Visual Estimation of the Severity of Aortic Stenosis and the Calcium Burden by 2-Dimensional Echocardiography
|
|
|
- Julianna Holmes
- 5 years ago
- Views:
Transcription
1 ORIGINAL RESEARCH Visual Estimation of the Severity of Aortic Stenosis and the Calcium Burden by 2-Dimensional Echocardiography Is It Reliable? Nishath Quader, MD, Susan Wilansky, MD, Roger L. Click, MD, Minako Katayama, MD, Hari P. Chaliki, MD Received November 18, 2014, from the Division of Cardiovascular Diseases, Mayo Clinic, Scottsdale, Arizona USA (N.Q., S.W., M.K., H.P.C.); and Division of Cardiovascular Diseases, Mayo Clinic, Rochester, Minnesota USA (R.L.C.). Revision requested December 7, Revised manuscript accepted for publication December 16, We thank Machiko T. Anderson for recruiting and research assistance. This study was supported by a Mayo Clinic intramural career development grant. Address correspondence to Hari P. Chaliki, MD, Division of Cardiovascular Diseases, Mayo Clinic, E Shea Blvd, Scottsdale, AZ USA. chaliki.hari@mayo.edu Abbreviations ACC, American College of Cardiology; AHA, American Heart Association; AU, arbitrary unit; CI, confidence interval; CT, computed tomography; PPV, positive predictive value; 2D, 2-dimensional doi: /ultra Objectives Guidelines have recommended aortic valve surgery in asymptomatic patients with severe aortic stenosis and a large aortic valve calcium burden. The purpose of this study was to determine whether visual assessment of aortic valve calcium and stenosis severity are reliable based on 2-dimensional echocardiography alone. Methods We prospectively enrolled 68 patients with aortic stenosis and compared them with 30 control participants without aortic stenosis. All had aortic valve calcium score assessment by computed tomography. In a random order, 2-dimensional images without hemodynamic data were independently reviewed by 2 level 3 trained echocardiographers, who then classified these patients into categories based on aortic valve calcium and stenosis severity. Results The 68 patients (mean age ± SD, 74 ± 10 years) were classified as having mild (n = 28), moderate (n = 22), and severe (n = 18) aortic stenosis. When the observers were asked to grade the degree of valve calcification, the agreement between them was poor (κ = ). The visual ability to determine stenosis severity compared with Doppler echocardiography had high specificity (81% and 88% for observers 1 and 2). However, sensitivity was unacceptably low (56% 67%), and the positive predictive value was poor (44% 50%). Agreement was fair (κ = ) between the observers for determining severe stenosis. Conclusions Our results suggest that visual assessment of aortic valve calcium has high interobserver variability; the visual ability to determine severe aortic stenosis has low sensitivity but high specificity. Our results may have important implications for treatment of patients with aortic stenosis and guiding the use of handheld echocardiography. Further research with larger cohorts is needed to validate the variability, sensitivity, and specificity reported in our study. Key Words aortic valve stenosis; echocardiography; computed tomography A ortic stenosis has substantial implications for overall health care associated costs, since the burden of this disease is projected to increase due to an aging population. In fact, according to the American Heart Association (AHA), the prevalence of moderate or severe aortic stenosis in patients 75 years and older is 2.8%. 1 Most common causes of aortic stenosis include calcification of a bicuspid or trileaflet aortic valve by the American Institute of Ultrasound in Medicine J Ultrasound Med 2015; 34:
2 Echocardiography has been a well-established method of diagnosing this disease, and cardiac catheterization is only recommended when echocardiography is nondiagnostic. 2 4 Currently, an aortic valve area of less than 1 cm 2 is considered severe according to the current American College of Cardiology ACC/AHA guidelines. 2 The aortic valve area can be calculated by using Doppler echocardiographic parameters. The aortic valve area can also be measured directly by visualization of the valve orifice on 2-dimensional (2D) 5 or 3-dimensional 6 transthoracic echocardiography or transesophageal echocardiography. 7 The American Society of Echocardiography has suggested that planimetry may be an alternative to aortic valve area measurement when Doppler methods are unreliable. 8 Over the years, we have encountered many clinicians who often ask the echocardiographer the questions Does the aortic valve stenosis look severe? and Is there a significant amount of calcium on the valve?. Similar questions will also invariably be raised in the era of handheld echo - cardiography, which lacks the capability of Doppler hemodynamics. Incorrect diagnosis using these newer handheld ultrasound devices, especially in some settings, such as emergency departments and intensive care units where time and resources are limited, may have profound implications. European Society of Cardiology and ACC/AHA guidelines have recommended aortic valve surgery in asymptomatic patients with severe aortic stenosis and a large aortic valve calcium burden. 2,9 However, it is not clear whether visual assessment of aortic valve calcium and stenosis severity are reliable based on 2D echocardiography alone. The aim of the study was to understand the accuracy of determining various degrees of aortic stenosis severity and calcium burden by visual impressions of highly experienced level 3 trained practicing echocardiographers at an academic institution. Materials and Methods We prospectively enrolled 68 patients with aortic stenosis and compared them with 30 controls without stenosis. Patients were only included if they had a clinical indication for an echocardiographic study. Exclusion criteria were an ejection fraction of less than 50%, greater than mild aortic regurgitation, moderate or greater stenosis or regurgitation in valves other than the aortic valve, prior myocardial infarction (defined as a wall motion abnormality on a resting echocardiogram), previous cardiac surgery, atrial fibrillation or flutter, the presence of a left bundle branch block, a pacemaker, poor echocardiographic images, infiltrative heart disease, hypertrophic cardiomyopathy, constriction or restriction, pregnancy or nursing, and a history of pulmonary embolism. The protocol was approved by the Mayo Foundation Institutional Review Board and written informed consent was obtained to participate in the study. Detailed baseline demographic and echocardiographic characteristics were recorded. All patients had assessment of their aortic valve calcium score by computed tomography (CT). Hemodynamic Assessment by Echocardiography The left ventricular outflow tract diameter was measured from a parasternal long-axis view according to the American Society of Echocardiography recommendations. 8 The left ventricular outflow tract time-velocity integral was then measured from the apical long-axis view by placing the pulsed wave Doppler sample volume at the left ventricular outflow tract, 5 mm proximal to the aortic valve to avoid spectral broadening and also to visualize the aortic valve closure click. Mean and peak gradients were measured from multiple windows by continuous wave Doppler imaging. The aortic valve area was then calculated by the continuity method. 8 Other standard echocardiographic characteristics were also measured. Visual Assessment of the Severity of Valve Calcification and Aortic Stenosis In a random order, 2D images of the aortic valve at parasternal long-axis, parasternal short-axis, and apical long-axis views (without hemodynamic data) were independently reviewed by 2 level 3 trained echocardiographers. These echocardiographers then classified these patients into 4 categories (none, mild, moderate, and severe) based on visual valve calcification and severity of aortic stenosis. Their assessment of stenosis severity and valve calcification was then compared with Doppler-derived hemodynamic measurements and CT-derived aortic valve calcium scores. Aortic Valve Calcium Scoring by CT Computed tomography of the heart was performed with commercially available multidetector scanners according to a coronary artery calcification scoring protocol with prospective electrocardiographic R-wave triggering and reconstruction of 2.5- to 3.0-mm axial images at 70% to 80% of the R-R interval. Aortic valve calcium scoring was performed, using accepted methods, 10,11 within valve leaflets, carefully excluding the calcium in the aortic wall, aortic annulus, and coronary arteries. The Agaston-Janowitz scale with a 130 Hounsfield unit threshold was used J Ultrasound Med 2015; 34:
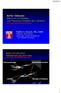
3 Statistical Analysis The data are presented as mean ± standard deviation and median. Patients were divided into 4 groups according to stenosis severity determined by the mean gradient through the aortic valve. Comparisons between groups were performed by a Kruskal-Wallis tests for continuous variables and χ 2 test for categorical variables. P <.05 was considered a statistically significant difference. Interobserver agreement between the echocardiographers was assessed by the κ method. Results The 68 patients (mean age, 74 ± 10 years; 62% male) were classified as having mild (mean gradient, mm Hg; n = 28), moderate (mean gradient, mm Hg; n = 22), and severe (mean gradient, >40 mm Hg; n = 18) aortic stenosis,compared with the 30 control participants without stenosis (mean gradient, <10 mm Hg). Age, sex, and comorbid conditions were not different among patients without stenosis and those with mild, moderate, or severe stenosis. The left ventricular ejection fraction was also not different among the 4 groups (Table 1). As expected, the mean gradient was minimal (4 ± 2 mm Hg) in patients with no aortic stenosis, whereas patients with mild, moderate, and severe stenosis had mean gradients of 17 ± 5, 32 ± 5, and 54 ± 9 mm Hg (P <.0001), respectively. Aortic Valve Calcium Score by CT and Visual Assessment by Echocardiography Computed tomographically measured aortic valve calcium scores were different among the 4 groups (92 ± 161 arbitrary units [AU] in patients with no stenosis versus 689 ± 616 AU in patients with mild stenosis, 1292 ± 693 AU in patients with moderate stenosis, and 2537 ± 1170 AU in patients with severe stenosis; P <.0001; Table 1). Visual assessment of valve calcification by echocardiography compared with the aortic valve calcium score by CT is presented in Table 2 and Figure 1. Mean calcium scores of controls and each grade of valve calcification determined visually by the observers as shown in Table 2 reveal that observer 2 had higher calcium scores for each grade of valve calcification compared with observer 1. Specifically, when observer 1 was asked to visually assess the calcium, that observer classified 1 patient as having no aortic valve calcification, corresponding to an aortic valve calcification score of 0 AU on CT, whereas observer 2 classified 12 patients as having no aortic valve calcification, corresponding to a score of 8 ± 17 AU on CT. Similarly, observer 1 classified 39 patients as having severe aortic valve calcification, corresponding to a CT-derived aortic valve calcium score of 1673 ± 1145 AU, whereas observer 2 classified 13 patients as having severe aortic valve calcification, corresponding to a CT-derived score of 2300 ± 1242 AU. Table 1. Baseline Demographics in Each Group Stenosis None Mild Moderate Severe Characteristic (n = 30) (n = 28) (n = 22) (n = 18) P Age, y 70 ± ± ± 5 75 ± Male, % Hypertension, % Hyperlipidemia, % Coronary artery disease, % Ejection fraction, % 64 ± 4 64 ± 5 67 ± 5 67 ± 4.09 Gradient, mm Hg 4 ± 2 17 ± 5 32 ± 5 54 ± 9 <.0001 Calcium score, AU 92 ± ± ± ± 1170 <.001 Table 2. Visual Assessment of Valve Calcification on Echocardiography and Aortic Valve Calcium Score on CT Calcium Score by Visual Calcification Assessment, AU (n) Observer None Mild Moderate Severe P 1 0 (1) 153 ± 392 (30) 939 ± 897 (28) 1673 ± 1145 (39) < ± 17 (12) 596 ± 914 (40) 1283 ± 832 (33) 2300 ± 1242 (13) <.0001 J Ultrasound Med 2015; 34:
4 When an aortic valve calcium score higher than 1000 AU was used to define severe aortic valve calcification, as defined by the current ACC/AHA guidelines, 2 40 patients (41%) had severe aortic valve calcification by the CT score. determined that 29 patients had severe calcification, resulting in sensitivity of 73%, whereas observer 2 determined that 12 patients had severe calcification, resulting in sensitivity of 30%. Specificity for observer 1 was slightly lower at 83% compared to 98% for observer 2 (Table 3). Agreement when compared with the CT score for observer 1 had a κ value of 0.55 (95% confidence interval [CI], ), whereas it was 0.32 (95% CI, ) for observer 2. However, when the echocardiographers assessments of whether severe aortic valve calcification was present was compared with each other, interobserver agreement was poor, with a κ value of 0.33 (95% CI, ; Table 4). Interobserver agreement on visual assessment of calcium was slightly better, with a κ of 0.39 (95% CI, ), when 4 categories were used (Table 5). Despite the Figure 1. Visual estimation of calcium and aortic valve calcium (AVC) scores between observers 1 and 2. Even though observers 1 and 2 classified the patients into the various categories ranging from no valve calcium to severe valve calcium, there were significant overlaps in the various categories compared to the CT-derived calcium score, indicating that visual estimation of calcium may not be so reliable given that even with experienced eyes, the level of discrepancy between visual assessment and the actual CT-derived calcium score can be significant. poor agreement between the observers regarding the visual calcium burden of a particular valve, each observer was able to discriminate the amount of calcium between various grades of aortic stenosis (Figure 1 and Table 2). Visual Assessment of Aortic Valve Stenosis Severity When the visual assessment of hemodynamic severity of aortic stenosis was categorized as severe versus not severe, sensitivity was poor (observer 1, 67%; observer 2, 56%) compared with Doppler echocardiography, whereas specificity was fair (observer 1, 81%; observer 2, 88%; Table 6). However, the positive predictive value (PPV) was not acceptable (observer 1, 44%; observer 2, 50%). Interobserver agreement on visual assessment of stenosis severity was acceptable, with a κ value of 0.58 (95% CI, ; Table 7). When 4 categories were used, the κ value was 0.69 (95% CI, ; Table 8). Table 3. Visual Assessment of Valve Calcification by Observers 1 and 2 Calcium Score Visual Estimate > Severe Nonsevere Sensitivity, 73%; specificity, 83%; κ = 0.55 ( ) Observer 2 Severe 12 1 Nonsevere Sensitivity, 30%; specificity, 98%; κ = 0.32 ( ) Table 4. Interobserver Agreement on Visual Assessment of Valve Calcification for Severe Versus Nonsevere Stenosis Observer 2 Severe Nonsevere Severe 12 1 Nonsevere κ = 0.33 ( ) Table 5. Interobserver Agreement on Visual Assessment of Valve Calcification for Stenosis Categories Observer 2 None Mild Moderate Severe Total None Mild Moderate Severe Total κ = 0.39 ( ) 1714 J Ultrasound Med 2015; 34:
5 Discussion This is the first study to our knowledge that compared visual assessment of aortic valve calcification with a CT-measured aortic valve calcium score. Our study shows that visual grading of aortic valve calcium compared with CT-measured calcium is discordant even in the eyes of experienced echocardiographers. More importantly, the interobserver agreement for classifying patients into 4 categories based on visual assessment alone is poor (κ = ). In terms of the hemodynamic severity of aortic stenosis, without the knowledge of Doppler data, interobserver agreement was fair (κ = ). When compared with Doppler-derived hemodynamic severity, visual assessment by the echocardiographers was specific (81% and 88%) for severe aortic stenosis, but sensitivity (67% and 56%) and PPVs (44% and 50%) were lower than acceptable levels. Table 6. Visual Assessment of Stenosis Severity by Observers 1 and 2 Hemodynamic Severity Visual Assessment Severe Nonsevere Severe Nonsevere 6 64 Sensitivity, 67%; specificity, 81%; PPV, 44% Observer 2 Severe Nonsevere 8 70 Sensitivity, 56%; specificity, 88%; PPV, 50% Table 7. Interobserver Agreement on Visual Assessment of Stenosis Severity Observer 2 Severe Nonsevere Severe 16 4 Nonsevere κ = 0.58 ( ) Table 8. Interobserver Agreement on Visual Assessment of Stenosis Severity for Stenosis Categories Observer 2 None Mild Moderate Severe Total None Mild Moderate Severe Total κ = 0.69 ( ) The example shown in Figure 2 further highlights the discrepancies even between the experienced eyes of level 3 trained echocardiographers and actual hemodynamic data and aortic valve calcium scores. In general, visual assessment is a mental process in which we qualitatively judge the aortic valve opening and intuitively compare it with the anatomic valve area proposed by guidelines (<1 cm 2 in cases of severe aortic stenosis). As shown in our study, this mental translation has low sensitivity but reasonable specificity. In other words, by visual assessment alone, we may misclassify patients with severe aortic stenosis as not having severe stenosis in the absence of Doppler data. Similarly, what one person considers severe calcification may vary from person to person depending on individual interpretation of severe valve calcification. In addition, thresholds of CT-derived aortic valve calcium scores separating various grades of aortic stenosis are variable between observers. Our study emphasizes the need for a full echocardiographic study in patients suspected to have more than mild aortic stenosis and CT-derived aortic valve calcium scores in selected patients with aortic stenosis before subjecting them to any intervention. Even though visual assessment is a surrogate of planimetry of the aortic valve, planimetry of the aortic valve to assess aortic stenosis severity has its own limitations. This technique may be inaccurate when there is excessive valve calcification, and one has to be able to differentiate the effective orifice area from the anatomic or geometric valve area. 4 In brief, the anatomic or geometric orifice area is the area of valve opening measured by planimetry. However, the effective orifice area refers to the crosssectional area of the jet downstream of the vena contracta as the jet accelerates out of the stenotic valve. 13 The differences between either effective or anatomic valve areas depend on valve geometry and can be affected by valve morphologic characteristics (bicuspid versus trileaflet valve). 14 It has been proposed that the anatomic valve area may have values higher than those calculated by a continuity equation in special cases of valve stenosis related to valve geometry. 15 Another limitation of 2D echocardiography and planimetry is acoustic shadowing due to valve calcification, as is frequently seen in severe aortic stenosis. In addition, the valve orifice could be miscalculated due to nonplanar alignment of the ultrasonic beam. 16 Threedimensional echocardiography with multiplanar reconstruction may provide better assessment of the anatomic valve orifice area because of the ease of aligning multiple planes orthogonal to the valve. 17 These factors may explain low sensitivity and low PPV in determining the severity of aortic stenosis by visual assessment alone in our study. J Ultrasound Med 2015; 34:
6 There is evidence suggesting that an aortic valve calcium score higher than 1100 AU has good sensitivity and specificity for diagnosing severe aortic stenosis. 10 Aortic valve calcium on multidetector CT is measured by using the valvular Agatston score. 12,18 This score is calculated by using a weighted value assigned to the highest density of valve calcium; the density is measured in Hounsfield units. This score is then multiplied by the area of valve calcification. Valve calcium is measured within the valve leaflets. On the contrary, visual impression of a 2D echocardiogram may overestimate valve calcium if there is annular calcification or if the image is overgained. It is also possible that a 2D echocardiogram could underestimate total valve calcium if there is substantial acoustic shadowing related to the valve calcium or annular calcification. Poor agreement between the observers may be partly related to the abovementioned factors in our study. Why should we care about visual assessment of aortic valve calcification? In the current era of transfemoral/ apical aortic valve replacement, the amount of valve calcification and location of valve calcium are predictive of procedural success and perivalvular aortic regurgitation, which in turn is linked to long-term mortality after the procedure. 19 In addition, decreased event-free survival was reported in patients with severe aortic valve calcium in one study 20 and valve calcium scores higher than 500 AU in another second study. 10 Furthermore the ACC/AHA guidelines recommend valve surgery in patients who have a high like lihood of rapid progression based on the amount of valve calcification. 2 Both visual assessment of the calcium burden and visual assessment of severity of aortic stenosis are linked. This relationship may be important with the recent advent and wide availability of handheld echocardiographic machines that display 2D images but without Doppler data. As demonstrated in this study, even when highly experienced level 3 echocardiographers were asked to review and classify patients with aortic stenosis into various categories based on the amount of valve calcium and aortic stenosis severity by visual impression alone, the sensitivity for determining severe aortic stenosis was poor and likely will be even worse when one uses the handheld echocardiographic machines, not only because of image size and quality but also because of their use by less experienced users in some cases. There were several limitations in this study. First, there is no standardized criterion for visual assessment of valve calcification using 2D echocardiography. Therefore, we did not provide the echocardiographers specific instructions for classification into none, mild, moderate, or severe valve calcification. This aspect might have caused less agreement between the observers because of different preconceptions of the severity of the valve calcification. Second, aortic valve calcium scoring by CT is a relatively new method within the past 10 to 20 years. The threshold for an aortic valve calcium score 10 indicating severe aortic Figure 2. Two-dimensional images from patients with severe aortic stenosis: examples of cases of aortic stenosis that can be seen in an echocardiography laboratory. The aortic valve calcium score was 3244 AU on CT. The mean gradient through the aortic valve was 51 mm Hg; the peak velocity was 4.4 m/s; and the calculated aortic valve area was 0.88 cm2 on echocardiography. When the observers were asked to classify these patients calcium burden and aortic stenosis severity, observer 1 classified them as having severe valve calcium and severe aortic stenosis, and observer 2 classified them as having moderate valve calcium and moderate aortic stenosis. Ao indicates aorta; LA, left atrium; LCC, left coronary cusp; LV, left ventricle; NCC, noncoronary cusp; RA, right atrium; RCC, right coronary cusp; and RVOT, right ventricular outflow tract J Ultrasound Med 2015; 34:
7 stenosis might be revised according to the progress of new scanners and medical physics. Also, the threshold for the severity of calcification 2 may need to be reconsidered according to the outcome measure or according to different age groups. Third, classification of the hemodynamic severity of aortic stenosis by a Doppler method has been also debated. 21 We used a mean gradient for categorizing aortic stenosis types into mild, moderate, and severe stenosis. Some cases have inconsistency between the mean gradient, peak velocity, and calculated aortic valve area. Different measures provide slightly different classifications for the aortic stenosis severity. In conclusion, visual assessment of aortic valve calcium has high interobserver variability. Computed tomography offers a more quantitative approach. The visual ability to determine severe aortic stenosis in older patients has low sensitivity but high specificity. Therefore, a full hemodynamic study is recommended in most cases of aortic stenosis regardless of the visual impression, especially in older patients. Our study results may have important implications in the management of asymptomatic severe aortic stenosis and in guiding the use of handheld echocardiographic machines in patients with aortic stenosis. Further research is needed with larger cohorts of patients to validate the interobserver variability, sensitivity, and specificity reported in our study. References 1. Go AS, Mozaffarian D, Roger VL, et al. Executive summary: heart disease and stroke statistics 2013 update: a report from the American Heart Association. Circulation 2013; 127: Nishimura RA, Otto CM, Bonow RO, et al AHA/ACC guideline for the management of patients with valvular heart disease: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines. Circulation 2014; 129:e521 e Chambers J, Bach D, Dumesnil J, Otto C, Shah P, Thomas J. Crossing the aortic valve in severe aortic stenosis: no longer acceptable? J Heart Valve Dis 2004; 13: Vahanian A, Baumgartner H, Bax J, et al. Guidelines on the management of valvular heart disease: the Task Force on the Management of Valvular Heart Disease of the European Society of Cardiology. Eur Heart J 2007; 28: Okura H, Yoshida K, Hozumi T, Akasaka T, Yoshikawa J. Planimetry and transthoracic two-dimensional echocardiography in noninvasive assessment of aortic valve area in patients with valvular aortic stenosis. J Am Coll Cardiol 1997; 30: Goland S, Trento A, Iida K, et al. Assessment of aortic stenosis by threedimensional echocardiography: an accurate and novel approach. Heart 2007; 93: Cormier B, Iung B, Porte JM, Barbant S, Vahanian A. Value of multiplane transesophageal echocardiography in determining aortic valve area in aortic stenosis. Am J Cardiol 1996; 77: Baumgartner H, Hung J, Bermejo J, et al. Echocardiographic assessment of valve stenosis: EAE/ASE recommendations for clinical practice. J Am Soc Echocardiogr 2009; 22: Vahanian A, Alfieri O, Andreotti F, et al. Guidelines on the management of valvular heart disease (version 2012). Eur Heart J 2012; 33: Messika-Zeitoun D, Aubry MC, Detaint D, et al. Evaluation and clinical implications of aortic valve calcification measured by electron-beam computed tomography. Circulation 2004; 110: Clavel MA, Messika-Zeitoun D, Pibarot P, et al. The complex nature of discordant severe calcified aortic valve disease grading: new insights from combined Doppler echocardiographic and computed tomographic study. J Am Coll Cardiol 2013; 62: Agatston AS, Janowitz WR, Hildner FJ, Zusmer NR, Viamonte M Jr, Detrano R. Quantification of coronary artery calcium using ultrafast computed tomography. J Am Coll Cardiol 1990; 15: Garcia D, Dumesnil JG, Durand LG, Kadem L, Pibarot P. Discrepancies between catheter and Doppler estimates of valve effective orifice area can be predicted from the pressure recovery phenomenon: practical implications with regard to quantification of aortic stenosis severity. J Am Coll Cardiol 2003; 41: Donal E, Novaro GM, Deserrano D, et al. Planimetric assessment of anatomic valve area overestimates effective orifice area in bicuspid aortic stenosis. J Am Soc Echocardiogr 2005; 18: Gilon D, Cape EG, Handschumacher MD, et al. Effect of threedimensional valve shape on the hemodynamics of aortic stenosis: three-dimensional echocardiographic stereolithography and patient studies. J Am Coll Cardiol 2002; 40: Gill EA, Pittenger B, Otto CM. Evaluation of the severity of valvular heart disease and timing of surgery [in Spanish]. Rev Esp Cardiol 2003; 56: Black D, Ahmad Z, Lim Z, Salmon A, Veltdman G, Vettukattil J. The accuracy of three-dimensional echocardiography with multiplanar reformatting in the assessment of the aortic valve annulus prior to percutaneous balloon aortic valvuloplasty in congenital heart disease. J Invasive Cardiol 2012; 24: Schmermund A, Baumgart D, Görge G, et al. Coronary artery calcium in acute coronary syndromes: a comparative study of electron-beam computed tomography, coronary angiography, and intracoronary ultrasound in survivors of acute myocardial infarction and unstable angina. Circulation 1997; 96: Kodali SK, Williams MR, Smith CR, et al. Two-year outcomes after transcatheter or surgical aortic-valve replacement. N Engl J Med 2012; 366: Rosenhek R, Binder T, Porenta G, et al. Predictors of outcome in severe, asymptomatic aortic stenosis. N Engl J Med 2000; 343: Minners J, Allgeier M, Gohlke-Baerwolf C, Kienzle RP, Neumann FJ, Jander N. Inconsistent grading of aortic valve stenosis by current guidelines: haemodynamic studies in patients with apparently normal left ventricular function. Heart 2010; 96: J Ultrasound Med 2015; 34:
Comprehensive Echo Assessment of Aortic Stenosis
 Comprehensive Echo Assessment of Aortic Stenosis Smonporn Boonyaratavej, MD, MSc King Chulalongkorn Memorial Hospital Bangkok, Thailand Management of Valvular AS Medical and interventional approaches to
Comprehensive Echo Assessment of Aortic Stenosis Smonporn Boonyaratavej, MD, MSc King Chulalongkorn Memorial Hospital Bangkok, Thailand Management of Valvular AS Medical and interventional approaches to
Imaging in TAVI. Jeroen J Bax Dept of Cardiology Leiden Univ Medical Center The Netherlands Davos, feb 2013
 Imaging in TAVI Jeroen J Bax Dept of Cardiology Leiden Univ Medical Center The Netherlands Davos, feb 2013 Research grants: Medtronic, Biotronik, Boston Scientific, St Jude, BMS imaging, GE Healthcare,
Imaging in TAVI Jeroen J Bax Dept of Cardiology Leiden Univ Medical Center The Netherlands Davos, feb 2013 Research grants: Medtronic, Biotronik, Boston Scientific, St Jude, BMS imaging, GE Healthcare,
Hemodynamic Assessment. Assessment of Systolic Function Doppler Hemodynamics
 Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
Hemodynamic Assessment Matt M. Umland, RDCS, FASE Aurora Medical Group Milwaukee, WI Assessment of Systolic Function Doppler Hemodynamics Stroke Volume Cardiac Output Cardiac Index Tei Index/Index of myocardial
Adult Echocardiography Examination Content Outline
 Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Adult Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 2 3 4 5 Anatomy and Physiology Pathology Clinical Care and Safety Measurement Techniques, Maneuvers,
Role of Transesophageal Echocardiography in the Diagnosis of Paradoxical Low Flow, Low Gradient Severe Aortic Stenosis
 Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Role of Transesophageal Echocardiography in the Diagnosis of Paradoxical Low Flow, Low Gradient Severe Aortic Stenosis
Original Article Print ISSN 1738-5520 On-line ISSN 1738-5555 Korean Circulation Journal Role of Transesophageal Echocardiography in the Diagnosis of Paradoxical Low Flow, Low Gradient Severe Aortic Stenosis
When Does 3D Echo Make A Difference?
 When Does 3D Echo Make A Difference? Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network 1 Practical Applications of 3D Echocardiography Recommended
When Does 3D Echo Make A Difference? Wendy Tsang, MD, SM Assistant Professor, University of Toronto Toronto General Hospital, University Health Network 1 Practical Applications of 3D Echocardiography Recommended
PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING
 PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING STANDARD - Primary Instrumentation 1.1 Cardiac Ultrasound Systems SECTION 1 Instrumentation Ultrasound instruments
PART II ECHOCARDIOGRAPHY LABORATORY OPERATIONS ADULT TRANSTHORACIC ECHOCARDIOGRAPHY TESTING STANDARD - Primary Instrumentation 1.1 Cardiac Ultrasound Systems SECTION 1 Instrumentation Ultrasound instruments
Low Gradient Severe? AS
 Low Gradient Severe? AS Philippe Pibarot, DVM, PhD, FACC, FAHA, FESC, FASE Canada Research Chair in Valvular Heart Diseases Institut Universitaire de Cardiologie et de Pneumologie de Québec / Québec Heart
Low Gradient Severe? AS Philippe Pibarot, DVM, PhD, FACC, FAHA, FESC, FASE Canada Research Chair in Valvular Heart Diseases Institut Universitaire de Cardiologie et de Pneumologie de Québec / Québec Heart
Aortic valve implantation using the femoral and apical access: a single center experience.
 Aortic valve implantation using the femoral and apical access: a single center experience. R. Hoffmann, K. Brehmer, R. Koos, R. Autschbach, N. Marx, G. Dohmen Rainer Hoffmann, University Aachen, Germany
Aortic valve implantation using the femoral and apical access: a single center experience. R. Hoffmann, K. Brehmer, R. Koos, R. Autschbach, N. Marx, G. Dohmen Rainer Hoffmann, University Aachen, Germany
Echocardiographic evaluation of mitral stenosis
 Echocardiographic evaluation of mitral stenosis Euroecho 2011 Philippe Unger, MD, FESC Erasme Hospital, ULB, Brussels, Belgium I have nothing to declare EuroHeart Survey Etiology of single native left-sided
Echocardiographic evaluation of mitral stenosis Euroecho 2011 Philippe Unger, MD, FESC Erasme Hospital, ULB, Brussels, Belgium I have nothing to declare EuroHeart Survey Etiology of single native left-sided
Revealing new insights. irotate electronic rotation and xplane adjustable biplane imaging. Ultrasound cardiology. irotate and xplane
 Ultrasound cardiology irotate and xplane Revealing new insights irotate electronic rotation and xplane adjustable biplane imaging Annemien van den Bosch and Jackie McGhie Department of Cardiology, Erasmus
Ultrasound cardiology irotate and xplane Revealing new insights irotate electronic rotation and xplane adjustable biplane imaging Annemien van den Bosch and Jackie McGhie Department of Cardiology, Erasmus
Aortic Stenosis and Perioperative Risk With Non-cardiac Surgery
 Aortic Stenosis and Perioperative Risk With Non-cardiac Surgery Aortic stenosis (AS) is characterized as a high-risk index for cardiac complications during non-cardiac surgery. A critical analysis of old
Aortic Stenosis and Perioperative Risk With Non-cardiac Surgery Aortic stenosis (AS) is characterized as a high-risk index for cardiac complications during non-cardiac surgery. A critical analysis of old
Low gradient severe aortic stenosis with preserved left ventricular ejection fraction
 Review Article Low gradient severe aortic stenosis with preserved left ventricular ejection fraction Alper Ozkan Heart and Vascular Institute, Cleveland Clinic, Cleveland, Ohio, USA Corresponding to: Alper
Review Article Low gradient severe aortic stenosis with preserved left ventricular ejection fraction Alper Ozkan Heart and Vascular Institute, Cleveland Clinic, Cleveland, Ohio, USA Corresponding to: Alper
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know
 Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
Aortic Valve Practice Guidelines: What Has Changed and What You Need to Know James F. Burke, MD Program Director Cardiovascular Disease Fellowship Lankenau Medical Center Disclosure Dr. Burke has no conflicts
Outcome of Patients With Aortic Stenosis, Small Valve Area, and Low-Flow, Low-Gradient Despite Preserved Left Ventricular Ejection Fraction
 Journal of the American College of Cardiology Vol. 60, No. 14, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2011.12.054
Journal of the American College of Cardiology Vol. 60, No. 14, 2012 2012 by the American College of Cardiology Foundation ISSN 0735-1097/$36.00 Published by Elsevier Inc. http://dx.doi.org/10.1016/j.jacc.2011.12.054
MITRAL STENOSIS. Joanne Cusack
 MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
MITRAL STENOSIS Joanne Cusack BSE Breakdown Recognition of rheumatic mitral stenosis Qualitative description of valve and sub-valve calcification and fibrosis Measurement of orifice area by planimetry
Investigations in valvular heart disease
 Clinical Medicine 2010, Vol 10, No 2: 172 6 Investigations in valvular heart disease Joanna D Arcy, cardiology registrar; Saul G Myerson, consultant cardiologist Department of Cardiology, John Radcliffe
Clinical Medicine 2010, Vol 10, No 2: 172 6 Investigations in valvular heart disease Joanna D Arcy, cardiology registrar; Saul G Myerson, consultant cardiologist Department of Cardiology, John Radcliffe
Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency
 Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency Rahul R. Jhaveri, MD, Muhamed Saric, MD, PhD, FASE, and Itzhak Kronzon, MD, FASE, New York, New York Background: Two-dimensional
Uncommon Doppler Echocardiographic Findings of Severe Pulmonic Insufficiency Rahul R. Jhaveri, MD, Muhamed Saric, MD, PhD, FASE, and Itzhak Kronzon, MD, FASE, New York, New York Background: Two-dimensional
ECHO HAWAII. Role of Stress Echo in Valvular Heart Disease. Not only ischemia! Cardiomyopathy. Prosthetic Valve. Diastolic Dysfunction
 Role of Stress Echo in Valvular Heart Disease ECHO HAWAII January 15 19, 2018 Kenya Kusunose, MD, PhD, FASE Tokushima University Hospital Japan Not only ischemia! Cardiomyopathy Prosthetic Valve Diastolic
Role of Stress Echo in Valvular Heart Disease ECHO HAWAII January 15 19, 2018 Kenya Kusunose, MD, PhD, FASE Tokushima University Hospital Japan Not only ischemia! Cardiomyopathy Prosthetic Valve Diastolic
ICE: Echo Core Lab-CRF
 APPENDIX 1 ICE: Echo Core Lab-CRF Study #: - Pt Initials: 1. Date of study: / / D D M M M Y Y Y Y 2. Type of Study: TTE TEE 3. Quality of Study: Poor Moderate Excellent Ejection Fraction 4. Ejection Fraction
APPENDIX 1 ICE: Echo Core Lab-CRF Study #: - Pt Initials: 1. Date of study: / / D D M M M Y Y Y Y 2. Type of Study: TTE TEE 3. Quality of Study: Poor Moderate Excellent Ejection Fraction 4. Ejection Fraction
Bogdan A. Popescu. University of Medicine and Pharmacy Bucharest, Romania. EAE Course, Bucharest, April 2010
 Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania EAE Course, Bucharest, April 2010 This is how it started Mitral stenosis at a glance 2D echo narrow diastolic opening of MV leaflets
Bogdan A. Popescu University of Medicine and Pharmacy Bucharest, Romania EAE Course, Bucharest, April 2010 This is how it started Mitral stenosis at a glance 2D echo narrow diastolic opening of MV leaflets
Aortic stenosis (AS) is common with the aging population.
 New Insights Into the Progression of Aortic Stenosis Implications for Secondary Prevention Sanjeev Palta, MD; Anita M. Pai, MD; Kanwaljit S. Gill, MD; Ramdas G. Pai, MD Background The risk factors affecting
New Insights Into the Progression of Aortic Stenosis Implications for Secondary Prevention Sanjeev Palta, MD; Anita M. Pai, MD; Kanwaljit S. Gill, MD; Ramdas G. Pai, MD Background The risk factors affecting
The Doppler Examination. Katie Twomley, MD Wake Forest Baptist Health - Lexington
 The Doppler Examination Katie Twomley, MD Wake Forest Baptist Health - Lexington OUTLINE Principles/Physics Use in valvular assessment Aortic stenosis (continuity equation) Aortic regurgitation (pressure
The Doppler Examination Katie Twomley, MD Wake Forest Baptist Health - Lexington OUTLINE Principles/Physics Use in valvular assessment Aortic stenosis (continuity equation) Aortic regurgitation (pressure
CIPG Transcatheter Aortic Valve Replacement- When Is Less, More?
 CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
CIPG 2013 Transcatheter Aortic Valve Replacement- When Is Less, More? James D. Rossen, M.D. Professor of Medicine and Neurosurgery Director, Cardiac Catheterization Laboratory and Interventional Cardiology
Back to Basics: Common Errors In Quantitation In Everyday Practice
 Back to Basics: Common Errors In Quantitation In Everyday Practice Deborah Agler, ACS, RDCS, FASE October 9, 2017 ASE: Echo Florida Rebecca T. Hahn, MD Director of Interventional Echocardiography Professor
Back to Basics: Common Errors In Quantitation In Everyday Practice Deborah Agler, ACS, RDCS, FASE October 9, 2017 ASE: Echo Florida Rebecca T. Hahn, MD Director of Interventional Echocardiography Professor
Cardiac MRI in ACHD What We. ACHD Patients
 Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Cardiac MRI in ACHD What We Have Learned to Apply to ACHD Patients Faris Al Mousily, MBChB, FAAC, FACC Consultant, Pediatric Cardiology, KFSH&RC/Jeddah Adjunct Faculty, Division of Pediatric Cardiology
Aortic Stenosis: Spectrum of Disease, Low Flow/Low Gradient and Variants
 Aortic Stenosis: Spectrum of Disease, Low Flow/Low Gradient and Variants Martin G. Keane, MD, FASE Professor of Medicine Lewis Katz School of Medicine at Temple University Basic root structure Parasternal
Aortic Stenosis: Spectrum of Disease, Low Flow/Low Gradient and Variants Martin G. Keane, MD, FASE Professor of Medicine Lewis Katz School of Medicine at Temple University Basic root structure Parasternal
Workshop Facing the challenge of TAVI 2016
 Workshop Facing the challenge of TAVI 2016 Congrès annuel de la SSC Lausanne 15 Juin 2016 Pitfalls in the severity assessment of aortic stenosis by echocardiography Hajo Müller, unité d échocardiographie,
Workshop Facing the challenge of TAVI 2016 Congrès annuel de la SSC Lausanne 15 Juin 2016 Pitfalls in the severity assessment of aortic stenosis by echocardiography Hajo Müller, unité d échocardiographie,
How to Assess and Treat Obstructive Lesions
 How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
How to Assess and Treat Obstructive Lesions Erwin Oechslin, MD, FESC, FRCPC, Director, Congenital Cardiac Centre for Adults Peter Munk Cardiac Centre University Health Network/Toronto General Hospital
Balloon mitral valvuloplasty
 Echo for selecting and monitoring procedures in mitral valve diseases Balloon mitral valvuloplasty Eric Brochet,MD Cardiology Department Hôpital Bichat. Paris France Conflict of interest : none Balloon
Echo for selecting and monitoring procedures in mitral valve diseases Balloon mitral valvuloplasty Eric Brochet,MD Cardiology Department Hôpital Bichat. Paris France Conflict of interest : none Balloon
Aortic Regurgitation & Aorta Evaluation
 VALVULAR HEART DISEASE Regurgitation Valvular Lessions 2017 Aortic Regurgitation & Aorta Evaluation Jorge Eduardo Cossío-Aranda MD, FACC Chairman of Outpatient Care Department Instituto Nacional de Cardiología
VALVULAR HEART DISEASE Regurgitation Valvular Lessions 2017 Aortic Regurgitation & Aorta Evaluation Jorge Eduardo Cossío-Aranda MD, FACC Chairman of Outpatient Care Department Instituto Nacional de Cardiología
Aortic stenosis aetiology: morphology of calcific AS,
 How to improve patient selection in aortic stenosis? Fausto J. Pinto, FESC Aortic stenosis aetiology: morphology of calcific AS, bicuspid valve, and rheumatic AS (Adapted from C. Otto, Principles of
How to improve patient selection in aortic stenosis? Fausto J. Pinto, FESC Aortic stenosis aetiology: morphology of calcific AS, bicuspid valve, and rheumatic AS (Adapted from C. Otto, Principles of
Boston, MA 2 Service Chief, Cardiovascular Imaging, Department of Radiology, Massachusetts General Hospital,
 Chapter 9: Cardiac imaging for TAVR: CTA, TTE, TEE, and valve sizing Lucy M. Safi, DO 1 ; Brian Ghoshhajra, MD, MBA 2 ; Jonathan J. Passeri, MD 3 1 Clinical and Research Fellow in Medicine, Massachusetts
Chapter 9: Cardiac imaging for TAVR: CTA, TTE, TEE, and valve sizing Lucy M. Safi, DO 1 ; Brian Ghoshhajra, MD, MBA 2 ; Jonathan J. Passeri, MD 3 1 Clinical and Research Fellow in Medicine, Massachusetts
Introduction. * Corresponding author. Tel: þ ; fax: þ address:
 European Journal of Echocardiography (2009) 10, 420 424 doi:10.1093/ejechocard/jen301 Usefulness of the right parasternal view and non-imaging continuous-wave Doppler transducer for the evaluation of the
European Journal of Echocardiography (2009) 10, 420 424 doi:10.1093/ejechocard/jen301 Usefulness of the right parasternal view and non-imaging continuous-wave Doppler transducer for the evaluation of the
Appendix II: ECHOCARDIOGRAPHY ANALYSIS
 Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Appendix II: ECHOCARDIOGRAPHY ANALYSIS Two-Dimensional (2D) imaging was performed using the Vivid 7 Advantage cardiovascular ultrasound system (GE Medical Systems, Milwaukee) with a frame rate of 400 frames
Tricuspid and Pulmonic Valve Disease
 Chapter 31 Tricuspid and Pulmonic Valve Disease David A. Tate Acquired disease of the right-sided cardiac valves is much less common than disease of the leftsided counterparts, possibly because of the
Chapter 31 Tricuspid and Pulmonic Valve Disease David A. Tate Acquired disease of the right-sided cardiac valves is much less common than disease of the leftsided counterparts, possibly because of the
Affecting the elderly Requiring new approaches. Echocardiographic Evaluation of Hemodynamic Severity. Increasing prevalence Mostly degenerative
 Echocardiographic Evaluation of Hemodynamic Severity Steven J. Lester MD, FACC, FRCP(C), FASE Mayo Clinic, Arizona Relevant Financial Relationship(s) None Off Label Usage None A re-emerging public-health
Echocardiographic Evaluation of Hemodynamic Severity Steven J. Lester MD, FACC, FRCP(C), FASE Mayo Clinic, Arizona Relevant Financial Relationship(s) None Off Label Usage None A re-emerging public-health
Correspondence should be addressed to Jason J. Paquin;
 Computational Medicine, Article ID 419689, 6 pages http://dx.doi.org/1.1155/214/419689 Research Article Reducing the Inconsistency between Doppler and Invasive Measurements of the Severity of Aortic Stenosis
Computational Medicine, Article ID 419689, 6 pages http://dx.doi.org/1.1155/214/419689 Research Article Reducing the Inconsistency between Doppler and Invasive Measurements of the Severity of Aortic Stenosis
When Should I Order a Stress Test or an Echocardiogram
 When Should I Order a Stress Test or an Echocardiogram Updates in Cardiology 2015 March 7, 2015 Donald L. Lappé, MD, FAHA, FACC Chairman, Cardiovascular Department Medical Director, Intermountain Cardiovascular
When Should I Order a Stress Test or an Echocardiogram Updates in Cardiology 2015 March 7, 2015 Donald L. Lappé, MD, FAHA, FACC Chairman, Cardiovascular Department Medical Director, Intermountain Cardiovascular
Clinical material and methods. Clinical Departments of 1 Radiology II and 2 Cardiology, Innsbruck Medical University, Innsbruck, Austria
 Aortic Valve Calcification as Quantified with Multislice Computed Tomography Predicts Short-Term Clinical Outcome in Patients with Asymptomatic Aortic Stenosis Gudrun M. Feuchtner 1, Silvana Müller 2,
Aortic Valve Calcification as Quantified with Multislice Computed Tomography Predicts Short-Term Clinical Outcome in Patients with Asymptomatic Aortic Stenosis Gudrun M. Feuchtner 1, Silvana Müller 2,
2019 Qualified Clinical Data Registry (QCDR) Performance Measures
 2019 Qualified Clinical Data Registry (QCDR) Performance Measures Description: This document contains the 18 performance measures approved by CMS for inclusion in the 2019 Qualified Clinical Data Registry
2019 Qualified Clinical Data Registry (QCDR) Performance Measures Description: This document contains the 18 performance measures approved by CMS for inclusion in the 2019 Qualified Clinical Data Registry
HOW IMPORTANT ARE THESE ECHO MEASUREMENTS ANYWAY?
 HOW IMPORTANT ARE THESE ECHO MEASUREMENTS ANYWAY? John D. Carroll, MD Professor, Director of Interventional Cardiology and Co-Medical Director of the Cardiac and Vascular Center, University of Colorado
HOW IMPORTANT ARE THESE ECHO MEASUREMENTS ANYWAY? John D. Carroll, MD Professor, Director of Interventional Cardiology and Co-Medical Director of the Cardiac and Vascular Center, University of Colorado
Low Gradient Severe AS: Who Qualifies for TAVR? Andrzej Boguszewski MD, FACC, FSCAI Vice Chairman, Cardiology Mid-Michigan Health Associate Professor
 Low Gradient Severe AS: Who Qualifies for TAVR? Andrzej Boguszewski MD, FACC, FSCAI Vice Chairman, Cardiology Mid-Michigan Health Associate Professor Michigan State University, Central Michigan University
Low Gradient Severe AS: Who Qualifies for TAVR? Andrzej Boguszewski MD, FACC, FSCAI Vice Chairman, Cardiology Mid-Michigan Health Associate Professor Michigan State University, Central Michigan University
Cigna - Prior Authorization Procedure List Cardiology
 Cigna - Prior Authorization Procedure List Cardiology Category CPT Code CPT Code Description 33206 Insertion of new or replacement of permanent pacemaker with transvenous electrode(s); atrial 33207 Insertion
Cigna - Prior Authorization Procedure List Cardiology Category CPT Code CPT Code Description 33206 Insertion of new or replacement of permanent pacemaker with transvenous electrode(s); atrial 33207 Insertion
Spotlight on Valvular Heart Disease Guidelines
 Spotlight on Valvular Heart Disease Guidelines Aortic Valve Disease Raphael Rosenhek Department of Cardiology Medical University of Vienna Palermo, April 26 th 2018 1998 2002 2006 2007 2008 2012 2014 2017
Spotlight on Valvular Heart Disease Guidelines Aortic Valve Disease Raphael Rosenhek Department of Cardiology Medical University of Vienna Palermo, April 26 th 2018 1998 2002 2006 2007 2008 2012 2014 2017
A Health Care Professional s Guide Aortic Stenosis in Seniors
 A Health Care Professional s Guide Aortic Stenosis in Seniors With highlights from the 2014 ACC/AHA practice guidelines for valve disease Aortic stenosis (AS) is primarily caused by calcification of the
A Health Care Professional s Guide Aortic Stenosis in Seniors With highlights from the 2014 ACC/AHA practice guidelines for valve disease Aortic stenosis (AS) is primarily caused by calcification of the
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor. Cardiothoracic Radiology
 New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
New Cardiovascular Devices and Interventions: Non-Contrast MRI for TAVR Abhishek Chaturvedi Assistant Professor Cardiothoracic Radiology Disclosure I have no disclosure pertinent to this presentation.
Imaging Assessment of Aortic Stenosis/Aortic Regurgitation
 Imaging Assessment of Aortic Stenosis/Aortic Regurgitation Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2014 Las Vegas Disclosure
Imaging Assessment of Aortic Stenosis/Aortic Regurgitation Craig E Fleishman, MD FACC FASE The Heart Center at Arnold Palmer Hospital for Children, Orlando SCAI Fall Fellows Course 2014 Las Vegas Disclosure
TAVR: Echo Measurements Pre, Post And Intra Procedure
 2017 ASE Florida, Orlando, FL October 10, 2017 8:00 8:25 AM 25 min TAVR: Echo Measurements Pre, Post And Intra Procedure Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
2017 ASE Florida, Orlando, FL October 10, 2017 8:00 8:25 AM 25 min TAVR: Echo Measurements Pre, Post And Intra Procedure Muhamed Sarić MD, PhD, MPA Director of Noninvasive Cardiology Echo Lab Associate
LUST trial. Echocardiography USER S MANUAL
 LUST trial Echocardiography USER S MANUAL Rosa Sicari, Luna Gargani Ins1tute of Clinical Physiology Na1onal Council of Research, Pisa, Italy Parameters required (1) Aortic root Measurement of aortic root
LUST trial Echocardiography USER S MANUAL Rosa Sicari, Luna Gargani Ins1tute of Clinical Physiology Na1onal Council of Research, Pisa, Italy Parameters required (1) Aortic root Measurement of aortic root
Left atrial function. Aliakbar Arvandi MD
 In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
In the clinic Left atrial function Abstract The left atrium (LA) is a left posterior cardiac chamber which is located adjacent to the esophagus. It is separated from the right atrium by the inter-atrial
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/38522 holds various files of this Leiden University dissertation. Author: Ewe, See Hooi Title: Aortic valve disease : novel imaging insights from diagnosis
Cover Page The handle http://hdl.handle.net/1887/38522 holds various files of this Leiden University dissertation. Author: Ewe, See Hooi Title: Aortic valve disease : novel imaging insights from diagnosis
Original Date: October 2009 TRANSESOPHAGEAL (TEE) ECHO Page 1 of 6
 National Imaging Associates, Inc. Clinical guideline Original Date: October 2009 TRANSESOPHAGEAL (TEE) ECHO Page 1 of 6 CPT codes: 93312, 93313, 93314, 93315, Last Review Date: September 2017 93316, 93317,
National Imaging Associates, Inc. Clinical guideline Original Date: October 2009 TRANSESOPHAGEAL (TEE) ECHO Page 1 of 6 CPT codes: 93312, 93313, 93314, 93315, Last Review Date: September 2017 93316, 93317,
Pulmonary Hypertension: Echocardiographic Evaluation of Pulmonary Hypertension and Right Ventricular Function. Irmina Gradus-Pizlo, MD
 Pulmonary Hypertension: Echocardiographic Evaluation of Pulmonary Hypertension and Right Ventricular Function Irmina Gradus-Pizlo, MD Disclosures: Nothing to disclose Overview Is pulmonary hypertension
Pulmonary Hypertension: Echocardiographic Evaluation of Pulmonary Hypertension and Right Ventricular Function Irmina Gradus-Pizlo, MD Disclosures: Nothing to disclose Overview Is pulmonary hypertension
The correlation of AVA measured by transthoracic, transesophageal echocardiography and cardiac CT
 The correlation of AVA measured by transthoracic, transesophageal echocardiography and cardiac CT R.Petr, H.Linkova, J.Knot, E.Paskova, J.Daniel, M.Labos Cardiocenter of University Hospital Kralovske Vinohrady
The correlation of AVA measured by transthoracic, transesophageal echocardiography and cardiac CT R.Petr, H.Linkova, J.Knot, E.Paskova, J.Daniel, M.Labos Cardiocenter of University Hospital Kralovske Vinohrady
«Paradoxical» low-flow, low-gradient AS with preserved LV function: A Silent Killer
 «Paradoxical» low-flow, low-gradient AS with preserved LV function: A Silent Killer Philippe Pibarot, DVM, PhD, FACC, FAHA, FESC, FASE Canada Research Chair in Valvular Heart Diseases Université LAVAL
«Paradoxical» low-flow, low-gradient AS with preserved LV function: A Silent Killer Philippe Pibarot, DVM, PhD, FACC, FAHA, FESC, FASE Canada Research Chair in Valvular Heart Diseases Université LAVAL
Assessment of the severity of aortic stenosis depends on measurement of. Aortic Stenosis: Physics and Physiology What Do the Numbers Really Mean?
 DIAGNOSTIC REVIEW Aortic Stenosis: Physics and Physiology What Do the Numbers Really Mean? Arthur E. Weyman, MD, Marielle Scherrer-Crosbie, MD, PhD Cardiology Division, Massachusetts General Hospital,
DIAGNOSTIC REVIEW Aortic Stenosis: Physics and Physiology What Do the Numbers Really Mean? Arthur E. Weyman, MD, Marielle Scherrer-Crosbie, MD, PhD Cardiology Division, Massachusetts General Hospital,
Prosthesis-Patient Mismatch or Prosthetic Valve Stenosis?
 EuroValves 2015, Nice Prosthesis-Patient Mismatch or Prosthetic Valve Stenosis? Philippe Pibarot, DVM, PhD, FACC, FAHA, FASE FESC Canada Research Chair in Valvular Heart Diseases Université LAVAL Disclosure
EuroValves 2015, Nice Prosthesis-Patient Mismatch or Prosthetic Valve Stenosis? Philippe Pibarot, DVM, PhD, FACC, FAHA, FASE FESC Canada Research Chair in Valvular Heart Diseases Université LAVAL Disclosure
Echocardiography: Guidelines for Valve Quantification
 Echocardiography: Guidelines for Echocardiography: Guidelines for Chamber Quantification British Society of Echocardiography Education Committee Richard Steeds (Chair), Gill Wharton (Lead Author), Jane
Echocardiography: Guidelines for Echocardiography: Guidelines for Chamber Quantification British Society of Echocardiography Education Committee Richard Steeds (Chair), Gill Wharton (Lead Author), Jane
Determinants of symptoms and exercise capacity in aortic stenosis: a comparison of resting haemodynamics and valve compliance during dobutamine stress
 European Heart Journal (2003) 24, 1254 1263 Determinants of symptoms and exercise capacity in aortic stenosis: a comparison of resting haemodynamics and valve compliance during dobutamine stress Paul Das
European Heart Journal (2003) 24, 1254 1263 Determinants of symptoms and exercise capacity in aortic stenosis: a comparison of resting haemodynamics and valve compliance during dobutamine stress Paul Das
MITRAL REGURGITATION ECHO PARAMETERS TOOL
 Comprehensive assessment of qualitative and quantitative parameters, along with the use of standardized nomenclature when reporting echocardiographic findings, helps to better define a patient s MR and
Comprehensive assessment of qualitative and quantitative parameters, along with the use of standardized nomenclature when reporting echocardiographic findings, helps to better define a patient s MR and
Policy #: 222 Latest Review Date: March 2009
 Name of Policy: MRI Phase-Contrast Flow Measurement Policy #: 222 Latest Review Date: March 2009 Category: Radiology Policy Grade: Active Policy but no longer scheduled for regular literature reviews and
Name of Policy: MRI Phase-Contrast Flow Measurement Policy #: 222 Latest Review Date: March 2009 Category: Radiology Policy Grade: Active Policy but no longer scheduled for regular literature reviews and
Pediatric Echocardiography Examination Content Outline
 Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Pediatric Echocardiography Examination Content Outline (Outline Summary) # Domain Subdomain Percentage 1 Anatomy and Physiology Normal Anatomy and Physiology 10% 2 Abnormal Pathology and Pathophysiology
Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM
 The Patient with Aortic Stenosis and Mitral Regurgitation Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM Aortic Stenosis + Mitral Regurgitation?
The Patient with Aortic Stenosis and Mitral Regurgitation Prof. Patrizio LANCELLOTTI, MD, PhD Heart Valve Clinic, University of Liège, CHU Sart Tilman, Liège, BELGIUM Aortic Stenosis + Mitral Regurgitation?
Low Gradient AS Normal LVEF
 Low Gradient AS Normal LVEF Shahbudin H. Rahimtoola MB, FRCP, MACP, MACC, FESC, D.Sc.(Hon) Distinguished Professor University of Southern California Griffith Professor of Cardiology Professor of Medicine
Low Gradient AS Normal LVEF Shahbudin H. Rahimtoola MB, FRCP, MACP, MACC, FESC, D.Sc.(Hon) Distinguished Professor University of Southern California Griffith Professor of Cardiology Professor of Medicine
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine
 Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
Chapter 24: Diagnostic workup and evaluation: eligibility, risk assessment, FDA guidelines Ashwin Nathan, MD, Saif Anwaruddin, MD, FACC Penn Medicine Mitral regurgitation, regurgitant flow between the
evicore cardiology procedures and services requiring prior authorization
 evicore cardiology procedures and services requiring prior authorization Moda Health Commercial Group and Individual Members* *Check EBT to verify member enrollment in evicore program Radiology Advanced
evicore cardiology procedures and services requiring prior authorization Moda Health Commercial Group and Individual Members* *Check EBT to verify member enrollment in evicore program Radiology Advanced
ECHOCARDIOGRAPHY DATA REPORT FORM
 Patient ID Patient Study ID AVM - - Date of form completion / / 20 Initials of person completing the form mm dd yyyy Study period Preoperative Postoperative Operative 6-month f/u 1-year f/u 2-year f/u
Patient ID Patient Study ID AVM - - Date of form completion / / 20 Initials of person completing the form mm dd yyyy Study period Preoperative Postoperative Operative 6-month f/u 1-year f/u 2-year f/u
PROSTHETIC VALVE BOARD REVIEW
 PROSTHETIC VALVE BOARD REVIEW The correct answer D This two chamber view shows a porcine mitral prosthesis with the typical appearance of the struts although the leaflets are not well seen. The valve
PROSTHETIC VALVE BOARD REVIEW The correct answer D This two chamber view shows a porcine mitral prosthesis with the typical appearance of the struts although the leaflets are not well seen. The valve
Aortic Regurgitation and Aortic Aneurysm - Epidemiology and Guidelines -
 Reconstruction of the Aortic Valve and Root - A Practical Approach - Aortic Regurgitation and Aortic Aneurysm Wednesday 14 th September - 9.45 Practice must always be founded on sound theory. Leonardo
Reconstruction of the Aortic Valve and Root - A Practical Approach - Aortic Regurgitation and Aortic Aneurysm Wednesday 14 th September - 9.45 Practice must always be founded on sound theory. Leonardo
Transcatheter Aortic Valve Replacement: Current and Future Devices: How do They Work, Eligibility, Review of Data
 Transcatheter Aortic Valve Replacement: Current and Future Devices: How do They Work, Eligibility, Review of Data Echo Florida 2013 Jonathan J. Passeri, M.D. Co-Director, Heart Valve Program Director,
Transcatheter Aortic Valve Replacement: Current and Future Devices: How do They Work, Eligibility, Review of Data Echo Florida 2013 Jonathan J. Passeri, M.D. Co-Director, Heart Valve Program Director,
PISA Evaluation of Mitral Regurgitation. Raymond Graber, MD Cardiac Anesthesia Group University Hospitals Case Medical Center 4/07/2011
 PISA Evaluation of Mitral Regurgitation Raymond Graber, MD Cardiac Anesthesia Group University Hospitals Case Medical Center 4/07/2011 Introduction Evaluation of MR. What is PISA? Physiologic basis Issues
PISA Evaluation of Mitral Regurgitation Raymond Graber, MD Cardiac Anesthesia Group University Hospitals Case Medical Center 4/07/2011 Introduction Evaluation of MR. What is PISA? Physiologic basis Issues
HISTORY. Question: What category of heart disease is suggested by the fact that a murmur was heard at birth?
 HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
HISTORY 23-year-old man. CHIEF COMPLAINT: Decreasing exercise tolerance of several years duration. PRESENT ILLNESS: The patient is the product of an uncomplicated term pregnancy. A heart murmur was discovered
Right Heart Hemodynamics: Echo-Cath Discrepancies
 Department of cardiac, thoracic and vascular sciences University of Padua, School of Medicine Padua, Italy Right Heart Hemodynamics: Echo-Cath Discrepancies Luigi P. Badano, MD, PhD, FESC, FACC **Dr. Badano
Department of cardiac, thoracic and vascular sciences University of Padua, School of Medicine Padua, Italy Right Heart Hemodynamics: Echo-Cath Discrepancies Luigi P. Badano, MD, PhD, FESC, FACC **Dr. Badano
Section 1: Initial Evaluation for Valvular Heart Disease Table 1: Initial Evaluation of an Asymptomatic Patient
 Section 1: Initial Evaluation for Valvular Heart Disease Table 1: Initial Evaluation of an Asymptomatic Patient Indication 1. Unexplained murmur or abnormal heart sounds 2. Reasonable suspicion of valvular
Section 1: Initial Evaluation for Valvular Heart Disease Table 1: Initial Evaluation of an Asymptomatic Patient Indication 1. Unexplained murmur or abnormal heart sounds 2. Reasonable suspicion of valvular
Outline. EuroScore II. Society of Thoracic Surgeons Score. EuroScore II
 SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
SURGICAL RISK IN VALVULAR HEART DISEASE: WHAT 2D AND 3D ECHO CAN TELL YOU AND WHAT THEY CAN'T Ernesto E Salcedo, MD Professor of Medicine University of Colorado School of Medicine Director of Echocardiography
Optimal Imaging Technique Prior to TAVI -Echocardiography-
 2014 KSC meeting Optimal Imaging Technique Prior to TAVI -Echocardiography- Geu-Ru Hong, M.D. Ph D Associate Professor of Medicine Division of Cardiology, Severance Cardiovascular Hospital Yonsei University
2014 KSC meeting Optimal Imaging Technique Prior to TAVI -Echocardiography- Geu-Ru Hong, M.D. Ph D Associate Professor of Medicine Division of Cardiology, Severance Cardiovascular Hospital Yonsei University
Detailed Order Request Checklists for Cardiology
 Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Next Generation Solutions Detailed Order Request Checklists for Cardiology 8600 West Bryn Mawr Avenue South Tower Suite 800 Chicago, IL 60631 www.aimspecialtyhealth.com Appropriate.Safe.Affordable 2018
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014
 Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Indications of Coronary Angiography Dr. Shaheer K. George, M.D Faculty of Medicine, Mansoura University 2014 Indications for cardiac catheterization Before a decision to perform an invasive procedure such
Adopted by Council March 2006, Revised March 2012, September 2015
 Guidelines, Policies and Statements E4 Education Protocol: Competences Required Of Cardiac Sonographers Who Practice Adult Transthoracic Cardiac Ultrasound Examinations Adopted by Council March 2006, Revised
Guidelines, Policies and Statements E4 Education Protocol: Competences Required Of Cardiac Sonographers Who Practice Adult Transthoracic Cardiac Ultrasound Examinations Adopted by Council March 2006, Revised
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction
 Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
Echocardiographic Cardiovascular Risk Stratification: Beyond Ejection Fraction October 4, 2014 James S. Lee, M.D., F.A.C.C. Associates in Cardiology, P.A. Silver Spring, M.D. Disclosures Financial none
found that some patients without stenotic lesions had blood velocity or pressure measurement across the
 Br Heart J 1985; 53: 640-4 Increased blood velocities in the heart and great vessels of patients with congenital heart disease An assessment of their significance in the absence of valvar stenosis STANLEY
Br Heart J 1985; 53: 640-4 Increased blood velocities in the heart and great vessels of patients with congenital heart disease An assessment of their significance in the absence of valvar stenosis STANLEY
Prosthetic valve dysfunction: stenosis or regurgitation
 Prosthetic valve dysfunction: stenosis or regurgitation Jean G. Dumesnil MD, FRCP(C), FACC, FASE(Hon) Quebec Heart and Lung Institute, Québec, Québec No disclosures Possible Causes of High Gradients in
Prosthetic valve dysfunction: stenosis or regurgitation Jean G. Dumesnil MD, FRCP(C), FACC, FASE(Hon) Quebec Heart and Lung Institute, Québec, Québec No disclosures Possible Causes of High Gradients in
Pre-procedural CT angiography for Transcatheter Aortic Valve Implantation: What a Radiologist Needs to Know?
 Pre-procedural CT angiography for Transcatheter Aortic Valve Implantation: What a Radiologist Needs to Know? E O Dwyer, C O Brien, I Murphy, C Shortt, O Buckley Department of Radiology, AMNCH, Dublin,
Pre-procedural CT angiography for Transcatheter Aortic Valve Implantation: What a Radiologist Needs to Know? E O Dwyer, C O Brien, I Murphy, C Shortt, O Buckley Department of Radiology, AMNCH, Dublin,
Rotation: Echocardiography: Transthoracic Echocardiography (TTE)
 Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Rotation: Echocardiography: Transthoracic Echocardiography (TTE) Rotation Format and Responsibilities: Fellows rotate in the echocardiography laboratory in each clinical year. Rotations during the first
Echocardiography. Guidelines for Valve and Chamber Quantification. In partnership with
 Echocardiography Guidelines for Valve and Chamber Quantification In partnership with Explanatory note & references These guidelines have been developed by the Education Committee of the British Society
Echocardiography Guidelines for Valve and Chamber Quantification In partnership with Explanatory note & references These guidelines have been developed by the Education Committee of the British Society
RIGHT VENTRICULAR SIZE AND FUNCTION
 RIGHT VENTRICULAR SIZE AND FUNCTION Edwin S. Tucay, MD, FPCC, FPCC, FPSE Philippine Society of Echocardiography Quezon City, Philippines Echo Mission, BRTTH, Legaspi City, July 1-2, 2016 NO DISCLOSURE
RIGHT VENTRICULAR SIZE AND FUNCTION Edwin S. Tucay, MD, FPCC, FPCC, FPSE Philippine Society of Echocardiography Quezon City, Philippines Echo Mission, BRTTH, Legaspi City, July 1-2, 2016 NO DISCLOSURE
Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension
 ESC Congress 2011.No 85975 Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension Second Department of Internal
ESC Congress 2011.No 85975 Evaluation of Left Ventricular Diastolic Dysfunction by Doppler and 2D Speckle-tracking Imaging in Patients with Primary Pulmonary Hypertension Second Department of Internal
Sténose aortique à Bas Débit et Bas Gradient
 3.6 m/s Sténose aortique à Bas Débit et Bas Gradient Philippe Pibarot, DVM, PhD, FACC, FAHA, FESC, FASE Canada Research Chair in Valvular Heart Diseases Doctorate Honoris Causa, Université de Liège Institut
3.6 m/s Sténose aortique à Bas Débit et Bas Gradient Philippe Pibarot, DVM, PhD, FACC, FAHA, FESC, FASE Canada Research Chair in Valvular Heart Diseases Doctorate Honoris Causa, Université de Liège Institut
DOPPLER HEMODYNAMICS (1) QUANTIFICATION OF PRESSURE GRADIENTS and INTRACARDIAC PRESSURES
 THORAXCENTRE DOPPLER HEMODYNAMICS (1) QUANTIFICATION OF PRESSURE GRADIENTS and INTRACARDIAC PRESSURES J. Roelandt DOPPLER HEMODYNAMICS Intracardiac pressures and pressure gradients Volumetric measurement
THORAXCENTRE DOPPLER HEMODYNAMICS (1) QUANTIFICATION OF PRESSURE GRADIENTS and INTRACARDIAC PRESSURES J. Roelandt DOPPLER HEMODYNAMICS Intracardiac pressures and pressure gradients Volumetric measurement
Echocardiographic Evaluation of Aortic Valve Prosthesis
 Echocardiographic Evaluation of Aortic Valve Prosthesis Amr E Abbas, MD, FACC, FASE, FSCAI, FSVM, RPVI Co-Director, Echocardiography, Director, Interventional Cardiology Research, Beaumont Health System
Echocardiographic Evaluation of Aortic Valve Prosthesis Amr E Abbas, MD, FACC, FASE, FSCAI, FSVM, RPVI Co-Director, Echocardiography, Director, Interventional Cardiology Research, Beaumont Health System
Planimetric and continuity equation assessment of aortic valve area (AVA): comparison between cardiac magnetic resonance (cmr) and echocardiography
 Planimetric and continuity equation assessment of aortic valve area (AVA): comparison between cardiac magnetic resonance (cmr) and echocardiography Poster No.: C-2058 Congress: ECR 2011 Type: Scientific
Planimetric and continuity equation assessment of aortic valve area (AVA): comparison between cardiac magnetic resonance (cmr) and echocardiography Poster No.: C-2058 Congress: ECR 2011 Type: Scientific
Diagnostic approach to heart disease
 Diagnostic approach to heart disease Initial work up History Physical exam Chest radiographs ECG Special studies Echocardiography Cardiac catheterization Echocardiography principles Technique of producing
Diagnostic approach to heart disease Initial work up History Physical exam Chest radiographs ECG Special studies Echocardiography Cardiac catheterization Echocardiography principles Technique of producing
Stage of Valvular AS. Outline 10/14/16. Low-flow and Other Challenges to the Assessment of Aortic Stenosis. Severe AS
 Low-flow and Other Challenges to the Assessment of Aortic Stenosis Nithima Ratanasit, MD, FACC, FASE Siriraj Hospital, Mahidol University Bangkok, Thailand Outline Types of low-flow aortic stenosis Assessment
Low-flow and Other Challenges to the Assessment of Aortic Stenosis Nithima Ratanasit, MD, FACC, FASE Siriraj Hospital, Mahidol University Bangkok, Thailand Outline Types of low-flow aortic stenosis Assessment
New imaging modalities for assessment of TAVI procedure and results. R Dulgheru, MD Heart Valve Clinic CHU, Liege
 New imaging modalities for assessment of TAVI procedure and results R Dulgheru, MD Heart Valve Clinic CHU, Liege Disclosure of Interest I, Raluca Dulgheru, DO NOT HAVE a financial interest/arrangement
New imaging modalities for assessment of TAVI procedure and results R Dulgheru, MD Heart Valve Clinic CHU, Liege Disclosure of Interest I, Raluca Dulgheru, DO NOT HAVE a financial interest/arrangement
What are the best diagnostic tools to quantify aortic regurgitation?
 What are the best diagnostic tools to quantify aortic regurgitation? Agnès Pasquet, MD, PhD Pôle de Recherche Cardiovasculaire Institut de Recherche Expérimentale et Clinique Université catholique de Louvain
What are the best diagnostic tools to quantify aortic regurgitation? Agnès Pasquet, MD, PhD Pôle de Recherche Cardiovasculaire Institut de Recherche Expérimentale et Clinique Université catholique de Louvain
Tissue Doppler Imaging in Congenital Heart Disease
 Tissue Doppler Imaging in Congenital Heart Disease L. Youngmin Eun, M.D. Department of Pediatrics, Division of Pediatric Cardiology, Kwandong University College of Medicine The potential advantage of ultrasound
Tissue Doppler Imaging in Congenital Heart Disease L. Youngmin Eun, M.D. Department of Pediatrics, Division of Pediatric Cardiology, Kwandong University College of Medicine The potential advantage of ultrasound
The Role of Imaging in Transcatheter Aortic Valve Implantation
 The Role of Imaging in Transcatheter Aortic Valve Implantation Helmut Baumgartner Westfälische Wilhelms-Universität Münster Division of Adult Congenital and Valvular Heart Disease Department of Cardiovascular
The Role of Imaging in Transcatheter Aortic Valve Implantation Helmut Baumgartner Westfälische Wilhelms-Universität Münster Division of Adult Congenital and Valvular Heart Disease Department of Cardiovascular
Chamber Quantitation Guidelines: What is New?
 Chamber Quantitation Guidelines: What is New? Roberto M Lang, MD J AM Soc Echocardiogr 2005; 18:1440-1463 1 Approximately 10,000 citations iase in itune Cardiac Chamber Quantification: What is New? Database
Chamber Quantitation Guidelines: What is New? Roberto M Lang, MD J AM Soc Echocardiogr 2005; 18:1440-1463 1 Approximately 10,000 citations iase in itune Cardiac Chamber Quantification: What is New? Database
Quantitation of right ventricular dimensions and function
 SCCS Basics of cardiac assessment Quantitation of right ventricular dimensions and function Tomasz Kukulski, MD PhD Dept of Cardiology, Congenital Heart Disease and Electrotherapy Silesian Medical University
SCCS Basics of cardiac assessment Quantitation of right ventricular dimensions and function Tomasz Kukulski, MD PhD Dept of Cardiology, Congenital Heart Disease and Electrotherapy Silesian Medical University
