Education Consortium. 8.1* or 6.75** contact hours (see below) 2.5* or 2.08** contact hours (see below)
|
|
|
- Bruno Maxwell
- 5 years ago
- Views:
Transcription
1 . For this class only Course materials that are used during class will be printed for you if you are registered for class. TCHP Education Consortium Advanced 12-Lead ECG Interpretation March 7 th, :30 a.m. 4:00 p.m. Minneapolis VA Health Care System Room 4U 106 (in the Medical Library) Description/Learning Outcome Being able to read ECG rhythms is a must in the critical care, telemetry, emergency, and surgery settings. Why not take it a step further and be able to interpret 12-lead ECG's? Learning Outcomes: After attending this class, the participant will self-report an improvement in their ability to analyze the 12-lead for abnormalities that indicate bundle branch block, myocardial ischemia, injury, and infarction, and non-mi causes of ECG changes. Target Audience/Pre-requisites This class was designed for nurses with at least one year of experience in reading basic ECG rhythms. Before You Come to Class You must complete the Advanced 12-lead ECG Interpretation Primer. 7:30-7:45 a.m. Registration 7:45-8:15 a.m. Introduction to 12-Lead ECG's Cleo Bonham 8:15-9:15 a.m. Bundle Branch Block Cleo Bonham 9:15-9:30 a.m. Break 9:30-10:30 a.m. Bundle Branch Block (con't) Cleo Bonham 10:30-11:30 a.m. The 12 Lead and the Heart: Myocardial Ischemia, Injury, and Infarction 11:30-12:30 p.m. Lunch Cleo Bonham 12:30-2:00 p.m. Practice ECG s Cleo Bonham 2:00-2:15 p.m. Break 2:15-3:00 p.m. Practice ECG s (con t) Cleo Bonham 3:00-4:00 p.m. Potpourri of Patient ECG Problems Cleo Bonham Continuing Education Credit For attending this class, you are eligible to receive: If you complete the primer for this class, you are eligible to receive an additional: 8.1* or 6.75** contact hours (see below) Criteria for successful completion: All participants must attend the program and complete verification and evaluation forms to receive contact hours. If you are an ANCC certified nurse, you must attend the ENTIRE activity to receive contact hours and complete the application process with TCHP. The Twin Cities Health Professionals Education Consortium is an approved provider of continuing nursing education by the Wisconsin Nurses Association, an accredited approver by the American Nurses Credentialing Center's Commission on Accreditation. 2.5* or 2.08** contact hours (see below) Criteria for successful completion for all: You must read the primer, complete the post-test and evaluation, and submit it to TCHP for processing. If you are an ANCC certified nurse, you must complete the application process with TCHP. *Denotes contact hours used for renewing licensure with the MN Board of Nursing or other Board that uses a 50 min/contact hour formula. These contact hours will be issued unless you request contact hours that comply with the ANCC formula. **Denotes contact hours used for renewing Nursing Certification with ANCC or other organization that uses the formula of 60 min/contact hour. You must request these contact hours on the verification form if you need them. Please Read! Check the attached map for directions to the class and assistance with parking. Certificates of attendance will be distributed at the end of the day. You should dress in layers to accommodate fluctuations in room temperature. Food, beverages, and parking costs are your responsibility. If you are unable to attend after registering, please notify the Education Department at your hospital or TCHP at In the case of bad weather, call the TCHP office at and check the answering message to see if a class has been cancelled. If a class has been cancelled, the message will be posted by 5:30 a.m. on the day of the program. More complete class information is available on the TCHP website at
2 Minneapolis VA Health Care System 4U-106 One Veterans Drive Minneapolis, MN Directions to the MVAHCS From the East (St. Paul): Take 35E south to West 7 th /Highway 5 exit. Turn right at the top of the exit ramp. Continue on 5 to the Fort Snelling exit and stay to the right as you follow the exit around. You will Y into traffic coming from the Mendota bridge. Move to the right and exit on 55 west. As you exit on 55 west, it will Y almost immediately. Stay to the left and go straight through the stoplight. You will be on Minnehaha. Follow Minnehaha to the stoplight in front of the VA and turn left into the parking lot. If you miss the Y continue to the next stoplight (54 th ) and turn left. Go to stop sign (Minnehaha) and turn left again. Go to the stoplight in front of the VA and turn right into the parking lot. From the Southeast: Take 35E to 110 W E west. Take the 55 west/fort Snelling exit. Go to the far righthand lane as soon as you S exit to continue on 55 west. Go over the Mendota Bridge, move to the right lane and exit to follow 55 west. As you exit on 55 west, it will Y almost immediately. Stay to the left and go straight through the stoplight. You will be on Minnehaha. Follow Minnehaha to the stoplight in front of the VA and turn left into the parking lot. If you miss the Y continue to the next stoplight (54 th ) and turn left. Go to stop sign (Minnehaha) and turn left again. Go to the stoplight in front of the VA and turn right into the parking lot. From the North: Take 35W south to 62 east. *Follow directions below. From the South: Take 35W north to 62 east. *Follow directions below. From the West: Take 494 east to 35W north. Take 62 east. *Follow directions below. 62 VA Health Care System = stoplight = stop sign Minnehaha *Directions, continued: Get into the right lane on 62 and exit on 55 west. At the top of the exit ramp, turn left to continue on 55 west. Go to the stoplight (Minnehaha) and turn left. Follow Minnehaha to the stoplight in front of the VA and turn left into the lot. For All: Park in the Visitor s Parking Lot to the left (parking is free). Enter through the outpatient entrance and take the elevator to the 4 th floor. Enter the Medical Library that is next to the bank of elevators. 4U-106 is located at the back of the library. Light Rail Transit: The LRT line stops right in front of the VA. Feel free to utilize the park and ride lots and take the LRT to the VA. Go to the LRT website for information about where to park, fares, and how to ride: N 55 west 54 th St 55 east
3 TCHP Education Consortium This home study is pre-reading for a class. ADVANCED 12-LEAD EKG INTER- PRETATION PRIMER 2000, TCHP Education Consortium. Revised 2007, This educational activity expires April 30, All rights reserved. Copying, electronic transmission and sharing without permission is forbidden.
4 ADVANCED 12-LEAD EKG INTERPRETATION PRIMER Introduction/Purpose Statement Recognizing changes on the 12-lead EKG is an important part of monitoring in the critical care and telemetry environments. Learning how to monitor the 12-lead EKG, however, can be an intimidating prospect. The purpose of this primer is to give you a starting point in learning how to interpret 12-lead EKGs. This primer can be used as either a stand-alone educational activity or as an introduction to the "Advanced 12-Lead EKG Interpretation" class. Target Audience This home study was designed for nurses with at least one year of experience in interpreting ECGs; however, other health care professionals are invited to complete this packet. Content Objectives: After Completing This Primer, You Will Be Able To: 1. Describe the electrophysiology behind cardiac electrical action. 2. Identify the normal conduction of electrical current and the waveforms this current produces. 3. Explain the basic factors that influence whether a waveform is upright or negative. 4. Describe the normal waveform configuration in each of the 12 leads. 5. Identify which leads look at which parts of the heart wall. 6. Identify the axis of the QRS complex in two different ways. Disclosures In accordance with ANCC requirements governing approved providers of education, the following disclosures are being made to you prior to the beginning of this educational activity: Requirements for successful completion of this educational activity: In order to successfully complete this activity you must read the home study, complete the post-test and evaluation, and submit them for processing. Conflicts of Interest It is the policy of the Twin Cities Health Professionals Education Consortium to provide balance, independence, and objectivity in all educational activities sponsored by TCHP. Anyone participating in the planning, writing, reviewing, or editing of this program are expected to disclose to TCHP any real or apparent relationships of a personal, professional, or financial nature. There are no conflicts of interest that have been disclosed to the TCHP Education Consortium. Expiration Date for this Activity: As required by ANCC, this continuing education activity must carry an expiration date. The last day that post tests will be accepted for this edition is April 30, 2018 your envelope must be postmarked on or before that day. Page 1
5 Planning Committee/Editors* *Linda Checky, BSN, RN, MBA, Program Manager for TCHP Education Consortium. *Lynn Duane, MSN, RN, Assistant Program Manager for TCHP Education Consortium. Cleo Bonham, MSN, RN, Critical Care Educator at the Minneapolis VA Health Care System. Author Karen Poor, MN, RN, former Program Manager of the TCHP Education Consortium. Content Experts *Cleo Bonham, MSN, RN, Critical Care Educator at the Minneapolis VA Health Care System. Helen Sullinger, MSN, RN, Clinical Practice Specialist in Cardiology at Regions Hospital. *Denotes the expert reviewer for the current edition. Contact Hour Information For completing this Home Study and evaluation, you are eligible to receive: 2.5* or 2.08** contact hours Criteria for successful completion: You must read the home study packet, complete the post-test and evaluation, and submit them to TCHP for processing. The Twin Cities Health Professionals Education Consortium is an approved provider of continuing nursing education by the Wisconsin Nurses Association, an accredited approver by the American Nurses Credentialing Center s Commission on Accreditation. *Denotes contact hours used for renewing licensure with the MN Board of Nursing or other Board that uses a 50 min/contact hour formula. These contact hours will be issued unless you request contact hours that comply with the ANCC formula. **Denotes contact hours used for renewing Nursing Certification with ANCC or other organization that uses the formula of 60 min/contact hour. You must request these contact hours on the evaluation form if you need them. Please see the last page of the packet for information on submitting your post-test and evaluation for contact hours. Page 2
6 INTRODUCTION The 12-lead electrocardiogram is a valuable tool in assessing the heart's electrical activity. It provides information related to dysrhythmias, heart chamber size and position, and cardiac ischemia or infarction. The first sensitive machine for recording the heart's electrical activity was developed in 1903 by Professor Einthoven from the Netherlands. His machine record electrical activity between three pairs of electrodes, which he named "lead I," "lead II," and "lead III." Professor Einthoven's invention allows us today to monitor the electrical activity of the heart in 12 leads. Before reviewing what the twelve leads monitor, we'd like to bring you through a tour of the anatomy and physiology of the heart. A BRIEF HISTORY OF ELECTROPHYSIOLOGY The heart is made up of two types of cells: those that generate or conduct electrical impulses, and those that contract and relax. We are focusing on the electrical cells in this learning activity. Electrical cells have several unique characteristics: automaticity: the cell can generate an electrical impulse without being stimulated excitability: the cell can change its internal electrical balance to reach threshold conductivity: the cell can move an electrical impulse to the next cell The Sodium-Potassium Pump The mechanism that is involved with both automaticity and excitability is called the sodiumpotassium pump. Look at the illustration below to see how it works: Na K N a K K N a Resting state=polarized Potassium is inside the cell, and sodium is outside of the cell. There is nothing happening electrically. Depolarization Potassium leaves the cell and sodium enters the cell very quickly. Repolarization Potassium reenters the cell and sodium leaves the cell more slowly. Page 3
7 The Action Potential The action potential has four phases of resting, depolarization, and repolarization. The fast response is seen with cells that conduct the impulses; the slow response is seen in pacemaker cells: Phase 0: depolarization sodium rushes into the cell Phase 1: initial repolarization chloride rushes in and an the fast inward sodium current is inactivated Phase 2: plateau phase slow inward movement of calcium and slow exit of potassium Fast response Slow response Phase 3: sudden repolarization potassium goes out more quickly and the slow calcium channel is inactivated Time in milliseconds Phase 4 potassium and sodium reverse concentrations to polarized (resting) state All of the information on the ionic movement in the cells is fine for physiologists, but what does it mean for electrocardiographic monitoring? The answer: alterations in the movement of ions can affect what happens electrically in the patient s heart. Another answer: we give medications that affect how the ions move into and out of the cell, such as lidocaine (sodium), calcium channel blockers (calcium), and potassium. The Conduction System The end result of ionic movement and action potential produces an electrical stimulus that is propagated from one cell to the other. The conduction system hooks all of the electrical cells together to conduct an impulse along an organized pathway. SA node AV node Bundle of His Right bundle branch Internodal tracts Left posterior bundle branch Left anterior bundle branch Page 4
8 Flow of Electrical Current In the normal person, the heart is located in the middle of the chest to the left of the mediastinum. The sinoatrial (SA) node is located in the top of the right atrium, the atrioventricular (AV) node is located in the bottom of the atrium, and the bundle branches conduct through the septum and ventricles. Because of this normal flow, the direction of flow (vector) is mainly from downward right to left. Impulse origin and atrial depolarization When the SA node, a pacemaker cell, fires off an impulse, the impulse travels down and toward the right and left atria. The direction -- or vector -- of this flow looks like this: The electrical flow is translated to the ECG as the P wave. The waveform is relatively small normally between 1.5 and 2.5 mm in width and less than 3 mm in height. p Septal depolarization The electrical flow stops briefly at the AV node, then travels quickly down the common bundle (Bundle of His) and through the q right and left bundle branches to the interventricular septum. The depolarization of the septum causes a small deflection a q wave in some leads; and a small r wave in others. Apical and early ventricular depolarization After depolarizing the septum, the impulse moves downward and to the left. This results in a large waveform either an R wave or an S wave. r Page 5
9 Late ventricular depolarization The final stage of depolarization takes place in the furthest stretches of the ventricle. The electrical stimulus moves upward, resulting in either a taller R wave or a smaller S wave. s Ventricular repolarization Finally, the electrical stimulus is completed, ending depolarization. The ions in the cells move back into their normal resting positions, from top to bottom, causing the T wave. The T wave should be the same vector as the mean QRS. t Putting the Whole Thing Together = atrial depolarization = P wave 2 = septal depolarization = Q wave 3 = early ventricular depolarization = tall R or S wave 4 = late ventricular depolarization = taller R wave or S wave after R wave 5 = ventricular repolarization = T wave 2 3 Page 6
10 THE 12-LEAD ELECTROCARDIOGRAM What the 12 Leads See There is one positive and one negative electrode on each lead. Current flows from the negative to the positive electrode. The direction of current flow from one electrode to the other (axis) is compared to the direction of current flow in the heart (vector). If both currents are flowing in the same direction, the waveforms are upright and tall. ECG lead flow (axis) Flow in the heart (vector) If the current in the heart is flowing obliquely to the axis of the lead, the waveforms are upright, but smaller. ECG lead flow (axis) Flow in the heart (vector) If the currents are perpendicular to each other, the waveform is flat. ECG lead flow (axis) Flow in the heart (vector) If the current of the heart is flowing obliquely away from the axis of the lead, the waveforms are deflected weakly downward. ECG lead flow (axis) Flow in the heart (vector) If the current of the heart is flowing directly away from the axis of the lead, the waveforms are deflected strongly downward. ECG lead flow (axis) Flow in the heart (vector) Page 7
11 ECG Waveforms The Isoelectric Line There is a place on the normal ECG rhythm that is electrically neutral - there is nothing electrically happening in the heart at that particular period. This is called the "isoelectric" line. This is located between the end of the T wave and the beginning of the next P wave. P Wave Indicates atrial depolarization Shape - round and smooth The duration of the normal P wave is < 0.11 secs. The height of the normal P wave is < 3 mm. PR Interval The time from the beginning of atrial depolarization to the beginning of ventricular depolarization It is measured from the beginning of the P wave until the start of the QRS complex The normal duration of the PR interval is seconds QRS Complex Represents ventricular depolarization Normal width is < 0.12 seconds (rarely < 0.06 seconds) In the bipolar leads (I, II, III), the value of the positive and negative deflections of the QRS (add the small boxes up and down) should be more than 6 mm. Less than 6 mm indicates low voltage. In the precordial leads (V1-V6), the QRS should be less than 30 mm in height. Where does the QRS complex start? The QRS complex starts with either an upward or downward deflection after the PR interval. If the deflection goes down past the isoelectric line, it is called a "q" wave. If the deflection goes up past the isoelectric line, it is called an "r" wave. Page 8
12 The Q wave The "Q" wave is the first negative deflection before an R wave. If there is no negative deflection before the R wave, there is no "Q". A q wave is normal in leads I, avl, V5 and V6 if it is < 0.04 seconds in width and < 25% the height of the R wave. The R wave The "R" wave is the first positive deflection after the PR interval. It is sometimes preceded by a "Q" wave. In some leads (avr and V1), there may not be an "R" wave. Instead, there may be a "Q" wave and an "S" wave (a QS complex). The S wave The "S" wave is the negative deflection that returns to the isoelectric line. It may be preceded by a "Q" wave, an "R" wave, or both. Where does the QRS complex end? The QRS ends at the "J" point: the point at which the S wave (or the R wave if there is no S wave) turns a corner where the waveform moves in another direction. Below are the J- points as the R or S wave returns to the isoelectric line. ST Segment Represents early ventricular repolarization The normal ST segment can be 1 mm (one small box) above or below the isoelectric line to be normal. The normal ST segment is > 0.08 secs in width. Early repolarization can be seen in some patients, where the ST segment appears to be elevated in leads V2 and V3. This is in fact a T wave that occurs early, and is not significant. Page 9
13 T Wave Represents repolarization of the ventricle The T wave should be < 5 mm in leads I, II, and III and < 10 mm in V1-V6 Refractory periods Absolute or effective refractory period (ERP): The first half of the T wave where an electrical stimulus will not cause a depolarization (regardless of the stimulus strength) Relative refractory period (RRP): The second half of the T wave, where a stronger than normal electrical stimulus may cause a depolarization The Bipolar (Frontal) Leads The first three leads are those that were discovered by Professor Einthoven. His theoretical model is called "Einthoven's Triangle," and looks like the diagram below: RA Lead II Lead I LL LA Lead III RA = right arm LA = left arm LL = left leg Lead I has the negative electrode on the right arm and positive electrode on the left arm. If you will look back to the Putting it All Together picture on the previous page, you will note that the current flows from right to left in Lead I. This flow matches the flow of the P, R, and T wave currents, so those waveforms should be upright. There is a q, representing septal flow, and an s, representing late ventricular depolarization. RA Lead I - LA Page 10
14 Lead II has the negative electrode on the right arm and positive electrode on the left leg. The flow is in almost exactly the same current flow as the heart. The P, R, and T waves are strongly positive, with slightly deeper Q and S waves than in Lead I. RA - Lead II Lead III has the negative electrode on the left arm and positive electrode on the left leg. The waveforms should look much the same as in Lead II, but the positive waveforms will be shorter than in Lead II. In fact, the R wave may be very flat. LL LL - LA Lead III The Augmented Unipolar Leads All unipolar (one pole) leads will have the letter V in the name. The following three leads have only one pole. The thought is that the negative pole is in the center of the heart and the positive pole is a lead on either the right arm, the left arm, or the left leg. Lead avr has the positive electrode on the right arm. The current flow is directly opposite of the heart s flow, so the P wave and T wave are inverted, and there is little or no R wave. Instead, there is often a deeper S wave. Lead avr looks at the right atrium and the upper portion of the right ventricle. RA Page 11
15 Lead avl has the positive electrode on the left arm. The current flow is perpendicular to the mean vector of current flow. There is often a deep Q and S wave, with flat, inverted, or upright P and T waves. Lead avl looks at the left atrium and the upper portion of the left ventricle. LA Lead avf has the positive electrode on the left leg. The current flow is the same as the mean vector of current flow. There is normally an upright P, R, and T wave, with small q and s waves. Lead avf looks at the lower portion of the left ventricle. LL The Precordial Leads The precordial leads are unipolar leads that also assume a negative pole in the center of the heart, just like the augmented leads. The precordial leads measure current flow that indicates what is happening in the right and left ventricles. V1 V2 1 V3 V6 V5 V4 Page 12
16 Lead V1 has the positive electrode at the fourth intercostal space at the right sternal border. It looks at the right ventricle and septum. The P and T" waves may be upright, inverted, or diphasic. Lead V2 has the positive electrode at the fourth intercostal space at the left sternal border. It looks at the right ventricle and septum. The P and T waves are usually upright, but may be inverted, or diphasic. Lead V3 has the positive electrode between the fourth and fifth intercostal space. This lead looks at the anterior wall of the left ventricle. The P and T waves are upright, and the R wave height is approximately the same as the S wave depth. Lead V4 has the positive electrode at the fifth intercostal space and the midclavicular line. This lead also looks at the anterior wall of the left ventricle. The P and T waves are upright, and the R wave height is either the same as or taller than the S wave depth. Either Lead V3 or V4 are known as the transition, where the QRS complex is equally above and below the baseline. Page 13
17 Lead V5 has the positive electrode at the fifth intercostal space and the left axillary line. This lead looks at the anterior and lateral walls of the left ventricle. The P and T waves are upright, and the R wave height is taller than the S wave depth. Lead V6 has the positive electrode at the fifth intercostal space and the left midaxillary line. This lead looks at the lateral wall of the left ventricle. The P and T waves are upright, and the R wave is dominant with only a small S wave (if any at all). Normal ECG Configurations Summary Sheet P wave < 3 mm in height Q wave < 0.04 seconds in width, and < 25% the height of the R wave QRS > 6 mm in I, II, III QRS < 30 mm in V1-V6 Lead P wave Q wave R wave S wave T wave ST segment I upright small largest wave small or none upright, < 5 mm 1 to -0.5 mm II upright none large small or none upright, < 5 mm 1 to -0.5 mm III variable small or none none to large none to large variable 1 to -0.5 mm avr inverted small, none, or small or none large inverted 1 to -0.5 mm large (QS) avl variable small, none, or small, none, none to large variable 1 to -0.5 mm large or large avf upright small or none small or none small, none, variable 1 to -0.5 mm or large V1 variable QS complex small or none large (QS) variable 0 to 2 mm V2 upright none larger than large upright, < 10 mm 0 to 2 mm V1 V3 upright none <, >, or = to S <, >, or = to R upright, < 10 mm 0 to 2 mm wave wave V4 upright none taller than V3 smaller than upright, < 10 mm 1 to -0.5 mm V3 V5 upright small larger than smaller than upright, < 10 mm 1 to -0.5 mm V4 V4 V6 upright small < V5 < V5 upright, 10 mm 1 to -0.5 mm Adapted from Menzel, L.K. (1989). The electrocardiogram during myocardial infarction, AACN Clinical Issues in Critical Care, 3(1), and Conover, M.B. (1996). Understanding Electrocardiography, Mosby. Page 14
18 PRACTICE It's time to practice! Take a look at the following 12-lead EKG's and look at each PQRST complex in each of the leads. In the spaces provided after each EKG, write down whether the complexes are normal or abnormal in each lead. 1. I avr V1 V4 II avl V2 V5 III avf V3 V6 Page 15
19 2. I avr V1 V4 II avl V2 V5 III avf V3 V6 Page 16
20 3. I avr V1 V4 II avl V2 V5 III avf V3 V6 Page 17
21 Answers to the Practice EKGs 1. I: normal II: normal III: normal avr: normal avl: normal avf: normal V1: normal V2: peaked T V3: peaked T V4: peaked T V5: peaked T V6: peaked T early transition at V2 2. I: no Q, large S, T, diphasic T wave II: large S, small R, T, diphasic T III: large S, small R, inverted T avr: normal avl: normal avf: diphasic T V1: diphasic T, QRS upright at V1 V2: QRS upright at V1 V3: QRS upright at V1 V4: depressed ST, QRS upright at V1 V5: depressed ST V6: depressed ST 3. I: normal II: inverted T III: Q wave, elevated ST, inverted T avr: normal avl: normal avf: inverted T V1: inverted T V2: inverted T V3: R<S, inverted T V4: R<S, inverted T V5: inverted T V6: normal late transition at V5 Page 18
22 THE ELECTROCARDIOGRAM In order to interpret the 12-lead EKG, a paper printout is obtained. All EKG paper is standardized, so that the width and height of the boxes can be easily measured in different patients and different facilities. The grid of the paper indicates two things: time and amplitude. The time refers to the milliseconds it takes for a waveform to traverse the heart. The amplitude refers to the voltage of the electrical current. Space between hash marks = 3 seconds Amplitude 1 small square = 1 mm = 0.1 mv 1 big square = 5 mm = 0.5 mv Time 1 small square = 1 mm = 40 milliseconds = 0.04 seconds 1 big square = 5 mm = 200 milliseconds = 0.20 seconds Most of the modern 12-lead EKG machines will be internally calibrated so that the PQRST complexes recorded will be at a standardized height. In other words, when the QRS is not large on the bedside monitor, we can adjust the "gain" or the height of the waveforms. This is helpful for staff to see waveforms the best. The 12-lead, however, depends on a standardized measurement so that the amplitude can be used for measuring the axis and determining chamber hypertrophy. Most of the 12 lead machines will print out measurements and interpretations. Among the things the machine will do: Ventricular rate -- measured in beats per minute PR interval -- measured in milliseconds QRS duration -- measured in milliseconds QT/QTc -- the QT interval and the corrected QT interval in milliseconds The P, R, and T axes Identify the rhythm Identify any chamber enlargement or axis deviation Identify any ST segment, T wave, or Q wave abnormalities as seen in ischemia/infarction Page 19
23 Garbage in - garbage out -- the same principle for computers is in place here. The information given to the computer is all that it has to work with. It is very important to place the leads and connect the cables correctly, have the patient lie still with as little respiratory variation as possible, and to correctly input the patient s age. There are normal variations with age; if the machine doesn't know the age of the patient, it will designate the variations as abnormal. STEPS IN INTERPRETING THE 12-LEAD After you obtain a 12-lead EKG on your patient, what do you do? There is a sequence of steps that are helpful to follow: 1. Assess the rate (atrial and ventricular) and regularity of the underlying rhythm. The 12-lead machine will generally print out a full 12-second strip of the rhythm at the very bottom of the 12- lead. This rhythm strip is generally from either II or V1. 2. Assess the usual intervals and widths: PR interval, QRS width, QT interval. 3. Interpret the rhythm itself. 4. Inspect the P wave: Is it going in the right direction for the lead you're looking at? What is the amplitude and the width? What is the shape of the P wave? Is it diphasic, round, notched, or peaked? 5. Inspect the QRS complex: Is it going in the direction that it should be for the lead you're looking at? What is the amplitude? Are there any Q waves? What is the configuration of the QRS? 6. Inspect the ST segment -- it may be normal if it is one mm above or two mm below the isoelectric line. 7. Inspect the T wave for: direction of deflection shape of the T wave amplitude of the T wave 8. Determine the axis. Page 20
24 Axis Determination One of the most confusing, complex, and aggravating parts of the 12-lead EKG to understand is the axis. We will look at what the axis is, what causes it to go astray, and a few practical ways of determining the axis. What Axis Is The axis is simply this: the direction of current flow. Each waveform (the P, QRS, and T) has an axis. For all practical purposes, the QRS is the axis that is most important. The QRS axis is an average, or mean, of all electrical flow in the ventricles For most people, the QRS axis or vector flows in a direction that puts it between 30 and 105 degrees For other people, the current of flow has moved to the right this is called a right axis deviation. The current flow is between 120 and 180 degrees. This deviation indicates that the right ventricle has enlarged and has moved to the left of the chest. Right axis deviation may be normal in very slender adults. Conditions that may cause right axis deviation include: Right ventricular hypertrophy Pulmonary conditions, such as pulmonary hypertension, COPD, pulmonary embolism Conduction defects, such as left posterior fascicular hemiblock and Wolff-Parkinson-White syndrome Congenital dextrocardia (born with your heart on the right side of your chest rather than the left) Tricuspid insufficiency Pulmonary valve stenosis or insufficiency Right Axis Deviation Page 21
25 Left axis deviation is present when the QRS axis is greater than 30 degrees. Although left axis deviation is normal in obese people, many pathologic conditions may cause LAD, including: Left ventricular hypertrophy Hypertension Aortic stenosis Conduction defects, such as left anterior hemiblock, Wolff- Parkinson-White syndrome, and left bundle branch block Acute inferior MI Elevated diaphragm from ascites or pregnancy Coarctation of the aorta 180 Left Axis Deviation There is a fourth area on the circle: that area between 180 degrees and 90 degrees. This area is called no-man s land or an indeterminate axis or northwest axis. This axis is helpful in determining if a wide-complex tachycardia is ventricular or supraventricular in nature. How To Determine Electrical Axis This section will outline three methods of determining QRS axis -- all of which are relatively easy. There are more complex methods of determining the axis; however, with the reliability of the modern 12-lead EKG machines, it is unusual for a practitioner to calculate the exact axis. Reading the Machine Method With the advent of the computerized 12-lead machines, and subsequent improvements, the easiest (and probably most accurate) way of determining the axis is by reading the machine print-out. The machine will come up with three numbers: the P wave axis, the QRS axis, and the T wave axis. Leads I and II Method This is the easiest method of determining axis, involving only memorization and the ability to monitor these leads on the bedside monitor. If the QRS complex is biphasic -- some of it is above and some of it is below the isoelectric line -- you will need to count the number of boxes above and below the isoelectric line to determine if the QRS is more positive or more negative. Normal Left axis deviation Right axis deviation No man s land Page 22
26 Quadrant Method This method requires monitoring for both Lead I and Lead avf. Looking first at Lead I, determine whether the majority of the QRS complex is positive or negative. If the QRS is mostly positive, shade the area that is to the right of the vertical line. If it is mostly negative, shade to the left of the vertical line. You may need to count the number of small boxes above and below the isoelectric line to determine whether the QRS is more positive or more negative. No man s land - Right axis deviation - Left axis deviation Normal Lead I Next, look at Lead avf. If the QRS complex is positive, shade the underneath the horizontal line. If it is mostly negative, shade on top of the horizontal line. The area where two shaded areas meet is the axis determination. Lead avf In the following example, Lead I is mostly positive and avf is mostly positive. The right of the vertical line was shaded, as was underneath the horizontal line. The intersecting quadrant was normal. - Lead I - No man s land Left axis deviation Lead I Right axis Normal Lead avf Lead avf Page 23
27 PRACTICE For each of the sets of QRS complexes below, calculate the QRS axis using both methods. Check your answers on the page following the practice sets! 1. Lead I Lead II Lead III Lead avf Leads I & II Method Quadrant Method 2. Lead I Lead II Lead III Lead avf Leads I & II Method Quadrant Method 3. Lead I Lead II Lead III Lead avf Leads I & II Method Quadrant Method Page 24
28 4. Lead I Lead II Lead III Lead avf Leads I & II Method Quadrant Method 5. Lead I Lead II Lead III Lead avf Leads I & II Method Quadrant Method 6. Lead I Lead II Lead III Lead avf Leads I & II Method Quadrant Method Page 25
29 Answers to the Axis Practice Questions 1. Leads I & II Method: Normal axis Quadrant Method: Normal axis 2. Leads I & II Method: Right axis deviation Quadrant Method: Right axis deviation 3. Leads I & II Method: Left axis deviation Quadrant Method: Left axis deviation 4. Leads I & II Method: Normal Quadrant Method: Normal 5. Leads I & II Method: Left axis deviation Quadrant Method: Left axis deviation 6. Leads I & II Method: No man's land Quadrant Method: No man's land Comments : An axis in "no man's land" usually indicates a ventricular origin of the QRS. Look to see if the QRS complex is wide. Page 26
30 MONITORING FOR MYOCARDIAL ISCHEMIA One of the prime reasons for performing a 12-lead EKG is to assess for myocardial ischemia, injury, or infarction. If myocardial hypoxia is suspected, the practitioner should look closely at all 12 leads, paying particular attention to those leads that show T wave inversion, ST segment changes, or Q wave development. Coronary Blood Supply Every cell and every tissue in the body needs oxygen. The heart is no exception. The heart receives oxygenated blood through a series of arteries, called the coronary arteries. The coronary arteries originate in the coronary ostia, located just under the flaps of the aortic valve. Because they are compressed during systole, coronary artery filling primarily occurs during diastole. Aorta Right coronary artery Posterior descending artery Left main coronary artery Left circumflex Left anterior descending artery Diagonal arteries Acute marginal branch The RCA The right coronary artery provides blood to the right atrium, right ventricle, and part of the interventricular septum. The first branch of the RCA is called the acute marginal branch, and it supplies the inferior surface of the right ventricle. In about 85% of people, the RCA also branches into the posterior descending artery, which supplies the right ventricular and the inferior wall of the left ventricle. The RCA and its branches supply the SA node in about 55% of hearts, and the AV node in 90% of hearts. The LMCA The left main coronary artery is quite short (1-25 mm) and branches almost immediately into the left anterior descending (LAD) and circumflex arteries. Page 27
31 LAD The LAD supplies much of the left ventricle -- the anterior two thirds of the interventricular septum, the anterior wall of the left ventricle, the right bundle branch, and part of the left bundle branch. Circumflex The circumflex (usually referred to as the "circ") supplies the AV node in the remaining 10% of hearts and the SA node in 45% of hearts. The obtuse marginal branch (OMD) of the circumflex artery -- not seen in the diagram -- runs around the back of the left heart and supplies the lateral and posterior surface of the LV. The other branch that may arise from the circumflex is the posterior descending artery (PDA) -- this occurs in about 15% of people. Collateral Circulation Over time, connections between the different arteries are made. This is a beneficial thing! With collateral circulation, an occlusion of one artery does not mean that the entire distal myocardium will be deprived of oxygen. Collateral connections -- or anastomoses -- go throughout the entire thickness of the myocardium, but the greatest number of collaterals are found near the endocardial surface. What speeds up collateral development? Increases in oxygen demand -- atherosclerotic heart disease, chronic anemia, hypoxia, hypertension, cardiomyopathy. What's the downside of collateral circulation? Collateral vessels work well in supplying the heart with oxygen at rest, but the effectiveness of this circulation is lost when the myocardial oxygen consumption (MVO2) increases with exercise. The Pathophysiology of Myocardial Ischemia, Injury, and Infarction Infarction Injury There are three degrees of hypoxia in tissues: ischemia, injury, and infarction. If injury is present, so is ischemia. If infarction is present, ischemia and injury are also -- like a big bruise: purple on the inside, gradually getting lighter on the outer edges. Ischemia 1. Ischemia is the result of inadequate blood or oxygen supply to the myocardium. EKG changes in repolarization are seen due to changes in the electrical potential of cells in the ischemic area. Page 28
32 2. The second degree of hypoxia is injury. Changes in the EKG are related to incomplete depolarization in the injured area. The injured area becomes more positive than the other tissue because of the release of hydrogen ions (H) from damaged cells, so the electrical impulse will travel toward that positive area. 3. The final degree of myocardial hypoxia is infarction. An infarction means that the cells die from lack of blood supply and/or oxygen. The area of death becomes electrically silent, causing the electrode that faces the area to record an abnormal negative deflection. Types of Myocardial Infarctions One way of categorizing myocardial infarctions is to determine the extent of the damage in terms of the number of layers the hypoxia has affected. 1. The transmural MI is one in which the entire thickness of the muscle wall is affected -- the epi, myo, and endocardium. This type of MI gives us the biggest EKG changes. 2. The intramural MI occurs only within the myocardium and does not affect the epicardium or endocardium. This type of MI is not common. 3. The third type is a subepicardial MI -- an MI in which damage to the epicardium (the outer layer) is seen. Again, this type of MI is not common. 4. And last, the subendocardial MI entails involvement of the inner layer of the cardiac wall only. This layer of the heart has a poorer blood supply than the other layers and so is more vulnerable to decreased blood supply. Why doesn't it have a good blood supply? First, during systole, the blood vessels in this layer of the heart get very, very compressed. Diastole is the only time that the subendocardial vessels are perfused. Second, the subendocardial vessels can only dilate to a certain extent, and when the other layers of the heart are starved, they will actually steal blood away from the subendocardial vessels. This type of MI is of particularly concern to practitioners because of the lack of good 12-lead signs. Page 29
33 The Eyes of the 12-Leads The leads that look at specific parts of the heart can be grouped together. The groups of leads include the: Inferior leads: II, III, avf Anterior leads: V1-V4 Lateral leads: I, avl, V5-V6 Posterior leads: V1-V3 avr V1-2 1 V1-4 V5-6 I avl Looking At the Heart Imagine that the bipolar and unipolar leads are like eyes -- they look up or down at the area of the myocardium. Lead avr looks primarily at the right atrium; it is the least useful of all of the 12 leads. Leads I and avl look from the left arm toward the lateral wall of the left ventricle. Leads II, III, and avf all look up toward the inferior wall of the left ventricle. II III avf Leads V1 and V2 look through the heart to the interventricular septum and left ventricle. In combination with V3 and V4, these four leads can see the bulk of the anterior left ventricle. Lastly, V5 and V6 look directly into the lateral wall of the left ventricle. You may notice that there are no leads that look directly at the right ventricle. This is because the left ventricular electrical current overpowers that of the right and because of the size of the left ventricle. Special leads, known as V1-6R need to be placed on the right side of the chest to assess the right ventricle. SUMMARY This independent-learning activity was designed to give you some of the basic principles of 12- lead EKG interpretation. Understanding what happens electrically in the heart, what each lead of the 12-lead EKG monitors, which leads reflect the different parts of the heart, and how to determine the QRS axis will start you on the path to understanding 12-lead EKGs. Page 30
34 BIBLIOGRAPHY Phalen, T. and Aehlert, B. (2012). The 12 Lead ECG in Acute Coronary Syndromes, 3 rd ed. Elsevier Mosby, Maryland Heights, MO. DIRECTIONS FOR SUBMITTING YOUR POST TEST FOR CONTACT HOURS 1. Go to the TCHP website Home Study page to get the electronic post-test: 2. The electronic post-test will take you to a quick and easy Survey Monkey post-test and evaluation. Fill in your answers and click done. Your certificate of completion will be sent to you in a week or 2 (Note: This process is not automatic so do not expect an immediate return of a certificate of completion). If you are having difficulty with Survey Monkey, please contact tchp@hcmed.org for help. Be sure to complete all the information requested on the post-test and evaluation. If required items are skipped, your post-test will automatically be classified as Incomplete in the survey system. The date recorded on your certificate of completion will be the date that your home study is received by TCHP. Any materials received with a time stamp after the expiration will be discarded. TCHP is not responsible for lost or misdirected mail/ . We suggest that you print out your post-test before submitting to keep a copy for your records as the post-test will not be returned with the certificate of completion. Page 31
Education Consortium. 8.1 Minnesota Board of Nursing contact hours / 6.75 ANCC contact hours.
 . For this class only Course materials that are used during class will be printed for you if you are registered for class. TCHP Education Consortium Advanced 12-Lead ECG Interpretation May 19, 2014 7:30
. For this class only Course materials that are used during class will be printed for you if you are registered for class. TCHP Education Consortium Advanced 12-Lead ECG Interpretation May 19, 2014 7:30
Education Consortium. For attending this class, you are eligible to receive:
 Bring money for Calipers TCHP Education Consortium ECG Rhythm Interpretation June 16 th & 19 th, 2017 7:30 a.m. - 3:30 p.m. Minneapolis VA Health Care System Room 4U-106 (in the Medical Library) For this
Bring money for Calipers TCHP Education Consortium ECG Rhythm Interpretation June 16 th & 19 th, 2017 7:30 a.m. - 3:30 p.m. Minneapolis VA Health Care System Room 4U-106 (in the Medical Library) For this
12-Lead ECG Interpretation. Kathy Kuznar, RN, ANP
 12-Lead ECG Interpretation Kathy Kuznar, RN, ANP The 12-Lead ECG Objectives Identify the normal morphology and features of the 12- lead ECG. Perform systematic analysis of the 12-lead ECG. Recognize abnormalities
12-Lead ECG Interpretation Kathy Kuznar, RN, ANP The 12-Lead ECG Objectives Identify the normal morphology and features of the 12- lead ECG. Perform systematic analysis of the 12-lead ECG. Recognize abnormalities
TCHP. Nursing Care of the Telemetry Patient. Education Consortium
 TCHP You must print out your own course materials! None will be available at the class. Click on the link below to access: www.tchpeducation.com/coursebooks/coursebooks_main.htm If the link does not work,
TCHP You must print out your own course materials! None will be available at the class. Click on the link below to access: www.tchpeducation.com/coursebooks/coursebooks_main.htm If the link does not work,
By the end of this lecture, you will be able to: Understand the 12 lead ECG in relation to the coronary circulation and myocardium Perform an ECG
 By the end of this lecture, you will be able to: Understand the 12 lead ECG in relation to the coronary circulation and myocardium Perform an ECG recording Identify the ECG changes that occur in the presence
By the end of this lecture, you will be able to: Understand the 12 lead ECG in relation to the coronary circulation and myocardium Perform an ECG recording Identify the ECG changes that occur in the presence
12 Lead ECG Skills: Building Confidence for Clinical Practice. Presented By: Cynthia Webner, BSN, RN, CCRN-CMC. Karen Marzlin, BSN, RN,CCRN-CMC
 12 Lead ECG Skills: Building Confidence for Clinical Practice NTI 2009 Preconference Session 803 Presented By: Karen Marzlin, BSN, RN,CCRN-CMC 1 12 Lead ECG Fundamentals: The Starting Place for Linking
12 Lead ECG Skills: Building Confidence for Clinical Practice NTI 2009 Preconference Session 803 Presented By: Karen Marzlin, BSN, RN,CCRN-CMC 1 12 Lead ECG Fundamentals: The Starting Place for Linking
ELECTROCARDIOGRAPHY (ECG)
 ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
ELECTROCARDIOGRAPHY (ECG) The heart is a muscular organ, which pumps blood through the blood vessels of the circulatory system. Blood provides the body with oxygen and nutrients, as well as assists in
ECG. Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13
 ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
ECG Prepared by: Dr.Fatima Daoud Reference: Guyton and Hall Textbook of Medical Physiology,12 th edition Chapters: 11,12,13 The Concept When the cardiac impulse passes through the heart, electrical current
Education Consortium. You must have attended the ECG Rhythm Interpretation class or complete the ECG Rhythm Interpretation Primer before class time.
 TCHP You must print out your own course materials! None will be available at the class. Click on the link below to access: www.tchpeducation.com/coursebooks/coursebooks_main.htm If the link does not work,
TCHP You must print out your own course materials! None will be available at the class. Click on the link below to access: www.tchpeducation.com/coursebooks/coursebooks_main.htm If the link does not work,
Relax and Learn At the Farm 2012
 Relax and Learn At the Farm 2012 Session 2: 12 Lead ECG Fundamentals 101 Cynthia Webner DNP, RN, CCNS, CCRN-CMC, CHFN Though for Today Mastery is not something that strikes in an instant, like a thunderbolt,
Relax and Learn At the Farm 2012 Session 2: 12 Lead ECG Fundamentals 101 Cynthia Webner DNP, RN, CCNS, CCRN-CMC, CHFN Though for Today Mastery is not something that strikes in an instant, like a thunderbolt,
Electrocardiogram ECG. Hilal Al Saffar FRCP FACC College of medicine,baghdad University
 Electrocardiogram ECG Hilal Al Saffar FRCP FACC College of medicine,baghdad University Tuesday 29 October 2013 ECG introduction Wednesday 30 October 2013 Abnormal ECG ( ischemia, chamber hypertrophy, heart
Electrocardiogram ECG Hilal Al Saffar FRCP FACC College of medicine,baghdad University Tuesday 29 October 2013 ECG introduction Wednesday 30 October 2013 Abnormal ECG ( ischemia, chamber hypertrophy, heart
Introduction to ECG Gary Martin, M.D.
 Brief review of basic concepts Introduction to ECG Gary Martin, M.D. The electrical activity of the heart is caused by a sequence of rapid ionic movements across cell membranes resulting first in depolarization
Brief review of basic concepts Introduction to ECG Gary Martin, M.D. The electrical activity of the heart is caused by a sequence of rapid ionic movements across cell membranes resulting first in depolarization
12 Lead ECG. Presented by Rebecca Sevigny BSN, RN Professional Practice & Development Dept.
 12 Lead ECG Presented by Rebecca Sevigny BSN, RN Professional Practice & Development Dept. Two Main Coronary Arteries RCA LCA which branches into Left Anterior Descending Circumflex Artery Two Main Coronary
12 Lead ECG Presented by Rebecca Sevigny BSN, RN Professional Practice & Development Dept. Two Main Coronary Arteries RCA LCA which branches into Left Anterior Descending Circumflex Artery Two Main Coronary
Introduction to Electrocardiography
 Introduction to Electrocardiography Class Objectives: Introduction to ECG monitoring Discuss principles of interpretation Identify the components and measurements of the ECG ECG analysis ECG Monitoring
Introduction to Electrocardiography Class Objectives: Introduction to ECG monitoring Discuss principles of interpretation Identify the components and measurements of the ECG ECG analysis ECG Monitoring
12 Lead ECG Interpretation: Color Coding for MI s
 12 Lead ECG Interpretation: Color Coding for MI s Anna E. Story, RN, MS Director, Continuing Professional Education Critical Care Nurse Online Instructional Designer 2004 Anna Story 1 Objectives review
12 Lead ECG Interpretation: Color Coding for MI s Anna E. Story, RN, MS Director, Continuing Professional Education Critical Care Nurse Online Instructional Designer 2004 Anna Story 1 Objectives review
INTRODUCTION TO ECG. Dr. Tamara Alqudah
 INTRODUCTION TO ECG Dr. Tamara Alqudah Excitatory & conductive system of the heart + - The ECG The electrocardiogram, or ECG, is a simple & noninvasive diagnostic test which records the electrical
INTRODUCTION TO ECG Dr. Tamara Alqudah Excitatory & conductive system of the heart + - The ECG The electrocardiogram, or ECG, is a simple & noninvasive diagnostic test which records the electrical
Consortium. ECG Rhythm Interpretation April 9 th and 10 th, :30 a.m. - 3:30 p.m. Hennepin County Medical Center Room BL.320
 For this class only Course materials that are used during class will be printed for you ( excluding primer) if you are registered for class. TCHP Education Consortium ECG Rhythm Interpretation April 9
For this class only Course materials that are used during class will be printed for you ( excluding primer) if you are registered for class. TCHP Education Consortium ECG Rhythm Interpretation April 9
Full file at
 MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
MULTIPLE CHOICE. Choose the one alternative that best completes the statement or answers the question. 1) What electrical event must occur for atrial kick to occur? 1) A) Atrial repolarization B) Ventricular
Electrocardiography for Healthcare Professionals. Chapter 14 Basic 12-Lead ECG Interpretation
 Electrocardiography for Healthcare Professionals Chapter 14 Basic 12-Lead ECG Interpretation 2012 The Companies, Inc. All rights reserved. Learning Outcomes 14.1 Discuss the anatomic views seen on a 12-lead
Electrocardiography for Healthcare Professionals Chapter 14 Basic 12-Lead ECG Interpretation 2012 The Companies, Inc. All rights reserved. Learning Outcomes 14.1 Discuss the anatomic views seen on a 12-lead
This presentation will deal with the basics of ECG description as well as the physiological basics of
 Snímka 1 Electrocardiography basics This presentation will deal with the basics of ECG description as well as the physiological basics of Snímka 2 Lecture overview 1. Cardiac conduction system functional
Snímka 1 Electrocardiography basics This presentation will deal with the basics of ECG description as well as the physiological basics of Snímka 2 Lecture overview 1. Cardiac conduction system functional
BASIC CONCEPT OF ECG
 BASIC CONCEPT OF ECG Electrocardiogram The electrocardiogram (ECG) is a recording of cardiac electrical activity. The electrical activity is readily detected by electrodes attached to the skin. After the
BASIC CONCEPT OF ECG Electrocardiogram The electrocardiogram (ECG) is a recording of cardiac electrical activity. The electrical activity is readily detected by electrodes attached to the skin. After the
ECG CONVENTIONS AND INTERVALS
 1 ECG Waveforms and Intervals ECG waveforms labeled alphabetically P wave== represents atrial depolarization QRS complex=ventricular depolarization ST-T-U complex (ST segment, T wave, and U wave)== V repolarization.
1 ECG Waveforms and Intervals ECG waveforms labeled alphabetically P wave== represents atrial depolarization QRS complex=ventricular depolarization ST-T-U complex (ST segment, T wave, and U wave)== V repolarization.
12 Lead ECG Interpretation
 12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
12 Lead ECG Interpretation Julie Zimmerman, MSN, RN, CNS, CCRN Significant increase in mortality for every 15 minutes of delay! N Engl J Med 2007;357:1631-1638 Who should get a 12-lead ECG? Also include
EKG. Danil Hammoudi.MD
 EKG Danil Hammoudi.MD What is an EKG? The electrocardiogram (EKG) is a representation of the electrical events of the cardiac cycle. Each event has a distinctive waveform, the study of which can lead to
EKG Danil Hammoudi.MD What is an EKG? The electrocardiogram (EKG) is a representation of the electrical events of the cardiac cycle. Each event has a distinctive waveform, the study of which can lead to
5- The normal electrocardiogram (ECG)
 5- The (ECG) Introduction Electrocardiography is a process of recording electrical activities of heart muscle at skin surface. The electrical current spreads into the tissues surrounding the heart, a small
5- The (ECG) Introduction Electrocardiography is a process of recording electrical activities of heart muscle at skin surface. The electrical current spreads into the tissues surrounding the heart, a small
- why the T wave is deflected upwards although it's a repolarization wave?
 Cardiac Electrograph: - why the T wave is deflected upwards although it's a repolarization wave? After depolarization the ventricle contracts but since the heart is a volume conductor (3D not 2D), when
Cardiac Electrograph: - why the T wave is deflected upwards although it's a repolarization wave? After depolarization the ventricle contracts but since the heart is a volume conductor (3D not 2D), when
ECG WORKBOOK. Rohan Jayasinghe
 ECG WORKBOOK Rohan Jayasinghe Contents Preface vii Foreword viii Acknowledgements ix The author x Reviewers xi Section 1 Basics of the ECG 1 Section 2 ECG-based diagnosis: pathology by ECG 21 Section 3
ECG WORKBOOK Rohan Jayasinghe Contents Preface vii Foreword viii Acknowledgements ix The author x Reviewers xi Section 1 Basics of the ECG 1 Section 2 ECG-based diagnosis: pathology by ECG 21 Section 3
Family Medicine for English language students of Medical University of Lodz ECG. Jakub Dorożyński
 Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
Family Medicine for English language students of Medical University of Lodz ECG Jakub Dorożyński Parts of an ECG The standard ECG has 12 leads: six of them are considered limb leads because they are placed
Electrocardiography Abnormalities (Arrhythmias) 7. Faisal I. Mohammed, MD, PhD
 Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
Electrocardiography Abnormalities (Arrhythmias) 7 Faisal I. Mohammed, MD, PhD 1 Causes of Cardiac Arrythmias Abnormal rhythmicity of the pacemaker Shift of pacemaker from sinus node Blocks at different
also aid the clinician in recognizing both the obvious and subtle abnormalities that may help guide therapy.
 Karen Lieberman, MS, CRNP f the many diagnostic tools used to screen for and evaluate cardiac abnormalities, the 12-lead electrocardiogram (ECG) is among the most basic. This inexpensive and noninvasive
Karen Lieberman, MS, CRNP f the many diagnostic tools used to screen for and evaluate cardiac abnormalities, the 12-lead electrocardiogram (ECG) is among the most basic. This inexpensive and noninvasive
12 LEAD EKG & CXR INTERPRETATION.
 12 LEAD EKG & CXR INTERPRETATION www.cherylherrmann.com cherrmann@frontier.com Audio Product Recording discount for participants $60 Nonparticipants = $190 o Get CEs and manual https://catalog.vyne.com
12 LEAD EKG & CXR INTERPRETATION www.cherylherrmann.com cherrmann@frontier.com Audio Product Recording discount for participants $60 Nonparticipants = $190 o Get CEs and manual https://catalog.vyne.com
REtrive. REpeat. RElearn Design by. Test-Enhanced Learning based ECG practice E-book
 Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning Test-Enhanced Learning based ECG practice E-book REtrive REpeat RElearn Design by S I T T I N U N T H A N G J U I P E E R I Y A W A
Understanding basics of EKG
 Understanding basics of EKG By Alula A.(R III) www.le.ac.uk Topic for discussion Understanding of cellular electrophysiology Basics Rate Rhythm Axis Intervals P wave QRS ST/T wave Abnormal EKGs Understanding
Understanding basics of EKG By Alula A.(R III) www.le.ac.uk Topic for discussion Understanding of cellular electrophysiology Basics Rate Rhythm Axis Intervals P wave QRS ST/T wave Abnormal EKGs Understanding
CARDIOVASCULAR SYSTEM
 CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CARDIOVASCULAR SYSTEM Overview Heart and Vessels 2 Major Divisions Pulmonary Circuit Systemic Circuit Closed and Continuous Loop Location Aorta Superior vena cava Right lung Pulmonary trunk Base of heart
CASE 10. What would the ST segment of this ECG look like? On which leads would you see this ST segment change? What does the T wave represent?
 CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
CASE 10 A 57-year-old man presents to the emergency center with complaints of chest pain with radiation to the left arm and jaw. He reports feeling anxious, diaphoretic, and short of breath. His past history
The Electrocardiogram part II. Dr. Adelina Vlad, MD PhD
 The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
The Electrocardiogram part II Dr. Adelina Vlad, MD PhD Basic Interpretation of the ECG 1) Evaluate calibration 2) Calculate rate 3) Determine rhythm 4) Determine QRS axis 5) Measure intervals 6) Analyze
Cardiovascular System Notes: Heart Disease & Disorders
 Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Cardiovascular System Notes: Heart Disease & Disorders Interesting Heart Facts The Electrocardiograph (ECG) was invented in 1902 by Willem Einthoven Dutch Physiologist. This test is still used to evaluate
Axis. B.G. Petty, Basic Electrocardiography, DOI / _2, Springer Science+Business Media New York 2016
 Axis 2 The electrical axis of any electrocardiogram (EKG) waveform is the average direction of electrical activity. It is not a vector, because by definition a vector has both direction and amplitude,
Axis 2 The electrical axis of any electrocardiogram (EKG) waveform is the average direction of electrical activity. It is not a vector, because by definition a vector has both direction and amplitude,
Lab Activity 24 EKG. Portland Community College BI 232
 Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
Lab Activity 24 EKG Reference: Dubin, Dale. Rapid Interpretation of EKG s. 6 th edition. Tampa: Cover Publishing Company, 2000. Portland Community College BI 232 Graph Paper 1 second equals 25 little boxes
Ask Mish. EKG INTERPRETATION part i
 EKG INTERPRETATION part i What is EKG? EKG or ECG= electrocardiogram(~graphy) means the recording of the heart electrical activity from Greek kardio= heart, graphein= to write cardiac cell physiology Cardiac
EKG INTERPRETATION part i What is EKG? EKG or ECG= electrocardiogram(~graphy) means the recording of the heart electrical activity from Greek kardio= heart, graphein= to write cardiac cell physiology Cardiac
The Fundamentals of 12 Lead EKG. ECG Recording. J Point. Reviewing the Cardiac Conductive System. Dr. E. Joe Sasin, MD Rusty Powers, NRP
 The Fundamentals of 12 Lead EKG Dr. E. Joe Sasin, MD Rusty Powers, NRP SA Node Intranodal Pathways AV Junction AV Fibers Bundle of His Septum Bundle Branches Purkinje System Reviewing the Cardiac Conductive
The Fundamentals of 12 Lead EKG Dr. E. Joe Sasin, MD Rusty Powers, NRP SA Node Intranodal Pathways AV Junction AV Fibers Bundle of His Septum Bundle Branches Purkinje System Reviewing the Cardiac Conductive
Ekg pra pr c a tice D.HAMMOUDI.MD
 Ekg practice D.HAMMOUDI.MD Anatomy Revisited RCA (Right Coronary Artery) Right ventricle Inferior wall of LV Posterior wall of LV (75%) SA Node (60%) AV Node (>80%) LCA (Left Coronary Artery) Septal wall
Ekg practice D.HAMMOUDI.MD Anatomy Revisited RCA (Right Coronary Artery) Right ventricle Inferior wall of LV Posterior wall of LV (75%) SA Node (60%) AV Node (>80%) LCA (Left Coronary Artery) Septal wall
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH
 ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
ECG ABNORMALITIES D R. T AM A R A AL Q U D AH When we interpret an ECG we compare it instantaneously with the normal ECG and normal variants stored in our memory; these memories are stored visually in
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC
 Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Matters of the Heart: Comprehensive Cardiology SARAH BEANLANDS RN BSCN MSC Who am I? Class Outline Gross anatomy of the heart Trip around the heart Micro anatomy: cellular and tissue level Introduction
Electrocardiography Normal 5. Faisal I. Mohammed, MD, PhD
 Electrocardiography Normal 5 Faisal I. Mohammed, MD, PhD 1 Objectives 2 1. Describe the different waves in a normal electrocardiogram. 2. Recall the normal P-R and Q-T interval time of the QRS wave. 3.
Electrocardiography Normal 5 Faisal I. Mohammed, MD, PhD 1 Objectives 2 1. Describe the different waves in a normal electrocardiogram. 2. Recall the normal P-R and Q-T interval time of the QRS wave. 3.
12 Lead EKG. The Basics
 12 Lead EKG The Basics Objectives Demonstrate proper 12 EKG lead placement Determine electrical axis Identify ST and T wave changes as they relate to myocardial ischemia Describe possible complications
12 Lead EKG The Basics Objectives Demonstrate proper 12 EKG lead placement Determine electrical axis Identify ST and T wave changes as they relate to myocardial ischemia Describe possible complications
Sheet 5 physiology Electrocardiography-
 *questions asked by some students Sheet 5 physiology Electrocardiography- -why the ventricles lacking parasympathetic supply? if you cut both sympathetic and parasympathetic supply of the heart the heart
*questions asked by some students Sheet 5 physiology Electrocardiography- -why the ventricles lacking parasympathetic supply? if you cut both sympathetic and parasympathetic supply of the heart the heart
ECG Interpretation Made Easy
 ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG Interpretation Made Easy Dr. A Tageldien Abdellah, MSc MD EBSC Lecturer of Cardiology- Hull University Hull York Medical School 2007-2008 ECG Interpretation Made Easy Synopsis Benefits Objectives Process
ECG INTERPRETATION MANUAL
 Lancashire & South Cumbria Cardiac Network ECG INTERPRETATION MANUAL THE NORMAL ECG Lancashire And South Cumbria Cardiac Physiologist Training Manual THE NORMAL ECG E.C.G CHECKLIST 1) Name, Paper Speed,
Lancashire & South Cumbria Cardiac Network ECG INTERPRETATION MANUAL THE NORMAL ECG Lancashire And South Cumbria Cardiac Physiologist Training Manual THE NORMAL ECG E.C.G CHECKLIST 1) Name, Paper Speed,
37 1 The Circulatory System
 H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
H T H E E A R T 37 1 The Circulatory System The circulatory system and respiratory system work together to supply cells with the nutrients and oxygen they need to stay alive. a) The respiratory system:
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
All About STEMIs. Presented By: Brittney Urvand, RN, BSN, CCCC. Essentia Health Fargo Cardiovascular Program Manager.
 All About STEMIs Presented By: Brittney Urvand, RN, BSN, CCCC Essentia Health Fargo Cardiovascular Program Manager Updated 10/2/2018 None Disclosures Objectives Identify signs and symptoms of a heart attack
All About STEMIs Presented By: Brittney Urvand, RN, BSN, CCCC Essentia Health Fargo Cardiovascular Program Manager Updated 10/2/2018 None Disclosures Objectives Identify signs and symptoms of a heart attack
The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits:
 1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
1 The cardiovascular system is composed of the heart and blood vessels that carry blood to and from the body s organs. There are 2 major circuits: pulmonary and systemic. The pulmonary goes out to the
ECG and Cardiac Electrophysiology
 ECG and Cardiac Electrophysiology Simon Some very basic electrophysiology Intracellular fluid: 10 mm Na, 140 mm K, etc. K Na-K ATPase Extracellular fluid: 140mM Na, 4mM K, etc. Na Ion gradient plus selective
ECG and Cardiac Electrophysiology Simon Some very basic electrophysiology Intracellular fluid: 10 mm Na, 140 mm K, etc. K Na-K ATPase Extracellular fluid: 140mM Na, 4mM K, etc. Na Ion gradient plus selective
12 LEAD EKG BASICS. By: Steven Jones, NREMT P CLEMC
 12 LEAD EKG BASICS By: Steven Jones, NREMT P CLEMC ECG Review Waves and Intervals P wave: the sequential activation (depolarization) of the right and left atria QRS complex: right and left ventricular
12 LEAD EKG BASICS By: Steven Jones, NREMT P CLEMC ECG Review Waves and Intervals P wave: the sequential activation (depolarization) of the right and left atria QRS complex: right and left ventricular
Lab 7. Physiology of Electrocardiography
 7.1 Lab 7. Physiology of Electrocardiography The heart is a muscular pump that circulates blood throughout the body. To efficiently pump the blood, cardiac contractions must be coordinated and are regulated
7.1 Lab 7. Physiology of Electrocardiography The heart is a muscular pump that circulates blood throughout the body. To efficiently pump the blood, cardiac contractions must be coordinated and are regulated
DR QAZI IMTIAZ RASOOL OBJECTIVES
 PRACTICAL ELECTROCARDIOGRAPHY DR QAZI IMTIAZ RASOOL OBJECTIVES Recording of electrical events in heart Established electrode pattern results in specific tracing pattern Health of heart i. e. Anatomical
PRACTICAL ELECTROCARDIOGRAPHY DR QAZI IMTIAZ RASOOL OBJECTIVES Recording of electrical events in heart Established electrode pattern results in specific tracing pattern Health of heart i. e. Anatomical
Lect.6 Electrical axis and cardiac vector Cardiac vector: net result Vector that occurs during depolarization of the ventricles Figure:
 Lect.6 Electrical axis and cardiac vector Objectives: 1. State the relationship between the direction of cardiac vector with the direction (-ve, +ve) and amplitude of an ECG waves. 2. Draw diagram indicting
Lect.6 Electrical axis and cardiac vector Objectives: 1. State the relationship between the direction of cardiac vector with the direction (-ve, +ve) and amplitude of an ECG waves. 2. Draw diagram indicting
11/10/2014. Muscular pump Two atria Two ventricles. In mediastinum of thoracic cavity 2/3 of heart's mass lies left of midline of sternum
 It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
It beats over 100,000 times a day to pump over 1,800 gallons of blood per day through over 60,000 miles of blood vessels. During the average lifetime, the heart pumps nearly 3 billion times, delivering
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
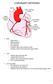 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Interpreting Electrocardiograms (ECG) Physiology Name: Per:
 Interpreting Electrocardiograms (ECG) Physiology Name: Per: Introduction The heart has its own system in place to create nerve impulses and does not actually require the brain to make it beat. This electrical
Interpreting Electrocardiograms (ECG) Physiology Name: Per: Introduction The heart has its own system in place to create nerve impulses and does not actually require the brain to make it beat. This electrical
ECG (MCQs) In the fundamental rules of the ECG all the following are right EXCEP:
 ECG (MCQs) 2010 1- In the fundamental rules of the ECG all the following are right EXCEP: a- It is a biphasic record of myocardial action potential fluctuations. b- Deflection record occurs only during
ECG (MCQs) 2010 1- In the fundamental rules of the ECG all the following are right EXCEP: a- It is a biphasic record of myocardial action potential fluctuations. b- Deflection record occurs only during
Atlantic Health System
 Atlantic Health System Morristown Medical Center Newton Medical Center Overlook Medical Center Basic Dysrhythmia Course Day 1 1 2 Chapter 1 Anatomy and Physiology Learning Objectives 1) Identify electrophysiology
Atlantic Health System Morristown Medical Center Newton Medical Center Overlook Medical Center Basic Dysrhythmia Course Day 1 1 2 Chapter 1 Anatomy and Physiology Learning Objectives 1) Identify electrophysiology
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series
 ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
ECG Basics Sonia Samtani 7/2017 UCI Resident Lecture Series Agenda I. Introduction II.The Conduction System III.ECG Basics IV.Cardiac Emergencies V.Summary The Conduction System Lead Placement avf Precordial
Electrocardiography negative zero LA/VL RA/VR LL/VF recording electrode exploring electrode Wilson right arm right arm, left arm left arm
 Electrocardiography In the previous lecture, we were talking about the unipolar limb leads. We said that to make the unipolar lead, you have to make the negative electrode as zero electrode, this is done
Electrocardiography In the previous lecture, we were talking about the unipolar limb leads. We said that to make the unipolar lead, you have to make the negative electrode as zero electrode, this is done
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology)
 ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
Electrocardiography. Hilal Al Saffar College of Medicine,Baghdad University
 Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
Electrocardiography Hilal Al Saffar College of Medicine,Baghdad University Which of the following is True 1. PR interval, represent the time taken for the impulse to travel from SA node to AV nose. 2.
BASIC PRINCIPLES OF ECG INTERPRETATION
 Chapter 1 BASIC PRINCIPLES OF ECG INTERPRETATION Cardiac rhythm analysis may be accomplished informally via cardiac monitoring and more diagnostically via a 12-lead electrocardiogram (ECG). An electrocardiogram
Chapter 1 BASIC PRINCIPLES OF ECG INTERPRETATION Cardiac rhythm analysis may be accomplished informally via cardiac monitoring and more diagnostically via a 12-lead electrocardiogram (ECG). An electrocardiogram
Myocardial Infarction. Reading Assignment (p66-78 in Outline )
 Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
Myocardial Infarction Reading Assignment (p66-78 in Outline ) Objectives 1. Why do ST segments go up or down in ischemia? 2. STEMI locations and culprit vessels 3. Why 15-lead ECGs? 4. What s up with avr?
ECG SIGNS OF HYPERTROPHY OF HEART ATRIUMS AND VENTRICLES
 Ministry of Health of Ukraine Kharkiv National Medical University ECG SIGNS OF HYPERTROPHY OF HEART ATRIUMS AND VENTRICLES Methodical instructions for students Рекомендовано Ученым советом ХНМУ Протокол
Ministry of Health of Ukraine Kharkiv National Medical University ECG SIGNS OF HYPERTROPHY OF HEART ATRIUMS AND VENTRICLES Methodical instructions for students Рекомендовано Ученым советом ХНМУ Протокол
Determining Axis and Axis Deviation on an ECG
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 7-15-2010 Determining Axis and Axis Deviation on an ECG Patrick Loftis
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Health Sciences, College of 7-15-2010 Determining Axis and Axis Deviation on an ECG Patrick Loftis
ELECTROCARDIOGRAPH. General. Heart Rate. Starship Children s Health Clinical Guideline
 General Heart Rate QRS Axis T Wave Axis PR Interval according to Heart Rate & Age P Wave Duration and Amplitude QRS Duration according to Age QT Interval R & S voltages according to Lead & Age R/S ratio
General Heart Rate QRS Axis T Wave Axis PR Interval according to Heart Rate & Age P Wave Duration and Amplitude QRS Duration according to Age QT Interval R & S voltages according to Lead & Age R/S ratio
Understanding the 12-lead ECG, part II
 Bundle-branch blocks Understanding the 12-lead ECG, part II Most common electrocardiogram (ECG) abnormality Appears as a wider than normal S complex Occurs when one of the two bundle branches can t conduct
Bundle-branch blocks Understanding the 12-lead ECG, part II Most common electrocardiogram (ECG) abnormality Appears as a wider than normal S complex Occurs when one of the two bundle branches can t conduct
CARDIOVASCULAR PHYSIOLOGY ECG. Dr. Ana-Maria Zagrean
 CARDIOVASCULAR PHYSIOLOGY ECG Dr. Ana-Maria Zagrean Electrocardiogram (ECG) ECG is a non-invasive method to record at the body surface the electrical activity of the heart. - the rate and regularity of
CARDIOVASCULAR PHYSIOLOGY ECG Dr. Ana-Maria Zagrean Electrocardiogram (ECG) ECG is a non-invasive method to record at the body surface the electrical activity of the heart. - the rate and regularity of
Left posterior hemiblock (LPH)/
 ECG OF THE MONTH Left Postero-inferior Depolarization Delay Keywords Electrocardiography Intraventricular conduction delay, Inferoposterior hemiblock, Left posterior fascicular block, Left posterior hemiblock
ECG OF THE MONTH Left Postero-inferior Depolarization Delay Keywords Electrocardiography Intraventricular conduction delay, Inferoposterior hemiblock, Left posterior fascicular block, Left posterior hemiblock
Cardiovascular System Notes: Physiology of the Heart
 Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
Cardiovascular System Notes: Physiology of the Heart Interesting Heart Fact Capillaries are so small it takes ten of them to equal the thickness of a human hair. Review What are the 3 parts of the cardiovascular
What the ECG is about
 What to expect from the ECG 00 The electricity of the heart 00 The shape of the ECG 00 The ECG electrical pictures 00 The shape of the QRS complex 00 Making a recording practical points 00 How to report
What to expect from the ECG 00 The electricity of the heart 00 The shape of the ECG 00 The ECG electrical pictures 00 The shape of the QRS complex 00 Making a recording practical points 00 How to report
3/26/15 HTEC 91. EKG Sign-in Book. The Cardiac Cycle. Parts of the ECG. Waves. Waves. Review of protocol Review of placement of chest leads (V1, V2)
 EKG Sign-in Book HTEC 91 Review of protocol Review of placement of chest leads (V1, V2) Medical Office Diagnostic Tests Week 2 http://www.cvphysiology.com/arrhythmias/a013c.htm The Cardiac Cycle Represents
EKG Sign-in Book HTEC 91 Review of protocol Review of placement of chest leads (V1, V2) Medical Office Diagnostic Tests Week 2 http://www.cvphysiology.com/arrhythmias/a013c.htm The Cardiac Cycle Represents
A few new tools for better detection and understanding of STEMIs in the field.
 A few new tools for better detection and understanding of STEMIs in the field. Let s talk, prep and placement. Try to shoot for quality, consistency and no artifact! (looking sometimes for 1 or 2 mm changes)
A few new tools for better detection and understanding of STEMIs in the field. Let s talk, prep and placement. Try to shoot for quality, consistency and no artifact! (looking sometimes for 1 or 2 mm changes)
Section V. Objectives
 Section V Landscape of an MI Objectives At the conclusion of this presentation the participant will be able to Outline a systematic approach to 12 lead ECG interpretation Demonstrate the process for determining
Section V Landscape of an MI Objectives At the conclusion of this presentation the participant will be able to Outline a systematic approach to 12 lead ECG interpretation Demonstrate the process for determining
PART I. Disorders of the Heart Rhythm: Basic Principles
 PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
PART I Disorders of the Heart Rhythm: Basic Principles FET01.indd 1 1/11/06 9:53:05 AM FET01.indd 2 1/11/06 9:53:06 AM CHAPTER 1 The Cardiac Electrical System The heart spontaneously generates electrical
Case 1. Case 2. Case 3
 Case 1 The correct answer is D. Occasionally, the Brugada syndrome can present similar morphologies to A and also change depending on the lead position but in the Brugada pattern the r is wider and ST
Case 1 The correct answer is D. Occasionally, the Brugada syndrome can present similar morphologies to A and also change depending on the lead position but in the Brugada pattern the r is wider and ST
Chapter 12: Cardiovascular Physiology System Overview
 Chapter 12: Cardiovascular Physiology System Overview Components of the cardiovascular system: Heart Vascular system Blood Figure 12-1 Plasma includes water, ions, proteins, nutrients, hormones, wastes,
Chapter 12: Cardiovascular Physiology System Overview Components of the cardiovascular system: Heart Vascular system Blood Figure 12-1 Plasma includes water, ions, proteins, nutrients, hormones, wastes,
Preface: Wang s Viewpoints
 AHA/ACCF/HRS Recommendations for the Standardization and Interpretation of the Electrocardiogram: Part IV, Ischemia and Infarction Presented by: WANG, TZONG LUEN, MD, PhD, JM, FACC, FESC, FCAPSC Professor,
AHA/ACCF/HRS Recommendations for the Standardization and Interpretation of the Electrocardiogram: Part IV, Ischemia and Infarction Presented by: WANG, TZONG LUEN, MD, PhD, JM, FACC, FESC, FCAPSC Professor,
Electrocardiography I Laboratory
 Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
Introduction The body relies on the heart to circulate blood throughout the body. The heart is responsible for pumping oxygenated blood from the lungs out to the body through the arteries and also circulating
BEDSIDE ECG INTERPRETATION
 BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
Birmingham Regional Emergency Medical Services System
 Birmingham Regional Emergency Medical Services System 2018 ALCTE Summer Conference EKG Basics Brian Gober, MAT, ATC, NRP, CSCS Education Services Manager ECC Training Center Coordinator Birmingham Regional
Birmingham Regional Emergency Medical Services System 2018 ALCTE Summer Conference EKG Basics Brian Gober, MAT, ATC, NRP, CSCS Education Services Manager ECC Training Center Coordinator Birmingham Regional
Chapter 4. Basic ECG Concepts and the Normal ECG. Brian Coyne, MEd, RCEP / Shel Levine, MS, CES
 Chapter 4 Basic ECG Concepts and the Normal ECG Brian Coyne, MEd, RCEP / Shel Levine, MS, CES Learning Objectives Upon completion of this chapter, the reader will be able to: 1. Identify standardized components
Chapter 4 Basic ECG Concepts and the Normal ECG Brian Coyne, MEd, RCEP / Shel Levine, MS, CES Learning Objectives Upon completion of this chapter, the reader will be able to: 1. Identify standardized components
Farah Khreisat. Raghad Abu Jebbeh. Faisal Mohammad. 1 P a g e
 5 Farah Khreisat Raghad Abu Jebbeh Faisal Mohammad 1 P a g e بسم هللا الرحمن الرحيم Hello guys, hope you're doing well, as you've seen in the previous lecture, the Dr started with an extremely important
5 Farah Khreisat Raghad Abu Jebbeh Faisal Mohammad 1 P a g e بسم هللا الرحمن الرحيم Hello guys, hope you're doing well, as you've seen in the previous lecture, the Dr started with an extremely important
The Normal Electrocardiogram
 C H A P T E R 1 1 The Normal Electrocardiogram When the cardiac impulse passes through the heart, electrical current also spreads from the heart into the adjacent tissues surrounding the heart. A small
C H A P T E R 1 1 The Normal Electrocardiogram When the cardiac impulse passes through the heart, electrical current also spreads from the heart into the adjacent tissues surrounding the heart. A small
Please check your answers with correct statements in answer pages after the ECG cases.
 ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
ECG Cases ECG Case 1 Springer International Publishing AG, part of Springer Nature 2018 S. Okutucu, A. Oto, Interpreting ECGs in Clinical Practice, In Clinical Practice, https://doi.org/10.1007/978-3-319-90557-0
Biology 212: Anatomy and Physiology II. Lab #5: Physiology of the Cardiovascular System For Labs Associated With Dr. Thompson s Lectures
 Biology 212: Anatomy and Physiology II Lab #5: Physiology of the Cardiovascular System For Labs Associated With Dr. Thompson s Lectures References: Saladin, KS: Anatomy and Physiology, The Unity of Form
Biology 212: Anatomy and Physiology II Lab #5: Physiology of the Cardiovascular System For Labs Associated With Dr. Thompson s Lectures References: Saladin, KS: Anatomy and Physiology, The Unity of Form
Chapter 20: Cardiovascular System: The Heart
 Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Chapter 20: Cardiovascular System: The Heart I. Functions of the Heart A. List and describe the four functions of the heart: 1. 2. 3. 4. II. Size, Shape, and Location of the Heart A. Size and Shape 1.
Abnormalities Caused by Left Bundle Branch Block
 Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Physician Assistant Studies, Department 12-17-2010 Abnormalities Caused by Left Bundle Branch
Marquette University e-publications@marquette Physician Assistant Studies Faculty Research and Publications Physician Assistant Studies, Department 12-17-2010 Abnormalities Caused by Left Bundle Branch
THE CARDIOVASCULAR SYSTEM. Heart 2
 THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
THE CARDIOVASCULAR SYSTEM Heart 2 PROPERTIES OF CARDIAC MUSCLE Cardiac muscle Striated Short Wide Branched Interconnected Skeletal muscle Striated Long Narrow Cylindrical PROPERTIES OF CARDIAC MUSCLE Intercalated
ELECTROCARDIOGRAPHY (III) THE ANALYSIS OF THE ELECTROCARDIOGRAM
 ELECTROCARDIOGRAPHY (III) THE ANALYSIS OF THE ELECTROCARDIOGRAM Scridon Alina, Șerban Răzvan Constantin Recording and analysis of the 12-lead ECG is part of the basic medical assessment performed for every
ELECTROCARDIOGRAPHY (III) THE ANALYSIS OF THE ELECTROCARDIOGRAM Scridon Alina, Șerban Răzvan Constantin Recording and analysis of the 12-lead ECG is part of the basic medical assessment performed for every
