Continuous stimulation of human glucagon-like peptide-1 (7 36) amide in a mouse model (NOD) delays onset of autoimmune type 1 diabetes
|
|
|
- Deirdre Gibbs
- 5 years ago
- Views:
Transcription
1 Diabetologia (27) 5: DOI 1.17/s ARTICLE Continuous stimulation of human glucagon-like peptide-1 (7 36) amide in a mouse model (NOD) delays onset of autoimmune type 1 diabetes J. Zhang & Y. Tokui & K. Yamagata & J. Kozawa & K. Sayama & H. Iwahashi & K. Okita & M. Miuchi & H. Konya & T. Hamaguchi & M. Namba & I. Shimomura & J-i. Miyagawa Received: 6 April 27 /Accepted: 14 May 27 / Published online: 14 July 27 # Springer-Verlag 27 Abstract Aims/hypothesis We examined the effect of glucagon-like peptide-1 (GLP-1) on the development of diabetes and islet morphology in NOD mice by administering GLP-1 to prediabetic mice. Methods Eight-week-old female NOD mice were infused subcutaneously with human GLP-1 via a mini-osmotic pump for 4 or 8 weeks. In mice treated with GLP-1 for 4 weeks, blood glucose levels and body weight were measured. An intraperitoneal glucose tolerance test (IPGTT) and evaluation of insulitis score were also performed. Beta cell area, proliferation, apoptosis, neogenesis from ducts and subcellular localisation of forkhead box O1 (FOXO1) were examined by histomorphometrical, BrdU-labelling, TUNEL, insulin/cytokeratin and FOXO1/ insulin double-immunostaining methods, respectively. J. Zhang and Y. Tokui contributed equally to this study. Electronic supplementary material The online version of this article (doi:1.17/s ) contains supplementary material, which is available to authorised users. J. Zhang : Y. Tokui : K. Yamagata : J. Kozawa : K. Sayama : H. Iwahashi : K. Okita : I. Shimomura Department of Metabolic Medicine, Graduate School of Medicine, Osaka University, Osaka, Japan M. Miuchi : H. Konya : T. Hamaguchi : M. Namba : J.-i. Miyagawa (*) Division of Diabetes and Metabolism, Department of Internal Medicine, Hyogo College of Medicine, 1-1 Mukogawa-cho, Nishinomiya, Hyogo , Japan miyagawa@hyo-med.ac.jp Results Mice treated with human GLP-1 for 4 weeks had lower blood glucose levels until 2 weeks after completion of treatment, showing improved IPGTT data and insulitis score. This effect continued even after cessation of the treatment. In addition to the increase of beta cell neogenesis, BrdU labelling index was elevated (.24 vs.13%, p<.1), while apoptosis was suppressed by 54.2% (p<.1) in beta cells. Beta cell area was increased in parallel with the translocation of FOXO1 from the nucleus to the cytoplasm. The onset of diabetes was delayed in mice treated with GLP-1 for 4 weeks, while mice treated with GLP-1 for 8 weeks did not develop diabetes by age 21 weeks compared with a 6% diabetes incidence in control mice at this age. Conclusions/interpretation Continuous infusion of human GLP-1 to prediabetic NOD mice not only induces beta cell proliferation and neogenesis, but also suppresses beta cell apoptosis and delays the onset of type 1 diabetes. Keywords Apoptosis. Diabetes mellitus. Forkhead box O1. FOXO1. GLP-1. Glucagon-like peptide-1. NOD mouse. Non-obese diabetic mouse Abbreviations BrdU L.I. percentage of BrdU-positive beta cells FOXO1 forkhead box O1 GLP-1 glucagon-like peptide-1 ICC islet-like cell cluster IPGTT intraperitoneal glucose tolerance test PI3-K phosphatidylinositol 3-kinase PKB protein kinase B
2 Diabetologia (27) 5: Introduction Glucagon-like peptide-1 (GLP-1) is an insulinotropic peptide that is secreted by the L-cells of the gastrointestinal tract in response to the ingestion of nutrients [1]. GLP-1 not only enhances glucose-dependent insulin secretion and glucose utilisation by the peripheral tissues [2], but also inhibits glucagon secretion, gastric emptying and gastric acid secretion, as well as reducing food intake [3 7]. It has also been demonstrated that GLP-1 agonists stimulate beta cell proliferation and neogenesis in rats, along with increased islet expression of pancreatic and duodenal homeobox gene 1 (Pdx1), Glut2 (also known as solute carrier family 2 [facilitated glucose transporter], member 2 [Slc2a2]) and glucokinase genes, as well as upregulation of insulin mrna [8]. The translocation of forkhead box O1 (FOXOl) from the nucleus to the cytoplasm results in upregulation of Pdx1 expression through insulin receptor substrate 2 (IRS2)-mediated activation of the phosphatidylinositol 3-kinase (PI3-K) protein kinase B (PKB) pathway [9]. More recent studies have demonstrated that administration of GLP-1 inhibits beta cell apoptosis via the PI3-K PKB signalling pathway [1 12]. Importantly, the anti-apoptotic action of GLP-1 has also been demonstrated in freshly isolated human islets [13]. Furthermore, GLP-1 increased the survival of immortalised rodent beta cell lines after challenge with various apoptotic stimuli [12, 14 17]. Because of these actions, GLP-1 offers several potential therapeutic advantages for patients with type 2 diabetes. For type 1 diabetes, treatment combining lisofyline (a synthetic modified methylxanthine) and the GLP-1 analogue exendin-4, with anti-lymphocyte serum and exendin-4 successfully reversed autoimmune diabetes, although treatment with exendin-4 alone was not successful in reversing glycaemic control in NOD mice [18, 19]. Like human autoimmune type 1 diabetes, the NOD mouse features a prediabetic phase that is characterised by insulitis (mononuclear cell infiltration into islets) without hyperglycaemia. The aim of the present study was to assess how GLP-1 treatment influences the development of diabetes in NOD mice during the prediabetic period. Methods Animals Our colony of NOD mice was originally purchased from CLEA Japan (Tokyo, Japan) and was maintained on standard laboratory chow under a 12 h light dark cycle. The mice were given free access to food and water. They were only fasted on the night before the glucose tolerance test. Institutional guidelines for the care and use of animals were followed. The incidence of diabetes reaches about 8% in female and 2% in male mice by 3 weeks of age. The 8-week-old female NOD mice selected for this study were divided into an experimental group and a control group. The protocols for the animal experiments were designed following the Principles of Laboratory Animal Care published by the National Institutes of Health and were approved by the Animal Care and Use Committee of Osaka University Medical School (Osaka, Japan). GLP-1 treatment and measurement of plasma GLP-1 The experimental group was treated with GLP-1 and the control group was treated with saline for 4 weeks. Human GLP-1 (7 36) amide (AnaSpec, San Jose, CA, USA) was infused at a constant rate of 1.5 pmol kg 1 min 1 via a mini-osmotic pump that delivers the solution continuously for up to 28 days (ALZET, model 24; DURECT, Cupertino, CA, USA) as described previously [2]. To initiate immediate pumping, we placed the pre-filled pumps in.8% saline for at least 4 h at 37 C before implantation. According to the manufacturer s guideline, GLP-1 was dissolved in 5% acetic acid buffer. Blood glucose levels and body weight were measured weekly during GLP-1 treatment for 4 weeks. To observe the changes of blood glucose levels after the completion of GLP-1 treatment, we also measured blood glucose levels until the end of monitoring. In a separate experiment, mice were treated with GLP-1 for 8 weeks from 8 weeks of age by replacing the first infusion pump by a second one to further examine the effect of continuous GLP-1 infusion on the development of diabetes. To confirm the efficacy of continuous GLP-1 infusion, we measured the active plasma GLP-1 concentration in age-matched NOD mice using an ELISA method before and at 2 and 4 weeks after pump implantation. Because at least 2 μl of plasma is necessary for one measurement, we used one animal to measure one point concentration. Whole-blood samples were obtained in mice before implantation of pumps (n=6) and 2 and 4 weeks after implantation of the GLP-1 pump (n=5 in each group). The plasma level of GLP-1 was measured with an ELISA kit [GLP-1 (Active) ELISA Kit; Linco Research, St Charles, MO, USA]. Intraperitoneal glucose tolerance test The intraperitoneal glucose tolerance test (IPGTT) was performed before GLP-1 treatment (at 8 weeks of age) and 4 weeks after the treatment (n=6 in each group). Glucose (2 g/kg) was administered intraperitoneally to conscious animals after an overnight fast. Blood samples were collected from the tail vein into heparinised packed cell
3 192 Diabetologia (27) 5: volume tubes at, 3, 6 and 12 min, and the blood glucose level was measured with a glucometer (Glutest Ace; Arkray Factory, Shiga, Japan). Plasma insulin levels were measured using a commercial ELISA kit (Glazyme; Sanyo-Kasei, Kyoto, Japan). Immunohistochemical study Immunostaining The pancreases were resected from 12- week-old female NOD mice after 4 weeks of either GLP-1 or saline infusion (n=6, in each group) and fixed in 1% phosphate-buffered neutral formalin. Paraffin-embedded sections (5 7 μm thick) cut at 5 μm intervals were stained with haematoxylin and eosin to observe mononuclear cell infiltration in and around the islet. Other sections were stained for insulin and BrdU using a polyclonal guinea pig anti-insulin and anti-brdu antibodies, respectively, and were visualised with diaminobenzidine as described previously [21]. The grade of insulitis was scored on haematoxylin and eosin-stained sections. Approximately 25 islets from three different pancreatic regions (>3 μm interval between each section) were examined in each animal and scored as follows: point for no apparent mononuclear cell infiltration in and around the islets; 1 point for 1 1% of the area occupied by mononuclear cell infiltration; 2 points for 1 25%; 3 points for 25 5%; and 4 points for >5% occupied [22]. Morphometric analysis Wemeasuredthebetacellareaon three sections of each pancreas stained for insulin. Morphometric evaluation of the total beta cell area was performed by computer-assisted image analysis (Win RooF software Ver. 5.5; Mitani, Fukui, Japan) using light and immunofluorescence microscopes (Provis AX8T and AX8TR equipped with HDTV system and colour charged-coupling device camera; Olympus, Tokyo, Japan). The area of insulin-positive cells and the total area of the tissue section were evaluated for each section. Then, the percentage beta cell area was determined by calculating the ratio of the area occupied by insulin-positive cells to the total pancreatic area. Since this method is unable to clearly distinguish between beta cells derived from neogenesis and pre-existing beta cells, insulin-positive cells were counted together. Beta cell replication BrdU is incorporated by newly synthesised DNA in replicating cells. Animals from both groups were injected with BrdU (1 μg/g body weight, i.p.) (Sigma, St Louis, MO, USA) at 6 h before the whole pancreas was removed. Sections were double immunostained to detect BrdU and insulin as described above. Then, the percentage of BrdUpositive beta cell nuclei relative to all beta cell nuclei was calculated and was taken to represent the percentage of BrdUpositive beta cells (BrdU L.I.). Beta cell neogenesis from ductal precursors To evaluate the effect of GLP-1 on beta cell neogenesis, double immunostaining was performed to detect insulin-positive cells and cytokeratin-positive duct cells (see Electronic supplementary material [ESM]). Using these sections, we quantified the newly formed beta cells in three different sections of each pancreas from six animals per group. We counted the number of insulin-positive cells in islet-like cell clusters (ICCs) in close contact with ducts, and the number localised in the duct cell lining (beta cells derived from neogenesis). The value for newly formed beta cells was calculated per square cm of the total pancreatic area. Localisation of FOXO1 in beta cells Sections from 8- and 12-week-old mice treated with GLP-1 or saline were examined to assess the subcellular localisation of FOXO1 in beta cells after double immunostaining for FOXO1 and insulin. The sections were first incubated overnight with anti-fkhr antibody (1:5) (Cell Signaling Technology, Danvers, MA, USA) at 4 C after microwave treatment at 95 C for 1 min in the target retrieval solution (DakoCytomation, Inc., Carpinteria, CA, USA). After washing, sections were incubated with biotinylated goat anti-rabbit immunoglobulin (Vector Laboratories, Burlingame, CA, USA) for 3 min and FOXO1 was visualised with streptavidin-conjugated Alexa Fluor 488 (Molecular Probes, Eugene, OR, USA). These sections were then immunostained for insulin as described above and were observed under a fluorescence microscope (AX8TR; Olympus). Beta cell apoptosis The pancreases from 17-week-old mice after treatment with GLP-1 (n=6)or saline(n=6) from 8 to 12 weeks of age were fixed in 1% phosphate-buffered neutral formalin and paraffin-embedded sections (5 7 μm thick) were cut at 3 μm intervals. Apoptosis was detected through labelling DNA strand breaks by the TUNEL method according to the manufacturer s protocol (TaKaRa in situ apoptosis detection kit; TaKaRa Biomedicals, Shiga, Japan), followed by staining for insulin to detect beta cells (for more details see ESM). At least 1,5 to 2, beta cell nuclei were counted per pancreas section at a final magnification of 1,. A fluorescence microscope was also used to confirm insulin and TUNEL positivity, thus identifying apoptotic beta cells by incubation with rhodamin-conjugated goat anti-guinea pig IgG for insulin. Monitoring of diabetes mellitus We monitored the occurrence of diabetes after cessation of the treatment from the age of 12 to 3 weeks in 1 mice per group. In addition, the occurrence of diabetes was further
4 Diabetologia (27) 5: examined separately in connection with the 8 weeks of treatment with GLP-1 infusion from the age of 8 to 21 weeks in five mice per group. The onset of diabetes was assessed by the detection of glucosuria using a glucose test strip (Taisei Medipac, Osaka, Japan) and was confirmed by blood glucose measurement three times per week from the day when positive glucosuria was detected. A blood glucose level >16.7 mmol/l (3 mg/dl) in three consecutive measurements was defined as indicating diabetes (date of onset is the first day). Statistical analyses Data are presented as the mean ± SEM. Statistical analysis was performed using Student s t test or ANOVA with the n 1 custom hypothesis test, as appropriate. Analysis of morning plasma glucose levels after GLP-1 treatment was performed using the Mann Whitney U test. The incidence of diabetes was analysed by Kaplan Meier life table analysis and Cox Mantel test. A p value of less than.5 was considered to indicate statistical significance. Results Plasma GLP-1 level The plasma levels of GLP-1 at 2 and 4 weeks after the pump implantation were 77.5±8.5 (n=5) and 7.2±5.8 pg/ml (n=6), respectively, while plasma GLP-1 before the implantation was 4.2±3.6 pg/ml (n=6) under normal feeding conditions. PlasmaconcentrationsofactiveGLP-1atboth2and4weeks after the pump implantation were significantly elevated (p<.1) and about 1.5-fold higher than before the pump implantation. We therefore considered this delivery system to be appropriate for this experiment. Improvement of glucose tolerance by GLP-1 GLP-1 treatment was initiated at 8 weeks of age. GLP-1- treated mice had significantly lower glucose levels from 2 weeks onwards during treatment (4.8±.1 mmol/l, n=14, p<.1 vs saline-treated mice 6.6±.2 mmol/l, at 4 weeks after the start of GLP-1 treatment) (Fig. 1a). Blood glucose levels were significantly lower in GLP-1 mice than in control mice at 13 weeks of age (4.7±.2 mmol/l, n=18, p<.1 vs saline-treated mice 6.1±.2 mmol/l ) and at 14 weeks of age (4.8±.2 mmol/l, n=18, p<.1 vs saline-treated mice 6.±.3 mmol/l). This effect also continued at 15 (4.9±.2 mmol/l, p<.1 vs saline-treated mice 7.6±1.3 mmol/l) and 17 weeks of age (5.9±.3 mmol/l, p<.5 vs saline-treated mice 8.7±1.4 mmol/l) (Fig. 1b). These results indicate that GLP-1 improved glycaemic control. There was no significant difference in body weight between GLP-1- and saline-treated mice (Fig. 1c), so the improved glycaemic control in GLP-1-treated mice did not result from weight loss. The IPGTT was performed before treatment and at 4 weeks after the treatment. It showed no differences between the two groups before the treatment. However, after 4 weeks of treatment, the blood glucose levels of GLP-1-treated mice were 3.2±.4 ( min), 1.2±.11 (3 min), 5.4±.37 (6 min) and 4.1±.26 mmol/l (12 min), whereas those of control mice were 4.±.9, 13.5±.11, 9.3±.36 and 6.5±.31 mmol/l, respectively (n=6 in each group). Blood glucose levels were significantly lower in GLP-1-treated mice than in saline-treated mice (Fig. 1d). At 4 weeks, the plasma insulin levels of GLP-1-treated mice were 87±15 ( min), 337±14 (3min), 226±41 (6 min) and 279±25 pmol/l (12 min), whereas the levels of saline-treated mice were 69±1, 224±24, 14±38 and 147±14 pmol/l, respectively. The insulin level in GLP-1-treated mice was significantly higher at 3 and 12 min (p<.1 for both, n=6) than in control mice (Fig. 1e). Morphometric analysis The islets seemed to be larger in GLP-1-treated mice (Fig. 2a) than control mice (Fig. 2b) at 12 weeks of age, so we measured the beta cell area in both groups. There was a significant increase in the beta cell area in the GLP-1 group (.65±.8%) compared with the saline group (.4±.4%, p<.5, n=6) at 4 weeks after GLP-1 treatment (Fig. 2c). Effect of GLP-1 on beta cell proliferation and neogenesis There are two possible ways to increase the beta cell mass: the proliferation of pre-existing beta cells, and neogenesis or differentiation from pancreatic stem or duct cells. To examine beta cell proliferation, we evaluated the BrdU L.I. of beta cells by double immunocytochemical staining for insulin and BrdU (Fig. 3a e). The BrdU L.I. of 12-week-old GLP-1-treated mice (.24±.2%) was significantly higher than that of control mice (.13±.1%; p<.1, n=5) (Fig. 3f). To evaluate the influence of GLP-1 on beta cell neogenesis, we counted the number of beta cells in the duct epithelium and the number in ICCs budding from the ducts. In NOD mice, the number of newly formed beta cells was more or less increased compared with those of other nondiabetic strains of mice (data not shown). However, the number of newly formed beta cells was further increased in the GLP-1 group (51.5±5./cm 2 ) compared with the control group (3.5±5.4/cm 2 ; p<.5, n=5) (ESM Fig. 1a c). (The
5 194 Diabetologia (27) 5: a Blood glucose (mmol/l) c Body weight (g) * * Time from start of infusion (weeks) Time from start of infusion (weeks) b 1. Fig. 1 Effect of GLP-1 on glucose tolerance in NOD mice. a The GLP-1 group (circles, also other panels) had significantly lower plasma glucose levels than the saline group (squares, also other panels) from 2 weeks of treatment onward. b After cessation of the treatment, the GLP-1 group had lower plasma glucose levels than the saline group at 13 and 14 weeks of age, as well as at 15 and 17 weeks. Open bars, saline group; closed bars, GLP-1 group. c Body weight Blood glucose (mmol/l) d Blood glucose (mmol/l) Age (weeks) * * Time (min) e Plasma insulin (pmol/l) * Time (min) profile during treatment. There was no difference in body weight between the GLP-1 and saline group. d, e IPGTT was performed after 4 weeks of GLP-1 treatment. Plasma glucose (d) and serum insulin levels (e) are shown. The GLP-1 group showed significantly improved glucose tolerance compared with the saline group. Serum insulin levels were significantly higher in the GLP-1 than in the saline group at 3 and 12 min *p<.5, p<.1, *p<.1 value is expressed as number of beta cells/cm 2 of the total pancreatic area.) Localisation of FOXO1 protein and insulin in beta cells To investigate the changes of subcellular localisation of FOXO1 protein in beta cells after GLP-1 treatment, we examined the localisation of FOXO1 and insulin in the pancreas by immunostaining. FOXO1 was predominantly localised in the nuclei of insulin-positive cells in 8-weekold mice (before treatment) (Fig. 4a c) and in saline-treated 12-week-old mice (Fig. 4g i). In contrast, this transcription factor was mainly detected in the cytoplasm of many insulin-positive cells in GLP-1-treated 12-week-old mice (Fig. 4d f). Thus, GLP-1 treatment altered the subcellular distribution of FOXO1 and promoted its translocation from the nucleus to the cytoplasm in beta cells. Effect of GLP-1 on beta cell apoptosis We observed a greater number of insulin-positive apoptotic cells in the pancreatic sections of saline-treated mice at 17 weeks of age than in sections from GLP-1-treated mice (Fig. 5a,b). To determine the percentage of TUNELpositive, insulin-containing cells, sections were doublestained for TUNEL and insulin. TUNEL-positive beta cells in saline- and GLP-1-treated NOD mice were.24±.1 and.11±.3%, respectively (p<.1, n=6). As a result, GLP-1 caused a 54.2% decrease in the relative number of apoptotic beta cells. Effect of GLP-1 on insulitis To evaluate mononuclear cell infiltration in and around the islets, histological examination of haematoxylin and eosinstained pancreatic sections was done in the GLP-1 and saline groups. The GLP-1-treated 12-week-old NOD mice had significantly more islets with no apparent mononuclear cell infiltration than did the control mice (74.6 vs 51.6%). Insulitis in the GLP-1 group at this time point (at scores 2, 3 or 4) was less severe than in the control mice (at scores 2, 3 and 4) (all p<.1, n=4) (ESM Fig. 2). When the mice were 17 weeks old, the degree of each insulitis score showed no significant difference between GLP-1 (n=5) and saline groups (n=5). Effect of GLP-1 on diabetes The occurrence of diabetes was compared between mice treated with GLP-1 (n=1) or saline (n=1) from 8 to
6 Diabetologia (27) 5: a c Relative beta cell area (%).8 * weeks old 17 weeks old Fig. 2 a, b Immunostaining for insulin in sections from the GLP-1 group and the saline group respectively after 4 weeks of treatment. In the pancreas of GLP-1-treated NOD mouse (a), islets were larger than in that of saline-treated NOD mouse (b). Single beta cell and ICCcontaining insulin-positive cells were seen in and in close contact to the ductal cell lining (arrow) (a). Bar 1 μm. c Relative beta cell area of the GLP-1 group (closed bars) was larger than that of the saline group (open bars) after 4 weeks of treatment (*p<.5), but there was no difference in the relative beta cell areas in 17-week-old mice b 3 weeks of age. As shown in Fig. 6a,b, the onset of diabetes was detected from 15 weeks in the saline group, vs 19 weeks in the GLP-1 group. Occurrence of diabetes tended to be suppressed by GLP-1 at 2 weeks of age with 2% of the GLP-1 group having diabetes versus 5% of the control group. However, from Kaplan Meier's life table analysis, the 5% duration of the non-diabetic period after GLP-1 and saline treatment was 11 and 9 weeks, respectively, while the cumulative incidence was not significant at the endpoint of observation by Cox Mantel test. When the GLP-1 group was treated for 8 weeks from 8 weeks of age (n=5 in each group), no diabetes was observed in that group, while 6% of mice in the saline group had developed diabetes by 21 weeks of age. Thus, in both separate experiments, continuous infusion of human GLP-1 appeared to delay or suppress the onset of diabetes. Discussion Glucagon-like peptide-1 is a potent intestinal insulinotropic hormone that augments insulin secretion in rodents as well as in humans with type 1 or type 2 diabetes [23 27]. GLP-1 has been demonstrated to promote the proliferation and differentiation of beta cells in vivo [28] and in vitro [29]. In this study, we demonstrated that the glucose tolerance of NOD mice treated with GLP-1 significantly improved after a glucose load. After treatment with GLP-1 for 2 weeks, the blood glucose level was also significantly lowered. More importantly, the blood glucose level remained lower for 2 weeks after the end of treatment. We also confirmed that the effect of GLP-1 on blood glucose was mainly the result of an increase in beta cell mass. Either proliferation of preexisting beta cells and/or beta cell neogenesis can lead to expansion of the beta cell mass [3]. In our study, 8-weekold NOD prediabetic mice showed early lymphocytic infiltration into the islets. BrdU-positive beta cells were found in islets with various degrees of lymphocytic infiltration in the GLP-1-treated mice and were hardly recognised in the control mice. The BrdU L.I. of beta cells in the GLP-1 group was significantly higher than in the control group. Therefore, we conclude that GLP-1 promoted the proliferation of pre-existing beta cells. a b c f.3 * d e BrdU L.I. (%).2.1 Saline GLP-1 Fig. 3 Effect of GLP-1 on beta cell proliferation. a e Double immunostaining for BrdU (brown) and insulin (dark grey) in islets with no apparent mononuclear cell infiltration (insulitis) (a, c, and d) and in islets with insulitis (b, e) from pancreases of the GLP-1 group (a c) and the saline group (d, e) after 4 weeks of treatment. BrdUpositive islet cells (arrow heads) were increased in the GLP-1 group. Most of these are insulin-positive (beta cells) as indicated by arrows (c) at higher magnification (bar 3 μm). Bar (e) 5μm. f The BrdU L.I. of beta cells after 4 weeks of treatment was significantly higher in the GLP-1 group than in the saline group. *p<.1, n=6
7 196 Diabetologia (27) 5: Fig. 4 Double immunostaining for insulin and FOXO1 in the pancreas from untreated 8-weekold mice (a c) and from 12- week-old mice treated with GLP-1 (d f) or saline (g i). Insulin and FOXO1 protein are identified by red and green fluorescence, respectively. When merged, FOXO1 is recognised predominantly in the nuclei of insulin-positive cells in untreated and saline-treated mice (c, i), while being mainly localised in the cytoplasm of insulin-positive cells in GLP-1 treated mice (f). Bar 1 μm It is generally believed that islet precursor cells exist in the pancreatic ducts [31]. GLP-1 has been shown to induce the production of PDX1 in ducts and the differentiation of duct cells toward insulin-producing cells [32]. In GLP-1- treated NOD mice, we found that the number of newly formed beta cells originating from pancreatic ducts was a b c TUNEL-positive beta cells (%) Saline GLP-1 Fig. 5 Effect of GLP-1 on beta cell apoptosis. a, b Double immnunostaining for apoptosis (TUNEL method, green, yellow) and insulin (red) in sections from the GLP-1 group (a) and the saline group (b) at 17 weeks of age. Apoptotic beta cells have TUNELpositive nuclei (arrowheads) surrounded by insulin-positive cytoplasm (red). Such cells were common in the saline group, but rarely seen in the GLP-1 group. Bar 5 μm. c The percentage of TUNELpositive beta cells in pancreatic sections from 17-week-old mice was lower in the GLP-1 group (.11±.1%) than in the saline group (.24±.1%). p<.1, n=6 increased. Thus, in addition to the promotion of preexisting beta cell proliferation, GLP-1 stimulated the differentiation of beta cells. Apart from direct killing of beta cells by autoreactive T cells, another possible mechanism of beta cell loss in autoimmune type 1 diabetes may be cytokine-induced apoptosis [33, 34]. Recently, it was reported that GLP-1 and other growth factors have an anti-apoptotic effect [11 13, 35]. To investigate whether GLP-1 has an anti-apoptotic effect on beta cells in NOD mice, double staining for insulin and TUNEL was done to directly identify apoptotic cells [36]. Apoptotic beta cells were more easily detected in the islets of control mice. In contrast, such cells were rarely found in the islets of GLP-1-treated mice, although apoptotic cells were seen in the insulin-negative parts in and around the islets. In fact, GLP-1 treatment caused a 54.2% decrease in apoptotic beta cells compared with the control group. This result suggests that GLP-1 protected beta cells against cytokine-mediated apoptosis. We also demonstrated that the insulitis score became lower and the insulin-positive islet area was larger in GLP-1-treated mice, indicating that the anti-apoptotic activity of GLP-1 might have led to the survival of more beta cells in NOD mice and to maintenance and/or an increase of the beta cell mass. As reported previously [1, 37, 38], the binding of GLP-1 to its receptor transduces several intracellular signals including the signalling pathways involved in the proliferation and apoptosis of pancreas islet cells. In beta cells, these signals induce the activation of PI3-K and PKB as well as translocation of FOXO1 to the cytoplasm; they also promote
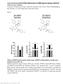
8 Diabetologia (27) 5: bdiabetes incidence (%) a Diabetes incidence (%) Age (weeks) Age (weeks) Fig. 6 Cumulative incidence of diabetes during and after 4 weeks (a) and 8 weeks (b) of GLP-1 treatment in NOD mice monitored from 8 weeks of age. In NOD mice treated with GLP-1 or saline for 4 weeks (a), the onset of diabetes was detected from 15 weeks of age in the saline group (dotted line; n=1), vs 19 weeks in the GLP-1 group (unbroken line; n=1). Incidence of diabetes in GLP-1- and saline-treated groups was 2 and 5% respectively at 2 weeks old, and 6 and 8% respectively at 3 weeks old. The occurrence of diabetes was apparently suppressed during and for 8 weeks after cessation of continuous stimulation with human GLP-1. b In NOD mice treated for 8 weeks with GLP-1 (unbroken line; n=5) or saline (dotted line; n=5), diabetes did not occur in the former group, either during GLP-1 treatment, or in the following period of 5 weeks. In contrast, 6% of the saline-treated mice developed diabetes from the age of 15 to 21 weeks. The difference in diabetes incidence between GLP-1- and saline-treated groups was not statistically significant in either of the experiments according to Kaplan Meier s life table analysis. Bold, two-arrowed line, duration of GLP-1 or saline treatment. Endpoint of the monitoring cell survival and insulin secretion. The results of a recent study also revealed that the protective effect of GLP-1 on cytokine-induced apoptosis requires activation of PKB [39]. FOXO1 undergoes translocation to the cytoplasm when stimulated by insulin and other growth factors via the activation of PI3-K and PKB, while this forkhead transcription factor is dephosphorylated and localised to the nucleus in the absence of insulin [4]. In the present study, continuous infusion of GLP-1 induced translocation of FOXO1 to the cytoplasm in many beta cells, while FOXO1 was predominantly localised in the nucleus of insulinpositive cells in untreated NOD mice or saline-treated mice. It has been reported that FOXO1 and PDX1 demonstrate mutually exclusive nuclear localisation in beta cells and that nuclear localisation of FOXO1 is associated with weak or negative PDX1 localisation [9]. Therefore, it can be suggested that beta cell proliferation in GLP-1-treated mice was associated with the induction of cytoplasmic FOXO1 translocation, although we were unable to find a clear relationship between the localisation of FOXO1 and PDX1 (data not shown). In the present study, we administered GLP-1 to prediabetic NOD mice for only 4 weeks. Yet it appeared to delay the development of diabetes. In addition, continuous infusion of GLP-1 for 8 weeks completely suppressed the development of diabetes during and at least until 5 weeks after cessation of the treatment. Our results demonstrate that GLP-1 had both an anti-apoptotic effect on pre-existing beta cells and also promoted the proliferation and/or differentiation of beta cells in NOD mice. In overtly diabetic NOD mice, it has been reported that a GLP-1 analogue (exendin-4) and anti-lymphocyte serum cured diabetes, while exendin-4 alone failed to achieve remission [18]. Although the mechanism leading to the remission of diabetes was not clearly demonstrated in the above experiment, the beta cell mass seemed to be increased by exendin-4 treatment. In fact, exendin-4 treatment of db/db mice has also been reported to delay the onset of diabetes through a mechanism involving expansion of the functional beta cell mass [1]. Recent treatment of autoimmune type 1 diabetes with islet transplantation has focused attention on cell-based insulin replacement strategies. Together with the current developments in islet transplantation and stem cell therapy, GLP-1 may be a useful agent for regenerative medicine. To date, in vivo effects of GLP-1 on beta cell proliferation and neogenesis have not been demonstrated in the human pancreas, while chronic and continuous stimulation with endogenous GLP-1 is not to be expected because of the short half-life of GLP-1 (2 3 min) due to the existence of the enzyme dipeptidyl peptidase-iv [41]. However, GLP-1 analogues of much longer half-life have been recently developed for the treatment of type 2 diabetes [42]. Longterm stimulation with these analogues might exert the chronic effects of GLP-1 as demonstrated in the present study. Thus, our findings that continuous stimulation with human GLP-1 not only promotes beta cell proliferation and neogenesis, but also protects beta cells from apoptosis in prediabetic NOD mice, may lead to a novel therapeutic approach for type 1 and type 2 diabetes. Acknowledgements We thank F. Katsube (Department of Internal Medicine and Molecular Science, Graduate School of Medicine, Osaka University) for her excellent technical assistance in immunohistochemistry. This work is supported in part by Grant-in-Aid for Researchers, Hyogo College of Medicine and Grant-in-Aid from the Japan Ministry of Education, Culture and Sports (for J. Miyagawa; no ). Duality of interest The authors declare that there is no duality of interest associated with this manuscript.
9 198 Diabetologia (27) 5: References 1. Kietter TJ, Habener JF (1999) The glucagon-like peptides. Endocr Rev 2: Gromada J, Holst JJ, Rorsman P (1998) Cellular regulation of islet hormone secretion by the incretin hormone glucagon-like peptide-1. Eur J Physiol 435: D Alessio DA, Fujimoto WY, Ensinck JW (1989) Effects of glucagon-like peptide 1(7 36) on release of insulin glucagon and somatostatin by rat pancreatic islet cell monolayer cultures. Diabetes 38: Komatsu R, Matsuyama T, Namba M et al (1989) Glucagonostatic and insulinotropic action of glucagons like peptide 1 (7 36)- amide. Diabetes 38: Willms B, Wemer J, Holst JJ, Orskov C, Creutzfeldt W, Nauck MA (1996) Gastric emptying, glucose responses and insulin secretion after a liquid test meal: effect of exogenous glucagonlike peptide 1 (GLP-1) (7 36) amide in type 2 (non-insulin dependent) diabetic patients. J Clin Endocrinol Metab 81: Schjoldager BTG, Mortensen PE, Christiansen J, Orskov C, Holst JJ (1989) GLP-1 (glucagon-like peptide 1) and truncated GLP-1, fragments of human proglucagon, inhibit gastric acid secretion in human. Dig Dis Sci 34: Turton MD, O Shea D, Gunn I et al (1996) A role for glucagonlike peptide in the central regulation of feeding. Nature 379: Perfetti R, Zhou J, Doyle ME, Egan JM (2) Glucagon-like peptide-1 induces cell proliferation and pancreatic-duodenum homeobox-1 expression and increases endocrine cell mass in the pancreas of old glucose-intolerant rats. Endocrinology 141: Kodama S, Toyonaga T, Kondo T et al (25) Enhanced expression of PDX-1 and ngn3 by exendin-4 during beta cell regeneration in STZ-treated mice. Biochem Biophys Res Commun 327: Wang Q, Brubaker PL (22) Glucagon-like peptide-1 treatment delays the onset of diabetes in 8 week-old db/db mice. Diabetologia 45: Farilla L, Hui H, Bertolotto C, Kang E, Bulotta A, Perfetti R (22) Glucagon-like peptide-1 promotes islet cell growth and inhibits apoptosis in Zucker diabetic rats. Endocrinology 143: Li Y, Hansotia T, Yusta B, Ris F, Halban PA, Drucker DJ (23) Glucagon-like peptide-1 receptor signaling modulates beta cell apoptosis. J Biol Chem 278: Farilla L, Bulotta A, Hirshbirg B et al (23) GLP-1 inhibits cell apoptosis and improves glucose responsiveness of freshly isolated human islets. Endocrinology 144: Trumper A, Trumper K, Horsch D (22) Mechanisms of mitogenic and anti-apoptotic signaling by glucose-dependent insulinotropic polypeptide in beta (INS-1)-cells. Endocrinology 174: Hui H, Nourparvar A, Zhao X, Perfetti R (23) Glucogon-like peptide-1 inhibits apoptosis of insulin-secreting cells via a cyclin 5 -adenosine monophosphate-dependent protein kinase and a phosphatidyl inositol 3-kinase-dependent pathway. Endocrinology 144: Ehses JA, Casilla VR, Doty T et al (23) Glucose-dependent insulinotropic polypeptide promotes beta (INS-1) cell survival via cyclic adenosine monophosphate-mediated caspase-3 inhibition and regulation of p38 mitogen-activated protein kinase. Endocrinology 144: Kwon G, Pappan KL, Marshall CA, Schaffer JE, McDaniel ML (24) Cyclic AMP dose-dependently prevents palmitate-induced apoptosis by both PKA-and camp-gef-dependent pathways in beta cells. J Biol Chem 279: Ogawa N, List JF, Habener JF, Maki T (24) Cure of overt diabetes in NOD mice by transient treatment with anti-lymphocyte serum and exendin-4. Diabetes 53: Yang Z, Chen M, Carter JD et al (26) Combined treatment with lisofyline and exendin-4 reverses autoimmune diabetes. Biochem Biophys Res Commun 344: Wang Y, Perfetti R, Greig NH et al (1997) Glucagon-like peptide-1 can reverse the age-related decline in glucose tolerance in rats. J Clin Invest 99: Yamamoto K, Miyagawa J, Waguri M et al (2) Recombinant human betacellulin promotes the neogenesis of beta cell and ameliorates glucose intolerance in mice with diabetes induced by selective alloxan perfusion. Diabetes 49: Douglas OS, Han J, Williams J, Yoon J-W, Jun H-S, Ahvazi B (22) Gamma interferon paradoxically inhibits the development of diabetes in the NOD mouse. J Autoimmun 19: Gutniak M, Orskov C, Holst JJ, Ahren B, Efendic S (1992) Antidiabetogenic effect of glucagon-like peptide(7 36) amide in normal subjects and patients with diabetes mellitus. N Engl J Med 326: Nauck MA, Heimesant MM, Orskov C, Holst JJ, Ebert R, Creutzfeldt W (1993) Preserved incretin activity of glucagon-like peptide(7 36) amide but not of synthetic human gastric inhibitory polypeptide in patients with type 2 diabetes mellitus. J Clin Invest 91: Natham DM, Schreiber E, Fogel H, Miisov S, Habener JF (1992) Insulinotropic action of glucagon-like peptide-1 (7 37) in diabetic and nondiabetic subjects. Diabetes Care 15: Nauck MA, Kleine N, Orskov C, Holst JJ, WiIIms B, Creutzfeldt W (1993) Normalization of fasting hyperglycaemia by exogenous glucagon like peptide (7 36) amide in type 2 (non-insulindependent) diabetic patients. Diabetologia 36: Todd JF, Wilding JP, Edwards CM, Khan FA, Ghatei MA, Bloom SR (1997) Glucagon-like peptide-1 (GLP-1): a trial in insulindependent diabetes mellitus. Eur J Clin Invest 27: Tourrel C, Baibe D, Meile M-J, Kergoat M, Portha B (21) Glucagon-like peptide 1 and exendin-4 stimulate beta cell neogenesis in streptozotocin-treated new born rats resulting in persistently improved glucose homeostasis at adult age. Diabetes 5: Zhou J, Wang X, Pineyro MA, Egan JM (1999) Glucagon-like peptide 1 and exendin-4 convert pancreatic AR42J cells into glucagon- and insulin-producing cells. Diabetes 48: Xu G, Stoffers DA, Habener JF, Bonner-Weir S (1999) Exendin-4 stimulates both beta cell replication and neogenesis, resulting in increased beta cell mass and improved glucose tolerance in diabetic rats. Diabetes 48: Pictet R, Rutter WJ (1972) Development of the embryonic pancreas. In: Steiner DF, Frenkel N (eds) Handbook of physiology, section 7. American Physiological Society, Washington DC, pp Brubaker PL, Drucker DJ (24) Minireview: glucagon-like peptides regulate cell proliferation and apoptosis in the pancreas, gut and central nervous system. Endocrinology 145: Mandrup-Poulsen T (21) Beta-cell apoptosis: stimuli and signaling. Diabetes 5: Uno S, Imagawa A, Okita K et al (27) Macrophages and dendritic cells infiltrating islets with or without beta cells produce tumor necrosis factor-α in patients with recent-onset type 1 diabetes. Diabetologia 5: Urusova AI, Farilla L, Hui H, D Amico E, Perfetti R (24) GLP-1 inhibition of pancreatic islet cell apoptosis. Trends Endocrinol Metab 15: Kurrer MO, Parala SV, Hanson HL, Katz JD (1997) Beta-cell apoptosis in T cell-mediated autoimmune diabetes. Proc Natl Acad Sci U S A 94: Thorens B (1992) Expression cloning of the pancreatic beta cell receptor for the gluco-incretin hormone glucagon-like peptide-1. Proc Nat Acad Sci U S A 89:
10 Diabetologia (27) 5: Li L, EI-Kholy W, Rhodes CJ, Brubaker PL (25) Glucagonlike peptide-1 protects beta cells from cytokine-induced apoptosis and necrosis: role of protein kinase B. Diabetologia 48: Accili D (24) The struggle for mystery in insulin action: from triumvirate to republic. Diabetes 53: Kitamura T, Nakae J, Kitamura Y, Kido Y, Accili D (22) The forkhead transcription factor Foxo1 links insulin signaling to Pdx1 regulation of pancreatic beta cell growth. J Clin Invest 11: Hansen L, Deacon CF, Ørskov C, Holst JJ (25) Glucagon-like peptide-1-(7 36)amide is transformed to glucagon-like peptide-1- (9 36)amide by dipeptidyl peptidase IV in the capillaries supplying the L cells of the porcine intestine. Endocrinology 14: Nauck MA, Meier JJ (25) Glucagon-like peptide 1 and its derivatives in the treatment of diabetes. Regul Pept 128:
NIH Public Access Author Manuscript Diabetologia. Author manuscript; available in PMC 2014 February 01.
 NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
NIH Public Access Author Manuscript Published in final edited form as: Diabetologia. 2013 February ; 56(2): 231 233. doi:10.1007/s00125-012-2788-6. Lipotoxicity impairs incretin signalling V. Poitout 1,2
Discussion & Conclusion
 Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
Discussion & Conclusion 7. Discussion DPP-4 inhibitors augment the effects of incretin hormones by prolonging their half-life and represent a new therapeutic approach for the treatment of type 2 diabetes
The Effects of Exenatide on the Autoimmune Development of Diabetes. A Senior Honors Thesis
 The Effects of Exenatide on the Autoimmune Development of Diabetes A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for Graduation with Distinction in Microbiology in the Undergraduate
The Effects of Exenatide on the Autoimmune Development of Diabetes A Senior Honors Thesis Presented in Partial Fulfillment of the Requirements for Graduation with Distinction in Microbiology in the Undergraduate
Near-normalisation of diurnal glucose concentrations by continuous administration of glucagon-like peptide-1 (GLP-1) in subjects with NIDDM
 Diabetologia (1997) : 5 11 Springer-Verlag 1997 Near-normalisation of diurnal glucose concentrations by continuous administration of glucagon-like peptide-1 () in subjects with NIDDM J. Rachman, B. A.
Diabetologia (1997) : 5 11 Springer-Verlag 1997 Near-normalisation of diurnal glucose concentrations by continuous administration of glucagon-like peptide-1 () in subjects with NIDDM J. Rachman, B. A.
Figure legends Supplemental Fig.1. Glucose-induced insulin secretion and insulin content of islets. Supplemental Fig. 2.
 Figure legends Supplemental Fig.. Glucose-induced insulin secretion and insulin content of islets. Insulin secretory responses to.,., and. mm glucose (A) (n = 7-), and the insulin content in the islets
Figure legends Supplemental Fig.. Glucose-induced insulin secretion and insulin content of islets. Insulin secretory responses to.,., and. mm glucose (A) (n = 7-), and the insulin content in the islets
SHORT COMMUNICATION. J. C. Reubi & A. Perren & R. Rehmann & B. Waser & E. Christ & M. Callery & A. B. Goldfine & M. E. Patti
 Diabetologia (2010) 53:2641 2645 DOI 10.1007/s00125-010-1901-y SHORT COMMUNICATION Glucagon-like peptide-1 (GLP-1) receptors are not overexpressed in pancreatic islets from patients with severe hyperinsulinaemic
Diabetologia (2010) 53:2641 2645 DOI 10.1007/s00125-010-1901-y SHORT COMMUNICATION Glucagon-like peptide-1 (GLP-1) receptors are not overexpressed in pancreatic islets from patients with severe hyperinsulinaemic
A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets
 Diabetologia () 5:77 DOI.7/s5--- SHORT COMMUNICATION A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets Q. Cheng & Y. C.
Diabetologia () 5:77 DOI.7/s5--- SHORT COMMUNICATION A novel role for vitamin D: modulation of expression and function of the local renin angiotensin system in mouse pancreatic islets Q. Cheng & Y. C.
islets scored 1 week month months
 Supplementary Table 1. Sampling parameters for the morphometrical analyses Time (post- DT) Control mice (age-matched) α-cells mice pancreatic surface (mm 2 ) scored DT-treated mice islets scored mice pancreatic
Supplementary Table 1. Sampling parameters for the morphometrical analyses Time (post- DT) Control mice (age-matched) α-cells mice pancreatic surface (mm 2 ) scored DT-treated mice islets scored mice pancreatic
Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans BO AHRÉN, MD, PHD 1 JENS J. HOLST, MD, PHD 2 ANDREA
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Characterization of GLP-1 Effects on -Cell Function After Meal Ingestion in Humans BO AHRÉN, MD, PHD 1 JENS J. HOLST, MD, PHD 2 ANDREA
GLP-1 agonists. Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK
 GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
GLP-1 agonists Ian Gallen Consultant Community Diabetologist Royal Berkshire Hospital Reading UK What do GLP-1 agonists do? Physiology of postprandial glucose regulation Meal ❶ ❷ Insulin Rising plasma
Scope. History. History. Incretins. Incretin-based Therapy and DPP-4 Inhibitors
 Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
Plasma Glucose (mg/dl) Plasma Insulin (pmol/l) Incretin-based Therapy and Inhibitors Scope Mechanism of action ผศ.ดร.นพ.ว ระเดช พ ศประเสร ฐ สาขาว ชาโภชนว ทยาคล น ก ภาคว ชาอาย รศาสตร คณะแพทยศาสตร มหาว ทยาล
(Incretin) ( glucagon-like peptide-1 GLP-1 ) GLP-1. GLP-1 ( dipeptidyl peptidase IV DPP IV ) GLP-1 DPP IV GLP-1 exenatide liraglutide FDA 2 2 2
 007 18 189-194 (Incretin) Incretin ( ) -1 ( glucagon-like peptide-1 ) ( dipeptidyl peptidase IV ) liraglutide FDA ( Type diabetes mellitus ) -1 ( Glucagon-like peptide-1, ) ( Incretin ) ( Dipeptidyl peptidase
007 18 189-194 (Incretin) Incretin ( ) -1 ( glucagon-like peptide-1 ) ( dipeptidyl peptidase IV ) liraglutide FDA ( Type diabetes mellitus ) -1 ( Glucagon-like peptide-1, ) ( Incretin ) ( Dipeptidyl peptidase
Supporting Information
 Supporting Information Pang et al. 10.1073/pnas.1322009111 SI Materials and Methods ELISAs. These assays were performed as previously described (1). ELISA plates (MaxiSorp Nunc; Thermo Fisher Scientific)
Supporting Information Pang et al. 10.1073/pnas.1322009111 SI Materials and Methods ELISAs. These assays were performed as previously described (1). ELISA plates (MaxiSorp Nunc; Thermo Fisher Scientific)
Perspectives Home > Literature > Perspectives > Holz et al., pp. pe2
 AAAS Science's STKE Holz et al., pp. pe2 http://stke.sciencemag.org/cgi/content/abstract/sigtrans;2005/268/pe2... Institution: NEW YORK UNIV MED CENTER Sign In as Individual Access Rights Subscription
AAAS Science's STKE Holz et al., pp. pe2 http://stke.sciencemag.org/cgi/content/abstract/sigtrans;2005/268/pe2... Institution: NEW YORK UNIV MED CENTER Sign In as Individual Access Rights Subscription
Supplementary Table 1. Antibodies and dilutions used in the immunohistochemical study
 Supplementary Table 1. Antibodies and dilutions used in the immunohistochemical study Antigen Species Clone Source Dilution Insulin Guinea pig - Dako, Carpinteria, 1:200 Glucagon Rabbit - Dako, Carpinteria,
Supplementary Table 1. Antibodies and dilutions used in the immunohistochemical study Antigen Species Clone Source Dilution Insulin Guinea pig - Dako, Carpinteria, 1:200 Glucagon Rabbit - Dako, Carpinteria,
Supporting Information
 Supporting Information Soltani et al. 10.1073/pnas.1102715108 SI Experimental Procedures Evaluation of Mice and Drug Administration. IPGTT, insulin tolerance test, and glucagon tolerance test were performed
Supporting Information Soltani et al. 10.1073/pnas.1102715108 SI Experimental Procedures Evaluation of Mice and Drug Administration. IPGTT, insulin tolerance test, and glucagon tolerance test were performed
Div. of Endocrinology and Metabolism Konyang University, School of Medicine. Byung-Joon Kim M.D., Ph.D.
 Diabetes and Thyroid Center Div. of Endocrinology and Metabolism Konyang University, School of Medicine Byung-Joon Kim M.D., Ph.D. Background Incretin effect and GLP 1 Receptor in L cells TGR5 receptor
Diabetes and Thyroid Center Div. of Endocrinology and Metabolism Konyang University, School of Medicine Byung-Joon Kim M.D., Ph.D. Background Incretin effect and GLP 1 Receptor in L cells TGR5 receptor
Gamma-aminobutyric acid (GABA) treatment blocks inflammatory pathways and promotes survival and proliferation of pancreatic beta cells
 Gamma-aminobutyric acid (GABA) treatment blocks inflammatory pathways and promotes survival and proliferation of pancreatic beta cells Gérald J. Prud homme, MD, FRCPC Keenan Research Centre for Biomedical
Gamma-aminobutyric acid (GABA) treatment blocks inflammatory pathways and promotes survival and proliferation of pancreatic beta cells Gérald J. Prud homme, MD, FRCPC Keenan Research Centre for Biomedical
Inflammation & Type 2 Diabetes Prof. Marc Y. Donath
 Inflammation & Type 2 Diabetes 1, MD Chief Endocrinology, Diabetes & Metabolism University Hospital Basel Petersgraben 4 CH-431 Basel, Switzerland MDonath@uhbs.ch Innate immunity as a sensor of metabolic
Inflammation & Type 2 Diabetes 1, MD Chief Endocrinology, Diabetes & Metabolism University Hospital Basel Petersgraben 4 CH-431 Basel, Switzerland MDonath@uhbs.ch Innate immunity as a sensor of metabolic
Megan Lawless. Journal Club. January 20 th, 2011
 Megan Lawless Journal Club January 20 th, 2011 Gut-expressed gustducin and taste receptors regulate secretion of glucagon-like peptide-1 Proceedings of the National Academy of Sciences September 2007 Abstract
Megan Lawless Journal Club January 20 th, 2011 Gut-expressed gustducin and taste receptors regulate secretion of glucagon-like peptide-1 Proceedings of the National Academy of Sciences September 2007 Abstract
adenosine triphosphate-sensitive K[ Citation Journal of Diabetes Investigation ( modifications or adaptations are ma
 Fructose induces glucose-dependent Titleglucagon-like peptide-1 and insulin adenosine triphosphate-sensitive K[ Seino, Yusuke; Ogata, Hidetada; Mae Author(s) Takako; Iida, Atsushi; Harada, Nori Susumu;
Fructose induces glucose-dependent Titleglucagon-like peptide-1 and insulin adenosine triphosphate-sensitive K[ Seino, Yusuke; Ogata, Hidetada; Mae Author(s) Takako; Iida, Atsushi; Harada, Nori Susumu;
SUPPLEMENTARY DATA. Supplementary Table 2. Antibodies used for Immunofluoresence. Supplementary Table 3. Real-time PCR primer sequences.
 Supplementary Table 2. Antibodies used for Immunofluoresence. Antibody Dilution Source Goat anti-pdx1 1:100 R&D Systems Rabbit anti-hnf6 1:100 Santa Cruz Biotechnology Mouse anti-nkx6.1 1:200 Developmental
Supplementary Table 2. Antibodies used for Immunofluoresence. Antibody Dilution Source Goat anti-pdx1 1:100 R&D Systems Rabbit anti-hnf6 1:100 Santa Cruz Biotechnology Mouse anti-nkx6.1 1:200 Developmental
Supplementary Table 1. The primers used for quantitative RT-PCR. Gene name Forward (5 > 3 ) Reverse (5 > 3 )
 770 771 Supplementary Table 1. The primers used for quantitative RT-PCR. Gene name Forward (5 > 3 ) Reverse (5 > 3 ) Human CXCL1 GCGCCCAAACCGAAGTCATA ATGGGGGATGCAGGATTGAG PF4 CCCCACTGCCCAACTGATAG TTCTTGTACAGCGGGGCTTG
770 771 Supplementary Table 1. The primers used for quantitative RT-PCR. Gene name Forward (5 > 3 ) Reverse (5 > 3 ) Human CXCL1 GCGCCCAAACCGAAGTCATA ATGGGGGATGCAGGATTGAG PF4 CCCCACTGCCCAACTGATAG TTCTTGTACAGCGGGGCTTG
Mouse GLP-2 EIA FOR LABORATORY USE ONLY
 YK142 Mouse GLP-2 EIA FOR LABORATORY USE ONLY Kasumigaseki place, 3-6-7, Kasumigaseki, Chiyoda-ku, Tokyo 100-0013 Japan http://www.sceti.co.jp/english/export e-mail exp-pet@sceti.co.jp
YK142 Mouse GLP-2 EIA FOR LABORATORY USE ONLY Kasumigaseki place, 3-6-7, Kasumigaseki, Chiyoda-ku, Tokyo 100-0013 Japan http://www.sceti.co.jp/english/export e-mail exp-pet@sceti.co.jp
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans
 The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
The enteroinsular axis in the pathogenesis of prediabetes and diabetes in humans Young Min Cho, MD, PhD Division of Endocrinology and Metabolism Seoul National University College of Medicine Plasma glucose
Diabetes: What is the scope of the problem?
 Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
Diabetes: What is the scope of the problem? Elizabeth R. Seaquist MD Division of Endocrinology and Diabetes Department of Medicine Director, General Clinical Research Center Pennock Family Chair in Diabetes
The glucoincretin hormone glucagon-like peptide-1
 Original Article Transcription Factor FoxO1 Mediates Glucagon-Like Peptide-1 Effects on Pancreatic -Cell Mass Jean Buteau, Marianne L. Spatz, and Domenico Accili The glucoincretin hormone glucagon-like
Original Article Transcription Factor FoxO1 Mediates Glucagon-Like Peptide-1 Effects on Pancreatic -Cell Mass Jean Buteau, Marianne L. Spatz, and Domenico Accili The glucoincretin hormone glucagon-like
EXENDIN-4 IS A 39-amino acid reptilian peptide that
 0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(7):3469 3473 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032001 Exendin-4 Normalized Postcibal
0021-972X/04/$15.00/0 The Journal of Clinical Endocrinology & Metabolism 89(7):3469 3473 Printed in U.S.A. Copyright 2004 by The Endocrine Society doi: 10.1210/jc.2003-032001 Exendin-4 Normalized Postcibal
Receptor-interacting Protein Kinases Mediate Necroptosis In Neural Tissue Damage After Spinal Cord Injury
 Receptor-interacting Protein Kinases Mediate Necroptosis In Neural Tissue Damage After Spinal Cord Injury Haruo Kanno, M.D., Ph.D., Hiroshi Ozawa, M.D., Ph.D., Satoshi Tateda, M.D., Kenichiro Yahata, M.D.,
Receptor-interacting Protein Kinases Mediate Necroptosis In Neural Tissue Damage After Spinal Cord Injury Haruo Kanno, M.D., Ph.D., Hiroshi Ozawa, M.D., Ph.D., Satoshi Tateda, M.D., Kenichiro Yahata, M.D.,
Endocannabinoid-activated Nlrp3 inflammasome in infiltrating macrophages mediates β- cell loss in type 2 diabetes
 Endocannabinoid-activated Nlrp3 inflammasome in infiltrating macrophages mediates β- cell loss in type 2 diabetes T Jourdan, G Godlewski, R Cinar, A Bertola, G Szanda, J Liu, J Tam, T Han, B Mukhopadhyay,
Endocannabinoid-activated Nlrp3 inflammasome in infiltrating macrophages mediates β- cell loss in type 2 diabetes T Jourdan, G Godlewski, R Cinar, A Bertola, G Szanda, J Liu, J Tam, T Han, B Mukhopadhyay,
Diabetes 2013: Achieving Goals Through Comprehensive Treatment. Session 2: Individualizing Therapy
 Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
Diabetes 2013: Achieving Goals Through Comprehensive Treatment Session 2: Individualizing Therapy Joshua L. Cohen, M.D., F.A.C.P. Professor of Medicine Interim Director, Division of Endocrinology & Metabolism
β-cell Preservation and Regeneration After Islet Transplantation
 β-cell Preservation and Regeneration After Islet Transplantation Jyuhn-Huarng Juang, MD Division of Endocrinology and Metabolism, Department of Internal Medicine, Chang Gung University and Memorial Hospital,
β-cell Preservation and Regeneration After Islet Transplantation Jyuhn-Huarng Juang, MD Division of Endocrinology and Metabolism, Department of Internal Medicine, Chang Gung University and Memorial Hospital,
Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients
 Diabetologia (2002) 45:1111 1119 DOI 10.1007/s00125-002-0878-6 Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients T. Vilsbøll 1, 2, T. Krarup
Diabetologia (2002) 45:1111 1119 DOI 10.1007/s00125-002-0878-6 Defective amplification of the late phase insulin response to glucose by GIP in obese Type II diabetic patients T. Vilsbøll 1, 2, T. Krarup
INJECTABLE THERAPIES IN DIABETES. Barbara Ann McKee Diabetes Specialist Nurse
 INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
INJECTABLE THERAPIES IN DIABETES Barbara Ann McKee Diabetes Specialist Nurse 1 Aims of the session Describe the different injectable agents for diabetes and when they would be used. Describe some common
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP
 Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
Sitagliptin: first DPP-4 inhibitor to treat type 2 diabetes Steve Chaplin MSc, MRPharmS and Andrew Krentz MD, FRCP KEY POINTS sitagliptin (Januvia) is a DPP-4 inhibitor that blocks the breakdown of the
Glucagon-like Peptide-1 Can Reverse the Age-related Decline in Glucose Tolerance in Rats
 Glucagon-like Peptide-1 Can Reverse the Age-related Decline in Glucose Tolerance in Rats Yihong Wang, Riccardo Perfetti, Nigel H. Greig, Harold W. Holloway, Kimberly A. DeOre, Chahrzad Montrose-Rafizadeh,
Glucagon-like Peptide-1 Can Reverse the Age-related Decline in Glucose Tolerance in Rats Yihong Wang, Riccardo Perfetti, Nigel H. Greig, Harold W. Holloway, Kimberly A. DeOre, Chahrzad Montrose-Rafizadeh,
Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/-
 Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Supplemental Material Results. Expression of acid base transporters in the kidney collecting duct in Slc2a7 -/- and Slc2a7 -/- mice. The expression of AE1 in the kidney was examined in Slc26a7 KO mice.
Role of incretins in the treatment of type 2 diabetes
 Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
Role of incretins in the treatment of type 2 diabetes Jens Juul Holst Department of Medical Physiology Panum Institute University of Copenhagen Denmark Diabetes & Obesity Spanish Society of Internal Medicine
la prise en charge du diabète de
 N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
N21 XIII Congrès National de Diabétologie, 29 mai 2011, Alger Intérêt et place des Anti DPP4 dans la prise en charge du diabète de type 2 Nicolas PAQUOT, MD, PhD CHU Sart-Tilman, Université de Liège Belgique
Glucagon-like peptide-1 treatment delays the onset of diabetes in 8 week-old db/db mice
 Diabetologia (2002) 45:1263 1273 DOI 10.1007/s00125-002-0828-3 Glucagon-like peptide-1 treatment delays the onset of diabetes in 8 week-old db/db mice Q. Wang 1, P. L. Brubaker 1, 2 1 Departments of Physiology
Diabetologia (2002) 45:1263 1273 DOI 10.1007/s00125-002-0828-3 Glucagon-like peptide-1 treatment delays the onset of diabetes in 8 week-old db/db mice Q. Wang 1, P. L. Brubaker 1, 2 1 Departments of Physiology
Chief of Endocrinology East Orange General Hospital
 Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Targeting the Incretins System: Can it Improve Our Ability to Treat Type 2 Diabetes? Darshi Sunderam, MD Darshi Sunderam, MD Chief of Endocrinology East Orange General Hospital Age-adjusted Percentage
Difference in glucagon-like peptide-1 concentrations between C-peptide negative type 1 diabetes mellitus patients and healthy controls
 Original Article Annals of Clinical Biochemistry 2015, Vol. 52(2) 220 225! The Author(s) 2014 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: 10.1177/0004563214544709 acb.sagepub.com
Original Article Annals of Clinical Biochemistry 2015, Vol. 52(2) 220 225! The Author(s) 2014 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: 10.1177/0004563214544709 acb.sagepub.com
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function
 Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Effect of macronutrients and mixed meals on incretin hormone secretion and islet cell function Background. Following meal ingestion, several hormones are released from the gastrointestinal tract. Some
Interleukin-6 enhances insulin secretion by increasing L cell and cell glucagon-like peptide-1 secretion
 Supplementary online material to Interleukin-6 enhances insulin secretion by increasing L cell and cell glucagon-like peptide-1 secretion Helga Ellingsgaard 1, Irina Hauselmann 1, Beat Schuler 2, Abdella
Supplementary online material to Interleukin-6 enhances insulin secretion by increasing L cell and cell glucagon-like peptide-1 secretion Helga Ellingsgaard 1, Irina Hauselmann 1, Beat Schuler 2, Abdella
Exendin-4-mediated cell proliferation in beta-cells: focusing on the transcription factors
 Exendin-4-mediated cell proliferation in beta-cells: focusing on the transcription factors Seo-Yoon Chang, Jae Min Cho, Yang-Hyeok Jo, Myung-Jun Kim Departments of Physiology, College of Medicine, The
Exendin-4-mediated cell proliferation in beta-cells: focusing on the transcription factors Seo-Yoon Chang, Jae Min Cho, Yang-Hyeok Jo, Myung-Jun Kim Departments of Physiology, College of Medicine, The
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES
 INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
INJECTABLE THERAPY FOR THE TREATMENT OF DIABETES ARSHNA SANGHRAJKA DIABETES SPECIALIST PRESCRIBING PHARMACIST OBJECTIVES EXPLORE THE TYPES OF INSULIN AND INJECTABLE DIABETES TREATMENTS AND DEVICES AVAILABLE
GLP 1 agonists Winning the Losing Battle. Dr Bernard SAMIA. KCS Congress: Impact through collaboration
 GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
GLP 1 agonists Winning the Losing Battle Dr Bernard SAMIA KCS Congress: Impact through collaboration CONTACT: Tel. +254 735 833 803 Email: kcardiacs@gmail.com Web: www.kenyacardiacs.org Disclosures I have
Update on GLP-1 Past Present Future
 Update on GLP-1 p Past Present Future Effects of GLP-1: Glucose Metabolism and Nutritional Balance L-Cells: Glp-1 release Betacellfollowing ingestion Stress Increases satiety reduces appetite Betacell-
Update on GLP-1 p Past Present Future Effects of GLP-1: Glucose Metabolism and Nutritional Balance L-Cells: Glp-1 release Betacellfollowing ingestion Stress Increases satiety reduces appetite Betacell-
22 Emerging Therapies for
 22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
22 Emerging Therapies for Treatment of Type 2 Diabetes Siddharth N Shah Abstract: The prevalence of Diabetes is progressively increasing world-wide and the growth of the disease in our country is phenomenal.
New and Emerging Therapies for Type 2 DM
 Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Dale Clayton MHSc, MD, FRCPC Dalhousie University/Capital Health April 28, 2011 New and Emerging Therapies for Type 2 DM The science of today, is the technology of tomorrow. Edward Teller American Physicist
Središnja medicinska knjižnica
 Središnja medicinska knjižnica Zibar K., Knežević Ćuća J., Blaslov K., Bulum T., Smirčić-Duvnjak L. (2015) Difference in glucagon-like peptide-1 concentrations between C-peptide negative type 1 diabetes
Središnja medicinska knjižnica Zibar K., Knežević Ćuća J., Blaslov K., Bulum T., Smirčić-Duvnjak L. (2015) Difference in glucagon-like peptide-1 concentrations between C-peptide negative type 1 diabetes
Glucagon-like peptide 1(GLP-1)
 Emerging Treatments and Technologies O R I G I N A L A R T I C L E Differential Effects of Acute and Extended Infusions of Glucagon-Like Peptide-1 on First- and Second-Phase Insulin Secretion in Diabetic
Emerging Treatments and Technologies O R I G I N A L A R T I C L E Differential Effects of Acute and Extended Infusions of Glucagon-Like Peptide-1 on First- and Second-Phase Insulin Secretion in Diabetic
GLP-1 receptor agonists for type 2 diabetes A rationale drug. development. Bo Ahrén
 PROF. BO AHREN (Orcid ID : 0000-0002-9804-5340) Article type : Mini Review GLP-1 receptor agonists for type 2 diabetes A rationale drug development Bo Ahrén Department of Clinical Sciences Lund, Lund University,
PROF. BO AHREN (Orcid ID : 0000-0002-9804-5340) Article type : Mini Review GLP-1 receptor agonists for type 2 diabetes A rationale drug development Bo Ahrén Department of Clinical Sciences Lund, Lund University,
Making Mature Human Islet Cells from Stem Cells to Model Disease and Treat Diabetes
 University of British Columbia Departments of Surgery and Cellular & Physiological Sciences Making Mature Human Islet Cells from Stem Cells to Model Disease and Treat Diabetes 2016 International Conference
University of British Columbia Departments of Surgery and Cellular & Physiological Sciences Making Mature Human Islet Cells from Stem Cells to Model Disease and Treat Diabetes 2016 International Conference
Supplementary Figure 1: Hsp60 / IEC mice are embryonically lethal (A) Light microscopic pictures show mouse embryos at developmental stage E12.
 Supplementary Figure 1: Hsp60 / IEC mice are embryonically lethal (A) Light microscopic pictures show mouse embryos at developmental stage E12.5 and E13.5 prepared from uteri of dams and subsequently genotyped.
Supplementary Figure 1: Hsp60 / IEC mice are embryonically lethal (A) Light microscopic pictures show mouse embryos at developmental stage E12.5 and E13.5 prepared from uteri of dams and subsequently genotyped.
Voglibose, an Alpha-glucosidase Inhibitor, to Increase Active Glucagon-like Peptide-1 Levels
 PharmSight TM DOI: 10.4255/mcpharmacol.09.22 Molecular and Cellular Pharmacology www.mcpharmacol.com Voglibose, an Alpha-glucosidase Inhibitor, to Increase Active Glucagon-like Peptide-1 Levels Yusuke
PharmSight TM DOI: 10.4255/mcpharmacol.09.22 Molecular and Cellular Pharmacology www.mcpharmacol.com Voglibose, an Alpha-glucosidase Inhibitor, to Increase Active Glucagon-like Peptide-1 Levels Yusuke
Supplementary Figure 1: Steviol and stevioside potentiate TRPM5 in a cell-free environment. (a) TRPM5 currents are activated in inside-out patches
 Supplementary Figure 1: Steviol and stevioside potentiate TRPM5 in a cell-free environment. (a) TRPM5 currents are activated in inside-out patches during application of 500 µm Ca 2+ at the intracellular
Supplementary Figure 1: Steviol and stevioside potentiate TRPM5 in a cell-free environment. (a) TRPM5 currents are activated in inside-out patches during application of 500 µm Ca 2+ at the intracellular
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM
 The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
The Mediterranean Diet: HOW and WHY It Works So Well for T2DM Susan L. Barlow, RD, CDE. Objectives 1. Discuss the effects of meal size on GLP-1 concentrations. 2. Compare and contrast the specific effects
Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
 Diabetologia (28) 1:632 64 DOI 1.17/s1-8-943-x ARTICLE Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
Diabetologia (28) 1:632 64 DOI 1.17/s1-8-943-x ARTICLE Near normalisation of blood glucose improves the potentiating effect of GLP-1 on glucose-induced insulin secretion in patients with type 2 diabetes
Rat Glicentin EIA FOR RESEARCH USE ONLY. <Distributed by> DF Kasumigaseki Place, 3-6-7, Kasumigaseki, Chiyoda-ku Tokyo Japan
 YK111 Rat Glicentin EIA FOR RESEARCH USE ONLY DF Kasumigaseki Place, 3-6-7, Kasumigaseki, Chiyoda-ku Tokyo 100-0013 Japan URL: http://www.sceti.co.jp/export/ e-mail: exp-pet@sceti.co.jp
YK111 Rat Glicentin EIA FOR RESEARCH USE ONLY DF Kasumigaseki Place, 3-6-7, Kasumigaseki, Chiyoda-ku Tokyo 100-0013 Japan URL: http://www.sceti.co.jp/export/ e-mail: exp-pet@sceti.co.jp
IMIDIA IMPROVING BETA-CELL FUNCTION AND IDENTIFICATION OF DIAGNOSTIC BIOMARKERS FOR TREATMENT MONITORING IN DIABETES. A. Ktorza, B.
 IMIDIA IMPROVING BETA-CELL FUNCTION AND IDENTIFICATION OF DIAGNOSTIC BIOMARKERS FOR TREATMENT MONITORING IN DIABETES A. Ktorza, B. Thorens DIABETES Definition Diabetes is a metabolic disease characterized
IMIDIA IMPROVING BETA-CELL FUNCTION AND IDENTIFICATION OF DIAGNOSTIC BIOMARKERS FOR TREATMENT MONITORING IN DIABETES A. Ktorza, B. Thorens DIABETES Definition Diabetes is a metabolic disease characterized
(A) PCR primers (arrows) designed to distinguish wild type (P1+P2), targeted (P1+P2) and excised (P1+P3)14-
 1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
1 Supplemental Figure Legends Figure S1. Mammary tumors of ErbB2 KI mice with 14-3-3σ ablation have elevated ErbB2 transcript levels and cell proliferation (A) PCR primers (arrows) designed to distinguish
Supplementary Information. Induction of human pancreatic beta cell replication by inhibitors of dual specificity tyrosine regulated kinase
 Journal: Nature Medicine Supplementary Information Induction of human pancreatic beta cell replication by inhibitors of dual specificity tyrosine regulated kinase 1,2 Peng Wang PhD, 1,2 Juan-Carlos Alvarez-Perez
Journal: Nature Medicine Supplementary Information Induction of human pancreatic beta cell replication by inhibitors of dual specificity tyrosine regulated kinase 1,2 Peng Wang PhD, 1,2 Juan-Carlos Alvarez-Perez
Islet viability assay and Glucose Stimulated Insulin Secretion assay RT-PCR and Western Blot
 Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Islet viability assay and Glucose Stimulated Insulin Secretion assay Islet cell viability was determined by colorimetric (3-(4,5-dimethylthiazol-2-yl)-2,5- diphenyltetrazolium bromide assay using CellTiter
Treating Type 2 Diabetes with Bariatric Surgery. Goal of Treating T2DM. Remission of T2DM with Bariatric
 Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Treating Type 2 Diabetes with Bariatric Surgery Number (in Millions) of Persons with Diagnosed Diabetes, United States, 198 25 The number of Americans with diabetes increased from 5.6 to 15.8 million Guilherme
Figure S1. B % of Phosphorylation 32H. 32ss
 Figure S1 8H 32ss 32H 32Hc % of Phosphorylation 3 32H 2 1 32ss 1 2 3 4 Extract (μg) C % of Phosphorylation 18 12 6-32H 32Hc 8H 32ss Dbait Figure S1. List of the Dbait molecules and activation of DN-PK
Figure S1 8H 32ss 32H 32Hc % of Phosphorylation 3 32H 2 1 32ss 1 2 3 4 Extract (μg) C % of Phosphorylation 18 12 6-32H 32Hc 8H 32ss Dbait Figure S1. List of the Dbait molecules and activation of DN-PK
Zurich Open Repository and Archive. The dipeptidyl peptidase IV inhibitor NVP-DPP728 reduces plasma glucagon concentration in cats
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 The dipeptidyl peptidase IV inhibitor NVP-DPP728 reduces plasma glucagon concentration
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2009 The dipeptidyl peptidase IV inhibitor NVP-DPP728 reduces plasma glucagon concentration
Journal Club WS 2012/13 Stefanie Nickl
 Journal Club WS 2012/13 Stefanie Nickl Background Mesenchymal Stem Cells First isolation from bone marrow 30 ys ago Isolation from: spleen, heart, skeletal muscle, synovium, amniotic fluid, dental pulp,
Journal Club WS 2012/13 Stefanie Nickl Background Mesenchymal Stem Cells First isolation from bone marrow 30 ys ago Isolation from: spleen, heart, skeletal muscle, synovium, amniotic fluid, dental pulp,
GLP-2 (Rat) ELISA. For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma
 GLP-2 (Rat) ELISA For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2RT-E01
GLP-2 (Rat) ELISA For the quantitative determination of glucagon-like peptide 2 (GLP-2) in rat serum and plasma For Research Use Only. Not For Use In Diagnostic Procedures. Catalog Number: 48-GP2RT-E01
My Journey in Endocrinology. Samuel Cataland M.D
 My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
My Journey in Endocrinology Samuel Cataland M.D. 1968-2015 Drs Berson M.D. Yalow phd Insulin Radioimmunoassay Nobel Prize Physiology or Medicine 1977 Rosalyn Yalow: Radioimmunoassay Technology Andrew Schally
Prior in vitro exposure to GLP-1 with or without GIP can influence the subsequent beta cell responsiveness
 Biochemical Pharmacology 68 (2004) 33 39 Prior in vitro exposure to GLP-1 with or without GIP can influence the subsequent beta cell responsiveness Dominique Delmeire, Daisy Flamez, Karen Moens, Simon
Biochemical Pharmacology 68 (2004) 33 39 Prior in vitro exposure to GLP-1 with or without GIP can influence the subsequent beta cell responsiveness Dominique Delmeire, Daisy Flamez, Karen Moens, Simon
Current Status of Incretin Based Therapies in Type 2 Diabetes
 Current Status of Incretin Based Therapies in Type 2 Diabetes DR.M.Mukhyaprana Prabhu Professor of Internal Medicine Kasturba Medical College, Manipal, Manipal University, India 2 nd International Endocrine
Current Status of Incretin Based Therapies in Type 2 Diabetes DR.M.Mukhyaprana Prabhu Professor of Internal Medicine Kasturba Medical College, Manipal, Manipal University, India 2 nd International Endocrine
THE INCRETIN hormones gastrin inhibitory polypeptide
 0021-972X/97/$03.00/0 Vol. 82, No. 3 Journal of Clinical Endocrinology and Metabolism Printed in U.S.A. Copyright 1997 by The Endocrine Society Rapid Oscillations in Plasma Glucagon-Like Peptide-1 (GLP-1)
0021-972X/97/$03.00/0 Vol. 82, No. 3 Journal of Clinical Endocrinology and Metabolism Printed in U.S.A. Copyright 1997 by The Endocrine Society Rapid Oscillations in Plasma Glucagon-Like Peptide-1 (GLP-1)
Abstract. Effect of sitagliptin on glycemic control in patients with type 2 diabetes. Introduction. Abbas Mahdi Rahmah
 Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
Effect of sitagliptin on glycemic control in patients with type 2 diabetes Abbas Mahdi Rahmah Correspondence: Dr. Abbas Mahdi Rahmah Consultant Endocrinologist, FRCP (Edin) Director of Iraqi National Diabetes
Despite substantial advances in our understanding
 Dipeptidyl Peptidase IV Inhibitor Treatment Stimulates -Cell Survival and Islet Neogenesis in Streptozotocin-Induced Diabetic Rats J. Andrew Pospisilik, 1 Jennifer Martin, 1 Timothy Doty, 1 Jan A. Ehses,
Dipeptidyl Peptidase IV Inhibitor Treatment Stimulates -Cell Survival and Islet Neogenesis in Streptozotocin-Induced Diabetic Rats J. Andrew Pospisilik, 1 Jennifer Martin, 1 Timothy Doty, 1 Jan A. Ehses,
Insulin Resistance. Biol 405 Molecular Medicine
 Insulin Resistance Biol 405 Molecular Medicine Insulin resistance: a subnormal biological response to insulin. Defects of either insulin secretion or insulin action can cause diabetes mellitus. Insulin-dependent
Insulin Resistance Biol 405 Molecular Medicine Insulin resistance: a subnormal biological response to insulin. Defects of either insulin secretion or insulin action can cause diabetes mellitus. Insulin-dependent
Abbreviations: P- paraffin-embedded section; C, cryosection; Bio-SA, biotin-streptavidin-conjugated fluorescein amplification.
 Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
Supplementary Table 1. Sequence of primers for real time PCR. Gene Forward primer Reverse primer S25 5 -GTG GTC CAC ACT ACT CTC TGA GTT TC-3 5 - GAC TTT CCG GCA TCC TTC TTC-3 Mafa cds 5 -CTT CAG CAA GGA
Short communication. Abstract
 Diabetologia (1999) 42: 574±578 Short communication Ó Springer-Verlag 1999 Immunological abnormalities in islets at diagnosis paralleled further deterioration of glycaemic control in patients with recent-onset
Diabetologia (1999) 42: 574±578 Short communication Ó Springer-Verlag 1999 Immunological abnormalities in islets at diagnosis paralleled further deterioration of glycaemic control in patients with recent-onset
Supplementary Table 1. Primer sequences for conventional RT-PCR on mouse islets
 Supplementary Table 1. Primer sequences for conventional RT-PCR on mouse islets Gene 5 Forward 3 5 Reverse 3.T. Product (bp) ( C) mnox1 GTTCTTGGGCTGCCTTGG GCTGGGGCGGCGG 60 300 mnoxa1 GCTTTGCCGCGTGC GGTTCGGGTCCTTTGTGC
Supplementary Table 1. Primer sequences for conventional RT-PCR on mouse islets Gene 5 Forward 3 5 Reverse 3.T. Product (bp) ( C) mnox1 GTTCTTGGGCTGCCTTGG GCTGGGGCGGCGG 60 300 mnoxa1 GCTTTGCCGCGTGC GGTTCGGGTCCTTTGTGC
SELECTED ABSTRACTS AND POSTER PRESENTATIONS
 SELECTED ABSTRACTS AND POSTER PRESENTATIONS The following summaries are based on abstracts and posters presented at the American Diabetes Association s 65th Annual Scientific Sessions held in San Diego,
SELECTED ABSTRACTS AND POSTER PRESENTATIONS The following summaries are based on abstracts and posters presented at the American Diabetes Association s 65th Annual Scientific Sessions held in San Diego,
Management of Type 2 Diabetes
 Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
Management of Type 2 Diabetes Pathophysiology Insulin resistance and relative insulin deficiency/ defective secretion Not immune mediated No evidence of β cell destruction Increased risk with age, obesity
NIH Public Access Author Manuscript Diabetes Res Clin Pract. Author manuscript; available in PMC 2011 March 1.
 NIH Public Access Author Manuscript Published in final edited form as: Diabetes Res Clin Pract. 2010 March ; 87(3): 322 328. doi:10.1016/j.diabres.2009.12.020. Lack of Preservation of Insulin Gene Expression
NIH Public Access Author Manuscript Published in final edited form as: Diabetes Res Clin Pract. 2010 March ; 87(3): 322 328. doi:10.1016/j.diabres.2009.12.020. Lack of Preservation of Insulin Gene Expression
Impact of Sox9 Dosage and Hes1-mediated Notch Signaling in Controlling the Plasticity of Adult Pancreatic Duct Cells in Mice
 Impact of Sox9 Dosage and Hes1-mediated Notch Signaling in Controlling the Plasticity of Adult Pancreatic Duct Cells in Mice Shinichi Hosokawa 1,3,Kenichiro Furuyama 1,3, Masashi Horiguchi 1,3,Yoshiki
Impact of Sox9 Dosage and Hes1-mediated Notch Signaling in Controlling the Plasticity of Adult Pancreatic Duct Cells in Mice Shinichi Hosokawa 1,3,Kenichiro Furuyama 1,3, Masashi Horiguchi 1,3,Yoshiki
ARTICLE. P. V. Højberg & T. Vilsbøll & R. Rabøl & F. K. Knop & M. Bache & T. Krarup & J. J. Holst & S. Madsbad
 Diabetologia (29) 52:199 27 DOI 1.17/s125-8-1195-5 ARTICLE Four weeks of near-normalisation of blood glucose improves the insulin response to glucagon-like peptide-1 and glucose-dependent insulinotropic
Diabetologia (29) 52:199 27 DOI 1.17/s125-8-1195-5 ARTICLE Four weeks of near-normalisation of blood glucose improves the insulin response to glucagon-like peptide-1 and glucose-dependent insulinotropic
In conjunction with the rising prevalence of diabetes,
 65S Incretin-Based Therapies A Clinical Need Filled by Unique Metabolic Effects Learning Objectives List the 2 major pathophysiologic defects associated with type 2 diabetes. Discuss the barriers to achieving
65S Incretin-Based Therapies A Clinical Need Filled by Unique Metabolic Effects Learning Objectives List the 2 major pathophysiologic defects associated with type 2 diabetes. Discuss the barriers to achieving
Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2],
![Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2], Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2],](/thumbs/86/93801604.jpg) Supplementary information Methods Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2], and A/Hong Kong/213/03 [H5N1]) were grown in Madin-Darby canine kidney (MDCK) cells
Supplementary information Methods Cells and viruses. Human isolates (A/Kawasaki/173/01 [H1N1], A/Yokohama/2057/03 [H3N2], and A/Hong Kong/213/03 [H5N1]) were grown in Madin-Darby canine kidney (MDCK) cells
Control of Glucose Metabolism
 Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
Glucose Metabolism Control of Glucose Metabolism The pancreas is both an exocrine and endocrine gland. It secretes digestive enzymes into the duodenum (exocrine) and 3 specific hormones into the bloodstream
Effect of Glucagon-Like Peptide-1 on - and -Cell Function in C-Peptide-Negative Type 1 Diabetic Patients
 ORIGINAL ARTICLE Endocrine Research Brief Report Effect of Glucagon-Like Peptide-1 on - and -Cell Function in C-Peptide-Negative Type 1 Diabetic Patients Urd Kielgast, Meena Asmar, Sten Madsbad, and Jens
ORIGINAL ARTICLE Endocrine Research Brief Report Effect of Glucagon-Like Peptide-1 on - and -Cell Function in C-Peptide-Negative Type 1 Diabetic Patients Urd Kielgast, Meena Asmar, Sten Madsbad, and Jens
The role of gut hormones in glucose homeostasis
 The role of gut hormones in glucose homeostasis Daniel J. Drucker J Clin Invest. 2007;117(1):24-32. https://doi.org/10.1172/jci30076. Review Series The gastrointestinal tract has a crucial role in the
The role of gut hormones in glucose homeostasis Daniel J. Drucker J Clin Invest. 2007;117(1):24-32. https://doi.org/10.1172/jci30076. Review Series The gastrointestinal tract has a crucial role in the
Incretin Effect and Glucagon Responses to Oral and Intravenous Glucose in Patients With Maturity-Onset Diabetes of the Young Type 2 and Type 3
 2838 Diabetes Volume 63, August 2014 Signe H. Østoft, 1,2,3 Jonatan I. Bagger, 1,2,3 Torben Hansen, 3,4 Oluf Pedersen, 3 Jens J. Holst, 2,3 Filip K. Knop, 1,2,3 and Tina Vilsbøll 1 Incretin Effect and
2838 Diabetes Volume 63, August 2014 Signe H. Østoft, 1,2,3 Jonatan I. Bagger, 1,2,3 Torben Hansen, 3,4 Oluf Pedersen, 3 Jens J. Holst, 2,3 Filip K. Knop, 1,2,3 and Tina Vilsbøll 1 Incretin Effect and
Phospho-AKT Sampler Kit
 Phospho-AKT Sampler Kit E 0 5 1 0 0 3 Kits Includes Cat. Quantity Application Reactivity Source Akt (Ab-473) Antibody E021054-1 50μg/50μl IHC, WB Human, Mouse, Rat Rabbit Akt (Phospho-Ser473) Antibody
Phospho-AKT Sampler Kit E 0 5 1 0 0 3 Kits Includes Cat. Quantity Application Reactivity Source Akt (Ab-473) Antibody E021054-1 50μg/50μl IHC, WB Human, Mouse, Rat Rabbit Akt (Phospho-Ser473) Antibody
Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting. protein3) regulate autophagy and mitophagy in renal tubular cells in. acute kidney injury
 Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting protein3) regulate autophagy and mitophagy in renal tubular cells in acute kidney injury by Masayuki Ishihara 1, Madoka Urushido 2, Kazu Hamada
Sestrin2 and BNIP3 (Bcl-2/adenovirus E1B 19kDa-interacting protein3) regulate autophagy and mitophagy in renal tubular cells in acute kidney injury by Masayuki Ishihara 1, Madoka Urushido 2, Kazu Hamada
Defects in glucose utilization & GLP-1
 Defects in glucose utilization & GLP-1 Song, Dae-Kyu Department of Physiology & Chronic Disease Research Center Keimyung University School of Medicine 2800 dalgubeol-daero, Dalseo-gu, Daegu, 704-701, Korea
Defects in glucose utilization & GLP-1 Song, Dae-Kyu Department of Physiology & Chronic Disease Research Center Keimyung University School of Medicine 2800 dalgubeol-daero, Dalseo-gu, Daegu, 704-701, Korea
glucagon receptor AgRP merged color map I corr = 0.76±0.024 glucagon receptor DAPI merged
 Hypothalamic glucagon signaling inhibits glucose production Patricia I. Mighiu*, Jessica T.Y. Yue*, Beatrice M. Filippi, Mona A. Abraham, Madhu Chari, Carol K.L. Lam, Clair S. Yang, Nikita R. Christian,
Hypothalamic glucagon signaling inhibits glucose production Patricia I. Mighiu*, Jessica T.Y. Yue*, Beatrice M. Filippi, Mona A. Abraham, Madhu Chari, Carol K.L. Lam, Clair S. Yang, Nikita R. Christian,
Metabolic Disease drug discovery at Evotec
 Metabolic Disease drug discovery at Evotec Evotec, Metabolic Disease Drug Discovery, 2016 Evotec, an ideal partner in metabolic disease drug discovery The different ways to work with us On your specific
Metabolic Disease drug discovery at Evotec Evotec, Metabolic Disease Drug Discovery, 2016 Evotec, an ideal partner in metabolic disease drug discovery The different ways to work with us On your specific
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury
 Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
Neutrophils contribute to fracture healing by synthesizing fibronectin+ extracellular matrix rapidly after injury Bastian OW, Koenderman L, Alblas J, Leenen LPH, Blokhuis TJ. Neutrophils contribute to
Spontaneously Diabetic Torii Lepr fa (SDT Fatty) Rat: A Novel Model of Obese Type 2 Diabetes
 30 The Open Diabetes Journal, 2011, 4, 30-36 Open Access Spontaneously Diabetic Torii Lepr fa (SDT Fatty) Rat: A Novel Model of Obese Type 2 Diabetes Sumiaki Fukuda, Katsuhiro Miyajima, Tomohiko Sasase
30 The Open Diabetes Journal, 2011, 4, 30-36 Open Access Spontaneously Diabetic Torii Lepr fa (SDT Fatty) Rat: A Novel Model of Obese Type 2 Diabetes Sumiaki Fukuda, Katsuhiro Miyajima, Tomohiko Sasase
Effects of glucagon-like peptide-1-(7 36)-amide on pancreatic islet and intestinal blood perfusion in Wistar rats and diabetic GK rats
 Clinical Science (2007) 112, 345 351 (Printed in Great Britain) doi:10.1042/cs20060272 345 Effects of glucagon-like peptide-1-(7 36)-amide on pancreatic islet and intestinal blood perfusion in Wistar rats
Clinical Science (2007) 112, 345 351 (Printed in Great Britain) doi:10.1042/cs20060272 345 Effects of glucagon-like peptide-1-(7 36)-amide on pancreatic islet and intestinal blood perfusion in Wistar rats
Glucagon-like peptide-1 (GLP-1), a 30 amino
 Chronic Exposure to GLP-1R Agonists Promotes Homologous GLP-1 Receptor Desensitization In Vitro but Does Not Attenuate GLP-1R Dependent Glucose Homeostasis In Vivo Laurie L. Baggio, Jung-Guk Kim, and Daniel
Chronic Exposure to GLP-1R Agonists Promotes Homologous GLP-1 Receptor Desensitization In Vitro but Does Not Attenuate GLP-1R Dependent Glucose Homeostasis In Vivo Laurie L. Baggio, Jung-Guk Kim, and Daniel
