Founders Seminar. Handout material. Challenging Cases in Head and Neck Surgical Pathology
|
|
|
- Jason Norton
- 5 years ago
- Views:
Transcription
1 Founders Seminar Handout material Challenging Cases in Head and Neck Surgical Pathology Robert A. Robinson Department of Pathology University of Iowa
2 American Academy of Oral and Maxillofacial Pathology International Association of Oral Pathologists Joint Meeting Vancouver, B.C. Canada
3 Challenging Cases in Head and Neck Surgical Pathology Sinonasal tumor in an 18 year old Thyroid tumor in a 55 year old 52 year old female with a neck mass and a sore throat Nasal tumor in a 56 year old Cases will range from one with a very broad differential to cases whose differential is more focused
4 Challenging Cases in Head and Neck Surgical Pathology The diagnosis of these cases will variably include the use of: Routine H&E stains Immunohistochemistry For some cases we will also discuss evolving NGS use
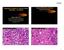
5 Case 1 An 18 year old female presented with a short history of headaches and sinus pain. Imaging revealed a mass in the left posterior wall of the maxillary sinus with involvement of the infratemporal fossa and some intracranial extension.
6 A Caldwell-Luc incision was made in the labio-gingival sulcus and a small opening was made in anterior face of the maxillary sinus. The posterior wall of the maxillary sinus was bulging forward and a biopsy of the mass was obtained from an incision into pterygopalatine fossa.
7 A sample for frozen section was evaluated and revealed fat. A second sample sent for frozen section was diagnosed as: Small blue cell tumor, defer to permanent sections for final diagnosis.
8 H&E stains show a blue cell tumor Immunohistochemical stains were performed What stains would you order?
9 EWS-PNET Ewing s Sarcoma Family of Tumors (ESFT)
10 Case 1 Round Cell Tumors of the Nasal Cavity, Paranasal Sinus and Skull Base
11 Objectives for Case 1 Discuss some of the lesions in the differential diagnosis of round cell tumors Identify hints on H&E slides that might help select the initial antibody panels in round cell tumors Discuss potential traps in histology and immunohistochemistry of undifferentiated tumors Discuss appropriate use of next generation (NGS) fusion panels in diagnostic pathology
12 Objectives for Case 1 Discuss some of the lesions in the differential diagnosis of round cell tumors Although we are focusing on sinonasal/nasal/skull base location for this case, the workup of round cell tumors anywhere is similar.
13 Objectives for Case 1 Identify hints on H&E slides that might help select the initial antibody panels in round cell tumors In my lab, I can choose between ~200 antibodies, but I can t choose them all!
14 Objectives for Case 1 Discuss traps in histology and immunohistochemistry Immunohistochemical antibodies can lead us into incorrect diagnoses because the antibodies sometimes bind to antigens that we weren t expecting to be on that specific tumor type.
15 Objectives for Case 1 Discuss appropriate use of fusion panels and next generation sequencing (NGS) in diagnostic pathology Molecular testing using NGS is increasing and can be useful in some cases.
16 Round Cell Tumors of the Nasal Cavity, Paranasal Sinus and Skull Base Many of these tumors are not seen everyday, yet common enough that you need to have a way to manage their diagnosis
17 Round cell tumor differential includes a broad spectrum of tissue types Neuroectodermal Mesenchymal Hematopoietic Epithelial
18 Hematopoietic differentiation Lymphoma Myeloid sarcoma Sinonasal / Skull Base Round Cell Tumors Neuroectodermal differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma Mesenchymal differentiation Rhabdomyosarcoma Synovial sarcoma Mesenchymal chondrosarcoma Desmoplastic small round cell tumor Small cell osteosarcoma
19 Sinonasal / Skull Base Round Cell Tumors Epithelial differentiation Adenoid cystic carcinoma Lymphoepithelial carcinoma Sinonasal primary vs extension from nasopharynx Sinonasal non-keratinizing squamous carcinoma Sinonasal basaloid carcinomas Sinonasal undifferentiated carcinoma (SNUC) NUT midline carcinoma SMARCB1 deficient carcinoma HPV-related carcinoma with adenoid cystic carcinoma- like features
20 Sinonasal / Skull Base Round Cell Tumors Neuroectodermal differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma
21 Sinonasal / Skull Base Round Cell Tumors Neuroectodermal differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma
22 Ewing s Sarcoma Family of Tumors (ESFT) All malignant All aggressive All histologically similar in appearance All have similar genetic translocation Most occur in children and young adults
23 Ewing s Sarcoma Family of Tumors (ESFT) PNET (primitive neuroectodermal tumor) (primitive peripheral neuroectodermal tumor) Ewing s sarcoma Askin s tumor (Thoraco-pulmonary tumor) Common term is EWS-PNET
24 Ewing s Sarcoma Family of Tumors (ESFT) PNET Ewing s sarcoma Askin s tumor (Thoraco-pulmonary tumor) These tumors are arranged on a spectrum
25 Common term is EWS-PNET PNET Classically soft tissue location Ewing s sarcoma Classically bone location Askin s tumor (Thoraco-pulmonary tumor) Classically thorax/pulmonary location
26 EWS/PNET The incidence for all ages is one case per 1 million people in the United States. In patients aged 10 to 19 years, the incidence is between nine and ten cases per 1 million people.
27 Presentation of EWS/PNET ~40 present in 1 st decade ~50% of cases in 2 nd decade Predilection for Caucasians Slight male predominance
28 Most common extraosseous primary sites Trunk (32%) Extremity (26%) Head and neck (18%) of these, 20% are in sinonasal tract Retroperitoneum (16%) Other sites (9%)
29 EWS/PNET Morphologic Variants Hyalinized Spindled Fasicular Adamantinoma-like Recently described Squamous differentiation Diffuse keratin expression
30 CD 99 CD 99 is a defining feature of primitive neuroectodermal which is peripheral non- Central Nervous System (CNS)
31 CD 99 CD99 is a 32kDa glycosylated transmembrane protein encoded by the MIC2 gene, highly expressed in all Ewing's sarcomas (EWS / PNET) CD99 has been involved in many cellular processes, such as cell adhesion, apoptosis and differentiation and intracellular trafficking
32 There are two subclassificatons of PNET Non-CNS CNS ppnet (peripheral Primitive Neuroectodermal Tumor spnet (supratentorial Primitive Neuroectodermal Tumor)
33 Primitive Neuroectodermal Tumor Peripheral vs. CNS Peripheral Primitive Neuroectodermal Tumor (ppnet): CD99 antigen (MIC2 gene expression of MIC2 antigen) FLI-1 (gene fusion product of EWS) is positive in many cases Central Nervous System Primitive Neuroectodermal Tumor (spnet): CD99 antigen (MIC2 antigen) is NOT expressed No FLI-1 expression
34 EWS-PNET result of EWS ETS translocation EWS gene (chromosome 22) encodes a widelyexpressed and highly-conserved RNA-binding protein ETS (erythroblastosis transforming-virus-1) family of transcription factors which are involved in cell proliferation, development, and tumorigenesis. FLI1 ERG (ETS related gene) ETV1 (ETS variant gene 1) ETV4 (ETS variant gene 4, E1AF ) ETV5 (5 th Ewing sarcoma variant, FEV)
35 Chromosomal translocations in EWS-PNET t(11;22)(q24;q12) FLI1-EWS genes : ~90% t(21;22)(q12q12) ERG-EWS genes : ~10% t(7;22)(p22;q12) ETV1-EWS genes : Rare t(17;22)(q12;q12) ETV4(EIAF)-EWS genes : Rare t(2;22)(q33;q12) ETV5(FEV)-EWS genes : Rare
36 t(11;22)(q24;q12) EWSR1 encodes RNA-binding protein involved in DNA transcription 5 sequences from the EWSR1 result in a strong transcriptional regulatory domain FLI1 is part of a family DNA transcription factors that contain Ets domain 3 sequences of FLI1 (or other Ets gene family member) provide for a DNA binding domain.
37 Oncogenic potential of EWS-ETS fusion proteins -EWS-FLI1 functions primarily as a transcription factor to regulate gene expression. EWS-FLI1 may orchestrate multiple oncogenic hits -Activate human telomerase activity through upregulation of TERT (telomerase reverse transcriptase) gene expression -Mediation by upregulation of LAMB3 expression, a gene encoding the ββ3 chain of laminin- 5, a protein often expressed in invading tumor cells
38 EWS-PNET How do we make the diagnosis? Correct histologic features on H&E Supporting immunohistochemistry Translocation testing: FISH NGS fusion panel
39 EWS-PNET How do we make the diagnosis with H&E?
40 Nuclear features of EWS - PNET Dispersed chromatin Micro-nucleoli No anaplasia Growth pattern: Nested or diffuse pattern Necrosis and dystrophic mineralization Monotonous monolayer of cells
41 Larger cells Atypical / Large cell EWS Larger nuclei More pleomorphism Behavior is the same as typical EWS
42 EWS-PNET How do we make the diagnosis? Correct histologic features on H&E Supporting immunohistochemistry Translocation testing: FISH RNA based NGS fusion panel
43 EWS-PNET Pre-1990 s, the only special techniques were to search for glycogen: 1) periodic acid Schiff (PAS) stain 2) Electron microscopy The clinical and radiologic findings were of upmost importance as well
44 Antibodies expressed in EWS-PNET CD99 FLI 1 ERG NSE Synaptophysin CD57 Neurofilament Vimentin: dot like/perinuclear Keratin (20-25%) Desmin S100 (rarely)
45 Antibodies helpful in diagnosis of EWS-PNET CD99: Strong diffuse linear membrane pattern FLI 1: Most EWS-PNET also express ERG: Generally, EWS-ERG fusion cases EWS-ERG fusion cases also express FLI 1 in most cases FLI1 is not considered specific to rearrangement type cross reactivity with the highly homologous ETS DNAbinding domain present in the C-terminus of both ERG and FLI1
46 Some other malignancies with CD99 expression: Small cell melanoma Neuroendocrine carcinoma Poorly differentiated carcinomas, multiple types Prostatic adenocarcinoma Esophageal adenocarcinoma Squamous cell carcinomas of multiple sites Hepatocellular carcinoma Endometrial carcinoma Renal cell carcinoma Urothelial carcinoma Mucoepidermoid carcinoma
47 Fli 1 Antibody (Friend Leukemia Integration 1) Nuclear staining Endothelial cells Small lymphocytes Positive: EWS / PNET Vascular lesions Variable: Melanoma Merkel cell Lymphoma (Lymphoblastic, ALC, AITC) Desmoplastic small round cell tumor
48 EWS-PNET How do we make the diagnosis? Correct histologic features on H&E Supporting immunohistochemistry Translocation testing: FISH Targeted NGS panel
49 EWS/PNET FISH t(11;22)(q24;q12) FLI1-EWS genes : ~90% Most cytogenetic FISH studies target this translocation FISH has a relatively fast turn around time However, since this could underestimate 10% of cases, additional FISH probes or other molecular technques should be used if the clinical and histologic/immunohistologic findings support EWS/PNET
50 Even though florescence in situ hybridization (FISH) technique is the current gold standard in fusion detection, it can generally not detect a large number of possible fusions in parallel.. Fusion targets for probe design must be known in FISH FISH lacks high-resolution evaluation of the molecular identity of these fusion partners.
51 Fusion panels Panels are developed to have broad coverage Identifies both gene partners in a rearrangement Diagnostic and therapeutic information from a sole sample. Panels are developed to use formalin fixed paraffin embedded tissue
52 When should NGS be employed in clinical practice? Some tumors can have identical H & E morphology with Ewing s that are not Ewing s. IHC or FISH negative for Ewing s NGS fusion panels may offer diagnostic help
53 Potential downsides for NGS Turn around time is 7-10 days (sometimes in cases of a failed run, 21). Expensive
54 Some tumors share EWS fusion These panels can also detect other EWS fusions Clear cell sarcoma (12;22) Desmoplastic round cell tumor (11;22) t(11;22)(p13;q11.2 or q12) Extraskeletal myxoid chondrosarcoma (9;22)
55 Round cell tumors can share with EWS-PNET: 1) Morphologic similarites 2) Some genetic abnormalities 3) Immunohistochemical studies
56 Prognosis of EWS/PNET Patients with Ewing sarcoma in the distal extremities have the best prognosis. Patients with Ewing sarcoma in the proximal extremities have an intermediate prognosis, followed by patients with central or pelvic sites. Infants and younger patients have a better prognosis than do patients aged 15 years and older
57 Small Round Blue Cell Tumors in the Sinonasal Region with Neuroectodermal Differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma
58 Olfactory neuroblastoma Arises in neuroepithelium in cribriform plate, superior nasal vault/nasal septum Incidence: ~ 3-5 % of sinonasal tumors Gender: Essentially equal Age range: Infancy to 90 s Most cases occur in 5 th and 6 th decades
59 Olfactory neuroblastoma Frequently over diagnosed microscopically Tumors masquerading as ONB Melanoma Sinonasal undifferentiated carcinoma Pituitary adenoma
60 Olfactory neuroblastoma : Lower Grades Cytoplasm Minimal cytoplasm Uniform cells Nuclei Round Salt and pepper chromatin Small chromocenters/nucleoli Mitoses uncommon, can be seen in grade 2 Neurofibrillary matrix Homer Wright rosettes ( Pseudorosettes )
61 Olfactory neuroblastoma : Higher Grades Cytoplasm Minimal cytoplasm, less than low grade Pleomorphism of cells Nuclei Round Coarse chromatin Mitoses No or minimal neurofibrillary matrix Flexner-Wintersteiner rosettes ( true rosettes) Necrosis can be seen
62 Olfactory neuroblastoma Nuclear pleomorphism Fibrillary matrix Mitoses Necrosis Rosettes Architecture
63 Hyams Grading System for Olfactory Neuroblastoma Grade Nuclear Fibrillary Matrix Rosettes Necrosis Pleomorphism I None Prominent HW rosettes None II Low Present HW rosettes None III Moderate Low FW rosettes Rare IV High Absent None Frequent
64 Hyams Grading System for Olfactory Neuroblastoma Grade Lobular Architecture Mitotic Index Preservation I Present Zero II Present Low III May or may not be present Moderate IV May or may not be present High
65 Synaptophysin Chromogranin NSE Olfactory neuroblastoma Positive Immunohistochemistry S-100 (sustentacular cells) Cytokeratin (some cases) Calretinin (seen in other tumors in the differential) Rarely muscle markers if rhabdomyoblastic differentiation( desmin, myogenin)
66 Olfactory neuroblastoma Negative Immunohistochemistry CD 99 FLI- 1 CD45 p63
67 Olfactory neuroblastoma Staging Morita modification of Kadish staging A) Tumor confined to nasal cavity B) Tumor involves nasal cavity and paranasal sinuses C) Tumor extends beyond the nasal cavity and paranasal sinuses D) Metastatic disease (regional or distant)
68 Olfactory neuroblastoma treatment Surgery with curative intent Cranial facial resection Endoscopic sinus surgery Postoperative radiotherapy combined with adjuvant cisplatin-based chemotherapy.
69 Olfactory neuroblastoma treatment Overall survival 85% at 5 years 75% at 10 years. If recurrence, usually it is within the first 4 years but can occur late
70 Neuroectodermal differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma
71 Sinonasal Melanoma Uncommon in sinonasal regions Cutaneous>Orbital>Sinonasal ~ 1% of all melanomas ~ 3-5% of sinonasal tumors Gender: 1:1 Age: Any age but usually 4 th to 8 th decade Usual sites: Nasal Cavity [Nasal septum, lateral nasal wall] Unusual sites: Maxillary sinus and nasopharynx
72 Sinonasal Melanoma BRAF mutations = < 5% in this location [~50-60% of cutaneous melanomas] NRAS mutations = 20% KIT mutations/amplification = ~ 25%
73 Sinonasal Melanoma Before establishing a diagnosis of primary sinonasal melanoma, we must assure that there are no sites of cutaneous melanoma. Rarely the sinonasal region can be a site for metastasis.
74 Sinonasal Melanoma Gross: Nasal melanomas are often polypoid. Microscopic patterns: Sheets Fascicles Organoid Solid Cell appearance: epithelioid clear spindled plasmacytoid rhabdoid small round cell Many cases may be amelanotic
75 IHC markers in the diagnosis of Melanoma S100 HMB45 MITF MART-1 / Melan A Sox 10
76 IHC markers useful for Melanoma S100 Neural crest (and other diverse cell types) HMB45 (Human Melanoma Black 45) - monoclonal antibody derived from lymph node tissue containing metastatic pigmented melanoma MITF- microphthalmia transcription factor (MITF); melanocyte master regulator; DNA-binding nuclear protein that regulates several melanocytic genes that play a central role in the development, differentiation, and survival of melanocytes. Mart 1 (melanoma antigen recognized by T-cells 1)/Melan A Sox 10-Sry-related HMG-BOX gene 10 (SOX10); nuclear transcription factor involved in the development of melanocytes and is expressed in all phases of the melanocyte life cycle, from neural crest stem cells to terminally differentiated melanocytes
77 S100 (Soluble 100% in ammonium sulfate) Neural crest derived tissue Schwann and glial cells, melanocytes Some breast epithelial cells Myoepithelial cells, cartilage, adipose Macrophages, Langerhans cells Apocrine and eccrine glands
78 S100 (Soluble 100% in ammonium sulfate) Neural crest derived tissue Schwann and glial cells, melanocytes ~ 95% of epithelioid melanoma ~ 85% of spindle melanoma
79 HMB45 HMB45 (Human Melanoma Black 45) monoclonal antibody derived from lymph node tissue containing metastatic pigmented melanoma Positive: Melanoma (85-90%) Negative: Some melanomas (desmoplastic, oral mucosal, spindle cell)
80 HMB45 Positive staining lesions PEComa Adrenal: Pheochromocytoma Soft tissue: Clear cell sarcoma of soft tissue [melanoma of soft tissues] Kidney: Angiomyolipoma Lung: Lymphangioleiomyomatosis [LAM]
81 MITF- microphthalmia transcription factor DNA-binding nuclear protein regulator of melanocytic-related genes MITF stains a variety of cells and tumors
82 Beware of MITF Other cells that are MITF + : Histiocytes-[ a real trap ] problematic if staining for occult melanoma cells in sentinel lymph nodes Perivascular epithelioid tumors: Angiomyolipoma Clear cell sarcoma Giant cell tumor Undifferentiated pleomorphic sarcoma Atypical fibroxanthoma
83 Melan A Melan A, a product of the MART-1 gene, is a melanocyte differentiation marker recognized by autologous cytotoxic T lymphocytes.
84 MART-1 positive lesions Sex cord stromal tumors Clear cell sarcoma of soft tissues Angiomyolipoma Lymphangioleiomyomatosis Adrenal cortical adenoma Adrenal cortical adenocarcinoma
85 Sox 10-Sry-related HMG-BOX gene 10 (SOX10) Nuclear transcription factor involved in the development of melanocytes Found in all phases of the melanocyte life cycle, from neural crest stem cells to terminally differentiated melanocytes
86 Sox 10 is expressed in normal tissues and a variety of tumors Breast Salivary Neural Normal myoepithelial cells Basal like/ triple negative carcinomas Normal: acini and both luminal and abluminal cells of intercalated ducts Carcinomas: acinic cell, adenoid cystic, epi-myoepithelial Pleomorphic adenoma Malignant peripheral nerve sheath tumor (useful to exclude synovial sarcoma) Schwannoma & Neurofibroma
87 Melanoma IHC markers Which is the best? Of these available markers, it is advisable to use at least two or more before diagnosing melanoma in an unusual location, such as the sinonasal region S100 HMB45 Melan A (MART 1) Sox 10
88 Melanoma IHC markers Which is the best? S100 HMB45 Melan A (MART 1) Sox 10 S100 and Sox 10 are a good combination
89 IHC markers that can also be positive in melanoma CD99 CD117 Synaptophysin
90 Sinonasal Melanoma Prognosis: Generally poor, 5yr survival <15-20% Local recurrence is common Very rarely the sinonasal region may be a site for metastases from melanoma elsewhere
91 Neuroectodermal differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma
92 Neuroendocrine carcinoma Well differentiated [carcinoid] Moderately differentiated [atypical carcinoid] Poorly differentiated [small cell carcinoma] [large cell neuroendocrine carcinoma]
93 Well differentiated [carcinoid] Moderately differentiated [atypical carcinoid] Carcinoid and atypical carcinoid are so rare in the sinonasal region as not to generally be considered
94 High grade neuroendocrine carcinoma Small cell neuroendocrine carcinoma Closely packed small cells with scant cytoplasm, extensive necrosis, and brisk mitotic activity Large cell neuroendocrine carcinoma Cytoplasm is moderate, nuclei are vesicular with prominent nucleoli, moderate pleomorphism is present
95 Crush artefact Small cell Histologic features Nuclear shapes ranging from angular to round No prominent nucleoli Azzopardi effect [staining of blood vessels by tumor cell nuclear material] High mitotic rate
96 Large cell neuroendocrine carcinoma Larger cells with cytoplasm Nuclei have coarse chromatin with a nucleolus Organoid / trabecular patterns Necrosis High mitotic rate
97 Sinonasal neuroendocrine carcinoma immunohistochemistry Positive: PanKeratin Chromogranin Synaptophysin Neuron specific enolase CD56 TTF -1, very common in high grade neuroendocrine carcinoma of the lung, is not so commonly expressed in sinonasal high grade neuroendocrine tumors
98 Chromogranin and Synaptophysin should always be used together in neuroendocrine carcinoma workup, as one can often be positive and the other negative. Dot-like pankeratin staining in high grade neuroendocrine carcinoma can be very useful to point to the correct diagnosi
99 Beware CD 56 Often ordered in the workup of neuroendocrine tumors (neuroendocrine carcinoma, olfactory neuroblastoma) I try not to order it as a first-line antibody In some cases, CD 56 will be the only antibody that stains a tumor. That might not prove the tumor is neuroendocrine
100 Beware CD 56 CD 56 can also be positive in: Myeloid cells T-cytotoxic cells Myeloma Rhabdomyosarcoma (solid, alveolar) If CD56 is the only antibody positive in a tumor which I believe may be neuroendocrine, I make a comment in the report noting that other tumors may also stain with this antibody
101 Neuroectodermal differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma
102 Pituitary adenoma Nested patterns a useful hint Reticulin stain helpful
103 Hematopoietic differentiation Lymphoma Myeloid sarcoma Sinonasal / Skull Base Round Cell Tumors Neuroectodermal differentiation Ewing s sarcoma/pnet (EWS-PNET) Olfactory neuroblastoma Melanoma Neuroendocrine carcinoma Pituitary adenoma Mesenchymal differentiation Rhabdomyosarcoma Synovial sarcoma Mesenchymal chondrosarcoma Desmoplastic small round cell tumor Small cell osteosarcoma
104 Rhabdomyosarcoma Alveolar Embryonal Pleomorphic Spindle cell
105 Rhabdomyosarcoma Incidence overall: 4-5/1,000,000 Sinonasal incidence: 0.35/ 1,000,000 Most common sinonasal sarcoma, children and adults Age: Embryonal <15 years [childhood, classically] Alveolar years [adult, classically] Gender: M = F, maybe slightly more M in ERMS Site: EMRS-orbit and parameningeal Alveolar-deeper soft tissues in H&N Paranasal sinuses > nasal cavity
106 Embryonal Rhabdomyosarcoma (EMRS) Variable histologies Cellular with myxoid zones Spindle to ovoid cells Rhabdomyoblasts Botryoid (exophytic/polypoid) Mixed EMRS/ARMS
107 Alveolar Rhabdomyosarcoma Small round blue cells separated by fibrous septa Minimal cytoplasm Mitotic figures common Tumor giant cells present
108 Rhabdomyosarcoma IHC Positive Desmin Myogenin MyoD1 Myoglobin Variable Vimentin CD56 Focal CD99 Occasional Pankeratin
109 Rhabdomyosarcoma IHC markers Myoglobin Desmin Muscle specific actin Myogenin MyoD1
110 Rhabdomyosarcoma IHC markers Myogenin & MyoD1 Both more specific than desmin and muscle specific actin Both more sensitive than myoglobin MyoD1: Diffuse cytoplasmic staining and staining of background non-tumor cells can be limiting on a practical basis. Nuclear staining should only be counted but MyoD1 can also be seen to stain nuclei in a number of tumors
111 Rhabdomyosarcoma Embryonal Desmin Myogenin (more variable staining) Myoglobin Muscle specific actin Smooth muscle specific actin Alveolar Desmin Myogenin (100% of cells, strong) Myoglobin Muscle specific actin Smooth muscle specific actin
112 Embryonal Rhabdomyosarcoma (EMRS) IHC: Desmin positive diffusely Myogenin positive, variable MYO-D1 positive, variable Smooth muscle actin- positive, variable Molecular findings: Lost of heterozygosity (LOH) at 11p 15.5 No PAX3 FOXO1 or PAX7 FOXO1 fusions (indicative of ARMS)
113 Alveolar Rhabdomyosarcoma IHC Desmin positive Myogenin positive MYO-D1 positive Molecular findings: PAX3 FOXO1 or PAX7 FOXO1 fusions
114 Myogenin staining also reported in -Synovial sarcoma -Desmoid -Non-neoplastic skeletal muscle (~60% in one study)
115 Rhabdomyosarcoma Other immunohistochemistry that can be positive: CD99 CD20 EMA Cytokeratin Chromogranin Synaptophysin CD56
116 Rhabdomyosarcoma We utilize sarcoma fusion panels in the diagnosis and classification of rhabdomyosarcoma when we have insufficient material for FISH testing or if there are equivocal FISH results, the latter often due to insufficient material.
117 Rhabdomyosarcoma Embryonal (EMRS) and Alveolar Clinical course: Alveolar worse prognosis
118 Desmoplastic small round cell tumor Peak incidence in young adults, described as between 20 and 24 years (range 10-40), There is a striking male predominance of at least 4:1
119 Desmoplastic small round cell tumor Majority present within the abdominal cavity and pelvis. More rarely as primary disease at other anatomic sites, including the head and neck. Can also present with nodal and visceral metastases without evidence of a primary site.
120 Desmoplastic small round cell tumor Histology: uniform small round cells in a fibroblastic/desmoplastic stroma, IHC: Epithelial, neural and muscle markers can be present. WT-1 common However, DSRCT is characterized by a recurrent t(11;22)(p13;q12) translocation, which leads to formation of the EWSR1-WT1 fusion oncogene
121 Desmoplastic small round cell tumor Immunohistochemistry Epithelial, neural and muscle markers can be present. Desmin WT-1 (~75% of cases) EMA Pan Keratin NSE CD57 Can be seen CD99 CD15 MOC-31 Not seen CK 20 CK 5/6
122 Desmoplastic small round cell tumor Outcome: Treatment has been along lines of that for Ewing sarcoma. However, treatment has been seen to work best with de-bulking of as much tumor as possible. In spite of initial significant response, recurrences are frequent and durable response is infrequent.
123 Small cell osteosarcoma Diffuse growth pattern Uniform, small cells Round to spindled Malignant osteoid, can be very focal Can be mixed with cartilage
124 Poor prognosis Small cell osteosarcoma Patients given therapy as for other osteosarcoma subtypes
125 Hematopoietic neoplasms Diffuse large B cell lymphoma Extranodal NK / T cell lymphoma Extramedullary plasmacytoma Myeloid sarcoma
126 Diffuse large B cell lymphoma Most commonly arises in the paranasal sinuses, followed by nasal cavity
127 Diffuse large B cell lymphoma Uniform population of cells Larger than small lymphs Less angioinvasion than in NK/T cell lymphoma
128 Diffuse large B cell lymphoma Uniform population of cells Larger than small lymphs CD45, CD20, CD79a EBV -- negative
129 Diffuse large B cell lymphoma IHC and Molecular markers Positive: CD45, CD20, CD79a Negative: CD 3 Note: cytokeratin can be expressed in DLBCL EBV -- negative Molecular: IgH gene rearrangement
130 NK-Cell Tumors Extra-nodal NK / T cell lymphomas, nasal type Extra-nodal NK / T cell lymphomas, non- nasal type NK cell leukemias
131 Extranodal NK / T cell lymphoma Angiocentric Mix of small to large cells Necrosis Non-lymphoid inflammatory cells
132 Extranodal NK / T cell lymphoma CD2: Positive CD3 cytoplasmic positive CD3 surface negative (fluorescence) CD5: Positive CD56 positive EBV: Positive
133 Extramedullary plasmacytoma Proliferation of monoclonal plasma cells outside of the marrow space and in the absence of multiple myeloma. Clinical: Age is usually 6-7 th decade Male predominance 3:1 Nasal cavity and paranasal sinuses, but multiple locations in the head and neck
134 Extramedullary plasmacytoma In the head and neck, most tumors are solitary May have obstructive symptoms, epistaxis Some patients have paraprotein, and if so, it is usually IgA
135 Extramedullary plasmacytoma CD138 CD38 Kappa and lambda light chains Note: Cytokeratin can be expressed
136 Myeloid sarcoma Defined by WHO as a tumor mass consisting of myeloid blasts, with or without maturation, occurring at extramedullary sites Leukemic infiltration is considered myeloid sarcoma only if it forms a mass that effaces tissue architecture Myeloid sarcoma is diagnostic of acute myeloid leukemia (AML) regardless of bone marrow or peripheral blood involvement
137 Myeloid sarcoma Myeloid sarcoma occurs in 3 settings: As initial presentation of AML Most often with concurrent AML, diagnosed by bone marrow biopsy or peripheral blood Relapsed AML
138 Myeloid sarcoma May represent progression from myelodysplastic syndrome (MDS) or MDS / myeloproliferative disorder (MPD) to a "blastic phase" of leukemia Often [~ 75%] misdiagnosed as large cell lymphoma
139 Myeloid sarcoma Presentation as a round cell tumor Primitive myeloid cells KP1 CD43 CD79a CD3 CD34 CD117 Myeloperoxidase Chloroacetate esterase Lysozyme
140 Epithelial differentiation Adenoid cystic carcinoma Lymphoepithelial carcinoma Sinonasal primary vs extension from nasopharynx Sinonasal basaloid carcinomas Sinonasal undifferentiated carcinoma (SNUC) NUT midline carcinoma SMARCB1 deficient carcinoma HPV-related carcinoma with adenoid cystic carcinoma- like features
141 Some of these tumors are not necessarily round cell in morphology, but their light microscopic appearances are in their combined differential diagnosis Adenoid cystic carcinoma Lymphoepithelial carcinoma Sinonasal primary vs extension from nasopharynx Sinonasal basaloid carcinomas Sinonasal undifferentiated carcinoma (SNUC) NUT midline carcinoma SMARCB1 deficient carcinoma HPV-related carcinoma with adenoid cystic carcinomalike features
142 Some of these tumors are not necessarily round cell in morphology, but their light microscopic appearances are in their combined differential diagnosis However, It is not uncommon to be faced with biopsy material that is less than ideal, i.e. nearly non-existent!
143 Epithelial differentiation Adenoid cystic carcinoma Lymphoepithelial carcinoma Sinonasal primary vs extension from nasopharynx Sinonasal basaloid carcinomas Sinonasal undifferentiated carcinoma (SNUC) NUT midline carcinoma SMARCB1 deficient carcinoma HPV-related carcinoma with adenoid cystic carcinoma- like features
144 Immunohistochemsitry Solid adenoid cystic carcinoma Positive p63 p40 CK 5/6 CK 7 34Beta E12 Negative Synaptophysin Chromogranin p16 EBER S100 Myb
145 Solid adenoid cystic carcinoma Chromosomal rearrangement t(6;9) (q21-24;p13-23) MYB-NFIB ~ %
146 Solid adenoid cystic carcinoma Solid nests of basaloid cells Small biopsies can be difficult to diagnose without cribriform or tubular patterns Minimal tissue may be available Consider NGS testing
147 Salivary gland NGS panel Custom made panel Works well with formalin fixed paraffin embedded tissue as well as fine needle aspirate specimens 14 genes, 13 targets, 100% coverage Can reflex to Ion 318 CHIP V2
148 Salivary gland NGS panel Useful for cytologic specimens Cell samples can be removed from the cytology air-dried smears that have been stained with metachromatic stain.
149 Epithelial differentiation Adenoid cystic carcinoma Lymphoepithelial carcinoma Sinonasal primary vs extension from nasopharynx Sinonasal basaloid carcinomas Sinonasal undifferentiated carcinoma (SNUC) NUT midline carcinoma SMARCB1 deficient carcinoma HPV-related carcinoma with adenoid cystic carcinoma- like features
150 Lymphoepithelial carcinoma Non-keratinizing squamous carcinoma as a primary tumor in the sinonasal region is rare and usually when found is direct extension from nasopharynx. Tumor cells grow in a syncytial growth pattern, with indistinct borders, and have markedly vesicular nuclei with prominent nucleoli.
151 Lymphoepithelial carcinoma Sinonasal lymphoepithelial carcinoma is rare Generally men, 4 th -7 th decades Most cases are in Asians Vast majority have EBV For a lymphoepithelial carcinoma to be considered primary to the sinonasal region, spread from a nearby nasopharyngeal carcinoma must be excluded.
152 Lymphoepithelial-like carcinoma Markers Positive EBV (EBER, at least in endemic regions) p63 p40 Negative S100 Synaptophysin Chromogranin HPV (p16) CK 5/6
153 Sinonasal basaloid carcinomas Group of tumors with similar histologies but with evolving separation based on new molecular studies Sinonasal undifferentiated carcinoma (SNUC) NUT midline carcinoma SMARCB1 deficient carcinoma HPV-related carcinoma with adenoid cystic carcinoma- like features
154 Sinonasal Undifferentiated Carcinoma (SNUC) Incidence: Uncommon; 3-5% of sinonasal carcinomas Age: 3-8 th decade; median 5-6 th decade Gender: More common in men Site: Paranasal sinuses Nasal cavity Invades skull base, brain, orbital apex Molecular: No specific findings
155 Sinonasal Undifferentiated Carcinoma (SNUC) Blue cell tumor, with a variety of cell sizes, not all small Minimal nuclear pleomorphism Prominent nucleolus, common Necrosis Vascular invasion
156 Sinonasal Undifferentiated Carcinoma (SNUC) Sheets, nests or trabeculae of cells No evidence of squamous or glandular differentiation No surface precursor; sometimes adjacent carcinoma in situ is seen
157 Positive in SNUC Pankeratin, CK7, CAM 5.2 p63 +/ - EMA NSE p16: variable results in literature. Some +, some Variable expression of HPV
158 Negative IHC in SNUC P40 / usually negative S100 (focally +) CEA Chromogranin & Synaptophysin (focally +) EBV: Usually negative, but + reported in some patients
159 Outcome: SNUC Rapid clinical course with presentation with advanced stage Multimodal therapy with surgery, radiation and chemotherapy 5 year survival = ~ 35%
160 NUT Midline Carcinoma Incidence: Rare Age: Usually in 25-30, ranges infancy to 8 th decade Site: Most cases in paranasal sinus and nasal cavity other sites include nasopharynx, laryngeal structures, orbit, salivary glands Usually midline
161 NUT Midline Carcinoma Rapidly growing mass with nasal obstruction, epistaxis and frequently proptosis Invades local structures extensively Often local lymph node and / or distant metastases
162 NUT Midline Carcinoma Sheets of monotonous undifferentiated round cells, foci of mature keratinized squamous cells occasionally seen Always necrosis
163 NUT Midline Carcinoma Rearrangements in nuclear protein in testis (NUT) gene (NUTM1) Most cases: NUTM1 is fused with BRD4 t(15;19) Can also fuse with BRD3, WHSC1L1 Some cases the fusion partner is not known
164 NUT Midline Carcinoma NUT positive by immunohistochemistry NUT antibody p40 p63 CK7 Can also use FISH, PCR or NGS
165 Prognosis is poor NUT Midline Carcinoma Multimodal therapy is attempted
166 SMARCB1 (INI-1) -deficient sinonasal basaloid carcinoma Recently a newly described entity of an undifferentiated sinonasal carcinoma characterized by loss of the tumor suppressor SMARCB1 (INI1) encoded by the SMARCB1 gene on chromosome 22q.
167 SMARCB1 (INI-1) -deficient sinonasal basaloid carcinoma SMARCB1 is a member of the SWItch/Sucrose Non-Fermentable (SWI/SNF) complex Group of >20 functionally closely related proteins involved in the regulation of gene expression, cell proliferation and differentiation.
168 SWI/SNF mutations in cancers of different histological subtypes occurring in different organs SWI/SNF-deficient neoplasms are generally unified by high frequency of undifferentiated anaplastic and/or rhabdoid cell phenotype
169 SMARCB1 (INI-1) -deficient sinonasal basaloid carcinoma Nasal cavity and sinuses Most tumors are basaloid but other SMARCB1- deficient cases have been found with rhabdoid, squamoid, oncocytic appearances
170 SMARCB1 (INI-1) -deficient sinonasal basaloid carcinoma Basaloid cells high N:C ratios Desmoplastic stroma Scattered plasmacytoid or rhabdoid-like cells Plasmacytoid or rhabdoid can be predominant in the tumor Occasional sarcomatoid patterns Can grow in a Pagetoid pattern in the overlying normal epithelium
171 SMARCB1 (INI-1) -deficient sinonasal basaloid carcinoma: Immunohistochemical findings p63: ~50% CK7: ~50% CK5: ~60% Synaptophysin, CD56: < 25%
172 SMARCB1 (INI-1) -deficient sinonasal basaloid carcinoma Few cases described but some patients have had responses to multimodal therapies
173 HPV related carcinoma with adenoid cystic-like carcinoma features Tumor appears restricted to the sinonasal tract and associated with HPV, particularly type 33 Nested growth pattern Basaloid component showing myoepithelial differentiation Microcystic spaces Squamous differentiation, when present, was restricted to the surface epithelium. Not associated with the MYB gene
174 Case 2 55 year old female had been previously diagnosed with a FIGO grade 2, uterine endometrioid adenocarcinoma, T1a (< 50% invasive into the myometrium). Three years later, she developed a thyroid mass and was subsequently diagnosed with follicular carcinoma of the thyroid. The tumor showed minimal invasion into the capsule, but with focal vascular invasion.
175 Case 2 She was treated with total thyroidectomy. Five years postthyroidectomy, she presented with voice alterations. On exam a large tumor in the neck was present. It was subsequently found to invade the larynx. A laryngectomy was performed. The slides presented are from the neck soft tissue and laryngectomy specimen.
176 Case 2 Thyroid columnar cell carcinoma
177 Objectives Recognize an aggressive variant of papillary carcinoma that lacks typical morphologic features, particularly nuclear, of papillary carcinoma Briefly review common primary thyroid carcinomas Review some of the primary thyroid tumors with uncommon morphology Review some of the most common tumors metastatic to the thyroid Discuss some observations about the use of NGS in the diagnosis of thyroid carcinoma
178 Main objective for this case Review thyroid tumors that don t remind you of typical thyroid tumors
179 Uncommon thyroid tumors Columnar cell carcinoma Clear cell carcinoma Cribriform-morular carcinoma Intrathyroid thymic carcinoma (formerly termed carcinoma showing thymus-like differentiation (CASTLE) Spindle Epithelial Tumor with Thymus Like Elements (SETTLE) Tumors metastatic to the thyroid
180 Common thyroid carcinomas Papillary carcinoma Follicular carcinoma Medullary thyroid carcinoma Anaplastic thyroid carcinoma
181 Columnar cell carcinoma Described in 1986 by Evans, as an aggressive form of thyroid carcinoma Recognized as an unusual variant of papillary thyroid carcinoma by many
182 Columnar cell carcinoma Variant of papillary carcinoma? Paradoxical findings for a thyroid papillary carcinoma
183 Histologic features not present in columnar cell carcinoma, but features that are seen in papillary thyroid carcinoma No intranuclear inclusions No ground glass nuclei No nuclear grooves
184 Columnar cell carcinoma Molecular pathology features Why is columnar cell carcinoma considered a variant of papillary carcinoma? B-raf (V600E) mutations in some patients
185 Columnar cell carcinoma Clinical features -Female predominant (8-10:1, F:M) -Age range Size 3-5 cm average (1-10 reported)
186 Columnar cell carcinoma -columnar cells -pseudostratified -sub and supranuclear vacuoles appearance similar to early secretory endometrium
187 Columnar cell carcinoma Histologic features Nuclei are elongate Does not have cleared nuclei or intranuclear inclusions -additional patterns: solid trabecular papillary follicular
188 Columnar cell carcinoma Immunohistochemistry TTF-1 (positive) Thyroglobulin (variable positive) CDX-2 can be positive (antibody generally used to identify cells of gastrointestinal origin)
189 CDX-2 positive tumors Gastrointestinal tumors / lesions : Lung: Esophageal adenocarcinomas and intestinal metaplasia in Barrett s esophagus Colon Polyps Adenocarcinomas Gastric carcinoma Gastrointestinal neuroendocrine carcinomas Small intestinal carcinomas Mucinous adenocarcinomas Gynecologic tumors Mucinous adenocarcinoma Cervical adenocarcinoma Endometrioid adenocarcinoma Testicular teratomas
190 Columnar cell carcinoma Differential diagnosis Follicular carcinoma Hyalinizing trabecular tumor Tall cell variant of papillary carcinoma Poorly differentiated carcinoma (Insular carcinoma) Metastatic carcinoma to the thyroid
191 Follicular carcinoma Vascular invasion in the capsule Tumor capsule invasion If cytoplasm exists around the nucleus, it is evenly distributed, not eccentrically placed or elongated.
192 Hyalinizing Trabecular Tumor Numerous intranuclear inclusions Hyalinizing stroma Trabecular cell arrangement Cells are palisaded
193 Poorly differentiated carcinoma Trabecular pattern No subnuclear or supranuclear clearing
194 Papillary carcinoma, tall cell variant No sub/supranuclear clearing Has all the nuclear features of usual papillary carcinoma Nuclear grooves Nuclear overlapping Nuclear clearing Often has oncocytic cytoplasm
195 Uncommon primary thyroid tumors Columnar cell carcinoma Clear cell carcinoma Carcinoma showing thymus-like differentiation (CASTLE) Spindle Epithelial Tumor with Thymus Like Elements (SETTLE)
196 Clear cell carcinoma of thyroid Classified as a variant of follicular carcinoma requires capsular &/or capsular vessel invasion to meet diagnostic criteria Cleared cytoplasm Cytoplasm contains variable elements of glycogen, lipid, thryoglobulin No nuclear features of papillary carcinoma
197 Clear cell carcinoma of thyroid Differential always includes clear cell tumors metastatic to the thyroid: Renal cell carcinoma, conventional clear cell type Parathyroid carcinoma
198 Clear cell carcinoma of thyroid Immunohistochemistry is positive for PAX8 TTF-1 The combination of these two antibodies is required to exclude metastatic clear cell renal cell carcinoma which is also PAX8 positive
199 Uncommon primary thyroid tumors Columnar cell carcinoma Clear cell carcinoma Intrathyroid thymic carcinoma [Carcinoma showing thymus-like differentiation (CASTLE)] Spindle Epithelial Tumor with Thymus Like Elements (SETTLE)
200 Intrathyroid thymic carcinoma Carcinoma showing thymus-like differentiation (CASTLE)
201 Intrathyroid thymic carcinoma Uncommon tumor with essentially equal female:male ratio Reported to be more common in Asian patients Histologic features are that of thymic carcinoma squamous carcinoma appearance with lymphoid associated component
202 Intrathyroid thymic carcinoma Immunohistochemistry CD 5 Bcl 2 p40
203 Uncommon primary thyroid tumors Columnar cell carcinoma Clear cell carcinoma Carcinoma showing thymus-like differentiation (CASTLE) Spindle Epithelial Tumor with Thymus Like Elements (SETTLE)
204 Spindle Epithelial Tumor with Thymus Like Elements (SETTLE) Uncommon tumor, usually affecting children and young adults (mean age ~ 20) Slow growing with overall survival at ~85% Known for very late metastases [25% early, 40% at 10 years]
205 Spindle Epithelial Tumor with Thymus Like Elements (SETTLE) Biphasic with glandular structures merging with spindled areas Usually biphasic but monophasic examples can be seen [differential diagnosis of synovial sarcoma] Mitoses generally rare Spindle cells with fine nuclear chromatin Glandular elements have cuboidal to columnar epithelial cells forming tubules, papillae or glomeruloid structures.
206 Metastatic tumors to the thyroid Most common: Lung Breast Melanoma Renal cell carcinoma
207 Columnar cell carcinoma: Therapy Total thyroidectomy Lymphadenectomy (ipse-lateral and central compartment neck dissection) Survey for distant metastasis. Postoperative radioactive iodine May be susceptible to treatment targeted against BRAF mutation if it exists External beam irradiation may be used in cases of incomplete resection.
208 Columnar cell carcinoma Outcome For histologically localized/circumscribed tumors: Good outcome (usually in younger females) For histologically aggressive tumors (usually in older males) recurrence and local invasion common
209 Case 3 52 year old female presented to her physician with a neck mass and a sore throat. Physical exam revealed only a neck mass. CT imaging revealed a neck mass and a lesion at the base of the tongue. Biopsy of the lesion at the base of the tongue was performed.
210 Case 3 Polymorphous Adenocarcinoma Cribriform Adenocarcinoma of Salivary Gland (CASG)
211 Objectives Review Polymorphous Adenocarcinoma 1) Polymorphous low grade adenocarcinoma (PLGA) 2) CASG (Cribriform adenocarcinoma of salivary gland) Identify criteria for the diagnosis Consider the differential diagnosis of CASG in neck FNA s
212 Polymorphous adenocarcinoma Polymorphous low grade adenocarcinoma Cribriform adenocarcinoma of salivary gland
213 Cribriform Adenocarcinoma of Salivary Gland Most recent WHO classification suggests PLGA and CASG are best classified as polymorphous adenocarcinoma and are related. Cribriform adenocarcinoma of salivary gland is considered a variant of polymorphous adenocarcinoma.
214 Cribriform Adenocarcinoma of Salivary Gland Described in 1999 by Michal et al as cribriform adenocarcinoma of the tongue Probably earlier reports of papillary adenocarcinoma of minor salivary gland or tubular carcinoma of the tongue represented CASG
215 Cribriform Adenocarcinoma of Salivary Gland Relatively few cases have still been reported True incidence is unknown as it is likely under-recognized Neoplasm often presents with synchronous neck lymph node metastases
216 Cribriform Adenocarcinoma of Salivary Gland Sites of occurrence Base of tongue Palate Retromolar trigone Parotid Oral cavity (NOS) Sinonasal
217 CASG Histologic findings, low power Vague, lobular arrangement Unencapsulated with infiltrative margins Clefting of epithelial cell nests from dense stroma Papillary patterns Hyalinized stroma Myxoid to mucoid matrix
218 CASG Histologic findings, low power Cribriform and solid growth patterns, sometimes demonstrating peripheral palisading peripheral clefting glomeruloid appearance.
219 CASG Cytologic findings Cytoplasmic variability Nuclear overlapping Nuclear grooves Nuclear membrane irregularity Optically clear, ground glass nuclei
220 Cribriform Adenocarcinoma of Salivary Gland Vague, lobular arrangement Unencapsulated with infiltrative margins Clefting between cells and stroma Papillary structures Optically clear, ground glass nuclei
221 Polymorphous low grade adenocarcinoma Whirled pattern of cells Small cribriform structures Myxoid to hyaline stroma
222 CASG- Differential diagnosis What else? Papillary thyroid carcinoma
223 Cytologic findings: CASG vs PTC CASG Nuclear overlap minimal Nuclei rounded Grooves not prominent No bubble gum colloid Stroma prominent PTC Nuclear overlap striking Nuclei elongate Grooves very prominent Bubble gum colloid Giant cells
224 Cribriform Adenocarcinoma of Salivary Gland Immunohistochemistry Positive: Negative Pan keratin AE 1/3 CK7 S-100 p63 CK5/6 Calponin Smooth muscle actin TTF Thyroglobulin
225 CASG often presents with synchronous neck lymph node metastases Patients presenting with neck masses are often assessed with fine needle aspiration of the neck lymph node FNA of these metastases can appear nearly identical to that of papillary thyroid carcinoma metastases
226 Cribriform Adenocarcinoma of Salivary Gland: Therapy Primary surgical therapy with negative margins is the goal Neck dissection, at least selective for clinically positive neck, is reasonable
227 Case 4 56 year old male presented with nasal swelling and was referred to an otolaryngologist. The otolaryngologist discovered a polypoid mass in posterior nasal septum and attempted to excise all of the tumor.
228 Case 4 Respiratory adenomatoid hamartoma (REAH)
229 Objectives Case 4 Describe the clinical findings of Respiratory Adenomatoid Hamartoma (REAH) Recognize the key histologic findings in REAH Differentiate REAH from similar lesions (Co- REAH; Seromucinous hamartoma) Separate histologically the nasal lesions in the differential diagnosis of REAH
230 REAH Clinical Findings Polypoid mass in the posterior nasal septum Predominantly males Inflammatory nasal polyps frequently adjacent to or preceding REAH
231 REAH Histology Benign overgrowth of submucosal ciliated respiratory glands Glands can be back to back Glandular connection to the polyp surface Pseudostratified columnar epithelium, some with goblet cells Periglandular hyalinization
232 Lesions that are similar to REAH Seromucinous hamartoma Chondro-Osseous Respiratory Epithelial Adenomatoid Hamartoma (CO-REAH)
233 Seromucinous hamartoma Clinical Posterior nasal septum and nasopharynx Polypoid mass Slight male predominance
234 Seromucinous hamartoma Pathology Small tubular glands arranged in lobular as well as in a haphazard pattern Serous cells that show eosinophilic cytoplasm Relatively few mucinous cells, despite the name May have REAH-like areas -intermixed respiratory glands -periglandular hyperplasia
235 Seromucinous hamartoma Posterior nasal septum and nasopharynx Polypoid mass Slight male predominance Small tubular glands arranged in lobular as well as in a haphazard pattern Serous cells that show eosinophilic cytoplasm
236 REAH vs Seromucinous Hamartoma There is some morphologic overlap between respiratory epithelial adenomatoid hamartoma and seroumucinous hamartoma Some authorities suggest they are related
237 Chondro-Osseous Respiratory Epithelial Adenomatoid Hamartoma (CO-REAH) All the features of REAH with Chondroid and Osseous metaplasia
238 Differentiatial diagnosis of nasal polypoid lesions Inflammatory nasal polyps Inverted Schneiderian papilloma Inverted Oncocytic papilloma Adenocarcinomas of the nose and paranasal sinuses Intestinal Non-intestinal types Metastatic (prostate carcinoma most common)
239 Differentiatial diagnosis of nasal polypoid lesions Inflammatory nasal polyps Inverted Schneiderian Papilloma Oncocytic/Columnar cell Papilloma Adenocarcinomas of the nose and paranasal sinuses Intestinal type Non-intestinal types Metastatic (prostate carcinoma most common)
240 Inverted Schneiderian Papilloma Nests of transitional type epithelium Epithelium connects to the surface Multiple layers of cells Neutrophils present
241 Schneiderian papilloma, oncocytic type Synonyms: Cylindric cell papilloma Definition: A histologically distinct Schneiderian papilloma that often has and exophytic and concurrent endophytic growth Unlike inverted or exophytic papilloma, oncocytic Schneiderian papillomas have no association with HPV
242 Schneiderian papilloma, oncocytic type Clinical findings: Near 100% on the lateral nasal wall, maxillary sinus or ethmoid sinus Epistaxis and nasal obstruction Polypoid growth
Small (and large) Blue Cell Tumors of the Skull Base
 Small (and large) Blue Cell Tumors of the Skull Base Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for
Small (and large) Blue Cell Tumors of the Skull Base Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for
Case 2. Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset
 Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Case 2 Dr. Sathima Natarajan M.D. Kaiser Permanente Medical Center Sunset History 24 year old male presented with a 3 day history of right flank pain, sharp in nature Denies fever, chills, hematuria or
Salivary Glands 3/7/2017
 Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Salivary Glands 3/7/2017 Goals and objectives Focus on the entities unique to H&N Common board type facts Information for your future practice Salivary Glands Salivary Glands Major gland. Paratid. Submandibular.
Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement
 Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center
Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology. Songlin Zhang, MD, PhD LSUHSC-Shreveport
 From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
From Morphology to Molecular Pathology: A Practical Approach for Cytopathologists Part 1-Cytomorphology Songlin Zhang, MD, PhD LSUHSC-Shreveport I have no Conflict of Interest. FNA on Lymphoproliferative
Case year old female presented with asymmetric enlargement of the left lobe of the thyroid
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 Diagnosis 2/21/2011 TGB
 Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Case 4 22 year old female presented with asymmetric enlargement of the left lobe of the thyroid gland. No information available relative to a prior fine needle aspiration biopsy. A left lobectomy was performed.
Objectives. Salivary Gland FNA: The Milan System. Role of Salivary Gland FNA 04/26/2018
 Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Salivary Gland FNA: The Milan System Dr. Jennifer Brainard Section Head Cytopathology Cleveland Clinic Objectives Introduce the Milan System for reporting salivary gland cytopathology Define cytologic
Lung Tumor Cases: Common Problems and Helpful Hints
 Lung Tumor Cases: Common Problems and Helpful Hints Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona Society of Pathologists
Lung Tumor Cases: Common Problems and Helpful Hints Brandon T. Larsen, MD, PhD Senior Associate Consultant Department of Laboratory Medicine and Pathology Mayo Clinic Arizona Arizona Society of Pathologists
Financial disclosures
 Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchc Geisel School of
Cutaneous Mesenchymal Neoplasms with EWSR1 Rearrangement By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchc Geisel School of
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells. Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital
 Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Differential diagnosis of hematolymphoid tumors composed of medium-sized cells Brian Skinnider B.C. Cancer Agency, Vancouver General Hospital Lymphoma classification Lymphoma diagnosis starts with morphologic
Presentation material is for education purposes only. All rights reserved URMC Radiology Page 1 of 98
 Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
Presentation material is for education purposes only. All rights reserved. 2011 URMC Radiology Page 1 of 98 Radiology / Pathology Conference February 2011 Brooke Koltz, Cytopathology Resident Presentation
1/10/2018. Soft Tissue Tumors Showing Melanocytic Differentiation. Overview. Desmoplastic/ Spindle Cell Melanoma
 2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
2016 MFMER slide-1 2016 MFMER slide-2 2016 MFMER slide-3 Soft Tissue Tumors Showing Melanocytic Differentiation Andrew L. Folpe, M.D. Professor of Laboratory Medicine and Pathology Mayo Clinic, Rochester,
Lesions Mimicking Adenoid Cystic Carcinoma. Diagnostic Problems in Salivary Gland Pathology An Update 5/29/2009
 Diagnostic Problems in Salivary Gland Pathology An Update Lesions Mimicking Adenoid Cystic Carcinoma Stacey E. Mills, M.D. W.S. Royster Professor of Pathology Director of Surgical and Cytopathology University
Diagnostic Problems in Salivary Gland Pathology An Update Lesions Mimicking Adenoid Cystic Carcinoma Stacey E. Mills, M.D. W.S. Royster Professor of Pathology Director of Surgical and Cytopathology University
Nasal Cavity and Paranasal Sinuses
 Chapter 2 Nasal Cavity and Paranasal Sinuses Introduction Included in this chapter are nasal cavities, frontal sinus, ethmoid complex, sphenoid sinus, and maxillary sinuses. These cavities and sinuses
Chapter 2 Nasal Cavity and Paranasal Sinuses Introduction Included in this chapter are nasal cavities, frontal sinus, ethmoid complex, sphenoid sinus, and maxillary sinuses. These cavities and sinuses
Mody. AIS vs. Invasive Adenocarcinoma of the Cervix
 Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
Common Problems in Gynecologic Pathology Michael T. Deavers, M.D. Houston Methodist Hospital, Houston, Texas Common Problems in Gynecologic Pathology Adenocarcinoma in-situ (AIS) of the Cervix vs. Invasive
Problem 1: Differential of Neuroendocrine Carcinoma 3/23/2017. Disclosure of Relevant Financial Relationships
 Differential of Neuroendocrine Carcinoma Alain C. Borczuk,MD Weill Cornell Medicine Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control
Differential of Neuroendocrine Carcinoma Alain C. Borczuk,MD Weill Cornell Medicine Disclosure of Relevant Financial Relationships USCAP requires that all faculty in a position to influence or control
Differential Diagnosis of Oral Masses. Palatal Lesions
 Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
Differential Diagnosis of Oral Masses Palatal Lesions Palatal Masses Periapical Abscess Torus Palatinus Mucocele Lymphoid Hyperplasia Adenomatous Hyperplasia Benign Salivary Neoplasms Malignant Salivary
Special slide seminar
 Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Special slide seminar Tomáš Rozkoš The Fingerland Department of Pathology Charles University Medical Faculty and Faculty Hospital in Hradec Králové Czech Republic Case history, 33 years old resistance
Nutn but a Small Biopsy How to approach small biopsy samples of the sinonasal tract
 California Society of Pathology Saturday Slide Seminar Nutn but a Small Biopsy How to approach small biopsy samples of the sinonasal tract Lester D. R. Thompson www.lester-thompson.com Learning Objectives
California Society of Pathology Saturday Slide Seminar Nutn but a Small Biopsy How to approach small biopsy samples of the sinonasal tract Lester D. R. Thompson www.lester-thompson.com Learning Objectives
Financial disclosures
 Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
Mesenchymal Neoplasms with Melanocytic Differentiation By Konstantinos Linos MD, FCAP, FASDP Bone, Soft Tissue and Dermatopathology Assistant Professor of Pathology Dartmouth-Hitchcock Medical Center Geisel
Enterprise Interest Nothing to declare
 Enterprise Interest Nothing to declare Diagnoses one would not like to miss in soft tissue pathology early in your career Marta Sbaraglia, MD Department of Pathology Hospital of Treviso University of Padua
Enterprise Interest Nothing to declare Diagnoses one would not like to miss in soft tissue pathology early in your career Marta Sbaraglia, MD Department of Pathology Hospital of Treviso University of Padua
5/22/2017. An Aggressive Nasopharyngeal Tumor. Case History
 An Aggressive Nasopharyngeal Tumor Head & Neck/Endocrine Evening Specialty Conference Martin Bullock, MD, FRCPC Dalhousie University, Halifax, Nova Scotia Case History 52-year-old male, 6 month history
An Aggressive Nasopharyngeal Tumor Head & Neck/Endocrine Evening Specialty Conference Martin Bullock, MD, FRCPC Dalhousie University, Halifax, Nova Scotia Case History 52-year-old male, 6 month history
Oncocytic-Appearing Salivary Gland Tumors. Oncocytic, Cystic, Mucinous, and High Grade Salivary Gland Tumors SALIVARY GLAND FNA: PART II
 William C. Faquin, MD, PhD Professor of Pathology Harvard Medical School Director of Head and Neck Pathology Massachusetts Eye and Ear Massachusetts General Hospital SALIVARY GLAND FNA: PART II Oncocytic,
William C. Faquin, MD, PhD Professor of Pathology Harvard Medical School Director of Head and Neck Pathology Massachusetts Eye and Ear Massachusetts General Hospital SALIVARY GLAND FNA: PART II Oncocytic,
Salivary Gland Cytology
 Salivary Gland Cytology Diagnostic challenges and potential pitfalls Tarik M. Elsheikh, MD Professor and Medical Director Anatomic Pathology Cleveland Clinic FNA Salivary Gland Lesions Indications Distinguish
Salivary Gland Cytology Diagnostic challenges and potential pitfalls Tarik M. Elsheikh, MD Professor and Medical Director Anatomic Pathology Cleveland Clinic FNA Salivary Gland Lesions Indications Distinguish
04/13/2017. Sinonasal Pathology. Sinonasal Tract Pathology Outline. 24 th Annual Seminar in Pathology Pittsburgh, PA April 27, 2017
 Sinonasal Pathology 24 th Annual Seminar in Pathology Pittsburgh, PA April 27, 2017 Bruce M. Wenig, MD Moffitt Cancer Center Tampa, FL Sinonasal Tract Pathology Outline Sinonasal (Schneiderian) papillomas
Sinonasal Pathology 24 th Annual Seminar in Pathology Pittsburgh, PA April 27, 2017 Bruce M. Wenig, MD Moffitt Cancer Center Tampa, FL Sinonasal Tract Pathology Outline Sinonasal (Schneiderian) papillomas
Tumores de células pequeñas, redondas y azules: diagnóstico diferencial cuando el tiempo apremia
 Tumores de células pequeñas, redondas y azules: diagnóstico diferencial cuando el tiempo apremia Sílvia Bagué Servei de Patologia Hospital de Sant Pau Barcelona Soft tissue sarcomas Heterogeneous group
Tumores de células pequeñas, redondas y azules: diagnóstico diferencial cuando el tiempo apremia Sílvia Bagué Servei de Patologia Hospital de Sant Pau Barcelona Soft tissue sarcomas Heterogeneous group
Financial disclosures
 An update on immunohistochemical markers in mesenchymal neoplasms By Konstantinos Linos MD, FCAP, FASDP Assistant Professor of Pathology Geisel School of Medicine at Dartmouth Dartmouth-Hitchcock Medical
An update on immunohistochemical markers in mesenchymal neoplasms By Konstantinos Linos MD, FCAP, FASDP Assistant Professor of Pathology Geisel School of Medicine at Dartmouth Dartmouth-Hitchcock Medical
Klinisch belang van chromosomale translocatie detectie in sarcomen
 Translocations in sarcomas Klinisch belang van chromosomale translocatie detectie in sarcomen Judith V.M.G. Bovée, M.D., Ph.D. Department of Pathology Leiden University Medical Center RNA binding DNA binding
Translocations in sarcomas Klinisch belang van chromosomale translocatie detectie in sarcomen Judith V.M.G. Bovée, M.D., Ph.D. Department of Pathology Leiden University Medical Center RNA binding DNA binding
FINALIZED SEER SINQ QUESTIONS
 0076 Source 1: WHO Class CNS Tumors pgs: 33 MP/H Rules/Histology--Brain and CNS: What is the histology code for a tumor originating in the cerebellum and extending into the fourth ventricle described as
0076 Source 1: WHO Class CNS Tumors pgs: 33 MP/H Rules/Histology--Brain and CNS: What is the histology code for a tumor originating in the cerebellum and extending into the fourth ventricle described as
04/09/2018. Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances
 Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory
Salivary Gland Pathology in the Molecular Era Old Friends, Old Foes, & New Acquaintances Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory
PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies CYTOLOGIC DIAGNOSIS:
 1 PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies GCDFP-15 S-100 CYTOLOGIC DIAGNOSIS: Consistent with mammary analogue secretory carcinoma.
1 PRELIMINARY CYTOLOGIC DIAGNOSIS: Suspicious for Acinic Cell Carcinoma. Cell Block: Immunohistochemical Studies GCDFP-15 S-100 CYTOLOGIC DIAGNOSIS: Consistent with mammary analogue secretory carcinoma.
Immunohistochemistry in Bone and Soft Tissue Tumors. Sahar Rassi Zankoul, MD
 Immunohistochemistry in Bone and Soft Tissue Tumors Sahar Rassi Zankoul, MD Introduction Bone tumors represent a wide variety of tumors of various origins and malignant potentials. These different tumor
Immunohistochemistry in Bone and Soft Tissue Tumors Sahar Rassi Zankoul, MD Introduction Bone tumors represent a wide variety of tumors of various origins and malignant potentials. These different tumor
Scotland and Northern Ireland EQA Scheme. Circulation 46
 Scotland and Northern Ireland EQA Scheme Circulation 46 Special Educational Cases E1 and E2 Presented by Dr K Robertson Case E1 Female 42 year old with heavy menstrual and intermenstrual bleeding. IUS
Scotland and Northern Ireland EQA Scheme Circulation 46 Special Educational Cases E1 and E2 Presented by Dr K Robertson Case E1 Female 42 year old with heavy menstrual and intermenstrual bleeding. IUS
THYMIC CARCINOMAS AN UPDATE
 THYMIC CARCINOMAS AN UPDATE Mark R. Wick, M.D. University of Virginia Medical Center Charlottesville, VA CARCINOMA OF THE THYMUS General Clinical Features No apparent gender predilection Age range of 35-75
THYMIC CARCINOMAS AN UPDATE Mark R. Wick, M.D. University of Virginia Medical Center Charlottesville, VA CARCINOMA OF THE THYMUS General Clinical Features No apparent gender predilection Age range of 35-75
4/17/2015. Case 1. A 37 year old man with a 2.2 cm solitary left thyroid mass.
 Case 1 A 37 year old man with a 2.2 cm solitary left thyroid mass. Case 1 Case 1 1 Case 1: Diagnosis? A. Benign B. Atypia of undetermined significance/follicular lesion of undetermined significance C.
Case 1 A 37 year old man with a 2.2 cm solitary left thyroid mass. Case 1 Case 1 1 Case 1: Diagnosis? A. Benign B. Atypia of undetermined significance/follicular lesion of undetermined significance C.
57th Annual HSCP Spring Symposium 4/16/2016
 An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
An Unusual Malignant Spindle Cell Lesion to Involve the Breast Erinn Downs-Kelly, D.O. Associate Professor of Pathology University of Utah & ARUP Laboratories No disclosures Case 39 y/o female with no
Update in Salivary Gland Pathology. Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016
 Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
What is New in the 2015 WHO Lung Cancer Classification? Zhaolin Xu, MD, FRCPC, FCAP
 What is New in the 2015 WHO Lung Cancer Classification? Zhaolin Xu, MD, FRCPC, FCAP Professor, Dept of Pathology, Dalhousie University, Canada Pulmonary Pathologist and Cytopathologist, QEII HSC Senior
What is New in the 2015 WHO Lung Cancer Classification? Zhaolin Xu, MD, FRCPC, FCAP Professor, Dept of Pathology, Dalhousie University, Canada Pulmonary Pathologist and Cytopathologist, QEII HSC Senior
Charles Halsey, DVM, PhD, DACVP Pfizer, Inc. IHC Resources
 Charles Halsey, DVM, PhD, DACVP Pfizer, Inc. IHC Resources 1 IHC Identification Targets Specimens Controls 2 Tissue controls Trouble Spots 3 The Key to Description IHC Description 4 Intermediate Filaments
Charles Halsey, DVM, PhD, DACVP Pfizer, Inc. IHC Resources 1 IHC Identification Targets Specimens Controls 2 Tissue controls Trouble Spots 3 The Key to Description IHC Description 4 Intermediate Filaments
Case Presentation. Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD. Department of Pathology Jordan University Hospital Amman, Jordan
 Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Case Presentation Maha Akkawi, MD, Fatima Obeidat, MD, Tariq Aladily, MD Department of Pathology Jordan University Hospital Amman, Jordan The 25th Annual Congress of the ADIAP The 8/11/2013 1 5th International
Note: The cause of testicular neoplasms remains unknown
 - In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
- In the 15- to 34-year-old age group, they are the most common tumors of men. - Tumors of the testis are a heterogeneous group of neoplasms that include: I. Germ cell tumors : 95%; all are malignant.
Review of the AP Part II Practical Examination. Dr David Clift Co Chief Examiner
 Review of the AP Part II Practical Examination Dr David Clift Co Chief Examiner General Remarks The part II practical examination involved 15 cases which were presented with sufficient clinical data to
Review of the AP Part II Practical Examination Dr David Clift Co Chief Examiner General Remarks The part II practical examination involved 15 cases which were presented with sufficient clinical data to
Pitfalls in thyroid tumor pathology. Prof.Valdi Pešutić-Pisac MD, PhD
 Pitfalls in thyroid tumor pathology Prof.Valdi Pešutić-Pisac MD, PhD Too many or... Tumour herniation through a torn capsule simulating capsular invasion fibrous capsule with a sharp discontinuity, suggestive
Pitfalls in thyroid tumor pathology Prof.Valdi Pešutić-Pisac MD, PhD Too many or... Tumour herniation through a torn capsule simulating capsular invasion fibrous capsule with a sharp discontinuity, suggestive
Effective January 1, 2018 ICD O 3 codes, behaviors and terms are site specific
 Effective January 1, 2018 codes, behaviors and terms are site specific Status /N 8010/3 Urachal carcinoma (C65.9, C66.9, C67. _, C68._) 8013/3 Combined large cell neuroendocrine carcinoma (C34. _, C37.9)
Effective January 1, 2018 codes, behaviors and terms are site specific Status /N 8010/3 Urachal carcinoma (C65.9, C66.9, C67. _, C68._) 8013/3 Combined large cell neuroendocrine carcinoma (C34. _, C37.9)
2018 ICD-O-3 Updates in Table Format with Annotation for Reference
 Status Histology Description (this may be preferred term or a synonym) Report Comments New term 8010 3 Urachal carcinoma (C65.9, C66.9, C67._, C68._) New term 8013 3 Combined large cell neuroendocrine
Status Histology Description (this may be preferred term or a synonym) Report Comments New term 8010 3 Urachal carcinoma (C65.9, C66.9, C67._, C68._) New term 8013 3 Combined large cell neuroendocrine
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Effective January 1, 2018 ICD O 3 codes, behaviors and terms are site specific
 Effective January 1, 2018 codes, behaviors and terms are site specific /N 8551/3 Acinar adenocarcinoma (C34. _) Lung primaries diagnosed prior to 1/1/2018 use code 8550/3 For prostate (all years) see 8140/3
Effective January 1, 2018 codes, behaviors and terms are site specific /N 8551/3 Acinar adenocarcinoma (C34. _) Lung primaries diagnosed prior to 1/1/2018 use code 8550/3 For prostate (all years) see 8140/3
Pitfalls in Sinonasal Pathology
 Pitfalls in Sinonasal Pathology Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical Sciences jhunt2@uams.edu
Pitfalls in Sinonasal Pathology Jennifer L. Hunt, MD, MEd Aubrey J. Hough Jr, MD, Endowed Professor of Pathology Chair of Pathology and Laboratory Medicine University of Arkansas for Medical Sciences jhunt2@uams.edu
59 yo male with past medical history of prostate carcinoma, presented with upper abdominal pain
 December 2016 59 yo male with past medical history of prostate carcinoma, presented with upper abdominal pain Contributed by: Divya Sharma, MD. Fellow, Gastrointestinal Pathology, Department of Pathology
December 2016 59 yo male with past medical history of prostate carcinoma, presented with upper abdominal pain Contributed by: Divya Sharma, MD. Fellow, Gastrointestinal Pathology, Department of Pathology
General: Brain tumors are lesions that have mass effect distorting the normal tissue and often result in increased intracranial pressure.
 1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
1 Lecture Objectives Know the histologic features of the most common tumors of the CNS. Know the differences in behavior of the different tumor types. Be aware of the treatment modalities in the various
WHO 2017: New Classification of Head and Neck Tumours
 WHO 2017: New Classification of Head and Neck Tumours Ilmo Leivo Department of Pathology University of Turku & Turku University Hospital FINLAND Suomen IAP Aulanko 18.05.2018 WHO 2017 New entities Simplification
WHO 2017: New Classification of Head and Neck Tumours Ilmo Leivo Department of Pathology University of Turku & Turku University Hospital FINLAND Suomen IAP Aulanko 18.05.2018 WHO 2017 New entities Simplification
Disclosure of Relevant Financial Relationships
 Ewing and Ewing like sarcomas Using Genetic Signatures in Refining Small Blue Round Cell Tumor Classification Cristina Antonescu, MD Department of Pathology Disclosure of Relevant Financial Relationships
Ewing and Ewing like sarcomas Using Genetic Signatures in Refining Small Blue Round Cell Tumor Classification Cristina Antonescu, MD Department of Pathology Disclosure of Relevant Financial Relationships
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Pathology Mystery and Surprise
 Pathology Mystery and Surprise Tim Smith, MD Director Anatomic Pathology Medical University of South Carolina Disclosures No conflicts to declare Some problem cases Kidney tumor Scalp tumor Bladder tumor
Pathology Mystery and Surprise Tim Smith, MD Director Anatomic Pathology Medical University of South Carolina Disclosures No conflicts to declare Some problem cases Kidney tumor Scalp tumor Bladder tumor
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING
 2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Eight Groups are Revised for 2018 Head & Neck Colon (includes rectosigmoid and rectum for cases diagnosed 1/1/2018 forward) Lung (2018 Draft not yet
2018 SEER Solid Tumor Manual 2018 KCR SPRING TRAINING Eight Groups are Revised for 2018 Head & Neck Colon (includes rectosigmoid and rectum for cases diagnosed 1/1/2018 forward) Lung (2018 Draft not yet
FNA OF SALIVARY GLANDS: A PRACTICAL APPROACH
 FNA OF SALIVARY GLANDS: A PRACTICAL APPROACH FNA of Salivary Glands: Challenges Wide range of neoplastic and non-neoplastic lesions Cytological overlap between the different benign and malignant tumors
FNA OF SALIVARY GLANDS: A PRACTICAL APPROACH FNA of Salivary Glands: Challenges Wide range of neoplastic and non-neoplastic lesions Cytological overlap between the different benign and malignant tumors
Normal endometrium: A, proliferative. B, secretory.
 Normal endometrium: A, proliferative. B, secretory. Nội mạc tử cung Nội mạc tử cung Cyclic changes in endometrium.. Approximate relationship of useful microscopic changes. Arias-Stella reaction in endometrial
Normal endometrium: A, proliferative. B, secretory. Nội mạc tử cung Nội mạc tử cung Cyclic changes in endometrium.. Approximate relationship of useful microscopic changes. Arias-Stella reaction in endometrial
Disclosures. An update on ancillary techniques in the diagnosis of soft tissue tumors. Ancillary techniques. Introduction
 Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
Desmoplastic Melanoma R/O BCC. Clinical Information. 74 y.o. man with lesion on left side of neck r/o BCC
 R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
R/O BCC Sabine Kohler, M.D. Professor of Pathology and Dermatology Dermatopathology Service Stanford University School of Medicine Clinical Information 74 y.o. man with lesion on left side of neck r/o
Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu
 Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu Loma Linda University Medical Center June 12, 2007 CASE 1 76 year-old gentleman Status post right parotidectomy 1 year ago for a rare tumor
Los Angeles Society Of Pathologists Dr. Shobha Castelino Prabhu Loma Linda University Medical Center June 12, 2007 CASE 1 76 year-old gentleman Status post right parotidectomy 1 year ago for a rare tumor
AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS
 AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS PAPILLARY THYROID CARCINOMA Clinical Any age Microscopic to large Female: Male= 2-4:1 Radiation history Lymph nodes Prognosis
AGGRESSIVE VARIANTS OF PAPILLARY THYROID CARCINOMA DIAGNOSIS AND PROGNOSIS PAPILLARY THYROID CARCINOMA Clinical Any age Microscopic to large Female: Male= 2-4:1 Radiation history Lymph nodes Prognosis
Case #1 FNA of nodule in left lobe of thyroid in 67 y.o. woman
 Challenging Cases Manon Auger M.D., F.R.C.P. (C) Professor, Department of Pathology McGill University Director, Cytopathology Laboratory McGill University it Health Center Case #1 FNA of nodule in left
Challenging Cases Manon Auger M.D., F.R.C.P. (C) Professor, Department of Pathology McGill University Director, Cytopathology Laboratory McGill University it Health Center Case #1 FNA of nodule in left
Pathology of the Thyroid
 Pathology of the Thyroid Thyroid Carcinoma Arising from Follicular Cells 2015-01-19 Prof. Dr. med. Katharina Glatz Pathologie Carcinomas Arising from Follicular Cells Differentiated Carcinoma Papillary
Pathology of the Thyroid Thyroid Carcinoma Arising from Follicular Cells 2015-01-19 Prof. Dr. med. Katharina Glatz Pathologie Carcinomas Arising from Follicular Cells Differentiated Carcinoma Papillary
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Polymorphous Low-Grade. December 5 th, 2008
 Polymorphous Low-Grade Adenocarcinoma December 5 th, 2008 Epidemiology Represents 2 nd or 3 rd most common minor salivary gland malignancy (17-26%) 1 st mucoepidermoid carcinoma Rare in reported Asian
Polymorphous Low-Grade Adenocarcinoma December 5 th, 2008 Epidemiology Represents 2 nd or 3 rd most common minor salivary gland malignancy (17-26%) 1 st mucoepidermoid carcinoma Rare in reported Asian
Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of
 Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
Tiền liệt tuyến Tiền liệt tuyến Gross appearance of nodular hyperplasia in material obtained from suprapubic prostatectomy. Note the multinodular appearance and the admixture of solid and microcystic areas.
An Alphabet Soup of Thyroid Neoplasms
 Overall Objectives An Alphabet Soup of Thyroid Neoplasms Lester D. R. Thompson www.lester-thompson.com What is the current management of papillary carcinoma? What are the trends and what can we do differently?
Overall Objectives An Alphabet Soup of Thyroid Neoplasms Lester D. R. Thompson www.lester-thompson.com What is the current management of papillary carcinoma? What are the trends and what can we do differently?
Breast - ductal carcinoma CK7 ER PR GATA3 Mammaglobin (50-70%) GCDFP-15 (50-70%) E-cadherin HMWCK CK20 PAX2 ER/PR/HER2 on all newly diagnosed cases
 Adrenal cortical carcinoma Inhibin Synap Melan-A Calretinin Vimentin Chromogr CK7 CK20 Breast - ductal carcinoma CK7 ER PR GATA3 Mammaglobin (50-70%) GCDFP-15 (50-70%) E-cadherin HMWCK CK20 PAX2 ER/PR/HER2
Adrenal cortical carcinoma Inhibin Synap Melan-A Calretinin Vimentin Chromogr CK7 CK20 Breast - ductal carcinoma CK7 ER PR GATA3 Mammaglobin (50-70%) GCDFP-15 (50-70%) E-cadherin HMWCK CK20 PAX2 ER/PR/HER2
Salivary gland neoplasms: an update 29th Annual Meeting of Arab Division of the International Academy of Pathology MUSCAT, OMAN 2017
 Salivary gland neoplasms: an update 29th Annual Meeting of Arab Division of the International Academy of Pathology MUSCAT, OMAN 2017 Dr Mary Toner Consultant Pathologist St James Hospital Trinity College
Salivary gland neoplasms: an update 29th Annual Meeting of Arab Division of the International Academy of Pathology MUSCAT, OMAN 2017 Dr Mary Toner Consultant Pathologist St James Hospital Trinity College
05/07/2018. Types of challenges. Challenging cases in uterine pathology. Case 1 ` 65 year old female Post menopausal bleeding Uterine Polyp
 Types of challenges Challenging cases in uterine pathology Nafisa Wilkinson Gynaecological Pathologist UCLH London Lack of complete history often, NO clinical history at all! Cases from other centres often
Types of challenges Challenging cases in uterine pathology Nafisa Wilkinson Gynaecological Pathologist UCLH London Lack of complete history often, NO clinical history at all! Cases from other centres often
4/12/2018. MUSC Pathology Symposium Kiawah Island April 18, Jesse K. McKenney, MD
 MUSC Pathology Symposium Kiawah Island April 18, 2018 Jesse K. McKenney, MD 1 Urothelial Carcinoma with Alternative Differentiation 2 Urothelial Carcinoma with Alternative Differentiation Recognition as
MUSC Pathology Symposium Kiawah Island April 18, 2018 Jesse K. McKenney, MD 1 Urothelial Carcinoma with Alternative Differentiation 2 Urothelial Carcinoma with Alternative Differentiation Recognition as
C.L. Davis Foundation Descriptive Veterinary Pathology Course
 C.L. Davis Foundation 2015 Descriptive Veterinary Pathology Course IHC Resources IHC Identification Targets Antibodies Antibodies 1 Antibodies Specimens Antigen Retrieval Unmasks antigen epitopes Methods
C.L. Davis Foundation 2015 Descriptive Veterinary Pathology Course IHC Resources IHC Identification Targets Antibodies Antibodies 1 Antibodies Specimens Antigen Retrieval Unmasks antigen epitopes Methods
Cancers of unknown primary : Knowing the unknown. Prof. Ahmed Hossain Professor of Medicine SSMC
 Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
Cancers of unknown primary : Knowing the unknown Prof. Ahmed Hossain Professor of Medicine SSMC Definition Cancers of unknown primary site (CUPs) Represent a heterogeneous group of metastatic tumours,
7 Omar Abu Reesh. Dr. Ahmad Mansour Dr. Ahmad Mansour
 7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
7 Omar Abu Reesh Dr. Ahmad Mansour Dr. Ahmad Mansour -Leukemia: neoplastic leukocytes circulating in the peripheral bloodstream. -Lymphoma: a neoplastic process in the lymph nodes, spleen or other lymphatic
Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors
 Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors. Monophasic tumors : myoepithelioma, acinic cell carcinoma, and salivary duct carcinoma. Biphasic tumors includes
Review and Updates of Immunohistochemistry in Selected Salivary Gland and Head and Neck Tumors. Monophasic tumors : myoepithelioma, acinic cell carcinoma, and salivary duct carcinoma. Biphasic tumors includes
Rhabdomyomas and Rhabdomyosarcomas (RMS) David M. Parham, MD Chief of Anatomic Pathology
 Rhabdomyomas and Rhabdomyosarcomas (RMS) David M. Parham, MD Chief of Anatomic Pathology Tumors of skeletal muscle: Rhabdomyomas and rhabdomyosarcomas Embryonal muscle 2 3 4 5 6 7 8 Rhabdomyoma Benign
Rhabdomyomas and Rhabdomyosarcomas (RMS) David M. Parham, MD Chief of Anatomic Pathology Tumors of skeletal muscle: Rhabdomyomas and rhabdomyosarcomas Embryonal muscle 2 3 4 5 6 7 8 Rhabdomyoma Benign
Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland
 Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland Two Main Topics Molecular insights in salivary gland
Molecular Diagnostics of Head and Neck Tumors Justin A. Bishop, M.D. Associate Professor of Pathology The Johns Hopkins University Baltimore, Maryland Two Main Topics Molecular insights in salivary gland
Technology from Abcam
 CD2 (EP222) CD2 is one of the earliest T-cell lineage restricted antigens to appear during T-cell differentiation and only rare CD2+ cells can be found in the bone marrow. Anti-CD2 is a pan-t-cell antigen
CD2 (EP222) CD2 is one of the earliest T-cell lineage restricted antigens to appear during T-cell differentiation and only rare CD2+ cells can be found in the bone marrow. Anti-CD2 is a pan-t-cell antigen
Head and Neck Squamous Subtypes
 1 Head and Neck Squamous Subtypes Adel K. El-Naggar, M.D., Ph.D. The University of Texas MD Anderson Cancer Center, Houston, Texas HNSCC 5 th -6 th most common cancer 400,000/year 50% mortality Considerable
1 Head and Neck Squamous Subtypes Adel K. El-Naggar, M.D., Ph.D. The University of Texas MD Anderson Cancer Center, Houston, Texas HNSCC 5 th -6 th most common cancer 400,000/year 50% mortality Considerable
Synonyms. Nephrogenic metaplasia Mesonephric adenoma
 Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
Nephrogenic Adenoma Synonyms Nephrogenic metaplasia Mesonephric adenoma Definition Benign epithelial lesion of urinary tract with tubular, glandular, papillary growth pattern Most frequently in the urinary
Disclosures. An update on ancillary techniques in the diagnosis of soft tissue tumors. Ancillary techniques. Introduction
 Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
Disclosures An update on ancillary techniques in the diagnosis of soft tissue tumors. I have nothing to disclose. Andrew Horvai, MD, PhD Clinical Professor, Pathology Introduction Ancillary techniques
Enterprise Interest None
 Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
Enterprise Interest None What are triple negative breast cancers? A synopsis of their histological patterns Ian Ellis Molecular Medical Sciences, University of Nottingham Department of Histopathology,
ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY. F ZAHRA ALY, MD, PhD
 ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY F ZAHRA ALY, MD, PhD The main areas sites amenable for cytopathology include lymph nodes, thyroid, major salivary glands especially
ARIZONA SOCIETY OF PATHOLOGISTS 13 TH APRIL 2013 HEAD AND NECK CYTOPATHOLOGY F ZAHRA ALY, MD, PhD The main areas sites amenable for cytopathology include lymph nodes, thyroid, major salivary glands especially
Applications of IHC. Determination of the primary site in metastatic tumors of unknown origin
 Applications of IHC Determination of the primary site in metastatic tumors of unknown origin Classification of tumors that appear 'undifferentiated' by standard light microscopy Precise classification
Applications of IHC Determination of the primary site in metastatic tumors of unknown origin Classification of tumors that appear 'undifferentiated' by standard light microscopy Precise classification
My Journey into the World of Salivary Gland Sebaceous Neoplasms
 My Journey into the World of Salivary Gland Sebaceous Neoplasms Douglas R. Gnepp Warren Alpert Medical School at Brown University Rhode Island Hospital Pathology Department Providence RI Asked to present
My Journey into the World of Salivary Gland Sebaceous Neoplasms Douglas R. Gnepp Warren Alpert Medical School at Brown University Rhode Island Hospital Pathology Department Providence RI Asked to present
POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT?
 POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT? AGGRESSIVE THYROID CANCERS PAPILLARY CARCINOMA CERTAIN SUBTYPES POORLY DIFFERENTIATED CARCINOMA HIGH GRADE DIFFERENTIATED
POORLY DIFFERENTIATED, HIGH GRADE AND ANAPLASTIC CARCINOMAS: WHAT IS EVERYONE TALKING ABOUT? AGGRESSIVE THYROID CANCERS PAPILLARY CARCINOMA CERTAIN SUBTYPES POORLY DIFFERENTIATED CARCINOMA HIGH GRADE DIFFERENTIATED
Educational Cases EQA November T.J. Palmer Raigmore Hospital Inverness
 Educational Cases EQA November 2013 T.J. Palmer Raigmore Hospital Inverness Case 2 Clinical Details Dob 11 February 1951 PMH: 1964 Extraction of 45 aet 13 yr 1966 Cyst between 44 and 46 enucleated 1973
Educational Cases EQA November 2013 T.J. Palmer Raigmore Hospital Inverness Case 2 Clinical Details Dob 11 February 1951 PMH: 1964 Extraction of 45 aet 13 yr 1966 Cyst between 44 and 46 enucleated 1973
USCAP 2012: Companion Meeting of the AAOOP. Update on lacrimal gland neoplasms: Molecular pathology of interest
 USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
USCAP 2012: Companion Meeting of the AAOOP Vancouver BC, Canada, March 17, 2012 Update on lacrimal gland neoplasms: Molecular pathology of interest Valerie A. White MD, MHSc, FRCPC Department of Pathology
Basement membrane in lobule.
 Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Bahram Memar, MD Basement membrane in lobule. Normal lobule-luteal phase Normal lobule-follicular phase Lactating breast Greater than 95% are adenocarcinomas in situ carcinomas and invasive carcinomas.
Disclosures. The Thin Red Line Between Neuropathology and Head & Neck Pathology. Introduction CASE 1. Current Issues Tihan
 Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Disclosures I have nothing to disclose The Thin Red Line Between Neuropathology and Head & Neck Pathology Tarik Tihan, MD, PhD UCSF, Department of Pathology Neuropathology Division Introduction Three cases
Neuroendocrine Carcinoma. Lebanon Neuroendocrine Neoplasms of H&N Nov /7/2011. Broad Classification:
 H&N Neuroendocrine Neoplasms: Classification and Diagnostic Considerations Adel K. El-Naggar, M.D., Ph.D. The University of Texas MD Anderson Cancer Center, Houston, Texas Broad Classification: A. Epithelial:
H&N Neuroendocrine Neoplasms: Classification and Diagnostic Considerations Adel K. El-Naggar, M.D., Ph.D. The University of Texas MD Anderson Cancer Center, Houston, Texas Broad Classification: A. Epithelial:
PSA. HMCK, p63, Racemase. HMCK, p63, Racemase
 Case 1 67 year old male presented with gross hematuria H/o acute prostatitis & BPH Urethroscopy: small, polypoid growth with a broad base emanating from the left side of the verumontanum Serum PSA :7 ng/ml
Case 1 67 year old male presented with gross hematuria H/o acute prostatitis & BPH Urethroscopy: small, polypoid growth with a broad base emanating from the left side of the verumontanum Serum PSA :7 ng/ml
DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES
 DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES Dr. Andrew J. Evans MD, PhD, FACP, FRCPC Consultant in Genitourinary Pathology University Health Network, Toronto, ON Case 1 43 year-old female,
DIAGNOSTIC SLIDE SEMINAR: PART 1 RENAL TUMOUR BIOPSY CASES Dr. Andrew J. Evans MD, PhD, FACP, FRCPC Consultant in Genitourinary Pathology University Health Network, Toronto, ON Case 1 43 year-old female,
Squamous Cell Carcinoma of Thyroid: possible thymic origin, so-called ITET/CASTLE 2012/03/22
 Squamous Cell Carcinoma of Thyroid: possible thymic origin, so-called ITET/CASTLE 2012/03/22 History of ITET/CASTLE First Report Gross Appearance and Prognosis 1) Miyauchi A et al: Intrathyroidal epithelial
Squamous Cell Carcinoma of Thyroid: possible thymic origin, so-called ITET/CASTLE 2012/03/22 History of ITET/CASTLE First Report Gross Appearance and Prognosis 1) Miyauchi A et al: Intrathyroidal epithelial
Renal tumours: use of immunohistochemistry & molecular pathology. Dr Lisa Browning John Radcliffe Hospital Oxford
 Renal tumours: use of immunohistochemistry & molecular pathology Dr Lisa Browning John Radcliffe Hospital Oxford Renal tumours: the use of immunohistochemistry & molecular pathology Classification of RCC
Renal tumours: use of immunohistochemistry & molecular pathology Dr Lisa Browning John Radcliffe Hospital Oxford Renal tumours: the use of immunohistochemistry & molecular pathology Classification of RCC
Slide seminar. Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana
 Slide seminar Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana Case 5 A 57-year-old man with a dermal/subcutaneous lesion on the scalp, which was interpreted
Slide seminar Asist. Prof. Jože Pižem, MD, PhD Institute of Pathology Medical Faculty, University of Ljubljana Case 5 A 57-year-old man with a dermal/subcutaneous lesion on the scalp, which was interpreted
CODING TUMOUR MORPHOLOGY. Otto Visser
 CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
CODING TUMOUR MORPHOLOGY Otto Visser INTRODUCTION The morphology describes the tissue of the tumour closest to normal tissue Well differentiated tumours are closest to normal Undifferentiated tumours show
Case year female. Routine Pap smear
 Case 1 57 year female Routine Pap smear Diagnosis? 1. Atypical glandular cells of unknown significance (AGUS) 2. Endocervical AIS 3. Endocervical adenocarcinoma 4. Endometrial adenocarcinoma 5. Adenocarcinoma
Case 1 57 year female Routine Pap smear Diagnosis? 1. Atypical glandular cells of unknown significance (AGUS) 2. Endocervical AIS 3. Endocervical adenocarcinoma 4. Endometrial adenocarcinoma 5. Adenocarcinoma
