The diagnosis and management of parasellar tumours of the pituitary
|
|
|
- Adela McCormick
- 5 years ago
- Views:
Transcription
1 REVIEW Endocrine-Related Cancer (2008) The diagnosis and management of parasellar tumours of the pituitary Gregory A Kaltsas, Jane Evanson 1, Alexandra Chrisoulidou 2 and Ashley B Grossman 3 Endocrine Unit, Department of Pathophysiology, National University of Athens, Athens, Greece 1 Department of Academic Radiology, St Bartholomew s Hospital, London, UK 2 Department of Endocrinology, Theagenion Hospital, Thessaloniki, Greece 3 Department of Endocrinology, St Bartholomew s Hospital, London EC1A 7BE, UK (Correspondence should be addressed to A B Grossman; a.b.grossman@qmul.ac.uk) Abstract The sellar and parasellar region is an anatomically complex area where a number of neoplastic, inflammatory, infectious, developmental and vascular diseases can develop. Although most sellar lesions are due to pituitary adenomas, a number of other pathologies involving the parasellar region can present in a similar manner. The diagnosis of such lesions involves a multidisciplinary approach, and detailed endocrinological, ophthalmological, neuroimaging, neurological and finally histological studies are required. Correct diagnosis prior to any intervention is essential as the treatment of choice will be different for each disorder, particularly in the case of primary malignant parasellar tumours. The complexity of structures that define the parasellar region can produce a variety of neoplastic processes, the malignant potential of which relies on histological grading. In the majority of parasellar tumours, a multimodal therapeutic approach is frequently necessary including surgery, radiotherapy, primary or adjuvant medical treatment and replacement of apparent endocrine deficits. Disease-specific medical therapies are mandatory in order to prevent recurrence or further tumour growth. This is particularly important as neoplastic lesions of the parasellar region tend to recur after prolonged follow-up, even when optimally treated. Apart from the type of treatment, identification of clinical and radiological features that could predict patients with different prognosis seems necessary in order to identify high-risk patients. Due to their rarity, central registration of parasellar tumours is required in order to be able to provide evidence-based diagnostic and mainly therapeutic approaches. Endocrine-Related Cancer (2008) Introduction The area immediately around the pituitary, the sellar and parasellar region, is an anatomically complex area that represents a crucial crossroads for important adjacent structures (Ruscalleda 2005). While the sellar region has specific anatomical landmarks, the parasellar region is not clearly delineated and includes all the structures that surround the sella turcica (Rennert & Doerfler 2007). Vital structures such as the brain parenchyma, meninges, visual pathways and other cranial nerves, major blood vessels, hypothalamopituitary system (HPS) and bony compartments may be involved. A diversity of clinical symptoms and signs can develop from a number of neoplastic, inflammatory, infectious, developmental and vascular diseases that occupy the parasellar area secondary to the location, size and growth potential of the lesions, and the subsequent damage to specific adjacent vital structures (Freda & Post 1999). Pituitary adenomas are the most common cause of a sellar mass extending to the parasellar region (Freda & Post 1999). However, in w9% of cases, an aetiology other than a pituitary adenoma is encountered, parasellar tumours being the second commonest cause after non-tumorous cystic lesions (Freda et al. 1996). The malignant potential of these tumours may be defined according to the World Health Organization (WHO) classification of tumours of the central nervous system (CNS), which relies on histological criteria: WHO grade I (tumours with low proliferative potential and the possibility of cure following surgical resection), Endocrine-Related Cancer (2008) /08/ q 2008 Society for Endocrinology Printed in Great Britain DOI: /ERC Online version via
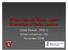
2 G A Kaltsas et al.: Parasellar tumours WHO grade II (infiltrative tumours with low mitotic activity that can recur and progress to higher grades of malignancy), WHO grade III (tumours with histological evidence of malignancy) and WHO grade IV (mitotically active tumours with rapid evolution of disease; Kleihues et al. 1993). The latest version of the WHO classification, including some new histologically identified variants that may have some clinical relevance, has recently been published (Louis et al. 2007). A number of other nonneoplastic lesions, such as inflammatory, granulomatous, infectious and/or vascular pathologies can also involve the parasellar region (Table 1). In this paper, we primarily attempt an overview of the clinical, endocrine and radiological features of Table 1 Classification of parasellar tumours according to malignant potential and other parasellar lesions Malignant parasellar tumours Gliomas Germ cell tumours Primary lymphomas Metastases Supratentorial primitive neuroectodermal tumours (PNET) Ependymoblastomas Potentially malignant parasellar tumours (low-grade malignant tumours) Craniopharyngiomas Chordomas/chondrosarcomas Haemangiopericytomas Langerhans cell histiocytosis (LCH) Benign parasellar tumours Meningiomas (except rare atypical and anaplastic meningiomas) Rathke s cyst Epidermoids/dermoids Hamartomas Paragangliomas Lipomas Neurinomas/Schwannomas Parasellar granular cell tumours Ganglion cell tumours Non-neoplastic pathologies of the parasellar region Granulomatous, infectious and inflammatory lesions Pituitary abscess, bacterial and fungal Tuberculosis Sarcoidosis Wegener s granulomatosis Mucocele (sphenoid) Hypophysitis (lymphocytic, granulomatous, xanthomatous) Tolosa Hunt syndrome Vascular lesions Aneurysms Cavernous sinus thrombosis Pituitary apoplexy Miscallaneous (CSF related) Empty sella syndrome Arachnoid cyst Suprasellar-chiasmatic arachnoiditis neoplastic parasellar tumours, taking into consideration their malignant potential (Table 1). In addition, currently available therapeutic schemes and the longterm prognosis of these tumours will also be discussed. Non-neoplastic parasellar lesions will also be briefly mentioned but not discussed into detail. Anatomical considerations The parasellar region includes, laterally, the dural walls of the cavernous sinus, a multi-lobulated venous structure containing the intracavernous portion of the internal carotid artery, cranial nerves III, IV, VI and the V 1 and V 2 branches of the trigeminal nerve (Smith 2005; Fig. 1). The relationships of the cavernous sinus are: inferiorly with the basisphenoid and sphenoid sinus; superiorly, the diaphragma sella, with the suprasellar subarachnoid spaces containing the optic nerves and chiasm, hypothalamus, tuber cinereum and anterior third ventricle (Ruscalleda 2005). The nasopharynx and the medial aspects of the temporal lobes are also closely related to the parasellar region; in addition, embryonal remnants can also be found contributing further to the diversity of the processes that are involved in delineating the anatomy of this region (Smith 2005). Clinical presentation Non-pituitary adenomatous parasellar lesions do not present with hypersecretory syndromes but rather with hypopituitarism or symptoms of mass effect due to compression of nearby vital surrounding structures, the Figure 1 Sagittal enhanced T 1 -weighted image of a hypothalamic glioma. This is partially cystic, partially solid and involves the chiasm and the hypothalamus
3 Endocrine-Related Cancer (2008) severity of which depends on the location, size and growth potential of the tumours (Glezer et al. 2008). Visual loss is a common presenting complaint due to the proximity of tumours to the optic nerves, chiasm and optic tracts. Headache develops either as a consequence of increased intracranial pressure (IP), distortion of the diaphragma or irritation of the parasellar dura (Freda & Post 1999). As parasellar tumours commonly originate or infiltrate structures within close proximity to the cranial nerves traversing through the cavernous sinus, cranial nerve abnormalities develop in w25% of cases (Jagannathan et al. 2007). Hypothalamic tumours in children may produce the diencephalic syndrome manifest as wasting, poor development and sexual immaturity, whereas in adults it may lead to disruption of the control of appetite and cause severe obesity or starvation (Freda & Post 1999). Involvement of the hypothalamus and pituitary leads to complete or partial pituitary hormonal deficiencies; hyperprolactinaemia may also develop secondary to stalk compression (Glezer et al. 2008). Diabetes insipidus (DI) is a common finding in parasellar tumours and indicates that the lesion is unlikely to be a pituitary adenoma; however, it cannot reliably distinguish among the various parasellar tumours (Freda & Post 1999). Imaging Radiological imaging of the parasellar region is challenging since the sella is a small volume region in close proximity to many complex structures (Ruscalleda 2005). Both thin-section computerised tomography (CT) and magnetic resonance imaging (MRI) play an important role in the anatomical delineation of lesions in this area (Boardman et al. 2008). MRI is the modality of choice providing multiplanar high-contrast images, whereas CT has a complementary role in delineating bony destruction and the visualisation of calcification (Rennert & Doerfler 2007). Conventional radiology is no longer in use, whereas digital subtraction angiography has been largely replaced by the continuous improvement in MR and CT angiographies (Rennert & Doerfler 2007). Although the radiological features of parasellar tumours have many similarities, some may have distinctive findings (Chong & Newton 1993, Freda & Post 1999, Ruscalleda 2005, Smith 2005; Table 2). However, the differential diagnosis among the various types of tumours remains difficult using currently available methods of morphological imaging. Diagnosis In formulating a management plan, histological confirmation is usually required unless there are lesion-specific clinical, endocrine and/or radiological features. Existing methods of skull base biopsy in the anatomically critical parasellar region include either open skull base approaches or image-guided needle biopsy (Day 2003, Samandouras et al. 2005). Imageguided techniques may help in diagnosis, but can be time-consuming and cannot reliably avoid surrounding critical neurovascular structures; in selected patients endoscopic transnasal biopsy can be applied (Frighetto et al. 2003, Samandouras et al. 2005). However, the use of such methods should be weighed along with the potential morbidity and mortality of the procedures when the risk of inducing damage to a vital structure is high, while the expected benefit from obtaining the correct diagnosis may be questionable. Therapy Surgery remains the treatment of choice for benign tumours and malignant tumours that are not responsive to other forms of treatment, and/or when surgical debulking is essential (Day 2003, Glezer et al. 2008). Surgical therapy Parasellar tumours usually have irregular margins and adhere to vital neurovascular structures, and thus do not allow a complete resection without the danger of affecting critical brain areas (Couldwell et al. 2004). Resection is attempted by craniotomy and/or transsphenoidally (TSS), particularly for smaller tumours approachable through the sella (Baskin & Wilson 1986, Honegger et al. 1992). For massive lesions, a two-stage removal procedure may be necessary; initially TSS debulking followed by craniotomy later. This approach may allow residual tumour to descend inferiorly, facilitating further resection (Maira et al. 1995). Recently, the development of advanced cranial base TSS approaches has facilitated the exposure of basal lesions by the removal of osseous structures, minimising brain retraction and providing safe alternatives when assessing lesions involving the tuberculum sella, suprasellar region, cavernous sinus or clivus (Couldwell et al. 2004). The TSS route can also be used for midline lesions without significant lateral extension (Day 2003). In cases of hydrocephalus, resection may be achieved following decompression of the ventricles and stabilisation of the clinical status of the patient. In the presence of large cystic lesions, as with craniopharyngiomas, fluid aspiration can be 887
4 G A Kaltsas et al.: Parasellar tumours Table 2 Imaging characteristics of parasellar tumours Diagnosis Malignant tumours Gliomas (hypothalamic or optic pathway) Germ cell tumours Metastases Lymphoma Plasmatocytoma Potentially malignant tumours Craniopharyngiomas Chordomas chondrosarcomas Haemangiopericytomas Langerhans cell histiocytosis Mostly benign tumours Meningioma Epidermoid cyst Dermoid cyst Hamartoma Schwannoma Rathke s cyst CT and/or MRI characteristics On CT hypo/isodense pre-contrast mass. Variable enhancement on post-contrast images Rarely calcifications, haemorrhages solid lesions. Occasionally small cystic or necrotic components in large legions. On MRI hypointense on T 1 -weighted images and hyperintense on T 2 images. Variable enhancement following contrast administration On CT, well-delineated masses, usually hyperdense lesions. Most cases show strong homogenous enhancement. On MRI, isointense on T 1 -weighted images and iso- to hyperintense on T 2 -weighted images On MRI, signal intensity varies depending on the primary tumour. Generally hypointense on T 1 -weighted images and hyperintense on T 2 -weighted images On MRI, slight hypointensity on both T 1 - and T 2 -weighted images On MRI, slight hypointensity on both T 1 - and T 2 -weighted images Calcifications occur in up to 80%, best depicted by CT. Cysts are present in the majority of craniopharyngiomas that tend to predominate in children containing highly proteinaceous fluid. The fluid is usually very bright on pre-contrast T 1 -weighted MRI. In adults the solid components are larger and the cysts tend to be small or multiloculated. The solid portions and cyst walls enhance usually heterogeneously On CT, bone destroying mass, centred on the spheno-occipital synchondrosis with occasional intratumoural calcifications. MR images show a heterogeneous mass with internal septations and heterogeneous enhancement. Chordomas are typically midline lesions On MRI, hypointense lesions on T 1 -weighted images and heterogeneously hyperintense on T 2 -weighted images On MRI uniform thickening of the pituitary stalk with homogenous enhancement of the hypothalamic stalk. Occasionally, solitary nodules may develop in the HP region On CT, isodense to slightly hyperdense with dense homogenous enhancement. Calcification is seen in 20 50%. On MRI appear isointense in both T 1 - and T 2 -weighted images although T 2 signal intensity may be more variable. Differ from pituitary adenomas due to differential uniform enhancing pattern. Majority exhibit broad dural attachment and show a dural tail on post-contrast imaging accompanied by bony hyperostosis and normal sellar dimension On CT lobulated mass with areas of calcification and attenuation values similar to CSF. On MRI, similar characteristics to CSF without post-contrast enhancement but bright on diffusion scans On CT, round or lobulated with negative density values and foci of calcification. There is no contrast enhancement or surrounding oedema. On T 1 -weighted images, high signal due to lipid content Pedunculated hypothalamic mass, isodense on CT and MRI, relatively to grey matter. It does not calcify or enhance following contrast administration On CT they appear as contrast enhancing masses that follow the course of involved nerves. On MRI they appear as well-defined masses isointense on T 1 -weighted images with strong contrast enhancement; on T 2 -weighted images appear isointense to hyperintense On MRI appear as discrete cystic lesions with variable signal intensity. They appear to have the density of CSF, with low intensity on T 1 and high intensity on T 2 -weighted images. Calcification of the cyst is usually absent and this may help differentiate them from craniopharyngiomas. Contrast enhancement is rare and when occurs it is confined to the cyst wall Data derived from the following references: FitzPatrick et al. (1999), Freda & Post (1999), Zee et al. (2003), Ruscalleda (2005), Smith (2005), Karavitaki et al. (2006), Rennert & Doerfler (2007), Glezer et al. (2008) and Jalali et al. (2008)
5 Endocrine-Related Cancer (2008) applied first as may provide relief of the obstruction and facilitate further tumour removal (Karavitaki et al. 2006). Radiotherapy (RT) Conventional RT has traditionally been used either as primary treatment or as a way to prevent further tumour growth or recurrence (Brada & Cruickshank 1999, Perks et al. 1999). More sophisticated radiotherapeutic techniques have recently been introduced. Stereotactic radiosurgery delivers a single fraction of high-dose ionising radiation on mapped targets, keeping the exposure of adjuvant tissues to a minimum and allowing for the delivery of maximum tolerated dose of between 10 and 15 Gy (Giller & Berger 2005). Stereotactic RT combines the accurate focal delivery of stereotactic radiosurgery with the radiobiological advances of fractionation; compared with conventional RT, it minimises long-term toxicities by offering optimal sparing to surrounding tissue (Tarbell et al. 1994). Robotically controlled frameless radiosurgery has also been developed and studies assessing its efficacy are awaited (Giller et al. 2005). In general, RT seems to be a valuable asset in the treatment of these tumours, albeit with potential adverse effects to nearby tissue and the HPS (Brada & Cruickshank 1999). Medical therapy Chemotherapy remains the primary therapy for responsive malignant tumours in either a neoadjuvant or adjuvant setting following surgery and/or RT. Patients with infrequently curable or unresectable tumours should be considered candidates for clinical trials that evaluate interstitial brachytherapy, radiosensitisers, hyperthermia, or intraoperative radiation therapy in conjunction with external RT to improve local tumour control. Such patients are also candidates for studies that evaluate new drugs and biological response modifiers following RT. Therapy of established or evolving specific pituitary and hypothalamic hormonal deficits should be detected and adequately treated (Lamberts et al. 1998). Optimum hormonal replacement therapy should be aimed for, although even with replacement therapy parasellar tumours, particularly craniopharyngiomas, have a worse prognosis compared with pituitary adenomas (Tomlinson et al. 2001). Follow-up Prognosis is dependent on patient status, comorbid conditions, tumour size and extension, and the precise histopathology. Children and adolescents should have careful monitoring of height, weight and pubertal status, while a dedicated neuroendocrine team should screen patients for endocrine and neuropsychological deficits at regular intervals. Post-operative imaging should be performed within 3 months of treatment and generally at 6 and 12 months to evaluate tumour recurrence or presence of residual tumour. Malignant tumours of the parasellar region Gliomas Gliomas may arise in the hypothalamus, optic chiasm, nerve or tract (Zee et al. 2003; Fig. 1). The main histopathological subtype is the pilocytic astrocytoma (WHO grade I), which is a low-grade malignant lesion associated occasionally with neurofibromatosis type 1 (NF1; Zee et al. 2003). In this instance, lesions can be multiple including optic nerve gliomas, low-grade brain stem gliomas and basal ganglia non-neoplastic hamartomas (Zee et al. 2003). The remainder of hypothalamic/optic chiasm lesions are diffuse astrocytomas (WHO grade II), representing 35% of all astrocytic brain tumours (Smith 2005). This type of tumour typically affects young adults and has a tendency for malignant progression to anaplastic astrocytoma and, very rarely, glioblastoma (WHO grades III VI). Hypothalamic/chiasmatic astrocytomas are primarily seen in adulthood presenting with impaired vision and retro orbital pain (Black & Pikul 1999). In children, they may present with visual loss, headache, proptosis and the diencephalic syndrome (Glezer et al. 2008). On imaging, hypothalamic/ chiasmal gliomas are usually large suprasellar masses, infiltrating the brain and third ventricle, which enhance homogeneously; rarely, there is necrosis, haemorrhage or calcification (FitzPatrick et al. 1999). There is uncertainty as to the optimum therapy, and many can be simply observed; obviously, visual loss will determine the need for surgery. The mean survival time after surgical intervention is between 6 and 8 years, with considerable individual variation (Kitange et al. 2003). Optic pathway gliomas generally behave benignly, with very slow growth; however, tumours around the chiasm/hypothalamus can be more aggressive, exhibiting a 50% 5-year survival (Kitange et al. 2003). Gliomas can also develop in the brainstem and extend into the parasellar region (Packer 2000, Guillamo et al. 2001). Diffuse intrinsic low-grade glioma (WHO grade II) is the most prominent type, whereas purely malignant brainstem glioma (WHO grades III VI) occurs in 31% of cases (Guillamo et al
6 G A Kaltsas et al.: Parasellar tumours 2001). The median survival of low-grade gliomas is 7.3 years whereas that of high-grade gliomas was 11.2 months (Guillamo et al. 2001). Stereotactic biopsy has been reported to provide the diagnosis with minimal morbidity (Packer 2000). Although glucocorticoids and irradiation may temporarily improve symptoms, there seems to be no long-term benefit (Recinos et al. 2007). Occasionally, mixed gliomas may occur, for which temozolomide, an oral derivative of dacarbazine, may be useful therapy. Clinical improvement has been noted in 51% of patients, with a radiological response rate of 31% (Hoang-Xuan et al. 2004). Germ cell tumours (GCTs) Primary intracranial GCTs are neoplasms most commonly present in the first two decades of life (Janmohamed et al. 2002; Fig. 2). Like other extragonadal GCTs, CNS variants develop around the midline, with 80% arising around the third ventricle, mostly in the region of the pineal gland, followed by the suprasellar compartment and anterior hypothalamic regions (Jennings et al. 1985). Synchronous GCTs at both these sites are found at w5 10% (Jennings et al. 1985). Germinomatous GCT (GGCT) are the most exquisitely radiosensitive, whereas non-ggct (NGGCT), comprising choriocarcinoma, teratoma, embryonal sinus (yolk sac) tumour and embryonal carcinoma, have a poorer overall response to treatment and a worse prognosis (Allen et al.1987, Balmaceda et al. 1996). Non-GCT can also contain germinomatous elements (Calaminus et al.2005). Pineal GCT classically give rise to raised IP, hydrocephalus and Parinaud s syndrome, whereas suprasellar GCT typically present with cranial DI, hypopituitarism and visual disturbance, and may lead to dissemination via the CSF (Legido et al. Figure 2 Sagittal enhanced T 1 -weighted image of a germinoma with both a suprasellar and pineal enhancing mass lesions. 1989, Janmohamed et al. 2002). Diagnosis is established by histology but a subgroup can be diagnosed on the basis of elevation of specific tumour markers (Calaminus et al. 2005), or typical clinical and radiological features. Yolk sac tumours secrete a-fetoprotein and choriocarcinomas b-human chorionic gonadotrophin (b-hcg) that can be detected in the serum and/or CSF (Calaminus et al.2005). Approximately 10% of germinomas may contain syncytiotrophoblastic elements and secrete b-hcg (Matsutani et al. 1997). Germinomas appear as large lesions typically slight hyperdense on CT that enhance after contrast medium administration (FitzPatrick et al. 1999). On MRI, they appear isointense to brain on T 1 -weighted images and isointense-slightly hyperintense on T 2 -weighted images (Rennert & Doerfler 2007). Although histological confirmation remains the gold standard diagnostic method, the combination of tumour marker estimation and imaging modalities can be used in secretory GCT (Packer et al. 2000, Calaminus et al. 2005). This diagnostic tool is underscored by the fact that several patients with parasellar GCT have developed surgical procedurerelated complications (Calaminus et al. 2005). It is therefore important to avoid aggressive surgical intervention and develop treatment planning on noninvasive modalities, and only if in doubt to proceed to a biopsy (Janmohamed et al. 2002, Calaminus et al. 2005). In cases of non-secretory GCT histological diagnosis is helpful, but again this may be associated with considerable morbidity (Packer et al. 2000). A biopsy can usually be obtained with using stereotactic neurosurgery or neuroendoscopy; occasionally, the small tissue fragments obtained can result in histological specimens that are not representative of the entire lesion (Packer et al. 2000). Treatment of GCT involves irradiation to the tumour bed to obtain local control, craniospinal irradiation to cover leptomeningeal tumour spread, and chemotherapy to eliminate leptomeningeal and systemic tumour dissemination (Gobel et al. 2001). When a pre-operative diagnosis of a GCT has been obtained, then surgical exploration is not necessary as these tumours are highly sensitive to chemotherapy and RT (Gobel et al. 2001, Janmohamed et al. 2002). Platinum-based chemotherapy has proven to be highly effective in non-seminomatous GCT (Allen 1987, Balmaceda et al.1996) A cumulative dose of cis-platin of over 300 mg/m 2 and tumour bed irradiation dose of w50 54 Gy, together with craniospinal irradiation, has a synergistic effect and achieves a long-term relapse-free survival between 60 and 70% (Janmohamed et al. 2002, Calaminus et al. 2005). Neoadjuvant chemotherapy and delayed residual tumour resection may be more appropriate 890
7 Endocrine-Related Cancer (2008) than primary tumour resection followed by the same chemotherapy (Janmohamed et al. 2002). The presence of CNS dissemination warrants more aggressive treatment, such as high-dose chemotherapy with stem-cell transplantation (Guillamo et al. 2001), or intraventicular treatment (Osuka et al. 2007). Two recent studies in children and adults have evaluated long-term treatment sequelae, revealing mainly impairment of endocrine function, and rare visual, hearing and neurological deficits (Legido et al. 1989). In general, our own approach has been to initiate treatment with chemotherapy in lesions that appear to be characteristic of germinomas, even in the absence of positive tumour markers, and then to re-image several weeks after initial chemotherapy; rapid shrinkage of the tumour will usually be confirmatory of the diagnosis, and the treatment completed. Primary parasellar lymphomas Primary CNS lymphomas account for less than 2% of all intracranial lesions (Fine & Mayer 1993; Fig. 3). By definition, these tumours are extranodal and arise primarily in the craniospinal axis, and are distinct from systemic lymphomas that secondarily metastasise to the CNS (Megan Ogilvie et al. 2005, Liu et al. 2007). Although initially described in immunocompromised patients, a significant increase in the incidence of such lesions has recently been documented in immunocompetent patients (Corn et al. 2000). Lymphomas involving the sellar/parasellar region are even rarer, representing less than 1% of all cases in a large cohort of patients who Figure 3 Coronal enhanced T 1 -weighted image of lymphoma. There is abnormal dural enhancement of both cavernous sinuses extending to involve the pituitary gland itself and with slight thickening of the stalk. underwent TSS (Freda & Post 1999). Recently, the number of primary parasellar lymphomas has substantially increased, the majority being of B-cell origin and only a minority of T-cell origin; a case of a NK/T-cell lymphoma has also been reported (Liu et al. 2007). Approximately 18 patients with sellar/parasellar lymphomas have been described with a mean age at presentation of 55.5 years and male/female ratio of 13:5 (Fine & Mayer 1993, Liu et al. 2007). Endocrine abnormalities are relatively common, with 72% of patients exhibiting anterior, and 39% posterior, pituitary deficiencies respectively (Megan Ogilvie et al. 2005, Liu et al. 2007). In a recent review systemic symptoms, such as fever of unknown origin, were the presenting symptoms in 22% of patients, whereas the commonest presenting compressive symptoms were headache (56%), diplopia (39%) and visual field defects (28%) respectively (Liu et al. 2007). MRI may demonstrate enhancing parasellar masses with diffuse enlargement of the pituitary (94%), suprasellar extension (44%), cavernous sinus extension (39%) and stalk thickening (22%; Liu et al. 2007). Lymphomas usually appear isoor hyperdense on CT scanning and isointense on T 1 - weighted and slightly hypointense on T 2 -weighted images and enhance homogeneously after gadolinium administration (Buhring et al. 2001). The diagnosis of primary lymphomas is established histologically and their treatment includes surgery, chemotherapy and RT according to established protocols (Megan Ogilvie et al. 2005, Glezer et al. 2008). Metastases to the parasellar region Metastases to the parasellar region are relatively rare, found in less than 1% of patients undergoing TSS for sellar/parasellar lesions (Komninos et al. 2004). However, autopsy series have revealed that metastases to the region comprise between 0.14 and 28.1% of brain metastases, the most common primaries being breast and lung cancer in women and men respectively; however, virtually any neoplasm can metastasise to the pituitary (Chiang et al. 1990, Sioutos et al. 1996, Megan Ogilvie et al. 2005). In a significant number of patients, the parasellar area and the pituitary gland may appear macroscopically normal besides the presence of metastases that remain clinically non-significant (Ito et al. 2001). Most cases are found in the sixth seventh decade of life as part of a generalised metastatic spread, commonly associated with multiple, particularly osseous metastases (Chiang et al. 1990, Sioutos et al. 1996). However, they can occur in young patients, and very occasionally are the first manifestation of an occult cancer or the only site of metastasis (Sioutos et al.1996)
8 G A Kaltsas et al.: Parasellar tumours Symptoms of mass effect and cranial nerve palsies are the most frequent symptoms; when metastatic lesions involve the pituitary gland, hormonal deficiencies, particularly DI, develop (Sioutos et al.1996, Komninos et al. 2004). Although clinically indistinguishable from other lesions involving the area, specific clinical settings may point to the diagnosis (Komninos et al. 2004). The rapidity of development of symptoms of mass effect, particularly ophthalmoplegia secondary to VI nerve involvement, in association with the sudden onset of DI in patients over 50 years, strongly suggests the presence of metastases irrespective of a history of malignancy (Ruelle et al. 1992, Sioutos et al. 1996, Morita et al. 1998). Although not specific, radiology can help identify parasellar metastases in the presence of other brain metastases and/or rapidly growing lesions; involvement of the infundibular recess favours a metastatic lesion (Morita et al.1998, Komninos et al.2004). In the absence of a primary and/or other metastatic lesions, confirmation of the diagnosis relies on histology (Chiang et al.1990). Treatment is mainly palliative and depends on the symptoms and the extent of systemic disease (Morita et al. 1998). Due to the invasive, vascular and haemorrhagic nature of the lesions, surgical excision is not usually possible (Sioutos et al. 1996). However, surgical debulking may offer improvement of symptoms of mass effect; this should be followed by local radiation, systemic chemotherapy and adequate hormonal substitution. Radiosurgery is sometimes a useful alternative, particularly for previously irradiated regions, and for smaller lesions (diameter!30 mm). The overall prognosis is poor, with a median survival of less than 2 years (Laigle-Donadey et al.2005). Supratentorial primitive neuroectodermal tumour is an embryonal tumour (WHO grade IV) of the cerebrum or suprasellar region composed of undifferentiated or poorly differentiated neuroepithelial cells, which have the capacity for differentiation along neuronal, astrocytic, ependymal, muscular or melanocytic lines (Ohba et al. 2008). Synonyms include cerebral medulloblastoma, cerebral neuroblastoma, cerebral ganglioneuroblastoma and blue tumour. This rare tumour occurs mainly in children with an overall 5-year survival rate of 34% (Ohba et al. 2008). Ependymoblastoma is a rare, malignant, embryonal brain tumour (WHO grade IV) that occurs in neonates and young children. Ependymoblastomas are often large and supratentorial and generally relate to the ventricles, though they can occur in the parasellar region (Matthay et al. 2003). These types of tumours grow rapidly, with craniospinal dissemination, and have a fatal outcome within 6 12 months of diagnosis (Matthay et al. 2003). Potentially malignant parasellar lesions Craniopharyngiomas Craniopharyngiomas are rare epithelial tumours that arise along the pathway of the craniopharyngeal duct (Bunin et al. 1998; Figs 4 and 5). They account for 2 5% of all primary intracranial neoplasms and follow a bimodal age distribution with a peak incidence rate in children and adults between the ages of 5 and 14 and 50 and 74 years respectively (Bunin et al. 1998). The majority show a suprasellar component (94 95%), and may extend into the anterior, middle or posterior fossa (Petito et al. 1976). Tumours can be solid (1 16%), but most are cystic or mixed (84 99%); cysts may be multiloculated and contain liquid that has high content of membrane lipids and cytokeratins (Karavitaki et al. 2006). Despite their benign histological appearance (WHO grade I), their infiltrative tendency into critical parasellar structures and aggressive behaviour, even after apparently successful treatment, heralds a significant morbidity and mortality (Karavitaki et al. 2006). Cases of malignant transformation have also been described, for which the role of previous RT has not been discounted (Nelson et al. 1988). There are two primary histological subtypes: the adamantinous and Figure 4 Sagittal unenhanced T 1 -weighted image of a craniopharyngioma. The mass is inseparable from the chiasm and hypothalamus and is predominantly of low T 1 signal suggesting a cystic mass, although without a high lipid content
9 Endocrine-Related Cancer (2008) Figure 5 Sagittal enhanced T 1 -weighted image of a solidly enhancing craniopharyngioma. This mass is inseparable from the hypothalamus and chiasm. There is an area of low signal within the mass representing calcification (confirmed on CT). the papillary, but transitional or mixed forms have also been recognised (Zhang et al. 2002). The adamantinous subtype is the most common and bears some similarity to the adamantinoma of the jaw (Karavitaki et al. 2006), accounting for the calcification and the development of teeth encountered particularly in children (Petito et al. 1976). Adamantinous craniopharyngiomas tend to adhere to the surrounding brain tissue, often making complete surgical resection impossible (Petito et al. 1976). The papillary variety, mostly found in adults, is well circumscribed and shows less infiltration to adjacent tissues (Karavitaki et al. 2006). Although, headaches, nausea/vomiting, papillo-oedema, cranial nerve palsies and hydrocephalus are more frequent in children, a large series found no differences when compared the presenting manifestations among children and adults (Karavitaki et al. 2006). Spontaneous rupture of cystic craniopharyngioma is rare, but when it occurs can cause chemical ventriculitis and meningitis (Zee et al. 2003). Endocrine dysfunction in children manifests as growth failure in 93% or delayed sexual development in w20% (Freda & Post 1999). Many adults present with a variety of anterior pituitary hormone deficiencies and 23% develop DI (Freda & Post 1999). CT is the ideal modality for the evaluation of the bony anatomy, identification of calcification and in distinguishing the solid and cystic components of the tumour (Pusey et al. 1987). Pre- and post-contrast enhanced images identify the cystic lesions as a non-enhancing areas of low attenuation; the solid component and the cystic capsule appear as contrast-enhancing areas (Pusey et al. 1987). MRI following contrast enhancement offers valuable topographic and structural analysis (Karavitaki et al. 2006; Table 2). Radical surgery may be successful in selected tumours; however, when surgical removal was substantiated with radiological confirmation, complete removal was accomplished in 18 84% of cases, clearly a wide range (Hald et al. 1994). Post-operative RT following either complete or incomplete tumour removal is associated with significantly decreased recurrence rate; RT alone provides 10-year recurrence rates between 0 and 23% (Rajan et al. 1997). Although the optimum total dose or fractionated protocols have not been established, it seems that recurrences are fewer with total doses above 54 Gy (Karavitaki et al. 2006). Recurrent tumours develop at a mean interval between 1 and 4.3 years, but recurrences as late as 26 years have been described (Coke et al. 1998); such tumours exhibit higher microvessel density values (Vidal et al. 2002), and chromosomal aberrations (Lefranc et al. 2003). Stereotactic radiosurgery is used for well-defined residual tumour tissue after surgery or for the treatment of small solid recurrent tumours, especially after failure of conventional RT (Suh & Gupta 2006). In large cystic portions, multimodality approaches with installation of radioisotopes or bleomycin may provide further benefits (Karavitaki et al. 2006). Recurring tumours and those that have undergone malignant transformation have been treated with systemic chemotherapy and interferon-a, albeit with short-lived results (Karavitaki et al. 2006). However, the treatment for aggressive tumours remains to be assessed by trials including large number of patients with adequate follow-up. In general, our own approach has been to attempt surgical removal, TSS where possible, but not to be radical where this may in any way compromise the hypothalamus; this would generally be followed by standard fractionated RT. Chordomas and chondrosarcomas Approximately 10% of non-pituitary parasellar lesions are cartilaginous, originating from the primitive notochord in the skull base, chordomas being more frequent than chondrosarcomas (Allan et al. 2001; Fig. 6). These are slowly growing tumours presenting with visual complaints, mainly diplopia, whereas a third of patients complain of headache (Korten et al. 1998). Less common presentations include dizziness, tinnitus, facial sensory deficits, ataxia and hemiparesis. Both tumours are associated with extensive bone 893
10 G A Kaltsas et al.: Parasellar tumours Figure 6 Coronal enhanced T 1 -weighted image of a chondrosarcoma. This is an enhancing mass involving the left side of the sella and the cavernous sinus, but arising from the skull base just off midline. destruction (Meyers et al. 1992) but significant endocrinopathy is unusual, although anterior pituitary deficiencies may be encountered, particularly with chordomas (Allan et al. 2001). Following the establishment of clearly defined histopathological criteria, a distinction can be made as both tumours are positive for S-100 protein but, unlike chordomas, chondrosarcomas are negative for cytokeratin markers (CAM 5 2) and epithelial membrane antigens (Salisbury & Isaacson 1986). Intracranial chordomas are most frequently seen around the third decade and in w10 15% can be intradural (Allan et al. 2001). Chordomas can reach considerable size at the time of diagnosis and patients may develop neck pain and nasopharyngeal obstruction, and some tumours may progress to malignant transformation (Rennert & Doerfler 2007). These tumours can extend along the entire skull base causing destruction of the sella instead of the ballooning often seen in pituitary adenomas (Glezer et al. 2008). Bone destruction and calcification occur in 50% of cases and are better seen on CT; on MRI they appear heterogeneously hyperintense on T 2 - weighted images and show marked contrast enhancement (Rennert & Doerfler 2007). Less than 200 cases of intracranial chondrosarcomas have been described (Korten et al. 1998). These malignant tumours (WHO grades II III) occur more commonly in the axial part of the skeleton, representing less than 5% of skull base tumours with w75% arising in the parasellar region (Kunanandam & Gooding 1995). Chondrosarcomas arise off the midline at the suture line, unlike chordomas that arise from the clivus in the midline. Radiological examination almost always reveals bone destruction and variable degrees of calcification on CT, involvement of the neural and vascular structures on MRI, and mostly hypovascularity on angiography (Korten et al. 1998). Occasionally, cyst-like hypodense centres secondary to necrosis can be found (Cohen-Gadol et al. 2003). Although chondrosarcomas rarely metastasise outside the skull they tend to have a better 5-year survival rate compared with chordomas, they expand locally and compress adjacent structures (Rosenberg et al. 1994). Surgery is the treatment of choice for both tumours; however, due to bone invasiveness, total excision is generally not possible (Glezer et al. 2008). Given the importance of residual tumour volume as a prognostic indicator, adjacent therapy is frequently employed (Allan et al. 2001). Standard external RT has been disappointing in achieving local control although most of the reported cases refer to chordomas, but radiosurgery may be more effective (Allan et al. 2001). Although a sustained response to the combination of ifosfamide and doxorubicin in a case of recurrent chondrosarcoma has been described, in most cases chemotherapy fails (La Rocca et al. 1999). Haemangiopericytomas Haemangiopericytomas are rare tumours accounting for less than 1% of all intracranial tumours (Glezer et al. 2008, Jalali et al. 2008). Although the majority are supratentorial, parasagittal or falcine, they can rarely arise in the sellar/parasellar region with less than ten cases reported (Jalali et al. 2008). These tumours are aggressive and highly vascular with numerous penetrating vessels; although previously considered as a subtype of angioblastic meningioma, they represent distinctive mesenchymal neoplasms arising from pericytes (Stout & Murray 1942). Besides the absence of firmly established histological criteria for grading haemangiopericytomas, they appear to correspond to WHO grades II III (Kleihues et al. 1993). Most patients present in middle aged with visual field defects, headaches and rarely symptoms of endocrine dysfunction; a case of acromegaly due to a GHRHsecreting haemangiopericytoma has been described (Yokota et al. 1985). Surgery followed by RT is the standard treatment; however, as haemapericytomas are highly vascular and tend to bleed profusely, it is critical that the neurosurgeon bases his approach on a reasonable pre-operative diagnosis (Mena et al. 1991, Suh & Gupta 2006). Local tumour recurrence following treatment is common, and late widespread metastasis can occur (Jalali et al. 2008). In two large 894
11 Endocrine-Related Cancer (2008) series haemangiopericytomas recurred in 91 and 85% after 15 years (Mena et al. 1991, Jalali et al. 2008). Cystic and necrotic areas, haemorrhage and prominent vascular channels contribute to the heterogeneity in signal intensity (Zee et al. 2003). Langerhans cell histiocytosis (LCH) LCH is a rare disease characterised by the clonal accumulation and/or proliferation of specific dendritic cells and in this manner represents a neoplastic disorder (Arceci 1999; Fig. 7). LCH shows a particular predilection for involvement of the HPS leading to DI and/or anterior pituitary dysfunction (Arceci 1999, Makras et al. 2007), but can virtually involve any organ such as bone, lung, skin, liver, spleen, lymph nodes and bone marrow (Makras et al. 2007). Making an early and accurate diagnosis is important as multisystem LCH is associated with a 20% mortality rate, and 50% of those who survive develop at least one permanent consequence (Makras et al. 2007). Although there is no specific MRI appearance of HPS LCH, almost all patients with LCH-induced DI demonstrate loss of the physiologic intense signal bright spot of the posterior pituitary; other common MRI findings are infundibular enlargement, and/or the presence of hypothalamic mass lesions (Kaltsas et al. 2000). In cases where a precise diagnosis cannot be obtained histological diagnosis from the parasellar pathology may be required (Kaltsas et al. 2000). Figure 7 Coronal enhanced T 1 -weighted image of Langerhans cell histiocytosis. There is diffuse enlargement and enhancement of both cavernous sinuses. The pituitary gland is bulky, although the stalk is not thickened. The combination of vinblastine with steroids is the most frequently used initial therapy of LCH involving the CNS and for multisystem disease (Arico et al. 2003). Although etoposide was initially extensively used, it is not used any long due to its associated high risk for the development of leukaemia (Arico et al. 2003). The purine analogue cladribine (2-- chlorodeoxyadenosine, 2-CdA) has been shown to be effective for patients with recurrent and/or disseminated disease (Makras et al. 2007). RT, at doses up to 25 Gy, has been used in patients with endocrine deficiencies and radiological involvement of the parasellar region with partial or temporary radiological improvement (Arico et al. 2003). Mainly benign lesions Meningiomas Meningiomas (WHO grade I) are the most common non-glial primary brain tumour comprising 15% of primary brain tumours with a peak incidence between 40 and 70 years (Zee et al. 2003; Figs 8 and 9). Tumours arise from the diaphragma sella, tuberculum sella, medial lesser wing of sphenoid, anterior clinoid, clivus cavernous sinus or optic nerve sheath (Smith 2005). In w10 15% of cases, meningiomas arise from the parasellar region and represent the commonest tumour of that region after pituitary adenomas; rarely, they occur entirely within the sella mimicking a pituitary adenoma (FitzPatrick et al. 1999). There is a strong association between meningiomas, NF (multiple tumours) and ionising radiation, depending on the dose applied (Hartmann et al. 2006). The clinical presentation is usually with visual disturbance and occasionally endocrine dysfunction with mildly raised prolactin levels (Freda & Post 1999). The visual field defects vary and depend on the location of the tumour; meningiomas may increase in size during pregnancy and then become symptomatic (Freda & Post 1999). Atypical (WHO grade II) meningiomas may develop in 4 7%, whereas anaplastic tumours (WHO grade III) are seen in 1 2.8% of cases (Hartmann et al. 2006). However, malignant behaviour, although very rare, may occur with any grade of meningioma (Bruna et al. 2007, Ko et al. 2007). Imaging features of meningiomas frequently allow pre-operative diagnosis, distinguishing them from other parasellar tumours (Smith 2005). Lesions arise from the dura and have a broad attachment to the dura or fill and expand the cavernous sinus. There may be a linear, enhancing dural tail extending along the dura away from the lesion. Bone reaction, with bone thickening and sclerosis, or expansion of the sphenoid 895
12 G A Kaltsas et al.: Parasellar tumours surgical excision, grade I tumours recur in 7 20%, whereas atypical and anaplastic recur in 39 40% and 50 78% respectively (Bruna et al. 2007, Ko et al. 2007, Nakane et al. 2007). Surgery and RT is used in selected cases, such as for patients with known or suspected residual disease or with recurrence after previous surgery, whereas radiation alone is used in patients with unresectable tumours (Freda & Post 1999, Aghi & Barker 2006). The prognosis is worse for patients with WHO grades II and III tumours as complete resection is less common and the proliferative capacity is greater (Bruna et al. 2007, Ko et al. 2007, Nakane et al. 2007). Malignant histology is generally associated with a poor prognosis with a survival less than 2 years (Hartmann et al. 2006, Bruna et al. 2007, Nakane et al. 2007). Figure 8 Sagittal enhanced T 1 -weighted image of a suprasellar meningioma. The mass lies above the pituitary (which is normal), involves the chiasm and extends anteriorly along the planum sphenoidale. sinus air space, may also be seen (Smith 2005). Meningiomas typically are similar to grey matter in CT density and T 1 - and T 2 -weighted MR image signal intensity, enhancing homogeneously and brightly with occasional areas of diffuse calcification (Smith 2005). In contrast to other parasellar tumours, meningiomas encase blood vessels and tend to narrow the lumen (Young et al. 1988). Surgical excision, particularly in the presence of symptomatic or growing lesions, remains the treatment of choice (WHO I). Following Rathke s cysts Rathke s cleft cysts arise from remnants of squamous epithelium of Rathke s pouch and consist of a single layer of epithelial cells with mucoid, cellular or serous components in the cyst fluid (Freda & Post 1999; Fig. 10). Although the majority has a major intrasellar component, about a third can extend into the parasellar region; occasionally they can be entirely suprasellar (Mukherjee et al. 1997, Freda & Post 1999). Many of these are small and asymptomatic, but they may become symptomatic due to compressive symptoms and pituitary hormonal deficiencies, when DI may develop in up to 20% (Mukherjee et al. 1997). Atypical presentations include haemorrhages into the cyst and Figure 9 Coronal enhanced T 1 -weighted image of a meningioma in the left cavernous sinus. The meningioma enhances avidly, expands the cavernous sinus and is causing some narrowing of the left cavernous carotid artery, which is of smaller calibre than the right carotid. Figure 10 Sagittal enhanced T 1 -weighted image of a Rathke s cleft cyst. The cyst is seen to be non-enhancing and lying on the superior aspect of the pituitary gland that appears flattened. It is causing elevation of the optic chiasm
13 Endocrine-Related Cancer (2008) abscess formation rarely can coexist with pituitary adenomas (Mukherjee et al. 1997). They are distinguished from craniopharyngiomas histologically by having walls composed of columnar or cuboidal epithelium (FitzPatrick et al. 1999). Although no specific radiological features have been identified, Rathke s cysts appear as discrete cystic and nonenhancing lesions on MRI with variable signal intensity on either T 1 -ort 2 -weighted images; these lesions need to be differentiated from craniopharyngiomas and arachnoid cysts (Mukherjee et al. 1997, Freda & Post 1999). Treatment involves drainage of the fluid with or without resection of the cystic wall (Mukherjee et al. 1997, Freda & Post 1999). Although these lesions tend not to recur, repeated resections may be required in as many as a third of patients; it has been suggested that many relapsing lesions may contain overlapping histological features with craniopharyngiomas (Mukherjee et al. 1997, Freda & Post 1999). The role of RT for recurrent lesions has not been clearly defined (Mukherjee et al. 1997). Epidermoids/dermoids These benign tumours (WHO grade I) comprise less than 2% of all intracranial tumours and arise as a result of incomplete separation of the neuroectoderm from cutaneous ectoderm (FitzPatrick et al. 1999). Epidermoids/dermoids occur in the cerebellopontine angle, pineal region, middle cranial fossa as well as in the suprasellar region, and consist of tissue of purely epidermal origin; dermoids also contain tissue of mesodermal origin (hair follicles, fat, sebaceous glands). Tumours are cystic structures lined by keratinised squamous epithelium and the clinical presentation may be due to local mass effect such as hydrocephalus, visual disturbance, hypopituitarism, DI and/or cranial nerve abnormalities (Freda & Post 1999). On CT scan, the cyst contents are very similar to CSF; both lesions are often hypointense on T 1 - and hyperintense on T 2 -weighted MR images and do not enhance with contrast. Depending upon fat and calcium content, dermoid tumours can show a hyperintense signal in T 1 images (Rennert & Doerfler 2007). Diffusion-weighted images can be helpful in epidermoids, typically showing a markedly increased signal (Rennert & Doerfler 2007). Hypothalamic hamartomas Hypothalamic hamartomas are of neuronal origin and represent congenital heterotopias usually located within the tuber cinereum and mostly affecting children causing precocious puberty and epileptic Figure 11 Sagittal enhanced T 1 -weighted image of a hypothalamic hamartoma. This is seen as a pedunculated mass hanging from the undersurface of the hypothalamus. It does not enhance and has the same signal as the grey matter of the brain parenchyma. seizures (Judge et al. 1977; Fig. 11). As they are usually less than 2 cm in diameter, they produce few symptoms of mass effect (Freeman et al. 2004). Typically, they appear as non-enhancing lesions and demonstrate rounded expansion of the tuber cinereum, best seen in coronal and sagittal images; they are isointense to the cerebral cortex in both T 1 - and T 2 -weighted MR images (Rennert & Doerfler 2007). The hamartomas associated with precocious puberty may contain GNRH1 neurons, and have been classically associated with gelastic (laughing) seizures. Paragangliomas Paragangliomas are rare, usually encapsulated and benign neoplasms (WHO grade I), that arise in specialised neural crest cells associated with segmental or collateral autonomic ganglia (Freeman et al. 2004). Although the majority develop in the carotid body and jugular glomus, paraganglionic cells have been demonstrated in the pituitary gland and adjacent structures (Steel et al. 1993). Only seven cases of intrasellar, two cases of suprasellar and four cases of parasellar nonmalignant paragangliomas have been described (Boari et al. 2006). Tumour location is more relevant than histology in assessing prognosis; the metastatic rate in para-aortic paragangliomas ranges between 28 and 42%, whereas only 5% of CNS paragangliomas exhibit metastatic potential (Boari et al. 2006). Symptoms of pituitary hormonal deficiency and mass effects are the 897
14 G A Kaltsas et al.: Parasellar tumours main presenting symptoms (Steel et al. 1993, Boari et al. 2006). Surgical excision, when possible, remains the treatment of choice; there are no data regarding the prophylactic effect of RT on tumour recurrence. Lipoma Lipomas are benign fatty tumours, derived from remnants of maldevelopment of the primitive meninx (Smith 2005; Fig. 12). In the sellar region, they occur as lesions adherent to the surface of the infundibulum, floor of the third ventricle or adjacent cranial nerves (Smith 2005). They are usually discovered incidentally but rarely may enlarge and produce symptoms. Lipomas are all well-circumscribed, homogeneous lesions that appear identical to fat on CT and all MRI sequences, do not enhance and usually exhibit rim calcification (Smith 2005). Schwannoma/Neurinoma Nerve sheath tumours (WHO grade I) in the parasellar region are very rare and usually arise from the trigeminal nerve (V 1 /V 2 ) or the III, IV and VI cranial nerves (Rennert & Doerfler 2007; Fig. 13). Neurinomas are slowly growing tumours, rarely causing bony remodelling of the lateral portion of the sella or the apex of the petrous bone (Rennert & Doerfler 2007). Schwannomas are slow-growing tumours that may erode the walls of cavernous sinus, are found in association with NF2 and exhibit inactivating mutations of the NF2 gene in 60% (Aghi & Barker 2006). They usually develop symptoms of trigeminal nerve Figure 13 Coronal enhanced T 1 -weighted image of a left sided Schwannoma of the trigeminal nerve. There is an enhancing mass expanding the left cavernous sinus which followed the course of the trigeminal nerve on other images. involvement and extremely rarely they can undergo malignant change (Aghi & Barker 2006). On MRI and CT, they show an intense (usually heterogeneous) contrast enhancement (Rennert & Doerfler 2007). Parasellar granular cell tumours These are rare tumours originating from either the neurohypophysis or infundibulum and include myoblastomas, choristomas and infundibulomas (Cone et al.1990, Cohen-Gadol et al.2003; Fig. 14). In 50% of cases cause anterior pituitary hormone deficiencies and hyperprolactinaemia, and rarely visual field defects (Freda & Post 1999). Although choristomas arise from the infundibulum and/or posterior lobe, only two cases of Figure 12 Sagittal unenhanced T 1 -weighted image of a suprasellar lipoma. The high signal mass containing fat is seen lying on the undersurface of the hypothalamus in the interpeduncular cistern. Figure 14 Sagittal enhanced T 1 -weighted image of a granular cell tumour. This enhancing mass lesion involves the pituitary stalk and the median eminence
Metastasis. 57 year old with progressive Headache and Right Sided Visual Loss
 Metastasis 1% of sellar/parasellar masses Usually occurs with known primary Can involve third ventricle, hypothalamus, infundibular stalk May be both supra-, intrasellar 57 year old with progressive Headache
Metastasis 1% of sellar/parasellar masses Usually occurs with known primary Can involve third ventricle, hypothalamus, infundibular stalk May be both supra-, intrasellar 57 year old with progressive Headache
PITUITARY PARASELLAR LESIONS. Kim Learned, MD
 PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
PITUITARY PARASELLAR LESIONS Kim Learned, MD DIFFERENTIALS Pituitary Sella Clivus, Sphenoid Sinus Suprasellar Optic chiasm, Hypothalamus, Circle of Willis Parasellar Cavernous Sinus Case 1 17 YEAR-OLD
Laurie A. Loevner, MD
 Laurie A. Loevner, MD Chief, Division of Neuroradiology UPHS Professor of Radiology, Otorhinolaryngology: Head & Neck Surgery, Neurosurgery, and Ophthalmology University of Pennsylvania Health System Disclosures
Laurie A. Loevner, MD Chief, Division of Neuroradiology UPHS Professor of Radiology, Otorhinolaryngology: Head & Neck Surgery, Neurosurgery, and Ophthalmology University of Pennsylvania Health System Disclosures
Case Studies in Sella/Parasellar Region. Child thirsty, increased urination. Imaging. Suprasellar Germ Cell Tumor (Germinoma) No Disclosures
 Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
Case Studies in Sella/Parasellar Region No Disclosures 2018 Head and Neck Imaging Conference Child thirsty, increased urination Suprasellar Germ Cell Tumor (Germinoma) Midline Pineal >> Suprasellar > Other
CNS TUMORS. D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria)
 CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
CNS TUMORS D r. Ali Eltayb ( U. of Omdurman. I ). M. Path (U. of Alexandria) CNS TUMORS The annual incidence of intracranial tumors of the CNS ISmore than intraspinal tumors May be Primary or Secondary
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours. Colin Kennedy March 2015
 Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
Optic Pathway Gliomas, Germinomas, Spinal Cord Tumours Colin Kennedy March 2015 Glioma of the optic chiasm. T1-weighted MRI with gadolinium enhancement, showing intense irregular uptake of contrast. The
DISCLOSURES LEARNING OBJECTIVES WE WILL NOT DISCUSS. CSB: Birdseye View MESSAGE NAVIGATING THE SELLA AND CENTRAL SKULL BASE
 NAVIGATING THE SELLA AND CENTRAL SKULL BASE Christopher P. Hess, M.D., Ph.D. DISCLOSURES Research Support, General Electric SLIDES: http://www.radiology.ucsf.edu/research/meetings/rsna LEARNING OBJECTIVES
NAVIGATING THE SELLA AND CENTRAL SKULL BASE Christopher P. Hess, M.D., Ph.D. DISCLOSURES Research Support, General Electric SLIDES: http://www.radiology.ucsf.edu/research/meetings/rsna LEARNING OBJECTIVES
Imaging The Turkish Saddle. Russell Goodman, HMS III Dr. Gillian Lieberman
 Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
Imaging The Turkish Saddle Russell Goodman, HMS III Dr. Gillian Lieberman Learning Objectives Review the anatomy of the sellar region Discuss the differential diagnosis of sellar masses Discuss typical
TABLES. Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging. Conclusions. Author (Year) Classification Process/Evid ence Class
 TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
TABLES Imaging Modalities Evidence Tables Table 1 Computed Tomography (CT) Imaging Author Clark (1986) 9 Reformatted sagittal images in the differential diagnosis meningiomas and adenomas with suprasellar
Where Has My Vision Gone? Evaluation of Sellar Lesions. Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008
 Where Has My Vision Gone? Evaluation of Sellar Lesions Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008 Objectives Present a case highlighting the clinical presentation and evaluation of a sellar
Where Has My Vision Gone? Evaluation of Sellar Lesions Caleb Stowell,, HMS III Gillian Lieberman, MD November 2008 Objectives Present a case highlighting the clinical presentation and evaluation of a sellar
Meningioma tumor. Meningiomas are named according to their location (Fig. 1) and cause various symptoms: > 1
 Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
Meningioma tumor Overview A meningioma is a type of tumor that grows from the protective membranes, called meninges, which surround the brain and spinal cord. Most meningiomas are benign (not cancer) and
EXPERT DIFFERENTIAL DIAGNOSIS:
 EXPERT DIFFERENTIAL DIAGNOSIS: Sellar Region Anne G. Osborn, M.D. DISCLOSURE: Published RSNA 2008 SELLA, PITUITARY: Normal Gross, 3T Anatomy SELLA, PITUITARY: Anatomically-Based Differential Diagnoses
EXPERT DIFFERENTIAL DIAGNOSIS: Sellar Region Anne G. Osborn, M.D. DISCLOSURE: Published RSNA 2008 SELLA, PITUITARY: Normal Gross, 3T Anatomy SELLA, PITUITARY: Anatomically-Based Differential Diagnoses
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
Brain tumors: tumor types
 Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Brain tumors: tumor types Tumor types There are more than 120 types of brain tumors. Today, most medical institutions use the World Health Organization (WHO) classification system to identify brain tumors.
Tumors of the Nervous System
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they present? What do they look like? How do they behave? 1
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Part II - Revising the sellar and parasellar region: differential diagnosis of a sellar region mass
 Part II - Revising the sellar and parasellar region: differential diagnosis of a sellar region mass Poster No.: C-1390 Congress: ECR 2015 Type: Educational Exhibit Authors: I. Candelaria, C. Figueira,
Part II - Revising the sellar and parasellar region: differential diagnosis of a sellar region mass Poster No.: C-1390 Congress: ECR 2015 Type: Educational Exhibit Authors: I. Candelaria, C. Figueira,
SURGICAL MANAGEMENT OF BRAIN TUMORS
 SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
SURGICAL MANAGEMENT OF BRAIN TUMORS LIGIA TATARANU, MD, Ph D NEUROSURGICAL CLINIC, BAGDASAR ARSENI CLINICAL HOSPITAL BUCHAREST, ROMANIA SURGICAL INDICATIONS CONFIRMING HISTOLOGIC DIAGNOSIS REDUCING TUMOR
Dosimetry, see MAGIC; Polymer gel dosimetry. Fiducial tracking, see CyberKnife radiosurgery
 Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
Subject Index Acoustic neuroma, neurofibromatosis type 2 complications 103, 105 hearing outcomes 103, 105 outcome measures 101 patient selection 105 study design 101 tumor control 101 105 treatment options
NANOS Patient Brochure
 NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
NANOS Patient Brochure Pituitary Tumor Copyright 2015. North American Neuro-Ophthalmology Society. All rights reserved. These brochures are produced and made available as is without warranty and for informational
Neuro - imaging. Sella. ssregypt.com
 Neuro - imaging Sella ssregypt.com Bony Sella AP diameter Depth Contents 16mm 14mm Pituitary gland, part of infundibular stalk, CSF CT Technique 5 mm slices Axial and coronal Contrast injection Bone and
Neuro - imaging Sella ssregypt.com Bony Sella AP diameter Depth Contents 16mm 14mm Pituitary gland, part of infundibular stalk, CSF CT Technique 5 mm slices Axial and coronal Contrast injection Bone and
Supra- and infratentorial brain tumors from childhood to maternity
 Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
Supra- and infratentorial brain tumors from childhood to maternity What to expect? I am going to show you the characteristic imaging findings of following tumors: Thierry A.G.M. Huisman, MD, FICIS, EQNR
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM MENINGIOMA CNS Site Group Meningioma Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION 3 2. PREVENTION
RADIOANATOMY OF SELLA TURCICA
 RADIOANATOMY OF SELLA TURCICA O.BAKKACHA, H.MALAJATI, M.RHISSASSI, H. BENCHAABOUNE, N.CHAKIR, My R. EL HASSANI,M.JIDDANE Department of Neuroradiology specialties Hospital. Rabat Objective: New imaging
RADIOANATOMY OF SELLA TURCICA O.BAKKACHA, H.MALAJATI, M.RHISSASSI, H. BENCHAABOUNE, N.CHAKIR, My R. EL HASSANI,M.JIDDANE Department of Neuroradiology specialties Hospital. Rabat Objective: New imaging
Peter Canoll MD. PhD.
 Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Tumors of the Nervous System Peter Canoll MD. PhD. What I want to cover What are the most common types of brain tumors? Who gets them? How do they ypresent? What do they look like? How do they behave?
Transplanum Approach for Suprasellar pathology
 Transplanum Approach for Suprasellar pathology Omar A. El-Banhawy Prof. of otorhinolaryngology El Menoufyia University, Egypt Why Endoscopic Approach For Suprasellar Pathology Constant improvements in
Transplanum Approach for Suprasellar pathology Omar A. El-Banhawy Prof. of otorhinolaryngology El Menoufyia University, Egypt Why Endoscopic Approach For Suprasellar Pathology Constant improvements in
Update on Pediatric Brain Tumors
 Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Update on Pediatric Brain Tumors David I. Sandberg, M.D. Director of Pediatric Neurosurgery & Associate Professor Dr. Marnie Rose Professorship in Pediatric Neurosurgery Pre-talk Questions for Audience
Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature
 Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Romanian Neurosurgery Volume XXX Number 4 2016 October - December Article Intrasphenoidal Rathke's Cleft Cyst: Case presentation and review of the literature Umit Kocaman, Muhammet Bahadir Yilmaz, Hakan
Pathologic Analysis of CNS Surgical Specimens
 2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
2015 Kenneth M. Earle Memorial Neuropathology Review Pathologic Analysis of CNS Surgical Specimens Peter C. Burger, MD Interdisciplinary Quality Control Familiarity with entities Use of diagnostic algorithm
Imaging pituitary gland tumors
 November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
November 2005 Imaging pituitary gland tumors Neel Varshney,, Harvard Medical School Year IV Two categories of presenting signs of a pituitary mass Functional tumors present with symptoms due to excess
Visual pathways in the chiasm
 Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Visual pathways in the chiasm Intracranial relationships of the optic nerve Fixation of the chiasm Chiasmatic pathologies The function of the optic chiasm may be altered by the presence of : 4) Artero
Case Studies in the Skull Base
 Case Studies in the Skull Base Amy C Tsai, MD Neuroradiology Fellow Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA No disclosures related
Case Studies in the Skull Base Amy C Tsai, MD Neuroradiology Fellow Department of Radiology and Imaging Sciences University of Utah Health Sciences Center Salt Lake City, Utah, USA No disclosures related
NON MALIGNANT BRAIN TUMOURS Facilitator. Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol
 NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
NON MALIGNANT BRAIN TUMOURS Facilitator Ros Taylor Advanced Neurosurgical Nurse Practitioner Southmead Hospital Bristol Neurosurgery What will be covered? Meningioma Vestibular schwannoma (acoustic neuroma)
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 12: CNS tumours 2/3 Pilocytic astrocytoma Relatively benign ( WHO grade 1) Occurs in children and young adults Mostly: in the cerebellum
Radiology of hypothalamic lesions: A pictorial essay depicting characteristic hypothalamic pathologies
 Radiology of hypothalamic lesions: A pictorial essay depicting characteristic hypothalamic pathologies Poster No.: C-2713 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: A. J. B. Baxi,
Radiology of hypothalamic lesions: A pictorial essay depicting characteristic hypothalamic pathologies Poster No.: C-2713 Congress: ECR 2010 Type: Scientific Exhibit Topic: Neuro Authors: A. J. B. Baxi,
Tumors of the Central Nervous System
 Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Tumors of the Central Nervous System 1 Financial Disclosures I have NO SIGNIFICANT FINANCIAL, GENERAL, OR OBLIGATION INTERESTS TO REPORT Introduction General: Brain tumors are lesions that have mass effect
Craniopharyngioma. Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital
 Craniopharyngioma Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital Objectives Incidence Clinical Presentation Treatment Options Perioperative concerns Long-term endocrine
Craniopharyngioma Michael Gottschalk, MD,PhD University of California San Diego Rady Children s Hospital Objectives Incidence Clinical Presentation Treatment Options Perioperative concerns Long-term endocrine
Skullbase Lesions. Skullbase Surgery Open vs endoscopic. Choice Of Surgical Approaches 12/28/2015. Skullbase Surgery: Evolution
 Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
Skullbase Lesions Skullbase Surgery Open vs endoscopic Prof Asim Mahmood,FRCS,FACS,FICS,FAANS, Professor of Neurosurgery Henry Ford Hospital Detroit, MI, USA Anterior Cranial Fossa Subfrontal meningioma
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions
 CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
CT & MRI Evaluation of Brain Tumour & Tumour like Conditions Dr. Anjana Trivedi 1, Dr. Jay Thakkar 2, Dr. Maulik Jethva 3, Dr. Ishita Virda 4 1 M.D. Radiology, Professor and Head, P.D.U. Medical College
Note: The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
- In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
Year 2003 Paper two: Questions supplied by Tricia
 question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
question 43 A 42-year-old man presents with a two-year history of increasing right facial numbness. He has a history of intermittent unsteadiness, mild hearing loss and vertigo but has otherwise been well.
Pediatric CNS Tumors. Disclosures. Acknowledgements. Introduction. Introduction. Posterior Fossa Tumors. Whitney Finke, MD
 Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Pediatric CNS Tumors Disclosures Whitney Finke, MD Neuroradiology Fellow PGY-6 University of Utah Health Sciences Center Salt Lake City, Utah None Acknowledgements Introduction Nicholas A. Koontz, MD Luke
Dr.Dafalla Ahmed Babiker Jazan University
 Dr.Dafalla Ahmed Babiker Jazan University Brain tumors are the second commonest malignancy in children Infratentorial tumors are more common As a general rule they do not metastasize out of the CNS, but
Dr.Dafalla Ahmed Babiker Jazan University Brain tumors are the second commonest malignancy in children Infratentorial tumors are more common As a general rule they do not metastasize out of the CNS, but
Essentials of Clinical MR, 2 nd edition. 51. Primary Neoplasms
 51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
51. Primary Neoplasms As with spinal central canal neoplasms in other regions, those of the lumbar spine may be classified as extradural, intradural extramedullary, and medullary. If an extradural lesion
Protocol for management of patients with pineal region tumours v1
 Protocol for management of patients with pineal region tumours v1 West Midlands Cancer Alliance Coversheet for Cancer Alliance Expert Advisory Group Agreed Documentation This sheet is to accompany all
Protocol for management of patients with pineal region tumours v1 West Midlands Cancer Alliance Coversheet for Cancer Alliance Expert Advisory Group Agreed Documentation This sheet is to accompany all
Case 7391 Intraventricular Lesion
 Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
Case 7391 Intraventricular Lesion Bastos Lima P1, Marques C1, Cabrita F2, Barbosa M2, Rebelo O3, Rio F1. 1Neuroradiology, 2Neurosurgery, 3Neuropathology, Coimbra University Hospitals, Portugal. University
CS Tumor Size CS Extension CS Tumor Size/Ext Eval CS Lymph Nodes CS Lymph Nodes Eval Reg LN Pos Reg LN Exam CS Mets at DX CS Mets Eval
 C70.0, C71.0-C71.9 C70.0 Cerebral meninges C71.0 Cerebrum C71.1 Frontal lobe C71.2 Temporal lobe C71.3 Parietal lobe C71.4 Occipital lobe C71.5 Ventricle, NOS C71.6 Cerebellum, NOS C71.7 Brain stem C71.8
C70.0, C71.0-C71.9 C70.0 Cerebral meninges C71.0 Cerebrum C71.1 Frontal lobe C71.2 Temporal lobe C71.3 Parietal lobe C71.4 Occipital lobe C71.5 Ventricle, NOS C71.6 Cerebellum, NOS C71.7 Brain stem C71.8
Juvenile Angiofibroma
 Juvenile Angiofibroma Disclaimer The pictures used in this presentation have been obtained from a number of sources. Their use is purely for academic and teaching purposes. The contents of this presentation
Juvenile Angiofibroma Disclaimer The pictures used in this presentation have been obtained from a number of sources. Their use is purely for academic and teaching purposes. The contents of this presentation
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis
 Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
Dr. T. Venkat Kishan Asst. Prof Department of Radiodiagnosis Schwannomas (also called neurinomas or neurilemmomas) constitute the most common primary cranial nerve tumors. They are benign slow-growing
-The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - include: I. Germ cell tumors : (95%); all are malignant. II. Sex cord-stromal tumors: from Sertoli or Leydig cells; usually
- In the 15- to 34-year-old age group, they are the most common tumors of men. - include: I. Germ cell tumors : (95%); all are malignant. II. Sex cord-stromal tumors: from Sertoli or Leydig cells; usually
Craniopharyngiomas (from Greek: κρανίον, skull
 J Neurosurg 119:1194 1207, 2013 AANS, 2013 Endoscopic endonasal surgery for craniopharyngiomas: surgical outcome in 64 patients Clinical article Maria Koutourousiou, M.D., 1 Paul A. Gardner, M.D., 1 Juan
J Neurosurg 119:1194 1207, 2013 AANS, 2013 Endoscopic endonasal surgery for craniopharyngiomas: surgical outcome in 64 patients Clinical article Maria Koutourousiou, M.D., 1 Paul A. Gardner, M.D., 1 Juan
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A
 Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
Cross sectional imaging of Intracranial cystic lesions Abdel Razek A Department of Radiology. Mansoura Faculty of Medicine, Mansoura. Egypt. arazek@mans.edu.eg Introduction Intracranial cystic lesions
FINALIZED SEER SINQ QUESTIONS
 0076 Source 1: WHO Class CNS Tumors pgs: 33 MP/H Rules/Histology--Brain and CNS: What is the histology code for a tumor originating in the cerebellum and extending into the fourth ventricle described as
0076 Source 1: WHO Class CNS Tumors pgs: 33 MP/H Rules/Histology--Brain and CNS: What is the histology code for a tumor originating in the cerebellum and extending into the fourth ventricle described as
Hypothalamic glioma masquerading as craniopharyngioma
 1 di 7 24/01/2014 18.58 J Neurosci Rural Pract. 2013 Jul-Sep; 4(3): 323 325. doi: 10.4103/0976-3147.118790 PMCID: PMC3821425 Hypothalamic glioma masquerading as craniopharyngioma Sameer Vyas, Nidhi Prabhakar,
1 di 7 24/01/2014 18.58 J Neurosci Rural Pract. 2013 Jul-Sep; 4(3): 323 325. doi: 10.4103/0976-3147.118790 PMCID: PMC3821425 Hypothalamic glioma masquerading as craniopharyngioma Sameer Vyas, Nidhi Prabhakar,
Pituitary Macroadenoma with Superior Orbital Fissure Syndrome
 1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
1 CASE REPORT OPEN ACCESS Pituitary Macroadenoma with Superior Orbital Fissure Syndrome Tapan Nagpal, Ankit Singhania ABSTRACT Introduction: Pituitary adenomas are benign tumours which arise within the
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution
 Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Oligodendroglioma: imaging findings, radio-pathological correlation and evolution Poster No.: C-2104 Congress: ECR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit A. Hernandez Castro, M. D. Monedero
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234)
 Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Somatotroph Pituitary Adenomas (Acromegaly) The Diagnostic Pathway (11-2K-234) Common presenting symptoms/clinical assessment: Pituitary adenomas are benign neoplasms of the pituitary gland. In patients
Advances In Orbital Neuropathology
 Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Advances In Orbital Neuropathology Charles G. Eberhart, MD PhD Associate Professor of Pathology, Ophthalmology and Oncology Johns Hopkins University School of Medicine Overview Non-neoplastic lesions Microphthalmos/pseudoglioma
Pediatric Brain Tumors Pre, Intra & Post Op Evaluation and Management. Timothy M. George, MD, FACS, FAAP
 Pediatric Brain Tumors Pre, Intra & Post Op Evaluation and Management Timothy M. George, MD, FACS, FAAP PEDIATRIC BRAIN TUMORS BACKGROUND: Incidence: Third most common pediatric tumor type (leukemia, neuroblastoma,
Pediatric Brain Tumors Pre, Intra & Post Op Evaluation and Management Timothy M. George, MD, FACS, FAAP PEDIATRIC BRAIN TUMORS BACKGROUND: Incidence: Third most common pediatric tumor type (leukemia, neuroblastoma,
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES
 PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM GERM CELL TUMOURS CNS Site Group Germ Cell Tumours Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
PRINCESS MARGARET CANCER CENTRE CLINICAL PRACTICE GUIDELINES CENTRAL NERVOUS SYSTEM GERM CELL TUMOURS CNS Site Group Germ Cell Tumours Author: Dr. Norm Laperriere Date: February 20, 2018 1. INTRODUCTION
Adult Brain and Spinal Cord Tumors
 Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
Adult Brain and Spinal Cord Tumors An adult central nervous system (CNS) tumor is a disease in which abnormal cells form in the tissues of the brain and or the spinal cord. Major Parts of the Brain Anatomy
Background Principles and Technical Development
 Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
Contents Part I Background Principles and Technical Development 1 Introduction and the Nature of Radiosurgery... 3 Definitions of Radiosurgery... 5 Consequences of Changing Definitions of Radiosurgery...
Pediatric Brain Tumors: Updates in Treatment and Care
 Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
Pediatric Brain Tumors: Updates in Treatment and Care Writer Classroom Rishi R. Lulla, MD MS Objectives Introduce the common pediatric brain tumors Discuss current treatment strategies for pediatric brain
EANS Training Course Moscow, 5 th 8 th May 2019 Tumours
 EANS Training Course Moscow, 5 th 8 th May 2019 Tumours SUNDAY, MAY 5 th, 2019 09:00 09:10 Welcome 09:15 10:30 Tumours Chair: Meling 09:15 09:30 Molecular biology of brain tumours Reinert 09:30 09:45 Imaging
EANS Training Course Moscow, 5 th 8 th May 2019 Tumours SUNDAY, MAY 5 th, 2019 09:00 09:10 Welcome 09:15 10:30 Tumours Chair: Meling 09:15 09:30 Molecular biology of brain tumours Reinert 09:30 09:45 Imaging
Structural and functional imaging for the characterization of CNS lymphomas
 Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
Structural and functional imaging for the characterization of CNS lymphomas Cristina Besada Introduction A few decades ago, Primary Central Nervous System Lymphoma (PCNSL) was considered as an extremely
A Journey Down The Canal
 A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
A Journey Down The Canal Radiological Assessment of Spinal Cord Masses John Berry-Candelario HMS III Gillian Lieberman, MD BIDMC Objectives Patient review Anatomy of the spine Imaging techniques Classification
Financial Disclosures I have no financial interests to disclose. Templar Eye Foundation Oppenheimer Family Foundation
 Financial Disclosures I have no financial interests to disclose. Templar Eye Foundation Oppenheimer Family Foundation 2 Case 7 year old girl Initially parents noticed photophobia Then started to complain
Financial Disclosures I have no financial interests to disclose. Templar Eye Foundation Oppenheimer Family Foundation 2 Case 7 year old girl Initially parents noticed photophobia Then started to complain
Leptomeningeal metastasis: management and guidelines. Emilie Le Rhun Lille, FR Zurich, CH
 Leptomeningeal metastasis: management and guidelines Emilie Le Rhun Lille, FR Zurich, CH Definition of LM LM is defined as the spread of tumor cells within the leptomeninges and the subarachnoid space
Leptomeningeal metastasis: management and guidelines Emilie Le Rhun Lille, FR Zurich, CH Definition of LM LM is defined as the spread of tumor cells within the leptomeninges and the subarachnoid space
Neoplasia part I. Dr. Mohsen Dashti. Clinical Medicine & Pathology nd Lecture
 Neoplasia part I By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 2 nd Lecture Lecture outline Review of structure & function. Basic definitions. Classification of neoplasms. Morphologic features.
Neoplasia part I By Dr. Mohsen Dashti Clinical Medicine & Pathology 316 2 nd Lecture Lecture outline Review of structure & function. Basic definitions. Classification of neoplasms. Morphologic features.
Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS
 Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
Multiple Primary and Histology Site Specific Coding Rules MALIGNANT CENTRAL NERVOUS SYSTEM TUMORS 1 Prerequisites 2 Completion of Multiple Primary and Histology General Coding Rules 3 There are many ways
Brain Tumors. Medulloblastoma. Pilocytic astrocytoma: Ahmed Koriesh, MD. Pathological finding
 NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
NeuroPathology Page 8 Brain Tumors Pathological finding Pseudorosette Rosenthal fibers Rosettes Wet Keratin Psammoma bodies Fried egg Tumor Ependymoma, SEGA Pilocytic astrocytoma Medulloblastoma Craniopharyngioma
Pituitary gland diseases
 Pituitary gland diseases Pituitary Gland Weight 600 mg Is located within the sella turcica Anatomically and functionally distinct anterior and posterior lobes Pituitary Development The pituitary originate
Pituitary gland diseases Pituitary Gland Weight 600 mg Is located within the sella turcica Anatomically and functionally distinct anterior and posterior lobes Pituitary Development The pituitary originate
Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined Approach
 Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
Radiosurgery as part of the neurosurgical armamentarium: Educational Symposium November 24 th 2011 Impact of Gamma Knife Radiosurgery on the neurosurgical management of skull-base lesions: The Combined
NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) BONE (Version , 03/28/18)
 BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
BONE (Version 2.2018, 03/28/18) NCCN GUIDELINES ON PROTON THERAPY (AS OF 4/23/18) Radiation Therapy Specialized techniques such as intensity-modulated RT (IMRT); particle beam RT with protons, carbon ions,
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary
 Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
Selected radiosurgery cases from the Rotating Gamma Institute Debrecen, Hungary László Bognár M.D., Ph.D., József G. Dobai M.D., Gábor Csiky and Imre Fedorcsák M.D., Ph.D. Department of Neurosurgery, Medical
Imaging the Spinal Cord & Intradural Disease
 Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Department of Radiology University of California San Diego Imaging the Spinal Cord & Intradural Disease John R. Hesselink, M.D. Spinal Cord Diseases Tumors Syringohydromyelia Trauma Ischemia / Infarction
Diseases of the breast (1 of 2)
 Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Blue-domed cyst with optic nerve compression
 Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 987-991 Blue-domed cyst with optic nerve compression MITCHELL D. BURNBAUM, JOHN W. HARBISON, JOHN B. SELHORST, AND HAROLD F. YOUNG From the
Journal ofneurology, Neurosurgery, and Psychiatry, 1978, 41, 987-991 Blue-domed cyst with optic nerve compression MITCHELL D. BURNBAUM, JOHN W. HARBISON, JOHN B. SELHORST, AND HAROLD F. YOUNG From the
Pediatric Spine Tumors (and other masses)
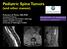 Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Pediatric Spine Tumors (and other masses) Francisco A Perez, MD, PhD Assistant Professor Neuroradiology and Pediatric Radiology Seattle Children s Hospital University of Washington, Seattle Commercial
Brain Tumors. Andrew J. Fabiano, MD FAANS. Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine
 Brain Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases Brain
Brain Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases Brain
RING ENCHANCING LESION BY M.S. HEMHNATH
 RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
RING ENCHANCING LESION BY M.S. HEMHNATH A 21 YRS FEMALE CAME WITH H/O HEADACHE AND SEIZURE FOR THE PAST ONE MONTH. NO OTHER FOCAL NEUROLOGICAL DEFICIT. DIFFERENTIAL DIAGNOSIS For this case are Neurocysticerosis
Aria Fallah MD, MSc, FRCSC
 Aria Fallah MD, MSc, FRCSC Department of Neurosurgery David Geffen School of Medicine at UCLA Pineal Region Tumors Brain Tumor Symposium August 22, 2015 Disclosures None Pineal Gland Arises from an invagination
Aria Fallah MD, MSc, FRCSC Department of Neurosurgery David Geffen School of Medicine at UCLA Pineal Region Tumors Brain Tumor Symposium August 22, 2015 Disclosures None Pineal Gland Arises from an invagination
Neurosurgical Management of Brain Tumours. Nicholas Little Neurosurgeon RNSH
 Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Neurosurgical Management of Brain Tumours Nicholas Little Neurosurgeon RNSH General Most common tumours are metastatic 10x more common than primary Incidence of primary neoplasms is 20 per 100000 per year
Role of imaging in RCC. Ultrasonography. Solid lesion. Cystic RCC. Solid RCC 31/08/60. From Diagnosis to Treatment: the Radiologist Perspective
 Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Role of imaging in RCC From Diagnosis to Treatment: the Radiologist Perspective Diagnosis Staging Follow up Imaging modalities Limitations and pitfalls Duangkamon Prapruttam, MD Department of Therapeutic
Endoscopic Assisted resection for congenital Midline Nasal Mass
 Endoscopic Assisted resection for congenital Midline Nasal Mass Ahmed Aly Ibrahim A.prof ORL Department Alexandria University Emad. A Magdy prof ORL Department Alexandria University Haytham Morsi,MD Mohammad
Endoscopic Assisted resection for congenital Midline Nasal Mass Ahmed Aly Ibrahim A.prof ORL Department Alexandria University Emad. A Magdy prof ORL Department Alexandria University Haytham Morsi,MD Mohammad
Diseases of pituitary gland
 Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
Diseases of pituitary gland A brief introduction Anterior lobe = adenohypophysis Posterior lobe = neurohypophysis The production of most pituitary hormones is controlled in large part by positively and
No Financial Interest
 Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pituitary Apoplexy Michael Vaphiades, D.O. Professor Department of Ophthalmology, Neurology, Neurosurgery University of Alabama at Birmingham, Birmingham, AL No Financial Interest N E U R O L O G I C
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Brain and Spine Tumors
 Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Brain and Spine Tumors Andrew J. Fabiano, MD FAANS Associate Professor of Neurosurgery Roswell Park Cancer Institute SUNY at Buffalo School of Medicine Brain Tumors Brain Tumor Basics Types of Tumors Cases
Neuro-oncology Update Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013
 Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
Neuro-oncology Update 2013 Andrew Kokkino, MD Medical Director, The Neurosciences Institute at Sacred Heart at Riverbend May 20, 2013 Case 1 58 year old man with recent facial droop and HA s Thin, cachectic
Evaluation of Neck Mass. Disclosure. Learning Objectives 3/24/2014. Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ. Nothing to disclose
 Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
Evaluation of Neck Mass Karen T. Pitman MD, FACS Banner MDACC, Gilbert AZ Nothing to disclose Disclosure Learning Objectives 1. Describe a systematic method to evaluate a patient with a neck mass 2. Select
NEURORADIOLOGY DIL part 5
 NEURORADIOLOGY DIL part 5 Masses and tumors K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL part
NEURORADIOLOGY DIL part 5 Masses and tumors K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL part
Non-Functioning Tumours and Pituitary Hormone Testing. Miguel Debono Consultant in Endocrinology
 Non-Functioning Tumours and Pituitary Hormone Testing Miguel Debono Consultant in Endocrinology Agenda Pituitary masses Non functioning pituitary adenomas Testing pituitary function Pituitary Hormone Replacement
Non-Functioning Tumours and Pituitary Hormone Testing Miguel Debono Consultant in Endocrinology Agenda Pituitary masses Non functioning pituitary adenomas Testing pituitary function Pituitary Hormone Replacement
Leukaemia 35% Lymphoma 14%
 Distribution ib ti of Cancers in Children under 15 years Leukaemia 35% Lymphoma 14% Neuroblastoma 9% Other 5% Liver 1% Retinoblastoma 3% Bone and STS 15% CNS 20% Wilms' 8% 30-40% Mortality Germ Cell Tumours
Distribution ib ti of Cancers in Children under 15 years Leukaemia 35% Lymphoma 14% Neuroblastoma 9% Other 5% Liver 1% Retinoblastoma 3% Bone and STS 15% CNS 20% Wilms' 8% 30-40% Mortality Germ Cell Tumours
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 3,500 108,000 1.7 M Open access books available International authors and editors Downloads Our
Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male
 Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Case Reports in Radiology Volume 2016, Article ID 6434623, 4 pages http://dx.doi.org/10.1155/2016/6434623 Case Report Intracranial Capillary Hemangioma in the Posterior Fossa of an Adult Male Jordan Nepute,
Masses of the Corpus Callosum
 Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Q&A. Fabulous Prizes. Collecting Cancer Data:CNS 2/7/12. NAACCR Webinar Series Collecting Cancer Data Central Nervous System
 Collecting Cancer Data Central Nervous System NAACCR 2012 2013 Webinar Series 2/7/2013 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants
Collecting Cancer Data Central Nervous System NAACCR 2012 2013 Webinar Series 2/7/2013 Q&A Please submit all questions concerning webinar content through the Q&A panel. Reminder: If you have participants
Radiology Pathology Conference
 Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
Radiology Pathology Conference Sharlin Johnykutty,, MD, Cytopathology Fellow Sara Majewski, MD, Radiology Resident Friday, August 28, 2009 Presentation material is for education purposes only. All rights
