Chapter 44 Neck Trauma
|
|
|
- Peter Hodges
- 6 years ago
- Views:
Transcription
1 Chapter 44 Neck Trauma Episode Overview: 1) Describe the landmarks and structures using the Zones of the neck & the Triangles of neck 2) List 6 hard and 6 soft signs of penetrating neck trauma. What are the indications for immediate OR vs CTA in managing penetrating neck trauma 3) Describe an approach to managing acute neck trauma in the ER 4) Describe the management of venous air embolism 5) Describe techniques for airway management in penetrating neck trauma 6) Describe the management of suspected pharyngoesophageal trauma. What are signs of esophageal injury? 7) List 3 hard signs of laryngotracheal trauma and describe airway management dilemmas Wisecracks: 1) Differentiate between choking, hanging and strangulation 2) Define judicial and non-judicial hanging and describe expected injury patterns Rosen s in Perspective Wide range of complications from minor wounds to severe hemorrhage, neurologic injury, to airway compromise Apparently stable patients can harbour life threatening injuries Three mechanisms of neck trauma: 1. Blunt 2. Penetrating 3. Strangulation / near hanging Four anatomic injury areas: 1. Laryngotracheal - airway 2. Pharynx oesophageal - digestive tract 3. Vascular system 4. Neurologic system Principles of Disease
2 Penetrating trauma: Aetiologies: o GSW s: High velocity: rifles > 2000 ft/s Have very predictable direct pathways through tissue: produce a large blast effect Can produce a cavitation effect (if >1100 ft/s) Cavitation: an immediate release of kinetic energy as the bullet enters the tissue- creating extensive soft tissue damage. Low velocity: handguns and air rifles: Bone penetration occurs at 300 ft/s These produce erratic pathways: with no direct relationship between entrance and exit wounds stab wounds, impalement, shrapnel Low energy injuries produce much less severe mechanisms of injury Many of these do not need surgical management Mortality 2-6% - from exsanguination Blunt trauma: From MVCs, clothesline injuries, strangulation, sports injuries Blunt vascular injuries are RARE, but often missed Blunt injuries to the aero digestive & vascular tracts are rare - but present in a delayed way with devastating consequences 1) Describe the landmarks and structures using the Zones of the neck & the Triangles of neck ANATOMY: Densely packed tissues with vital structures: vascular injury can be tamponaded by fascial planes and neighbouring structures can be massively distorted. Two fascial layers cover the neck: a. Superficial fascia: This layer COVERS the platysma muscle, and is just below the skin Because the platysma muscle is sandwiched between both fascial layers: its violation suggests deep structure injuries Blind probing of neck wounds is discouraged - due to clot disruption possibilities b. Deep cervical fascia Has three parts: all three form to make the carotid sheath Investing layer: Surrounds the neck and encases SCLM and trapezius muscles Pre-tracheal layer: Adheres to the cricoid and thyroid cartilages travels to sternum and inserts on the anterior pericardium *****missed aerodigestive injuries: can lead to mediastinitis
3 Pre-vertebral layer: Envelops the pre-vertebral muscles to form the Axillary sheath and covers the subclavian artery Two ways of describing the neck: ZONES APPROACH I: thoracic outlet Sternal notch/clavicles -> cricoid cartilage Thoracic, mediastinal, neck structures affected. II: mid neck Cricoid cartilage angle of the mandible Easier surgical control and exploration III : upper neck: Angle of the mandible to the base of the skull Difficult surgical access and control TRIANGLES APPROACH Anterior triangle: Contains neurovascular. And aero digestive tracts: Midline -- sternocleidomastoid muscle -- lower edge of the mandible Posterior triangle: Sternocleidomastoid muscle - clavicle - trapezius muscle Fewer vital structures
4 From: 2) List 6 hard and 6 soft signs of penetrating neck trauma. What are the indications for immediate OR vs CTA in managing penetrating neck trauma Most injuries have nonspecific signs/symptoms: serial examination is key Presence of soft signs suggests non-vascular injury, but 5-15% may still have a vascular injury
5 Features of decompensation: 1. Dyspnea 2. Dysphonia 3. Stridor 4. Drooling 5. Expanding hematoma 6. Bruit 7. Cerebral ischemia 8. Shock HARD SIGNS - very high likelihood of vascular injury 1. Expanding Hematoma 2. Arterial bleed 3. Roaring bruit 4. Neurologic Deficits 5. Stridor 6. Ischemia 7. No radial or weak pulse 8. Shock Diagnostic strategies Key debate is whether physical exam is sensitive enough to diagnose significant injury Thought to be able to identify vascular and esophageal injuries Use hard and soft signs as a guide Soft signs present indicate that surgical repair is less likely needed 3) Describe an approach to managing acute neck trauma in the ER Management: Stable patients Transport to trauma centre Basic wound compression and occlusion (to prevent air embolus) Neurologic deficits should prompt consideration for cervical collar Unstable patients AIRWAY #1 priority! C-spine immobilization - only in the context of blunt trauma or evidence of SCI RSI - is usually*** safe Consider pneumothorax/hemothorax/paralysis in zone I injuries VASCULAR CONCERNS Usually wounds with active bleeding shouldn t be probed - as it may dislodge a clot AVOID blind clamping of bleeding vessels/structures!
6 Trendelenburg reduces the risk of air embolism Place IV access on the uninjured side CERVICAL SPINE hard collar may obscure visualization THORACOTOMY Consider venous air embolism (to be discussed below) With: cardiac arrest NG TUBES Should ideally not be placed in the awake - because the valsalva and retching may cause the patient to dislodge a clot (risk benefit decision!) Disposition: Almost everyone gets a CT head/neck with contrast Based on degree of injury - often need surgery and ICU Anyone with platysma violation needs admission - or surgical evaluation in the ER Patients with blunt neck injury: May have delayed signs of viscero-vascular injury Most need to be transported to a trauma center 4) Describe the management of venous air embolism Vascular trauma may lead to Venous Air Embolism (VAE): Anatomy: Vessels of concern: carotid > subclavian > vertebral arteries, int/ext jugular veins. Pathology: Exsanguination, expanding-compressive hematoma, direct vessel occlusion or embolization (stroke or embolism). Epidemiology: Penetrating injuries Commonly cause exsanguination May have other HARD signs of vascular injury Blunt injuries Usually affects the carotid arteries (rarely vertebral) Patients may be asymptomatic - and may present days to months later Pathophysiology Penetrating trauma usually directly injuries the structures, but the blast may also cause damage Blunt trauma - can tear, thrombose, dissect, and create pseudoaneruysm formation Due to neck hyperextension and hyper-rotation, intra-oral trauma, basilar skull #s, MVCs, fights, etc. Clinical features Imaging is needed - as physical exam will miss injuries. The absence of hard AND soft signs of neck trauma Blunt trauma: ½ of patients with dissections are asymptomatic
7 Diagnostics: Delayed presentation presents at TIA/Cerebral ischemia - ⅓ present after 24 hrs These are some of the most under-reported injuries due to their insidious presentation and catastrophic neurologic outcome Horner s syndrome Symptoms: Carotid artery = contralateral sensory/motor deficits Vertebral arteries = ataxia, emesis, visual field defects, vertigo Denver and Memphis criteria may help in deciding who gets imaging, but generally older adults, anyone with hard signs, significant coma or trauma should get imaging! **the seat-belt signs on the neck - very few (0.8%) have a significant vascular injury** CT-A may miss pseudoaneurysms, but has a % sens and specificity in penetrating trauma These numbers are lower in blunt trauma - ~80% sens Duplex U/S - is mediocre at identifying zone 2 injuries to the carotid, but very limited in zone 1 / 3 injuries MRI-A: sensitivity is equal to CTA and worse when vertebral dissections are suspected. Consider obtaining chest radiographs Management: Penetrating injuries to the carotid - usually all get surgical repair; but some need ligation in cases of existing stroke Blunt trauma: Options depend on the nature of the injury: 1) surgery: ligation, resection, thrombectomy, endovascular stent placement 2) anticoagulation: heparin/lmwh vs. ASA 3) observation Venous air embolisms: Can occur from blunt/iatrogenic/penetrating mechanisms Results in devastating ischemic stroke - more commonly in the venous system. Shock, cardiac arrest; stroke-like symptoms +/- THORACOTOMY Consider venous air embolism Management: Direct occlusive pressure over the site! Head down Left lateral decubitus position (air should move to the right atrium) Aspiration of air from the right ventricle using ultrasound or direct visualization!! (after thoracotomy) ****careful when performing BVM in someone with neck trauma this may lead to massive SC emphysema and possible air embolism
8 5) Describe techniques for airway management in penetrating neck trauma Airway considerations: Orotracheal RSI Should be considered the first line technique Usually successful even in neck trauma with airway distortion contraindications to oro-rsi: Massive facial trauma Laryngotracheal injury ***consider doing an awake look (+/- inline stabilization if C-spine injury) prior to paralysis Important to have backup plans and anesthesia / ENT on hand if needed Nasotracheal intubation Blind-nasotracheal intubation was once taught in ATLS but this is no longer advertised due to risks of: bleeding, vomiting, aspiration, increased ICP, infections Blind nasotracheal intubation should only be done in spontaneously breathing patients Contraindicated in suspected midface or basilar skull #s or laryngeal #s. McGill forceps will be helpful to help guide the tube in the right spot Surgical invasive airways Contraindications to cricothyrotomy: Large anterior neck hematoma Potential laryngeal injury Jet ventilation is a rescue option, with some serious downsides as well MISC techniques Fibreoptic laryngoscopy & Bronchoscopy These can be difficult with +++bleeding Rescue techniques exist with: LMA or King tube Pediatric considerations Higher, more anterior, with the narrowest portion at the cricoid cartilage make airway management more difficult Cricothyrotomy is contraindicated < 10 yrs of age Trans-tracheal ventilation can be a salvage technique oro-rsi is still the best first line choice unless it is contraindicated Cervical spine RSI - with IN-LINE C-SPINE stabilization is safe in blunt and penetrating neck trauma Indecision around airway management definitely leads to hypoxia and secondary neurologic injury Deciding whether to explore surgically or not to? Selective surgical management is the mainstay of current thinking Especially in a non-military setting with low velocity projectiles (handgun) and knives
9 Similar mortality rates in those explored and those without exploration in zone II injuries Transcervical gunshot wounds 2x increase in injuries that cross the midline - due to vascular damage (48%) and Cspine (24%) injuries. Most prospective studies suggest that STABLE patients with TS-GSW s can have a selective surgical approach 6) Describe the management of suspected pharyngoesophageal trauma. What are signs of esophageal injury? Pharyngoesophageal trauma: Esophagus RARELY damaged, if so penetrating > blunt trauma. Usually the distal cervical segment ***important to find esophageal injuries early: Spillage of orogastric contents into mediastinum = potential severe inflammation and infection very often a missed injury - with a 20% mortality rate There are NO pathognomonic signs of esophageal injury: Soft signs: Hematemesis / blood in saliva/ngt Odynophagia / dysphagia Subcutaneous Emphysema Dyspnea / hoarseness / stridor / cough Pain / neck tenderness / resistance to neck movement ***physical exam is unreliable*** Timely diagnosis is essential, a delay of 24 hrs can lead to higher mortality and morbidity Diagnosis depends on: Imaging CXR and neck x-ray are only helpful if there is pneumomediastinum or retropharyngeal air Contrast-esophagography % sensitivity Using a gastrograffin study followed by barium swallow if the gastrograffin study is negative Flexible endoscopy is insensitive as well Combination of endoscopy and contrast swallow is - 100% sensitive CT scan with contrast - Has some utility in tracking the wound/bullet/knife path, but will miss some injuries - making it inadequate as a stand-alone diagnostic modality CT depends on surrogate markers: paraesophageal air/fluid, esophageal edema Which patients to screen for injury? Obtunded trauma patients Those with soft signs: Hematemesis, painful swallowing, sub-cutaneous emphysema Very few should have a watch and wait approach Management: Broad spectrum Abx - with anaerobic coverage NPO NGT placement under endoscopic guidance
10 Uncontained perforations NEED surgery ASAP Contained perforations can be watched and reimaged Esophageal stents - are gaining popularity Pharyngeal injuries are watched 7) List 3 hard signs of laryngotracheal trauma and describe airway management dilemmas Laryngotracheal trauma: RARE! And most involve the cervical trachea Mechanisms: MVCs - extended neck being crushed on steeringwheel Clothesline injuries / poor fitting harnesses Assaults / near hangings / athletic events May be penetrating or blunt (think Cspine injury!) Fractures of the cricoid cartilage can lead to DEATH due to complete airway obstruction Children do not have a calcified larynx - so it will not be seen on plain film: The degree of airway obstruction after blunt trauma is inversely related to the degree of cartilage calcification - children are at highest risk!! Clinical signs: Bubbling of any neck wound Massive subcutaneous Air Bony crepitus Clothesline mechanism of injury Soft signs: Dysphonia / aphonia / dyspnea / stridor / hemoptysis / subcutaneous emphysema / laryngeal crepitus Loss of anatomic landmarks / Pain with tongue movement Hoarseness Tenderness over larynx Diagnostics: Plain radiographs: Looking for: extraluminal air, edema, foreign bodies, # of larynx Laryngoscopy - with possible rigid laryngoscopy CT scans - with 1 mm cuts and multiplanar reconstructions % sensitivity - good to assess hyoid, cartilages, hematomas, crico/arytenoid joints, vocal cord integrity Not as good to find mucosal perforations May not be as good in pediatric uncalcified structures Management: Delayed airway occlusion can happen at anytime - and may be rapid and lifethreatening. ***lots of debate regarding the best way to intubate these patients*** Awake fibreoptic intubation is probably the best if available There is a risk of completing a partial LT separation and creating a FALSE passage **don t paralyse a patient, unless you are prepared for a surgical airway** Consider also prepping for a tracheostomy If the distal trachea has retracted into the chest - tracheal hooks are needed to recover the trachea
11 LMA s are not a good rescue device given the risk for completing the LT separation All unstable patients need surgery Stable pts: Analgesia, humidified air Elevated HOB, antibiotics, steroids, antireflux meds, Vocal rest Wisecracks: 1) Differentiate between choking, hanging and strangulation Choking: something inside your mouth/pharynx/trachea blocking air flow Hanging: a. Various terms - complete/incomplete ; typical/atypical i. Based on whether or not the victim's feet were totally suspended and the location of the knot Strangulation = may be either manual or ligature due to hands or a device compressing the neck independent from the weight of the patient 2) Define judicial and non-judicial hanging and describe expected injury patterns Near hanging or hanging: Very common cause of suicide Pathophysiology: Judicial hanging - usually distracts the head from the rest of the body due to the high fall, causing a fracture through the pedicles of C2 (hangman s), complete cord transection, and vascular disruption Non-judicial hangings usually lead to venous stasis ---> congested blood flow loss of consciousness and body relaxation When the person is limp the ligature / force can tighten further leading to complete arterial occlusion and brain death Vagal pressures on the carotid body may also produce fatal dysrhythmias ***Vascular occlusion leads to death, rather than airway occlusion in most cases!** Clinical features: External trauma may or may not be evident Marks from ligatures, hands, scratches may be present Look for petechial hemorrhages: aka Tardieu s spots In the conjunctiva, MM, and skin cephalad to the ligature marks They occur due to rising venous pressure above the ligature Laryngeal fractures, Thyroid/hyoid # s can be present as well Delayed vascular injuries are less common - but can cause carotid intimal dissection or thrombus formation Consider risk for cervical fractures based on mechanism Management: CT head and neck CTA - neck
12 Comatose patients need intubation and ventilation - with PEEP due to pulmonary edema or ARDS ****initial GCS is NOT predictive of outcome*** Prevent secondary neurologic injury MISC other injuries not covered on the podcast: Neurological injury: Be aware of the brachial plexus and peripheral nerve roots Cervical sympathetic chain, cranial nerves VII, IX, X, XI and XII Spinal cord Complete cord injury results in paraplegia, neurogenic shock, bradycardia, hypotension Brown sequard syndrome: Ipsilateral hemiplegia and contralateral sensory changes Direct injury to the spinal cord - more common in GSW s but still quite rare Direct injury to the recurrent laryngeal nerve - causing hoarseness with paralysis of the ipsilateral vocal cord Thoracic Duct/glandular/retropharyngeal injuries Thoracic duct damage presents as a chylothorax Endocrine gland damage - rare
Evaluation & Management of Penetrating Wounds to the NECK
 Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
Evaluation & Management of Penetrating Wounds to the NECK Goal Effectively identify patients with a high probability of injury requiring surgical intervention Define the role of diagnostic tests in assessing
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2019 #3 Penetrating Neck Trauma Penetrating neck injury (PNI) comprises 5 to 10 percent of traumatic injuries
Penetrating Neck Trauma. Herve J. LeBoeuf, MD Francis B. Quinn, MD
 Penetrating Neck Trauma Herve J. LeBoeuf, MD Francis B. Quinn, MD Introduction 5-10% of all trauma Overall mortality rate as high as 11% Major vessel injury fatal in 65%, including prehospital deaths Attending
Penetrating Neck Trauma Herve J. LeBoeuf, MD Francis B. Quinn, MD Introduction 5-10% of all trauma Overall mortality rate as high as 11% Major vessel injury fatal in 65%, including prehospital deaths Attending
Tips & Techniques in Operative Surgery II: Neck Exploration
 Tips & Techniques in Operative Surgery II: Neck Exploration ศ.ดร.นพ. พรช ย โอเจร ญร ตน สาขาว ชาศ ลยศาสตร ศ รษะ-คอ และเต านม ภาคว ชาศ ลยศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล Indications to Explore a Neck Removing
Tips & Techniques in Operative Surgery II: Neck Exploration ศ.ดร.นพ. พรช ย โอเจร ญร ตน สาขาว ชาศ ลยศาสตร ศ รษะ-คอ และเต านม ภาคว ชาศ ลยศาสตร คณะแพทยศาสตร ศ ร ราชพยาบาล Indications to Explore a Neck Removing
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
vel 2 Level 2 3,034 c-spine evaluations with CSR Level 3 detected injury only 53% of the time. Level 3 False (-) rate 47%
 Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
Objectives Blunt and Penetrating Neck Trauma Julie Mayglothling, MD, FACEP Virginia Commonwealth University Richmond, VA Summit to Sound, May 20 th, 2011 Blunt Neck Trauma Evaluation of the low mechanism,
DR. SAAD AL-MUHAYAWI, M.D., FRCSC. ORL Head & Neck Surgery
 TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
TRAUMA IN ORL DR. SAAD AL-MUHAYAWI, M.D., FRCSC Associate Professor & Consultant ORL Head & Neck Surgery TYPES OF TRAUMA EAR & TEMPORAL BONE TRAUMA NOSE & FACIAL BONES TRAUMA LARYNGEAL TRAUMA NECK TRAUMA
International Journal of Scientific & Engineering Research, Volume 5, Issue 9, September ISSN
 International Journal of Scientific & Engineering Research, Volume 5, Issue 9, September-2014 1196 Pneumomediastinum and subcutaneous emphysema secondary to blunt laryngeal traumafavourable outcome with
International Journal of Scientific & Engineering Research, Volume 5, Issue 9, September-2014 1196 Pneumomediastinum and subcutaneous emphysema secondary to blunt laryngeal traumafavourable outcome with
A CASE PRESENTATION AND DISCUSSION ON HEAD AND NECK TRAUMA
 A CASE PRESENTATION AND DISCUSSION ON HEAD AND NECK TRAUMA Nolan Ortega Aludino, M.D. Department of Surgery Ospital ng Maynila Medical Center General Data: B.R. 64 year old Male Tondo Manila Chief Complaint:
A CASE PRESENTATION AND DISCUSSION ON HEAD AND NECK TRAUMA Nolan Ortega Aludino, M.D. Department of Surgery Ospital ng Maynila Medical Center General Data: B.R. 64 year old Male Tondo Manila Chief Complaint:
PEMSS PROTOCOLS INVASIVE PROCEDURES
 PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
PEMSS PROTOCOLS INVASIVE PROCEDURES Panhandle Emergency Medical Services System SURGICAL AND NEEDLE CRICOTHYROTOMY Inability to intubate is the primary indication for creating an artificial airway. Care
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Tony Capizzani, MD, FACS
 Tony Capizzani, MD, FACS Trauma Medical Director Hillcrest Hospital Cleveland Clinic October 2, 2017 No disclosures Goals and Objectives Describe airway anatomy and innervation Recognize the association
Tony Capizzani, MD, FACS Trauma Medical Director Hillcrest Hospital Cleveland Clinic October 2, 2017 No disclosures Goals and Objectives Describe airway anatomy and innervation Recognize the association
Faculty of Clinical Forensic Medicine Committee 1/2018
 Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
Case Review: Airway Trauma Case 1: Tracheal Transection Pre-hospital:
 (Prepared by: A. Bacevice, MD) The following two cases were submitted for the case competition in 2016. They are presented to illustrate the theme of airway trauma. Case Review: Airway Trauma Case 1: Tracheal
(Prepared by: A. Bacevice, MD) The following two cases were submitted for the case competition in 2016. They are presented to illustrate the theme of airway trauma. Case Review: Airway Trauma Case 1: Tracheal
Ears. Mouth. Jowls 6 Major Bones of the Face Nasal bone Two
 1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
1 2 3 4 5 Chapter 25 Injuries to the Face, Neck, and Eyes Injuries to the Face and Neck Face and neck are to injury Relatively unprotected positions on body Some injuries are life-threatening. trauma to
Brain & Vascular Choke. Definition. The Choke Hold Don Muzzi MD & Larry Lovelace DO. Submission Breakdown UFC Events 4/27/17! 15% of Cardiac Output
 The Choke Hold Don Muzzi MD & Larry Lovelace DO Submission Breakdown UFC Events 25% of fights end in submission anaconda! d acre! 74% of submissions are result of choke hold Does not reflect opinions of
The Choke Hold Don Muzzi MD & Larry Lovelace DO Submission Breakdown UFC Events 25% of fights end in submission anaconda! d acre! 74% of submissions are result of choke hold Does not reflect opinions of
Tracheal Trauma: Management and Treatment. Kosmas Iliadis, MD, PhD, FECTS
 Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Tracheal Trauma: Management and Treatment Kosmas Iliadis, MD, PhD, FECTS Thoracic Surgeon Director of Thoracic Surgery Department Hygeia Hospital, Athens INTRODUCTION Heterogeneous group of injuries mechanism
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
The Primary Survey. C. Clay Cothren, MD FACS. Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado
 The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
The Primary Survey C. Clay Cothren, MD FACS Attending Surgeon, Denver Health Medical Center Assistant Professor of Surgery, University of Colorado Outlining the ABCs Why do we need such an approach? The
In ESH we usually see blunt chest trauma but penetrating injuries also treated here (usually as single injuries, like stab wound)
 Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Chest Trauma Dr Csaba Dioszeghy MD PhD FRCEM FFICM FERC East Surrey Hospital Emergency Department Scope Thoracic injuries are common and can be life threatening In ESH we usually see blunt chest trauma
Face and Throat Injuries. Chapter 26
 Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
Face and Throat Injuries Chapter 26 Anatomy of the Head Landmarks of the Neck Injuries to the Face Injuries around the face can lead to upper airway obstructions. Bleeding from the face can be profuse.
11/3/16. Understanding and Addressing Strangulation. Jenifer Markowitz ND, RN, WHNP-BC, SANE-A, DF-IAFN. Copyright Notice
 Understanding and Addressing Strangulation Jenifer Markowitz ND, RN, WHNP-BC, SANE-A, DF-IAFN Copyright Notice This multimedia presentation contains the creative work of others and is used by permission,
Understanding and Addressing Strangulation Jenifer Markowitz ND, RN, WHNP-BC, SANE-A, DF-IAFN Copyright Notice This multimedia presentation contains the creative work of others and is used by permission,
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
The ABC s of Chest Trauma
 The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
Penetrating Trauma in Pediatric Patients. Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017
 Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
The Neck. BY: Lina Abdullah & Rahaf Jreisat
 The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
Imaging in the Trauma Patient
 Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Aerodigestive Traumatic Injuries in the Pediatric Population
 Aerodigestive Traumatic Injuries in the Pediatric Population Prasad John Thottam Clinical Assistant Professor Michigan State University Michigan Pediatric Ear, Nose and Throat Associates Beaumont Children
Aerodigestive Traumatic Injuries in the Pediatric Population Prasad John Thottam Clinical Assistant Professor Michigan State University Michigan Pediatric Ear, Nose and Throat Associates Beaumont Children
AVOIDING THE CRASH: OPTIMIZE YOUR PRE, PERI, AND POST AIRWAY MANAGEMENT AVOIDING THE CRASH 1: DON T INTUBATE, OPTIMIZE PRE-AIRWAY MANAGEMENT
 AVOIDING THE CRASH: OPTIMIZE YOUR PRE, PERI, AND POST AIRWAY MANAGEMENT Robert J. Vissers MD Chief, Emergency Medicine, Quality Chair, Legacy Emanuel Medical Center Adjunct Associate Professor, OHSU Portland,
AVOIDING THE CRASH: OPTIMIZE YOUR PRE, PERI, AND POST AIRWAY MANAGEMENT Robert J. Vissers MD Chief, Emergency Medicine, Quality Chair, Legacy Emanuel Medical Center Adjunct Associate Professor, OHSU Portland,
Esophageal injuries. 新光急診張志華醫師 Facebook.com/jack119
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Oncologic Emergencies
 Oncologic Emergencies Peter Bjerkerot RN, OCN 1339 Normandy Drive Atlanta, GA 30306-2574 404.754.5952 WebPage http://boyrn.com peter.bjerkerot@mindspring.com Full Disclosure Statement Celgene Nurse Advisory
Oncologic Emergencies Peter Bjerkerot RN, OCN 1339 Normandy Drive Atlanta, GA 30306-2574 404.754.5952 WebPage http://boyrn.com peter.bjerkerot@mindspring.com Full Disclosure Statement Celgene Nurse Advisory
Esophageal injuries. Pre-test /11/10. 新光急診張志華醫師 Facebook.com/jack119. O What is the most common cause of esophageal injuries?
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 O What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic 1 Pre-test 2 O Which contrast
The Primary Survey. Clay Cothren Burlew, MD FACS
 The Primary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining the
The Primary Survey Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Attending Surgeon, Denver Health Medical Center Associate Professor of Surgery, University of Colorado Outlining the
3. D Objective: Chapter 4, Objective 4 Page: 79 Rationale: A carbon dioxide level below 35 mmhg indicates hyperventilation.
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Objectives. Thoracic Inlet. Thoracic Inlet Boundaries. Thoracic Inlet Sagittal View ANTERIOR SCALENE ANTERIOR SCALENE
 Objectives Thoracic Inlet Deborah L. Reede M.D. SUNY Downstate Medical Center Learn the anatomy of the thoracic inlet (TI) Review the clinical and radiographic findings of common lesions encountered in
Objectives Thoracic Inlet Deborah L. Reede M.D. SUNY Downstate Medical Center Learn the anatomy of the thoracic inlet (TI) Review the clinical and radiographic findings of common lesions encountered in
RCH Trauma Guideline. Management of Traumatic Pneumothorax & Haemothorax. Trauma Service, Division of Surgery
 RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
RCH Trauma Guideline Management of Traumatic Pneumothorax & Haemothorax Trauma Service, Division of Surgery Aim To describe safe and competent management of traumatic pneumothorax and haemothorax at RCH.
Management of Penetrating Neck Trauma
 Management of Penetrating Neck Trauma Shashidhar S. Reddy, MD, MPH Faculty Advisor: Shawn D. Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation
Management of Penetrating Neck Trauma Shashidhar S. Reddy, MD, MPH Faculty Advisor: Shawn D. Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation
Mediastinitis. Jonathan Parks, MD Kings County Medical Center December 3, 2015
 Mediastinitis Jonathan Parks, MD Kings County Medical Center December 3, 2015 Case Presentation 69 year-old male from nursing home PMHx: COPD, asthma, HTN, Afib on pradaxa, PTSD, BPH c/o pulled pork stuck
Mediastinitis Jonathan Parks, MD Kings County Medical Center December 3, 2015 Case Presentation 69 year-old male from nursing home PMHx: COPD, asthma, HTN, Afib on pradaxa, PTSD, BPH c/o pulled pork stuck
ITLS Advanced Pre-Test Annotated Key 8 th Edition
 1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
1. A Objective: Chapter 1, Objective 3 Page: 14 Rationale: The sudden increase in acceleration produces posterior displacement of the occupants and possible hyperextension of the cervical spine if the
Penetrating Neck Trauma January 1999
 TITLE: Penetrating Neck Trauma SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds Presentation DATE: January 26, 1999 RESIDENT: Herve J. LeBoeuf, M.D. FACULTY: Francis B. Quinn, Jr., M.D. SERIES EDITOR:
TITLE: Penetrating Neck Trauma SOURCE: Dept. of Otolaryngology, UTMB, Grand Rounds Presentation DATE: January 26, 1999 RESIDENT: Herve J. LeBoeuf, M.D. FACULTY: Francis B. Quinn, Jr., M.D. SERIES EDITOR:
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Anatomy notes-thorax.
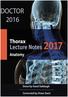 Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
Anatomy notes-thorax. Thorax: the part extending from the root of the neck to the abdomen. Parts of the thorax: - Thoracic cage (bones). - Thoracic wall. - Thoracic cavity. ** The thoracic cavity is covered
How Do I Manage Penetrating Neck Trauma?
 Review Article ISSN 2508-5298 How Do I Manage Penetrating Neck Trauma? Hyun Min Cho Department of Trauma and Surgical Critical Care, Pusan National University Hospital, Busan, Korea Penetrating neck trauma
Review Article ISSN 2508-5298 How Do I Manage Penetrating Neck Trauma? Hyun Min Cho Department of Trauma and Surgical Critical Care, Pusan National University Hospital, Busan, Korea Penetrating neck trauma
Oral and Maxillofacial Surgeons and the seriously injured patient. Barts and The London NHS Trust
 Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Oral and Maxillofacial Surgeons and the seriously injured patient Barts and The London NHS Trust How do you assess this? Primary Survey A B C D E Airway & Cervical Spine Breathing & Ventilation Circulation
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
PRE-HOSPITAL EMERGENCY CARE COURSE.
 PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
PRE-HOSPITAL EMERGENCY CARE COURSE www.basics.org.uk Chest Assessment & Management BASICS Education March 2016 Objectives To understand the importance of oxygenation and ventilation To be able to describe
Congenital Neck Masses C. Stefan Kénel-Pierre, MD
 Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
Congenital Neck Masses C. Stefan Kénel-Pierre, MD SUNY-LICH Medical Center Department of Surgery Case Presentation xx year old male presents with sudden onset left lower neck swelling x 1 week Denies pain,
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN
 CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
Spinal Cord Injuries: The Basics. Kadre Sneddon POS Rounds October 1, 2003
 Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Spinal Cord Injuries: The Basics Kadre Sneddon POS Rounds October 1, 2003 Anatomy Dorsal columntouch, vibration Corticospinal tract- UMN Anterior horn-lmn Spinothalamic tractpain, temperature (contralateral)
Tracheo-innominate artery fistula (TIF) is an uncommon
 Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Technique for Managing Tracheo-Innominate Artery Fistula Gorav Ailawadi, MD Tracheo-innominate artery fistula (TIF) is an uncommon complication (0.1-1%) following both open and percutaneous tracheostomy.
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
Pan Scan Instead of Clinical Exam? David A. Spain, MD
 Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
ITLS Pediatric Provider Course Advanced Pre-Test
 ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Advanced Pre-Test 1. You arrive at the scene of a motor vehicle crash and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
SPINE EVALUATION AND CLEARANCE Basic Principles
 SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
SPINE EVALUATION AND CLEARANCE Basic Principles General 1. Entire spine is immobilized during primary survey. 2. Radiographic clearance of the spine is not required before emergent surgical procedures.
The Management of Chest Trauma. Tom Scaletta, MD FAAEM Immediate Past President, AAEM
 The Management of Chest Trauma Tom Scaletta, MD FAAEM Immediate Past President, AAEM Trichotomizing Rib Fractures Upper 1-3 vascular injuries Middle 4-9 Lower 10-12 12 liver/spleen injuries Management
The Management of Chest Trauma Tom Scaletta, MD FAAEM Immediate Past President, AAEM Trichotomizing Rib Fractures Upper 1-3 vascular injuries Middle 4-9 Lower 10-12 12 liver/spleen injuries Management
Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore
 CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
CENTRAL VENOUS CATHETERIZATION Dr. prakruthi Dept. of anaesthesiology, Rrmch, bangalore OBJECTIVES Introduction Indications and Contraindications Complications Technique Basic principles Specifics by Site
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
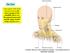 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Chapter 39 Trauma in the Elderly
 Chapter 39 Trauma in the Elderly Episode Overview 1) 5 Risk Factors for falls in the elderly? 2) What anatomic and physiologic changes in the elderly patient are important for the management of trauma
Chapter 39 Trauma in the Elderly Episode Overview 1) 5 Risk Factors for falls in the elderly? 2) What anatomic and physiologic changes in the elderly patient are important for the management of trauma
Screening and Management of Blunt Cereberovascular Injuries (BCVI)
 Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Neck Ultrasound. Faculty Info: Amy Kule, MD
 Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Neck Ultrasound Date: Friday, October 19, 2018 Time: 11:00 AM Location: SMALL GROUP LABORATORY SSOM L71 Watch: Ø Neck Ultrasound Scanning Protocol (4:00): https://www.youtube.com/watch?v=zozd2x2ll4q Faculty
Evaluation and Stabilization of the Athlete with Possible Spine Injury
 Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
CHEST TRAUMA. Dr Naeem Zia FCPS,FACS,FRCS
 CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
Trauma Overview. Chapter 22
 Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
ESOPHAGEAL PERFORATION. Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013
 ESOPHAGEAL PERFORATION Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013 OUTLINE Risk factors Diagnosis Management GOALS Make sure you don t miss it If
ESOPHAGEAL PERFORATION Anju Sidhu MD University of Louisville Gastroenterology, Hepatology, and Nutrition January 24, 2013 OUTLINE Risk factors Diagnosis Management GOALS Make sure you don t miss it If
Section 4.1 Paediatric Tracheostomy Introduction
 Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
Bite- sized training from the GTC Section 4.1 Paediatric Tracheostomy Introduction This is one of a series of bite- sized chunks of educational material developed by the Global Tracheostomy Collaborative.
H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital,
 H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital, Montreal General Hospital, McGill University Health Center
H. Mitchell Shulman MDCM FRCPC CSPQ Assistant Professor, Dept. of Surgery, McGill Medical School Attending Physician, Royal Victoria Hospital, Montreal General Hospital, McGill University Health Center
Selective Spine Assessment & Spinal Motion Restriction
 Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
Selective Spine Assessment & Spinal Motion Restriction Supersedes: 02-09-15 Effective: 10-20-15 Spinal cord injury may be the result of direct blunt and/or penetrating trauma, compression forces (axial
General Medical Procedure. Emergency Airway Techniques (General Airway Protocol)
 General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
General Medical Procedure Appropriate airway management is often the most important intervention a prehospital care provider makes, as ensuring adequate oxygenation and ventilation is crucial to the survival
4. Neoplastic: benign & malignant. 5. Allergic rhinitis & nasal polyp. 6. hypertrophied tonsils or adenoids. L 5
 L 5 Stertor& Stridor Stertor& stridor are both auditory manifestation of disordered respiratory function. Stertor: Is a low pitched snoring or snuffly sound caused by obstruction of the airway above the
L 5 Stertor& Stridor Stertor& stridor are both auditory manifestation of disordered respiratory function. Stertor: Is a low pitched snoring or snuffly sound caused by obstruction of the airway above the
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Chapter 5 Medical Evidence in Non-Fatal Strangulation Cases
 Chapter 5 Medical Evidence in Non-Fatal Strangulation Cases by William Green, M.D. Strangulation is one of the most lethal forms of domestic violence. Minimal pressure on the neck can cause serious injury,
Chapter 5 Medical Evidence in Non-Fatal Strangulation Cases by William Green, M.D. Strangulation is one of the most lethal forms of domestic violence. Minimal pressure on the neck can cause serious injury,
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
Respiratory System. Clinical notes. Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz)
 Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz) Respiratory System The test of the respiratory system follows the general rules for written tests (see Continuous
Published on Second Faculty of Medicine, Charles University ( https://www.lf2.cuni.cz) Respiratory System The test of the respiratory system follows the general rules for written tests (see Continuous
Head & Neck Clinical Sub Group. Network Agreed Imaging Guidelines for UAT and Thyroid Cancer. Measure Nos: 11-1C-105i & 11-1C-106i
 Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Greater Manchester, Lancashire & South Cumbria Strategic Clinical Network & Senate Head & Neck Clinical Sub Group Network Agreed Imaging Guidelines for UAT and Thyroid Cancer Measure Nos: 11-1C-105i &
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
North Oaks Trauma Symposium Friday, November 3, 2017
 + Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
+ Evaluation and Management of Facial Trauma D Antoni Dennis, MD North Oaks ENT an Allergy November 3, 2017 + Financial Disclosure I do not have any conflicts of interest or financial interest to disclose
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for
 Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Post-op Carotid Complications A Nursing Perspective of What to Watch Out for By Kariss Peterson, ARNP Swedish Medical Center Inpatient Neurology Team 1 Post-op Carotid Management Objectives Review the
Airway Management. Teeradej Kuptanon, MD
 Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Airway Management Teeradej Kuptanon, MD Outline Anatomy Detect difficult airway Rapid sequence intubation Difficult ventilation Difficult intubation Surgical airway access ICU setting Intubation Difficult
Bundeswehrkrankenhaus Ulm Abteilung HNO Kopf-Halschirurgie
 Kai Johannes Lorenz and Klaus Effinger Department of Otorhinolaryngology, Head and Neck Surgery Department of Radiology and interventional Radiology German Armed Forces Hospital Incidence of hemorrhage
Kai Johannes Lorenz and Klaus Effinger Department of Otorhinolaryngology, Head and Neck Surgery Department of Radiology and interventional Radiology German Armed Forces Hospital Incidence of hemorrhage
Trauma operating room
 Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
Section 1 Chapter 1 Operating Room General Conduct Trauma operating room Kenji Inaba and Lisa L. Schlitzkus Operating room A large operating room (OR) situated near the emergency department, elevators,
ISPUB.COM. GSW To The Face: "Hunting Camp" C Perry, B Phillips CASE REPORT
 ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
ISPUB.COM The Internet Journal of Rescue and Disaster Medicine Volume 2 Number 2 C Perry, B Phillips Citation C Perry, B Phillips.. The Internet Journal of Rescue and Disaster Medicine. 2000 Volume 2 Number
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
EAST MULTICENTER STUDY DATA DICTIONARY. Temporary Intravascular Shunt Study Data Dictionary
 EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
Tympanic Bulla Temporal Bone. Digastric Muscle. Masseter Muscle
 Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Carotid Stenosis 1/24/2019. Review of Primary Studies. NASCET- Moderate stenosis. ACAS (Asymptomatic Carotid Atherosclerosis Study) NASCET
 Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
Review of Primary Studies Carotid Stenosis NINDS National Institute of Neurological Disorders and Stroke 2 large studies to determine who would benefit from surgery NASCET North American Symptomatic Carotid
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
