Quantitative diffusion MRI of hippocampus as a surrogate marker for post-traumatic epileptogenesis
|
|
|
- Clare Hampton
- 5 years ago
- Views:
Transcription
1 doi: /brain/awm268 Brain (2007), 130,3155^3168 Quantitative diffusion MRI of hippocampus as a surrogate marker for post-traumatic epileptogenesis Irina Kharatishvili, 1 Riikka Immonen, 2 Olli Gro«hn 2 and Asla Pitka«nen 1,3 1 Epilepsy Research Group, 2 Biomedical NMR Research Group, Department of Neurobiology, A.I. Virtanen Institute for Molecular Sciences and 3 Department of Neuroscience and Neurology, University of Kuopio, FIN Kuopio, Finland Correspondence to: Dr Asla Pitka«nen, A.I. Virtanen Institute for Molecular Sciences, University of Kuopio, PO Box 1627, FIN , Kuopio, Finland. asla.pitkanen@uku.fi The need to use animal models to develop imaging markers that could be linked to electrophysiological abnormalities in epilepsy and able to predict epileptogenicity in human studies is widely acknowledged. This study aimed to investigate the value of early magnetic resonance imaging (MRI) in predicting the long-term increased seizure susceptibility in the clinically relevant model of post-traumatic epilepsy (PTE). Moderate traumatic brain injury (TBI) was induced by lateral fluid-percussion in two groups of adult rats (34 injured, 16 controls). In Experiment 1, MRI follow-up was performed using a 4.7 T magnet at 3 h, 3 days, 9 days, 23 days, 2 months, 3 months and 6 months after TBI. T2 and 1/3 of the trace of the diffusion tensor (D av ) were quantified from a single slice using a fast spin-echo sequence. In Experiment 2, MRI was performed at 7 and 11 months post-injury. In both groups, seizure susceptibility was tested by injecting a single dose of pentylenetetrazol at 12 months post-injury. Electrographic and behavioural responses were monitored for 1h. Total number of spikes, total number of epileptiform discharges (EDs) and latency to first spike were measured. Finally, the severity of mossy fibre sprouting was evaluated. In both experiments, EEG parameters such as total number of spikes or EDs proved to be reliable indicators of increased seizure susceptibility in injured animals when compared to controls (P _ 0.05). In the hippocampus ipsilateral to TBI, D av correlated with these EEG parameters at both early (3 h), and chronic (23 days, 2, 3, 6, 7 and 11 months) time points after TBI, as well as withthedensityofmossyfibresprouting.theseresultsforthefirsttimedemonstratethatquantitativediffusion MRI can serve as a tool to facilitate prediction of increased seizure susceptibility in a clinically relevant model of human PTE. Keywords: traumatic brain injury; magnetic resonance imaging; surrogate marker; post-traumatic epilepsy; video-eeg monitoring Abbreviations: MRI = magnetic resonance imaging; PTE = post-traumatic epilepsy; TBI = traumatic brain injury; FPBI = fluid-percussion brain injury Received July 3, Revised September 24, Accepted October 16, 2007 Introduction Epilepsy is a major source of morbidity after TBI, which can complicate up to 50% of cases of severe head injury and % of cases of mild to moderate injury (Salazar et al., 1985; Asikainen et al., 1999; Frey, 2003). Posttraumatic epilepsy (PTE) is the most common cause of new-onset epilepsy in young people (Annegers, 1996) and the cause of epilepsy in 5% of patients referred to specialized epilepsy centres (Annegers et al., 1980; Hauser et al., 1991; Semah et al., 1998). PTE is often refractory to medical treatment (Herman, 2002). Attempts have been made to develop prophylactic antiepileptogenic therapy, but none have been successful so far (Temkin et al., 1990; Schierhout and Roberts, 1998; Haltiner et al., 1999; Temkin et al., 1999). It is now generally acknowledged that in the process of continuing the search for treatments that could prevent epileptogenesis after TBI, it is important to identify and characterize potential surrogate markers of epileptogenesis and epilepsy. That is, indices that can be objectively measured and evaluated as indicators of evolving pathogenic processes (Curing Epilepsy 2000, Benchmarks for Epilepsy Research, research/epilepsyweb/benchmarks.htm). Magnetic resonance imaging (MRI) has become the imaging method of choice for identifying the structural basis of seizure disorders (Duncan, 1997, 2002). ß The Author (2007). Published by Oxford University Press on behalf ofthe Guarantors of Brain. Allrights reserved. For Permissions, please journals.permissions@oxfordjournals.org
2 3156 Brain (2007),130, 3155^3168 I. Kharatishvili et al. Quantitative MRI procedures have been used successfully to characterize the structural abnormalities associated with head injury (Assaf et al., 1997; Wieshmann et al., 1999b; Rugg-Gunn et al., 2001a) and post-traumatic epilepsy (Wieshmann et al., 1999a; Gupta et al., 2005). Nevertheless, currently there is little information regarding potential correlations of quantitative MRI changes with histological and neurological outcomes after TBI. The purpose of this study was to investigate the utility of quantitative diffusion MRI as a potential marker of secondary cerebral damage leading to seizures in PTE. We used longitudinal/serial MRI measurements during evolving epileptogenesis in a well-established model of closed head injury, in which 50% of animals develop epilepsy with structural and functional changes closely resembling those of human PTE (Kharatishvili et al., 2006). We studied the association between quantitative diffusion MRI measures obtained at various time points after the lateral fluidpercussion brain injury (FPBI) and the EEG indicators of long-lasting susceptibility to seizures after FPBI. We also studied the association of MRI and EEG changes with mossy fibre synaptic reorganization that is a common histological finding in surgically treated patients with TLE, and thus, a marker for hyperexcitable hippocampus. Material and Methods Study design The study design is summarized in Fig. 1 and consisted of two independent experiments. In Experiment 1, 14 animals subjected to lateral FPBI and 6 controls underwent MRI investigation at 3 h, 3 days, 9 days, 23 days, 2 months, 3 months and 6 months after the brain injury. In Experiment 2, 20 animals with lateral FPBI and 10 controls were imaged at 7 and 11 months after the brain injury to rule out the influence of repetitive imaging under anaesthesia on the natural course of post-traumatic epileptogenesis. Eleven months post-injury in both the experiments, animals were implanted with cortical electrodes and underwent continuous Fig. 1 Study design. Quantitative MRI framework after lateral FPBI in two independent experiments (Experiment 1 and Experiment 2). The study duration is 12 months. Each black rectangle represents one imaging session. In both experiments, at 11 months post-injury animals underwent electrode implantation procedure for video- EEG monitoring; at 12 months post-injury the pentylenetetrazol test was performed. Finally, all animals were sacrificed for histology. Abbreviations: FPBI, fluid-percussion brain injury; MRI, magnetic resonance imaging; mo, months; PTZ, pentylenetetrazol test. 3-week video-eeg monitoring. Twelve months post-injury animals were subjected to the pentylenetetrazol (PTZ) test and afterwards sacrificed for histology. Animals Adult male Harlan Sprague-Dawley rats (50 injured, 16 controls, g; Harlan Netherlands B.V., Horst, the Netherlands) were used for the study. The animals were housed in individual cages and kept under controlled laboratory conditions (light regime of 12 h light/12 h dark, light on at 07:00 a.m.; temperature, 22 1 C; air humidity, 50 60%, ad libitum access to food and water). All animal procedures were approved by the Committee for the Welfare of Laboratory Animals of the University of Kuopio and the Provincial Government of Kuopio, and conducted in accordance with the guidelines set by the European Community Council Directives 86/609/EEC. Lateral fluid-percussion brain injury TBI was induced by lateral FPBI as originally described (McIntosh et al., 1989; Kharatishvili et al., 2006). Briefly, following anaesthesia, the head of the animal was mounted in a Kopf stereotactic frame (David Kopf Instruments, Tujunga, CA). A midline scalp incision was made and the underlying periosteum dissected. The scalp and left temporal muscle were reflected, exposing the skull and a 5 mm circular craniectomy was performed with a trephine over the left parietal lobe midway between lambda and bregma, with the lateral edge of craniectomy adjacent to the left lateral ridge. A modified Luer Lock cap was cemented over the craniectomy and filled with saline. At 90 min after administration of anaesthesia, animals were connected to the fluid-percussion device (AmScien Instruments, Richmond, VA, USA) through the male Luer Lock fitting and brain injury of atm severity was induced as originally described by McIntosh et al. (1989). Control animals received anaesthesia and all surgical procedures without FPBI injury. MRI MRI data were acquired using a 4.7 T Magnex magnet interfaced to a Varian UNITY INOVA console (Varian Inc., Palo Alto, CA, USA). A quadrature half-volume radio frequency coil with two 1.8 cm loops (HF Imaging LLC, Minneapolis, MN, USA) was used as transmitter and receiver. Rats were anaesthetized with 1% halothane in N 2 O/O 2 (70%/30%). Animals were positioned in the MRI compatible stereotactic holder and the head was securely fixed using ear bars and a nose bar to prevent any movement artefacts. Warm water ( C) was circulated in a heating element to control the temperature of the animals. MRI was performed 3 h, 3 days, 9 days, 23 days, 2 months, 3 months and 6 months after FPBI in Experiment 1, and at 7 months and 11 months in Experiment 2. Volumetric changes were detected using a T2-weighted spin-echo multi-slice sequence with adiabatic refocusing RF pulses to minimize the influence of a moderately inhomogeneous B1 field (echo time 70 ms, repetition time 3 s, field of view of mm 2 covered with data points, slice thickness 0.75 mm, 19 consecutive slices covering rat cerebrum). T2 and 1/3 of the trace of diffusion tensor (D av ) were quantified from a single slice using a magnetization-prepared fast spin-echo sequence with adiabatic BIR-4 refocusing pulses
3 D av as a marker for post-traumatic epileptogenesis Brain (2007), 130, 3155 ^ (repetition time 3.0 s, 16 echoes/excitation, centre-out k-space filling, echo spacing 10 ms, field of view of mm 2 covered with data points, slice thickness 1.5 mm). T2 relaxation time was measured using a spin-echo preparation block consisting of an adiabatic half passage (AHP), two hyperbolic secant (HS) adiabatic full passages, reverse AHP and crusher gradient in front of the fast spin-echo sequence (echo times 20, 38, 52, 76 ms). One-third of the trace of the diffusion tensor was quantified using the same pulse sequence with a diffusion sensitizing gradient pair positioned around each refocusing RF pulse in the magnetization preparation block. Three images with different degrees of diffusion weighting (b = 90, 496, 1014 s/mm 2, diffusion time = 29 ms) were obtained in three different orthogonal orientations. Quantitative relaxation and diffusion maps were calculated by fitting the data to standard single exponential formulae in Matlab. Seven regions of interest (ROI) were manually outlined in T2-weighted images and transferred to T2 maps and diffusion maps as follows: the parietal cortex (excluding the lesion area) bilaterally, the hippocampus bilaterally, the lesion area and the lateral ventricles (Fig. 2). Electrode implantation and video-eeg monitoring Eleven months after the TBI, animals in Experiments 1 and 2 were anaesthetized with a single intraperitoneal (i.p.) injection (6 ml/kg) Fig. 2 Images from a representative animal that developed hyperexcitability after FPBI. (A) A T2-weighted MR image used as an anatomic map to outline the regions of interest. Open arrow indicates the location of the cortical FPBI at 7 months post-injury. (B) Diffusion map from the corresponding level in the same rat. (C) Coronal thionin-stained section from the same rat at the level of MRI slice. Open arrow points to the cortical lesion. Note also the thalamic hemiatrophy on the side of the lesion. (D) Timm-stained section from the level corresponding to MRI analysis. Note mossy fibre sprouting in the inner molecular layer (arrows) of the dentate gyrus. (E) Absolute D av and T2 maps from a representative animal during the 6 months follow-up. Because the half-volume radio frequency coil was used, ventral parts of the brain show lower signal-to-noise ratio. Abbreviations: H, hilus; HC, hippocampus; i, inner molecular layer; m, mid molecular layer, o, outer molecular layer; PCx, parietal cortex; V, lateral ventricle; scale bars: panel C, 1mm; panel D 100 mm. Grayscale bar units 10 3 mm 2 s 1.
4 3158 Brain (2007),130, 3155^3168 I. Kharatishvili et al. mixture containing sodium pentobarbital (58 mg/kg), chloral hydrate (60 mg/kg), magnesium sulphate (127.2 mg/kg), propylene glycol (42.8%) and absolute ethanol (11.6%). Animals were then mounted in a stereotactic frame (lambda and bregma on the same horizontal level). Two cortical screw electrodes (E363/20 Plastics One Inc., Roanoke, VA, USA) were placed over the parietal cortex, one rostral to the craniectomy, and the other contralateral to the centre of the craniectomy. The electrode implantation paradigm in the present study was based on the results from our previous experiments (Kharatishvili et al., 2006). According to the data from long-term (12 months) video-eeg monitoring in rats with chronic spontaneous seizures, epileptiform activity detected by the depth electrode located in the ventral hippocampus ipsilateral to injury invariably rapidly propagated to the cortex, both ipsi- and contralateral to the lesion. We concluded consequently, that if any spontaneous epileptiform activity arises in the hippocampus it will be picked up by the cortical electrode as well. Therefore, the depth hippocampal electrode had not been implanted to avoid additional mortality in the brain-injured animals of this age due to breathing problems caused by prolonged anaesthesia. Two cortical screw electrodes were placed over the left and right frontal cortex and were used as supplementary electrodes if there was a problem in obtaining a good-quality signal from the parietal electrodes. Two stainless steel screw electrodes were inserted into the skull bilaterally over the cerebellum and served as indifferent and ground electrodes. All electrode pins were inserted into the plastic pedestal, and the entire assembly was cemented to the calvarium with dental acrylic. Details of the methodology of long-term video-eeg monitoring were described previously (Nissinen et al., 2000). Briefly, electrical brain activity was recorded with the Nervus EEG Recording System connected with a Nervus magnus 32/8 amplifier (Taugagreining, Iceland), and filtered (High-pass filter 0.3 Hz cutoff, low-pass 100 Hz). The behaviour of the animals was monitored using the WV-BP330/GE video camera (Panasonic) that was positioned above the cages and connected to a SVT-N72P time lapse VCR (Sony) and a PVM-145E video monitor (Sony). A wide-angle lens allowed simultaneous videotaping of eight animals. Rats were first continuously video-eeg monitored for 3 weeks to detect the occurrence of epileptiform activity: spontaneous seizures or spiking. The spike was defined as paroxysmal potential (i.e. arising suddenly from the background), very sharp in contour, with the duration of ms, usually followed by a low-voltage slow potential (about 200 ms duration) before re-establishing the baseline. Thereafter, animals were subjected to PTZ test and monitored for 60 min following the injection. Pentylenetetrazol test To detect any enhanced seizure susceptibility in post-tbi rats, we used a single dose of PTZ to challenge rats 12 months after TBI and compared these with age-matched controls that received the same dose of PTZ. To determine whether seizure threshold was reduced after TBI, we selected a normally subconvulsant dose of PTZ based on earlier works showing that mg/kg of PTZ (intraperitoneal) is subconvulsant for adult male Sprague-Dawley rats (Golarai et al., 2001; Velisek, 2006). All tests were performed between 9.00 a.m. and 2.00 p.m. Pentylenetetrazol (1,5-pentamethylenetetrazole, 98%, Sigma-Aldrich YA-Kemia Oy, Finland) was dissolved in sterile 0.9% saline (12.5 mg/ml solution) and injected i.p. at a dose of 30 mg/kg of body weight in Experiment 1 and 25 mg/kg in Experiment 2. Each rat received a single injection of PTZ. Following the PTZ injection, rats were placed separately into transparent plexiglas cages ( cm 3 ) where they could move freely, and video-eeg was recorded from parietal electrodes for 60 min after PTZ administration. An electrographic seizure was defined as a 45 s duration high-amplitude rhythmic discharge with a clear onset, temporal evolution in wave morphology and amplitude, and offset. Electrographic interictal epileptiform discharge (ED) was defined as a high-amplitude rhythmic discharge containing a burst of slow waves, spike-wave and/or polyspike-wave components and lasting 55 s. A spike was defined as a high-amplitude (twice a baseline) sharply contoured waveform with a duration of ms. Latency to the first spike, total number of spikes and total number of epileptiform discharges were calculated during 60 min after PTZ administration. These parameters were chosen according to the unpublished results from our previous experiment (Kharatishvili et al., 2006). Spike counting did not include the electrographic seizure events. In addition to continuous video recording, behaviour was monitored by an observer. The time of the occurrence of epileptiform behavioural events was recorded and scored according to a modified Racine type scale (1 = twitching, freezing, 2 = myoclonic jerks of one forelimb; 3 = bilateral forelimb clonus; 4 = forelimb clonus with rearing; 5 = tonic clonic convulsion). Histology Fixation and processing of tissue The rats were perfused transcardially for histological analysis immediately after finishing the PTZ test. The animals were deeply anaesthetized and perfused according to the following fixation protocol: 0.37% sulphide solution (30 ml/min) for 10 min followed by 4% paraformaldehyde in 0.1 M phosphate buffer, ph 7.4 (30 ml/ min), 4 C, for 10 min. The brains were removed from the skull and post-fixed in buffered 4% paraformaldehyde for 4 h and then cryoprotected in a solution containing 20% glycerol in 0.02 M potassium phosphate-buffered saline (KPBS) for 24 h. The brains were then blocked, frozen in dry ice and stored at 70 C until cut. The brains were sectioned in the coronal plane (30 mm, 1-in-5 series) with a sliding microtome. The first series of sections were stored in formalin for thionin staining, for cytoarchitectonic characterization of various brain areas and localization of the lesion. The remaining series were stored in a cryoprotectant tissue-collecting solution (TCS, 30% ethylene glycol, 25% glycerol in 0.05 M sodium phosphate buffer) at 20 C until processed. Timm histochemistry Timm staining was used to visualize mossy fibre reorganization in the inner molecular layer of the dentate gyrus that accompanies epileptogenesis (Sutula et al., 1989; Cavazos et al., 1991). Mossy fibre sprouting was analysed from sections stained with the Timm sulphide/silver method (Sloviter, 1982; Nissinen et al., 2000). For staining, all coronal sections (30 mm, 1-in-5 series) where the hippocampus was present were mounted on gelatincoated slides and dried at 37 C. Staining was performed in the dark according to the following procedure: working solution that contained gum arabic (300 g/l), sodium citrate buffer (25.5 g/l citric acid monohydrate and 23.4 g/l sodium citrate),
5 D av as a marker for post-traumatic epileptogenesis Brain (2007), 130,3155^ hydroquinone (16.9 g/l) and silver nitrate (84.5 mg/l) were poured into the staining dish that contained the slides. The sections were developed until an appropriate staining intensity was attained (60 75 min). The slides were then rinsed in tap water for 30 min and placed in 5% solution of sodium thiosulfate for 12 min. Finally, sections were dehydrated through an ascending series of ethanol, cleared in xylene, and coverslipped with DePeX mounting medium (BDH, Laboratory Supplies, England). Mossy fibre sprouting was analysed along the septotemporal axis of the hippocampus. The septal end included the coronal sections between AP levels 2.3 and 6.0 mm posterior from bregma. The dorsal mid-portion and ventral mid-portion of the dentate gyrus included dorsal and ventral parts of the hippocampus where the granule cell layer of the septal and temporal ends becomes fused and forms an easily identifiable and standardized oval-shaped layer (AP level mm) posterior to bregma. The density of mossy fibre sprouting was scored according to Cavazos et al. (1991): Score 0 = no granules, Score 1 = sparse granules in the supragranular region and in the inner molecular layer, Score 2 = granules evenly distributed throughout the supragranular region and the inner molecular layer, Score 3 = almost a continuous band of granules in the supragranular region and inner molecular layer, Score 4 = continuous band of granules in the supragranular region and in the inner molecular layer, Score 5 = confluent and dense laminar band of granules that covers most of the inner molecular layer, in addition to the supragranular region. The scoring was performed by an observer that was blinded to the identity of the rat. Statistics All data were analysed using SPSS for Windows (version 14.0). The Mann Whitney U-test was used to assess differences between the two groups. The Spearman rank correlation coefficient was used as a non-parametric test to assess correlations between MRI data, EEG data and histological results. A P-value of was considered to be significant. Data are presented as mean SD. Results Injury severity and acute (_72 h) mortality In Experiment 1, the total animal number was 20. One animal died during the anaesthesia before induction of FPBI. From the remaining 19 animals, subjected to FPBI, 5 died within 72 h of the injury, so the final number of animals included in the analysis was 14. In Experiment 2, the total number of animals was 30. One animal died immediately after anaesthesia, one during the operation before induction of FPBI. From the remaining 28 animals, 6 died within 72 h after trauma. One animal died 7 days after the injury (intracranial bleeding), one was euthanized 26 days after the injury because of the severe weight-loss and weakness. The final number of animals included in the study was 20. Mortality during the first 72 h post-injury was used as a marker of injury severity (Thompson et al., 2005). In Experiment 1, the force of the applied pressure pulse in FPBI varied from 2.3 to 3.2 atm (mean 2.64 atm). The mortality rate was 25% (three animals died on the day of injury, two died within 72 h after FPBI). In Experiment 2, the force of the applied pressure pulse in FPBI was 3.0 to 3.1 atm (mean 2.86 atm). The mortality rate was 21% (four animals died on the day of injury, and two animals within 72 h after FPBI). Thus, in both experiments the severity of injury corresponded to moderate injury (McIntosh et al., 1989; Thompson et al., 2005; Dubreuil et al., 2006). Mortality values as well as MRI data on lesion size and progression proved that the injury was similar in both experiments. Mortality during the time course (`72 h post-injury) of the experiments In Experiment 1, three animals died during the imaging sessions at 3 days, 9 days and 6 months time points, likely reason of death halothane anaesthesia/overdose. One animal had to be euthanized on the third week after the injury because of the severe eye infection (probable cause the tattoo colour/rat number on the ear); this rat has had several spontaneous seizures within 2 weeks post-injury but was not included in the analysis. In Experiment 2, one animal was operated 10 months post-injury due to a large tumour in the jaw area, and died soon after the operation. After participating in the second MRI session, two animals with FPBI had to be euthanized due to the paresis of the intestine and severe weight-loss, two more animals were euthanized (did not recover from the anaesthesia during the electrode implantation) 11 months after the injury because of the tumours on the neck/ear and abdominal area, respectively. One control animal died after anaesthesia during the electrode implantation, another one lost the headset and had to be euthanized because of the strong bleeding from the wound. Video-EEG monitoring Eleven months post-injury animals were implanted with cortical electrodes and underwent continuous 3-week video-eeg monitoring. In both Experiments 1 and 2, video-eeg monitoring did not reveal spontaneous seizure activity in any of the experimental animals. This may relate to a low-seizure frequency in this model and the single video-eeg monitoring session at the end of the study which was probably not long enough for seizure detection (compare with Kharatishvili et al., 2006). Also, animals had milder TBI than in the previous study, thus lower expectancy of epilepsy. Epileptiform activity was, however, recorded in 80% of rats with FPBI in the form of isolated spikes (similar results in Experiments 1 and 2). In injured animals, spiking activity was registered by the cortical electrode placed over the parietal cortex on the side of the injury; in some cases bilateral spike discharges were registered over the parietal cortex with a spike of smaller amplitude on the contralateral side (propagation). No spiking activity was observed in any of the control animals during the 3 weeks of video-eeg monitoring.
6 3160 Brain (2007),130, 3155^3168 I. Kharatishvili et al. Analysis of post-traumatic seizure susceptibility using PTZ test The behavioural signs of seizure activity that typically occurred sequentially after the PTZ administration were as follows: (i) myoclonic twitch sudden, involuntary jerking of the whole body, (ii) clonic movements of forelimbs with preservation of the righting reflex and (iii) generalized clonic seizure with loss of righting reflex that corresponds to the observations previously published by Löscher et al. (1991). In the EEG, a single dose of PTZ induced electrographic epileptiform discharges (brief bursts of high amplitude slow waves, spikes and/or spike-and-wave episodes) in all animals of both injured and control groups. Brief (41 s) spike-wave and high-amplitude delta bursts corresponded to myoclonic twitches, while ictal epileptiform discharges of 45 s duration corresponded to clonic seizures. The general evolution of EEG record after the PTZ injection was as follows: (i) brief bursts of highamplitude slow waves, (ii) isolated spike-waves or burst of several spike-waves lasting 41 s, (iii) electrographic seizure. In Experiment 1, 6 MR-imaged controls and 10 out of 14 MR-imaged rats with FPBI survived 12 months and participated in the PTZ test. After a 30 mg/kg dose of PTZ injection, all animals survived for at least 60 min following the injection. One animal with FPBI lost a headset during a seizure induced by PTZ and was excluded from the EEG analysis. All rats with FPBI and four out of six controls experienced clonic convulsions (behavioural score 2 5). As summarized in Fig. 3, the total number of spikes during the 60-min follow-up was higher in injured animals (n = 9) as compared to controls (n = 6) (mean versus 40 32, P50.05). Also, the total number of epileptiform discharges was higher in injured animals as compared to controls (mean versus 32 26, P50.05). The latency to the first spike was shorter in injured animals as compared to controls (mean s versus s, P50.05) (Fig. 3). There was a negative correlation between latency to the first spike and the total number of spikes (r = 0.41, P50.05, n = 15). Similar to our previous experiment [animals included in the study by Kharatishvili et al. (2006), data not shown], no difference was found between the groups in the latency to the first behavioural symptom, latency to the (first) electrographic/ behavioural seizure or in electrographic/behavioural seizure duration and severity. In Experiment 2, 8 of 10 MR-imaged controls and 15 out of 20 MR-imaged rats with FPBI survived 12 months. All control animals and 14 injured (one rat with FPBI was excluded because of the extracranial haematoma attached to Fig. 3 Results of PTZ test are shown as bar graphs in panel A for Experiment 1 (30 mg/kg, i.p.), and in panel B for Experiment 2 (25 mg/ kg, i.p.). Parameters used to asses lowered seizure threshold in the PTZ test in controls and in rats with FPBI included the latency to the fist spike (A 1,B 1 ), number of spikes (A 2,B 2 ) and number of epileptiform discharges (A 3,B 3 ). Note that rats with FPBI had shorter latency to the first spike, increased number of spikes and increased number of epileptiform discharges indicating hyperexcitability. In animals with the lower dose (25 mg/kg) pentylenetetrazol, the seizure duration was shorter than in those animals which received 30 mg/kg dose (67 35 s versus s). The latency to the first electrographic seizure was substantially longer in Experiment 2 ( s versus s). Thus, the time-window for calculation of epileptiform activity was bigger in Experiment 2 compared to Experiment 1, which explains the higher number of counted spikes and EDs in Experiment 2. Abbreviations: FPBI, fluid-percussion brain injury; PTZ, pentylenetetrazol; s, second; Statistical significances: P50.05, P50.01, P between the control and FPBI groups (Mann^Whitney s U-test). Error bars show SD.
7 D av as a marker for post-traumatic epileptogenesis Brain (2007), 130, 3155 ^ the skull and suspicion of epidural haematoma in MR images) participated in the PTZ test. In this experiment, we reduced the dose of PTZ from 30 to 25 mg/kg to avoid a very rapid and robust response to PTZ which was seen in a majority of animals with TBI in Experiment 1. The wider range of convulsive response in injured animals also allowed us to better correlate the various outcome parameters of lowered seizure threshold with histological and MRI findings. After injecting 25 mg/kg of PTZ, all animals survived for at least 60 min. In both the FPBI and control groups, 50% of rats exhibited clonic convulsions (behavioural score 2 5). Two out of 14 animals with TBI developed status epilepticus and had a large amount of artefacts in EEG. In these animals, EEG analysis of the number of spikes and the number of EDs could not have been performed. As in Experiment 1, the total number of spikes during the 60-min follow up was higher in injured animals (n = 12) as compared to controls (n = 8) (mean versus 34 60, P50.05). Also, the total number of epileptiform discharges was higher in injured animals as compared to controls (mean versus 64 55, P50.05). The latency to the first spike was shorter in injured animals as compared to controls (mean s versus s, P50.05) (Fig. 3). There was no difference between the groups in latency to the first behavioural symptom, latency to the electrographic/behavioural seizure and electrographic/behavioural seizure duration and severity. The PTZ test results showed that a substantial proportion of the rats had developed a lowered seizure threshold and, hence, were likely undergoing epileptogenesis at the moment of PTZ test (Figs 3 and 4). MR imaging The aim of the present study was to investigate the association between the severity of MRI changes during the course of epileptogenesis with seizure susceptibility that develops later on. Unlike expected, the cortical damage did not associate with the lowered seizure threshold. However, in the hippocampus ipsilateral to the injury, from two parameters measured (D av, T2), the abnormality of D av was consistently associated with the lowered seizure threshold, and therefore, the most of the description of imaging part of the study is focused on D av in the hippocampus as a predictor of increased epileptogenicity. Data are summarized in Fig. 5. Severity and progression of the cortical lesion In the cortex ipsilateral to injury, there was a progressive increase in T2 values in FPBI animals compared to controls at all time points (P50.05). However, we observed a substantial variation in injured animals in T2 values from 9 days time point onwards which can be explained by interanimal variability in lesion progression, but also, by the problems we had experienced in drawing the ROI Fig. 4 Representative EEG traces from three animals recorded simultaneously 10 min after the pentylenetetrazol injection (PTZ 25 mg/kg). Electrodes were located over the parietal cortex ipsilateral (upper trace) and contralateral (lower trace) to injury. (A) EEG from the animal with D av drop (42 SD from control mean) in the hippocampus ipsilateral to trauma at 3 h post-injury. (B)EEG from the animal with milder D av drop (52 SD from control mean) at 3 h time point. (C) EEG from control animal. Note the increased number of spikes in the animal with severe D av drop. Both animals with FPBI developed a generalized seizure as a response to PTZ later on. Control animal had spikes and epileptiform discharges but did not develop a seizure. Fig. 5 The time course of post-injury changes in MRI parameters in the hippocampus ipsilateral to trauma in animals with FPBI and controls.data are presented from the two differentexperiments. (A)T2 relaxation time. Note that there was a trend int2 increase in Experiment1, but significant elevation was found only at a very chronic stage (7 and11months in Experiment 2). (B) D av.note the initial diffusion drop at 3 h, and the steady increase in D av over time, proposing progression of damage. Data are presented as mean SD. P50.05, P50.01, P50.001between the controland FPBI groups (Mann^Whitney s U-test). Abbreviations: FPBI, fluidpercussion brain injury; mo, months. Error bars show SD.
8 3162 Brain (2007),130, 3155^3168 I. Kharatishvili et al. accurately (identification of boundary between the lesioned cortex and enlarged ventricle). We did not find any association between the T2 values and indicators of lowered seizure threshold at any of the time points. T2 values from the contralateral parietal cortex remained stable within 3 h 6 months time window and no difference was found between the control and TBI groups. In the ipsilateral cortex, there was a trend towards D av increase in FPBI animals when compared to controls starting from day 9. This increase was significant only at 2 months time point when there was also an association between the D av and the number of epileptiform discharges at 12 months (r = 0.55; P50.05). In the contralateral cortex, D av showed a non-significant trend towards slight increase during ageing both in injured animals and controls. No difference was found between the groups at any time point. Severity and progression of the hippocampal lesion A significant elevation in the hippocampal T2 ipsilateral to injury was found only at chronic stage (7 and 11 months in Experiment 2; Fig. 5A). In Experiment 1, D av measures of the hippocampus ipsilateral to the lesion were significantly different from those of controls at most of the time points (Fig. 5). At the acute phase (3 h post-injury), 4 out of 14 injured animals showed a severe magnetic susceptibility artefact in MRI caused by a large extracranial blood clot, and were excluded from the analysis at that time point. Temporal evolution of D av changes showed the diffusion drop by mm 2 s 1 at 3 h after the injury, followed by a brief temporary increase in some of the animals, and a secondary drop within the control levels during 3 9 days post-injury. Elevation in D av was observed after day 9 and the increase became significant at 2 months after the FPBI (Fig. 5). D av in the ipsilateral hippocampus at 7 months in Experiment 2 was similar to that at 6 months in Experiment 1 ( mm 2 s 1 versus mm 2 s 1, respectively), suggesting the results were reproducible (Fig. 5). D av at 11 months ( mm 2 s 1 ) did not differ from that at 6 months in Experiment 1 either. Contralaterally, T2 values remained stable within 3 h 6 months time window and no difference was found between the control and TBI groups. Like in cortex, D av showed a non-significant trend towards increase during ageing both in injured animals and controls. No difference was found between the groups at any time point. Changes in ipsilateral hippocampal D av associate with increased seizure susceptibility Data are summarized in Fig. 6. In Experiment 1, the D av drop at 3 h correlated with the increase in the total number of spikes at 12 months (r = 0.61, P50.05, n = 14). At later Fig. 6 Correlation of D av with the EEG measures of increased seizure susceptibility. Scatterplots show the correlation between the number of spikes at 12 months and D av values in the hippocampus ipsilateral to the injury at 3 h (A,Experiment 1),7 months (B, Experiment 2) and 11 months (C, Experiment 2) after lateral FPBI. Closed circles refer to animals with FPBI and open circles to controls. Animals with D av values52sdor42sdofcontrolmean are shown in red colour. The solid line indicates the mean value in control animals. The dashed lines show the values that are the mean plus (B, C) orminus(a) 1 SD or 2 SD of the control mean. In A, note that 75% (three out of four) of animals with severe D av drop at 3 h post-injury (42 SD from control mean, red circles within grey rectangle) had increased spiking at 12 months after trauma. Similarly, 75% and 83% (six out of eight, and five out of six) of animals with increased D av values (42 SD from control mean) at 7 or 11 months (B and C, respectively) had increased spiking at 12 months. Abbreviations: n, number of animals; r, Spearman correlation coefficient. time points, D av increase at 23 days (r = 0.73, P50.01, n = 14), 2 months (r = 0.72, P50.01, n = 14), 3 months (r = 0.80, P50.001, n = 14) and at 6 months (r = 0.76, P50.01, n = 14) post-injury correlated with the increase in the total number of epileptiform discharges at 12 months. Similar associations between the D av increase and the hyperexcitability were obtained at more chronic time points
9 D av as a marker for post-traumatic epileptogenesis Brain (2007), 130, 3155 ^ in Experiment 2, in which D av increase at 7 months correlated with all three EEG parameters of the increased seizure susceptibility, including shortening in the latency to the first spike (r = 0.50, P50.05, n = 16), increase in the total number of spikes (r = 0.62, P50.05, n = 16) and increase in the total number of epileptiform discharges (r = 0.55, P50.05, n = 16). At 11 months post-injury, D av correlated with the shortening in the latency to the first spike (r = 0.60, P50.05, n = 14) and increase in the total number of spikes (r = 0.72, P50.01, n = 14). Next we subdivided all FPBI animals into a severe injury group (animals with D av values 52 SD from the control mean at 3 h) and a moderate injury group (the rest of the FPBI animals). We noticed that the D av in the severe group differed from controls at 23 days (P50.05), 2 months (P50.01), 3 months (P50.01) and 6 months (P50.01) post-injury. The severe group also had a higher number of spikes (P50.05, Fig. 6) and epileptiform discharges (P50.05) in the PTZ test at 12 months postinjury as compared to controls. Interestingly, no difference was found between moderate group and controls in any of the EEG indicators of the increased seizure susceptibility. Changes in ipsilateral hippocampal D av and increased seizure susceptibility associate with increased mossy fibre sprouting Injured animals had mossy fibre sprouting into the inner molecular layer of the dentate gyrus ipsilateral to the lesion as compared to controls in both Experiment 1 [mean sprouting score (range , median 1) versus controls (mean , range 0 0.5, median 0.15), (P50.01)] and Experiment 2 [ (range 1 3.5, median 2.2) versus (range 0 0.4, median 0.09) (P50.001)]. As summarized in Fig. 7, the severity of mossy fibre sprouting correlated positively with the EEG indicators of increased seizure susceptibility in both the experiments. Analysis of PTZ data from rats included in our previous experiment (Kharatishvili et al., 2006) indicated similar association between mossy fibre sprouting and seizure susceptibility in PTZ test in a population of rats, in which some of the animals had behaviourally and electrographically verified spontaneous seizures (data shown in Fig. 7C). Mossy fibre sprouting scores correlated with D av values at 3 h (r = 0.74, P50.01, n = 14), 2 months (r = 0.75, P50.01, n = 14), 3 months (r = 0.73, P50.01, n = 14), 6 months (r = 0.64, P50.05, n = 14), 7 months (r = 0.77, P50.001, n = 16) and 11 months (r = 0.49, P50.05, n = 16) after lateral FPBI. Fig. 7 Scatterplots show the correlation between the mossy fibre sprouting in the dentate gyrus ipsilateral to injury with total number of spikes in Experiments 1 (A) and 2(B). Closed circles refer to animals with FPBI and open circles to controls. The solid line indicates the mean value in control animals. The dashed lines show the values that are plus 1 SD or 2 SD of the control mean. In A, note that 75% (three out of four) of animals with increased mossy fibre sprouting (42 SD from control mean, closed circles within grey rectangle) had increased spiking at 12 months after trauma. Similarly, in B, 75%(six out of eight) of animals with increased mossy fibre sprouting (42 SD from control mean)had increased spiking at 12 months (C). Reanalysis of data from the previous experiment with severe TBI resulting in post-traumatic epilepsy (Kharatishvili et al., 2006). Correlation between the number of spikes and mossy fibre sprouting in injured animals with (two rats, grey circles) or without (nine rats, closed circles) electrographic spontaneous recurrent seizures. White circle refers to a control animal. Abbreviations: MFS, mossy fibre sprouting; n, number of animals; r, Spearman correlation coefficient. Discussion The present study describes the long-term MRI alterations in hippocampal T2 and D av in a model of human PTE. We hypothesized that acute and subchronic alterations in these parameters reflecting the severity of initial hippocampal impact and consequent brain pathology can serve as surrogate markers for the development of long-term hyperexcitability in post-traumatic brain. There were three
10 3164 Brain (2007),130, 3155^3168 I. Kharatishvili et al. major findings. First, from the two common clinical MRI parameters analysed, hippocampal D av showed more consistent differences between the control and injured brain than T2. Second, an early hippocampal diffusion drop at 3 h as well as a later diffusion increase observed first at 23 days post-injury were associated with the hyperexcitability at 12 months post-injury. Third, the changes in hippocampal D av associate with the severity of mossy fibre sprouting that is a common pathological finding in patients operated on due to drug-refractory PTE. The implications of the present finding for using hippocampal D av as a surrogate marker for post-traumatic epileptogenesis are discussed. Moderate TBI results in hyperexcitability at 11 months post-injury In the two independent experiments, we observed injuryinduced mortality in 21 25% of animals, consistent with previous reports inducing FPI of moderate severity (McIntosh et al., 1989; Saatman et al., 1997; Dubreuil et al., 2006). In humans, moderate head injury is usually defined by the following criteria: (i) Glasgow Coma Score (GCS) 9 12, (ii) post-traumatic amnesia up to 24 h, (iii) loss of consciousness from a few minutes to few hours, (iv) operative intracranial lesion, (v) abnormal imaging findings. The risk of developing epilepsy after moderate TBI is 0.7% within 1 year and 1.6% to 4.2% in 5 years (Annegers et al., 1980, 1998). Thus, the present experimental data are in line with clinical observations that risk of epilepsy after moderate injury is substantially lower than after severe injury that results in epilepsy in 50% of rats and up to 53% in humans (Salazar et al., 1985; Frey, 2003; Kharatishvili et al., 2006). In animals with FPBI, long-term video-eeg monitoring and quantification of chronic spontaneous seizures (i.e. severity of epilepsy) was not feasible in this study because of the interference of EEG with MRI measurements. In a single 3-week video-eeg recording at 11 months post-injury we did not observe any spontaneous seizures, but 80% of FPBI animals in both Experiments 1 and 2 had spiking, suggesting hyperexcitability. To further assess the presence of hyperexcitability as an index of increased epileptogenicity, we performed PTZ test under video-eeg control at 12 months after FPBI. Assessing the susceptibility to seizures induced by PTZ is a standard and widely used experimental model of clinical generalized seizures with both face and construct validity (Loscher et al., 1991). Systemic administration of the chemoconvulsant PTZ for induction of generalized clonic seizures in rodents is widely employed to identify potential anticonvulsants (Swinyard et al., 1989). PTZ test has been used to show lowered seizure threshold in many epileptogenic aetiologies, including genetically modified animals, and the PTZ seizure threshold has been shown to be lower in epileptic animals as compared to non-epileptic (Velisek, 2006). Although there was variability within each group that was comparable with the previously published work on PTZ in normal rats (Mason and Cooper, 1972; Golarai et al., 1992), we were able to observe lowered seizure threshold in injured animals as compared to controls in both Experiments 1 and 2. EEG parameters such as increase in total number of spikes and EDs as well as the shortened latency to the first spike in the injured rats proved to be reliable indicators of increased seizure susceptibility. The data obtained from the PTZ test confirmed our previous observations of consistently enhanced susceptibility to PTZ-induced convulsions at 12 months in animals with PTE after FPBI (Kharatishvili et al., 2006). Taken together, rats with lateral FPBI-induced moderate TBI develop lowered seizure threshold in chronic follow-up, which is in record with the data previously reported in a weight-drop animal model of impact head injury by Golarai and colleagues (Golarai et al., 2001). However, it is important to keep in mind that currently there are no long-term prospective studies that had directly addressed the question whether the lowered threshold for induced seizures triggered by PTZ reliably predicts the later development of spontaneous seizures, that is, the end product of the epileptogenic process. Finally, the pressure of fluid pulse within the range of atm applied to the brain did not correlate with the decrease in seizure threshold in the injured animals. Similarly, according to our previous data (Kharatishvili et al., 2006) no correlation was found between the development of spontaneous epileptic activity and pressure ( atm) of the fluid pulse applied. Therefore, it is the brain injury triggered by the impact rather than the impact force itself that is critical for alteration in seizure threshold and imaging parameters. Post-traumatic abnormalities in hippocampal water diffusion are progressive Diffusion MRI is a non-invasive technique allowing quantification of water diffusion due to thermal Brownian motion. We measured apparent average diffusion constant (D av ) = 1/3 of the trace of diffusion tensor which is an orientation-independent measure of water diffusion in the tissue. Previous studies on diffusion after TBI in humans have reported that diffusion MRI identifies the largest number of overall lesions as well as the largest volume of trauma-related signal abnormalities in diffuse axonal injury (DAI) compared with conventional MRI sequences that include T2-weighted fast spin-echo, fluid attenuated inversion recovery (FLAIR) and T2 -weighted gradient echo sequences (Huisman et al., 2003). The total volume of diffusion-weighted imaging (DWI) signal abnormalities encountered in DAI correlate better than other imaging variables with the acute GCS and the subacute Rankin scale score (Schaefer et al., 2004). Two animal studies showed a decreased diffusion within 1 h of injury of moderate severity
11 D av as a marker for post-traumatic epileptogenesis Brain (2007), 130,3155^ in an FPBI model (Smith et al., 1995; Alsop et al., 1996). Another two experimental TBI studies evaluated in vivo the temporal evolution of DWI changes up to 7 days (closed head injury, Assaf et al., 1997) or 2 weeks (lateral FPBI, Albensi et al., 2000) and compared signal changes with histopathological and neurological outcome measures. They found a significant decrease in the apparent diffusion coefficients (ADC) in the injured area at 1 24 h post-injury, followed by abnormal increase in ADC as early as 7 14 days post-injury, which was in good correlation with infarct size as obtained by histology (Assaf et al., 1997; Albensi et al., 2000). Neurological assessment indicated that such changes were observed at the level of injury that produced moderate impairment 2 weeks after the insult (Albensi et al., 2000). No long-term studies have, however, been reported. The hippocampus was selected as a ROI because it is located just beneath the trauma, and thus represents the tissue at risk for primary and secondary damage (McCarthy, 2003). Previous studies have demonstrated substantial hippocampal damage after TBI both in experimental models and humans (Kotapka et al., 1993, 1994; Hicks et al., 1996; Tate and Bigler, 2000; Grady et al., 2003; Tomaiuolo et al., 2004; Wilde et al., 2007). In addition, the hippocampus ipsilateral to injury is a candidate focus for seizure initiation in PTE after lateral FPBI according to our long-term video-eeg monitoring studies (Kharatishvili et al., 2006) as in patients with PTE (Mathern et al., 1994; Diaz-Arrastia et al., 2000). We did not consider D av measurements in the ipsilateral cortical ROI as reliable and informative as those of the hippocampus due to difficulties in unequivocally separating highly odematous cortex from CSF and progressive changes in the CSF volume fraction. In the hippocampus ipsilateral to the lesion we observed an early (3 h) and transient diffusivity decrease in the animals subjected to lateral FPBI with little evidence of changes in T2-weighted MR images, which is in line with previous TBI studies (Assaf et al., 1997; Albensi et al., 2000). Similar early diffusivity drop was described in animals during and 24 hours after the kainic acid (KA)-induced status epilepticus and in the cortical electroshock model (Nakasu et al., 1995; Ebisu et al., 1996; Zhong et al., 1993, 1997). This early decrease is usually attributed to cellular swelling due to cytotoxic oedema (Wang et al., 1996). The ADC changes were closely correlated with assumed epileptogenic brain areas and the resulting histopathological changes such as neuronal pyknosis and neuropil vacuolization (Nakasu et al., 1995). Interestingly, peri-ictal and early post-ictal human studies using DWI showed transiently decreased local diffusivity in patients with status epilepticus (Kim et al., 2001) or with intractable focal epilepsy (Diehl et al., 1999, 2001; Hufnagel et al., 2003; Diehl et al., 2005) potentially in concordance with the epileptogenic zone. Studies on the temporal evolution of diffusion changes have shown that decrease of ADC in the hippocampus, amygdala and piriform cortex after KA-induced status epilepticus was maximal at 24 h and resolved by 9 days. In our study, after 9 days post-injury we observed a consistent increase in diffusivity values in the hippocampus ipsilateral to injury, which may be explained by ongoing slowly progressive neurodegeneration resulting in expanded extracellular space over the time (Smith et al., 1997), eventually leading to hippocampal sclerosis described previously in lateral FPBI-induced PTE in rats (Lowenstein et al., 1992; Coulter et al., 1996; Hicks et al., 1996; Toth et al., 1997; Kharatishvili et al., 2006) as well as in human PTE (Diaz- Arrastia et al., 2000, Swartz et al., 2006). In human PTE, the functional significance of early and chronic diffusion abnormalities has not been examined. Several diffusion studies have, however, demonstrated areas of increased diffusivity in the chronic phase in a proportion of patients with refractory partial epilepsies, including temporal lobe epilepsy (TLE), where diffusivity was invariably and significantly increased in the epileptogenic hippocampus (Hugg et al., 1999; Wieshmann et al., 1999a; Rugg-Gunn et al., 2001b, 2002; Kantarci et al., 2002; Yoo et al., 2002; Assaf et al., 2003; Lee et al., 2004; Sundgren et al., 2004; Thivard et al., 2005). Based on some of these studies and their own results, Hufnagel and colleagues suggested increased ADC as a potential surrogate marker to lateralize intractable epileptogenic seizure foci (Hufnagel et al., 2003). Post-traumatic abnormalities in hippocampal quantitative diffusion-weighted imaging predict the development of post-traumatic hyperexcitability D av was not only shown to be a sensitive method to detect early brain damage, but more importantly this initial diffusivity drop correlated with the increased susceptibility to seizures as well as with mossy fibre synaptic reorganization 12 months later. Starting at the second week postinjury we observed a consistent increase in diffusivity values in the hippocampus ipsilateral to injury. At 23 days post- FPBI, and at all later time points hippocampal diffusivity values correlated with the EEG markers of the increased susceptibility to seizures in the PTZ test, including shortening of the latency to the first spike, total number of spikes and total number of epileptiform discharges. The role of sprouting of granule cell axons (mossy fibres) in epileptogenesis and ictogenesis is under dispute (Elmer et al., 1997; Longo and Mello, 1998; Sloviter, 1999; Nissinen et al., 2001). However, several histopathological studies in tissue resected from patients who underwent surgery due to drug-refractory epilepsy caused by different aetiologies, including PTE (Sutula et al., 1989; Houser et al., 1990; Mathern et al., 1995a, b, 1996; Swartz et al., 2006) as well as in models of post-status epilepticus, post-traumatic or post-stroke epilepsy have demonstrated that mossy fibre sprouting is present in a large majority of epileptic subjects (Sutula et al., 1988; Golarai et al., 1992; Mello et al., 1993;
Intracranial Studies Of Human Epilepsy In A Surgical Setting
 Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Intracranial Studies Of Human Epilepsy In A Surgical Setting Department of Neurology David Geffen School of Medicine at UCLA Presentation Goals Epilepsy and seizures Basics of the electroencephalogram
Introduction to seizure and epilepsy
 Introduction to seizure and epilepsy 1 Epilepsy : disorder of brain function characterized by a periodic and unpredictable occurrence of seizures. Seizure : abnormal increased electrical activity in the
Introduction to seizure and epilepsy 1 Epilepsy : disorder of brain function characterized by a periodic and unpredictable occurrence of seizures. Seizure : abnormal increased electrical activity in the
epilepticus (SE) or trauma. Between this injury and the emergence of recurrent
 Introduction Epilepsy is one of the oldest medical disorders known. The word epilepsy derived from the Greek word epilamhanein, meaning to be seized or to be overwhelmed by surprise. Epilepsy is one of
Introduction Epilepsy is one of the oldest medical disorders known. The word epilepsy derived from the Greek word epilamhanein, meaning to be seized or to be overwhelmed by surprise. Epilepsy is one of
EEG workshop. Epileptiform abnormalities. Definitions. Dr. Suthida Yenjun
 EEG workshop Epileptiform abnormalities Paroxysmal EEG activities ( focal or generalized) are often termed epileptiform activities EEG hallmark of epilepsy Dr. Suthida Yenjun Epileptiform abnormalities
EEG workshop Epileptiform abnormalities Paroxysmal EEG activities ( focal or generalized) are often termed epileptiform activities EEG hallmark of epilepsy Dr. Suthida Yenjun Epileptiform abnormalities
Assessment of Inhibition and Epileptiform Activity in the Septal Dentate Gyrus of Freely Behaving Rats During the First Week After Kainate Treatment
 The Journal of Neuroscience, November 15, 1999, 19(22):10053 10064 Assessment of Inhibition and Epileptiform Activity in the Septal Dentate Gyrus of Freely Behaving Rats During the First Week After Kainate
The Journal of Neuroscience, November 15, 1999, 19(22):10053 10064 Assessment of Inhibition and Epileptiform Activity in the Septal Dentate Gyrus of Freely Behaving Rats During the First Week After Kainate
Assessment of anti-seizure properties of two proprietary compounds in the electrical kindling model of epilepsy. Date
 Assessment of anti-seizure properties of two proprietary compounds in the electrical kindling model of epilepsy Date This study was conducted under the terms of a Laboratory Services Agreement between
Assessment of anti-seizure properties of two proprietary compounds in the electrical kindling model of epilepsy Date This study was conducted under the terms of a Laboratory Services Agreement between
Case reports functional imaging in epilepsy
 Seizure 2001; 10: 157 161 doi:10.1053/seiz.2001.0552, available online at http://www.idealibrary.com on Case reports functional imaging in epilepsy MARK P. RICHARDSON Medical Research Council Fellow, Institute
Seizure 2001; 10: 157 161 doi:10.1053/seiz.2001.0552, available online at http://www.idealibrary.com on Case reports functional imaging in epilepsy MARK P. RICHARDSON Medical Research Council Fellow, Institute
EEG IN FOCAL ENCEPHALOPATHIES: CEREBROVASCULAR DISEASE, NEOPLASMS, AND INFECTIONS
 246 Figure 8.7: FIRDA. The patient has a history of nonspecific cognitive decline and multiple small WM changes on imaging. oligodendrocytic tumors of the cerebral hemispheres (11,12). Electroencephalogram
246 Figure 8.7: FIRDA. The patient has a history of nonspecific cognitive decline and multiple small WM changes on imaging. oligodendrocytic tumors of the cerebral hemispheres (11,12). Electroencephalogram
Progression from frontal parietal to mesial temporal epilepsy after fluid percussion injury in the rat
 doi:10.1093/brain/awh337 Brain (2005), 128, 174 188 Progression from frontal parietal to mesial temporal epilepsy after fluid percussion injury in the rat Raimondo D Ambrosio, 1,2,4 Jason S. Fender, 1
doi:10.1093/brain/awh337 Brain (2005), 128, 174 188 Progression from frontal parietal to mesial temporal epilepsy after fluid percussion injury in the rat Raimondo D Ambrosio, 1,2,4 Jason S. Fender, 1
Epilepsy: diagnosis and treatment. Sergiusz Jóźwiak Klinika Neurologii Dziecięcej WUM
 Epilepsy: diagnosis and treatment Sergiusz Jóźwiak Klinika Neurologii Dziecięcej WUM Definition: the clinical manifestation of an excessive excitation of a population of cortical neurons Neurotransmitters:
Epilepsy: diagnosis and treatment Sergiusz Jóźwiak Klinika Neurologii Dziecięcej WUM Definition: the clinical manifestation of an excessive excitation of a population of cortical neurons Neurotransmitters:
Supplementary Figure S1: Histological analysis of kainate-treated animals
 Supplementary Figure S1: Histological analysis of kainate-treated animals Nissl stained coronal or horizontal sections were made from kainate injected (right) and saline injected (left) animals at different
Supplementary Figure S1: Histological analysis of kainate-treated animals Nissl stained coronal or horizontal sections were made from kainate injected (right) and saline injected (left) animals at different
Supplementary Figure 1
 Supplementary Figure 1 Miniature microdrive, spike sorting and sleep stage detection. a, A movable recording probe with 8-tetrodes (32-channels). It weighs ~1g. b, A mouse implanted with 8 tetrodes in
Supplementary Figure 1 Miniature microdrive, spike sorting and sleep stage detection. a, A movable recording probe with 8-tetrodes (32-channels). It weighs ~1g. b, A mouse implanted with 8 tetrodes in
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration.
 Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
Implanting an Adult Rat with the Single-Channel Epoch Transmitter for Recording Electrocardiogram in the Type II electrode configuration. Recommended Surgical Tools A. Scalpel handle B. Scalpel blade (#15)
*Pathophysiology of. Epilepsy
 *Pathophysiology of Epilepsy *Objectives * At the end of this lecture the students should be able to:- 1.Define Epilepsy 2.Etio-pathology of Epilepsy 3.Types of Epilepsy 4.Role of Genetic in Epilepsy 5.Clinical
*Pathophysiology of Epilepsy *Objectives * At the end of this lecture the students should be able to:- 1.Define Epilepsy 2.Etio-pathology of Epilepsy 3.Types of Epilepsy 4.Role of Genetic in Epilepsy 5.Clinical
The Sonification of Human EEG and other Biomedical Data. Part 3
 The Sonification of Human EEG and other Biomedical Data Part 3 The Human EEG A data source for the sonification of cerebral dynamics The Human EEG - Outline Electric brain signals Continuous recording
The Sonification of Human EEG and other Biomedical Data Part 3 The Human EEG A data source for the sonification of cerebral dynamics The Human EEG - Outline Electric brain signals Continuous recording
ELSEVIER SECOND PROOF EPLP: Effects of Aging on Seizures and Epilepsy. Introduction. Background
 a0005 Effects of Aging on Seizures and Epilepsy L Velíšek, Departments of Neurology and Neuroscience, Albert Einstein College of Medicine, Bronx, NY C E Stafstrom, Section of Pediatric Neurology, Departments
a0005 Effects of Aging on Seizures and Epilepsy L Velíšek, Departments of Neurology and Neuroscience, Albert Einstein College of Medicine, Bronx, NY C E Stafstrom, Section of Pediatric Neurology, Departments
Introduction to EEG del Campo. Introduction to EEG. J.C. Martin del Campo, MD, FRCP University Health Network Toronto, Canada
 Introduction to EEG J.C. Martin, MD, FRCP University Health Network Toronto, Canada What is EEG? A graphic representation of the difference in voltage between two different cerebral locations plotted over
Introduction to EEG J.C. Martin, MD, FRCP University Health Network Toronto, Canada What is EEG? A graphic representation of the difference in voltage between two different cerebral locations plotted over
Occurrence and Risk Factors for Post-traumatic Epilepsy in Civilian Poulations December 2, 2012
 Occurrence and Risk Factors for Post-traumatic Epilepsy in Civilian Poulations December 2, 2012 Dale C Hesdorffer, PhD GH Sergievsky Center Columbia University American Epilepsy Society Annual Meeting
Occurrence and Risk Factors for Post-traumatic Epilepsy in Civilian Poulations December 2, 2012 Dale C Hesdorffer, PhD GH Sergievsky Center Columbia University American Epilepsy Society Annual Meeting
Diffusion Tensor Imaging 12/06/2013
 12/06/2013 Beate Diehl, MD PhD FRCP University College London National Hospital for Neurology and Neurosurgery Queen Square London, UK American Epilepsy Society Annual Meeting Disclosure None Learning
12/06/2013 Beate Diehl, MD PhD FRCP University College London National Hospital for Neurology and Neurosurgery Queen Square London, UK American Epilepsy Society Annual Meeting Disclosure None Learning
TOBY Cerebral Function Monitoring Addition to CFM handbook for users of the Olympic CFM 6000
 ISRCTN 89547571 TOBY Cerebral Function Monitoring Addition to CFM handbook for users of the Olympic CFM 6000 2 The contents of this booklet were originally produced for the website http://www.azzopardi.freeserve.co.uk/cfm
ISRCTN 89547571 TOBY Cerebral Function Monitoring Addition to CFM handbook for users of the Olympic CFM 6000 2 The contents of this booklet were originally produced for the website http://www.azzopardi.freeserve.co.uk/cfm
Rapamycin Attenuates the Development of Posttraumatic Epilepsy in a Mouse Model of Traumatic Brain Injury.
 Current Literature In Basic Science Prophylaxis for Post-Traumatic Epilepsy: Can Your Kinase Do That? Rapamycin Attenuates the Development of Posttraumatic Epilepsy in a Mouse Model of Traumatic Brain
Current Literature In Basic Science Prophylaxis for Post-Traumatic Epilepsy: Can Your Kinase Do That? Rapamycin Attenuates the Development of Posttraumatic Epilepsy in a Mouse Model of Traumatic Brain
There are several types of epilepsy. Each of them have different causes, symptoms and treatment.
 1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
Diagnosing Complicated Epilepsy: Mapping of the Epileptic Circuitry. Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA
 Diagnosing Complicated Epilepsy: Mapping of the Epileptic Circuitry Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA Overview Definition of epileptic circuitry Methods of mapping
Diagnosing Complicated Epilepsy: Mapping of the Epileptic Circuitry Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA Overview Definition of epileptic circuitry Methods of mapping
Toward a noninvasive automatic seizure control system with transcranial focal stimulations via tripolar concentric ring electrodes
 Toward a noninvasive automatic seizure control system with transcranial focal stimulations via tripolar concentric ring electrodes Oleksandr Makeyev Department of Electrical, Computer, and Biomedical Engineering
Toward a noninvasive automatic seizure control system with transcranial focal stimulations via tripolar concentric ring electrodes Oleksandr Makeyev Department of Electrical, Computer, and Biomedical Engineering
Nature Neuroscience: doi: /nn Supplementary Figure 1
 Supplementary Figure 1 Hippocampal recordings. a. (top) Post-operative MRI (left, depicting a depth electrode implanted along the longitudinal hippocampal axis) and co-registered preoperative MRI (right)
Supplementary Figure 1 Hippocampal recordings. a. (top) Post-operative MRI (left, depicting a depth electrode implanted along the longitudinal hippocampal axis) and co-registered preoperative MRI (right)
Early seizure propagation from the occipital lobe to medial temporal structures and its surgical implication
 Original article Epileptic Disord 2008; 10 (4): 260-5 Early seizure propagation from the occipital lobe to medial temporal structures and its surgical implication Naotaka Usui, Tadahiro Mihara, Koichi
Original article Epileptic Disord 2008; 10 (4): 260-5 Early seizure propagation from the occipital lobe to medial temporal structures and its surgical implication Naotaka Usui, Tadahiro Mihara, Koichi
EEG in Medical Practice
 EEG in Medical Practice Dr. Md. Mahmudur Rahman Siddiqui MBBS, FCPS, FACP, FCCP Associate Professor, Dept. of Medicine Anwer Khan Modern Medical College What is the EEG? The brain normally produces tiny
EEG in Medical Practice Dr. Md. Mahmudur Rahman Siddiqui MBBS, FCPS, FACP, FCCP Associate Professor, Dept. of Medicine Anwer Khan Modern Medical College What is the EEG? The brain normally produces tiny
EMG, EEG, and Neurophysiology in Clinical Practice
 Mayo School of Continuous Professional Development EMG, EEG, and Neurophysiology in Clinical Practice Matthew T. Hoerth, M.D. Ritz-Carlton, Amelia Island, Florida January 29-February 4, 2017 2016 MFMER
Mayo School of Continuous Professional Development EMG, EEG, and Neurophysiology in Clinical Practice Matthew T. Hoerth, M.D. Ritz-Carlton, Amelia Island, Florida January 29-February 4, 2017 2016 MFMER
Vagus nerve stimulation for refractory epilepsy
 Seizure 2001; 10: 456 460 doi:10.1053/seiz.2001.0628, available online at http://www.idealibrary.com on CASE REPORT Vagus nerve stimulation for refractory epilepsy PAUL BOON, KRISTL VONCK, JACQUES DE REUCK
Seizure 2001; 10: 456 460 doi:10.1053/seiz.2001.0628, available online at http://www.idealibrary.com on CASE REPORT Vagus nerve stimulation for refractory epilepsy PAUL BOON, KRISTL VONCK, JACQUES DE REUCK
Subconvulsive Dose of Kainic Acid Transiently Increases the Locomotor Activity of Adult Wistar Rats
 Physiol. Res. 64: 263-267, 2015 SHORT COMMUNICATION Subconvulsive Dose of Kainic Acid Transiently Increases the Locomotor Activity of Adult Wistar Rats V. RILJAK 1, D. MAREŠOVÁ 1, J. POKORNÝ 1, K. JANDOVÁ
Physiol. Res. 64: 263-267, 2015 SHORT COMMUNICATION Subconvulsive Dose of Kainic Acid Transiently Increases the Locomotor Activity of Adult Wistar Rats V. RILJAK 1, D. MAREŠOVÁ 1, J. POKORNÝ 1, K. JANDOVÁ
PRESURGICAL EVALUATION. ISLAND OF COS Hippocrates: On the Sacred Disease. Disclosure Research-Educational Grants. Patients with seizure disorders
 PRESURGICAL EVALUATION Patients with seizure disorders Gregory D. Cascino, MD Mayo Clinic Disclosure Research-Educational Grants Mayo Foundation Neuro Pace, Inc. American Epilepsy Society American Academy
PRESURGICAL EVALUATION Patients with seizure disorders Gregory D. Cascino, MD Mayo Clinic Disclosure Research-Educational Grants Mayo Foundation Neuro Pace, Inc. American Epilepsy Society American Academy
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences
 Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
Experimental Assessment of Infarct Lesion Growth in Mice using Time-Resolved T2* MR Image Sequences Nils Daniel Forkert 1, Dennis Säring 1, Andrea Eisenbeis 2, Frank Leypoldt 3, Jens Fiehler 2, Heinz Handels
The EEG in focal epilepsy. Bassel Abou-Khalil, M.D. Vanderbilt University Medical Center
 The EEG in focal epilepsy Bassel Abou-Khalil, M.D. Vanderbilt University Medical Center I have no financial relationships to disclose that are relative to the content of my presentation Learning Objectives
The EEG in focal epilepsy Bassel Abou-Khalil, M.D. Vanderbilt University Medical Center I have no financial relationships to disclose that are relative to the content of my presentation Learning Objectives
9/30/2016. Advances in Epilepsy Surgery. Epidemiology. Epidemiology
 Advances in Epilepsy Surgery George Jallo, M.D. Director, Institute for Brain Protection Sciences Johns Hopkins All Children s Hospital St Petersburg, Florida Epidemiology WHO lists it as the second most
Advances in Epilepsy Surgery George Jallo, M.D. Director, Institute for Brain Protection Sciences Johns Hopkins All Children s Hospital St Petersburg, Florida Epidemiology WHO lists it as the second most
Focal epilepsy recruiting a generalised network of juvenile myoclonic epilepsy: a case report
 Clinical commentary Epileptic Disord 2014; 16 (3): 370-4 Focal epilepsy recruiting a generalised network of juvenile myoclonic epilepsy: a case report Myo Khaing 1,2, Kheng-Seang Lim 1, Chong-Tin Tan 1
Clinical commentary Epileptic Disord 2014; 16 (3): 370-4 Focal epilepsy recruiting a generalised network of juvenile myoclonic epilepsy: a case report Myo Khaing 1,2, Kheng-Seang Lim 1, Chong-Tin Tan 1
EEG in the ICU: Part I
 EEG in the ICU: Part I Teneille E. Gofton July 2012 Objectives To outline the importance of EEG monitoring in the ICU To briefly review the neurophysiological basis of EEG To introduce formal EEG and subhairline
EEG in the ICU: Part I Teneille E. Gofton July 2012 Objectives To outline the importance of EEG monitoring in the ICU To briefly review the neurophysiological basis of EEG To introduce formal EEG and subhairline
The secrets of conventional EEG
 The secrets of conventional EEG The spike/sharp wave activity o Electro-clinical characteristics of Spike/Sharp wave The polymorphic delta activity o Electro-clinical characteristics of Polymorphic delta
The secrets of conventional EEG The spike/sharp wave activity o Electro-clinical characteristics of Spike/Sharp wave The polymorphic delta activity o Electro-clinical characteristics of Polymorphic delta
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting?
 High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
High Resolution Ictal SPECT: Enhanced Epileptic Source Targeting? Marvin A Rossi MD, PhD RUSH Epilepsy Center Research Lab http://www.synapticom.net Chicago, IL USA Medically-Refractory Epilepsy 500,000-800,000
Imaging and EEG in Post-traumatic Epilepsy
 Imaging and EEG in Post-traumatic Epilepsy Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA American Epilepsy Society Annual Meeting Disclosure Name Upsher-Smith Sunovion, Eisai,
Imaging and EEG in Post-traumatic Epilepsy Michael R. Sperling, M.D. Thomas Jefferson University Philadelphia, PA American Epilepsy Society Annual Meeting Disclosure Name Upsher-Smith Sunovion, Eisai,
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Focal Cooling for the Prevention and Treatment of Epilepsy: From Patients to Models (and back again)
 Focal Cooling for the Prevention and Treatment of Epilepsy: From Patients to Models (and back again) December 7 th, 2013 Matthew D. Smyth, MD FAANS FACS FAAP Washington University, St. Louis MO St. Louis
Focal Cooling for the Prevention and Treatment of Epilepsy: From Patients to Models (and back again) December 7 th, 2013 Matthew D. Smyth, MD FAANS FACS FAAP Washington University, St. Louis MO St. Louis
SUPPLEMENTARY INFORMATION. Supplementary Figure 1
 SUPPLEMENTARY INFORMATION Supplementary Figure 1 The supralinear events evoked in CA3 pyramidal cells fulfill the criteria for NMDA spikes, exhibiting a threshold, sensitivity to NMDAR blockade, and all-or-none
SUPPLEMENTARY INFORMATION Supplementary Figure 1 The supralinear events evoked in CA3 pyramidal cells fulfill the criteria for NMDA spikes, exhibiting a threshold, sensitivity to NMDAR blockade, and all-or-none
Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy
 Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy 1. Introduction Epilepsy is a common neurological disorder, which affects about 1 %
Automated detection of abnormal changes in cortical thickness: A tool to help diagnosis in neocortical focal epilepsy 1. Introduction Epilepsy is a common neurological disorder, which affects about 1 %
The American Approach to Depth Electrode Insertion December 4, 2012
 The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
The American Approach to Depth Electrode Insertion December 4, 2012 Jonathan Miller, MD Director, Epilepsy Surgery University Hospitals Case Medical Center/Case Western Reserve University Cleveland, Ohio
C O N F I D E N T I A L ASSESSMENT OF XXX EFFECTS ON RECURRENT SEIZURE ACTIVITY IN THE RAT PILOCARPINE MODEL
 C O N F I D E N T I A L ASSESSMENT OF XXX EFFECTS ON RECURRENT SEIZURE ACTIVITY IN THE RAT PILOCARPINE MODEL 6 May 2015 This study was conducted under the terms of a Research Agreement between NeuroDetective
C O N F I D E N T I A L ASSESSMENT OF XXX EFFECTS ON RECURRENT SEIZURE ACTIVITY IN THE RAT PILOCARPINE MODEL 6 May 2015 This study was conducted under the terms of a Research Agreement between NeuroDetective
Multimodal Imaging in Extratemporal Epilepsy Surgery
 Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Open Access Case Report DOI: 10.7759/cureus.2338 Multimodal Imaging in Extratemporal Epilepsy Surgery Christian Vollmar 1, Aurelia Peraud 2, Soheyl Noachtar 1 1. Epilepsy Center, Dept. of Neurology, University
Nature Methods: doi: /nmeth Supplementary Figure 1. Activity in turtle dorsal cortex is sparse.
 Supplementary Figure 1 Activity in turtle dorsal cortex is sparse. a. Probability distribution of firing rates across the population (notice log scale) in our data. The range of firing rates is wide but
Supplementary Figure 1 Activity in turtle dorsal cortex is sparse. a. Probability distribution of firing rates across the population (notice log scale) in our data. The range of firing rates is wide but
Localization a quick look
 Localization a quick look Covering the basics Differential amplifiers Polarity convention 10-20 electrode system Basic montages: bipolar and referential Other aspects of displaying the EEG Localization
Localization a quick look Covering the basics Differential amplifiers Polarity convention 10-20 electrode system Basic montages: bipolar and referential Other aspects of displaying the EEG Localization
Surgery for Medically Refractory Focal Epilepsy
 Surgery for Medically Refractory Focal Epilepsy Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence
Surgery for Medically Refractory Focal Epilepsy Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence
Traumatic Brain Injury TBI Presented by Bill Masten
 1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
Presenter Disclosure
 Presenter Disclosure Presenter s name: Wanida Nuwisait, Department of Physiology, Faculty of Medicine, University of Toronto I do not have an affiliation (financial or otherwise) with a commercial organization
Presenter Disclosure Presenter s name: Wanida Nuwisait, Department of Physiology, Faculty of Medicine, University of Toronto I do not have an affiliation (financial or otherwise) with a commercial organization
Common Ictal Patterns in Patients with Documented Epileptic Seizures
 THE ICTAL IRAQI PATTERNS POSTGRADUATE IN EPILEPTIC MEDICAL JOURNAL PATIENTS Common Ictal Patterns in Documented Epileptic Seizures Ghaieb Bashar ALJandeel, Gonzalo Alarcon ABSTRACT: BACKGROUND: The ictal
THE ICTAL IRAQI PATTERNS POSTGRADUATE IN EPILEPTIC MEDICAL JOURNAL PATIENTS Common Ictal Patterns in Documented Epileptic Seizures Ghaieb Bashar ALJandeel, Gonzalo Alarcon ABSTRACT: BACKGROUND: The ictal
Focal fast rhythmic epileptiform discharges on scalp EEG in a patient with cortical dysplasia
 Seizure 2002; 11: 330 334 doi:10.1053/seiz.2001.0610, available online at http://www.idealibrary.com on CASE REPORT Focal fast rhythmic epileptiform discharges on scalp EEG in a patient with cortical dysplasia
Seizure 2002; 11: 330 334 doi:10.1053/seiz.2001.0610, available online at http://www.idealibrary.com on CASE REPORT Focal fast rhythmic epileptiform discharges on scalp EEG in a patient with cortical dysplasia
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES. Mr. Johnson. Seizures at 29 Years of Age. Dileep Nair, MD Juan Bulacio, MD
 Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
Invasive Evaluation for Epilepsy Surgery Lesional Cases NO DISCLOSURES Dileep Nair, MD Juan Bulacio, MD Mr. Johnson Seizures at 29 Years of Age Onset of seizures at 16 years of age bed wetting episodes
CHAPTER 6 INTERFERENCE CANCELLATION IN EEG SIGNAL
 116 CHAPTER 6 INTERFERENCE CANCELLATION IN EEG SIGNAL 6.1 INTRODUCTION Electrical impulses generated by nerve firings in the brain pass through the head and represent the electroencephalogram (EEG). Electrical
116 CHAPTER 6 INTERFERENCE CANCELLATION IN EEG SIGNAL 6.1 INTRODUCTION Electrical impulses generated by nerve firings in the brain pass through the head and represent the electroencephalogram (EEG). Electrical
Supplementary Figure 1. ACE robotic platform. A. Overview of the rig setup showing major hardware components of ACE (Automatic single Cell
 2 Supplementary Figure 1. ACE robotic platform. A. Overview of the rig setup showing major hardware components of ACE (Automatic single Cell Experimenter) including the MultiClamp 700B, Digidata 1440A,
2 Supplementary Figure 1. ACE robotic platform. A. Overview of the rig setup showing major hardware components of ACE (Automatic single Cell Experimenter) including the MultiClamp 700B, Digidata 1440A,
Neurophysiology & EEG
 Neurophysiology & EEG PG4 Core Curriculum Ian A. Cook, M.D. Associate Director, Laboratory of Brain, Behavior, & Pharmacology UCLA Department of Psychiatry & Biobehavioral Sciences Semel Institute for
Neurophysiology & EEG PG4 Core Curriculum Ian A. Cook, M.D. Associate Director, Laboratory of Brain, Behavior, & Pharmacology UCLA Department of Psychiatry & Biobehavioral Sciences Semel Institute for
Myoclonic status epilepticus in hypoxic ischemic encephalopathy which recurred after somatosensory evoked potential testing
 ANNALS OF CLINICAL NEUROPHYSIOLOGY CASE REPORT Ann Clin Neurophysiol 2017;19(2):136-140 Myoclonic status epilepticus in hypoxic ischemic encephalopathy which recurred after somatosensory evoked potential
ANNALS OF CLINICAL NEUROPHYSIOLOGY CASE REPORT Ann Clin Neurophysiol 2017;19(2):136-140 Myoclonic status epilepticus in hypoxic ischemic encephalopathy which recurred after somatosensory evoked potential
Electroencephalography. Role of EEG in NCSE. Continuous EEG in ICU 25/05/59. EEG pattern in status epilepticus
 EEG: ICU monitoring & 2 interesting cases Electroencephalography Techniques Paper EEG digital video electroencephalography Dr. Pasiri Sithinamsuwan PMK Hospital Routine EEG long term monitoring Continuous
EEG: ICU monitoring & 2 interesting cases Electroencephalography Techniques Paper EEG digital video electroencephalography Dr. Pasiri Sithinamsuwan PMK Hospital Routine EEG long term monitoring Continuous
Approximately 70% of childhood SURGICAL TREATMENTS FOR PEDIATRIC EPILEPSY PROCEEDINGS. Ronald P. Lesser, MD KEY POINTS
 ASIM May p153-158 5/14/01 9:19 AM Page 153 SURGICAL TREATMENTS FOR PEDIATRIC EPILEPSY Ronald P. Lesser, MD KEY POINTS Most children with epilepsy refractory to drugs can improve with surgery Temporal lobe
ASIM May p153-158 5/14/01 9:19 AM Page 153 SURGICAL TREATMENTS FOR PEDIATRIC EPILEPSY Ronald P. Lesser, MD KEY POINTS Most children with epilepsy refractory to drugs can improve with surgery Temporal lobe
Does AED Prophylaxis Work in Posttraumatic Epilepsy December 2, 2012
 Does AED Prophylaxis Work in Posttraumatic Epilepsy December 2, 2012 Marc A. Dichter, MD, PhD University of Pennsylvania American Epilepsy Society Annual Meeting Disclosure Name of Commercial Interest
Does AED Prophylaxis Work in Posttraumatic Epilepsy December 2, 2012 Marc A. Dichter, MD, PhD University of Pennsylvania American Epilepsy Society Annual Meeting Disclosure Name of Commercial Interest
Database of paroxysmal iceeg signals
 POSTER 2017, PRAGUE MAY 23 1 Database of paroxysmal iceeg signals Ing. Nikol Kopecká 1 1 Dept. of Circuit Theory, Czech Technical University, Technická 2, 166 27 Praha, Czech Republic kopecnik@fel.cvut.cz
POSTER 2017, PRAGUE MAY 23 1 Database of paroxysmal iceeg signals Ing. Nikol Kopecká 1 1 Dept. of Circuit Theory, Czech Technical University, Technická 2, 166 27 Praha, Czech Republic kopecnik@fel.cvut.cz
Nature Neuroscience: doi: /nn Supplementary Figure 1. Large-scale calcium imaging in vivo.
 Supplementary Figure 1 Large-scale calcium imaging in vivo. (a) Schematic illustration of the in vivo camera imaging set-up for large-scale calcium imaging. (b) High-magnification two-photon image from
Supplementary Figure 1 Large-scale calcium imaging in vivo. (a) Schematic illustration of the in vivo camera imaging set-up for large-scale calcium imaging. (b) High-magnification two-photon image from
File name: Supplementary Information Description: Supplementary Figures, Supplementary Table and Supplementary References
 File name: Supplementary Information Description: Supplementary Figures, Supplementary Table and Supplementary References File name: Supplementary Data 1 Description: Summary datasheets showing the spatial
File name: Supplementary Information Description: Supplementary Figures, Supplementary Table and Supplementary References File name: Supplementary Data 1 Description: Summary datasheets showing the spatial
Supplementary Material for
 Supplementary Material for Selective neuronal lapses precede human cognitive lapses following sleep deprivation Supplementary Table 1. Data acquisition details Session Patient Brain regions monitored Time
Supplementary Material for Selective neuronal lapses precede human cognitive lapses following sleep deprivation Supplementary Table 1. Data acquisition details Session Patient Brain regions monitored Time
Successful Treatment of Mesial Temporal Lobe Epilepsy with Bilateral Hippocampal Atrophy and False Temporal Scalp Ictal Onset: A case report
 Hiroshima J. Med. Sci. Vol. 61, No. 2, 37~41, June, 2012 HIJM 61 7 37 Successful Treatment of Mesial Temporal Lobe Epilepsy with Bilateral Hippocampal Atrophy and False Temporal Scalp Ictal Onset: A case
Hiroshima J. Med. Sci. Vol. 61, No. 2, 37~41, June, 2012 HIJM 61 7 37 Successful Treatment of Mesial Temporal Lobe Epilepsy with Bilateral Hippocampal Atrophy and False Temporal Scalp Ictal Onset: A case
Physiological Markers of Pharmacoresistant Epilepsy December 2, 2011
 Physiological Markers of Pharmacoresistant Epilepsy December 2, 2011 Jerome Engel, Jr., MD, PhD Director of the Seizure Disorder Center The Jonathan Sinay Distinguished Professor of Neurology, Neurobiology,
Physiological Markers of Pharmacoresistant Epilepsy December 2, 2011 Jerome Engel, Jr., MD, PhD Director of the Seizure Disorder Center The Jonathan Sinay Distinguished Professor of Neurology, Neurobiology,
Electroencephalography
 The electroencephalogram (EEG) is a measure of brain waves. It is a readily available test that provides evidence of how the brain functions over time. The EEG is used in the evaluation of brain disorders.
The electroencephalogram (EEG) is a measure of brain waves. It is a readily available test that provides evidence of how the brain functions over time. The EEG is used in the evaluation of brain disorders.
Gross Organization I The Brain. Reading: BCP Chapter 7
 Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
Gross Organization I The Brain Reading: BCP Chapter 7 Layout of the Nervous System Central Nervous System (CNS) Located inside of bone Includes the brain (in the skull) and the spinal cord (in the backbone)
RASMUSSEN S ENCEPHALITIS - A CASE REPORT. Dr. Suchithra.J DNB PG RAILWAY HOSPITAL
 RASMUSSEN S ENCEPHALITIS - A CASE REPORT Dr. Suchithra.J DNB PG RAILWAY HOSPITAL Master Naveen Kumar, 7/Mch, first born of nonconsanguinous marriage presented to us with Left hemiparesis Seizures on L
RASMUSSEN S ENCEPHALITIS - A CASE REPORT Dr. Suchithra.J DNB PG RAILWAY HOSPITAL Master Naveen Kumar, 7/Mch, first born of nonconsanguinous marriage presented to us with Left hemiparesis Seizures on L
Impact of Injury Location and Severity on Posttraumatic Epilepsy in the Rat: Role of Frontal Neocortex
 Cerebral Cortex July 2011;21:1574--1592 doi:10.1093/cercor/bhq218 Advance Access publication November 26, 2010 Impact of Injury Location and Severity on Posttraumatic Epilepsy in the Rat: Role of Frontal
Cerebral Cortex July 2011;21:1574--1592 doi:10.1093/cercor/bhq218 Advance Access publication November 26, 2010 Impact of Injury Location and Severity on Posttraumatic Epilepsy in the Rat: Role of Frontal
Toward a more accurate delimitation of the epileptic focus from a surgical perspective
 Toward a more accurate delimitation of the epileptic focus from a surgical perspective Margitta Seeck Department of Clinical Neurosciences EEG & Epilepsy Unit University Hospital of Geneva Geneva, Switzerland
Toward a more accurate delimitation of the epileptic focus from a surgical perspective Margitta Seeck Department of Clinical Neurosciences EEG & Epilepsy Unit University Hospital of Geneva Geneva, Switzerland
Development of Ultrasound Based Techniques for Measuring Skeletal Muscle Motion
 Development of Ultrasound Based Techniques for Measuring Skeletal Muscle Motion Jason Silver August 26, 2009 Presentation Outline Introduction Thesis Objectives Mathematical Model and Principles Methods
Development of Ultrasound Based Techniques for Measuring Skeletal Muscle Motion Jason Silver August 26, 2009 Presentation Outline Introduction Thesis Objectives Mathematical Model and Principles Methods
Case report. Epileptic Disord 2005; 7 (1): 37-41
 Case report Epileptic Disord 2005; 7 (1): 37-41 Periodic lateralized epileptiform discharges (PLEDs) as the sole electrographic correlate of a complex partial seizure Gagandeep Singh, Mary-Anne Wright,
Case report Epileptic Disord 2005; 7 (1): 37-41 Periodic lateralized epileptiform discharges (PLEDs) as the sole electrographic correlate of a complex partial seizure Gagandeep Singh, Mary-Anne Wright,
Microcircuitry coordination of cortical motor information in self-initiation of voluntary movements
 Y. Isomura et al. 1 Microcircuitry coordination of cortical motor information in self-initiation of voluntary movements Yoshikazu Isomura, Rie Harukuni, Takashi Takekawa, Hidenori Aizawa & Tomoki Fukai
Y. Isomura et al. 1 Microcircuitry coordination of cortical motor information in self-initiation of voluntary movements Yoshikazu Isomura, Rie Harukuni, Takashi Takekawa, Hidenori Aizawa & Tomoki Fukai
Telemetric EEG and the Rat: A Guide For Neuroscientists
 Editorial Telemetric EEG and the Rat: A Guide For Neuroscientists Jafri Malin Abdullah 1, Mohammad Rafiqul Islam 2 1 Malaysian Journal of Medical Sciences, Universiti Sains Malaysia Press, Universiti Sains
Editorial Telemetric EEG and the Rat: A Guide For Neuroscientists Jafri Malin Abdullah 1, Mohammad Rafiqul Islam 2 1 Malaysian Journal of Medical Sciences, Universiti Sains Malaysia Press, Universiti Sains
Nature Medicine: doi: /nm.4084
 Supplementary Figure 1: Sample IEDs. (a) Sample hippocampal IEDs from different kindled rats (scale bar = 200 µv, 100 ms). (b) Sample temporal lobe IEDs from different subjects with epilepsy (scale bar
Supplementary Figure 1: Sample IEDs. (a) Sample hippocampal IEDs from different kindled rats (scale bar = 200 µv, 100 ms). (b) Sample temporal lobe IEDs from different subjects with epilepsy (scale bar
Asian Epilepsy Academy (ASEPA) EEG Certification Examination
 Asian Epilepsy Academy (ASEPA) EEG Certification Examination EEG Certification Examination Aims To set and improve the standard of practice of Electroencephalography (EEG) in the Asian Oceanian region
Asian Epilepsy Academy (ASEPA) EEG Certification Examination EEG Certification Examination Aims To set and improve the standard of practice of Electroencephalography (EEG) in the Asian Oceanian region
True Epileptiform Patterns (and some others)
 True Epileptiform Patterns (and some others) a) What is epileptiform b) Some possible surprises c) Classification of generalized epileptiform patterns An epileptiform pattern Interpretative term based
True Epileptiform Patterns (and some others) a) What is epileptiform b) Some possible surprises c) Classification of generalized epileptiform patterns An epileptiform pattern Interpretative term based
Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity
 Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity December 10, 2013 Joyce Y. Wu, MD Associate Professor Division of Pediatric Neurology David Geffen School of Medicine
Interictal High Frequency Oscillations as Neurophysiologic Biomarkers of Epileptogenicity December 10, 2013 Joyce Y. Wu, MD Associate Professor Division of Pediatric Neurology David Geffen School of Medicine
Implantable Microelectronic Devices
 ECE 8803/4803 Implantable Microelectronic Devices Fall - 2015 Maysam Ghovanloo (mgh@gatech.edu) School of Electrical and Computer Engineering Georgia Institute of Technology 2015 Maysam Ghovanloo 1 Outline
ECE 8803/4803 Implantable Microelectronic Devices Fall - 2015 Maysam Ghovanloo (mgh@gatech.edu) School of Electrical and Computer Engineering Georgia Institute of Technology 2015 Maysam Ghovanloo 1 Outline
Clinically focused workflow with unique ability to integrate fmri, DTI, fiber tracks and perfusion in a single, multi-layered 3D rendering
 Clinically focused workflow with unique ability to integrate fmri, DTI, fiber tracks and perfusion in a single, multi-layered 3D rendering Neurosurgeons are demanding more from neuroradiologists and increasingly
Clinically focused workflow with unique ability to integrate fmri, DTI, fiber tracks and perfusion in a single, multi-layered 3D rendering Neurosurgeons are demanding more from neuroradiologists and increasingly
Supplementary Figure 1: Kv7 currents in neonatal CA1 neurons measured with the classic M- current voltage-clamp protocol.
 Supplementary Figures 1-11 Supplementary Figure 1: Kv7 currents in neonatal CA1 neurons measured with the classic M- current voltage-clamp protocol. (a), Voltage-clamp recordings from CA1 pyramidal neurons
Supplementary Figures 1-11 Supplementary Figure 1: Kv7 currents in neonatal CA1 neurons measured with the classic M- current voltage-clamp protocol. (a), Voltage-clamp recordings from CA1 pyramidal neurons
Magnetic Resonance Imaging. Basics of MRI in practice. Generation of MR signal. Generation of MR signal. Spin echo imaging. Generation of MR signal
 Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Magnetic Resonance Imaging Protons aligned with B0 magnetic filed Longitudinal magnetization - T1 relaxation Transverse magnetization - T2 relaxation Signal measured in the transverse plane Basics of MRI
Objectives. Amanda Diamond, MD
 Amanda Diamond, MD Objectives Recognize symptoms suggestive of seizure and what those clinical symptoms represent Understand classification of epilepsy and why this is important Identify the appropriate
Amanda Diamond, MD Objectives Recognize symptoms suggestive of seizure and what those clinical symptoms represent Understand classification of epilepsy and why this is important Identify the appropriate
Scope. EEG patterns in Encephalopathy. Diffuse encephalopathy. EEG in adult patients with. EEG in diffuse encephalopathy
 Scope EEG patterns in Encephalopathy Dr.Pasiri Sithinamsuwan Division of Neurology Department of Medicine Phramongkutklao Hospital Diffuse encephalopathy EEG in specific encephalopathies Encephalitides
Scope EEG patterns in Encephalopathy Dr.Pasiri Sithinamsuwan Division of Neurology Department of Medicine Phramongkutklao Hospital Diffuse encephalopathy EEG in specific encephalopathies Encephalitides
Morphometric MRI Analysis of the Parahippocampal Region in Temporal Lobe Epilepsy
 Morphometric MRI Analysis of the Parahippocampal Region in Temporal Lobe Epilepsy NEDA BERNASCONI, a ANDREA BERNASCONI, ZOGRAFOS CARAMANOS, FREDERICK ANDERMANN, FRANÇOIS DUBEAU, AND DOUGLAS L. ARNOLD Department
Morphometric MRI Analysis of the Parahippocampal Region in Temporal Lobe Epilepsy NEDA BERNASCONI, a ANDREA BERNASCONI, ZOGRAFOS CARAMANOS, FREDERICK ANDERMANN, FRANÇOIS DUBEAU, AND DOUGLAS L. ARNOLD Department
Asian Epilepsy Academy (ASEPA) & ASEAN Neurological Association (ASNA) EEG Certification Examination
 Asian Epilepsy Academy (ASEPA) & ASEAN Neurological Association (ASNA) EEG Certification Examination EEG Certification Examination Aims To set and improve the standard of practice of Electroencephalography
Asian Epilepsy Academy (ASEPA) & ASEAN Neurological Association (ASNA) EEG Certification Examination EEG Certification Examination Aims To set and improve the standard of practice of Electroencephalography
fmri (functional MRI)
 Lesion fmri (functional MRI) Electroencephalogram (EEG) Brainstem CT (computed tomography) Scan Medulla PET (positron emission tomography) Scan Reticular Formation MRI (magnetic resonance imaging) Thalamus
Lesion fmri (functional MRI) Electroencephalogram (EEG) Brainstem CT (computed tomography) Scan Medulla PET (positron emission tomography) Scan Reticular Formation MRI (magnetic resonance imaging) Thalamus
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Spike frequency is dependent on epilepsy duration and seizure frequency in temporal lobe epilepsy
 Original article Epileptic Disord 2005; 7 (4): 355-9 Spike frequency is dependent on epilepsy duration and seizure frequency in temporal lobe epilepsy Jozsef Janszky 1,2,3, M. Hoppe 1, Z. Clemens 3, I.
Original article Epileptic Disord 2005; 7 (4): 355-9 Spike frequency is dependent on epilepsy duration and seizure frequency in temporal lobe epilepsy Jozsef Janszky 1,2,3, M. Hoppe 1, Z. Clemens 3, I.
Myers Psychology for AP*
 Myers Psychology for AP* David G. Myers PowerPoint Presentation Slides by Kent Korek Germantown High School Worth Publishers, 2010 *AP is a trademark registered and/or owned by the College Board, which
Myers Psychology for AP* David G. Myers PowerPoint Presentation Slides by Kent Korek Germantown High School Worth Publishers, 2010 *AP is a trademark registered and/or owned by the College Board, which
Abstract. Introduction. Keywords: AHP, odour-learning, piriform cortex, pyramidal cells
 European Journal of Neuroscience, Vol. 10, pp. 1518 1523, 1998 European Neuroscience Association SHORT COMMUNICATION Reduced after-hyperpolarization in rat piriform cortex pyramidal neurons is associated
European Journal of Neuroscience, Vol. 10, pp. 1518 1523, 1998 European Neuroscience Association SHORT COMMUNICATION Reduced after-hyperpolarization in rat piriform cortex pyramidal neurons is associated
A Comparative study of the Anti convulsant effect of Nimodipine and Ketamine combination with standard anticonvulsant drug in Rodents
 Original Article A Comparative study of the Anti convulsant effect of Nimodipine and Ketamine combination with standard anticonvulsant drug in Rodents Prasanand S 1, Pushpalatha C 2, Mohsin MD 3, Sam Pavan
Original Article A Comparative study of the Anti convulsant effect of Nimodipine and Ketamine combination with standard anticonvulsant drug in Rodents Prasanand S 1, Pushpalatha C 2, Mohsin MD 3, Sam Pavan
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy
 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy Reference: NHS England xxx/x/x 1 Clinical Commissioning Policy: Deep Brain Stimulation for Refractory Epilepsy First published:
Supplementary Methods
 1 Supplementary Methods Social Preference Test Subjects Seventy-four Long-Evans, male rats served as subjects (S-rats) in the foodpreference test, with 40 assigned to the CXT-Same (CXT-S) Condition and
1 Supplementary Methods Social Preference Test Subjects Seventy-four Long-Evans, male rats served as subjects (S-rats) in the foodpreference test, with 40 assigned to the CXT-Same (CXT-S) Condition and
Periodic and Rhythmic Patterns. Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina
 Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Periodic and Rhythmic Patterns Suzette M LaRoche, MD Mission Health Epilepsy Center Asheville, North Carolina Continuum of EEG Activity Neuronal Injury LRDA GPDs SIRPIDs LPDs + NCS Burst-Suppression LPDs
Analysis of Seizure Onset on the Basis of Wideband EEG Recordings
 Epilepsia, (Suppl. ):9, 00 Blackwell Publishing, Inc. C International League Against Epilepsy Ictogenesis Analysis of Seizure Onset on the Basis of Wideband EEG Recordings Anatol Bragin, Charles L. Wilson,
Epilepsia, (Suppl. ):9, 00 Blackwell Publishing, Inc. C International League Against Epilepsy Ictogenesis Analysis of Seizure Onset on the Basis of Wideband EEG Recordings Anatol Bragin, Charles L. Wilson,
Supplemental Figure 1
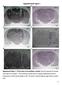 A C E Supplemental Figure 1 AP 1mm A+C 1mm Apo 1mm B D 1mm CGS F 1mm All 1mm Supplemental Figure 1. The locations of microinfusion cannulae. Each dot represents the cannula tip of a given rat in Figure.
A C E Supplemental Figure 1 AP 1mm A+C 1mm Apo 1mm B D 1mm CGS F 1mm All 1mm Supplemental Figure 1. The locations of microinfusion cannulae. Each dot represents the cannula tip of a given rat in Figure.
Nature Neuroscience doi: /nn Supplementary Figure 1. Characterization of viral injections.
 Supplementary Figure 1 Characterization of viral injections. (a) Dorsal view of a mouse brain (dashed white outline) after receiving a large, unilateral thalamic injection (~100 nl); demonstrating that
Supplementary Figure 1 Characterization of viral injections. (a) Dorsal view of a mouse brain (dashed white outline) after receiving a large, unilateral thalamic injection (~100 nl); demonstrating that
