MALE REPRODUCTIVE SYSTEM
|
|
|
- Kerrie Nicholson
- 5 years ago
- Views:
Transcription
1 MALE REPRODUCTIVE SYSTEM
2 Mythology and history In Greek mythology, Priapus or Priapos,was a minor rustic fertility god, protector of livestock, fruit plants, gardens and male genitalia. Priapus is marked by his absurdly oversized, permanent erection, which gave rise to the medical term priapism
3 Statuette of Osiris with phallus and amulets Phallic-Head Plate, Gubbio, Italy, 1536 Polyphallic wind chime from Pompeii; a bell hung from each phallus
4 The male hormonal control
5
6 Hormonal Control of Male Reproductive Functions GnRH, FSH, and LH Testosterone gonadotropin-releasing hormone (GnRH), released by the hypothalamus to stimulate the release of pituitary gonadotropins - follicle-stimulating hormone (FSH) and luteinizing hormone (LH) from the anterior pituitary gland. In both males and females these two hormones act to promote gametogenesis and androgen/estrogen secretion.
7
8
9
10
11
12 In short, this is a known list of sex organs that evolve from the same tissue in a human life. Indifferent Male Female Gonad Testis Ovary Mullerian duct Appendix testis Fallopian tubes Mullerian duct Prostatic utricle Uterus, proximal vagina Wolffian duct Rete testis Rete ovarii Mesonephric tubules Efferent ducts Epoophoron Wolffian duct Epididymis Gartner's duct Wolffian duct Vas deferens Wolffian duct Seminal vesicle Wolffian duct Prostate Skene's glands Urogenital sinus Bladder, urethra Bladder, urethra, distal vagina Urogenital sinus Bulbourethral gland Bartholin's gland Genital swelling Scrotum Labia majora Urogenital folds Distal urethra Labia minora Genital tubercle Penis Clitoris Prepuce Foreskin Clitoral hood Bulb of penis Vestibular bulbs Glans penis Clitoral glans Crus of penis Clitoral crura
13 The anatomy and abnormalities it self
14 The male reproductive system Two testes Scrotum Spermatic cords Accessory glands Penis Prepuce The male duct system vasa efferentia vas deferens urethra external
15 Male Reproductive System Pathway of spermatozoa Epididymis Ductus deferens (Vas deferens) Ejaculatory duct Accessory organs Seminal vesicles Prostate gland Bulbourethral glands Scrotal sac encloses testes Penis
16 The Male Reproductive System Figure 28.1
17 The Male Reproductive System in Anterior View Figure 28.3
18 The foreskin has twelve known functions. They are: to cover and bond with the synechia so as to permit the development of the mucosal surface of the glans and inner foreskin. to protect the infant's glans from feces and ammonia in diapers. to protect the glans penis from friction and abrasion throughout life. to keep the glans moisturized and soft with emollient oils. to lubricate the glans. to coat the glans with a waxy protective substance. to provide sufficient skin to cover an erection by unfolding. to provide an aid to masturbation and foreplay. to serve as an aid to penetration. to reduce friction and chafing during intercourse. to serve as erogenous tissue because of its rich supply of erogenous receptors. to contact and stimulate the G-spot of the female partner.
19
20 1. Testicles 2. Epididymis 3. Corpus cavernosa 4. Foreskin 5. Frenulum 6. Urethral opening 7. Glans penis 8. Corpus spongiosum 9. Penis 10. Scrotum
21 hypospadias
22
23 Epispadias
24 Testes Epididymis Ductus deferens Urethra Penis
25
26 The word "penis" is taken from the Latin word for "tail."
27
28
29
30
31 priapism Malignant priapism secondary to osteogenic sarcoma RB Nerli, A Koura, V Prabha, SB Alur, S Devaraju, S Godhi, MB Hiremath Department of Urology, KLE University's KLES Kidney Foundation, KLES Dr. Prabhakar Kore Hospital & MRC, Belgaum , India
32
33
34 Aphallia (penile agenesis) results from failure of the genital tubercle to develop incidence: 1/10,000,000 live male births (only 70 reported cases) usually has appearance of welldeveloped scrotum with bilaterally descended testes, but no penile shaft urethral opening most often on the anal verge adjacent to a small skin tag; otherwise, may be in rectum associated anomalies: cryptorchidism, horseshoe kidney, renal agenesis, imperforate anus
35 Bifid penis Surgic ally done
36 Diphallus: duplication of the penis rare anomaly that may range from small accessory penis to the real deal...times two. associated anomalies: hypospadias, bifid scrotum, duplicated bladder, renal agenesis/ ectopia,
37 Control of erection Hypothalamus (conscious control) Parasympathetic nerves neurotransmitter- nitric oxide promotes blood flow into penis (Viagra- promotes vasodilation) Control of emission and ejaculation sympathetic nerves- muscle contraction The man whose non-erect penis is smallish will usually achieve about a 100 per cent increase in length during sexual excitement. The man whose non-erect penis is on the largish size will probably manage about a 75 per cent increase. This means the great majority of penises measure between 15cm and 18cm (6-7 inches) when erect, with the average figure being about 16.5cm (6.5 inches).
38
39 A view of the frenulum, foreskin retracted
40
41 Penis post ejaculation, notice all the vasculature [veinous]
42 phemosis
43 phemosis
44 Scrotum Skin Dartos muscle (smooth) Septum Cremaster muscle (skeletal)
45 dartos
46
47 Scrotum Temperature Optimal for sperm development is 3 C below body temp (~91 F) Controlled by muscles Spermatic cord Testicular artery Plexus of veins Nerves vas deferens 24.2
48
49 The Scrotum Intrascrotal temperature is kept constant by two sets of muscles: Dartos smooth muscle that wrinkles scrotal skin. regulate the temperature of the testicles, which promotes spermatogenesis. It does this by expanding or contracting to wrinkle the scrotal skin. Contraction reduces the surface area available for heat loss, thus reducing heat loss and warming the testicles. Conversely, expansion increases the surface area, promoting heat loss and thus cooling the testicles. Cremaster bands of skeletal muscle that elevate the testes, Its function is to raise and lower the testes in order to regulate the temperature of the testes and promote spermatogenesis. Contraction may also occur during arousal which can prevent injury to the testicles during sex In human females, the cremaster muscle is smaller and is found on the round ligament.
50 Scrotal ligament
51
52 Hydrocele in a 40 Year Old man
53 Testes
54
55 MALE REPRODUCTIVE SYSTEM TESTIS TUNICA ALBUGINEA - thick connective tissue capsule - connective tissue septa divide testis into 250 lobules - each lobule contains 1-4 seminiferous tubules and interstitial connective tissue (1) SEMINIFEROUS TUBULES - produce sperm INTERSTITIAL TISSUE - contains Leydig cells which produce testosterone (2) RECTUS TUBULES (3) RETE TESTIS (4) EFFERENT DUCTULES (5) EPIDIDYMIS
56 MALE REPRODUCTIVE SYSTEM TESTIS EPIDIDYMIS LOBULES TUNICA ALBUGINEA
57 Testes (single testis) Divided into wedge shaped lobules. Testes and ovaries are from the same tissue Seminiferous tubules: Cells specialties 1). Leydig cells 2). Spermatogenic cells Testis
58 Layers of the testis: Tunica vaginalis (peritoneum) Tunica albuginea (dense connective tissue) Septa radiate from mediastinum testes Dividing testes into lobules Each has 1-4 tubules (Seminiferous tubules) testes
59 Testes are formed in abdomen and descend into scrotum at 7th month of development Temperature in scrotum is slightly lower than in body Spermatogenesis (formation of sperm) sperm-forming cells Sertoli cells interstitial cells-produce testosterone Process takes about 9 weeks
60 Testes The testes have, like the ovaries, two functions: they produce the male gametes or spermatozoa, they produce male sexual hormone, testosterone, which stimulates the accessory male sexual organs and causes the development of the masculine extragenital sex characteristics.
61 The testis is surrounded by a thick capsule, the tunica albuginea, from which a conical mass of connective tissue, the mediastinum testis, projects into the testis. The tunica albuginea is covered externally by a serosa. From the mediastinum, delicate fibrous septa radiate towards the tunica albuginea and divide the parenchyma of the testis into about 300 lobuli testis. Each lobule contains 1-4 convoluted seminiferous tubules (about µm in diameter, cm long). Interstitial tissue between the convoluted tubules is continuous with a layer of loose vascular connective tissue, the tunica vasculosa testis, which is found beneath the tunica albuginea. Each seminiferous tubule continues near the mediastinum into a straight tubule, a tubulus rectus. The straight tubules continue into the rete testis, a labyrinthine system of cavities in the mediastinum
62 The Structure of the Testes Figure 28.4
63
64
65
66
67
68 EPIDIDYMIS EFFERENT DUCTULES
69 The Epididymus Figure 28.9
70 BulbourethralGlands (Cowper s Glands) Pea-sized glands inferior to the prostate Produce thick, clear, alkaline mucus prior to ejaculation that neutralizes traces of acidic urine in the urethra
71 Contents of Semen Typical ejaculate = 2-5 ml fluid Contains between million spermatozoa per ml Seminal fluid A distinct ionic and nutritive glandular secretion
72 MALE REPRODUCTIVE SYSTEM TESTIS TUNICA VAGINALIS TUNICA ALBUGINEA SEMINIFEROUS TUBULES SEMINIFEROUS EPITHELIUM - complex stratified epithelium containing two basic cell populations: (1) SPERMATOGENIC CELLS (2) SERTOLI CELLS
73 TESTIS H&E SEMINIFEROUS TUBULES
74 TESTIS H&E SEMINIFEROUS TUBULES SEMINIFEROUS TUBULES INTERSTITIAL CONN. TISSUE
75 TESTIS H&E SEMINIFEROUS TUBULES SEMINIFEROUS TUBULES INTERSTITIAL CONN. TISSUE
76 The Seminiferous Tubules Figure 28.5a, b
77 Male reproductive tract Testes produce mature spermatozoa Sperm enter epididymus Elongated tubule with head, body and tail regions Monitors and adjusts fluid in seminiferous tubules Stores and protects spermatozoa Facilitates functional maturation of spermatozoa
78 MALE REPRODUCTIVE SYSTEM TESTIS SEMINIFEROUS TUBULES SEMINIFEROUS EPITHELIUM - complex stratified epithelium containing two basic cell populations: (1) SPERMATOGENIC CELLS stem cells which regularly replicate and differentiate into mature sperm as they migrate toward the lumen (2) SERTOLI CELLS nonreplicating physical support cells INTERSTITIAL CONNECTIVE TISSUE (1) LEYDIG CELLS produce and release testosterone
79 The Seminiferous Tubules Figure 28.5c
80 Function of the Seminal Vesicles Each seminal vesicle is a tortuous, loculated tube lined with a secretory epithelium that secretes a mucoid material containing an abundance of fructose, citric acid, and other nutrient substances, as well as large quantities of prostaglandins and fibrinogen. During the process of emission and ejaculation, each seminal vesicle empties its contents into the ejaculatory duct shortly after the vas deferens empties the sperm. This adds greatly to the bulk of the ejaculated semen, and the fructose and other substances in the seminal fluid are of considerable nutrient value for the ejaculated sperm until one of the sperm fertilizes the ovum. Prostaglandins are believed to aid fertilization in two ways: (1) by reacting with the female cervical mucus to make it more receptive to sperm movement (2) by possibly causing backward, reverse peristaltic contractions in the uterus and fallopian tubes to move the ejaculated sperm toward the ovaries (a few sperm reach the upper ends of the fallopian tubes within 5 minutes)
81 SPERMATOGENESIS SPERM FORMATION Seminiferous tubules Contain Stem spermatogonia cells involved in spermatogenesis Contain Sustain sustentacular cells and promote development of sperm
82 Hormonal Factors That Stimulate Spermatogenesis We shall discuss the role of hormones in reproduction later, but at this point, let us note that several hormones play essential roles in spermatogenesis. Some of these are as follows: 1. Testosterone, secreted by the Leydig cells located in the interstitium of the testis, is essential forgrowth and division of the testicular germinal cells, which is the first stage in forming sperm.
83 Maturation of Sperm in the Epididymis After formation in the seminiferous tubules, the sperm require several days to pass through the 6-meter-long tubule of the epididymis. Sperm removed from the seminiferous tubules and from the early portions of the epididymis are nonmotile, and they cannot fertilize an ovum. However, after the sperm have been in the epididymis for some 18 to 24 hours, they develop the capability of motility, even though several inhibitory proteins in the epididymal fluid still prevent final motility until after ejaculation
84 2. Luteinizing hormone, secreted by the anterior pituitary gland, stimulates the Leydig cells to secrete testosterone. 3. Follicle-stimulating hormone, also secreted by the anterior pituitary gland, stimulates the Sertoli cells; without this stimulation, the conversion of the spermatids to sperm (the process of spermiogenesis) will not occur. 4. Estrogens, formed from testosterone by the Sertoli cells when they are stimulated by folliclestimulating hormone, are probably also essential for spermiogenesis. 5. Growth hormone (as well as most of the other body hormones) is necessary for controlling background metabolic functions of the testes. Growth hormone specifically promotes early division of the spermatogonia themselves; in its absence, as in pituitary dwarfs, spermatogenesis is severely deficient or absent, thus causing infertility.
85 Storage of Sperm. The two testes of the human adult form up to 120 million sperm each day. A small quantity of these can be stored in the epididymis, but most are stored in the vas deferens. They can remain stored, maintaining their fertility, for at least a month. During this time, they are kept in a deeply suppressed inactive state by multiple inhibitory substances in the secretions of the ducts. Conversely, with a high level of sexual activity and ejaculations, storage may be no longer than a few days. After ejaculation, the sperm become motile, and they also become capable of fertilizing the ovum, a process called maturation. The Sertoli cells and the epithelium of the epididymis secrete a special nutrient fluid that is ejaculated along with the sperm. This fluid contains hormones (including both testosterone and estrogens), enzymes, and special nutrients that are essential for sperm maturation.
86 Spermatogenesis Figure 28.7
87
88 SPERMATOGENESIS THREE PHASES: (1) Spermatogonial Phase (Mitosis) (2) Spermatocyte Phase (Meiosis) (3) Spermatid Phase (Spermiogenesis) - acrosome formation; golgi granules fuse to form acrosome that contains hydrolytic enzymes which will enable the spermatozoa to move through the investing layers of the oocyte - flagellum formation; centrioles and associate axoneme (arrangement of microtubules in cilia) - changes in size and shape of nucleus; chromatin condenses and shedding of residual body (cytoplasm)
89 MALE REPRODUCTIVE SYSTEM SPERMATOGENESIS SPERMATOGONIA 1º SPERMATOCYTE 2º SPERMATOCYTE SPERMATIDS SPERMATIDS 2º SPERMATOCYTE 1º SPERMATOCYTE SERTOLI CELLS: - columnar with adjoining lateral processes - extend from basal lamina to lumen - Sertoli-Sertoli junctions divide seminiferous tubules into basal and adluminal compartments SERTOLI CELLS SPERMATOGONIA
90 Spermiogenesis and Spermatozoon Structure Figure 28.8
91 SPERMATOGENESIS MALE REPRODUCTIVE SYSTEM THREE PHASES: (1) Spermatogonial Phase (Mitosis) - spermatogonia proliferate by mitotic divisions to provide stem cells and cells which will proceed through spermatogenesis (1º spermatocytes) (2) Spermatocyte Phase (Meiosis) - diploid cells (2n) created in spermatogonial phase give rise to haploid cells (1n) - Meiosis I (reduction division) & Meiosis II (equatorial division) - 1º spermatocytes enter Meiosis I to form 2º spermatocytes which then enter Meiosis II and result in spermatids (3) Spermatid Phase (Spermiogenesis) - spermatid differentiation into spermatazoa SEMINIFEROUS TUBULES
92
93
94 MALE REPRODUCTIVE SYSTEM SPERMIOGENESIS Mature sperm 60µm long and acquire full motility in epididymis (1) HEAD - nucleus and acrosome (2) NECK - centriole and connecting piece (3) TAIL - middle piece (axoneme, outer dense fibers, mitochondial sheath) - principal piece (axoneme, outer dense fibers, fibrous sheath) - end piece (axoneme)
95 MALE REPRODUCTIVE SYSTEM SPERMIOGENESIS
96
97
98
99 MALE REPRODUCTIVE SYSTEM HORMONAL REGULATION OF MALE REPRODUCTIVE FUNCTION HYPOTHALAMUS REGULATES ACTIVITY OF ANTERIOR PITUITARY (ADENOHYPOPHYSIS) ADENOHYPOPHYSIS SYNTHESIZES HORMONES (LH and FSH) THAT MODULATE ACTIVITY OF SERTOLI AND LEYDIG CELLS Luteinizing Hormone (LH): stimulates testosterone production by Leydig cells Follicle Stimulating Hormone (FSH): stimulates production of sperm in conjunction with testosterone by regulating activity of Sertoli cells SERTOLI CELLS STIMULATED BY FSH AND TESTOSTERONE RELEASE ANDROGEN BINDING PROTEIN WHICH BINDS TESTOSTERONE; THEREBY INCREASING TESTOSTERONE CONCENTRATION WITHIN THE SEMINIFEROUS TUBULES AND STIMULATING SPERMATOGENESIS
100 MALE REPRODUCTIVE SYSTEM EFFERENT DUCTULES CONNECT RETE TESTIS WITH EPIDIDYMIS IRREGULAR LUMINAL APPEARANCE DUE TO TALL CILIATED CELLS AND SHORT NON-CILIATED CELLS CILIATED CELLS BEAT TOWARD EPIDIDYMIS; THIN LAYER OF SMOOTH MUSCLE ALSO AIDS MOVEMENT INTO EPIDIDYMIS
101 MALE REPRODUCTIVE SYSTEM EPIDIDYMIS RECEIVES EFFERENT DUCTULES DIVIDED INTO HEAD, BODY, AND TAIL PSEUDOSTRATIFIED EPITHELIUM CONSISTING OF PRINCIPAL AND BASAL CELLS SMOOTH MUSCLE IN HEAD AND TAIL CONTRACT SPONTANEOUSLY; SMOOTH MUSCLE IN TAIL REQUIRES SYMPATHETIC INNERVATION FOR CONTRACTION
102 EPIDIDYMIS STEREOCILIA MATURE SPERM
103 EFFERENT DUCTULES EPIDIDYMIS
104 EFFERENT DUCTULES EPIDIDYMIS
105 EPIDIDYMIS
106 MALE REPRODUCTIVE SYSTEM VAS DEFERENS CONNECTS EPIDIDYMIS WITH SEMINAL VESICLES PSEUDOSTRATIFIED COLUMNAR EPITHELIUM SMOOTH MUSCLE ARRANGED IN 3 LAYERS SMOOTH MUSCLE CONTRACTION VIA SYMPATHETIC STIMULATION DURING EJACULATION
107 VAS DEFERENS MALE REPRODUCTIVE SYSTEM Ductus Deferens and Ejaculatory Duct Runs from the epididymis through the inguinal canal into the pelvic cavity Its terminus expands to form the ampulla and then joins the duct of the seminal vesicle to form the ejaculatory duct Propels sperm from the epididymis to the urethra Vasectomy cutting and ligating the ductus deferens, which is a nearly 100% effective form of birth control
108 VAS DEFERENS H&E
109 MALE REPRODUCTIVE SYSTEM SEMINAL VESICLES MUCOSA HIGHLY FOLDED EPITHELIUM PSEUDOSTRATIFIED SECRETIONS ARE HIGH IN FRUCTOSE AND BASIC REGULAR SMOOTH MUSCLE CONTRACTS DURING EJACULATION
110 MALE REPRODUCTIVE SYSTEM SEMINAL VESICLES EPITHELIUM PSEUDOSTRATIFIED
111 MALE REPRODUCTIVE SYSTEM PROSTATE SIMPLE OR PSEUDOSTRATIFIED COLUMNAR EPITHELIUM TUBULOALVEOLAR GLANDS WHICH EMPTY INTO URETHRA PROSTATIC SECRETIONS RICH IN CITRIC ACID, ACID PHOSPHATASE, AND PROTEOLYTIC ENZYMES
112 MALE REPRODUCTIVE SYSTEM PROSTATE SIMPLE OR PSEUDOSTRATIFIED COLUMNAR EPITHELIUM
113 MALE REPRODUCTIVE SYSTEM PROSTATE PROSTATIC CONCRETIONS - precipitation of secretory product
114 PENIS CC CC URETHRA CS
115 PENIS ERECTILE BODIES
116 Sustentacular (Sertoli) cells Nurse cells Extend from basal lamina to lumen Connected to each other by tight junctions Nourish spermatogenic cells Transport spermatogenic cells Phagocytize excess cytoplasm Secretions regulate spermatogenesis 24.4c
117
118 Sustentacular cells 2 Sertoli cells with associated spermatogenesis cells. 24.4c
119 Interstitial (Leydig) cells Secretes testosterone ser for steroid production Controlled by LH from pituitary 24.3b
120 The Ductus Deferens and Accessory Glands Figure 28.10a-e
121 Accessory glands Seminal vesicles Active secretory gland Contributes ~60% total volume of semen Secretions contain fructose, prostaglandins, fibrinogen 60% of semen Fructose to nourish sperm
122 Accessory glands Prostate gland Secretes slightly acidic prostate fluid Bulbourethral glands Secrete alkaline mucus with lubricating properties
123 PROSTATE
124 Prostate Macroscopically the prostrate can be divided into lobes, lobes In good histological sections it is possible to distinguish three concentric zones, which surround the prostatic part of the urethra. The peripheral zone contains large, so-called main glands, whose ducts run posteriorly to open into the urethra. The internal zone consists of the so-called submucosal glands, whereas the innermost zone contains mucosal glands. This subdivision of the prostate is of clinical importance. With age the prostate becomes enlarged due to benign nodular hyperplasia. hyperplasia The onset age of these hyperplastic changes is 45. About 3/4 of the males above 60 are affected of which half will be symptomatic. This condition affects the mucosal glands. Cancer of the prostate, which is the second most common malignant tumor in western males, involves the peripheral zone.
125 During orgasm, sperm is transmitted from the ductus deferens into the male urethra via the ejaculatory ducts, which lie within the prostate gland. The prostate is sometimes referred to as the "male G-spot". Some men are able to achieve orgasm solely through stimulation of the prostate gland, such as prostate massage or receptive anal intercourse. Men who report the sensation of prostate stimulation often give descriptions similar to female's accounts of G-spot stimulation
126 Function of the Prostate Gland The prostate gland secretes a thin, milky fluid that contains calcium, citrate ion, phosphate ion, a clotting enzyme, and a profibrinolysin. During emission, the capsule of the prostate gland contracts simultaneously with the contractions of the vas deferens so that the thin, milky fluid of the prostate gland adds further tothe bulk of the semen. A slightly alkaline characteristic of the prostatic fluid may be quite important for successful fertilization of the ovum, because the fluid of the vas deferens is relatively acidic owing to the presence of citric acid and metabolic end products of the sperm and, consequently, helps to inhibit sperm fertility. Also, the vaginal secretions of the female are acidic (ph of 3.5 to 4.0). Sperm do not become optimally motile until the ph of the surrounding fluids rises to about 6.0 to 6.5. Consequently, it is probable that the slightly alkaline prostatic fluid helps to neutralize the acidity of the other seminal fluids during ejaculation, and thus enhances the motility and fertility of the sperm.
127
128
129 Corpora amylacea Are small hyaline masses of unknown significance found in the prostate gland, neuroglia, and pulmonary alveoli. They are derived from degenerate cells or thickened secretions and occur more frequently with advancing age. While their significance is unknown, they can be used to identify these organs microscopically
130 Prostate Gland Prostate gland Surrounds prostatic urethra 30% of semen Supports sperm 24.9
131 The prostate gland is shaped like an inverted cone and lies just below the neck of the urinary bladder. It is about 5 cm (3 inches) long and 3-4cm wide. The urethra, which runs from the bladder through the middle of the prostate gland and through the penis, carries urine from the bladder. The smooth muscle of the urethra is the internal urinary sphincter. Just below the prostate gland is a muscular diaphragm that acts as the external urinary sphincter. This sphincter, which encircles the urethra, is under both reflex and voluntary control Along the back wall of the urethra in the prostate, there is an elevation called the verumontanum, and it is into this elevation that sperm (through the ejaculatory ducts) and spermatic secretions from the seminal vesicles and prostate enter the urethra
132
133 PS Level ng/ml Condition <4 Normal 4 to 10 Borderline >10 Abnormally High
134 BPH
135
136
137 Ducts Epididymis Ductus deferens Ejaculatory duct (urethra) 24.1
138 Epididymis Located in scrotum Between seminiferous tubules and vas deferens ~6 m long 24.3a
139 Epididymis Pseudostratified columnar epithelium With stereocilia (long microvilli) Smooth muscle Sperm mature and stored 24.6a
140 Epididymis:
141 Ductus (vas) deferens From scrotum to pelvis Forms ejaculatory duct with seminal vesicle duct Empties into prostatic urethra Thick muscularis Propels sperm during ejaculation 24.1
142 Ductus deferens Microscopic anatomy Pseudostratified epithelium Lamina propria Muscularis Inner longitudinal Middle circular Outer longitudinal 24.6b
143 Urethra Shared with urinary system Prostatic urethra Membranous urethra Spongy (penile) urethra 24.8
144 MALE REPRODUCTIVE SYSTEM URETHRA PROSTATIC, MEMBRANOUS, SPONGY (PENILE)
145 Urethra Conveys both urine and semen (at different times) Consists of three regions Prostatic portion surrounded by the prostate Membranous Membranou lies in the urogenital diaphragm Spongy, or penile runs through the penis and opens to the outside at the external urethral orifice
146 Ejaculation Sympathetic activation Peristaltic contraction of smooth muscles in ducts and glands ejaculation Constriction of arteries blood pressure in erectile bodies 24.8
147
148 Brain-Testicular Axis Hormonal regulation of spermatogenesis and testicular androgen production involving the hypothalamus, anterior pituitary gland, the testes Testicular regulation involves three sets of hormones: GnRH, GnRH, from the hypothalamus stimulates the pituitary to produce gonadotropins: gonadotropins Follicle stimulating hormone (FSH) Luteinizing hormone (LH) Gonadotropins, Gonadotropins, directly stimulate the testes Testicular hormones, which exert negative feedback controls
149 Hormonal Regulation of Testicular Function The hypothalamus releases gonadotropinreleasing hormone (GnRH) GnRH stimulates the anterior pituitary to secrete FSH and LH FSH stimulates sperm production by causing sustentacular cells to release androgen-binding protein (ABP) ABP prompts spermatogenic cells to bind and concentrate testosterone LH stimulates interstitial cells to release testosterone Stimulates spermatogenesis Causes secondary sexual characteristics Feedback inhibition on the hypothalamus and pituitary results from: Rising levels of testosterone Increased inhibin
150 Mechanism and Effects oftestosterone Activity Testosterone is synthesized from cholesterol It must be transformed to exert its effects on some target cells Prostate it is converted into dihydrotestosterone (DHT) before it can bind within the nucleus Neurons it is converted into estrogen to bring abou stimulatory effects in certain neurons Testosterone targets all accessory organs and its deficiency causes these organs to atrophy
151 Male Secondary Sex Characteristics Male hormones make their appearance at puberty and induce changes in nonreproductive organs, including Appearance of pubic, axillary, and facial hair Enhanced growth of the chest and deepening of the voice Skin thickens and becomes oily Bones grow and increase in density Skeletal muscles increase in size and mass Testosterone is the basis of libido in both males and females
Primary sex organs (gonads): testes and ovaries. Accessory reproductive organs: ducts, glands, and external genitalia
 Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Primary sex organs (gonads): testes and ovaries Produce sex cells (gametes) Secrete steroid sex hormones Androgens (males) Estrogens and progesterone (females) Accessory reproductive
Male Reproductive System Dr. Gary Mumaugh
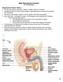 Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
Male Reproductive System Dr. Gary Mumaugh Reproductive System Basics Primary sex organs (gonads) testes in males, ovaries in females Gonads produce sex cells called gametes (gametes means spouses) and
The Reproductive System
 PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
PowerPoint Lecture Slide Presentation by Patty Bostwick-Taylor, Florence-Darlington Technical College The Reproductive System 16PART A The Reproductive System Gonads primary sex organs Testes in males
Male Reproductive System. Dr Maan Al-Abbasi PhD, MSc, MBChB, MD
 Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
Male Reproductive System Dr Maan Al-Abbasi PhD, MSc, MBChB, MD Learning Objectives 1. Describe the General Anatomy of the Male Reproductive System 2. Identify the structures that are related to the prostate.
The Male Reproductive System
 The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
The Male Reproductive System The male reproductive system Testes Genital ducts Accessory sex glands: seminal vesicles prostate bulbourethral glands External genitalia: penis Structure of the Testis Tunica
- production of two types of gametes -- fused at fertilization to form zygote
 Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
Male reproductive system I. Sexual reproduction -- overview - production of two types of gametes -- fused at fertilization to form zygote - promotes genetic variety among members of a species -- each offspring
The Reproductive System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 16 The Reproductive System Slides 16.1 16.20 Lecture Slides in PowerPoint by Jerry L. Cook The Reproductive System Gonads
The Reproductive System
 16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
16 PART A The Reproductive System PowerPoint Lecture Slide Presentation by Jerry L. Cook, Sam Houston University ESSENTIALS OF HUMAN ANATOMY & PHYSIOLOGY EIGHTH EDITION ELAINE N. MARIEB The Reproductive
Histology of Male Reproductive System
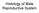 Histology of Male Reproductive System Lecture Objectives Describe the histological features of the male reproductive system Male Reproductive System The male structures of reproduction include the: testes,
Histology of Male Reproductive System Lecture Objectives Describe the histological features of the male reproductive system Male Reproductive System The male structures of reproduction include the: testes,
Male Reproductive System
 Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive System organs that function in: gamete and hormone production not all in abdominal cavity paired testicles = controlled by LH & FSH duct systems accessory glands Testis: Gross Histology
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization
 Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Male Reproductive Structures I. Overview A. Main functions: 1. Produce a haploid male gamete (sperm) 2. Deposit sperm in the female so fertilization may occur! A. Scrotum 1. Muscular pouch that holds the
Reproductive System Purpose General Structures Male Structures Functions Female Anatomy Structures Functions Clinical Applications
 The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
The Reproductive System: Male, Ch 23 Outline of class lecture After studying the male reproductive system you should be able to: 1. Define the purpose of reproduction and identify the general organs of
Chapter 26: Reproductive Systems. Male 11/29/2015. Male reproductive system is composed of... BIO 218 Fall Gonads (testes)
 Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Chapter 26: Reproductive Systems BIO 218 Fall 2015 Male Male reproductive system is composed of... Gonads (testes) Duct system (epididymis, ductus deferens, ejaculatory ducts, urethra) Accessory sex glands
Pathology of Male Reproductive System 1
 Pathology of Male Reproductive System 1 Professor dr Ali Hassan Altimimi Professor of Pathology& Histology MSc, PHD, MD(UK) MALE REPRODUCTIVE SYSTEM The internal male genitalia consist of the testes with
Pathology of Male Reproductive System 1 Professor dr Ali Hassan Altimimi Professor of Pathology& Histology MSc, PHD, MD(UK) MALE REPRODUCTIVE SYSTEM The internal male genitalia consist of the testes with
MALE REPRODUCTIVE SYSTEM
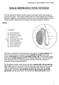 MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
MALE REPRODUCTIVE SYSTEM The male reproductive system consists of primary sex organs (testes) and secondary or accessory sex organs. The secondary organs consist of a series of genital ducts (ductules
The Male Reproductive System
 The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
The Male Reproductive System YONG-MEI CHEN ( 陈咏梅 ) Dept. of Anatomy, Histology & Embryology Peking Union Medical College Tel:69156461 E-mail address: pumc_he@126.com Content Spermatogenesis Spermiogenesis
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM
 Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Human Anatomy Unit 3 REPRODUCTIVE SYSTEM In Anatomy Today Male Reproductive System Gonads = testes primary organ responsible for sperm production development/maintenan ce of secondary sex characteristics
Basic histology 5/4/2015
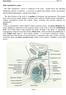 Male reproductive system The male reproductive system is composed of the testes, genital ducts (the adjoining epididymis, and the vas deferens, a accessory sex glands (the seminal vesicles, the prostrate
Male reproductive system The male reproductive system is composed of the testes, genital ducts (the adjoining epididymis, and the vas deferens, a accessory sex glands (the seminal vesicles, the prostrate
Chapter 28: REPRODUCTIVE SYSTEM: MALE
 Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Chapter 28: REPRODUCTIVE SYSTEM: MALE I. FUNCTIONAL ANATOMY (Fig. 28.1) A. Testes: glands which produce male gametes, as well as glands producing testosterone 2. Seminiferous tubules (Fig.28.3; 28.5) a.
Histology of Male Reproductive system (1)
 Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Histology of Male Reproductive system (1) Prof. Dr. Malak A. Al-yawer Learning Objectives At the end of this lecture, the medical student will be able to: State the organization of the testis Define seminiferous
Male Reproductive System
 Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Male Reproductive System Constitution of male reproductive system Genital gland ----testis Genital ducts epididymis / ductus deferens / urinary duct Accessory sex glands Penis prostate gland Seminal vesicle
Male Reproductive System
 21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
21-1 21-2 Reproductive System Male Reproductive System Genital Tract In males the testes, held outside the body in the scrotum (optimum temp of about 35 0 C), produce sperm. Sperm mature in coiled tubes
Anatomy Lecture Notes Chapter 24
 primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
primary sex organs = gonads produce gametes secrete hormones that control reproduction secondary sex organs = accessory structures Development and Differentiation A. gonads develop from mesoderm starting
Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature
 REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
REPRODUCTION Testes (male gonads) -Produce sperm -Produce sex hormones -Found in a sac called the scrotum -Suspended outside of the body cavity for temperature reduction -Testes wall made of fibrous connective
MALE REPRODUCTIVE SYSTEM
 1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
1 MALE REPRODUCTIVE SYSTEM SCPA 602 Anatomical Basis for Pathological Study Updated: 20.09.2018 Lect. Nisamanee Charoenchon, PhD nisamanee.cha@mahidol.ac.th Department of Pathobiology, Mahidol University
Lecture 28, The Reproductive System
 Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
Fundamentals of Anatomy & Physiology Lecture 28, The Reproductive System SIXTH EDITION Frederic H. Martini Lecturer: Dr. Barjis Room: P313 Phone: (718) 260-5285 E-Mail: ibarjis@citytech.cuny.edu Copyright
SISTEMA REPRODUCTOR (LA IDEA FIJA) Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
SISTEMA REPRODUCTOR (LA IDEA FIJA) How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development,
Physiologic Anatomy of the Male Sexual Organs
 Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Reproductive and Hormonal Functions of the Male The reproductive functions of the male can be divided into three major subdivisions: (1) spermatogenesis, which means simply the formation of sperm; (2)
Male Reproductive Physiology
 Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
Male Reproductive Physiology Overview Anatomy Function Endocrine and spermatogenesis Testis epididymus,vas deferens,seminal vesicles and prostate Hypothalamic pituitary testicular axis Hormones of the
FIGURE The tunica albuginea is a connective tissue capsule forming the outer part of each testis.
 Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
Testicular Histology (see p. 1034 in text) FIGURE 28.3 1. The tunica albuginea is a connective tissue capsule forming the outer part of each testis. 2. Septa are extensions of the tunica albuginea that
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception
 PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
PELVIS II: FUNCTION TABOOS (THE VISCERA) Defecation Urination Ejaculation Conception REVIEW OF PELVIS I Pelvic brim, inlet Pelvic outlet True pelvis-- --viscera Tilt forward Mid-sagital views-- --how the
The Repr duct ve System. Function: producing offspring
 The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
The Repr duct ve System Function: producing offspring Anatomy of male reproductive system Location: The reproductive organs are classified as external and internal genitalia. The external genitalia are
Aniko Szabo Hill 1 of 12
 Common Function: produce offsprings endocrine glands: sex hormone production Primary organs or gonads: sex cell or gametes production Secondary or accessory organs: glands nourish gametes ducts transport
Common Function: produce offsprings endocrine glands: sex hormone production Primary organs or gonads: sex cell or gametes production Secondary or accessory organs: glands nourish gametes ducts transport
To General Embryology Dr: Azza Zaki
 Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
Introduction To General Embryology The Human Development is a continuous process that begins when an ovum from a female is fertilized by a sperm from a male. Cell division, growth and differentiation transform
MALE REPRODUCTIVE SYSTEM
 MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
MALE REPRODUCTIVE SYSTEM 1. The male reproductive system is made up of the following structures, EXCEPT: a. prostate; b. testicle; c. spermatic ducts; d. vestibular bulbs; e. seminal vesicles. 2.The testicle:
The Reproductive System
 Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Essentials of Anatomy & Physiology, 4th Edition Martini / Bartholomew The Reproductive System PowerPoint Lecture Outlines prepared by Alan Magid, Duke University Slides 1 to 84 Overview of Reproduction
Chapter 22 Reproductive Systems. Male Reproductive Organs. Male Reproductive Organs. Specialized to produce, maintain the male sex cells (sperm)
 Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Chapter 22 Reproductive Systems Male reproductive organs 1 Male Reproductive Organs posterior view 2 Male Reproductive Organs Specialized to produce, maintain the male sex cells (sperm) Transport these
Outline. Male Reproductive System Testes and Sperm Hormonal Regulation
 Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Outline Male Reproductive System Testes and Sperm Hormonal Regulation Female Reproductive System Genital Tract Hormonal Levels Uterine Cycle Fertilization and Pregnancy Control of Reproduction Infertility
Grade 9 Science - Human Reproduction
 Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Grade 9 Science - Human Reproduction The human reproductive system is a series of organs that work together for one purpose: reproduction (creating new humans). Each part has a specific role in the reproductive
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems 3. Male Reproductive anatomy and physiology. Testes = paired
Reproductive System. Where it all begins
 Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Reproductive System Where it all begins When it comes the reproductive anatomy of my gender, I would rate my knowledge (1 very poor, 10 excellent) When it comes the reproductive anatomy of the opposite
Male Reproduction Organs. 1. Testes 2. Epididymis 3. Vas deferens 4. Urethra 5. Penis 6. Prostate 7. Seminal vesicles 8. Bulbourethral glands
 Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
Outline Terminology Human Reproduction Biol 105 Lecture Packet 21 Chapter 17 I. Male Reproduction A. Reproductive organs B. Sperm development II. Female Reproduction A. Reproductive organs B. Egg development
describe the parts and function of semen and the glands that contribute to it
 You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
You need to be able to: describe spermatogenesis (How is sperm made?) describe the anatomy of a sperm describe the parts and function of semen and the glands that contribute to it How is sperm made? Spermatogenesis
Study Guide Answer Key Reproductive System
 Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
Biology 12 Human Biology Textbook: BC Biology 12 Study Guide Answer Key Reproductive System 1. Distinguish between a gamete and a gonad using specific examples from the male and female systems. Gonads
HISTOLOGY OF THE MALE REPRODUCTIVE SYSTEM
 HISTOLOGY OF THE MALE REPRODUCTIVE SYSTEM Learning Objectives: 1. Describe the histology of and identify, in order, the passageways through which sperm pass as they exit from the body. 2. Describe the
HISTOLOGY OF THE MALE REPRODUCTIVE SYSTEM Learning Objectives: 1. Describe the histology of and identify, in order, the passageways through which sperm pass as they exit from the body. 2. Describe the
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5)
 IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
IB 140 Midterm #1 PRACTICE EXAM (lecture topics 1-5) For all the questions on this exam, the correct answer is the single best answer that is available in the answer key. 1) Which of the following is NOT
STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM
 Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Unit 7A STRUCTURE AND FUNCTION OF THE MALE REPRODUCTIVE SYSTEM LEARNING OBJECTIVES 1. Learn the structures of the male reproductive system. 2. Learn the functions of the male reproductive system. 3. Learn
Lab #9: Kidney: Gross Anatomy & Histology
 Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
Name Date Lab #9: Kidney: Gross Anatomy & Histology Lab #10: Male Reproductive System: Human Models & Histology Lab #11: Female Reproductive System: Human Models & Histology Stuff to Know Dr. L. Bacha
Chapter 22 The Reproductive System (I)
 Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Chapter 22 The Reproductive System (I) An Overview of Reproductive Physiology o The Male Reproductive System o The Female Reproductive System 22.1 Reproductive System Overview Reproductive system = all
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question.
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) Which of the following hormones controls the release of anterior pituitary gonadotropins? A) LH
18 Urinary system. 19 Male reproductive system. Female reproductive system. Blok 11: Genital and Urinary Tract Diseases
 Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
Blok 11: Genital and Urinary Tract Diseases 18 Urinary System 19 Male Genital System 20 Female Genital System 18 Urinary system You should be able to: 1. Describe the structures and associated functions
The Reproductive System
 The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
The Reproductive System The Reproductive System Gonads primary sex organs Testes in males Ovaries in females Gonads produce gametes (sex cells) and secrete hormones Sperm male gametes Ova (eggs) female
Male reproduction. Cross section of Human Testis ผศ.ดร.พญ.ส ว ฒณ ค ปต ว ฒ ภาคว ชาสร รว ทยา คณะแพทยศาสตร ศ ร ราชพยาบาล 1. Aims
 Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Aims Male reproduction Male reproductive structure Spermatogenesis ส ว ฒณ ค ปต ว ฒ ห อง 216 โทร: 7578 Hypothalamo-pituitary-testicular axis Male sex hormone action Male reproductive structure Male reproductive
Human Sexuality - Ch. 2 Sexual Anatomy (Hock)
 Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
Human Sexuality - Ch. 2 Sexual Anatomy (Hock) penis penile glans corona frenulum penile shaft erection foreskin circumcision corpora cavernosa corpus spongiosum urethra scrotum spermatic cords testicles
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM
 LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
LABORATORY EXERCISES FOR MALE REPRODUCTIVE SYSTEM Slide #101 (1096). Testis, rat. sustentacular ( Sertoli ) cells Nuclei of Sustentacular cells Leydig cells Spermatogonia Spermatocytes Spermatids pale
Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems
 CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
CH. 15 - REPRODUCTIVE SYSTEM Objectives: 1. Review male & female reproductive anatomy 2. Gametogenesis & steroidogenesis 3. Reproductive problems Review of Male Reproductive Anatomy Fig 15.9 Vas deferens
BIOL 2402 Reproductive Systems
 Collin College Dr. Chris Doumen BIOL 2402 Reproductive Systems 1 Reproductive System Most systems between males and females in the human body are similar in structure. The exception of course are the organs
Collin College Dr. Chris Doumen BIOL 2402 Reproductive Systems 1 Reproductive System Most systems between males and females in the human body are similar in structure. The exception of course are the organs
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE
 ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
ESUR SCROTAL AND PENILE IMAGING WORKING GROUP MULTIMODALITY IMAGING APPROACH TO SCROTAL AND PENILE PATHOLOGIES 2ND ESUR TEACHING COURSE NORMAL ANATOMY OF THE SCROTUM MICHAEL NOMIKOS M.D. F.E.B.U. UROLOGICAL
Male Anatomy. testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics
 Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Male Anatomy Male Anatomy Primary Organ testes, genetically determined in mammals - testis releases hormones that then control the development of secondary sex characteristics 1) Secondary Organs internal
Unit 15 ~ Learning Guide
 Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Unit 15 ~ Learning Guide Name: INSTRUCTIONS Complete the following notes and questions as you work through the related lessons. You are required to have this package completed BEFORE you write your unit
Male reproductive system The physiology of sexual act
 Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
Male reproductive system The physiology of sexual act Gabriella Kékesi 65. The development and physiology of the male reproductive system. The physiology of the sexual act Define chromosomal, gonadal and
Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport
 Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport (epididymis, ductus deferens(vas deferens), ejaculatory
Male Reproductive System I. Overview A. gonads organs producing sex cells (gametes) = B. support for gonads = C. ducts for storage and transport (epididymis, ductus deferens(vas deferens), ejaculatory
REPRODUCTIVE SYSTEM OBJECTIVES
 REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
REPRODUCTIVE SYSTEM OBJECTIVES OBJECTIVES: 1. List the organs and functions of the reproductive system. Female Organs Male Organs Functions 1 OVARIES 1 TESTES 1 Produce gametes 2 fallopian tubes 2 scrotum
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes
 Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Functions of male Reproductive System: produce gametes deliver gametes protect and support gametes Spermatogenesis occurs in the testes after puberty. From the testes they are deposited into the epididymas
Human Reproduction. Human Reproductive System. Scrotum. Male Reproductive System
 Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
Human Reproductive System Human Reproduction Chapter 41 Contraceptives Scrotum Testes Epididymus Vas Deferens Seminal Vesicles Prostate Gland Bulbourethral Gland Penis Scrotum Sac of smooth muscle tissue
a. the tail disappears b. they become spermatids c. they undergo capacitation d. they have been stored in the uterus for several days
 (2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
(2 points each) Multiple Choice. Read each question thoroughly before answering. From the choices available, choose the answer that is the most correct. Place all answers on the accompanying answer sheet.
Student Academic Learning Services Page 1 of 5 Reproductive System Practice
 Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
Student Academic Learning Services Page 1 of 5 Reproductive System Practice Fill in the blanks using the words listed: accessory glands, vas deferens, penis, scrotum, fallopian tube, testes, urethra, vagina,
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 27.3 Using Figure 27.3, match the following: 1) The stage called ovulation. 2) Corpus
Human Reproductive System
 Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
Human Reproductive System I. The male reproductive anatomy is a delivery system for sperm. A. The male=s external reproductive organs consist of the scrotum and penis. 1. The penis is the external organ
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O.
 UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O. OBJECTIVES Introduction Functional anatomy of male sex organ Functional anatomy of female sex organ
UNIVERSITY OF MEDICAL SCIENCES, ONDO DEPARTMENT OF PHYSIOLOGY REPRODUCTION LECTURER: MR. AKINOLA A.O. OBJECTIVES Introduction Functional anatomy of male sex organ Functional anatomy of female sex organ
REPRODUCCIÓN. La idea fija. Copyright 2004 Pearson Education, Inc., publishing as Benjamin Cummings
 REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
REPRODUCCIÓN La idea fija How male and female reproductive systems differentiate The reproductive organs and how they work How gametes are produced and fertilized Pregnancy, stages of development, birth
Health Science: the structures & functions of the reproductive system
 Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Health Science: the structures & functions of the reproductive BELLWORK 1. List (4) careers that are r/t the Reproductive, Urinary, and Endocrine Systems 2. Copy down the following terms: -ologist = one
Bio 104 Reproductive System
 63 Lecture Outline: Reproductive System Hole s HAP [Chapters 22, 23] I. Introduction A. Primary sex characteristics Male Female B. Secondary sex characteristics Male: 9 14 yrs. Reproductive development
63 Lecture Outline: Reproductive System Hole s HAP [Chapters 22, 23] I. Introduction A. Primary sex characteristics Male Female B. Secondary sex characteristics Male: 9 14 yrs. Reproductive development
Overview of Anatomy and Physioloy II Second Year Students
 WELCOME University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad, Ph.D. Electrolyte and Mineral Physiology
WELCOME University of Baghdad College of Nursing Department of Basic Medical Sciences Overview of Anatomy and Physioloy II Second Year Students Asaad Ismail Ahmad, Ph.D. Electrolyte and Mineral Physiology
Male Reproductive System. Figure 80-1 Copyright 2011 by Saunders, an imprint of Elsevier Inc.
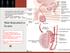 Male reprodctive system anatomy: briefly: composed of testis and external genetilia, the testis seminefrous tubules with space for spermatogenesis...the path is from the epidedimys-->vas defans-->prostatic
Male reprodctive system anatomy: briefly: composed of testis and external genetilia, the testis seminefrous tubules with space for spermatogenesis...the path is from the epidedimys-->vas defans-->prostatic
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Indifferent ducts of embryo Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Y chromosome present Y chromosome absent Phenotypic sex is depends on development of external
Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor)
 Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Indifferent ducts of embryo Y chromosome present Y chromosome absent Male Female penis ovary uterus vagina testis Biology of gender Sex chromosomes determine gonadal sex (testis-determining factor) Phenotypic
Chapter 14 The Reproductive System
 Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Biology 12 Name: Reproductive System Per: Date: Chapter 14 The Reproductive System Complete using BC Biology 12, page 436-467 14. 1 Male Reproductive System pages 440-443 1. Distinguish between gametes
Chapter 14 Reproduction Review Assignment
 Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Date: Mark: _/45 Chapter 14 Reproduction Review Assignment Multiple Choice Identify the choice that best completes the statement or answers the question. 1. Use the diagram above to answer the next question.
Human Reproductive Anatomy The female anatomy first just the reproductive parts:
 Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Human Reproduction: Structures, Functions, and Hormones Human reproduction differs from the mechanisms in lower vertebrates and many invertebrates. We depend on internal fertilization sperm are deposited
Biology of Reproduction-Biol 326
 Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
Biology of Reproduction-Biol 326 READ ALL INSTRUCTIONS CAREFULLY. ANSWER ALL THE QUESTIONS ON THE ANSWER SHEET. THE ANSWER ON THE ANSWER SHEET IS YOUR OFFICIAL ANSWER REGARDLESS OF WHAT YOU MARK ON THE
1. Both asexual and sexual reproduction occur in the animal kingdom
 1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
1. Both asexual and sexual reproduction occur in the animal kingdom Asexual reproduction involves the formation of individuals whose genes all come from one parent. There is no fusion of sperm and egg.
Lab Activity 33. Anatomy of the Reproductive System. Portland Community College BI 233
 Lab Activity 33 Anatomy of the Reproductive System Portland Community College BI 233 Scrotum Sac of skin and superficial fascia that hangs outside the abdominopelvic cavity at the root of the penis Contains
Lab Activity 33 Anatomy of the Reproductive System Portland Community College BI 233 Scrotum Sac of skin and superficial fascia that hangs outside the abdominopelvic cavity at the root of the penis Contains
6.7 IN. Continuity through Reproduction. What are the differences between male and female gametes? Discuss their formation and physical attributes.
 6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
6.7 IN What are the differences between male and female gametes? Discuss their formation and physical attributes. Males - 4 sperm per parent cell; Females - 1 ovum per parent cell Sperm - motile (tail);
Male Reproductive System
 Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Male Reproductive System The male reproductive system consists of a number of sex organs that are part of the reproductive process. The following sections describe the function of each part of the male
Reproductive Systems. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 17 Reproductive Systems Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Special Parts: Gender. Why Have Sex?
 Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Why Have Sex? Lots of animals clone themselves... 100% of their genes are passed on! Sex requires sharing, it s expensive (time, mate selection, special parts, prenuptial gifts...) So why do it? Special
Individually, humans don t need to reproduce to survive. But to survive as a species,
 Chapter 13 Why Ask Y?: The Male Reproductive System In This Chapter Explaining the parts of male reproduction Understanding meiosis and what happens to chromosomes Individually, humans don t need to reproduce
Chapter 13 Why Ask Y?: The Male Reproductive System In This Chapter Explaining the parts of male reproduction Understanding meiosis and what happens to chromosomes Individually, humans don t need to reproduce
FEMALE REPRODUCTIVE SYSTEM
 FEMALE REPRODUCTIVE SYSTEM UTERUS (made up of muscular walls, a lining called the endometrium, and a cervix. The uterus is also called womb ) houses and protects embryo/fetus/baby allows nutrient & waste
FEMALE REPRODUCTIVE SYSTEM UTERUS (made up of muscular walls, a lining called the endometrium, and a cervix. The uterus is also called womb ) houses and protects embryo/fetus/baby allows nutrient & waste
Embryology 3. Spermatogenesis:
 Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Embryology 3 Spermatogenesis: The 2 testis in males are each divided into lobes and lobules by connective tissue septa forming 250 lobule and in each lobule there are 1 to 4 seminefrous tubule ( so almost
Urinary System Chapter 16
 Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Urinary System Chapter 16 1 Urology- the branch of medicine that treats male and female urinary systems as well as the male reproductive system. Nephrology- the scientific study of the anatomy, physiology,
Sperm production. Sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
 Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production Ductus deferens Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Sperm production. Sperm production. Controlling sperm production. Meiosis. Mitosis. The cells of Leydig in testes secrete
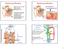 Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
Ductus deferens Sperm production Epididymis The cells of Leydig in testes secrete Seminiferous testosterone (T) tubules T secreted at puberty produces 2 o sex characteristics, spermatogenesis, & maintain
The Reproductive System
 Biology 212: Anatomy and Physiology II The Reproductive System References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapters
Biology 212: Anatomy and Physiology II The Reproductive System References: Saladin, KS: Anatomy and Physiology, The Unity of Form and Function 8 th (2018). Required reading before beginning this lab: Chapters
Development of the Genital System
 Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
Development of the Genital System Professor Alfred Cuschieri Department of Anatomy University of Malta The mesonephros develops primitive nephrotomes draining into a mesonephric duct nephrotome mesonephric
under its influence, male development occurs; in its absence, female development is established.
 Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
Sex differentiation is a complex process that involves many genes, including some that are autosomal. The key to sexual dimorphism is the Y chromosome, which contains the testis determining gene called
 MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
MOCK TEST I (HUMAN REPRODUCTION) 1. In human transfer of sperms into female genital tract is called as 1) Fertilization 2) Implantation 3) Insemination 4) Gestation 2. In male human scrotum maintains the
For more information about how to cite these materials visit
 Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
Author: A. Kent Christensen, Ph.D., 2009 License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution Share Alike 3.0 License: http://creativecommons.org/licenses/by-sa/3.0/
HUMAN REPRODUCTION SYSTEM
 HUMAN REPRODUCTION SYSTEM The human reproductive system usually involves internal fertilization by sexual intercourse. During this process, the male inserts his erect penis into the female's vagina and
HUMAN REPRODUCTION SYSTEM The human reproductive system usually involves internal fertilization by sexual intercourse. During this process, the male inserts his erect penis into the female's vagina and
