Pancreatic injury remains uncommon and its management
|
|
|
- Marylou Daniels
- 6 years ago
- Views:
Transcription
1 The Journal of TRAUMA Injury, Infection, and Critical Care Predictors of Morbidity after Traumatic Pancreatic Injury Lillian S. Kao, MD, Eileen M. Bulger, MD, David L. Parks, Gregory F. Byrd, MD, and Gregory J. Jurkovich, MD Background: Although relatively uncommon, traumatic pancreatic injury is associated with significant morbidity and mortality. The objectives of this review were to validate the American Association for the Surgery of Trauma organ injury grading system for pancreatic injury by defining its relationship to subsequent morbidity and to characterize the independent predictors of postoperative Methods: We undertook a retrospective review of all patients with a pancreatic injury, confirmed by laparotomy, admitted to our Level I trauma center from 1986 and Pancreatic injury severity was assessed on the basis of the operative report. Outcome parameters included mortality, pancreatic complications (pancreatic fistula, pseudocyst, pancreatitis), intensive care unit (ICU) complications (acute respiratory distress syndrome, pneumonia, renal failure, multiple organ failure syndrome), abdominal complications (abscess, wound infection, ventral hernia, enteric fistula), and length of stay. Results: There were 193 patients identified. Mortality was 12%. Overall morbidity in the series was 50%, with a 22% prevalence of pancreas-related Multivariate analysis revealed that the grade of pancreatic injury was an independent predictor of both pancreatic complications (odds ratio, 4.4; 95% confidence interval, ) and mortality (odds ratio, 2.6; 95% confidence interval, ). Pancreatic and ICU complications were associated with longer ICU and hospital stays. Conclusion: The American Association for the Surgery of Trauma Organ Injury Score predicts the development of complications and mortality after pancreatic injury and identifies patients who will require extensive resources and may benefit from transfer to a Level I trauma center. Key Words: Pancreatic trauma, Abdominal trauma, Pancreatic fistula. J Trauma. 2003;55: Pancreatic injury remains uncommon and its management complex. Pancreatic trauma occurs in only 0.2% of blunt injuries and 1.1% of all patients with penetrating wounds. 1 Penetrating pancreatic injury is usually diagnosed at laparotomy and carries a high mortality because of associated injuries of neighboring major blood vessels. Blunt pancreatic injury is complicated by difficulty in establishing the diagnosis, which can lead to delay in diagnosis and increased morbidity. 2 Grading of pancreatic injury severity has been proposed to help with management and comparison of outcomes. 2,3 The pancreatic Organ Injury Score (OIS) of the American Association for the Surgery of Trauma (AAST) is listed in Table 1. 4 The major points of this grading system are the location of the injury (proximal vs. distal pancreas) and the status of the main pancreatic duct. Although this scoring system was developed by a committee of experts, it has not Submitted for publication October 28, Accepted for publication July 21, Copyright 2003 by Lippincott Williams & Wilkins, Inc. From the Department of Surgery, University of Texas Health Science Center at Houston (L.S.K.), Houston, Texas, University of Washington, Harborview Medical Center (E.M.B., G.J.J.), and University of Washington Medical Center (D.L.P., G.F.B.), Seattle, Washington. Poster presentation at the 61st Annual Meeting of the American Association for the Surgery of Trauma, September 26 28, 2002, Orlando, Florida. Address for reprints: Eileen M. Bulger, MD, Harborview Medical Center, 325 9th Avenue, Box , Seattle, WA 98104; ebulger@u.washington.edu. DOI: /01.TA C undergone formal validation. The purpose of this study was therefore to validate the AAST-OIS for the pancreas by defining its relationship to subsequent morbidity and mortality and to characterize the independent predictors of postoperative MATERIALS AND METHODS We undertook a retrospective review of all patients with a pancreatic injury, confirmed by laparotomy, admitted to our Level I trauma center from January 1985 to December Complete records were available for 193 patients. Medical records were reviewed and data collected using a standardized data abstraction form. Approval was obtained from the University of Washington Institutional Review Board for Human Subjects before data collection. Data collected included age, gender, mechanism of injury (blunt vs. penetrating), Injury Severity Score (ISS), abdominal Abbreviated Injury Severity Scale (AIS) score, presence of shock at admission, select laboratory and imaging studies, presence of concomitant bowel injury or other solid organ injury, AAST- OIS grade of pancreatic injury, operative management, length of stay, postoperative complications, and mortality. Patients with gunshot wounds underwent exploration in the operating room with few preoperative diagnostic studies. Patients with stab wounds underwent local wound exploration and, if fascial penetration was evident, diagnostic peritoneal lavage or computed tomographic (CT) scanning. Patients with blunt abdominal trauma were evaluated by diagnostic peritoneal lavage, ultrasound, or CT scanning de- 898 November 2003
2 Predictors of Morbidity after Traumatic Pancreatic Injury Table 1 Pancreatic Organ Injury Scale per the AAST a Grade Description I Hematoma Minor contusion without duct injury Laceration Superficial laceration without duct injury II Hematoma Major contusion without duct injury Laceration Major laceration without duct injury or tissue loss III Laceration Distal transection or parenchymal injury with duct injury IV Laceration Proximal b transection or parenchymal injury involving ampulla V Laceration Massive disruption of pancreatic head a Data from Moore et al., b Proximal pancreas is to the patients right of the superior mesenteric vein. * Advance one grade for multiple injuries to the same organ. Based on most accurate assessment at autopsy, laparotomy, or radiologic study. pending on their hemodynamic stability and level of suspicion for intra-abdominal injury. A delay in diagnosis was defined as a time interval greater than 24 hours between injury and diagnosis. Pancreatic injuries were graded according to the pancreatic injury severity score as defined by the AAST 4 (Table 1). This was done retrospectively, on the basis of review of the operative note. For the purpose of data analysis, postoperative morbidity was divided into three groups: pancreatic complications, nonpancreatic abdominal complications, and intensive care unit (ICU) Pancreatic complications included pancreatic fistula, pseudocyst, and pancreatitis. A pancreatic fistula was defined as persistent drainage of amylase-rich fluid for greater than 14 days. A pseudocyst was defined as an encapsulated peripancreatic fluid collection, and was diagnosed by CT scan. Pancreatitis was defined as persistent inflammation of the pancreas manifested by continued hyperamylasemia (amylase 100 IU) and abdominal pain. Abdominal complications included intra-abdominal abscesses, enterocutaneous fistulas, wound infections, and ventral hernias. An intra-abdominal abscess was defined as a purulent fluid collection requiring percutaneous or operative drainage. Wound infections were characterized by erythema or drainage requiring that the wound be opened and drained. ICU complications included the acute respiratory distress syndrome (ARDS), renal failure, pneumonia, and multiple organ failure syndrome (MOFS). ARDS was defined by the definition as developed by the American-European Consensus Conference as follows: PaO 2 /FIO 2 ratio less than 200, bilateral opacities on chest radiograph, and pulmonary capillary wedge pressure less than or equal to 18 or no clinical evidence of cardiogenic pulmonary edema. 5 Pneumonia was diagnosed by the presence of an infiltrate on chest radiography or purulent sputum in combination with a fever greater than 38.5 C or leukocytosis and treatment with antibiotics. Renal failure was defined by the need for dialysis. MOFS was defined as the failure of more than one organ system during the ICU course. The data were analyzed using Stata, a statistical software program. Univariate statistical analysis of discrete variables was performed using 2 analysis and continuous variables were analyzed using Student s t test. Logistic regression was used for categorical values and linear regression for continuous variables. Independent predictors of morbidity and mortality were determined by stepwise logistic regression. Significance was defined as a value of p RESULTS Demographics Over this 14-year period, a total of 49,054 trauma patients were admitted, with 193 having laparotomy-documented pancreatic injury (0.004%). The mean age of the population was 29.8 years and ranged from 1 to 88 years old. The group of patients included 69% male and 31% female patients. The mechanism of injury was blunt in 61% of patients and penetrating in 39%. Blunt abdominal injury was primarily caused by motor vehicle collisions (68%). Penetrating injuries included gunshot (62%) and stab wounds (38%). Other mechanisms of injury are listed in Table 2. The mean ISS was (range, 4 59) and the mean AIS score for the abdomen was (range, 2 5). At admission, 34 patients (18%) were in shock, defined as a systolic blood pressure less than 90 mm Hg. The pancreatic injuries were graded according to the AAST-OIS for the pancreas. The majority of the patients (47%) had grade I injuries. There was no statistical difference Table 2 Mechanism of Injury Mechanism of Injury Total Patients % Blunt Motor vehicle collision Motorcycle collision 8 4 Pedestrian vs. vehicle 7 4 Fall 7 4 Crush injury 7 4 Assault 4 2 Bicycle collision 2 1 Injury by animal (horse, bull) 2 1 Penetrating Gunshot wound Stab wound Volume 55 Number 5 899
3 The Journal of TRAUMA Injury, Infection, and Critical Care Table 3 Stratification of Patients by Grade Grade I Grade II Grade III Grade IV Grade V No % of total Age (yr) ISS AIS abdomen Mortality Pancreatic morbidity in age, ISS, or abdominal AIS score between patients with different grades of injury (Table 3). Operative Management The operative procedure correlated with the grade of the injury. See Table 4 for the operations performed. The majority of patients with a grade I or II injury, in which by definition the pancreatic duct is intact, underwent exploration alone or with drainage. Distal pancreatectomy was performed primarily in patients with grade III or IV injuries, although in a few cases of grade II injuries, the surgeon could not convincingly exclude a ductal injury. Grade IV injuries were not treated in any one consistent manner, although all patients who survived greater than 48 hours with a grade V injury by necessity underwent a pancreaticoduodenectomy. Evaluation of the Main Pancreatic Duct Intraoperative assessment of the pancreatic duct was performed in 19 patients using cholecystography with retrograde filling of the pancreatic duct (n 11), duodenotomy with cannulation of the ampulla of Vater (n 7), and intraoperative endoscopic retrograde pancreatography (ERCP) (n 1). Intraoperative imaging of the pancreatic duct was successful in 15 (79%) of the patients. Two patients had main pancreatic ductal disruptions, 2 patients had extravasation from a tertiary pancreatic radical with an intact main duct, and the remaining 11 patients had no evidence of a ductal injury. The two patients with main ductal disruptions underwent distal resections at the demonstrated site of injury, and the two patients with extravasation from tertiary radicals underwent drainage alone. Both of the patients who underwent resection, as did both of the patients with leakage from radicals, developed postoperative pancreatic fistulas. Of the remaining patients, none developed a fistula, but one patient did develop postoperative pancreatitis. Postoperative ERCP was attempted in eight cases and was successful in seven instances. Three of the patients underwent immediate postoperative ERCP within 24 hours of the initial laparotomy, in an attempt to clarify the status of the duct. In one of the three immediately attempted ERCPs, the patient had a ductal transection that prompted return to the operating room for definitive management. The second patient had a normal duct and the third patient had an unsuccessful ERCP. The five remaining patients underwent delayed postoperative ERCPs for persistent pancreatic fistulae (four of five) and hyperbilirubinemia (one of five). In three of the four cases performed for fistulae, the pancreatograms were normal without evidence of main duct injury or stricture. In the fourth patient, a pancreatic ampullary stent was placed. The patient with hyperbilirubinemia had a normal ERCP. Management was therefore altered in two of eight (25%) patients total on the basis of postoperative ERCP. Overall, pancreatography was attempted in 27 patients, and the status of the pancreatic duct was successfully determined in 22 patients (81%). Morbidity Overall, 50% of patients had one or more postoperative The complications were subdivided into pancreatic, nonpancreatic abdominal, and ICU-related Pancreatic Complications The pancreas-related morbidity of the series was 21.8% (42 of 193). These complications included pancreatic fistula (n 42 [22%]), pancreatitis (n 19 [10%]), and pseudocyst (n 5 [3%]). Pancreatic fistulae were managed by drainage, usually with intraoperatively placed drains. Octreotide was used in the management of 16 of the 42 patients with pancreatic fistulae. In 98% of the patients, the fistulae resolved without further intervention. One patient underwent postoperative ERCP with stenting of the pancreatic duct. None of the patients with pseudocysts required operative drainage, and all of the patients with traumatic pancreatitis had mild, self-limiting courses. The length of intensive care unit stay was significantly longer in patients with a pancreatic complication than in those Table 4 Operative Management by Grade of Injury in Patients Surviving > 48 H Grade I Grade II Grade III Grade IV Grade V No Exploration only (%) Drainage (%) Distal pancreatectomy (%) Resection plus internal drainage (%) Pyloric exclusion (%) Whipple (%) November 2003
4 Predictors of Morbidity after Traumatic Pancreatic Injury Table 5 Operative Management of Patients Surviving < 48 H Grade of Pancreatic Injury Associated Injuries Operations I Liver, hepatic vein, splenic vessels, renal vein injuries Exploratory laparotomy, pericardial window I Liver and splenic injuries Exploratory laparotomy, splenectomy, hepatorrhaphy I Liver laceration, splenic injury, small and large bowel injuries Exploratory laparotomy 2, damage control, bowel resection, drainage of the pancreas I Liver and splenic injuries, IVC injury Exploratory laparotomy, thoracotomy I Liver injury involving porta hepatis Exploratory laparotomy, pericardial window II SMA/SMV injury Exploratory laparotomy, left thoracotomy II IVC injury Exploratory laparotomy III Splenic injury, retroperitoneal hematoma Exploratory laparotomy, left thoracotomy III Splenic and liver injury, subdural hematoma Exploratory laparotomy, pericardial window, distal pancreatectomy and splenectomy, craniotomy, thoracotomy III Liver and splenic injuries, pelvic fracture Exploratory laparotomy, left thoracotomy III Liver and splenic injuries Exploratory laparotomy, distal pancreatectomy and splenectomy, liver packs III Diaphragmatic rupture, kidney and stomach injuries, thoracic aortic injury Exploratory laparotomy, distal pancreatectomy and splenectomy, nephrectomy, repair gastrotomy, bilateral thoracotomies III Liver and splenic injuries, SMV injury Exploratory laparotomy 2, damage control packed injuries, repair of SMV III Liver injury, IVC and portal vein injury Exploratory laparotomy, pericardial window III Aortic injury Exploratory laparotomy, distal pancreatectomy and splenectomy, thoracotomy IV Liver injury, IVC injury Exploratory laparotomy, thoracotomy V IVC injury Exploratory laparotomy IVC, inferior vena cava; SMA, superior mesenteric artery; SMV, superior mesenteric vein. without (13 23 days vs days, p 0.01). The total hospital stay was also significantly longer in patients with a pancreatic complication (36 39 days vs days, p 0.001). Patients with a pancreatic complication required an increased number of subsequent operations as well ( vs , p 0.001). The independent predictors of pancreatic complications included grade of injury (odds ratio [OR], 4.4; 95% confidence interval [CI], ) and the presence of an associated bowel injury (OR, 2.4; 95% CI, 1.1 5). Age, presence of an associated solid organ injury, shock at admission, and ISS were not predictive of the development of pancreatic Abdominal Complications Forty patients (21%) developed at least one abdominal complication. These included intra-abdominal abscesses (n 34 [17.6%]), enterocutaneous fistulas (n 11 [5.7%]), wound infections (n 20 [10.3%]), and ventral hernias (n 9 [4.7%]). The independent predictors of an abdominal complication were grade of injury (OR, 3.2; 95% CI, ; p 0.003) and the presence of a pancreatic complication (OR, 14; 95% CI, ; p 0.001). ICU Complications The ICU-related morbidity of the series was 33% (64 of 193) and included pneumonia (n 64 [33%]), ARDS (n 35 [18%]), MOFS (n 23 [12%]), and renal failure (n 8 [4%]). The independent predictors of ICU complications included age 55 (OR, 20; 95% CI, ), ISS (OR per category, 2.0; 95% CI, ), and the presence of a pancreatic complication (OR, 2.9; 95% CI, ). Mortality There were 24 deaths, for an overall mortality of 12.4%. Eighteen (75%) of the deaths occurred within the first 48 hours of admission (Table 5). In all of the cases, the pancreatic injury was not the cause of death; rather, associated solid organ or vascular injuries were primarily responsible. When the patient did not immediately exsanguinate, drainage was Volume 55 Number 5 901
5 The Journal of TRAUMA Injury, Infection, and Critical Care Fig. 1. Relationship of grade to mortality. performed for grade I or II injuries and distal pancreatectomy with splenectomy was performed for grade III injuries. Six deaths occurred after 48 hours of admission and were secondary to sepsis, ARDS, MOFS, or severe neurologic injury. Only one of the patients with a late death had a pancreatic complication. Mortality was dependent on grade of pancreatic injury (OR, 2.6; 95% CI, ), age (OR, 11.9; 95% CI, ), ISS (OR, 2.5; 95% CI, ), and shock at admission (OR, 1.8; 95% CI, ). Relationship between Grade of Injury and Outcome Mortality for injuries without disruption of the main pancreatic duct (grades I and II) was 7% versus 29% for more severe injuries (grades III, IV, and V; p 0.005) (Fig. 1). In addition, postoperative morbidity increased with increasing grade of injury (Fig. 2). As illustrated, the rate of ICU and abdominal complications increased with each successive grade of injury; however, the rate of pancreatic complication was highest for patients with grade III injuries (62%). This was most likely because of a high rate of pancreatic fistula formation for patients undergoing distal pancreatectomy (39%). Fig. 2. Relationship of grade to pancreatic and abdominal The Relationship between Delay in Diagnosis and Outcome Seventeen patients had a delay in diagnosis, defined as recognition and treatment of a pancreatic injury more than 24 hours after the traumatic event. Fifteen (13%) of the 117 patients who sustained blunt abdominal trauma had a delay in diagnosis. The other two patients presented to the hospital late after stab wounds. Overall, the rate of pancreatic complications was higher in the blunt trauma patients with a delayed diagnosis (6 of 15 [40%]) when compared with those patients diagnosed within 24 hours (18 of 102 [18%]). ICU complications occurred in 38 of 102 (37%) patients without a delay in diagnosis compared with 6 of 15 (40%) patients with a delayed diagnosis. Only one patient with a delay in diagnosis died. The majority of the pancreatic injuries in this subpopulation (12 of 17 [71%]) were grade I or II. Of the five patients with grade III or IV injuries, four patients survived greater than 48 hours. Two of the four patients (50%) developed a complication, and two patients (50%) developed an ICU complication. As a comparison, 14 patients who had a grade III or higher pancreatic injury from blunt abdominal trauma, without a delay in diagnosis, survived greater than 48 hours. Five patients (36%) developed a pancreatic complication and five patients (36%) developed an ICU complication. Among the initial survivors, the average length of stay for patients with a grade III or higher injury with a delay in diagnosis was days compared with days for patients without a delay in diagnosis. Likewise, the length of ICU stay was longer in cases with a delay (18 26 days vs. 7 5 days) for these patients. DISCUSSION These data support the use of the AAST-OIS for the pancreas in defining a population of patients likely to have a complicated postoperative course. Furthermore, they emphasize the importance of determining the status of the main pancreatic duct in defining the injury grade. Previous authors have documented a correlation between ductal status and outcome using a scoring system similar to the AAST-OIS system. 6 Smego et al. 6 demonstrated a correlation between grade of pancreatic injury and outcome using this scale. Patients with duct transection and proximal crush injuries who were managed with resection had increased morbidity as opposed to the less severely injured patients who were managed with drainage alone. These authors concluded that ductal status is an important predictor of outcome in pancreatic trauma and is essential for establishing the basis for treatment decisions. Bradley et al. 2 similarly reported a significant association between a main pancreatic duct injury and an increased incidence of pancreas-related complications (p 0.040), and in particular, an increased incidence of pancreatic fistula (p 0.018). The AAST-OIS for the pancreas does take into account the status of the main pancreatic duct and the location of the 902 November 2003
6 Predictors of Morbidity after Traumatic Pancreatic Injury pancreatic injury. Pancreas-related complications are reported to occur in 11% to 62% of patients after traumatic pancreatic injury, with an average morbidity rate of 36.6%. 3 The most commonly reported complications are pseudocysts, pancreatitis, pancreatic fistula, and abscess. Our series demonstrated comparable figures, with 22% of patients having had at least one pancreas-related complication (pseudocyst, fistula, and pancreatitis). The rate increased to 30% if patients with intra-abdominal abscesses were included as well. The prevalences of the individual complications were also comparable to those described by other authors: 22% pancreatic fistulas (7 15% 1,3,7 9 ), 18% intra-abdominal abscesses (8 25% 1 ), 9.8% pancreatitis (7 14% 1,8 ), and 2.5% pseudocysts (2 3% 8,10 ). The most common pancreatic complication, both in this series and in the literature, is a pancreatic fistula. Although there appears to be a consensus regarding the significant contribution of a main pancreatic ductal injury to the development of a pancreatic fistula, the literature is controversial regarding the extent of perioperative assessment required to determine the presence of such an injury. Several authors advocate intraoperative assessment alone for the determination of operative strategy. 8,9 Opponents of this approach argue that the addition of pancreatography or intraoperative ERCP adds operative time, increases operative risk, and does not contribute significantly to the management algorithm. In a study by Patton et al., 9 patients were categorized as having either a proximal injury (to the right of the mesenteric vessels) that was managed with closed suction drainage alone or a distal injury that was managed with either drainage alone or resection and drainage, the decision made on the basis of the surgeon s assessment of probability of a ductal injury. They noted no difference in overall morbidity in patients with an indeterminate injury who were managed with drainage alone versus those managed with distal resection (27 vs. 33%, p 0.60) and concluded that the high morbidity was associated with the severity of the underlying pancreatic injury rather than the management strategy. 9 They further argued that assessment of the ductal status intraoperatively (other than direct inspection) was not indicated, as the information gained would not alter the choice of operative procedure. However, because the status of the duct was never directly determined in those patients in whom drainage alone was used, these conclusions remain as opinion. Other authors argue that intraoperative inspection alone is inadequate and that determination of the ductal status changes management. Berni et al. 11 reported a 40% decrease in major pancreatic complications, from 55% to 15% after institution of intraoperative pancreatography. Furthermore, other studies have suggested that resection versus drainage are not equivalent treatment options for patients with a distal pancreatic ductal injury, 7,12 reporting lower morbidity and mortality associated with resection rather than drainage. In our series, three of four (75%) patients with a grade III injury treated with drainage alone developed pancreatic fistulas versus 13 of 42 (31%) patients treated with resection. Although the data are limited, the higher rate of pancreatic fistulas with drainage alone suggests that these patients probably should have undergone distal resection for management of the suspected ductal injury. Intraoperative pancreatography was used selectively in this series (19 of 193), and was successful in demonstrating the main pancreatic duct in 15 of 19 (78%). Two of the patients had a change in operative strategy dictated by the demonstration of a main ductal injury, namely, they underwent distal pancreatic resection. Although limited, these data suggest intraoperative imaging of the pancreatic duct is successful the majority of the time, and if an unsuspected pancreatic duct injury is found, distal resection should be used. However, because these numbers are small, further prospective studies are required to confirm the role of intraoperative imaging of the pancreatic duct in assessing the injury grade and guiding management. This study does demonstrate that grade of injury is predictive of a pancreatic complication (OR, 4.4; 95% CI, ). Grade III injuries were associated with the highest pancreatic morbidity (Fig. 1), because of the high rate of pancreatic fistulas. In this series, 32 patients were determined retrospectively to have a grade III injury. Four of these patients underwent drainage alone and three (75%) developed a fistula. Twenty-six patients with grade III injuries underwent distal pancreatectomy with or without splenectomy, and 12 (43%) developed a pancreatic fistula. This leak rate is significantly higher than the 14% to 26% rate reported in recent studies of complications after distal pancreatectomy for all indications. 13,14 The reason for the increased rate observed in our patients is unclear but may be related to the definition of a fistula. A pancreatic fistula has been variably defined, ranging from drainage of more than 50 ml/day of fluid with elevated amylase level for at least 3 consecutive days 15 to drainage of fluid high in amylase from trans-abdominal drains for greater than 10 days. 1 For the purposes of this study, a pancreatic fistula was defined as drainage of amylase-rich fluid for greater than 14 days. The lack of a standardized definition may contribute to differences in reported rates of fistulas; nonetheless, the prevalence was still high in our series. Method of stump closure and underlying pathophysiology have been proposed as contributing to the development of a pancreatic fistula after distal resection. However, the data are conflicting. Fahy et al. 13 found that pancreatic leaks occurred more frequently in patients who underwent distal pancreatectomy for trauma and who underwent sutured pancreatic stump closure. However, Sheehan et al. 14 found that neither the underlying pathologic process nor the method of stump closure affected the rate of fistula formation. In our series, complete data are not available regarding method of stump closure, so no definitive conclusion could be made. This study demonstrated that the presence of a pancreatic complication is a risk factor for an ICU complication (OR, 2.9; 95% CI, ). Figure 3 demonstrates that the prev- Volume 55 Number 5 903
7 The Journal of TRAUMA Injury, Infection, and Critical Care Fig. 3. Relationship of grade to ICU alence of ICU complications rises with increasing grade of pancreatic injury. Furthermore, the presence of a pancreatic complication was associated with a significantly longer ICU stay (13 23 days vs days, p 0.01), as was the presence of an ICU complication (19 21 days vs days, p 0.001). Overall length of hospital stay was also increased in patients with a pancreatic complication (36 39 days vs days, p 0.001) and an ICU complication (39 38 days vs days, p 0.001). Therefore, grade of injury not only is predictive of pancreatic and ICU complications but is associated with an increased use of hospital resources, as demonstrated by a greater need for higher level care and a longer ICU and hospital stay. A delay in diagnosis of pancreatic injury has been demonstrated to increase pancreas-related morbidity and mortality Delays in diagnosis are more common in blunt abdominal trauma, given that most patients with penetrating injuries undergo exploratory laparotomy for associated injuries. Given the retroperitoneal location of the pancreas, diagnosis of a pancreatic injury can be difficult. Symptoms may be minimal, laboratory tests such as serum amylase are not reliable, 19,20 and CT scan findings may underestimate the severity of the injury, especially in the first 24 hours after trauma. 21,22 In our series, 17 patients had a delay in diagnosis of a pancreatic injury of greater than 24 hours. A delay in diagnosis was associated with increased pancreas-related morbidity. ICU morbidity was similar overall but increased in patients with more severe injuries. In addition, patients diagnosed late had an increased ICU and hospital stay. The overall mortality of this series was 12.4%, which is comparable to the 19.1% mortality reported by Asensio et al. 3 The literature suggests that the cause of mortality differs depending on the temporal relationship to the trauma. Early deaths in patients with pancreatic injury are typically secondary to exsanguination. 23,24 Similarly, in our series, 75% of deaths occurred in the first 48 hours after admission, because of massive hemorrhage and subsequent cardiac arrest. Late deaths are usually related to associated injuries rather than the pancreatic injury itself. 3,25 In our series, only one late death had a pancreatic complication that contributed to his mortality. Therefore, pancreatic complications did not appear to predict late mortality. Although pancreatic complications were not significantly associated with mortality, grade of injury was predictive of mortality in our series. Previous studies have attempted to validate the AAST-OIS as a predictor of mortality. Cogbill et al. 15 performed a multi-institutional study that failed to demonstrate a conclusive relationship because of a small number of patients and inadequate representation in each category of injury grade. Another study by Glancy 25 demonstrated a correlation between operative procedure and mortality. The lowest mortality of 10.9% was associated with drainage alone and the highest mortality of 100% was associated with total pancreatectomy. Because the more complex surgical procedures are typically associated with the higher grade injuries, these results are suggestive of a correlation between grade and mortality. The current series demonstrates a statistically significant correlation between grade of injury and mortality. Grade I and II injuries had a 7% mortality, whereas grades III and IV were associated with 29% mortality. Grade of injury was a predictor of mortality, with an odds ratio of 2.6. Thus, this study validates that grade of pancreatic injury is a predictor of mortality. In conclusion, the status of the main pancreatic duct and location of the pancreatic injury constitute the basis for the AAST scoring system. This scale should be used as a guide to operative strategy and as a predictor of patient outcome. This study validates the AAST scale as correlating to both pancreatic complications and mortality. Therefore, this scoring system should be used to identify patients who may have a prolonged hospital stay and higher morbidity such that early transfer to a specialized trauma center may be indicated. REFERENCES 1. Akhrass R, Yaffe MB, Brandt CP, Reigle M, Fallon WF Jr, Malangoni MA. Pancreatic trauma: a ten-year multi-institutional experience. Am Surg. 1997;63: Bradley EL III, Young PR Jr, Chang MC, et al. Diagnosis and initial management of blunt pancreatic trauma: guidelines from a multiinstitutional review. Ann Surg. 1998;227: Asensio JA, Demetriades D, Hanpeter DE, Gambaro E, Chahwan S. Management of pancreatic injuries. Curr Probl Surg. 1999; 36: Moore E, Cogbill T, Malangoni M, et al. Organ injury scaling, II: pancreas, duodenum, small bowel, colon, and rectum. J Trauma. 1990;30: Bernard GR, Artigas A, Brigham KL, et al. The American-European Consensus Conference on ARDS: definitions, mechanisms, relevant outcomes, and clinical trial coordination. Am J Respir Crit Care Med. 1994;149: Smego DR, Richardson JD, Flint LM. Determinants of outcome in pancreatic trauma. J Trauma. 1985;25: Young PR Jr, Meredith JW, Baker CC, Thomason MH, Chang MC. Pancreatic injuries resulting from penetrating trauma: a multiinstitution review. Am Surg. 1998;64: Heitsch R, Knutson C, Fulton R, Jones C. Delineation of critical factors in the treatment of pancreatic trauma. J Trauma. 1976; 80: Patton JH Jr, Lyden SP, Croce MA, et al. Pancreatic trauma: a simplified management guideline. J Trauma. 1997;43: November 2003
8 Predictors of Morbidity after Traumatic Pancreatic Injury 10. Wilson RH, Moorehead RJ. Current management of trauma to the pancreas. Br J Surg. 1991;78: Berni GA, Bandyk DF, Oreskovich MR, Carrico CJ. Role of intraoperative pancreatography in patients with injury to the pancreas. Am J Surg. 1982;143: Heitsch RC, Knutson CO, Fulton RL, Jones CE. Delineation of critical factors in the treatment of pancreatic trauma. Surgery. 1976; 80: Fahy BN, Frey CF, Ho HS, Beckett L, Bold RJ. Morbidity, mortality, and technical factors of distal pancreatectomy. Am J Surg. 2002;183: Sheehan MK, Beck K, Creech S, Pickleman J, Aranha GV. Distal pancreatectomy: does the method of closure influence fistula formation? Am Surg. 2002;68: Cogbill TH, Moore EE, Morris JA Jr, et al. Distal pancreatectomy for trauma: a multicenter experience. J Trauma. 1991;31: Bach RD, Frey CF. Diagnosis and treatment of pancreatic trauma. Am J Surg. 1971;121: Wisner D, Wold R, Frey C. Diagnosis and treatment of pancreatic injuries. Arch Surg. 1990;125: Leppaniemi A, Haapiainen R, Kiviluoto T, Lempinen M. Pancreatic trauma: acute and late manifestations. Br J Surg. 1988; 75: Buechter KJ, Arnold M, Steele B, et al. The use of serum amylase and lipase in evaluating and managing blunt abdominal trauma. Am Surg. 1990;56: Takishima T, Sugimoto K, Hirata M, Asari Y, Ohwada T, Kakita A. Serum amylase level on admission in the diagnosis of blunt injury to the pancreas: its significance and limitations. Ann Surg. 1997; 226: Jeffrey RB Jr, Federle MP, Crass RA. Computed tomography of pancreatic trauma. Radiology. 1983;147: Dodds WJ, Taylor AJ, Erickson SJ, Lawson TL. Traumatic fracture of the pancreas: CT characteristics. J Comput Assist Tomogr. 1990; 14: Jones RC. Management of pancreatic trauma. Ann Surg. 1978; 187: Graham JM, Mattox KL, Jordan GL Jr. Traumatic injuries of the pancreas. Am J Surg. 1978;136: Glancy KE. Review of pancreatic trauma. West J Med. 1989;151: Volume 55 Number 5 905
Management of Blunt Pancreatic Trauma in Children
 Surg Today (2009) 39:115 119 DOI 10.1007/s00595-008-3823-6 Management of Blunt Pancreatic Trauma in Children IVO JURIĆ, ZENON POGORELIĆ, MIHOVIL BIOČIĆ, DAVOR TODORIĆ, DUBRAVKO FURLAN, and TOMISLAV ŠUŠNJAR
Surg Today (2009) 39:115 119 DOI 10.1007/s00595-008-3823-6 Management of Blunt Pancreatic Trauma in Children IVO JURIĆ, ZENON POGORELIĆ, MIHOVIL BIOČIĆ, DAVOR TODORIĆ, DUBRAVKO FURLAN, and TOMISLAV ŠUŠNJAR
Penetrating abdominal trauma clinical view. Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland
 Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Surgical management of pancreatic trauma: a retrospective case series.
 Research Article http://www.alliedacademies.org/trauma-and-critical-care/ Surgical management of pancreatic trauma: a retrospective case series. Hamdy S Abdallah*, Sherif A Saber Gastrointestinal Surgery
Research Article http://www.alliedacademies.org/trauma-and-critical-care/ Surgical management of pancreatic trauma: a retrospective case series. Hamdy S Abdallah*, Sherif A Saber Gastrointestinal Surgery
Complex pancreatico- duodenal injuries. Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University
 Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
Complex pancreatico- duodenal injuries Elmin Steyn Head, Division of Surgery Faculty of Health Sciences Stellenbosch University Pancreatic and duodenal trauma: daunting or simply confusing? 2-4% of abdominal
IMAGING OF BLUNT ABDOMINAL TRAUMA, PART I
 IMAGING OF BLUNT ABDOMINAL TRAUMA, PART I QuickTime and a TIFF (Uncompressed) decompressor are needed to see this picture. Ruedi F. Thoeni, M. D. D University of California, San Francisco SCBT-MR Summer
IMAGING OF BLUNT ABDOMINAL TRAUMA, PART I QuickTime and a TIFF (Uncompressed) decompressor are needed to see this picture. Ruedi F. Thoeni, M. D. D University of California, San Francisco SCBT-MR Summer
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Multilevel Duodenal Injury after Blunt Trauma
 J Korean Surg Soc 2009;77:282-286 DOI: 10.4174/jkss.2009.77.4.282 증 례 Multilevel Duodenal Injury after Blunt Trauma Department of Surgery, College of Medicine, Hallym University, Chuncheon, Korea Jeong
J Korean Surg Soc 2009;77:282-286 DOI: 10.4174/jkss.2009.77.4.282 증 례 Multilevel Duodenal Injury after Blunt Trauma Department of Surgery, College of Medicine, Hallym University, Chuncheon, Korea Jeong
Management of blunt pancreatic trauma: what s new?
 Eur J Trauma Emerg Surg (2015) 41:239 250 DOI 10.1007/s00068-015-0510-3 REVIEW ARTICLE Management of blunt pancreatic trauma: what s new? D. A. Potoka 1 B. A. Gaines 1 A. Leppäniemi 3 A. B. Peitzman 1,2
Eur J Trauma Emerg Surg (2015) 41:239 250 DOI 10.1007/s00068-015-0510-3 REVIEW ARTICLE Management of blunt pancreatic trauma: what s new? D. A. Potoka 1 B. A. Gaines 1 A. Leppäniemi 3 A. B. Peitzman 1,2
Which Blunt Trauma Patients Should Be Studied by Abdominal CT?
 MDCT of Bowel and Mesenteric Injury: How Findings Influence Management 4 th Nordic Trauma Radiology Course 2006 4 th Nordic Trauma Radiology Course 2006 Stuart E. Mirvis, M.D., FACR Department of Radiology
MDCT of Bowel and Mesenteric Injury: How Findings Influence Management 4 th Nordic Trauma Radiology Course 2006 4 th Nordic Trauma Radiology Course 2006 Stuart E. Mirvis, M.D., FACR Department of Radiology
Traumatic pancreatic injury - an elusive diagnosis: experience from a developing country urban trauma referral centre
 440 ORIGINAL ARTICLE Traumatic pancreatic injury - an elusive diagnosis: experience from a developing country urban trauma referral centre Ayaz Ahmed Memon, Hasnain Zafar, Rushna Raza, Ghulam Murtaza Abstract
440 ORIGINAL ARTICLE Traumatic pancreatic injury - an elusive diagnosis: experience from a developing country urban trauma referral centre Ayaz Ahmed Memon, Hasnain Zafar, Rushna Raza, Ghulam Murtaza Abstract
Laparotomy for Abdominal Injury in Traffic Accidents
 Qasim O. Al-Qasabi, FRCS; Mohammed K. Alam, MS, FRCS (Ed); Arun K. Tyagi, FRCS; Abdulla Al-Kraida, FRCS; Mohammed I. Al-Sebayel, FRCS From the Departments of Surgery, Riyadh Central Hospital (Drs. Al-Qasabi,
Qasim O. Al-Qasabi, FRCS; Mohammed K. Alam, MS, FRCS (Ed); Arun K. Tyagi, FRCS; Abdulla Al-Kraida, FRCS; Mohammed I. Al-Sebayel, FRCS From the Departments of Surgery, Riyadh Central Hospital (Drs. Al-Qasabi,
Epidural analgesia improves outcome after multiple rib fractures
 Epidural analgesia improves outcome after multiple rib fractures Eileen M. Bulger, MD, Thomas Edwards, PhD, MD, Patricia Klotz, RN, and Gregory J. Jurkovich, MD, Seattle, Wash Background. Rib fractures
Epidural analgesia improves outcome after multiple rib fractures Eileen M. Bulger, MD, Thomas Edwards, PhD, MD, Patricia Klotz, RN, and Gregory J. Jurkovich, MD, Seattle, Wash Background. Rib fractures
A prospective evaluation of the predictive value of serum amylase levels in the assessment of patients with blunt abdominal trauma
 A prospective evaluation of the predictive value of serum amylase levels in the assessment of patients with blunt abdominal trauma I E Donkin, R Jones, C Aldous, D L Clarke Department of General Surgery,
A prospective evaluation of the predictive value of serum amylase levels in the assessment of patients with blunt abdominal trauma I E Donkin, R Jones, C Aldous, D L Clarke Department of General Surgery,
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
LIVER INJURIES PROFF. S.FLORET
 LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
Cover Page. The handle holds various files of this Leiden University dissertation
 Cover Page The handle http://hdl.handle.net/1887/22997 holds various files of this Leiden University dissertation Author: Wilden, Gwendolyn M. van der Title: The value of surgical treatment in abdominal
Cover Page The handle http://hdl.handle.net/1887/22997 holds various files of this Leiden University dissertation Author: Wilden, Gwendolyn M. van der Title: The value of surgical treatment in abdominal
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Safety of Repair for Severe Duodenal Injuries
 World J Surg (2008) 32:7 12 DOI 10.1007/s00268-007-9255-4 Safety of Repair for Severe Duodenal Injuries George C. Velmahos Æ Constantinos Constantinou Æ George Kasotakis Published online: 22 October 2007
World J Surg (2008) 32:7 12 DOI 10.1007/s00268-007-9255-4 Safety of Repair for Severe Duodenal Injuries George C. Velmahos Æ Constantinos Constantinou Æ George Kasotakis Published online: 22 October 2007
Management of Pancreatic Fistulae
 Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Management of Pancreatic Fistulae Jose Ramos University of the Witwatersrand Donald Gordon Medical Centre Fistula definition A Fistula is a permanent abnormal passageway between two organs (epithelial
Diagnosis & Management of Kidney Trauma. LAU - Urology Residency Program LOP Urology Residents Meeting
 Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
ORIGINAL ARTICLE. Complications Following Renal Trauma
 ORIGINAL ARTICLE Complications Following Renal Trauma Margaret Starnes, MD; Demetrios Demetriades, MD, PhD; Pantelis Hadjizacharia, MD; Kenji Inaba, MD; Charles Best, MD; Linda Chan, PhD Objectives: To
ORIGINAL ARTICLE Complications Following Renal Trauma Margaret Starnes, MD; Demetrios Demetriades, MD, PhD; Pantelis Hadjizacharia, MD; Kenji Inaba, MD; Charles Best, MD; Linda Chan, PhD Objectives: To
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE
 PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
PENETRATING COLON TRAUMA: THE CURRENT EVIDENCE Samuel Hawkins MD CASE PRESENTATION 22M BIBEMS s/p multiple GSW ABCs intact Normotensive, non-tachycardic Secondary Survey: 4 truncal bullet holes L superior
Surgical Management of Modern Combat-Related Pancreatic Injuries: Traditional Management and Unique Strategies
 MILITARY MEDICINE, 179, 3:315, 2014 Surgical Management of Modern Combat-Related Pancreatic Injuries: Traditional Management and Unique Strategies MAJ Amy Vertrees, MC USA* ; CAPT Eric Elster, MC USN ;
MILITARY MEDICINE, 179, 3:315, 2014 Surgical Management of Modern Combat-Related Pancreatic Injuries: Traditional Management and Unique Strategies MAJ Amy Vertrees, MC USA* ; CAPT Eric Elster, MC USN ;
BRANDON REGIONAL HEALTH CENTER; WHIPPLE S PROCEDURE AND ESOPHAGECTOMY AUDIT
 BRANDON REGIONAL HEALTH CENTER; WHIPPLE S PROCEDURE AND ESOPHAGECTOMY AUDIT By: Amy Cisyk Home for the Summer Program July, 2016 Brandon, Manitoba Supervisor: Dr. Marvin Goossen Whipple s Procedure Audit
BRANDON REGIONAL HEALTH CENTER; WHIPPLE S PROCEDURE AND ESOPHAGECTOMY AUDIT By: Amy Cisyk Home for the Summer Program July, 2016 Brandon, Manitoba Supervisor: Dr. Marvin Goossen Whipple s Procedure Audit
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Practice Variability in the Management of Pediatric Pancreatic Trauma
 Practice Variability in the Management of Pediatric Pancreatic Trauma Bindi Naik-Mathuria, MD and members of the Pediatric Trauma Study Group Falcone R Burd R Puapong D Mooney D Campbell B Kreyekes N Fenton
Practice Variability in the Management of Pediatric Pancreatic Trauma Bindi Naik-Mathuria, MD and members of the Pediatric Trauma Study Group Falcone R Burd R Puapong D Mooney D Campbell B Kreyekes N Fenton
Radiological Investigations of Abdominal Trauma
 76 77 Investigations of Abdominal Trauma Introduction: Trauma to abdominal organs is a common cause of patient morbidity and mortality among trauma patients. Causes of abdominal trauma include blunt injuries,
76 77 Investigations of Abdominal Trauma Introduction: Trauma to abdominal organs is a common cause of patient morbidity and mortality among trauma patients. Causes of abdominal trauma include blunt injuries,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/39153 holds various files of this Leiden University dissertation. Author: Hommes, M. Title: The injured liver : management and hepatic injuries in the traumapatient
Cover Page The handle http://hdl.handle.net/1887/39153 holds various files of this Leiden University dissertation. Author: Hommes, M. Title: The injured liver : management and hepatic injuries in the traumapatient
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Factors Affecting Pneumonia Occurring to Patients with Multiple Rib Fractures
 Korean J Thorac Cardiovasc Surg 2013;46:130-134 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Clinical Research http://dx.doi.org/10.5090/kjtcs.2013.46.2.130 Factors Affecting Pneumonia Occurring to
Korean J Thorac Cardiovasc Surg 2013;46:130-134 ISSN: 2233-601X (Print) ISSN: 2093-6516 (Online) Clinical Research http://dx.doi.org/10.5090/kjtcs.2013.46.2.130 Factors Affecting Pneumonia Occurring to
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH
 AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr ABDOMINAL ABSCESS A SEQUEL OF EXPLORATORY LAPAROTOMY FOR
AMERICAN JOURNAL OF BIOLOGICAL AND PHARMACEUTICAL RESEARCH e-issn - 2348-2184 Print ISSN - 2348-2176 Journal homepage: www.mcmed.us/journal/ajbpr ABDOMINAL ABSCESS A SEQUEL OF EXPLORATORY LAPAROTOMY FOR
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY 2013/12/21
 THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
THE CRITICAL COMPLCATIONS AND MANAGEMENTS AFTER PANCREATIC SURGERY Tsann-Long Hwang, MD, FACS Department of Surgery Chang Gung Memorial Hospital Chang Gung University Taipei, TAIWAN 2013/12/21 THE DIFFICULTY
A Review on the Role of Laparoscopy in Abdominal Trauma
 10.5005/jp-journals-10007-1109 ORIGINAL ARTICLE WJOLS A Review on the Role of Laparoscopy in Abdominal Trauma Aryan Ahmed Specialist General Surgeon, ATLS Instructor, Department of General Surgery, Hamad
10.5005/jp-journals-10007-1109 ORIGINAL ARTICLE WJOLS A Review on the Role of Laparoscopy in Abdominal Trauma Aryan Ahmed Specialist General Surgeon, ATLS Instructor, Department of General Surgery, Hamad
Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article
 Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article Authors: Dr Vaibhav Pandey 1*, Dr. Pranay Panigrahi 2 Srivastav 4 & Dr Rakesh Kumar
Title: Post traumatic Diaphragmatic hernia in children: Diagnostic Dilemmas and lessons learned. Type: Original article Authors: Dr Vaibhav Pandey 1*, Dr. Pranay Panigrahi 2 Srivastav 4 & Dr Rakesh Kumar
LIVER TRAUMA. Jonathan R. Hiatt, MD
 Jonathan R. Hiatt, MD HISTORY 1880 1900 1908 MORTALITY OF LIVER INJURY MODERN CONCEPTS PACKS, RESECTION PRINGLE WW II 27% KOREA 14% VIETNAM 8.5% URBAN TRAUMA CTRS. EPIDEMIOLOGY CLASSIFICATION THERAPEUTIC
Jonathan R. Hiatt, MD HISTORY 1880 1900 1908 MORTALITY OF LIVER INJURY MODERN CONCEPTS PACKS, RESECTION PRINGLE WW II 27% KOREA 14% VIETNAM 8.5% URBAN TRAUMA CTRS. EPIDEMIOLOGY CLASSIFICATION THERAPEUTIC
Management of Blunt Renal Trauma in Srinagarind Hospital: 10-Year Experience
 Management of Blunt Renal Trauma in Srinagarind Hospital: 10-Year Experience Chaiyut Thanapaisal MD*, Wichien Sirithanaphol MD* * Department of Surgery, Faculty of Medicine, Khon Kaen University, Khon
Management of Blunt Renal Trauma in Srinagarind Hospital: 10-Year Experience Chaiyut Thanapaisal MD*, Wichien Sirithanaphol MD* * Department of Surgery, Faculty of Medicine, Khon Kaen University, Khon
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury
 TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
TEVAR for trauma is here to stay: Advances in the Treatment of Blunt Thoracic Aortic Injury Megan Brenner MD MS RPVI FACS Associate Professor of Surgery Division of Trauma/Surgical Critical Care, RA Cowley
Urgent pulmonary lobectomy for blunt chest trauma: report of three cases without mortality
 Short Communication Urgent pulmonary lobectomy for blunt chest trauma: report of three cases without mortality Marco Chiarelli 1, Martino Gerosa 1, Angelo Guttadauro 2, Francesco Gabrielli 2, Giuseppe
Short Communication Urgent pulmonary lobectomy for blunt chest trauma: report of three cases without mortality Marco Chiarelli 1, Martino Gerosa 1, Angelo Guttadauro 2, Francesco Gabrielli 2, Giuseppe
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
A Z OF ABDOMINAL RADIOLOGY
 Z OF BDOMINL RDIOLOGY bdominal trauma to Z of bdominal Radiology Clinical characteristics general discussion, followed by organ-specific summaries, is given below. bdominal trauma is managed as part of
Z OF BDOMINL RDIOLOGY bdominal trauma to Z of bdominal Radiology Clinical characteristics general discussion, followed by organ-specific summaries, is given below. bdominal trauma is managed as part of
A Severely Injured Pediatric Trauma Patient: Case Presentation and Discussion
 A Severely Injured Pediatric Trauma Patient: Case Presentation and Discussion Christopher Butts PhD, DO Surgical Critical Care Fellow Cooper University Hospital H&P 10 year old female presents as a trauma
A Severely Injured Pediatric Trauma Patient: Case Presentation and Discussion Christopher Butts PhD, DO Surgical Critical Care Fellow Cooper University Hospital H&P 10 year old female presents as a trauma
SAS Journal of Surgery ISSN SAS J. Surg., Volume-2; Issue-1 (Jan-Feb, 2016); p Available online at
 SAS Journal of Surgery ISSN 2454-5104 SAS J. Surg., Volume-2; Issue-1 (Jan-Feb, 2016); p-53-59 Available online at http://sassociety.com/sasjs/ Original Research Article Clinical Study, Evaluation and
SAS Journal of Surgery ISSN 2454-5104 SAS J. Surg., Volume-2; Issue-1 (Jan-Feb, 2016); p-53-59 Available online at http://sassociety.com/sasjs/ Original Research Article Clinical Study, Evaluation and
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
EAST MULTICENTER STUDY DATA DICTIONARY
 EAST MULTICENTER STUDY DATA DICTIONARY Does the Addition of Daily Aspirin to Standard Deep Venous Thrombosis Prophylaxis Reduce the Rate of Venous Thromboembolic Events? Data Entry Points and appropriate
EAST MULTICENTER STUDY DATA DICTIONARY Does the Addition of Daily Aspirin to Standard Deep Venous Thrombosis Prophylaxis Reduce the Rate of Venous Thromboembolic Events? Data Entry Points and appropriate
The Abdominal Compartment Syndrome
 The Abdominal Compartment Syndrome Andre R. Campbell, MD, FACS, FACP, FCCM Professor of Surgery, UCSF Endowed Chair of Surgical Education San Francisco General Hospital Outline Case presentations Review
The Abdominal Compartment Syndrome Andre R. Campbell, MD, FACS, FACP, FCCM Professor of Surgery, UCSF Endowed Chair of Surgical Education San Francisco General Hospital Outline Case presentations Review
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health
 UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Analysis of Urobilinogen and Urine Bilirubin for Intra-Abdominal Injury in Blunt Trauma Patients
UC Irvine Western Journal of Emergency Medicine: Integrating Emergency Care with Population Health Title Analysis of Urobilinogen and Urine Bilirubin for Intra-Abdominal Injury in Blunt Trauma Patients
Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography
 AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
AISP - 29 th National Congress. Bologna (Italy). September 15-17, 2005. Imaging Techniques for Acute Necrotizing Pancreatitis: Multidetector Computed Tomography Lucia Calculli 1, Raffaele Pezzilli 2, Riccardo
RESUSCITATION IN TRAUMA. Important things I have learnt
 RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
RESUSCITATION IN TRAUMA Important things I have learnt Trauma resuscitation through the decades What was hot and now is not 1970s 1980s 1990s 2000s Now 1977 Fluids Summary Dogs subjected to arterial hemorrhage
Evaluation of Children with Blunt Abdominal Trauma. James F. Holmes, MD, MPH UC Davis School of Medicine
 Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC
 INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC Pages with reference to book, From 14 To 16 S. Amjad Hussain, Chinda Suriyapa, Karl Grubaugh ( Depts. of Surger and
INTRA-THORACIC AND INTRA-ABDO-MINAL PERFORATION OF THE COLON IN TRAUMATIC DIAPHRAGMATIC Pages with reference to book, From 14 To 16 S. Amjad Hussain, Chinda Suriyapa, Karl Grubaugh ( Depts. of Surger and
GCS as a predictor of mortality in patients with traumatic inferior vena cava injuries: a retrospective review of 16 cases
 Cudworth et al. World Journal of Emergency Surgery 2013, 8:59 WORLD JOURNAL OF EMERGENCY SURGERY RESEARCH ARTICLE Open Access GCS as a predictor of mortality in patients with traumatic inferior vena cava
Cudworth et al. World Journal of Emergency Surgery 2013, 8:59 WORLD JOURNAL OF EMERGENCY SURGERY RESEARCH ARTICLE Open Access GCS as a predictor of mortality in patients with traumatic inferior vena cava
PROTOCOLS. Lap-belt syndrome. Principal investigator. Background
 Lap-belt syndrome Principal investigator Claude Cyr, MD, Centre hospitalier universitaire de Sherbrooke, 3001 12 e Avenue Nord, Sherbrooke QC J1H 5N4; tel.: (819) 346-1110, ext. 14634; fax: (819) 564-5398;
Lap-belt syndrome Principal investigator Claude Cyr, MD, Centre hospitalier universitaire de Sherbrooke, 3001 12 e Avenue Nord, Sherbrooke QC J1H 5N4; tel.: (819) 346-1110, ext. 14634; fax: (819) 564-5398;
KNIFED IN THE ABDOMEN
 Originally Posted: November 01, 2014 KNIFED IN THE ABDOMEN Resident(s): Andrew Duarte, MD Attending(s): Ryan Scott, MD & David Kay, MD Program/Dept(s): St. Joseph s Hospital and Medical Center, Phoenix,
Originally Posted: November 01, 2014 KNIFED IN THE ABDOMEN Resident(s): Andrew Duarte, MD Attending(s): Ryan Scott, MD & David Kay, MD Program/Dept(s): St. Joseph s Hospital and Medical Center, Phoenix,
Reinterventions belong to complications
 Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Reinterventions belong to complications Pancreatic surgery is the archetypus of complex abdominal surgery Mortality (1-4%) and morbidity (7-60%) rates are relevant even at high volume centres Reinterventions
Pancreatic Benign April 27, 2016
 Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
Department of Surgery Pancreatic Benign April 27, 2016 James Choi Dr. Hernandez Objectives Medical Expert: 1. Anatomy and congenital anomalies of the pancreas and pancreatic duct (divisum, annular pancreas
DELAYED COMPLICATION OF PANCREATIC
 HPB Surgery, 1991, Vol. 5, pp. 49-60 Reprints available directly from the publisher Photocopying permitted by license only 1991 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
HPB Surgery, 1991, Vol. 5, pp. 49-60 Reprints available directly from the publisher Photocopying permitted by license only 1991 Harwood Academic Publishers GmbH Printed in the United Kingdom CASE REPORT
Pediatric Abdomen Trauma
 Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
Delayed Splenic Rupture After Non-Operative Management of Blunt Splenic Injury A AAST Multi-Institutional Prospective Trial Data Collection Tool
 Delayed Splenic Rupture After Non-Operative Management of Blunt Splenic Injury A AAST Multi-Institutional Prospective Trial Data Collection Tool Enrolling Center: Patient Number (sequential within center):
Delayed Splenic Rupture After Non-Operative Management of Blunt Splenic Injury A AAST Multi-Institutional Prospective Trial Data Collection Tool Enrolling Center: Patient Number (sequential within center):
In any operation. Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications.
 In any operation Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications. Abdominal operation I position for operation Supine Abdominal operation I position for
In any operation Indications. Anaesthesia. Position of the patient. Incision. Steps of the operation. Complications. Abdominal operation I position for operation Supine Abdominal operation I position for
Data Collection Tool. Standard Study Questions: Admission Date: Admission Time: Age: Gender:
 Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
Data Collection Tool Standard Study Questions: Admission Date: Admission Time: Age: Gender: Specifics of Injury: Time of Injury: Mechanism of Injury Blunt vs Penetrating? Injury Severity Score? Injuries:
The ABC s of Chest Trauma
 The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
The ABC s of Chest Trauma J Bradley Pickhardt MD, FACS Providence St Patrick Hospital What s the Problem? 2/3 of trauma patients have chest trauma Responsible for 25% of all trauma deaths Most injuries
Internal Injury Documentation Guidelines
 Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
NON-OPERATIVE MANAGEMENT OF PEDIATRIC SOLID ORGAN INJURY
 NON-OPERATIVE MANAGEMENT OF PEDIATRIC SOLID ORGAN INJURY JESSICA A. NAIDITCH, MD TRAUMA MEDICAL DIRECTOR, DELL CHILDREN S MEDICAL CENTER OF CENTRAL TEXAS ASSISTANT PROFESSOR OF SURGERY AND PERIOPERATIVE
NON-OPERATIVE MANAGEMENT OF PEDIATRIC SOLID ORGAN INJURY JESSICA A. NAIDITCH, MD TRAUMA MEDICAL DIRECTOR, DELL CHILDREN S MEDICAL CENTER OF CENTRAL TEXAS ASSISTANT PROFESSOR OF SURGERY AND PERIOPERATIVE
Disclosures. Dr. Hall is a paid consultant to the American College of Surgeons (ACS) as Associate Director of ACS-NSQIP
 Does Routine Drainage of the Operative Bed following Elective Distal Pancreatectomy reduce Complications? An Analysis of the ACS-NSQIP Pancreatectomy Demonstration Project Stephen W. Behrman, MD 1, Ben
Does Routine Drainage of the Operative Bed following Elective Distal Pancreatectomy reduce Complications? An Analysis of the ACS-NSQIP Pancreatectomy Demonstration Project Stephen W. Behrman, MD 1, Ben
Renal Trauma: Management Options
 Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Changing Trends in the Management of Penetrating Abdominal Trauma - from Mandatory Laparotomy towards Conservative Management.
 DOI: 10.21276/aimdr.2016.2.6.SG6 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Changing Trends in the Management of Penetrating Abdominal Trauma - from Mandatory Laparotomy towards Conservative
DOI: 10.21276/aimdr.2016.2.6.SG6 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Changing Trends in the Management of Penetrating Abdominal Trauma - from Mandatory Laparotomy towards Conservative
PARA107 Summary. Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38:
 PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
Negative Laparotomy in Trauma: Are We Getting Better?
 Negative Laparotomy in Trauma: Are We Getting Better? BEAT SCHNÜRIGER, M.D., LYDIA LAM, M.D., KENJI INABA, M.D., LESLIE KOBAYASHI, M.D., RAFFAELLA BARBARINO, M.D., DEMETRIOS DEMETRIADES, M.D., PH.D. From
Negative Laparotomy in Trauma: Are We Getting Better? BEAT SCHNÜRIGER, M.D., LYDIA LAM, M.D., KENJI INABA, M.D., LESLIE KOBAYASHI, M.D., RAFFAELLA BARBARINO, M.D., DEMETRIOS DEMETRIADES, M.D., PH.D. From
SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad
 SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad Trauma Emergency Room layout Ideally the trauma emergency room is centrally located to provide
SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad Trauma Emergency Room layout Ideally the trauma emergency room is centrally located to provide
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign
 Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
Acute abdominal venous thromboses- the hyperdense noncontrast CT sign Poster No.: C-1095 Congress: ECR 2011 Type: Educational Exhibit Authors: M. Goldstein, K. Jhaveri; Toronto, ON/CA Keywords: Abdomen,
World Journal of Colorectal Surgery
 World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 9 ISSUE 1 Perforation Of The Caecum Owing To Benign Rectal Obstruction: A Paradigm Of Damage Control In Emergency Colorectal Surgery DIMITRIOS
World Journal of Colorectal Surgery Volume 3, Issue 1 2013 Article 9 ISSUE 1 Perforation Of The Caecum Owing To Benign Rectal Obstruction: A Paradigm Of Damage Control In Emergency Colorectal Surgery DIMITRIOS
Michael Minarich, MD General Surgery Resident, PGY4 Cooper University Hospital
 BMI as Major Preoperative Risk Factor for Intraabdominal Infection After Distal Pancreatectomy: an Analysis of National Surgical Quality Improvement Program Database Michael Minarich, MD General Surgery
BMI as Major Preoperative Risk Factor for Intraabdominal Infection After Distal Pancreatectomy: an Analysis of National Surgical Quality Improvement Program Database Michael Minarich, MD General Surgery
IVC. Fig. ACS. 84/60mmHg. CT Fig. 2 AAA. 30 declamp. declamp. Tel:
 12 633 637 2003 IVC 3 4 5 3 12 633 637 2003 1 ACS ACS 1 6 3 ACS 3 Tel: 0566-75-2111 446-8602 28 2003 7 18 2003 10 15 Fig. 1 4 5 1 71 12 5 COPD 14 10 30 60 CT AAA 84/60mmHg 8.2g/dl6.6g/dl2.5mg/dl CT Fig.
12 633 637 2003 IVC 3 4 5 3 12 633 637 2003 1 ACS ACS 1 6 3 ACS 3 Tel: 0566-75-2111 446-8602 28 2003 7 18 2003 10 15 Fig. 1 4 5 1 71 12 5 COPD 14 10 30 60 CT AAA 84/60mmHg 8.2g/dl6.6g/dl2.5mg/dl CT Fig.
Conservative Management of Renal Trauma: Ten Years Experience Reem Al-Bareeq MRCSI, CABU* Kadem Zabar CABS** Mohammed Al-Tantawi CABS***
 Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Conservative Management of Renal Trauma: Ten Years Experience Reem Al-Bareeq MRCSI, CABU* Kadem Zabar CABS** Mohammed Al-Tantawi CABS*** Objective:
Bahrain Medical Bulletin, Vol. 28, No. 3, September 2006 Conservative Management of Renal Trauma: Ten Years Experience Reem Al-Bareeq MRCSI, CABU* Kadem Zabar CABS** Mohammed Al-Tantawi CABS*** Objective:
Abdominal Compartment Syndrome. Jeff Johnson, MD
 Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
Abdominal Compartment Syndrome Jeff Johnson, MD Acute Care Surgeon, Denver Health Associate Professor of Surgery, University of Colorado Denver The Abdomen A Forgotten Closed Compartment Early Animal Models
Muscle spasm Diminished bowel sounds Nausea/vomiting
 3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
Management of biliary complications following damage control surgery for liver trauma
 Eur J Trauma Emerg Surg DOI 10.1007/s00068-013-0304-4 ORIGINAL ARTICLE Management of biliary complications following damage control surgery for liver trauma M. Hommes G. Kazemier N. W. L. Schep E. J. Kuipers
Eur J Trauma Emerg Surg DOI 10.1007/s00068-013-0304-4 ORIGINAL ARTICLE Management of biliary complications following damage control surgery for liver trauma M. Hommes G. Kazemier N. W. L. Schep E. J. Kuipers
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
Note: Page numbers of article titles are in boldface type. A Adenocarcinoma, pancreatic ductal, laparoscopic distal pancreatectomy for, 61 Adrenal cortical carcinoma, laparoscopic adrenalectomy for, 114
PONGSASIT SINGHATAS, M.D. Department of Surgery Faculty of Medicine, Ramathibodi Hospital Mahidol University
 PONGSASIT SINGHATAS, M.D. Department of Surgery Faculty of Medicine, Ramathibodi Hospital Mahidol University Patient survive Low morbidity GOOD JUDGMENT COMES FROM EXPERIENCE EXPERIENCE COMES FROM BAD
PONGSASIT SINGHATAS, M.D. Department of Surgery Faculty of Medicine, Ramathibodi Hospital Mahidol University Patient survive Low morbidity GOOD JUDGMENT COMES FROM EXPERIENCE EXPERIENCE COMES FROM BAD
General Surgery PURPLE SERVICE MUHC-RVH Site
 Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Preamble HPB is a clinical teaching unit with several different vocations: It regroups all solid organ Transplantation as well as most advanced Hepatobiliary and Pancreatic clinical activities performed
Pancreatic injury in children: a case report and review of the literature
 Haider et al. Journal of Medical Case Reports (2017) 11:217 DOI 10.1186/s13256-017-1383-3 CASE REPORT Open Access Pancreatic injury in children: a case report and review of the literature Fayza Haider
Haider et al. Journal of Medical Case Reports (2017) 11:217 DOI 10.1186/s13256-017-1383-3 CASE REPORT Open Access Pancreatic injury in children: a case report and review of the literature Fayza Haider
Management of the Open Abdomen
 Management of the Open Abdomen Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Associate Professor of Surgery Denver Health Medical Center / University of Colorado The Open Abdomen
Management of the Open Abdomen Clay Cothren Burlew, MD FACS Director, Surgical Intensive Care Unit Associate Professor of Surgery Denver Health Medical Center / University of Colorado The Open Abdomen
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/39153 holds various files of this Leiden University dissertation. Author: Hommes, M. Title: The injured liver : management and hepatic injuries in the traumapatient
Cover Page The handle http://hdl.handle.net/1887/39153 holds various files of this Leiden University dissertation. Author: Hommes, M. Title: The injured liver : management and hepatic injuries in the traumapatient
Medical - Clinical Research & Reviews
 Research Article Research Article Medical - Clinical Research & Reviews ISSN 2575-6087 Management of Kidney in Saiful Anwar General Hospital Malang Indonesia Besut Daryanto, I Made Udiyana Indradiputra,
Research Article Research Article Medical - Clinical Research & Reviews ISSN 2575-6087 Management of Kidney in Saiful Anwar General Hospital Malang Indonesia Besut Daryanto, I Made Udiyana Indradiputra,
EAST MULTICENTER STUDY DATA DICTIONARY. Temporary Intravascular Shunt Study Data Dictionary
 EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
EAST MULTICENTER STUDY DATA DICTIONARY Temporary Intravascular Shunt Study Data Dictionary Data Entry Points and appropriate definitions / clarifications: Entry space Definition / Instructions 1. Specific
SSRG International Journal of Medical Science (SSRG-IJMS) volume 1 Issue 2 December 2014
 Blunt Abdominal Trauma: Making Decision of Management with Conventional and Ultrasonography Evaluation Dr.Naveen K G 1, Dr. Ravi N 2, Dr. Nagaraj B R 3 1(senior resident-department of radiology, Bangalore
Blunt Abdominal Trauma: Making Decision of Management with Conventional and Ultrasonography Evaluation Dr.Naveen K G 1, Dr. Ravi N 2, Dr. Nagaraj B R 3 1(senior resident-department of radiology, Bangalore
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Imaging in abdominal trauma
 Imaging in abdominal trauma Dilyana Baleva Medical University Varna Landesklinikum Mistelbach-Gänserndorf Learning objectives Definition, demographics and etiology Imaging modalities and protocols Common
Imaging in abdominal trauma Dilyana Baleva Medical University Varna Landesklinikum Mistelbach-Gänserndorf Learning objectives Definition, demographics and etiology Imaging modalities and protocols Common
A Clinical Study of Blunt Injury Abdomen in a Tertiary Care Hospital
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/167 A Clinical Study of Blunt Injury Abdomen in a Tertiary Care Hospital J Amuthan 1, A Vijay 2, C Pradeep 2, Heber
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/167 A Clinical Study of Blunt Injury Abdomen in a Tertiary Care Hospital J Amuthan 1, A Vijay 2, C Pradeep 2, Heber
Case Conference. Discussion. Indications of Trauma Blue. Trauma Protocol In SKH. Trauma Blue VS. Trauma Red. Supervisor:VS 楊毓錚 Presenter:R1 周光緯
 Case Conference Supervisor:VS 楊毓錚 Presenter:R1 周光緯 Discussion 2010.7.14 2/81 Trauma Protocol In SKH Indications of Trauma Blue Trauma Blue VS. Trauma Red 3/81 Severe trauma mechanism : 1. Trauma to multiple
Case Conference Supervisor:VS 楊毓錚 Presenter:R1 周光緯 Discussion 2010.7.14 2/81 Trauma Protocol In SKH Indications of Trauma Blue Trauma Blue VS. Trauma Red 3/81 Severe trauma mechanism : 1. Trauma to multiple
TEVAR FOR! THORACIC AORTIC TRAUMA"
 10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
10th HKL Vascular Surgery Conference and Workshop" TEVAR FOR! THORACIC AORTIC TRAUMA" Dr Hanif Hussein" Vascular and General Surgeon" Department of Surgery" Hospital Kuala Lumpur" Source: MIROS! Thoracic
Acute, Blood, Trauma /ecr2015/C-2116
 The Baltimore CT Severity Index (CTSI) versus the American Association of Surgical Trauma (AAST) for grading splenic Injury on CT: Use and implications of an imaging based grading system for splenic injury
The Baltimore CT Severity Index (CTSI) versus the American Association of Surgical Trauma (AAST) for grading splenic Injury on CT: Use and implications of an imaging based grading system for splenic injury
UBC Department of Urologic Sciences Lecture Series. Urological Trauma
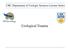 UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
The Questionable Utility of Oral Contrast for the Patient with Abdominal Pain in the Emergency Department
 The Questionable Utility of Oral Contrast for the Patient with Abdominal Pain in the Emergency Department Jonathan Rakofsky, MD PGY3 Henry Ford Hospital Emergency Medicine Program December 2014 All patients
The Questionable Utility of Oral Contrast for the Patient with Abdominal Pain in the Emergency Department Jonathan Rakofsky, MD PGY3 Henry Ford Hospital Emergency Medicine Program December 2014 All patients
Severe necrotizing pancreatitis. ICU Fellowship Training Radboudumc
 Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Severe necrotizing pancreatitis ICU Fellowship Training Radboudumc Acute pancreatitis Patients with acute pancreatitis van Dijk SM. Gut 2017;66:2024-2032 Diagnosis Revised Atlanta classification Abdominal
Duodenal Injury after Blunt Abdominal Trauma in Children: Experience with 22 Cases
 Annals of Pediatric Surgery, Vol 2, No 2, April 26, PP 99-15 Original Article Duodenal Injury after Blunt Abdominal Trauma in Children: Experience with 22 Cases Mohamed E Hassan, Amira Waly, Wael E Lotfy
Annals of Pediatric Surgery, Vol 2, No 2, April 26, PP 99-15 Original Article Duodenal Injury after Blunt Abdominal Trauma in Children: Experience with 22 Cases Mohamed E Hassan, Amira Waly, Wael E Lotfy
Liver lacerations in abdominal trauma management based on anatomical knowledge: A Case report
 American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Case Report Liver lacerations in abdominal trauma management based on anatomical Ashfaq ul Hassan 1*, Rohul 1, Shifan 2,
American Journal of Advances in Medical Science www.arnaca.com eissn: 2347-2766 Case Report Liver lacerations in abdominal trauma management based on anatomical Ashfaq ul Hassan 1*, Rohul 1, Shifan 2,
