Annotation. Outcomes of infants and children with inflicted traumatic brain injury
|
|
|
- Winifred Turner
- 5 years ago
- Views:
Transcription
1 Outcomes of infants and children with inflicted traumatic brain injury Kathi L Makaroff* MD, Research Instructor of Pediatrics; Frank W Putnam MD, Director, Mayerson Center for Safe and Healthy Children, Children s Hospital Medical Center, Cincinnati, OH, USA. Annotation *Correspondence to first author at Mayerson Center for Safe and Healthy Children, Children s Hospital Medical Center, SEB-5, 3333 Burnet Avenue, Cincinnati, OH 45229, USA. makok0@chmcc.org Inflicted traumatic brain injury (ITBI) or shaken baby syndrome is recognized as a major cause of disability and death in the pediatric population. Although advances have been made in the recognition of the clinical, radiographic, and pathological findings of ITBI, less is known about the long-term outcomes of survivors. Health care providers recognize that these infants and children frequently have poor outcomes. Although an infant or child who sustains an ITBI may look well immediately after the trauma, that child may be left with serious and permanent disabilities. Here we review articles published since 1975 that discuss the outcomes of infants and children with ITBI. Only articles that had more specific outcome information than just survival were included in the survey. To find the articles, the Medline bibliographic database was searched with the following search terms: shaken baby syndrome, head injury, traumatic brain injury, impact injury, shaking impact syndrome, non-accidental injury, child abuse, inflicted injury, follow-up, outcome, neurological outcome, and vision. A bibliography search of articles was also used. Data extracted from the articles included: the number of patients studied, the patient s age at injury, the interval to outcome measurement (or age of patient at outcome measurement), the definition and qualification of injury, the outcome measures, and patient outcomes. Patients were categorized into outcome groups when possible (Table I), but ophthalmologic outcomes were not categorized into groups (Table II). Outcome groups include no deficits, mild deficits, moderate deficits, severe deficits, and death. Mild deficits include minor physical, cognitive, or behavioral problems that are still compatible with a normal life. Moderate deficits include more disabling physical, cognitive, or behavioral problems. A severe deficit includes moderate deficits that would require assistance for activities of daily living, and includes patients in a vegetative state. The articles are summarized in Tables I and II. Overview of acute injuries The precise type of inflicted trauma is seldom known because accurate histories are rarely provided, or might be deliberately misleading in cases of abusive head injury. However, there is a constellation of clinical, radiological, and pathological findings associated with ITBI that can help in making the diagnosis. The symptoms and physical signs may include those of head injury and/or increased intracranial pressure: seizures, apnea, decreased level of consciousness, and neurological abnormalities. Often, however, there are only mild neurological signs such as fussiness, vomiting in the absence of diarrhea, or a history of lethargy. Although not always present, bruising of the head or face in an infant or non-mobile child is associated with abusive head injury. 1 Retinal hemorrhages are present in up to 80% of cases; they can be unilateral or bilateral. 2 Retinal hemorrhages infrequently occur from accidental and non-traumatic events. When retinal hemorrhages do occur after accidental injury they are usually few and confined to the posterior pole, which often differs from the extent of hemorrhages seen with ITBI. 2 Other ocular findings associated with ITBI include retinal folds or detachments and other internal eye injuries. 2 ITBI is usually associated with radiological findings. Subdural and subarachnoid hemorrhages are frequently noted, while skull and other fractures of the skeletal system are seen less frequently. Shaking while holding or squeezing the thorax can result in rib fractures and/or metaphyseal fractures. Parenchymal brain lesions such as shearing injuries, axonal injury, and hypoxic ischemic changes may be present but are challenging to identify with standard imaging techniques. Autopsy may reveal brain parenchymal lesions in cases of fatal inflicted brain injury that were not visible radiographically. The autopsy may also show cerebral tissue tears, contusions, subgaleal hemorrhage, and other signs of head impact not noted clinically. Axonal disruptions can be discovered on autopsy, but special stains or immunohistology techniques are often necessary to demonstrate these disruptions. Localized or generalized brain swelling is frequently noted as well. Some infants and children who suffer fatal inflicted brain injuries also have damage of the cervical spinal cord; evidence of this injury is sometimes visible only on post-mortem specimens. 3 Acute Developmental Medicine & Child Neurology 2003, 45:
2 skeletal fractures are sometimes not evident radiographically but are picked up on autopsy. Overview of outcomes The majority of patients with inflicted head injuries have poor outcomes. In reviewed articles from the past 27 years, almost one-fifth of the patients died, and about half were left with some impairment. Only 22% of patients had no impairments (see Tables I and II). Most of the surviving children with inflicted head injury were left with impairments in their motor and cognitive abilities, language, vision, and behavior. These impairments affect a child s capacity to interact with the environment, which in turn might contribute to later problems with education and social attainment. Table I: Outcomes of infants and children with inflicted traumatic brain injury Reference n Age at injury Interval to [age at] outcome Definition of injury pts <6mo; N/A Confirmed diagnosis of non-accidental head injury 3 pts >1y mo; 3 122mo; Non-accidental head injury : head injury plus two of the mean: 5.1mo mean: 33mo following: retinal hemorrhages, skeletal fractures, soft tissue injury, inconsistent history mo; 3mo Inflicted traumatic brain injury : algorithm similar to mean: 9.3mo Duhaime et al mean: 10.6mo mean: 1.3mo Inflicted traumatic brain injury : algorithm similar to Duhaime et al d 4.5y; [4 34mo; mean: 17.4mo] Confirmed non-accidental head injury : witnessed event, mean: 12.2mo N/A perpetrator confession, felony conviction or physical evidence of injury without trauma history wk 21mo 4 14y; Whiplash shaken infant syndrome : intraocular and mean: 7.2y intracranial hemorrhages in absence of traumatic or non-traumatic mechanism pts: 0 12mo; 1mo 5y; Shaken baby syndrome : subdural hematomas, 24 pts: 13 36mo mean: 26mo skeletal injuries, no history mo; 12 56mo Shaken baby syndrome : intraocular hemorrhages, mean: 10.5mo intracranial hemorrhages, absence of external signs of head trauma mo 2y; [ y; mean: 9y] Shaken-impact syndrome : extracranial bleed in mean: 6.4mo absence of other diagnosis and other supportive findings mo, 7mo, N/A Non-accidental injury : children under two years of age 9mo, 3mo; with an unexplained subdural hematoma and determined mean: 6mo to be child abuse by case conference Pt, patient. 498 Developmental Medicine & Child Neurology 2003, 45:
3 The reasons for the poor outcomes in infants and children who sustain ITBI are not known. Some authors have shown that infants and children who suffer non-accidental head injuries have evidence of ischemia and hypoxia, as measured by blood pressure, arterial hypoxia, 4 and cerebral perfusion pressure. 5 These authors postulate that early brain hypoxia ischemia is an important cause of poor outcomes in this Table I: continued Outcome measures Outcomes/comments group. Another explanation involves secondary neuronal injury from a metabolic insult. The initial trauma (i.e. shaking) is the initiating event that causes a metabolic cascade of neurotoxic factors which continue to damage neurons once the trauma has ceased. Other investigators have shown that cervical spine injury may influence the degree of injury. Feldman and colleagues demonstrated that four of five children with fatal abusive head injury had extra-axial bleeds at the level of the cervical spinal cord on autopsy. 3 This paper and earlier work predicted that cervical spine injury might have a role in the outcomes of these children. 3,6 Although the mechanisms are not fully understood, it is well recognized by clinicians that most infants and children who sustain ITBI do not do well after the injury. Six-point outcome scale Glasgow Outcome Scale Bayley-II Bayley Behavior Scale Glasgow Outcome Scale Bayley-II Stanford-Binet McCarthy Denver II Neurological examinations Vision screening Assessments: General Neurological Psychological Social Testing: Gesell WISC Terman Neurological examination Late neurological score Grades similar to Glasgow Outcome Scale 9 pts had no deficits 7 pts had moderate deficits 8 pts had severe deficits 4 pts died 7 pts had no deficits 2 pts had mild deficits 3 pts had moderate deficits 3 pts had severe deficits Pts in inflicted group scored lower in all domains than a control group 4 pts had no deficits 13 pts had moderate deficits 3 pts had severe deficits 2 pts had mild deficits 3 pts had moderate deficits 6 pts had severe deficits 3 pts died 11 pts had moderate to severe deficits 1 pt died 22 pts had no deficits 8 pts had a mild deficit 26 pts had a severe deficit 36 pts died for 31 pts there was no information 2 pts had mild deficits 5 pts had moderate to severe deficits 4 pts were unavailable for follow-up 2 pts had no deficits 5 pts had moderate deficits 6 pts had a severe deficits 1 pt died 1 pt had mild deficits 1 pt had moderate deficits 2 pts had severe deficits Developmental and behavioral outcomes Few studies have systematically studied the effect of ITBI on developmental and behavioral outcomes (Table I). Ewing- Cobbs and colleagues 7 performed developmental measures on infants and children after ITBI at an average of 1.3 months after the injury: 45% of the patients scored in the mentally deficient range for cognitive testing (group mean: 78.2) and 25% of the patients scored in the mentally deficient range for motor testing (group mean: 80.3). In a second study, Ewing-Cobbs and colleagues 8 evaluated infants and young children with ITBI at an average of 4.6 months after injury. Mean scores for both the cognitive and motor domains were in the low average range. Almost half of the infants and young children also had impaired scores for emotional regulation and motor quality. Other studies have demonstrated that most children with non-accidental head injury show developmental delays and mental retardation*. 9,10 Impairments such as learning disabilities and behavior problems might not manifest until a child attends school, and so continuing developmental evaluations are important to ensure that children with late sequelae from traumatic brain injury are recognized. Visual outcomes Visual impairment and blindness are documented problems after ITBI (Table II). In one large study, over 70% of patients were reported to see well, as measured by visual acuity and visual fields testing, at their last follow-up visit; 25% of patients had some visual impairment, as measured by visual acuity and visual fields testing. 11 Cortical injury, and not retinal hemorrhage, is thought to be the most significant cause of long-term visual impairment and blindness after ITBI. Studies that examine the visual outcomes of infants and children who sustain ITBI show a variety of causes for the impairment, including occipital lobe injury, occipital lobe atrophy, optic atrophy, retinal fibrosis, and retinal scarring. Visual impairments can also contribute to developmental deficits, learning problems, and social attainment Age at time of injury and outcomes In the literature for the past 27 years that we reviewed, the mean age of all patients at time of injury (in studies in which the age at time of injury was reported) was 6.2 months (SD 2.7). Mean age of the patients at time of injury who died as a result of their injuries was 7.7 months (SD 7.2). Mean age of patients at *UK usage: learning disability. Annotation 499
4 time of injury with no impairment was 5.2 months (SD 3.2) and the mean ages of patients at time of injury with mild and moderate to severe impairments were 6.5 months (SD 2.8) and 5.9 months (SD 8.0) respectively (see Tables I and II). There was no statistical difference in age at the time of injury among these outcome groups. Although no difference in age was identified in this review sample, future investigators should be alert to the possibility that age at injury might influence outcomes. Table I: continued Reference n Age at injury Interval to [age at] outcome Definition of injury mo; 3mo 3y; Non-accidental head injury : clinical, radiological and/or mean: 5.6mo mean: 14.8mo ophthalmologic evidence or if inconsistent history d 34mo; N/A Shaken baby syndrome : all presented with neurological mean: 6.4mo or cardiorespiratory symptoms mo; N/A Confirmed shaken baby syndrome : intraocular mean: 5.5mo hemorrhages, subdural or subarachnoid hemorrhages with a history of suspected abuse mo; [8 15y; mean: 10.1y] Shaken baby syndrome : intracranial and retinal mean: 4.1mo hemorrhages in absence of head trauma wk 4mo; 4mo 1y; Non-accidental head injury : (also had cortical mean: 10.6wk mean: 6.4mo tears by ultrasound) mo; N/A Whiplash shaken infant syndrome : history of shaking mean: 4.6mo or intracranial and intraocular hemorrhages in the absence of signs of external trauma mo, 5wk, N/A, N/A, Shaking injuries : neurological and ophthalmologic 6wk, 4mo 5mo, [10mo] abnormalities mo; N/A Shaken baby syndrome : perpetrator confession or no other mean: 5.8mo diagnosis for findings mo, 3.5mo, [7y, 5.2y, 4.2y] Brain damage : by shaking, swinging, hitting, and throwing 7mo Pt, patient. Table II: Ophthalmologic outcomes of infants and children with inflicted traumatic brain injury Reference n Age at injury Interval to outcome Definition of injury pts: 0 12mo; 1mo 7y; Shaken baby syndrome : subdural hematomas, 24 pts: 13 36mo mean: 21mo skeletal injuries, no history mo; 1 36mo; Shaken baby syndrome : bilateral retinal hemorrhages, mean: 9.3mo mean: 6.7mo inconsistent history, other signs of abuse or previous suspicious episode of abuse 25 6 mean: 9.1mo 12 55mo; Shaken baby syndrome : retinal, vitreous or subhyaloid mean: 29.8mo hemorrhage with intracranial injury and without external signs of head trauma Pt, patient. 500 Developmental Medicine & Child Neurology 2003, 45:
5 Some investigators have demonstrated that age less than or equal to 6 months is an indicator of poor prognosis. 12,14 The mean interval to the time of outcome measures (in studies in which interval to the time of outcome measures was reported) was 15 months (SD 13.6). Some deficits might not have been apparent at that time because some learning disabilities and behavior problems might not manifest until a child is older and is attending school. Table I: continued Outcome measures Developmental status Behavioral status Visual status Neurological examinations Cognitive status Behavioral status Neurological assessment Developmental assessment Developmental evaluations Psychological testing Assessment of neurol. status Developmental status Developmental status Table II: continued Outcome measures Ophthalmologic examination Ophthalmologic examination Ophthalmologic examination Outcomes/comments 1 pt had mild deficits 4 pts had moderate deficits 7 pts had severe deficits 14 pts had no deficits 4 pts had mild deficits 6 pts had severe deficits 1 for 2 pts there was no information 2 pts had no deficits 2 pts had moderate to severe deficits 1 pt had severe deficits 3 pts had no deficits 7 pts had some deficits 5 pts had moderate to severe deficits 1 pt died 3 pts had mild deficits 4 pts had moderate deficits 7 pts had severe deficits 4 pts had severe deficits 7 pts had no deficits 10 pts had moderate to severe deficits 3 pts died 3 pts had severe deficits Outcomes/comments 49 pts had good vision 19 pts had poor vision (only 68 pt records could be assessed) 17 pts had a good visual outcome 5 pts were left with poor vision 8 pts died 1 pt had a minor visual deficit 2 pts had moderate visual loss in one eye 3 pts had profound visual loss Conclusions Because the outcomes of many children who have sustained ITBI are poor, efforts should be directed at improving the identification of the specific deficits and improving outcomes. Although research has been directed toward the rehabilitation of children with traumatic brain injury, more investigation is needed in the specific rehabilitation of infants and children with ITBI, because the type of injury sustained by these two groups and, therefore, their outcomes, might differ. Neurological, behavioral, and developmental impairments can be seen after ITBI even when there is apparent early, good recovery. Because of this, developmental assessments of these children should be continued throughout the school years. Finally, given the high incidence of death and disabilities that follows an ITBI, the negative psychosocial effects on the children, and the high health care costs required for diagnosis and treatment, prevention programs should be increased. Research into prevention should be encouraged, and parents, future parents, and caregivers must be educated about the dangers of shaking infants and children. DOI: /S Accepted for publication 4th February References 1. Sugar NF, Taylor JA, Feldman KW. (1999) Bruises in infants and toddlers: those who don t cruise rarely bruise. Arch Pediatr Adolesc Med 153: Levin AV. (2000) Retinal hemorrhages and child abuse. In: David TJ, editor. Recent Advances in Pediatrics. London: Churchill Livingston. p Feldman KW, Weinberger E, Milstein J, Fligner CL. (1997) Cervical spine MRI in abused infants. Child Abuse Neglect 21: Johnson DL, Boal D, Baule R. (1995) Role of apnea in nonaccidental head injury. Pediatr Neurosurg 23: Barlow KM, Minns RA. (1999) The relationship between intracranial pressure and outcome in non-accidental head injury. Dev Med Child Neurol 4: Hadley M, Sonntag V, Rekate H, Murphy A. (1989) The infant whiplash-shake injury syndrome: a clinical and pathological study. Neurosurgery 24: Ewing-Cobbs L, Kramer L, Prasad M, Canales DN, Louis PT, Fletcher JM, Vollero H, Landry SH, Cheung K. (1998) Neuroimaging, physical, and developmental findings after inflicted and noninflicted traumatic brain injury in young children. Pediatrics 102: Ewing-Cobbs L, Prasad M, Kramer L, Landry S. (1999) Inflicted traumatic brain injury: relationship of developmental outcome to severity of injury. Pediatr Neurosurg 31: Gilles EE, Nelson MD. (1998) Cerebral complications of nonaccidental head injury in childhood. Pediatr Neurol 19: Bonnier C, Nassogne MC, Evrard P. (1995) Outcome and prognosis of whiplash shaken infant syndrome: late consequences after a symptom-free interval. Dev Med Child Neurol 37: Kivlin JD, Simons KB, Lazoritz S, Ruttum MS. (2000) Shaken baby syndrome. Ophthalmology 107: Wilkerson WS, Han DP, Rappley MD, Owings CL. (1989) Retinal hemorrhage predicts neurologic injury in the shaken baby syndrome. Arch Ophthalmol 107: McCabe F, Donahue SP. (2000) Prognostic indicators for vision and mortality in shaken baby syndrome. Arch Ophthalmol 118: Annotation 501
6 14. Duhaime AC, Christian C, Moss E, Seidl T. (1996) Long-term outcome in infants with the shaking-impact syndrome. Pediatr Neurosurg 24: Fung ELW, Sung RYT, Nelson EAS, Poon WS. (2002) Unexplained subdural hematoma in young children: is it always child abuse? Pediatr Int 44: Haviland J, Russel RI. (1997) Outcome after severe nonaccidental head injury. Arch Dis Child 77: Swenson J, Levitt C. (1997) Shaken baby syndrome diagnosis and prevention. Minn Med 80: Matthews GP, Das A. (1996) Dense vitreous hemorrhages predict poor visual and neurological prognosis in infants with shaken baby syndrome. J Pediatr Ophthalmol Strabismus 33: Fischer H, Allasio D. (1994) Permanently damaged: long-term follow-up of shaken babies. Pediatrics 33: Jaspan T, Narborough G, Punt JAG, Lowe J. (1992) Cerebral contusional tears as a marker of child abuse-detection by cranial sonography. Pediatr Radiol 22: Sinal SH, Ball MR. (1987) Head trauma due to child abuse: serial computerized tomography in diagnosis and management. South Med J 80: Frank Y, Zimmerman R, Leeds NMD. (1985) Neurological manifestations in abused children who have been shaken. Dev Med Child Neurol 27: Ludwig S, Warman M. (1984) Shaken baby syndrome: a review of 20 cases. Ann Emerg Med 13: Oliver JE. (1975) Microcephaly following baby battering and shaking. BMJ 2: Han DP, Wilkinson WS. (1990) Late ophthalmic manifestations of the shaken baby syndrome. J Pediatr Ophthalmol Strabismus 27: Duhaime AC, Alario AJ, Lewander WJ, Schut L, Sutton LN, Seidl TS, Nudelman S, Budnez D, Hertle R, Tsiaras W, Loporchio S. (1992) Head injury in very young children : mechanisms, injury types, and ophthalmologic findings in 100 hospitaliized patients younger than 2 years of age. Pediatrics 90: Mac Keith Meetings Programme Placenta (Closed meeting) 2 days 27th October 2003 New Neurosurgery for Children (Open meeting) 1 day 5 November 2003 Organizers: M Prendergast & J Punt Autistic Sub-groups with More Favourable Outcomes (Open meeting) 1 day 23 February 2004 Organizer: M Prendergast Diagnostic Labelling & Stigma (Closed meeting) 2 days 15 March 2004 To reserve places at Open Meetings please contact: Rachel Beresford-Peirse, Academic Administrator, Mac Keith Meetings, CME Department, The Royal Society of Medicine, 1 Wimpole Street, London W1M 8AE, UK. Tel: +44 (0) , Fax: +44 (0) Developmental Medicine & Child Neurology 2003, 45:
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
ARTICLE. Intracranial Hemorrhage in Children Younger Than 3 Years
 Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation **
 PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
Brain and Cervico-Medullary Injury : Patterns and Mechanisms
 Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review
 Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review M B Moss, MD; L Lanier, MD; R Slater; C L Sistrom, MD; R G Quisling, MD; I M Schmalfuss, MD; and D Rajderkar, MD Contact:
Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review M B Moss, MD; L Lanier, MD; R Slater; C L Sistrom, MD; R G Quisling, MD; I M Schmalfuss, MD; and D Rajderkar, MD Contact:
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines
 Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Evaluation of a Pediatric Patient
 September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages.
 Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Si n c e John Caffey first identified maltreatment as the. Neck injuries in young pediatric homicide victims. Clinical article
 J Neurosurg Pediatrics 3:000 000, 3:232 239, 2009 Neck injuries in young pediatric homicide victims Clinical article La u r a K. Br e n n a n, M.D., 1,2 Dav i d Ru b i n, M.D., M.S.C.E., 1,2 Ci n d y W.
J Neurosurg Pediatrics 3:000 000, 3:232 239, 2009 Neck injuries in young pediatric homicide victims Clinical article La u r a K. Br e n n a n, M.D., 1,2 Dav i d Ru b i n, M.D., M.S.C.E., 1,2 Ci n d y W.
S ubdural haemorrhage (SDH) in infants and young
 947 ORIGINAL ARTICLE Neuroradiological aspects of subdural haemorrhages S Datta, N Stoodley, S Jayawant, S Renowden, A Kemp... See end of article for authors affiliations... Correspondence to: Dr S Datta,
947 ORIGINAL ARTICLE Neuroradiological aspects of subdural haemorrhages S Datta, N Stoodley, S Jayawant, S Renowden, A Kemp... See end of article for authors affiliations... Correspondence to: Dr S Datta,
Suspected Physical Abuse Clinical Practice Guideline
 Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Eye findings associated with abusive head. trauma (AHT) Mark Jacobs Staff Specialist Ophthalmologist Sydney Children s Hospital
 Eye findings associated with abusive head Mark Jacobs Staff Specialist Ophthalmologist Sydney Children s Hospital Gaurav Bhardwaj Ophthalmology Fellow trauma (AHT) Retinal haemorrhages in AHT Retinal anatomy
Eye findings associated with abusive head Mark Jacobs Staff Specialist Ophthalmologist Sydney Children s Hospital Gaurav Bhardwaj Ophthalmology Fellow trauma (AHT) Retinal haemorrhages in AHT Retinal anatomy
Validity of Caregivers Reports on Head Trauma Due to Falls in Young Children Aged Less than 2 Years
 Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
Head Injury: Classification Most Severe to Least Severe
 Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
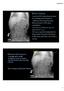 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age. DRAFT REVIEW May 2008
 Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Screening and Management of Blunt Cereberovascular Injuries (BCVI)
 Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Subdural haematoma and effusion in children aged < 2 years
 Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Visual Impairment & Eye Health in Children. Susan Cotter, OD, MS So CA College of Optometry Marshall B Ketchum University Fullerton, CA
 Visual Impairment & Eye Health in Children Susan Cotter, OD, MS So CA College of Optometry Marshall B Ketchum University Fullerton, CA Consequences of Childhood VI Social Emotional Physical Educational
Visual Impairment & Eye Health in Children Susan Cotter, OD, MS So CA College of Optometry Marshall B Ketchum University Fullerton, CA Consequences of Childhood VI Social Emotional Physical Educational
Common Abusive Skeletal Injuries
 Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults
 Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage
 July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
Abuse Or Not? Interactive Visual Clues in Child Abuse
 Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
THE VEGETATIVE STATE IN INFANCY AND CHILDHOOD
 THE VEGETATIVE STATE IN INFANCY AND CHILDHOOD Stephen Ashwal MD, Professor of Pediatrics and Neurology, Chief, Division of Child Neurology, Department of Pediatrics, Loma Linda University School of Medicine,
THE VEGETATIVE STATE IN INFANCY AND CHILDHOOD Stephen Ashwal MD, Professor of Pediatrics and Neurology, Chief, Division of Child Neurology, Department of Pediatrics, Loma Linda University School of Medicine,
OVERVIEW OF CHILD PHYSICAL ABUSE
 2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
The Viewing Study Guide for Physical Abuse Slides
 The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
Mild Traumatic Brain Injury
 Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
Mild Traumatic Brain Injury Concussions This presentation is for information purposes only, not for any commercial purpose, and may not be sold or redistributed. David Wesley, M.D. Outline Epidemiology
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains
 5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
Abusive HeadTrauma. Antonia Chiesa, MD a, *, Ann-Christine Duhaime, MD b
 Abusive HeadTrauma Antonia Chiesa, MD a, *, Ann-Christine Duhaime, MD b KEYWORDS Child abuse Abusive head trauma Pediatric traumatic brain injury Shaken baby syndrome Nonaccidental trauma Child physical
Abusive HeadTrauma Antonia Chiesa, MD a, *, Ann-Christine Duhaime, MD b KEYWORDS Child abuse Abusive head trauma Pediatric traumatic brain injury Shaken baby syndrome Nonaccidental trauma Child physical
Traumatic Brain Injury TBI Presented by Bill Masten
 1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
Head injuries are a common cause of death in
 Late Neurologic and Cognitive Sequelae of Inflicted Traumatic Brain Injury in Infancy Karen M. Barlow, MB, ChB, MRCPCH*; Elaine Thomson, BSc ; David Johnson, PhD ; and Robert A. Minns, MD, PhD, FRCPCH
Late Neurologic and Cognitive Sequelae of Inflicted Traumatic Brain Injury in Infancy Karen M. Barlow, MB, ChB, MRCPCH*; Elaine Thomson, BSc ; David Johnson, PhD ; and Robert A. Minns, MD, PhD, FRCPCH
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
102 Results RESULTS. Age Mean=S.D Range 42= years -84 years Number % <30 years years >50 years
 102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
102 Results RESULTS A total of 50 cases were studied 39 males and 11females.Their age ranged between 16 years and 84 years (mean 42years). T1 and T2WI were acquired for all cases in sagittal and axial
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Pediatric Head Trauma August 2016
 PEDIATRIC HEAD TRAUMA AUGUST 2016 Pediatric Head Trauma August 2016 EDUCATION COMMITTEE PEER EDUCATION Quick Review of Pathophysiology of TBI Nuggets of knowledge to keep in mind with TBI Intracranial
PEDIATRIC HEAD TRAUMA AUGUST 2016 Pediatric Head Trauma August 2016 EDUCATION COMMITTEE PEER EDUCATION Quick Review of Pathophysiology of TBI Nuggets of knowledge to keep in mind with TBI Intracranial
Causes of TBI vary with age
 Endocrinopathies after Traumatic Brain Injury Susan R. Rose, MD Professor Cincinnati Children s Hospital Medical Center University of Cincinnati Supported by Pfizer, Inc Investigator-Initiated Research
Endocrinopathies after Traumatic Brain Injury Susan R. Rose, MD Professor Cincinnati Children s Hospital Medical Center University of Cincinnati Supported by Pfizer, Inc Investigator-Initiated Research
Anton-Babinski syndrome as a rare complication of chronic bilateral subdural hematomas
 DOI: 10.2478/romneu-2018-0050 Article Anton-Babinski syndrome as a rare complication of chronic bilateral subdural hematomas D. Adam, D. Iftimie, Cristiana Moisescu, Gina Burduşa ROMANIA Romanian Neurosurgery
DOI: 10.2478/romneu-2018-0050 Article Anton-Babinski syndrome as a rare complication of chronic bilateral subdural hematomas D. Adam, D. Iftimie, Cristiana Moisescu, Gina Burduşa ROMANIA Romanian Neurosurgery
of Trauma Assembly 27 th Page 1
 Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Pediatric Traumatic Brain Injury. Seth Warschausky, PhD Department of Physical Medicine and Rehabilitation University of Michigan
 Pediatric Traumatic Brain Injury Seth Warschausky, PhD Department of Physical Medicine and Rehabilitation University of Michigan Modules Module 1: Overview Module 2: Cognitive and Academic Needs Module
Pediatric Traumatic Brain Injury Seth Warschausky, PhD Department of Physical Medicine and Rehabilitation University of Michigan Modules Module 1: Overview Module 2: Cognitive and Academic Needs Module
Role of ultrasound in congenital cataract: Our experience
 Role of ultrasound in congenital cataract: Our experience Ayat Aziz Al-Alwan (1) Hazim Kamil Haddad (1) Rana Ahmad Alkrimeen (1) Mohammad Jalal Alsa aideh (2) Mu taz Ghalib Halasah (1) (1) Jordanian Royal
Role of ultrasound in congenital cataract: Our experience Ayat Aziz Al-Alwan (1) Hazim Kamil Haddad (1) Rana Ahmad Alkrimeen (1) Mohammad Jalal Alsa aideh (2) Mu taz Ghalib Halasah (1) (1) Jordanian Royal
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
ORTHOPEDIC ASPECTS CHILD ABUSE. A summary of the physical, metaphysical, psychological, and sociological aspects of Non-
 ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
Neuropathology Of Head Trauma. Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center
 Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Mild TBI (Concussion) Not Just Less Severe But Different
 Mild TBI (Concussion) Not Just Less Severe But Different Disclosures Funded research: 1. NIH: RO1 Physiology of concussion 2016-2021, Co-PI, $2,000,000 2. American Medical Society of Sports Medicine: RCT
Mild TBI (Concussion) Not Just Less Severe But Different Disclosures Funded research: 1. NIH: RO1 Physiology of concussion 2016-2021, Co-PI, $2,000,000 2. American Medical Society of Sports Medicine: RCT
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES
 TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
TRAUMATIC CAROTID &VERTEBRAL ARTERY INJURIES ALBERTO MAUD, MD ASSOCIATE PROFESSOR TEXAS TECH UNIVERSITY HEALTH SCIENCES CENTER EL PASO PAUL L. FOSTER SCHOOL OF MEDICINE 18TH ANNUAL RIO GRANDE TRAUMA 2017
Pearls, Pitfalls and Advances in Neuro-Ophthalmology
 Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Pearls, Pitfalls and Advances in Neuro-Ophthalmology Nancy J. Newman, MD Emory University Atlanta, GA Consultant for Gensight Biologics, Santhera Data Safety Monitoring Board for Quark AION Study Medical-legal
Long-term outcome of abusive head trauma
 DOI 10.1007/s00247-014-3169-8 SPECIAL ISSUE: ABUSIVE HEAD TRAUMA Long-term outcome of abusive head trauma Mathilde P. Chevignard & Katia Lind Received: 23 January 2014 /Revised: 22 May 2014 /Accepted:
DOI 10.1007/s00247-014-3169-8 SPECIAL ISSUE: ABUSIVE HEAD TRAUMA Long-term outcome of abusive head trauma Mathilde P. Chevignard & Katia Lind Received: 23 January 2014 /Revised: 22 May 2014 /Accepted:
Functional Neuroanatomy and Traumatic Brain Injury The Frontal Lobes
 Functional Neuroanatomy and Traumatic Brain Injury The Frontal Lobes Jessica Matthes, Ph.D., ABN Barrow TBI Symposium March 23, 2019 jessica.matthes@dignityhealth.org Outline TBI Mechanisms of Injury Types
Functional Neuroanatomy and Traumatic Brain Injury The Frontal Lobes Jessica Matthes, Ph.D., ABN Barrow TBI Symposium March 23, 2019 jessica.matthes@dignityhealth.org Outline TBI Mechanisms of Injury Types
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
Introduction to Neurosurgical Subspecialties: Trauma and Critical Care Neurosurgery Brian L. Hoh, MD 1, Gregory J. Zipfel, MD 2 and Stacey Q. Wolfe, MD 3 1 University of Florida, 2 Washington University,
PA SYLLABUS. Syllabus for students of the FACULTY OF MEDICINE No.2
 Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
Approved At the meeting of the Faculty Council Medicine No. of Approved At the meeting of the chair of Neurosurgery No. of Dean of the Faculty Medicine No.2 PhD, associate professor M. Betiu Head of the
Can we abolish skull x-rays for head injury?
 ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Disclosure Statement. Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk.
 Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Nicolas Bianchi M.D. May 15th, 2012
 Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Nicolas Bianchi M.D. May 15th, 2012 New concepts in TIA Differential Diagnosis Stroke Syndromes To learn the new definitions and concepts on TIA as a condition of high risk for stroke. To recognize the
Traumatic brain injury (TBI) is a major cause of mortality, cognitive and
 Disorder: Traumatic Brain Injury (TBI) Essay Title: Paediatric Traumatic Brain Injury (TBI) Title: Associate Professor Name: Cathy Surname: Catroppa Qualifications: BBSc., DipEdPsych., M.Ed.Psych., PhD
Disorder: Traumatic Brain Injury (TBI) Essay Title: Paediatric Traumatic Brain Injury (TBI) Title: Associate Professor Name: Cathy Surname: Catroppa Qualifications: BBSc., DipEdPsych., M.Ed.Psych., PhD
GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA
 GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA Approximately 800 patients with head injuries die or are hospitalized in the state of Alaska each year 1. In addition, thousands
GUIDELINES FOR THE MANAGEMENT OF HEAD INJURIES IN REMOTE AND RURAL ALASKA Approximately 800 patients with head injuries die or are hospitalized in the state of Alaska each year 1. In addition, thousands
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Virtual Mentor American Medical Association Journal of Ethics August 2008, Volume 10, Number 8:
 Virtual Mentor American Medical Association Journal of Ethics August 2008, Volume 10, Number 8: 516-520. CLINICAL PEARL The Hazards of Stopping a Brain in Motion: Evaluation and Classification of Traumatic
Virtual Mentor American Medical Association Journal of Ethics August 2008, Volume 10, Number 8: 516-520. CLINICAL PEARL The Hazards of Stopping a Brain in Motion: Evaluation and Classification of Traumatic
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Case SCIWORA in patient with congenital block vertebra
 Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Case 15428 SCIWORA in patient with congenital block vertebra Lucas Walgrave 1, Charlotte Vanhoenacker 1-2, Thomas Golinvaux 3, Filip Vanhoenacker3-5 1: Leuven University Hospital, Department of Radiology,
Fundus findings in spontaneous subarachnoid hemorrhage and their correlation with neurologic characteristics
 European Journal of Ophthalmology / Vol. 19 no. 3, 2009 / pp. 460-465 Fundus findings in spontaneous subarachnoid hemorrhage and their correlation with neurologic characteristics MORTEZA ENTEZARI 1, SHIRZAD
European Journal of Ophthalmology / Vol. 19 no. 3, 2009 / pp. 460-465 Fundus findings in spontaneous subarachnoid hemorrhage and their correlation with neurologic characteristics MORTEZA ENTEZARI 1, SHIRZAD
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
ABUSIVE HEAD TRAUMA (AHT) IS
 ORIGINAL CONTRIBUTION Analysis of Missed Cases of Abusive Head Trauma Carole Jenny, MD, MBA Lt Col Kent P. Hymel, MD, USAF, MC Alene Ritzen, MD, JD Steven E. Reinert, MS Thomas C. Hay, DO ABUSIVE HEAD
ORIGINAL CONTRIBUTION Analysis of Missed Cases of Abusive Head Trauma Carole Jenny, MD, MBA Lt Col Kent P. Hymel, MD, USAF, MC Alene Ritzen, MD, JD Steven E. Reinert, MS Thomas C. Hay, DO ABUSIVE HEAD
What neuroimaging should be performed in children in whom inflicted brain injury (ibi) is suspected? A systematic review
 Clinical Radiology (2009) 64, 473e483 What neuroimaging should be performed in children in whom inflicted brain injury (ibi) is suspected? A systematic review A.M. Kemp a, S. Rajaram b, M. Mann c, V. Tempest
Clinical Radiology (2009) 64, 473e483 What neuroimaging should be performed in children in whom inflicted brain injury (ibi) is suspected? A systematic review A.M. Kemp a, S. Rajaram b, M. Mann c, V. Tempest
The Evaluation of Suspected Child Physical Abuse
 CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care The Evaluation of Suspected Child Physical Abuse Cindy W. Christian, MD, FAAP, COMMITTEE ON CHILD ABUSE AND NEGLECT Child physical
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care The Evaluation of Suspected Child Physical Abuse Cindy W. Christian, MD, FAAP, COMMITTEE ON CHILD ABUSE AND NEGLECT Child physical
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Brain and Central Nervous System Cancers
 Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Brain and Central Nervous System Cancers NICE guidance link: https://www.nice.org.uk/guidance/ta121 Clinical presentation of brain tumours History and Examination Consider immediate referral Management
Cognitive Rehabilitation with Current Research and Transition of Care
 Cognitive Rehabilitation with Current Research and Transition of Care Mike Dichiaro, MD Pediatric Rehabilitation Medicine Carin Rowan, MPT Pediatric Physical Therapy Financial Disclosures No relevant financial
Cognitive Rehabilitation with Current Research and Transition of Care Mike Dichiaro, MD Pediatric Rehabilitation Medicine Carin Rowan, MPT Pediatric Physical Therapy Financial Disclosures No relevant financial
O ne million patients are treated annually in United
 859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Recurrent Subdural Hematomas in Benign Macrocrania of Infancy
 Case Report imedpub Journals http://www.imedpub.com Medical & Clinical DOI: 10.21767/2471-299X.100032 Recurrent Subdural Hematomas in Benign Macrocrania of Infancy Ademar Lucas Junior São Camilo Diagnostic
Case Report imedpub Journals http://www.imedpub.com Medical & Clinical DOI: 10.21767/2471-299X.100032 Recurrent Subdural Hematomas in Benign Macrocrania of Infancy Ademar Lucas Junior São Camilo Diagnostic
 Revisited imaging findings and pathophysiology of abusive head trauma with emphasis on diffusionweighted imaging (eede-219) I. Elhelf *, R. Oral, T. Sato, A. Capizzano, Y. Sato, M. Amarneh, T. Sasaki,
Revisited imaging findings and pathophysiology of abusive head trauma with emphasis on diffusionweighted imaging (eede-219) I. Elhelf *, R. Oral, T. Sato, A. Capizzano, Y. Sato, M. Amarneh, T. Sasaki,
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Author Manuscript. Received Date : 27-Oct Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 Received Date : 27-Oct-2016 Revised Date : 09-Jan-2017 Accepted Date : 31-Jan-2017 Article type ABSTRACT : Original Contribution
Head Injury כל הזכויות שמורות למד"א מרחב ירושלים. Dan Drory, EMT-P, Instructor
 Head Injury Dan Drory, EMT-P, Instructor Anatomy on a fingertip The brain is a soft and gentle tissue. The brain is the most important organ. כל הזכויות שמורות למד"א מרחב ירושלים Protective layers of the
Head Injury Dan Drory, EMT-P, Instructor Anatomy on a fingertip The brain is a soft and gentle tissue. The brain is the most important organ. כל הזכויות שמורות למד"א מרחב ירושלים Protective layers of the
a. Ischemic stroke An acute focal infarction of the brain or retina (and does not include anterior ischemic optic neuropathy (AION)).
 12.0 Outcomes 12.1 Definitions 12.1.1 Neurologic Outcome Events a. Ischemic stroke An acute focal infarction of the brain or retina (and does not include anterior ischemic optic neuropathy (AION)). Criteria:
12.0 Outcomes 12.1 Definitions 12.1.1 Neurologic Outcome Events a. Ischemic stroke An acute focal infarction of the brain or retina (and does not include anterior ischemic optic neuropathy (AION)). Criteria:
Outcomes of Infants with Neonatal Abstinence Syndrome
 Outcomes of Infants with Neonatal Abstinence Syndrome Caroline O. Chua, MD, FAAP Medical Director, Division of Neonatology Director, Neonatal Follow Up Clinic Nemours Children s Hospital Orlando, Florida
Outcomes of Infants with Neonatal Abstinence Syndrome Caroline O. Chua, MD, FAAP Medical Director, Division of Neonatology Director, Neonatal Follow Up Clinic Nemours Children s Hospital Orlando, Florida
Intracranial Injury with Severe Shaking Trauma:
 Peer Reviewed Received 3 January2016 Received in revised form 22 March 2016 Accepted 2 April 2016 Available online 12 April 2016 Intracranial Injury with Severe Shaking Trauma: Spinal Subarachnoid Hemorrhage
Peer Reviewed Received 3 January2016 Received in revised form 22 March 2016 Accepted 2 April 2016 Available online 12 April 2016 Intracranial Injury with Severe Shaking Trauma: Spinal Subarachnoid Hemorrhage
The determination of eligible population for this measure requires administrative claims data.
 Overuse of Imaging Measure 6: Ratio of Magnetic Resonance Imaging Scans to Computed Tomography Scans for the Evaluation of Children with Atraumatic Headache Description This measure assesses the ratio
Overuse of Imaging Measure 6: Ratio of Magnetic Resonance Imaging Scans to Computed Tomography Scans for the Evaluation of Children with Atraumatic Headache Description This measure assesses the ratio
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast
 The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
Recognising and Managing Child Abuse in General Practice. Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital
 Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
