Foramen Magnum Meningiomas
|
|
|
- Marlene Green
- 6 years ago
- Views:
Transcription
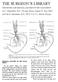
1 Foramen Magnum Meningiomas Part II: Surgical Approaches, Surgical Anatomy, Complications of Treatment and Results Kenan I. Arnautovic, M.D., and Ossama AI-Mefty, M.D. Learning Objectives: After reading this article, the participant should be able to: 1. Identify the surgical anatomy and approaches to the foramen magnum region. 2. Recall the transcondylar approach to foramen magnum meningiomas. 3. Describe the suboccipital approach to foramen magnum meningiomas. 4. Explain the postoperative care and complications related to surgical techniques offoramen magnum meningiomas. Operative Indications and Aims of Operation Meningiomas arising at the foramen magnum are a neurosurgical challenge because of the large number of vital anatomic elements concentrated in this deep, hidden, central, and small area. These lesions can be divided into two distinct groups according to their site of attachment and position: anterior or anterolateral, and posterior or posterolateral. These two types differ in operative approach and resectability, the rate of complications, and prognosis. The medulla and the upper cervical spinal cord and adjacent anatomic elements are displaced posteriorly by a tumor originating anteriorly. Anterior origin is most common, occurring in 68% to 98% of patients. Removal is difficult, the rate of total resection is lower, and the rates of complications, morbidity, and mortality are higher. Meningiomas that originate posteriorly (2% to 32% of these lesions) displace structures anteriorly. The surgical goal, regardless of the size of a foramen magnum meningioma, should be to preserve and improve neurological function by radical tumor removal. Such removal should be attempted zealously at the initial operation, which is the best time to achieve a cure. The surgeon sometimes may be forced to accept subtotal removal, however, when the tumor is severely adherent to vital neurovascular structures. Dr. Arnautovic' is a resident, and Dr. Al-Mefty is Professor and Chairman, Department of Neurosurgery, 4301 West Markham, Slot 507, University ofarkansas for Medical Sciences, Little Rock, Arkansas The authors have disclosed that they have no significant relationships with or financial interests in any commercial organizations pertaining to this educational activity. Surgical Approaches and Surgical Anatomy Two surgical approaches are routinely used to treat foramen magnum meningiomas: the transcondylar approach and the inferior suboccipital approach. Hemilaminectomy of the atlas and the axis is added to either of these two approaches as indicated. The transcondylar avenue is used for anterior or anterolaterally located meningiomas at the foramen magnum. Meningiomas located posteriorly or posterolaterally are approached through the inferior suboccipital route with a suboccipital craniotomy and a laminectomy. The approach is determined according to the individual circumstances of each tumor. For example, large tumors may require additional exposure. Those extending inferiorly require an additional laminectomy of the atlas and the axis. Tumors that extend superiorly require the petrosal or retrosigmoidal approach, whereas meningiomas extending laterally into the jugular foramen require infratemporal exposure. The transoral approach to the foramen magnum provides direct midline exposure of a foramen magnum meningioma. We do not favor this approach, however. Its midline exposure is limited laterally, there is a significant risk of contamination by flora of the oral cavity, not all neurovascular structures can be visualized during dissection, and the operative field is deep. Category: Tumor Key Words: Foramen magnum, Meningioma, Transcondylar Approach, Suboccipital Approach.
2 Transcondylar Approach and General Surgical Strategy We prefer the transcondylar approach for ventral and ventrolateral foramen magnum meningiomas. This approach may be referred to by different name-e.g., far lateral, posterolateral, extreme lateral, or transcondylar. In essence, however, it is one approach with variations in the patient's position, the skin incision, muscle reflection, and craniotomy. The following paragraphs describe the transcondylar approach as we use it. Patient position. The anesthetized patient is placed supine. The head and neck are kept in a neutral position to maintain the anatomic course of the vertebral artery and for easier stabilization, if necessary. The patient is then logrolled rotated approximately 40. The patient's head is fixed in position with a Mayfield-Kees headrest. The arch for the frameless stereotaxy is attached to it, encircling the head. Care is taken to avoid any obstruction of the surgical view. The ipsilateral shoulder is gradually pulled downward and taped to keep it from obstructing the field. The ipsilateral thigh also is prepared and draped for the removal of fat and fascia lata (Fig. 1). Skin incision. The skin is incised behind the ear in a curvilinear fashion two fingerbreadths behind the mastoid. The curved incision begins at the level of the external auditory canal and turns downward to the level of the C4 vertebra, where it gradually curves anteriorly into the horizontal neck crease. The skin flap is then retracted laterally and secured with fishhook retractors. Two nerves, the greater auricular nerve laterally and the lesser occipital nerve medially, are identified in subcutaneous tissue as potential graft donors. This skin flap is well vascularized and can easily be tailored to accommodate other approaches, if necessary. Muscle dissection. The muscles are dissected in three layers. First, the sternocleidomastoid muscle is detached from its origin at the occipital bone (the superior nuchal line) and mastoid and retracted inferiorly and medially. Its innervation (by the accessory nerve) should be preserved and freed as it enters the medial aspect of the muscle at the level of the C3 vertebra. The splenius capitis, longissimus Figure 1. Operative position of the patient. Note the 40 log-rolled rotation of the patient, maintaining the head and neck in the neutral position. Note also the skin incision, the ipsilateral shoulder taped and pulled out of the way, the EMG electrodes in place for intraoperative monitoring, and the arch of the frameless stereotaxy (arrows) attached to the head rest. capitis, and semispinalis muscles-the muscles of the second muscular layer-are also detached along with the sternocleidomastoid muscle and retracted inferiorly and medially. This retraction turns the muscles away from the working area, which is mainly lateral. Between the second and third muscular layers lies a rich suboccipital venous plexus, which may be a source of bleeding or air embolism. Another source is the mastoid emissary vein, which is encountered as it exits the mastoid foramen. This emissary vein connects the sigmoid dural venous sinus and the complex extracranial venous system in the suboccipital area. The muscles of the third, deep layer create two triangles-the superior and inferior suboccipital triangles. The superior suboccipital triangle is delineated by the rectus capitis, posterior major, obliquus capitis superior, and obliquus capitis inferior muscles. In the depth of this triangle is the venous compartment, which cushions the horizontal part of the suboccipital vertebral artery, its branches,
3 and the Cl nerve. The inferior suboccipital triangle is delineated by the obliquus capitis inferior, semispinalis cervicis, and longissimus cervicis muscles. Within this triangle is the vertical part of the suboccipital vertebral artery, its branches, its surrounding venous plexus, and the C2 nerve with its anterior and posterior rami. The lateral corners of both triangles meet at the transverse process of the atlas, which is located 1 em below the mastoid tip. The muscles of this third layer are detached and reflected medially orresected. To improve exposure, the posterior belly of the digastric muscle also can be detached and reflected laterally. Exposure, mobilization and transposition of the vertebral artery complex. In most people, the vertebral artery is larger on the left side. During surgery of a foramen magnum meningioma, two segments of the vertebral artery are encountered: the suboccipital (V3) and the intracranial (V4). Exposing and mobilizing the V3 complex allows full proximal control of the artery. Transposing the V3 complex allows drilling of the condyle, ventral exposure of the tumor, and safe dissection. The V3 segment is subdivided into two parts, the vertical (V3v) and horizontal (V3h). The venous compartment located between the occipital bone and the atlas was earlier named the suboccipital cavernous sinus because of its similarity to the cavernous sinus. It is bordered posteriorly by the posterior atlanto-occipital membrane, anteriorly by the occipital condyle and the atlanto-occipital dura, laterally by the lateral periosteal ring at the transverse foramen of the atlas, and medially by the dural ring, which surrounds the vertebral artery as it pierces the dura. V3h, its branches, and the Cl nerve are cushioned within this compartment. V3h has two arterial branches[em]the muscular artery, which originates at its midportion and courses dorsally, and the posterior meningeal artery, which originates a few millimeters proximal to the dural ring. These two arteries are coagulated and divided. V3v extends from the transverse foramen of the axis, where the artery makes an inferomedialloop, and immediately turns into the inferolateralloop, which brings the artery into the transverse foramen of the atlas. V3v is surrounded by a venous plexus, which is an inferior continuation of the suboccipital cavernous sinus (Fig. 2). The V3v complex is crossed dorsally at its midportion by an anterior ramus of the C2 nerve. This nerve is attached to V3v by a fibrous adhesion, which must be released to allow caudomedial transposition of the V3 complex. V3v gives off two branches, the radiculomuscular artery medially and the muscular artery laterally. These branches also must be divided to allow caudomedial transposition of the vertebral artery. In the transverse foramen of the atlas, the V3 complex is surrounded by a periosteal, lateral ring. At this point, V3v turns into V3h through the superolateral loop and enters the suboccipital cavernous sinus. Once the posterior atlanto-occipital membrane is opened, the posterior wall of the transverse foramen of the atlas is drilled, and careful, subperiosteal dissection is done. This dissection spares the lateral (periosteal) ring, which is used to manipulate the V3 complex. The suboccipital cavernous sinus anastomoses through the condylar veins with the jugular bulb and vein. These vessels must be divided to allow caudomedial transposition of the V3 complex. 3 Figure 2. Right-sided intraoperative illustration after the dissection and retraction of muscles and detachment of the posterior atlantooccipital membrane. The suboccipital cavernous sinus (SCS) is exposed, cushioning the horizontal part of the suboccipital VA. Note also the vertical part of the suboccipital VA surrounded by a VA venous plexus (VAVP), lateral (periosteal) ring (LR) after the drilling of the transverse foramen of C1, posterior (PCV) and lateral (LCV) condylar veins, which are divided (arrows), the jugular vein (JV), the atlas (C1), the second cervical nerve (C2n), the axis (C2), the external vertebral venous plexus (EVP) and the eleventh nerve (XI) entering the sternocleidomastoid muscle. (Reprinted with permission from Arnautovic KI, AI-Mefty 0, Husain M: Ventral foramen magnum meningiomas. J Neurosurgery (Spine) 92:71, 2000.) The posterior ramus of the Cl nerve (the suboccipital nerve) must be sacrificed. In addition, the retroglenoid ligament, which connects the V3h complex and the occipital condyle, must be divided to unlock the sinus. The fibrous membrane around the sinus along with the areolar tissue on that membrane must be kept intact to prevent bleeding and the possibility of an air embolus. Any venous bleeding can be easily controlled with Gelfoam and gentle compression. The V3 complex (preferably with intact venous structures around it) is then transposed caudomedially if the intraoperative situation requires, as decided by the inferior extension of the tumor beyond the atlas, the encasement of the vertebral artery, and the extension of the tumor to the contralateral side. Bony resection. For bony resection, a lateral, posterior fossa craniotomy is done, and the mastoid tip is drilled to expose the occipital condyle. The sigmoid sinus and jugular bulb are fully exposed, and the atlantal and occipital condyles are drilled. Drilling of the condyle must be tailored to suit the needs of each case. For ventrally located tumors, extensive drilling is required, whereas laterally placed tumors need only partial drilling of the condyle. In other words, the more ventrally the tumor extends, or the more it extends across the midline, the more of the condyle is drilled. Drilling of the condyle never extends to more than half of it, however. Thus, stabilization is not required. Laminectomy of the atlas often is necessary, and sometimes laminectomy of the axis is required as well.
4 Dural opening. The dura mater of the foramen magnum, and, therefore, any meningioma located there, is supplied by the following arterial branches: the posterior meningeal artery originating from the V3 segment of the vertebral artery; the anterior meningeal artery originating from the V2 segment of the vertebral artery; the meningeal branch of the occipital artery entering the cranium through the foramen with the mastoid emissary vein; and the meningeal branch of the ascending pharyngeal artery, which enters the cranium through the hypoglossal canal. Occasionally, the intracranial segment of the vertebral artery, the posterior inferior cerebellar artery (PICA), the posterior spinal arteries, and the internal carotid artery may also vascularize the tumor. These branches mutually anastomose. The vertebral artery and the branches of the occipital artery are encountered early in the surgical exposure and should be dissected, coagulated, and divided to reduce the bleeding rate and permit easier removal of the tumor. The dural incision is centered on the dural ring surrounding the vertebral artery. Opening the dural ring leaves a dural cuff of sufficient size around the artery. An incision along the sigmoid sinus is extended inferiorly to the dural ring. This incision extends further inferiorly and laterally to the level of the atlas, or lower if necessary. The dura is tented laterally. Intradural tumor dissection. In up to one half of patients, a meningioma at the foramen magnum encases the intracranial segment of the vertebral artery. The tumor also can displace this intracranial segment of the vertebral artery backward and laterally. In many instances, the tumor around the vertebral artery can be separated from the vessel because of an intervening arachnoidal membrane. If the tumor is located laterally, the vertebral artery is hidden beneath it. In patients with ventrally located meningiomas, the vertebral artery is at the lateral aspect of the tumor. The PICA usually is displaced dorsally or medially; it also may be embedded in the tumor. The anterior and posterior spinal arteries usually adhere to the tumor. Intra-arachnoidal dissection allows these arteries to be preserved. The brain stem and cervical spinal cord are displaced posteriorly and to the contralateral side by an anteriorly or anterolaterally located meningioma. This displacement facilitates the exposure and the approach to the most anterior segment and dural attachment of the tumor. Early debulking of the tumor decreases the pressure on and displacement of the surrounding structures and makes the subsequent surgery easier and safer. The tumor is debulked with either the ultrasonic aspirator or suction and bipolar coagulation (Fig. 3). The upper pole of the tumor should be separated from the lower cranial nerves; the lower pole is separated from the medulla and the spinal cord at its lower extension into the spinal canal. The length of the spinal portion of the accessory nerve varies, and the nerve often is short. Freeing this nerve may allow additional mobilization and create more working space. The accessory nerve usually is stretched, and its rootlets spread over the lateral aspect of the tumor. The glossopharyngeal, vagal, and hypoglossal nerves usually are displaced superiorly. Crucial factors in preserving these Figure 3. Right-sided intraoperative illustration after the VA complex transposition and the dural opening; the arachnoid membrane is opened. Note the transposed suboccipital VA complex (horizontal part) cushioned in the 8C8, the vertical part of the suboccipital VA surrounded by the VA venous plexus (VAVP), the posterior inferior cerebellar artery (PICA), the dural ring (DR) around the VA, cranial nerves IX through XII, the sigmoid sinus (88), the jugular bulb (JB), and the jugular vein (JV). Cavitron ultrasonic aspiration of the tumor is underway. (Reprinted with permission from Arnautovic KI, AI-Mefty 0, Husain M: Ventral foramen magnum meningiomas. J Neurosurgery (Spine) 92:71,2000.) nerves are the presence of an arachnoidal membrane and dissection within this membrane and along these nerves and their rootlets. Dividing the first dentate ligament, which is attached to the dura behind and above the dural ring, increases the amount of maneuvering and working space. The dural attachment of the tumor should be devascularized as early as possible. The dura also must be excised. The tumor often invades the adjacent dura, and clusters of tumor cells often can be verified histologically within the dura. Any hyperostotic bone should be drilled away, because it represents tumor invasion. This surgical strategy allows removal of the tumor to Simpson grades I and II, and significantly decreases the recurrence rate (Fig. 4). Closure. After the tumor is removed and meticulous hemostasis has been attained, the dura is closed in a watertight fashion. A dural cuff of sufficient size at the dural ring, left around the vertebral artery at opening, facilitates dural closure and prevents leakage of cerebrospinal fluid. The routine use of autologous fat grafts, fascia lata grafts, and rotated posterior cervical muscles during closure also can prevent a postoperative leak of cerebrospinal fluid. The Inferior Suboccipital Approach The median inferior suboccipital approach and its modifications have been used since the earliest attempts at surgery of foramen magnum meningiomas. We use this approach for posterior and posterolateral foramen magnum meningiomas. The approach often is done with the patient in a sitting position, but prone and lateral positions also have been used. 4
5 Figure 4. Right-sided intraoperative illustration after the tumor resection. Note the previous site of tumor attachment after the dural resection and the bone drilling (*), Simpson grades I and II. The same anatomic elements seen in Figures 2 and 3 are shown after radical tumor resection. (Reprinted with permission from Arnautovic KI, AI-Mefty 0, Husain M: Ventral foramen magnum meningiomas. J Neurosurgery (Spine) 92:71, 2000.) The pertaining inferior suboccipital approach regional anatomy is described earlier in this lesson. In its classic form, this approach is done through a midline skin incision from the occipital protuberance down to the C2-C3 spinous process. The posterior cervical muscles are split at the midline to expose the suboccipital squama and atlanto-axial spinous processes. Even if transposition of the V3 complex (the suboccipital cavernous sinus) is not necessary, exposing this complex is recommended to allow the surgeon secure proximal control of the artery should it be necessary. After a single bur hole is drilled below the level of the external occipital protuberance and the torcula herophili, the dura is freed from the internal table of the occipital bone. A craniotomy is performed, and the foramen magnum is opened. Laminectomies of the atlas and the axis are done according to the extension of the tumor into the spinal canal. The dura is opened longitudinally, with two laterosuperior and lateroinferior extensions on each end. The arachnoid over the cerebellomedular (magna) cistern is incised, and the midline araclmoidal septum can be observed. Cerebrospinal fluid is released, and the medulla and spinal cord are displaced posteriorly and to the contralateral side. The general surgical strategy and tumor removal techniques described earlier in this lesson pertain to this approach as well. Postoperative Care and Complications The rate of complications in the treatment of foramen magnum meningiomas is relatively high, and it is higher for anterior tumors than for posterior ones. Morbidity ensues primarily from deficits of lower cranial nerves, specifically the glossopharyngeus, the vagus, and the hypoglossus. Such complications may lead to aspiration pneumonia. Other important complications are leakage of cerebrospinal fluid and meningitis. In the case of cerebrospinal fluid leak, additional stitches and compressive dressing and external lumbar drainage may be used. If the leak persists, operative revision may be indicated. In the case of hydrocephalus, a ventriculoperitoneal shunt is indicated. Patients with low preoperative clinical grading scores are particularly prone to complications and poor outcomes. After surgery, careful assessment of the caudal cranial nerves is paramount to the patient's successful recovery. Aspiration precautions should be taken before the patient is allowed oral intake, and the diet is advanced gradually from a dysphagia diet to a regular one as indicated. Speech pathologists and otolaryngologists are involved early in the postoperative course. Intensive pulmonary care, aggressive pulmonary toilet, and antibiotic prophylaxis are used to prevent fatal respiratory complications in patients with deficits of the lower cranial nerves. Patients with a deficit of the glossopharyngeal and vagus nerves may need an aggressive tracheostomy to protect the airway and manage secretions, and also may require a gastric tube or a gastrostomy. Paralysis of the vocal cords early in the postoperative course can be approximated by vocal cord medialization, or the cord can be injected with Gelfoam or Teflon. Such treatment protects the airway until the nerve recovers or the patient learns to compensate for the deficit, which may take up to 8 months. Postoperative images are obtained routinely after surgery. These images help the surgeon evaluate the extent of tumor removal and possible complications and also serve as a baseline for future follow-up. Computed tomography (CT) scan and magnetic resonance imaging (MRI) are obtained immediately after the surgery, followed by MRIs at 3 months, 6 months, 12 months, and annually thereafter. Prognosis Surgical results in patients with foramen magnum meningiomas are worse than those for patients with meningiomas in most other locations. Worse results appear in three categories: mortality; the patient's postoperative clinical status and complications; and the degree of tumor removal. The radicality of the tumor removal and the perioperative mortality rates are understandably worse for patients with ventrally placed foramen magnum meningiomas. Fortunately; postoperative results for this category have improved over time. In the past 15 years, mortality has decreased, and ranges from 0% to 29%. The rate of radical ("gross total Jl ) removal has also increased, and ranges from 60% to 75%. The improved results are greatly influenced by the use of microsurgical techniques and the transcondylar approach. Acknowledgments We are indebted to Ms. Julie Yamamoto for editorial assistance and Mr. Ron M. Tribell for original artwork. Readings Al-Mefty 0, Borba LAB, Aoki N, et al: The transcondylar approach to extradural normeoplastic lesions of the craruovertebral junction. JNeurosurg 84:
6 Al-Mefty 0: Operative Atlas ofmeningiomas. Philadelphia: Lippincott-Raven, 1997, pp Arnautovic KI, Al-Mefty 0: Foramen magnum meningiomas, in Kaye A, Black PMcL (eds): Operative NeurosurgeryVol 1. London: Harcourt Brace, 2000, pp Arnautovic KI, Al-Mefty 0, Husain M: Ventral foramen magnum meningiomas. J NeurosurgenJ (Spine) 92:71,2000 Arnautovic Kl, Al-Mefty 0, PaitTG, et al: The suboccipital cavernous sinus. J Neurosurg 86:252,1997 Bertalanffy H, Seeger W: The dorsolateral, suboccipital, transcondylar approach to the lower clivus and anterior portion of the craniocervical junction. NeurosurgenJ 29:815,1991 Caruso RD, Rosenbaum AE, Chang]K, et al: Craniocervical junction venous anatomy on enhanced MRl images: the suboccipital cavernous sinus. AJNR 20:1127, 1999 de Oliveira E, Rhoton AL Jr, Peace D: Microsurgical anatomy of the region of the foramen magnum. Surg NeuroI24:293, 1985 George B, Lot G: Anterolateral and posterolateral approaches to the foramen magnum: technical description and experience from 97 cases. Skull Base Surg 5:9,1995 George B, Lot G, Boissonnet H: Meningioma of the foramen magnum: a series of 40 cases. Surg Neurol 47:371, 1997 Guidetti B, Spallone A: Benign extramedullary tumors of the foramen magnum. Adv Tech Stand Neurosurg 16:83, 1988 Kratimenos Gp, Crockard HA: The far lateral approach for ventrally placed foramen magnlun and upper cervical spine tumors. Br JNeurosurg 7:29, 1993 Miller E, Crockard A: Transoral transclival removal of anteriorly placed meningiomas at the foramen magnlun. Neurosurgery 20:966,1987 Salas E, Sekhar LN, Ziyal I, et al: Variations of the extreme-lateral craniocervical approach: anatomical study and clinical analysis of 69 patients. JNeurosurg (Spine) 90: 206, 1999 Sarnii M, KJekamp J, Carwalho G: Surgical results for meningioma of the craniovertebral junction. Neurosurgery 39: 1086, 1996 ScottEW, RhotonALJr. Foramen magnlunmeningiomas, inal-mefty 0 (ed): Meningiomas. New York: Raven Press, 1991, pp Sen CN, Sekhar LN: An extreme lateral approach to intradural lesions of the cervical spine and foramen magnlun. Neurosurgery 27: 197,1990 Welling B, Park YK, Al-Mefty 0: Primary extramedullary tumors of the craniovertebral junction, in Dickman CA, Spetzler RF, Sonntag VKH (eds): Surgery of the Craniovertebral Junction. New York: Thieme, 1998, pp Yasargil MG: Microneurosurgery ofcns Tumors. Vol IVb. Stuttgart: Georg Thieme Verlag, 1996, pp To earn CME credit, you must read the CME article and complete the quiz, answering at least 70% of the questions correctly. Select the best answer, and darken the corresponding space on the response card. Use #2 pencil only. To earn credit for this article, response card must be mailed on or before February 22, Lippincott Williams & Wilkins is accredited by tile Accreditation Council for Continuing Medical Education to provide continuing medical education for physicians. Lippincott Williams & Wilkins designates this educational activity for a maximum of 1.5 hours in category 1 credit of the AMA Physician's Recognition Award. Each physician should claim only those hours of credit that he/she actually spent in the educational activity. 1. Anterior or anterolateral foramen magnum meningiomas are 6. The posterior meningeal artery is a branch of the middle best removed through the transcondylar approach. meningeal artery. 2. The rich suboccipital venous plexus usually is located under 7. The meningeal branch of the ascending pharyngeal artery the sternocleidomastoid muscle layer. enters the cranium through the jugular foramen. 3. The muscles of the third deepest layer to be exposed in 8. The transcondylar approach is needed for posterior and postranscondylar approach form two (inferior and superior) tri- terolateral meningiomas. angles. 9. The most serious postoperative complication after surgery of 4. Drilling of the occipital condyle is indicated to provide more foramen magnum meningiomas is related to lower cranial ventral exposure of the cervicomedullary junction. nerve dysfunction. 5. Drilling of 50% of the condyle is always an indication for occip- 10. Encasement of the vertebral artery by foramen magnum itocervical stabilization. meningiomas occurs in up to 50% of cases / 6
Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach
 J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer
 Review article The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer 1Dr. Jaspreet Singh Badwal, 2 Dr. Upkardeep Singh, 3 Dr. Neha Bharti, 4 Dr.Shivani Garg, 5 Dr.Simarpreet Singh
Review article The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer 1Dr. Jaspreet Singh Badwal, 2 Dr. Upkardeep Singh, 3 Dr. Neha Bharti, 4 Dr.Shivani Garg, 5 Dr.Simarpreet Singh
Unilateral extended suboccipital approach for a C1 dumbbell schwanoma
 38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
5.5. RETROSIGMOID APPROACH
 5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
5.5. RETROSIGMOID APPROACH The retrosigmoid approach provides good access to the cerebellopontine angle. It is by far simpler and faster with much less need for bone removal than other more extensive lateral
Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass
 32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
32 Large Dumbbell-Shaped C1 Schwannoma Presenting as a Foramen Magnum Mass Jody Helms, M.D. 1 Lattimore Madison Michael II, M.D., F.A.A.N.S., F.A.C.S. 1, 2 1 Department of Neurosurgery, University of Tennessee
The Back OUTLINE. Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region
 The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
The area around the foramen magnum
 OPERATIVE NUANCES FAR-LATERAL APPROACH TO THE CRANIOCERVICAL JUNCTION Giuseppe Lanzino, M.D. Peoria, Illinois Sergio Paolini, M.D. Peoria, Illinois THE FAR-LATERAL APPROACH is an extension of the standard
OPERATIVE NUANCES FAR-LATERAL APPROACH TO THE CRANIOCERVICAL JUNCTION Giuseppe Lanzino, M.D. Peoria, Illinois Sergio Paolini, M.D. Peoria, Illinois THE FAR-LATERAL APPROACH is an extension of the standard
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Neck-2. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Neck-2 ` Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Triangles of the neck Side of the neck Midline Lower border of mandible Line between angle of mandible and mastoid Superior nuchal
Brain ميهاربا لض اف دمح ا د The Meninges 1- Dura Mater of the Brain endosteal layer does not extend meningeal layer falx cerebri tentorium cerebelli
 .احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
.احمد د فاضل ابراهيم Lecture 15 Brain The Meninges Three protective membranes or meninges surround the brain in the skull: the dura mater, the arachnoid mater, and the pia mater 1- Dura Mater of the Brain
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
Neurosurgical Techniques
 Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
Neurosurgical Techniques Neurosurgical Techniques Laminectomy for the Removal of Spinal Cord Tumors J. GRAFTON LOVE, M.D. Section of Neurologic Surgery, Mayo Clinic and Mayo Foundation, Rochester, Minnesota
The Anatomy of the Atlantoaxial Complex
 The Anatomy of the Atlantoaxial Complex T. GLENN PAIT, M.D., KENAN 1. ARNAUTOVIC, M.D., and LUIS A.B. BORBA, M.D. Operating on the atlantoaxial complex has always posed a challenge to the surgeon because
The Anatomy of the Atlantoaxial Complex T. GLENN PAIT, M.D., KENAN 1. ARNAUTOVIC, M.D., and LUIS A.B. BORBA, M.D. Operating on the atlantoaxial complex has always posed a challenge to the surgeon because
25/06/2010. Scaricato da 1
 Approcci chirurgici al Clivus DIPARTIMENTO DI NEUROCHIRURGIA SECONDA UNIVERSITÀ DI NAPOLI Prof. Aldo Moraci Surgical Anatomy of the Clivus Scaricato da www.sunhope.it 1 Midsagittal Section of the Skull
Approcci chirurgici al Clivus DIPARTIMENTO DI NEUROCHIRURGIA SECONDA UNIVERSITÀ DI NAPOLI Prof. Aldo Moraci Surgical Anatomy of the Clivus Scaricato da www.sunhope.it 1 Midsagittal Section of the Skull
Fusion and instrumentation at C1 3 via the high anterior cervical approach
 J Neurosurg (Spine 1) 92:24 29, 2000 Fusion and instrumentation at C1 3 via the high anterior cervical approach JOHN R. VENDER, M.D., STEVEN J. HARRISON, M.S., AND DENNIS E. MCDONNELL, M.D. Division of
J Neurosurg (Spine 1) 92:24 29, 2000 Fusion and instrumentation at C1 3 via the high anterior cervical approach JOHN R. VENDER, M.D., STEVEN J. HARRISON, M.S., AND DENNIS E. MCDONNELL, M.D. Division of
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
The suboccipital cavernous sinus
 The suboccipital cavernous sinus Kenan I. Arnautovic, M.D., Ossama Al-Mefty, M.D., T. Glenn Pait, M.D., Ali F. Krisht, M.D., and Muhammad M. Husain, M.D. Departments of Neurosurgery and Pathology, University
The suboccipital cavernous sinus Kenan I. Arnautovic, M.D., Ossama Al-Mefty, M.D., T. Glenn Pait, M.D., Ali F. Krisht, M.D., and Muhammad M. Husain, M.D. Departments of Neurosurgery and Pathology, University
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
Unit 18: Cranial Cavity and Contents
 Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
Unit 18: Cranial Cavity and Contents Dissection Instructions: The calvaria is to be removed without damage to the dura mater which is attached to the inner surface of the calvaria. Cut through the outer
For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER
 GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]
![_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come] _CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]](/thumbs/81/84146690.jpg) 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Foramen magnum lesions represent only 0.3% 3.2%
 Neurosurg Focus 35 (6):E12, 2013 AANS, 2013 The far-lateral approach for foramen magnum meningiomas Bruno C. Flores, M.D., Benjamin P. Boudreaux, M.D., Daniel R. Klinger, M.D., Bruce E. Mickey, M.D., and
Neurosurg Focus 35 (6):E12, 2013 AANS, 2013 The far-lateral approach for foramen magnum meningiomas Bruno C. Flores, M.D., Benjamin P. Boudreaux, M.D., Daniel R. Klinger, M.D., Bruce E. Mickey, M.D., and
The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University
 The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University The Trunk and Spinal Column Vertebral column 24 articulating vertebrae 31 pairs of spinal nerves Abdominal muscles some
The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University The Trunk and Spinal Column Vertebral column 24 articulating vertebrae 31 pairs of spinal nerves Abdominal muscles some
Dr.Noor Hashem Mohammad Lecture (5)
 Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
University of Palestine. Midterm Exam 2013/2014 Total Grade:
 Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
Muscles of the Upper Limb that are dissected in the Back Region Muscle Origin Insertion Action Innervation Artery Notes
 Muscles of Upper Limb that are dissected in Back Region Muscle Origin Insertion Action Innervation Artery Notes floor of thoraco thoraco inserting spines from intertubercular arm nerve (C7,8) a. tendon
Muscles of Upper Limb that are dissected in Back Region Muscle Origin Insertion Action Innervation Artery Notes floor of thoraco thoraco inserting spines from intertubercular arm nerve (C7,8) a. tendon
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Cranial Cavity REFERENCES: OBJECTIVES OSTEOLOGY. Stephen A. Gudas, PT, PhD
 Stephen A. Gudas, PT, PhD Cranial Cavity REFERENCES: Moore and Agur, Essential Clinical Anatomy (ECA), 3rd ed., pp. 496 498; 500 507; 512 514 Grant s Atlas 12 th ed., Figs 7.6; 7.19 7.30. Grant s Dissector
Stephen A. Gudas, PT, PhD Cranial Cavity REFERENCES: Moore and Agur, Essential Clinical Anatomy (ECA), 3rd ed., pp. 496 498; 500 507; 512 514 Grant s Atlas 12 th ed., Figs 7.6; 7.19 7.30. Grant s Dissector
Intraoperative monitoring of foramen occipitalis magnum meningiomas surgery significantly improves the preservation of neurological functions
 Activitas Nervosa Superior Rediviva Volume 57 No. 3 2015 This paper has been published under Creative Common Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0) allowing to download
Activitas Nervosa Superior Rediviva Volume 57 No. 3 2015 This paper has been published under Creative Common Attribution-NonCommercial-NoDerivatives 4.0 International (CC BY-NC-ND 4.0) allowing to download
Inferior view of the skull showing foramina (Atlas of Human Anatomy, 5th edition, Plate 12)
 Section 1 Head and Neck Skull, Basal View Incisive foramen Choanae Foramen ovale Foramen lacerum Foramen spinosum Carotid canal Jugular fossa Mastoid process Inferior view of the skull showing foramina
Section 1 Head and Neck Skull, Basal View Incisive foramen Choanae Foramen ovale Foramen lacerum Foramen spinosum Carotid canal Jugular fossa Mastoid process Inferior view of the skull showing foramina
Cervical Spine Anatomy and Biomechanics. Typical Cervical Vertebra C3 6. Typical Cervical Vertebra Anterior 10/5/2017
 Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli.
 Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
We describe some of the conceptual nuances and
 Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
Suprasellar Meningiomas Ivan Ciric, M.D., Sami Rosenblatt, M.D. Division of Neurosurgery, Evanston Northwestern Healthcare, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois
nerve sheath tumors: Analysis of 32 cases
 C 1 : Analysis of 32 cases Original Article Parmatma Maurya, Kulwant Singh, Vivek Sharma Department of Neurosurgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi - 221 005, India Abstract
C 1 : Analysis of 32 cases Original Article Parmatma Maurya, Kulwant Singh, Vivek Sharma Department of Neurosurgery, Institute of Medical Sciences, Banaras Hindu University, Varanasi - 221 005, India Abstract
Tympanic Bulla Temporal Bone. Digastric Muscle. Masseter Muscle
 Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Structure and Function of the Vertebral Column
 Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
JlntSocPlastination, Vol4:16-22,
 JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
JlntSocPlastination, Vol4:16-22, 1990 16 SECTIONAL ANATOMY: STANDARDIZED METHODOLOGY Alexander Lane, Coordinator of Anatomy and Physiology, Triton College, Visiting Associate Professor, University of Illinois
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach
 Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach Joseph Naiem.S Aziz 1 and Ahmed Khaled Al-Hrabi2 1 Deparment of Anatomy, Faculty
Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach Joseph Naiem.S Aziz 1 and Ahmed Khaled Al-Hrabi2 1 Deparment of Anatomy, Faculty
Skull-2. Norma Basalis Interna. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE
 Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
Superior View of the Skull (Norma Verticalis) Anteriorly the frontal bone articulates with the two parietal bones AT THE CORONAL SUTURE 1 The two parietal bones articulate in the midline AT THE SAGITTAL
You have 24 vertebrae in your spinal column. Two are special enough to be individually named.
 You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Brain Meninges, Ventricles and CSF
 Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Brain Meninges, Ventricles and CSF Lecture Objectives Describe the arrangement of the meninges and their relationship to brain and spinal cord. Explain the occurrence of epidural, subdural and subarachnoid
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
The Back. Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa
 The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal
 AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
Biology 218 Human Anatomy. Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division
 Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Main Menu. Trunk and Spinal Column click here. The Power is in Your Hands
 1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
The Neck. BY: Lina Abdullah & Rahaf Jreisat
 The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
The Neck BY: Lina Abdullah & Rahaf Jreisat Boundaries of the Neck: generally from base of the skull to root of the neck Superior margin :From superior nuchal line of occipital bone up to mastoid process
The far-lateral craniotomy: tips and tricks A craniotomia extremo-lateral: dicas e truques
 DOI: 10.1590/0004-282X20140130 ARTICLE The far-lateral craniotomy: tips and tricks A craniotomia extremo-lateral: dicas e truques Feres Chaddad-Neto 1,2,3, Hugo Leonardo Doria-Netto 2,3,4, José Maria de
DOI: 10.1590/0004-282X20140130 ARTICLE The far-lateral craniotomy: tips and tricks A craniotomia extremo-lateral: dicas e truques Feres Chaddad-Neto 1,2,3, Hugo Leonardo Doria-Netto 2,3,4, José Maria de
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR.
 The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
Anatomy and Physiology II. Review Spine and Neck
 Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Craniocervical Junction Venous Anatomy on Enhanced MR Images: The Suboccipital Cavernous Sinus
 AJNR Am J Neuroradiol 20:1127 1131, June/July 1999 Craniocervical Junction Venous Anatomy on Enhanced MR Images: The Suboccipital Cavernous Sinus Ronald D. Caruso, Arthur E. Rosenbaum, Ja Kwei Chang, and
AJNR Am J Neuroradiol 20:1127 1131, June/July 1999 Craniocervical Junction Venous Anatomy on Enhanced MR Images: The Suboccipital Cavernous Sinus Ronald D. Caruso, Arthur E. Rosenbaum, Ja Kwei Chang, and
The posterolateral thoracotomy is still probably the
 Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Posterolateral Thoracotomy Jean Deslauriers and Reza John Mehran The posterolateral thoracotomy is still probably the most commonly used incision in general thoracic surgery. It provides not only excellent
Anterior triangle of neck
 Anterior triangle of neck Dept. of Anatomy Zhou Hong Ying Outline boundary and subdivisions of ant. triangle contents of the triangle Muscles: suprahyoid muscles, infrahyoid muscles Nerves: CNⅩ, CNⅪ, CNⅫ,
Anterior triangle of neck Dept. of Anatomy Zhou Hong Ying Outline boundary and subdivisions of ant. triangle contents of the triangle Muscles: suprahyoid muscles, infrahyoid muscles Nerves: CNⅩ, CNⅪ, CNⅫ,
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Thyroidectomy. Siu Kwan Ng. Modified Radical Neck Dissection Type II 47
 06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
06 Thyroidectomy Siu Kwan Ng Modified Radical Neck Dissection Type II 47 Thyroidectomy STEP 1. EXPOSING THE THYROID GLAND The collar incision Figure 1 (curvilinear skin crease incision) is made at 1.5-2
5. COMMON APPROACHES. Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2.
 5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
5. COMMON APPROACHES Each of the described approaches is also demonstrated on supplementary videos, please see Appendix 2. 5.1. LATERAL SUPRAORBITAL APPROACH The most common craniotomy approach used in
STEP 1 INCISION AND ELEVATION OF SKIN FLAP STEP 3 SEPARATE PAROTID GLAND FROM SCM STEP 2 IDENTIFICATON OF GREAT AURICULAR NERVE
 STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
STEP 1 INCISION AND ELEVATION OF SKIN FLAP Create a modified Blair Figure 1 or facelift incision. Figure 2 Raise a superficial cervico-fascial flap between the Superficial Musculo Aponeurotic System (SMAS)
Alexander C Vlantis. Total Laryngectomy 57
 07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
07 Total Laryngectomy Alexander C Vlantis Total Laryngectomy 57 Total Laryngectomy STEP 1 INCISION AND POSITION OF STOMA A superiorly based apron flap incision is marked with the horizontal limb placed
Microsurgery for ruptured cerebellar arteriovenous malformations
 European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
European Review for Medical and Pharmacological Sciences Microsurgery for ruptured cerebellar arteriovenous malformations S.-F. GONG 1,2, X.-B. WANG 1,3, Y.-Q. LIAO 1,2, T.-P. JIANG 1,2, J.-B. HE 1,2,
THE SURGEON S LIBRARY
 THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
THE SURGEON S LIBRARY THE HISTORY AND SURGICAL ANATOMY OF THE VAGUS NERVE Lee J. Skandalakis, M.D., Chicago, Illinois, Stephen W. Gray, PH.D., and John E. Skandalakis, M.D., PH.D., F.A.C.S., Atlanta, Georgia
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Resection of malignant tumors invading the thoracic inlet
 Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
Resection of Superior Sulcus Tumors: Anterior Approach Marc de Perrot, MD, MSc Resection of malignant tumors invading the thoracic inlet represents a technical challenge because of the complex anatomy
ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 )
 2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
2 Neck Anatomy ANTERIOR CERVICAL TRIANGLE (Fig. 2.1 ) The boundaries are: Lateral: sternocleidomastoid muscle Superior: inferior border of the mandible Medial: anterior midline of the neck This large triangle
THE BACK THE SPINAL CORD
 THE BACK THE SPINAL CORD The structures in the vertebral canal: the spinal cord spinal nerve roots spinal meninges the neurovascular structures THE SPINAL CORD The spinal cord occupies the superior 2/3
THE BACK THE SPINAL CORD The structures in the vertebral canal: the spinal cord spinal nerve roots spinal meninges the neurovascular structures THE SPINAL CORD The spinal cord occupies the superior 2/3
Lecture 4 The BRAINSTEM Medulla Oblongata
 Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
Lecture 4 The BRAINSTEM Medulla Oblongata Introduction to brainstem 1- Medulla oblongata 2- Pons 3- Midbrain - - - occupies the posterior cranial fossa of the skull. connects the narrow spinal cord
SURGICAL AND APPLIED ANATOMY
 Página 1 de 6 Copyright 2001 Lippincott Williams & Wilkins Bucholz, Robert W., Heckman, James D. Rockwood & Green's Fractures in Adults, 5th Edition SURGICAL AND APPLIED ANATOMY Part of "37 - HIP DISLOCATIONS
Página 1 de 6 Copyright 2001 Lippincott Williams & Wilkins Bucholz, Robert W., Heckman, James D. Rockwood & Green's Fractures in Adults, 5th Edition SURGICAL AND APPLIED ANATOMY Part of "37 - HIP DISLOCATIONS
Dr. Weyrich G07: Superior and Posterior Mediastina. Reading: 1. Gray s Anatomy for Students, chapter 3
 Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
Dr. Weyrich G07: Superior and Posterior Mediastina Reading: 1. Gray s Anatomy for Students, chapter 3 Objectives: 1. Subdivisions of mediastinum 2. Structures in Superior mediastinum 3. Structures in Posterior
HEAD/NECK VESSELS. Objectives
 Objectives Arterial Supply to Head and Neck Arteries to Head Surrounding Brain Common carotid arteries Arteries to Head Surrounding Brain External carotid arteries Arteries to Head Surrounding Brain External
Objectives Arterial Supply to Head and Neck Arteries to Head Surrounding Brain Common carotid arteries Arteries to Head Surrounding Brain External carotid arteries Arteries to Head Surrounding Brain External
The SCALP. Prof. Dr. Muhammad Imran Qureshi
 The SCALP By Prof. Dr. Muhammad Imran Qureshi The SCALP includes FIVE layers external to the Calvaria. These are: S: Skin & Superficial Fascia C: Connective Tissue A: Aponeurosis (Epicranial) L: Loose
The SCALP By Prof. Dr. Muhammad Imran Qureshi The SCALP includes FIVE layers external to the Calvaria. These are: S: Skin & Superficial Fascia C: Connective Tissue A: Aponeurosis (Epicranial) L: Loose
Gross Anatomy Faculty: Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Melissa McGinn. Welcome to Gross and Developmental Anatomy
 Welcome to Gross and Developmental Anatomy M1 Anatomy Gross Anatomy Faculty: Dr. Richard Krieg Dr. Milton Sholley Dr. David Simpson 1 2 Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Steve Gudas Dr.
Welcome to Gross and Developmental Anatomy M1 Anatomy Gross Anatomy Faculty: Dr. Richard Krieg Dr. Milton Sholley Dr. David Simpson 1 2 Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Steve Gudas Dr.
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull
جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull
The Pharynx. Dr. Nabil Khouri MD. MSc, Ph.D
 The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
locomotice system Plastinated specimensⅠ: Silicone specimens Regional specimens and organs
 locomotice system Plastinated specimensⅠ: Silicone specimens Regional specimens and organs Art-No. Name Description The locomotor system SL001 Two hundred pieces of plastinated bones (without six The bones
locomotice system Plastinated specimensⅠ: Silicone specimens Regional specimens and organs Art-No. Name Description The locomotor system SL001 Two hundred pieces of plastinated bones (without six The bones
