BONE DISEASE FOR R2. By.. Rungnapa Laortanakul
|
|
|
- Dominick Reed
- 5 years ago
- Views:
Transcription
1 BONE DISEASE FOR R2 By.. Rungnapa Laortanakul
2 Bone Mineral Metabolism Hypercalcemia Hypocalcemia Vitamin D deficiency Basic Bone Biology Osteoporosis Osteomalacia
3 Vitamin D synthesis and metabolism Previtamin D3 vitamind3 via thermal isomerization UVB Skin Major source circulation
4 Parathyroid hormone Vitamin D
5
6 PTH action Hypocalcimia stimulate PTH secretion Bone bone resorption Ca,PO 4 Kidney Ca resorption PO 4 excretion Calcitriol Net effect is Ca PO 4
7 Calcitriol 1,25-dihydroxyvitamin D Small intestine resorption of Ca,PO 4 Bone bone resorption Kidney excretion of Ca,PO 4 Net effect is Ca PO 4
8 Hypercalcemia Clinical depend on time onset and level Normal level is mg/dl Calcium level mg/dl asymptomatic Calcium level >12 usually symptomatic
9 Clinical presentation Renal Nephrolithiasis/ Nephrocalcinosis Nephrogenic DI Polydipsia/ Polyuria Distal RTA Renal insufficiency Chronic hypercalcemic nephropathy nephrocalcinosis
10 GI Constipation, Anorexia, Abdominal pain, Pancreatitis, Increase gastrin secretion PU CNS Anxiety, Depression, Cognitive dysfunction, Confuse, Psychosis, Coma CVS Calcify valve, HT, Shortened QT interval Skeleton Gout, Pseudogout, Chondrocalcinosis, Osteoporosis, Osteopenia, Osteitis fibrosa cystica
11 Causes of hypercalcemia Parathyroid-dependent hypercalcemia 1 hyperparathyroidism 3 hyperparathyroidism Familial hypocalciuric hypercalcemia Lithium-associated Antagonist autoantibodies to the calcium-sensing receptor Williams texbook 11th ed.
12 Parathyroid-independent hypercalcemia Neoplasm -PTHrP dependent -Other humoral syndromes -Local osteolytic dz (including metastasis) PTHrP excess (non-neoplasia) Excess vit D action -Ingestion of excess vit D or vit D analogues -Topical vit D analogues -Granulomatous dz -Williams syndrome Thyrotoxicosis Adrenal insufficiency Renal failure -ARF -CRF with aplastic bone dz Immobilization Jansen s dz Drugs : vit A intoxication milk-alkali syndrome thiazide diuretics theophylline Williams texbook 11th ed.
13 Hyper Ca Ionized Ca High Clinical evaluation Hx,PE, e lyte,bun,cr,po 4,ALP Normal Hemoconcentration or Serum protein abnormality S&S malignancy Normal or high S.PTH Low Search for occult malignancy Chest radiograph Serum/urine IEP Mammogram Abdominal/chest CT PTH dependent PTH independent Evaluate for Other causes of PTH-independent Select appropriate tx, consider bisphosphonate
14 PTH dependent YES 24-hr urine calcium & Cr U ca < 100 mg/day or Cl ca /Cl cr < 0.01 NO PTH normal PTH high 1 hyperparathyroidism Li therapy Age<40 or Family hx YES NO BMD Review criteria Ca High Stop Li Ca normal Presumptive FHH; Consider family screening For surgery Li induce hyperpth
15 Work up Ca, PO 4 level Film find evidence of bone abnormality Find the solid organ tumor eg. CXR Alkaline phosphatase bone lysis Hyperchloric metabolic acidosis suggest hyperpth TFT hyperthyroidism Cortisol adrenal insufficiency Intact PTH level hyperparathyroidism PTH-rP, vit D Urine calcium
16 Primary hyperparathyroidism Present in one of four ways: 1. Asymptomatic hypercalcemia detected by routine biochemical screening 2. Symptomatic hypercalcemia 3. During evaluation for manifestations of hyperparathyroidism such as osteopenia, osteoporosis, or nephrolithiasis 4. Rarely, hyperparathyroid bone disease (osteitis fibrosa cystica) or parathyroid crisis
17 Primary hyperparathyroidism Adenoma Carcinoma Glandular hyperplasia MEN 1 MEN 2A Familial hyperparathyroidism
18 Multiple endocrine neoplasia Type 1 Primary hyperparathyroidism (>90 percent) Pituitary tumors (10 to 20 percent) Prolactinoma Growth hormone-secreting Corticotropin-secreting Non-hormone-secreting Enteropancreatic tumors (60 to 70 percent) Gastrinoma (Zollinger-Ellison syndrome) Insulinoma Vasoactive-intestinal polypeptidesecreting Glucagonoma Pancreatic polypeptide-secreting Non-hormone-secreting Other Type 2A Medullary thyroid cancer (>90 percent) Pheochromocytoma (40 to 50 percent) Parathyroid hyperplasia (10 to 20 percent) Cutaneous lichen amyloidosis Type 2B Medullary thyroid cancer Pheochromocytoma Other -Mucosal neuromas -Intestingal ganglioneuromas -Marfanoid habitus Familial medullary thyroid cancer (variant of 2A) Medullary thyroid cancer
19
20 Band keratopathy Subepithelial Ca-PO 4 deposits in the cornea
21 Sub-periosteal resorption
22 Cystic brown tumors Chondrocalcinosis
23 National Institutes of Health Consensus Conference in 2008 Asymptomatic PHPT candidates for surgery Age < 50 yr Serum calcium level 1.0 mg/dl (0.25 mmol/liter) above upper limits of normal Cr.Cl reduced to 60 ml/min by MDRD equation no.7 Osteoporosis by T-score History of kidney stones or fractures J Clin Endocrinol Metab 94: , 2009
24 Symptomatic PHPT Cohort studies : after parathyroidectomy BMD & fracture rate : improve Cognitive function:improve Kidney stones : incidence declines after surgery. CVD & premature death : decrease
25 Sestamibi scan Noninvasive Most popular Localize abnormal parathyroid glands Quality varies Nonlocalizing sestamibi -Multigland disease -Small parathyroid gl. -Coexistent thyroid dz.
26 Secondary and tertiary hyperparathyroidism 2 hyperparathyroidism Severe chronic kidney disease Usually have low or normal serum calcium concentrations Prolonged disease, may develop hypercalcemia 'Adynamic bone disease 3 hyperparathyroidism Advanced renal failure Due to progression from appropriate parathyroid hyperplasia to autonomous overproduction of PTH UTD18.1
27 Milk-alkali syndrome Triad of hypercalcemia, metabolic alkalosis, and renal insufficiency Associated with the ingestion of large amounts of calcium and absorbable alkali Typically occurs in the setting of excess calcium carbonate supplementation to treat osteoporosis or dyspepsia UTD18.1
28 Milk-alkali syndrome Metabolic alkalosis can directly stimulating calcium reabsorption in the distal tubule, thereby diminishing calcium excretion Calcium-induced decline in renal function, due to renal vasoconstriction Chronic hypercalcemia, renal structural injury, can also contribute to the inability to excrete the excess calcium Renal function usually returns to baseline after cessation of milk or calcium carbonate intake, but irreversible injury can occur in patients who have prolonged hypercalcemia UTD18.1
29 Milk-alkali syndrome What remains unexplained is the apparent difference in sensitivity of individuals to increased intake of calcium and alkali Some individuals may not suppress calcitriol levels in response to large doses of calcium carbonate UTD18.1
30 Malignancies associated with hypercalcemia Osteolytic metastases: Breast cancer Multiple myeloma Lymphoma Leukemia Humoral hypercalcemia (PTHrP): Squamous cell carcinomas Renal carcinomas Bladder carcinoma Breast cancer Ovarian carcinoma Non-Hodgkin lymphoma CML Leukemia Lymphoma 1,25- dihydroxyvitamin D: Lymphoma (Non-Hodgkin, Hodgkin, lymphomatosis/granulomatosis) Ovarian dysgerminomas Ectopic PTH sectretion: Ovarian carcinoma Lung carcinomas Neuroectodermal tumor Thyroid papillary carcinoma Rhabdomyosarcoma Pancreatic cancer UTD18.1
31 Treatment of hypercalcemia Saline therapy Loop diuretic Initiated routinely once fluid repletion had been achieved to further increase urinary calcium excretion Calcitonin Bisphosphonate Dialysis UTD18.1
32 Calcitonin Reduce serum calcium by increasing renal calcium excretion Decreasing bone reabsorption via interference with osteoclast maturation Salmon calcitonin (4 international units/kg) is usually administered IM or SC every 12 hour Limited to first 48 hours, even with repeated doses, indicating the development of tachyphylaxis, perhaps due to receptor downregulation UTD18.1
33 Bisphosphonates Intravenous zoledronic acid or pamidronate Side effects Flu-like symptoms (fever, arthralgias, myalgia, fatigue, bone pain) Ocular inflammation (uveitis) Hypocalcemia Hypophosphatemia Impaired renal function/nephrotic syndrome Osteonecrosis of the jaw UTD18.1
34 Glucocorticoid Responsible for the hypercalcemia associated Excess ingestion of vitamin D Endogenous overproduction of calcitriol (1,25-dihydroxyvitamin D) Chronic granulomatous diseases eg, sarcoidosis Lymphoma UTD18.1
35 Hypocalcemia Clinical manifestations of hypocalcemia depend upon the severity and chronicity of hypocalcemia Each 1 g/dl reduction in the serum albumin concentration will lower the total calcium concentration by approximately 0.8 mg/dl
36 Clinical manifestations of hypocalcemia Acute Neuromuscular irritability (Tetany) Paresthesias (peri-oral, extremities) Muscle twitching Carpopedal spasm Trousseau's sign Chvostek's sign Seizures Laryngospasm Bronchospasm Cardiac Prolonged QT interval Hypotension Heart failure Arrhythmia Papilledema Chronic Ectopic calcification (basal ganglia) Extrapyramidal signs Parkinsonism Dementia Subcapsular cataracts Abnormal dentition Dry skin
37 Major causes of hypocalcemia Low PTH (hypoparathyroidism) Genetic disorders Abnormal parathyroid gland development Abnormal PTH synthesis Activating mutations of calcium sensing receptor (autosomal dominant hypocalcemia or sporadic isolated hypoparathyroidism) Post-surgical : thyroidectomy, parathyroidectomy, radical neck dissection Autoimmune Autoimmune polyglandular syndrome (associated with chronic mucocutaneous candidiasis and primary adrenal insufficiency) Isolated hypoparathyroidism due to activating antibodies to calcium sensing receptor Infiltration of the parathyroid gland : granulomatous, iron overload, metastases Radiation induced destruction parathyroid glands Hungry bone syndrome (post parathyroidectomy) HIV infection UTD18.1
38 Major causes of hypocalcemia Low PTH (hypoparathyroidism) Genetic disorders Abnormal parathyroid gland development Abnormal PTH synthesis Activating mutations of calcium sensing receptor (autosomal dominant hypocalcemia or sporadic isolated hypoparathyroidism) Post-surgical : thyroidectomy, parathyroidectomy, radical neck dissection Autoimmune Autoimmune polyglandular syndrome (associated with chronic mucocutaneous candidiasis and primary adrenal insufficiency) Isolated hypoparathyroidism due to activating antibodies to calcium sensing receptor Infiltration of the parathyroid gland : granulomatous, iron overload, metastases Radiation induced destruction parathyroid glands Hungry bone syndrome (post parathyroidectomy) HIV infection
39 Major causes of hypocalcemia High PTH (secondary hyperparathyroidism in response to hypocalcemia) Vitamin D deficiency or resistance Parathyroid hormone resistance Pseudohypoparathyroidism Hypomagnesemia Renal disease Loss of calcium from the circulation Hyperphosphatemia Tumor lysis Acute pancreatitis Osteoblastic metastases Acute respiratory alkalosis Sepsis or acute severe illness Drugs Inhibitors of bone resorption (bisphosphonates, calcitonin), especially in vitamin D deficiency Cinacalcet Calcium chelators (EDTA, citrate, phosphate) Foscarnet (due to intravascular complexing with calcium) Phenytoin (due to conversion of vitamin D to inactive metabolites) Fluoride poisoning Disorders of magnesium metabolism Hypomagnesemia can reduce PTH secretion or cause PTH resistance and is therefore associated with normal, low, or high PTH levels UTD18.1
40 Approach to hypocalcemia Measure serum albumin Family history of hypocalcemia genetic cause Chronic hypocalcemia Activating mutation of calcium sensing receptor Pseudohypoparathyroidism Acquired hypoparathyroidism Postsurgical or autoimmune damage Autoimmune hypoparathyroidism Isolated abnormality/polyglandular autoimmune syndrome type I Lab : ipth, Cr, Mg, PO4, 25(OH) vitd UTD18.1
41 N Engl J Med 2004;350:
42 PTH Correct Ca PO4 Mg 25(OH)D 1,25(OH)D Cr Hypoparathyroid Activating mutation calcium sensing receptor Hypo Mg PTH resistance (pseudohypoparathyroid) Vitamin D deficiency Chronic kidney disease UTD18.1
43 PTH Correct Ca PO4 Mg 25(OH)D 1,25(OH)D Cr Hypoparathyroid Activating mutation calcium sensing receptor Hypo Mg PTH resistance (pseudohypoparathyroid) Vitamin D deficiency Chronic kidney disease UTD18.1
44 Osteoporosis Decrease bone strength and increase fracture Imbalance of bone resorption and bone formation Bone strength Structural properties : Size, Shape, Microarchitecture Material properties : Mineral, Collagen
45 WHO definition of Osteoporosis Diagnostic Category T-score Normal > -1 Osteopenia -1 to -2.5 Osteoporosis -2.5 Severe Osteoporosis -2.5 and 1 fragility fracture
46 ข อบ งช ในการส งตรวจ BMD Thai osteoporosis guideline
47 Thai osteoporosis guideline
48 BMD (DEXA) Central Lumbar spine (L1-L4) Femoral area Peripheral Radius
49 BMD
50 BMD
51 BMD
52 BMD
53 Common causes for secondary osteoporosis Endocrine diseases Diabetes mellitus GH deficiency (rare) Acromegaly (rare) Hypercortisolism Hyperparathyroidism Hyperthyroidism Premature menopause Male hypogonadism GI disorders Gastrectomy Celiac disease Inflammatory bowel disease Liver cirrhosis Chronic biliary tract obstruction Chronic therapy with proton pump inhibitors European Journal of Endocrinology (2010)
54 Common causes for secondary osteoporosis Hematologic diseases Myeloma Monoclonal gammopathy of undetermined significance Lymphoma/leukemia Systemic mastocytosis (rare) Disseminated carcinoma Chemotherapy Rheumatological Rheumatoid arthritis Ankylosing spondylitis Systemic lupus erythematosus Other Osteogenesis imperfecta Anorexia nervosa European Journal of Endocrinology (2010)
55 Glucocorticoid excess Glucocorticoids impairs skeletal health Inhibition of bone formation due to induction of osteoblast and osteocyte apoptosis European Journal of Endocrinology (2010)
56 Glucocorticoid excess Predominant spinal bone loss and vertebral fractures Increased risk of falls due to muscular atrophy and altered neuromuscular function Low doses of glucocorticoids (prednisolone mg/day) associated with a 2.6-fold higher risk of vertebral fractures European Journal of Endocrinology (2010)
57 Glucocorticoid-induce Osteoporosis N Engl J Med 2011;365:62-70
58 Glucocorticoid-induce Osteoporosis National osteoporosis foundation Prednisolone 5 mg/day for at least 3 months Yearly BMD testing Threshold for treatment : T-score 2.5 Calcium 1200 mg/day, vitamin D 2000 units/day Bisphosphonate Teriparatide : only for patients at high risk N Engl J Med 2011;365:62-70
59 Hyperthyroidism Thyroid hormone excess (suppressed TSH) Activation of thyroid hormone receptor a on osteoblasts and osteoclasts results in enhanced bone resorption and bone loss European Journal of Endocrinology (2010)
60 Hyperthyroidism Large study of 686 postmenopausal women serum TSH level < 0.1 miu/l 4x 5x risk of hip and vertebral fractures Meta-analysis of 21 studies indicated that thyroid hormone therapy for TSH suppression in differentiated thyroid cancer subclinical hyperthyroidism is associated with osteoporosis in postmenopausal women European Journal of Endocrinology (2010)
61 Drug-induced osteoporosis Numerous drugs affect bone metabolism interfere Absorption of vitamin D, Ca, and PO 4 Vitamin D metabolism and action Direct cellular effects on osteoblasts, osteoclasts, and osteocytes Interference amount or quality of bone matrix proteins European Journal of Endocrinology (2010)
62 Drug-induced osteoporosis TZDs (rosiglitazone and pioglitazone) Insulin sensitizers Act as agonists of the peroxisome proliferatoractivated receptor-gamma 3-5 fold higher risk of fractures of the humerus, femur, and hip in postmenopausal women European Journal of Endocrinology (2010)
63 Drug-induced osteoporosis TZD Shunting pluripotent mesenchymal stem cells Osteoblastic lineage Adipocyte European Journal of Endocrinology (2010)
64 Drug-induced osteoporosis Drug class Examples Indications Glucocorticoids Prednisolone Autoimmune diseases Chemotherapeutic drugs Methotrexate, ifosfamide Tyrosine kinase inhibitors Imatinib Chronic myelogenous leukemia Thiazolidinediones Rosiglitazone, pioglitazone Type 2 diabetes mellitus Proton pump inhibitor Omeprazole and pantoprazole Peptic ulcer and reflux diseases Thyroid hormone L-thyroxine Replacement therapy for hypothyroidism, thyroid cancer Anticonvulsants Valproic acid Chronic seizure disorders Antidepressants Selective serotonin reuptake inhibitors Chronic depression Anti-retroviral drugs Tenofovir HIV disease European Journal of Endocrinology (2010)
65 Diagnostic tests in the work-up of secondary osteoporosis Diagnostic tests CBC Renal and Liver function test Ca and PO 4 Serum bone specific or ALP Serum 25-hydroxyvitamin D Serum TSH FBS Intact PTH Serum protein electrophoresis, immunofixation Purpose Anemia as in myeloma or celiac disease, Leukocytosis as in leukemia Renal or liver failure, alcohol abuse Primary hyperparathyroid, myeloma Paget disease, osteomalacia Vitamin D deficiency, osteomalacia Hyperthyroidism Diabetic mellitus Primary hyperparathyroidism MGUS, myeloma European Journal of Endocrinology (2010)
66 Diagnostic tests Serum free testosterone Serum CRP Diagnostic tests in the work-up of secondary osteoporosis Purpose Male hypogonadism 24 hour urine calcium excretion Hypercalciuria Anti-tissue transglutaminase antibodies Anti-HIV antibodies Morning fasting serum cortisol after dexamethasone suppression Serum tryptase levels, urinary histamine excretion COL1A genetic testing Iliac crest bone biopsy Chronic infection/inflammation Celiac disease HIV disease, AIDS Cushing s syndrome Systemic mastocytosis Osteogenesis imperfecta Systemic mastocytosis, MGUS/myeloma, osteomalacia, lymphoma/leukemia European Journal of Endocrinology (2010)
67 Laboratory Evaluation CBC Renal function Chemistry : Ca, PO 4, ALP, LFT ESR, CRP Thyroid function test 25- hydroxyvitamin D Gonadal function
68 Treatment of Osteoporosis Pharmacotherapy Secondary cause Lifestyle Modification
69 Factor Influencing Fractures Hormone Shape & architecture Postural reflexes Nutrition Bone mass Bone strength Fracture Exercise & Life style Material properties Falls Soft tissue padding
70 Lifestyle Modification Weight-bearing exercise : jogging, aerobic dancing, jumping rope Physical activity : 30 min / most day of week Fall prevention
71 Treatment (NOF 2008) Postmenopausal women and men older than 50 yr A hip or vertebral fracture fracture T score < -2.5 at femoral neck, total hip or spine Low bone mass (T score -1 to -2.5 at femoral neck, total hip or spine) with other prior fracture Low bone mass (T score -1 to -2.5 at femoral neck, total hip or spine) with secondary causes associated with high risk fracture Low bone mass (T score -1 to -2.5 at femoral neck, total hip or spine) and 10- yr probability of hip fracture 3% or a 10-yr probability of any major osteoporosis related fracture 20%
72 การร กษาภาวะโรคกระด กพร น Thai osteoporosis guideline
73 Thai osteoporosis guideline
74 Thai osteoporosis guideline
75 Pharmacotherapy Adequate Calcium and vitamin D intake NOF 2008 : -Ca 1200 mg per day, -Vitamin D IU per day Thai : -Ca ; yr : 1000 mg per day, >50 yr : 800 mg per day -Vitamin D : IU per day
76 Which drugs should be used? Antiresorptive agents Bisphosphonate Calcitonin Hormone replacement therapy Selective estrogen receptor modulators Bone formative (anabolic) agents Teriparatide (1-34 PTH) Double action Strontium ranelate
77 Bisphosphonate Targeting of bisphosphonates to bone, localized release during osteoclastic bone resorption Intestinal absorption is low Taken with a glass of tap water and 30 min before food or other fluids 40-60% absorbed bisphosphonate not bound to bone & not metabolized Eliminated unchanged by renal excretion
78 Flu-like symptoms Bisphosphonates IV can block FPP production in monocytes Accumulation of isopentenyl diphosphate (IPP) Because IPP is also a bacterial antigen, peripheral blood T cells recognize this as bacterial infection Releasing TNF-α and IFN-γ, increasing IL-6 and CRP, and causing flu-like symptoms Associated with 1 st bisphosphonate doses
79 Esophagitis and ulceration Before absorption, bisphosphonates taken orally can bind to gastric cells Inhibition of FPP synthase rapidly leads to cell death. This may explain the ability of orally administered N-BPs to cause esophagitis and ulceration
80 Osteonecrosis of the Jaw (ONJ) Rarely with oral bisphosphonates Most cases of Pt cancer with IV bisphosphonates Risk factors -Cancer -Concomitant therapies (chemotherapy, radiotherapy and corticosteroids) -Poor oral hygiene -Comorbid eg. anemia, coagulopathy, infection -Duration of exposure, and older age CKD
81 Osteonecrosis of Jaw
82 Prevention(recommend) Before use bisphosphonates :removal of all foci of dental infection. Routine dental care Regular oral examinations
83 Osteomalacia Osteomalacia : disorder of mineralization of newly formed matrix in adults Rickets : disorder of defective mineralization of cartilage in the epiphyseal growth plates of children, leading to widening of the ends of long bones, growth retardation, and skeletal deformities.
84 Normal bone Osteoporosis Decreased bone mineralization and matrix Osteomalacia Decreased bone mineralization with normal or increased matrix Osteoporosis + osteomalacia Suggest osteomalacia Bone pain, tenderness Myopathy Pseudofracture Increased alkaline P
85 Causes of osteomalacia Abnormal vitamin D metabolism : 2 hyperparathyroidism & hypophosphatemia Deficient intake or absorption Dietary Inadequate sunlight exposure Malabsorption Gastrectomy Small bowel disease Vitamin D Pancreatic insufficiency Defective 25-hydroxylation Biliary cirrhosis Alcoholic cirrhosis Anticonvulsants Loss of vitamin D binding protein Nephrotic syndrome Defective 1-alpha 25-hydroxylation Hypoparathyroidism Renal failure Vitamin D-dependent rickets type 1 Defective target organ response to calcitriol Vitamin D-dependent rickets, type II (Hereditary vitamin D resistant rickets, HVDRR)
86 Causes of osteomalacia Mineralization defects Abnormal matrix Chronic renal failure Osteogenesis imperfecta Fibrogenesis imperfecta Axial osteomalacia Enzyme deficiency Hypophosphatasia Inhibitors of mineralization Fluoride Aluminium Bisphosphonates Phosphate deficiency Decreased intake Antacids Impaired renal reabsorption -Primary defects X-linked hypophosphatemic rickets (vitamin D resistant rickets, VDRR) Hereditary hypophosphatemic rickets with hypercalciuria Sporadic acquired hypophosphatemic rickets Fanconi Syndrome-Wilson disease, cystinosis, multiple myeloma -Secondary defects Primary hyperparathyroidism Secondary hyperparathyroidism (renal tubular acidosis, type 1 and disorders of vitamin D metabolism) Oncogenic osteomalacia
87 CLINICAL PRESENTATION Asymptomatic and present radiologically as osteopenia Proximal muscle weakness Muscle wasting, hypotonia, and discomfort with movement Waddling gait Bone pain lower spine, pelvis, lower extremities may be associated with tenderness to palpation dull & aching, aggravated by activity & weight bearing Fractures may occur with little or no trauma ribs, vertebrae, long bones Skeletal deformities are infrequent in adults. Abnormal spinal curvature or deformity of the thorax or pelvis appears only in severe osteomalacia of long duration
88
89 Two theories have been proposed: 1. Stress fractures that have been repaired by the laying down of inadequately mineralized osteoid 2. Result of erosion by arterial pulsations. Looser zones : pseudofractures or narrow radiolucent lines
90 Disorder Phosphate Calcium ALP Vit D deficiency with 2 hyper PTH Low Low to low normal Elevated Metabolic acidosis Normal Normal Normal Proximal RTA Low Normal Normal Hypophosphatasia Normal Normal Low Osteogenesis imperfecta and axial osteomalacia Normal Normal Normal Osteoporosis Normal Normal Normal
91 Vitamin D deficiency 25-Hydroxyvitamin D levels are inversely associated with parathyroid hormone levels until the former reach 30 to 40 ng per milliliter, at which point PTH begin to level off (at their nadir) Vitamin D insufficiency.. 25-hydroxyvitamin D < 30 ng per milliliter Vitamin D intoxication.. 25-hydroxyvitamin D > 150 ng per milliliter
92 Treatment Preventive and Maintenance to Avoid Deficiency IU of vitamin D3/day 50,000 IU of vitamin D2 every 2 wk or every month Treatment of Deficiency 50,000 IU of vitamin D2 every wk for 8 weeks Then repeat treatment for another 8 wk if 25- hydroxyvitamin D <30 ng/ml
Approach to a patient with hypercalcemia
 Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Approach to a patient with hypercalcemia Ana-Maria Chindris, MD Division of Endocrinology Mayo Clinic Florida 2013 MFMER slide-1 Background Hypercalcemia is a problem frequently encountered in clinical
Hypocalcemia 6/8/12. Normal value. Physiologic functions. Nephron a functional unit of kidney. Influencing factors in Calcium and Phosphate Balance
 Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
Normal value Hypocalcemia Serum calcium Total mg/dl Ionized mg/dl Cord blood 9.0 ~ 11.5 5.0 ~ 6.o New born (1 st 24 hrs) 9.0 ~ 10.6 4.3 ~ 5.1 24~ 48 hrs 7.0 ~12.0 4.0 ~4.7 Child 8.8 ~10.8 4.8 ~4.92 There
HYPERCALCEMIA. Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences
 HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
HYPERCALCEMIA Babak Tamizi Far MD. Assistant professor of internal medicine Al-zahra hospital, Isfahan university of medical sciences ESSENTIALS OF DIAGNOSIS Serum calcium level > 10.5 mg/dl Serum ionized
CALCIUM BALANCE. James T. McCarthy & Rajiv Kumar
 CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
CALCIUM BALANCE James T. McCarthy & Rajiv Kumar CALCIUM BALANCE TOTAL BODY CALCIUM (~ 1000g in a normal 60 kg adult) - > 99% in bones - ~ 0.6% in the intracellular space - ~ 0.1% in the extracellular space
Practical Management Of Osteoporosis
 Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
Practical Management Of Osteoporosis CONFERENCE 2012 Education Centre, Bournemouth.19 November The following companies have given funding towards the cost of this meeting but have no input into the agenda
Calcium and Parathyroid Disorders
 Calcium and Parathyroid Disorders Hussain Mahmud, MD Clinical Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism University of Pittsburgh Butler Memorial Hospital November
Calcium and Parathyroid Disorders Hussain Mahmud, MD Clinical Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism University of Pittsburgh Butler Memorial Hospital November
Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes.
 Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
Academic lectures 3rd year of Medical faculty Figures and tables in this presentation were adopted from various printed and electronic resorces and serve strictly for educational purposes. ENDOCRINOLOGY
HYPERCALCAEMIA 101 FOR THE INTERNIST
 HYPERCALCAEMIA 101 FOR THE INTERNIST Dr Chionh Siok Bee Dept of Medicine, National University Hospital siok_bee_chionh@nuhs.edu.sg Medicine Review Course 18/09/2011 Outline of Talk Definition of hypercalcaemia
HYPERCALCAEMIA 101 FOR THE INTERNIST Dr Chionh Siok Bee Dept of Medicine, National University Hospital siok_bee_chionh@nuhs.edu.sg Medicine Review Course 18/09/2011 Outline of Talk Definition of hypercalcaemia
hypercalcemia of malignancy hyperparathyroidism PHPT the most common cause of hypercalcemia in the outpatient setting the second most common cause
 hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
hyperparathyroidism A 68-year-old woman with documented osteoporosis has blood tests showing elevated serum calcium and parathyroid hormone (PTH) levels: 11.2 mg/dl (8.8 10.1 mg/dl) and 88 pg/ml (10-60),
Hypercalcemia & Parathyroid Disorders. W. Reid Litchfield, MD, FACE, ECNU Desert Endocrinology
 Hypercalcemia & Parathyroid Disorders W. Reid Litchfield, MD, FACE, ECNU Desert Endocrinology Objectives Review diagnostic workup for hypercalcemia Review management of primary hyperparathyroidism Review
Hypercalcemia & Parathyroid Disorders W. Reid Litchfield, MD, FACE, ECNU Desert Endocrinology Objectives Review diagnostic workup for hypercalcemia Review management of primary hyperparathyroidism Review
Case 4 Generalised bone pain
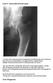 Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Case 4 Generalised bone pain C A 34- year- old woman presented complaining of multifocal pain in her chest and legs. The pain was intermittent, was aggravated by weight bearing. Initially was alleviated
Agents that Affect Bone & Mineral Homeostasis
 Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
Agents that Affect Bone & Mineral Homeostasis 1 Agents that Affect Bone & Mineral Homeostasis Calcium and phosphate are the major mineral constituents of bone. They are also two of the most important minerals
PRIMARY HYPERPARATHYROIDISM PRIMARY HYPERPARATHYROIDISM. Hyperparathyroidism Etiology. Common Complex Insidious Chronic Global Only cure is surgery
 ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
ENDOCRINE DISORDER PRIMARY HYPERPARATHYROIDISM Roseann P. Velez, DNP, FNP Francis J. Velez, MD, FACS Common Complex Insidious Chronic Global Only cure is surgery HYPERPARATHYROIDISM PARATHRYOID GLANDS
Clinical biochemistry of calcium and vitamin D
 Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Clinical biochemistry of calcium and vitamin D Dr Andrew Day Consultant in Clinical Biochemistry and Metabolic Medicine University Hospitals Bristol NHS Trust e-mail: andrew.day@uhbristol.nhs.uk A 48-year
Hypercalcemia. Brian Rose, M.D. Bozeman Health June 6, 2018
 Hypercalcemia Brian Rose, M.D. Bozeman Health June 6, 2018 Hypercalcemia Diagnosis PTH Mediated Primary Hyperparathyroidism Lithium Familial Hypocalciuric Hypercalcemia Non PTH mediated Malignancy Humoral
Hypercalcemia Brian Rose, M.D. Bozeman Health June 6, 2018 Hypercalcemia Diagnosis PTH Mediated Primary Hyperparathyroidism Lithium Familial Hypocalciuric Hypercalcemia Non PTH mediated Malignancy Humoral
Diagnosis and Treatment of Osteoporosis. Department of Endocrinology and Metabolism Ajou University School of Medicine.
 Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
Diagnosis and Treatment of Osteoporosis Department of Endocrinology and Metabolism Ajou University School of Medicine Yoon-Sok CHUNG WCIM, COEX, Seoul, 27Oct2014 Case 1 71-year old woman Back pain Emergency
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate (start to develop symptoms) 3.0 3.4
Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff.
 Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
Authoriser: Fiona Davidson Page 1 of 5 Hypercalcaemia Definition Elevated Adjusted Calcium > 2.6 mmol/l (adjusted for albumin), taken without using a cuff. Mild (usually no symptoms) 2.6 3.0 mmol/l Moderate
BMD: A Continuum of Risk WHO Bone Density Criteria
 Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Calcium metabolism and the Parathyroid Glands. Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands
 Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Calcium metabolism and the Parathyroid Glands Calcium, osteoclasts and osteoblasts-essential to understand the function of parathyroid glands Calcium is an essential element for contraction of voluntary/smooth
Endocrine Regulation of Calcium and Phosphate Metabolism
 Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Endocrine Regulation of Calcium and Phosphate Metabolism Huiping Wang ( 王会平 ), PhD Department of Physiology Rm C516, Block C, Research Building, School of Medicine Tel: 88208252 Email: wanghuiping@zju.edu.cn
Southern Derbyshire Shared Care Pathology Guidelines. Primary Hyperparathyroidism
 Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Southern Derbyshire Shared Care Pathology Guidelines Primary Hyperparathyroidism Please use this Guideline in Conjunction with the Hypercalcaemia Guideline Definition Driven by hyperfunction of one or
Magnesium Homeostasis
 ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
ECTS PhD Training Course, Rome 3 rd September 2008 Disorders of Calcium, Phosphate h and Magnesium Homeostasis Richard Eastell Professor of Bone Metabolism Academic Unit of Bone Metabolism University of
Bone Metastases. Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital
 Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Bone Metastases Sukanda Denjanta, M.Sc., BCOP Pharmacy Department, Chiangrai Prachanukroh Hospital 1 Outline Pathophysiology Signs & Symptoms Diagnosis Treatment Spinal Cord Compression 2 General Information
Overview. Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases. People Centred Positive Compassion Excellence
 Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
Overview Osteoporosis and Metabolic Bone Disease Dr Chandini Rao Consultant Rheumatologist Bone Biology Osteoporosis Osteomalacia Paget s Disease Cases Bone Biology Osteoporosis Increased bone remodelling
Disclosure and Conflicts of Interest Steven T Harris MD Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis
 Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis Steven T Harris MD FACP Clinical Professor of Medicine University of California, San Francisco Disclosure and Conflicts of Interest
Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis Steven T Harris MD FACP Clinical Professor of Medicine University of California, San Francisco Disclosure and Conflicts of Interest
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD
 The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
The Calcium Conundrum: When, What and How to Give Calcium in Pediatric CKD/ESRD Jess Tower MS RD LD 3/18/19 Children s Mercy Hospital jdtower@cmh.edu 816 460 1067 Disclosures Nothing to disclose 1 How
Hyperparathyroidism. When to Suspect, How to Diagnose, When and How to Intervene. Johanna A. Pallotta, MD, FACP, FACE
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline Definition of hyperparathyroidism
Osteoporosis. When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of.
 Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
Osteoporosis When we talk about osteoporosis, we have to be familiar with the constituents of bone and what it is formed of. Osteoblasts by definition are those cells present in the bone and are involved
PRIMARY HYPERPARATHYROIDISM
 PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
PRIMARY HYPERPARATHYROIDISM HYPERPARATHYROIDISM Inappropriate excess secretion of Parathyroid Hormone in Primary Hyperparathyroidism Appropriate Hypersecretion in Secondary Hyperparathyroidism PTH and
Awaisheh. Mousa Al-Abbadi. Abdullah Alaraj. 1 Page
 f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
f #3 Awaisheh Abdullah Alaraj Mousa Al-Abbadi 1 Page *This sheet was written from Section 1 s lecture, in the first 10 mins the Dr. repeated all the previous material relating to osteoporosis from the
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis
 Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
Investigations for Disorders of Calcium, Phosphate and Magnesium Homeostasis Tutorial for Specialist Portfolio Biomedical Scientists 03/02/2014 Dr Petros Kampanis Clinical Scientist 1. Calcium Most abundant
David Bruyette, DVM, DACVIM
 VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
VCAwestlaspecialty.com David Bruyette, DVM, DACVIM Disorders of calcium metabolism are common endocrine disorders in both dogs and cats. In this article we present a logical diagnostic approach to patients
Disclosure. Topic Outline. Calcium, Vitamin D, PTH Disorders. PTH/Calcium-Normal Physiology. I have nothing to disclose
 Disclosure Calcium, Vitamin D, PTH Disorders I have nothing to disclose Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF Topic Outline Calcium/Vitamin D/PTH physiology
Disclosure Calcium, Vitamin D, PTH Disorders I have nothing to disclose Chienying Liu MD Associate Clinical Professor Division of Endocrinology & Metabolism UCSF Topic Outline Calcium/Vitamin D/PTH physiology
Hypercalcemia. Hypercalcemia: When to Worry, When to Treat! Mineral Metabolism : A Short Course
 Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Hypercalcemia: When to Worry, When to Treat! Michael A. Levine has no financial relationships to disclose or Conflicts of Interest to resolve. Michael A. Levine, M.D. This presentation will not involve
Ca, Mg metabolism, bone diseases. Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary
 Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
Ca, Mg metabolism, bone diseases Tamás Kőszegi Pécs University, Department of Laboratory Medicine Pécs, Hungary Calcium homeostasis Ca 1000g in adults 99% in bones (extracellular with Mg, P) Plasma/intracellular
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE
 HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
HYPERPARATHYROIDIS M FAISAL GHANI SIDDIQUI MBBS; FCPS; PGDIP-BIOMEDICAL ETHICS; MCPS-HPE PROFESSOR OF SURGERY J I N N A H S I N D H M E D I C A L U N I V E R S I T Y PREAMBLE Anatomy & physiology of the
Kristen M. Nebel, DO PENN/ LGHP Geriatrics. Temple Family Medicine Review
 Kristen M. Nebel, DO PENN/ LGHP Geriatrics 10/3/17 Temple Family Medicine Review OBJECTIVES Define Revised 2017 American College of Physician Recommendations Screening, Prevention and Treatment Application
Kristen M. Nebel, DO PENN/ LGHP Geriatrics 10/3/17 Temple Family Medicine Review OBJECTIVES Define Revised 2017 American College of Physician Recommendations Screening, Prevention and Treatment Application
dr. Judit Tőke DISEASES OF THE PARATHYROID GLAND METABOLIC BONE DISEASES OSTEOPOROSIS SEMMELWEIS UNIVERSITY 2nd Department of Medicine
 DISEASES OF THE PARATHYROID GLAND METABOLIC BONE DISEASES OSTEOPOROSIS dr. Judit Tőke SEMMELWEIS UNIVERSITY 2nd Department of Medicine Diseases of the parathyroid gland Outline Primary hyperparathyroidism
DISEASES OF THE PARATHYROID GLAND METABOLIC BONE DISEASES OSTEOPOROSIS dr. Judit Tőke SEMMELWEIS UNIVERSITY 2nd Department of Medicine Diseases of the parathyroid gland Outline Primary hyperparathyroidism
Sachin Soni DNB Pediatrics
 Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Sachin Soni DNB Pediatrics Vitamin D physiology Introduction Etiology Clinical feature Radiology Diagnosis Lab Treatment Source: -Fish, liver and oil, - Human milk (30-40 IU/L) - Exposure to sun light
Persistent post transplant hyperparathyroidism. Shiva Seyrafian IUMS-97/10/18-8/1/2019
 Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
Persistent post transplant hyperparathyroidism Shiva Seyrafian IUMS-97/10/18-8/1/2019 normal weight =18-160 mg In HPT= 500-1000 mg 2 Epidemiology Mild 2 nd hyperparathyroidism (HPT) resolve after renal
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS. BY: Shifaa Qa qa
 NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
NEOPLASMS OF THE THYROID PATHOLOGY OF PARATHYROID GLANDS BY: Shifaa Qa qa Neoplasmas of the thyroid thyroid nodules Neoplastic ---- benign, malignant Non neoplastic Solitary nodules ----- neoplastic Nodules
Case study Group 2 presentation
 Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Case study Group 2 presentation Patient profile HN 3095-57 Female 60 years old Hometown : Sa Kaeo province Occupation : farmer No drug and food allergy Chief complain Left neck mass 10 years PTA that gradually
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Vitamin D Deficiency. Micol Rothman, MD Assistant Professor of Medicine Clinical Director Metabolic Bone Program University of CO-Denver
 Vitamin D Deficiency Micol Rothman, MD Assistant Professor of Medicine Clinical Director Metabolic Bone Program University of CO-Denver 50 yo woman referred for osteoporosis What is striking about her
Vitamin D Deficiency Micol Rothman, MD Assistant Professor of Medicine Clinical Director Metabolic Bone Program University of CO-Denver 50 yo woman referred for osteoporosis What is striking about her
Vitamin D Hormone Du Jour
 Vitamin D Hormone Du Jour J R Minkoff MD, FACP Endocrinology Clinical Professor of Family and Community Medicine UCSF Why Is Vitamin D Important? Musculo-skeletal effects Possible other effects Immunomodulatory
Vitamin D Hormone Du Jour J R Minkoff MD, FACP Endocrinology Clinical Professor of Family and Community Medicine UCSF Why Is Vitamin D Important? Musculo-skeletal effects Possible other effects Immunomodulatory
Osteoporosis/Fracture Prevention
 Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Skeletal Manifestations
 Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy
 "Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
"Asymptomatic" Hyperparathyroidism: Reasons for Parathyroidectomy Rebecca S. Sippel, M.D. Assistant Professor Department of Surgery Section of Endocrine Surgery University of Wisconsin Primary Hyperparathyroidism
John J. Wolf, DO Family Medicine
 John J. Wolf, DO Family Medicine Objectives: 1. Review incidence & Risk of Osteoporosis 2.Review indications for testing 3.Review current pharmacologic & Non pharmacologic Tx options 4.Understand & Utilize
John J. Wolf, DO Family Medicine Objectives: 1. Review incidence & Risk of Osteoporosis 2.Review indications for testing 3.Review current pharmacologic & Non pharmacologic Tx options 4.Understand & Utilize
Metabolic Bone Disease (Past, Present and Future Challenges in the Management)
 Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Metabolic Bone Disease 871 151 Metabolic Bone Disease (Past, Present and Future Challenges in the Management) SNA RIZVI INTRODUCTION The past 40 years have seen some important historical events leading
Clinical Approach to Hypercalcemia For the Primary Care Provider
 Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
Clinical Approach to Hypercalcemia For the Primary Care Provider Christina Maser, MD FACS UCSF Fresno Department of Surgery, Endocrine Surgery 2/2/19 Objectives Recognition of pitfalls of diagnosis of
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
Hyper and hypocalcaemia. Prof Tricia Tan
 Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
Hyper and hypocalcaemia Prof Tricia Tan Learning Objectives Basic physiology of Ca regulation Case presentations Take home messages Calcium Total body calcium content ~1300g 99% in bone 1% intracellular
Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017
 Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide was developed to assist Primary Care physicians
Kaiser Permanente National CLINICAL PRACTICE GUIDELINES Osteoporosis/Fracture Prevention Clinician Guide SEPTEMBER 2017 Introduction This Clinician Guide was developed to assist Primary Care physicians
Potential conflicts of interest: None
 Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Hyperparathyroidism When to Suspect, How to Diagnose, When and How to Intervene November 6, 2013 Johanna A. Pallotta, MD, FACP, FACE Potential conflicts of interest: None Johanna A. Pallotta, MD Outline
Current and Emerging Strategies for Osteoporosis
 Current and Emerging Strategies for Osteoporosis I have nothing to disclose. Anne Schafer, MD Assistant Professor of Medicine Division of Endocrinology & Metabolism December 12, 2014 Outline Osteoporosis
Current and Emerging Strategies for Osteoporosis I have nothing to disclose. Anne Schafer, MD Assistant Professor of Medicine Division of Endocrinology & Metabolism December 12, 2014 Outline Osteoporosis
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD
 Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
Hypoparathyroidism By John Halpern, DO, FACEP Coauthored by N. Ewen Wang, MD Reprinted with permission from: E-Medicine: Instant Access to the Minds of Medicine http://www.emedicine.com/emerg/topic276.htm
The parathyroid glands participate in the regulation
 41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
41 HERNAN I. VARGAS STANLEY R. KLEIN The parathyroid glands participate in the regulation of calcium metabolism. Disorders of the parathyroid gland are most commonly a result of hyperfunction and rarely
Osteoporosis. Treatment of a Silently Developing Disease
 Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
Osteoporosis Treatment of a Silently Developing Disease Marc K. Drezner, MD Senior Associate Dean Emeritus Professor of Medicine Emeritus University of Wisconsin-Madison Auditorium The Forest at Duke October
Guideline for the investigation and management of osteoporosis. for hospitals and General Practice
 Guideline for the investigation and management of osteoporosis for hospitals and General Practice Background Low bone density is an important risk factor for fracture. The aim of assessing bone density
Guideline for the investigation and management of osteoporosis for hospitals and General Practice Background Low bone density is an important risk factor for fracture. The aim of assessing bone density
The Bare Bones of Osteoporosis. Wendy Rosenthal, PharmD
 The Bare Bones of Osteoporosis Wendy Rosenthal, PharmD Definition A systemic skeletal disease characterized by low bone mass and microarchitectural deterioration of bone tissue, with a consequent increase
The Bare Bones of Osteoporosis Wendy Rosenthal, PharmD Definition A systemic skeletal disease characterized by low bone mass and microarchitectural deterioration of bone tissue, with a consequent increase
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life.
 B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
Osteoporosis - New Guidelines. Michelle Glass B.Sc. (Pharm) June 15, 2011
 Osteoporosis - New Guidelines Michelle Glass B.Sc. (Pharm) June 15, 2011 Outline What is Osteoporosis? Who is at risk? What treatments are available? Role of the Pharmacy technician Definition of Osteoporosis
Osteoporosis - New Guidelines Michelle Glass B.Sc. (Pharm) June 15, 2011 Outline What is Osteoporosis? Who is at risk? What treatments are available? Role of the Pharmacy technician Definition of Osteoporosis
Symptom management: Hypercalcemia
 Symptom management: Hypercalcemia Dr Claire Higham 10.11.16 NLCFN National Conference 2016 Consultant Endocrinologist The Christie Hospital Manchester, UK Hypercalcemia of malignancy 2-30% of patients
Symptom management: Hypercalcemia Dr Claire Higham 10.11.16 NLCFN National Conference 2016 Consultant Endocrinologist The Christie Hospital Manchester, UK Hypercalcemia of malignancy 2-30% of patients
What is Osteoporosis?
 What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
What is Osteoporosis? 2000 NIH Definition A skeletal disorder characterized by compromised bone strength predisposing a person to an increased risk of fracture. Bone strength reflects the integration of
Bone Densitometry Pathway
 Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Bone Densitometry Pathway The goal of the Bone Densitometry pathway is to manage our diagnosed osteopenic and osteoporotic patients, educate and monitor the patient population at risk for bone density
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
CKD: Bone Mineral Metabolism. Peter Birks, Nephrology Fellow
 CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
CKD: Bone Mineral Metabolism Peter Birks, Nephrology Fellow CKD - KDIGO Definition and Classification of CKD CKD: abnormalities of kidney structure/function for > 3 months with health implications 1 marker
Normal Bone Health and Bone Disease. Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017
 Normal Bone Health and Bone Disease Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017 Learning outcomes Understand the structure and function of bone and articular cartilage Explain
Normal Bone Health and Bone Disease Mr Ryan Trickett Consultant Hand and Wrist Surgeon 6 th February 2017 Learning outcomes Understand the structure and function of bone and articular cartilage Explain
Clinician s Guide to Prevention and Treatment of Osteoporosis
 Clinician s Guide to Prevention and Treatment of Osteoporosis Published: 15 August 2014 committee of the National Osteoporosis Foundation (NOF) Tipawan khiemsontia,md outline Basic pathophysiology screening
Clinician s Guide to Prevention and Treatment of Osteoporosis Published: 15 August 2014 committee of the National Osteoporosis Foundation (NOF) Tipawan khiemsontia,md outline Basic pathophysiology screening
INDEX. Note: Page numbers of issue and article titles are in boldface type. cell carcinoma. ENDOCRINE SURGERY
 ENDOCRINE SURGERY INDEX Note: Page numbers of issue and article titles are in boldface type. Adenylate cyclase, in signal transduction 425-426 Adrenal incidentalomas, 499-509 imaging of, 502-504 in patients
ENDOCRINE SURGERY INDEX Note: Page numbers of issue and article titles are in boldface type. Adenylate cyclase, in signal transduction 425-426 Adrenal incidentalomas, 499-509 imaging of, 502-504 in patients
Aromatase Inhibitors & Osteoporosis
 Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 2 Available Product Indication Dosing and Administration Natpara (parathyroid hormone)
Hyperparathyroidism: Operative Considerations. Financial Disclosures: None. Hyperparathyroidism. Hyperparathyroidism 11/10/2012
 Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Hyperparathyroidism: Operative Considerations Financial Disclosures: None Steven J Wang, MD FACS Associate Professor Dept of Otolaryngology-Head and Neck Surgery University of California, San Francisco
Secondary Osteoporosis
 Secondary Osteoporosis Endocrine diseases Gastrointestinal disorders Hematologic diseases Rheumatological diseases Drug-induced osteoporosis other causes Christoph Henzen ... a systemic skeletal disease
Secondary Osteoporosis Endocrine diseases Gastrointestinal disorders Hematologic diseases Rheumatological diseases Drug-induced osteoporosis other causes Christoph Henzen ... a systemic skeletal disease
10/26/2017. Aging Population = more osteoporosis
 Sandra Scholten, FNP-BC Discuss burden of osteoporosis (OP) and clinical consequences of OP fractures. Define OP and techniques used to assess bone density and quality. Improve awareness, diagnosis, and
Sandra Scholten, FNP-BC Discuss burden of osteoporosis (OP) and clinical consequences of OP fractures. Define OP and techniques used to assess bone density and quality. Improve awareness, diagnosis, and
76 year-old female presents with muscle cramps. Jess Hwang 12/6/12
 76 year-old female presents with muscle cramps Jess Hwang 12/6/12 HPI Worked up for outpatient hypercalcemia Calcium had been 10.3-11.1, PTH ~120 No h/o osteoporosis, CKD, kidney stones Not taking calcium
76 year-old female presents with muscle cramps Jess Hwang 12/6/12 HPI Worked up for outpatient hypercalcemia Calcium had been 10.3-11.1, PTH ~120 No h/o osteoporosis, CKD, kidney stones Not taking calcium
Renal Tubular Acidosis
 1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
1 Renal Tubular Acidosis Mohammad Tariq Ibrahim 6 th Grade Diyala College Of Medicine supervisor DR. Sabah Almaamoory 2 *Renal Tubular Acidosis:- RTA:- is a disease state characterized by a normal anion
TREATMENT OF OSTEOPOROSIS
 TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
GLOSSARY OF TERMS. produced in response to an antigen to bond with and neutralize that antigen / the body's way of destroying foreign invaders
 TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
TERM 24-hour urine acidosis acquired aemia (prefix) albumin alkalosis anemia antibodies antigen autocrine autoimmune basal ganglion bone turnover calcilytic calcimimetic calcitonin Calcitriol Calcium carbonate
20F With Hypocalcemia
 20F With Hypocalcemia Isabel Casimiro, MD PhD * 5/11/17 * has no relevant financial relationships with any commercial interests. How to Approach Hypocalcemia? How to Approach Hypocalcemia? Etiology: Think
20F With Hypocalcemia Isabel Casimiro, MD PhD * 5/11/17 * has no relevant financial relationships with any commercial interests. How to Approach Hypocalcemia? How to Approach Hypocalcemia? Etiology: Think
Vitamin D: Is it a superhero??
 Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
Vitamin D: Is it a superhero?? Dr. Ashraf Abdel Basset Bakr Prof. of Pediatrics 1 2 History of vitamin D discovery Sources of vitamin D and its metabolism 13 Actions of vitamin D 4 Vitamin D deficiency
DISEASES WITH ABNORMAL MATRIX
 DISEASES WITH ABNORMAL MATRIX MSK-1 FOR 2 ND YEAR MEDICAL STUDENTS Dr. Nisreen Abu Shahin CONGENITAL DISEASES WITH ABNORMAL MATRIX OSTEOGENESIS IMPERFECTA (OI): also known as "brittle bone disease" a group
DISEASES WITH ABNORMAL MATRIX MSK-1 FOR 2 ND YEAR MEDICAL STUDENTS Dr. Nisreen Abu Shahin CONGENITAL DISEASES WITH ABNORMAL MATRIX OSTEOGENESIS IMPERFECTA (OI): also known as "brittle bone disease" a group
Osteoporosis. Overview
 v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
Conflict of Interest. Objectives. Learner Outcome
 Foundations of Orthopaedic Nursing Care, Part Four: Metabolic Bone Disease, highlighting Osteoporosis and Paget s Disease Conflict of Interest I hereby certify that, to the best of my knowledge, no aspect
Foundations of Orthopaedic Nursing Care, Part Four: Metabolic Bone Disease, highlighting Osteoporosis and Paget s Disease Conflict of Interest I hereby certify that, to the best of my knowledge, no aspect
Osteoporosis Clinical Guideline. Rheumatology January 2017
 Osteoporosis Clinical Guideline Rheumatology January 2017 Introduction Osteoporosis is a condition of low bone mass leading to an increased risk of low trauma fractures. The prevalence of osteoporosis
Osteoporosis Clinical Guideline Rheumatology January 2017 Introduction Osteoporosis is a condition of low bone mass leading to an increased risk of low trauma fractures. The prevalence of osteoporosis
Primary Hyperparathyroidism
 Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Primary Hyperparathyroidism Copyright Copyright 2019 2019 American American Associa7on Associa7on of Clinical of Clinical Endocrinologists Endocrinologists 1 Primary Hyperparathyroidism In primary hyperparathyroidism
Osteoporosis, Osteomalasia & rickets. Bone disorders
 Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
Osteoporosis, Osteomalasia & rickets Bone disorders Thank You for Your comments Voice--- Ok Lecture too long--- this is in schedule??? More interaction--- I can do that inshalla Slides are crowded--- but
Current Management of Metastatic Bone Disease
 Current Management of Metastatic Bone Disease Evaluation and Medical Management Dr. Sara Rask Head, Medical Oncology Simcoe Muskoka Regional Cancer Centre www.rvh.on.ca Objectives 1. Outline an initial
Current Management of Metastatic Bone Disease Evaluation and Medical Management Dr. Sara Rask Head, Medical Oncology Simcoe Muskoka Regional Cancer Centre www.rvh.on.ca Objectives 1. Outline an initial
PARATHYROID, VITAMIN D AND BONE
 PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
PARATHYROID, VITAMIN D AND BONE G M Kellerman Pathology North Hunter Service 30/01/2015 BIOLOGY OF BONE Bone consists of protein, polysaccharide components and mineral matrix. The mineral is hydroxylapatite,
BARTS ENDOCRINE E-PROTOCOLS CALCIUM DISORDERS AND BONE
 HYPERCALCAEMIA CALCIUM DISORDERS Clinical features to record Symptoms: Thirst, polyuria, nocturia, tiredness, poor concentration, depression, constipation, episodes of renal colic/calculi, hypertension,
HYPERCALCAEMIA CALCIUM DISORDERS Clinical features to record Symptoms: Thirst, polyuria, nocturia, tiredness, poor concentration, depression, constipation, episodes of renal colic/calculi, hypertension,
The Parathyroid Glands
 The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
The Parathyroid Glands Bởi: OpenStaxCollege The parathyroid glands are tiny, round structures usually found embedded in the posterior surface of the thyroid gland ([link]). A thick connective tissue capsule
Download slides:
 Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
Download slides: https://www.tinyurl.com/m67zcnn https://tinyurl.com/kazchbn OSTEOPOROSIS REVIEW AND UPDATE Boca Raton Regional Hospital Internal Medicine Conference 2017 Benjamin Wang, M.D., FRCPC Division
454 Secondary Causes of Osteoporosis Mayo Clin Proc, May 2002, Vol 77 Table 1. Secondary Causes of Osteoporosis Endocrine disorders Acromegaly Adrenal
 Mayo Clin Proc, May 2002, Vol 77 Secondary Causes of Osteoporosis 453 Review Secondary Causes of Osteoporosis LORRAINE A. FITZPATRICK, MD Secondary causes of bone loss are not often considered in patients
Mayo Clin Proc, May 2002, Vol 77 Secondary Causes of Osteoporosis 453 Review Secondary Causes of Osteoporosis LORRAINE A. FITZPATRICK, MD Secondary causes of bone loss are not often considered in patients
DISORDERS OF THE PARATHYROID GLANDS. Mona Fouda Neel MBBS,FRCPEdin.,FACE Professor of medicine and Endocrinology Consultant Endocrinologist
 DISORDERS OF THE PARATHYROID GLANDS Mona Fouda Neel MBBS,FRCPEdin.,FACE Professor of medicine and Endocrinology Consultant Endocrinologist Disorders of the Parathyroid Glands Maintenance of calcium, phosphate
DISORDERS OF THE PARATHYROID GLANDS Mona Fouda Neel MBBS,FRCPEdin.,FACE Professor of medicine and Endocrinology Consultant Endocrinologist Disorders of the Parathyroid Glands Maintenance of calcium, phosphate
Bone Health in the Cancer Patient. Stavroula Otis, M.D. Primary Care and Oncology: Practical Lessons Conference Brea Community Center May 10, 2018
 Bone Health in the Cancer Patient Stavroula Otis, M.D. Primary Care and Oncology: Practical Lessons Conference Brea Community Center May 10, 2018 Overview Healthy bone is in a constant state of remodelling
Bone Health in the Cancer Patient Stavroula Otis, M.D. Primary Care and Oncology: Practical Lessons Conference Brea Community Center May 10, 2018 Overview Healthy bone is in a constant state of remodelling
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary
 Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
Natpara (parathyroid hormone) Prior Authorization with Quantity Limit Program Summary FDA APPROVED INDICATIONS DOSAGE 1 Agent Indication Dosing and Administration Natpara (parathyroid hormone) subcutaneous
OSTEOPOROSIS AND WHAT TO DO AFTER A VERTEBRAL FRACTURE. Lydia Au Geriatrics Ng Teng Fong Hospital
 OSTEOPOROSIS AND WHAT TO DO AFTER A VERTEBRAL FRACTURE Lydia Au Geriatrics Ng Teng Fong Hospital LET S START WITH WHAT YOU WANT TO KNOW AND DO WITH A VERT FRACTURE Vertebral fractures Most common (550K
OSTEOPOROSIS AND WHAT TO DO AFTER A VERTEBRAL FRACTURE Lydia Au Geriatrics Ng Teng Fong Hospital LET S START WITH WHAT YOU WANT TO KNOW AND DO WITH A VERT FRACTURE Vertebral fractures Most common (550K
Osteoporosis. Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective. Old Definition of Osteoporosis
 Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective Dr Dicky T.K. Choy Physician Jockey Club Centre for Osteoporosis Care and Control, CUHK Osteoporosis Global public health
Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective Dr Dicky T.K. Choy Physician Jockey Club Centre for Osteoporosis Care and Control, CUHK Osteoporosis Global public health
