Hydronephrosis * delivery of filtrate to the distal nephron resulting. in overperfusion of that portion. Finally, varying
|
|
|
- Catherine Chase
- 6 years ago
- Views:
Transcription
1 Journal of Clinical Investigation Vol. 45, No. 1, 1966 Patterns of Nephron Perfusion in Acute and Chronic Hydronephrosis * WADI SUKI, GARABED EKNOYAN, FLOYD C. RECTOR, JR., AND DONALD WV. SELDIN t (From the Department of Internal Medicine, The University of Texas Southwestern Medical School, Dallas, Texas) Partial urinary tract obstruction is known to produce, in addition to a nonspecific depression in renal function, certain characteristic derangements, especially profound polyuria (1-5); release of the obstruction may result in a transient salt-wasting state (6, 7). Three hypotheses may be advanced to explain the altered function of the hydronephrotic kidney. It is possible that with the elevation of intrapelvic pressure a significant fraction of the nephron mass stops functioning, due either to mechanical damage or cessation of filtration, whereas the remaining nephrons continue to function with decreased tubular flow. This decreased rate of tubular flow could be due to reduced filtration per nephron or increased proximal fractional reabsorption, or both. This hypothesis would imply a reduced delivery of filtrate to the loop of Henle and the distal convoluted tubule and would, therefore, result in a pattern of nephron underperfusion (8). An alternative possibility is that the initially elevated intrapelvic pressure results in a reduction in nephron mass; the subsequent return of intrapelvic pressure towards normal might produce a compensatory increase in the rate of tubular flow in the residual nephrons (9). The increased rate of tubular flow could result from increased filtration per nephron or diminished proximal fractional reabsorption, or both. The increased tubular flow per nephron increases the * Submitted for publication August 19, 1965; accepted October 13, Supported in part by grants I-SOI-FR 5426 and 5TI HE-5469 from the National Institutes of Health, U. S. Public Health Service. Presented in part at the National Meeting of the American Society for Clinical Investigation on May 2, 1965; a preliminary report appeared in J. clin. Invest. 1965, 44, t Address requests for reprints to Dr. Donald W. Seldin, Dept. of Internal Medicine, The University of Texas Southwestern Medical School, Dallas, Texas delivery of filtrate to the distal nephron resulting in overperfusion of that portion. Finally, varying degrees of nephron damage might be superimposed on either of the two patterns of nephron perfusion. No studies are available to determine which of these theoretical considerations best fits the observed disorders of renal function. This study was undertaken, therefore, to clarify the pattern of renal function in hydronephrosis. The excretion of salt and water during water and hypotonic saline diuresis was examined in dogs with either acute or chronic unilateral hydronephrosis; the contralateral kidney served as an internal control. The results from these two models of hydronephrosis were compared to those from an experimental model known to result in nephron underperfusion, namely, renal arterial constriction (8). Methods The effects of acute and chronic hydronephrosis and of renal arterial constriction were studied in 14 female mongrel dogs weighing 8 to 15 kg and fed commercial diets. A total of 22 studies was performed during water diuresis followed by hypotonic saline diuresis. Water diuresis was induced by the administration of 50 ml of water per kg body wt via a gastric tube and maintained by the intravenous infusion of 2.5% solution 122 of dextrose in distilled water at a rate of 10 ml per minute. When the water diuresis was well established, two or three urine and blood collections were made. Hypotonic saline solution (0.45 to 0.58%) was then started at a rate of 20 ml per minute, and 30 to 45 minutes later two or three more urine and blood collections were made. After the termination of the urine collections during hypotonic saline diuresis, the maximal tubular transport rate for p-aminohippurate (TmPAH) was measured in four experiments during acute hydronephrosis and four experiments during chronic hydronephrosis by the infusion of loading and maintenance doses of PAH sufficient to produce a plasma level of 11 to 30 mg per 100 ml. This insured a load to Tm ratio of at least 2 to 3, even in the presence of marked reductions in renal blood flow (10).
2 RENAL FUNCTION IN ACUTE AND CHRONIC HYDRONEPHROSIS 123 Acute hydronephrosis was induced in seven dogs by the elevation to variable levels (60 to 80 cm H20) of a polyethylene tube inserted in the left ureter. The animals were first anesthetized with 30 mg per kg pentobarbital int-venously, and then through a midline abdominal incisiun each ureter was cannulated with a polyethylene tube reaching into the renal pelvis. The renal artery was constricted in four anesthetized animals. Through a left flank incision, a silk tie was placed around the left renal artery, which was constricted sufficiently to reduce blood pressure distal to the constriction by 50%. The blood pressure was monitored by a small needle in the renal artery distal to the point of constriction, connected to a Statham strain gauge and a Sanborn recorder. Both ureters were cannulated with polyethylene tubing. In six dogs a bladder-splitting operation was first performed to permit the collection of urine from each kidney separately (11). Nine to 12 days later a control study was performed to ascertain whether glomerular filtration rate (GFR), sodium excretion, and free water clearance (CH20) were equal on the two sides. Through a paramedian abdominal incision the left ureter was then exposed and a silk tie placed around it, partially occluding it in the region of the ureteropelvic junction. In one dog the induction of chronic hydronephrosis was preceded by the cannulation of the left ureter and a study of acute hydronephrosis. These chronically hydronephrotic animals were then studied 7 to 124 days after the constriction of the ureter. The GFR was measured by the clearance of inulin. Inulin, PAH, sodium, potassium, and urinary solute concentrations were measured by previously published methods (8). The data were analyzed by a nonparametric median test (12). Results Figure 1, constructed from our previously published data (8), depicts the effects of acute renal arterial -constriction. During water diuresis GFR, urinary flow, and urinary sodium concentration (UNa) were always lower, and total solute concentration (Uosm) always higher, on the constricted than on the control side. During hypotonic saline diuresis, two striking changes were seen: first, UNa on the control side rose sharply, but little or no change was noted on the constricted side; second, UOsm on the constricted side, which was above the control side during water diuresis, fell to a value below that of the control side. A typical experiment during acute hydronephrosis is shown in Figure 2. The results of this study disclose a pattern similar to that of renal arterial constriction. During water diuresis GFR, urinary flow, and UNa were lower, whereas Uosm was higher, on the hydronephrotic than on the control 0 FIG. 1. THE EFFECTS OF RENAL ARTERIAL CONSTRICTION ON WATER AND ELECTROLYTE EXCRETION DURING WATER AND HYPOTONIC SALINE DIURESIS. GFR = glomerular filtration rate. side. During hypotonic saline diuresis UNa on the normal side rose with little or no change on the hydronephrotic side, and Uosm fell from a value above that of the normal side during water diuresis to below the normal side during hypotonic saline diuresis. A representative experiment on an animal with chronic hydronephrosis is shown in Figure 3. In contrast to acute hydronephrosis, UNa was markedly higher on the hydronephrotic than the control side during both water and hypotonic saline diuresis. The failure of the U..m on the hydronephrotic side to fall from a value above that of the control side during water diuresis to below the control side during hypotonic saline diuresis also is in marked contrast to the pattern seen in both renal arterial constriction and acute hydronephrosis. The effects of all three experimental models on the process of urinary dilution are shown in Figure 4 and the results expressed as the ratio of the experimental to the control side. Renal arterial
3 124 SUKI, EKNOYAN, RECTOR, AND SELDIN Normal Kidney Hydronephrotic Kidney 0-0- GFR mvmin URINE FLOW ml/min -~~~~~~ URINE SODIUM CONCENTRATION meq/l TOTAL URINARY SOLUTE mosm/l L 35 1~ F 40 _ WATER Dog M HYPOTONIC SALINE. O ~ : ; 20 A 0a p 0... Name 0 -Noma FIG. 2. THE EFFECTS OF ACUTE HYDRONEPHROSIS ON WATER AND ELECTROLYTE EXCRETION DURING WATER AND HYPOTONIC SALINE DIURESIS. constriction and acute hydronephrosis yielded similar results: the Uosm from the experimental side was invariably higher during water diuresis and lower during hypotonic saline diuresis than that of the control side. In contrast, during chronic hydronephrosis UOsm was higher on the hydronephrotic side in both water diuresis (6 of 11 studies) and hypotonic saline diuresis (9 of 11 studies). The difference in Uosm between acute and chronic hydronephrosis during hypotonic saline II ai D---* 0---O Normal Kidney 0-S-M Hydronephrotic Kidney GFR mi/min URINE FLOW ml/min _ 10 WATER Dog 19 I HYPOTONIC SALINE I a00 ~~~~~~~~~ _. URINE SODIUM CONCENTRATION meq/l 2 TOTAL 10 URINARY SOLUTE mosm/l 5 15 OC-O0o e "Owwgo-----O FIG. 3. THE EFFECTS OF CHRONIC HYDRONEPHROSIS ON WATER AND ELECTROLYTE EXCRETION DURING WATER AND HYPOTONIC SALINE DIURESIS. This experiment was performed 5 weeks after permanent ureteral constriction. diuresis was highly significant with a p value of < The effects of renal arterial constriction and acute hydronephrosis on free water clearance (CH2o) were also similar. During both water and hypotonic saline diuresis the absolute CH2o 1 Henceforth, the p values reported refer to the difference between acute and chronic hydronephrosis. RAC = RENAL ARTERY CONSTRICTION (4 EXPS) AH = ACUTE HYDRONEPHROSIS (7 EXPS) CH = CNRONIC HYDRONEPHROSIS (II EXPS) 3 2 (Uosm) EX P (Uosm) CONT.8.6 (CH2O) EXP (CH2O)CONT.4..2 FIG. 4. THE EFFECTS OF RENAL ARTERIAL CONSTRICTION AND ACUTE AND CHRONIC HYDRONEPHROSIS ON URINARY SOL- UTE CONCENTRATION (U.sm), ABSOLUTE SOLUTE-FREE WATER CLEARANCE (CH2o), AND FRACTIONAL FREE WATER CLEARANCE (CH2o X 100/GFR). The vertical bars represent the mean of the ratios of the experimental to the control side standard error.
4 RENAL FUNCTION IN ACUTE AND CHRONIC HYDRONEPHROSIS (Figure 4, middle panel) and the fractional excretion of free water [CHoG per 100 ml GFR (Figure 4, panel on the right)] were always lower on the side with renal arterial constriction or acute hydronephrosis than on the control side. In chronic hydronephrosis, by contrast, although the absolute CH20 was lower on the experimental than on the control side (Figure 4, middle panel), CHO per 100 ml GFR was greater on the hydronephrotic than on the control side (Figure 4, panel on the right) in 8 of 10 studies during water diuresis (p < 0.01) and 7 of 10 studies during hypotonic saline diuresis (p.< 0.05). The effects of renal arterial constriction and acute and chronic hydronephrosis on urinary sodium are shown in Figure 5. Urinary sodium concentration was always lower on the side with renal arterial constriction than on the control side during both water and hypotonic saline diuresis. In acute hydronephrosis a pattern similar to that of renal arterial constriction was seen in all experiments. In contrast, in chronic hydronephrosis the urinary sodium concentration was always greater on the hydronephrotic side than on the 125 control side (p < 0.05 during water diuresis and < during hypotonic saline diuresis). The absolute rate of sodium excretion (UNaV) and the fractional rate of sodium excretion [ (CNa/ inulin clearance) X 100] were always lower on the side with renal arterial constriction than on the control side (Figure 5). A similar effect on the absolute and fractional rates of sodium excretion was obtained in the experiments with acute hydronephrosis. Chronic hydronephrosis, on the other hand, resulted in higher absolute rates of sodium excretion in 9 of 10 experiments during water diuresis (p < 0.01) and 6 of 10 experiments during hypotonic saline diuresis (p < 0.005); the fractional rate of sodium excretion was uniformly greater on the side- with chronic hydronephrosis than on the control side (p < 0.01 during water diuresis and < during hypotonic saline diuresis). The effect of acute and chronic hydronephrosis on the relationship between nephron perfusion and tubular mass was also examined. The GFR on the experimental, as compared with the control, side was reduced 24 to 42%o in renal arterial con- WATER RAC = RENAL ARTERY CONSTRICTION (4 EXPS) AH ACUTE HYDRONEPHROSIS (7 EXPS) HYPOTONIC SALINE C H = CHRONIC HYDRONEPHROSIS (II EXPS) RAC AH CH RAC AH CH RAC AH CH [UN,] EXP [UN,] CONT uill Y -t, F (UNaV) EXP (UNOV) CONT. FIG. 5. THE EFFECTS OF RENAL ARTERIAL CONSTRICTION AND ACUTE AND CHRONIC HYDRONEPHROSIS ON URINARY SO- DIUM CONCENTRATION (UN), AND ABSOLUTE (UN.V) AND FRACTIONAL (CNx X 100/INULIN CLEARANCE) RATES OF SO- DIUM EXCRETION. The vertical bars represent the mean of the ratios of the experimental to the control side ± standard error.
5 126 striction, 14 to 77% in acute hydronephrosis, and 5 to 92%o in chronic hydronephrosis. The TmPAHE on the experimental side was reduced below that of the control side in both acute and chronic hydronephrosis. The relative effects of acute hydronephrosis and of chronic hydronephrosis on the GFR and TmPAH expressed as a ratio are shown in Table I. It is apparent that in acute hydronephrosis the ratio of the GFR to TmPAH was consistently reduced on the hydronephrotic side as compared to the control side; the ratio on the experimental side was 9 to 37% lower than on the control side, indicating that there was a disproportionate fall of GFR compared to TmPAH. These findings in acute hydronephrosis are similar to those of Thompson, Barrett, and Pitts in animals where renal underperfusion was induced by the inflation of a balloon in the aorta (13). In chronic hydronephrosis a different pattern was evident; the ratio of GFR to TmPAH was 18 to 76%o higher on the hydronephrotic side than on the control side. SUKI, EKNOYAN, RECTOR, AND SELDIN Discussion The terms nephron overperfusion and nephron underperfusion are usually taken to mean increased or decreased GFR per nephron. For purposes of the present study, however, where the diluting capacity of the kidney is used as an index of perfusion, it is more useful to redefine these terms in a -more restrictive sense as the amount of fluid delivered to the diluting segment, without specifying the mechanism that might be responsible for alterations in delivery rate. This requires that a standard be available in terms of which delivery rate to the diluting segment can be assessed; the contralateral control kidney serves this purpose. Thus redefined, underperfusion and overperfusion mean, respectively, reduced or increased tubular flow through individual distal nephrons,2 as compared to the flow of the contralateral control kidney. 2 For purposes of this discussion the distal nephron is defined as that portion of the nephron that is impermeable to water during maximal suppression of antidiuretic hormone (ADH). This presumably includes the ascending limb of Henle's loop, the distal convoluted tubule, and the collecting duct. The proximal nephron includes those segments proximal to the water-impermeable segment and consists of the proximal convoluted tubule, pars recta, and the descending limb of Henle's loop. Constriction of the renal artery in the present experiments reduced the glomerular filtration rate by 24 to 42%. Although it has been demonstrated that glomerulotubular balance is maintained under such circumstances so that the percentage of filtrate reabsorbed in the proximal tubule remains constant (14-16), the absolute delivery of filtrate to the distal nephron is sharply reduced. Constriction of the renal artery, therefore, furnishes an excellent model to examine the pattern of urinary formation during underperfusion of the distal nephron. Two consequences result from diminished delivery of filtrate to the distal nephron. First, sodium reabsorption is more complete and therefore the formation of solute-free water per unit volume of tubular fluid is enhanced. Second, back-diffusion of free water in the collecting duct per unit volume of tubular fluid is augmented, thereby increasing free water loss. Which of these processes will predominate during slowed flow depends principally on whether sodium reabsorption in the diluting segment is already functioning near its limiting concentration gradient. During water diuresis the concentration gradient of sodium across the distal nephron is near a maximal value. Slowed flow will augment sodium reabsorption slightly; this will increase free water formation per unit volume only minimally, but will markedly lower UNa. The absolute volume of free water formed is diminished due to the reduction of the volume of fluid delivered to the diluting segment. An additional effect of slowed flow during water diuresis will be seen in the collecting duct where the loss of the same, or even reduced, absolute amounts of free water from a markedly diminished volume of fluid will result in a sharp reduction in CH2O per unit volume of tubular fluid and a rise in Uosm. During water diuresis, therefore, the side with renal arterial constriction will display a reduced rate of CH20 because reduced delivery of filtrate to the diluting segment diminishes free water formation; a lower UNa, because the magnitude of reabsorption during slowed flow, though small in absolute amount, is proportionately greater than the rate of back-diffusion of free water; and a higher Uosm because free water back-diffusion concentrates nonsodium solutes, principally urea,
6 RENAL FUNCTION IN ACUTE AND CHRONIC HYDRONEPHROSIS 127 even though the excretion of urea is sharply reduced owing to a fall in GFR. During hypotonic saline diuresis without renal arterial constriction (Figure 1, normal kidney) expansion of extracellular fluid volume results in increased delivery of tubular fluid to the distal nephron; this is associated with a greater production of free water and rise in UNa with little change in Uosm. The constancy of Uosm while UNa rises sharply is a result of the dilution of nonsodium urinary solutes by the increased excretion of sodiumcontaining urine. During hypotonic saline diuresis the superimposition of renal arterial constriction results in a fall in the urinary concentrations of both sodium and total solute (Figure 1, panel on right). The reduced Uosm is the opposite effect from that observed when the renal artery is constricted during water diuresis. Since, under the condition of increased sodium delivery (hypotonic saline diuresis), the diluting segment is operating above its limiting concentration gradient, the greatly increased reabsorption of sodium as a result of slowed flow (renal arterial constriction) will augment the formation of solute-free water per unit tubular volume. In consequence, UNa and U1,m fall. The fall in Uosm on the constricted side during the transition from water diuresis to hypotonic saline diuresis (Figure 1) is attributable to dilu- tion of nonsodium urinary solutes by augmented urinary flow. These findings define the physiologic pattern of distal nephron underperfusion. During water diuresis acute reduction in GFR results in decreased UNa (Figure 5) and increased Uo.m (Figure 4), whereas in hypotonic saline diuresis reduced GFR diminishes both UNa and Uosm; CH2O per 100 ml GFR is reduced during water diuresis and hypotonic saline diuresis (Figure 4). Since the findings in acute hydronephrosis are similar to those in renal arterial constriction, we conclude that acute hydronephrosis produces underperfusion of the distal nephron. The pattern of renal function observed in chronic hydronephrosis differed markedly from that resulting from renal arterial constriction and acute hydronephrosis. The chronically hydronephrotic kidney compared with its contralateral control displayed a higher UNa, a higher absolute and fractional UNaV (Figure 5), a higher Uo.m during water diuresis that did not fall during hypotonic saline diuresis'(figure 4), and a lower CHIo (Figure 4). This pattern of renal function in chronic hydronephrosis could represent the superimposition of tubular damage on the distal underperfusion characteristic of acute hydronephrosis. Tubular damage, by impairing sodium transport in the diluting cc 0 E SN S E ui U z a: 3: Lus CZ k 12-8p~ 4 ado *0 *:o 00 * CONTROL O CHRONIC 0 * oo a * HYDRONEPHROSIS d ~~~~0 * Oo 0 0a URINE FLOW ml/min/100ml GFR FIG. 6. FRACTIONAL FREE WATER CLEARANCE AT VARYING FRACTIONAL RATES OF URINARY FLOW IN CHRONIC HYDRONEPHROSIS AS COMPARED TO NOR- MAL. Points represent values obtained during both water and hypotonic saline diuresis.
7 128 SUKI, EKNOYAN, RECTOR, AND SELDIN TABLE I The ratio of glomerular filtration rate (GFR) to maximal tubular transport rate for p-aminohippurate (TmPAH) in acute and chronic hydronephrosis GFR/TmPAH Experimental model Experi- mental Control Exp./Cont. Acute hydronephrosis Mean ±SD *40.1 Chronic hydronephrosis Mean -SD :: *40.2 *p <0.01. segment, could result in the high UNa, high Uo.m, and low CH2o characteristic of chronic hydronephrosis. To examine the functional integrity of the diluting segment, we plotted Cia2o per 100 ml GFR against urinary flow.(v) per 100 ml GFR (Figure 6). CH20 was plotted against V rather than solute clearance (Co.m) because the rate of urinary flow in water diuresis is a closer approximation of the rate of delivery of filtrate to the loop of Henle than is Cosm.3 If free water formation were significantly impaired, less CH20 should be found on the hydronephrotic than on the normal side at any given rate of urinary flow. This is, however, not the case. It is apparent from Figure 6 that, at comparable rates of delivery, the normal and chronically hydronephrotic kidneys generate the same CH20. Therefore, there is no apparent defect in CH20 in chronic hydronephrosis. Since CH20 represents- a balance between free water formation and free water back-diffusion, might be argued that a defect in formation could be masked by a commensurate reduction in backdiffusion. The shrinkage and scarring of the medulla so characteristic of chronic hydronephrosis undoubtedly prevents the establishment of 3 During water diuresis the distal convoluted tubule and the collecting duct are relatively impermeable to water. The rate of urinary flow, therefore, is the best index of the rate of delivery of tubular fluid to the distal nephron. Urinary flow, however, does not equal the rate of delivery since some back-diffusion of water from the collecting duct is known to occur even in the absence of ADH (8, 11, 17, 18). it medullary hypertonicity and impairs diffusion of water out of the collecting duct. However, reduction in free water loss would contribute equally to urinary flow and CH20. Consequently, although a reduction in free water back-diffusion would increase CH2o, it would not correct the low CH20 to a normal value when C1120 is compared to urinary flow. Since the relations between CH20 and urinary flow in the normal and hydronephrotic kidney are superimposable, this would constitute evidence against the hypothesis that the pattern of urinary formation in chronic hydronephrosis is attributable to a combination of underperfusion of nephrons, tubular damage, and reduced free water back-diffusion. None of these arguments excludes the possibility that some degree of tubular damage might exist, and that free water back-diffusion might be reduced. Indeed, the profound destruction of the medulla almost certainly means that the normal back-diffusion of free water is drastically curtailed. We merely wish to emphasize that the combination of tubular damage and reduced free water back-diffusion cannot readily explain the striking increase in sodium excretion in the face of normal CH120 in the setting of distal nephron underperfusion. The changes in sodium and water excretion in chronic hydronephrosis can be more easily explained on the basis of reduced nephron mass with overperfusion of residual nephrons. It is not unreasonable to assume that the GFR per nephron in chronic hydronephrosis is elevated. Although intrapelvic pressure rises sharply with acute obstruction of the ureter, it has been shown that with the persistence of obstruction the intrapelvic pressure falls gradually towards normal values (9). Despite the fall in intrapelvic pressure some nephrons never regain function and the functional renal mass is reduced. When the intrapelvic pressure falls, however, the remaining nephrons of the hydronephrotic kidney may respond in a similar manner to those of a kidney damaged from any other cause by a compensatory increase in the rate of filtration per nephron (19). Furthermore, the data relating the GFR to renal tubular mass (TmPAH) are consistent with the presence of increased GFR per nephron in chronic, as distinct from acute, hydronephrosis (Table I). In renal underperfusion due to inflation of a balloon in the aorta a fall in maximal tubular trans-
8 RENAL FUNCTION IN ACUTE AND CHRONIC HYDRONEPHROSIS 129 port of glucose (TmgiucO,,,) (13) has been reported. Acute elevation of ureteral pressure has also been reported to result in a reduction in Tmglu,08e (10) and TmpAH [(10) and present study]. In both experimental procedures the fall in GFR almost always exceeded the fall in the tubular maximum, thus suggesting a reduced filtration rate per nephron. In chronic hydronephrosis, however, the fall of TmPAH was always in excess of the fall in GFR. The increased GFR per TmPAH may be interpreted as an increased filtration rate per nephron. It is likely, therefore, that the combination of an elevated GFR per nephron and diminished fractional reabsorption of filtrate in the proximal nephron results in marked overperfusion of the distal nephron. The larger volume of fluid delivered to each distal nephron results not only in greater CH2o per 100 ml GFR, but also in a higher rate of sodium excretion and a higher Uosm in water diuresis. The low absolute rates of CH20 must be due to a diminution in the total number of nephrons. The striking difference in the pattern of water excretion between acute and chronic hydronephrosis is displayed in Figure 7, where the fraction of the glomerular filtrate excreted into the urine (V/GFR) on the experimental side is compared to that of the contralateral control kidney during both water and hypotonic saline diuresis. It is evident that at any given level of fractional volume excretion on the control side, fractional excretion is lower on the side with renal arterial constriction or acute hydronephrosis and higher on the side with chronic hydronephrosis. The proportion of the GFR that is excreted into the urine during maximal suppression of antidiuretic hormone represents the difference between fractional delivery to, and fractional water loss from, the distal nephron. The low fractional volume excretion during acute hydronephrosis and renal arterial constriction is probably the consequence of diminished delivery of filtrate to the diluting segment in the face of a well-maintained absolute rate of free water back-diffusion out of the collecting duct. The well-maintained absolute rate of free water back-diffusion will result in an increased fractional 'loss of water and a diminished fractional volume excretion. The demonstration by Levinsky, Davidson, and Berliner (20) that during antidiuresis ' 40 o X F WATER DIURES/S HIYPOTONIC SALINE D/IRES/S. b 25 '.. 20 '5 p a 0 so a 0 a o0, l a / /0 / V Cornzrol Xidnry GFiv X 100 FIG. 7. FRACTION OF GFR (V/GFR X 100) DELIVERED TO THE DILUTING SEGMENT IN RENAL ARTERIAL CONSTRICTION AND ACUTE AND CHRONIC HYDRO- NEPHROSIS, COMPARED TO THE CONTROL SIDE. Graph to the left represents data obtained during water diuresis, graph to the right during hypotonic saline diuresis. Lines drawn are the theoretic lines of equal fractional delivery.
9 130 SUKI, EKNOYAN, RECTOR, AND SELDIN renal arterial constriction sufficient to reduce GFR by 50% results in only a 15 to 20% reduction in medullary sodium concentration supports the view that medullary hypertonicity is preserved despite underperfusion of the distal nephron. The increased fractional volume excretion during chronic hydronephrosis could result from two factors. Unquestionably the diminution in free water back-diffusion secondary to medullary destruction contributes to the augmented fractional volume excretion. A second contributing factor, also the consequence of medullary destruction, would be diminished loss of fluid from the descending limb of Henle's loop (21) resulting in increased fractional delivery of filtrate to the diluting segment. Clinically, chronic hydronephrosis is characterized by a marked propensity towards polyuria with impaired concentrating ability, which at times reaches the proportions of frank nephrogenic diabetes insipidus (1-5). This syndrome occurs with some frequency in hypocalcemic and hypokalemic nephropathy, but only rarely in parenchymal renal disease (1, 22-24). Since most forms of chronic renal insufficiency do not produce nephrogenic diabetes insipidus, there must be something distinctive in chronic hydronephrosis that predisposes to this derangement. A plausible explanation may reside in the gross anatomical differences between chronic hydronephrosis and other forms of renal disease. The renal parenchyma in hydronephrosis of some duration is thinned out with flattening of the papilla and narrowing of the medulla, whereas in other forms of renal disease, medullary renal architecture is better preserved. The disproportionately severe destruction of the medulla in chronic hydronephrosis results in diminished medullary tonicity, which may increase the excretion of dilute urine by two derangements. First, the abstraction of water from the descending limb of Henle's loop will be greatly reduced; the resulting augmentation of fractional delivery of filtrate to the diluting segment will increase free water formation. Second, free water back-diffusion out of the collecting duct will be greatly reduced. The combination of increased free water formation and reduced free water loss could account for the increased frequency of nephrogenic diabetes insipidus in chronic hydronephrosis, as contrasted to other forms of parenchymal renal disease. Summary The effects of acute and chronic hydronephrosis on renal function were investigated and compared to those of renal arterial constriction during water and hypotonic saline diuresis. In acute hydronephrosis there was a reduction in urinary sodium concentration, sodium excretion, and free water clearance (CH2o) per 100 ml glomerular filtration rate (GFR). The urinary osmolality was higher on the hydronephrotic side than on the control side during water diuresis and fell to below that of the control side during hypotonic saline diuresis. This pattern was similar to that of renal arterial constriction and, therefore, was due to distal nephron underperfusion. Chronic hydronephrosis resulted in a markedly different pattern characterized by an increase in urinary solute concentration, urinary sodium concentration, and sodium excretion; CH2O was decreased, whereas CH2O per 100 ml GFR was increased. This pattern is best explained by a combination of reduced renal mass with overperfusion of residual nephrons as a result of increased filtration and diminished fractional reabsorption in the proximal nephron. Reduced back-diffusion of free water in the distal nephron may also contribute to the increased fractional excretion of water. References 1. Roussak, N. J., and S. Oleesky. Water-losing nephritis: a syndrome simulating diabetes insipidus. Quart. J. Med. 1954, 23, Earley, L. E. Extreme polyuria in obstructive uropathy. Report of a case of "water-losing nephritis" in an infant, with a discussion of polyuria. New Engl. J. Med. 1956, 255, Winberg, J. Renal function in water-losing syndrome due to lower urinary tract obstruction before and after treatment. Acta paediat. (Uppsala) 1959, 48, Dorhout Mees, E. J. Reversible water losing state, caused by incomplete ureteric obstruction. Acta med. scand. 1960, 168, Berlyne, G. M. Distal tubular function in chronic hydronephrosis. Quart. J. Med. 1961, 30, Wilson, B., D. D. Reisman, and C. A. Moyer. Fluid balance in the urologic patient: disturbances in the renal regulation of the excretion of water and so-
10 RENAL FUNCTION IN ACUTE AND CHRONIC HYDRONEPHROSIS 131 dium salts following decompression of the urinary bladder. J. Urol. (Baltimore) 1951, 66, Bricker, N. S., E. L. Shwayri, J. B. Rearden, D. Kellog, J. P. Merrill, and J. H. Holmes. An abnormality in renal function resulting from urinary tract obstruction. Amer. J. Med. 1957, 23, Van Giesen, G., M. Reese, F. Kiil, F. C. Rector, Jr., and D. W. Seldin. The characteristics of renal hypoperfusion in dogs with acute and chronic reductions in glomerular filtration rate as disclosed by the pattern of water and solute excretion after hypotonic saline infusions. J. clin. Invest. 1964, 43, Kiil, F. The Function of the Ureter and Renal Pelvis. Philadelphia, Saunders, Malvin, R. L., H. Kutchai, and F. Ostermann. Decreased nephron population resulting from increased ureteral pressure. Amer. J. Physiol. 1964, 207, Berliner, R. W., and D. G. Davidson. Production of hypertonic urine in the absence of pituitary antidiuretic hormone. J. clin. Invest. 1957, 36, Ostle, B. Statistics in Research. Ames, Iowa, Iowa State University Press, Thompson, D. D., M. J. Barrett, and R. F. Pitts. Significance of glomerular perfusion in relation to variability of filtration rate. Amer. J. Physiol. 1951, 167, Dirks, J. H., W. J. Cirksena, and R. W. Berliner. The effect of saline infusion on sodium reabsorption by the proximal tubule of the dog. J. clin. Invest. 1965, 44, Glabman, S., H. S. Aynedjian, and N. Bank. Micropuncture study of the effect of acute reductions in glomerular filtration rate on sodium and water reabsorption by the proximal tubules of the rat. J. clin. Invest. 1965, 44, Brunner, F. P., F. C. Rector, Jr., and D. W. Seldin. Unpublished observations. 17. Kiil, F., and K. Aukland. Renal tubular localization of water and sodium reabsorption in antidiuresis and water diuresis. Scand. J. clin. Lab. Invest. 1960, 12, Gottschalk, C. W. Micropuncture studies of tubular function in the mammalian kidney. Physiologist 1961, 4, Bricker, N. S., P. A. F. Morrin, and S. W. Kime, Jr. The pathologic physiology of chronic Bright's disease. An exposition of the "intact nephron hypothesis." Amer. J. Med. 1960, 28, Levinsky, N. G., D. G. Davidson, and R. W. Berliner. Effects of reduced glomerular filtration on urine concentration in the presence of antidiuretic hormone. J. clin. Invest. 1959, 38, Earley, L. E., and R. M. Friedler. Observations on the mechanism of decreased tubular reabsorption of sodium and water during saline loading. J. clin. Invest. 1964, 43, Carone, F. A., and F. H. Epstein. Nephrogenic diabetes insipidus caused by amyloid disease. Evidence in man of the role of the collecting ducts in concentrating urine. Amer. J. Med. 1960, 29, Kleeman, C. R., and F. H. Epstein. An illustrative case of chronic pyelonephritis with persistently hypotonic urine. Amer. J. Med. 1957, 23, Kleeman, C. R., W. L. Hewitt, and L. B. Guze. Pyelonephritis. Medicine (Baltimore) 1960, 39, 3.
20 Barton et al. Fourteen female mongrel dogs, weighing between 10 to 20 kg, were studied. Light pentobarbital anesthesia
 20 Barton et al. critical determinant of the occurrence and magnitude of natriuresis. It is possible that volume expansion suppresses sodium reabsorption in the loop, and that in the absence of this inhibitory
20 Barton et al. critical determinant of the occurrence and magnitude of natriuresis. It is possible that volume expansion suppresses sodium reabsorption in the loop, and that in the absence of this inhibitory
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Increased sodium reabsorption in the proximal and distal tubule of caval dogs
 Increased sodium reabsorption in the proximal and distal tubule of caval dogs George J. Kaloyanides,, Nancy C. Pablo, Jerome G. Porush J Clin Invest. 1969;48(8):1543-1551. https://doi.org/1.1172/jci1612.
Increased sodium reabsorption in the proximal and distal tubule of caval dogs George J. Kaloyanides,, Nancy C. Pablo, Jerome G. Porush J Clin Invest. 1969;48(8):1543-1551. https://doi.org/1.1172/jci1612.
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
proximal tubule. and hyperperfusion of the distal nephron. They further suggested that back-diffusion of solute free water was
 Downloaded from http://www.jci.org on January 1, 218. https://doi.org/1.1172/jci16588 The Postobstructive Kidney. Observations on Nephron Function after the Relief of 24 hr of reteral Ligation in the Dog
Downloaded from http://www.jci.org on January 1, 218. https://doi.org/1.1172/jci16588 The Postobstructive Kidney. Observations on Nephron Function after the Relief of 24 hr of reteral Ligation in the Dog
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Faculty version with model answers
 Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
Faculty version with model answers Urinary Dilution & Concentration Bruce M. Koeppen, M.D., Ph.D. University of Connecticut Health Center 1. Increased urine output (polyuria) can result in a number of
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
absolute rate of net transfer had occurred. These rate of sodium reabsorption by the proximal
 Journal of Clinical Investigation Vol. 44, No. 8, 1965 Micropuncture Study of the Effect of Acute Reductions in Glomerular Filtration Rate on Sodium and Water Reabsorption by the Proximal Tubules of the
Journal of Clinical Investigation Vol. 44, No. 8, 1965 Micropuncture Study of the Effect of Acute Reductions in Glomerular Filtration Rate on Sodium and Water Reabsorption by the Proximal Tubules of the
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System)
 NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
NOTES: CH 44 Regulating the Internal Environment (Homeostasis & The Urinary System) HOMEOSTASIS **Recall HOMEOSTASIS is the steady-state physiological condition of the body. It includes: 1) Thermoregulation:
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
P215 Spring 2018: Renal Physiology Chapter 18: pp , Chapter 19: pp ,
 P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
P215 Spring 2018: Renal Physiology Chapter 18: pp. 504-520, 525-527 Chapter 19: pp. 532-548, 553-560 I. Main Components of the Renal System 1. kidneys 2. ureters 3. urinary bladder 4. urethra 4 Major Functions
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
Chapter 23. The Nephron. (functional unit of the kidney
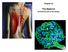 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Urinary bladder provides a temporary storage reservoir for urine
 Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Urinary System Organs Kidney Filters blood, allowing toxins, metabolic wastes, and excess ions to leave the body in urine Urinary bladder provides a temporary storage reservoir for urine Paired ureters
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance
 Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Human Anatomy and Physiology - Problem Drill 23: The Urinary System, Fluid, Electrolyte and Acid-Base Balance Question No. 1 of 10 Which of the following statements about the functions of the urinary system
Anatomy/Physiology Study Guide: Unit 9 Excretory System
 Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
5.Which part of the nephron removes water, ions and nutrients from the blood?
 Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Chapter 32 Excretion
 Chapter 32 Excretion 3.4 Learning Objectives 3.4.6 The Excretory System in Humans 1. Role of the excretory system in homeostasis. 2. Importance of temperature regulation within the body. 3. Outline the
Chapter 32 Excretion 3.4 Learning Objectives 3.4.6 The Excretory System in Humans 1. Role of the excretory system in homeostasis. 2. Importance of temperature regulation within the body. 3. Outline the
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Osmoregulation and Renal Function
 1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
1 Bio 236 Lab: Osmoregulation and Renal Function Fig. 1: Kidney Anatomy Fig. 2: Renal Nephron The kidneys are paired structures that lie within the posterior abdominal cavity close to the spine. Each kidney
Functions of Proximal Convoluted Tubules
 1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
1. Proximal tubule Solute reabsorption in the proximal tubule is isosmotic (water follows solute osmotically and tubular fluid osmolality remains similar to that of plasma) 60-70% of water and solute reabsorption
Stimulation by Isoproterenol
 Depression of Proximal Tubular Sodium Reabsorption in the Dog in Response to Renal Beta Adrenergic Stimulation by Isoproterenol JOHN R. Giu, JR., and ALFRED G. T. CASPER From the Endocrinology Branch of
Depression of Proximal Tubular Sodium Reabsorption in the Dog in Response to Renal Beta Adrenergic Stimulation by Isoproterenol JOHN R. Giu, JR., and ALFRED G. T. CASPER From the Endocrinology Branch of
2) This is a Point and Click question. You must click on the required structure.
 Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
Class: A&P2-1 Description: Test: Excretory Test Points: 144 Test Number: 28379 Printed: 31-March-10 12:03 1) This is a Point and Click question. You must click on the required structure. Click on the Bowman's
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
A. Incorrect! The urinary system is involved in the regulation of blood ph. B. Correct! The urinary system is involved in the synthesis of vitamin D.
 Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Human Anatomy - Problem Drill 22: The Urinary System Question No. 1 of 10 1. Which of the following statements about the functions of the urinary system is not correct? Question #01 (A) The urinary system
Urinary Physiology. Chapter 17 Outline. Kidney Function. Chapter 17
 Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Urinary Physiology Chapter 17 Chapter 17 Outline Structure and Function of the Kidney Glomerular Filtration Reabsorption of Salt and Water Renal Plasma Clearance Renal Control of Electrolyte and Acid-Base
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Nephrology - the study of the kidney. Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system
 Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
Urinary System Nephrology - the study of the kidney Urology - branch of medicine dealing with the male and female urinary systems and the male reproductive system Functions of the Urinary System 1. Regulation
IN THE DOG. by means of a soft indwelling rubber catheter. At the beginning of each study the dogs were given a quantity
 THE EFFECT OF VARIATIONS IN SOLUTE EXCRETION AND VASOPRESSIN DOSAGE ON THE EXCRETION OF WATER IN THE DOG By JACK ORLOFF, HENRY N. WAGNER, JR., AND DOUGLAS G. DAVIDSON (From the Laboratory of Kidney and
THE EFFECT OF VARIATIONS IN SOLUTE EXCRETION AND VASOPRESSIN DOSAGE ON THE EXCRETION OF WATER IN THE DOG By JACK ORLOFF, HENRY N. WAGNER, JR., AND DOUGLAS G. DAVIDSON (From the Laboratory of Kidney and
Excretory System. Biology 2201
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations ORGANS
Excretory System. Excretory System
 Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Excretory System Biology 2201 Excretory System How does the excretory system maintain homeostasis? It regulates: Body heat Water-salt concentrations Acid-base concentrations Metabolite concentrations 1
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System BIO 250. Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat. Routes of Waste Elimination
 Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Urinary System BIO 250 Waste Products of Metabolism Urea Carbon dioxide Inorganic salts Water Heat Routes of Waste Elimination Skin: Variable amounts of heat, salts, and water; small amounts of urea and
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Effects of Increased Sodium Delivery on Distal Tubular Sodium Reabsorption
 Effects of Increased Sodium Delivery on Distal Tubular Sodium Reabsorption with and without Volume Expansion in Man VARDAMAN M. BUCKALEW, JR., BAimy R. WALKER, JULES B. PusCmETT, and MARTIN GOLDBERG From
Effects of Increased Sodium Delivery on Distal Tubular Sodium Reabsorption with and without Volume Expansion in Man VARDAMAN M. BUCKALEW, JR., BAimy R. WALKER, JULES B. PusCmETT, and MARTIN GOLDBERG From
the Laboratory of Kidney and Elcctrolye Metabolism, National Hcart Institute, Bethesda, Aid.) sites in the nephron where urinary (lilution occurs.
 THE EFFECTS OF INFUSIONS OF CHLOROTHIAZIDE ON lurinvary DILUTION AND CONCENTRATION IN THE DOG (Fronm By LAURENCE E. EARLEY, NMELVTIN- KAHN * AND JACK ORLOFF the Laboratory of Kidney and Elcctrolye Metabolism,
THE EFFECTS OF INFUSIONS OF CHLOROTHIAZIDE ON lurinvary DILUTION AND CONCENTRATION IN THE DOG (Fronm By LAURENCE E. EARLEY, NMELVTIN- KAHN * AND JACK ORLOFF the Laboratory of Kidney and Elcctrolye Metabolism,
Counter-Current System Regulation of Renal Functions
 Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
Counter-Current System Regulation of Renal Functions Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most
1.&Glomerular/Pressure&Filtration&
 Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
Urine&Formation& Overall&Process&! Urine gets rid of wastes (NH 3, urea, uric acid, creatinine) and other substances (vitamins, penicillin, histamines) found in excess in the blood!! blood is filtered
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
BIOL2030 Human A & P II -- Exam 6
 BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
BIOL2030 Human A & P II -- Exam 6 Name: 1. The kidney functions in A. preventing blood loss. C. synthesis of vitamin E. E. making ADH. B. white blood cell production. D. excretion of metabolic wastes.
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi
 Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Done By: Lulu Al-Obaid - Abdulrahman Al-Rashed Reviewed By: Mohammed Jameel Khulood Al-Raddadi At the end of this lecture student should be able to describe: The loop of Henle is referred to as countercurrent
Renal Functions: Renal Functions: Renal Function: Produce Urine
 Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
Renal Functions: Excrete metabolic waste products Reabsorb vital nutrients Regulate osmolarity: Maintain ion balance Regulate extracellular fluid volume (and thus blood pressure) Renal Functions: Regulate
BIOLOGY - CLUTCH CH.44 - OSMOREGULATION AND EXCRETION.
 !! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
!! www.clutchprep.com Osmoregulation regulation of solute balance and water loss to maintain homeostasis of water content Excretion process of eliminating waste from the body, like nitrogenous waste Kidney
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
URINARY SYSTEM CHAPTER 28 I ANATOMY OF THE URINARY SYSTEM. Student Name
 Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Student Name CHAPTER 28 URINARY SYSTEM L iving produces wastes. Wherever people live or work or play, wastes accumulate. To keep these areas healthy, there must be a method of disposing of these wastes
Osmoregulation and Excretion
 Animal Life and Excretion Harder for multicellular organisms Internal circulation Coordination, information transfer Structural maintenance Movement Maintenance of homeostatic internal environment 15 July
Animal Life and Excretion Harder for multicellular organisms Internal circulation Coordination, information transfer Structural maintenance Movement Maintenance of homeostatic internal environment 15 July
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
41B. Metabolism produces wastes that must be eliminated from the body. This. Renal System Physiology: Computer Simulation
 41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
41B E X E R C I S E Renal System Physiology: Computer Simulation O B J E C T I V E S 1. To define the following terms: glomerulus, glomerular capsule, renal corpuscle, renal tubule, nephron, proximal convoluted
Kidney and urine formation
 Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Kidney and urine formation Renal structure & function Urine formation Urinary y concentration and dilution Regulation of urine formation 1 Kidney and urine formation 1.Renal structure & function 1)General
Sodium Reabsorption in the Distal Nephron of Dogs
 Effect of Extracellular Volume Expansion upon Sodium Reabsorption in the Distal Nephron of Dogs CiEAVES M. BiNM= From the Divisions of Nephrology, Departments of Medicine, Duke University Medical Center,
Effect of Extracellular Volume Expansion upon Sodium Reabsorption in the Distal Nephron of Dogs CiEAVES M. BiNM= From the Divisions of Nephrology, Departments of Medicine, Duke University Medical Center,
Questions? Homework due in lab 6. PreLab #6 HW 15 & 16 (follow directions, 6 points!)
 Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
Questions? Homework due in lab 6 PreLab #6 HW 15 & 16 (follow directions, 6 points!) Part 3 Variations in Urine Formation Composition varies Fluid volume Solute concentration Variations in Urine Formation
NORMAL POTASSIUM DISTRIBUTION AND BALANCE
 NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
NORMAL POTASSIUM DISTRIBUTION AND BALANCE 98% of body potassium is contained within cells, principally muscle cells, and is readily exchangeable. Only 2% is in ECF. Daily intake exceeds the amount in ECF.
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Chapter 25: Urinary System
 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Question 1: Solution 1: Question 2: Question 3: Question 4: Class X The Excretory System Biology
 A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion.
 The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
The Kidney Vertebrates possess kidneys: internal organs which are vital to ion and water balance and excretion. The kidney has 6 roles in the maintenance of homeostasis. 6 Main Functions 1. Ion Balance
Physio 12 -Summer 02 - Renal Physiology - Page 1
 Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Physiology 12 Kidney and Fluid regulation Guyton Ch 20, 21,22,23 Roles of the Kidney Regulation of body fluid osmolarity and electrolytes Regulation of acid-base balance (ph) Excretion of natural wastes
Unit #4 Waste and Excretion. The Kidneys
 Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Unit #4 Waste and Excretion The Kidneys Renal Hilus (Hilus) the doorway of the kidney Ureter leaves this region blood and lymphatic vessels enter and exit here Renal Capsule (Capsule) smooth fibrous tissue
Other Factors Affecting GFR. Chapter 25. After Filtration. Reabsorption and Secretion. 5 Functions of the PCT
 Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Other Factors Affecting GFR Chapter 25 Part 2. Renal Physiology Nitric oxide vasodilator produced by the vascular endothelium Adenosine vasoconstrictor of renal vasculature Endothelin a powerful vasoconstrictor
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Excretion and Water Balance
 Excretion and Water Balance 1. Osmoregulation (water balance) a. Most marine invertebrates are osmoconformers in which the concentration of solutes in their body fluid is equal to that of their environment.
Excretion and Water Balance 1. Osmoregulation (water balance) a. Most marine invertebrates are osmoconformers in which the concentration of solutes in their body fluid is equal to that of their environment.
Regulation of Extracellular Fluid Osmolarity and Sodium Concentration
 C H A P T E R 2 8 Regulation of Extracellular Fluid Osmolarity and Sodium Concentration For the cells of the body to function properly, they must be bathed in extracellular fluid with a relatively constant
C H A P T E R 2 8 Regulation of Extracellular Fluid Osmolarity and Sodium Concentration For the cells of the body to function properly, they must be bathed in extracellular fluid with a relatively constant
EXCRETORY SYSTEM E. F. G. H.
 XRTORY SYSTM 1. Label the following parts of the nephron in the diagram below:..... F. G. H. I. J. K. L. 2. Identify the following as either True or False: There is a greater osmotic concentration in the
XRTORY SYSTM 1. Label the following parts of the nephron in the diagram below:..... F. G. H. I. J. K. L. 2. Identify the following as either True or False: There is a greater osmotic concentration in the
Diagram of the inner portions of the kidney
 Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
Excretory and Endocrine functions of the kidney The kidneys are the main excretory organs which eliminate in the urine, most metabolites primarily those containing nitrogen such as ammonia, urea and creatinine.
Normal Renal Function
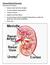 Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
Normal Renal Function Functions of the Kidney: balances solute and water transport excretes metabolic waste products conserves nutrient regulates acid-base balance secretes hormones that help regulate
The Excretory System
 The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
The Excretory System The excretory system The excretory system includes the skin, lungs and kidneys which all release metabolic wastes from the body. The kidneys, skin and the lungs are the principle organs
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
PHGY210 Renal Physiology
 PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
PHGY210 Renal Physiology Tomoko Takano, MD, PhD *Associate Professor of Medicine and Physiology McGill University *Nephrologist, McGill University Health Centre Lecture plan Lecture 1: Anatomy, basics
Regulating the Internal Environment. AP Biology
 Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Regulating the Internal Environment 2006-2007 Conformers vs. Regulators Two evolutionary paths for organisms regulate internal environment maintain relatively constant internal conditions conform to external
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Answers and Explanations
 Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
Answers and Explanations 1. The answer is D [V B 4 b]. Distal K + secretion is decreased by factors that decrease the driving force for passive diffusion of K + across the luminal membrane. Because spironolactone
I. Metabolic Wastes Metabolic Waste:
 I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
I. Metabolic Wastes Metabolic Waste: a) Carbon Dioxide: by-product of cellular respiration. b) Water: by-product of cellular respiration & dehydration synthesis reactions. c) Inorganic Salts: by-product
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
