S ubdural haemorrhage (SDH) in infants and young
|
|
|
- Emery Bailey
- 5 years ago
- Views:
Transcription
1 947 ORIGINAL ARTICLE Neuroradiological aspects of subdural haemorrhages S Datta, N Stoodley, S Jayawant, S Renowden, A Kemp... See end of article for authors affiliations... Correspondence to: Dr S Datta, Specialist Registrar in Radiology, Department of Radiology, University Hospital of Wales, Heath Park, Cardiff CF14 4XW, UK; shalinidatta@btinternet. com Accepted 15 June Arch Dis Child 2005;90: doi: /adc Aims: To review the neuroimaging of a series of infants and young children admitted to hospital with subdural haemorrhage (SDH). Methods: Neuroradiological investigations of 74 children under 2 years of age, from South Wales and southwest England, in whom an SDH or subdural effusion had been diagnosed between 1992 and 2001, were reviewed. Two paediatric neuroradiologists blinded to the original radiological report reviewed all the relevant images. Results: Neuroradiological review of images identified radiological features which were highly suggestive of non-accidental head injury (NAHI). Interhemispheric haemorrhages and SDHs in multiple sites or of different densities were almost exclusively seen in NAHI. MRI was more sensitive in identifying SDHs of different signal characteristics, posterior and middle cranial fossa bleeds, and parenchymal changes in the brain. CT scans, if performed with suboptimal protocols, were likely to miss small subdural bleeds. Conclusions: Guidelines for neuroimaging in suspected NAHI are recommended. A radiologist with experience in NAHI should report or review these scans. The initial investigation should be CT, but MRI will also be necessary in most cases. Head CT should be an integral part of the skeletal survey in all infants less than 6 months of age referred for child protection investigation, and in children less than 2 years where child abuse is suspected and there are neurological signs, retinal haemorrhages, or s. S ubdural haemorrhage (SDH) in infants and young children has an incidence of per in children less than 1 year, 1 3 and most cases are due to physical abuse. Other causes include accidental trauma, meningitis, coagulopathy, vascular malformations, and rare metabolic disorders. These infants present with varied and usually non-specific symptoms. Initial neuroimaging may be undertaken by radiologists without particular expertise in paediatric neuroimaging, but the initial investigations are critical to the crucial decisions which are made within the child protection and legal process. It is therefore essential that the methods of investigation and interpretation are standardised and well understood. The Royal College of Radiologists, 4 the American Academy of Pediatrics, 5 6 and recently Jaspan and colleagues 7 have suggested guidance in the neuroimaging of NAHI. The diagnosis of SDH is made by cranial imaging, mainly computed tomography (CT) and magnetic resonance imaging (MRI); the features of SDH due to non-accidental head injury (NAHI) are well described MRI is used as an adjunct to CT in the radiological assessment of SDH to detect subdural blood in areas not well seen on CT, or small volume SDHs, to differentiate subdural and subarachnoid blood and to show parenchymal injuries. Our study aims to review the neuroimaging of a series of infants and young children admitted to hospital with SDH, and highlight features typical of NAHI. We make recommendations for neuroimaging in suspected cases of abuse in young children based on these findings. SUBJECTS AND METHODS We undertook a retrospective analysis of 74 patients under the age of 2 years with SDH or subdural effusion diagnosed between 1992 and The following selection criteria were used to identify NAHI: N Confession by the perpetrator N A criminal conviction for child abuse where there was supportive evidence from unexplained extracranial injuries N SDH and associated findings, where NAHI was concluded at case conference. Cases from South Wales and southwest England were identified using the Welsh Paediatric Surveillance System, ICD patient coding, radiology databases, admission data, ascertainment from clinicians, pathologists, HM coroners, and expert witnesses in child protection cases. Case notes were obtained and reviewed. Note was made of clinical features and type and timing of the imaging study. Two paediatric neuroradiologists blinded to the initial report reviewed all the images. Location of bleeding was recorded as convexity, interhemispheric, posterior fossa, middle cranial fossa, or subarachnoid space. Brain parenchymal changes were recorded as contusions, haematomas, infarcts, focal atrophy, diffuse axonal injury (DAI), focal or generalised swelling, and oedema. MREC approval was granted. RESULTS Neuroradiological review was completed in all 74 cases. Forty nine cases were identified as NAHI, classified as follows: N Confession by the perpetrator (n = 12) N Criminal conviction (n = 8) N NAHI agreed at case conference (n = 29). NAHI was suspected in a further 11 cases, but the cases did not fulfil the study child abuse inclusion categories; these cases were excluded from the detailed radiological analysis. Three cases followed serious, independently witnessed accidents. Abbreviations: CT, computed tomography; DAI, diffuse axonal injury; MRI, magnetic resonance imaging; NAHI, non-accidental head injury; SDH, subdural haemorrhage
2 948 Datta, Stoodley, Jayawant, et al Eleven SDH resulted from miscellaneous causes: N 7 meningitis N 2 postoperative rebleeds N 1 haemorrhagic disease of the newborn N 1 benign effusion which resolved on follow up. Seventy nine per cent of NAHI cases (39/49) were less than 6 months old. Presenting symptoms varied from drowsiness and malaise to fitting and coma. One child died soon after arrival. Forty seven patients had one or more extracranial injuries such as retinal haemorrhages, bruising, or s. Retinal haemorrhages were common; bilateral in 25 and unilateral in 10 cases. Bruising was present in 26 children, 20 cases involving the scalp or face. Two patients had no extracranial injuries; both were under 6 months of age. Twelve infants had increased head circumference on admission. Results of lumbar puncture were documented in 19 patients. In all cases the cerebrospinal fluid was haemorrhagic. Fractures were seen in 29/49 cases. Rib s were commonest (14 patients), with limb s in 11 and multiple s in 21 patients. Skull s were found in 11 patients; 4 had more than one. Evidence of impact to the head was seen in 16 cases (11 skull s with or without scalp swelling and 5 with swelling alone) (table 1). In 15 of 16 children with evidence of impact, SDHs were present in multiple sites, both at and away from the impact site. Vertebral s were seen in one child. In 73/74 patients CT was the first neuroimaging investigation; one had an MRI scan. Twenty five patients had MRI scans 1 12 days later. The initial CT scan was performed at a district hospital in 90% of cases. In 10 patients only 10 mm slices were obtained through the whole brain (eight of these children were scanned between the years 1992 and 1995), and in one patient only a post-contrast study was performed. In 7/49 children with NAHI the original CT was reported as normal or not suggestive of NAHI. The diagnosis of NAHI was subsequently made following neuroradiological review prompted by high clinical suspicion of abuse. Table 1 Details of injury in cases with definite evidence of impact Evidence of impact Skull s Bruising Subdural site In seven cases, subdural collections followed meningitis (all Streptococcus pneumoniae). In six cases these were detected within 2 5 days of symptom onset, but in one case they were detected three weeks later. Two of these children had unilateral, and five bilateral collections. Subdural taps occurred in five of these seven cases, and in four of these the fluid was haemorrhagic. The initial lumbar puncture was also haemorrhagic in six of these seven cases. Bleeding followed a subdural tap in only one case. All post-meningitis subdurals were convexity collections. Neuroradiological findings are summarised in table 2. CT and MRI were performed in 25 children, and additional SDHs were identified on MRI in 19 cases: N 7 convexity N 3 interhemispheric N 5 posterior fossa N 4 middle fossa bleeds. Subdural collections of different appearances (density or intensity) were seen in 26 children with NAHI, and in six this feature was seen only on the MRI scan. Ultrasound was performed before CT in 12 cases; SDHs were not seen in seven of these. Subdural collections were seen in more than two sites in 32/49 in the NAHI group; in 26/49 the SDHs had components of different CT densities suggestive of bleeds of different ages. In the miscellaneous group multifocal subdural collections were only seen in the infant with coagulopathy and the two children involved in road traffic accidents (one of whom had retinal haemorrhages). The child who fell 7.5 ft down the stairs had an isolated SDH at the site of skull and no retinal haemorrhage. In all these four children, the SDHs were hyperdense on CT, consistent with acute blood. Radiological DAI was seen in one case of NAHI. Cerebral oedema (focal or generalised) was seen in 12/49 cases. Generalised oedema associated with SDH was seen only in the NAHI group. No contusional tears were seen on CT or MRI, although in seven cases there were focal parenchymal Case 1 Right parietal, left occipital Bruising on opposite side of Multiple SDHs of different densities, below and away from Case 2 2 separate parieto-occipital Bruises to face Multiple SDHs of different densities, below and away from Case 3 Left parietal No bruising Multiple SDHs of different densities, below and away from Case 4 Right parietal Swelling at site of SDH underlying Case 5 Occipital No bruising Multiple SDHs of different densities, away from Case 6 Right parietal, left parietal Swelling at site of Multiple SDHs, below and away from Case 7 Right parietal Swelling at site of Multiple SDHs of different densities, below and away from Case 8 Left parietal linear, old occipital Overlying cephalohaematoma Multiple SDHs, below and away from Case 9 Left sided parietal Soft tissue swelling away from site Multiple SDHs, below and away from of Case 10 Posterior parietal Bruises on neck Multiple SDHs of different densities, below and away from Case 11 Left posterior parietal Bruising on face, upper and lower arm, Multiple SDHs, below and away from torn frenulum, old scar on forehead Case 12 None Bruise right side of forehead Multiple SDHs, below and away from bruise Case 13 None Bruise right side of forehead Multiple SDHs, below and away from bruise Case 14 None Bruised forehead Multiple SDHs of different densities, below and away from bruise Case 15 None Right occipital bruise Multiple SDHs of different densities, below and away from bruise Case 16 None Left parietal bruise Multiple SDHs, below and away from bruise
3 Neuroradiological aspects of subdural haemorrhages 949 Table 2 Imaging features in various groups changes such as contusions, atrophy, and infarcts. Only two of these had signs suggestive of recent impact. Definite evidence of previous abuse was present in 20 cases of NAHI (table 3). All three children involved in accidental trauma sustained a skull with SDH seen at the site. In one case (involved in road traffic accident) acute subdural blood was also seen distant from the site. DISCUSSION Imaging features in NAHI are well documented and recommendations have been made regarding imaging in NAHI. CT should be the first imaging investigation (due to its availability, the relative ease with which sick infants can be scanned, and its ability to detect acute blood). MRI should be performed as a second line investigation within the first few days following injury and for follow up Advanced MR techniques such as MR spectroscopy may give useful prognostic information at relatively early stages following the injury, 15 and MRI diffusion weighted imaging shows patterns of abnormality consistent with hypoxic-ischaemic changes following NAHI, a finding which also has prognostic significance Previous studies have shown improved detection of SDH with MRI compared to CT, 14 although subarachnoid Table 3 Case Case 1 Case 2 Case 3 Case 4 Case 5 Case 6 Case 7 Case 8 Case 9 Case 10 Case 11 Case 12 Case 13 Case 14 Case 15 Case 16 Case 17 Case 18 Case 19 Case 20 NAHI Accidental trauma Miscellaneous (n = 49) (n = 3) (n = 11) Age (0 6 mth) Age (6 24 mth) Convexity collection 44 (7/25) 2 11 Interhemispheric fissure bleeds 38 (3/25) 2 1 PCF bleeds 14 (5/25) 2 1 MCF bleeds 9 (4/25) 2 Focal oedema Generalised oedema 3 Parenchymal changes 12 (5/25) 3 Subarachnoid haemorrhage 7 2 Skull 11 (SDH away 3 (SDH away from # site in 10) from # site in 1) DAI 1 SDH of apparently different ages 26 (6/25) SDH in multiple sites Figures in parentheses represent the number of children where the imaging feature was shown only on MRI but not on CT scan. haemorrhage may be better detected by CT scans than MRI. 19 Other MRI studies have also shown SDH at sites poorly seen on CT. 12 Our study confirms these findings: some SDHs of low CT density, middle and posterior cranial fossa bleeds, and parenchymal changes were detected only on MRI scanning in several cases. DAI was found in only one case, consistent with neuropathological evidence suggesting that DAI is less common following NAHI than previously thought. 20 CT may underestimate DAI, which is better seen on MRI, but this was only available in half of the NAHI cases. In the neuropathological study of fatal NAHI by Geddes et al, brain weight was increased in 82% of cases, 21 suggesting cerebral oedema. Our series highlights the association of generalised or focal oedema in NAHI. Although CT is less sensitive in detecting cerebral oedema or ischaemia, particularly when performed early, diffusion weighted MRI is exquisitely sensitive at showing these changes very early after injury, and should be considered as a part of the MRI protocol in NAHI where available. The finding of SDH in different sites or of apparently different ages or of generalised oedema in association with SDH is strongly suggestive of NAHI. The commonest site for SDH in our study was over the cerebral convexities with isolated convexity collections being the least discriminatory Evidence to support there having been repeated episodes of abuse in cases with SDHs of different ages Evidence Multiple bruises, some noted few weeks before admission, torn frenulum, old rib Old rib Previous admission with subconjunctival haemorrhage and sudden onset squint, retinal haemorrhages Multiple bruises, cigarette burns, adult bite marks, NAI queried on previous admission, retinal haemorrhages Multiple bruises on scalp and chest, retinal haemorrhages, seen by GP 3 times in 2 weeks prior to admission Presented with bruises two weeks previously, retinal haemorrhages Two week history of being unwell, shaking admitted, retinal haemorrhages Multiple bruises, cigarette burns, retinal haemorrhages, witnessed episodes of repeated abuse Multiple bruises, retinal haemorrhages, increasing OFC noted on previous admission Old s, retinal haemorrhages Bruising around chest, failure to thrive, retinal haemorrhages, father admitted shaking Seen previously with episodes of apnoea and painful leg Repeated admissions with vomiting and increasing OFC Previous admission with rib s, retinal haemorrhages Old rib s Multiple bruises, bruised frenulum, retinal haemorrhages Old rib s, retinal haemorrhages Multiple bruises, concern regarding increasing OFC on previous admission Two previous admissions with fits 1 week apart, scratches on face Admitted previously with bruising, retinal haemorrhages NAI, non-accidental injury; OFC, occipitofrontal circumference.
4 950 Datta, Stoodley, Jayawant, et al What is already known on this topic N SDH in infants raises the possibility of NAHI N NAHI may be missed if not thoroughly investigated feature. The interhemispheric fissure was the next commonest site, followed by the posterior and middle cranial fossa. This is similar to the findings of Sato and colleagues, 14 but differs from the observations of Barlow and colleagues, 13 who cite the subtemporal region as the commonest site of SDH in NAHI. Interhemispheric blood was most often seen following NAHI; indeed, apart from NAHI, SDH in the interhemispheric fissures, and posterior and middle cranial fossa was only otherwise seen following severe accidental trauma (cases of road traffic accident) and coagulopathy. Most children with NAHI were 6 months old or less, and most had extracranial injuries and retinal haemorrhages. However, two of this group had SDH with no extracranial injuries. These two infants presented with neurological symptoms and were imaged on the basis of a discrepancy between history and clinical presentation. Sato and colleagues 14 and Morris and colleagues 22 have also cited cases where SDHs were the only objective finding of abuse. SDHs of apparently different ages were found in 26 patients with NAHI. Legal questions often arise regarding the possibility of rebleeding into pre-existing SDH in these cases. In 20/26 cases there was extracranial evidence of previous abuse, supporting the interpretation that the SDHs were due to different episodes of NAHI. These children presented with either signs of raised intracranial pressure or encephalopathy on a background of having generally being unwell. It is accepted that rebleeding can occur following minimal trauma in the elderly population. The pattern of the more acute bleeding in cases of NAHI is different to that seen in adult rebleeds, being usually multifocal rather than unifocal, of small volumes, and in a distribution typical of that seen in the primary NAHI. Therefore, this pattern of bleeding in the presence of subdural haematomas of apparently different ages is more likely to be due to further episodes of abuse rather than to spontaneous, synchronous multifocal rebleeds. Also the volumes of blood associated with these possible rebleeds is rarely of such a volume as to cause either a significant acute rise in intracranial pressure or to be the direct cause of an acute encephalopathic illness. We did not come across any cases where further SDH arose spontaneously in post-meningitic effusions. Rebleeding occurred only in one patient after surgical evacuation. Any young child with neurological symptoms, retinal haemorrhages of unknown origin, or any other features of non-accidental injury should have a head CT scan. Based on our study findings and the high incidence of SDHs in children less than 6 months, we would recommend that a head CT scan should be part of the skeletal survey in children under 6 months of age where physical abuse is suspected. This condition presents with a variety of clinical signs and symptoms and carries a serious morbidity. 1 We believe that if a clinician has sufficient clinical concern to request a skeletal survey, then a CT head scan should be performed to look for intracranial injury. Suboptimal CT protocols were used at a few hospitals. Slices of only 10 mm throughout the whole head, or postcontrast only studies are more likely to miss small SDHs, especially those in the posterior fossa. MRI performed in the acute stage as the first neuroimaging investigation may miss small volume acute SDH and subarachnoid haemorrhages. What this study adds N Neuroimaging features highly suggestive of NAHI N Clear guidelines for investigation in suspected NAHI Ultrasound has no role in excluding an SDH, even in experienced hands, but may be used to monitor resolution of SDH diagnosed on CT/MRI and in looking for subtle shearing lesions at grey-white interface. The introduction of a more uniform protocol in the investigation of these cases would be of great value, and we endorse the proposals of Jaspan and colleagues 7 who rightly emphasise the importance of early MRI in these cases. Optimal neuroimaging is important from the point of view of child protection, and the results have implications for the child s long term neurodevelopmental outcome. The interpretation of these scans is also of great importance, and we recommend that these cases should be reported or reviewed by a radiologist experienced in paediatric neuroimaging. When is neuroimaging indicated? N We recommend that it should be performed to guidelines in all young children with unexplained neurological symptoms, retinal haemorrhage, or non-accidental s, or if blood stained CSF is found on lumbar puncture in encephalopathic infants. N We recommend that it should be performed to guidelines in all children under 6 months of age where sufficient grounds exist for considering the possibility of child abuse. N A CT scan should be strongly considered as part of the skeletal survey when it forms part of the investigation of any child who is being investigated for physical abuse. Conclusions N MRI adds further information to CT findings in neuroimaging children with suspected NAHI and should be performed in all cases. N Adherence to published imaging guidelines will improve quality of diagnosis. N Interhemispheric haemorrhages, and SDHs in multiple sites or of different densities suggest NAHI. In association with history, clinical presentation, and other investigations, these findings confirm the probability that the infant has suffered serious physical abuse N Neuroimaging should be performed in all infants under 6 months of age where the possibility of physical abuse is being investigated radiologically. N Imaging studies should be reported or reviewed by radiologists with experience in paediatric neuroimaging.... Authors affiliations S Datta, A Kemp, Dept of Neuroradiology and Child Health, University Hospital of Wales, Cardiff, UK N Stoodley, S Renowden, Dept of Neuroradiology, Frenchay Hospital, Bristol, UK S Jayawant, Dept of Paediatrics, John Radcliffe Hospital, Oxford, UK Competing interests: none declared REFERENCES 1 Kemp AM, Stoodley N, Cobley C, et al. Apnoea and brain swelling in nonaccidental head injury. Arch Dis Child 2003;88: Barlow KM, Minns RA. Annual incidence of shaken impact syndrome in young children. Lancet 2000;356:
5 Neuroradiological aspects of subdural haemorrhages Jayawant S, Rawlinson A, Gibbon F, et al. Subdural haemorrhages in infants: population based study. BMJ 1998;317: The Royal College of Radiologists. Making the best use of a department of clinical radiology: guidelines for doctors, 5th edn. London: Royal College of Radiologists, American Academy of Pediatrics Committee on Child Abuse and Neglect. Shaken baby syndrome: inflicted cerebral trauma. Pediatrics 1993;92: American Academy of Pediatrics. Diagnostic imaging of child abuse. Pediatrics 2000;105: Jaspan T, Griffiths PD, McConachie NS, et al. Neuroimaging for nonaccidental head injury in childhood: a proposed protocol. Clin Radiol 2003;58: Cohen RA, Kaufman RA, Myers PA, et al. Cranial computed tomography in the abused child with head injury. Am J Roentgenol 1986;146: Zimmerman RA, Bilaniuk LT, Bruce D, et al. Computed tomography of craniocerebral injury in the abused child. Radiology 1979;130: Ewing-Cobbs L, Prasad M, Kramer L, et al. Acute neuroradiologic findings in young children with inflicted or noninflicted traumatic brain injury. Childs Nerv Syst 2000;16: Rao P, Carty H, Pierce A. The acute reversal sign: comparison of medical and non-accidental injury patients. Clin Radiol 1999;54: Alexander RC, Schor DP, Smith WL Jr. Magnetic resonance imaging of intracrahial injuries from child abuse. J Pediatr 1986;109: Barlow KM, Gibson RJ, McPhillips M, et al. Magnetic resonance imaging in acute non-accidental head injury. Acta Paediatr 1999;88: Sato Y, Yuh WT, Smith WL, et al. Head injury in child abuse: evaluation with MR imaging. Radiology 1989;173: Haseler LJ, Arcinue E, Danielsen ER, et al. Evidence from proton magnetic resonance spectroscopy for a metabolic cascade of neuronal damage in shaken baby syndrome. Pediatrics 1997;99: Biousse V, Suh DY, Newman NJ, et al. Diffusion-weighted magnetic resonance imaging in shaken baby syndrome. Am J Ophthalmol 2002;133: Suh DY, Davies PC, Hopkins KL, et al. Nonaccidental pediatric head injury: diffusion-weighted imaging findings. Neurosurgery 2001;49: Johnson DL, Boal D, Baule R. Role of apnea in nonaccidental head injury. Pediatr Neurosurg 1995;23: Atlas SW. MR imaging is highly sensitive for acute subarachnoid haemorrhage not! Radiology 1993;186: Geddes JF, Vowels GH, Hackshaw AK, et al. Neuropathology of inflicted head injury in children. II. Microscopic brain injury in infants. Brain 2001;124: Geddes JF, Hackshaw AK, Vowels GH, et al. Neuropathology of inflicted head injury in children. 1. Patterns of brain damage. Brain 2001;124: Morris MW, Smith S, Cressman J, et al. Evaluation of infants with subdural hematoma who lack external evidence of abuse. Pediatrics 2000;105(3 pt 1): ARCHIVIST... Chronic non-bacterial osteomyelitis C hronic non-bacterial osteomyelitis (CNO) in children may present as single or multiple lesions and there may be a single episode or recurrent episodes. Chronic recurrent multifocal osteomyelitis (CRMO) is thought to be the childhood equivalent of the synovitis, acne, pustulosis, hyperostosis, and osteitis/osteomyelitis (SAPHO) syndrome that affects adults. Although there have been reports of bacterial growths from CRMO lesions (Staphylococcus aureus, Mycoplasma hominis, Propionibacterium acnes, Bartonela henselae, and Coxiella burnetti have all been reported) most microbiological studies, including PCR testing, have given negative results. Antibiotic treatment does not work but anti-inflammatory agents do (non-steroidal anti-inflammatory drugs are effective and steroids, interferon a, interferon c, biphosphonates, and tumour necrosis factor antagonists have been used). Little has been written about the long term course of the disease but a follow up study has recently been reported from Germany (H J Girschick and colleagues. Annals of Rheumatic Diseases 2005;64:279 85). They followed up 30 children (aged 2 17 years at symptom onset, mean 10.3 years; 21 girls) for at least 5 years (mean 5.6 years). The mean age at diagnosis was 11 years (range 2 21 years) and time from first symptoms to diagnosis 5 9 months. Nine children had a single lesion and no recurrence, three had a single lesion on more than one occasion, nine had multiple lesions with no recurrence, and nine had multiple recurrent lesions (CRMO). The most commonly affected bones were the clavicle and the calcaneum but altogether 59 different bones were affected. Only one patient had multiple lesions in any one bone. The clinical features were those of osteomyelitis. Twenty-four children had joint involvement; seven had cutaneous pustules. Laboratory test results (haemoglobin, leucocyte count, erythrocyte sedimentation rate (ESR), serum ferritin, serum IgG) were generally normal. Serum IgM was moderately raised in four multifocal cases and serum IgA in three. Tests for antinuclear antibody were negative. Twenty-five children had biopsies of bone lesions and all showed the histology of chronic osteomyelitis usually with reparative changes (marrow fibrosis, trabecular osteoid apposition, and periosteal hyperostosis). Patients with CRMO were more likely to have granulocyte infiltration and hyperostosis. Microbiological investigations were negative. Twenty-seven patients were treated with naproxen, which appeared to be effective in general. Children with a single episode needed less lengthy treatment than those with recurrent episodes (mean 13.4 months vs 25 months). One patient with non-relapsing multifocal disease and four with CRMO were treated with prednisone in addition to naproxen before achieving remission. Other treatments (sulfasalazine, biphosphate, hyperbaric oxygen, surgical decortication) were apparently ineffective. All lesions were quiescent 5 years after disease onset. Bone growth was not affected but one patient had difficulty eating because of unilateral mandibular hypertrophy. There appears to be a spectrum of CNO ranging from a single non-recurrent lesion to recurrent multifocal lesions (CRMO). The cause is not known but the prognosis is good.
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age. DRAFT REVIEW May 2008
 Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
ARTICLE. Intracranial Hemorrhage in Children Younger Than 3 Years
 Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
O ne million patients are treated annually in United
 859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
859 ORIGIAL ARTICLE Can we abolish skull x rays for head injury? M J Reed, J G Browning, A G Wilkinson, T Beattie... See end of article for authors affiliations... Correspondence to: Matthew J Reed, Accident
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Annotation. Outcomes of infants and children with inflicted traumatic brain injury
 Outcomes of infants and children with inflicted traumatic brain injury Kathi L Makaroff* MD, Research Instructor of Pediatrics; Frank W Putnam MD, Director, Mayerson Center for Safe and Healthy Children,
Outcomes of infants and children with inflicted traumatic brain injury Kathi L Makaroff* MD, Research Instructor of Pediatrics; Frank W Putnam MD, Director, Mayerson Center for Safe and Healthy Children,
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Subdural haematoma and effusion in children aged < 2 years
 Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain and Cervico-Medullary Injury : Patterns and Mechanisms
 Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Evaluation of Craniocerebral Trauma Using Computed Tomography
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 57-62 Evaluation of Craniocerebral Trauma Using Computed Tomography
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 13, Issue 9 Ver. IV (Sep. 2014), PP 57-62 Evaluation of Craniocerebral Trauma Using Computed Tomography
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review
 Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review M B Moss, MD; L Lanier, MD; R Slater; C L Sistrom, MD; R G Quisling, MD; I M Schmalfuss, MD; and D Rajderkar, MD Contact:
Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review M B Moss, MD; L Lanier, MD; R Slater; C L Sistrom, MD; R G Quisling, MD; I M Schmalfuss, MD; and D Rajderkar, MD Contact:
The significance of traumatic haematoma in the
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
What neuroimaging should be performed in children in whom inflicted brain injury (ibi) is suspected? A systematic review
 Clinical Radiology (2009) 64, 473e483 What neuroimaging should be performed in children in whom inflicted brain injury (ibi) is suspected? A systematic review A.M. Kemp a, S. Rajaram b, M. Mann c, V. Tempest
Clinical Radiology (2009) 64, 473e483 What neuroimaging should be performed in children in whom inflicted brain injury (ibi) is suspected? A systematic review A.M. Kemp a, S. Rajaram b, M. Mann c, V. Tempest
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Validity of Caregivers Reports on Head Trauma Due to Falls in Young Children Aged Less than 2 Years
 Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Can we abolish skull x-rays for head injury?
 ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
ADC Online First, published on April 25, 2005 as 10.1136/adc.2004.053603 Can we abolish skull x-rays for head injury? Matthew J Reed, Jen G Browning, A. Graham Wilkinson & Tom Beattie Corresponding author:
Suspected Physical Abuse Clinical Practice Guideline
 Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Dating the abusive head trauma episode and perpetrator statements: key points for imaging
 DOI 10.1007/s00247-014-3171-1 SPECIAL ISSUE: ABUSIVE HEAD TRAUMA Dating the abusive head trauma episode and perpetrator statements: key points for imaging Catherine Adamsbaum & Baptiste Morel & Béatrice
DOI 10.1007/s00247-014-3171-1 SPECIAL ISSUE: ABUSIVE HEAD TRAUMA Dating the abusive head trauma episode and perpetrator statements: key points for imaging Catherine Adamsbaum & Baptiste Morel & Béatrice
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Chronic non-bacterial Osteomyelitis/Osteitis (or CRMO)
 www.printo.it/pediatric-rheumatology/gb/intro Chronic non-bacterial Osteomyelitis/Osteitis (or CRMO) Version of 2016 1. WHAT IS CRMO 1.1 What is it? Chronic Recurrent Multifocal Osteomyelitis (CRMO) is
www.printo.it/pediatric-rheumatology/gb/intro Chronic non-bacterial Osteomyelitis/Osteitis (or CRMO) Version of 2016 1. WHAT IS CRMO 1.1 What is it? Chronic Recurrent Multifocal Osteomyelitis (CRMO) is
A bout million patients present to UK hospitals
 420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
420 ORIGINAL ARTICLE Application of the Canadian CT head rules in managing minor head injuries in a UK emergency department: implications for the implementation of the NICE guidelines H Y Sultan, A Boyle,
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Lumbar puncture. Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: ml Replenished: 4-6 h Routine LP (3-5 ml): <1h
 Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Lumbar puncture Lumbar puncture Invasive procedure: diagnostic or therapeutic. The subarachnoid space 4-13 ys: 65-150ml Replenished: 4-6 h Routine LP (3-5 ml):
Common Abusive Skeletal Injuries
 Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE
 THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
Evaluation of a Pediatric Patient
 September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines
 Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Neuropathology Of Head Trauma. Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center
 Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Neuropathology Of Head Trauma Mary E. Case, M.D. Professor of Pathology St. Louis University Health Sciences Center Nothing to disclose Disclosure Introduction 500,000 cases/year of serious head injury
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
S ubdural haemorrhage (SDH) arising from
 98 REVIEW Investigating subdural haemorrhage in infants A M Kemp... When an infant or young child presents with subdural haemorrhage, the diagnostic priority is to exclude physical child abuse. A team
98 REVIEW Investigating subdural haemorrhage in infants A M Kemp... When an infant or young child presents with subdural haemorrhage, the diagnostic priority is to exclude physical child abuse. A team
Chronic recurrent multifocal osteomyelitis (CRMO) advancing the diagnosis
 Roderick et al. Pediatric Rheumatology (2016) 14:47 DOI 10.1186/s12969-016-0109-1 SHORT REPORT Chronic recurrent multifocal osteomyelitis (CRMO) advancing the diagnosis M. R. Roderick 1,2*, R. Shah 2,
Roderick et al. Pediatric Rheumatology (2016) 14:47 DOI 10.1186/s12969-016-0109-1 SHORT REPORT Chronic recurrent multifocal osteomyelitis (CRMO) advancing the diagnosis M. R. Roderick 1,2*, R. Shah 2,
Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury
 Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
The clinical scenario in this patient has been well reviewed by expert witnesses.
 September 29, 2014 Michael J. Cronkright, Esq. Kronzek & Cronkight, PLLC 420 S. Waverly Road, Suite 100 Lansing, MI 48917 Re: Preliminary Report on Naomi Burns Dear Mr. Cronkright, I have reviewed all
September 29, 2014 Michael J. Cronkright, Esq. Kronzek & Cronkight, PLLC 420 S. Waverly Road, Suite 100 Lansing, MI 48917 Re: Preliminary Report on Naomi Burns Dear Mr. Cronkright, I have reviewed all
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
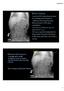 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
Head injuries in children. Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead
 Head injuries in children Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead Objectives Approach to minor head injury Child protection issues Concussion
Head injuries in children Dr Jason Hort Paediatrician Paediatric Emergency Physician, June 2017 Children s Hospital Westmead Objectives Approach to minor head injury Child protection issues Concussion
Brain Tumors. What is a brain tumor?
 Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
Scan for mobile link. Brain Tumors A brain tumor is a collection of abnormal cells that grows in or around the brain. It poses a risk to the healthy brain by either invading or destroying normal brain
5 Diagnosis. Timely diagnosis. Back to contents
 5 5 Diagnosis Back to contents Study Advisory Group questions: Are there delays in diagnosis? Is there variation in how the cerebral palsies are described? signs can fluctuate, to avoid over-diagnosis
5 5 Diagnosis Back to contents Study Advisory Group questions: Are there delays in diagnosis? Is there variation in how the cerebral palsies are described? signs can fluctuate, to avoid over-diagnosis
The Viewing Study Guide for Physical Abuse Slides
 The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
Case Report Nonbacterial Osteitis of the Clavicle: Longitudinal Imaging Series from Initial Diagnosis to Clinical Improvement
 Case Reports in Rheumatology Volume 2015, Article ID 182731, 4 pages http://dx.doi.org/10.1155/2015/182731 Case Report Nonbacterial Osteitis of the Clavicle: Longitudinal Imaging Series from Initial Diagnosis
Case Reports in Rheumatology Volume 2015, Article ID 182731, 4 pages http://dx.doi.org/10.1155/2015/182731 Case Report Nonbacterial Osteitis of the Clavicle: Longitudinal Imaging Series from Initial Diagnosis
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
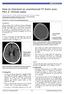 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
Recognising and Managing Child Abuse in General Practice. Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital
 Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
CORE STANDARDS STANDARDS USED IN TARN REPORTS
 CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
CORE STANDARDS Time to CT Scan BEST PRACTICE TARIFF SECTION 4.10 MAJOR TRAUMA 7 If the patient is admitted directly to the MTC or transferred as an emergency, the patient must be received by a trauma team
HEAD INJURY. Dept Neurosurgery
 HEAD INJURY Dept Neurosurgery INTRODUCTION PATHOPHYSIOLOGY CLINICAL CLASSIFICATION MANAGEMENT - INVESTIGATIONS - TREATMENT INTRODUCTION Most head injuries are due to an impact between the head and another
HEAD INJURY Dept Neurosurgery INTRODUCTION PATHOPHYSIOLOGY CLINICAL CLASSIFICATION MANAGEMENT - INVESTIGATIONS - TREATMENT INTRODUCTION Most head injuries are due to an impact between the head and another
Brain abscess rupturing into the lateral ventricle causing meningitis: a case report
 Brain abscess rupturing into the lateral ventricle causing meningitis: a case report Endry Martinez, and Judith Berger SBH Health System, 4422 Third Ave, Bronx, NY 10457 Key words: brain abscess, rupture
Brain abscess rupturing into the lateral ventricle causing meningitis: a case report Endry Martinez, and Judith Berger SBH Health System, 4422 Third Ave, Bronx, NY 10457 Key words: brain abscess, rupture
An Unusual Kind Of Traumatic Intracranial Hemorrhage: Post Traumatic Bleed Into The Schizencephalic Cleft
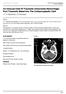 ISPUB.COM The Internet Journal of Radiology Volume 8 Number 2 An Unusual Kind Of Traumatic Intracranial Hemorrhage: Post Traumatic Bleed Into The Schizencephalic J T, V Rajendran, E Devarajan Citation
ISPUB.COM The Internet Journal of Radiology Volume 8 Number 2 An Unusual Kind Of Traumatic Intracranial Hemorrhage: Post Traumatic Bleed Into The Schizencephalic J T, V Rajendran, E Devarajan Citation
Fracture of the Temporal Bone: A Tomographic V/S Autopsy Study
 Fracture of the Temporal Bone: A Tomographic V/S Autopsy Study * Dr. Mukesh Kumar Goel, ** Dr. Rashmi Goel, *** Dr. Shiv R Kochar, **** Dr. M. R. Goel, *Asst Proff, Department of Forensic Medicine, People,s
Fracture of the Temporal Bone: A Tomographic V/S Autopsy Study * Dr. Mukesh Kumar Goel, ** Dr. Rashmi Goel, *** Dr. Shiv R Kochar, **** Dr. M. R. Goel, *Asst Proff, Department of Forensic Medicine, People,s
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study of Paediatric Head Injuries and Its Outcome Raje Vinayak, Raje Vaishali, Pednekar Akshay,
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article A Study of Paediatric Head Injuries and Its Outcome Raje Vinayak, Raje Vaishali, Pednekar Akshay,
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
Where is the contre-coup? Atypical localization of occipital brain contusion
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Where is the contre-coup? Atypical localization of occipital brain contusion A.I. Cucu, Claudia Florida Costea, R.A. Sascau, B. Dobrovat,
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Where is the contre-coup? Atypical localization of occipital brain contusion A.I. Cucu, Claudia Florida Costea, R.A. Sascau, B. Dobrovat,
ORIGINAL ARTICLE. Temporal Lobe Injury in Temporal Bone Fractures. imaging (MRI) to evaluate lesions of the temporal
 ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
ORIGINAL ARTICLE Temporal Lobe Injury in Temporal Bone Fractures Richard M. Jones, MD; Michael I. Rothman, MD; William C. Gray, MD; Gregg H. Zoarski, MD; Douglas E. Mattox, MD Objective: To determine the
Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults
 Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
Research Brief Clinical Report: Recognizing Subdural Hemorrhage in Older Adults Mark T. Pfefer, RN, MS, DC *1 ; Richard Strunk MS, DC 2 Address: 1 Professor and Director of Research, Cleveland Chiropractic
Injuries in Non Mobile Infants Protocol
 Injuries in Non Mobile Infants Protocol Contents 1. Introduction 2. Definition 3. Recommended Action 4. Specific considerations for disabled children 5. Accidental / non-accidental / inconclusive categories
Injuries in Non Mobile Infants Protocol Contents 1. Introduction 2. Definition 3. Recommended Action 4. Specific considerations for disabled children 5. Accidental / non-accidental / inconclusive categories
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation **
 PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes
 Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
 Revisited imaging findings and pathophysiology of abusive head trauma with emphasis on diffusionweighted imaging (eede-219) I. Elhelf *, R. Oral, T. Sato, A. Capizzano, Y. Sato, M. Amarneh, T. Sasaki,
Revisited imaging findings and pathophysiology of abusive head trauma with emphasis on diffusionweighted imaging (eede-219) I. Elhelf *, R. Oral, T. Sato, A. Capizzano, Y. Sato, M. Amarneh, T. Sasaki,
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Recurrent Subdural Hematomas in Benign Macrocrania of Infancy
 Case Report imedpub Journals http://www.imedpub.com Medical & Clinical DOI: 10.21767/2471-299X.100032 Recurrent Subdural Hematomas in Benign Macrocrania of Infancy Ademar Lucas Junior São Camilo Diagnostic
Case Report imedpub Journals http://www.imedpub.com Medical & Clinical DOI: 10.21767/2471-299X.100032 Recurrent Subdural Hematomas in Benign Macrocrania of Infancy Ademar Lucas Junior São Camilo Diagnostic
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
GUIDELINE FOR THE MANAGEMENT OF
 GUIDELINE FOR THE MANAGEMENT OF Reference: Febrile Convulsions Version No: 1 Applicable to All children admitted with Febrile Convulsion to the Children s Hospital for Wales Classification of document:
GUIDELINE FOR THE MANAGEMENT OF Reference: Febrile Convulsions Version No: 1 Applicable to All children admitted with Febrile Convulsion to the Children s Hospital for Wales Classification of document:
Imaging the Premature Brain- New Knowledge
 Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Imaging the Premature Brain- New Knowledge Stein Magnus Aukland Haukeland University Hospital University of Bergen NORWAY No disclosure Imaging modalities O Skull X-ray O Computer Tomography O Cerebral
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Update sulle lesioni emorragiche posttraumatiche
 Update sulle lesioni emorragiche posttraumatiche Corrado Iaccarino Neurochirurgia-Neurotraumatologia AOU Parma Neurochirurgia d'urgenza IRCCS ASMN Reggio Emilia LAW UPDATING This document provides recommendations
Update sulle lesioni emorragiche posttraumatiche Corrado Iaccarino Neurochirurgia-Neurotraumatologia AOU Parma Neurochirurgia d'urgenza IRCCS ASMN Reggio Emilia LAW UPDATING This document provides recommendations
Index. aneurysm, 92 carotid occlusion, 94 ICA stenosis, 95 intracranial, 92 MCA, 94
 A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
Traumatic Brain Injury TBI Presented by Bill Masten
 1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
Audit Report. National Audit of Paediatric Radiology Services in Hospitals
 Audit Report National Audit of Paediatric Radiology Services in Hospitals www.rcr.ac.uk 2 Contents Introduction 3 Standards 4 Material and methods 5 Results 6 Discussion 8 References 10 www.rcr.ac.uk 3
Audit Report National Audit of Paediatric Radiology Services in Hospitals www.rcr.ac.uk 2 Contents Introduction 3 Standards 4 Material and methods 5 Results 6 Discussion 8 References 10 www.rcr.ac.uk 3
Bilateral blunt carotid artery injury: A case report and review of the literature
 CASE REPORT Bilateral blunt carotid artery injury: A case report and review of the literature S Cheddie, 1 MMed (Surg), FCS (SA); B Pillay, 2 FCS (SA), Cert Vascular Surgery; R Goga, 2 FCS (SA) 1 Department
CASE REPORT Bilateral blunt carotid artery injury: A case report and review of the literature S Cheddie, 1 MMed (Surg), FCS (SA); B Pillay, 2 FCS (SA), Cert Vascular Surgery; R Goga, 2 FCS (SA) 1 Department
Bacillus anthracis meningitis during an outbreak of injectional anthrax in Scotland
 Bacillus anthracis meningitis during an outbreak of injectional anthrax in Scotland Dr Simon Dewar Microbiology Registrar and PhD Fellow University of Dundee SMA Free-paper session 31/10/15 Bacillis Anthraxis
Bacillus anthracis meningitis during an outbreak of injectional anthrax in Scotland Dr Simon Dewar Microbiology Registrar and PhD Fellow University of Dundee SMA Free-paper session 31/10/15 Bacillis Anthraxis
Complications of Spontaneous Intracranial Hypotension
 Complications of Spontaneous Intracranial Hypotension Poster No.: C-0890 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit K. Endo, Y. Kubo, M. Ida; Tokyo/JP Hemorrhage, Embolism / Thrombosis,
Complications of Spontaneous Intracranial Hypotension Poster No.: C-0890 Congress: ECR 2015 Type: Authors: Keywords: DOI: Scientific Exhibit K. Endo, Y. Kubo, M. Ida; Tokyo/JP Hemorrhage, Embolism / Thrombosis,
There are several types of epilepsy. Each of them have different causes, symptoms and treatment.
 1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
1 EPILEPSY Epilepsy is a group of neurological diseases where the nerve cell activity in the brain is disrupted, causing seizures of unusual sensations, behavior and sometimes loss of consciousness. Epileptic
Referral Criteria for Medical CT Radiation Exposures. Neuro Referrals
 Referral Criteria for Medical CT Radiation Exposures Neuro Referrals CHH & HRI The Ionising Radiation (Medical Exposure) Regulations 2017 Document Control Reference No: 3.2 First published: 2016 Version:
Referral Criteria for Medical CT Radiation Exposures Neuro Referrals CHH & HRI The Ionising Radiation (Medical Exposure) Regulations 2017 Document Control Reference No: 3.2 First published: 2016 Version:
CORE-INFO: fractures in children
 CORE-INFO: fractures in children This leaflet summarises what is currently known about the relationship between fractures and physical abuse and will be of particular interest to paediatricians, general
CORE-INFO: fractures in children This leaflet summarises what is currently known about the relationship between fractures and physical abuse and will be of particular interest to paediatricians, general
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
MR imaging as predictor of delayed posttraumatic cerebral hemorrhage
 J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
CLINICAL PRESENTATION AND RADIOLOGY QUIZ QUESTION
 Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Donald L. Renfrew, MD Radiology Associates of the Fox Valley, 333 N. Commercial Street, Suite 100, Neenah, WI 54956 3/12/2011 Radiology Quiz of the Week # 11 Page 1 CLINICAL PRESENTATION AND RADIOLOGY
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature
 Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Intraoperative contralateral extradural hematoma during evacuation of traumatic acute extradural hematoma: A case report with review of literature Anand Sharma 1, Arti Sharma 2, Yashbir Dewan 1 1 Artemis
Pott s Puffy Tumor. Shahad Almohanna 15/1/2018
 Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Pott s Puffy Tumor Shahad Almohanna R2 15/1/2018 Definition First described in 1760 by Sir Percival Pott. s he originally suggested that trauma of the frontal bone was causative for this lesion, but later,
Head injuries. Severity of head injuries
 Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
Head injuries ED Teaching day 23 rd October Severity of head injuries Minor GCS 14-15 Must not have any of the following: Amnesia 10min Neurological sign or symptom Skull fracture (clinically or radiologically)
The tale of global hypoxic ischaemic injury
 The tale of global hypoxic ischaemic injury Poster No.: C-0400 Congress: ECR 2016 Type: Educational Exhibit Authors: L. M. Zammit, R. Grech ; Paola/MT, Dublin 9/IE Keywords: CNS, CT, MR, Education, Computer
The tale of global hypoxic ischaemic injury Poster No.: C-0400 Congress: ECR 2016 Type: Educational Exhibit Authors: L. M. Zammit, R. Grech ; Paola/MT, Dublin 9/IE Keywords: CNS, CT, MR, Education, Computer
Spectrum of various patterns of injuries in cranio-cerebral trauma: CT evaluation
 Original article: Spectrum of various patterns of injuries in cranio-cerebral trauma: CT evaluation 1Dr. Kaleem Ahmad, 2 Dr. RK Rauniyar, 3 Dr. Sajid Ansari, 4 Dr. Mukesh Kumar Gupta 1Associate Professor,
Original article: Spectrum of various patterns of injuries in cranio-cerebral trauma: CT evaluation 1Dr. Kaleem Ahmad, 2 Dr. RK Rauniyar, 3 Dr. Sajid Ansari, 4 Dr. Mukesh Kumar Gupta 1Associate Professor,
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Only 30% to 40% of acute subdural hematoma (SDH)
 Contralateral Acute Epidural Hematoma After Decompressive Surgery of Acute Subdural Hematoma: Clinical Features and Outcome Thung-Ming Su, MD, Tsung-Han Lee, MD, Wu-Fu Chen, MD, Tao-Chen Lee, MD, and Ching-Hsiao
Contralateral Acute Epidural Hematoma After Decompressive Surgery of Acute Subdural Hematoma: Clinical Features and Outcome Thung-Ming Su, MD, Tsung-Han Lee, MD, Wu-Fu Chen, MD, Tao-Chen Lee, MD, and Ching-Hsiao
Guideline scope Subarachnoid haemorrhage caused by a ruptured aneurysm: diagnosis and management
 0 0 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Subarachnoid haemorrhage caused by a ruptured aneurysm: diagnosis and management The Department of Health and Social Care in England
0 0 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Subarachnoid haemorrhage caused by a ruptured aneurysm: diagnosis and management The Department of Health and Social Care in England
SKULL RADIOGRAPH IN HEAD INJURIES. Authors: ** Njeze, Ngozi R Umerah, B.C Mgbor, S.O
 SKULL RADIOGRAPH IN HEAD INJURIES Authors: ** Njeze, Ngozi R Umerah, B.C Mgbor, S.O **Address: Department of Radiation Medicine University of Nigeria Teaching Hospital, Enugu, Nigeria. E-mail: ngozinjeze
SKULL RADIOGRAPH IN HEAD INJURIES Authors: ** Njeze, Ngozi R Umerah, B.C Mgbor, S.O **Address: Department of Radiation Medicine University of Nigeria Teaching Hospital, Enugu, Nigeria. E-mail: ngozinjeze
PORT WINE STAINS AND STURGE-WEBER SYNDROME
 PORT WINE STAINS AND STURGE-WEBER SYNDROME Ong Hian Tat It is important for general practitioners to recognize cutaneous port-wine stains as these could signify important association with Sturge Weber
PORT WINE STAINS AND STURGE-WEBER SYNDROME Ong Hian Tat It is important for general practitioners to recognize cutaneous port-wine stains as these could signify important association with Sturge Weber
MUSCULOSKELETAL INFECTIONS IN CHILDREN. Dr Caren Landes Alder Hey Children s NHS Foundation Trust Liverpool
 MUSCULOSKELETAL INFECTIONS IN CHILDREN Dr Caren Landes Alder Hey Children s NHS Foundation Trust Liverpool MUSCULOSKELETAL INFECTIONS Common and uncommon infections Common and uncommon presentations Imaging
MUSCULOSKELETAL INFECTIONS IN CHILDREN Dr Caren Landes Alder Hey Children s NHS Foundation Trust Liverpool MUSCULOSKELETAL INFECTIONS Common and uncommon infections Common and uncommon presentations Imaging
Imaging of Acute Cerebral Trauma
 July, 2005 Imaging of Acute Cerebral Trauma Louis Rivera, Harvard Medical School, Year III 46 y/o Female s/p Trauma - Unrestrained? MVC requiring Med Flight - Facial bruising/swelling - DEEP COMA - SEIZURES
July, 2005 Imaging of Acute Cerebral Trauma Louis Rivera, Harvard Medical School, Year III 46 y/o Female s/p Trauma - Unrestrained? MVC requiring Med Flight - Facial bruising/swelling - DEEP COMA - SEIZURES
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council
 American Society of Neuroradiology What Is a Stroke? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair
American Society of Neuroradiology What Is a Stroke? From the Cerebrovascular Imaging and Intervention Committee of the American Heart Association Cardiovascular Council Randall T. Higashida, M.D., Chair
