Evolution of semi-quantitative whole joint assessment of knee OA: MOAKS (MRI Osteoarthritis Knee Score)
|
|
|
- Edgar Morrison
- 5 years ago
- Views:
Transcription
1 Osteoarthritis and Cartilage 19 (2011) 990e1002 Evolution of semi-quantitative whole joint assessment of knee OA: MOAKS (MRI Osteoarthritis Knee Score) D.J. Hunter y *, A. Guermazi z, G.H. Lo xk, A.J. Grainger {, P.G. Conaghan #, R.M. Boudreau yy, F.W. Roemer zzz y Rheumatology Department, Royal North Shore Hospital, Northern Clinical School, University of Sydney, Sydney, NSW, Australia z Quantitative Imaging Center (QIC), Department of Radiology, Boston University, School of Medicine, Boston, MA, USA x Medical Care Line, Research Care Line, and Houston Health Services Research and Development (HSR&D) Center of Excellence, Michael E. DeBakey Veterans Administration Medical Center, Houston, TX, USA k Department of Medicine, Section of Immunology, Allergy and Rheumatology, Baylor College of Medicine, Houston, TX, USA { Department of Radiology, Leeds Teaching Hospitals & NIHR Leeds Musculoskeletal Biomedical Research Unit, Leeds, UK # Section of Musculoskeletal Disease, University of Leeds & NIHR Leeds Musculoskeletal Biomedical Research Unit, Leeds, UK yy Department of Epidemiology, Graduate School of Public Health, University of Pittsburgh, Pittsburgh, PA, USA zz Department of Radiology, Klinikum Augsburg, Augsburg, Germany article info summary Article history: Received 28 January 2011 Accepted 11 May 2011 Keywords: MRI Knee osteoarthritis Semi-quantitative score Reliability Objective: In an effort to evolve semi-quantitative scoring methods based upon limitations identified in existing tools, integrating expert readers experience with all available scoring tools and the published data comparing the different scoring systems, we iteratively developed the magnetic resonance imaging (MRI) Osteoarthritis Knee Score (MOAKS). The purpose of this report is to describe the instrument and its reliability. Methods: The MOAKS instrument refines the scoring of bone marrow lesions (BMLs) (providing regional delineation and scoring across regions), cartilage (sub-regional assessment), and refines the elements of meniscal morphology (adding meniscal hypertrophy, partial maceration and progressive partial maceration) scoring. After a training and calibration session two expert readers read MRIs of 20 knees separately. In addition, one reader re-read the same 20 MRIs 4 weeks later presented in random order to assess intra-rater reliability. The analyses presented here are for both intra- and inter-rater reliability (calculated using the linear weighted kappa and overall percent agreement). Results: With the exception of inter-rater reliability for tibial cartilage area (kappa ¼ 0.36) and tibial osteophytes (kappa ¼ 0.49); and intra-rater reliability for tibial BML number of lesions (kappa ¼ 0.54), Hoffa-synovitis (kappa ¼ 0.42) all measures of reliability using kappa statistics were very good (0.61e0.8) or reached near-perfect agreement (0.81e1.0). Only intra-rater reliability for Hoffa-synovitis, and interrater reliability for tibial and patellar osteophytes showed overall percent agreement <75%. Conclusion: MOAKS scoring shows very good to excellent reliability for the large majority of features assessed. Further iterative development and research will include assessment of its validation and responsiveness. Ó 2011 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. Introduction Magnetic resonance imaging (MRI) semi-quantitative scoring of knee osteoarthritis (OA) has proven to be a valuable method for performing multi-feature joint assessment 1,2. Such approaches * Address correspondence and reprint requests to: D.J. Hunter, Rheumatology Department, Northern Clinical School, Royal North Shore Hospital, University of Sydney, St Leonards, Sydney, NSW 2065, Australia. Tel: ; Fax: address: David.Hunter@sydney.edu.au (D.J. Hunter). score, in a semi-quantitative manner, a variety of features that are currently believed to be relevant to the functional integrity of the knee and/or are potentially involved in the pathophysiology of OA. These articular features include articular cartilage morphology, subchondral bone marrow lesions (BMLs) and cysts, osteophytes, the menisci, the anterior and posterior cruciate ligaments, the collateral ligaments, synovitis, joint effusion, bone attrition, intraarticular loose bodies, and periarticular cysts/bursitis. Several methods for semi-quantitative assessment of knee OA have been developed 3e5. The first of the published instruments, the Whole-Organ MRI Score (WORMS), was developed cognizant of the /$ e see front matter Ó 2011 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi: /j.joca
2 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e potential of MRI to provide a measure of all potentially relevant knee OA structures 4. After identifying some limitations with WORMS 6,7, work was undertaken to develop the Boston Leeds OA Knee Score (BLOKS) 5. Both of these tools are in widespread use in various observational studies and clinical trials. Both WORMS and BLOKS have been widely disseminated and used, although the number of direct comparisons of the two instruments to date was quite limited 5. Recently the validity and reliability of WORMS and BLOKS was compared 8e10. This comparison has been helpful in identifying the relative merits and weaknesses of these instruments with regards to certain features assumed to be most relevant to the natural history of the disease including cartilage, meniscus and BMLs. Both instruments had certain limitations and if one were to use the extant literature on published semi-quantitative scoring instruments the discerning investigator would need to choose from a complex array of measures from these two different instruments. For example, WORMS meniscal scoring method mixes multiple different constructs and for BLOKS, application of the BML scoring system was cumbersome and complex and parts of it seemed redundant. Both of these tools have also undergone unpublished iterations that have made it difficult for the naïve reader to determine the differences between the original instruments description and that which has been used in published research. To facilitate appraisal it is important that iterative developments be made public. A number of large epidemiologic studies and clinical trials are maturing to the point where large scale scoring is commencing, and it is important that iterative evolution of existing instruments occur with past research findings in mind. In an effort to evolve semiquantitative scoring methods based upon limitations identified in existing tools, integrating expert readers experience with all available scoring tools and the published data comparing the different scoring systems, we iteratively developed the MRI OA Knee Score (MOAKS). The purpose of this report is to describe the instrument and its reliability. Methods Upon recognition of the limitations in existing scoring methods iterations were made to elements of the original instruments. The experts (DJH, AG, GHL, AJG, PGC, FR, DG) involved met to consider the limitations of the existing scoring for each pathological feature: BMLs and meniscal abnormalities were the most important areas for revision. The focus of the current exercise was therefore to refine the scoring of BMLs, to include sub-regional assessment, to omit some areas of redundancy in cartilage and BML scoring, and to refine the elements of meniscal morphology. After consensus was reached on the new definitions, a intra- and inter-rater reliability exercise was undertaken. Fig. 1. Subregional division of the patella in the axial plane. Axial T2w image shows the medial (M) and lateral (L) portions of the patella as divided in MOAKS. Note that the patellar apex is part of the medial subregion (arrow). 1. The patella is divided into two sub-regions, the medial and lateral patella on the axial view (see Fig. 1). The patellar crista (also called apex) is allocated to the medial subregion. 2. The femur is divided into six sub-regions e medial and lateral trochlea, medial and lateral central femur, and the medial and lateral posterior femur. Method of dividing the sub-regions (see Fig. 2): i. Trochlea is defined as the femoral articular surface of the patellofemoral (PF) joint. For the division between the trochlea and central regions, on the sagittal image a line is drawn tangentially to the anterior aspect of the proximal tibia (at the margin of the tibial plateau) until it intersects the femoral surface. The division between the central femur and the posterior femur is a line constructed vertically from the posterior aspect of the tibia. (The rationale for choosing these Description of MOAKS The MOAKS instrument was developed and tested on images obtained on a 3.0 T MRI system with a dedicated peripheral knee coil. Other systems with different field strengths will need to be evaluated. Delineation of subregional divisions OA can affect one or multiple compartments in the knee. In MOAKS the knee is divided into 14 articular sub-regions for scoring articular cartilage and BMLs and in addition the subspinous region is added for BML scoring: Fig. 2. Anatomical delineation of femur into trochlea (T), central (C) and posterior (P) regions on sagittal projection. Sagittal projection depicts delineation of the tibia into anterior, central and posterior sub-regions, which is divided into equal thirds.
3 992 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e1002 Table I Scoring system for BMLs Size of BML (including volume of any associated cysts) by volume No. of BMLs counted % of lesion that is BML (vs cyst) 0: none 0: none 1: <33% of subregional volume 1: <33% 2: 33e66% of subregional volume 2: 33e66% 3: >66% of subregional volume 3: >66% 1. BMLs and Cysts BMLs and cysts e include areas of presumed BML [areas of ill-delineated signal within the trabecular bone that are hypointense on T1-weighted images and hyperintense on T2-weighted fat-suppressed (fs) images] and associated subarticular bone marrow cysts (defined as well-delineated lesions of fluid equivalent signal directly adjacent to the subchondral plate). Fig. 3. Coronal IW image shows anatomical delineation of the tibia into medial, subspinous (SS) and lateral sub-regions. The femur is divided into the medial and lateral femoral condyle. The intercondylar notch is considered to be part of the medial femur. divisions, as opposed to choosing the meniscal boundaries, was the concern that meniscal subluxation and degeneration would introduce variability into this delineation if used). ii. Anterior and posterior tibial margins are defined irrespective of the presence of osteophytes iii. The femoral notch is defined as being part of the medial femur. iv. The superior border of the femur is the physeal line. The posterior border of the trochlea region is the anterior 50% of this region (as measured along the length of the epiphyseal line) (see Fig. 2). 3. The tibia is divided into three medial (anterior, central and posterior) and three lateral (anterior, central and posterior) subregions covered by articular cartilage, and the subspinous subregion [SS-region delineated by the tibial spines (Fig. 3)]. For the anterior, central and posterior divisions the tibia is divided into equal thirds excluding the presence of osteophytes. Special considerations for scoring in any region. If a lesion spans more than one subregion, the lesion needs to be scored in all subregions, especially as the MOAKS system is modified into a volumeoriented approach and not lesional. Also, if a feature occurs within the subspinous region, but extends also into one or more of the medial or lateral tibial sub-regions, the lesion will be scored in the subspinous region but also in the additional tibial sub-regions separately. Description of scoring for individual features Each feature is scored separately. We have chosen a number of commonly recognized features based on their likely relevance to pain and structural damage or progression of OA. The scoring for BMLs and articular cartilage described is by sub-regions as outlined above. Scoring of osteophytes will be performed at defined locations or sites. For each joint morphologic feature, we have listed the number (if there are multiple abnormalities), its location and grade. For BML and cartilage which are scored by region the score is assigned for the region. We have also described preferred pulse sequences to delineate each feature. BMLs will be scored based on the standardized regions outlined previously (p 4e5). Multiple BMLs can occur within each region. Each region will generate a single grade for size inclusive of all BMLs into one score, the number of BMLs per subregion will be counted and % of lesions that is BML as distinct from cyst will be coded (see Table I). a. Each subregion will be graded for BML (including ill-defined lesion and cysts) size in regard to the total volume of the subregion occupied by BML(s) (see Fig. 4). Consequently, a BML in a smaller subregion will be smaller when compared to a BML that is assigned the same grade but is present in a larger subregion, or two BMLs of the same absolute size might be assigned different grades if present in sub-regions with differing volume. b. Percentage of the volume of each BML that is BML (as distinct from cyst) is graded as; grade 0 ¼ none, grade 1 <33%, grade 2 ¼ 33e66% and grade 3 >66%. c. If a cyst is present without an associated BML, then cysts will be scored as a 0 for size % of lesion that is BML. The scoring for size should be identical to that for BMLs (Table I). In contrast, if a BML does not include any portion of a cyst, the % of the lesion that is BML vs cyst score would be 3. d. Do not score marrow signal within osteophytes, however if the lesion extends beyond the osteophyte then it should be scored. Pulse sequences. Suggested pulse sequences to evaluate BMLs are turbo spin-echo (TSE) T2-/intermediate- or proton-density (PD)- weighted fat-saturated or Short TI Inversion Recovery (STIR) sequences in the axial, coronal, and sagittal planes 11. T1-weighted fs images after intravenous administration of a gadolinium-based contrast agent may be used alternatively 12. 3D TSE sequences such as Cube (GE), XETA (extended Echo Train Acquisition) or SPACE (Sampling Perfection with Application optimized Contrasts using different flip angle Evolution, Siemens) might possibly be of use for BML assessment in the future 13e15. Gradient echo-type sequences, even with robust fat suppression or water excitation, are notoriously insensitive to bone marrow abnormalities due to trabecular magnetic susceptibility of T2* effects, which may result in underestimation of the size of noncystic BMLs 16,17. Recent studies have demonstrated that these sequences are also less sensitive in the detection of non-cystic BMLs when using fluid-sensitive fast spin-echo (FSE) sequences as the reference standard 16,18e21. We do not recommend the use of these sequences for scoring BMLs.
4 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e Fig. 4. BML grading. Grade 0 ¼ none, grade 1 <33% of subregional volume, grade 2 ¼ 33e66% of subregional volume and grade 3 >66% of subregional volume. A. Coronal T2 w image shows small grade 1 BML in central subregion of medial tibia. B. A grade 2 BML is depicted in central subregion of medial femur. C. Grade 3 BMLs in the central sub-regions of the medial femur (arrows) and central medial tibia (arrowheads). D. Coronal image shows BML consisting of non-cystic/ill-defined portion (arrowheads) and cystic (arrow) part. 2. Articular cartilage Although many joint structures are affected in OA, articular cartilage is one of the main tissues involved in the disease process. The rationale for the cartilage score was to provide separate scores for the size (i.e., area affected) and depth of cartilage damage in each of the sub-regions. Each articular cartilage region (except the subspinous region) is graded for size of any cartilage loss (including partial and fullthickness loss) as a % of surface area as related to the size of each individual region surface (see Fig. 5) and % of loss in this subregion that is full-thickness loss (Table II and Fig. 5). Description of morphology at individual sites is not to be used to create cumulative scores of the knee as histopathology is unclear and this scale is not necessarily linear. Pulse sequences. Optimal pulse sequences to evaluate cartilage are still undergoing extensive review. We refer to current state-of-the art reviews of imaging of articular cartilage 22. For assessment of early OA commonly used gradient-echo sequences such as spoiled gradient recalled acquisition (SPGR), Fast Low Angle Shot Water Excitation (FLASH), dual echo steady state (DESS) or similar are not suitable as these depict focal defects in an inferior manner when compared to standard T2/IW (Intermediate-Weighted)- or PD (Proton Density)-w fs turbo-spin-echo sequences 23e Osteophytes Osteophytes are osteo-cartilaginous protrusions growing at the margins of osteoarthritic joints from a process that involves endochondral ossification. Previous radiographic studies have highlighted this feature as a hallmark of disease 27. For MOAKS, osteophytes are scored in each of the 12 locations or sites outlined below (Table III) and graded according to size where: Grade 0 ¼ none; Grade 1 ¼ small; Grade 2 ¼ medium; Grade 3 ¼ large. Osteophytes along the trochlea, central and posterior margins of the femoral condyles and tibial plateaus, and along the medial, lateral, superior and inferior margins of the patella. Posterior Table II Delineation of grading for cartilage Size of any cartilage loss (including partial and full-thickness loss) % full-thickness cartilage loss of the region as a % of surface area as related to the size of each individual region 0: none 0: none 1: <10% of region of cartilage surface area 1: <10% of region of cartilage surface area 2: 10e75% of region of cartilage surface area 2: 10e75% of region of cartilage surface area 3: >75% of region of cartilage surface area 3: >75% of region of cartilage surface area
5 994 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e1002 As commonly employed contrast-enhanced sequences are not available in large OA studies due to cost concerns and possible side reactions, a surrogate of signal changes in Hoffa s fat pad has been applied that has been shown on biopsy to represent mild chronic synovitis 32. This abnormality is best described as diffuse hyperintense signal on T2/PD/IW-w fat suppressed sequences within the fat pad. It has to be noted that in addition to synovitis these signal changes could also be attributed to other etiologies such as post-arthroscopic changes or Hoffa s disease 33. Despite this non-specificity these signal changes are referred to as Hoffa-synovitis in MOAKS. i. Hoffa-synovitis score (on sagittal image) (one single score for assessment of degree of hyperintensity in Hoffa s fat pad) based on the region highlighted in Fig. 8. Score is based on size: 0 ¼ normal; 1 ¼ mild, 2 ¼ moderate, 3 ¼ severe. Fig. 5. Grade for size of any cartilage loss as a % of surface area as related to the size of each individual region. Grade 0 ¼ none, grade 1 <10% of region of cartilage surface area, grade 2 ¼ 10e75% of region of cartilage surface area and grade 3 >75% of region of cartilage surface area. (Drawing courtesy of Daichi Hayashi, MD). femoral osteophytes are assessed peripherally and centrally. The larger osteophyte for either, peripheral or central, location will be scored (Fig. 6). a. Size of osteophyte should reflect protuberance (how far the osteophyte extends from the joint) rather than total volume of osteophyte (see Fig. 7). b. Score the largest osteophyte within a given location. Pulse sequences. Optimal pulse sequences to evaluate osteophytes are standard non-fs short echo time (TE)-weighted (preferably T1 over PD) or gradient-echo-type such as SPGR, FLASH, DESS etc. images in the axial, coronal, and sagittal planes. They may also be assessed on fs water-sensitive sequences Hoffa s synovitis and synovitis e effusion Synovitis and effusion are frequently present in OA and in some studies this feature correlated with pain and other clinical outcomes although the literature is conflicting 28e30. Quantitative MRI markers of synovitis include thickness (or volume) of synovial tissue and the rate of synovial enhancement following intravenous injection of contrast material 31. Table III Sites for osteophyte scoring Osteophyte location Slice orientation Anterior femur (trochlea) Medial Sagittal/Axial Lateral Posterior femur Medial Sagittal/Axial Lateral Central femur Medial Coronal Lateral Patella Superior Sagittal Inferior Medial Axial Lateral Tibia Medial Coronal Lateral Pulse sequences. Suggested pulse sequences to evaluate regions for Hoffa-synovitis are T2/IW- or PD-weighted fat-saturated images in the mid-slices of the sagittal plane 28,29. Effusions occur frequently in OA. Recent studies suggest that large synovial effusions may be associated with pain and stiffness in patients with OA 28. It is important to note that effusion (fluid equivalent signal within the joint cavity) on T2/IW/PDw images includes synovitis and effusion 34. Thus, this imaging measure should preferably referred to as effusion-synovitis. Scores (Table IV) should be obtained from axial views (Fig. 9). Paraarticular cysts and ganglia should not be included in this score as they are considered separately. Pulse sequences. True amount of joint effusion may be assessed as intra-articular hypointensity on T1w images after i.v. contrast administration. T2/IW/PDw images show intra-articular hyperintensity that represents a composite of effusion and synovitis Meniscus The meniscus has many functions in the knee, including load bearing, shock absorption, stability enhancement and lubrication 35. Degenerative meniscal lesions such as horizontal cleavages, oblique or complex tears are associated with older age 36. By the time radiographic disease develops, the overwhelming majority of persons have meniscal lesions 36,37. The studies that have explored the relationship between the meniscus and risk of disease progression in OA provide a clear indication of the increased risk inherent with damage to this vital tissue 38,39. Changes in position (also termed subluxation or extrusion) and meniscal morphologic change manifest as tears or loss of substance have both been shown to predispose to cartilage loss. We chose a scoring system that delineated both of these items and provided detail on what the abnormality was and where in the meniscus this occurred. a. Extrusion: Four areas where extrusion is scored: 1. Medial meniscus: Medial extrusion relative to medial tibial margin (coronal image). 2. Medial meniscus: Anterior extrusion (sagittal image) e where extrusion is maximum. 3. Lateral meniscus: Lateral extrusion relative to lateral tibial margin (coronal image). 4. Lateral meniscus: Anterior extrusion (sagittal image) where extrusion is maximum. Grading for extrusion: Grade 0:<2 mm; Grade 1: 2e2.9 mm, Grade 2: 3e4.9 mm; Grade 3: >5 mm.
6 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e Fig. 6. Locations for osteophytes scoring. A. Coronal plane. Osteophytes are scored at the marginal locations of the medial and lateral femur and tibia, respectively (arrowheads). B. Sagittal plane. Osteophytes are scored at the superior and inferior patellar pole (arrowheads). C. Axial plane. Osteophytes are scored at the medial and lateral patella poles (arrowheads), at the anterior medial and lateral femur (black arrows) and the posterior femur medial and lateral (white arrows). Note that there are two locations medially and laterally for osteophytes scoring at the posterior femur, the central and peripheral location. Only the larger osteophyte for either the central or peripheral location will be scored. Note: we wanted to capture anterior extrusion to see if this is independently predictive of cartilage loss/pain/etc. compared with medial or lateral extrusion. For each measurement the reference will be the edge of the tibial plateau (excluding any osteophytes). b. Morphology: (scored on medial and lateral meniscus for the anterior, body and posterior horn). The anterior and posterior horn regions are scored using the sagittal sequences and the body is scored using the coronal sequences. Morphologic features scored: i. Signal (not extending through meniscal surface i.e., not a tear): Y/N. a. Signal is defined as above as compared with tears which are defined as high signal extending to an articular surface on at least two slices. ii. Vertical tear (includes radial and longitudinal tears) e must extend to both the femoral and tibial surfaces: Y/N. iii. Horizontal and radial tear: must extend from the periphery of the meniscus to either a femoral or tibial surface. Y/N. iv. Complex tear: as defined by high signal that extends to both the tibial and femoral surfaces and 3 points on those surfaces). Y/N. v. Root tear (posterior horn): Y/N. vi. Partial maceration: as defined by loss of morphological substance of the meniscus and with or without associated increased signal in the remaining meniscal tissue. Y/N. vii. Progressive partial maceration: Progressive partial maceration as compared to the previous visit. Y/N. viii. Complete maceration: No meniscal substance is visible. Y/N. ix. Meniscal cyst: Y/N. x. Meniscal hypertrophy is defined as definite increase in meniscal volume in given subregion when compared to normal: Y/N. Pulse sequences. Optimal sequences to evaluate menisci are T1, T2w or PD fat-saturated images in both coronal and sagittal planes 40,41. As for BMLs, newly developed 3D FSE sequences might alternatively be used for meniscal assessment Ligaments/tendon Anterior cruciate ligament (ACL) tears will be recorded as either absent or present. Partial tears are infrequent and reportedly prone to poor reliability on interpretation 43. Thus, partial tears are scored as normal in MOAKS. Only definite complete tears will be scored. a. ACL: Score: normal (0)/complete tear (1). i. Associated with BML/cyst at site of insertion or origin?: Y/N. ii. ACL Repair: Y/N.
7 996 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e1002 Fig. 7. Scoring of osteophytes. Grade 0 ¼ none, grade 1 ¼ small, grade 2 ¼ medium and grade 3 ¼ large. A. Grade 1 osteophyte medial femur. B. Grade 2 osteophyte lateral femur. C. Grade 3 osteophyte lateral femur. Size of osteophyte should reflect protuberance (how far the osteophyte extends from the joint) rather than total volume of osteophyte. b. Posterior Cruciate Ligament (PCL): Score: normal (0)/complete tear (1). i. Associated with BML/cyst at site of insertion or origin?: Y/N. c. Patellar tendon: Score: 0: no signal abnormality/1: signal abnormality present. Pulse sequences. Optimal sequences to evaluate the aforementioned ligaments are coronal, axial and sagittal, PD or IW, fat TSE images, while 3D sequences also appear promising 17,44,45. Additional paracoronal T2-w sequences might be helpful to differentiate partial from full-thickness tears Periarticular features a. Pes anserine bursitis e absent/present This is a bursa that lies anterior and inferior to the medial tibial plateau and is a potential source of pain around the knee. If there is increased signal in this bursa, bursitis is scored as being present. b. Iliotibial band (ITB) signal e absent/present The ITB is a strong, dense, broad layer of fascia that is part of the fascia lata. The ITB encases the tensor fasciae lata which helps to steady the trunk on the thigh. 3 / 4 of the gluteus maximus inserts into the iliotibial tract and the distal end inserts at the lateral tibial plateau. High signal between the ITB and the femoral cortex may represent irritation of the ITB and is common in medial OA. However, this is also Table IV Delineation of grading for effusion-synovitis Fig. 8. Hoffa-synovitis. Sagittal T2w image shows grade 2 hyperintense signal changes in Hoffa s fat pad consistent with Hoffa-synovitis. Size of effusion-synovitis 0: physiologic amount 1: small e fluid continuous in the retropatellar space 2: medium e with slight convexity of the suprapatellar bursa 3: large e evidence of capsular distention
8 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e Fig. 9. Effusion-synovitis. Hyperintensity within the articular cavity represents a composite of effusion and synovial thickening that cannot be distinguished from each other in the absence of contrast. Grade 0 ¼ none, grade 1 ¼ small, grade 2 ¼ medium and grade 3 ¼ large. A. Grade 0 effusion-synovitis. Normal intra-articular hyperintensity is depicted. B. Grade 1 effusion-synovitis. C. Grade 2 effusion-synovitis. D. Grade 3 effusion-synovitis. anon-specific finding and often asymptomatic 47. If there is high signal in this structure, ITB signal should be scored as being present. c. Popliteal cyst-absent/present Popliteal cysts are not true cysts and represent fluid in the semimembranosusemedial gastrocnemius bursa. The communication between the joint space and gastrocnemiusesemimembranosus bursa allows intra-articular joint fluid to communicate with this bursa 48. If there is any fluid in this region, this feature should be scored as being present. Pulse sequence. Optimal sequences for evaluating popliteal cysts are PD or T2-weighted axial images. d. Infrapatellar bursa signal e absent/present This is a bursa located inferior to Hoffa s fat pad adjacent to the patellar tendon and is a potential source of pain around the knee. If there is high signal in this bursa, this feature should be scored as being present. e. Prepatellar bursa signal e absent/present This is a bursa that lies anterior to the patella and is a potential source of pain around the knee. High signal anterior to the patella tendon is a very common non-specific finding of often no clinical relevance. True bursitis is characterized by well demarcated fluid equivalent signal within this structure; only then should this feature be scored as being present. f. Ganglion cyst i. Associated with the tibio-fibular joint: present/absent. ii. Associated with PCL and ACL: present/absent. iii. Other: present/absent. Loose bodies: Scale: absent/present. Table V provides a summary of the changes in the new score (MOAKS) from older instruments including BLOKS 5 and WORMS 4. Study images for reliability exercise. The images for the reliability exercise were chosen at random from MRI scans undertaken
9 998 Table V Features that are scored in MOAKS in comparison to the original BLOKS instrument and WORMS score. We used BLOKS as the starting point, and the alterations in MOAKS reflect deviation from BLOKS MRI feature Original BLOKS score Original WORMS score Alteration in MOAKS BML size Score of 0e3 applied for BML volume in nine different articular sub-regions. Each BML within a subregion receives an individual size score. Summed BML size/volume for subregion from 0 to 3 in regard to percentage of subregional bone volume. Modify thresholds from 10 e 85% to 33e66%. Instead of scoring EACH BML, the entire subregion receives one size score based on the threshold listed above. Grade for regions-use same sub-regions as proposed for cartilage e with the addition of the subspinous region. Count no. of lesions. BML % area Score of 0e3 applied for % surface area adjacent to subchondral plate. e Omitted from new scoring system. % of lesion BML rather than cyst Cartilage 1 Score of 0e3 for % of lesion that is BML as distinct from cyst. Score of 0e3 for size of loss and % of loss in region that is full thickness. Summed cyst size/volume for subregion from 0 to 3 in regard to percentage of subregional bone volume. Subregional approach: Scores from 0 to 6 depending on depth and extent of cartilage loss. Intrachondral cartilage signal additionally scored as present/absent. No change. Further subdivision of the medial and lateral tibial region into anterior, central and posterior and subdivision of the weight-bearing femur into central and posterior. Cartilage 2 Extent of any cartilage loss at specified points. e Omitted from new scoring system. Osteophyte Score of 0e3 applied for osteophyte size in Score of 0e7 applied for osteophyte size at No change. 12 locations. 16 sites. Synovitis Score of 0e3 applied for synovial volume. Combined effusion/synovitis score. Score of 0e3 applied to signal changes in Hoffa s fat pad. Feature renamed as Hoffa-synovitis Effusion Score of 0e3 applied for size of effusion. Score of 0e3 applied for size of effusion. Feature renamed to Effusion-synovitis Scoring parameters are unchanged. Meniscal extrusion Score of 0e3 applied for amount of Not scored. No change. extrusion in four locations. Meniscal signal Scored as present or absent in six regions. Not scored. No change. Meniscus tear Type of tear or degenerative process scored as present or absent in six regions. Anterior horn, body, posterior horn scored separately in medial/lateral meniscus from 0 to 4: Add meniscal hypertrophy, partial maceration and progressive partial maceration. 1: minor radial or parrot beak tear 2: non-displaced tear or prior surgical repair 3: displaced tear or partial resection 4: complete maceration/destruction or complete resection. Ligaments Presence/absence of tear. Presence/absence of tear. No change. Periarticular features Presence/absence. Presence/absence. No change. D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e1002
10 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e Table VI The reliability for reading of MOAKS features (weighted kappa and percent agreement) MOAKS feature Region Intra-rater Inter-rater Weighted kappa (95%CI) Percent agreement Weighted kappa (95%CI) Percent agreement Cartilage area Femoral 0.92 (0.77e1.00) (0.27e0.98) 0.80 Tibial 0.73 (0.47e1.00) (0.05e0.67) 0.70 Patella 0.71 (0.43e0.99) (0.42e0.99) 0.75 Cartilage depth Femoral 0.95 (0.85e1.00) (0.60e0.98) 0.80 Tibial 0.83 (0.69e0.96) (0.52e0.94) 0.75 Patella 0.92 (0.82e1.00) (0.72e0.98) 0.80 BML size Femoral 0.85 (0.69e1.00) (0.69e0.95) 0.80 Tibial 0.76 (0.55e0.98) (0.86e1.00) 0.95 Patella 1.00 (1.00e1.00) (0.74e1.00) 0.85 Subspinous 0.79 (0.60e0.99) (0.57e0.94) 0.75 BML, %cyst Femoral 0.57 (0.18e0.95) (0.40e1.00) 0.90 Tibial 0.50 (0.23e0.97) (0.46e1.00) 0.85 Patella 0.88 (0.73e1.00) (1.00e1.00) 1.00 Subspinous 0.70 (0.36e1.00) (0.36e0.93) 0.75 BML, no. of lesions Femoral 0.84 (0.68e1.00) (0.64e0.92) 0.75 Tibial 0.54 (0.30e0.77) (0.62e1.00) 0.85 Patella 0.90 (0.77e1.00) (0.82e1.00) 0.90 Subspinous 0.80 (0.63e0.97) (0.51e0.93) 0.75 Meniscus morphology Medial 1.00 (1.00e1.00) (0.89e1.00) 0.95 Lateral 0.91 (0.77e1.00) (0.86e1.00) 0.95 Meniscal extrusion Medial 0.82 (0.67e0.98) (0.46e0.86) 0.60 Lateral 0.89 (0.75e1.00) (0.67e0.91) 0.80 Osteophytes Femoral 0.64 (0.36e0.92) (0.58e1.00) 0.95 Tibial 0.70 (0.50e0.91) (0.24e0.74) 0.55 Patella 0.84 (0.67e1.00) (0.39e0.89) 0.65 Hoffa-synovitis e 0.42 (0.14e0.70) (0.47e0.93) 0.75 Effusion-synovitis e 0.90 (0.78e1.00) (0.52e0.92) 0.70 within the National Institutes of Health (NIH) OA Initiative (OAI, The OAI is a multi-center, longitudinal, prospective observational study of knee OA. The overall aim of the OAI is to develop a public domain research resource to facilitate the scientific evaluation of biomarkers for OA as potential surrogate endpoints for disease onset and progression. The OAI database provides an unparalleled state-of-the-art database showing both the natural progression of the disease and information on imaging and biochemical biomarkers and outcome measures. From 329 participants in the OAI Progression subcohort within OAI Group C (those enrolled through 4/30/2005) with MRI performed on both knees at baseline, all knees with K&L grade 2 or 3 were identified (n ¼ 339). A 2 2 factorial design was formed incorporating the factors of side (left vs right knee) and Kellgren and Lawrence (KL) grade (2 or 3). For subjects with both knees having K&L grade 2 or 3, only one knee was randomly selected for potential inclusion. The final 2 2 factorial random sample of 20 knees for the reliability study included five randomly selected knees in each of the four cells. A computerized uniform random number between 0 and 1 was assigned to each knee, sorted, then the five knees in each cell with the lowest assigned numbers comprised the randomly selected knees in each cell (e.g., n ¼ 5 of 90 knees in cell left knee with K&L grade ¼ 3 were randomly selected, etc.). MRI acquisition. MRI of both knees was performed on 3 T systems (Siemens Trio, Erlangen, Germany). MRIs were acquired with a USA Instruments (USAI) quadrature transmit/receive knee coil. The coronal IW 2D turbo spin-echo, a sagittal 3D DESS sequence, coronal and axial multiplanar reformations of the 3D DESS and a sagittal IW fs FSE sequence were used for scoring MOAKS. Details of the full OAI pulse sequence protocol and the sequence parameters have been published in detail recently 49. The sagittal T2 mapping and coronal 3D T1-weighted Fast Low Angle Shot Water Excitation (FLASH WE) sequences were not used for semiquantitative assessment. Assessment of reliability. After an initial training and calibration session on 10 cases that were not included in the reliability exercise, two expert readers with 10 and 8 years experience in semiquantitative MRI assessment of knee OA respectively, (AG, FR) independently read MRIs of the 20 knees from the OAI. In addition, one reader (FR) re-read the same 20 MRIs 4 weeks later presented in random order to assess intra-rater reliability. The analyses presented here are for both intra- and inter-rater reliability [calculated using the linear weighted kappa (95% confidence interval (CI))] and the percent agreement of the scoring exercise. Results The reliability of the instrument was assessed on 20 subjects with a mean age of 57.8 years [standard deviation (SD) 9.8] and a mean body mass index (BMI) of 31.4 kg/m 2 (SD 5.0). Fifty-five percent (n ¼ 11) were female. Of the 20 knees that were assessed their Kellgren and Lawrence Grades were K&L ¼ 2 in 10 knees, K&L ¼ 3 in 10 knees. The reliability for the features described above is reported in Table VI. With the exception of inter-rater reliability for tibial cartilage surface area (kappa ¼ 0.36), tibial osteophytes (kappa ¼ 0.49) and intercondylar synovitis (kappa ¼ 0.49); and intra-rater reliability for tibial BML number of lesions (kappa ¼ 0.54), infrapatellar synovitis (kappa ¼ 0.42) and intercondylar synovitis (kappa ¼ 0.57) all measures of reliability were very good (0.61e0.8) or reached near-perfect agreement (0.81e1.0) according to the criteria developed by Landis and Koch 50. The low prevalence of certain features in certain sub-regions may have adversely affected the kappa results hence the percent agreement was also calculated. The majority of features were scored with overall percent agreement above 75% for both, the intra- and inter-reader exercise. Only intrarater reliability for Hoffa-synovitis (55%), and inter-rater reliability for tibial (55%) and patellar (65%) osteophytes showed overall percent agreement <75%.
11 1000 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e1002 Discussion The structural determinants of mechanical dysfunction and pain in arthritis are presently not well understood, but probably involve a multitude of interactive pathways characterized by changes in structure and function of the whole joint 51. The current practice of monitoring only a few of these features (usually radiographicallyassessed joint-space narrowing and osteophytes) provides only a restricted view of the disease process and lessens the utility of such assessments. Semi-quantitative MRI scoring will continue to provide important insights into the etiopathogenesis of disease as well as structureefunction relationships. As new insights continue to develop the field, this scoring instrument, used to assess structural change in knee OA will similarly need to evolve. This report provides data on the reliability of structural features scored using MOAKS: a semi-quantitative scoring instrument for MRI assessment of knee OA that builds on the prior experiences of BLOKS and other semi-quantitative scoring tools. The MOAKS instrument refines the scoring of BMLs (providing regional delineation and scoring across regions), cartilage (subregional assessment), and refines the elements of meniscal morphology (adding meniscal hypertrophy, partial maceration and progressive partial maceration) and subluxation scoring. In addition we decided to omit some areas of redundancy including the second cartilage scoring method that was part of the original BLOKS instrument and assessed cartilage at defined locations in a specific image and also omitted BML adjacency to subchondral plate scoring. The timing of this work is relevant as large scale scoring exercises are about to commence in a number of studies including the OAI. Importantly, the measurement properties (including construct and predictive validity and the responsiveness) of these modifications will need to be assessed to ensure their credibility. The reliability of most of the features that were scored in this exercise was substantial or almost perfect agreement according to Landis and Koch criteria 50. Some of the features however had only moderate agreement when using kappa statistics including intrarater reliability for femoral and tibial cystic portions of BMLs, count of tibial BMLs, and Hoffa-synovitis, and inter-rater reliability for tibial cartilage area and tibial osteophytes. For some of these features low frequencies of non-zero scores are accountable for these kappa values. Overall percent agreement was good to perfect for almost all features. Some of the features listed are exploratory in nature and warrant further investigation, including measures of meniscal extrusion. The magnitude of the meniscal extrusion is the same that we have previously used in BLOKS and that has been used in prior analyses 39,52,53. The extent of analysis in the research literature describing the importance of anterior or posterior extrusion is limited. In our previous analyses anterior extrusion has been associated with an increased risk of cartilage loss 39. In conclusion, we have refined an existing scoring instrument and assessed its reliability. MOAKS demonstrates reasonable reliability. Further iterative development and research will include assessment of its validation and responsiveness for use in both clinical trials and epidemiological studies. This will allow determination of the significance of specific features to determine if there are subsets that can be consolidated or eliminated to simplify the instrument. Contributions DJH conceived and designed the study, drafted the manuscript and takes responsibility for the integrity of the work as a whole, from inception to finished article. All authors contributed to acquisition of the data. All authors critically revised the manuscript and gave final approval of the article for submission. Conflict of interest statement The corresponding author had full access to all the data in the study and had final responsibility for the decision to submit for publication. David Hunter receives research or institutional support from AstraZeneca, DonJoy, Lilly, Merck, NIH, Pfizer, Stryker and Wyeth. Ali Guermazi receives research or institutional support from NIH and GE Healthcare. He is consultant to MerckSerono, Stryker, Genzyme and Novartis. He is President of BICL (Boston Imaging Core Lab), LLC, a company providing radiologic image assessment services. Frank Roemer is shareholder of Boston Imaging Core Lab (BICL) LLC., a company providing radiologic image assessment services. Other authors declared no conflict of interest. Acknowledgments Dr Hunter is supported by an Australian Research Council Future Fellowship. We would like to acknowledge the support of Dr Daniel Gale who contributed to BLOKS and the initial development of MOAKS. References 1. Hunter DJ, Zhang W, Conaghan PG, Hirko K, Menashe L, Reichmann WM, et al. Responsiveness and reliability of MRI in knee osteoarthritis: a meta-analysis of published evidence. Osteoarthritis Cartilage 2011;19:589e Hunter DJ, Zhang W, Conaghan PG, Hirko K, Menashe L, Li L, et al. Systematic review of the concurrent and predictive validity of MRI biomarkers in OA. Osteoarthritis Cartilage 2011;19:557e Kornaat PR, Ceulemans RY, Kroon HM, Riyazi N, Kloppenburg M, Carter WO, et al. MRI assessment of knee osteoarthritis: knee osteoarthritis scoring system (KOSS)einter-observer and intraobserver reproducibility of a compartment-based scoring system. Skeletal Radiol 2005;34:95e Peterfy CG, Guermazi A, Zaim S, Tirman PF, Miaux Y, White D, et al. Whole-organ magnetic resonance imaging score (WORMS) of the knee in osteoarthritis. Osteoarthritis Cartilage 2004;12:177e Hunter DJ, Lo GH, Gale D, Grainger AJ, Guermazi A, Conaghan PG. The reliability of a new scoring system for knee osteoarthritis MRI and the validity of bone marrow lesion assessment: BLOKS (Boston Leeds Osteoarthritis Knee Score). Ann Rheum Dis 2008;67:206e Hunter D, Conaghan P, Peterfy C, Bloch D, Guermazi A, Woodworth T, et al. Responsiveness, effect size, and smallest detectable difference of magnetic resonance imaging in knee osteoarthritis. Osteoarthritis Cartilage 2006;14(Suppl 1):112e5. 7. Conaghan P, Tennant A, Peterfy C, Woodworth T, Stevens R, Guermazi A, et al. Examining a whole-organ magnetic resonance imaging scoring system for osteoarthritis of the knee using Rasch analysis. Osteoarthritis Cartilage 2006;14(Suppl 1): 116e Lynch JA, Roemer FW, Nevitt MC, Felson DT, Niu J, Eaton CB, et al. Comparison of BLOKS and WORMS scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions on knee MRI: data from the osteoarthritis initiative. Osteoarthritis Cartilage 2010;18:1393e401.
12 D.J. Hunter et al. / Osteoarthritis and Cartilage 19 (2011) 990e Felson DT, Lynch J, Guermazi A, Roemer FW, Niu J, McAlindon T, et al. Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance: data from the osteoarthritis initiative. Osteoarthritis Cartilage 2010;18:1402e Hunter DJ, Zaim S, Mosher TJ. What semi-quantitative scoring instrument for knee OA MRI should you use? Osteoarthritis Cartilage 2010;18:1363e Roemer FW, Frobell R, Hunter DJ, Crema MD, Fischer W, Bohndorf K, et al. MRI-detected subchondral bone marrow signal alterations of the knee joint: terminology, imaging appearance, relevance and radiological differential diagnosis. Osteoarthritis Cartilage 2009;17:1115e Roemer FW, Khrad H, Hayashi D, Jara H, Ozonoff A, Fotinos-Hoyer AK, et al. Volumetric and semiquantitative assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis: a comparison of contrast-enhanced and non-enhanced imaging. Osteoarthritis Cartilage 2010;18: 1062e Ristow O, Steinbach L, Sabo G, Krug R, Huber M, Rauscher I, et al. Isotropic 3D fast spin-echo imaging versus standard 2D imaging at 3.0 T of the kneeeimage quality and diagnostic performance. Eur Radiol 2009;19:1263e Welsch GH, Zak L, Mamisch TC, Paul D, Lauer L, Mauerer A, et al. Advanced morphological 3D magnetic resonance observation of cartilage repair tissue (MOCART) scoring using a new isotropic 3D proton-density, turbo spin echo sequence with variable flip angle distribution (PD-SPACE) compared to an isotropic 3D steady-state free precession sequence (True-FISP) and standard 2D sequences. J Magn Reson Imaging 2011;33: 180e Kijowski R, Davis KW, Woods MA, Lindstrom MJ, De Smet AA, Gold GE, et al. Knee joint: comprehensive assessment with 3D isotropic resolution fast spin-echo MR imagingediagnostic performance compared with that of conventional MR imaging at 3.0 T. Radiology 2009;252:486e Guermazi A, Kwok C, Hannon M, Moore C, Jakicic J, Green S, et al. Subchondral bone marrow lesions of the knee: a comparison of semiquantitative assessment of fatsuppressed intermediate-weighted fast spin echo (IW) and double echo steady state (DESS) sequences at 3T. Osteoarthritis Cartilage 2009;17(Suppl 1). Ref Type: Abstract. 17. Peterfy CG, Gold G, Eckstein F, Cicuttini F, Dardzinski B, Stevens R. MRI protocols for whole-organ assessment of the knee in osteoarthritis. Osteoarthritis Cartilage 2006;14(Suppl A):A95eA111 [Review] [32 refs]. 18. Kijowski R, Blankenbaker DG, Woods MA, Shinki K, De Smet AA, Reeder SB. 3.0-T evaluation of knee cartilage by using three-dimensional IDEAL GRASS imaging: comparison with fast spin-echo imaging. Radiology 2010;255:117e Kijowski R, Blankenbaker DG, Klaers JL, Shinki K, De Smet AA, Block WF. Vastly undersampled isotropic projection steady-state free precession imaging of the knee: diagnostic performance compared with conventional MR. Radiology 2009;251:185e Yoshioka H, Stevens K, Hargreaves BA, Steines D, Genovese M, Dillingham MF, et al. Magnetic resonance imaging of articular cartilage of the knee: comparison between fat-suppressed three-dimensional SPGR imaging, fat-suppressed FSE imaging, and fat-suppressed three-dimensional DEFT imaging, and correlation with arthroscopy. J Magn Reson Imaging 2004;20:857e Duc SR, Koch P, Schmid MR, Horger W, Hodler J, Pfirrmann CW. Diagnosis of articular cartilage abnormalities of the knee: prospective clinical evaluation of a 3D waterexcitation true FISP sequence. Radiology 2007;243:475e Gold GE, Chen CA, Koo S, Hargreaves BA, Bangerter NK. Recent advances in MRI of articular cartilage. AJR Am J Roentgenol 2009;193:628e Roemer FW, Kwoh CK, Hannon MJ, Crema MD, Moore CE, Jakicic JM, et al. Semiquantitative assessment of focal cartilage damage at 3T MRI: A comparative study of dual echo at steady state (DESS) and intermediate-weighted (IW) fat suppressed fast spin echo sequences. Eur J Radiol Mohr A, Roemer FW, Genant HK, Liess C. Using fat-saturated proton density-weighted MR imaging to evaluate articular cartilage. AJR Am J Roentgenol 2003;181:280e Stahl R, Luke A, Ma CB, Krug R, Steinbach L, Majumdar S, et al. Prevalence of pathologic findings in asymptomatic knees of marathon runners before and after a competition in comparison with physically active subjects-a 3.0 T magnetic resonance imaging study. Skeletal Radiol 2008;37:627e Masi JN, Sell CA, Phan C, Han E, Newitt D, Steinbach L, et al. Cartilage MR imaging at 3.0 versus that at 1.5 T: preliminary results in a porcine model. Radiology 2005;236:140e Altman RD, Hochberg M, Murphy WAJ, Wolfe F, Lequesne M. Atlas of individual radiographic features in osteoarthritis. Osteoarthritis Cartilage 1995;3(Suppl A):3e Hill CL, Gale DG, Chaisson CE, Skinner K, Kazis L, Gale ME, et al. Knee effusions, popliteal cysts, and synovial thickening: association with knee pain in osteoarthritis. Journal of Rheumatology 2001;28:1330e Hill CL, Hunter DJ, Niu J, Clancy M, Guermazi A, Genant H, et al. Synovitis detected on magnetic resonance imaging and its relation to pain and cartilage loss in knee osteoarthritis. Ann Rheum Dis 2007;66:1599e Roemer FW, Zhang Y, Niu J, Lynch JA, Crema MD, Marra MD, et al. Tibiofemoral joint osteoarthritis: risk factors for MR-depicted fast cartilage loss over a 30-month period in the multicenter osteoarthritis study. Radiology 2009;252: 772e Loeuille D, Rat AC, Goebel JC, Champigneulle J, Blum A, Netter P, et al. Magnetic resonance imaging in osteoarthritis: which method best reflects synovial membrane inflammation? Correlations with clinical, macroscopic and microscopic features. Osteoarthritis Cartilage 2009;17:1186e Fernandez-Madrid F, Karvonen RL, Teitge RA, Miller PR, An T, Negendank WG. Synovial thickening detected by MR imaging in osteoarthritis of the knee confirmed by biopsy as synovitis. Magn Reson Imaging 1995;13:177e Roemer FW, Guermazi A, Zhang Y, Yang M, Hunter DJ, Crema MD, et al. Hoffa s fat pad: evaluation on unenhanced MR images as a measure of patellofemoral synovitis in osteoarthritis. AJR Am J Roentgenol 2009;192:1696e Roemer FW, Kassim JM, Guermazi A, Thomas M, Kiran A, Keen R, et al. Anatomical distribution of synovitis in knee osteoarthritis and its association with joint effusion assessed on non-enhanced and contrast-enhanced MRI. Osteoarthritis Cartilage 2010;18:1269e Seedhom BB, Dowson D, Wright V. Proceedings: functions of the menisci. A preliminary study. Annals of the Rheumatic Diseases 1974;33: Englund M, Guermazi A, Gale D, Hunter DJ, Aliabadi P, Clancy M, et al. Incidental meniscal findings on knee MRI in middle-aged and elderly persons. N Engl J Med 2008;359: 1108e15 [see comment]. 37. Bhattacharyya T, Gale D, Dewire P, Totterman S, Gale ME, McLaughlin S, et al. The clinical importance of meniscal tears demonstrated by magnetic resonance imaging in
Osteoarthritis and Cartilage 18 (2010) 1393e1401
 Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
Osteoarthritis and Cartilage 18 (2010) 1393e1401 Comparison of BLOKS and scoring systems part I. Cross sectional comparison of methods to assess cartilage morphology, meniscal damage and bone marrow lesions
Osteoarthritis and Cartilage 18 (2010) 1402e1407
 Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
Osteoarthritis and Cartilage 18 (2010) 1402e1407 Comparison of BLOKS and WORMS scoring systems part II. Longitudinal assessment of knee MRIs for osteoarthritis and suggested approach based on their performance:
ARTICLE IN PRESS. International Cartilage Repair Society
 Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
Osteoarthritis and Cartilage (2009) jj, jjjejjj ª 2006 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.11.014 Strong association of
Peripatellar synovitis: comparison between non-contrast-enhanced and contrast-enhanced MRI and association with pain.
 Osteoarthritis and Cartilage 21 (2013) 413e418 Peripatellar synovitis: comparison between non-contrast-enhanced and contrast-enhanced MRI and association with pain. The MOST study M.D. Crema yz *, D.T.
Osteoarthritis and Cartilage 21 (2013) 413e418 Peripatellar synovitis: comparison between non-contrast-enhanced and contrast-enhanced MRI and association with pain. The MOST study M.D. Crema yz *, D.T.
Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding
 Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding Poster No.: P-0073 Congress: ESSR 2012 Type: Scientific Exhibit Authors: F. K. Nielsen,
Bone marrow lesions in knee osteoarthritis: MR-assessment by manual segmentation and computer-assisted tresholding Poster No.: P-0073 Congress: ESSR 2012 Type: Scientific Exhibit Authors: F. K. Nielsen,
MR imaging of the knee in marathon runners before and after competition
 Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
Skeletal Radiol (2001) 30:72 76 International Skeletal Society 2001 ARTICLE W. Krampla R. Mayrhofer J. Malcher K.H. Kristen M. Urban W. Hruby MR imaging of the knee in marathon runners before and after
MRI of Cartilage. D. BENDAHAN (PhD)
 MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI of Cartilage D. BENDAHAN (PhD) Centre de Résonance Magnétique Biologique et Médicale UMR CNRS 7339 Faculté de Médecine de la Timone 27, Bd J. Moulin 13005 Marseille France david.bendahan@univ-amu.fr
MRI KNEE WHAT TO SEE. Dr. SHEKHAR SRIVASTAV. Sr.Consultant KNEE & SHOULDER ARTHROSCOPY
 MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
MRI KNEE WHAT TO SEE Dr. SHEKHAR SRIVASTAV Sr.Consultant KNEE & SHOULDER ARTHROSCOPY MRI KNEE - WHAT TO SEE MRI is the most accurate and frequently used diagnostic tool for evaluation of internal derangement
Imaging of Osteoarthritis
 Imaging of Osteoarthritis Ali Guermazi, MD, PhD a, *, Daichi Hayashi, MD, PhD a, Felix Eckstein, MD b, David J. Hunter, MBBS, MSc, PhD, FRACP c, Jeff Duryea, PhD d, Frank W. Roemer, MD a KEYWORDS Osteoarthritis
Imaging of Osteoarthritis Ali Guermazi, MD, PhD a, *, Daichi Hayashi, MD, PhD a, Felix Eckstein, MD b, David J. Hunter, MBBS, MSc, PhD, FRACP c, Jeff Duryea, PhD d, Frank W. Roemer, MD a KEYWORDS Osteoarthritis
This presentation is the intellectual property of the author. Contact them for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Outline Coils, Patient Positioning Acquisition Parameters, Planes and Pulse Sequences Knee Arthrography Normal
A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis
 Osteoarthritis and Cartilage 21 (2013) 806e814 A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis C. Ratzlaff y *, A. Guermazi z, J. Collins
Osteoarthritis and Cartilage 21 (2013) 806e814 A rapid, novel method of volumetric assessment of MRI-detected subchondral bone marrow lesions in knee osteoarthritis C. Ratzlaff y *, A. Guermazi z, J. Collins
Meniscal Tears with Fragments Displaced: What you need to know.
 Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
Meniscal Tears with Fragments Displaced: What you need to know. Poster No.: C-1339 Congress: ECR 2015 Type: Authors: Keywords: DOI: Educational Exhibit M. V. Ferrufino, A. Stroe, E. Cordoba, A. Dehesa,
This presentation is the intellectual property of the author. Contact them at for permission to reprint and/or distribute.
 MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
MRI of the Knee Jennifer Swart, M.D. Musculoskeletal Radiology South Texas Radiology Group Financial Disclosure Dr. Jennifer Swart has no relevant financial relationships with commercial interests to disclose.
Oak foundation for donating the 3T Siemens Verio scanner. Board of directors BBH and Frh Hospitals for supporting the
 Knee pain and inflammation in the infrapatellar fat pad estimated by conventional and dynamic contrast-enhanced magnetic resonance imaging in obese patients with osteoarthritis: a crosssectional study
Knee pain and inflammation in the infrapatellar fat pad estimated by conventional and dynamic contrast-enhanced magnetic resonance imaging in obese patients with osteoarthritis: a crosssectional study
Thanks. As something to help remember. Thanks 07/02/14. Arthroscopy TKR V Uni. Arthroscopy TKR V Uni. Role of arthroscopy to choose operation
 07/02/14 Thanks Role of arthroscopy to choose operation TKR Versus Uni Francois and Philippe Faculty Audience Audiovisual Pierre and Vincent Myles Coolican Val d Isere 2014 Thanks Francois and Philippe
07/02/14 Thanks Role of arthroscopy to choose operation TKR Versus Uni Francois and Philippe Faculty Audience Audiovisual Pierre and Vincent Myles Coolican Val d Isere 2014 Thanks Francois and Philippe
Comparative study of imaging at 3.0 T versus 1.5 T of the knee
 Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
Skeletal Radiol (2009) 38:761 769 DOI 10.1007/s00256-009-0683-0 SCIENTIFIC ARTICLE Comparative study of imaging at 3.0 T versus 1.5 T of the knee Scott Wong & Lynne Steinbach & Jian Zhao & Christoph Stehling
Definition of osteoarthritis on MRI: results of a Delphi exercise
 Osteoarthritis and Cartilage 19 (2011) 963e969 Definition of osteoarthritis on MRI: results of a Delphi exercise D.J. Hunter y *, N. Arden z, P.G. Conaghan x, F. Eckstein k, G. Gold {#yy, A. Grainger zz,
Osteoarthritis and Cartilage 19 (2011) 963e969 Definition of osteoarthritis on MRI: results of a Delphi exercise D.J. Hunter y *, N. Arden z, P.G. Conaghan x, F. Eckstein k, G. Gold {#yy, A. Grainger zz,
RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE
 In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
In Practice RECENT ADVANCES IN CLINICAL MR OF ARTICULAR CARTILAGE By Atsuya Watanabe, MD, PhD, Director, Advanced Diagnostic Imaging Center and Associate Professor, Department of Orthopedic Surgery, Teikyo
Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study
 Osteoarthritis and Cartilage 18 (2010) 1386e1392 Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study A. Guermazi
Osteoarthritis and Cartilage 18 (2010) 1386e1392 Cyst-like lesions of the knee joint and their relation to incident knee pain and development of radiographic osteoarthritis: the MOST study A. Guermazi
Imaging of Articular Cartilage
 Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
Clinical Imaging of Articular Cartilage Imaging of Articular Cartilage Prof. Dr. K. Verstraete Ghent University Introduction : Articular Cartilage Histology and biochemical composition Review of Imaging
E. ÇAĞLAR, G. ŞAH N 1, T. OĞUR, E. AKTAŞ. Introduction. Abstract. OBJECTIVE: To identify changes in
 European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
European Review for Medical and Pharmacological Sciences Quantitative evaluation of hyaline articular cartilage T2 maps of knee and determine the relationship of cartilage T2 values with age, gender, articular
Post-injury painful and locked knee
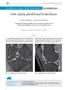 H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
H R J Post-injury painful and locked knee, p. 54-59 Clinical Case - Test Yourself Musculoskeletal Imaging Post-injury painful and locked knee Ioannis I. Daskalakis 1, 2, Apostolos H. Karantanas 1, 2 1
What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
 ARTHRITIS & RHEUMATOLOGY Vol. 67, No. 8, August 2015, pp 2085 2096 DOI 10.1002/art.39176 VC 2015, American College of Rheumatology What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
ARTHRITIS & RHEUMATOLOGY Vol. 67, No. 8, August 2015, pp 2085 2096 DOI 10.1002/art.39176 VC 2015, American College of Rheumatology What Comes First? Multitissue Involvement Leading to Radiographic Osteoarthritis
MRI of the Knee: Part 2 - menisci. Mark Anderson, M.D. University of Virginia Health System
 MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
MRI of the Knee: Part 2 - menisci Mark Anderson, M.D. University of Virginia Health System Learning Objectives At the end of the presentation, each participant should be able to: describe the normal anatomy
Prevalence of Meniscal Radial Tears of the Knee Revealed by MRI After Surgery
 Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Downloaded from www.ajronline.org by 46.3.207.114 on 12/22/17 from IP address 46.3.207.114. Copyright RRS. For personal use only; all rights reserved Thomas Magee 1 Marc Shapiro David Williams Received
Summary. Introduction
 Osteoarthritis and Cartilage (1999) 7, 526 532 1999 OsteoArthritis Research Society International 1063 4584/99/060526+07 $12.00/0 Article No. joca.1999.0256, available online at http://www.idealibrary.com
Osteoarthritis and Cartilage (1999) 7, 526 532 1999 OsteoArthritis Research Society International 1063 4584/99/060526+07 $12.00/0 Article No. joca.1999.0256, available online at http://www.idealibrary.com
Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings
 Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Chin J Radiol 2005; 30: 199-204 199 Stability of Post Traumatic Osteochondritis Dissecans of the Knee: MR Imaging Findings YU-CHUNG HUNG 1 JON-KWAY HUANG 1,2 Department of Radiology 1, Mackay Memorial
Why Talk About Technique? MRI of the Knee:
 Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
Why Talk About Technique? MRI of the Knee: Part 1 - Imaging Techniques Mark Anderson, M.D. University of Virginia Health Sciences Center Charlottesville, Virginia Always had an interest teach our fellows
The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic Knee Osteoarthritis
 ARTHRITIS & RHEUMATISM Vol. 54, No. 3, March 2006, pp 795 801 DOI 10.1002/art.21724 2006, American College of Rheumatology The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic
ARTHRITIS & RHEUMATISM Vol. 54, No. 3, March 2006, pp 795 801 DOI 10.1002/art.21724 2006, American College of Rheumatology The Association of Meniscal Pathologic Changes With Cartilage Loss in Symptomatic
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA
 Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Knee MRI Update Case Review 2009 Russell C. Fritz, M.D. National Orthopedic Imaging Associates San Francisco, CA Meniscal Tears -linear increased signal extending to an articular surface is the hallmark
Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence and Progression
 ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
ARTHRITIS & RHEUMATISM Vol. 65, No. 2, February 2013, pp 355 362 DOI 10.1002/art.37726 2013, American College of Rheumatology Valgus Malalignment Is a Risk Factor for Lateral Knee Osteoarthritis Incidence
Imaging the Athlete s Knee. Peter Lowry, MD Musculoskeletal Radiology University of Colorado
 Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Imaging the Athlete s Knee Peter Lowry, MD Musculoskeletal Radiology University of Colorado None Disclosures Knee Imaging: Radiographs Can be performed weight-bearing or non-weight-bearing View options
Quantitative Comparison of 2D and 3D MRI Techniques for the Evaluation of Chondromalacia Patellae in 3.0T MR Imaging of the Knee
 doi: 10.5505/actamedica.2016.81905 Acta Medica Anatolia Volume 4 Issue 3 2016 Quantitative Comparison of 2D and 3D MRI Techniques for the Evaluation of Chondromalacia Patellae in 3.0T MR Imaging of the
doi: 10.5505/actamedica.2016.81905 Acta Medica Anatolia Volume 4 Issue 3 2016 Quantitative Comparison of 2D and 3D MRI Techniques for the Evaluation of Chondromalacia Patellae in 3.0T MR Imaging of the
The Knee. Prof. Oluwadiya Kehinde
 The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
The Knee Prof. Oluwadiya Kehinde www.oluwadiya.sitesled.com The Knee: Introduction 3 bones: femur, tibia and patella 2 separate joints: tibiofemoral and patellofemoral. Function: i. Primarily a hinge joint,
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration
 Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
Meniscus T2 Relaxation Time at Various Stages of Knee Joint Degeneration Richard Kijowski, Michael Fazio, Benjamin Beduhn, and Fang Liu Department of Radiology University of Wisconsin School of Medicine
MY PATIENT HAS KNEE PAIN. David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging
 MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
MY PATIENT HAS KNEE PAIN David Levi, MD Chief, Division of Musculoskeletal l limaging Atlantic Medical Imaging Causes of knee pain Non traumatic Trauma Osteoarthritis Patellofemoral pain Menisci or ligaments
Andrew J Grainger Leeds, UK
 Andrew J Grainger Leeds, UK Osteoarthri6s (OA) How do we diagnose OA of the knee at MRI? What associated features do we see? Why do they maeer? When is it not OA? We think we have a clear understanding
Andrew J Grainger Leeds, UK Osteoarthri6s (OA) How do we diagnose OA of the knee at MRI? What associated features do we see? Why do they maeer? When is it not OA? We think we have a clear understanding
Meniscal tears on 3T MR: Patterns, pearls and pitfalls
 Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
Meniscal tears on 3T MR: Patterns, pearls and pitfalls Poster No.: C-2221 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: J. C. Kandathil; Singapore/SG Keywords: Knee injuries,
Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA
 Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA 1. Overview... 1 1.1 SAS dataset... 1 1.2 Contents of dataset... 1 1.3 Merging
Central Reading of Knee X-rays for Kellgren & Lawrence Grade and Individual Radiographic Features of Tibiofemoral Knee OA 1. Overview... 1 1.1 SAS dataset... 1 1.2 Contents of dataset... 1 1.3 Merging
Frequency of Baker s Cysts in Cases of Meniscal Injury
 International Journal of Research Studies in Biosciences (IJRSB) Volume 4, Issue 1, January 2016, PP 10-14 ISSN 2349-0357 (Print) & ISSN 2349-0365 (Online) http://dx.doi.org/10.20431/2349-0365.0401003
International Journal of Research Studies in Biosciences (IJRSB) Volume 4, Issue 1, January 2016, PP 10-14 ISSN 2349-0357 (Print) & ISSN 2349-0365 (Online) http://dx.doi.org/10.20431/2349-0365.0401003
D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1.
 Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
Responsiveness of qualitative and quantitative MRI measures over 2.7 years D. Doré 1, C. Ding 1,2, J.P. Pelletier 3, J. Martel-Pelletier 3, F. Cicuttini 2, G. Jones 1. 1 Menzies Research Institute Tasmania,
Knee: Cruciate Ligaments
 72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
72 Knee: Cruciate Ligaments R. Kent Sanders Sagittal oblique 2.5-mm sequences along the plane of the anterior cruciate ligament (ACL) typically yield three to four images of the ACL, with the first medial
MENISCAL INJURY. Meniscus. Anterior Roots. Medial Meniscus. Lateral Meniscus. Posterior Roots. MRI and Arthroscopic Findings
 Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
Meniscus Anterior Roots MENISCAL INJURY MRI and Arthroscopic Findings Medial Meniscus AH PH PH AH Lateral Meniscus Rawiwan Pattaweerakul Naresuan University Hospital Posterior Roots Meniscus Normal Meniscus
International Cartilage Repair Society
 Osteoarthritis and Cartilage (2009) 17, 748e753 ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.09.013 The association of meniscal
Osteoarthritis and Cartilage (2009) 17, 748e753 ª 2008 Osteoarthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2008.09.013 The association of meniscal
Magnetic resonance imaging in knee synovitis: Clinical utility in differentiating asymptomatic and symptomatic meniscal tears
 bs_bs_banner Journal of Medical Imaging and Radiation Oncology 59 (2015) 1 6 RADIOLOGY REVIEW ARTICLE Magnetic resonance imaging in knee synovitis: Clinical utility in differentiating asymptomatic and
bs_bs_banner Journal of Medical Imaging and Radiation Oncology 59 (2015) 1 6 RADIOLOGY REVIEW ARTICLE Magnetic resonance imaging in knee synovitis: Clinical utility in differentiating asymptomatic and
Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies
 Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
Original article: Comparative study of high resolusion ultrasonography and magnetic resonance imaging in diagnosing traumatic knee injuries & pathologies Dr. Rakesh Gujjar*, Dr. R. P. Bansal, Dr. Sandeep
International Cartilage Repair Society
 OsteoArthritis and Cartilage (2006) 14, 1081e1085 ª 2006 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.05.011 MRI of bone marrow
OsteoArthritis and Cartilage (2006) 14, 1081e1085 ª 2006 OsteoArthritis Research Society International. Published by Elsevier Ltd. All rights reserved. doi:10.1016/j.joca.2006.05.011 MRI of bone marrow
JMSCR Vol 05 Issue 01 Page January
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.28 Diagnostic Accuracy of Magnetic Resonance
The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and Radiographic Progression in Men and Women With Knee Osteoarthritis
 ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
ARTHRITIS & RHEUMATISM Vol. 52, No. 10, October 2005, pp 3152 3159 DOI 10.1002/art.21296 2005, American College of Rheumatology The Relationship Between Cartilage Loss on Magnetic Resonance Imaging and
FAI syndrome with or without labral tear.
 Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
Case This 16-year-old female, soccer athlete was treated for pain in the right groin previously. Now has acute onset of pain in the left hip. The pain was in the groin that was worse with activities. Diagnosis
The Knee. Tibio-Femoral
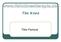 The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
The Knee Tibio-Femoral Osteology Distal Femur with Proximal Tibia Largest Joint Cavity in the Body A modified hinge joint with significant passive rotation Technically, one degree of freedom (Flexion/Extension)
dgemric Effectively Predicts Cartilage Damage Associated with Femoroacetabular Impingement
 Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Riccardo Lattanzi 1,2 Catherine Petchprapa 2 Daniele Ascani 1 Roy I. Davidovitch 3 Thomas Youm 3 Robert J. Meislin 3 Michael. Recht 2 1 The Bernard and Irene Schwartz Center for Biomedical Imaging, New
Correspondence should be addressed to Thomas Kurien;
 Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Case Reports in Orthopedics Volume 2016, Article ID 6043497, 5 pages http://dx.doi.org/10.1155/2016/6043497 Case Report Resection and Resolution of Bone Marrow Lesions Associated with an Improvement of
Knee Joint Anatomy 101
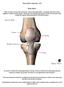 Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Knee Joint Anatomy 101 Bone Basics There are three bones at the knee joint femur, tibia and patella commonly referred to as the thighbone, shinbone and kneecap. The fibula is not typically associated with
Standardised. knee. scanning of the. Basic pathology. Nemanja Damjanov. University of Belgrade Institute of Rheumatology
 Standardised scanning of the Nemanja Damjanov University of Belgrade Institute of Rheumatology knee Basic pathology Disclosure Lecturer: Pfizer, Abbvie, Roche, MSD, Boehringer-Ingelheim, Gedeon Richter,
Standardised scanning of the Nemanja Damjanov University of Belgrade Institute of Rheumatology knee Basic pathology Disclosure Lecturer: Pfizer, Abbvie, Roche, MSD, Boehringer-Ingelheim, Gedeon Richter,
Musculoskeletal Imaging Original Research
 Musculoskeletal Imaging Original Research Isotropic Resolution 3D FSE MRI of Articular Cartilage of Knee Joint Musculoskeletal Imaging Original Research Cristy N. Gustas 1 Donna G. Blankenbaker 2 Alejandro
Musculoskeletal Imaging Original Research Isotropic Resolution 3D FSE MRI of Articular Cartilage of Knee Joint Musculoskeletal Imaging Original Research Cristy N. Gustas 1 Donna G. Blankenbaker 2 Alejandro
The association between meniscal and cruciate ligament damage and knee pain in community residents
 Osteoarthritis and Cartilage 19 (2011) 1422e1428 The association between meniscal and cruciate ligament damage and knee pain in community residents H.A. Kimyz *,I.Kimx, Y.W. Songk,D.H.Kim{,J.Niu#, A.Guermaziyy,
Osteoarthritis and Cartilage 19 (2011) 1422e1428 The association between meniscal and cruciate ligament damage and knee pain in community residents H.A. Kimyz *,I.Kimx, Y.W. Songk,D.H.Kim{,J.Niu#, A.Guermaziyy,
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries
 What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
What is the most effective MRI specific findings for lateral meniscus posterior root tear in ACL injuries Kazuki Asai 1), Junsuke Nakase 1), Kengo Shimozaki 1), Kazu Toyooka 1), Hiroyuki Tsuchiya 1) 1)
MRI of Bucket-Handle Te a rs of the Meniscus of the Knee 1
 MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
MRI of ucket-handle Te a rs of the Meniscus of the Knee 1 Joon Yong Park, M.D., Young-uk Lee M.D., Eun-Chul Chung M.D., Hae-Won Park M.D., E u n - Kyung Youn M.D., Shin Ho Kook, M.D., Young Rae Lee, M.D.
Joints of the Lower Limb II
 Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
Joints of the Lower Limb II Lecture Objectives Describe the components of the knee and ankle joint. List the ligaments associated with these joints and their attachments. List the muscles acting on these
MRI of distended bursa around the knee
 MRI of distended bursa around the knee Poster No.: C-2240 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: P. Papadopoulou, I. Kalaitzoglou, N. Michailidis, I. Tsifoundoudis,
MRI of distended bursa around the knee Poster No.: C-2240 Congress: ECR 2010 Type: Educational Exhibit Topic: Musculoskeletal Authors: P. Papadopoulou, I. Kalaitzoglou, N. Michailidis, I. Tsifoundoudis,
Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis Initiative (OAI)
 Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 RESEARCH ARTICLE Open Access Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis
Bruns et al. BMC Musculoskeletal Disorders 2014, 15:32 RESEARCH ARTICLE Open Access Meniscus body position and its change over four years in asymptomatic adults: a cohort study using data from the Osteoarthritis
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation. Disclosures. Outline. Joint Effusion. Suprapatellar recess
 Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Knee, Ankle, and Foot: Normal and Abnormal Features with MRI and Ultrasound Correlation Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan
Distribution of MR-detected cartilage defects of the patellofemoral joint in chronic knee pain
 OsteoArthritis and Cartilage (2003) 11, 494 498 Crown Copyright 2003 Published by Elsevier Science Ltd on behalf of OsteoArthritis Research Society International. All rights reserved. doi:10.1016/s1063-4584(03)00084-0
OsteoArthritis and Cartilage (2003) 11, 494 498 Crown Copyright 2003 Published by Elsevier Science Ltd on behalf of OsteoArthritis Research Society International. All rights reserved. doi:10.1016/s1063-4584(03)00084-0
and K n e e J o i n t Is the most complicated joint in the body!!!!
 K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
K n e e J o i n t K n e e J o i n t Is the most complicated joint in the body!!!! 1-Consists of two condylar joints between: A-The medial and lateral condyles of the femur and The condyles of the tibia
Meniscal Tears: Role of Axial MRI Alone and in Combination with Other Imaging Planes
 Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Nefise Cagla Tarhan 1,2 Christine. Chung 1 urea Valeria Rosa Mohana-orges 1 Tudor Hughes 1 Donald Resnick 1 Received September 30, 2003; accepted after revision February 2, 2004. 1 Department of Radiology,
Original Research JOURNAL OF MAGNETIC RESONANCE IMAGING 22: (2005)
 JOURNAL OF MAGNETIC RESONANCE IMAGING 22:788 793 (2005) Original Research STIR vs. T1-Weighted Fat-Suppressed Gadolinium- Enhanced MRI of Bone Marrow Edema of the Knee: Computer-Assisted Quantitative Comparison
JOURNAL OF MAGNETIC RESONANCE IMAGING 22:788 793 (2005) Original Research STIR vs. T1-Weighted Fat-Suppressed Gadolinium- Enhanced MRI of Bone Marrow Edema of the Knee: Computer-Assisted Quantitative Comparison
Unlocking the locked Knee
 Unlocking the locked Knee Poster No.: P-0027 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. P. SINGH, S. Srivastava, S. S. BAIJAL ; Gurgaon, Delhi 1 1 2 1 2 NCR/IN, LUCKNOW, UTTAR PRADESH/IN
Unlocking the locked Knee Poster No.: P-0027 Congress: ESSR 2013 Type: Scientific Exhibit Authors: J. P. SINGH, S. Srivastava, S. S. BAIJAL ; Gurgaon, Delhi 1 1 2 1 2 NCR/IN, LUCKNOW, UTTAR PRADESH/IN
ORIGINAL ARTICLE. ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel
 ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
ROLE OF MRI IN EVALUATION OF TRAUMATIC KNEE INJURIES Saurabh Chaudhuri, Priscilla Joshi, Mohit Goel 1. Associate Professor, Department of Radiodiagnosis & imaging, Bharati Vidyapeeth Medical College and
Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping
 TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
TR_002 Technical Reports Knee Articular Cartilage in an Asymptomatic Population : Comparison of T1rho and T2 Mapping Min A Yoon 1,*, Suk-Joo Hong 1, Chang Ho Kang 2, Baek Hyun Kim 3 1 Korea University
BASELINE QUESTIONNAIRE (SURGEON)
 SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
SECTION A: STUDY INFORMATION Subject ID: - - Study Visit: Baseline Site Number: Date: / / Surgeon ID: SECTION B: INITIAL SURGEON HISTORY B1. Previous Knee Surgery: Yes No Not recorded B2. Number of Previous
ADVANCED IMAGING OF THE KNEE
 MENISCAL ANATOMY ADVANCED IMAGING OF THE KNEE MENISCAL ABNORMALITIES MENISCAL FUNCTION MENISCAL FUNCTION load transmission shock absorption stability The menisci DO NOT function as primary stabilizers
MENISCAL ANATOMY ADVANCED IMAGING OF THE KNEE MENISCAL ABNORMALITIES MENISCAL FUNCTION MENISCAL FUNCTION load transmission shock absorption stability The menisci DO NOT function as primary stabilizers
Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study
 Osteoarthritis and Cartilage 20 (2012) 1227e1233 Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study D.
Osteoarthritis and Cartilage 20 (2012) 1227e1233 Knee malalignment is associated with an increased risk for incident and enlarging bone marrow lesions in the more loaded compartments: the MOST study D.
FieldStrength. Achieva 3.0T enables cutting-edge applications, best-in-class MSK images
 FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
FieldStrength Publication for the Philips MRI Community Issue 33 December 2007 Achieva 3.0T enables cutting-edge applications, best-in-class MSK images Palo Alto Medical Clinic Sports Medicine Center employs
Cartilage Repair Options
 Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging of Cartilage Repair Carl S. Winalski, MD Imaging Institute Department of Biomedical Engineering Cleveland Clinic Cartilage Repair Options Direct repair Marrow stimulation Autologous transplantation
Imaging the Knee 17/10/2017. Friction syndrome Common in runners or cyclists Fluid between ITB and Lateral femoral condyle
 17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
17/10/2017 Imaging the Knee Alicia M. Yochum RN, DC, DACBR, RMSK Iliotibial Band Syndrome Ligamentous Tears (ACL, PCL, MCL, LCL) Meniscal Tears Cartilage Degeneration Quadriceps/Patellar tendinosis Osteochondral
Original article RHEUMATOLOGY
 RHEUMATOLOGY Rheumatology 2017;56:113 120 doi:10.1093/rheumatology/kew368 Advance Access publication 25 October 2016 Original article Predictive value of MRI features for development of radiographic osteoarthritis
RHEUMATOLOGY Rheumatology 2017;56:113 120 doi:10.1093/rheumatology/kew368 Advance Access publication 25 October 2016 Original article Predictive value of MRI features for development of radiographic osteoarthritis
Conservative surgical treatments for osteoarthritis: A Finite Element Study
 Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
Conservative surgical treatments for osteoarthritis: A Finite Element Study Diagarajen Carpanen, BEng (Hons), Franziska Reisse, BEng(Hons), Howard Hillstrom, PhD, Kevin Cheah, FRCS, Rob Walker, PhD, Rajshree
Ultrasound of the Knee
 Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Ultrasound of the Knee Jon A. Jacobson, M.D. Professor of Radiology Director, Division of Musculoskeletal Radiology University of Michigan Disclosures: Consultant: Bioclinica Book Royalties: Elsevier Advisory
Osteoarthritis and Cartilage 18 (2010)
 Osteoarthritis and Cartilage 18 (2010) 547 554 Sensitivity to change of cartilage morphometry using coronal FLASH, sagittal DESS, and coronal MPR DESS protocols comparative data from the osteoarthritis
Osteoarthritis and Cartilage 18 (2010) 547 554 Sensitivity to change of cartilage morphometry using coronal FLASH, sagittal DESS, and coronal MPR DESS protocols comparative data from the osteoarthritis
Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries
 Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Original Research Article Role of magnetic resonance imaging in the evaluation of traumatic knee joint injuries Dudhe Mahesh 1*, Rathi Varsha 2 1 Resident, 2 Professor, Department of Radio-Diagnosis, Grant
Planning knee OA prevention studies in obese populations Lessons from the Multicenter Osteoarthritis Study (MOST) and Osteoathritis Initiative (OAI)
 Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
Planning knee OA prevention studies in obese populations Lessons from the (MOST) and Osteoathritis Initiative (OAI) Michael Nevitt, PhD UCSF Epidemiology and Biostatistics OAI and MOST Coordinating Centers
Osteoarthritis and Cartilage 19 (2011) 1433e1439
 Osteoarthritis and Cartilage 19 (2011) 1433e1439 Comparing non-enhanced and enhanced sequences in the assessment of effusion and synovitis in knee OA: associations with clinical, macroscopic and microscopic
Osteoarthritis and Cartilage 19 (2011) 1433e1439 Comparing non-enhanced and enhanced sequences in the assessment of effusion and synovitis in knee OA: associations with clinical, macroscopic and microscopic
White Rose Research Online URL for this paper: Version: Accepted Version
 This is a repository copy of Osteoarthritic bone marrow lesions almost exclusively colocate with denuded cartilage: a 3D study using data from the Osteoarthritis Initiative. White Rose Research Online
This is a repository copy of Osteoarthritic bone marrow lesions almost exclusively colocate with denuded cartilage: a 3D study using data from the Osteoarthritis Initiative. White Rose Research Online
Clinics in diagnostic imaging (177)
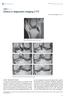 Singapore Med J 2017; 58(5): 241-245 doi: 10.11622/smedj.2017038 CMEArticle Clinics in diagnostic imaging (177) Poh Lye Paul See, MBBS, FRCR Fig. 1 Sagittal proton density (PD)-weighted fast spin-echo
Singapore Med J 2017; 58(5): 241-245 doi: 10.11622/smedj.2017038 CMEArticle Clinics in diagnostic imaging (177) Poh Lye Paul See, MBBS, FRCR Fig. 1 Sagittal proton density (PD)-weighted fast spin-echo
Case study #11 Rt. knee
 The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
The patient is a 55 year old female who presents with bilateral knee pain. Patient is a collegiate softball coach and has a very active lifestyle and career that is hampered by her chronic knee pain. She
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping
 Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Medial Knee Osteoarthritis Precedes Medial Meniscal Posterior Root Tear with an Event of Painful Popping Dhong Won Lee, M.D, Ji Nam Kim, M.D., Jin Goo Kim, M.D., Ph.D. KonKuk University Medical Center
Viviane Khoury, MD. Assistant Professor Department of Radiology University of Pennsylvania
 U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
U Penn Diagnostic Imaging: On the Cape Chatham, MA July 11-15, 2016 Viviane Khoury, MD Assistant Professor Department of Radiology University of Pennsylvania Hip imaging has changed in recent years: new
The Impact of Age on Knee Injury Treatment
 The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
The Impact of Age on Knee Injury Treatment Focus on the Meniscus Dr. Alvin J. Detterline, MD Sports Medicine and Orthopaedic Surgery Towson Orthopaedic Associates University of Maryland St. Joseph Medical
Osteoarthritis year 2011 in review: imaging in OA e a radiologists perspective
 Osteoarthritis and Cartilage 20 (2012) 207e214 Review Osteoarthritis year 2011 in review: imaging in OA e a radiologists perspective D. Hayashi y, F.W. Roemer yz, A. Guermazi y * y Department of Radiology,
Osteoarthritis and Cartilage 20 (2012) 207e214 Review Osteoarthritis year 2011 in review: imaging in OA e a radiologists perspective D. Hayashi y, F.W. Roemer yz, A. Guermazi y * y Department of Radiology,
The relationship between chondromalacia patella, medial meniscal tear and medial periarticular bursitis in patients with osteoarthritis
 research article 401 The relationship between chondromalacia patella, medial meniscal tear and medial periarticular bursitis in patients with osteoarthritis Mustafa Resorlu 1, Davut Doner 2, Ozan Karatag
research article 401 The relationship between chondromalacia patella, medial meniscal tear and medial periarticular bursitis in patients with osteoarthritis Mustafa Resorlu 1, Davut Doner 2, Ozan Karatag
Chronic knee pain in adults - a multimodality approach or which modality to choose and when?
 Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Chronic knee pain in adults - a multimodality approach or which modality to choose and when? Poster No.: P-0157 Congress: ESSR 2013 Type: Authors: Keywords: DOI: Scientific Exhibit E. Ilieva, V. Tasseva,
Original Report. The Reverse Segond Fracture: Association with a Tear of the Posterior Cruciate Ligament and Medial Meniscus
 Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Eva M. Escobedo 1 William J. Mills 2 John. Hunter 1 Received July 10, 2001; accepted after revision October 1, 2001. 1 Department of Radiology, University of Washington Harborview Medical enter, 325 Ninth
Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A
 Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
Clinical > Pediatric Imaging Case Report: Knee MR Imaging of Haemarthrosis in a Case of Haemophilia A M. A. Weber, J. K. Kloth University Hospital Heidelberg, Department of Diagnostic and Interventional
MRI of the Knee: Part 4 - normal variants that may simulate disease. Mark Anderson, M.D. University of Virginia
 MRI of the Knee: Part 4 - normal variants that may simulate disease Mark Anderson, M.D. University of Virginia discuss the most common normal variants in the pediatric knee that may simulate pathology
MRI of the Knee: Part 4 - normal variants that may simulate disease Mark Anderson, M.D. University of Virginia discuss the most common normal variants in the pediatric knee that may simulate pathology
Publication for the Philips MRI Community
 FieldStrength Publication for the Philips MRI Community Issue 38 Summer 2009 Pediatric MSK imaging benefits from tailored scan protocols Vanderbilt University Children s Hospital builds dedicated scans
FieldStrength Publication for the Philips MRI Community Issue 38 Summer 2009 Pediatric MSK imaging benefits from tailored scan protocols Vanderbilt University Children s Hospital builds dedicated scans
High Prevalence of Abnormal MR Findings of the Distal Semimembranosus Tendon: Contributing Factors Based on Demographic, Radiographic, and MR Features
 Musculoskeletal Imaging Original Research Yoon et al. MRI of the Distal Semimembranosus Tendon Musculoskeletal Imaging Original Research Min A Yoon 1 Ja-Young Choi Hyun Kyong Lim Hye Jin Yoo Sung Hwan
Musculoskeletal Imaging Original Research Yoon et al. MRI of the Distal Semimembranosus Tendon Musculoskeletal Imaging Original Research Min A Yoon 1 Ja-Young Choi Hyun Kyong Lim Hye Jin Yoo Sung Hwan
Knee: Meniscus Back to Basics
 Knee: Meniscus Back to Basics Kyung Jin Suh kyungjin.suh@gmail.com Doctor Radiology, Daegu, KOREA Medial Lateral 7.7 10.2 11.6 9.6 10.6 mm Posterior > Anterior horn 10.6 mm Posterior = Anterior horn Medial
Knee: Meniscus Back to Basics Kyung Jin Suh kyungjin.suh@gmail.com Doctor Radiology, Daegu, KOREA Medial Lateral 7.7 10.2 11.6 9.6 10.6 mm Posterior > Anterior horn 10.6 mm Posterior = Anterior horn Medial
a - CM EARTICLE Clinics in diagnostic imaging (139) !Medical Education Singapore Med J 2012; 53(4) CASE PRESENTATION
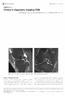 !Medical Education Singapore Med J 2012; 53(4) 283 CM EARTICLE Clinics in diagnostic imaging (139) Wei Yang Liml, MBBS, FRCR, Nor Azam Mahmud2, MD, MMed, Wilfred CG Peh3, FRCP, FRCR a - - - Fig. 1 Sagittal
!Medical Education Singapore Med J 2012; 53(4) 283 CM EARTICLE Clinics in diagnostic imaging (139) Wei Yang Liml, MBBS, FRCR, Nor Azam Mahmud2, MD, MMed, Wilfred CG Peh3, FRCP, FRCR a - - - Fig. 1 Sagittal
