NTI 2010 Boot Camp. Paradigm Shift. Hemodynamics: Cardiac Output. Basic Hemodynamic Formula
|
|
|
- Melvin Bradley
- 6 years ago
- Views:
Transcription
1 Cardiovascular Assessment and Hemodynamic Principles NTI 2010 Boot Camp Hemodynamics does not equal invasive monitoring Paradigm Shift Karen Marzlin MSN, RN, CCNS, CCRN-CMC Cardiovascular Nursing Education Associates Circulation: Heart Arteries Veins Blood Volume 3 4 Hemodynamics: Cardiac Output Understanding basic hemodynamic principles and their impact on the forward propulsion of blood. Basic Hemodynamic Formula Cardiac Output Heart Rate X Stroke Volume Preload Afterload Contractility Stroke Volume: Volume of blood ejected with each beat ml/beat 5 6 Associates 1
2 Cardiac Output Right Sided vs. Left Side System Volume of blood ejected by the ventricle each minute Measures effectiveness of the heart as a pump Other terms: Stroke Volume: Volume of blood ejected with each beat. Normal: ml/beat Ejection Fraction: Percent of blood ejected from the ventricle Normal: 55%-60% 7 8 Preload Right and Left Sided Preload End-diastolic stretch on myocardial muscles fibers Determined by: Volume of blood filling the ventricle at end of diastole Greater the volume the greater the stretch (muscle fiber length) Greater the stretch the greater the contraction Greater the contraction the greater cardiac output TO A POINT Right Preload Measured by right atrial pressure (RAP) or central venous pressure (CVP) Noninvasive assessment JVD Hepatojugular reflux Peripheral edema * Weight* Left Preload Measured by the pulmonary artery occlusive pressure (PAOP) Noninvasive Assessment Lungs sounds Lymph drainage Blood pressure** Urine output / BUN/Creatinine Ratio** Weight* 9 10 Factors Influencing Preload Body Position Venous Tone Intrathoracic pressure Intrapericardial pressure Atrial Kick LV Function Circulating blood volume Hypervolemia Hypovolemia Third spacing Distribution of blood volume Sepsis Anaphylaxis Venous vasodilators Key Points about Preload Preload may need to be continuously balanced in cardiac patients Changes in pressure do not always = the same changes in volume Dilated versus noncompliant ventricle Heart failure does not mean congestion Right and left sided preload are closely related. Left heart preload is dependent on the right heart Associates 2
3 Afterload Afterload Pressure ventricle needs to overcome to eject blood volume Blood pressure is major component of afterload but it does not equal afterload Blood Pressure = Cardiac Output x Systemic Vascular Resistance (Afterload) Other components Valve compliance Viscosity of blood Arterial wall compliance Aortic compliance Right ventricular afterload Measured by pulmonary vascular resistance (PVR) Normal: dynes/sec/cm -5 Left ventricular afterload Measured by systemic vascular resistance (SVR) Normal dynes/sec/cm -5 Diastolic BP is closest noninvasive measurement (narrow pulse pressure) Causes of Increased LV Afterload Arterial vasoconstrictors Hypertension Aortic valve stenosis Increased blood viscosity Hypothermia Compensatory vasoconstriction from hypotension in shock Causes of Decreased LV Afterload Arterial vasodilators Hyperthermia Vasogenic shock states (sepsis and anaphylactic) where the body cannot compensate with vasoconstriction Aortic Regurgitation hyperdynamic cardiac output therefore lowering systemic vascular resistance 15 Increased Right Sided Afterload Pulmonary hypertension mpap > 25 mmhg or > 30 mmhg with exercise PVR > 250 dynes/sec/cm -5 Causes Hypoxemia Acidosis Inflammation Hypothermia Excess sympathetic stimulation Pulmonary endothelial dysfunction Impaired nitric oxide and prostacyclin (PGI2) release Primary pulmonary hypertension 16 Contractility Ability of myocardium to contract independent of preload or afterload Velocity and extent of myocardial fiber shortening Inotropic state Noninvasive Assessment: Ejection Fraction Contractility Related to degree of myocardial fiber stretch (preload) and wall tension (afterload). Influences myocardial oxygen consumption contractility myocardial workload myocardial oxygen consumption Associates 3
4 Contractility Measured on right by right ventricular stroke work index (5-12g-m/m 2 ) Measured on left by left ventricular stroke work index (45-65g-m/m 2 ) No ability to directly measure contractility. 19 Factors Altering Contractility Decreased contractility Excessive preload or afterload Drugs negative inotropes Myocardial damage Ischemia Cardiomyopathy Hypothyroidism Changes in ionic environment:hypoxia, acidosis or electrolyte imbalance Increased contractility Drugs Positive inotropes Hyperthyroidism Adrenal Medulla Tumor 20 Contractility Heart Rate Low cardiac output does not necessarily mean diminished contractility Correct preload and afterload problems first Inotropic Medication Sympathomimetics PDE Inhibitors Cardiac Glycosides Medications which increase contractility impact not only cardiac output but also myocardial oxygen demand. Mathematically heart rate increases cardiac output Physiological limit where increased heart rate will decrease cardiac output due to decreased filling time (decreased preload) Consider as first line strategy to increase cardiac output when temporary pacemaker in place Left Ventricular Function Curves Left Ventricular Function: Preload B A Associates 4
5 Left Ventricular Function: Contractility Left Ventricular Function: Afterload B B A A The Goal: Tissue Oxygenation Delivery of oxygen to the tissues is a function of cardiac output (or cardiac index) x arterial oxygen content Arterial oxygen content is impacted based on hemoglobin and arterial oxygenation saturation Delivery of oxygen = C.O. x Hgb X SaO 2 Poor oxygenation delivery can be improved by improving any of the above 3 parameters. Oxygen Delivery Always assess hemoglobin and oxygenation saturation in conjunction with cardiac performance Hypoxemia Ventilation Abnormalities PaCO 2 Rate and tidal volume Diffusion Barriers PaO2 and SaO 2 Oxygen and PEEP Oxygen Demand Critical illness can cause an increase in oxygen demand Surgery Pain Anxiety Infection Cellular Hypoxia Imbalance of supply and demand Cells unable to extract oxygen Result: Oxygen debt and anaerobic metabolism; eventual organ dysfunction Assessment: serum ph, lactate levels Associates 5
6 Other Factors Impacting Tissue Oxygenation Relationship between oxygen and hemoglobin (affinity) for proper uptake and unloading Temperature Hyperthermia Hypothermia ph Acidosis Alkalosis New StO 2 monitoring. Auscultatory Areas Utilization of Oxygenation By the Cells Cardiac Diastole (Atrial and Ventricular): Early Passive Filling Atrial Systole & Ventricular Diastole: Late Active Filling 33 Atrial Kick 34 Beginning Ventricular Systole: Isovolumic Contraction Ventricular Systole: Ejection Associates 6
7 FIRST HEART SOUND Basic Heart Sounds S 1 Closure of the Mitral (M 1 ) valve and the Tricuspid (T 1 )valve Beginning of Ventricular Systole and Atrial Diastole Isovolumic contraction Basic Heart Sounds S 1 Location: Mitral area at the hearts apex Intensity: Directly related to force of contraction Duration: Short Quality: Dull SECOND HEART SOUND Basic Heart Sounds S 2 Closure of Aortic (A 2 ) Valve and Pulmonic (P 2 ) Valve End of Ventricular Systole Beginning of Ventricular Diastole Basic Heart Sounds S 2 Location: Pulmonic area Intensity: Directly related to closing pressure in the aorta and pulmonary artery Duration: Shorter than S 1 Quality: Booming Associates 7
8 Third and Fourth Heart Sounds S 3 and S 4 Ventricular diastolic filling sounds Low frequency sounds Produced by ventricular filling rather than valve closure Normal in children and young adults THIRD HEART SOUND S 3 Ventricular Gallop Ventricular Gallop Early diastole Caused by increased diastolic pressure Left or Right Sided S 3 Left lateral position Location: Left Sided Mitral area Right Sided Tricuspid area Intensity: Left Sided Heard Best during expiration Right Sided Heard Best during inspiration Duration: Short Quality: dull, thudlike Pitch: Low S 4 Atrial Gallop S 4 Atrial Gallop Late diastole Caused by atrial contraction and the propulsion of blood into a noncompliant ventricle Associates 8
9 Left or Right Sided S 4 Left Lateral position Location: Left Sided Mitral Area Right Sided Tricuspid area Intensity: Left Sided Louder on expiration Right Sided Louder on inspiration Duration: Short Quality: Thudlike Pitch: Low Summation Gallop Combination of S3 and S MURMURS Murmur Fundamentals Turbulence Murmur: If turbulence is intracardiac Bruit: If turbulence is extracardiac Murmur Fundamentals Causes of Turbulence Forward flow through a stenotic valve Murmur Fundamentals Causes of Turbulence Flow through a septal defect or an AV fistula Backward flow through an incompetent valve Flow into a dilated chamber or a portion of a vessel Associates 9
10 Murmur Fundamentals Murmur Fundamentals Stenotic Murmurs Valve does not open appropriately Heard during the part of the cardiac cycle when the valve is open Regurgitant Murmurs Valve does not close appropriately Heard during the part of the cardiac cycle when the valve is to be closed Timing Systolic Holosystolic Ejection (midsystolic) Late Diastolic Early Middiastolic Late Location Place heard the loudest Radiation Direction in which murmur radiates Murmur Fundamentals Systolic Murmurs Configuration Crescendo Gets louder Decrescendo Gets softer Crescendo Decrescendo Louder then softer Plateau Even intensity throughout Pitch High Pitched - diaphragm Low Pitched bell Quality Soft Harsh Blowing Musical Rumbling Rough Tricuspid and Mitral Valve Closed Tricuspid Regurgitation Mitral Regurgitation Pulmonic and Aortic Valve Open Pulmonic Stenosis Aortic Stenosis Aortic Stenosis Systolic Ejection Murmur Timing: Midsystolic Location: Best heard over aortic area Radiation: Toward right side of neck Crescendo-decrescendo Pitch: Medium to high Quality: Harsh Pulmonic Stenosis Systolic Ejection Murmur Timing: Midsystolic Location: Best heard over pulmonic area Radiation: Left neck of left shoulder Crescendo-decrescendo Pitch: Medium Quality: Harsh Associates 10
11 Systolic Murmurs Mitral Regurgitation Timing: Holosystolic Location: Mitral area Radiation: To the left axilla Plateau Quality: Blowing, harsh or musical Systolic Murmurs Tricuspid Regurgitation Timing: Holosystolic Location: Tricuspid area Radiation: To the right of sternum Plateau Quality: Scratchy or blowing Diastolic Murmurs Diastolic regurgitant murmurs Retrograde flow across an incompetent semilunar valve Diastolic filling murmurs Forward flow across stenotic or obstructed AV valves Diastolic Murmurs Tricuspid and Mitral Valves Open Tricuspid Stenosis Mitral Stenosis Pulmonic and Aortic Valves Close Pulmonic Regurgitation Aortic Regurgitation Diastolic Murmurs Aortic Regurgitation Timing: Early diastole Location: Aortic area Radiation: Toward apex Decrescendo Quality: Blowing Diastolic Murmurs Pulmonic Regurgitation Timing: Early diastole Location: Pulmonic area Erb s Point Radiation: Toward apex Decrescendo Quality: Blowing Associates 11
12 Diastolic Murmurs Mitral Stenosis Diastolic Murmur Tricuspid Stenosis Timing: Mid to Late diastole Location: Mitral area Radiation: None Crescendo Pitch: Low Quality: Rumbling 67 Timing: Mid to Late diastole Location: Tricuspid area Radiation: None Decrescendo Pitch: Low Quality: Rumbling Increases during inspiration and decreases during expiration 68 Other Sounds Pericardial Friction Rub Timing: Systolic, Early diastolic and late diastolic Location: Tricuspid area and Xyphoid area Radiation: None Plateau May get louder during inspiration Quality: Grating, scratching Other Sounds Ventricular Septal Defect or Rupture Timing: Continuous Location: 3-4 LSB Radiation: Widely throughout the precordium Plateau Quality: Harsh Other Sounds REMEMBER: Papillary Muscle Rupture Same as Mitral Regurgitation The most important part of the stethoscope is the part between the ear pieces Associates 12
13 JVP (Jugular Venous Pressure) Other Assessment Tools Reflects volume and pressure in right side of heart Visual inspection HOB degree angle 45 degree angle will cause venous pulsation to rise 1 to 3 cm above the manubrium Measuring JVD Raise HOB until pulsation in internal jugular seen (usually degrees) Use targeted light Use centimeter ruler Measure distance from angle of Louis (Manubriosternal joint) to top column of blood Draw imaginary horizontal line from column to sternal angle JVD (Jugular Venous Distension) Normal JVD level is 3 cm above the sternal angle Sternal angle is 5cm above right atrium JVD of 3 cm + 5cm = estimated CVP of 8cm Estimated CVP> 8 cm Increased blood volume Usually RV failure Tricuspid valve regurgitation Pulmonary hypertension Tips to Take Away for JVD Assessment If unable to accurately assess Lie patient flat to visualize and then raise HOB If venous congestion is expected may need to sit or stand patient to see top of column No Low Perfusion CI 2.2 at Rest Profiles of Perfusion and Congestion Yes Congestion at Rest No Yes Warm and Dry Warm and Wet No congestion Congestion No hypoperfusion No hypoperfusion Cold and Dry No congestion Hypoperfusion PWP 18 Cold and Wet Congestion Hypoperfusion Associates 13
14 Cardiac Assessment Arterial vs. Venous Disease Edema Evaluated on a 4-point scale. 0 = None present. 1+ = 0 to 1 4 inch Trace. 2+ = 1 4 to 1 2 inch Mild. 3+ = 1 2 to 1 inch Moderate. 4+ = > than 1 inch Severe. Described as pitting or non-pitting. Anasarca: generalized edema Pulses 4 point scale (0-3) 0 = absent 1+ = Palpable but thready and weak, easily obliterated 2+ = Normal, easily identified, not easily obliterated 3+ = Full, bounding, cannot obliterate Central Cyanosis Occurs when more than 5 grams/dl of hemoglobin is deoxygenated Results in a bluish or steel-gray discoloration of the skin and mucous membranes Bluish or steel-gray discoloration of the lips can be from central or peripheral cyanosis Oral mucosa or the tongue may be better tools for assessment of central cyanosis Usually not seen until oxygen saturation drops to between 73% to 78% Absence of cyanosis does not exclude hypoxemia Peripheral Cyanosis Caused by peripheral vasoconstriction and decreased local blood flow May occur with or without central cyanosis (i.e., with or without hypoxemia) Usually observed in the nailbeds of the hands or feet, the earlobes or nose Should improve with warming 83 Pulsus Paradoxus To measure the pulsus paradoxus, patients are often placed in a semirecumbent position; respirations should be normal. The blood pressure cuff is inflated to at least 20 mm Hg above the systolic pressure and slowly deflated until the first Korotkoff sounds are heard only during expiration. At this pressure reading, if the cuff is not further deflated and a pulsus paradoxus is present, the first Korotkoff sound is not audible during inspiration. As the cuff is further deflated, the point at which the first Korotkoff sound is audible during both inspiration and expiration is recorded. If the difference between the first and second measurement is greater than 12 mm Hg, an abnormal pulsus paradoxus is present. (Yarlagadda, Chakri, 2005 Cardiac Tamponade. Retrieved from 84 Associates 14
15 Blood Pressure Definitions: BP = CO X SVR Systolic: Maximum pressure when blood is expelled from the left ventricle Diastolic:Measures rate of flow of ejected blood and vessel elasticity Pulse Pressure: Difference between systolic and diastolic pressure Clinical Significance Blood Pressure Control Rapid adjustments in BP are controlled by baroreceptor reflexes Baroreceptor reflex is sluggish with orthostatic hypotension Additional mechanisms for blood pressure control Nerve fibers: limbic system and hypothalamus (emotionally triggered) Neural input from midbrain (pain) Chemoreceptors: Hypercapnia and hypoxia Calcium: Vascular tone and contractility Renin angiotensin aldosterone system (RAAS) Vasopressin (Antidiuretic hormone) Endothelial response Etiology of Hypotension Blood pressure does not equal blood flow. BP 88/72 CO SVR BP CO SVR 82/ Gratitude 89 Associates 15
Cardiovascular Boot Camp April 2009
 Advanced Cardiac Dynamics Presented by: Karen Marzlin BSN, RN, CCRN-CMC CNEA 2009 1 Hemodynamics does not equal invasive monitoring Paradigm Shift 2 www.cardionursing.com 1 3 Circulation: Heart Arteries
Advanced Cardiac Dynamics Presented by: Karen Marzlin BSN, RN, CCRN-CMC CNEA 2009 1 Hemodynamics does not equal invasive monitoring Paradigm Shift 2 www.cardionursing.com 1 3 Circulation: Heart Arteries
Heart sounds and murmurs. Dr. Szathmári Miklós Semmelweis University First Department of Medicine 15. Oct
 Heart sounds and murmurs Dr. Szathmári Miklós Semmelweis University First Department of Medicine 15. Oct. 2013. Conditions for auscultation of the heart Quiet room Patient comfortable Chest fully exposed
Heart sounds and murmurs Dr. Szathmári Miklós Semmelweis University First Department of Medicine 15. Oct. 2013. Conditions for auscultation of the heart Quiet room Patient comfortable Chest fully exposed
Hemodynamic Monitoring
 Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Perform Procedure And Interpret Results Hemodynamic Monitoring Tracheal Tube Cuff Pressure Dean R. Hess PhD RRT FAARC Hemodynamic Monitoring Cardiac Rate and Rhythm Arterial Blood Pressure Central Venous
Topics to be Covered. Cardiac Measurements. Distribution of Blood Volume. Distribution of Pulmonary Ventilation & Blood Flow
 Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
Topics to be Covered MODULE F HEMODYNAMIC MONITORING Cardiac Output Determinants of Stroke Volume Hemodynamic Measurements Pulmonary Artery Catheterization Control of Blood Pressure Heart Failure Cardiac
CARDIAC EXAMINATION MINI-QUIZ
 CARDIAC EXAMINATION MINI-QUIZ 1. Sitting bolt upright, your dyspneic (short of breath) patient has visible jugular venous pulsations to the angle of his jaw, which is 12 cm above his sternal angle. What
CARDIAC EXAMINATION MINI-QUIZ 1. Sitting bolt upright, your dyspneic (short of breath) patient has visible jugular venous pulsations to the angle of his jaw, which is 12 cm above his sternal angle. What
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Cardiac Cycle MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Cardiac Cycle MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 1- Regarding the length of systole and diastole: a- At heart rate 75 b/min, the duration of
Cardiac Ausculation in the Elderly
 Cardiac Ausculation in the Elderly 박성하 신촌세브란스병원심장혈관병원심장내과 Anatomy Surface projection of the Heart and Great Vessels Evaluating pulsation Superior vena cava Rt. pulmonary artery Right atrium Right ventricle
Cardiac Ausculation in the Elderly 박성하 신촌세브란스병원심장혈관병원심장내과 Anatomy Surface projection of the Heart and Great Vessels Evaluating pulsation Superior vena cava Rt. pulmonary artery Right atrium Right ventricle
Murmur Sounds made by turbulence in the heart or blood stream. 1. Timing. 5. Intensity 2. Shape. 6. Pitch 3. Location of maximum intensity
 Definition Items in description of Timing Shape Location of maximum intensity Murmur Sounds made by turbulence in the heart or blood stream. 1. Timing 5. Intensity 2. Shape 6. Pitch 3. Location of maximum
Definition Items in description of Timing Shape Location of maximum intensity Murmur Sounds made by turbulence in the heart or blood stream. 1. Timing 5. Intensity 2. Shape 6. Pitch 3. Location of maximum
Introduction. Invasive Hemodynamic Monitoring. Determinants of Cardiovascular Function. Cardiovascular System. Hemodynamic Monitoring
 Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
Introduction Invasive Hemodynamic Monitoring Audis Bethea, Pharm.D. Assistant Professor Therapeutics IV January 21, 2004 Hemodynamic monitoring is necessary to assess and manage shock Information obtained
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
2. The heart sounds are produced by a summed series of mechanical events, as follows:
 Heart Sounds. Phonocardiography 1 Objectives 1. Phonocardiography - Definition 2. What produces the heart sounds 3. Where to listen for the heart sounds 4. How to record a phonocardiogram 5. Normal heart
Heart Sounds. Phonocardiography 1 Objectives 1. Phonocardiography - Definition 2. What produces the heart sounds 3. Where to listen for the heart sounds 4. How to record a phonocardiogram 5. Normal heart
HISTORY. Question: What category of heart disease is suggested by this history? CHIEF COMPLAINT: Heart murmur present since early infancy.
 HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
HISTORY 18-year-old man. CHIEF COMPLAINT: Heart murmur present since early infancy. PRESENT ILLNESS: Although normal at birth, a heart murmur was heard at the six week check-up and has persisted since
Cardiovascular System
 Cardiovascular System Chapter 8 1 Cardiovascular System Functions: pump saturated oxygenated blood into arterial system cells pump desaturated deoxygenated blood to lungs via veins for reoxygenation Heart
Cardiovascular System Chapter 8 1 Cardiovascular System Functions: pump saturated oxygenated blood into arterial system cells pump desaturated deoxygenated blood to lungs via veins for reoxygenation Heart
FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART
 FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART CINDY BITHER, MSN, ANP, ANP, AACC, CHFN CHIEF NP, ADV HF PROGRAM MEDSTAR WASHINGTON HOSPITAL CENTER CONFLICTS OF INTEREST NONE
FUNDAMENTALS OF HEMODYNAMICS, VASOACTIVE DRUGS AND IABP IN THE FAILING HEART CINDY BITHER, MSN, ANP, ANP, AACC, CHFN CHIEF NP, ADV HF PROGRAM MEDSTAR WASHINGTON HOSPITAL CENTER CONFLICTS OF INTEREST NONE
CARDIOVASCULAR PHYSIOLOGY
 CARDIOVASCULAR PHYSIOLOGY LECTURE 4 Cardiac cycle Polygram - analysis of cardiac activity Ana-Maria Zagrean MD, PhD The Cardiac Cycle - definitions: the sequence of electrical and mechanical events that
CARDIOVASCULAR PHYSIOLOGY LECTURE 4 Cardiac cycle Polygram - analysis of cardiac activity Ana-Maria Zagrean MD, PhD The Cardiac Cycle - definitions: the sequence of electrical and mechanical events that
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Relax and Learn At the Farm Session 9: Invasive Hemodynamic Assessment and What to Do with the Data Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Function of CV system is to deliver
Cardiac Examination. Pediatrics Clinical Examination
 Pediatrics Clinical Examination Symptoms of Cardiovascular Affection: Cardiac Examination 1. Perinatal history: Maternal DM, cyanosis, respiratory distress 2. Symptoms of lung congestion: Poor interrupted
Pediatrics Clinical Examination Symptoms of Cardiovascular Affection: Cardiac Examination 1. Perinatal history: Maternal DM, cyanosis, respiratory distress 2. Symptoms of lung congestion: Poor interrupted
Cardiovascular Physiology. Heart Physiology. Introduction. The heart. Electrophysiology of the heart
 Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
Cardiovascular Physiology Heart Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through
COLIC AND MURMURS: AN OVERVIEW
 COLIC AND MURMURS: AN OVERVIEW Gunther van Loon, DVM, PhD, Department of Large Animal Internal Medicine, Ghent University, Merelbeke, Belgium Introduction Many horses with colic present with a cardiac
COLIC AND MURMURS: AN OVERVIEW Gunther van Loon, DVM, PhD, Department of Large Animal Internal Medicine, Ghent University, Merelbeke, Belgium Introduction Many horses with colic present with a cardiac
Principles of Biomedical Systems & Devices. Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont
 Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
Principles of Biomedical Systems & Devices Lecture 8: Cardiovascular Dynamics Dr. Maria Tahamont Review of Cardiac Anatomy Four chambers Two atria-receive blood from the vena cave and pulmonary veins Two
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
IP: Regulation of Cardiac Output
 ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
ANP 1105D Winter 2013 Assignment 9: The Heart, part 2: Chap... Assignment 9: The Heart, part 2: Chapter 18 Signed in as Alex Sokolowski Help Close Resources Due: 11:59pm on Monday, March 25, 2013 Note:
Congestive Heart Failure Patient Profile. Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption
 Congestive Heart Failure Patient Profile Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption Chief Complaint - SOB - When asked: Increasing difficulty
Congestive Heart Failure Patient Profile Patient Identity - Mr. Douglas - 72 year old man - No drugs, smokes, moderate social alcohol consumption Chief Complaint - SOB - When asked: Increasing difficulty
Chapter 9, Part 2. Cardiocirculatory Adjustments to Exercise
 Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Chapter 9, Part 2 Cardiocirculatory Adjustments to Exercise Electrical Activity of the Heart Contraction of the heart depends on electrical stimulation of the myocardium Impulse is initiated in the right
Heart and Neck Vessels
 CHAPTER 12 Heart and Neck Vessels ANATOMY The precordium is the area on the anterior chest overlying the heart and great vessels. The heart extends from the second to the fifth intercostal space, and from
CHAPTER 12 Heart and Neck Vessels ANATOMY The precordium is the area on the anterior chest overlying the heart and great vessels. The heart extends from the second to the fifth intercostal space, and from
1. how a careful cardiovascular evaluation can accurately assess pathology and physiology at the bedside, and
 This program will demonstrate: 1. how a careful cardiovascular evaluation can accurately assess pathology and physiology at the bedside, and 2. the importance of integrating this information with selected
This program will demonstrate: 1. how a careful cardiovascular evaluation can accurately assess pathology and physiology at the bedside, and 2. the importance of integrating this information with selected
Review of Cardiac Mechanics & Pharmacology 10/23/2016. Brent Dunworth, CRNA, MSN, MBA 1. Learning Objectives
 Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
Brent Dunworth, CRNA, MSN, MBA Associate Director of Advanced Practice Division Chief, Nurse Anesthesia Vanderbilt University Medical Center Nashville, Tennessee Learning Objectives Review the principles
Physical Exam Of The Cardio- Vascular System. James G. Laws D.O. MACOI
 Physical Exam Of The Cardio- Vascular System James G. Laws D.O. MACOI An Important Part Of The Physical Exam Of The Cardio-Vascular System That Is Commonly Overlooked Is? 20% 20% 20% 20% 20% 1. Palpation
Physical Exam Of The Cardio- Vascular System James G. Laws D.O. MACOI An Important Part Of The Physical Exam Of The Cardio-Vascular System That Is Commonly Overlooked Is? 20% 20% 20% 20% 20% 1. Palpation
Case year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50
 Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Case 1 65 year old female nursing home resident with a hx CAD, PUD, recent hip fracture Transferred to ED with decreased mental status BP in ED 80/50 Case 1 65 year old female nursing home resident with
Clinical significance of cardiac murmurs: Get the sound and rhythm!
 Clinical significance of cardiac murmurs: Get the sound and rhythm! Prof. dr. Gunther van Loon, DVM, PhD, Ass Member ECVDI, Dip ECEIM Dept. of Large Animal Internal Medicine Ghent University, Belgium Murmurs
Clinical significance of cardiac murmurs: Get the sound and rhythm! Prof. dr. Gunther van Loon, DVM, PhD, Ass Member ECVDI, Dip ECEIM Dept. of Large Animal Internal Medicine Ghent University, Belgium Murmurs
Cardiovascular Physiology
 Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
Cardiovascular Physiology Introduction The cardiovascular system consists of the heart and two vascular systems, the systemic and pulmonary circulations. The heart pumps blood through two vascular systems
BACK TO THE BASICS: ASSESSING YOUR PATIENT S CARDIOVASCULAR STATUS WITHOUT ALL THE BELLS AND WHISTLES.
 BACK TO THE BASICS: ASSESSING YOUR PATIENT S CARDIOVASCULAR STATUS WITHOUT ALL THE BELLS AND WHISTLES. NTI 2012 Session Number: 381 Presented By: Cynthia L. Webner, DNP, RN, CCNS, CCRN-CMC www.cardionursing.com
BACK TO THE BASICS: ASSESSING YOUR PATIENT S CARDIOVASCULAR STATUS WITHOUT ALL THE BELLS AND WHISTLES. NTI 2012 Session Number: 381 Presented By: Cynthia L. Webner, DNP, RN, CCNS, CCRN-CMC www.cardionursing.com
Nothing to Disclose. Severe Pulmonary Hypertension
 Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Severe Ronald Pearl, MD, PhD Professor and Chair Department of Anesthesiology Stanford University Rpearl@stanford.edu Nothing to Disclose 65 year old female Elective knee surgery NYHA Class 3 Aortic stenosis
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
The production of murmurs is due to 3 main factors:
 Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
CARDIOVASCULAR SYSTEM 1. Resting membrane potential of the ventricular myocardium is: A. -55 to-65mv B. --65 to-75mv C. -75 to-85mv D. -85 to-95 mv E. -95 to-105mv 2. Regarding myocardial contraction:
Cardiovascular Assessment in Emergency Situations
 Cardiovascular Assessment in Emergency Situations Karen Marzlin DNP, RN, CCNS, CCRN-CMC, CHFN Key Choice / CNEA Prepared to handle emergencies with calm, cool, critical thinking! 3 Components Key Assessment
Cardiovascular Assessment in Emergency Situations Karen Marzlin DNP, RN, CCNS, CCRN-CMC, CHFN Key Choice / CNEA Prepared to handle emergencies with calm, cool, critical thinking! 3 Components Key Assessment
PHYSIOLOGY MeQ'S (Morgan) All the following statements related to blood volume are correct except for: 5 A. Blood volume is about 5 litres. B.
 PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
PHYSIOLOGY MeQ'S (Morgan) Chapter 5 All the following statements related to capillary Starling's forces are correct except for: 1 A. Hydrostatic pressure at arterial end is greater than at venous end.
Heart Pump and Cardiac Cycle. Faisal I. Mohammed, MD, PhD
 Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
Heart Pump and Cardiac Cycle Faisal I. Mohammed, MD, PhD 1 Objectives To understand the volume, mechanical, pressure and electrical changes during the cardiac cycle To understand the inter-relationship
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein THE BLOOD SYSTEM 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS
 Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS Program Director, Cardiovascular Technology Florida SouthWestern State College Fort Myers, FL Disclosures Speaker s Bureau: None Stockholder: None
Hemodynamics: Cardiac and Vascular Jeff Davis, RRT, RCIS Program Director, Cardiovascular Technology Florida SouthWestern State College Fort Myers, FL Disclosures Speaker s Bureau: None Stockholder: None
Cardiac Output MCQ. Professor of Cardiovascular Physiology. Cairo University 2007
 Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
Cardiac Output MCQ Abdel Moniem Ibrahim Ahmed, MD Professor of Cardiovascular Physiology Cairo University 2007 90- Guided by Ohm's law when : a- Cardiac output = 5.6 L/min. b- Systolic and diastolic BP
CV Lecture. Heart as a pump cardiac performance Polygram - analysis of cardiac activity. Dr. Ana-Maria Zagrean
 CV Lecture Heart as a pump cardiac performance Polygram - analysis of cardiac activity Dr. Ana-Maria Zagrean Coronary Circulation Left coronary artery: for the anterior & left lateral portions of LV. Right
CV Lecture Heart as a pump cardiac performance Polygram - analysis of cardiac activity Dr. Ana-Maria Zagrean Coronary Circulation Left coronary artery: for the anterior & left lateral portions of LV. Right
Echocardiography as a diagnostic and management tool in medical emergencies
 Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Echocardiography as a diagnostic and management tool in medical emergencies Frank van der Heusen MD Department of Anesthesia and perioperative Care UCSF Medical Center Objective of this presentation Indications
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
The Cardiac Cycle Clive M. Baumgarten, Ph.D.
 The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
The Cardiac Cycle Clive M. Baumgarten, Ph.D. OBJECTIVES: 1. Describe periods comprising cardiac cycle and events within each period 2. Describe the temporal relationships between pressure, blood flow,
Cardiovascular Assessment in Emergency Situations
 Cardiovascular Assessment in Emergency Situations Cynthia Webner DNP, RN, CCNS, CCRN-CMC, CHFN Karen Marzlin DNP, RN, CCNS, CCRN-CMC, CHFN www.cardionursing.com www.cardionursing.com 1 Key Assessment Tools
Cardiovascular Assessment in Emergency Situations Cynthia Webner DNP, RN, CCNS, CCRN-CMC, CHFN Karen Marzlin DNP, RN, CCNS, CCRN-CMC, CHFN www.cardionursing.com www.cardionursing.com 1 Key Assessment Tools
The production of murmurs is due to 3 main factors:
 Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
Heart murmurs The production of murmurs is due to 3 main factors: high blood flow rate through normal or abnormal orifices forward flow through a narrowed or irregular orifice into a dilated vessel or
CATCH A WAVE.. INTRODUCTION NONINVASIVE HEMODYNAMIC MONITORING 4/12/2018
 WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
WAVES CATCH A WAVE.. W I S C O N S I N P A R A M E D I C S E M I N A R A P R I L 2 0 1 8 K E R I W Y D N E R K R A U S E R N, C C R N, E M T - P Have you considered that if you don't make waves, nobody
Physiology lecture 15 Hemodynamic
 Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
Physiology lecture 15 Hemodynamic Dispensability (D) : proportional change in volume per unit change in pressure D = V/ P*V It is proportional (divided by the original volume). Compliance (C) : total change
IB TOPIC 6.2 THE BLOOD SYSTEM
 IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
IB TOPIC 6.2 THE BLOOD SYSTEM THE BLOOD SYSTEM TERMS TO KNOW circulation ventricle artery vein 6.2.U1 - Arteries convey blood at high pressure from the ventricles to the tissues of the body Circulation
What s That Sound? Pediatric Murmur Evaluation
 What s That Sound? Pediatric Murmur Evaluation Jamie S. Sutherell, M.D, M.Ed. Associate Professor, Pediatrics Division of Cardiology Director, Medical Student Education in Pediatrics Director, Pediatric
What s That Sound? Pediatric Murmur Evaluation Jamie S. Sutherell, M.D, M.Ed. Associate Professor, Pediatrics Division of Cardiology Director, Medical Student Education in Pediatrics Director, Pediatric
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm 2012 Session 7: Noninvasive Hemodynamic Assessment Without the Bells and Whistles Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Tom Ahrens HEMODYNAMIC MONITORING
Relax and Learn At the Farm 2012 Session 7: Noninvasive Hemodynamic Assessment Without the Bells and Whistles Carol Jacobson RN, MN Cardiovascular Nursing Education Associates Tom Ahrens HEMODYNAMIC MONITORING
Cardiology. the Sounds: #7 HCM. LV Outflow Obstruction: Aortic Stenosis. (Coming Soon - HCM)
 A Cardiology HCM LV Outflow Obstruction: Aortic Stenosis (Coming Soon - HCM) the Sounds: #7 Howard J. Sachs, MD www.12daysinmarch.com E-mail: Howard@12daysinmarch.com Aortic Valve Disorders Stenosis Regurgitation
A Cardiology HCM LV Outflow Obstruction: Aortic Stenosis (Coming Soon - HCM) the Sounds: #7 Howard J. Sachs, MD www.12daysinmarch.com E-mail: Howard@12daysinmarch.com Aortic Valve Disorders Stenosis Regurgitation
Weeks 1-3:Cardiovascular
 Weeks 1-3:Cardiovascular Cardiac Output The total volume of blood ejected from the ventricles in one minute is known as the cardiac output. Heart Rate (HR) X Stroke Volume (SV) = Cardiac Output Normal
Weeks 1-3:Cardiovascular Cardiac Output The total volume of blood ejected from the ventricles in one minute is known as the cardiac output. Heart Rate (HR) X Stroke Volume (SV) = Cardiac Output Normal
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
During exercise the heart rate is 190 bpm and the stroke volume is 115 ml/beat. What is the cardiac output?
 The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
The Cardiovascular System Part III: Heart Outline of class lecture After studying part I of this chapter you should be able to: 1. Be able to calculate cardiac output (CO) be able to define heart rate
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1
 BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
BIPN100 F15 Human Physiol I (Kristan) Lecture 14 Cardiovascular control mechanisms p. 1 Terms you should understand: hemorrhage, intrinsic and extrinsic mechanisms, anoxia, myocardial contractility, residual
HISTORY. Question: How do you interpret the patient s history? CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: 45-year-old man.
 HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
HISTORY 45-year-old man. CHIEF COMPLAINT: Dyspnea of two days duration. PRESENT ILLNESS: His dyspnea began suddenly and has been associated with orthopnea, but no chest pain. For two months he has felt
I. Cardiac Output Chapter 14
 10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
10/24/11 I. Cardiac Output Chapter 14 Cardiac Output, Blood Flow, and Blood Pressure Lecture PowerPoint Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. Cardiac
Circulation. Blood Pressure and Antihypertensive Medications. Venous Return. Arterial flow. Regulation of Cardiac Output.
 Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
Circulation Blood Pressure and Antihypertensive Medications Two systems Pulmonary (low pressure) Systemic (high pressure) Aorta 120 mmhg Large arteries 110 mmhg Arterioles 40 mmhg Arteriolar capillaries
SHOCK. Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital
 SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
SHOCK Emergency pediatric PICU division Pediatric Department Medical Faculty, University of Sumatera Utara H. Adam Malik Hospital 1 Definition Shock is an acute, complex state of circulatory dysfunction
Valvular Heart Disease: Volume Versus Pressure and the Hemodynamic Compromise
 Valvular Heart Disease: Volume Versus Pressure and the Hemodynamic Compromise Cynthia Webner BSN, RN, CCRN, CMC www.cardionursing.com NTI 2009 Class Code 112 1 Mastery is not something that strikes in
Valvular Heart Disease: Volume Versus Pressure and the Hemodynamic Compromise Cynthia Webner BSN, RN, CCRN, CMC www.cardionursing.com NTI 2009 Class Code 112 1 Mastery is not something that strikes in
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Collage of medicine Cardiovascular Physiology 3- Arterial and venous blood Pressure.
 University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
University of Babylon Collage of medicine Dr. Ghafil Seyhood Hassan Al-Shujiari Cardiovascular Physiology 3- Arterial and venous blood Pressure. UArterial blood pressureu: Arterial pressure = COP X Peripheral
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Physiology of Circulation
 Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Physiology of Circulation Dr. Ali Ebneshahidi Blood vessels Arteries: Blood vessels that carry blood away from the heart to the lungs and tissues. Arterioles are small arteries that deliver blood to the
Copyright 2011, 2007 by Mosby, Inc., an affiliate of Elsevier Inc. Normal Cardiac Anatomy
 Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
Mosby,, an affiliate of Elsevier Normal Cardiac Anatomy Impaired cardiac pumping Results in vasoconstriction & fluid retention Characterized by ventricular dysfunction, reduced exercise tolerance, diminished
Ejection across stenotic aortic valve requires a systolic pressure gradient between the LV and aorta. This places a pressure load on the LV.
 Valvular Heart Disease Etiology General Principles Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Valvular Heart Disease Etiology General Principles Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
-12. -Ensherah Mokheemer - ABDULLAH ZREQAT. -Faisal Mohammad. 1 P a g e
 -12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
-12 -Ensherah Mokheemer - ABDULLAH ZREQAT -Faisal Mohammad 1 P a g e In the previous lecture we talked about: - cardiac index: we use the cardiac index to compare the cardiac output between different individuals,
Cor pulmonale. Dr hamid reza javadi
 1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
1 Cor pulmonale Dr hamid reza javadi 2 Definition Cor pulmonale ;pulmonary heart disease; is defined as dilation and hypertrophy of the right ventricle (RV) in response to diseases of the pulmonary vasculature
Means failure of heart to pump enough blood to satisfy the need of the body.
 Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
Means failure of heart to pump enough blood to satisfy the need of the body. Due to an impaired ability of the heart to adequately to fill or eject blood. HEART FAILURE Heart failure (HF) means decreased
PHONOCARDIOGRAPHY (PCG)
 PHONOCARDIOGRAPHY (PCG) The technique of listening to sounds produced by the organs and vessels of the body is called auscultation. The areas at which the heart sounds are heard better are called auscultation
PHONOCARDIOGRAPHY (PCG) The technique of listening to sounds produced by the organs and vessels of the body is called auscultation. The areas at which the heart sounds are heard better are called auscultation
10. Thick deposits of lipids on the walls of blood vessels, called, can lead to serious circulatory issues. A. aneurysm B. atherosclerosis C.
 Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Heart Student: 1. carry blood away from the heart. A. Arteries B. Veins C. Capillaries 2. What is the leading cause of heart attack and stroke in North America? A. alcohol B. smoking C. arteriosclerosis
Physical Exam Part II
 Physical Exam Part II University of Michigan Cardiovascular Center Kim A. Eagle, MD Albion Walter Hewlett Professor Director Physical Exam: Part II Heart Sounds Heart Murmurs HEART SOUNDS S1 MITRAL + TRICUSPID
Physical Exam Part II University of Michigan Cardiovascular Center Kim A. Eagle, MD Albion Walter Hewlett Professor Director Physical Exam: Part II Heart Sounds Heart Murmurs HEART SOUNDS S1 MITRAL + TRICUSPID
Valvular Stenosis and Regurgitation: Barriers to Flow
 Valvular Stenosis and Regurgitation: Barriers to Flow Presented By: Cynthia Webner BSN, RN,CCRN-CMC www.cardionursing.com CNEA 2009 1 Cardiac Valves Prevent Backward Flow Permit Forward Flow 2 www.cardionursing.com
Valvular Stenosis and Regurgitation: Barriers to Flow Presented By: Cynthia Webner BSN, RN,CCRN-CMC www.cardionursing.com CNEA 2009 1 Cardiac Valves Prevent Backward Flow Permit Forward Flow 2 www.cardionursing.com
Ejection across stenotic aortic valve requires a systolic pressure gradient between the LV and aorta. This places a pressure load on the LV.
 Valvular Heart Disease General Principles Etiology Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Valvular Heart Disease General Principles Etiology Cellular and molecular mechanism of valve damage Structural pathology Functional pathology - stenosis/regurgitation Loading conditions - pressure/volume
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Failing Heart. Cardiac Resynchronization: novel therapy for the
 Advanced Studies in Medicine Cardiac Resynchronization: novel therapy for the Failing Heart Module 1: Understanding the Scope of Heart Failure, A Review of the Concepts of Anatomy & Physiology THE JOHNS
Advanced Studies in Medicine Cardiac Resynchronization: novel therapy for the Failing Heart Module 1: Understanding the Scope of Heart Failure, A Review of the Concepts of Anatomy & Physiology THE JOHNS
The Heart. Size, Form, and Location of the Heart. 1. Blunt, rounded point; most inferior part of the heart.
 12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
12 The Heart FOCUS: The heart is composed of cardiac muscle cells, which are elongated, branching cells that appear striated. Cardiac muscle cells behave as a single electrical unit, and the highly coordinated
BIOH122 Session 6 Vascular Regulation
 BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
BIOH122 Session 6 Vascular Regulation To complete this worksheet, select: Module: Distribution Title: Vascular Regulation Introduction 1. a. How do Mean Arterial Blood Pressure (MABP) and Systemic Vascular
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #12 Understanding Preload and Afterload
 McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #12 Understanding Preload and Afterload Cardiac output (CO) represents the volume of blood that is delivered
McHenry Western Lake County EMS System Paramedic, EMT-B and PHRN Optional Continuing Education 2018 #12 Understanding Preload and Afterload Cardiac output (CO) represents the volume of blood that is delivered
HEALTH ASSESSMENT. Afnan Tunsi BSN, RN, MSc.
 HEALTH ASSESSMENT Afnan Tunsi BSN, RN, MSc. Learning Outcomes 2 After completion of this lecture, the student will be able to: Describe suggested sequencing to conduct a thorax and lungs physical health
HEALTH ASSESSMENT Afnan Tunsi BSN, RN, MSc. Learning Outcomes 2 After completion of this lecture, the student will be able to: Describe suggested sequencing to conduct a thorax and lungs physical health
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
The Cardiovascular System
 The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
The Cardiovascular System The Cardiovascular System A closed system of the heart and blood vessels The heart pumps blood Blood vessels allow blood to circulate to all parts of the body The function of
Shock Management. Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate. PDF created with pdffactory Pro trial version
 Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
Shock Management Seyed Tayeb Moradian MSc, Critical Care Nursing Ph.D Candidate Definition of Shock The definition of shock does not involve low blood pressure, rapid pulse or cool clammy skin - these
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU
 Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
Cath Lab Essentials: Basic Hemodynamics for the Cath Lab and ICU Ailin Barseghian El-Farra, MD, FACC Assistant Professor, Interventional Cardiology University of California, Irvine Department of Cardiology
Technique. Technique. Technique. Monitoring 1. Local anesthetic? Aseptic technique Hyper-extend (if radial)
 Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Critical Care Monitoring Hemodynamic Monitoring Arterial Blood Pressure Cannulate artery Uses 2 Technique Sites Locate artery, prep 3 1 Technique Local anesthetic? Aseptic technique Hyper-extend (if radial)
Cardiovascular System
 Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
Cardiovascular System The Heart Cardiovascular System The Heart Overview What does the heart do? By timed muscular contractions creates pressure gradients blood moves then from high pressure to low pressure
*Generating blood pressure *Routing blood: separates. *Ensuring one-way blood. *Regulating blood supply *Changes in contraction
 *Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
*Generating blood pressure *Routing blood: separates pulmonary and systemic circulations *Ensuring one-way blood flow: valves *Regulating blood supply *Changes in contraction rate and force match blood
Cardiac Output (C.O.) Regulation of Cardiac Output
 Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
Cardiac Output (C.O.) Is the volume of the blood pumped by each ventricle per minute (5 Litre) Stroke volume: Is the volume of the blood pumped by each ventricle per beat. Stroke volume = End diastolic
PART I: HEART ANATOMY
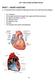 Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Pathophysiology: Left To Right Shunts
 Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Pathophysiology: Left To Right Shunts Daphne T. Hsu, MD dh17@columbia.edu Learning Objectives Learn the relationships between pressure, blood flow, and resistance Review the transition from fetal to mature
Cardiovascular Patient Assessment. Dr. Gary Mumaugh Western Physical Assessment
 Cardiovascular Patient Assessment Dr. Gary Mumaugh Western Physical Assessment Objectives Outline a systematic approach to cardiovascular assessment. Differentiate normal from abnormal findings when assessing
Cardiovascular Patient Assessment Dr. Gary Mumaugh Western Physical Assessment Objectives Outline a systematic approach to cardiovascular assessment. Differentiate normal from abnormal findings when assessing
Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations
 ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
Impedance Cardiography (ICG) Method, Technology and Validity
 Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
Method, Technology and Validity Hemodynamic Basics Cardiovascular System Cardiac Output (CO) Mean arterial pressure (MAP) Variable resistance (SVR) Aortic valve Left ventricle Elastic arteries / Aorta
