The AMP-activated protein kinase α2 catalytic subunit controls whole-body insulin sensitivity
|
|
|
- Kory Horton
- 6 years ago
- Views:
Transcription
1 The AMP-activated protein kinase α2 catalytic subunit controls whole-body insulin sensitivity Benoit Viollet, 1 Fabrizio Andreelli, 1 Sebastian B. Jørgensen, 2 Christophe Perrin, 3 Alain Geloen, 4 Daisy Flamez, 5 James Mu, 6 Claudia Lenzner, 1 Olivier Baud, 1 Myriam Bennoun, 1 Emmanuel Gomas, 1 Gaël Nicolas, 1 Jørgen F.P. Wojtaszewski, 2 Axel Kahn, 1 David Carling, 7 Frans C. Schuit, 5 Morris J. Birnbaum, 6 Erik A. Richter, 2 Rémy Burcelin, 3 and Sophie Vaulont 1 1 Department of Genetic, Development, and Molecular Pathology, Institut Cochin, Institut National de la Santé et de la Recherche Médicale (INSERM), Centre National de la Recherche Scientifique (CNRS), René Descartes University, Paris, France 2 Copenhagen Muscle Research Centre, Department of Human Physiology, Institute of Exercise and Sport Sciences, University of Copenhagen, Copenhagen, Denmark 3 Unité Mixte de Recherche 5018, CNRS, Paul Sabatier University, Rangueil Hospital, Toulouse, France 4 INSERM, Institut National des Sciences Appliquées-Lyon, Villeurbanne, France 5 Diabetes Research Center, Laboratory of Biochemistry, Vrije Universiteit Brussel, Brussels, Belgium 6 Howard Hughes Medical Institute, University of Pennsylvania School of Medicine, Philadelphia, Pennsylvania, USA 7 Cellular Stress Group, Medical Research Council Clinical Sciences Centre, Hammersmith Hospital, London, United Kingdom AMP-activated protein kinase (AMPK) is viewed as a fuel sensor for glucose and lipid metabolism. To better understand the physiological role of AMPK, we generated a knockout mouse model in which the AMPKα2 catalytic subunit gene was inactivated. AMPKα2 / mice presented high glucose levels in the fed period and during an oral glucose challenge associated with low insulin plasma levels. However, in isolated AMPKα2 / pancreatic islets, glucose- and L-arginine stimulated insulin secretion were not affected. AMPKα2 / mice have reduced insulin-stimulated whole-body glucose utilization and muscle glycogen synthesis rates assessed in vivo by the hyperinsulinemic euglycemic clamp technique. Surprisingly, both parameters were not altered in mice expressing a dominant-negative mutant of AMPK in skeletal muscle. Furthermore, glucose transport was normal in incubated isolated AMPKα2 / muscles. These data indicate that AMPKα2 in tissues other than skeletal muscles regulates insulin action. Concordantly, we found an increased daily urinary catecholamine excretion in AMPKα2 / mice, suggesting altered function of the autonomic nervous system that could explain both the impaired insulin secretion and insulin sensitivity observed in vivo. Therefore, extramuscular AMPKα2 catalytic subunit is important for whole-body insulin action in vivo, probably through modulation of sympathetic nervous activity. J. Clin. Invest. 111:91 98 (2003). doi: /jci Introduction The AMP-activated protein kinase (AMPK) has been proposed to act as a fuel sensor capable of mediating the cellular adaptation to nutritional and environmental variations (1). AMPK is a ubiquitous serine/threonine protein kinase activated in response to environmental or nutritional stress factors that deplete intracellular ATP levels. AMPK is a heterotrimeric enzyme consisting of an Received for publication August 1, 2002, and accepted in revised form November 12, Address correspondence to: B. Viollet, Institut Cochin, Département GDPM, 24 Rue du Faubourg Saint-Jacques Paris, France. Phone: ; Fax: ; viollet@cochin.inserm.fr. Benoit Viollet and Fabrizio Andreelli contributed equally to this work. Conflict of interest: The authors have declared that no conflict of interest exists. Nonstandard abbreviations used: AMP-activated protein kinase (AMPK); 5-aminoimidazole-4-carboxamide-1-β-D-ribofuranoside (AICAR); kinase-dead AMPKα2 transgenic (Tg-KD-AMPKα2); oral glucose tolerance test (OGTT); acetyl-coa carboxylase (ACC). α catalytic subunit and noncatalytic regulatory β and γ subunits. Two isoforms have been identified for both the α subunit (α1 and α2) and β subunit (β1 and β2), and three isoforms have been reported for the γ subunit (γ1, γ2, and γ3). Regulation of AMPK activity is complex, involving allosteric activation by AMP and covalent modification by phosphorylation via an upstream AMPK kinase (2). Phosphorylation of threonine 172 in the α subunit of AMPK is essential for its activation (2). Metabolic actions of AMPK have been extensively studied in skeletal muscle. Activation of AMPK by 5-aminoimidazole-4-carboxamide-1-β-D-ribofuranoside (AICAR) has been demonstrated to increase muscle glucose uptake in vivo and in vitro via an acute insulin-independent mechanism (3, 4) and to decrease the glycogen synthase activity ratio (5). Implication of AMPK in the physiology of tissues other than skeletal muscle has also been suggested by findings in liver (6 8), pancreas (9, 10), and adipose tissue (4, 7, 11, 12). Lastly, AMPK is also expressed in the CNS (13), but the role of AMPK in this tissue remains to be determined. The Journal of Clinical Investigation January 2003 Volume 111 Number 1 91
2 In skeletal muscle, the actions of AMPK are thought to be mediated mainly through the AMPKα2 isoform (5, 14, 15). In other tissues, the physiological role of this isoform in vivo is less clear. To get more insights into this issue, we knocked out the AMPKα2 gene. In the present study, we show that AMPKα2 / mice exhibit glucose intolerance that is associated with low plasma insulin levels and reduced muscle glycogen synthesis during hyperinsulinemic clamp conditions. Reduction of insulin sensitivity was not dependent on muscle AMPK activity, since mice expressing a dominant-negative mutant of AMPK in skeletal muscle are not insulin resistant. Finally, AMPKα2 / mice have increased catecholamine urinary excretion, suggesting increased sympathetic tone. Consequently, our data suggest that the α2 catalytic subunit of AMPK plays a major role in vivo as a fuel metabolic sensor by modulating the activity of the autonomous nervous system. Methods Gene targeting and generation of AMPKα2 gene knockout mice. AMPKα2 genomic clones were isolated after screening a mouse 129 strain genomic library (Stratagene, Loyola, California, USA). The targeting construct was generated by flanking exon C, which encodes the AMPKα2 catalytic domain (corresponding to amino acids ), with loxp sites for the Cre recombinase and inserting a PGK promoter driven neomycin selection cassette flanked by an additional loxp site. The targeting construct was linearized and electroporated into 129/Sv MPI-I embryonic stem cells. Targeted clones were identified by Southern blot analysis of HindIIIdigested DNA using a flanking 5 DNA fragment as a hybridization probe and PCR analysis. Cells expanded from targeted clones were injected into C57BL6 blastocysts, and germline-transmitting chimeric animals were mated with C57BL/6 mice. The resulting heterozygous offspring were bred with deleter EIIa-Cre transgenic mice, in which Cre is expressed in the germ cells, to produce AMPKα2 +/ mice (16). These mice were crossed to generate control and mutant mice. Southern blot analysis of HindIII-digested DNA with an internal probe (Figure 1a) and PCR analysis were used to genotype mice. Animals. Control, AMPKα2 /, and kinase-dead AMPKα2 transgenic (Tg-KD-AMPKα2) male mice were studied at 12 weeks of age. The establishment and characterization of Tg-KD-AMPKα2 mice were previously reported (17). Animals were housed under controlled temperature (21 C) and lighting, with 12 hours of light (7:00 am to 7:00 pm) and 12 hours of dark (7:00 pm to 7:00 am), and had free access to water and a standard mouse chow diet. All procedures were performed in accordance with the principles and guidelines established by the European Convention for the Protection of Laboratory Animals. Body weight, food intake, and body composition. Mice were weighed weekly after 3 weeks of age. Food intake was measured daily for a period of 3 days using metabolic cages (Marty Technologie, Paris, France) that allow free access to tap water and food. Body composition analysis was performed on anesthetized living mice by a dual-energy x-ray absorptiometry method using a small animal densitometer (PIXImus Lunar; GE Medical Systems, Madison, Wisconsin, USA). Careful dissection and weighing of individual organs was also performed. Tissue triglycerides were extracted with acetone, and triglyceride content was measured with a commercial kit (Sigma-Aldrich, St. Louis, Missouri, USA). Blood and urinary parameters. Blood was withdrawn from the tail using EDTA-aprotinin as the anticoagulant. In the fed state, blood was collected at 9:00 pm. For fasting experiments, food was removed at 5:00 pm, and the mice were kept in a clean new cage for 5 hours before blood collection. During the oral glucose tolerance test (OGTT) and AICAR tolerance test, blood glucose levels were assessed using a glucometer (Glucotrend II; Roche Diagnostics, Meylan, France). Serum insulin concentrations were assessed using a rat insulin ELISA kit with a mouse insulin standard (Crystal Chem Inc., Chicago, Illinois, USA). Serum leptin concentrations were assessed with a mouse leptin ELISA kit (Crystal Chem Inc.). Serum concentrations of potassium, sodium, triglycerides, FFAs, glycerol, total and HDL cholesterol, creatinine, and urea were determined using an automated Monarch device (Instrumentation Laboratory Co., Lexington, Massachusetts, USA). For determination of urinary levels of catecholamines, animals were housed in individual metabolic cages, and daily urinary catecholamine excretion during 3 consecutive days was determined by reverse-phase HPLC (performed at Cochin Hospital, Paris, France). Glucose and AICAR tolerance tests. During OGTT and AICAR tolerance testing, blood was collected from the tail vein at 0, 20, 40, 60, 80, 100, and 120 minutes for determination of glucose levels. OGTTs were performed in the morning after an overnight fast by oral administration of 3 g glucose per kg body weight. Blood was also collected at time 20 minutes in chilled heparinized tubes for determination of plasma insulin levels. To study the effect of α-adrenergic antagonist on glucose tolerance, mice were injected intraperitoneally with 10 mg/kg phentolamine 30 minutes before glucose challenge. To study the effect of β-adrenergic antagonist on glucose tolerance, mice were injected intraperitoneally with 10 mg/kg propranolol 30 minutes before glucose challenge. AICAR tolerance tests were performed in the morning by intraperitoneal injection of 0.25 g AICAR per kg body weight into overnight-fasted mice (17). Hyperinsulinemic euglycemic clamp procedures. To determine the rate of glucose utilization, an indwelling catheter was inserted into the femoral vein under anesthesia, sealed under the back skin, and glued on top of the skull (18). The mice were then housed individually. After 2 days, they showed normal feeding behavior and motor activity. The mice were allowed to recover for 4 6 days. On the day of the experiment, the mice were fast- 92 The Journal of Clinical Investigation January 2003 Volume 111 Number 1
3 Figure 1 Generation of mice lacking AMPKα2. (a) Schematic representation (not to scale) of genomic structure of AMPKα2 wild-type allele, AMPKα2 gene-targeting construct, AMPKα2 targeted allele, and AMPKα2 null allele. Squares indicate loxp sites and H s indicate HindIII restriction sites. C corresponds to the exon encoding the AMPKα2 catalytic domain (amino acids ) (b) Southern blot analysis after HindIII digestion of tail DNA from offspring derived from heterozygous intercrosses. Expected fragment sizes of the AMPKα2 wild-type (+/+; 5.3 kb) and null ( / ; 3.8 kb) alleles after HindIII digestion and hybridization with the indicated probe (solid bar in a) are shown. (c) Western blot analysis of AMPKα1 and AMPKα2 proteins in liver and gastrocnemius muscle from control (+/+) and AMPKα2 / mice. (d) Phosphorylation level of ACC in liver and gastrocnemius muscle from control and AMPKα2 / mice. ed for 6 hours. The whole-body glucose utilization rate was determined under basal and hyperinsulinemic euglycemic conditions. In the basal state, HPLC-purified D-(3-3 H)-glucose (NEN Life Science Products Inc., Boston, Massachusetts, USA) was continuously infused through the femoral vein at a rate of 10 µci/kg.min for 3 hours. In the hyperinsulinemic condition, insulin was infused at a rate of 6 mu/kg.min for 3 hours; D-(3-3 H)- glucose was infused at rate of 30 µci/kg.min a higher rate than for the basal condition, to ensure a detectable plasma D-(3-3 H)-glucose enrichment. Throughout the infusion, blood glucose was assessed from blood samples and euglycemia was maintained by periodically adjusting a variable infusion of 16.5% (wt/vol) glucose. Plasma glucose concentrations, D-(3-3 H)-glucose specific activity, and 3 H 2 O and D-(3-3 H)-glucose enrichments were determined as previously described (18). Glucose turnover and whole-body glycolysis rate were calculated as described (18). Whole-body glycogen synthesis was calculated by subtracting the whole-body glycolytic rate from the glucose turnover rate. The mean was calculated for each timepoint for this period. The mean value of mice from the same group was reported. Mice showing variations in specific activity larger than 15% were excluded from the study. Determination of total glycogen content and glycogen synthesis rate in skeletal muscle and liver. At completion of the infusion, the hind limb and the main lobe of the liver were removed and ground into liquid nitrogen for determination of total glycogen content and glycogen synthesis rate. Total glycogen was extracted from 20 mg of liver or 100 mg of muscle by digesting tissue samples in KOH. An aliquot was neutralized with HCl and the glycogen content was assessed using amyloglucosidase (19). Muscle glycogen synthesis rate was determined by extracting glycogen with perchloric acid (6% wt/vol) and precipitating glycogen with ethanol as described previously (20). The radioactive glycogen was counted and divided by the D-(3-3 H)-glucose specific activity to determine the rate of synthesis. Deoxyglucose uptake in isolated muscles. Mice were anesthetized with pentobarbital and soleus and extensor digitorum longus muscles were exposed. Ligatures were placed around the tendon at each end of the muscle. Muscles were suspended at resting tension (4 5 m Newtons) and incubated at 30 C for 10 minutes at basal conditions in incubation chambers (Multi myograph system organ bath 700MO; Danish Myo Technology A/S, Aarhus, Denmark) oxygenated with 95% O 2 and 5% CO 2 gas. Basal medium consisted of 0.01% BSA, 8 mm mannitol, and 2 mm pyruvate in Krebs-Henseleit buffer (118.5 mm NaCl, 24.7 mm NaHCO 3, 4.74 mm KCl, 1.18 mm MgSO 3, 1.18 KH 2 PO 4, and 2.5 CaCl 2, ph 7.4). After basal incubation the medium was aspirated and exchanged with medium containing 600 µu insulin/ml (100 IU/ml Actrapid; Novo Nordisk A/S, Bagsvær, Denmark) for 30 minutes. 2-deoxy-D-glucose uptake measurements were initiated by incubation in a medium containing 600 µu insulin/ml, 1 mm 2-[2,6-3 H]deoxy- D-glucose with a specific activity in the medium of mci/ml, and 8 mm [1-14 C]mannitol with a specific activity in the medium of mci/ml (Amersham Biosciences Europe, Freiburg, Germany). Uptake was measured for 10 minutes before the muscle was washed in ice-cold Krebs-Henseleit buffer and quickly frozen with aluminum tongs precooled in liquid nitrogen. Frozen muscles were digested in 250 µl 1 M NaOH at 80 C for 10 minutes. The solution was neutralized with 250 µl 1 M NaCl and spun at 13,000 g for 2 minutes. Radioactivity in the supernatant was measured using liquid scintillation (Tri-Carb 2000; Packard Instruments, Greve, Denmark). Insulin release from isolated islets of Langerhans. The insulin-secretory response of AMPKα2 / β cells was studied in collagenase-isolated islets of Langerhans. After isolation, islets were cultured for 16 hours in Ham s F10 medium containing 10 mm glucose. Insulin release was measured by perifusion experiments in a multiple microchamber module (Endotronics Inc., Coon Rapids, Minnesota, USA) as previously described (21). Approximately 200 islets were loaded onto Biogel P2 (Biorads Labs, Richmond, California, USA) in a col- The Journal of Clinical Investigation January 2003 Volume 111 Number 1 93
4 Table1 Body composition, food intake, and triglyceride content of liver, gastrocnemius muscle, and pancreas of AMPKα2 / mice umn and preperifused for 20 minutes in Ham s F10 medium supplemented with 0.5% (wt/vol) BSA, 2 mm glutamine, 2 mm CaCl 2, and 3 mm glucose, equilibrated with 95% O 2 and 5% CO 2. At a flow rate of 0.5 ml/min, 15-minute pulses of 3 mm glucose were alternated with 10-minute pulses of 7.5 mm glucose, 10 mm glucose, 20 mm glucose, and 10 mm glucose with 20 mm L-arginine (Sigma-Aldrich). Samples were collected every minute and assayed for immunoreactive insulin with guinea pig anti-insulin serum (Linco Research Inc., St. Charles, Missouri, USA). Results were expressed as percentages of the insulin content measured in each individual batch of islets after finishing the experiment by sonicating the Biogel P2 containing the islets in 5 ml of 2 mm acetic acid and 0.25% (wt/vol) BSA. Western blot analysis. Liver AMPK was obtained by polyethylene glycol precipitation (2), and muscle AMPK was prepared as previously described (5). AMPK catalytic subunits were detected using specific anti- AMPKα1 and anti-ampkα2 antibodies (kindly provided by G. Hardie, Dundee University, Dundee, Scotland, United Kingdom). The phosphorylation status of acetyl-coa carboxylase (ACC) was visualized using an anti phospho-acc (serine 79) antibody (Upstate Biotechnology Inc., Lake Placid, New York, USA). Statistical analysis. Data are expressed as mean ± SEM. Statistical analyses were carried out using an unpaired, two-tailed Student t test, and the null hypothesis was rejected at Results Animal model: AMPKα2 / mice. AMPKα2 gene knockout was obtained using a targeting vector inserting loxp sites flanking the sequence containing the enzymatic catalytic site (Figure 1a). Deletion of the targeted allele was carried out by mating to EIIa-Cre transgenic mice to cause germline excision (16). Mice harboring the deleted allele were identified by Control AMPKα2 / Body weight (g) 28.8 ± ± 0.8 Fat-free mass (g) A 21.6 ± ± 0.6 % fat mass A 7.1 ± ± 0.2 Food intake (g/d) 3.7 ± ± 0.1 Liver TG content (mg/g tissue) 11.2 ± ± 3.2 Muscle TG content (mg/g tissue) 11.7 ± ± 0.9 Pancreas TG content (mg/g tissue) 6.1 ± ± 0.6 A Body composition was assessed by biphotonic absorptiometry. All data are expressed as mean ± SEM (n = 6 10 mice/group). P not significant between groups by unpaired, two-tailed Student t test. TG, triglyceride. Southern blot analysis (Figure 1b). Using RT-PCR analysis, no amplification of the region corresponding to the catalytic domain of AMPKα2 was observed in the liver, skeletal muscle, or pancreas of AMPKα2 / mice (data not shown). Western blot analysis of protein extracts prepared from AMPKα2 / liver and skeletal muscle showed undetectable AMPKα2 protein (Figure 1c). The AMPKα1 protein level was similar in the liver of AMPKα2 / and control mice (Figure 1c). In contrast, in AMPKα2 / mice, AMPKα1 protein was increased 1.8-fold in gastrocnemius muscle (Figure 1c). Phosphorylation of ACC was decreased in gastrocnemius muscle 3.5-fold, while it was unchanged in the liver compared with controls (Figure 1d). Physical appearance, body weight, body composition, and triglyceride content in tissues of AMPKα2 / mice. AMPKα2 / mice from heterozygous mating were born with the expected mendelian ratio. AMPKα2 / mice are fertile, appear indistinguishable from their wildtype littermates, and have a normal life span. No significant difference in body weight or food intake was observed between the two groups (Table 1). Body composition was similar for both groups as assessed both by biphotonic absorptiometry (Table 1) and careful dissection and weighing of individual organs (data not shown). Triglyceride content in liver, gastrocnemius muscle, and pancreas was similar in AMPKα2 / mice and controls (Table 1). Metabolic parameters. In fasted conditions, plasma glucose and insulin levels were similar in AMPKα2 / mice and controls, while plasma FFA concentrations were increased in AMPKα2 / mice (Table 2). Glycerol plasma levels have a tendency to be higher in AMPKα2 / mice but do not reach statistical significance (Table 2). In the fed state, AMPKα2 / mice were characterized by higher plasma glucose and plasma FFA concentrations than were found in control mice, while plasma insulin and leptin levels were lower (Table 2). No difference between plasma levels of total and HDL cholesterol, sodium, potassium, creatinine, or urea were noted between AMPKα2 / and control mice (Table 2 and data not shown). Table 2 Metabolic parameters of AMPKα2 / mice in fasted and fed periods Fasted Fed Control AMPKα2 / Control AMPKα2 / Glycemia (mg/dl) 102 ± ± ± ± 9 B Insulin (ng/ml) 0.46 ± ± ± ± 0.12 B Leptin (ng/ml) 0.38 ± ± ± ± 0.49 A FFA (mm) 1.10 ± ± 0.06 A 0.73 ± ± 0.07 B Glycerol (µm) 367 ± ± ± ± 31 TG (mm) 0.58 ± ± ± ± 0.13 β-hydroxybutyrate (mm) 0.98 ± ± ± ± 0.01 Total cholesterol (mm) 2.3 ± ± ± ± 0.3 HDL cholesterol (mm) 1.7 ± ± ± ± 0.2 All data are expressed as mean ± SEM (n = 6 10 mice/group). A P < 0.01, B P < 0.05 vs. control group by unpaired, two-tailed Student t test. 94 The Journal of Clinical Investigation January 2003 Volume 111 Number 1
5 Figure 2 AMPKα2 / mice are AICAR-resistant, glucose intolerant, and exhibit impaired glucose-stimulated insulin secretion. (a) AICAR tolerance test. (b) OGTT. (c) Plasma glucose and insulin levels at time 20 minutes during OGTT. All results are expressed as mean ± SEM (n = 6 10). *P < 0.05, **P < 0.001, ***P < vs. control group by unpaired, two-tailed Student t test. NS, not significant. AMPKα2 / mice are AICAR-resistant, glucose intolerant, and have reduced glucose-stimulated insulin secretion. To investigate in vivo to what extent remaining AMPKα1 protein levels can substitute for AMPKα2, we performed an AICAR tolerance test. The relative insensitivity to hypoglycemia-mediated AICAR effects observed in AMPKα2 / mice (Figure 2a) suggests that AMPKα1 cannot fully compensate for the lack of AMPKα2 in AMPKα2 / mice. To investigate the dynamic response of AMPKα2 / mice to increased glucose concentrations, an oral glucose challenge was performed. Following glucose absorption, AMPKα2 / mice have a markedly increased blood glucose excursion, demonstrating glucose intolerance (Figure 2b). Insulinemia determined at time 20 minutes was significantly lower in AMPKα2 / mice (Figure 2c). Glucose- and L-arginine stimulated insulin secretion are normal in isolated pancreatic islets of AMPKα2 / mice. No significant difference in insulin release was observed between control and AMPKα2 / pancreatic islets for basal (3 mm glucose) and stimulatory glucose concentrations (7.5 mm, 10 mm, and 20 mm glucose) or when challenged with 20 mm L-arginine (Figure 3). Furthermore, the insulin content of AMPKα2 / and control islets was similar (67.2 ± 16.2 vs ± 16.5 ng/islet in controls; P not significant). AMPKα2 / mice are insulin resistant while Tg-KD- AMPKα2 mice are not. In the basal condition, endogenous glucose production, glycolysis rate, and wholebody glycogen synthesis rate were similar between AMPKα2 / and control mice (Table 3). In vivo muscle glycogen synthesis rate and total glycogen content were similar in both groups (Table 3). During hyperinsulinemic euglycemic clamp, plasma glucose and insulinemia were comparable in AMPKα2 / and control mice (plasma glucose: ± 7.2 mg/dl in AMPKα2 / mice vs ± 3.6 mg/dl in controls, P not significant; plasma insulin: ± 22.6 mu/l in AMPKα2 / mice vs ± 22.5 mu/l in controls, P not significant). Insulin-stimulated whole-body glucose turnover rate was decreased in AMPKα2 / mice compared with controls (Table 3). Insulin-stimulated whole-body glycolysis was similar in both groups, while the insulin-stimulated whole-body glycogen synthesis rate was dramatically decreased in AMPKα2 / mice (Table 3). Muscle glycogen synthesis rate and total muscle glycogen content were severely reduced in AMPKα2 / mice compared with controls at the end of the clamp (Table 3). Because glucose uptake is largely rate limiting for glycogen synthesis in muscle during clamp study, we assayed uptake of deoxyglucose into isolated muscle in the presence of insulin. Basal and insulin-stimulated glucose uptake were similar in isolated extensor digitorum longus and soleus muscles from controls and AMPKα2 / mice (Figure 4, a and b). In addition, total glycogen content in skeletal muscle of random-fed animals was similar between AMPKα2 / and control mice (0.312 ± vs ± µg/mg in controls, respectively, P not significant). Lastly, endogenous hepatic glucose production was totally inhibited in both groups, suggesting no hepatic insulin resistance (data not shown). Furthermore, no defect was detected in glycogen synthesis or total glycogen content in the liver of AMPKα2 / and control mice in either basal or clamp studies (data not shown). To further investigate the role of muscle AMPK in the development of insulin resistance, we performed hyperinsulinemic euglycemic clamps in transgenic mice expressing a kinase-dead mutant of AMPK in skeletal muscle (Tg-KD-AMPKα2 mice) and their respective nontransgenic controls (17). Oral glucose tolerance was comparable between the two groups (data not shown). During the clamp, plasma glucose Figure 3 Glucose- and L-arginine stimulated (L-Arg) insulin secretion in isolated AMPKα2 / islets. All results are expressed as mean ± SEM (n = 4). P not significant between groups by unpaired, two-tailed Student t test. The Journal of Clinical Investigation January 2003 Volume 111 Number 1 95
6 Table 3 Metabolic parameters of AMPKα2 / and Tg-KD-AMPKα2 mice during basal and hyperinsulinemic euglycemic clamp studies Weight Whole-body Whole-body Whole-body glycogen Muscle glycogen Muscle glycogen glucose turnover glycolysis rate synthesis rate synthesis rate content (g) (mg/kg/min) (mg/kg/min) (mg/kg/min) (ng/mg/min) (µg/mg) Basal Control 24.7 ± ± ± ± ± ± AMPKα2 / 24.7 ± ± ± ± ± ± Clamp Control 22.3 ± ± ± ± ± ± AMPKα2 / 21.4 ± ± 2.9 A 21.8 ± ± 2.9 A ± 17.0 A 0.137± B NTg 27.2 ± ± ± ± ± ± Tg-KD-AMPKα ± ± ± ± ± ± All data are expressed as mean ± SEM (n = 6 12 mice/group). A P < 0.01, B P < 0.05 vs. control group by unpaired, two-tailed Student t test. NTg, nontransgenic. and insulinemia were comparable in Tg-KD-AMPKα2 and nontransgenic mice (plasma glucose: 93.6 ± 1.8 mg/dl in Tg-KD-AMPKα2 mice vs ± 9.0 mg/dl in nontransgenic controls, P not significant; plasma insulin: ± 24.8 mu/l in Tg-KD-AMPKα2 mice vs ± 22.9 mu/l in nontransgenic controls, P not significant). Insulin-stimulated whole-body glucose turnover, whole-body glycogen synthesis rate, muscle glycogen synthesis rate, and total muscle glycogen content were similar in both groups (Table 3). Increased daily urinary catecholamine excretion in AMPKα2 / mice. Daily epinephrine, norepinephrine, and dopamine excretion were significantly higher in AMPKα2 / mice than in controls (Figure 5, a c). The response to a glucose challenge was dramatically improved in AMPKα2 / mice after treatment with α-adrenergic blockers, while no change was observed in control mice (Figure 5, d and e). In contrast, β-adrenergic blockers did not modify glucose tolerance of AMPKα2 / mice (Figure 5, d and e). Discussion The primary goal of this study was to assess the role of the AMPKα2 isoform in controlling glucose metabolism in vivo. AMPKα2 / mice appear indistinguishable from their control littermates. Importantly, there is no difference in body composition, adiposity, or food intake between mutant and control mice. The most striking observation is reduced glucose tolerance in AMPKα2 / mice. We showed that this defect is linked with both reduced insulin release and decreased insulin sensitivity of peripheral tissues. Few data are available concerning regulation of insulin release by AMPK. Activation of AMPK has been shown to inhibit insulin secretion in vitro (9, 10). Here, we showed that while glucose-induced insulin secretion is clearly impaired in AMPKα2 / mice in vivo, basal and glucose- and L-arginine stimulated insulin secretion in isolated pancreatic islets are similar in AMPKα2 / mice and controls. Furthermore, insulin content of islets and insulin gene transcription (data not shown) were not affected by AMPKα2 gene deletion. Taken together, these data indicate that the lack of insulin secretion observed in vivo in AMPKα2 / mice is not due to a primary defect in β cell function. Hypokalemia or hyperleptinemia (22), known to modulate insulin secretion negatively in vivo, are not observed in AMPKα2 / mice. In addition, lipid content in pancreas was similar in AMPKα2 / mice and controls, excluding a deleterious effect on insulin release by chronic accumulation of lipids (23, 24). An important regulator of insulin secretion is the fine-tuning of the balance between sympathetic and parasympathetic activity. This is critical for the β cells, since epinephrine and norepinephrine directly and potently suppress β cell function (25). AMPKα2 / mice exhibited higher catecholamine urinary excretion than did controls. Since catecholamines are known to inhibit insulin release, dysregulation in sympathetic tone observed in AMPKα2 / mice could be implicated in the reduction of insulin secretion. More importantly, no defect in glucose and insulin plasma levels was observed in mutant mice in the fasted state, suggesting that dysregulation of sympathetic tone is predominant in the fed period. Glucose intolerance is due to both impaired insulin secretion and reduced insulin-stimulated glucose utilization. Therefore, we examined insulin sensitivity in peripheral tissues of AMPKα2 / mice using hyperinsu- Figure 4 Insulin-stimulated glucose transport in isolated muscles from AMPKα2 / mice. Basal and insulin-stimulated glucose transport in (a) soleus and (b) extensor digitorum longus muscles from control and AMPKα2 / mice. All results are expressed as mean ± SEM (n = 4 7). *P < 0.05, **P < 0.01 vs. basal conditions by unpaired, two-tailed Student t test; P not significant (NS) vs. control group. 96 The Journal of Clinical Investigation January 2003 Volume 111 Number 1
7 linemic euglycemic clamp studies. To our surprise, AMPKα2 / mice displayed decreased whole-body insulin sensitivity, with a dramatic reduction in insulin-stimulated glycogen synthesis in skeletal muscle, while hepatic insulin sensitivity was preserved. Does α2 deletion in skeletal muscle directly alter insulin sensitivity? This does not seem to be the case since insulin sensitivity is unaltered in Tg-KD- AMPKα2 mice, which express a dominant-negative mutant of AMPK in skeletal muscle (17). This points out that lack of AMPK activity in skeletal muscle is unable by itself to alter insulin sensitivity or glycogen synthesis in this tissue. Likewise, comparable muscle glycogen contents of AMPKα2 / and control mice during the random-fed period suggest that the balance between degradation and repletion of glycogen in muscle is intact in this model. In consequence, a defect in muscular glycogen synthesis was specifically observed in AMPKα2 / mice when insulinemia reached supraphysiological levels. Glucose uptake is largely rate limiting for glycogen synthesis in muscle during clamp study. As insulin induced a similar increase in deoxyglucose uptake in incubated extensor digitorum longus and soleus muscles, it is unlikely that primary defective glucose transport in muscle contributes to AMPKα2 / insulin resistance. Another known important mechanism of insulin resistance in skeletal muscle is increased lipid availability or increased tissue uptake of FFA (26). AMPK regulates lipid oxidation in muscle by reducing ACC activity, which in turn decreases malonyl coenzyme A levels and increases mitochondrial uptake of FFAs. In AMPKα2 / gastrocnemius muscle, we showed that α1 protein was increased by 1.8-fold (Figure 1c) but ACC phosphorylation was reduced by 3.5-fold (Figure 1d). These data suggest that in skeletal muscle, the increased α1 protein levels in AMPKα2 / mice is not sufficient to ensure normal phosphorylation of ACC. However, the 24-hour respiratory quotient, monitored by indirect calorimetry, was similar in AMPKα2 / and control mice (data not shown), suggesting that whole-body lipid oxidation is not altered by the lack of the AMPKα2 subunit. Furthermore, comparable skeletal muscle lipid content in both groups argues against any alteration of lipid oxidation rate in AMPKα2 / mice. Finally, we know that adipose tissue operates as an endocrine organ that releases a large number of hormones in response to specific extracellular stimuli or changes in metabolic status. Alteration of secretion of these proteins (which include TNF-α, leptin, adipsin, resistin, and adiponectin) as a possible mechanism of AMPKα2 / mouse insulin resistance needs further investigation. So how can we explain insulin resistance in AMPKα2 / mice? The observation that AMPKα2 / mice exhibit altered glucose metabolism in vivo but not in isolated organs suggests that the defect is of central origin. It is known that integration of peripheral and central metabolic signals in the CNS during different metabolic situations such as fasting, fed state, and hyperinsulinemic clamp activates the autonomous nervous system, which in turn regulates glucose metabolism in peripheral tissues (27 30). As AMPKα2 is widely expressed in the brain (13), we hypothesized that lack of AMPKα2 in neurons could contribute to the metabolic defects observed in AMPKα2 / mice. Supporting this hypothesis, AMPKα2 / mice exhibited a significant increase in daily urinary catecholamine excretion, suggesting higher sympathetic activation in these mice. Furthermore, the glucose intolerance of AMPKα2 / mice was dramatically improved after intraperitoneal injection of phentolamine (an α-adrenergic receptor antagonist), while no change was observed after treatment of AMPKα2 / mice by propranolol (a β-adrenergic receptor antagonist). This suggested that the α-adrenergic but not the β-adrenergic pathway is involved in the glucose intolerance observed in AMPKα2 / mice. It is well known that epinephrine overproduction inhibits insulin secretion, reduces insulin-stimulated glucose uptake in skeletal muscles, and alters muscle glycogen synthesis (31 35); all of these defects are present in AMPKα2 / mice in vivo. Moreover, normality of some metabolic parameters (fasting glucose and insulin plasma levels or skeletal muscle glycogen content in random-fed animals) suggests that exaggerated sympathetic tone in AMPKα2 / mice is not permanent but is restricted to particular nutritional situations such as glucose challenge and hyperinsulinemic euglycemic clamps. Figure 5 Increased daily urinary catecholamine excretion in AMPKα2 / mice. Daily urinary (a) epinephrine, (b) norepinephrine, and (c) dopamine excretion in AMPKα2 / mice. All results are expressed as mean ± SEM (n = 6). *P < 0.05, **P < 0.01 vs. control group by unpaired, two-tailed t test. Also shown are effect of phentolamine and propranolol, α- and β-adrenergic blockers, respectively, on the response of glucose challenge of control (d) and AMPKα2 / (e) mice. All results are expressed as mean ± SEM (n = 5). *P < 0.05, **P < 0.01, saline- vs. phentolamine-treated group by unpaired, two-tailed Student t test; P not significant for saline- vs. propranolol-treated group. The Journal of Clinical Investigation January 2003 Volume 111 Number 1 97
8 The data presented here identify AMPKα2 as a major component in the control of insulin sensitivity and insulin secretion in vivo. We clearly demonstrated that the metabolic function of AMPKα2 / isolated skeletal muscle and pancreatic islets is normal, suggesting that the origin of the defects observed in vivo is located outside these tissues. In addition, we showed significant increased catecholamine excretion in AMPKα2 / mice. Thus, we hypothesize that lack of AMPKα2 in neurons reduces the ability to integrate peripheral metabolic signals into the brain and consequently alters the control of peripheral insulin sensitivity and insulin secretion by increasing sympathetic nervous activity. Acknowledgments We are grateful to A.K. Voss for the kind gift of embryonic stem cells. We thank D. Desmoulins (Cochin Hospital, Paris) for catecholamine measurement; M. Muffat-Joly and J. Bauchet (Centre d Explorations Fonctionnelles Intégré, Faculté de Médecine Xavier Bichat, Paris) for metabolic cage studies and determination of blood parameters; and C. Silve (Bichat Hospital) and GE Medical Systems for access to dual-energy x-ray absorptiometry. We appreciate assistance from D. Beaumont, T. Busnel, C. Postic, and A. Wood. This work was supported by INSERM, CNRS, the French Ministry for Research, the Danish National Research Foundation (grant ), and the European Commission (grant QLG1-CT ). F. Andreelli and S.B. Jørgensen were supported by postdoctoral fellowships from the European Commission, J.F.P. Wojtaszewski was supported by a postdoctoral fellowship from the Danish Medical Research Council, and G. Nicolas was supported by a postdoctoral fellowship from Aventis Laboratories. 1. Hardie, D.G., and Hawley, S.A AMP-activated protein kinase: the energy charge hypothesis revisited. Bioessays. 23: Hawley, S.A., et al Characterization of the AMP-activated protein kinase kinase from rat liver and identification of threonine 172 as the major site at which it phosphorylates AMP-activated protein kinase. J. Biol. Chem. 271: Hayashi, T., Hirshman, M.F., Kurth, E.J., Winder, W.W., and Goodyear, L.J Evidence for 5 AMP-activated protein kinase mediation of the effect of muscle contraction on glucose transport. Diabetes. 47: Bergeron, R., et al Effect of AMPK activation on muscle glucose metabolism in conscious rats. Am. J. Physiol. 276:E938 E Wojtaszewski, J.F., Jorgensen, S.B., Hellsten, Y., Hardie, D.G., and Richter, E.A Glycogen-dependent effects of 5-aminoimidazole-4-carboxamide (AICA)-riboside on AMP-activated protein kinase and glycogen synthase activities in rat skeletal muscle. Diabetes. 51: Vincent, M.F., Marangos, P.J., Gruber, H.E., and Van den Berghe, G Inhibition by AICA riboside of gluconeogenesis in isolated rat hepatocytes. Diabetes. 40: Bergeron, R., et al Effect of 5-aminoimidazole-4-carboxamide-1- beta-d-ribofuranoside infusion on in vivo glucose and lipid metabolism in lean and obese Zucker rats. Diabetes. 50: Zhou, G., et al Role of AMP-activated protein kinase in mechanism of metformin action. J. Clin. Invest. 108: doi: /jci Salt, I.P., Johnson, G., Ashcroft, S.J., and Hardie, D.G AMP-activated protein kinase is activated by low glucose in cell lines derived from pancreatic beta cells, and may regulate insulin release. Biochem. J. 335: Kowluru, A., Chen, H.Q., Modrick, L.M., and Stefanelli, C Activation of acetyl-coa carboxylase by a glutamate- and magnesium-sensitive protein phosphatase in the islet beta-cell. Diabetes. 50: Sullivan, J.E., et al Inhibition of lipolysis and lipogenesis in isolated rat adipocytes with AICAR, a cell-permeable activator of AMP-activated protein kinase. FEBS Lett. 353: Corton, J.M., Gillespie, J.G., Hawley, S.A., and Hardie, D.G aminoimidazole-4-carboxamide ribonucleoside. A specific method for activating AMP-activated protein kinase in intact cells? Eur. J. Biochem. 229: Turnley, A.M., et al Cellular distribution and developmental expression of AMP-activated protein kinase isoforms in mouse central nervous system. J. Neurochem. 72: Vavvas, D., et al Contraction-induced changes in acetyl-coa carboxylase and 5 -AMP-activated kinase in skeletal muscle. J. Biol. Chem. 272: Musi, N., et al AMP-activated protein kinase activity and glucose uptake in rat skeletal muscle. Am. J. Physiol. Endocrinol. Metab. 280:E677 E Holzenberger, M., et al Cre-mediated germline mosaicism: a method allowing rapid generation of several alleles of a target gene. Nucleic Acids Res. 28:E Mu, J., Brozinick, J.T., Jr., Valladares, O., Bucan, M., and Birnbaum, M.J A role for AMP-activated protein kinase in contraction- and hypoxia-regulated glucose transport in skeletal muscle. Mol. Cell. 7: Burcelin, R., Crivelli, V., DaCosta, A., Roy-Tirelli, A., and Thorens, B Heterogeneous metabolic adaptation of C57BL/6J mice to highfat diet. Am. J. Physiol. 282:E834 E Burcelin, R., et al Excessive glucose production, rather than insulin resistance, accounts for hyperglycaemia in recent-onset streptozotocin-diabetic rats. Diabetologia. 38: Massillon, D., et al Quantitation of hepatic glucose fluxes and pathways of hepatic glycogen synthesis in conscious mice. Am. J. Physiol. 269:E1037 E Flamez, D., et al Mouse pancreatic beta-cells exhibit preserved glucose competence after disruption of the glucagon-like peptide-1 receptor gene. Diabetes. 47: Koyama, K., et al Beta-cell function in normal rats made chronically hyperleptinemic by adenovirus-leptin gene therapy. Diabetes. 46: Zhou, Y.P., and Grill, V.E Long-term exposure of rat pancreatic islets to fatty acids inhibits glucose-induced insulin secretion and biosynthesis through a glucose fatty acid cycle. J. Clin. Invest. 93: Paolisso, G., et al Opposite effects of short- and long-term fatty acid infusion on insulin secretion in healthy subjects. Diabetologia. 38: Schuit, F.C., and Pipeleers, D.G Differences in adrenergic recognition by pancreatic A and B cells. Science. 232: McGarry, J.D Banting lecture 2001: dysregulation of fatty acid metabolism in the etiology of type 2 diabetes. Diabetes. 51: Kamohara, S., Burcelin, R., Halaas, J.L., Friedman, J.M., and Charron, M.J Acute stimulation of glucose metabolism in mice by leptin treatment. Nature. 389: Burcelin, R., Dolci, W., and Thorens, B Portal glucose infusion in the mouse induces hypoglycemia. Evidence that the hepatoportal glucose sensor stimulates glucose utilization. Diabetes. 49: Obici, S., et al Central melanocortin receptors regulate insulin action. J. Clin. Invest. 108: doi: /jci Yoshimatsu, H., Oomura, Y., Katafuchi, T., Niijima, A., and Sato, A Lesions of the ventromedial hypothalamic nucleus enhance sympathoadrenal function. Brain Res. 339: Exton, J.H Mechanisms involved in alpha-adrenergic phenomena: role of calcium ions in actions of catecholamines in liver and other tissues. Am. J. Physiol. 238:E3 E Haynes, W.G., Morgan, D.A., Walsh, S.A., Mark, A.L., and Sivitz, W.I Receptor-mediated regional sympathetic nerve activation by leptin. J. Clin. Invest. 100: Nonogaki, K New insights into sympathetic regulation of glucose and fat metabolism. Diabetologia. 43: Marfaing, P., et al Effects of counterregulatory hormones on insulin-induced glucose utilization by individual tissues in rats. Diabetes Metab. 17: Chiasson, J.L., Shikama, H., Chu, D.T., and Exton, J.H Inhibitory effect of epinephrine on insulin-stimulated glucose uptake by rat skeletal muscle. J. Clin. Invest. 68: The Journal of Clinical Investigation January 2003 Volume 111 Number 1
Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus
 Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Emerging Science Role of fatty acids in the development of insulin resistance and type 2 diabetes mellitus George Wolf Insulin resistance is defined as the reduced responsiveness to normal circulating
Hormonal regulation of. Physiology Department Medical School, University of Sumatera Utara
 Hormonal regulation of nutrient metabolism Physiology Department Medical School, University of Sumatera Utara Homeostasis & Controls Successful compensation Homeostasis reestablished Failure to compensate
Hormonal regulation of nutrient metabolism Physiology Department Medical School, University of Sumatera Utara Homeostasis & Controls Successful compensation Homeostasis reestablished Failure to compensate
Metformin inhibits hepatic gluconeogenesis in mice independently of the LKB1/AMPK pathway via a decrease in hepatic energy state
 Related Commentary, page 2267 Research article Metformin inhibits hepatic gluconeogenesis in mice independently of the LKB1/AMPK pathway via a decrease in hepatic energy state Marc Foretz, 1,2 Sophie Hébrard,
Related Commentary, page 2267 Research article Metformin inhibits hepatic gluconeogenesis in mice independently of the LKB1/AMPK pathway via a decrease in hepatic energy state Marc Foretz, 1,2 Sophie Hébrard,
Final Review Sessions. 3/16 (FRI) 126 Wellman (4-6 6 pm) 3/19 (MON) 1309 Surge 3 (4-6 6 pm) Office Hours
 Final Review Sessions 3/16 (FRI) 126 Wellman (4-6 6 pm) 3/19 (MON) 1309 Surge 3 (4-6 6 pm) Office ours 3/14 (WED) 9:30 11:30 am (Rebecca) 3/16 (FRI) 9-11 am (Abel) Final ESSENTIALS Posted Lecture 20 ormonal
Final Review Sessions 3/16 (FRI) 126 Wellman (4-6 6 pm) 3/19 (MON) 1309 Surge 3 (4-6 6 pm) Office ours 3/14 (WED) 9:30 11:30 am (Rebecca) 3/16 (FRI) 9-11 am (Abel) Final ESSENTIALS Posted Lecture 20 ormonal
BIOL212 Biochemistry of Disease. Metabolic Disorders - Obesity
 BIOL212 Biochemistry of Disease Metabolic Disorders - Obesity Obesity Approx. 23% of adults are obese in the U.K. The number of obese children has tripled in 20 years. 10% of six year olds are obese, rising
BIOL212 Biochemistry of Disease Metabolic Disorders - Obesity Obesity Approx. 23% of adults are obese in the U.K. The number of obese children has tripled in 20 years. 10% of six year olds are obese, rising
UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS An Overview WHAT IS HOMEOSTASIS? Homeostasis
ENERGY FROM INGESTED NUTREINTS MAY BE USED IMMEDIATELY OR STORED
 QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
QUIZ/TEST REVIEW NOTES SECTION 1 SHORT TERM METABOLISM [METABOLISM] Learning Objectives: Identify primary energy stores of the body Differentiate the metabolic processes of the fed and fasted states Explain
AMPK. Tomáš Kučera.
 AMPK (AMP- ACTIVATED PROTEIN KINASE ) Tomáš Kučera tomas.kucera@lfmotol.cuni.cz Department of Medical Chemistry and Clinical Biochemistry 2nd Faculty of Medicine, Charles University in Prague and Motol
AMPK (AMP- ACTIVATED PROTEIN KINASE ) Tomáš Kučera tomas.kucera@lfmotol.cuni.cz Department of Medical Chemistry and Clinical Biochemistry 2nd Faculty of Medicine, Charles University in Prague and Motol
Modifications of Pyruvate Handling in Health and Disease Prof. Mary Sugden
 Modifications of Handling Modifications of Handling Centre for Diabetes and Metabolic Medicine Institute of Cell and Molecular Science Barts and the London School of Medicine and Dentistry 1 Potential
Modifications of Handling Modifications of Handling Centre for Diabetes and Metabolic Medicine Institute of Cell and Molecular Science Barts and the London School of Medicine and Dentistry 1 Potential
SUPPLEMENTARY INFORMATION
 Supplementary Figures Supplementary Figure S1. Binding of full-length OGT and deletion mutants to PIP strips (Echelon Biosciences). Supplementary Figure S2. Binding of the OGT (919-1036) fragments with
Supplementary Figures Supplementary Figure S1. Binding of full-length OGT and deletion mutants to PIP strips (Echelon Biosciences). Supplementary Figure S2. Binding of the OGT (919-1036) fragments with
Metabolism of cardiac muscle. Dr. Mamoun Ahram Cardiovascular system, 2013
 Metabolism of cardiac muscle Dr. Mamoun Ahram Cardiovascular system, 2013 References This lecture Mark s Basic Medical Biochemistry, 4 th ed., p. 890-891 Hand-out Why is this topic important? Heart failure
Metabolism of cardiac muscle Dr. Mamoun Ahram Cardiovascular system, 2013 References This lecture Mark s Basic Medical Biochemistry, 4 th ed., p. 890-891 Hand-out Why is this topic important? Heart failure
7/31/2009. G.Y. Prince Used Cars 10 am Los Angelos, CA Mullholland Drive..later that day. Would you buy a car without taking it for a spin first?
 7/31/29 My Anna will love it! Who needs a test drive? Or a Warranty? It looked great in the lot! Do mean to say that you never actually test drove the car? G.Y. Prince Used Cars 1 am Los Angelos, CA Mullholland
7/31/29 My Anna will love it! Who needs a test drive? Or a Warranty? It looked great in the lot! Do mean to say that you never actually test drove the car? G.Y. Prince Used Cars 1 am Los Angelos, CA Mullholland
What systems are involved in homeostatic regulation (give an example)?
 1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
1 UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DIVISION OF BASIC MEDICAL SCIENCES DISCIPLINE OF BIOCHEMISTRY AND MOLECULAR BIOLOGY GLUCOSE HOMEOSTASIS (Diabetes Mellitus Part 1): An Overview
Week 3 The Pancreas: Pancreatic ph buffering:
 Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
Week 3 The Pancreas: A gland with both endocrine (secretion of substances into the bloodstream) & exocrine (secretion of substances to the outside of the body or another surface within the body) functions
AMPK Phosphorylation Assay Kit
 AMPK Phosphorylation Assay Kit Catalog Number KA3789 100 assays Version: 02 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle
AMPK Phosphorylation Assay Kit Catalog Number KA3789 100 assays Version: 02 Intended for research use only www.abnova.com Table of Contents Introduction... 3 Intended Use... 3 Background... 3 Principle
Supplementary Figure 1. DJ-1 modulates ROS concentration in mouse skeletal muscle.
 Supplementary Figure 1. DJ-1 modulates ROS concentration in mouse skeletal muscle. (a) mrna levels of Dj1 measured by quantitative RT-PCR in soleus, gastrocnemius (Gastroc.) and extensor digitorum longus
Supplementary Figure 1. DJ-1 modulates ROS concentration in mouse skeletal muscle. (a) mrna levels of Dj1 measured by quantitative RT-PCR in soleus, gastrocnemius (Gastroc.) and extensor digitorum longus
AMPK. Tomáš Kuc era. Ústav lékar ské chemie a klinické biochemie 2. lékar ská fakulta, Univerzita Karlova v Praze
 AMPK (AMP- ACTIVATED PROTEIN KINASE ) Tomáš Kuc era Ústav lékar ské chemie a klinické biochemie 2. lékar ská fakulta, Univerzita Karlova v Praze 2013 AMPK AMP-ACTIVATED PROTEIN KINASE present in all eukaryotic
AMPK (AMP- ACTIVATED PROTEIN KINASE ) Tomáš Kuc era Ústav lékar ské chemie a klinické biochemie 2. lékar ská fakulta, Univerzita Karlova v Praze 2013 AMPK AMP-ACTIVATED PROTEIN KINASE present in all eukaryotic
Supplementary Information. Glycogen shortage during fasting triggers liver-brain-adipose. neurocircuitry to facilitate fat utilization
 Supplementary Information Glycogen shortage during fasting triggers liver-brain-adipose neurocircuitry to facilitate fat utilization Supplementary Figure S1. Liver-Brain-Adipose neurocircuitry Starvation
Supplementary Information Glycogen shortage during fasting triggers liver-brain-adipose neurocircuitry to facilitate fat utilization Supplementary Figure S1. Liver-Brain-Adipose neurocircuitry Starvation
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM
 5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
5.0 HORMONAL CONTROL OF CARBOHYDRATE METABOLISM Introduction: Variety of hormones and other molecules regulate the carbohydrates metabolism. Some of these have already been cited in previous sections.
THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals
 Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Br. J. Anaesth. (1981), 53, 131 THE GLUCOSE-FATTY ACID-KETONE BODY CYCLE Role of ketone bodies as respiratory substrates and metabolic signals J. C. STANLEY In this paper, the glucose-fatty acid cycle
Role of the ventromedial hypothalamic Steroidogenic Factor 1/ Adrenal 4. glucose metabolism in mice.
 Role of the ventromedial hypothalamic Steroidogenic Factor 1/ Adrenal 4 Binding Protein neurons in the regulation of whole body energy and glucose metabolism in mice. Eulalia Coutinho Department of Physiological
Role of the ventromedial hypothalamic Steroidogenic Factor 1/ Adrenal 4 Binding Protein neurons in the regulation of whole body energy and glucose metabolism in mice. Eulalia Coutinho Department of Physiological
Supplementary Information
 Supplementary Information Akt regulates hepatic metabolism by suppressing a Foxo1 dependent global inhibition of adaptation to nutrient intake Mingjian Lu 1, Min Wan 1, Karla F. Leavens 1, Qingwei Chu
Supplementary Information Akt regulates hepatic metabolism by suppressing a Foxo1 dependent global inhibition of adaptation to nutrient intake Mingjian Lu 1, Min Wan 1, Karla F. Leavens 1, Qingwei Chu
For pair feeding, mice were fed 2.7g of HFD containing tofogliflozin
 Materials and Methods Pair Feeding Experiment For pair feeding, mice were fed 2.7g of HFD containing tofogliflozin (0.005%), which is average daily food intake of mice fed control HFD ad libitum at week
Materials and Methods Pair Feeding Experiment For pair feeding, mice were fed 2.7g of HFD containing tofogliflozin (0.005%), which is average daily food intake of mice fed control HFD ad libitum at week
BALANCING THE SCALES USING A NOVEL CELLULAR ENERGY SENSOR
 The West London Medical Journal 2010 Vol 2 No 4 pp 29-35 BALANCING THE SCALES USING A NOVEL CELLULAR ENERGY SENSOR Sairah Akbar The topic of obesity is rarely out of the public eye with an increasingly
The West London Medical Journal 2010 Vol 2 No 4 pp 29-35 BALANCING THE SCALES USING A NOVEL CELLULAR ENERGY SENSOR Sairah Akbar The topic of obesity is rarely out of the public eye with an increasingly
18. PANCREATIC FUNCTION AND METABOLISM. Pancreatic secretions ISLETS OF LANGERHANS. Insulin
 18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
18. PANCREATIC FUNCTION AND METABOLISM ISLETS OF LANGERHANS Some pancreatic functions have already been discussed in the digestion section. In this one, the emphasis will be placed on the endocrine function
AMPK as a metabolic switch in rat muscle, liver and adipose tissue after exercise
 Acta Physiol Scand 23, 78, 43 442 AMPK as a metabolic switch in rat muscle, liver and adipose tissue after exercise N. B. Ruderman, H. Park, V. K. Kaushik, D. Dean, S. Constant, M. Prentki 2 and A. K.
Acta Physiol Scand 23, 78, 43 442 AMPK as a metabolic switch in rat muscle, liver and adipose tissue after exercise N. B. Ruderman, H. Park, V. K. Kaushik, D. Dean, S. Constant, M. Prentki 2 and A. K.
Integration Of Metabolism
 Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Integration Of Metabolism Metabolism Consist of Highly Interconnected Pathways The basic strategy of catabolic metabolism is to form ATP, NADPH, and building blocks for biosyntheses. 1. ATP is the universal
Energy metabolism - the overview
 Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
Energy metabolism - the overview Josef Fontana EC - 40 Overview of the lecture Important terms of the energy metabolism The overview of the energy metabolism The main pathways of the energy metabolism
Glucose. Glucose. Insulin Action. Introduction to Hormonal Regulation of Fuel Metabolism
 Glucose Introduction to Hormonal Regulation of Fuel Metabolism Fasting level 3.5-5 mmol (1 mmol = 18 mg/dl) Postprandial 6-10 mmol Amount of glucose in circulation is dependent on: Absorption from the
Glucose Introduction to Hormonal Regulation of Fuel Metabolism Fasting level 3.5-5 mmol (1 mmol = 18 mg/dl) Postprandial 6-10 mmol Amount of glucose in circulation is dependent on: Absorption from the
Overall Energy metabolism: Integration and Regulation
 Overall Energy metabolism: Integration and Regulation We have discussed various fuels which are oxidized via different catabolic pathways to generate ATP, or reducing equivalents required to carry out
Overall Energy metabolism: Integration and Regulation We have discussed various fuels which are oxidized via different catabolic pathways to generate ATP, or reducing equivalents required to carry out
Intermediary metabolism. Eva Samcová
 Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
Intermediary metabolism Eva Samcová Metabolic roles of tissues Four major tissues play a dominant role in fuel metabolism : liver, adipose, muscle, and brain. These tissues do not function in isolation.
SUPPLEMENTARY DATA. Supplementary Table 1. Primers used in qpcr
 Supplementary Table 1. Primers used in qpcr Gene forward primer (5'-3') reverse primer (5'-3') β-actin AGAGGGAAATCGTGCGTGAC CAATAGTGATGACCTGGCCGT Hif-p4h-2 CTGGGCAACTACAGGATAAAC GCGTCCCAGTCTTTATTTAGATA
Supplementary Table 1. Primers used in qpcr Gene forward primer (5'-3') reverse primer (5'-3') β-actin AGAGGGAAATCGTGCGTGAC CAATAGTGATGACCTGGCCGT Hif-p4h-2 CTGGGCAACTACAGGATAAAC GCGTCCCAGTCTTTATTTAGATA
Integrative Metabolism: Significance
 Integrative Metabolism: Significance Energy Containing Nutrients Carbohydrates Fats Proteins Catabolism Energy Depleted End Products H 2 O NH 3 ADP + Pi NAD + NADP + FAD + Pi NADH+H + NADPH+H + FADH2 Cell
Integrative Metabolism: Significance Energy Containing Nutrients Carbohydrates Fats Proteins Catabolism Energy Depleted End Products H 2 O NH 3 ADP + Pi NAD + NADP + FAD + Pi NADH+H + NADPH+H + FADH2 Cell
EFFECTS OF VANADATE ON OLEIC ACID INDUCED INSULIN RESISTANCE IN CULTURED RAT HEPATOCYTES
 1 Department of Physiology, School of Dentistry, University of Zagreb, Gunduliæeva 5, HR-1 Zagreb, Croatia Department of Physiology, School of Medicine, University of Zagreb, Šalata 3, HR-1 Zagreb, Croatia
1 Department of Physiology, School of Dentistry, University of Zagreb, Gunduliæeva 5, HR-1 Zagreb, Croatia Department of Physiology, School of Medicine, University of Zagreb, Šalata 3, HR-1 Zagreb, Croatia
(Stratagene, La Jolla, CA) (Supplemental Fig. 1A). A 5.4-kb EcoRI fragment
 SUPPLEMENTAL INFORMATION Supplemental Methods Generation of RyR2-S2808D Mice Murine genomic RyR2 clones were isolated from a 129/SvEvTacfBR λ-phage library (Stratagene, La Jolla, CA) (Supplemental Fig.
SUPPLEMENTAL INFORMATION Supplemental Methods Generation of RyR2-S2808D Mice Murine genomic RyR2 clones were isolated from a 129/SvEvTacfBR λ-phage library (Stratagene, La Jolla, CA) (Supplemental Fig.
Medical Biochemistry and Molecular Biology department
 Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
Medical Biochemistry and Molecular Biology department Cardiac Fuels [Sources of energy for the Cardiac muscle] Intended learning outcomes of the lecture: By the end of this lecture you would be able to:-
Regulation of Metabolism
 Regulation of Metabolism Pratt and Cornely Chapter 19 Regulation by Compartmentalization Form of reciprocal regulation Degradation vs biosynthesis Requires transporters 1 Specialization of organs Fuel
Regulation of Metabolism Pratt and Cornely Chapter 19 Regulation by Compartmentalization Form of reciprocal regulation Degradation vs biosynthesis Requires transporters 1 Specialization of organs Fuel
INSULIN RESISTANCE: MOLECULAR MECHANISM
 INSULIN RESISTANCE: MOLECULAR MECHANISM Ashish K. Saha ABSTRACT Insulin resistance in skeletal muscle is present in humans with type 2 diabetes (non-insulin dependent diabetes mellitus) and obesity and
INSULIN RESISTANCE: MOLECULAR MECHANISM Ashish K. Saha ABSTRACT Insulin resistance in skeletal muscle is present in humans with type 2 diabetes (non-insulin dependent diabetes mellitus) and obesity and
Metabolic integration and Regulation
 Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
Metabolic integration and Regulation 109700: Graduate Biochemistry Trimester 2/2016 Assistant Prof. Dr. Panida Khunkaewla kpanida@sut.ac.th School of Chemistry Suranaree University of Technology 1 Overview
Insulin Resistance. Biol 405 Molecular Medicine
 Insulin Resistance Biol 405 Molecular Medicine Insulin resistance: a subnormal biological response to insulin. Defects of either insulin secretion or insulin action can cause diabetes mellitus. Insulin-dependent
Insulin Resistance Biol 405 Molecular Medicine Insulin resistance: a subnormal biological response to insulin. Defects of either insulin secretion or insulin action can cause diabetes mellitus. Insulin-dependent
Hormones. Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6
 Hormones Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6 Tel. 030-8385-6920 (Sekret.) 030-8385-6922 (direkt) e-mail: vhaucke@chemie.fu-berlin.de http://userpage.chemie.fu-berlin.de/biochemie/aghaucke/teaching.html
Hormones Prof. Dr. Volker Haucke Institut für Chemie-Biochemie Takustrasse 6 Tel. 030-8385-6920 (Sekret.) 030-8385-6922 (direkt) e-mail: vhaucke@chemie.fu-berlin.de http://userpage.chemie.fu-berlin.de/biochemie/aghaucke/teaching.html
PKC-θ knockout mice are protected from fat-induced insulin resistance
 Research article PKC-θ knockout mice are protected from fat-induced insulin resistance Jason K. Kim, 1 Jonathan J. Fillmore, 1 Mary Jean Sunshine, 2 Bjoern Albrecht, 2 Takamasa Higashimori, 1 Dong-Wook
Research article PKC-θ knockout mice are protected from fat-induced insulin resistance Jason K. Kim, 1 Jonathan J. Fillmore, 1 Mary Jean Sunshine, 2 Bjoern Albrecht, 2 Takamasa Higashimori, 1 Dong-Wook
History of Investigation
 Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
Acini - Pancreatic juice (1º) (2º) Secretions- neuronal and hormonal mechanisms 1) Secretin - bicarbonate rich 2) Cholecystokinin - enzyme rich Islets of Langerhans (contain 4 cell types) Alpha cells (α)-
Requires Signaling though Akt2 Independent of the. Transcription Factors FoxA2, FoxO1, and SREBP1c
 Cell Metabolism, Volume 14 Supplemental Information Postprandial Hepatic Lipid Metabolism Requires Signaling though Akt2 Independent of the Transcription Factors FoxA2, FoxO1, and SREBP1c Min Wan, Karla
Cell Metabolism, Volume 14 Supplemental Information Postprandial Hepatic Lipid Metabolism Requires Signaling though Akt2 Independent of the Transcription Factors FoxA2, FoxO1, and SREBP1c Min Wan, Karla
GPR120 *** * * Liver BAT iwat ewat mwat Ileum Colon. UCP1 mrna ***
 a GPR120 GPR120 mrna/ppia mrna Arbitrary Units 150 100 50 Liver BAT iwat ewat mwat Ileum Colon b UCP1 mrna Fold induction 20 15 10 5 - camp camp SB202190 - - - H89 - - - - - GW7647 Supplementary Figure
a GPR120 GPR120 mrna/ppia mrna Arbitrary Units 150 100 50 Liver BAT iwat ewat mwat Ileum Colon b UCP1 mrna Fold induction 20 15 10 5 - camp camp SB202190 - - - H89 - - - - - GW7647 Supplementary Figure
anabolic pathways- Catabolic Amphibolic
 METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
METABOLISM Introduction The fate of dietary components after digestion and absorption constitute metabolism regulated by metabolic pathway 3 types: anabolic pathways- Synthesis of compound e.g. synthesis
NUTRITION & MALIGNANCY: An Overview
 NUTRITION & MALIGNANCY: An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ Temple 1 Malignancy and Weight loss (Cachexia)
NUTRITION & MALIGNANCY: An Overview UNIVERSITY OF PNG SCHOOL OF MEDICINE AND HEALTH SCIENCES DISCIPLINE OF BIOCHEMISTRY & MOLECULAR BIOLOGY PBL MBBS II SEMINAR VJ Temple 1 Malignancy and Weight loss (Cachexia)
Pathogenesis of Diabetes Mellitus
 Pathogenesis of Diabetes Mellitus Young-Bum Kim, Ph.D. Associate Professor of Medicine Harvard Medical School Definition of Diabetes Mellitus a group of metabolic diseases characterized by hyperglycemia
Pathogenesis of Diabetes Mellitus Young-Bum Kim, Ph.D. Associate Professor of Medicine Harvard Medical School Definition of Diabetes Mellitus a group of metabolic diseases characterized by hyperglycemia
9.3 Stress Response and Blood Sugar
 9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
9.3 Stress Response and Blood Sugar Regulate Stress Response Regulate Blood Sugar Stress Response Involves hormone pathways that regulate metabolism, heart, rate and breathing The Adrenal Glands a pair
Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS
 Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS Alternate Fuel Sources When glucose levels are low Proteins and Triglycerides will be metabolized Tissues will use different fuel sources depending on:
Physiology Unit 1 METABOLISM OF LIPIDS AND PROTEINS Alternate Fuel Sources When glucose levels are low Proteins and Triglycerides will be metabolized Tissues will use different fuel sources depending on:
SUPPLEMENTARY INFORMATION
 SUPPLEMENTARY INFORMATION doi:10.1038/nature11464 Supplemental Figure S1. The expression of Vegfb is increased in obese and diabetic mice as compared to lean mice. a-b, Body weight and postprandial blood
SUPPLEMENTARY INFORMATION doi:10.1038/nature11464 Supplemental Figure S1. The expression of Vegfb is increased in obese and diabetic mice as compared to lean mice. a-b, Body weight and postprandial blood
Central insulin action regulates peripheral glucose and fat metabolism in mice
 Research article Central insulin action regulates peripheral glucose and fat metabolism in mice Linda Koch, 1 F. Thomas Wunderlich, 1 Jost Seibler, 2 A. Christine Könner, 1 Brigitte Hampel, 1 Sigrid Irlenbusch,
Research article Central insulin action regulates peripheral glucose and fat metabolism in mice Linda Koch, 1 F. Thomas Wunderlich, 1 Jost Seibler, 2 A. Christine Könner, 1 Brigitte Hampel, 1 Sigrid Irlenbusch,
Integration of Metabolism
 Integration of Metabolism Metabolism is a continuous process. Thousands of reactions occur simultaneously in order to maintain homeostasis. It ensures a supply of fuel, to tissues at all times, in fed
Integration of Metabolism Metabolism is a continuous process. Thousands of reactions occur simultaneously in order to maintain homeostasis. It ensures a supply of fuel, to tissues at all times, in fed
Supplementary Information
 Supplementary Information Overexpression of Fto leads to increased food intake and results in obesity Chris Church, Lee Moir, Fiona McMurray, Christophe Girard, Gareth T Banks, Lydia Teboul, Sara Wells,
Supplementary Information Overexpression of Fto leads to increased food intake and results in obesity Chris Church, Lee Moir, Fiona McMurray, Christophe Girard, Gareth T Banks, Lydia Teboul, Sara Wells,
CARBOHYDRATE METABOLISM 1
 CARBOHYDRATE METABOLISM 1 web 2017 József Mandl Strategy of metabolism 1 Strategy of metabolism to extract energy ( hydrogen ) from the environment to store the energy excess to store hydrogen CH 3 O 2
CARBOHYDRATE METABOLISM 1 web 2017 József Mandl Strategy of metabolism 1 Strategy of metabolism to extract energy ( hydrogen ) from the environment to store the energy excess to store hydrogen CH 3 O 2
Integration & Hormone Regulation
 Integration Branchpoints in metabolism where metabolites can go several directions 1. Glucose 6-phosphate Energy needed (low energy charge): glycolysis Low blood sugar: high [glucagon], low [insulin] glycogen
Integration Branchpoints in metabolism where metabolites can go several directions 1. Glucose 6-phosphate Energy needed (low energy charge): glycolysis Low blood sugar: high [glucagon], low [insulin] glycogen
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1
 GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
GENERAL CHARACTERISTICS OF THE ENDOCRINE SYSTEM FIGURE 17.1 1. The endocrine system consists of glands that secrete chemical signals, called hormones, into the blood. In addition, other organs and cells
In The Name Of God. In The Name Of. EMRI Modeling Group
 In The Name Of God In The Name Of God EMRI Modeling Group Cells work together in functionally related groups called tissues Types of tissues: Epithelial lining and covering Connective support Muscle movement
In The Name Of God In The Name Of God EMRI Modeling Group Cells work together in functionally related groups called tissues Types of tissues: Epithelial lining and covering Connective support Muscle movement
AdPLA ablation increases lipolysis and prevents obesity induced by high fat feeding or leptin deficiency
 AdPLA AdPLA ablation increases lipolysis and prevents obesity induced by high fat feeding or leptin deficiency Kathy Jaworski, Maryam Ahmadian, Robin E. Duncan, Eszter Sarkadi-Nagy, Krista A. Va rady,
AdPLA AdPLA ablation increases lipolysis and prevents obesity induced by high fat feeding or leptin deficiency Kathy Jaworski, Maryam Ahmadian, Robin E. Duncan, Eszter Sarkadi-Nagy, Krista A. Va rady,
Glycolysis. Intracellular location Rate limiting steps
 Glycolysis Definition Fx Fate Site Intracellular location Rate limiting steps Regulation Consume ATP Subs level phosphoryla tion Key reactions control points Nb Oxidation of glucose to give pyruvate (
Glycolysis Definition Fx Fate Site Intracellular location Rate limiting steps Regulation Consume ATP Subs level phosphoryla tion Key reactions control points Nb Oxidation of glucose to give pyruvate (
Metabolism of acylglycerols and sphingolipids. Martina Srbová
 Metabolism of acylglycerols and sphingolipids Martina Srbová Types of glycerolipids and sphingolipids 1. Triacylglycerols function as energy reserves adipose tissue (storage of triacylglycerol), lipoproteins
Metabolism of acylglycerols and sphingolipids Martina Srbová Types of glycerolipids and sphingolipids 1. Triacylglycerols function as energy reserves adipose tissue (storage of triacylglycerol), lipoproteins
Supplemental Information. Increased 4E-BP1 Expression Protects. against Diet-Induced Obesity and Insulin. Resistance in Male Mice
 Cell Reports, Volume 16 Supplemental Information Increased 4E-BP1 Expression Protects against Diet-Induced Obesity and Insulin Resistance in Male Mice Shih-Yin Tsai, Ariana A. Rodriguez, Somasish G. Dastidar,
Cell Reports, Volume 16 Supplemental Information Increased 4E-BP1 Expression Protects against Diet-Induced Obesity and Insulin Resistance in Male Mice Shih-Yin Tsai, Ariana A. Rodriguez, Somasish G. Dastidar,
PXL770, a novel direct AMPK activator, improves metabolic disorders in a diet-induced mice model of obesity and diabetes
 PXL770, a novel direct AMPK activator, improves metabolic disorders in a diet-induced mice model of obesity and diabetes Sébastien Bolze 1 ; Sophie Hallakou-Bozec 1 ; Michael Roden 2, 3,4 ; Julien Roux
PXL770, a novel direct AMPK activator, improves metabolic disorders in a diet-induced mice model of obesity and diabetes Sébastien Bolze 1 ; Sophie Hallakou-Bozec 1 ; Michael Roden 2, 3,4 ; Julien Roux
Therapy: Metformin takes a new route to clinical
 Therapy: Metformin takes a new route to clinical efficacy. Marc Foretz, Benoit Viollet To cite this version: Marc Foretz, Benoit Viollet. Therapy: Metformin takes a new route to clinical efficacy.. Nature
Therapy: Metformin takes a new route to clinical efficacy. Marc Foretz, Benoit Viollet To cite this version: Marc Foretz, Benoit Viollet. Therapy: Metformin takes a new route to clinical efficacy.. Nature
Role of the Pyruvate
 Role of the Pyruvate Dehydrogenase Complex in the Regulation of Blood Glucose Robert A. Harris Indiana University School of Medicine Indianapolis, Indiana Kyungpook National University School of Medicine
Role of the Pyruvate Dehydrogenase Complex in the Regulation of Blood Glucose Robert A. Harris Indiana University School of Medicine Indianapolis, Indiana Kyungpook National University School of Medicine
Adrenal Hormone Mineralocorticoids Aldosterone
 Adrenal gland Adrenal Hormone Mineralocorticoids Aldosterone Cortex 80 % Glucocorticoids Cortisol Sex hormones Androgen Medulla 20% Catecholamines E, NE 1 2 Adrenal cortex hormones Glucocorticoid Mineralocorticoids
Adrenal gland Adrenal Hormone Mineralocorticoids Aldosterone Cortex 80 % Glucocorticoids Cortisol Sex hormones Androgen Medulla 20% Catecholamines E, NE 1 2 Adrenal cortex hormones Glucocorticoid Mineralocorticoids
General Laboratory methods Plasma analysis: Gene Expression Analysis: Immunoblot analysis: Immunohistochemistry:
 General Laboratory methods Plasma analysis: Plasma insulin (Mercodia, Sweden), leptin (duoset, R&D Systems Europe, Abingdon, United Kingdom), IL-6, TNFα and adiponectin levels (Quantikine kits, R&D Systems
General Laboratory methods Plasma analysis: Plasma insulin (Mercodia, Sweden), leptin (duoset, R&D Systems Europe, Abingdon, United Kingdom), IL-6, TNFα and adiponectin levels (Quantikine kits, R&D Systems
AMPK Assay. Require: Sigma (1L, $18.30) A4206 Aluminum foil
 AMPK Assay Require: Acetone Sigma (1L, $18.30) A4206 Aluminum foil Ammonium sulfate Fisher BP212R-1 AMP Sigma A1752 ATP Sigma A6144 (alt. use A7699) Beta-mercaptoethanol Sigma M6250 (alt. use M7154) Bio-Rad
AMPK Assay Require: Acetone Sigma (1L, $18.30) A4206 Aluminum foil Ammonium sulfate Fisher BP212R-1 AMP Sigma A1752 ATP Sigma A6144 (alt. use A7699) Beta-mercaptoethanol Sigma M6250 (alt. use M7154) Bio-Rad
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature12652 Supplementary Figure 1. PRDM16 interacts with endogenous EHMT1 in brown adipocytes. Immunoprecipitation of PRDM16 complex by flag antibody (M2) followed by Western blot analysis
doi:10.1038/nature12652 Supplementary Figure 1. PRDM16 interacts with endogenous EHMT1 in brown adipocytes. Immunoprecipitation of PRDM16 complex by flag antibody (M2) followed by Western blot analysis
Shelagh Wilson. KEY WORDS: fl agonist; acetyl-coa carboxylase.
 Bioscience Reports, Vol. 9, No. 1, 1989 Effect of the fl-adrenoceptor Agonist BRL 26830 on Fatty Acid Synthesis and on the Activities ofpyruvate Dehydrogenase and Acetyl-CoA Carboxylase in Adipose Tissues
Bioscience Reports, Vol. 9, No. 1, 1989 Effect of the fl-adrenoceptor Agonist BRL 26830 on Fatty Acid Synthesis and on the Activities ofpyruvate Dehydrogenase and Acetyl-CoA Carboxylase in Adipose Tissues
BBSG 501 Section 4 Metabolic Fuels, Energy and Order Fall 2003 Semester
 BBSG 501 Section 4 Metabolic Fuels, Energy and Order Fall 2003 Semester Section Director: Dave Ford, Ph.D. Office: MS 141: ext. 8129: e-mail: fordda@slu.edu Lecturers: Michael Moxley, Ph.D. Office: MS
BBSG 501 Section 4 Metabolic Fuels, Energy and Order Fall 2003 Semester Section Director: Dave Ford, Ph.D. Office: MS 141: ext. 8129: e-mail: fordda@slu.edu Lecturers: Michael Moxley, Ph.D. Office: MS
Adrenal gland And Pancreas
 Adrenal gland And Pancreas Structure Cortex Glucocorticoids Effects Control of secretion Mineralocorticoids Effects Control of secretion Sex steroids Medulla Catecholamines Adrenal cortex 80% of an adrenal
Adrenal gland And Pancreas Structure Cortex Glucocorticoids Effects Control of secretion Mineralocorticoids Effects Control of secretion Sex steroids Medulla Catecholamines Adrenal cortex 80% of an adrenal
Chapter 10. Introduction to Nutrition and Metabolism, 3 rd edition David A Bender Taylor & Francis Ltd, London 2002
 Chapter 10 Introduction to Nutrition and Metabolism, 3 rd edition David A Bender Taylor & Francis Ltd, London 2002 Chapter 10: Integration and Control of Metabolism Press the space bar or click the mouse
Chapter 10 Introduction to Nutrition and Metabolism, 3 rd edition David A Bender Taylor & Francis Ltd, London 2002 Chapter 10: Integration and Control of Metabolism Press the space bar or click the mouse
Lecture 5: Cell Metabolism. Biology 219 Dr. Adam Ross
 Lecture 5: Cell Metabolism Biology 219 Dr. Adam Ross Cellular Respiration Set of reactions that take place during the conversion of nutrients into ATP Intricate regulatory relationship between several
Lecture 5: Cell Metabolism Biology 219 Dr. Adam Ross Cellular Respiration Set of reactions that take place during the conversion of nutrients into ATP Intricate regulatory relationship between several
Implications of mitochondrial skeletal muscle metabolism on diabetes and obesity before and after weight loss
 GG2 Implications of mitochondrial skeletal muscle metabolism on diabetes and obesity before and after weight loss Dr Giacomo Gastaldi CHRU Montpellier Folie 1 GG2 19.10.2009 GG_PC; 12.10.2009 Plan Introduction
GG2 Implications of mitochondrial skeletal muscle metabolism on diabetes and obesity before and after weight loss Dr Giacomo Gastaldi CHRU Montpellier Folie 1 GG2 19.10.2009 GG_PC; 12.10.2009 Plan Introduction
BIOL212- Biochemistry of Disease. Metabolic Disorders: Diabetes
 BIOL212- Biochemistry of Disease Metabolic Disorders: Diabetes Diabetes mellitus is, after heart disease and cancer, the third leading cause of death in the west. Insulin is either not secreted in sufficient
BIOL212- Biochemistry of Disease Metabolic Disorders: Diabetes Diabetes mellitus is, after heart disease and cancer, the third leading cause of death in the west. Insulin is either not secreted in sufficient
Cell Signaling part 2
 15 Cell Signaling part 2 Functions of Cell Surface Receptors Other cell surface receptors are directly linked to intracellular enzymes. The largest family of these is the receptor protein tyrosine kinases,
15 Cell Signaling part 2 Functions of Cell Surface Receptors Other cell surface receptors are directly linked to intracellular enzymes. The largest family of these is the receptor protein tyrosine kinases,
Insulin and the brain. Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD
 Insulin and the brain Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD 1921 Banting & Macleod Nobel Prize 1923 White, M. F. (2003) Science Berg, J. M., Tymoczko, J. L. and Stryer, L. (2007) Biochemistry
Insulin and the brain Mary ET Boyle, Ph. D. Department of Cognitive Science UCSD 1921 Banting & Macleod Nobel Prize 1923 White, M. F. (2003) Science Berg, J. M., Tymoczko, J. L. and Stryer, L. (2007) Biochemistry
Oxidation of Long Chain Fatty Acids
 Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
Oxidation of Long Chain Fatty Acids Dr NC Bird Oxidation of long chain fatty acids is the primary source of energy supply in man and animals. Hibernating animals utilise fat stores to maintain body heat,
A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets
 Diabetologia () 5:77 DOI.7/s5--- SHORT COMMUNICATION A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets Q. Cheng & Y. C.
Diabetologia () 5:77 DOI.7/s5--- SHORT COMMUNICATION A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets Q. Cheng & Y. C.
Module C CHEMISTRY & CELL BIOLOGY REVIEW
 Module C CHEMISTRY & CELL BIOLOGY REVIEW Note: This module is provided for A&P courses that do not have a prerequisite class which includes chemistry and cell biology. Content covered by required prerequisite
Module C CHEMISTRY & CELL BIOLOGY REVIEW Note: This module is provided for A&P courses that do not have a prerequisite class which includes chemistry and cell biology. Content covered by required prerequisite
Defective Hepatic Autophagy in Obesity Promotes ER Stress and Causes Insulin Resistance
 Cell Metabolism, Volume 11 Supplemental Information Defective Hepatic Autophagy in Obesity Promotes ER Stress and Causes Insulin Resistance Ling Yang, Ping Li, Suneng Fu, Ediz S. Calay, and Gökhan S. Hotamisligil
Cell Metabolism, Volume 11 Supplemental Information Defective Hepatic Autophagy in Obesity Promotes ER Stress and Causes Insulin Resistance Ling Yang, Ping Li, Suneng Fu, Ediz S. Calay, and Gökhan S. Hotamisligil
Control 7 d cold 7 d CL
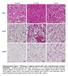 Control 7 d cold 7 d ibat iwat gwat Supplementary Figure 1. Histology of adipose tissues after cold or 3-adrenergic receptor stimulation. C57BL/6J wild-type mice were housed at 4 C or injected daily with
Control 7 d cold 7 d ibat iwat gwat Supplementary Figure 1. Histology of adipose tissues after cold or 3-adrenergic receptor stimulation. C57BL/6J wild-type mice were housed at 4 C or injected daily with
EAT TO LIVE: THE ROLE OF THE PANCREAS. Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008
 EAT TO LIVE: THE ROLE OF THE PANCREAS Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008 THE ROLE OF THE PANCREAS Exocrine pancreas Endocrine pancreas THE ROLE OF THE PANCREAS EXOCRINE
EAT TO LIVE: THE ROLE OF THE PANCREAS Felicia V. Nowak, M.D., Ph.D. Ohio University COM 22 January, 2008 THE ROLE OF THE PANCREAS Exocrine pancreas Endocrine pancreas THE ROLE OF THE PANCREAS EXOCRINE
3-Thia Fatty Acids A New Generation of Functional Lipids?
 Conference on Food Structure and Food Quality 3-Thia Fatty Acids A New Generation of Functional Lipids? Rolf K. Berge rolf.berge@med.uib.no Fatty acids- Essential cellular metabolites Concentrations must
Conference on Food Structure and Food Quality 3-Thia Fatty Acids A New Generation of Functional Lipids? Rolf K. Berge rolf.berge@med.uib.no Fatty acids- Essential cellular metabolites Concentrations must
Fig. S1. REGN1500 reduces plasma levels of cholesterol, TG and NEFA in WT and Ldlr -/- mice. (A) WT
 Figure Legends for Supplementary Figures. Fig. S1. REGN15 reduces plasma levels of cholesterol, TG and NEF in WT and Ldlr -/- mice. () WT and Ldlr -/- mice were injected with control IgG or REGN15 (1 mg/kg)
Figure Legends for Supplementary Figures. Fig. S1. REGN15 reduces plasma levels of cholesterol, TG and NEF in WT and Ldlr -/- mice. () WT and Ldlr -/- mice were injected with control IgG or REGN15 (1 mg/kg)
23.1 Lipid Metabolism in Animals. Chapter 23. Micelles Lipid Metabolism in. Animals. Overview of Digestion Lipid Metabolism in
 Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Denniston Topping Caret Copyright! The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Chapter 23 Fatty Acid Metabolism Triglycerides (Tgl) are emulsified into fat droplets
Moh Tarek. Razi Kittaneh. Jaqen H ghar
 14 Moh Tarek Razi Kittaneh Jaqen H ghar Naif Karadsheh Gluconeogenesis is making glucose from non-carbohydrates precursors. Although Gluconeogenesis looks like Glycolysis in many steps, it is not the simple
14 Moh Tarek Razi Kittaneh Jaqen H ghar Naif Karadsheh Gluconeogenesis is making glucose from non-carbohydrates precursors. Although Gluconeogenesis looks like Glycolysis in many steps, it is not the simple
Supplementary Figure 1
 Supplementary Figure 1 how HFD how HFD Epi WT p p Hypothalamus p p Inguinal WT T Liver Lean mouse adipocytes p p p p p p Obese mouse adipocytes Kidney Muscle Spleen Heart p p p p p p p p Extracellular
Supplementary Figure 1 how HFD how HFD Epi WT p p Hypothalamus p p Inguinal WT T Liver Lean mouse adipocytes p p p p p p Obese mouse adipocytes Kidney Muscle Spleen Heart p p p p p p p p Extracellular
AMPK activity and isoform protein expression are similar in muscle of obese subjects with and without type 2 diabetes
 Am J Physiol Endocrinol Metab 286: E239 E244, 2004. First published October 7, 2003; 10.1152/ajpendo.00326.2003. AMPK activity and isoform protein expression are similar in muscle of obese subjects with
Am J Physiol Endocrinol Metab 286: E239 E244, 2004. First published October 7, 2003; 10.1152/ajpendo.00326.2003. AMPK activity and isoform protein expression are similar in muscle of obese subjects with
Exercise and insulin stimulate glucose transport
 Ca 2 and AMPK Both Mediate Stimulation of Glucose Transport by Muscle Contractions David C. Wright, Kathleen A. Hucker, John O. Holloszy, and Dong Ho Han It is now generally accepted that activation of
Ca 2 and AMPK Both Mediate Stimulation of Glucose Transport by Muscle Contractions David C. Wright, Kathleen A. Hucker, John O. Holloszy, and Dong Ho Han It is now generally accepted that activation of
2013 W. H. Freeman and Company. 12 Signal Transduction
 2013 W. H. Freeman and Company 12 Signal Transduction CHAPTER 12 Signal Transduction Key topics: General features of signal transduction Structure and function of G protein coupled receptors Structure
2013 W. H. Freeman and Company 12 Signal Transduction CHAPTER 12 Signal Transduction Key topics: General features of signal transduction Structure and function of G protein coupled receptors Structure
Companion to Biosynthesis of Ketones & Cholesterols, Regulation of Lipid Metabolism Lecture Notes
 Companion to Biosynthesis of Ketones & Cholesterols, Regulation of Lipid Metabolism Lecture Notes The major site of acetoacetate and 3-hydorxybutyrate production is in the liver. 3-hydorxybutyrate is the
Companion to Biosynthesis of Ketones & Cholesterols, Regulation of Lipid Metabolism Lecture Notes The major site of acetoacetate and 3-hydorxybutyrate production is in the liver. 3-hydorxybutyrate is the
Glycolysis Part 2. BCH 340 lecture 4
 Glycolysis Part 2 BCH 340 lecture 4 Regulation of Glycolysis There are three steps in glycolysis that have enzymes which regulate the flux of glycolysis These enzymes catalyzes irreversible reactions of
Glycolysis Part 2 BCH 340 lecture 4 Regulation of Glycolysis There are three steps in glycolysis that have enzymes which regulate the flux of glycolysis These enzymes catalyzes irreversible reactions of
MBB317. Dr D MANGNALL OBESITY. Lecture 2
 MBB317 Dr D MANGNALL OBESITY Lecture 2 When the structure of the insulin receptor was first discovered it was assumed that the active beta subunit tyrosine kinase would phosphorylate some intracellular
MBB317 Dr D MANGNALL OBESITY Lecture 2 When the structure of the insulin receptor was first discovered it was assumed that the active beta subunit tyrosine kinase would phosphorylate some intracellular
Published on Second Faculty of Medicine, Charles University (http://www.lf2.cuni.cz )
 Published on Second Faculty of Medicine, Charles University (http://www.lf2.cuni.cz ) Biochemistry Submitted by Marie Havlová on 8. February 2012-0:00 Syllabus of Biochemistry Mechanisms of enzyme catalysis.
Published on Second Faculty of Medicine, Charles University (http://www.lf2.cuni.cz ) Biochemistry Submitted by Marie Havlová on 8. February 2012-0:00 Syllabus of Biochemistry Mechanisms of enzyme catalysis.
the fates of acetyl coa which produced by B oixidation :
 Ketone bodies the fates of acetyl coa which produced by B oixidation : 1) oxidized at the TCA cycle 2)synthesis of ketone bodies Ketone bodies : 1)acetoacetate 2) acetone 3) 3_hydroxybutyrate Naming acetonacetone:
Ketone bodies the fates of acetyl coa which produced by B oixidation : 1) oxidized at the TCA cycle 2)synthesis of ketone bodies Ketone bodies : 1)acetoacetate 2) acetone 3) 3_hydroxybutyrate Naming acetonacetone:
AAV-TBGp-Cre treatment resulted in hepatocyte-specific GH receptor gene recombination
 AAV-TBGp-Cre treatment resulted in hepatocyte-specific GH receptor gene recombination Supplementary Figure 1. Generation of the adult-onset, liver-specific GH receptor knock-down (alivghrkd, Kd) mouse
AAV-TBGp-Cre treatment resulted in hepatocyte-specific GH receptor gene recombination Supplementary Figure 1. Generation of the adult-onset, liver-specific GH receptor knock-down (alivghrkd, Kd) mouse
The Role of Glycogen Synthase Kinase-3 in Insulin-resistant Skeletal Muscle
 The Role of Glycogen Synthase Kinase-3 in Insulin-resistant Skeletal Muscle Item Type text; Electronic Dissertation Authors Dokken, Betsy B. Publisher The University of Arizona. Rights Copyright is held
The Role of Glycogen Synthase Kinase-3 in Insulin-resistant Skeletal Muscle Item Type text; Electronic Dissertation Authors Dokken, Betsy B. Publisher The University of Arizona. Rights Copyright is held
Obesity in aging: Hormonal contribution
 Obesity in aging: Hormonal contribution Hormonal issues in obesity and aging Hormonal role in regulation of energy balance Genetic component in hormonal regulation Life style contribution to hormonal changes
Obesity in aging: Hormonal contribution Hormonal issues in obesity and aging Hormonal role in regulation of energy balance Genetic component in hormonal regulation Life style contribution to hormonal changes
