Dating the abusive head trauma episode and perpetrator statements: key points for imaging
|
|
|
- Angela Sanders
- 6 years ago
- Views:
Transcription
1 DOI /s SPECIAL ISSUE: ABUSIVE HEAD TRAUMA Dating the abusive head trauma episode and perpetrator statements: key points for imaging Catherine Adamsbaum & Baptiste Morel & Béatrice Ducot & Guillemette Antoni & Caroline Rey-Salmon Received: 13 January 2014 /Revised: 30 May 2014 /Accepted: 20 August 2014 # Springer-Verlag Berlin Heidelberg 2014 Abstract Shaken baby syndrome/abusive head trauma is a leading cause of morbidity and mortality in infants. The presence of a diffuse subdural hematoma without evidence of accident is a key diagnostic clue. The hematoma is typically attributed to rupture of the cerebral bridging veins due to violent shaking, with or without impact. Dating the incident, however, remains controversial. The aim of this article is to review the most reliable features used for dating the incident, based on both legal statements by perpetrators and medical documentation. The key points are: 1) The high (yet likely underestimated) frequency of repeated shaking is around 50%, 2) Children do not behave normally immediately after shaking, and the time of onset of even mild symptoms appears to be the best clue for dating the incident and 3) Brain imaging provides strong indicators of age-different injuries but the ranges for dating the causal event are wide. The density pattern in a single subdural hematoma location provides no reliable clues for assessing repeated violence. Only the finding of different density in two distant subdural hematomas argues in favor of age-different injuries, i.e. repeated violence. MRI is difficult to interpret in terms B. Ducot: G. Antoni Université Paris Sud, Faculté de Médecine, Le Kremlin Bicêtre, France C. Adamsbaum (*): B. Morel AP-HP, CHU Bicêtre, Service d Imagerie Pédiatrique, Paris, France c.adamsbaum@bct.aphp.fr B. Ducot INSERM CESP U 1018, Paris, France C. Rey-Salmon AP-HP, CHU Hôtel Dieu, Unité Médico-Judiciaire, Paris, France of dating subdural hemorrhages and must be analyzed in conjunction with CT. Most importantly, all of the child s previous clinical and radiological data must be carefully studied and correlated to provide accurate information on the date and repetition of the trauma. Keywords Subdural hematoma. Dating. Magnetic resonance imaging. Computed tomography. Abusive head trauma. Infant Introduction Shaken baby syndrome also known as abusive head trauma is acknowledged as the most common cause of morbidity and mortality in infants. Diffuse subdural hematoma with no evidence of accident is a key diagnostic marker thought to be related to the tearing of the cerebral bridging veins due to violent shaking [1, 2]. Hypoxic-ischemic injuries are known to be frequently associated to the subdural hematoma and responsible for the outcome of the injured child [1, 2]. Dating the incident, however, remains very controversial as perpetrators rarely admit their actions. The aim of this article is to review the most reliable features used for dating the incident, based on both a literature review including perpetrator admissions [3 5] and our own experience from a retrospective observational series, itself an extension of a previously published study [6]. From a cohort of 280 cases referred to 65 French courts for suspected SBS ( ), we selected 66 cases for which detailed confessions obtained during either police custody or forensic investigations were available. Inclusion criteria were children younger than 4 years of age presenting with a subdural hematoma on
2 computed tomography (CT) and perpetrator admission of a causal relationship between the violence inflicted and the child s symptoms. We analyzed all the written legal statements and correlated them with all the medical records from birth to diagnosis. As judicial experts in France are independent of all parties and lawsuits and work only with and for an independent judge, there was no conflict of interest. Postmortem considerations are excluded from this review. What do we learn from perpetrator statements? In Starling s article[3], perpetrators admitted to abuse in 81 of 453 cases of inflicted traumatic brain injury (80 involved an acute and/or chronic subdural hematoma and one involved an isolated subarachnoid hemorrhage). In 69 cases, there was enough information provided to define the mechanism as impact alone in 29%, shaking alone in 46%, and a combination of impact and shaking in 25%. Retinal hemorrhage was seen in 83%. The mean age was fairly low (3.5 months, range: months) and the sex ratio was 35% female (28/81). Death occurred in 19% of patients. The most common initial symptoms reported by the perpetrators were hypotonia (36%), seizures (31%), vomiting (30%), loss of consciousness (28%) and breathing problems (26%). Information about the time between injury and symptoms was available in 57 cases. Most of the perpetrators (91%, or 52/57) reported symptoms immediately after the injury was inflicted. Interestingly, none of the five infants (9%) in whom the symptoms were described as delayed was observed closely in the period immediately following the injury. In both Biron s [4] and Willman s [5] S579 articles including 52 and 95 cases of inflicted trauma, respectively, the initial symptoms were described as occurring immediately after the injury if no epidural hematoma was present [5]. Our series also showed the classic demographic data [2]. The male-to-female ratio was 2:14 (45 boys, 21 girls). The median age was 4.4 months (3 weeks-41 months). All of the perpetrator statements described extremely violent shaking. Head impact was reported fairly infrequently (12%, or 8/66). Ophthalmological examination was performed on 65 children and found retinal hemorrhage in 86% of cases. At the time of the diagnosis, 44% of children (29/66) had bruising, including on the face (50%) and chest (11%). The skeletal surveys revealed fractures in 36% (24/66) of patients. In 53 cases, the perpetrator was asked during questioning to describe the initial symptoms presented by the baby. In 100% of cases, changes in behavior were described immediately after the shaking, or even during the shaking. The perpetrator described the infant as having a period of calm or silence ( the baby stops crying ) or a period of tiredness/sleeping (55%, or 29/53), hypotonia (41.5% or 22/53), loss of consciousness (38%, or 20/53), breathing problems (24%, or 13/ 53) or pallor (15%, or 8/53). Immediate vomiting was described in 11% (6/53) of cases. The more severe the symptoms, the faster medical help was sought. In the subsequent time period, i.e. from approximately 30 min to 15 h after the shaking ended, the perpetrators reported abnormal movements that we have interpreted as seizures (32%, or 17/53), secondary vomiting without diarrhea or fever (9%, or 5/53), or focal neurological deficits (6%, or 3/53 cases) leading to a trip to the emergency department. In those cases, the earliest symptoms were often missed, probably because the child fell asleep. Fig. 1 Typical shaken baby syndrome/abusive head trauma. a, b CT of an 8-month-old boy presenting with loss of consciousness, left hemiparesis, seizures and bilateral retinal hemorrhages. Subdural hematoma of heterogeneous density is shown in the right frontotemporal area (arrowheads). Mass effect is visible with midline shift, compression of the right ventricle and blurring of the ipsilateral sulci. There is subtle hyperdensity of the posterior part of the inter hemispheric fissure (arrows)
3 S580 Pediatr Radiol (2014) 44 (Suppl 4):S578 S588 Fig. 2 Changes in subdural hematoma densities over time. The father of this 6-week-old term boy admitted one episode of violent shaking with immediate symptoms. a-d CT at Day 0 when the neonate presented with pallor, seizures, bruising and right retinal hemorrhages. An isodense subdural hematoma is seen in the posterior fossa (a, arrows), subarachnoid hemorrhage in the right lateral sulcus (b) associated with a thin right frontotemporal subdural hematoma (b, c, white arrows). The interhemispheric fissure appears almost normal (b, c, black arrow). Small hyperdense clot is seen in the subdural frontal space on the left side (c, arrowhead). A large hyper dense clot is located at the convexity on the right side (d) e-i CT at Day 1. A hyperdense subdural hematoma is now seen in the posterior fossa (e, arrowhead, and f) with a thinner right frontotemporal subdural hematoma (g, short arrows). The interhemispheric fissure becomes hyperdense (g-i, long arrow). Small hyperdense frontal clot is seen on the left side (i, arrowhead). j, k CT at Day 3. Increasing of the hyperdensity of the interhemispheric fissure (arrow). Note also the re-expansion of the sulci. (l-n): MRI at Day 4, T1-weighted spin-echo, right parasagittal slice (l) and T2-weighted fast spin-echo axial slices (m, n) confirmed the hemorrhages and a left frontal hemorrhagic spot that likely corresponds to a bridging vein thrombosis (n, arrow)
4 S581 Dating based on imaging is inaccurate Estimating the age of subdural hematoma with neuroimaging is imprecise and it would be more accurate to use the term staging rather than dating. In theory, there are four stages: hyperacute, with an isodense appearance, less than 3 h old; acute, with a hyperdense appearance, less than about 10 days old; subacute, with an isodense appearance, 2 3 weeks old; and chronic (old), with a hypodense appearance, more than 3 weeks old [7]. On CT, acute bleeding shows high attenuation if the blood has clotted normally. In our experience of abusive head trauma, however, more than half of subdural hematomas in the frontotemporal region show a mixture of low, high and intermediate densities that is difficult to interpret (Fig. 1). Moreover, analysis of subdural hematoma density in abusive head trauma often reveals a combination of multiple subdural hematomas with different attenuation [4]. Interestingly, the terminology used to describe the attenuation of extra-axial hemorrhage on CT varies considerably between studies; old is used to qualify a hypodense subdural hematoma, and acute is often used without additional detail about the density, thereby perpetuating the confusion [8]. In fact, several factors can affect the appearance of subdural hematoma on imaging studies, and these can vary from day to day. Examples include the hemoglobin level, the concentration and hydration state of the red blood cells, the integrity of the cell membranes, the protein content of the blood clot, the sedimentation rate, clotting disorders, the amount of cerebrospinal fluid within the collection and the presence of an old hematoma (Fig. 2) [9]. Thus, an acute hyperdense subdural hematoma can be homogeneous or heterogeneous (mixed density pattern) for 8 10 days, as influenced by these factors. Some case studies have reported traumatic tears in the arachnoid membranes leading to a mixture of cerebrospinal fluid and blood in an acute subdural hematoma [10]. In particular, it is important to remember that a pattern of heterogeneous or multilayered densities within the subdural hematoma does not necessarily imply repeated injury, since there is ample documentation that subdural hematomas may rebleed spontaneously due to the presence of inflammatory membranes with newly formed capillaries (Fig. 3) [1, 2, 11]. In addition, subdural hematomas in the posterior fossa and interhemispheric fissure only become evident i.e. marked by hyper density a few hours or days after the first symptoms (Fig. 2) [7]. Patterns of time-related MRI signal changes within subdural collections can also be used to date the traumatic event, but they are more difficult to interpret than Fig. 3 CT 3 months after an acute shaking episode in a child (boy) who had been in protective custody since the diagnosis of shaken baby syndrome/abusive head trauma at age 4 months. Major brain atrophy and spontaneous hyperdense rebleeding in the left frontal subdural space is seen CT dating. For example, a hyperacute subdural hematoma (less than 24 h old) is hypo- or isointense on T1- weighted sequences and hyperintense on T2-weighted sequences. The signal intensity will decrease on T2-W sequences in the acute stage (less than 3 days) and then increase on T1-weighted sequences; the subacute stage is considered to last for up to 2 months. The hemosiderin deposits (low signal at T2-weighted gradient echo) can last months or even years. Several papers have, however, pointed out the lack of evidence in dating subdural collections [1, 2, 7 9, 11]. Of interest is that membranes within subdural hematoma begin to form after 2 weeks and may be exquisitely demonstrated with MRI [12]. Parenchymal brain or cervical cord abnormalities are interesting to consider when estimating the age of the causal injury. In particular, diffusion-weighted imaging (DWI) is invaluable in demonstrating acute cytotoxic cell edema, which lasts for a few days usually less than a week (Fig. 4). However, while a strong association between hypoxic-ischemic injury and abusive head trauma has been well-established, the mechanism of hypoxic-ischemic injury is not yet fully understood [13, 14]. It may be related to initial cardiorespiratory arrest and/or to seizures through excitotoxic processes. While the presence of cytotoxic edema indicates early hypoxic-ischemic injury, it does not preclude a traumatic injury from a few days earlier, since the cytotoxic brain edema may be secondary to seizures, which may themselves be delayed after the shaking.
5 S582 Pediatr Radiol (2014) 44 (Suppl 4):S578 S588 Fig. 4 A 6-month-old girl in a coma due to acute abusive head trauma. a, b CT at Day 0. Hypodense bilateral anterior subdural hematoma (absence of sulcal enlargement) is combined with hyperdense subdural hematomas in the interhemispheric fissure and at the convexity (arrows). Subtle parenchymal hypodensities are seen in the temporooccipital areas (a). c, d Three days later, diffusion-weighted MRI (c) and apparent diffusion coefficient (ADC) map (d) show multiple areas of cytotoxic edema (decreased ADC) in the occipital white matter and the gray-white matter junctions in the frontal lobes and basal ganglia. This age-different pattern is well correlated with a rapid increase in head circumference since age 2monthse Head circumference chart shows a rapid increase since age 2 months followed with a stagnation (arrow) since the acute event Some recent papers have highlighted the possibility of identifying bridging vein thrombosis secondary to rupture based on patterns of tubular or round-shaped clots at the vertex [14, 15] (Fig. 5). These clots are
6 S583 Fig. 5 A 3-month-old boy who suffered abusive head trauma. a-c CT at admission shows thin frontotemporal subdural hematomas of heterogeneous low density and large parenchymal hypodensities with loss of gray/white matter contrast due to hypoxic-ischemic injuries (a, b). There is a hyperdense spot at the vertex on the right side (c, arrow) andmild hyperdensity in the interhemispheric fissure (c, arrowhead). d-g MRI 2 days later with diffusion-weighted imaging (d), T1-weighted inversion recovery (e) and T2*-weighted imaging (f, g) confirm hypoxic-ischemic injury predominantly on the left side (d) and rounded/tubular spots of hemosiderin at the convexity corresponding to bridging vein thrombosis (e-g) better demonstrated by MRI (gradient echo or susceptibility imaging sequences) than by CT. Not only are they invaluable in diagnosing abusive head trauma by providing direct proof of acceleration/deceleration trauma, they also indicate recent injury if they present with an acute pattern (hyperdense appearance on CT less than about 10 days old) according to the usual changes of a hematoma overtime [7, 9]. However, due to the time interval between in vivo imaging and autopsy, there is no study that specifically correlates the histological features of bridging vein thrombosis with the imaging patterns. It is impossible to estimate the age of a skull fracture because healing takes a few months and there is no periosteal thickening [16]. And while the presence of a scalp hematoma indicates an acute impact, the volume of the swelling will depend on the conditions of the impact and the status of the child at the time of the impact, i.e. hypovolemic shock, anemia, etc. Nor are non-skull skeletal fractures, which are found in approximately one-third of the cases in our series [6], of any help in dating the causal event because healing appears within 8 10 days [17]. Thus, imaging cannot currently be used to accurately date the causal event. Is it possible to identify repeated episodes of violence? In 55% of the cases, the offenders admitted that shakings took place over a period of weeks or months, and were repeated from 2 to 30 times (mean: 10) because it stopped the infant s crying (62.5%) [6]. Extending our investigation from 29 to 66 cases confirms these data. Knowing the high prevalence of habitual shaking brings up two issues. First, neuroimaging-based dating is even more uncertain in non-accidental than in accidental trauma because the latter are a onetime occurrence. Second, how can we recognize, on the basis of neuroimaging, the age-different patterns that strongly indicate at least two distinct episodes of violence with any confidence? We have seen that because it is influenced by a number of factors, the attenuation within one area of subdural hematoma cannot be used as an indicator of age-different injuries. In particular, the frequently observed mixed density/intensity pattern is not necessarily associated with repeated episodes of violence. We therefore hypothesize that only subdural hematomas with two different densities in two distant locations on CT can be considered an indicator of age-different injuries. Practically, the sites of
7 S584 Pediatr Radiol (2014) 44 (Suppl 4):S578 S588 Fig. 6 Age-different pattern in abusiveheadtrauma.a, b CT in a 6-month-old boy. Hypodense bilateral frontal subdural hematomas are combined with mild hyperdense subdural hematoma of the tentorium (arrowhead). In a statement, the caretaker admitted repeated daily shakings over a period of weeks. Episodes of vomiting, feeding troubles and pallor were reported by the parents 8 days prior to admission for loss of consciousness subdural hematomas can be simply divided in five locations, which are (1) right and (2) left frontoparietotemporal subdural spaces, (3) interhemispheric fissure and (4) the tentorium. The fifth location specifically considers the vertex (five last reformatted upper slices of 3 mm in thickness) in which round or tubular hyperdense clots are frequently observed in abusive head trauma. Thereby, for example, an age-different pattern might be a hypodense frontoparietal or frontoparietotemporal (older than days) in combination with a frankly hyperdense (younger than approximately 10 days) hematoma in the posterior fossa. Also, an age-different pattern can be marked Fig. 7 Age-different pattern in abusive head trauma. The father admitted at least eight or nine episodes of violent shaking to calm his 2-monthold daughter, who then fell asleep. No retinal hemorrhages were seen. a-c CT at admission for loss of consciousness after 5 days of abnormal vomiting. The combination of intermediate-density frontal subdural hematomas (white arrows) with frankly hyperdense subdural hematomas in other locations, e.g., tentorium and interhemispheric fissure (black arrows and arrowheads), and hyperdense clots at the right convexity is suggestive of an age-different pattern. d-g MRI 4 days after admission with T1- weighted inversion recovery (d, e) and T2*-weighted imaging (f, g) confirms the CT features and helps demonstrate bridging vein thrombosis (f, g, arrows)
8 with a hypodense frontoparietal subdural hematoma associated to hyperdense clots at the vertex (Figs. 6 and 7). While migration of subdural hematomas due to gravity may be seen, the detection of new hyperdensities far from the lateral hypodense (old) subdural hematoma is very likely evidence of true new bleeding [6, 8, 18]. Conversely, in cases in which all the sites of bleeding are mostly consisting of hyperdensities, whether homogeneous or heterogeneous, it s not possible to conclude to an agedifferent pattern. Indeed, in our personal series including 66 cases for which detailed confessions from police inquiries or judicial investigations were available, we have evaluated this age-different pattern of two frankly different densities in two distant locations (at least one hypodense subdural hematoma and one hyperdense subdural hematoma/clot among the five defined locations) and we have found that it was strongly associated with confessions of repeated episodes of violence (81%, or 26/32), yet present in only 44% (15/34) cases of a single episode of violence (P=0.006) (results presented at the international conference on shaken baby syndrome/abusive head trauma, Paris, May 4 6, 2014). Of course, it is not possible to determine how many episodes of violence have occurred. However, we have also observed a lack of age-different patterns despite admissions of repeated shaking. We have interpreted this as the consequence of brain edema, where the swelling masks a previous old subdural hematoma (Figs. 8 and 9) [6]. Also, all hypodense subdural hematomas without age-different pattern may also be the result of abusive head trauma with habitual repetitive shaking [6]. On the other hand, we assume that the false-positive age-different pattern may, however, be due to minimized confessions in some cases [6]. Interestingly, it was much easier in our experience to assess the age-different pattern of subdural hematomas with CT than with MRI, due to the highest sensitivity of MRI to hemoglobin degradation products and thus the complexity for reasoning in dating the hemorrhages with MRI. Nevertheless, MRI can help to demonstrate repeated violence as the analysis of parenchymal injuries can also provide strong indicators for assessing the pattern of age-different injuries, e.g., the association of acute hypoxic-ischemic injuries or venous infarcts, exquisitely depicted on DWI sequences, with a fluidlike appearance of the subdural hematoma, close to the cerebrospinal fluid signal intensity (Figs. 4 and 6). A fluid-like appearance of subdural hematoma may be associated with benign enlargement of subarachnoid spaces, if the sulci are also enlarged. An analysis of the head circumference chart can be very helpful: a rapid, S585 unexplained increase in head circumference in the few weeks or months prior to admission may be an indicator of previous subdural hematomas, in combination with mild symptoms (Fig. 4). We should also emphasize that there are no consistent data in the literature to support the hypothesis that benign enlargement of subarachnoid spaces predisposes infants to subdural hematomas [1, 2, 19]. Conversely and importantly, sulcal expansion may be a consequence of abusive head trauma, in the context of brain atrophy and/or impaired cerebrospinal fluid resorption (Fig. 10). In addition to neuroimaging, other features must be carefully analyzed when assessing repetitive violence. Close attention should be paid to the child s medical history and previous events reported by the parents and caregivers, to look for earlier, mild signs that may prove invaluable in identifying previous violence. Clinical indicators of previous shaking may include unexplained Fig. 8 Lack of an age-different pattern despite a number of violent shakings admitted by the mother of this 5-month-old girl. a, b CT shows only a thin hyperdense subdural hematoma over the left frontal lobe and in the interhemispheric fissure (arrows). The brain edema may mask a previous hematoma
9 S586 Pediatr Radiol (2014) 44 (Suppl 4):S578 S588 Fig. 9 No age-different pattern despite the father admitting to several previous episodes of violent shaking, slaps and impacts to this 3-month old boy presenting with seizures and hemiplegia. A rapid increase in head circumference was noticed over the previous 2 weeks. a, b Initial CT shows a large, low-density subdural hematoma with areas of mild hyperdensity (arrows) located over the left hemisphere and in the interhemispheric fissure. Major compression and displacement of normal structures are visible. c T2-weighted MRI a few hours after evacuation reveals a right subdural enlargement (arrow) and parenchymal injuries of the left hemisphere marked with a loss of contrast between gray and white matter. Post-surgical air is seen in the left frontal subdural space (arrowhead). d Fluid-attenuated inversion recovery MRI 3 weeks later show enlarged sulci and ventricles due to atrophy. There are areas of necrosis in the frontal and occipital lobes on the left side and persistence of bilateral subdural hematomas (arrows), predominantly on the left side vomiting without diarrhea or fever and/or unexplained bruises or oral injury in nonambulatory children, in the medical records from birth to the time of diagnosis [20]. Painstaking examination of a high-detail skeletal survey to look for healed fractures is crucial, as these are a strong indicator of previous violence [21 23]. In doubtful cases, particularly for rib fractures, it may be helpful to do a skeletal survey after 10 days, as this can provide evidence of a healing injury not apparent on initial radiographs [21 23]. In clinical practice, there is no scientific data to aid in estimating the age of a bruise from its color, since bruise characteristics are influenced by the location, the skin color, the force of the injury, and the depth and extent of subcutaneous extravasation [24]. Retinal hemorrhage is a major indicator of possible abusive head trauma, though it is absent in approximately 15% of cases. Ophthalmological examination should include full indirect examination through a dilated pupil by an ophthalmologist within 72 h of the acute presentation, and ideally within the first 24 h. However, ophthalmological examination is usually not reliable enough to determine whether the injuries are age-different, or to date them [1, 2, 25]. Conclusion Although perpetrator admissions are not scientific evidence, they provide information crucial to our understanding. The high prevalence of repeated shaking (50%) is probably still an
10 S587 Fig. 10 Evolution of subdural hematomas. The caregiver admitted to three episodes of shaking a 6-month-old boy over a period of a few weeks. a, b First CT at admission for seizures and hypotonia shows bilateral frontotemporal subdural hematomas of low intermediate densitywithmildinterhemispheric hyperdensity at the vertex (arrow). c Diffusion-weighted MRI 24 h later shows bilateral hyperintensities in the temporo-occipital areas related to recent hypoxic-anoxic injuries. d CT 3 months later demonstrates changes in the densities of the subdural hematomas. e CT 6 months later shows enlargement of both ventricles and sulci due to atrophy. f CT 14 months later shows mild enlargement of ventricles and sulci related to atrophy underestimate. Children do not behave normally immediately after shakings, and the time of onset of even mild symptoms appears to be the best clue for dating the incident. Brain imaging offers wide ranges for dating the causal event. The density/intensity pattern in a single subdural hematoma location provides no reliable clues for assessing repeated violence. However, brain imaging is a strong marker to argue in favor of age-different injuries, i.e. repeated violence, using strict criteria. MRI must be analyzed in conjunction with CT to evaluate the age of a subdural hemorrhage. Most importantly, all of the child s previous clinical and radiologic data must be carefully studied and correlated to provide accurate information on the date and repetition of the trauma. Acknowledgments We would like to thank Anne Laurent-Vannier, MD, for sharing her experience and Pascale Zerbini for her help with the manuscript. Conflicts of interest None
11 S588 References 1. Laurent-Vannier A, Nathanson M, Quiriau F et al (2011) A public hearing «shaken baby syndrome: guidelines on establishing a robust diagnosis and the procedures to be adopted by healthcare and social services staff». Guidelines issued by the hearing commission. Ann Phys Rehabil Med 54: Laurent-Vannier A, Nathanson M, Quiriau F et al (2011) A public hearing «shaken baby syndrome: guidelines on establishing a robust diagnosis and the procedures to be adopted by healthcare and social services staff». Scoping report. Ann Phys Rehabil Med 54: Starling SP, Patel S, Burke BL et al (2004) Analysis of perpetrator admissions to inflicted traumatic brain injury in children. Arch Pediatr Adolesc Med 158: Biron D, Shelton D (2005) Perpetrator accounts in infant abusive head trauma brought about by a shaking event. Child Abuse Negl 29: Willman KY, Bank DE, Senac M et al (1997) Restricting the time of injury in fatal inflicted head injuries. Child Abuse Negl 21: Adamsbaum C, Grabar S, Méjean N et al (2010) Abusive head trauma (AHT): judicial admissions highlight violent and repetitive shaking. Pediatrics 126: Vezina G (2009) Assessment of the nature and age of subdural collections in non accidental head injury with CT and MRI. Pediatr Radiol 39: Kemp AM, Jaspan T, Griffiths J et al (2011) Neuroimaging: what neuro radiological features distinguish abusive from non-abusive head trauma? A systematic review. Arch Dis Child 96: Vinchon M, Noulé N, Tchofo PJ et al (2004) Imaging of head injuries in infants: temporal correlates and forensic implications for the diagnosis of child abuse. J Neurosurg 101: Joy HM, Anscombe AM, Gawne-Cain ML (2007) Blood-stained, acute subdural hygroma mimicking a subacute subdural haematoma in non-accidental head injury. Clin Radiol 62: Bradley WG Jr (1993) MR appearance of hemorrhage in the brain. Radiology 189:15 26 Pediatr Radiol (2014) 44 (Suppl 4):S578 S Hedlund GL (2012) Subdural hemorrhage in abusive head trauma: imaging challenges and controversies. J Am Osteopath Coll Radiol 1: Geddes JF, Hackshaw AK, Vowles GH et al (2001) Neuropathology of inflicted head injury in children. II. Microscopic brain injury in infants. Brain 124: Zimmerman RA, Bilaniuk LT, Farina L (2007) Non-accidental brain trauma in infants: diffusion imaging, contributions to understanding the injury process. J Neuroradiol 34: Adamsbaum C, Rambaud C (2012) Abusive head trauma (AHT): don t overlook bridging vein thrombosis. Pediatr Radiol 42: Slovis TL (2008) Traumatic lesions of the skull. In: Slovis TL (ed) Caffey s pediatric diagnostic imaging, 11th edn. Mosby, Philadelphia, pp Prosser I, Maguire S, Harrison SK et al (2005) How old is this fracture? Radiologic dating of fractures in children: a systematic review. AJR Am J Roentgenol 184: Barnes PD, Krasnokutsky M (2007) Imaging of the central nervous system in suspected or alleged non accidental injury, including the mimics. Top Magn Reson Imaging 18: Raul JS, Roth S, Ludes B et al (2008) Influence of the benign enlargement of the subarachnoid space on the bridging veins strain during shaking event: a finite element study. Int J Legal Med 122: Sheets LK, Leach ME, Koszewski IJ et al (2013) Sentinel injuries in infants evaluated for child physical abuse. Pediatrics 131: Adamsbaum C, Méjean N, Merzoug V et al (2010) How to explore and report children with suspected non-accidental trauma. Pediatr Radiol 40: American Academy of Pediatrics (2000) Diagnostic imaging of child abuse. Pediatrics 105: Kleinman PK, Nimkin K, Spevak MR et al (1996) Follow-up skeletal surveys in suspected child abuse. AJR Am J Roentgenol 167: Maguire S, Mann MK, Sibert J et al (2005) Can you age bruises accurately in children? A systematic review. Arch Dis Child 90: Pierre-Kahn V, Roche O, Dureau P et al (2003) Ophthalmologic findings in suspected child abuse victims with subdural hematomas. Ophthalmology 110:
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE
 THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review
 Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review M B Moss, MD; L Lanier, MD; R Slater; C L Sistrom, MD; R G Quisling, MD; I M Schmalfuss, MD; and D Rajderkar, MD Contact:
Neuroradiological Findings in Non- Accidental Trauma Educational Pictorial Review M B Moss, MD; L Lanier, MD; R Slater; C L Sistrom, MD; R G Quisling, MD; I M Schmalfuss, MD; and D Rajderkar, MD Contact:
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
ARTICLE. Intracranial Hemorrhage in Children Younger Than 3 Years
 Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
The clinical scenario in this patient has been well reviewed by expert witnesses.
 September 29, 2014 Michael J. Cronkright, Esq. Kronzek & Cronkight, PLLC 420 S. Waverly Road, Suite 100 Lansing, MI 48917 Re: Preliminary Report on Naomi Burns Dear Mr. Cronkright, I have reviewed all
September 29, 2014 Michael J. Cronkright, Esq. Kronzek & Cronkight, PLLC 420 S. Waverly Road, Suite 100 Lansing, MI 48917 Re: Preliminary Report on Naomi Burns Dear Mr. Cronkright, I have reviewed all
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Index. aneurysm, 92 carotid occlusion, 94 ICA stenosis, 95 intracranial, 92 MCA, 94
 A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
A ADC. See Apparent diffusion coefficient (ADC) Aneurysm cerebral artery aneurysm, 93 CT scan, 93 gadolinium, 93 Angiography, 13 Anoxic brain injury, 25 Apparent diffusion coefficient (ADC), 7 Arachnoid
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Brain and Cervico-Medullary Injury : Patterns and Mechanisms
 Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
MR Characteristics of Subdural Hematomas and Hygromas at 1.5 T
 687 MR Characteristics of Subdural Hematomas and Hygromas at 1.5 T Edward S. Fobben 1 Robert I. Grossman Scott W. tlas David B. Hackney Herbert I. Goldberg Robert. Zimmerman Larissa T. Bilaniuk MR images
687 MR Characteristics of Subdural Hematomas and Hygromas at 1.5 T Edward S. Fobben 1 Robert I. Grossman Scott W. tlas David B. Hackney Herbert I. Goldberg Robert. Zimmerman Larissa T. Bilaniuk MR images
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
S ubdural haemorrhage (SDH) in infants and young
 947 ORIGINAL ARTICLE Neuroradiological aspects of subdural haemorrhages S Datta, N Stoodley, S Jayawant, S Renowden, A Kemp... See end of article for authors affiliations... Correspondence to: Dr S Datta,
947 ORIGINAL ARTICLE Neuroradiological aspects of subdural haemorrhages S Datta, N Stoodley, S Jayawant, S Renowden, A Kemp... See end of article for authors affiliations... Correspondence to: Dr S Datta,
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Recurrent Subdural Hematomas in Benign Macrocrania of Infancy
 Case Report imedpub Journals http://www.imedpub.com Medical & Clinical DOI: 10.21767/2471-299X.100032 Recurrent Subdural Hematomas in Benign Macrocrania of Infancy Ademar Lucas Junior São Camilo Diagnostic
Case Report imedpub Journals http://www.imedpub.com Medical & Clinical DOI: 10.21767/2471-299X.100032 Recurrent Subdural Hematomas in Benign Macrocrania of Infancy Ademar Lucas Junior São Camilo Diagnostic
Subdural haematoma and effusion in children aged < 2 years
 Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases
 How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
How to interpret an unenhanced CT brain scan. Part 2: Clinical cases Thomas Osborne a, Christine Tang a, Kivraj Sabarwal b and Vineet Prakash c a Radiology Registrar; b Radiology Foundation Year 1 Doctor;
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
41 year old female with headache. Elena G. Violari MD and Leo Wolansky MD
 41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
 Revisited imaging findings and pathophysiology of abusive head trauma with emphasis on diffusionweighted imaging (eede-219) I. Elhelf *, R. Oral, T. Sato, A. Capizzano, Y. Sato, M. Amarneh, T. Sasaki,
Revisited imaging findings and pathophysiology of abusive head trauma with emphasis on diffusionweighted imaging (eede-219) I. Elhelf *, R. Oral, T. Sato, A. Capizzano, Y. Sato, M. Amarneh, T. Sasaki,
Common Abusive Skeletal Injuries
 Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
SWISS SOCIETY OF NEONATOLOGY. Severe apnea and bradycardia in a term infant
 SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
SWISS SOCIETY OF NEONATOLOGY Severe apnea and bradycardia in a term infant October 2014 2 Walker JH, Arlettaz Mieth R, Däster C, Division of Neonatology, University Hospital Zurich, Switzerland Swiss Society
Imaging of Acute Cerebral Trauma
 July, 2005 Imaging of Acute Cerebral Trauma Louis Rivera, Harvard Medical School, Year III 46 y/o Female s/p Trauma - Unrestrained? MVC requiring Med Flight - Facial bruising/swelling - DEEP COMA - SEIZURES
July, 2005 Imaging of Acute Cerebral Trauma Louis Rivera, Harvard Medical School, Year III 46 y/o Female s/p Trauma - Unrestrained? MVC requiring Med Flight - Facial bruising/swelling - DEEP COMA - SEIZURES
Traumatic Brain Injury TBI Presented by Bill Masten
 1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
1 2 Cerebrum two hemispheres and four lobes. Cerebellum (little brain) coordinates the back and forth ballet of motion. It judges the timing of every movement precisely. Brainstem coordinates the bodies
The significance of traumatic haematoma in the
 Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Journal of Neurology, Neurosurgery, and Psychiatry 1986;49:29-34 The significance of traumatic haematoma in the region of the basal ganglia P MACPHERSON, E TEASDALE, S DHAKER, G ALLERDYCE, S GALBRAITH
Tips and tricks for detecting diffuse axonal injury on CT and MR neuroimaging
 Tips and tricks for detecting diffuse axonal injury on CT and MR neuroimaging Poster No.: C-3080 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Marinkic, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords:
Tips and tricks for detecting diffuse axonal injury on CT and MR neuroimaging Poster No.: C-3080 Congress: ECR 2018 Type: Educational Exhibit Authors: M. Marinkic, D. Zadravec ; Zagreb/HR, Zageb/HR Keywords:
Paravertebral calcification as a potential indicator for nonaccidental trauma
 Paravertebral calcification as a potential indicator for nonaccidental trauma Katsuaki Kojima 1*, Jennifer Nimtz 1, Steven W Martin 1, Stephen R Guertin 1, Ellen C Cavenagh 2 1. Department of Pediatrics
Paravertebral calcification as a potential indicator for nonaccidental trauma Katsuaki Kojima 1*, Jennifer Nimtz 1, Steven W Martin 1, Stephen R Guertin 1, Ellen C Cavenagh 2 1. Department of Pediatrics
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE
 WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
WHITE PAPER: A GUIDE TO UNDERSTANDING SUBARACHNOID HEMORRHAGE Subarachnoid Hemorrhage is a serious, life-threatening type of hemorrhagic stroke caused by bleeding into the space surrounding the brain,
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
SWI including phase and magnitude images
 On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
On-line Table: MRI imaging recommendation and summary of key features Sequence Pathologies Visible Key Features T1 volumetric high-resolution whole-brain reformatted in axial, coronal, and sagittal planes
ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA. Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
 Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score
 Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Outcome Evaluation of Chronic Subdural Hematoma Using Glasgow Outcome Score Mehdi Abouzari, Marjan Asadollahi, Hamideh Aleali Amir-Alam Hospital, Medical Sciences/University of Tehran, Tehran, Iran Introduction
Validity of Caregivers Reports on Head Trauma Due to Falls in Young Children Aged Less than 2 Years
 Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results of Cerebral Perfusion MR Imaging
 pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
pissn 2384-1095 eissn 2384-1109 imri 2018;22:56-60 https://doi.org/10.13104/imri.2018.22.1.56 Complete Recovery of Perfusion Abnormalities in a Cardiac Arrest Patient Treated with Hypothermia: Results
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
NEURORADIOLOGY DIL part 3
 NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
Evaluation of a Pediatric Patient
 September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
Outline. Neuroradiology. Diffusion Imaging in. Clinical Applications of. Basics of Diffusion Imaging. Basics of Diffusion Imaging
 Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
Clinical Applications of Diffusion Imaging in Neuroradiology No disclosures Stephen F. Kralik Assistant Professor of Radiology Indiana University School of Medicine Department of Radiology and Imaging
Acute stroke. Ischaemic stroke. Characteristics. Temporal classification. Clinical features. Interpretation of Emergency Head CT
 Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
Ischaemic stroke Characteristics Stroke is the third most common cause of death in the UK, and the leading cause of disability. 80% of strokes are ischaemic Large vessel occlusive atheromatous disease
A characteristic feature of acute haematomas in the brain on echo-planar diffusion-weighted imaging
 Neuroradiology (2002) 44: 907 911 DOI 10.1007/s00234-002-0860-5 DIAGNOSTIC NEURORADIOLOGY N. Morita M. Harada K. Yoneda H. Nishitani M. Uno A characteristic feature of acute haematomas in the brain on
Neuroradiology (2002) 44: 907 911 DOI 10.1007/s00234-002-0860-5 DIAGNOSTIC NEURORADIOLOGY N. Morita M. Harada K. Yoneda H. Nishitani M. Uno A characteristic feature of acute haematomas in the brain on
POST-INJURY INTERVALS 1
 POST-INJURY INTERVALS 1 Introduction 1 Contusion dating 2 Skin 2 Brain 5 Hypoxic/ischemic injury and increased intracranial pressure 18 Brain incidentals (non-injurious) 21 Sexual violence 27 INTRODUCTION
POST-INJURY INTERVALS 1 Introduction 1 Contusion dating 2 Skin 2 Brain 5 Hypoxic/ischemic injury and increased intracranial pressure 18 Brain incidentals (non-injurious) 21 Sexual violence 27 INTRODUCTION
Diffusion-weighted magnetic resonance imaging (MRI) allows for tissue
 MAGNETIC RESONANCE IMAGING / IMAGERIE PAR RÉSONANCE MAGNÉTIQUE Nonischemic causes of hyperintense signals on diffusion-weighted magnetic resonance images: a pictorial essay Jeffrey M. Hinman, MD; James
MAGNETIC RESONANCE IMAGING / IMAGERIE PAR RÉSONANCE MAGNÉTIQUE Nonischemic causes of hyperintense signals on diffusion-weighted magnetic resonance images: a pictorial essay Jeffrey M. Hinman, MD; James
Subdural Hygroma versus Atrophy on MR Brain Scans: "The Cortical Vein Sign"
 Subdural Hygroma versus Atrophy on MR Brain Scans: "The Cortical Vein Sign" Kerry W. McCiuney, 1 Joel W. Yeakley, 1 Marc J. Fenstermacher, 1 Samuel H. Baird, 1 and Carmen M. Bonmati 1 PURPOSE: To determine
Subdural Hygroma versus Atrophy on MR Brain Scans: "The Cortical Vein Sign" Kerry W. McCiuney, 1 Joel W. Yeakley, 1 Marc J. Fenstermacher, 1 Samuel H. Baird, 1 and Carmen M. Bonmati 1 PURPOSE: To determine
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Masses of the Corpus Callosum
 Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
Masses of the Corpus Callosum Kesav Raghavan, HMS Year III Dr. Agenda Corpus Callosum Development and Anatomy Our Patient: Clinical Presentation Differential Diagnosis of Masses in the Corpus Callosum
A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage
 July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
THE ESSENTIAL BRAIN INJURY GUIDE
 THE ESSENTIAL BRAIN INJURY GUIDE Neuroanatomy & Neuroplasticity Section 2 Contributors Erin D. Bigler, PhD Michael R. Hoane, PhD Stephanie Kolakowsky-Hayner, PhD, CBIST, FACRM Dorothy A. Kozlowski, PhD
THE ESSENTIAL BRAIN INJURY GUIDE Neuroanatomy & Neuroplasticity Section 2 Contributors Erin D. Bigler, PhD Michael R. Hoane, PhD Stephanie Kolakowsky-Hayner, PhD, CBIST, FACRM Dorothy A. Kozlowski, PhD
CNS pathology Third year medical students. Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure
 CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
CNS pathology Third year medical students Dr Heyam Awad 2018 Lecture 5: disturbed fluid balance and increased intracranial pressure ILOs Understand causes and symptoms of increased intracranial pressure.
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines
 Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Traumatic brain injuries are caused by external mechanical forces such as: - Falls - Transport-related accidents - Assault
 PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
PP2231 Brain injury Cerebrum consists of frontal, parietal, occipital and temporal lobes Diencephalon consists of thalamus, hypothalamus Cerbellum Brain stem consists of midbrain, pons, medulla Central
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
MR imaging as predictor of delayed posttraumatic cerebral hemorrhage
 J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy
 AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
AJNR Am J Neuroradiol 25:1269 1273, August 2004 Diffusion-Weighted and Conventional MR Imaging Findings of Neuroaxonal Dystrophy R. Nuri Sener BACKGROUND AND PURPOSE: Neuroaxonal dystrophy is a rare progressive
Pre-hospital Response to Trauma and Brain Injury. Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center
 Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
Pre-hospital Response to Trauma and Brain Injury Hans Notenboom, M.D. Asst. Medical Director Sacred Heart Medical Center Traumatic Brain Injury is Common 235,000 Americans hospitalized for non-fatal TBI
The Role of Neuroimaging in Acute Stroke. Bradley Molyneaux, HMS IV
 The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
The Role of Neuroimaging in Acute Stroke Bradley Molyneaux, HMS IV Patient CR 62 yo F w/ 2 wk h/o altered mental status Presents to ED w/ confusion following a fall 1 day prior New onset left facial droop
Marc Norman, Ph.D. - Do Not Use without Permission 1. Cerebrovascular Accidents. Marc Norman, Ph.D. Department of Psychiatry
 Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Cerebrovascular Accidents Marc Norman, Ph.D. Department of Psychiatry Neuropsychiatry and Behavioral Medicine Neuropsychology Clinical Training Seminar 1 5 http://www.nlm.nih.gov/medlineplus/ency/images/ency/fullsize/18009.jpg
Where is the contre-coup? Atypical localization of occipital brain contusion
 Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Where is the contre-coup? Atypical localization of occipital brain contusion A.I. Cucu, Claudia Florida Costea, R.A. Sascau, B. Dobrovat,
Romanian Neurosurgery Volume XXXII Number 1 2018 January-March Article Where is the contre-coup? Atypical localization of occipital brain contusion A.I. Cucu, Claudia Florida Costea, R.A. Sascau, B. Dobrovat,
SWISS SOCIETY OF NEONATOLOGY. Neonatal cerebral infarction
 SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
SWISS SOCIETY OF NEONATOLOGY Neonatal cerebral infarction May 2002 2 Mann C, Neonatal and Pediatric Intensive Care Unit, Landeskrankenhaus und Akademisches Lehrkrankenhaus Feldkirch, Austria Swiss Society
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
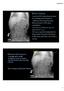 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
NEURORADIOLOGY DIL part 4
 NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 4 Strokes and infarcts K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR
 High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR Yutaka Araki, Ryuichirou Ashikaga, Satoru Takahashi, Jun Ueda, and Osamu Ishida PURPOSE: To determine the MR imaging
High Signal Intensity of the Infundibular Stalk on Fluid-Attenuated Inversion Recovery MR Yutaka Araki, Ryuichirou Ashikaga, Satoru Takahashi, Jun Ueda, and Osamu Ishida PURPOSE: To determine the MR imaging
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
CASE OF THE WEEK PROFESSOR YASSER METWALLY
 CLINICAL PICTURE CLINICAL PICTURE 26 years old male patient presented clinically with a grand male fit, confusion, fever, headache, and nausea. Examination showed bilateral papilledema and left sided extensor
CLINICAL PICTURE CLINICAL PICTURE 26 years old male patient presented clinically with a grand male fit, confusion, fever, headache, and nausea. Examination showed bilateral papilledema and left sided extensor
Predicting the need for operation in the patient with an occult traumatic intracranial hematoma
 J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
J Neurosurg 55:75-81, 1981 Predicting the need for operation in the patient with an occult traumatic intracranial hematoma SAM GALBRAITH, M.D., F.R.C.S., AND GRAHAM TEASDALE, M.R.C.P., F.R.C.S. Department
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation **
 PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
Dating Neurological Injury
 Dating Neurological Injury wwwwwwwww Jeff L. Creasy Dating Neurological Injury A Forensic Guide for Radiologists, Other Expert Medical Witnesses, and Attorneys Jeff L. Creasy Associate Professor of Neuroradiology
Dating Neurological Injury wwwwwwwww Jeff L. Creasy Dating Neurological Injury A Forensic Guide for Radiologists, Other Expert Medical Witnesses, and Attorneys Jeff L. Creasy Associate Professor of Neuroradiology
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
with susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine
 Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
Emerg Radiol (2012) 19:565 569 DOI 10.1007/s10140-012-1051-2 CASE REPORT Susceptibility-weighted imaging and computed tomography perfusion abnormalities in diagnosis of classic migraine Christopher Miller
The Viewing Study Guide for Physical Abuse Slides
 The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report
 214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
The dura is sensitive to stretching, which produces the sensation of headache.
 Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Dural Nerve Supply Branches of the trigeminal, vagus, and first three cervical nerves and branches from the sympathetic system pass to the dura. Numerous sensory endings are in the dura. The dura is sensitive
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
NEURO IMAGING OF ACUTE STROKE
 1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
1 1 NEURO IMAGING OF ACUTE STROKE ALICIA RICHARDSON, MSN, RN, ACCNS-AG, ANVP-BC WENDY SMITH, MA, RN, MBA, SCRN, FAHA LYNN HUNDLEY, APRN, CNRN, CCNS, ANVP-BC 2 2 1 DISCLOSURES Alicia Richardson: Stryker
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury
 Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Chin J Radiol 2005; 30: 173-177 173 Concomitant Traumatic Spinal Subdural Hematoma and Hemorrhage from Intracranial Arachnoid Cyst Following Minor Injury HUI-YI CHEN 1 YING-SHYUAN LI 1 CHUNG-HO CHEN 1
Cerebral Venous Thrombosis: A Potential Mimic of Primary Traumatic Brain Injury in Infants
 Pediatric Imaging Clinical Perspective Krasnokutsky Cerebral Venous Thrombosis in Infants Pediatric Imaging Clinical Perspective Michael V. Krasnokutsky 1 Krasnokutsky MV Keywords: abusive head injury,
Pediatric Imaging Clinical Perspective Krasnokutsky Cerebral Venous Thrombosis in Infants Pediatric Imaging Clinical Perspective Michael V. Krasnokutsky 1 Krasnokutsky MV Keywords: abusive head injury,
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Carrera J-P, Forrester N, Wang E, et al. Eastern equine encephalitis
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Carrera J-P, Forrester N, Wang E, et al. Eastern equine encephalitis
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
Role of MRI in acute disseminated encephalomyelitis
 Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Original Research Article Role of MRI in acute disseminated encephalomyelitis Shashvat Modiya 1*, Jayesh Shah 2, C. Raychaudhuri 3 1 1 st year resident, 2 Associate Professor, 3 HOD and Professor Department
Head Injury: Classification Most Severe to Least Severe
 Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
Head Injury: Classification Most Severe to Least Severe Douglas I. Katz, MD Professor, Dept. Neurology, Boston University School of Medicine, Boston MA Medical Director Brain Injury Program, HealthSouth
Imaging ischemic strokes: Correlating radiological findings with the pathophysiological evolution of an infarct
 Imaging ischemic strokes: Correlating radiological findings with the pathophysiological evolution of an infarct Jay Chyung,, PhD, HMS III Patient A: history 91 y.o. woman Acute onset R sided weakness and
Imaging ischemic strokes: Correlating radiological findings with the pathophysiological evolution of an infarct Jay Chyung,, PhD, HMS III Patient A: history 91 y.o. woman Acute onset R sided weakness and
It has been demonstrated that postmortem MDCT, or virtual
 Published April 5, 2012 as 10.3174/ajnr.A2966 ORIGINAL RESEARCH A.B. Smith G.E. Lattin Jr P. Berran H.T. Harcke Common and Expected Postmortem CT Observations Involving the Brain: Mimics of Antemortem
Published April 5, 2012 as 10.3174/ajnr.A2966 ORIGINAL RESEARCH A.B. Smith G.E. Lattin Jr P. Berran H.T. Harcke Common and Expected Postmortem CT Observations Involving the Brain: Mimics of Antemortem
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN
 Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
