Recording and interpretation of intracranial pressure
|
|
|
- Valentine Gibbs
- 6 years ago
- Views:
Transcription
1 CLINICAL ARTICLE Evaluation of a novel noninvasive ICP monitoring device in patients undergoing invasive ICP monitoring: preliminary results Oliver Ganslandt, MD, 1 Stylianos Mourtzoukos, MD, 1 Andreas Stadlbauer, PhD, 2 Björn Sommer, MD, 2 and Rudolf Rammensee, MD 2 1 Department of Neurosurgery, Klinikum Stuttgart; and 2 Department of Neurosurgery, University of Erlangen, Germany OBJECTIVE There is no established method of noninvasive intracranial pressure (NI-ICP) monitoring that can serve as an alternative to the gold standards of invasive monitoring with external ventricular drainage or intraparenchymal monitoring. In this study a new method of NI-ICP monitoring performed using algorithms to determine ICP based on acoustic properties of the brain was applied in patients undergoing invasive ICP (I-ICP) monitoring, and the results were analyzed. METHODS In patients with traumatic brain injury and subarachnoid hemorrhage who were undergoing treatment in a neurocritical intensive care unit, the authors recorded ICP using the gold standard method of invasive external ventricular drainage or intraparenchymal monitoring. In addition, the authors simultaneously measured the ICP noninvasively with a device (the HS-1000) that uses advanced signal analysis algorithms for acoustic signals propagating through the cranium. To assess the accuracy of the NI-ICP method, data obtained using both I-ICP and NI-ICP monitoring methods were analyzed with MATLAB to determine the statistical significance of the differences between the ICP measurements obtained using NI-ICP and I-ICP monitoring. RESULTS Data were collected in 14 patients, yielding 2543 data points of continuous parallel ICP values in recordings obtained from I-ICP and NI-ICP. Each of the 2 methods yielded the same number of data points. For measurements at the 17 mm Hg cutoff, which was arbitrarily chosen for this preliminary analysis, the sensitivity and specificity for the NI-ICP monitoring were found to be and , respectively. Linear regression analysis indicated that there was a strong positive relationship between the measurements. Differential pressure between NI-ICP and I-ICP was within ± 3 mm Hg in 63% of data-paired readings and within ± 5 mm Hg in 85% of data-paired readings. The receiver operating characteristic area under the curve analysis revealed that the area under the curve was 0.895, corresponding to the overall performance of NI-ICP monitoring in comparison with I-ICP monitoring. CONCLUSIONS This study provides the first clinical data on the accuracy of the HS-1000 NI-ICP monitor, which uses advanced signal analysis algorithms to evaluate properties of acoustic signals traveling through the brain in patients undergoing I-ICP monitoring. The findings of this study highlight the capability of this NI-ICP device to accurately measure ICP noninvasively. Further studies should focus on clinical validation for elevated ICP values. KEY WORDS intracranial pressure monitoring; diagnostic technique; traumatic brain injury Recording and interpretation of intracranial pressure (ICP) is one of the most important diagnostic tools in neurosurgery and neurology. 9 There is growing evidence that ICP monitoring and protocol-driven therapy help to improve clinical outcome in a number of pathologies such as traumatic brain injury (TBI), brain infections such as meningitis, and brain tumors. 22 To date, ICP monitoring is still an invasive procedure in which a burr hole is used to introduce a transducer-coupled probe into the brain parenchyma or into the ventricles. Invasive ICP ABBREVIATIONS AUC = area under the curve; CPP = cerebral perfusion pressure; EVD = external ventricular drainage; I-ICP = invasive intracranial pressure; ICU = intensive care unit; IPM = intraparenchymal monitor; NI-ICP = noninvasive ICP; ONSD = optic nerve sheath diameter; ROC = receiver operating characteristic; TBI = traumatic brain injury. SUBMITTED September 27, ACCEPTED November 17, INCLUDE WHEN CITING Published online August 8, 2017; DOI: / JNS AANS, 2017 J Neurosurg August 8,
2 O. Ganslandt et al. monitoring coupled with the use of external ventricular drainage (EVD) is still considered the gold standard of ICP monitoring and is part of the standard patient management in the intensive care unit (ICU). 3,8,18,20,31,34 The invasive nature of this method and the methodology itself makes invasive ICP (I-ICP) monitoring both a potentially harmful and technically difficult technique. 17,23 The main concerns with using EVD include an associated high infection rate, which ranges from 3.4% to 32.2%; 7 the rate of malplacement of the ventricular catheter, which in one study was as high as 12.3%; 28 and the problem of technically inaccurate recordings due to calibration errors. 24 When considering the disadvantages of I-ICP monitoring, it is understandable that efforts have been made to introduce an alternative measure that would allow for noninvasive ICP (NI-ICP) monitoring performed using surrogate parameters that correspond to the ICP but can be recorded from the outside of the skull. Of these techniques, transcranial Doppler ultrasonography, 32 tympanic membrane displacement, 12 and optic nerve sheath diameter (ONSD) 19 have been investigated. However, all methods have distinctive limitations that have prevented them from being used as replacements for invasive monitoring. Raboel et al. stated that NI-ICP monitoring techniques are inaccurate and cannot be used as an alternative to invasive techniques. 24 In this study we investigated a new approach to NI-ICP monitoring. The NI-ICP monitor used in our study consists of a device (HS-1000; HeadSense Medical, Ltd.) that generates an acoustic signal that propagates through the cranium. The modulations of the signal in different physiological and pathophysiological conditions are processed using advanced signal analysis. The device displays the recorded ICP as quantitative data (in mm Hg) but is capable of analyzing a multitude of other parameters through evaluation of the respiratory and cardiac cycles and intracranial vessel properties, along with other parameters. In this study we focused on a correlative investigation in which ICP measurements obtained using the NI-ICP monitor were compared with those obtained using invasive EVD and intraparenchymal monitoring techniques. Methods Patients and/or next of kin consented to participation in this study. In most cases consent was given by next of kin and was later affirmed by the patient if possible. This was in congruence with the local ethics committee requirements. The study was approved by the local ethics committees of our institutions. The study design was a prospective parallel comparison of I-ICP and NI-ICP values. The I-ICP measurements were obtained with one of 2 methods, the EVD I-ICP monitor (Spiegelberg GmbH & Co. KG) or the intraparenchymal ICP monitor (IPM) (Codman ICP MicroSensor; Codman, Johnson & Johnson), and data from the 2 methods were combined. The NI-ICP values were obtained with the HS-1000 (HeadSense Medical, Ltd.). The study was performed at the Departments of Neurosurgery at the University Hospital of Erlangen and Klinikum Stuttgart. Fourteen patients were enrolled, all of whom were undergoing continuous I-ICP monitoring in a neurocritical ICU because of either TBI or subarachnoid hemorrhage. Data were collected and stored for further retrospective analysis of the pseudonymized digital recordings. Some of the patients were treated with EVD; continuous I-ICP monitoring was performed in conjunction with the EVD system as part of the standard ICU management. We also included patients in whom an IPM was used for I-ICP monitoring. All patients underwent NI- ICP monitoring. Exclusion criteria included ear disease or ear trauma, rhinorrhea or otorrhea, skull defect, pregnancy, and severe open head trauma, as well as age younger than 18 years. Throughout all parallel ICP monitoring sessions, each patient was positioned supine with the head placed at a 30 angle. Invasive ICP Monitoring The intraparenchymal monitoring involved intraparenchymal placement of a catheter. The pressure value, which was measured in mm Hg, was relayed electronically via a strain-gauge microchip located at the tip of the catheter, which was mounted in a titanium case at the tip of a 100-cm flexible nylon tube. 16 Ventricular ICP monitoring (performed with EVD) is considered a gold standard for ICP monitoring and has been described previously. 30 The EVD system is based on a probe, which is inserted via Kocher s point into the lateral ventricle and is used for both drainage of CSF and pressure monitoring. The EVD system diverts CSF by using a combination of gravity and intracerebral pressure. The drainage rate depends on the height at which the EVD system is placed relative to the patient s anatomy. When the EVD valve is closed, the ICP measurement is attainable. Continuous ICP monitoring cannot be performed during CSF drainage; when the EVD valve is open, the ICP value is not accurate and no measurements should be taken. In the present study, if the ventricular catheter was open for drainage, the line was closed and the system was allowed to equilibrate for 2 minutes before a reading was taken. Noninvasive ICP Monitoring For NI-ICP monitoring we used the HS-1000 device (HeadSense Medical Ltd.). This device uses advanced signal analysis algorithms that evaluate an acoustic signal. This signal includes a short beep at 66 db for approximately 6 seconds, which is emitted from the ipsilateral ear. It then propagates through the cranium and is detected together with other physiological sounds from the brain by the receiving sensor located in the contralateral ear. The HS-1000 data are continuously recorded in 6-second epochs on the corresponding device s monitor. At the end of signal transmission, the HS-1000 device s monitor is programmed to automatically take a snapshot of the I- ICP monitor screen or the patient s monitor (including date and time, ICP value in mm Hg, and blood pressure). These values are saved in a database for future comparative evaluations. Each NI-ICP monitoring session was approximately minutes long, as the patient s clinical condition permitted. The limiting factor for the length of the monitoring session was the patient s ability to tolerate closure of the EVD valve throughout the monitoring 2 J Neurosurg August 8, 2017
3 Noninvasive intracranial pressure monitoring session. In cases in which the patient s condition did not allow continuous recording (e.g., when the patient s CSF had to be drained or the patient s management required some form of intervention), the recording was stopped. It was resumed only when the patient s state allowed proper recording conditions (lying in a supine position without any movement or intervention from the clinicians). Once all recordings were complete, the ICP values from the I- ICP monitor were saved in the study s database. For purposes of analysis, ranges of I-ICP were formulated and the data pairs of I-ICP and NI-ICP were randomly sampled to accrue the number of values needed for analysis and to calculate sensitivity and specificity (Fig. 1). Parallel ICP Monitoring Each parallel monitoring interval in which both the NI- ICP and I-ICP methods were used consisted of between 30 minutes and 6 hours of aggregate recording performed either continuously or in separate recording sessions as the patient s condition allowed, which was repeated 3 times per day for up to 48 hours. There were a minimum of 3 to as many as 8640 data points per patient. Both EVD and intraparenchymal monitoring were assumed to be gold standards; we recorded in parallel from both of the I-ICP monitors and the NI-ICP monitor and compared the values. The raw data on acoustic signals collected by the HS (generated signal and accompanying physiological signals) were analyzed for approximately 5 seconds, and the NI-ICP value was calculated using a proprietary signal-processing algorithm and displayed to the user in mm Hg. Each NI-ICP monitoring cycle lasted approximately 15 seconds (including 6 seconds for the signal to be transmitted and received, approximately 5 seconds for snapshots to be taken, and 4 seconds for calculation of the ICP value). This translates to approximately 4 measurements per minute. We defined the mean ICP independent score as the corresponding I-ICP value that is determined every consecutive period of approximately 11 seconds as the sum of sample values divided by the number of samples. This is an acceptable time window compared with current state-of-the-art methodologies that range between 5 and 15 seconds in duration. During the test, no manipulations to change the ICP were done, and nothing was changed in the usual patient management protocols. Statistical Analysis Data were analyzed using MATLAB. Pearson correlation analysis of the I-ICP and NI-ICP values was completed to compare the ICP values from all devices. For 95% confidence, a p value 0.05 was considered statistically significant. The difference between the NI-ICP and I-ICP monitoring results was plotted against the mean of the 2 measures (I-ICP and NI-ICP). Receiver operating characteristics (ROCs) with the area under the curve (AUC) were calculated to present the tradeoff between sensitivity and specificity for all measurements at the 15 mm Hg cutoff. The AUC was calculated for all data points to provide an estimator for the cumulative measurements. Differential pressure (in mm Hg) was defined as the difference between I-ICP and NI-ICP per data point. The Bland-Altman FIG. 1. Photograph showing the HS-1000 device during a recording session. Figure is available in color online only. method was used to examine the percentages of total data points below the 6 mm Hg and 5 mm Hg differential pressure. The relationship of the paired data points was assessed using linear regression analysis, which showed the relationship between NI-ICP measurements and those obtained using the I-ICP. The slope of the line of best fit was used to examine the predictability of I-ICP from NI- ICP measurements. Results Parallel ICP Monitoring Fourteen patients met the study s inclusion criteria (Table 1); 1 patient was excluded because of a skull defect. The data from each patient were collected over a session of approximately 30 minutes to 1 hour. Throughout the study, no adverse effects were observed. ICP data were collected from all enrolled patients, yielding 2543 data points of continuous parallel ICP values in recordings obtained using I-ICP and NI-ICP devices. The I-ICP results reported are a combination of data obtained with the EVD (12 patients) and IPM (2 patients) I-ICP methods. Differences between I-ICP and NI-ICP readings (i.e., differential pressure of direct readings) were obtained. Differential pressures within ± 3 mm Hg were observed in 1606 (63%) readings, and differential pressures within ± 5 mm Hg were observed in 2154 (85%) readings. The numbers of measurements for each patient varied, but the mean ICP values were 10 ± 6.1 mm Hg (with a range of 0 26 mm Hg) and 9.5 ± 4.7 mm Hg (with a range of 0 21 mm Hg) for the I-ICP and NI-ICP measures, respectively. The ICP values from an I-ICP session were plotted against the NI-ICP values (Fig. 2). The trend plot revealed a Pearson r correlation of 0.82 between the measurements and a 95% CI for r of (p < ). A Bland-Altman plot, in which the difference between ICP readings obtained using the I-ICP and NI-ICP were plotted against the ICP as the average of the 2 methods, showed an average bias of 0.54 mm Hg, with 95% limits of agreement of -6.3 mm Hg and 7.38 mm Hg (Fig. 3). Linear regression analysis yields a line of best fit with the following equation: y = *x (Fig. 4). This J Neurosurg August 8,
4 O. Ganslandt et al. TABLE 1. Baseline characteristics of 14 patients enrolled in the ICP monitoring study Variable No. of Patients (%)* Sex Male 11 (79) Female 4 (29) Age range in yrs (14) (21) (43) (29) Diagnosis Subarachnoid hemorrhage 6 (43) Acute subdural hematoma 1 (7) Intracranial hemorrhage 6 (43) Malignant MCA infarction 1 (7) MCA = middle cerebral artery. * The totals for sex and age add up to 15, but 1 patient was excluded from monitoring because of a skull defect. equation best predicts the NI-ICP results from the I-ICP results. It also shows that there is a strong positive relationship between the measurements obtained with the NI-ICP and I-ICP devices. As presented in Fig. 5, ROC curve analysis revealed an AUC of 0.895, corresponding to overall performance of the NI-ICP to correctly identify I-ICP values. For measurements at the 17 mm Hg cutoff, which was arbitrarily chosen for this preliminary analysis, the sensitivity and specificity for the NI-ICP monitoring were found to be and , respectively. FIG. 2. Trend plot showing 2348 continuous parallel recordings of ICP values obtained from I-ICP compared with NI-ICP. Pearson r = 0.824, and 95% CI for r: (p < ). Figure is available in color online only. Discussion This study provides the first clinical data on the accuracy of the HS-1000 device (an NI-ICP monitor) in patients undergoing an I-ICP monitoring procedure for various clinical conditions resulting from TBI and/or SAH. The data points of continuous parallel recordings of ICP values were obtained from I-ICP and NI-ICP simultaneously. The overall findings showed that there was a good correlation between the measurements obtained with these 2 modalities (r = 0.82; p < ), revealing the potential of the noninvasive HS-1000 monitor for measurement of quantitative ICP. The average ICP readings for the I-ICP and NI- ICP methods were 10 ± 6.1 mm Hg and 9.5 ± 4.7 mm Hg, respectively. For measurements at the 17 mm Hg cutoff, sensitivity and specificity for the NI-ICP monitoring were and , respectively. Bias and agreement analysis performed using the Bland-Altman plot showed good concordance between the 2 measures. We have demonstrated a systematic way to incorporate NI-ICP monitoring via use of the HS-1000 device in a neurocritical ICU environment. Currently, I-ICP monitoring is a fundamental tool that provides primary surveillance management of patients in neurocritical ICUs. For the I-ICP measurement modality, probes are inserted into the brain parenchyma or ventricles. The predominant methods of invasive continuous ICP monitoring are performed via intraparenchymal or intraventricular probes. Arguably, the latter is considered the gold standard for ICP monitoring. The EVD system allows therapeutic CSF drainage and clearance of intraventricular blood. 2,14,27 More importantly, an elevated ICP is considered a medical emergency and can be managed medically via placement of an EVD system. The fundamental indication for management of elevated ICP is to prevent secondary ischemia due to the decrease in cerebral perfusion, which may lead to brain herniation. 3 The methodology of ICP monitoring via an EVD system is meant to allow continuous monitoring as well as drainage, but not to perform both simultaneously. The standard of care is to drain by opening the EVD valve (transducer) only for elevations at or above the 20 mm Hg threshold (ICP 20 mm Hg) and to relieve elevated ICP. In clinical practice, the EVD valve is kept closed for ICP measurements and to assess the continued need for CSF drainage. The inability of IPMs to allow drainage does not impede their usefulness in ICP monitoring, yet the accuracy level may be compromised when subjected to varying degrees of zero drift during the monitoring, due to the inherent inability to recalibrate the sensor in situ. 4,15 As for the indications, the ICP threshold at which herniation may occur is not absolute, and may vary between patients in regard to interindividual heterogeneity and the location of the intracranial mass lesion. 1 Cerebral perfusion can be monitored indirectly by measuring cerebral perfusion pressure (CPP), which is equal to the difference between mean arterial pressure and ICP. The CPP can be evaluated and managed by manipulation of arterial pressure, and is derived from ICP-monitored patients. 15 The above-mentioned threshold of 20 mm Hg is not a clear cutoff, yet it is considered a clinical target for ICP management for the treatment of severe TBI. Evidently, research supports ICP thresholds of mm Hg to promote investigation and treatment of elevated ICP. 5 Nevertheless, in a meta-analysis investigating ICP monitoring in patients with TBI, the authors concluded that it is still essential to identify the optimal threshold value of ICPdirected treatment, even in recent reviews of ICP monitor- 4 J Neurosurg August 8, 2017
5 Noninvasive intracranial pressure monitoring FIG. 3. Bland-Altman plot showing a good concordance between I-ICP and NI-ICP values. Figure is available in color online only. ing. 33 We introduced a new method for continuous NI-ICP monitoring and compared it to the main state-of-the-art methods currently available in neurocritical ICUs. Although, for reasons described below, we consider our NI-ICP modality to be highly accurate, our comparison was confined to protocol-driven management for elevated ICP, and therefore we were unable to compare data points when the patient s condition did not allow continuous recording. During this study, data collection was possible only when the EVD valve was closed, unless the patient s management protocol required some form of intervention (based on a diagnosis of elevated ICP). Therefore, we were FIG. 4. Linear regression analysis showing a strong positive relationship between the NI-ICP and I-ICP values. Figure is available in color online only. J Neurosurg August 8,
6 O. Ganslandt et al. FIG. 5. The ROC curve for all measurements. The AUC was Thd = threshold. Figure is available in color online only. able to obtain measurements within a range of 0 26 mm Hg (mean ICP 10 ± 6.1 mm Hg) or 0 21 mm Hg (mean ICP 9.5 ± 4.7 mm Hg) for the I-ICP and NI-ICP measures, respectively. Continuous ICP monitoring is of paramount importance for the treatment of elevated ICP; it is essential for maintaining a satisfactory CPP and to avoid inadequate oxygen delivery that may lead to secondary injury. Although ICP measurement is widely accepted as a core parameter in most neurocritical ICUs worldwide, invasive modalities have a number of drawbacks. The main challenge is that both intraparenchymal and intraventricular catheters have risks of complications; i.e., infection or postoperative hemorrhage. Moreover, invasive monitoring requires constant management and continuous monitoring, which may be burdensome to the ICU staff and in some cases may limit ICP monitoring. 21 The EVD system presents some clear advantages over intraparenchymal monitoring because it allows CSF drainage, which may significantly decrease the need for surgical decompression. 15 However, it is associated with a higher risk of infection compared with intraparenchymal monitoring. 26 As mentioned above, drainage requires opening the EVD valve (i.e., the mounted transducer) and exposing it to atmospheric pressure. Furthermore, drainage requires completing a zeroing procedure to obtain the zero reference point, which hinders the integrity of the sterile closed drainage system. This limits the accuracy of ICP reading to periods in which it is clinically possible to close the mounted transducer. 29 The accuracy of ICP readings via the EVD system is also dependent on maintaining the patient in a constant position where the transducer is fixed at the level of the foramen of Monro. This is done by creating an imaginary point of intersection between the ipsilateral medial canthus of the orbit and the tragus of the ear. 14 All of these considerations present significant drawbacks and limit the accuracy of the EVD system s ICP monitors. However, EVD devices are considered the most accurate, reliable, and cost-effective ICP monitoring methodology today, 2,15 with functional accuracy of 87%. 14 To overcome these obstacles, a variety of NI-ICP monitoring modalities have been explored in recent years, but according to several comparative analyses, none are as accurate as the invasive modalities. 24,27 Yet, as the results of these analyses indicate, some noninvasive modalities may yield more clinically useful results in the presence of elevated ICP: these include ultrasound and color Doppler ultrasonography. Ultrasound measures of the ONSD present a unique noninvasive tool for detecting ICP hypertension. Research suggests ONSD as a possible indicator of elevated ICP. The underlying principle states that an increase in ICP results in distension of the ONSD (millimetric increase) within seconds. The accepted consensus for an elevated ICP is ONSD above a threshold of 0.5 cm. 11,25 Rajajee et al. 25 conducted a comparison between ONSD and I-ICP measurements, EVD, and intraparenchymal monitoring, indicating that the optimal ONSD for detection of ICP 20 mm Hg was 0.48 cm (sensitivity 96% and specificity 94%). Spearman s correlation coefficient of an ONSD of 0.52 cm for detection of ICP 20 mm Hg was The main limitation of this method is that the measurement accuracy corresponds to the operator s experience and equipment, as well as the fact that the ONSD criterion (i.e., cutoff for ICP hypertension) is not well established. 13,25 All of the aforementioned drawbacks can be counterproductive to the implementation of this method and its effectiveness in ICUs. In this study, differences between data-paired readings were also calculated for each patient recording. Major differences in the mean ICP were first observed by Fernandes et al., who demonstrated sudden shifts in the mean ICP while simultaneously using 2 separate IPMs (1 Codman microsensor and 1 Camino fiberoptic device). 10 In our study, the differential pressure between NI-ICP and I-ICP was within ± 3 mm Hg in 63% of data-paired readings and within ± 5 mm Hg in 85% of data-paired readings. We believe these findings to be particularly interesting because similar differences have been reported for studies comparing 2 invasive modalities, intraventricular and intraparenchymal ICP. Chambers et al. reported similar results (79%) that were within ± 5 mm Hg for simultaneously comparisons of readings from the Spiegelberg transducer and the EVD system. 6 With the HS-1000, the mean difference between ICP readings obtained using the I-ICP and NI-ICP is plotted against the ICP as the average of the 2 methods, and shows an average bias of 0.54 mm Hg, with 95% limits of agreement of -6.3 mm Hg and 7.38 mm Hg. Similarly, reported comparisons between the EVD system and intraparenchymal monitoring measurements obtained using different modalities were consistent with the results of the mean ICP differences in our study. Lescot et al. found a bias of -0.6 mm Hg with 95% limits of agreement of -8.1 mm Hg and 6.9 mm Hg between the Pressio IPM and the EVD system, and 0.3 mm Hg and limits of agreement of -6.6 and 7.1 mm Hg between the Codman IPM and the EVD system J Neurosurg August 8, 2017
7 Noninvasive intracranial pressure monitoring Conclusions Further investigation of the HS-1000 ICP monitor should focus on the accuracy of elevated ICP values. The findings of this study highlight the capability of the HS to provide information about normal and elevated ICP levels in a clinical setting. The HS-1000 could be extremely beneficial as an adjunct modality by assisting clinicians in deciding if a patient requires an I-ICP monitor. It may also serve as a unique tool for continuous ICP monitoring, especially in third-world ICUs, in which the sanitation level and general care are not comparable to those in first-world, Western hospitals. The use of this NI- ICP monitoring device may help avoid the immediate risk of infection and/or hemorrhage associated with the use of I-ICP methods and reduce the morbidity and mortality rates in neurocritical ICUs. References 1. Andrews BT, Chiles BW III, Olsen WL, Pitts LH: The effect of intracerebral hematoma location on the risk of brain-stem compression and on clinical outcome. J Neurosurg 69: , Berlin T, Murray-Krezan C, Yonas H: Comparison of parenchymal and ventricular intracranial pressure readings utilizing a novel multi-parameter intracranial access system. Springerplus 4:10, Bhatia A, Gupta AK: Neuromonitoring in the intensive care unit. I. Intracranial pressure and cerebral blood flow monitoring. Intensive Care Med 33: , Bratton SL, Chestnut RM, Ghajar J, McConnell Hammond FF, Harris OA, Hartl R, et al: Guidelines for the management of severe traumatic brain injury. VII. Intracranial pressure monitoring technology. J Neurotrauma 24 (Suppl 1):S45 S54, 2007 (Erratum in J Neurotrauma 25: , 2008) 5. Bratton SL, Chestnut RM, Ghajar J, McConnell Hammond FF, Harris OA, Hartl R, et al: Guidelines for the management of severe traumatic brain injury. VIII. Intracranial pressure thresholds. J Neurotrauma 24 (Suppl 1):S55 S58, 2007 (Erratum in J Neurotrauma 25: , 2008) 6. Chambers IR, Siddique MS, Banister K, Mendelow AD: Clinical comparison of the Spiegelberg parenchymal transducer and ventricular fluid pressure. J Neurol Neurosurg Psychiatry 71: , Collins CD, Hartley JC, Chakraborty A, Thompson DN: Long subcutaneous tunnelling reduces infection rates in paediatric external ventricular drains. Childs Nerv Syst 30: , Cremer OL: Does ICP monitoring make a difference in neurocritical care? Eur J Anaesthesiol Suppl 42:87 93, Czosnyka M, Pickard JD: Monitoring and interpretation of intracranial pressure. J Neurol Neurosurg Psychiatry 75: , Fernandes HM, Bingham K, Chambers IR, Mendelow AD: Clinical evaluation of the Codman microsensor intracranial pressure monitoring system. Acta Neurochir Suppl 71:44 46, Galetta S, Byrne SF, Smith JL: Echographic correlation of optic nerve sheath size and cerebrospinal fluid pressure. J Clin Neuroophthalmol 9:79 82, Gwer S, Sheward V, Birch A, Marchbanks R, Idro R, Newton CR, et al: The tympanic membrane displacement analyser for monitoring intracranial pressure in children. Childs Nerv Syst 29: , Hightower S, Chin EJ, Heiner JD: Detection of increased intracranial pressure by ultrasound. J Spec Oper Med 12:19 22, Kakarla UK, Kim LJ, Chang SW, Theodore N, Spetzler RF: Safety and accuracy of bedside external ventricular drain placement. Neurosurgery 63 (1 Suppl 1):ONS162 ONS167, Kasotakis G, Michailidou M, Bramos A, Chang Y, Velmahos G, Alam H, et al: Intraparenchymal vs extracranial ventricular drain intracranial pressure monitors in traumatic brain injury: less is more? J Am Coll Surg 214: , Koskinen LO, Olivecrona M: Intracranial pressure monitoring using the Codman MicroSensor. Neurosurgery 67:221, 2010 (Letter) 17. Lescot T, Reina V, Le Manach Y, Boroli F, Chauvet D, Boch AL, et al: In vivo accuracy of two intraparenchymal intracranial pressure monitors. Intensive Care Med 37: , Lozier AP, Sciacca RR, Romagnoli MF, Connolly ES Jr: Ventriculostomy-related infections: a critical review of the literature. Neurosurgery 51: , Maissan IM, Dirven PJ, Haitsma IK, Hoeks SE, Gommers D, Stolker RJ: Ultrasonographic measured optic nerve sheath diameter as an accurate and quick monitor for changes in intracranial pressure. J Neurosurg 123: , March K: Intracranial pressure monitoring: why monitor? AACN Clin Issues 16: , McKeating EG, Andrews PJ, Tocher JI, Menon DK: The intensive care of severe head injury: a survey of non-neurosurgical centres in the United Kingdom. Br J Neurosurg 12:7 14, Padayachy LC, Figaji AA, Bullock MR: Intracranial pressure monitoring for traumatic brain injury in the modern era. Childs Nerv Syst 26: , Pople IK, Muhlbauer MS, Sanford RA, Kirk E: Results and complications of intracranial pressure monitoring in 303 children. Pediatr Neurosurg 23:64 67, Raboel PH, Bartek J Jr, Andresen M, Bellander BM, Romner B: Intracranial pressure monitoring: invasive versus non-invasive methods a review. Crit Care Res Pract 2012:950393, Rajajee V, Vanaman M, Fletcher JJ, Jacobs TL: Optic nerve ultrasound for the detection of raised intracranial pressure. Neurocrit Care 15: , Rebuck JA, Murry KR, Rhoney DH, Michael DB, Coplin WM: Infection related to intracranial pressure monitors in adults: analysis of risk factors and antibiotic prophylaxis. J Neurol Neurosurg Psychiatry 69: , Rosenberg JB, Shiloh AL, Savel RH, Eisen LA: Non-invasive methods of estimating intracranial pressure. Neurocrit Care 15: , Saladino A, White JB, Wijdicks EF, Lanzino G: Malplacement of ventricular catheters by neurosurgeons: a single institution experience. Neurocrit Care 10: , Schimpf MM: Diagnosing increased intracranial pressure. J Trauma Nurs 19: , Smith M: Monitoring intracranial pressure in traumatic brain injury. Anesth Analg 106: , Steiner LA, Andrews PJ: Monitoring the injured brain: ICP and CBF. Br J Anaesth 97:26 38, Wakerley BR, Kusuma Y, Yeo LL, Liang S, Kumar K, Sharma AK, et al: Usefulness of transcranial Dopplerderived cerebral hemodynamic parameters in the noninvasive assessment of intracranial pressure. J Neuroimaging 25: , Yuan Q, Wu X, Sun Y, Yu J, Li Z, Du Z, et al: Impact of intracranial pressure monitoring on mortality in patients with traumatic brain injury: a systematic review and metaanalysis. J Neurosurg 122: , 2015 J Neurosurg August 8,
8 O. Ganslandt et al. 34. Zhong J, Dujovny M, Park HK, Perez E, Perlin AR, Diaz FG: Advances in ICP monitoring techniques. Neurol Res 25: , 2003 Disclosures The authors report no conflict of interest concerning the materials or methods used in this study or the findings specified in this paper. Author Contributions Conception and design: Ganslandt. Acquisition of data: Ganslandt, Mourtzoukos, Sommer, Rammensee. Analysis and interpretation of data: all authors. Drafting the article: Ganslandt, Stadlbauer, Sommer, Rammensee. Critically revising the article: Ganslandt, Stadlbauer, Rammensee. Reviewed submitted version of manuscript: Ganslandt. Approved the final version of the manuscript on behalf of all authors: Ganslandt. Study supervision: Ganslandt. Correspondence Oliver Ganslandt, Klinikum Stuttgart, Katharinenhospital, Kriegsbergstrasse 60, Stuttgart 70174, Germany. klinikum-stuttgart.de. 8 J Neurosurg August 8, 2017
Comparison of parenchymal and ventricular intracranial pressure readings utilizing a novel multi-parameter intracranial access system
 Berlin et al. SpringerPlus 2015, 4:10 a SpringerOpen Journal RESEARCH Open Access Comparison of parenchymal and ventricular intracranial pressure readings utilizing a novel multi-parameter intracranial
Berlin et al. SpringerPlus 2015, 4:10 a SpringerOpen Journal RESEARCH Open Access Comparison of parenchymal and ventricular intracranial pressure readings utilizing a novel multi-parameter intracranial
Experimental evaluation of the Spiegelberg intracranial pressure and intracranial compliance monitor
 Neurosurg Focus 9 (5):Article 1, Journal of Neurosurgery Preview Article for December 2000, Click here to return to Table of Contents Experimental evaluation of the Spiegelberg intracranial pressure and
Neurosurg Focus 9 (5):Article 1, Journal of Neurosurgery Preview Article for December 2000, Click here to return to Table of Contents Experimental evaluation of the Spiegelberg intracranial pressure and
Traumatic brain Injury- An open eye approach
 Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Continuous cerebral autoregulation monitoring
 Continuous cerebral autoregulation monitoring Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Determinants of cerebral blood flow Thanks
Continuous cerebral autoregulation monitoring Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Determinants of cerebral blood flow Thanks
Neurocritical Care Monitoring. Academic Half Day Critical Care Fellows
 Neurocritical Care Monitoring Academic Half Day Critical Care Fellows Clinical Scenarios for CNS monitoring No Universally accepted Guidelines Traumatic Brain Injury Intracerebral Hemorrhage Subarachnoid
Neurocritical Care Monitoring Academic Half Day Critical Care Fellows Clinical Scenarios for CNS monitoring No Universally accepted Guidelines Traumatic Brain Injury Intracerebral Hemorrhage Subarachnoid
Stroke & Neurovascular Center of New Jersey. Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center
 Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Stroke & Neurovascular Center of New Jersey Jawad F. Kirmani, MD Director, Stroke and Neurovascular Center Past, present and future Past, present and future Cerebral Blood Flow Past, present and future
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and
 Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
Intracranial pressure: measurement and monitoring. CSF pressure as a golden standard. Intraparenchymal pressure. Sensors, drifts, errors and monitoring techniques GUILLAUME J, JANNY P. [Continuous intracranial
Medical Management of Intracranial Hypertension. Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center
 Medical Management of Intracranial Hypertension Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center Anatomic and Physiologic Principles Intracranial compartments Brain 80% (1,400
Medical Management of Intracranial Hypertension Joao A. Gomes, MD FAHA Head, Neurointensive Care Unit Cerebrovascular Center Anatomic and Physiologic Principles Intracranial compartments Brain 80% (1,400
APP Placement of ICP Monitors. Sanjay Patra, MD
 APP Placement of ICP Monitors Sanjay Patra, MD Can midlevel providers place external ventricular drains safely and accurately? Sanjay Patra MD MSc Director Epilepsy Surgery Director Brain Trauma Spectrum
APP Placement of ICP Monitors Sanjay Patra, MD Can midlevel providers place external ventricular drains safely and accurately? Sanjay Patra MD MSc Director Epilepsy Surgery Director Brain Trauma Spectrum
Diagnostic Accuracy of Optic Nerve Ultrasonography and Ophthalmoscopy in Prediction of Elevated Intracranial Pressure
 54 Emergency (2015); 3 (2): 54-58 ORIGINAL RESEARCH Diagnostic Accuracy of Optic Nerve Ultrasonography and Ophthalmoscopy in Prediction of Elevated Intracranial Pressure Keihan Golshani 1, Mehdi Ebrahim
54 Emergency (2015); 3 (2): 54-58 ORIGINAL RESEARCH Diagnostic Accuracy of Optic Nerve Ultrasonography and Ophthalmoscopy in Prediction of Elevated Intracranial Pressure Keihan Golshani 1, Mehdi Ebrahim
Original Research Paper ISSN : e- ISSN , p-issn X
 OPTIC NERVE SHEATH DIAMETER () MEASUREMENT WITH OPTIC NERVE ULTRASOUND (ONUS) IN THE EVALUATION OF ELEVATED INTRACRANIAL PRESSURE: A COMPARATIVE STUDY WITH CT SCAN IN HEAD TRAUMA PATIENTS. 1 Shreyas Patel,
OPTIC NERVE SHEATH DIAMETER () MEASUREMENT WITH OPTIC NERVE ULTRASOUND (ONUS) IN THE EVALUATION OF ELEVATED INTRACRANIAL PRESSURE: A COMPARATIVE STUDY WITH CT SCAN IN HEAD TRAUMA PATIENTS. 1 Shreyas Patel,
Update on Guidelines for Traumatic Brain Injury
 Update on Guidelines for Traumatic Brain Injury Current TBI Guidelines Shirley I. Stiver MD, PhD Department of Neurosurgery Guidelines for the management of traumatic brain injury Journal of Neurotrauma
Update on Guidelines for Traumatic Brain Injury Current TBI Guidelines Shirley I. Stiver MD, PhD Department of Neurosurgery Guidelines for the management of traumatic brain injury Journal of Neurotrauma
The use of intracranial pressure (ICP) monitoring in the
 Training Protocol for Intracranial Pressure Monitor Placement by Nonneurosurgeons: 5-Year Experience Kathryn Ko, MD, and Alicia Conforti, RN Background: This report evaluates a protocol for training nonneurosurgeon
Training Protocol for Intracranial Pressure Monitor Placement by Nonneurosurgeons: 5-Year Experience Kathryn Ko, MD, and Alicia Conforti, RN Background: This report evaluates a protocol for training nonneurosurgeon
Review Article Intracranial Pressure Monitoring: Invasive versus Non-Invasive Methods A Review
 Hindawi Publishing Corporation Critical Care Research and Practice Volume 2012, Article ID 950393, 14 pages doi:10.1155/2012/950393 Review Article Intracranial Pressure Monitoring: Invasive versus Non-Invasive
Hindawi Publishing Corporation Critical Care Research and Practice Volume 2012, Article ID 950393, 14 pages doi:10.1155/2012/950393 Review Article Intracranial Pressure Monitoring: Invasive versus Non-Invasive
Eide et al. Eide et al. BioMedical Engineering OnLine 2012, 11:66
 Simultaneous monitoring of static and dynamic intracranial pressure parameters from two separate sensors in patients with cerebral bleeds: comparison of findings Eide et al. Eide et al. BioMedical Engineering
Simultaneous monitoring of static and dynamic intracranial pressure parameters from two separate sensors in patients with cerebral bleeds: comparison of findings Eide et al. Eide et al. BioMedical Engineering
An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings
 An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings Eide and Sorteberg Eide and Sorteberg BioMedical Engineering
An intracranial pressure-derived index monitored simultaneously from two separate sensors in patients with cerebral bleeds: comparison of findings Eide and Sorteberg Eide and Sorteberg BioMedical Engineering
Point-of-care ultrasound for detecting elevated intracranial pressure in the field
 Point-of-care ultrasound for detecting elevated intracranial pressure in the field Stephen Aylward, Ph.D. 1, Sam Gerber, Ph.D. 1, Maeliss Jallais 1, Matt McCormick, Ph.D. 1 Sean Montgomery, M.D. 2 Luv
Point-of-care ultrasound for detecting elevated intracranial pressure in the field Stephen Aylward, Ph.D. 1, Sam Gerber, Ph.D. 1, Maeliss Jallais 1, Matt McCormick, Ph.D. 1 Sean Montgomery, M.D. 2 Luv
Accuracy of intracranial pressure monitoring: systematic review and metaanalysis
 Zacchetti et al. Critical Care (2015) 19:420 DOI 10.1186/s13054-015-1137-9 RESEARCH Accuracy of intracranial pressure monitoring: systematic review and metaanalysis Lucia Zacchetti 1, Sandra Magnoni 2,
Zacchetti et al. Critical Care (2015) 19:420 DOI 10.1186/s13054-015-1137-9 RESEARCH Accuracy of intracranial pressure monitoring: systematic review and metaanalysis Lucia Zacchetti 1, Sandra Magnoni 2,
Precision Medicine in Neurocritical Care: Should we individualize care?
 Precision Medicine in Neurocritical Care: Should we individualize care? Victoria McCredie Toronto Western Hospital Critical Care Canada Forum 2 nd November 2016 Conflicts of interest None Outline 1. Precision
Precision Medicine in Neurocritical Care: Should we individualize care? Victoria McCredie Toronto Western Hospital Critical Care Canada Forum 2 nd November 2016 Conflicts of interest None Outline 1. Precision
NON-INVASIVE ICP AND VRx AS NON-INVASIVE PRx Arminas Ragauskas
 ICM+ Workshop 2018 University of Cambridge NON-INVASIVE ICP AND VRx AS NON-INVASIVE PRx Arminas Ragauskas Disclosure A.R. - inventor and co-inventor of patented non-invasive ICP absolute value measurement
ICM+ Workshop 2018 University of Cambridge NON-INVASIVE ICP AND VRx AS NON-INVASIVE PRx Arminas Ragauskas Disclosure A.R. - inventor and co-inventor of patented non-invasive ICP absolute value measurement
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Early Experience of Automated Intraventricular Type Intracranial Pressure Monitoring (LiquoGuard ) for Severe Traumatic Brain Injury Patients
 CLINICAL ARTICLE Korean J Neurotrauma 2016;12(1):28-33 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2016.12.1.28 Early Experience of Automated Intraventricular Type Intracranial Pressure
CLINICAL ARTICLE Korean J Neurotrauma 2016;12(1):28-33 pissn 2234-8999 / eissn 2288-2243 http://dx.doi.org/10.13004/kjnt.2016.12.1.28 Early Experience of Automated Intraventricular Type Intracranial Pressure
Brain under pressure Managing ICP. Giuseppe
 Brain under pressure Managing ICP Giuseppe Citerio giuseppe.citerio@unimib.it @Dr_Cit Intro Thresholds Treating HICP Conclusions NO COI for this presentation Produces pressure gradients: herniation HIGH
Brain under pressure Managing ICP Giuseppe Citerio giuseppe.citerio@unimib.it @Dr_Cit Intro Thresholds Treating HICP Conclusions NO COI for this presentation Produces pressure gradients: herniation HIGH
Baseline pressure errors (BPEs) extensively influence intracranial pressure scores: results of a prospective observational study. Eide et al.
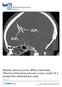 Baseline pressure errors (BPEs) extensively influence intracranial pressure scores: results of a prospective observational study Eide et al. Eide et al. BioMedical Engineering OnLine 2014, 13:7 Eide et
Baseline pressure errors (BPEs) extensively influence intracranial pressure scores: results of a prospective observational study Eide et al. Eide et al. BioMedical Engineering OnLine 2014, 13:7 Eide et
Transesophageal Echocardiography in Children: An Interactive Session on Common Congenital Cardiac Defects
 Transesophageal Echocardiography in Children: An Interactive Session on Common Congenital Cardiac Defects Wanda C. Miller-Hance, M.D. Objective: At the conclusion of this workshop the participant should
Transesophageal Echocardiography in Children: An Interactive Session on Common Congenital Cardiac Defects Wanda C. Miller-Hance, M.D. Objective: At the conclusion of this workshop the participant should
Monitoring of Regional Cerebral Blood Flow Using an Implanted Cerebral Thermal Perfusion Probe Archived Medical Policy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
The misplacement of external ventricular drain by freehand method in emergent neurosurgery
 Acta Neurol. Belg., 2011, 111, 22-28 Original articles The misplacement of external ventricular drain by freehand method in emergent neurosurgery Cheng-Ta HsieH 1,2, Guann-Juh CHen 1, Hsin-i Ma 1, Cheng-Fu
Acta Neurol. Belg., 2011, 111, 22-28 Original articles The misplacement of external ventricular drain by freehand method in emergent neurosurgery Cheng-Ta HsieH 1,2, Guann-Juh CHen 1, Hsin-i Ma 1, Cheng-Fu
Intracranial Pressure (ICP) Monitoring Market Research Report- Forecast to 2024
 Report Information More information from: https://www.marketresearchfuture.com/reports/703 Intracranial Pressure (ICP) Monitoring Market Research Report- Forecast to 2024 Report / Search Code: MRFR/HC/0232-CRR
Report Information More information from: https://www.marketresearchfuture.com/reports/703 Intracranial Pressure (ICP) Monitoring Market Research Report- Forecast to 2024 Report / Search Code: MRFR/HC/0232-CRR
Mannitol for Resuscitation in Acute Head Injury: Effects on Cerebral Perfusion and Osmolality
 Original articles Mannitol for Resuscitation in Acute Head Injury: Effects on Cerebral Perfusion and Osmolality J. A. MYBURGH*, S. B. LEWIS *Intensive Care Unit, Royal Adelaide Hospital, Adelaide, SOUTH
Original articles Mannitol for Resuscitation in Acute Head Injury: Effects on Cerebral Perfusion and Osmolality J. A. MYBURGH*, S. B. LEWIS *Intensive Care Unit, Royal Adelaide Hospital, Adelaide, SOUTH
S ome hydrocephalic patients with extracranial shunts
 PAPER Quantitative analysis of continuous intracranial pressure recordings in symptomatic patients with extracranial shunts P K Eide... Competing interests: none declared... Correspondence to: Dr Per Kristian
PAPER Quantitative analysis of continuous intracranial pressure recordings in symptomatic patients with extracranial shunts P K Eide... Competing interests: none declared... Correspondence to: Dr Per Kristian
perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP?
 7. Cerebral perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP? Douglas J. Miller Miller JD, Stanek A, Langfitt
7. Cerebral perfusion pressure: Definitions. Implication on management protocols. What happens when CPP is too low, and when it is too high? Non-invasive CPP? Douglas J. Miller Miller JD, Stanek A, Langfitt
Non-invasive assessment of intracranial pressure using ocular sonography in neurocritical care patients
 Intensive Care Med (2008) 34:2062 2067 DOI 10.1007/s00134-008-1149-x ORIGINAL Thomas Geeraerts Sybille Merceron Dan Benhamou Bernard Vigué Jacques Duranteau Non-invasive assessment of intracranial pressure
Intensive Care Med (2008) 34:2062 2067 DOI 10.1007/s00134-008-1149-x ORIGINAL Thomas Geeraerts Sybille Merceron Dan Benhamou Bernard Vigué Jacques Duranteau Non-invasive assessment of intracranial pressure
State of the Art Multimodal Monitoring
 State of the Art Multimodal Monitoring Baptist Neurological Institute Mohamad Chmayssani, MD Disclosures I have no financial relationships to disclose with makers of the products here discussed. Outline
State of the Art Multimodal Monitoring Baptist Neurological Institute Mohamad Chmayssani, MD Disclosures I have no financial relationships to disclose with makers of the products here discussed. Outline
Do Iatrogenic Factors Bias the Placement of External Ventricular Catheters? A Single Institute Experience and Review of the Literature
 Neurol Med Chir (Tokyo) 5, 8 86, Do Iatrogenic Factors Bias the Placement of External Ventricular Catheters? A Single Institute Experience and Review of the Literature Christoph M. WOERNLE, Jan-Karl BURKHARDT,
Neurol Med Chir (Tokyo) 5, 8 86, Do Iatrogenic Factors Bias the Placement of External Ventricular Catheters? A Single Institute Experience and Review of the Literature Christoph M. WOERNLE, Jan-Karl BURKHARDT,
Neuro Quiz 29 Transcranial Doppler Monitoring
 Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D Neuro Quiz 29 Transcranial Doppler Monitoring This
Verghese Cherian, MD, FFARCSI Penn State Hershey Medical Center, Hershey Quiz Team Shobana Rajan, M.D Suneeta Gollapudy, M.D Angele Marie Theard, M.D Neuro Quiz 29 Transcranial Doppler Monitoring This
Noninvasive estimation of intracranial pressure using TCD
 Noninvasive estimation of intracranial pressure using TCD Background: Transcranial Doppler-derived indices of cerebral autoregulation are related to outcome after head injury. TCD measurements on patients
Noninvasive estimation of intracranial pressure using TCD Background: Transcranial Doppler-derived indices of cerebral autoregulation are related to outcome after head injury. TCD measurements on patients
INVASIVE VS NON-INVASIVE ICP MONITORING BASED ON A COMBINATION OF ONSD AND TCD METHODS IN BRAIN INJURED PATIENTS
 INVASIVE VS NON-INVASIVE ICP MONITORING BASED ON A COMBINATION OF ONSD AND TCD METHODS IN BRAIN INJURED PATIENTS Study protocol TABLE OF CONTENTS 1. LIST OF ABBREVIATIONS AND RELEVANT DEFINITIONS...4 2.
INVASIVE VS NON-INVASIVE ICP MONITORING BASED ON A COMBINATION OF ONSD AND TCD METHODS IN BRAIN INJURED PATIENTS Study protocol TABLE OF CONTENTS 1. LIST OF ABBREVIATIONS AND RELEVANT DEFINITIONS...4 2.
External ventricular drain (EVD) placement for cerebrospinal. FOCUS Neurosurg Focus 43 (5):E5, 2017
 NEUROSURGICAL FOCUS Neurosurg Focus 43 (5):E5, 2017 Real-time ultrasound-guided external ventricular drain placement: technical note James H. Manfield, MBBS, MSc, MRCS, 1 and Kenny K. H. Yu, MBBS, MRCS,
NEUROSURGICAL FOCUS Neurosurg Focus 43 (5):E5, 2017 Real-time ultrasound-guided external ventricular drain placement: technical note James H. Manfield, MBBS, MSc, MRCS, 1 and Kenny K. H. Yu, MBBS, MRCS,
Department of Neurology, University of California, San Francisco, California
 J Neurosurg 120:901 907, 2014 AANS, 2014 Assessment of a noninvasive cerebral oxygenation monitor in patients with severe traumatic brain injury Clinical article Guy Rosenthal, M.D., 1 Alex Furmanov, R.N.,
J Neurosurg 120:901 907, 2014 AANS, 2014 Assessment of a noninvasive cerebral oxygenation monitor in patients with severe traumatic brain injury Clinical article Guy Rosenthal, M.D., 1 Alex Furmanov, R.N.,
What is elevated ICP?
 What is elevated ICP? and When should it be treated? David Menon Professor of Anaesthesia, University of Cambridge ICP monitoring recommended to reduce inhospital & 2-wk mortality Rx ICP > 22 mm Hg as
What is elevated ICP? and When should it be treated? David Menon Professor of Anaesthesia, University of Cambridge ICP monitoring recommended to reduce inhospital & 2-wk mortality Rx ICP > 22 mm Hg as
Cerebral autoregulation is a complex intrinsic control. Time course for autoregulation recovery following severe traumatic brain injury
 J Neurosurg 111:695 700, 2009 Time course for autoregulation recovery following severe traumatic brain injury Clinical article Gi l l E. Sv i r i, M.D., M.Sc., 1 Ru n e Aa s l i d, Ph.D., 2 Co l l e e
J Neurosurg 111:695 700, 2009 Time course for autoregulation recovery following severe traumatic brain injury Clinical article Gi l l E. Sv i r i, M.D., M.Sc., 1 Ru n e Aa s l i d, Ph.D., 2 Co l l e e
Body position and eerebrospinal fluid pressure. Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point
 Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Body position and eerebrospinal fluid pressure Part 2' Clinical studies on orthostatic pressure and the hydrostatic indifferent point BJORN MAGNAES, M.D. Department of Neurosurgery, Rikshospitalet, Oslo
Complications of intracranial pressure monitoring in children with head trauma
 J Neurosurg (Pediatrics 2) 101:53 58, 2004 Complications of intracranial pressure monitoring in children with head trauma RICHARD C. E. ANDERSON, M.D., PETER KAN, M.D., PAUL KLIMO, M.D., M.P.H., DOUGLAS
J Neurosurg (Pediatrics 2) 101:53 58, 2004 Complications of intracranial pressure monitoring in children with head trauma RICHARD C. E. ANDERSON, M.D., PETER KAN, M.D., PAUL KLIMO, M.D., M.P.H., DOUGLAS
Lisa T. Hannegan, MS, CNS, ACNP. Department of Neurological Surgery University of California, San Francisco
 Lisa T. Hannegan, MS, CNS, ACNP Department of Neurological Surgery University of California, San Francisco Era of Clinical Neuro Monitoring Clinical Examination Heart rate Blood Pressure Body temperature
Lisa T. Hannegan, MS, CNS, ACNP Department of Neurological Surgery University of California, San Francisco Era of Clinical Neuro Monitoring Clinical Examination Heart rate Blood Pressure Body temperature
Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples.
 Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples. Optimization of cerebral perfusion pressure: Relationship
Pressure reactivity: Relationship between ICP and arterial blood pressure (ABP). Pressure-reactivity index, computational methods. Clinical examples. Optimization of cerebral perfusion pressure: Relationship
Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections in Patients with Hydrocephalus
 The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
The Scientific World Journal Volume 2013, Article ID 461896, 4 pages http://dx.doi.org/10.1155/2013/461896 Clinical Study The Value of Programmable Shunt Valves for the Management of Subdural Collections
Improving TBI outcome
 Improving TBI outcome Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Background Stein, S. C., Georgoff, P., et al. (2010). Journal of Neurotrauma
Improving TBI outcome Dr Peter Smielewski ps10011@cam.ac.uk 20/10/2017 Division of Neurosurgery, Department of Clinical Neurosciences Background Stein, S. C., Georgoff, P., et al. (2010). Journal of Neurotrauma
GLYCEMIC CONTROL IN NEUROCRITICAL CARE PATIENTS
 GLYCEMIC CONTROL IN NEUROCRITICAL CARE PATIENTS David Zygun MD MSc FRCPC Professor and Director Division of Critical Care Medicine University of Alberta Zone Clinical Department Head Critical Care Medicine,
GLYCEMIC CONTROL IN NEUROCRITICAL CARE PATIENTS David Zygun MD MSc FRCPC Professor and Director Division of Critical Care Medicine University of Alberta Zone Clinical Department Head Critical Care Medicine,
ICP (Intracranial Pressure) Monitoring Brain Tissue Oxygen Monitoring Jugular Venous Bulb Oximetry
 ICP (Intracranial Pressure) Monitoring Secondary brain injury may be a direct consequence of intracranial hypertension. Therefore monitoring of ICP and cerebral perfusion pressure (CPP) are immediate priority
ICP (Intracranial Pressure) Monitoring Secondary brain injury may be a direct consequence of intracranial hypertension. Therefore monitoring of ICP and cerebral perfusion pressure (CPP) are immediate priority
Postanesthesia Care of the Patient Suffering From Traumatic Brain Injury
 Postanesthesia Care of the Patient Suffering From Traumatic Brain Injury By: Susan Letvak, PhD, RN Rick Hand, CRNA, DNSc Letvak, S. & Hand, R. (2003). Postanesthesia care of the traumatic brain injured
Postanesthesia Care of the Patient Suffering From Traumatic Brain Injury By: Susan Letvak, PhD, RN Rick Hand, CRNA, DNSc Letvak, S. & Hand, R. (2003). Postanesthesia care of the traumatic brain injured
Current bedside monitors of brain blood flow and oxygen delivery
 24. Brain Chemistry Current bedside monitors of brain blood flow and oxygen delivery Global monitors Cannot detect regional abnormalities Local monitors Sample only a small region of the brain and highly
24. Brain Chemistry Current bedside monitors of brain blood flow and oxygen delivery Global monitors Cannot detect regional abnormalities Local monitors Sample only a small region of the brain and highly
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
TCD IN THE NICU, PICU AND OTHER APPLICATIONS. Dorothy Bulas M.D. Professor of Pediatrics & Radiology Children s National Washington D.C.
 TCD IN THE NICU, PICU AND OTHER APPLICATIONS Dorothy Bulas M.D. Professor of Pediatrics & Radiology Children s National Washington D.C. Objectives Recognize normal and abnormal cranial blood flow patterns
TCD IN THE NICU, PICU AND OTHER APPLICATIONS Dorothy Bulas M.D. Professor of Pediatrics & Radiology Children s National Washington D.C. Objectives Recognize normal and abnormal cranial blood flow patterns
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Integra B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE
 Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Integra 110-4B: Camino OLM Intracranial Pressure Monitoring Kit SURGICAL TECHNIQUE Surgical Technique Th OLM ICP Kit was developed in cooperation with Richard C. Ostrup, M.D., Thomas G. Luerssen, M.D.
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Agreement Between Computed Tomography And Magnetic Resonance Imaging In Measuring Optic Nerve Sheath Diameter
 Global Journal of Health Science; Vol. 10, No. 4; 2018 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Agreement Between Computed Tomography And Magnetic Resonance
Global Journal of Health Science; Vol. 10, No. 4; 2018 ISSN 1916-9736 E-ISSN 1916-9744 Published by Canadian Center of Science and Education Agreement Between Computed Tomography And Magnetic Resonance
Infusion studies in clinical practice. Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London
 Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
Infusion studies in clinical practice Kristian Aquilina Consultant paediatric neurosurgeon Great Ormond Street Hospital London 10 th September 2018 infusion study + hydrocephalus 216 publications Clinical
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery
 Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
Neurosurgery Review. Mudit Sharma, MD May 16 th, 2008
 Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Neurosurgery Review Mudit Sharma, MD May 16 th, 2008 Dr. Mudit Sharma, Neurosurgeon Manassas, Fredericksburg, Virginia http://www.virginiaspinespecialists.com Phone: 1-855-SPINE FIX (774-6334) Fundamentals
Any closer to evidence based practice? Asma Salloo Chris Hani Baragwantah Academic Hospital University of Witwatersrand
 Any closer to evidence based practice? Asma Salloo Chris Hani Baragwantah Academic Hospital University of Witwatersrand Evidence Pathophysiology Why? Management Non-degenerative, Non-congenital insult
Any closer to evidence based practice? Asma Salloo Chris Hani Baragwantah Academic Hospital University of Witwatersrand Evidence Pathophysiology Why? Management Non-degenerative, Non-congenital insult
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Management of Traumatic Brain Injury (and other neurosurgical emergencies)
 Management of Traumatic Brain Injury (and other neurosurgical emergencies) Laurel Moore, M.D. University of Michigan 22 nd Annual Review February 7, 2019 Greetings from Michigan! Objectives for Today s
Management of Traumatic Brain Injury (and other neurosurgical emergencies) Laurel Moore, M.D. University of Michigan 22 nd Annual Review February 7, 2019 Greetings from Michigan! Objectives for Today s
Chapter 8: Cerebral protection Stephen Lo
 Chapter 8: Cerebral protection Stephen Lo Introduction There will be a variety of neurological pathologies that you will see within the intensive care. The purpose of this chapter is not to cover all neurological
Chapter 8: Cerebral protection Stephen Lo Introduction There will be a variety of neurological pathologies that you will see within the intensive care. The purpose of this chapter is not to cover all neurological
Traumatic brain injury (TBI) remains a lethal injury. Marked reduction in mortality in patients with severe traumatic brain injury.
 J Neurosurg 119:1583 1590, 2013 AANS, 2013 Marked reduction in mortality in patients with severe traumatic brain injury Clinical article Linda M. Gerber, Ph.D., 1 Ya-Lin Chiu, M.S., 1 Nancy Carney, Ph.D.,
J Neurosurg 119:1583 1590, 2013 AANS, 2013 Marked reduction in mortality in patients with severe traumatic brain injury Clinical article Linda M. Gerber, Ph.D., 1 Ya-Lin Chiu, M.S., 1 Nancy Carney, Ph.D.,
excellence in care Procedure Neuroprotection For Review Aug 2015
 Neuro Projection HELI.CLI.14 Purpose This procedure outlines the management principles of patients being retrieved with traumatic brain injury (TBI), spontaneous intracranial haemorrhage (including subarachnoid
Neuro Projection HELI.CLI.14 Purpose This procedure outlines the management principles of patients being retrieved with traumatic brain injury (TBI), spontaneous intracranial haemorrhage (including subarachnoid
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: INTRACRANIAL PRESSURE MONITORING USING ICP CODMAN DEVICE MONITORING BOLT AND INTRACRANIAL PRESSURE MONITORING DRAINAGE OF CEREBRAL SPINAL
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: INTRACRANIAL PRESSURE MONITORING USING ICP CODMAN DEVICE MONITORING BOLT AND INTRACRANIAL PRESSURE MONITORING DRAINAGE OF CEREBRAL SPINAL
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
CATCH A WAVE.. INTRODUCTION NONINVASIVE HEMODYNAMIC MONITORING 4/12/2018
 WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
Hemorrhage Rates Associated with Two Methods of Ventriculostomy: External Ventricular Drainage vs. Ventriculoperitoneal Shunt Procedure
 ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 545 551, 2014 doi: 10.2176/nmc.oa.2013-0178 Online February 10, 2014 Hemorrhage Rates Associated with Two Methods of Ventriculostomy: External Ventricular Drainage
ORIGINAL ARTICLE Neurol Med Chir (Tokyo) 54, 545 551, 2014 doi: 10.2176/nmc.oa.2013-0178 Online February 10, 2014 Hemorrhage Rates Associated with Two Methods of Ventriculostomy: External Ventricular Drainage
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS.
 External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
External Ventricular Drainage & Lumbar Drainage Procedure and Care. Amey R. Savardekar Assistant Professor Neurosurgery, NIMHANS. External Ventricular Drain Indications: Therapeutic (To relieve raised
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
11. Traumatic brain injury. Links between ICP, CPP, PRx monitoring and outcome after TBI. Does CT picture help in prediction of outcome?
 11. Traumatic brain injury. Links between ICP, CPP, PRx monitoring and outcome after TBI. Does CT picture help in prediction of outcome? Critical levels of CPP, ICP and PRx Percentage of patients in outcome
11. Traumatic brain injury. Links between ICP, CPP, PRx monitoring and outcome after TBI. Does CT picture help in prediction of outcome? Critical levels of CPP, ICP and PRx Percentage of patients in outcome
TCD in Intensive Care
 TCD in Intensive Care Background: Transcranial Doppler (TCD) ultrasonography is a technique that uses a hand-held Doppler transducer (placed on the surface of the cranial skin) to measure the velocity
TCD in Intensive Care Background: Transcranial Doppler (TCD) ultrasonography is a technique that uses a hand-held Doppler transducer (placed on the surface of the cranial skin) to measure the velocity
Aneurysmal Subarachnoid Hemorrhage Presentation and Complications
 Aneurysmal Subarachnoid Hemorrhage Presentation and Complications Sherry H-Y. Chou MD MMSc FNCS Department of Critical Care Medicine, Neurology and Neurosurgery University of Pittsburgh School of Medicine
Aneurysmal Subarachnoid Hemorrhage Presentation and Complications Sherry H-Y. Chou MD MMSc FNCS Department of Critical Care Medicine, Neurology and Neurosurgery University of Pittsburgh School of Medicine
Traumatic Brain Injury Pathways for Adult ED Patients Being Admitted to Trauma Service
 tic Brain Injury Pathways for Adult ED Patients Being Admitted to Service Revision Team Tyler W. Barrett, MD, MSCI Elizabeth S. Compton, NP Bradley M. Dennis, MD Oscar D. Guillamondegui, MD, MPH Michael
tic Brain Injury Pathways for Adult ED Patients Being Admitted to Service Revision Team Tyler W. Barrett, MD, MSCI Elizabeth S. Compton, NP Bradley M. Dennis, MD Oscar D. Guillamondegui, MD, MPH Michael
Accuracy of the Free Hand Placement of an External Ventricular Drain (EVD)
 KOR J CEREBROVASCULAR SURGERY June 2O10 Vol. 12 No 2, page 82-6 Accuracy of the Free Hand Placement of an External Ventricular Drain (EVD) Department of Neurosurgery, Gachon University of Medicine & Science,
KOR J CEREBROVASCULAR SURGERY June 2O10 Vol. 12 No 2, page 82-6 Accuracy of the Free Hand Placement of an External Ventricular Drain (EVD) Department of Neurosurgery, Gachon University of Medicine & Science,
CV frequently results in devastating neurologic outcomes
 Published March 15, 2012 as 10.3174/ajnr.A2971 CLINICAL REPORT E.M. Deshaies W. Jacobsen A. Singla F. Li R. Gorji Brain Tissue Oxygen Monitoring to Assess Reperfusion after Intra-Arterial Treatment of
Published March 15, 2012 as 10.3174/ajnr.A2971 CLINICAL REPORT E.M. Deshaies W. Jacobsen A. Singla F. Li R. Gorji Brain Tissue Oxygen Monitoring to Assess Reperfusion after Intra-Arterial Treatment of
Edinburgh Imaging Academy online distance learning courses. Statistics
 Statistics Semester 1 / Autumn 10 Credits Each Course is composed of Modules & Activities. Modules: Introduction to Statistics IMSc NI4R How to Read a Paper IMSc NI4R Assessing the Accuracy of Diagnostic
Statistics Semester 1 / Autumn 10 Credits Each Course is composed of Modules & Activities. Modules: Introduction to Statistics IMSc NI4R How to Read a Paper IMSc NI4R Assessing the Accuracy of Diagnostic
A comparison between the transfer function of ABP to ICP and compensatory reserve index in TBI
 Acta Neurochir Suppl (28) 12: 9 13 # Springer-Verlag 28 A comparison between the transfer function of AB to IC and compensatory reserve index in TBI Sima Shahsavari & Tomas McKelvey & Thomas Skoglund &
Acta Neurochir Suppl (28) 12: 9 13 # Springer-Verlag 28 A comparison between the transfer function of AB to IC and compensatory reserve index in TBI Sima Shahsavari & Tomas McKelvey & Thomas Skoglund &
The management of ICH when to operate when not to?
 The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
The management of ICH when to operate when not to? Intracranial Hemorrhage High Incidence o Accounts for 10-15% of all strokes 1,2,5 o 80,000 cases in US; 2 million WW 2,5 o Incidence doubles for African-
Clinical Study Optic Nerve Sonography in the Diagnostic Evaluation of Pseudopapilledema and Raised Intracranial Pressure: A Cross-Sectional Study
 Neurology Research International Volume 2015, Article ID 146059, 4 pages http://dx.doi.org/10.1155/2015/146059 Clinical Study Optic Nerve Sonography in the Diagnostic Evaluation of Pseudopapilledema and
Neurology Research International Volume 2015, Article ID 146059, 4 pages http://dx.doi.org/10.1155/2015/146059 Clinical Study Optic Nerve Sonography in the Diagnostic Evaluation of Pseudopapilledema and
Optimum sodium levels in children with brain injury. Professor Sunit Singhi, Head, Department of Pediatrics, Head, Pediatric
 India Optimum sodium levels in children with brain injury Professor Sunit Singhi, Head, Department of Pediatrics, Head, Pediatric Sodium and brain Sodium - the major extracellular cation and most important
India Optimum sodium levels in children with brain injury Professor Sunit Singhi, Head, Department of Pediatrics, Head, Pediatric Sodium and brain Sodium - the major extracellular cation and most important
Continuous Peritransplant Assessment of Consciousness using Bispectral Index Monitoring for Patients with Fulminant Hepatic Failure
 Continuous Peritransplant Assessment of Consciousness using Bispectral Index Monitoring for Patients with Fulminant Hepatic Failure Purpose: Deterioration of consciousness is the most critical problem
Continuous Peritransplant Assessment of Consciousness using Bispectral Index Monitoring for Patients with Fulminant Hepatic Failure Purpose: Deterioration of consciousness is the most critical problem
Transfusion & Mortality. Philippe Van der Linden MD, PhD
 Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
Transfusion & Mortality Philippe Van der Linden MD, PhD Conflict of Interest Disclosure In the past 5 years, I have received honoraria or travel support for consulting or lecturing from the following companies:
DISCLOSURES. Specific TCD clinical applications for patients with traumatic brain injury 1/10/2015. FTE, Private Practice for profit TBI TBI: SCOPE
 DISCLOSURES Specific TCD clinical applications for patients with traumatic brain injury FTE, Private Practice for profit Alexander Razumovsky, PhD, FAHA 38 35 th Annual Meeting 38 35 th Annual Meeting
DISCLOSURES Specific TCD clinical applications for patients with traumatic brain injury FTE, Private Practice for profit Alexander Razumovsky, PhD, FAHA 38 35 th Annual Meeting 38 35 th Annual Meeting
R Adams Cowley Founder of the R Adams Cowley Shock Trauma Center and Maryland EMS System in Baltimore, Maryland.
 R Adams Cowley 1917 -- 1991 Founder of the R Adams Cowley Shock Trauma Center and Maryland EMS System in Baltimore, Maryland. ...That the primary purpose of medicine was to save lives, that every critically
R Adams Cowley 1917 -- 1991 Founder of the R Adams Cowley Shock Trauma Center and Maryland EMS System in Baltimore, Maryland. ...That the primary purpose of medicine was to save lives, that every critically
NEUROSURGERY LiquoGuard
 NEUROSURGERY LiquoGuard Member of CENTROTEC Group a new InTRODUCTION TO LiquoGuard CSF Management LiquoGuard (Liquor = German for CSF) represents a revolutionary step in CSF drainage, maximizing patient
NEUROSURGERY LiquoGuard Member of CENTROTEC Group a new InTRODUCTION TO LiquoGuard CSF Management LiquoGuard (Liquor = German for CSF) represents a revolutionary step in CSF drainage, maximizing patient
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation
 J Neurosurg 94:392 396, 2001 Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation ANDERS EKLUND, MSC.E.P., AINA ÅGREN-WILSSON, M.D.,
J Neurosurg 94:392 396, 2001 Two computerized methods used to analyze intracranial pressure B waves: comparison with traditional visual interpretation ANDERS EKLUND, MSC.E.P., AINA ÅGREN-WILSSON, M.D.,
9/16/2018. Recognizing & Managing Seizures in Pediatric TBI. Objectives. Definitions and Epidemiology
 Recognizing & Managing Seizures in Pediatric TBI UW Medicine EMS & Trauma 2018 Conference September 17 and 18, 2018 Mark Wainwright MD PhD Herman and Faye Sarkowsky Professor of Neurology Division Head,
Recognizing & Managing Seizures in Pediatric TBI UW Medicine EMS & Trauma 2018 Conference September 17 and 18, 2018 Mark Wainwright MD PhD Herman and Faye Sarkowsky Professor of Neurology Division Head,
PVDOMICS: Right Heart Catheterization Training
 PVDOMICS: Right Heart Catheterization Training Cardiovascular Physiology Core Cleveland Clinic, Cleveland OH November 7, 2016 NHLBI Pulmonary Vascular Disease Phenomics Program Funded by the National Heart,
PVDOMICS: Right Heart Catheterization Training Cardiovascular Physiology Core Cleveland Clinic, Cleveland OH November 7, 2016 NHLBI Pulmonary Vascular Disease Phenomics Program Funded by the National Heart,
Chapter 57: Nursing Management: Acute Intracranial Problems
 Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
Chapter 57: Nursing Management: Acute Intracranial Problems NORMAL INTRACRANIAL PRESSURE Intracranial pressure (ICP) is the hydrostatic force measured in the brain CSF compartment. Normal ICP is the total
Supratentorial cerebral arteriovenous malformations : a clinical analysis
 Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
Original article: Supratentorial cerebral arteriovenous malformations : a clinical analysis Dr. Rajneesh Gour 1, Dr. S. N. Ghosh 2, Dr. Sumit Deb 3 1Dept.Of Surgery,Chirayu Medical College & Research Centre,
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
Insertion of an external ventricular drain (EVD) is a
 Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Short Communication Intracerebral Hemorrhage With Severe Ventricular Involvement Lumbar Drainage for Communicating Hydrocephalus Hagen B. Huttner, MD; Simon Nagel, MD; Elena Tognoni; Martin Köhrmann, MD;
Online Supplementary Appendix
 Online Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lehman * LH, Saeed * M, Talmor D, Mark RG, and Malhotra
Online Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Lehman * LH, Saeed * M, Talmor D, Mark RG, and Malhotra
