Non-Accidental Trauma (NAT) Protocol
|
|
|
- Herbert Walton
- 6 years ago
- Views:
Transcription
1 Non-Accidental Trauma (NAT) Protocol All children suspected of non-accidental trauma will have a complete work-up including a complete history and physical exam with a focus on injuries and explanation for the injuries. Major Areas of Evaluation: 1. A complete history (document from/by whom & if it contradicts prior story) a. Including review of prior PCP, ED, and inpatient records as well as prior radiologic studies performed at outside hospitals (if available) to look for sentinel injuries 2. Head to toe physical exam with particular attention to: a. Growth parameters b. Thorough skin exam, including scalp and hair (undress patient completely) c. Palpation of legs, arms, hands, feet and ribs to feel for crepitus or deformities d. Complete neurologic examination e. Oral examination with attention to the lips, tongue, buccal mucosa, frenula, palate and teeth f. Auricle exam g. Genitalia examination 3. Head Imaging a. Infants < 12 months of age should have a CT scan without contrast or MRI of the brain (preferred if patient has no sign of injury and normal mental status) to evaluate for intracranial injuries. This should be performed regardless of the presence or absence of neurologic findings. b. Children > 12 months of age should have a CT scan without contrast if there is mental status depression or any other signs of neurological injury. This may also include external signs of head injury, such as facial bruising or scalp hematoma. c. If the CT scan without contrast or MRI indicates signs of trauma, MRI of the c- spine should be considered. Last revised 2/24/2017 Page 1
2 d. If there is a suspicion of a skull fracture, consider ordering a CT scan with 3D reconstruction, to better clarify fracture versus suture (must be ordered prior to the CT scan being done). e. If there is clinical concern or disagreement with the outside study, order a formal second opinion read. Having the outside report is helpful but not necessary. 4. Abdominal Imaging a. Any child who presents with signs/symptoms of abdominal trauma, bruising to the abdomen or torso, or an ALT/AST that is higher than twice normal should have a CT of the abdomen/pelvis with IV contrast. b. Consider abdominal CT if urinalysis has >10 RBCs and/or positive stool guaiac. 5. Skeletal Survey (should be obtained Monday through Friday during normal business hours UNLESS this would delay discharge) a. Children < 3 years of age should have a skeletal survey to evaluate for occult fractures. When ordering a skeletal survey, be sure to include oblique x-rays of the ribs. b. Children > 3 years of age can have x-rays focusing on areas of concern rather than the entire skeleton. c. Consider getting a full skeletal survey in children > 3 years of age with developmental delays. d. For skeletal surveys performed at outside hospitals, consider reviewing it with a Pediatric Radiologist to determine the completeness and quality of the study and the potential need for additional films. e. Follow up skeletal survey should be obtained at Upstate two weeks following the suspected trauma to check for fractures that are too acute to show up on initial survey (i.e. rib fractures). 6. Ophthalmology Evaluation a. Children < 12 months of age should have an ophthalmologic evaluation to look for retinal hemorrhages. Retinal photographs should be obtained, when possible. b. Children > 12 months of age should have an ophthalmologic evaluation when eye injuries are suspected, when head injury is suspected, and/or when there is facial bruising. Last revised 2/24/2017 Page 2
3 c. Ophthalmologic examination should be obtained as soon as possible. However, the dilated eye exam should be deferred in children with head injuries pending neurosurgery clearance. 7. Lab Evaluation a. The following labs should be ordered routinely on all children suspected of NAT: CBC with diff and platelets Amylase Lipase CMP PT/PTT/INR Urinalysis with microscopic Stool for occult blood b. Consider a UDS/toxicology evaluation if there is clinical suspicion of exposure to substances or in children < 2 years of age with altered mental status. c. Consider Vitamin D 25 Hydroxy, Calcium, Phosphorus and PTH if clinically indicated. 8. Medical Photography a. Order Medical Photography as soon as possible to document any skin findings at the time of presentation, since they can change rapidly. Medical Photography is available Monday through Friday 9-5. b. When there are skin findings and Medical Photography is not available, the social workers have access to a camera that can document injuries. c. When Medical Photography is unavailable the MD/NP/PA will photograph the patient with the camera provided by social work. See policy C-06 d. A healthcare provider must be present while the photographs are taken in order to direct the photographer s attention to areas of concern. 9. Severe Abuse a. Victims of severe abuse should have a toxicology evaluation. b. Victims of severe abuse should have a SANE evaluation if clinical concerns regarding sexual abuse or other need for forensic evidence collection. Last revised 2/24/2017 Page 3
4 10. Siblings 11. Admission 12. Discharge All siblings or other at risk children in the home of patients that are victims of suspected NAT should be evaluated by their PCP within 24 hours. Upon identification of other possible at risk individuals in the home of a NAT patient, the service managing the patient at the time of discovery should consult Social Work and request Child Protective Services be made aware of those individuals and document accordingly in the progress notes. a. Admit all patients that have a clinical indication. Patients with identified traumatic injuries or who are undergoing an NAT work up will be admitted to an appropriate surgical service. If Pediatric Surgery is not the primary team, they should be consulted to ensure the NAT work-up is completed and appropriate follow-up is in place. b. Patients undergoing an NAT work-up meet criteria for inpatient status. c. Admit patients when there is a concern about the safety of the patient, especially if there is a disagreement between the provider and CPS. d. Children < 24 months with suspected or documented head injury should have serial head circumferences measured daily. a. All children evaluated in the ED where there is concern for possible NAT but who do not meet criteria for inpatient admission should receive a social work consult and CARE clinic should be notified for determination of need for outpatient follow-up. b. All children admitted for NAT work-up should have a follow-up appointment with the Pediatric Trauma Clinic ( ) or be connected with the CARE Program at the McMahon-Ryan Child Advocacy Center (315) c. All children who get a skeletal survey as part of their work-up should have a follow up skeletal survey ordered in EPIC prior to discharge. This should be ordered as an orders only encounter. This should be obtained at Upstate two weeks following the suspected trauma. Last revised 2/24/2017 Page 4
5 d. Patients following up at Fly Road Pediatric Non-accidental Trauma patient s following up at Fly Road Medical Center with Orthopedics Protocol. Pediatric Trauma will contact the pediatric orthopedic division to request the study: (315) The secretarial staff will notify the Orthopedic MD treating the patient and the order will be placed and scheduled to be done at their scheduled follow-up appointment. Upstate Orthopedic X-Ray techs will "scan" the orders for open skeletal survey studies Upstate Orthopedic surgeons to inquire with parent/guardian about additional scheduled studies. e. For patients with head injuries: Consider referral for Early Intervention and a hearing evaluation Document head circumference on discharge summary f. If feasible, all follow-up appointments with Pediatric Surgery, CARE, Ophthalmology, Orthopedics, Neurosurgery and/or ENT should be scheduled prior to discharge. 13. Impact Statements a. An impact statement is a letter written by a health care provider that informs, interprets and provides a medical opinion for child protective workers or the court regarding the level of concern for non-accidental trauma and the impact on the child. b. Impact Statements should: Describe the situation and your relationship to the patient. Use layman s terms to describe medical issues. Clearly define your concerns in terms that are meaningful to the court and child protective services. Answer questions that CPS has asked. Identify your opinion if you have one, but refrain from outright advocacy if possible. Usually outline next steps for medical and/or legal needs. Last revised 2/24/2017 Page 5
6 c. The primary team responsible for the patient should generate the impact statement. See Addendum A for Rating Scale for Abuse Likelihood. For documentation tips and sample impact statements, go to the CHAMP website at: ADDENDUM A Rating Scale for Abuse Likelihood 1. Definitely not inflicted injury (significant, independently verifiable mechanism such as MVC, disinterested witness such as police, ambulance, video documentation, mimic i.e. Mongolian spot) 2. Not concerning for inflicted injury (mechanism explains all injuries, consistent history) 3. Mildly concerning for inflicted injury (somewhat concerning injuries with no offered history - i.e. unexplained humerus fracture in a 10-month-old or otherwise unconcerning injury with past suspicious injury and same caregiver) 4. Intermediately concerning for inflicted injury (insufficient information to offer an opinion, sequence of events clear but uncertain whether they constitute abuse, necessary lab tests/consultations pending, concerning injury in the setting of bone fragility/bleeding diathesis) 5. Very concerning for inflicted injury (given history unlikely to produce documented injuries or concerning injury with no history of trauma i.e. 4 month old with femur fracture) 6. Representative of substantial evidence of inflicted injury (severe injury with no offered history in a child incapable of inflicting the injury on himself or herself, history inconsistent with Last revised 2/24/2017 Page 6
7 identified injuries, serious injury with changing history or history inconsistent between caregivers, inappropriate delay in seeking care, multiple severe injuries of different ages without plausible explanation) 7. Definite inflicted injury (pattern bruises/burns, unexplained posterior rib fractures, characteristic retinal hemorrhages, reliable eye witness, suspicious injury and concurrently abused sibling, obvious injury with significant, unexplained delay in seeking care i.e. serious burn, unresponsive child, apparent prolonged seizures) NAT Smart Phrases Available in EPIC 1. Bruising.NORMALBRUISING : Normal toddler bruising occurs in exploratory surfaces and over bony prominences such as the shins, lower arms, under the chin, the forehead, hips, elbows and ankles. Bruising to the upper arms, torso, cheek, ears, neck, genitalia and buttocks are more likely to be the result of abuse. Bruising to the helix (upper part of the ear) is usually caused by pulling or pinching the top of the ear. Any bruising in a nonambulatory child with a lack of history of trauma and without evidence of a bleeding disorder is concerning for non-accidental trauma. 2. Head Injuries.SHORTFALL: Falls are the most common cause of injury bringing children to the emergency department and requiring hospital admission. Accidental household falls from furniture most commonly result in minor trauma such as concussion or skull fracture. Serious head injuries purported to be accidental, unless related to a motor vehicle accident or a fall from a significant height, are very likely to be the result of abuse, particularly if the injuries are ascribed to falls from short heights that occur at home, unwitnessed by objective observers (i.e. fall from bed, couch or chair)..subduralhematoma: A subdural hemorrhage is a collection of blood between the brain and the dura, the brain s tough outer covering. They are most often caused by moderate to high energy forces to the head and result when bridging veins are stretched and tear during rapid acceleration-deceleration forces. This can occur in a high speed car Last revised 2/24/2017 Page 7
8 accident, fall from extreme height or violent shaking. Generally, acute subdural hematomas are less than 72 hours old. The subacute phase begins 3-7 days after initial injury, and chronic subdural hematomas develop over the course of weeks. These time lines offer a general guideline and are not exact. Acute subdural hematomas most often occur shortly after moderate to severe head injury. Symptoms in infants can include loss of consciousness, seizures, lethargy, irritability, poor feeding, vomiting, bulging fontanelle, and pallor. Symptoms usually appear immediately but in some cases, there may be a lucid interval of a few hours after the injury where the child appears relatively well and normal but subsequently deteriorates as the hematoma forms depending on the location, severity and rapidity with which the hematoma develops. Therefore, it is not possible to provide a precise timeline. The finding of subdural hematomas and retinal hemorrhages in infants are significantly more common in non-accidental trauma than in accidental injury. Retinal hemorrhages are found in non-inflicted head trauma less than 3% of the time..bess: Benign familial hydrocephalus, also described as benign external hydrocephalus, idiopathic external hydrocephalus, benign extraaxial collections of infancy, or benign subdural effusions of infancy has been raised as a possible cause of spontaneous subdural hematoma. Children with this condition have benign enlargement of the subarachnoid spaces (BESS) on radiologic imaging. Although there remains controversy regarding the possible mechanism, it continues to be proposed in the literature that the presence of BESS is a risk factor for development of SDH from minor unrecognized trauma. There are case reports of patients with BESS who have been incidentally found to have SDH. To my knowledge, none of these children had additional findings of retinal hemorrhages. 3. Fractures.BIRTHRELATEADFRACTURES: Rib fractures due to birth trauma can occur, typically in large newborns with a difficult vaginal birth. Healing rib fractures in children older than 3 months or acute fractures in infants older than 1 week are likely the result of nonaccidental trauma. Clavicular fractures are the most common birth-related skeletal injury, and a healing fracture in the first 7-10 days of life must be regarded as accidental..clavicle: Any acute clavicular fracture identified after 10 days of life without evidence of healing is suggestive of abuse. Accidental fractures in the medial or lateral end of the clavicle are uncommon in children less than 3 years of age. These fractures are likely the result of shaking..femurfractures: Spiral femur fractures occur when a rotational force is applied to the leg during twisting or shaking, torsion when the leg is used as a handle for shaking, or from a direct blow. These fractures typically result from high-energy trauma, such as that caused by a fall from a height or a motor vehicle accident. The presence of a spiral femur fracture in the absence of a history of high energy trauma is very concerning for inflicted injury. Last revised 2/24/2017 Page 8
9 .HUMERUSFRACTURES: Most non-inflicted humeral fractures are supracondylar in location (near the elbow) and are more common in older children. Abuse related fractures can occur when the arm is used as a handle to the assailant as the infant is pulled, swung or shaken..metaphysealfractures: Metaphyseal fractures, otherwise known as corner fractures, bucket handle fractures or classic metaphyseal lesions, require biomechanical forces that are not produced by the usual accidental trauma of infancy. These fractures result from shearing forces due to rapid acceleration and deceleration as seen with shaking or rotational forces generated from violent traction or twisting of the extremity and are highly specific for non-accidental injury..ribfractures: Rib fractures in infancy are the result of child abuse more than 80% of the time. Most exceptions to this rule result from high energy trauma. Mechanisms can include squeezing, rotation of the ribs posteriorly with squeezing action, crush injury, or direct trauma. The presence of rib fractures in the absence of a history of high energy trauma is highly suggestive of non-accidental trauma..skullfracture: The presence of a skull fracture indicates direct impact either from a blow to the head or the rapidly moving head brought up against a static object. Most accidental skull fractures are simple, non-displaced linear fractures occurring over the parietal/occipital region resulting from an accidental fall, are not usually associated with significant clinical problems and do not require treatment..toddlerfracture: Non-displaced spiral fractures of the tibia are a relatively common accidental injury seen in children who are able to stand, cruise or walk (typically 9 months old through age 3). This type of fracture is also known as a toddler fracture or a "Childhood Accidental Spiral Tibial (CAST) fracture. This occurs during routine play activities and may result from running and slipping, jumping and falling, and even sliding with a difficult landing. There may be a delay in seeking medical care because the injury does not initially appear significant. Fractures of this type typically involve the distal half to distal third of the tibia. Fractures of the more proximal tibia may be suspicious for non-accidental trauma. Fracture Types.OBLIQUE: Oblique fractures are similar to spiral fractures. They typically result from a bending force with superimposed axial compression, causing the bone to break at an angle. They can result from indirect twisting forces and can be seen in both accidental and non-accidental injury..spiralfracture: Spiral fractures result from indirect twisting or torsion forces to the bone. They can be associated with abusive injuries primarily in infants and young Last revised 2/24/2017 Page 9
10 toddlers. They can also be seen in accidental injury in ambulatory children with a history of a twisting injury. They can also be seen in ambulatory toddlers without a history of trauma (childhood accidental spiral tibia fractures)..transverse: Transverse fractures result from a direct fore to the bone and can be associated with both accidental and non-accidental injury. 4. Eye Injuries.RETINALHEME: Retinal hemorrhages (bleeding within the light sensitive tissue that lines the inside of the back of the eye ball) can occur when there is an elevation of intracranial pressure (the pressure inside the skull and brain tissues), intracranial hemorrhage (bleeding that occurs inside the skull), hypoxia (deficiency in the amount of oxygen reaching the tissues), anemia (deficiency of red blood cells or hemoglobin) and increased intrathoracic pressure (increased pressure within the pleural cavity). Significant hemorrhagic retinopathy is most often seen in repetitive acceleration-deceleration forces that accompany high energy trauma such as a car accident or abusive head trauma which cause unique shearing forces inside the eye and orbit that result in significant retinal hemorrhage. The bleeding can be in one eye or both eyes and can be asymmetric. A few retinal hemorrhages confined to the posterior pole may be very non-specific and could result from numerous other causes, but massive retinal hemorrhage throughout the entire retina is rarely reported in any other condition than abusive head trauma. Excessive coughing and/or vomiting are unlikely to produce significant retinal hemorrhages. The finding of subdural hematomas and retinal hemorrhages in infants are significantly more common in non-accidental trauma than in accidental injury. Retinal hemorrhages are found in non-inflicted head trauma less than 3% of the time..retinoschisis: The presence of retinoschisis (splitting of the retinal layers) is highly specific for abusive head trauma and results from repeated accelerationdeceleration forces (Levin, 2016). In children less than 3 years of age, the vitreous (a clear, jelly-like substance that fills the middle of the eye) is quite firmly adherent to the macula (an oval, yellow-pigmented area on the central retina) and retinal blood vessels, much more so than in the adult. As a result, the repetitive acceleration-deceleration forces applied indirectly to the vitreous exert shearing tractional forces on the retina causing it to split its layers, forming a cystic cavity that fills with blood. A single rapid accelerationdeceleration force such as a fall would not cause retinal hemorrhages or retinoschisis unless the force rose to the level of a fatal impact or crush (i.e. a motor-vehicle crash or fall from greater than 10 meters). There is overwhelming evidence in the literature that supports the conclusion that severe hemorrhagic retinopathy in an otherwise previously well child without obvious history to the contrary (fatal head crush) suggests that the child has been subjected to abusive repetitive acceleration-deceleration trauma. 5. Abuse Likelihood scale.likelihoodscale: After history, exam, and diagnostic studies, it is my opinion injuries/findings are ***. Last revised 2/24/2017 Page 10
11 ***Rating Scale for Abuse Likelihood (Pick One) 1. Definitely not inflicted injury (significant, independently verifiable mechanism such as MVC, disinterested witness such as police, ambulance, video documentation, mimic i.e. Mongolian spot) 2. Not concerning for inflicted injury (mechanism explains all injuries, consistent history) 3. Mildly concerning for inflicted injury (somewhat concerning injuries with no offered history - i.e. unexplained humerus fracture in a 10-month-old or otherwise unconcerning injury with past suspicious injury and same caregiver) 4. Intermediately concerning for inflicted injury (insufficient information to offer an opinion, sequence of events clear but uncertain whether they constitute abuse, necessary lab tests/consultations pending, concerning injury in the setting of bone fragility/bleeding diathesis) 5. Very concerning for inflicted injury (given history unlikely to produce documented injuries or concerning injury with no history of trauma i.e. 4 month old with femur fracture) 6. Representative of substantial evidence of inflicted injury (severe injury with no offered history in a child incapable of inflicting the injury on himself or herself, history inconsistent with identified injuries, serious injury with changing history or history inconsistent between caregivers, inappropriate delay in seeking care, multiple severe injuries of different ages without plausible explanation) 6. Definite inflicted injury (pattern bruises/burns, unexplained posterior rib fractures, characteristic retinal hemorrhages, reliable eye witness, suspicious injury and concurrently abused sibling, obvious injury with significant, unexplained delay in seeking care i.e. serious burn, unresponsive child, apparent prolonged seizures) 7. Impact Statement *** County CPS Attn: *** *** ***, NY *** Last revised 2/24/2017 Page 11
12 Dear ***: As you know, who was admitted to Upstate Golisano Children s Hospital for ***. The history as reported by ***, is that ***. On exam in our Emergency was found to have was admitted to the hospital under my service. Due to concern for possible child abuse, a full non-accidental trauma work up has been initiated per our hospital protocol. The work-up has revealed the following: 1. Routine laboratory studies {were/were not:19694} remarkable. The coagulation profile and platelet count {were/were not:19694} normal indicating {does/does not:19886} have a bleeding disorder that could cause abnormal bruising in the absence of trauma. *** 2. Head CT was {gen negative/positive:315881} for head injury. *** 3. Dilated eye exam was {gen negative/positive:315881} for intraretinal hemorrhages (bleeding with the eye tissues). 4. A skeletal survey (series of full body x-rays) was obtained and {Desc; did/not:14019} show additional injuries. This will be repeated in 2 weeks for routine follow-up to make sure there are no additional findings that are too recent to show up on the initial study. 5. Examination of the skin was {Desc; normal/abnormalwildcard:19619}. There are several aspects s history, imaging and/or clinical findings that are concerning for non-accidental trauma. Please let me know if anything in this letter requires further clarification. Sincerely, 8. NAT Consult Template (*not currently in use).natconsult Date of PEDIATRIC NON-ACCIDENTAL TRAUMA CONSULT NOTE Last revised 2/24/2017 Page 12
13 Consult Requested By: Dr. *** Chief Complaint History of Present Illness History obtained from: *** who presents with *** Additional history: *** Developmental Milestones Rolling: {yes/no/unk:311367} Cruising: {yes/no/unk:311367} Walking: {yes/no/unk:311367} Parental concern for delays: {yes/no/unk:311367} NAT Screen (history red flags) Unwitnessed injury: {Blank single:19197::"yes", "no"} No history/history inconsistent with injury: {Blank single:19197::"yes", "no"} Changing history: {Blank single:19197::"yes", "no"} Delay in seeking care: {Blank single:19197::"yes", "no"} Prior ED visit: {Blank single:19197::"yes", "no", "unknown"} Domestic violence in the home: {Blank single:19197::"yes", "no", "unknown"} Premature infant (<37 weeks): {Blank single:19197::"yes", "no", "unknown"} Low birth weight/iugr: {Blank single:19197::"yes", "no", "unknown"} Chronic medical conditions: {Blank single:19197::"yes", "no", "unknown"} Past Medical Birth History: *** Immunizations: {Blank single:19197::"up to date", "not up to date", "unkown"} Past Surgical Home Last revised 2/24/2017 Page 13
14 Family/Social History History of DA, SA, DV, mental health disorders, or prior CPS involvement:{blank single:19197::"yes - ***", "no", "not asked"} Cultural or social issues to be aware of: {Blank single:19197::"yes - ***", "no", "not asked"} Any major illness in the immediate family: {Blank single:19197::"yes - ***", "no", "not asked"} Anesthetic complications/allergies: {Blank single:19197::"yes - ***", "no", "not asked"} Bleeding disorders: {Blank single:19197::"yes - ***", "no", "not asked"} Are there other young children that reside in the home: {Blank single:19197::"yes - ***", "no", "not asked"} Review Of Physical General appearance: *** HEENT (note condition of lips, tongue, buccal mucosa, frenula, palate, and teeth): *** Neck: *** CVS: *** Lungs: *** Abdomen: *** Musculoskeletal: *** Neuro: *** GU: *** Skin (note auricle exam, scalp/hair): *** NAT Screen (physical exam red flags) Torn frenulum: {Blank single:19197::"yes", "no"} Evidence of FTT: {Blank single:19197::"yes", "no"} Infant with large head: {Blank single:19197::"yes", "no"} Patterned Scars: {Blank single:19197::"yes", "no"} ANY bruise in a non-ambulatory child: {Blank single:19197::"yes", "no"} Bruising in a non-exploratory location in a child less than 4 yrs old (torso, ears, neck): {Blank single:19197::"yes", "no"} Tests Ordered/Reviewed LFTs elevated: {Blank single:19197::"yes", "no", "no results yet"} Last revised 2/24/2017 Page 14
15 If LFTs are elevated above twice normal, CT of abdomen/pelvis should be obtained. Imaging: NAT Screen (radiographic red flags) Metaphyseal corner fractures: {Blank single:19197::"yes", "no", "skeletal survey pending"} Rib fractures (especially posterior) in infants: {Blank single:19197::"yes", "no", "skeletal survey pending"} ANY fracture in a non-ambulatory child: {Blank single:19197::"yes", "no"} Any undiagnosed healing fracture: {Blank single:19197::"yes", "no", "skeletal survey pending"} SDH and/or SAH in the absence of a skull fracture in a child < 1 year: {Blank single:19197::"yes", "no", "head imaging pending} who presents with ***. After history, physical exam, laboratory tests and imaging studies, there {is/is not:320031} concern for possible non-accidental trauma. Plan Admit to: {Blank single:19197::"pediatric Surgery", "***"} Consults: {NAT consults:22895} Imaging: {NAT Imaging:22896} Labs: CBC with platelets, PT/PTT/INR, amylase, lipase, ALT/AST, urine dip for blood and stool for guaiac per protocol - if not already done. Other: *** Last revised 2/24/2017 Page 15
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May Leslie M. Quinn M.D.
 CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
Suspected Physical Abuse Clinical Practice Guideline
 Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
CORE-INFO: fractures in children
 CORE-INFO: fractures in children This leaflet summarises what is currently known about the relationship between fractures and physical abuse and will be of particular interest to paediatricians, general
CORE-INFO: fractures in children This leaflet summarises what is currently known about the relationship between fractures and physical abuse and will be of particular interest to paediatricians, general
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines
 Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics
 Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics Disclosure I have nothing to disclose Objectives Describe common accidental injuries which can be confused with child abuse Describe
Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics Disclosure I have nothing to disclose Objectives Describe common accidental injuries which can be confused with child abuse Describe
10/8/17. I have no disclosures. What are they? Upper extremity fractures Lower extremity fractures Non accidental trauma
 I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast
 The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
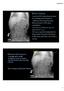 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
Evaluation of a Pediatric Patient
 September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
The Viewing Study Guide for Physical Abuse Slides
 The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains
 5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
Disclosure. Physical Abuse. Objectives. What is the Mechanism of the Injury?
 Disclosure Abuse or Not Abuse: What is the Answer? Natalie Kissoon, MD Assistant Professor Division of Child Abuse Pediatrics University of Texas Health Science Natalie Kissoon, MD has no relationships
Disclosure Abuse or Not Abuse: What is the Answer? Natalie Kissoon, MD Assistant Professor Division of Child Abuse Pediatrics University of Texas Health Science Natalie Kissoon, MD has no relationships
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age. DRAFT REVIEW May 2008
 Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Evidence Base for Child Abuse Fractures
 Evidence Base for Child Abuse Fractures SPR Sunrise Session May 17, 2018 Megan B. Marine, MD, FAAP Assistant Professor of Clinical Radiology, Pediatric Division Co-Director, Pediatric Radiology Fellowship
Evidence Base for Child Abuse Fractures SPR Sunrise Session May 17, 2018 Megan B. Marine, MD, FAAP Assistant Professor of Clinical Radiology, Pediatric Division Co-Director, Pediatric Radiology Fellowship
Date of Admission: [DATE]. Date of Discharge:
![Date of Admission: [DATE]. Date of Discharge: Date of Admission: [DATE]. Date of Discharge:](/thumbs/74/71277118.jpg) Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes. Lisa Schwing, RN Trauma Program Manager Dayton Children s
 Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Common Abusive Skeletal Injuries
 Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Homework Assignment Complete and Place in Binder
 Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
Homework Assignment Complete and Place in Binder Chapter # 34/35: Pediatric & Geriatric Emergencies 1. The first month of life after birth is referred to as the: A) neonatal period. B) toddler period.
OVERVIEW OF CHILD PHYSICAL ABUSE
 2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Bone Injuries and Treatment. Fractures and Dislocations
 Bone Injuries and Treatment Fractures and Dislocations Bellwork Research the small bones in the foot and wrist. Draw them in your notes. State Standards 16) Understand principles of and successfully perform
Bone Injuries and Treatment Fractures and Dislocations Bellwork Research the small bones in the foot and wrist. Draw them in your notes. State Standards 16) Understand principles of and successfully perform
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Concussion. Concussion is a disturbance of brain function caused by a direct or indirect force to the head.
 Concussion Concussion is a disturbance of brain function caused by a direct or indirect force to the head. Disturbances of brain tissue is largely related to neurometabolic dysfunction rather then structural
Concussion Concussion is a disturbance of brain function caused by a direct or indirect force to the head. Disturbances of brain tissue is largely related to neurometabolic dysfunction rather then structural
Orthopedics. 1. GOAL: Understand the pediatrician's role in preventing and screening for
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages.
 Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation **
 PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
EPIPHYSEAL PLATE IN FEMUR
 Reviewing: Epiphyseal Plates (younger skeletons) eventually will disappear. Bones grow lengthwise up and down from each plate, and in a circular collar like fashion around the diaphysis. These plates will
Reviewing: Epiphyseal Plates (younger skeletons) eventually will disappear. Bones grow lengthwise up and down from each plate, and in a circular collar like fashion around the diaphysis. These plates will
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History: History of Fractures Questionnaire
 PhenX Measure: Fracture History (#170900) PhenX Protocol: Fracture History (#170901) Date of Interview/Examination (MM/DD/YYYY): Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History:
PhenX Measure: Fracture History (#170900) PhenX Protocol: Fracture History (#170901) Date of Interview/Examination (MM/DD/YYYY): Part I : Study of Osteoporotic Fractures (SOF) Fractures and Falls History:
CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect
 CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect I. IDENTIFY THE CHILD WHO MAY BE A VICTIM OF ABUSE OR NEGLECT. A. Injuries
CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect I. IDENTIFY THE CHILD WHO MAY BE A VICTIM OF ABUSE OR NEGLECT. A. Injuries
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Neuropathology Of Head Trauma. Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center
 Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition
 Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Injuries to the Head and Spine From Bradys Emergency Care 10 th Edition 1. When performing the four-rescuer log roll, which responder pulls the board into position? A.) Head B.) Waist C.) Knee D.) Shoulder
Disclosure. Pediatric Orthopedic Emergencies. I have no actual or potential conflict of interest in relation to this program or presentation.
 Pediatric Orthopedic Emergencies Robin Pearce MSN, RN-BC Trauma Performance Improvement Manager Henrico Doctors Hospital, Forest Disclosure I have no actual or potential conflict of interest in relation
Pediatric Orthopedic Emergencies Robin Pearce MSN, RN-BC Trauma Performance Improvement Manager Henrico Doctors Hospital, Forest Disclosure I have no actual or potential conflict of interest in relation
Eye findings associated with abusive head. trauma (AHT) Mark Jacobs Staff Specialist Ophthalmologist Sydney Children s Hospital
 Eye findings associated with abusive head Mark Jacobs Staff Specialist Ophthalmologist Sydney Children s Hospital Gaurav Bhardwaj Ophthalmology Fellow trauma (AHT) Retinal haemorrhages in AHT Retinal anatomy
Eye findings associated with abusive head Mark Jacobs Staff Specialist Ophthalmologist Sydney Children s Hospital Gaurav Bhardwaj Ophthalmology Fellow trauma (AHT) Retinal haemorrhages in AHT Retinal anatomy
ORTHOPEDIC ASPECTS CHILD ABUSE. A summary of the physical, metaphysical, psychological, and sociological aspects of Non-
 ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
SPRINGFIELD CLINIC S
 SPRINGFIELD CLINIC S HEAD INJURY MANAGEMENT GUIDE FOR PARENTS Given the complexities of concussion management, Springfield Clinic recognizes the importance of managing concussions on an individualized
SPRINGFIELD CLINIC S HEAD INJURY MANAGEMENT GUIDE FOR PARENTS Given the complexities of concussion management, Springfield Clinic recognizes the importance of managing concussions on an individualized
Present-on-Admission (POA) Coding
 1 Present-on-Admission (POA) Coding Michael Pine, MD, MBA Michael Pine and Associates, Inc 2 POA and Coding Guidelines (1) Unless otherwise specified, a POA modifier must be assigned to each principal
1 Present-on-Admission (POA) Coding Michael Pine, MD, MBA Michael Pine and Associates, Inc 2 POA and Coding Guidelines (1) Unless otherwise specified, a POA modifier must be assigned to each principal
They re not little adults, but they are little humans. Pearls for your next pediatric trauma patient. Children are little humans
 They re not little adults, but they are little humans Pearls for your next pediatric trauma patient Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago Alisa McQueen
They re not little adults, but they are little humans Pearls for your next pediatric trauma patient Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago Alisa McQueen
6/23/2017. What do you see? skull fracture
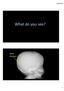 What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries. Differentiate when an orthopedic injury is a medical emergency
 1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
1 2 How to Triage Orthopaedic Care David W. Gray, M.D. OBJECTIVES: Define basic assessments skills needed to identify orthopedic injuries Differentiate when an orthopedic injury is a medical emergency
CASE NO: 1 PATIENT DETAILS : Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO :
 CASE NO: 1 PATIENT DETAILS : Name : XXXX Age : 53yr Sex : Female Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO : 201518441 CHIEF COMPLAINTS : - Pain in the right knee since
CASE NO: 1 PATIENT DETAILS : Name : XXXX Age : 53yr Sex : Female Occupation : Housewife Date Of Admission :11/06/15 Residence : Nalgonda IP NO : 201518441 CHIEF COMPLAINTS : - Pain in the right knee since
General appearance examination
 Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
Childhood athletic participation has dramatically increased over the past twenty years. Children are being introduced to organised sports at increasingly immature stages of physical development. It is
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
4/28/11 OBJECTIVES CASE. Solving a Mystery of Child Sexual Abuse: The Roles of the Clinician and CPS
 Solving a Mystery of Child Sexual Abuse: The Roles of the Clinician and CPS ANN S. BOTASH, MD DIRECTOR, CARE PROFESSOR OF PEDIATRICS OBJECTIVES Explain why all children suspected of being sexually abused
Solving a Mystery of Child Sexual Abuse: The Roles of the Clinician and CPS ANN S. BOTASH, MD DIRECTOR, CARE PROFESSOR OF PEDIATRICS OBJECTIVES Explain why all children suspected of being sexually abused
Referral Criteria for Medical CT Radiation Exposures. Neuro Referrals
 Referral Criteria for Medical CT Radiation Exposures Neuro Referrals CHH & HRI The Ionising Radiation (Medical Exposure) Regulations 2017 Document Control Reference No: 3.2 First published: 2016 Version:
Referral Criteria for Medical CT Radiation Exposures Neuro Referrals CHH & HRI The Ionising Radiation (Medical Exposure) Regulations 2017 Document Control Reference No: 3.2 First published: 2016 Version:
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
Faculty of Clinical Forensic Medicine Committee 1/2018
 Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Guideline Subject: Clinical Forensic Assessment and Management of Non-Fatal Strangulation Approval Date: January 2018 Review Date: January 2021 Review By: Number: Faculty of Clinical Forensic Medicine
Pediatric Fractures. Objectives. Epiphyseal Complex. Anatomy and Physiology. Ligaments. Bony matrix
 1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
1 Pediatric Fractures Nicholas White, MD Assistant Professor of Pediatrics Eastern Virginia Medical School Attending, Pediatric Emergency Department Children s Hospital of The King s Daughters Objectives
The scapula is located on the back side of the ribcage and helps provide part of the shoulder joint and movement for the arms.
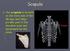 The scapula is located on the back side of the ribcage and helps provide part of the shoulder joint and movement for the arms. Scapula Humerus (Upper Arm Bone) Radius and Ulna Radius on Top Ulna on Bottom
The scapula is located on the back side of the ribcage and helps provide part of the shoulder joint and movement for the arms. Scapula Humerus (Upper Arm Bone) Radius and Ulna Radius on Top Ulna on Bottom
Introduction to Fractures. Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 3
 Introduction to Fractures Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 3 Definitions A fracture is an interruption in the continuity of bone Fracture = Break Fracture: mechanical damage produced in a
Introduction to Fractures Traumatology RHS 231 Dr. Einas Al-Eisa Lecture 3 Definitions A fracture is an interruption in the continuity of bone Fracture = Break Fracture: mechanical damage produced in a
Overview. Overview. Chapter 30. Injuries to the Head and Spine 9/11/2012. Review of the Nervous and Skeletal Systems. Devices for Immobilization
 Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Chapter 30 Injuries to the Head and Spine Slide 1 Overview Review of the Nervous and Skeletal Systems The Nervous System The Skeletal System Devices for Immobilization Cervical Spine Short Backboards Long
Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures
 July 2006 Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures Denise De Las Nueces, Harvard Medical School Year IV General Overview Introduction
July 2006 Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures Denise De Las Nueces, Harvard Medical School Year IV General Overview Introduction
New Patient Pain Evaluation
 New Patient Pain Evaluation Name: Date: Using the following symbols, mark the areas of the body diagrams which are affected by your pain: \\ = Stabbing * = Electrical X = Aching N = Numbness 0 = Dull S
New Patient Pain Evaluation Name: Date: Using the following symbols, mark the areas of the body diagrams which are affected by your pain: \\ = Stabbing * = Electrical X = Aching N = Numbness 0 = Dull S
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C)
 Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Critical Incidents Reported to Manitoba Health
 Critical Incidents Reported to Manitoba Health April 1, 2013 - June 30, 2013 Degree of PCH resident had unwitnessed fall resulting in fractured hip. Found on floor with walker by feet. Surgical repair
Critical Incidents Reported to Manitoba Health April 1, 2013 - June 30, 2013 Degree of PCH resident had unwitnessed fall resulting in fractured hip. Found on floor with walker by feet. Surgical repair
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
UPPER BODY STANDING 12. March in place (hand to opposite knee) For more intensity raise arms above head if your balance is GOOD. 13.
 LOW IMPACT EXERCISES SITTING 1. Breathe 2. Half circles with head 3. Neck movements (Chin to chest, ear to shoulder) 4. Neck Stretch Sitting in your chair, reach down and grab the side of the chair with
LOW IMPACT EXERCISES SITTING 1. Breathe 2. Half circles with head 3. Neck movements (Chin to chest, ear to shoulder) 4. Neck Stretch Sitting in your chair, reach down and grab the side of the chair with
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Home Address. City Postal Code Home Telephone # Business Telephone # Address. Emergency Contact Name, Address, Phone#
 Date Name / / last first middle initial Personal Health # - Male Female Home Address City Postal Code Home Telephone # Business Telephone # Cell # E-Mail Address Best way to contact you: Home # Work #
Date Name / / last first middle initial Personal Health # - Male Female Home Address City Postal Code Home Telephone # Business Telephone # Cell # E-Mail Address Best way to contact you: Home # Work #
Pediatric Orthopedics
 Pediatric Orthopedics Alexander Rogers, MD Associate Professor Emergency Medicine and Pediatrics Michigan Medicine/University of Michigan Disclosures I have no conflicts of interest to disclose I will
Pediatric Orthopedics Alexander Rogers, MD Associate Professor Emergency Medicine and Pediatrics Michigan Medicine/University of Michigan Disclosures I have no conflicts of interest to disclose I will
Med 536 Communicating About Prognosis Workshop. Case 1
 Med 536 Communicating About Prognosis Workshop Case 1 ID / CC: 39 year-old woman status-post motor-vehicle collision History of the Presenting Illness Previously healthy 39 year-old woman was found in
Med 536 Communicating About Prognosis Workshop Case 1 ID / CC: 39 year-old woman status-post motor-vehicle collision History of the Presenting Illness Previously healthy 39 year-old woman was found in
Name Date Score. Skeletal System. Indicate if the following statements are true or false. Correct false statements
 Name Date Score Skeletal System True/False Indicate if the following statements are true or false. Correct false statements 1. Bones surround vital organs to protect them. 2. Bones store most of the calcium
Name Date Score Skeletal System True/False Indicate if the following statements are true or false. Correct false statements 1. Bones surround vital organs to protect them. 2. Bones store most of the calcium
 3 The definition of elder physical abuse is any action by a caregiver that is meant to cause harm or fear in another person. Physical abuse includes pain or injury, hitting, pushing, pinching, and
3 The definition of elder physical abuse is any action by a caregiver that is meant to cause harm or fear in another person. Physical abuse includes pain or injury, hitting, pushing, pinching, and
of Trauma Assembly 27 th Page 1
 Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Injuries to Muscles, Bones and Joints. Emergency Medical Response
 Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Major Functions of the Skeletal System
 Skeletal System Major Functions of the Skeletal System 1. Provide shape and support. 2. Enables you to move 3. Protects your organs 4. Produces blood cells 5. stores minerals and other materials until
Skeletal System Major Functions of the Skeletal System 1. Provide shape and support. 2. Enables you to move 3. Protects your organs 4. Produces blood cells 5. stores minerals and other materials until
A N.S. Technologists Experiences
 A N.S. Technologists Experiences I have nothing to disclose What does appropriate imaging mean For radiologists? For technologists? How does this affect patients and technologists? Discuss ordering trends
A N.S. Technologists Experiences I have nothing to disclose What does appropriate imaging mean For radiologists? For technologists? How does this affect patients and technologists? Discuss ordering trends
Evaluation and Stabilization of the Athlete with Possible Spine Injury
 Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Evaluation and Stabilization of the Athlete with Possible Spine Injury Jeffrey H. Bohmer, MD, FACEP Emergency Physician Northwestern Medicine Central DuPage Hospital June 12, 2015 Introduction Goals: 1.
Common Orthopaedic Injuries in Children
 Common Orthopaedic Injuries in Children Rakesh P. Mashru, M.D. Division of Orthopaedic Trauma Cooper University Hospital Cooper Medical School of Rowan University December 1, 2017 1 Learning Objectives
Common Orthopaedic Injuries in Children Rakesh P. Mashru, M.D. Division of Orthopaedic Trauma Cooper University Hospital Cooper Medical School of Rowan University December 1, 2017 1 Learning Objectives
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Prevention Diagnosis
 Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
Prevention and Management of Positional Skull Deformities in Infants John Persing, MD, Hector James, MD, Jack Swanson, MD, John Kattwinkel, MD, Committee on Practice and Ambulatory Medicine, Section on
Surgery-Ortho. Fractures of the tibia and fibula. Management. Treatment of low energy fractures. Fifth stage. Lec-6 د.
 Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
Fifth stage Lec-6 د. مثنى Surgery-Ortho 28/4/2016 Indirect force: (low energy) Fractures of the tibia and fibula Twisting: spiral fractures of both bones Angulatory: oblique fractures with butterfly segment.
A Patient s Guide to Nursemaid's Elbow in Children. PHYSIO.coza
 A Patient s Guide to Nursemaid's Elbow in Children SANDTON MEDICLINIC 011 706 7495 FAIRWAYS LIFE HOSPITAL 011 875 1827 ST STITHIANS 082 378 9642 JEPPE BOYS HIGH SCHOOL 084 816 5457 JOHANNESBURG, SANDTON@PHYSIO.CO.ZA
A Patient s Guide to Nursemaid's Elbow in Children SANDTON MEDICLINIC 011 706 7495 FAIRWAYS LIFE HOSPITAL 011 875 1827 ST STITHIANS 082 378 9642 JEPPE BOYS HIGH SCHOOL 084 816 5457 JOHANNESBURG, SANDTON@PHYSIO.CO.ZA
Pediatric Injuries/Fractures. Rena Heathcote
 Pediatric Injuries/Fractures Rena Heathcote INTRODUCTION Incidence Anatomy of the Growing Bone Injury Patterns What can we X-ray PEDIATRIC FRACTURES INCIDENCE What makes children susceptible to fractures?
Pediatric Injuries/Fractures Rena Heathcote INTRODUCTION Incidence Anatomy of the Growing Bone Injury Patterns What can we X-ray PEDIATRIC FRACTURES INCIDENCE What makes children susceptible to fractures?
Goals. Initial management skeletal trauma. Physical Exam ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT 12/4/2010
 ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
ABC OF PRIMARY CARE MEDICINE FRACTURE MANAGEMENT Brian Feeley, MD UCSF Sports Medicine and Shoulder Surgery Goals Discuss common fractures and initial management, treatment guidelines Let your patients
Basic Care of Common Fractures Utku Kandemir, MD
 Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Basic Care of Common Fractures Utku Kandemir, MD Assistant Clinical Professor Trauma & Sports Medicine Dept. of Orthopaedic Surgery UCSF / SFGH History Physical Exam Radiology Treatment History Acute trauma
Abuse Or Not? Interactive Visual Clues in Child Abuse
 Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
August 2012 CE. Site code # E Reading the Scene
 August 2012 CE Site code # 107200E-1212 Reading the Scene Prepared by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit: www.advocatehealth.com/condell/body.cfm?id=422 Date of
August 2012 CE Site code # 107200E-1212 Reading the Scene Prepared by Sharon Hopkins, RN, BSN, EMT-P To view on the Advocate Condell website visit: www.advocatehealth.com/condell/body.cfm?id=422 Date of
Activity Three: Where s the Bleeding?
 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
OSTEOPOROSIS. stay active and exercise TO STAY STRONG
 OSTEOPOROSIS stay active and exercise TO STAY STRONG INTRODUCTION 1 TIPS FOR DAILY ACTIVITIES 1 WEIGHT-BEARING EXERCISES 2 OVERALL STRENGTHENING EXERCISES 2 EXERCISES TO AVOID 2 POSTURAL STRENGTHENING
OSTEOPOROSIS stay active and exercise TO STAY STRONG INTRODUCTION 1 TIPS FOR DAILY ACTIVITIES 1 WEIGHT-BEARING EXERCISES 2 OVERALL STRENGTHENING EXERCISES 2 EXERCISES TO AVOID 2 POSTURAL STRENGTHENING
UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT
 UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT PremierOrtho.com UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT Table of Contents Introduction...3 Causes...4 Who s at Risk?...5
UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT PremierOrtho.com UNDERSTANDING FRACTURE CARE CAUSES, DIAGNOSIS, AND TREATMENT Table of Contents Introduction...3 Causes...4 Who s at Risk?...5
TRAINING LAB SKELETAL REMAINS: IDENTIFYING BONES NAME
 TRAINING LAB SKELETAL REMAINS: IDENTIFYING BONES NAME Background: Skeletal remains are important pieces of evidence. The flesh, muscle, and organs of a victim rapidly decompose; however, the victim s skeleton
TRAINING LAB SKELETAL REMAINS: IDENTIFYING BONES NAME Background: Skeletal remains are important pieces of evidence. The flesh, muscle, and organs of a victim rapidly decompose; however, the victim s skeleton
Coding Companion for Emergency Medicine. A comprehensive illustrated guide to coding and reimbursement
 Coding Companion for Emergency Medicine A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Skin/Incision...1 Debridement...7 Excision...14
Coding Companion for Emergency Medicine A comprehensive illustrated guide to coding and reimbursement 2013 Contents Getting Started with Coding Companion...i Skin/Incision...1 Debridement...7 Excision...14
