hemorrhage, which is useful in planning surgery or treatment. ICG of MAs will show well-defined areas of hyperfluoresence. Standardized A-scan and B-scan echography can also be helpful
5 Kester and Walker Clinical Care 429 in diagnosing MAs before vitrectomy when dense vitreous hemorrhage obscures the retina. Echographic features characteristic of MAs include irregular internal reflectivity and a pulsatile vascular structure at the anterior aspect of the lesion. 28 Treatment The decision to treat a macroaneurysm or the hemorrhages associated with it depends on several factors. Because the majority of MAs will undergo spontaneous involution, with no residual vision loss, a strong case can be made for observation. 17 Vander et al. 29 suggested the following general recommendations: (1) patients with good vision and no macular involvement should be observed; (2) patients with decreased vision on the basis of intraretinal, preretinal, or vitreous hemorrhage should be observed over several months for spontaneous resolution before treatment is given; and (3) patients with macular involvement (edema, exudates, or submacular hemorrhage) or retinal detachment should be treated. The treatment options for MAs include direct and indirect laser photocoagulation and, in some cases, surgical excision with vitrectomy. Laser photocoagulation, whether direct or indirect, uses Argon green or dye yellow tunable laser at low energy levels to create light to medium burns on the retina. The goal of direct treatment is to accelerate the involution of the macroaneurysm, thereby eliminating the source of leakage. Indirect treatment applies laser burns to the retina surrounding the MA, forming a barrier between the leaking MA and the macula. The complications from direct and indirect laser treatment include arteriolar occlusion, severe foveal capillary dropout, and subretinal scarring. 30 In cases in which the MA is too large or cannot be treated by photocoagulation, or when recurrences are a problem, surgical excision has emerged as an alternative. 31 The complications are similar to those of laser photocoagulation, and although photocoagulation remains the first treatment of choice for MAs, surgical excision may be a suitable option for severe cases. 31 Vitreous hemorrhage associated with MAs has a good prognosis for visual recovery and can usually be observed. In general, pars plana vitrectomy should be considered for nonclearing hemorrhage (usually considered after 3 to 6 months) or when the hemorrhage interferes with additional treatment needed to prevent vision loss. 32 Preretinal (subinternal limiting membrane) hemorrhage can also spontaneously resorb with no vision loss; however, the potential exists for epiretinal membrane formation and irreversible retinal damage caused by the toxic effects of the preretinal blood. 33,34 Historically, when treatment was indicated, pars plana vitrectomy was performed. 35 However, for recent, dense preretinal hemorrhage, the use of neodymiumyttrium-aluminum-garnet (Nd:YAG) laser has been reported. 36 The focal disruption to the internal limiting membrane allows the hemorrhage to drain into the vitreous where it can be absorbed more quickly. 33,36,37 However, it must be noted that visual improvement may be limited if a subretinal/submacular hemorrhage exists or if the resultant vitreous hemorrhage is dense and nonclearing, eventually requiring a vitrectomy. 33,35 The Nd:YAG laser procedure also has potential complications such as macular hole and retinal detachment. 35 Before this procedure can be established as the standard of care, a randomized, prospective study is needed to compare observation, primary vitrectomy, and Nd:YAG laser treatment. 35,38 Intraretinal hemorrhages associated with retinal arterial macroaneurysms usually resorb completely and spontaneously with little or no visual compromise. 9,17,34 However, a subretinal hemorrhage has the potential to be visually devastating, especially if submacular, and the best treatment is not known. In cases of localized, thin-layered hemorrhage, the prognosis for visual recovery is better than in cases of dense, thick-clotted hemorrhage caused by the toxic effects of prolonged bleeding to the photoreceptors and retinal pigment epithelium and the development of fibrin within the clots. 17,39 Clearance of the subretinal blood is essential to improve cellular functioning and prevent further vision loss. 20,36 This can be accomplished via submacular surgery or pneumatic displacement. Both procedures have been studied using tissue plasminogen activator (tpa) to facilitate fibrinolysis and thrombolysis. 36,40 Submacular surgery attempts to remove the hemorrhage via pars plana vitrectomy, drainage of the submacular hemorrhage through a retinotomy, a fluid-air exchange, and then insufflation with an intravitreal gas. The patient is required to have facedown head positioning for about 1 week. 39,40 An alternative to submacular surgery is pneumatic displacement. Pneumatic displacement is less invasive than submacular surgery; it uses an intraocular gas bubble and facedown head positioning to move or displace the hemorrhage, rather than remove it. 36 Pneumatic displacement offers a simpler procedure at a lower cost compared with submacular surgery. Both procedures share potential complications, such as cataract formation, retinal breaks or detachment, epiretinal membrane formation, proliferative vitreo-retinopathy, and endophthalmitis. However, pneumatic displacement might be expected to have less frequent and less severe complications. 36 Conclusion Optometrists should be aware of the many presentations and differential diagnoses of retinal arterial macroaneurysms. Given the high percentage of associated systemic disease, a systemic workup may be required. A multidisciplinary approach, including primary eye provider, retina specialist, and internist/primary care provider may be necessary. Treatment options may include laser photocoagulation, vitrectomy, and surgical excision. Although, as seen in the case discussed, careful observation often is sufficient for an excellent prognosis.
6 430 Optometry, Vol 80, No 8, August 2009 References 1. Doyne RW. Case of peculiar condition of the retina due possibly to the formation of small aneurysms and large extravasation of blood which has become decolourised. Trans Ophthalmol Soc UK 1896;16: Loring FB. Peculiar anatomical development of one of the central arteries of the retina. Trans Am Ophthalmol Soc 1881;3: Robertson DM. Macroaneurysms of the retinal arteries. Ophthalmology 1973;77: Lavin MJ, Marsh RJ, Peart S, et al. Retinal areterial macroaneurysms: a retrospective study of 40 patients. Br J Ophthalmol 1987;71(11): Ohno- Matsui K, Hayano M, Futagami S, et al. Spontaneous involution of a large retinal arterial macroaneurysm. Acta Ophthalmol Scand 2000;78(1): Brown GC, Weinstock F. Arterial macroaneurysm on the optic disk presenting as a mass lesion. Ann Opthalmol 1985;17: Spalter HF. Retinal macroaneurysms: a new masquerade syndrome. Trans Am Ophthalmol Soc 1982;80: Panton RW, Goldberg MF, Farber MD. Retinal arterial macroaneurysms: risk factors and natural history. Br J Ophthalmol 1990;74(10): Moosavi RA, Fong KC, Chopdar A. Retinal artery macroaneurysms: clinical and fluorescein angiographic features in 34 patients. Eye 2006;20(9): Colucciello M. Retinal vascular disease in hypertension. Risk factor modification optimizes vision outcomes. Postgrad Med 2005;117(6): 33-8, Sekuri C, Kayikcioglu M, Kayikcioglu O. Retinal artery macroaneurysm as initial presentation of hypertension. Int J Cardiol 2004;93(1): Fitche C, Streeten BW, Freedman AH. A histopathologic study of retinal arterial aneurysms. Am J Ophthalmol 1978;85: Abdel-Khalk MN, Richardson J. Retinal macroaneurysm: natural history and guideline for treatment. Br J Opthalmol 1986;70(1): Palestine AG, Robertson DM, Goldstein B. Macroaneurysms of the retinal arteries. Am J Ophthalmol 1982;93: Lewis RA, Norton EWD, Gass JDM. Acquired arterial macroaneurysm of the retinal arteries. Br J Ophthalmol 1976;60: Cleary PE, Kohner EM, Hamilton AM, et al. Retinal macroaneurysms. Br J Ophthalmol 1975;59: Rabb M, Gagliano D, Teske M. Retinal arterial macroaneurysm. Surv Ophthalmol 1988;33(2): Spraul CW, Grossniklaus HE. Vitreous hemorrhage. Surv Ophthalmol 1997;42(1): Arthur SM, Mason J, Roberts B, et al. Secondary acute angle closure glaucoma associated with vitreous hemorrhage after ruptured retinal arterial macroaneurysm. Am J Ophthalmol 2004;138(4): Toth CA, Morse LS, Hjelmeland LM, et al. Fibrin directs early retinal damage after experimental subretinal hemorrhage. Arch Ophthalmol 1991;109(5): Tonotsuka T, Imai M, Saito K, et al. Visual prognosis for symptomatic retinal arterial macroaneurysm. Jpn J Ophthalmol 2003;47(5): Lindgren G, Sjodell L, Lindblom B. A prospective study of dense spontaneous vitreous hemorrhage. Am J Ophthalmol 1995;119(4): Sheilds CL, Sheilds JA. Subretinal hemorrhage from a retinal arterial macroaneurysm simulating a choroidal melanoma. Ophthalmic Surg Lasers 2001;32(1): Brent BD, Gonce M, Diamond JG. Pars plana vitrectomy for complications of retinal arterial macroaneurysms a case series. Ophthalmic Surg 1993;24(8): Bischoff PM, Flower RW. Ten years experience with choroidal angiography using indocyanine green dye: a new routine examination or an epilogue? Doc Ophthalmol 1985;60(3): Townsend-Pico WA, Meyers SM, Lewis H. Indocyanine green angiography in the diagnosis of retinal arterial macroaneurysms associated with submacular and preretinal hemorrhages: a case series. Am J Ophthalmol 2000;129(1): Guyer DR, Yannuzi LA, Slakter JS, et al. Digital indocyanine-green videoangiography of occult choroidal neovascularization. Ophthalmology 1994;101(10): Tang WM, Pulido JS, Connor TB, et al. Echographic characteristics of retinal arterial macroaneurysm. Retina 1998;18(6): Vander JF, Duker JS, Jaeger EA. Miscellaneous diseases of the fundus. In: Tasman W, Jaeger E, eds. Duane s clinical ophthalmology. Revised ed. Vol 3. Philadelphia: Lippincott-Raven; 1997: Brown DM, Sobol WM, Folk JC, et al. Retinal arteriolar macroaneurysms: long term visual outcome. Br J Ophthalmol 1994;78: Oie Y, Emi K. Surgical excision of retinal macroaneurysms with submacular hemorrhage. Jpn J Ophthalmol 2006;50: Goff MJ, McDonald HR, Johnson RN, et al. Causes and treatment of vitreous hemorrhage. Compr Ophthalmol Update 2006;7(3): Gedik S, Gur S, Yilmaz G, et al. Retinal arterial macroaneurysm rupture following fundus fluorescein angiography and treatment with Nd: YAG laser membranectomy. Ophthalmic Surg Lasers Imaging 2007; 38(2): Gurwood A, Nicholson CR. Retinal arterial macroaneurysm: a case report. J Am Optom Assoc 1998;69: Ulbig MW, Mangouritsas G, Rothbacher HH, et al. Long-term results after drainage of premacular subhyaloid hemorrhage into the vitreous with a pulsed Nd:YAG laser. Arch Ophthalmol 1998; 116(11): Wu TT, Sheu SJ. Intravitreal tissue plasminogen activator and pneumatic displacement of submacular hemorrhage secondary to retinal artery macroaneurysm. J Ocul Pharmacol Ther 2005;21(1): Iijima H, Satoh S, Tsukahara S. Nd:YAG laser photodisruption for preretinal hemorrhage due to retinal macroaneurysm. Retina 1998;18(5): Celebi S, Kukner AS. Photodisruptive Nd:YAG laser in the management of premacular subhyaloid hemorrhage. Eur J Ophthalmol 2001;11(3): Tan CS, Au Eong KG. Surgical drainage of submacular haemorrhage from ruptured retinal arterial macroaneurysm. Acta Ophthalmol Scand 2005;83(2): Humayun M, Lewis H, Flynn HW Jr, et al. Management of submacular hemorrhage associated with retinal arterial macroaneurysms. Am J Ophthalmol 1998;126:
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion
 Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Case Report: Indocyanine Green Dye Leakage from Retinal Artery in Branch Retinal Vein Occlusion Hiroki Fujita, Kyoko Ohno-Matsui, Soh Futagami and Takashi Tokoro Department of Visual Science, Tokyo Medical
Retinal Imaging Conference. Brooke LW Nesmith, M.D. University of Louisville Department of Ophthalmology and Visual Sciences 8/7/2014
 Retinal Imaging Conference Brooke LW Nesmith, M.D. University of Louisville Department of Ophthalmology and Visual Sciences 8/7/2014 Patient Presentation CC: Routine yearly diabetic eye exam HPI: 59yo
Retinal Imaging Conference Brooke LW Nesmith, M.D. University of Louisville Department of Ophthalmology and Visual Sciences 8/7/2014 Patient Presentation CC: Routine yearly diabetic eye exam HPI: 59yo
The Human Eye. Cornea Iris. Pupil. Lens. Retina
 The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
The Retina Thin layer of light-sensitive tissue at the back of the eye (the film of the camera). Light rays are focused on the retina then transmitted to the brain. The macula is the very small area in
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Diabetic Retinopathy Diabetes can be classified into type 1 diabetes mellitus and type 2 diabetes mellitus, formerly known as insulin-dependent diabetes mellitus, and non-insulin diabetes mellitus, respectively.
Case Report Nd: YAG laser puncture for spontaneous premacular hemorrhage
 Int J Clin Exp Med 2017;10(1):1353-1357 www.ijcem.com /ISSN:1940-5901/IJCEM0037966 Case Report Nd: YAG laser puncture for spontaneous premacular hemorrhage Qing Liu, Wenli Duan, Yingjun Min Department
Int J Clin Exp Med 2017;10(1):1353-1357 www.ijcem.com /ISSN:1940-5901/IJCEM0037966 Case Report Nd: YAG laser puncture for spontaneous premacular hemorrhage Qing Liu, Wenli Duan, Yingjun Min Department
Retina Conference. Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014
 Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
Retina Conference Janelle Fassbender, MD, PhD University of Louisville Department of Ophthalmology and Visual Sciences 09/04/2014 Subjective CC/HPI: 64 year old Caucasian female referred by outside ophthalmologist
ZEISS AngioPlex OCT Angiography. Clinical Case Reports
 Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Clinical Case Reports Proliferative Diabetic Retinopathy (PDR) Case Report 969 PROLIFERATIVE DIABETIC RETINOPATHY 1 1-year-old diabetic female presents for follow-up of proliferative diabetic retinopathy
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome)
 Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
Recurrent intraocular hemorrhage secondary to cataract wound neovascularization (Swan Syndrome) John J. Chen MD, PhD; Young H. Kwon MD, PhD August 6, 2012 Chief complaint: Recurrent vitreous hemorrhage,
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Clinical Case Presentation. Branch Retinal Vein Occlusion. Sarita M. Registered Nurse Whangarei Base Hospital
 Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinical Case Presentation on Branch Retinal Vein Occlusion Sarita M. Registered Nurse Whangarei Base Hospital Introduction Case Study Pathogenesis Clinical Features Investigations Treatment Follow-up
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA
 OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
OCCLUSIVE VASCULAR DISORDERS OF THE RETINA Learning outcomes By the end of this lecture the students would be able to Classify occlusive vascular disorders (OVD) of the retina. Correlate the clinical features
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion
 Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
Neovascular Glaucoma Associated with Cilioretinal Artery Occlusion Combined with Perfused Central Retinal Vein Occlusion Man-Seong Seo,* Jae-Moon Woo* and Jeong-Jin Seo *Department of Ophthalmology, Chonnam
PART 1: GENERAL RETINAL ANATOMY
 PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
PART 1: GENERAL RETINAL ANATOMY General Anatomy At Ora Serrata At Optic Nerve Head Fundoscopic View Of Normal Retina What Is So Special About Diabetic Retinopathy? The WHO definition of blindness is
Vitreous Hemorrhage Caused by Ruptured Retinal Macroaneurysm
 Published online: February 1, 2014 1663 2699/14/0051 0044$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Published online: February 1, 2014 1663 2699/14/0051 0044$39.50/0 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial 3.0 Unported license (CC BY-NC)
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Large capillary aneurysms secondary to retinal venous obstruction
 British Journal of Ophthalmology, 1981, 65, 36-41 Large capillary aneurysms secondary to retinal venous obstruction JOEL SCHULMAN, LEE M. JAMPOL, AND MORTON F. GOLDBERG From the University of Illinois
British Journal of Ophthalmology, 1981, 65, 36-41 Large capillary aneurysms secondary to retinal venous obstruction JOEL SCHULMAN, LEE M. JAMPOL, AND MORTON F. GOLDBERG From the University of Illinois
RETINAL CONDITIONS RETINAL CONDITIONS
 GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
GENERAL INFORMATION RETINAL CONDITIONS RETINAL CONDITIONS WHAT ARE RETINAL CONDITIONS? Retinal conditions affect the light-sensitive tissue at the back of eye known as the retina. They include diseases
Diabetic Retinopathy
 Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetic Retinopathy Diabetes mellitus is one of the leading causes of irreversible blindness worldwide. In the United States, it is the most common cause of blindness in people younger than 65 years.
Diabetes & Your Eyes
 Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Diabetes & Your Eyes Diabetes is a disease that occurs when the pancreas does not secrete enough insulin or the body is unable to process it properly. Insulin is the hormone that regulates the level of
Moncef Khairallah, MD
 Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Moncef Khairallah, MD Department of Ophthalmology, Fattouma Bourguiba University Hospital Faculty of Medicine, University of Monastir Monastir, Tunisia INTRODUCTION IU: anatomic form of uveitis involving
Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage
 Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
Case Report Brunei Int Med J. 2015; 11 (1): 49-53 Tuberous sclerosis presenting as atypical aggressive retinal astrocytoma with proliferative retinopathy and vitreous haemorrhage Pui Ling TANG and Mae-Lynn
Central serous chorioretinopathy (CSCR) was
 Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
Case Report 777 Perfluorocarbon Liquid-Assisted External Drainage in the Management of Central Serous Chorioretinopathy with Bullous Serous Retinal Detachment Hung-Chiao Chen, MD; Jau-Der Ho, MD; San-Ni
OCT Angiography in Primary Eye Care
 OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
OCT Angiography in Primary Eye Care An Image Interpretation Primer Julie Rodman, OD, MS, FAAO and Nadia Waheed, MD, MPH Table of Contents Diabetic Retinopathy 3-6 Choroidal Neovascularization 7-9 Central
Grand Rounds. Eddie Apenbrinck M.D. University of Louisville School of Medicine Department of Ophthalmology & Visual Sciences 6/20/2014
 Grand Rounds Eddie Apenbrinck M.D. University of Louisville School of Medicine Department of Ophthalmology & Visual Sciences 6/20/2014 Subjective CC: sudden painless loss of vision OD HPI: 75 year old
Grand Rounds Eddie Apenbrinck M.D. University of Louisville School of Medicine Department of Ophthalmology & Visual Sciences 6/20/2014 Subjective CC: sudden painless loss of vision OD HPI: 75 year old
Fluorescein and Indocyanine Green Videoangiography of Choroidal Melanomas
 luorescein and Indocyanine Green Videoangiography of Choroidal Melanomas Leyla S. Atmaca, igen Batioğlu and Pelin Atmaca Eye Clinic, Ankara University Medical School, Ankara, Turkey Purpose: This study
luorescein and Indocyanine Green Videoangiography of Choroidal Melanomas Leyla S. Atmaca, igen Batioğlu and Pelin Atmaca Eye Clinic, Ankara University Medical School, Ankara, Turkey Purpose: This study
The use of a high-intensity laser to create an anastomotic
 Case Report 866 Laser Chorioretinal Venous Anastomosis for Progressive Nonischemic Central Retinal Vein Occlusion Chih-Hsin Chen, MD; Chien-Hsiung Lai 1, MD; Hsi-Kung Kuo, MD The use of high or medium-intensity
Case Report 866 Laser Chorioretinal Venous Anastomosis for Progressive Nonischemic Central Retinal Vein Occlusion Chih-Hsin Chen, MD; Chien-Hsiung Lai 1, MD; Hsi-Kung Kuo, MD The use of high or medium-intensity
Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD
 Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
Microperimetric Evaluation of Brilliant Blue G- assisted Internal Limiting Membrane Peeling By Yasser R. Serag, MD Tamer Wasfi, MD El- Saied El-Dessoukey, MD Magdi S. Moussa, MD Anselm Kampik, MD The internal
ISSN X (Print) RC, Mandhana, Kanpur , Uttar Pradesh, India. *Corresponding author Dr. Nutan Saxena
 Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(9B):3302-3306 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
Scholars Journal of Applied Medical Sciences (SJAMS) Sch. J. App. Med. Sci., 2015; 3(9B):3302-3306 Scholars Academic and Scientific Publisher (An International Publisher for Academic and Scientific Resources)
EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion
 EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina
EyePACS Grading System (Part 2): Detecting Presence and Severity of Background (Non-Proliferative) Diabetic Retinopathy Lesion George Bresnick MD MPA Jorge Cuadros OD PhD Anatomy of the eye: 3 Normal Retina
OCULAR HEMORRHAGES. ROSCOE J. KENNEDY, M.D. Department of Ophthalmology
 OCULAR HEMORRHAGES ROSCOE J. KENNEDY, M.D. Department of Ophthalmology Ocular hemorrhages are important not only because they produce visual loss but also because they usually indicate a disorder elsewhere
OCULAR HEMORRHAGES ROSCOE J. KENNEDY, M.D. Department of Ophthalmology Ocular hemorrhages are important not only because they produce visual loss but also because they usually indicate a disorder elsewhere
Guidelines for the Management of Diabetic Retinopathy for the Internist
 Visual Disorder Guidelines for the Management of Diabetic Retinopathy for the Internist JMAJ 45(1): 1 7, 2002 Sadao HORI Professor, Department of Ophthalmology, Tokyo Women s Medical University Abstract:
Visual Disorder Guidelines for the Management of Diabetic Retinopathy for the Internist JMAJ 45(1): 1 7, 2002 Sadao HORI Professor, Department of Ophthalmology, Tokyo Women s Medical University Abstract:
Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
 Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Columbia International Publishing Journal of Ophthalmic Research (2014) Research Article Optical Coherence Tomograpic Features in Idiopathic Retinitis, Vasculitis, Aneurysms and Neuroretinitis (IRVAN)
Authors. Introduction. Introduction. Materials and Methods. Objective 10/27/2015
 Idiopathic Polypoidal Choroidal Vasculopathy (IPCV) in Thai Population Presenting with Choroidal Neovascularization (CNV) A multicenter study Authors Yonrawee Piyacomn 1, Chavakij Bhoomibunchoo 1, Yosanan
Idiopathic Polypoidal Choroidal Vasculopathy (IPCV) in Thai Population Presenting with Choroidal Neovascularization (CNV) A multicenter study Authors Yonrawee Piyacomn 1, Chavakij Bhoomibunchoo 1, Yosanan
Mild NPDR. Moderate NPDR. Severe NPDR
 Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
Diabetic retinopathy Diabetic retinopathy is the most common cause of blindness in adults aged 35-65 years-old. Hyperglycaemia is thought to cause increased retinal blood flow and abnormal metabolism in
ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS
 ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
ORIGINAL ARTICLE ROLE OF LASER PHOTOCOAGULATION VERSUS INTRAVITREAL TRIAMCINOLONE ACETONIDE IN ANGIOGRAPHIC MACULAR EDEMA IN DIABETES MELLITUS Aggarwal Somesh VP 1, Shah Sonali N 2, Bharwada Rekha M 3,
Laser and Anti Vascular Endothelial Growth Factor Agent Treatments for Retinal Arterial Macroaneurysm
 original clinical study Laser and Anti Vascular Endothelial Growth actor Agent Treatments for Retinal Arterial acroaneurysm Yen-Yi Chen,* Lo-Yi Lin,* Pei-Yao Chang,* ang-ting Chen* Elsa L.C. ai,* and Jia-Kang
original clinical study Laser and Anti Vascular Endothelial Growth actor Agent Treatments for Retinal Arterial acroaneurysm Yen-Yi Chen,* Lo-Yi Lin,* Pei-Yao Chang,* ang-ting Chen* Elsa L.C. ai,* and Jia-Kang
Oishi A, Miyamoto K, Yoshimura N. Etiology of carotid cavernous fistula in Japanese. Jpn J Ophthalmol. 2009;53:40-43.
 Kimura T, Takagi H, Miyamoto K, Kita M, Watanabe D, Yoshimura N. Macular hole with epiretinal membrane after triamcinolone-assisted vitrectomy for proliferative diabetic retinopathy. Retinal Cases Brief
Kimura T, Takagi H, Miyamoto K, Kita M, Watanabe D, Yoshimura N. Macular hole with epiretinal membrane after triamcinolone-assisted vitrectomy for proliferative diabetic retinopathy. Retinal Cases Brief
Sudden Vision Loss. Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists
 Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
Sudden Vision Loss Brendan Girschek, MD, FRCSC, FACS Vitreoretinal Surgery Cedar Valley Medical Specialists My Credentials -Residency in Ophthalmology at the LSU Eye Center in New Orleans, LA -Fellowship
FA Conference. Lara Rosenwasser Newman, M.D. 10/2/14 University of Louisville Department of Ophthalmology and Visual Sciences
 FA Conference Lara Rosenwasser Newman, M.D. 10/2/14 University of Louisville Department of Ophthalmology and Visual Sciences Patient Presentation CC: (sent by optometrist) Blurry/foggy vision HPI: 62 yo
FA Conference Lara Rosenwasser Newman, M.D. 10/2/14 University of Louisville Department of Ophthalmology and Visual Sciences Patient Presentation CC: (sent by optometrist) Blurry/foggy vision HPI: 62 yo
VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY
 Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
Basrah Journal Of Surgery VITREOUS FLOATERS AND PHOTOPSIA AS PREDICTORS OF VITREORETINAL PATHOLOGY Salah Zuhair Al-Asadi MB,ChB, FRCS, FIBMS, Lecturer of Ophthalmology, College of Medicine, University
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Ophthalmology Macular Pathways
 Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Ophthalmology Macular Pathways Age related Macular Degeneration Diabetic Macular Oedema Macular Oedema secondary to Central Retinal Macular Oedema secondary to Branch Retinal CNV associated with pathological
Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema
 Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
Original Research Article Study of clinical significance of optical coherence tomography in diagnosis & management of diabetic macular edema Neha Kantilal Desai 1,*, Somesh Vedprakash Aggarwal 2, Sonali
COEXISTENCE OF OPTIC NERVE HEAD DRUSEN
 COEXISTENCE OF OPTIC NERVE HEAD DRUSEN AND COMBINED HAMARTOMA OF THE RETINA AND RETINAL PIGMENT EPITHELIUM IN A TAIWANESE MALE Yo-Chen Chang 1 and Rong-Kung Tsai 2,3 1 Department of Ophthalmology, Kaohsiung
COEXISTENCE OF OPTIC NERVE HEAD DRUSEN AND COMBINED HAMARTOMA OF THE RETINA AND RETINAL PIGMENT EPITHELIUM IN A TAIWANESE MALE Yo-Chen Chang 1 and Rong-Kung Tsai 2,3 1 Department of Ophthalmology, Kaohsiung
Vitrectomy for Diabetic Cystoid Macular Edema
 Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
Vitrectomy for Diabetic Cystoid Macular Edema Yukihiro Sato, Zeon Lee and Hiroyuki Shimada Department of Ophthalmology, Nihon University School of Medicine, Tokyo, Japan Purpose: We evaluated visual outcomes
HIGH DOSE TISSUE PLASMINOGEN ACTIVATOR (TPA) (100 MCG/0.1 ML) AND C3F8 GAS IN PNEUMATIC DISPLACEMENT OF SUBMACULAR
 HIGH DOSE TISSUE PLASMINOGEN ACTIVATOR (TPA) (100 MCG/0.1 ML) AND C3F8 GAS IN PNEUMATIC DISPLACEMENT OF SUBMACULAR HAEMORRHAGE. Stephen A.M. De Souza MD, FRCSC Matthew J Welch MD, Raza M Shah MD, Alan
HIGH DOSE TISSUE PLASMINOGEN ACTIVATOR (TPA) (100 MCG/0.1 ML) AND C3F8 GAS IN PNEUMATIC DISPLACEMENT OF SUBMACULAR HAEMORRHAGE. Stephen A.M. De Souza MD, FRCSC Matthew J Welch MD, Raza M Shah MD, Alan
Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (CSC)
 HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
HPTER 12 Misdiagnosed Vogt-Koyanagi-Harada (VKH) disease and atypical central serous chorioretinopathy (S) linical Features VKH disease is a bilateral granulomatous panuveitis often associated with exudative
ISPUB.COM. Photopsia post flu: A case of MEWDS. S Baisakhiya, S Dulani, S Lele INTRODUCTION CASE HISTORY
 ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
ISPUB.COM The Internet Journal of Ophthalmology and Visual Science Volume 8 Number 1 Photopsia post flu: A case of MEWDS S Baisakhiya, S Dulani, S Lele Citation S Baisakhiya, S Dulani, S Lele. Photopsia
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? WHAT CAUSES DIABETIC RETINOPATHY? WHAT ARE THE STAGES OF DIABETIC RETINOPATHY?
 Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Diabetic Retinopathy WHAT IS DIABETIC RETINOPATHY? Diabetic retinopathy affects 8 million Americans with diabetes. A leading cause of blindness in American adults, it is caused by damage to the small blood
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD
 Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
Interferon-Associated Retinopathy: Communicating with Internal Medicine Ari Wes, Esther S. Hong, MD, and Thomas A. Oetting, MS, MD July 26, 2010 Chief Complaint: New floaters in both eyes. History of Present
OCT Assessment of the Vitreoretinal Relationship in CSME
 December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
December 2007 Sonia Rani John et al. - IFIS 375 ORIGINAL ARTICLE OCT Assessment of the Vitreoretinal Relationship in CSME Dr. Manoj S. DNB FRCS, Dr. Unnikrishnan Nair MS DO FRCS, Dr. Gargi Sathish MS Introduction
Five Things You re Missing with Your Fundus Camera
 ebook Five Things You re Missing with Your Fundus Camera By Donald J. Siegel, OD, Sun City West Eye Care Sponsored by: Before I began incorporating EIDON true-color imaging into my practice, my retinal
ebook Five Things You re Missing with Your Fundus Camera By Donald J. Siegel, OD, Sun City West Eye Care Sponsored by: Before I began incorporating EIDON true-color imaging into my practice, my retinal
Introduction How the eye works
 1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
1 Introduction Diabetic retinopathy is a condition that can cause permanent loss of eyesight and even blindness. It is a major cause of loss of vision. But if a person with diabetes receives proper eye
Diabetic retinopathy damage to the blood vessels in the retina. Cataract clouding of the eye s lens. Cataracts develop at an earlier age in people
 Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Diabetic Retinopathy What is diabetic eye disease? Diabetic eye disease refers to a group of eye problems that people with diabetes may face as a complication of diabetes. All can cause severe vision loss
Photocoagulation of disciform macular lesions
 British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
British Journal of Ophthalmology, 1979, 63, 669-673 Photocoagulation of disciform macular lesions with krypton laser A. C. BIRD AND R. H. B. GREY From the Institute of Ophthalmology, Moorfields Eye Hospital,
GENERAL INFORMATION DIABETIC EYE DISEASE
 GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
GENERAL INFORMATION DIABETIC EYE DISEASE WHAT IS DIABETIC EYE DISEASE? Diabetic eye disease is a term used to describe the common eye complications seen in people with diabetes. It includes: Diabetic retinopathy
Vascular Disease Ocular Manifestations of Systemic Hypertension
 Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
Vascular Disease Ocular Manifestations of Systemic Hypertension Maynard L. Pohl, OD, FAAO Pacific Cataract & Laser Institute 10500 NE 8 th Street, Suite 1650 Bellevue, WA 98004 USA 425-462-7664 Cerebrovascular
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
Retinal Tears and Detachments
 Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
Retinal Tears and Detachments Understanding Retinal Problems When your eyes are working well, it s easy to take them for granted. But a tear or detachment of your eye s retina (the light-sensing lining
Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion
 European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
European Journal of Ophthalmology / Vol. 13 no. 7, 2003 / pp. 648-652 Diabetes mellitus: A risk factor affecting visual outcome in branch retinal vein occlusion J. SWART 1,2, J.W. REICHERT-THOEN 1, M.S.
VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT
 The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
The Professional Medical Journal DOI: 10.17957/TPMJ/16.2856 ORIGINAL PROF-2856 VISUAL OUTCOME IN DIABETIC MACULAR EDEMA AFTER GRID LASER TREATMENT 1. MBBS.FCPS Assistant Professor Ophthalmology Independent
Intro to Glaucoma/2006
 Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
Intro to Glaucoma/2006 Managing Patients with Glaucoma is Exciting Interesting Challenging But can often be frustrating! Clinical Challenges To identify patients with risk factors for possible glaucoma.
NEPTUNE RED BANK BRICK
 NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
NEPTUNE RED BANK BRICK Diabetes & The Eye Diabetics are more likely to develop Cataracts at a younger age. Diabetics are twice as likely to develop Glaucoma when compared to non-diabetics. The primary
Diabetic Management beyond traditional risk factors and LDL-C control: Can we improve macro and microvascular risks?
 Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Local Intra-arterial Fibrinolysis in Treatment of Incomplete Ophthalmic Artery Occlusion A Case Report
 CASE REPORT Local Intra-arterial Fibrinolysis in Treatment of Incomplete Ophthalmic Artery Occlusion A Case Report Shih-Ting Fang, Pao-Sheng Yen 1, Chien-Chung Chen, Yuan-Chieh Lee Department of Ophthalmology,
CASE REPORT Local Intra-arterial Fibrinolysis in Treatment of Incomplete Ophthalmic Artery Occlusion A Case Report Shih-Ting Fang, Pao-Sheng Yen 1, Chien-Chung Chen, Yuan-Chieh Lee Department of Ophthalmology,
optic disc neovascularisation
 British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
British Journal of Ophthalmology, 1979, 63, 412-417 A comparative study of argon laser and krypton laser in the treatment of diabetic optic disc neovascularisation W. E. SCHULENBURG, A. M. HAMILTON, AND
Retinal Detachment PATIENT EDUCATION
 Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
Retinal Detachment PATIENT EDUCATION What is Retinal Detachment (RD)? Retina is the light-sensitive layer at the back of the eye that converts light images into nerve impulses that are relayed to the brain
World Sight Day Case Studies. Mark Frost Screening Manager South East London DESP
 World Sight Day 2015 Case Studies Mark Frost Screening Manager South East London DESP Introduction All of the following cases have been identified in our screening programme over the last 3 years. The
World Sight Day 2015 Case Studies Mark Frost Screening Manager South East London DESP Introduction All of the following cases have been identified in our screening programme over the last 3 years. The
Understanding Diabetic Retinopathy
 Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Understanding Diabetic Retinopathy What Is Diabetic Retinopathy? Diabetes damages blood vessels in the rear of the eye. This condition is called diabetic retinopathy. It can lead to vision loss or blindness.
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema. Jonathan A. Micieli, MD Valérie Biousse, MD
 Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Non-arteritic anterior ischemic optic neuropathy (NAION) with segmental optic disc edema Jonathan A. Micieli, MD Valérie Biousse, MD A 75 year old white woman lost vision in the inferior part of her visual
Retinal Detachments
 Retinal Detachments What is a retinal detachment? The retina is the light sensitive layer covering the inside of the back of the eye. It is analogous to the film in a camera. The retina has many layers.
Retinal Detachments What is a retinal detachment? The retina is the light sensitive layer covering the inside of the back of the eye. It is analogous to the film in a camera. The retina has many layers.
Progressive Symptomatic Retinal Detachment Complicating Retinoschisis. Initial Reporting Questionnaire
 Progressive Symptomatic Retinal Detachment Complicating Retinoschisis In association with the British Ophthalmological Surveillance Unit Ethics ref: 13/NW/0037 Initial Reporting Questionnaire Case Definition:
Progressive Symptomatic Retinal Detachment Complicating Retinoschisis In association with the British Ophthalmological Surveillance Unit Ethics ref: 13/NW/0037 Initial Reporting Questionnaire Case Definition:
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Can intravitreal tissue plasminogen activator and SF6 gas facilitate management of macular degeneration with photodynamic therapy?
 European Journal of Ophthalmology / Vol. 18 no. 4, 2008 / pp. 591-594 Can intravitreal tissue plasminogen activator and SF6 gas facilitate management of macular degeneration with photodynamic therapy?
European Journal of Ophthalmology / Vol. 18 no. 4, 2008 / pp. 591-594 Can intravitreal tissue plasminogen activator and SF6 gas facilitate management of macular degeneration with photodynamic therapy?
Photodisruptive Nd:YAG laser in the management of premacular subhyaloid hemorrhage
 European Journal of Ophthalmology / Vol. 11 no. 3, 2000 / pp. 281-286 Photodisruptive Nd:YAG laser in the management of premacular subhyaloid hemorrhage S. ÇELEBI, A.S. KÜKNER Department of Ophthalmology,
European Journal of Ophthalmology / Vol. 11 no. 3, 2000 / pp. 281-286 Photodisruptive Nd:YAG laser in the management of premacular subhyaloid hemorrhage S. ÇELEBI, A.S. KÜKNER Department of Ophthalmology,
Fundus Autofluorescence. Jonathan A. Micieli, MD Valérie Biousse, MD
 Fundus Autofluorescence Jonathan A. Micieli, MD Valérie Biousse, MD The retinal pigment epithelium (RPE) has many important functions including phagocytosis of the photoreceptor outer segments Cone Rod
Fundus Autofluorescence Jonathan A. Micieli, MD Valérie Biousse, MD The retinal pigment epithelium (RPE) has many important functions including phagocytosis of the photoreceptor outer segments Cone Rod
Brampton Hurontario Street Brampton, ON L6Y 0P6
 Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Diabetic Retinopathy What is Diabetic Retinopathy Diabetic retinopathy is one of the leading causes of blindness world-wide. Diabetes damages blood vessels in many organs of the body including the eyes.
Case Follow Up. Sepi Jooniani PGY-1
 Case Follow Up Sepi Jooniani PGY-1 Triage 54 year old M Pt presents to prelim states noticed today he had reddness to eyes, states worse in R eye. Pt denies any pain or itching. No further complaints.
Case Follow Up Sepi Jooniani PGY-1 Triage 54 year old M Pt presents to prelim states noticed today he had reddness to eyes, states worse in R eye. Pt denies any pain or itching. No further complaints.
Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and
 British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
British Journal of Ophthalmology, 1977, 61, 278-284 Preliminary report on effect of retinal panphotocoagulation on rubeosis iridis and neovascular glaucoma LEILA LAATIKAINEN From Moorfields Eye Hospital,
Cilioretinal collateral circulation after occlusion of the central retinal artery
 British Journal of Ophthalmology, 1985, 69, 805-809 Cilioretinal collateral circulation after occlusion of the central retinal artery MICHAEL F MARMOR,' LEE M JAMPOL,2 AND LISA WOHL2 From the 'Division
British Journal of Ophthalmology, 1985, 69, 805-809 Cilioretinal collateral circulation after occlusion of the central retinal artery MICHAEL F MARMOR,' LEE M JAMPOL,2 AND LISA WOHL2 From the 'Division
What Is O.C.T. and Why Should I Give A Rip? OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist 5/19/2014
 OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
OCT & Me How Optical Coherence Tomography Changed the Life of a Small Town Optometrist Email: myoder@wcoil.com Mark A. Yoder, O.D. 107 N. Main Street PO Box 123 Bluffton, OH 45817 @yoderod 115.02 Histoplasma
New vessel formation in retinal branch vein occlusion
 Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
Brit. 7. Ophthal. (I 976) 6o, 8io New vessel formation in retinal branch vein occlusion JOHN S. SHILLING AND EVA M. KOHNER From the Retinal Diagnostic Unit, Moorfields Eye Hospital, London Neovascularization
LECTURE # 7 EYECARE REVIEW: PART III
 LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
LECTURE # 7 EYECARE REVIEW: PART III HOW TO TRIAGE EYE EMERGENCIES STEVE BUTZON, O.D. EYECARE REVIEW: HOW TO TRIAGE EYE EMERGENCIES FOR PRIMARY CARE PHYSICIANS Steve Butzon, O.D. Member Director IDOC President
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION
 THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
THE ROLE OF anti-vegf IN DIABETIC RETINOPATHY AND AGE RELATED MACULAR DEGENERATION MOESTIDJAB DEPARTMENT OF OPHTHALMOLOGY SCHOOL OF MEDICINE AIRLANGGA UNIVERSITY DR SOETOMO HOSPITAL SURABAYA INTRODUCTION
Disease-Specific Fluorescein Angiography
 Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Ruth E. Picchiottino, CRA Disease-Specific Fluorescein Angiography 15 Disease-Specific Fluorescein Angiography Recommendations for tailoring retinal fluorescein angiography to diabetic retinopathy, macular
Patient AB. Born in 1961 PED
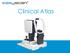 Clinical Atlas Patient AB Born in 1961 PED Autofluorescence Dilated 45 EasyScan Zero-dilation IR 45 Fundus Dilated 45 In the fundus photos (Canon CX1) the PED is not able to be seen. However, the extent
Clinical Atlas Patient AB Born in 1961 PED Autofluorescence Dilated 45 EasyScan Zero-dilation IR 45 Fundus Dilated 45 In the fundus photos (Canon CX1) the PED is not able to be seen. However, the extent
Retinal Tear and Detachment
 Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Retinal Tear and Detachment Introduction The retina is the layer of tissue in the back of the eye that is responsible for vision. It is attached to the choroid tissue, which supplies the retina with blood.
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient
 Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
Eyes on Diabetics: How to Avoid Blindness in Diabetic Patient Rova Virgana FK Unpad Pusat Mata Nasional RS Mata Cicendo Bandung Eye Center (Hospital and Clinic) PIT IDI Jabar 2018 Keys Facts from WHO
연령연관황반변성에서망막혈관종성증식과동반된망막색소상피박리의임상양상과일차적인광역학치료의결과
 연령연관황반변성에서망막혈관종성증식과동반된망막색소상피박리의임상양상과일차적인광역학치료의결과 40 Table. Clinical characteristics and results of patients undergoing photodynamic therapy for retinal angiomatous proliferation Patients No. Age/ sex Eye
연령연관황반변성에서망막혈관종성증식과동반된망막색소상피박리의임상양상과일차적인광역학치료의결과 40 Table. Clinical characteristics and results of patients undergoing photodynamic therapy for retinal angiomatous proliferation Patients No. Age/ sex Eye
For details on measurement and recording of visual acuity, refer to Annex 1. VISION INTERPRETING RESULTS ABSTRACT
 management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
management update on functional decline in older adults 2012 Unit No. 5 VISION Dr Au Eong Kah Guan, Ms Yulianti, Ms Fifiana ABSTRACT Among Singaporean adults of Chinese origin aged 40 to 79 years old,
EFFICACY OF ANTI-VASCULAR ENDOTHELIAL GROWTH FACTOR AGENTS IN RETINAL DISORDER FOR BETTER VISUAL ACUITY
 EFFICACY OF ANTI-VASCULAR ENDOTHELIAL GROWTH FACTOR AGENTS IN RETINAL DISORDER FOR BETTER VISUAL ACUITY Diwakar chaudhary *1, 2, Hu shuqiong, Long Yuan and Xiong kun 1 Yangtze University, 1 Nanhuan Road
EFFICACY OF ANTI-VASCULAR ENDOTHELIAL GROWTH FACTOR AGENTS IN RETINAL DISORDER FOR BETTER VISUAL ACUITY Diwakar chaudhary *1, 2, Hu shuqiong, Long Yuan and Xiong kun 1 Yangtze University, 1 Nanhuan Road
Age-Related Macular Degeneration
 Age-Related Macular Degeneration Age-Related Macular Degeneration Age-related macular degeneration (AMD) is one of the most common causes of poor vision after age 60. AMD is a deterioration or breakdown
Age-Related Macular Degeneration Age-Related Macular Degeneration Age-related macular degeneration (AMD) is one of the most common causes of poor vision after age 60. AMD is a deterioration or breakdown
Spontaneous Large Serous Retinal Pigment Epithelial Tear
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Optical Coherence Tomography: Pearls for the Anterior Segment Surgeon Basic Science Michael Stewart, M.D.
 Optical Coherence Tomography: Pearls for the Anterior Segment Surgeon Basic Science Michael Stewart, M.D. Disclosure OCT Optical Coherence Tomography No relevant financial relationships I will refer to
Optical Coherence Tomography: Pearls for the Anterior Segment Surgeon Basic Science Michael Stewart, M.D. Disclosure OCT Optical Coherence Tomography No relevant financial relationships I will refer to
Choroidal Neovascularization in Sympathetic Ophthalmia
 Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
Choroidal Neovascularization in Sympathetic Ophthalmia Lucia Sobrin, Miguel Cordero Coma, C. Stephen Foster Case Report A 49-year-old man presented after a ruptured globe repair of his left eye status
chorioretinal atrophy
 British Journal of Ophthalmology, 1987, 71, 757-761 Retinal microangiopathy in pigmented paravenous chorioretinal atrophy SURESH R LIMAYE AND MUNEERA A MAHMOOD From the Ophthalmology Service, DC General
British Journal of Ophthalmology, 1987, 71, 757-761 Retinal microangiopathy in pigmented paravenous chorioretinal atrophy SURESH R LIMAYE AND MUNEERA A MAHMOOD From the Ophthalmology Service, DC General
CHAPTER 13 CLINICAL CASES INTRODUCTION
 2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
2 CHAPTER 3 CLINICAL CASES INTRODUCTION The previous chapters of this book have systematically presented various aspects of visual field testing and is now put into a clinical context. In this chapter,
Leo Semes, OD, FAAO UAB Optometry
 Leo Semes, OD, FAAO UAB Optometry Safe; inert Has long track record - over 45 years Mixes with plasma and highlights blood vessel compromise Using specific exciting (490 nm)and absorption (510 nm) filters
Leo Semes, OD, FAAO UAB Optometry Safe; inert Has long track record - over 45 years Mixes with plasma and highlights blood vessel compromise Using specific exciting (490 nm)and absorption (510 nm) filters
