During the past decade, nephrogenic systemic fibrosis
|
|
|
- Tyler Crawford
- 5 years ago
- Views:
Transcription
1 Low Risk for Nephrogenic Systemic Fibrosis in Nondialysis Patients Who Have Chronic Kidney Disease and Are Investigated with Gadolinium-Enhanced Magnetic Resonance Imaging Constantina Chrysochou,* Albert Power, Aladdin E. Shurrab,* Sayed Husain, Steven Moser, James Lay, Alan D. Salama, and Philip A. Kalra* *Renal Department, Salford Royal Hospital, Salford, Greater Manchester, United Kingdom; Renal Section, Division of Medicine, and Department of Imaging, Imperial College London, Hammersmith Hospital, London, United Kingdom; and Radiology Department, Bolton Royal Hospital, Bolton, Greater Manchester, United Kingdom Background and objectives: During the past decade, nephrogenic systemic fibrosis (NSF) has been reported in patients who have severe renal impairment and have been exposed to a gadolinium (Gd)-based contrast agent during magnetic resonance imaging (MRI). As a result of positive reporting bias, many suitable patients with chronic kidney disease (CKD) are being denied a highly important form of investigation that can be safely undertaken. We analyzed the safety of Gd-MRI in patients with CKD and varying levels of estimated GFR (egfr). Design, setting, participants, & measurements: We performed a retrospective analysis of 2053 unselected patients who had CKD and had received Gd-MRI between 1999 and 2009, so as to determine the risk for NSF related to level of CKD, nature of Gd preparation, and Gd dosage. Results: Overall, 2053 patients (63.5% men; mean age years) had 2278 Gd-MRI scans; their mean egfr was ml/min. A total of 918 (44.7%) patients had stage 3, 491 (23.9%) had stage 4, and 117 (5.7%) had predialysis stage 5 CKD. No cases of NSF were identified during an average follow-up period of months. Conclusions: In this study, no patients developed NSF during extended follow-up, even after multiple Gd doses in some. Gd-MRI can be safely undertaken in the majority of patients with CKD, but caution is merited for dialysis patients and those with acute kidney injury, with relative caution for predialysis patients with stage 5 CKD. Clin J Am Soc Nephrol 5: , doi: /CJN During the past decade, nephrogenic systemic fibrosis (NSF) has been reported in patients who have severe renal impairment and have been exposed to a gadolinium (Gd)-based contrast agent during magnetic resonance imaging (MRI). Although NSF is a rare condition, it has caused much controversy in the literature and sparked a dramatic change of MR investigational policy and protocols. We believe that, as a consequence, many suitable patients are being denied a highly important form of investigation that can be safely undertaken. For example, many radiology departments are precluding patients with estimated GFR (egfr) of 30 ml/min and, remarkably, some patients with egfr of 60 ml/min from undergoing Gd-enhanced MRI (Gd-MRI), despite critical review of the literature suggesting that in uncomplicated chronic kidney disease (CKD), NSF almost never occurs when Received September 16, Accepted November 30, Published online ahead of print. Publication date available at Correspondence: Dr. Constantina Chrysochou, Renal Department, Salford Royal Hospital, Stott Lane, Salford, Greater Manchester, M6 8HD, UK. Phone: ; Fax: ; tinachrys@doctors.org.uk or tinachrysochou@yahoo.co.uk egfr is 15 ml/min (1). We wished to add to the literature by emphasizing the safety of Gd-MRI for patients who had CKD and varying levels of egfr and had undergone the investigations at two large UK nephrology centers. Materials and Methods The two centers that participated in the audit were the renal departments of Salford Royal Hospital, Greater Manchester and the Hammersmith Hospital, London. Data were obtained from each center s radiology department records of all patients who had undergone either investigation for atheromatous renovascular disease with MR angiography (MRA) or MRA of the pelvic vessels (usually pretransplantation assessment) between 2000 and Data derived from a portion of the patients from Salford Royal Hospital, collected between 1999 and 2007, were reported in a previous article (1). This study includes an additional 24-month cohort of Gd-MRI exposed patients at this center, as well as more prolonged follow-up and expanded information compared with the previous report from the cohort. The closest available blood test to the time of the Gd-MRI scan was used to calculate the egfr, using the four-variable Modification of Diet in Renal Disease (MDRD) equation. Patients had their notes and electronic records scrutinized for any signs or symptoms resembling NSF after the MRA scan. This included any new dermatology or rheumatology referrals. Symptoms of NSF would include new dermatologic or rheumatologic com- Copyright 2010 by the American Society of Nephrology ISSN: /
2 Clin J Am Soc Nephrol 5: , 2010 Risk for NSF in CKD 485 plaints such as pruritus, dysesthesia, skin changes, or mobility restriction. Signs included skin tightening, thickening, tethering, or hyperpigmentation as well as joint contractures. Any patient who had received a skin biopsy for any indication after Gd exposure had this result scrutinized, even when this occurred years after Gd exposure. The data were collected and amalgamated in When the cause of death was not recorded on the hospital records, the records around the time of death were analyzed, and the patient s family physician was contacted for further information. MRI Protocols Salford Royal Hospital. Patients received Magnevist (n 572); Dotarem (n 86); Omniscan (n 40); and, more recently, Gadovist (n 69), Vasovist (n 5), and Multihance (n 3), depending on the favored contrast modality at the time. All patients had been scanned according to the department s protocol whereby 0.2 mmol/kg Gdcontaining contrast agent was administered; however, from July 2007, a single dose was administered (0.1 mmol/kg). No special prophylactic precautions were undertaken. All of the patients had undergone MRA directed at imaging the renal arteries. Hammersmith Hospital. All patients received contrast with Multihance Gd (gadobenate dimeglumine; 0.1 mmol/kg), and, again, no special prophylactic precautions were undertaken. A total of 94.1% of the 1328 patients who were studied had undergone MRA of the renal arteries, whereas 5.9% were investigated with pelvic Gd-MRA. Statistical Analysis Continuous data (e.g., age, follow-up) were expressed as mean SD and categorical data as n (%). All statistical analyses were performed using SPSS Results A total of 690 patients (636 patients with complete data) were followed up at Salford Royal Hospital and an additional 89 patients in its peripheral referral center at Bolton Royal Hospital. Complete data were available for 1328 patients who had had MRA in the Department of Radiology at the Hammersmith Hospital. Thus, a total of 2053 patients were included in the study. Baseline demographics of age, gender, and renal function are provided in Table 1. A total of 63.5% were men, mean age was years, and among them they had 2278 Gd-MRI scans. Mean follow-up of the cohort was months (range 0.0 to months), with a total follow-up period of patientyears. A total of 89 (4.3%) patients had stage 1 CKD 1 at the time of imaging, 305 (14.9%) had stage 2 CKD, 918 (44.7%) had stage 3 CKD, 491 (23.9%) had stage 4 CKD, and 250 (12.2%) had stage 5 CKD. Thus 741 (36.1%) patients had either stage 4 or 5 CKD, with 133 of the latter being dialysis patients (Table 1). A total of 453 (21.4%) patients had renal transplants. Patients were also subdivided by which agent they received, with further subdivision of stage 5 CKD into whether they were predialysis or receiving dialysis (Table 2 and Figure 1). No patients developed any symptoms or signs suggestive of NSF during follow-up; 400 (19.5%) patients had died, but there was no record of any of the deaths being related to NSF. A total of 190 patients had received two MRA scans. From the Salford Royal database, 21 patients were found to have had a follow-up appointment for a known rheumatologic or dermatologic condition, and 14 had routine dermatologic Table 1. Patients who underwent Gd-containing scans subdivided by CKD stage CKD (n [%]) Follow-up (Months; egfr (ml/min; Creatinine ( mol/l; Gender (M:F; %) Age (Years; Parameter 165 (12.4) 278 (20.9) 600 (45.2) 225 (16.9) 60 (4.5) (0.0 to 71.0) (3.0 to 135.0) (46.0 to ) 848:480 (63.6:36.1) (18.0 to 93.0) Hammersmith Hospital (n 1328) 85 (11.7) 213 (29.4) 318 (43.9) 80 (11.0) 29 (4.0) (0.0 to 115.0) (5.0 to 133.0) (36.0 to 884.0) 455:270 (62.8:37.2) (19.0 to 92.0) Salford Royal Hospital (n 725) 250 (12.2) 491 (23.9) 918 (44.7) 305 (14.9) 89 (4.3) (0.0 to 115.0) (3.0 to 135.0) (36.0 to ) 1303:750 (63.5:36.5) Total (n 2053) (18.0 to 93.0)
3 486 Clinical Journal of the American Society of Nephrology Clin J Am Soc Nephrol 5: , 2010 Table 2. Individual patients renal function at the time of MRI according to the Gd agents received Agent Parameter Gadobenate Dimeglumine (Bracco Diagnostics) Gadopentetate Dimeglumine (Schering) Gadodiamide (GE Healthcare) Gadoterate Meglumine (Guerbay) Gado-butrol (Bayer Schering Pharma) Gadofosveset Trisodium (Bayer Schering Pharma) Trade name Multihance Magnevist Omniscan Dotarem Gadovist Vasovist Type of agent Ionic linear Ionic linear Nonionic linear Ionic cyclic Nonionic cyclic Ionic linear Patients (n [%]) 1331 (64.8) 522 (25.4) 40 (1.9) 86 (4.2) 69 (3.4) 5 (0.2) egfr of patients who received the agent (ml/min; mean SD [range]) (3.0 to 135.0) (5.0 to 133.0) (8.0 to 87.0) (14.0 to 82.0) (14.0 to 90.0) Receiving double dose of the Gd agent (n [%]) No. of patients with stage 4 CKD No. of patients with stage 5 CKD No. of patients on dialysis (16.0 to 40.0) 0 (0.0) 495 (94.8) 40 (100.0) 0 (0.0) 0 (0.0) 5 (100.0) follow-up as part of their posttransplantation skin surveillance protocol. Twenty patients had a new referral to dermatology or rheumatology after imaging. The new diagnoses after referral were basal cell carcinoma (n 6), osteoporosis (n 3), actinic keratosis (n 1), shingles (n 1), lymphomatoid papulosis (n 1), bullous pemphigoid (n 1), paraesthesia-associated carpal tunnel syndrome (n 1), musculoskeletal pain resolved spontaneously (n 1), gout (n 1), skin squamous cell carcinoma (n 1), chondrodermatitis of the ear (n 1), diabetic foot ulcer (n 1), and tuberculosis-associated skin change (n 1). There were no indeterminate diagnoses or diagnoses confirming cutaneous sclerosis or systemic fibrosis. Eighteen new skin biopsies were performed on these patients after referral. The histologic diagnoses identified on biopsy were basal cell carcinoma (n 5), actinic keratosis (n 2), squamous cell carcinoma (n 1), bullous pemphigoid (n 1), psoriasis (n 1), and chondrodermatitis (n 1). Figure 1. Numbers of patients with CKD stage 4 and 5 predialysis who received single or double dose gadolinium agents. Discussion NSF is undeniably a rare but devastating disease, presenting with a spectrum of clinical and histopathologic manifestations (2,3). It is associated with increased tissue deposition of collagen in the skin, subcutaneous fascia, striated muscles, joints, diaphragm, lungs, liver, and myocardium (4). Five percent of cases run a fulminant course (5), and the severity of the cutaneous lesions correlates with poor prognosis and death (6). Our study, which incorporates 2053 patients encompassing 5126 patient-years of follow-up, provides more evidence that Gd- MRI can be used safely for patients with stages 4 and 5 (nondialysis) CKD. To date, 315 cases of NSF have been reported in the literature (5); however, in the past 20 or so years, 200 million patients have been exposed to Gd-based contrast agents worldwide; 30 million have received Omniscan, and at least 80 million have received Magnevist. The majority of cases of NSF have been in patients with severe renal impairment, with 90% having dialysis-dependent CKD and the remaining 10% having acute kidney injury (AKI) or hepatorenal failure (7 9). In addition, the least stable Gd-based MR contrast agents, those that are linear, or nonionic (e.g., Omniscan, Magnevist), have been
4 Clin J Am Soc Nephrol 5: , 2010 Risk for NSF in CKD 487 more commonly linked to the development of NSF, which often occurs on the background of an inflammatory process (10). Evaluating the precise risk for developing NSF is hampered by a lack of prospective studies, which, given the strong causal relationship between Gd and NSF, would now be considered unethical; however, retrospective studies have provided some insight into the risk for dialysis patients. For example, in a cohort of 102 patients with varying degrees of renal function, NSF was found in 18% after exposure to gadodiamide (Omniscan). All patients with NSF had stage 5 CKD, and most had received high dosages of gadodiamide (typically 0.3 mmol/kg) (11). In another study, Prince et al. (12) assessed the incidence of NSF in two large US medical centers. Of 83,121 patients who received Gd-based contrast agents, 15 (0.02%) developed NSF. These patients all had received a higher-than-standard dosage of Gd and had either AKI or acute deterioration of CKD at the time of their scan. The prevalence of NSF within dialysis groups has been variably reported from 1.6% (13) to 4% (9) of patients, but these figures need to be examined with consideration for the frequency of MRI use in individual dialysis centers and the risk of positive reporting bias. Repeated doses of Gd seem to increase the risk for NSF, but no association has been found between residual urine volume or creatinine clearance in dialysis patients and the risk for NSF (13). There is no definitive cure for NSF. Anecdotal reports suggested partial responses to various therapies such as plasmapheresis, steroids, extracorporeal photopheresis, or treatment with thalidomide (5). Some have reported slowing or even reversal of the disease after renal transplantation or accompanying improvements in renal function (14,15). Dialysis after Gd-MRA/MRI does not always prevent occurrence of NSF (9) but is nonetheless recommended promptly after imaging for patients who are already receiving dialysis. Selective removal of both free and d Gd (gadopentetate dimeglumine and gadodiamide) by nanostructure silica materials in dialysis and hemoperfusion systems (16) has shown some experimental promise, potentially allowing for Gd removal from high-risk patients after Gd-MR exposure. As a result of the adverse literature linking CKD and Gd exposure to risk for NSF, various radiologic guidelines that initially recommended avoidance of Gd-MRI for patients with egfr 30 ml/min and the exercising of caution for patients who are being investigated with egfr between 30 and 60 ml/min were developed (17). This has provided a major investigative problem for clinicians, because Gd-MRI examinations have become indispensable to clinicians for certain indications. In addition, the functional information that is provided by MRI extends and complements the usefulness of MR studies (18). Although caution should be retained when undertaking Gd- MRI in the high-risk dialysis group, there is minimal evidence in the literature to suggest similar risk for patients with stages 1 through 4 CKD. Within the multicenter Angioplasty and STent for Renal Artery Lesions (ASTRAL) trial (19), in which 30% of the patients had stage 4 or 5 CKD, there was only one case of NSF in 1735 of the screened patients (incidence 0.06%), and that patient had acutely deteriorating stage 5 CKD (1). The only case series that described patients who had stages 2 and 3 CKD and had NSF has been criticized because of inaccuracies in the calculation of the egfr (20). Further confirmation of the safety of Gd-MRI in earlier stages of CKD comes from a recent prospective study (21) that examined the incidence of NSF in 168 patients with stage 3 CKD after intravenous exposure to gadobenate dimeglumine (Multihance; linear, ionic structure). No cases of NSF were reported in this cohort. As a result of the heightened awareness of NSF in patients with CKD, less stable Gd agents are now no longer being used in advanced CKD; Omniscan in particular is not recommended in any stage of renal impairment (22), because it is reported to carry a3to7%risk for causing NSF in at-risk (stages 4 and 5 CKD) patients. Magnevist carries a 0.1 to 1.0% risk (23). In addition, radiology reports now indicate whether Gd has been administered during a scan as well as the dosage used. The American College of Radiology Blue Ribbon Panel on MR Safety has updated its MR Safe Practice Guidelines, which exist to ensure safe and responsible practices in clinical and research MR environments (22). They advise that patients who have moderate CKD to ESRD (stages 3 through 5) and are to undergo Gd-MRI examinations of any kind have a written approval order from the radiologist involved. The guidelines also recommend refraining from administration of any Gd-containing contrast agents in patients with CKD unless a risk benefit assessment for a particular patient indicates that the benefits clearly outweigh the potential risk (22); however, no unambiguous distinction is made between patients with more advanced (stages 4 and 5) and milder forms (stage 3) of CKD. Knowledge of a patient s renal function and exclusion of AKI would be considered good practice before undertaking Gd-MRI and considered mandatory before administration of a Gd agent that has been associated with development of NSF by the European Society of Urogenital Radiology (23). All requests for MR should state whether a history of kidney disease or dialysis exists; further pragmatic guidance includes use of the lowest dosage of Gd that would provide the diagnostic benefit being sought and allowing a sufficient period of time for elimination of Gd from the body before re-administration in cases for which repeat scans are required. Our study has several limitations. First, the egfr was based on a single serum sample before imaging. As such, the egfr provides only an estimate of renal function, even in patients with steady-state CKD, and this should never supervene clinical judgment. In addition, this value may be unrepresentative in patients with AKI and oliguria, with the result that the renal function may be much worse than the serum creatinine indicates for that point in time. In such cases, the advisability of using Gd should be very carefully considered. Second, this was a retrospective analysis because NSF was described as a complication related to imaging with MRI-Gd only in A flaw of the retrospective design is that the diagnosis of NSF would have depended on the keenness of insight and accurate documentation of the clinicians who saw the patients, as well as the availability of adequate long-term follow-up of patients, and it is possible that there may have been cases of NSF that were undetected or incorrectly diagnosed. To improve confidence in the accuracy of our data relating to this, in one of the centers,
5 488 Clinical Journal of the American Society of Nephrology Clin J Am Soc Nephrol 5: , 2010 we analyzed all clinical entries, biopsy results, and new referral letters that were available on our computerized records so as to detect any signs or symptoms that may have been overlooked as NSF as a result of lack of awareness of its existence. Third, it is likely that there was underestimation of the amount of Gd to which some of our patients were exposed, because only renal and abdominal MRA scans were included. Nevertheless, we believe that our study serves to fill a gap in the literature concerning the safety of Gd in large cohorts of patients with stages 4 and 5 CKD before dialysis. The fear of NSF should not result in denial of Gd-MRI when clinically indicated. Our view is shared by the UK Royal College of Radiologists (24), whose guidelines allow for selective use of Gd-MRI in patients with low GFR when the clinical need for information is considered greater than that of NSF risk (24), albeit patients with stages 4 and 5 CKD are regarded as high risk for NSF in their guidelines. This last clause may result in clinicians being reluctant to image patients with stage 4 CKD and stable stage 5 CKD because of an unjustified concern of high NSF risk in nondialysis patients with CKD. Following this guidance and further to our two centers experience of outcomes, we would make the following recommendations: 1. Knowledge of not just a patient s egfr but also the trend in egfr should be sought before imaging patients with Gd- MRI. 2. Caution is merited for patients who have dialysis-requiring CKD or AKI especially with concomitant vascular comorbidities and are being considered for Gd-MRI. The latter should be undertaken only when the advantages of imaging far outweigh the risk for NSF. 3. Relative caution is required for patients who have stable stage 5 CKD and are not on dialysis, and, when possible, other imaging modalities should be considered (e.g., non Gd-MRI, computed tomographic angiography), or Gd-MRI with safer, cyclic agents (see point 6) should be used. 4. We believe that the risk for NSF is minimal for patients with stable stages 3 and 4 CKD (egfr 15 ml/min) and that these patients can safely be subjected to Gd-MRI when clinically indicated, notwithstanding the need for an informed discussion between clinician and patient and the application of other broad safety principles. 5. The minimum dosage of Gd required to obtain the required information should be used. We recommend one standard dosage of Gd or lower. 6. Safer structural Gd compounds (cyclic, ionic structure) should be used when possible, especially when Gd-MRI needs to be performed in the highest risk patients (dialysisrequiring CKD, AKI) and ideally in patients with non dialysis-treated stage 5 CKD. A candid discussion between the physician and the patient with CKD is therefore necessary. Our study is supportive of the low risk for NSF in patients with stages 1 through 4 CKD and those with predialysis stage 5 CKD, some of whom even received multiple and repeated doses of Gd. We believe that the risk for NSF is minimal for patients with stage 3 and 4 CKD (egfr 15 ml/min), provided that their renal function is stable, notwithstanding the need for application of other, broad safety principles. Disclosures None. References 1. Chrysochou C, Buckley DL, Dark P, Cowie A, Kalra PA: Gadolinium-enhanced magnetic resonance imaging for renovascular disease and nephrogenic systemic fibrosis: Critical review of the literature and UK experience. J Magn Reson Imaging 29: , Deng A, Bilu MD, Spillane A, Chwalek J, Surin-Lord S, Brooks S, Petrali J, Sina B, Gaspari A, Kao G: Nephrogenic systemic fibrosis with a spectrum of clinical and histopathological presentation: A disorder of aberrant dermal remodeling. J Cutan Pathol March 31, 2009 [epub ahead of print] 3. Marckmann P, Skov L, Rossen K, Thomsen HS: Clinical manifestation of gadodiamide-related nephrogenic systemic fibrosis. Clin Nephrol 69: , Gibson SE, Farver CF, Prayson RA: Multiorgan involvement in nephrogenic fibrosing dermopathy: An autopsy case and review of the literature. Arch Pathol Lab Med 130: , Cowper SE. Nephrogenic Fibrosing Dermopathy [ICNSFR Website] Available at: Accessed August 13, Mendoza FA, Artlett CM, Sandorfi N, Latinis K, Piera- Velazquez S, Jimenez SA: Description of 12 cases of nephrogenic fibrosing dermopathy and review of the literature. Semin Arthritis Rheum 35: , Marckmann P: An epidemic outbreak of nephrogenic systemic fibrosis in a Danish hospital. Eur J Radiol 66: , Shabana WM, Cohan RH, Ellis JH, Hussain HK, Francis IR, Su LD, Mukherji SK, Swartz RD: Nephrogenic systemic fibrosis: A report of 29 cases. AJR Am J Roentgenol 190: , Broome DR, Girguis MS, Baron PW, Cottrell AC, Kjellin I, Kirk GA: Gadodiamide-associated nephrogenic systemic fibrosis: Why radiologists should be concerned. AJR Am J Roentgenol 188: , Swaminathan S, Shah SV: New insights into nephrogenic systemic fibrosis. J Am Soc Nephrol 18: , Rydahl C, Thomsen HS, Marckmann P: High prevalence of nephrogenic systemic fibrosis in chronic renal failure patients exposed to gadodiamide, a gadolinium-containing magnetic resonance contrast agent. Invest Radiol 43: , Prince MR, Zhang H, Morris M, MacGregor JL, Grossman ME, Silberzweig J, DeLapaz RL, Lee HJ, Magro CM, Valeri AM: Incidence of nephrogenic systemic fibrosis at two large medical centers. Radiology 248: , Heinz-Peer G, Neruda A, Watschinger B, Vychytil A, Geusau A, Haumer M, Weber M: Prevalence of NSF following intravenous gadolinium-contrast media administration in dialysis patients with endstage renal disease. Eur J Radiol July 18, 2009 [epub ahead of print] 14. Maloo M, Abt P, Kashyap R, Younan D, Zand M, Orloff M,
6 Clin J Am Soc Nephrol 5: , 2010 Risk for NSF in CKD 489 Jain A, Pentland A, Scott G, Bozorgzadeh A: Nephrogenic systemic fibrosis among liver transplant recipients: A single institution experience and topic update. Am J Transplant 6: , Cowper SE: Nephrogenic fibrosing dermopathy: The first 6 years. Curr Opin Rheumatol 15: , Yantasee W, Fryxell GE, Porter GA, Pattamakomsan K, Sukwarotwat V, Chouyyok W, Koonsiripaiboon V, Xu J, Raymond KN: Novel sorbents for removal of gadoliniumbased contrast agents in sorbent dialysis and hemoperfusion: Preventive approaches to nephrogenic systemic fibrosis. Nanomedicine May 15, 2009 [epub ahead of print] 17. Public Assessment Report: Increased risk of nephrogenic fibrosing dermopathy/nephrogenic systemic fibrosis and gadolinium-containing MRI contrast agents. Available at: Accessed August 13, Michaely HJ, Sourbron S, Dietrich O, Attenberger U, Reiser MF, Schoenberg SO: Functional renal MR imaging: An overview. Abdom Imaging December 7, 2006 [epub ahead of print] 19. Wheatley K, Ives N, Gray R, Kalra PA, Moss JG, Baigent C, Carr S, Chalmers N, Eadington D, Hamilton G, Lipkin G, Nicholson A, Scoble J: Revascularization versus medical therapy for renal-artery stenosis. N Engl J Med 361: , Saab G, bu-alfa A: Are patients with moderate renal failure at risk for developing nephrogenic systemic fibrosis? Radiology 244: , Bryant BJ, Im K, Broome DR: Evaluation of the incidence of nephrogenic systemic fibrosis in patients with moderate renal insufficiency administered gadobenate dimeglumine for MRI. Clin Radiol 64: , Kanal E, Barkovich AJ, Bell C, Borgstede JP, Bradley WG Jr, Froelich JW, Gilk T, Gimbel JR, Gosbee J, Kuhni- Kaminski E, Lester JW Jr, Nyenhuis J, Parag Y, Schaefer DJ, Sebek-Scoumis EA, Weinreb J, Zaremba LA, Wilcox P, Lucey L, Sass N: ACR guidance document for safe MR practices: AJR Am J Roentgenol 188: , ESUR Guideline: Gadolinium based contrast media and nephrogenic systemic fibrosis, July 17, Available at: Final.pdf. Accessed September 3, The Royal College of Radiologists, Board of the Faculty of Clinical Radiology: Gadolinium-based Contrast Media and Nephrogenic Systemic Fibrosis, London, The Royal College of Radiologists, November Available at: NSF_guidanceNov07.pdf. Accessed August 6, 2009
Gadolinium Based Contrast Agent Recommendations (Revised 06/07/2018)
 Gadolinium Based Contrast Agent Recommendations (Revised 06/07/2018) Introduction: Nephrogenic systemic fibrosis is the only known adverse health effect related to gadoliniumbased contrast agents (GBCAs).
Gadolinium Based Contrast Agent Recommendations (Revised 06/07/2018) Introduction: Nephrogenic systemic fibrosis is the only known adverse health effect related to gadoliniumbased contrast agents (GBCAs).
University of Virginia Institutional Review Board - Health Sciences Research Guidelines for Researchers Using Gadolinium-Enhanced MRI in Research
 University of Virginia Institutional Review Board - Health Sciences Research Guidelines for Researchers Using Gadolinium-Enhanced MRI in Research Page 1 of 16 Table of Contents New Information:... 3 IRB-HSR
University of Virginia Institutional Review Board - Health Sciences Research Guidelines for Researchers Using Gadolinium-Enhanced MRI in Research Page 1 of 16 Table of Contents New Information:... 3 IRB-HSR
Global reports and findings of NSF and its effects
 Safety Forum: MR Safety Update - SMRT 2008 Sunday May 8, 2:25 p.m. Global reports and findings of NSF and its effects Tim Leiner, MD PhD Assistant Professor of Radiology, Department of Radiology, Maastricht
Safety Forum: MR Safety Update - SMRT 2008 Sunday May 8, 2:25 p.m. Global reports and findings of NSF and its effects Tim Leiner, MD PhD Assistant Professor of Radiology, Department of Radiology, Maastricht
Information for Healthcare Professionals and other Stakeholders
 Information for Healthcare Professionals and other Stakeholders NEPHROGENIC SYSTEMIC FIBROSIS: AN UNCOMMON AND DEBILITATING DISEASE POSSIBLY ASSOCIATED WITH GADOLINIUM CHELATES Villepinte, February 2014
Information for Healthcare Professionals and other Stakeholders NEPHROGENIC SYSTEMIC FIBROSIS: AN UNCOMMON AND DEBILITATING DISEASE POSSIBLY ASSOCIATED WITH GADOLINIUM CHELATES Villepinte, February 2014
Administration of Gadolinium Contrast in Adults Procedural Guideline
 Administration of Gadolinium Contrast in Adults Procedural Guideline This procedural guideline is designed to assist Radiologists by providing an analytical framework for the evaluation of gadolinium contrast
Administration of Gadolinium Contrast in Adults Procedural Guideline This procedural guideline is designed to assist Radiologists by providing an analytical framework for the evaluation of gadolinium contrast
Protocol for iv. iodine and gadolinium contrast studies
 Protocol for iv. iodine and gadolinium contrast studies Royal College of Radiologists Standard The individual administering the contrast agent must ensure that the patient understands that it is to be
Protocol for iv. iodine and gadolinium contrast studies Royal College of Radiologists Standard The individual administering the contrast agent must ensure that the patient understands that it is to be
PLEASE SCROLL DOWN FOR ARTICLE
 This article was downloaded by:[danish Veterinary and Agricultural Library] [Danish Veterinary and Agricultural Library] On: 24 June 2007 Access Details: [subscription number 773444395] Publisher: Informa
This article was downloaded by:[danish Veterinary and Agricultural Library] [Danish Veterinary and Agricultural Library] On: 24 June 2007 Access Details: [subscription number 773444395] Publisher: Informa
Information for Healthcare Professionals and other Stakeholders
 Information for Healthcare Professionals and other Stakeholders NEPHROGENIC SYSTEMIC FIBROSIS: AN UNCOMMON AND DEBILITATING DISEASE POSSIBLY ASSOCIATED WITH GADOLINIUM CHELATES Villepinte, April 2013 Any
Information for Healthcare Professionals and other Stakeholders NEPHROGENIC SYSTEMIC FIBROSIS: AN UNCOMMON AND DEBILITATING DISEASE POSSIBLY ASSOCIATED WITH GADOLINIUM CHELATES Villepinte, April 2013 Any
Gadolinium-Based Contrast Media
 Gadolinium-Based Contrast Media Wm. Faulkner, B.S.,R.T.(R)(MR)CT, FSMRT, MRSO (MRSC ) Kristan Harrington, MBA, R.T.(R)(MR), MRSO (MRSC TM ) Gadolinium ( 64 Gd) 7 un-paired electrons chelate, any of a class
Gadolinium-Based Contrast Media Wm. Faulkner, B.S.,R.T.(R)(MR)CT, FSMRT, MRSO (MRSC ) Kristan Harrington, MBA, R.T.(R)(MR), MRSO (MRSC TM ) Gadolinium ( 64 Gd) 7 un-paired electrons chelate, any of a class
NSF Coming and Going
 NSF Coming and Going Martin R. Prince, MD, PhD Cornell and Columbia Universities Patent agreements: GE, Philips, Siemens, Hitachi, Medrad, Epix, Lantheus, Bayer, Bracco, Nemoto, Mallinckrodt and Topspins
NSF Coming and Going Martin R. Prince, MD, PhD Cornell and Columbia Universities Patent agreements: GE, Philips, Siemens, Hitachi, Medrad, Epix, Lantheus, Bayer, Bracco, Nemoto, Mallinckrodt and Topspins
DIVISION OF MEDICAL IMAGING AND HEMATOLOGY PRODUCTS
 DIVISION OF MEDICAL IMAGING AND HEMATOLOGY PRODUCTS MEMORANDUM TO THE FILE i. NDA: 20-123, 22-066 Product: Omniscan ii. NDA: 19-596, 21-037 Product: Magnevist iii. NDA: 20-976, 20-937,20-975 Product: OptiMARK
DIVISION OF MEDICAL IMAGING AND HEMATOLOGY PRODUCTS MEMORANDUM TO THE FILE i. NDA: 20-123, 22-066 Product: Omniscan ii. NDA: 19-596, 21-037 Product: Magnevist iii. NDA: 20-976, 20-937,20-975 Product: OptiMARK
Beyond NSF: Acute GBCA adverse reactions
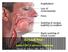 Source images Beyond NSF: Acute GBCA adverse reactions Martin R. Prince, MD, PhD, FACR Disclosures Patent Agreements: GE, Siemens, Philips, Hitachi, Toshiba, Bayer, Bracco, Mallinckrodt, Medrad, Nemoto,
Source images Beyond NSF: Acute GBCA adverse reactions Martin R. Prince, MD, PhD, FACR Disclosures Patent Agreements: GE, Siemens, Philips, Hitachi, Toshiba, Bayer, Bracco, Mallinckrodt, Medrad, Nemoto,
Gadolinium-Based MR Contrast Agents
 Gadolinium-Based MR Contrast Agents Wm. Faulkner, BS,RT(R)(MR)(CT), FSMRT, MRSO (MRSC ) Kristan Harrington, MBA, RT(R)(MR) ARRT, MRSO (MRSC ) Magnetic Resonance Imaging, Vol 3, pp27-35, 1985 0.35 T 35/1600
Gadolinium-Based MR Contrast Agents Wm. Faulkner, BS,RT(R)(MR)(CT), FSMRT, MRSO (MRSC ) Kristan Harrington, MBA, RT(R)(MR) ARRT, MRSO (MRSC ) Magnetic Resonance Imaging, Vol 3, pp27-35, 1985 0.35 T 35/1600
Seeing is Believing... Look Beneath the Surface
 References 1. Idee JM, Port C, Raynal I, et al. Clinical and geological consequences of transmetallation induced by contrast agents for magnetic resonance imaging: a review. Fundamental and Clinical Pharmacology.
References 1. Idee JM, Port C, Raynal I, et al. Clinical and geological consequences of transmetallation induced by contrast agents for magnetic resonance imaging: a review. Fundamental and Clinical Pharmacology.
A Safety Update on the Gadolinium Chelates
 Control # 1029 A Safety Update on the Gadolinium Chelates Val M. Runge, MD Universitätsinstitut für Diagnostische, Interventionelle und Pädiatrische Radiologie University Hospital Bern Allergic Reactions
Control # 1029 A Safety Update on the Gadolinium Chelates Val M. Runge, MD Universitätsinstitut für Diagnostische, Interventionelle und Pädiatrische Radiologie University Hospital Bern Allergic Reactions
SUBJECT: ASSESSMENT OF LAB RESULTS PRIOR TO INJECTING GADOLINIUM-BASED CONTRAST MEDIA.
 ASSESSMENT OF PATIENTS: IMAGING SERVICES Policy #: 300.02 Effective Date: 6/29/09 Last Revision Date: 10/07 Page 1 of 5 SUBJECT: ASSESSMENT OF LAB RESULTS PRIOR TO INJECTING GADOLINIUM-BASED CONTRAST MEDIA
ASSESSMENT OF PATIENTS: IMAGING SERVICES Policy #: 300.02 Effective Date: 6/29/09 Last Revision Date: 10/07 Page 1 of 5 SUBJECT: ASSESSMENT OF LAB RESULTS PRIOR TO INJECTING GADOLINIUM-BASED CONTRAST MEDIA
Gadolinium-Based MR Contrast Agents
 Gadolinium-Based MR Contrast Agents Magnetic Resonance Imaging, Vol 3, pp27-35, 1985 Wm. Faulkner, BS,RT(R)(MR)(CT), FSMRT, MRSO (MRSC ) Kristan Harrington, MBA, RT(R)(MR) ARRT, MRSO (MRSC ) 0.35 T 0.35
Gadolinium-Based MR Contrast Agents Magnetic Resonance Imaging, Vol 3, pp27-35, 1985 Wm. Faulkner, BS,RT(R)(MR)(CT), FSMRT, MRSO (MRSC ) Kristan Harrington, MBA, RT(R)(MR) ARRT, MRSO (MRSC ) 0.35 T 0.35
Gadolinium-Based Contrast Agents for Magnetic Resonance Imaging (marketed as Magnevist, MultiHance, Omniscan, OptiMARK, ProHance)
 Information for Healthcare Professionals Page 1 of 5 FDA ALERT [6/2006, updated 12/2006 and 5/23/2007: This updated Alert highlights FDA s request for addition of a boxed warning and new warnings about
Information for Healthcare Professionals Page 1 of 5 FDA ALERT [6/2006, updated 12/2006 and 5/23/2007: This updated Alert highlights FDA s request for addition of a boxed warning and new warnings about
MR Contrast Agents. Why Use Contrast Agents in MRI? Why Use Contrast Agents in MRI? US Agents. Understanding and Embracing Change
 Why Use Contrast Agents in MRI? Improve disease detection and characterization Increase sensitivity to extent of disease MR Contrast Agents Understanding and Embracing Change Kristan Harrington, MBA, RT
Why Use Contrast Agents in MRI? Improve disease detection and characterization Increase sensitivity to extent of disease MR Contrast Agents Understanding and Embracing Change Kristan Harrington, MBA, RT
Frequency and Severity of Acute Allergic-Like Reactions to Gadolinium-Containing IV Contrast Media in Children and Adults
 Reactions to Gadolinium- Containing Contrast Media MR Imaging Original Research Jonathan R. Dillman 1 James H. Ellis 1 Richard H. Cohan 1 Peter J. Strouse 2 Sophia C. Jan 1 Dillman JR, Ellis JH, Cohan
Reactions to Gadolinium- Containing Contrast Media MR Imaging Original Research Jonathan R. Dillman 1 James H. Ellis 1 Richard H. Cohan 1 Peter J. Strouse 2 Sophia C. Jan 1 Dillman JR, Ellis JH, Cohan
INTRODUCTION CLINICAL EXPERIENCE CLINICAL EFFICACY PEDIATRIC EXPERIENCE DOSING SUMMARY
 1 2 DOTAREM Administered Doses 3 Molecular Structure of DOTAREM DOTAREM offers high thermodynamic and kinetic stability provided by its macrocyclic and ionic structure* 3 *The clinical significance of
1 2 DOTAREM Administered Doses 3 Molecular Structure of DOTAREM DOTAREM offers high thermodynamic and kinetic stability provided by its macrocyclic and ionic structure* 3 *The clinical significance of
Please see Important Safety Information, including Boxed Warnings for Gadavist and Magnevist below.
 August 15 th, 2018 Dear Valued Customer: Thank you for your continued patience over the last several months as we have worked to resolve our contrast supply interruption. The purpose of this letter is
August 15 th, 2018 Dear Valued Customer: Thank you for your continued patience over the last several months as we have worked to resolve our contrast supply interruption. The purpose of this letter is
Annex III. Amendments to relevant sections of the product information
 Annex III Amendments to relevant sections of the product information Note: These amendments to the relevant sections of the product information are the outcome of the referral procedure. The product information
Annex III Amendments to relevant sections of the product information Note: These amendments to the relevant sections of the product information are the outcome of the referral procedure. The product information
Nephrogenic systemic fibrosis associated with gadolinium based contrast agents: A summary of the medical literature reporting
 European Journal of Radiology 66 (2008) 230 234 Nephrogenic systemic fibrosis associated with gadolinium based contrast agents: A summary of the medical literature reporting Dale R. Broome Department of
European Journal of Radiology 66 (2008) 230 234 Nephrogenic systemic fibrosis associated with gadolinium based contrast agents: A summary of the medical literature reporting Dale R. Broome Department of
Contrast-enhanced MRI: how do changing EU regulations impact daily practice?
 Safety considerations in contrast enhanced procedures Carlo Catalano Sapienza University of Rome Contrast-enhanced MRI: how do changing EU regulations impact daily practice? CE MRI: EU regulations - Initial
Safety considerations in contrast enhanced procedures Carlo Catalano Sapienza University of Rome Contrast-enhanced MRI: how do changing EU regulations impact daily practice? CE MRI: EU regulations - Initial
Public Assessment Report
 Public Assessment Report Increased risk of nephrogenic fibrosing dermopathy/nephrogenic systemic fibrosis and gadolinium-containing MRI contrast agents Executive summary 2 Introduction 3 Data assessed
Public Assessment Report Increased risk of nephrogenic fibrosing dermopathy/nephrogenic systemic fibrosis and gadolinium-containing MRI contrast agents Executive summary 2 Introduction 3 Data assessed
William G. Bradley, Jr, MD, PhD, FACR
 William G. Bradley, Jr, MD, PhD, FACR Professor of Radiology Chair, Dept of Radiology University of California, San Diego Medical Center San Diego, California Learning Objectives Identify emerging safety
William G. Bradley, Jr, MD, PhD, FACR Professor of Radiology Chair, Dept of Radiology University of California, San Diego Medical Center San Diego, California Learning Objectives Identify emerging safety
Instructions for the safe administration of gadolinium based contrast agents (GBCA). 1. PREADMINISTRATION PRECAUTIONS:
 POLICY NUMBER: RM 6-18 CATEGORY: Patient Care DATE: June 2016 NEXT REVIEW DATE: April 2017 SUBJECT: PURPOSE: POLICY: Intravenous Gadolinium Based Contrast Administration To prevent complications associated
POLICY NUMBER: RM 6-18 CATEGORY: Patient Care DATE: June 2016 NEXT REVIEW DATE: April 2017 SUBJECT: PURPOSE: POLICY: Intravenous Gadolinium Based Contrast Administration To prevent complications associated
This copy is for personal use only. To order printed copies, contact Purpose: Materials and Methods: Results: Conclusion:
 This copy is for personal use only. To order printed copies, contact reprints@rsna.org No Incidence of Nephrogenic Systemic Fibrosis after Gadobenate Dimeglumine Administration in Patients Undergoing Dialysis
This copy is for personal use only. To order printed copies, contact reprints@rsna.org No Incidence of Nephrogenic Systemic Fibrosis after Gadobenate Dimeglumine Administration in Patients Undergoing Dialysis
Nephrogenic Systemic Fibrosis: Possible Association with a Predisposing Infection
 MR Imaging Original Research MR Imaging Original Research Lauren Parks Golding 1,2 James M. Provenzale 3 Golding LP, Provenzale JM Keywords: connective tissue disorders, contrast media, dialysis, infections,
MR Imaging Original Research MR Imaging Original Research Lauren Parks Golding 1,2 James M. Provenzale 3 Golding LP, Provenzale JM Keywords: connective tissue disorders, contrast media, dialysis, infections,
Extracellular gadolinium-based contrast media: An overview
 European Journal of Radiology 66 (2008) 160 167 Extracellular gadolinium-based contrast media: An overview Marie-France Bellin, Aart J. Van Der Molen University Paris-Sud 11, Department of Radiology, University
European Journal of Radiology 66 (2008) 160 167 Extracellular gadolinium-based contrast media: An overview Marie-France Bellin, Aart J. Van Der Molen University Paris-Sud 11, Department of Radiology, University
Clinical Study Nephrogenic Systemic Fibrosis Risk and Liver Disease
 International Nephrology, Article ID 679605, 6 pages http://dx.doi.org/10.1155/2014/679605 Clinical Study Nephrogenic Systemic Fibrosis Risk and Liver Disease Robert F. Hanna, 1 Lee A. Finkelstone, 1 Daniel
International Nephrology, Article ID 679605, 6 pages http://dx.doi.org/10.1155/2014/679605 Clinical Study Nephrogenic Systemic Fibrosis Risk and Liver Disease Robert F. Hanna, 1 Lee A. Finkelstone, 1 Daniel
Information for Healthcare Professionals and other Stakeholders
 Information for Healthcare Professionals and other Stakeholders NEPHROGENIC SYSTEMIC FIBROSIS: AN UNCOMMON AND DEBILITATING DISEASE POSSIBLY ASSOCIATED WITH GADOLINIUM CHELATES Villepinte, 2 july 2008
Information for Healthcare Professionals and other Stakeholders NEPHROGENIC SYSTEMIC FIBROSIS: AN UNCOMMON AND DEBILITATING DISEASE POSSIBLY ASSOCIATED WITH GADOLINIUM CHELATES Villepinte, 2 july 2008
Magnetic resonance imaging (MRI) scans are significantly
 Mini-Review Current Status of Gadolinium Toxicity in Patients with Kidney Disease Mark A. Perazella Department of Medicine, Section of Nephrology, Yale University School of Medicine, New Haven, Connecticut
Mini-Review Current Status of Gadolinium Toxicity in Patients with Kidney Disease Mark A. Perazella Department of Medicine, Section of Nephrology, Yale University School of Medicine, New Haven, Connecticut
Gadolinium Use in Patients with Kidney Disease: A Cause for Concern
 Editorial Gadolinium Use in Patients with Kidney Disease: A Cause for Concern Mark A. Perazella* and Roger A. Rodby *Section of Nephrology, Department of Medicine, Yale University School of Medicine, New
Editorial Gadolinium Use in Patients with Kidney Disease: A Cause for Concern Mark A. Perazella* and Roger A. Rodby *Section of Nephrology, Department of Medicine, Yale University School of Medicine, New
PATIENT CARE AND MRI SAFETY Module 7
 PATIENT CARE AND MRI SAFETY Module 7 1 Biological Considerations There are no reported adverse biological effects of extended exposure to MRI. However, several inconsequential and reversible effects of
PATIENT CARE AND MRI SAFETY Module 7 1 Biological Considerations There are no reported adverse biological effects of extended exposure to MRI. However, several inconsequential and reversible effects of
Imaging in the time of NFD/NSF: do we have to change our routines concerning renal insufficiency?
 DI 10.1007/s10334-007-0071-5 EDITRIAL REVIEW Imaging in the time of FD/SF: do we have to change our routines concerning renal insufficiency? Georg Bongartz Accepted: 7 March 2007 ESMRMB 2007 Abstract To
DI 10.1007/s10334-007-0071-5 EDITRIAL REVIEW Imaging in the time of FD/SF: do we have to change our routines concerning renal insufficiency? Georg Bongartz Accepted: 7 March 2007 ESMRMB 2007 Abstract To
Side Effects and Complications of Magnetic Resonance Contrast Media
 HOSPITAL CHRONICLES 2012, 7(4): 208 214 Review Side Effects and Complications of Magnetic Resonance Contrast Media Ekaterini Tavernaraki, MD, PhD, Anna Skoula MD, Stylianos Benakis, MD, Dimitrios Exarhos
HOSPITAL CHRONICLES 2012, 7(4): 208 214 Review Side Effects and Complications of Magnetic Resonance Contrast Media Ekaterini Tavernaraki, MD, PhD, Anna Skoula MD, Stylianos Benakis, MD, Dimitrios Exarhos
Please see Important Safety Information, including Boxed Warnings for Gadavist, Eovist and Magnevist on the following pages.
 Dear Valued Customer: As a valued partner we want to inform you that a technical issue occurred at our Berlin manufacturing center where final formulation and packaging of Bayer MRI (Magnetic Resonance
Dear Valued Customer: As a valued partner we want to inform you that a technical issue occurred at our Berlin manufacturing center where final formulation and packaging of Bayer MRI (Magnetic Resonance
Incidence of Immediate Gadolinium Contrast Media Reactions
 Health Care Policy and Quality Original Research Prince et al. Immediate Gadolinium Contrast Media Reactions Health Care Policy and Quality Original Research Martin R. Prince 1 Honglei Zhang Zhitong Zou
Health Care Policy and Quality Original Research Prince et al. Immediate Gadolinium Contrast Media Reactions Health Care Policy and Quality Original Research Martin R. Prince 1 Honglei Zhang Zhitong Zou
Important Update - Availability of Bayer s MRI (Magnetic Resonance Imaging) Contrast agents
 Important Update - Availability of Bayer s MRI (Magnetic Resonance Imaging) Contrast agents Certain batches of pharmaceutical products from our company s Supply Center in Berlin where final formulation
Important Update - Availability of Bayer s MRI (Magnetic Resonance Imaging) Contrast agents Certain batches of pharmaceutical products from our company s Supply Center in Berlin where final formulation
Update in Nephrology. Case: Question 1. Case presentation. Acute Kidney Injury. For her hypertension management, you decide to:
 Update in Nephrology Chronic Kidney Disease Renoprotection and Proteinuria, ACE and/or ARB Anemia management Update in Nephrology Renal artery stenosis Nephrogenic systemic fibrosis Division of Nephrology
Update in Nephrology Chronic Kidney Disease Renoprotection and Proteinuria, ACE and/or ARB Anemia management Update in Nephrology Renal artery stenosis Nephrogenic systemic fibrosis Division of Nephrology
Nephrogenic Systemic Fibrosis in Denmark A Nationwide Investigation
 A Nationwide Investigation Tina R. Elmholdt 1,2 *, Anne B. B. Olesen 2, Bettina Jørgensen 3, Stinne Kvist 3, Lone Skov 4, Henrik S. Thomsen 5, Peter Marckmann 6,7, Michael Pedersen 1,8 1 Institute of Clinical
A Nationwide Investigation Tina R. Elmholdt 1,2 *, Anne B. B. Olesen 2, Bettina Jørgensen 3, Stinne Kvist 3, Lone Skov 4, Henrik S. Thomsen 5, Peter Marckmann 6,7, Michael Pedersen 1,8 1 Institute of Clinical
Pro-enkephalin and Renal Disease. Alan H. Wu, Ph.D. University of California, San Francisco 12 th Annual UCSD Biomarkers of Cardiac Disease
 Pro-enkephalin and Renal Disease Alan H. Wu, Ph.D. University of California, San Francisco 12 th Annual UCSD Biomarkers of Cardiac Disease The presenter has received relevant grants and /or consulting
Pro-enkephalin and Renal Disease Alan H. Wu, Ph.D. University of California, San Francisco 12 th Annual UCSD Biomarkers of Cardiac Disease The presenter has received relevant grants and /or consulting
CKD IN THE CLINIC. Session Content. Recommendations for commonly used medications in CKD. CKD screening and referral
 CKD IN THE CLINIC Family Physician Refresher Course Lisa M. Antes, MD April 19, 2017 No disclosures Session Content 1. 2. Recommendations for commonly used medications in CKD Basic principles /patient
CKD IN THE CLINIC Family Physician Refresher Course Lisa M. Antes, MD April 19, 2017 No disclosures Session Content 1. 2. Recommendations for commonly used medications in CKD Basic principles /patient
Annex II. Scientific conclusions
 Annex II Scientific conclusions 31 Scientific conclusions In accordance with Article 107k of Directive 2001/83/EC, the CHMP considered the PRAC recommendation adopted on 6 July 2017. Overall summary of
Annex II Scientific conclusions 31 Scientific conclusions In accordance with Article 107k of Directive 2001/83/EC, the CHMP considered the PRAC recommendation adopted on 6 July 2017. Overall summary of
Department of Radiology
 DUKE UNIVERSITY HEALTH SYSTEM Duke University Hospital Department of Radiology Policies and Procedures Name: MRI Screening of Patients and Other Individuals Effective Date: 03/2017 Review / Revision History:
DUKE UNIVERSITY HEALTH SYSTEM Duke University Hospital Department of Radiology Policies and Procedures Name: MRI Screening of Patients and Other Individuals Effective Date: 03/2017 Review / Revision History:
Gadolinium a specific trigger for the development of nephrogenic fibrosing dermopathy and nephrogenic systemic fibrosis?
 Nephrol Dial Transplant (2006) 21: 1104 1108 doi:10.1093/ndt/gfk062 Advance Access publication 23 January 2006 Interesting Case Gadolinium a specific trigger for the development of nephrogenic fibrosing
Nephrol Dial Transplant (2006) 21: 1104 1108 doi:10.1093/ndt/gfk062 Advance Access publication 23 January 2006 Interesting Case Gadolinium a specific trigger for the development of nephrogenic fibrosing
Policy #: 291 Latest Review Date: February 2013
 Effective for dates of service on or after April 1, 2013, refer to: https://www.bcbsal.org/providers/policies/carecore.cfm Name of Policy: Magnetic Resonance Angiography (MRA) of the Chest (excluding the
Effective for dates of service on or after April 1, 2013, refer to: https://www.bcbsal.org/providers/policies/carecore.cfm Name of Policy: Magnetic Resonance Angiography (MRA) of the Chest (excluding the
Clinical Safety & Effectiveness Cohort 4-UTHSCSA. MRI Contrast Mis-administrations. May 21, 2010
 Clinical Safety & Effectiveness Cohort 4-UTHSCSA MRI Contrast Mis-administrations May 21, 2010 1 2 UTHSCSA/UHS The Team Ken Kist, MD (cohort member) Gilbert Cortez (cohort member) Kristi Hill-Herrera (cohort
Clinical Safety & Effectiveness Cohort 4-UTHSCSA MRI Contrast Mis-administrations May 21, 2010 1 2 UTHSCSA/UHS The Team Ken Kist, MD (cohort member) Gilbert Cortez (cohort member) Kristi Hill-Herrera (cohort
RAS Epidemiology. Renal Artery Stenosis. Pathophysiology of RAS. Disclosure of Potential Conflicts. Background Pathophysiology of RAS.
 Renal Artery Stenosis RAS Epidemiology Common Disease Incidence General Population 0.1% Hypertensive Population 4% HTN & Suspected CAD 10-20% Malignant HTN 20-30% Malignant HTN and CKD 30-40% Alexander
Renal Artery Stenosis RAS Epidemiology Common Disease Incidence General Population 0.1% Hypertensive Population 4% HTN & Suspected CAD 10-20% Malignant HTN 20-30% Malignant HTN and CKD 30-40% Alexander
Disclosure of Potential Conflicts. Renal Artery Stenosis. RAS Epidemiology. Road Map. Background. ASDIN 7th Annual Scientific Meeting
 Renal Artery Stenosis Disclosure of Potential Conflicts Cytopherx, Inc. R4 Vascular, Inc. Bard Peripheral Vascular Spectranetics, Inc. Alexander S. Yevzlin, MD Associate Professor of Medicine (CHS) ASDIN
Renal Artery Stenosis Disclosure of Potential Conflicts Cytopherx, Inc. R4 Vascular, Inc. Bard Peripheral Vascular Spectranetics, Inc. Alexander S. Yevzlin, MD Associate Professor of Medicine (CHS) ASDIN
Gadolinium Deposition in the Brain: Summary of Known Science and Recommendations from the International Society for Magnetic Resonance in Medicine
 Gadolinium Deposition in the Brain: Summary of Known Science and Recommendations from the International Society for Magnetic Resonance in Medicine Vikas Gulani, MD, PhD 1-4*, Fernando Calamante, PhD 5,6,
Gadolinium Deposition in the Brain: Summary of Known Science and Recommendations from the International Society for Magnetic Resonance in Medicine Vikas Gulani, MD, PhD 1-4*, Fernando Calamante, PhD 5,6,
Complications of nephrogenic systemic fibrosis following repeated exposure to gadolinium in a man with hypothyroidism: a case report
 JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Complications of nephrogenic systemic fibrosis following repeated exposure to gadolinium in a man with hypothyroidism: a case report Arpita Aggarwal
JOURNAL OF MEDICAL CASE REPORTS CASE REPORT Open Access Complications of nephrogenic systemic fibrosis following repeated exposure to gadolinium in a man with hypothyroidism: a case report Arpita Aggarwal
ARTICLE IN PRESS European Journal of Radiology xxx (2011) xxx xxx
 European Journal of Radiology xxx (2011) xxx xxx Contents lists available at ScienceDirect European Journal of Radiology journal homepage: www.elsevier.com/locate/ejrad Tolerability and diagnostic value
European Journal of Radiology xxx (2011) xxx xxx Contents lists available at ScienceDirect European Journal of Radiology journal homepage: www.elsevier.com/locate/ejrad Tolerability and diagnostic value
Figure 1 Figure 1: Energy diagram illustrates formation of a chelate (ML) created by combining two chemicals free Gd 3 (M), which is a metal ion, and
 Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, use the Radiology Reprints form at the end of this article.
Note: This copy is for your personal, non-commercial use only. To order presentation-ready copies for distribution to your colleagues or clients, use the Radiology Reprints form at the end of this article.
Mechanism of NSF: New evidence challenging the prevailing theory
 Thomas Jefferson University Jefferson Digital Commons Scleroderma Center Faculty Papers Scleroderma Center of Thomas Jefferson University 11-2009 Mechanism of NSF: New evidence challenging the prevailing
Thomas Jefferson University Jefferson Digital Commons Scleroderma Center Faculty Papers Scleroderma Center of Thomas Jefferson University 11-2009 Mechanism of NSF: New evidence challenging the prevailing
Contrast media Purpose of using contrast Contrast reaction Nephrotoxicity from contrast Nephrogenic systemic fibrosis When should contrast be used
 Contrast vs Non-Contrast When to Order Stephen McManus, M.D. Contrast media Purpose of using contrast Contrast reaction Nephrotoxicity from contrast Nephrogenic systemic fibrosis When should contrast be
Contrast vs Non-Contrast When to Order Stephen McManus, M.D. Contrast media Purpose of using contrast Contrast reaction Nephrotoxicity from contrast Nephrogenic systemic fibrosis When should contrast be
Gadolinium and nephrogenic systemic fibrosis
 mini review http://www.kidney-international.org & 2007 International Society of Nephrology Gadolinium and nephrogenic systemic fibrosis T Grobner 1 and FC Prischl 2 1 2nd Department of Medicine/Nephrology,
mini review http://www.kidney-international.org & 2007 International Society of Nephrology Gadolinium and nephrogenic systemic fibrosis T Grobner 1 and FC Prischl 2 1 2nd Department of Medicine/Nephrology,
FDA Advisory Committee Briefing Document. Medical Imaging Drugs Advisory Committee. Meeting to be held on February 14, 2013
 FDA Advisory Committee Briefing Document Medical Imaging Drugs Advisory Committee Meeting to be held on February 14, 2013 New Drug Application 204-781 Gadoterate meglumine Injection (Dotarem ), sponsored
FDA Advisory Committee Briefing Document Medical Imaging Drugs Advisory Committee Meeting to be held on February 14, 2013 New Drug Application 204-781 Gadoterate meglumine Injection (Dotarem ), sponsored
Gadolinium in Humans: A Family of Disorders
 Residents Section Clinical Perspective Semelka et al. Gadolinium in Humans Residents Section Clinical Perspective Residents inradiology Richard C. Semelka 1 Miguel Ramalho 1,2 Mamdoh AlObaidy 1,3 Joana
Residents Section Clinical Perspective Semelka et al. Gadolinium in Humans Residents Section Clinical Perspective Residents inradiology Richard C. Semelka 1 Miguel Ramalho 1,2 Mamdoh AlObaidy 1,3 Joana
Nephrology. 2. To facilitate a trainee to acquire the knowledge, clinical skills, procedural competence and professional attributes in Nephrology.
 Nephrology I) OBJECTIVES 1. To provide a broad training and in-depth experience at a level sufficient for trainees to acquire competence and professionalism required of a specialist in Nephrology. 2. To
Nephrology I) OBJECTIVES 1. To provide a broad training and in-depth experience at a level sufficient for trainees to acquire competence and professionalism required of a specialist in Nephrology. 2. To
Clinical guidelines to reduce the risk of contrast induced nephropathy
 Nephrology Subject: Objective: Prepared by: Consultation: Clinical guidelines to reduce the risk of contrast induced nephropathy To implement all possible measures to reduce the risk of nephropathy from
Nephrology Subject: Objective: Prepared by: Consultation: Clinical guidelines to reduce the risk of contrast induced nephropathy To implement all possible measures to reduce the risk of nephropathy from
Renal artery disease: MR Techniques and Interpretation
 Renal artery disease: MR Techniques and Interpretation Prof. Dr. Stefan O. Schoenberg Professor and Chairman of Radiology Department of Clinical Radiology and Nuclear Medicine University Medicine Mannheim
Renal artery disease: MR Techniques and Interpretation Prof. Dr. Stefan O. Schoenberg Professor and Chairman of Radiology Department of Clinical Radiology and Nuclear Medicine University Medicine Mannheim
Outline. Outline. Introduction CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 8/11/2011
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Assessment of physicians awareness levels on nephrogenic systemic fibrosis
 Original research-orijinal araştırma Assessment of physicians awareness levels on nephrogenic systemic fibrosis Klinisyenlerin nefrojenik sistemik fibrozis hakkındaki farkındalık düzeyinin araştırılması
Original research-orijinal araştırma Assessment of physicians awareness levels on nephrogenic systemic fibrosis Klinisyenlerin nefrojenik sistemik fibrozis hakkındaki farkındalık düzeyinin araştırılması
Case # 2 3/27/2017. Disclosure of Relevant Financial Relationships. Clinical history. Clinical history. Laboratory findings
 Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Case # 2 Christopher Larsen, MD Arkana Laboratories Disclosure of Relevant Financial Relationships USCAP requires that all planners (Education Committee) in a position to influence or control the content
Clinical Safety and Diagnostic Value of the Gadolinium Chelate Gadoterate Meglumine (Gd-DOTA)
 ORIGINAL ARTICLE Clinical Safety and Diagnostic Value of the Gadolinium Chelate Gadoterate Meglumine (Gd-DOTA) Christoph U. Herborn, MD,* Elmar Honold, MD, Michael Wolf, Jörn Kemper, MD, Sonja Kinner,
ORIGINAL ARTICLE Clinical Safety and Diagnostic Value of the Gadolinium Chelate Gadoterate Meglumine (Gd-DOTA) Christoph U. Herborn, MD,* Elmar Honold, MD, Michael Wolf, Jörn Kemper, MD, Sonja Kinner,
Elevation of Serum Creatinine: When to Screen, When to Refer. Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC
 Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
Elevation of Serum Creatinine: When to Screen, When to Refer Bruce F. Culleton, MD, FRCPC; and Jolanta Karpinski, MD, FRCPC Presented at the University of Calgary s CME and Professional Development 2006-2007
ORIGINALLY DESIGNATED
 OBSERVATION UV-A1 Therapy for Nephrogenic Systemic Fibrosis Kien T. Tran, MD, PhD; Heidi B. Prather, BS; Clay J. Cockerell, MD; Heidi Jacobe, MD Background: Nephrogenic systemic fibrosis (NSF) is a rare
OBSERVATION UV-A1 Therapy for Nephrogenic Systemic Fibrosis Kien T. Tran, MD, PhD; Heidi B. Prather, BS; Clay J. Cockerell, MD; Heidi Jacobe, MD Background: Nephrogenic systemic fibrosis (NSF) is a rare
THE PROGNOSIS OF PATIENTS WITH CHRONIC KIDNEY DISEASE AND DIABETES MELLITUS
 214 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 21(3):23-212 doi: 1.2478/rjdnmd-214-25 THE PROGNOSIS OF PATIENTS WITH CHRONIC KIDNEY DISEASE AND DIABETES
214 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 21(3):23-212 doi: 1.2478/rjdnmd-214-25 THE PROGNOSIS OF PATIENTS WITH CHRONIC KIDNEY DISEASE AND DIABETES
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care
 SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
SERVICE SPECIFICATION 6 Conservative Management & End of Life Care Table of Contents Page 1 Key Messages 2 2 Introduction & Background 2 3 Relevant Guidelines & Standards 2 4 Scope of Service 3 5 Interdependencies
Outline. Introduction. Outline CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW 6/26/2012
 CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
CHRONIC KIDNEY DISEASE UPDATE: WHAT THE GENERALIST NEEDS TO KNOW MICHAEL G. SHLIPAK, MD, MPH CHIEF-GENERAL INTERNAL MEDICINE, SAN FRANCISCO VA MEDICAL CENTER PROFESSOR OF MEDICINE, EPIDEMIOLOGY AND BIOSTATISTICS,
Poster No.: B-229 Congress: ECR 2011 Scientific Paper. Authors: E. De Kerviler 1, S. Gaillard 2 ; 1 Paris/FR, 2 Villepinte/FR
 Pharmacovigilance based on spontaneous adverse event reporting of meglumine gadoterate (Gd-DOTA) after 15 million administrations and 20 years of clinical use Poster No.: B-229 Congress: ECR 2011 Type:
Pharmacovigilance based on spontaneous adverse event reporting of meglumine gadoterate (Gd-DOTA) after 15 million administrations and 20 years of clinical use Poster No.: B-229 Congress: ECR 2011 Type:
Objectives. Pre-dialysis CKD: The Problem. Pre-dialysis CKD: The Problem. Objectives
 The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
The Role of the Primary Physician and the Nephrologist in the Management of Chronic Kidney Disease () By Brian Young, M.D. Assistant Clinical Professor of Medicine David Geffen School of Medicine at UCLA
Diabetes and renal disease: who does what?
 CLINICAL PRACTICE Clinical Medicine 2013, Vol 13, No 5: 460 4 Diabetes and renal disease: who does what? Ruth K Jones, David Hampton, Daniel J O Sullivan and Aled O Phillips ABSTRACT Care of patients with
CLINICAL PRACTICE Clinical Medicine 2013, Vol 13, No 5: 460 4 Diabetes and renal disease: who does what? Ruth K Jones, David Hampton, Daniel J O Sullivan and Aled O Phillips ABSTRACT Care of patients with
1Pulse sequences for non CE MRA
 MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
MRI: Principles and Applications, Friday, 8.30 9.20 am Pulse sequences for non CE MRA S. I. Gonçalves, PhD Radiology Department University Hospital Coimbra Autumn Semester, 2011 1 Magnetic resonance angiography
The Health Problem: Guidelines: NHS Priority:
 PRIORITY BRIEFING The purpose of this briefing paper is to aid Stakeholders in prioritising topics to be taken further by PenCLAHRC as the basis for a specific evaluation or implementation research project.
PRIORITY BRIEFING The purpose of this briefing paper is to aid Stakeholders in prioritising topics to be taken further by PenCLAHRC as the basis for a specific evaluation or implementation research project.
Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York
 Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York 4th International Conference on Nephrology & Therapeutics September 14, 2015 Baltimore,
Narender Goel et al. Middletown Medical PC, Montefiore Medical Center & Albert Einstein College of Medicine, New York 4th International Conference on Nephrology & Therapeutics September 14, 2015 Baltimore,
THE ADVANCED CHRONIC KIDNEY DISEASE MANAGEMENT TOOLKIT
 THE ADVANCED CHRONIC KIDNEY DISEASE MANAGEMENT TOOLKIT Approximately 20 million Americans have some degree of kidney disease 1 demonstrated by decreased glomerular filtration rate (GFR) (
THE ADVANCED CHRONIC KIDNEY DISEASE MANAGEMENT TOOLKIT Approximately 20 million Americans have some degree of kidney disease 1 demonstrated by decreased glomerular filtration rate (GFR) (
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Diagnostics Assessment Programme
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Diagnostics Assessment Programme Point-of-care creatinine tests to assess kidney function before administering intravenous contrast for computed tomography
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Diagnostics Assessment Programme Point-of-care creatinine tests to assess kidney function before administering intravenous contrast for computed tomography
Chapter 9 A 65-Year-Old Woman with Hardened Skin, Joint Contractures, and Yellow Scleral Plaques
 Chapter 9 A 65-Year-Old Woman with Hardened Skin, Joint Contractures, and Yellow Scleral Plaques Jonathan Kay Keywords Nephrogenic systemic fibrosis Chronic kidney disease Contrast media Gadolinium Gadolinium
Chapter 9 A 65-Year-Old Woman with Hardened Skin, Joint Contractures, and Yellow Scleral Plaques Jonathan Kay Keywords Nephrogenic systemic fibrosis Chronic kidney disease Contrast media Gadolinium Gadolinium
Department of Vascular Surgery, Maastricht University, Maastricht - The Netherlands 2
 The Journal of Vascular Access 2007; 8: 281-286 ORIGINAL ARTICLE Accessory veins and radial-cephalic arteriovenous fistula non-maturation: a prospective analysis using contrast-enhanced magnetic resonance
The Journal of Vascular Access 2007; 8: 281-286 ORIGINAL ARTICLE Accessory veins and radial-cephalic arteriovenous fistula non-maturation: a prospective analysis using contrast-enhanced magnetic resonance
Safety of Gadoterate Meglumine (Gd-DOTA) as a Contrast Agent for Magnetic Resonance Imaging
 ORIGINAL RESEARCH ARTICLE Drugs R D 2010; 10 (3): 133-145 1179-6901/10/0003-0133 ª 2010 Ishiguchi & Takahashi, publisher and licensee Adis Data Information BV. This is an open access article published
ORIGINAL RESEARCH ARTICLE Drugs R D 2010; 10 (3): 133-145 1179-6901/10/0003-0133 ª 2010 Ishiguchi & Takahashi, publisher and licensee Adis Data Information BV. This is an open access article published
Available online at Nanomedicine: Nanotechnology, Biology, and Medicine 6 (2010) 1 8. Feature Article
 Available online at www.sciencedirect.com Nanomedicine: Nanotechnology, Biology, and Medicine 6 (2010) 1 8 Feature Article Novel sorbents for removal of gadolinium-based contrast agents in sorbent dialysis
Available online at www.sciencedirect.com Nanomedicine: Nanotechnology, Biology, and Medicine 6 (2010) 1 8 Feature Article Novel sorbents for removal of gadolinium-based contrast agents in sorbent dialysis
Concept and General Objectives of the Conference: Prognosis Matters. Andrew S. Levey, MD Tufts Medical Center Boston, MA
 Concept and General Objectives of the Conference: Prognosis Matters Andrew S. Levey, MD Tufts Medical Center Boston, MA General Objectives Topics to discuss What are the key outcomes of CKD? What progress
Concept and General Objectives of the Conference: Prognosis Matters Andrew S. Levey, MD Tufts Medical Center Boston, MA General Objectives Topics to discuss What are the key outcomes of CKD? What progress
The CARI Guidelines Caring for Australasians with Renal Impairment. Uric acid GUIDELINES. No recommendations possible based on Level I or II evidence.
 Date written: July 2004 Final submission: July 2004 Author: David Johnson Uric acid GUIDELINES No recommendations possible based on Level I or II evidence. SUGGESTIONS FOR CLINICAL CARE (Suggestions are
Date written: July 2004 Final submission: July 2004 Author: David Johnson Uric acid GUIDELINES No recommendations possible based on Level I or II evidence. SUGGESTIONS FOR CLINICAL CARE (Suggestions are
Report on the Investigation Results
 This English version is intended to be a reference material for the convenience of users. In the event of inconsistency between the Japanese original and this English translation, the former shall Report
This English version is intended to be a reference material for the convenience of users. In the event of inconsistency between the Japanese original and this English translation, the former shall Report
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE SCOPE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic kidney disease: early identification and management of adults with chronic kidney disease in primary and secondary
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE 1 Guideline title SCOPE Chronic kidney disease: early identification and management of adults with chronic kidney disease in primary and secondary
Minimizing Risk of Nephrogenic systemic fibrosis in Cardiovascular Magnetic Resonance
 Reiter et al. Journal of Cardiovascular Magnetic Resonance 2012, 14:31 REVIEW Open Access Minimizing Risk of Nephrogenic systemic fibrosis in Cardiovascular Magnetic Resonance Theresa Reiter 1*, Oliver
Reiter et al. Journal of Cardiovascular Magnetic Resonance 2012, 14:31 REVIEW Open Access Minimizing Risk of Nephrogenic systemic fibrosis in Cardiovascular Magnetic Resonance Theresa Reiter 1*, Oliver
ACR Appropriateness Criteria Suspected Lower Extremity Deep Vein Thrombosis EVIDENCE TABLE
 . Fowkes FJ, Price JF, Fowkes FG. Incidence of diagnosed deep vein thrombosis in the general population: systematic review. Eur J Vasc Endovasc Surg 003; 5():-5.. Hamper UM, DeJong MR, Scoutt LM. Ultrasound
. Fowkes FJ, Price JF, Fowkes FG. Incidence of diagnosed deep vein thrombosis in the general population: systematic review. Eur J Vasc Endovasc Surg 003; 5():-5.. Hamper UM, DeJong MR, Scoutt LM. Ultrasound
Perfusion, Viability, Edema and Hemorrhage: How it Can (and Should) Change Clinical Practice. Rohan Dharmakumar, Ph.D.
 Perfusion, Viability, Edema and Hemorrhage: How it Can (and Should) Change Clinical Practice Rohan Dharmakumar, Ph.D. Director, Translational Cardiac Imaging Research Associate Director, Biomedical Imaging
Perfusion, Viability, Edema and Hemorrhage: How it Can (and Should) Change Clinical Practice Rohan Dharmakumar, Ph.D. Director, Translational Cardiac Imaging Research Associate Director, Biomedical Imaging
Prof. Andrzej Wiecek Department of Nephrology, Endocrinology and Metabolic Diseases Medical University of Silesia Katowice, Poland.
 What could be the role of renal denervation in chronic kidney disease? Andrzej Wiecek, Katowice, Poland Chairs: Peter J. Blankestijn, Utrecht, The Netherlands Jonathan Moss, Glasgow, UK Prof. Andrzej Wiecek
What could be the role of renal denervation in chronic kidney disease? Andrzej Wiecek, Katowice, Poland Chairs: Peter J. Blankestijn, Utrecht, The Netherlands Jonathan Moss, Glasgow, UK Prof. Andrzej Wiecek
Revascularization versus Medical Therapy for Renal-Artery Stenosis
 The new england journal of medicine original article versus Medical Therapy for Renal-Artery Stenosis The ASTRAL Investigators* Abstract Background Percutaneous revascularization of the renal arteries
The new england journal of medicine original article versus Medical Therapy for Renal-Artery Stenosis The ASTRAL Investigators* Abstract Background Percutaneous revascularization of the renal arteries
THE KIDNEY AND SLE LUPUS NEPHRITIS
 THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
THE KIDNEY AND SLE LUPUS NEPHRITIS JACK WATERMAN DO FACOI 2013 NEPHROLOGY SIR RICHARD BRIGHT TERMINOLOGY RENAL INSUFFICIENCY CKD (CHRONIC KIDNEY DISEASE) ESRD (ENDSTAGE RENAL DISEASE) GLOMERULONEPHRITIS
CLINICAL IMAGING. When Should Abdominal Magnetic Resonance Imaging Be Used? Patient Safety and Diagnostic Accuracy
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:610 615 CLINICAL IMAGING When Should Abdominal Magnetic Resonance Imaging Be Used? JOSÉ A. GONÇALVES NETO, MOHAMED ELAZZAZZI, ERSAN ALTUN, and RICHARD C.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:610 615 CLINICAL IMAGING When Should Abdominal Magnetic Resonance Imaging Be Used? JOSÉ A. GONÇALVES NETO, MOHAMED ELAZZAZZI, ERSAN ALTUN, and RICHARD C.
Chronic renal disease in the elderly: are all pigs to be considered equal?
 Chronic renal disease in the elderly: are all pigs to be considered equal? W. Van Biesen, Ghent University Hospital Elwood et al, cjasn, 2013 Elderly and CKD: a thematic synthesis Overview CKD in the
Chronic renal disease in the elderly: are all pigs to be considered equal? W. Van Biesen, Ghent University Hospital Elwood et al, cjasn, 2013 Elderly and CKD: a thematic synthesis Overview CKD in the
Primary Care Approach to Management of CKD
 Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Primary Care Approach to Management of CKD This PowerPoint was developed through a collaboration between the National Kidney Foundation and ASCP. Copyright 2018 National Kidney Foundation and ASCP Low
Safety and clinical usefulness of gadoteric acid including post-marketing surveillance
 Safety and clinical usefulness of gadoteric acid including post-marketing surveillance MRI is an essential diagnostic tool in making definite diagnoses and determining therapeutic strategies. Extracellular
Safety and clinical usefulness of gadoteric acid including post-marketing surveillance MRI is an essential diagnostic tool in making definite diagnoses and determining therapeutic strategies. Extracellular
