(Received 20 March 1940)
|
|
|
- Cory Terry
- 5 years ago
- Views:
Transcription
1 336 J. Physiol. (I940) 98, I THE MECHANISMS OF DILUTION DIURESIS IN THE ISOLATED KIDNEY AND THE ANAESTHETIZED DOG BY M. GRACE EGGLETON,1 J. R. PAPPENHEIMER AND F. R. WINTON Departments of Physiology, University of Cambridge, and Pharmacology, University College, London (Received 20 March 1940) THE important contributions to the theory of renal secretion made by students of dilution diuresis began with Starling's [1899] consideration of the influence of the colloid osmotic pressure of plasma proteins on the rate of glomerular filtration. Despite Magnus's [1900] impression, based on extensive observations, that the diuresis was too great to be attributed solely to a change in glomerular activity, the view that tubular activity was not directly affected gained ground and was supported by Barcroft & Straub's [1910] finding that dilution diuresis was unaccompanied by increase in metabolism of the kidney and was therefore a "mechanical" diuresis. This view was reinforced by Knowlton's [1911] comparison of the effects of saline with gum-saline and gelatine-saline solutions, which identified the diuretic stimulus as a reduction in colloid osmotic pressure of the plasma. The purely "mechanical" view of dilution diuresis was strongly advocated by Cushny [1917] and has since been generally accepted as evidence in favour of the filtration theory of glomerular function in the mammal. Cushny [1917] concedes that "the change in the amount of urine in Magnus's experiments is out of all proportion to the change in the concentration of the colloids", but he felt able to explain away the discrepancy on the grounds that the proportion of filtrate reabsorbed in the tubules would be lower during the diuresis, and that this would magnify the change in glomerular filtration rate which he apparently took to be proportional to the reduction in concentration of plasma colloids. More recently, observations on perfused kidneys have directed attention to the disproportionately great diuresis produced by a small reduction in colloid osmotic pressure of the plasma in comparison with that 1 Assisted by a grant from the Medical Research Council.
2 MECHANISMS OF DILUTION DIURESIS 337 produced by an equivalent rise in arterial pressure [Winton, 1937], with the implied suggestion that dilution diuresis is in part due to a direct action on tubular activity, inhibiting reabsorption of water. It is the main purpose of the experiments described below to measure this disproportion in the anaesthetized dog and in the isolated kidney, and to attempt to evaluate the glomerular and tubular factors co-operating in the production of dilution diuresis. The decision as to whether a form of diuresis is to be attributed to change in glomerular or tubular activity encounters a difficulty which is simply explained by an illustration. Suppose we may measure the glomerular filtration rate in terms of the creatinine clearance, and that a twofold diuresis involves an increase of urine flow from 1 to 2 % of the filtration rate. If the amount of water reabsorbed in the tubules remains unchanged, we should expect only 1% increase in creatinine clearance, a change too small to detect with confidence in view of the other hazards of biological experiment. It would seem difficult to discover, therefore, whether even a considerable diuresis is due to a small increase in glomerular filtration rate or to a small diminution of reabsorption in the tubules. Fortunately, the difficulty can be surmounted if the meanings attached to "change in glomerular activity" and "change in tubular activity" or more shortly "glomerular diuresis " and "tubular diuresis " are properly chosen and precisely defined. As far as we know, a change in glomerular filtration rate always involves characteristic and determinate changes in tubular activity, and glomerular diuresis should, therefore, be taken to imply the whole complex of glomerular and tubular changes consequent upon an increase in filtration rate. Similarly, tubular diuresis implies the changes occurring when diuresis is unaccompanied by increase in filtration rate. To assign a particular type of diuresis to the glomerular or tubular class requires standards of reference. The standard here chosen for a glomerular diuresis is the change in a number of the constituents of urine produced by an increase in renal arterial pressure, and the standard chosen for a tubular diuresis is the corresponding change produced by increase in the urea content of the plasma. It is a further aim of this communication to give rather more formal precision to the ideas underlying this way of distinguishing between changes in glomerular and tubular activity, though the ideas themselves have been implicit in several earlier communications [e.g. Verney & Winton, 1930]. The mechanism of dilution diuresis is particularly concerned with the difference between the glomerular capillary pressure and the intracap-
3 338 M. G. EGGLETON AND OTHERS sular pressure, and in suitable circumstances [Winton, 1931 a] changes in the latter can be estimated if the pressure fall from the glomerular capsule to the ureter be kept approximately constant by preventing changes in urine flow by appropriate changes in ureter pressure. We have, therefore, compared dilution diuresis with the standard forms of diuresis not only when the increase in urine flow is allowed to become manifest, without intentional changes in pressure head, i.e. "isobaric diuresis", but also when the urine flow is kept constant by suitable adjustment to the pressure head, and the "isorrheic diuresis" is measured in terms of the change in arterial or ureter pressure. METHODS The technique employed in experiments with the double pump-lungkidney preparation was the same as that described in our previous communication [Eggleton, Pappenheimer & Winton, 1940 a]. The chemical methods were also as there described. Observations on the kidney in situ were conducted on dogs anaesthetized with chloralose, 0X1 g./kg. Ureters were cannulated, and in some experiments the left kidney was denervated. The pressure in the renal artery was varied by adjusting a clamp placed on the thoracic aorta. This and certain details of procedure are described in more detail by Shannon & Winton [1940]. Dilution of the blood was achieved by adding a Ringer-Locke's solution containing NaCl 076%, KCI 0-042%, CaCl %, MgCl %, NaHCO3 020 %, dextrose 0 05 %. The higher value of bicarbonate than is usual was chosen in pump-lung-kidney experiments so that an appropriate ph would result from ventilation of the lungs with 5% C02. The degree of dilution of the plasma was estimated by measuring the total solids. Two or three consecutive samples of urine were collected under any given set of conditions after an appropriate time had been allowed for the composition to reach a steady value. It was observed that the usual procedure of allowing a definite volume of urine, say 3 c.c., to be formed in the hope that such a "wash-out sample" would be sufficient was unsatisfactory at high urine flows-the volume of the " wash-out sample " being greater the higher the urine flow. At high rates of flow we often discarded 10 c.c. or more before beginning the collection of test samples.
4 MECHANISMS OF DILUTION DIURESIS 339 RESULTS The comparison of dilution diuresis with glomerular and tubular diuresis under isobaric conditions Isolated kidney. The disproportion between the degree of diuresis due to blood dilution and that due to an arterial pressure change which might be expected to produce about the same change in glomerular filtration pressure is shown in Table I. As a first approximation, the glomerular TABLE I. Diuretic action of the changes in arterial pressure and in plasma protein concentration which may produce comparable changes in glomerular filtration pressure Percentage increase in urine flow due to Pressure diuresis (per 5 mm. Hg change in arterial pressure) Ringer diuresis (per 3 mm. Hg change in colloid osmotic pressure) Isolated kidney 21*1 ± ±20 (9) (7) Anaesthetized dog 12-0± ±31 (denervated) (2) (10) Anaesthetized dog 12-3 ± ±30 (innervated) (8) (20) capillary pressure in the isolated kidney may be taken as 60% of the arterial pressure [Winton, 1931 b], a reduction of 1% (e.g. from 8 to 7 %) in the serum protein concentration would imply a reduction of colloid osmotic pressure of about 3 mm. Hg, and the equivalent rise in arterial pressure should, therefore, be about 5 mm. Hg. If this were so, the disproportion between pressure and dilution diuresis would be six- to sevenfold. More precisely, the relevant osmotic pressure is the properly calculated average of that in the serum entering the glomerular capillary, and that in the serum as it leaves the capillary deprived of the glomerular fluid. If this be taken into account, the reduction of colloid osmotic pressure effective in glomerular filtration corresponding with a change by 1% in the serum protein concentration may fairly be put at 4 mm. lug and the equivalent increase in arterial pressure should, therefore, be about 6 mm. Hg. This consideration, however, only reduces the disproportion between dilution and pressure diuresis to one of fivefold. A first approach to the problem whether the disproportionate magnitude of dilution diuresis is due to an unexpectedly large increase in glomerular filtration or to a direct influence on the tubules reducing their reabsorptive activity may be made by comparing the data represented in Figs The curves illustrate the changes in urine flow, and in the
5 ~~~~~~~~~~~~~~~~~~~~~~~~1200 // 340 M. G. EGGLETON AND OTHERS chloride, creatinine and urea clearances characteristically associated with diuresis due to (1) dilution of serum, (2) increase in arterial pressure, and (3) increase in the urea content of the serum. The figures represent observations on different kidneys. The experiment on pressure diuresis (Fig. 2) l /// p 250 _X _ 200,oe Urea clearance O-_M/ 50 1/~~~~~~~~~~~~~~0 4)o I ; 800 _Chloride clearancee +7'~~~~ 4200-U fl 01 _-g~~~~~~ i 1 ~~~.1 IQO Serum protein (% normal value) Fig. 1. Dilution diuresis in the isolated kidney. The percentage increase in urine flow, and in creatinine, urea, and chloride clearances with increasing dilution of serum protein by Ringer's fluid. Double pump-lung single kidney preparation. Initial values: kidney weight 15-5 g., urine flow 0*18 c.c./min., creatinine clearance 8.7 c.c./min., urea clearance 2-44 c.c./min., chloride clearance c.c./min. was performed on the single pump-lung-kidney preparation. In the other experiments (Figs. 1, 3), each kidney was perfused alternately from two pump-lung circuits, the control circuit containing defibrinated blood the composition of which was kept as far as possible constant throughout the experiment, the second circuit being used for the addition of the diuretic
6 MECHANISMS OF DILUTION DIURESIS agent in several stages. The blood in a double pump-lung single kidney preparation was well mixed, the two circuits only being separated shortly before the transfer of the kidney from the control circuit to that in which either Ringer's solution or extra urea had been added to the defibrinated blood. -AM 341 Urea clearance 4.0~~~~ 00 ioo~ O0 d! c 20C 100 )O _ Chloride clearance / // I~~~~ -0 Urine flow wv LU 14U 160 Arterial pressure (mm. Hg) Fig. 2. Pressure diuresis in the isolated kidney. The percentage increase in urine flow, and in creatinine, urea, and chloride clearances with increase in arterial pressure. Singie pump-lung-kidney preparation. Initial values: urine flow c.c./min., creatinine clearance 5.4 c.c./min., urea clearance 0 59 c.c./min., chloride clearance c.c./min. Any point on the curves represents the increase in value when the kidney was on the diuretic circuit over the average of the two values obtained just before and after, when the kidney was on the control circuit. Inspection of Figs. 1-3 immediately shows that dilution diuresis is much more closely related to pressure diuresis than it is to urea diuresis.
7 342 M. G. EGGLETON AND OTHERS In both dilution and pressure diuresis the creatinine clearance increases, and the urea clearance increases relatively more. The increase in chloride clearance is less marked in dilution diuresis than in pressure diuresis, but in both there is a systematic increase which contrasts with the more complicated relation shown in urea diuresis. 0 0GO Go 0 U Serum urea (mg./100 c.c.) Fig. 3. Urea diuresis in the isolated kidney. The percentage changes in urine flow, and in creatinine, urea, and chloride clearances with increasing serum urea concentration. Double pump-lung single kidney preparation. Initial values: kidney weight 23 g., urine flow c.c./min., creatinine clearance 12-5 c.c./min., urea clearance 4-2 c.c./ mi., chloride clearance c.c./min. In Table II we have brought together for quantitative comparison a series of values from a considerable number of experiments of the same kind. We have calculated all values for a doubling of urine flow assuming proportionality between the increase in the value and the increase in the
8 MECHANISMS OF DILUTION DIURESIS 343 TABLE II. Isolated kidney. Isobaric diuresis. Showing the percentage changes in clearances, etc., calculated for a doubling of urine flow by different diuretic agents Percentage increase in Arterial pressure Ringer's fluid Urea Creatinine clearance 31 ±8 24±7-5 ±4 Urea clearance 60 ±10 45 ± ±4 Chloride clearance 220±50 90±13 63 ±16 Total osmotic work 38 ±3 41 ±4 63 ±7 Number of observations Mean percentage increase in urine flow 183 ± ± ±51 urine flow. It will be seen from the curves given that such an assumption is only an approximation. Each value is expressed in terms of the mean, and the standard error of the mean. The increases in urine flow actually observed are included in the table, and the fact that the Ringer diuresis was considerably greater than the two other forms of diuresis should not be entirely ignored in a comparison of the other values shown. The salient features of the results expressed in Table II are (1) the increase in creatinine clearance in dilution diuresis and in pressure diuresis is considerable and not very different in amount, whereas, by contrast, there is no such increase in urea diuresis. Considerable urea diuresis usually involves a small reduction in creatinine clearance due to increased intrarenal pressure [Winton, 1933], and comparable with the reduction of 18% found [Bickford & Winton, 1937] when water reabsorption is blocked by cooling the kidney. (2) In view of the greater increase in urine flow in the dilution diuresis, the increase in urea clearance is probably rather greater in pressure diuresis than in dilution diuresis, there being no increase in urea diuresis. The lessening in reabsorption of urea with diuresis is, therefore, on the average less marked with dilution than with pressure diuresis. (3) Increases in chloride clearance occur in all three forms of diuresis, the increase being larger in pressure diuresis. Dilution diuresis differs from pressure diuresis in promoting the reabsorption of chloride. The evidence of Table II as to whether dilution diuresis is to be regarded as "glomerular" or "tubular " is, therefore, confficting. It appears to be mainly glomerular with reference to the creatinine and urea clearances, but mainly tubular with reference to chloride clearance. As far as the elimination of water is concerned, however, and the problem of the disproportionately great dilution diuresis is primarily concerned with this constituent of the urine, the creatinine clearance is the surest guide to the mechanism involved, and this would suggest that in the isolated kidney dilution diuresis is mainly a glomerular diuresis. This suggestion PH. XCVIII. 23
9 344 M. G. EGGLETON AND OTHERS is supported by our previous finding [Eggleton et al a] that the increase in total osmotic work done in pressure and dilution diuresis is not significantly different, whereas that in urea diuresis is usually somewhat higher. This involves the conclusion that a given change in colloid osmotic pressure of the serum produces a much greater change in glomerular filtration rate than does a comparable change in hydrostatic pressure across the glomerular membrane, i.e. that either the permeability or the surface area of the glomerular membrane has undergone substantial increase. Anaesthetized dog. The disproportion between dilution diuresis and the pressure diuresis due to a change in hydrostatic pressure comparable with the change in colloid osmotic pressure is even greater in the anaesthetized dog than in the pump-lung-kidney preparation. If a change in arterial pressure of 5 mm. Hg be regarded as equivalent to a change by 1% in the concentration of serum protein, as above, dilution produces about fifteenfold-the diuresis produced by an equivalent change in hydrostatic pressure (Table I). We have separated our results on innervated and denervated kidneys in Table I to indicate that they are sufficiently alike to justify considering them together in Table III. If, for reasons given in the previous section, the arterial pressure equivalent of a change by 1 % in serum protein be taken as 6 mm. Hg, the disproportion in diuresis is reduced to one of about thirteenfold, which still implies a major discrepancy in the theory of dilution diuresis currently adopted. The plan of the experiments on anaesthetized dogs from which the data in Table III were obtained was less elaborate than that adopted in TABLE III. Anaesthetized dog. Isobaric diuresis. Showing the percentage changes in clearances, calculated for a doubling of urine flow by different diuretic agents Arterial Ringer's Percentage increase in pressure fluid Urea Creatinine clearance 14±3 4±3-10±2 Urea clearance 35 ±2 20 ±5 1 ±4 Chloride clearance 475 ±70 400±70 52±30 Number of observations Mean percentage increase 167 ± ± ±30 in urine flow connexion with Table II; it is illustrated in Fig. 4 and involves following the progressive changes due to successive doses of the diuretic agent without the intermediate returns to control conditions rendered possible by the double perfusion arrangement. Such a procedure has greater justification in the anaesthetized dog, for under our experimental conditions the urinary output and composition remain fairly constant if not
10 ' ' p.m. Fig.4. Dilution diuresis in the chloralosed dog. The increase in urine flow, and changes in the creatinine, urea, and chloride clearances with decreasing concentration of serum protein due to addition of Ringer's fluid. A broken line is inserted at 1% total solids, so that the values above this indicate the approximate concentration of plasma protein. Dog 10.5 kg. Kidney denervated. Arterial pressure increased from 95mm. Hg to l10 mm. before 3.30 p.m. and was kept approximately at that value thereafter by appropriate removal of blood.
11 346 M. G. EGGLETON AND OTHERS intentionally changed as indicated in Fig. 7, whereas the output of the isolated kidney systematically declines as the experiment progresses as indicated in Fig. 6. The characteristic effects of dilution diuresis are seen in Fig. 4 and in more quantitative form in Table III. In contrast with the isolated kidney, the kidney in situ responds to dilution of the plasma with a change in creatinine clearance which is definitely smaller than that associated with the same increase in urine flow produced by raising the arterial pressure. In our few observations on the action of urea in the anaesthetized dog secreting under isobaric conditions the creatinine clearance decreased, and it might be fair in respect of this variable to place dilution diuresis about half-way between pressure diuresis and urea diuresis, although dilution diuresis produced no significant increase in creatinine clearance. The fall in creatinine clearance during urea diuresis may well have been due to a rise in intrarenal pressure, and a similar rise may have prevented a greater increase in clearance during dilution diuresis. It may be recalled that pressure diuresis differs from urea diuresis in being unaccompanied by a change in intrarenal pressure [Winton, 1936]. The urea clearance increases in dilution diuresis by something of the order of one-half the increase in pressure diuresis, there being no change in clearance during urea diuresis. The increase in chloride clearance due to dilution is about the same as that in pressure diuresis in the anaesthetized dog, whereas in the isolated perfused organ dilution diuresis resembles urea diuresis more closely in this respect. The evidence with regard to the mechanism of dilution diuresis in the anaesthetized dog is, therefore, more definite than it is in the isolated kidney. A twofold increase in urine flow accompanied by little increase in creatinine clearance, which is substantially less than the increase produced in pressure diuresis of the same extent, cannot be attributed solely to an increased rate of glomerular filtration. It is clear that in this preparation dilution of the plasma produces a specific change in tubular activity inhibiting reabsorption of water, and that dilution diuresis is in large part due to this action on the tubules, and only in a smaller degree to an increase in glomerular filtration. The comparison of dilution diuresis with glomerular and tubular diuresis under isorrheic conditions Isolated kidney. A more exact analysis of the effects of dilution of the serum can be based on observations in which the increase in urine flow is just prevented by suitable reduction of the pressure head governing the
12 MECHANISMS OF DILUTION DIURESIS formation of urine, and measuring both these changes in pressure and the changes in the composition of the urine. Such an experiment can be conducted in two ways, each having its advantages. The urine flow may be kept constant by variations in arterial pressure (Fig. 5); although the 0 Creatinine cearance (c.c.min.) Urine flow (c.e.i/min.) w. n *z a * * Ot Fig. 5. Isorrheic dilution diuresis in the isolated kidney. Showing absence of effect of dilution on creatinine clearance, and the relation between arterial pressure and degree of dilution when urine flow is kept constant. Double pump-lung single kidney preparation. Kidney weight 22 g. Initial blood flow 105 cc./min. tubular activity can then be said to remain unaffected by the pressure change, for a purely "glomerular diuresis" has been defined so as to include the characteristically associated changes in tubule function (Fig. 2), the relation between the changes in arterial and glomerular capillary pressure are not certainly known. The urine flow may be kept
13 348 M. G. EGGLETON AND OTHERS constant by variations in ureter pressure (Fig. 6); this provides for a direct comparison of the forms of diuresis due to arterial pressure, dilution and urea acting under isorrheic conditions, and probably enables the variations in pressure in the glomerular capsule to be measured fairly accurately [Winton, 1931 a]; nevertheless we have recently discovered a small effect of ureter pressure on tubular activity [Eggleton, Pappenheimer & Winton, 1940b] and this complicates the interpretation of the changes in composition of the urine. The procedure adopted in experiments designed to compare dilution and pressure diuresis under isorrheic conditions is illustrated in Fig. 5. When the kidney is transferred to the circuit containing diluted blood, the arterial pressure is also reduced to an extent necessitated by the condition that the urine flow is to remain unchanged. This adjustment is not easy and requires experience and constant attention throughout the experiment. The adjustments were made relatively quickly and precisely with the aid of the recording urine flow-meter described by one of us [Winton, 1939]. After a suitable delay during which a steady state was obtained, two or three consecutive samples of urine secreted from the diluted blood were collected. The kidney was then restored to the control circuit, the arterial pressure being raised just far enough to compensate for the more concentrated blood, and after suitable delay two or three successive samples of urine were collected. In this way the composition of the urine and the arterial pressure during isorrheic dilution diuresis could be fairly compared with the average value for the same variables obtained before and after on undiluted blood, in spite of the gradual decline in the creatinine clearance. The main points demonstrated by Fig. 5 are the order of accuracy of our technique in keeping the urine flow constant, the fact that the steady decline in creatinine clearance is not substantially accelerated or retarded during the periods of dilution diuresis, and the relation between the degree of dilution of the serum and the change in arterial pressure needed to neutralize its effect on the urine flow. For simplicity, the variations in urea and chloride clearances have been omitted from Fig. 5, but included in the summary of data in Table IV. A corresponding experiment in which an increase in ureter pressure was adjusted so as to neutralize the increase in urine flow due to serum dilution is illustrated in Fig. 6. It shows again the order of accuracy achieved in matching the urine flows, it shows the relation between the equivalent ureter pressures and serum dilution when the serum is progressively diluted, but it differs from Fig. 5 especially in showing a small
14 MECHANISMS OF DILUTION DIURESIS 349 but systematic reduction in creatinine clearance during dilution diuresis. We have found a similar decline in creatinine clearance when a rise in ureter pressure is neutralized by an increase in arterial pressure, the composition of the blood remaining unchanged [Eggleton et al b], and the decline shown in Fig. 6 cannot, therefore, be attributed to serum dilution. i.u IJ.U 7.0p.m. Fig. 6. Isorrheic dilution diuresis in the isolated kidney. Showing relation between ureter pressure and degree of dilution when urine flow is kept constant, and the small decrease in creatinine clearance due to rise in ureter pressure. Double pump-lung single kidney preparation. Kidney weight 20 g. Initial blood flow 135 c.c./min. Arterial pressure mm. Hg. Our observations on isorrheic diuresis in the isolated kidney are summarized in Table IV, all values being reduced to the percentage change per 100 mm. Hg, on the assumption that the change in value is proportional to the change in pressure. -This assumption is made for simplicity in presentation, and is only approximately true. It should be
15 350 M. G. EGGLETON AND OTHERS TABLE IV. Isolated kidney. Isorrheic diuresis. Showing the percentage changes in clearances when increase of urine flow due to various diuretic agents was prevented by decrease in arterial pressure or by increase in ureter pressure. Results expressed per 100 mm. Hg change in pressure Controlled by Controlled by changes in ureter pressure changes in arterial pressure Arterial Ringer's Diuretic agent... Ringer's fluid pressure fluid Urea Percentage change in Creatinine clearance ±15-47±12-73 ± ±15 Urea clearance +6 6±8-20±10-17 ±20-144±23 Chloride clearance - 80 ±39-19 ± ±53-24 ±52 Number of observations Mean increase in pressure (mm. Hg) noted that whereas 100 mm. Hg change in ureter pressure probably represents nearly the same change in pressure in the glomerular capsule, a change of 100 mm. in arterial pressure probably represents only mm. change in the glomerular capillaries. The salient features of these results are (1) with reference to the creatinine clearance, both arterial and ureter pressure experiments indicate an approach of dilution diuresis to pressure diuresis, but taken together both suggest that this approach may be incomplete and that a small inhibition of tubular reabsorption of water may contribute to the phenomena, (2) with reference to urea clearance, the approach of dilution to pressure diuresis seems complete in both types of experiment, urea diuresis giving widely different values, and (3) with reference to chloride clearance, there appears in both types of experiment to be a smaller output of chloride during dilution diuresis than in pressure diuresis, and the few observations on isorrheic urea diuresis suggest that dilution diuresis involves also a smaller output of chloride than does urea diuresis. The averages of the increases in pressure actually observed are given at the foot of the table, and show that the magnitude of isorrheic diuresis was of the same order in the different classes of experiment tabulated. Anaesthetized dog. The observations on the kidney in situ secreting under isorrheic conditions were planned less elaborately than those on the isolated kidney for reasons described at the beginning of the section on isobaric diuresis in the whole animal. Many of the experiments summarized in Table V were simpler and more direct in design than that depicted in Fig. 7, which was chosen for illustration because it showed in one experiment many of the important features of both dilution and urea diuresis as manifested in both its isobaric and isorrheic forms. Isobaric
16 MECHANISMS OF DILUTION DIURESIS 351 dilution diuresis is shown to produce only a trivial increase in creatinine clearance, but a more considerable increase in the urea and chloride Fig. 7. Isorrheic diuresis in the chloralosed dog. Changes in creatinine, urea, and chloride clearances when the increased urine flow due to (a) Ringer's fluid, (b) urea, is reduced to the pre-diuretic level by rise in ureter pressure. A broken line is inserted at 1% total solids, so that the values above this indicate the approximate concentration of plasma protein. Dog 18 kg. Kidney denervated. clearances. A rather severe isobaric urea diuresis, on the other hand, is accompanied by a fall in creatinine clearance, no great change in urea clearance and a rise in chloride clearance.
17 352 M. G. EGGLETON AND OTHERS The influence of isorrheic dilution diuresis on the composition of the urine is shown in the summary of our observations in Table V. The chief reason for the differences in the decline of creatinine and urea clearances shown under the headings " arterial pressure" and " ureter pressure" is TABLE V. Anaesthetized dog. Isorrheic diuresis. Showing the percentage changes in clearances in dilution diuresis when urine flow is prevented from rising by a decrease in arterial pressure or by an increase in ureter pressure. Results expressed per 100 mm. Hg change in pressure Controlled by Controlled by changes in arterial changes in ureter pressure pressure Creatinine clearance -57 ± Urea clearance -32± Chloride clearance -44± ±245 Number of observations 5 8 Mean increase in pressure (mm. Hg) that 100 mm. change in arterial pressure represents only about two-thirds of the change in glomerular pressure which is produced by 100 mm. change in ureter pressure. It is not known whether ureter pressure modifies tubular activity in the whole animal in any way comparable with the small effect of this kind it produces in the isolated kidney. It is clear that if dilution of the plasma is accompanied by a change in pressure, such that there is no change in urine flow, there is reduction in creatinine clearance, and probably also in urea clearance. The changes in chloride clearance are variable. The hydrostatic pressure equivalent to a change in the colloid osmotic pressure of the serum The technique of measuring pressure changes during isorrheic dilution diuresis is sufficiently described in connexion with the experiments charted in Figs These measurements are summarized in Table VI, and for the sake of comparison are expressed as the change in pressure calculated for a change by 1% in plasma protein. The hydrostatic pressures given in the table are thus equivalent in their diuretic effect to a change in colloid osmotic pressure of the plasma of about 3 mm. Hg. The disproportion between these pressure changes and the change in colloid osmotic pressure is immediately apparent, and corresponds with the disproportion in the extent of the isobaric diuresis due to dilution described above (Table I). The disproportion in the pressure equivalents in comparisons made on the anaesthetized dog might be attributed to the change in tubular activity accompanying dilution diuresis which seemed
18 MECHANISMS OF DILUTION DIURESIS 353 TABLE VI. Pressure changes (mm. Hg) required to neutralize the diuretic action of a 1% reduction (e.g. from 8%to 7 %) ofplasma proteinsdue to dilutionwith Ringer's fluid Ureter pressure Anaesthetized dog Isolated kidney Denervated Innervated Pressure increase 21 ±2 1 21±4 36 ±12 Number of observations Average reduction in % concentration of plasma proteins Arterial pressure Anaesthetized dog Isolated kidney Denervated Innervated Pressure decrease 15±1-9 18±0-3 50±3 Number of observations Average reduction in % concentration ofplasma proteins to be indicated by observations summarized in Tables III and V. In the isolated kidney, however, the observations summarized in Tables II and IV have emphasized that an increase in glomerular filtration appears to be the major factor in dilution diuresils. To appreciate the significance of the values of the pressure equivalents given in Table VI it is essential to take account of the presence of intrarenal pressure and the fact that it appears to increase during dilution diuresis but not during pressure diuresis [Winton, 1936]. Take, for example, the arterial pressure equivalent in the isolated kidney; the 15 mm. change in the artery would correspond with about 10 mm. change in the glomerular capillaries, but to this reduction in pressure head should be added a value, probably about 10 mm., corresponding to the increase in intrarenal pressure due to dilution of the serum, this 10 mm. acting like a back pressure comparable with that of ureter pressure. If there had been no change in intrarenal pressure, the arterial pressure equivalent might well have been 30 mm. instead of 15 mm. In our observations on the ureter pressure equivalent on the isolated kidney we contrived to prevent such masking of the true pressure equivalents by raising the ureter pressure at the beginning of the experiment above any likely intrarenal pressure, and measuring the further increase in ureter pressure equivalent to serum dilution from this base line. This value of 21 mm. may be a few per cent too high for reasons given elsewhere [Eggleton et al. 1940b], and our fairest estimate of the change in hydrostatic pressure head across the glomerular membrane equivalent to a change by 1% in serum protein would be 20 mm. Hg in the isolated kidney. The observations on the ureter pressure equivalent in the anaesthetized dog were unfortunately conducted without the precaution of an initial rise in ureter pressure. Since a pre-existing intrarenal pressure would act like a small ureter pressure, whereas when the ureter pressure was raised during isorrheic dilution diuresis this would mask all effects of intrarenal pressure, the values for ureter pressure equivalents may be too high by an amount equal to the intrarenal pressure, if any, in the anaesthetized dog before aministration of the diuretic. Consequently, referring to the values in Table VI, the arterial pressure equivalents are lower than and po#sibly only one-half the true equivalents, the ureter pressure equivalent on the anaesthetized dog is, if anything, too high, and only the ureter pressure equivalent in the isolated kidney should be accepted as fairly representing the pressure change across the glomerular membrane.
19 354 M. G. EGGLETON AND OTHERS The question as to whether the hydrostatic pressure equivalent is proportional to serum dilution has not been investigated, but the average values of the dilutions actually used were sufficiently alike, as shown in Table VI, in the different classes of our experiments to yield fairly comparable results. The change in blood flow through the kidney accompanying dilution diuresis It has previously been observed [Whittaker & Winton, 1933] that when an isolated kidney perfused with defibrinated blood is suddenly transferred to perfusion with Ringer's solution at the same temperature, after ,+250 _ 0 ~ * Decrease in % serum protein Fig. 8. The percentage change in blood flow through the isolated kidney during dilution diuresis, compared with changes in the hindlimb under similar perfusion conditions. a quite transient increase, the Ringer flow settles down to a lower value than the blood flow, and is often as low as one-third its original value. This was attributed [Winton, 1937] to the phenomenal increase in intrarenal pressure which obstructs the outflow of the Ringer's solution from the kidney, and so reduces the effective pressure head, thus masking the consequences of reducing the viscosity of the perfusion fluid from that of blood to that of Ringer's solution.
20 MECHANISMS OF DILUTION DIURESIS 355 We have recorded the variations in blood flow in all our experiments on isolated kidneys, and though the effects of dilution of the serum are somewhat variable, it would be fair to say that we usually found very little change in blood flow with moderate dilution, and some reduction in flow with considerable dilution. The characteristic relation is well shown in Fig. 8, in which the change in blood flow through the isolated kidney is contrasted with that in the hindlimb of the dog perfused under similar conditions. The curve for the hindlimb is deduced from data given by Whittaker and Winton, appropriate allowance being made for the change in concentration of serum protein in the fashion indicated by Trevan [1918]. The interpretation of the relation in Fig. 8 would appear to be that a small dilution of the blood may produce a small increase in blood flow, appropriate to the reduction in the viscosity of the blood. If dilution proceeds beyond this, the development of intrarenal pressure obstructs the outflow of blood and thus produces a reduction of pressure head which about compensates for the further reduction in the viscosity of the blood. Beyond a dilution corresponding with a reduction of serum protein by about 3% (e.g. from 8 to 5 %) this compensation breaks down, the intrarenal pressure rising more steeply and effectively reducing the blood flow. DIsCUSSION The disproportionately great effect of serum dilution when the diuresis due to a given change in colloid osmotic pressure is compared with that due to about the same change in hydrostatic pressure across the glomerular membrane has been shown both in the isolated kidney and in the anaesthetized dog. In the isolated kidney the disproportion appears to average about sevenfold, there being good agreement between the measurements made under isobaric and isorrheic conditions. In the anaesthetized dog, while the disproportion appeared about the same or a little less in a few observations under isorrheic conditions, it was greater, amounting to fifteenfold in the more numerous observations on isobaric diuresis. The fact that the disproportion is greater in the organ in situ than after isolation is due to the smaller change in urine flow for a given change in arterial pressure; the increase in flow for a given degree of dilution of the plasma is about the same in the denervated kidney as it is in the isolated kidney (Table I). The interpretation of the disproportion appears to be rather different in the two preparations. In the isolated kidney, comparing equal changes in serum colloid osmotic pressure and in hydrostatic pressure in the glomerulus, dilution produces not only a sevenfold increase in urine flow but about a sixfold
21 356 M. G. EGGLETON AND OTHERS increase in creatinine clearance. Moreover, if the increase in urine flow due to dilution be prevented by reducing the arterial pressure, the isorrheic dilution diuresis is accompanied by a hardly perceptible reduction in creatinine clearance. Now Shannon & Winton (1940) have shown that the creatinine clearance is not a safe guide to the glomerular filtration rate in the isolated kidney, particularly at high U/P ratios. In the experiments described in this communication, however, the U/P ratios were below 40, and, therefore, within the range over which creatinine and inulin U/P ratios are identical. It would seem fair, therefore, to adopt the creatinine clearance as at least a qualitative guide to the rate of glomerular filtration. If so, it is clear that the chief reason for the unexpectedly great diuretic action of serum dilution is an unexpectedly great increase in glomerular filtration, supplemented in quite a minor way by a change in tubular activity, involving a smaller reabsorption of water. A possibility may be envisaged, that the excessive diuresis following dilution of the blood is due to an increase in glomerular capillary pressure, comparable with that produced by caffeine, without change in renal arterial pressure. This possibility can be excluded for two reasons: (1) diuresis due to considerable dilution could often only be explained by a rise of glomerular pressure well above the arterial pressure, and (2) isorrheic diuresis would be accompanied by a reduction in the viscosity of blood in the vasa afferentia and efferentia, which for reasons already indicated [Winton, 1937] would if anything lower the glomerular pressure slightly in relation to the arterial pressure rather than raise it. The reason for this great increase in rate of glomerular filtration in dilution diuresis when the pressure head across the membrane is unchanged must be either that the surface area of the membrane is greatly enlarged or that the permeability of the membrane is correspondingly increased. Reasons have been given against supposing that the proportion of active glomeruli varies in the mammalian kidney [White, 1939], and the grounds for regarding this proportion as constant in the isolated kidney under our conditions have also been given [Winton, 1937]. In any case, a considerable increase in the number of active glomeruli would give quite -a different value of creatinine clearance from that observed in the isorrheic form of dilution diuresis. Increase in the surface area of individual capillaries in the glomerular tuft would, however, produce the required consequences, but such a change seems in conflict with the histological evidence [Brodie, 1914] that during diuresis it is the intracapsular space rather than the glomerular tuft which increases in size.
22 MECHANISMS OF DILUTION DIURESIS 357 The hypothesis of a variation in permeability of the glomerular membrane has fallen into disrepute because it has commonly been used as a cloak for ignorance of the mechanism of diuresis, and entirely without specific reference to the pressure-flow relation across the membrane. Dilution diuresis in the isolated kidney, however, has now been shown to involve a large increase in filtration rate in circumstances involving little change in filtration pressure (isobaric diuresis), whereas a large reduction in filtration pressure is required to prevent the filtration rate changing from its prediuretic value (isorrheic diuresis). This describes a change in pressure-flow relation which may fairly be taken to define an increase in permeability to water of the glomerular membrane. When ultrafiltration is proceeding across the glomerular membrane at its usual high rate, the layer of serum in immediate contact with the membrane must contain protein in higher concentration than the average protein concentration of the serum in the capillary. Such a highly concentrated layer would presumably present considerable obstruction to ultrafiltration comparable with that encountered in ultrafiltration through artificial membranes. If so, dilution of the serum might produce a reduction in this obstruction and a fall in pressure head greatly in excess of the small theoretical change associated with the change in colloid osmotic pressure. It is not certain, therefore, that the increase in permeability due to dilution of the serum involves a change in the properties of the cells constituting the glomerular membrane. The variations in the urea clearance during dilution diuresis will be discussed in a future communication devoted to an analysis of the urea/ creatinine clearance ratios in various forms of diuresis. The chloride clearance is substantially lower in dilution diuresis, in both its isobaric and isorrheic forms, than in a corresponding pressure diuresis; this is so in spite of the increase in chloride content of the serum which accompames dilution produced, as it has been in our experiments, by adding Ringer's solution to the blood. It would seem that such dilution has a direct effect on the tubule cells, promoting reabsorption of chloride, but whether the effective stimulus is the reduction of colloid osmotic pressure or some slight change in ionic balance in the serum cannot certainly be decided. In the anaesthetized dog the justification for regarding the creatinine clearance as a measure of the rate of glomerular filtration is supported by the identity of the inulin and creatinine clearances at all U/P -ratios [Shannon & Winton, 1940]. In isobaric dilution diuresis there may be no change in creatinine clearance, or there may be an increase which is, however, considerably smaller than that accompanying pressure diuresis
23 358 M. G. EGGLETON AND OTHERS of the same magnitude. The creatinine clearance in considerable isobaric urea diuresis falls, presumably owing to the development of intrarenal pressure, though this has not been measured in the anaesthetized animal. It is evident that dilution diuresis in the whole animal involves a much greater change in tubular activity than in the isolated kidney. The inhibition of tubular reabsorption of water is a factor in the diuresis at least as important as, and possibly more important than, the increase in the formation of glomerular filtrate. This interpretation is confirmed by those observations on isorrheic diuresis in which dilution of the blood was accompanied by a suitable reduction in arterial pressure, there being a substantial fall in creatinine clearance although the urine flow is unchanged. The significance of the observations in which a rise in ureter pressure counteracted the diuretic influence of blood dilution is doubtful, because no information is yet available about the direct effect of ureter pressure on tubular activity in the anaesthetized animal. It has become usual in recent years to regard the phenomena of water diuresis and of dilution diuresis as entirely distinct, the former being attributed to inhibition of the tubular reabsorption of water, and the latter to an increase in glomerular filtration. As we have now demonstrated that there is an inhibition of tubular reabsorption of water which is a major factor in dilution diuresis, this distinction is no longer so clear cut. It should be emphasized that this tubular factor is detected by contrasting dilution with pressure diuresis, and the changes in tubule activity concomitant on increased glomerular filtration in pressure diuresis are not concerned in the evaluation of this factor. The question whether the effect of blood dilution on the tubules is due to a change in colloid osmotic pressure, and if so whether this effect is a direct one on the tubule cells or an indirect, involving possibly some hormonal mechanism in the animal, is under investigation by our colleague Dr L. Podhradszky. The changes in chloride clearance during dilution diuresis are again rather different in the anaesthetized dog from those found in the isolated kidney. In the whole animal there is in isobaric diuresis an increase in chloride clearance nearly as great as that in pressure diuresis, but since this is accompanied by an increase in creatinine clearance which is much smaller than that in pressure diuresis, we may infer an inhibition of reabsorption of chloride as a consequence of blood dilution. A similar inference may be drawn from our observations on isorrheic dilution diuresis in the anaesthetized animal.
24 MECHANISMS OF DILUTION DIURESIS 359 As disillusion has so often followed the most convincing advocacy of renal theories, it may be well, in conclusion, to summarize those of our results which can easily be expressed in a form independent of theoretical beliefs, even the belief that the creatinine clearance is related to the rate of glomerular filtration. We may set out (Table VII) the characteristic TABLE VII. The difference between pressure and dilution diuresis expressed as a percentage of the difference between pressure and urea diuresis (from data in Tables II-V) Isolated kidney,- A Anaesthetized dog Isobaric Isorrheic Isobaric diuresis diuresis diuresis Creatinine clearance Urea clearance Chloride clearance Total osmotic work 12 changes in the composition of the urine induced during dilution diuresis, compared with the standards of reference we have chosen, namely, pressure diuresis and urea diuresis. Each figure in the table represents the difference between the values for dilution and pressure diuresis in respect of one variable, expressed as a percentage of the corresponding difference between the values for pressure and urea diuresis. Those who believe that pressure diuresis is primarily due to increase in glomerular filtration, or who define " glomerular diuresis " in this way, and that urea diuresis is primarily due to change in activity of the tubules, or who define "tubular diuresis" in this way, would interpret the values in Table VII as giving a guide to the magnitude of the tubular factors operating in dilution diuresis. SUMMARY 1. The mechanism of dilution diuresis has been investigated in the anaesthetized dog and pump-lung-kidney preparation by comparison with pressure diuresis and urea diuresis, both under isobaric conditions, i.e. when the pressure head is not changed, and under isorrheic conditions, i.e. when the urine flow is kept constant by suitable adjustments of arterial or ureter pressure. 2. Dilution diuresis (isobaric) due to a given change in colloid osmotic pressure of the plasma is disproportionately greater than pressure diuresis due to an equivalent change in hydrostatic pressure across the glomerular membrane. The disproportion is about sixfold in the isolated kidney and fifteenfold in the anaesthetized dog (Table I). 3. The increase in urine flow due to a reduction in colloid osmotic pressure of the serum of 3 mm. Hg can just be prevented by a mean PH. XCVIII. 24
25 360 M. G. EGGLETON AND OTHERS increase in ureter pressure of (11) mm. Hg in experiments on the isolated kidney so designed as to prevent interference by changes in intrarenal pr9ssure. Disproportionately high arterial and ureter pressure equivalents were also found in isorrheic diuresis in the anaesthetized dog (Table VI). 4. Comparisons of changes in creatinine and urea clearances in both the isobaric and isorrheic forms of diuresis due to dilution, pressure and urea show that dilution diuresis in the isolated kidney is mainly due to increase in the rate of glomerular filtration, whereas in the anaesthetized dog a change in tubular activity Involving reduction in the reabsorption of water is a major factor (Tables II-V). 5. In spite of the increase in plasma chloride concentration after administration of Ringer's solution, there is an increased reabsorption of chloride in the isolated kidney. In the anaesthetized dog, on the other hand, dilution diuresis involves diminished reabsorption of chloride. 6. The disproportionately increased glomerular filtration rate during dilution diuresis in the isolated kidney is attributed to increased permeability to water of the glomerular membrane, possibly owing to lessening of an obstruction due to protein in the layer in immediate contact with the membrane, the protein being highly concentrated because left behind during rapid ultrafiltration. REFERENCES tbarcroft, J. & Straub, H. [1910]. J. Phy8iol. 41, 145. Bickford, R. J. & Winton, F. R. [1937]. J. Phy8iol. 89, 198. Brodie, T. G. [1914]. Proc. Roy. Soc. B, 87, 571. Cushny, A. R. [1917]. The Secretion of Urine, p London. Eggleton, M. G., Pappenheimer, J. R. & Winton, F. R. [1940a]. J. Physiol. 97, 363. Eggleton, M. G., Pappenheimer, J. R. & Winton, F. R. [1940b]. (In preparation for publication.) Knowlton, F. P. [1911]. J. Phy8iol. 43, 219. Magnus, R. [1900]. Arch. exp. Path. Pharmak. 44, 68, 396. Shannon, J. A. & Winton, F. R. [1940]. J. Physiol. (in the Press). 'Starling, E. H. [1899]. J. Physiol. 24, 317. Trevan, J. W. [1918]. Biochem. J. 12, 60. Verney, E. B. & Winton, F. R. [1930]. J. Physiol. 69, 153. White, H. L. [1939]. Amer. J. Physiol. 128, 159. Whittaker, S. R. F. & Winton, F. R. [1933]. J. Physiol. 78, 339. Winton, F. R. [1931a]. J. Physiol. 71, 382. Winton, F. R. [1931b]. J. Physiol. 72, 361. Winton, F. R. [1933]. J. Physiol. 78, 9P. Winton, F. R. [1936]. J. Physiol. 87, 18P. Winton, F. R. [1937]. Physiol. Rev. 17, 408. Winton, F. R. [1939]. J. Physiol. 95, 60P.
capillaries, and a consequent increased transudation, without necessarily altering to any marked extent the total circulation of blood
 612.463.4 THE CONTROL OF THE GLOMERULAR PRESSURE BY VASCULAR CHANGES WITHIN THE ISOLATED MAMMALIAN KIDNEY, DEMONSTRATED BY THE ACTIONS OF ADRENALINE. BY F. R. WINT0N (Beit Memorial Research Fellow). (Depaortment
612.463.4 THE CONTROL OF THE GLOMERULAR PRESSURE BY VASCULAR CHANGES WITHIN THE ISOLATED MAMMALIAN KIDNEY, DEMONSTRATED BY THE ACTIONS OF ADRENALINE. BY F. R. WINT0N (Beit Memorial Research Fellow). (Depaortment
(ethanol) suggests that it is similar to the diuresis following ingestion of water.
 435 J. Physiol. (I946) I04, 435-442 6I2.464.I THE EFFECT OF ETHYL ALCOHOL AND SOME OTHER DIURETICS ON CHLORIDE EXCRETION IN MAN BY M. GRACE EGGLETON AND ISABEL G. SMITH, From the Physiology Department,
435 J. Physiol. (I946) I04, 435-442 6I2.464.I THE EFFECT OF ETHYL ALCOHOL AND SOME OTHER DIURETICS ON CHLORIDE EXCRETION IN MAN BY M. GRACE EGGLETON AND ISABEL G. SMITH, From the Physiology Department,
Ludwig also recognized that the effects of increase in capsular. Heidenhain, however, emphasized particularly the reduction in
 6I2.463.5:6I2.I44 THE INFLUENCE OF VENOUS PRESSURE ON THE ISOLATED MAMMALIAN KIDNEY. BY F. R. WINTON. Beit Memorial Fellow. (From the Department of Pharmacology, University College, London.) INTRODUCTION.
6I2.463.5:6I2.I44 THE INFLUENCE OF VENOUS PRESSURE ON THE ISOLATED MAMMALIAN KIDNEY. BY F. R. WINTON. Beit Memorial Fellow. (From the Department of Pharmacology, University College, London.) INTRODUCTION.
College of Medicine, Newcastle-upon-Tyne.)
 GLUCOSE ABSORPTION IN THE RENAL TUBULES OF THE FROG. BY G. A. CLARK. (From the Physiological Laboratory of the University of Durham College of Medicine, Newcastle-upon-Tyne.) OPINION is divided on the
GLUCOSE ABSORPTION IN THE RENAL TUBULES OF THE FROG. BY G. A. CLARK. (From the Physiological Laboratory of the University of Durham College of Medicine, Newcastle-upon-Tyne.) OPINION is divided on the
simultaneously excreted. They also brought forward some evidence to
 THE EXCRETION OF CHLORIDES AND BICARBON- ATES BY THE HUMAN KIDNEY. BY H. W. DAVIES, M.B., B.S., J. B. S. HALDANE, M.A. AND G. L. PESKETT, B.A. (From the Laboratory, Cherwell, Oxford.) AM BARD and PAPI
THE EXCRETION OF CHLORIDES AND BICARBON- ATES BY THE HUMAN KIDNEY. BY H. W. DAVIES, M.B., B.S., J. B. S. HALDANE, M.A. AND G. L. PESKETT, B.A. (From the Laboratory, Cherwell, Oxford.) AM BARD and PAPI
GLUCOSE is the most important diffusible substance in the blood which
 ON THE ACTION OF PHLORHIZIN ON THE KIDNEY. By E. B. MAYRS. (From the Department of Pharmacology, Edinburgh.) GLUCOSE is the most important diffusible substance in the blood which is completely held back
ON THE ACTION OF PHLORHIZIN ON THE KIDNEY. By E. B. MAYRS. (From the Department of Pharmacology, Edinburgh.) GLUCOSE is the most important diffusible substance in the blood which is completely held back
necessity for an investigation into possible different types of urine acidity. In
 456 J. Physiol. (I947) io6, 456-465 6I2.46i SOME FACTORS AFFECTING THE ACIDITY OF URINE IN MAN BY M. GRACE EGGLETON From the Department of Physiology, University College, London (Received 22 February 1947)
456 J. Physiol. (I947) io6, 456-465 6I2.46i SOME FACTORS AFFECTING THE ACIDITY OF URINE IN MAN BY M. GRACE EGGLETON From the Department of Physiology, University College, London (Received 22 February 1947)
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
Renal Quiz - June 22, 21001
 Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Renal Quiz - June 22, 21001 1. The molecular weight of calcium is 40 and chloride is 36. How many milligrams of CaCl 2 is required to give 2 meq of calcium? a) 40 b) 72 c) 112 d) 224 2. The extracellular
Cushny(4) has shown, however, that the amount of urea in the kidney. by some vital process, retain those diflusible substances which are of
 THE FUNCTION OF THE TUBULES IN KIDNEY EXCRETION. BY E. B. MAYRS. (From the Department of Pharmacology, Edinburgh.) IT is becoming generally recognised that filtration through the glomeruli and some degree
THE FUNCTION OF THE TUBULES IN KIDNEY EXCRETION. BY E. B. MAYRS. (From the Department of Pharmacology, Edinburgh.) IT is becoming generally recognised that filtration through the glomeruli and some degree
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015
 RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
RNPDC CCNP Anatomy and Physiology: Renal System Pre-Quiz 2015 1. In which abdominal cavity do the kidneys lie? a) Peritoneum. b) Anteperitoneal. c) Retroperitoneal. d) Parietal peritoneal 2. What is the
clamped. At 30- or 60-minute intervals urine specimens were collected and the bladder washed out with saline
 Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
Downloaded from http://www.jci.org on January 11, 218. https://doi.org/1.1172/jci11171 THE MECHANISM OF THE EXCRETION OF VITAMIN C BY THE HUMAN KIDNEY AT LOW AND NORMAL PLASMA LEVELS OF ASCORBIC ACID 1
corresponding to the pulsatile flow of blood normally produced by
 THE HEART, LUNG, KIDNEY PREPARATION. BY F. A. BAINBRIDGE AND C. L. EVANS. (From the Institute of Physiology, University College, London.) THE methods hitherto generally employed for the perfusion of isolated
THE HEART, LUNG, KIDNEY PREPARATION. BY F. A. BAINBRIDGE AND C. L. EVANS. (From the Institute of Physiology, University College, London.) THE methods hitherto generally employed for the perfusion of isolated
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
entirely by glomerular filtration and was neither reabsorbed nor secreted
 6I2.46I.63 INORGANIC SULPHATE EXCRETION BY THE HUMAN KIDNEY. BY CUTHBERT L. COPE. (From the Biochemistry Department, Oxford, and the Radcliffe Infirmary, Oxford.) IN putting forward his modern theory of
6I2.46I.63 INORGANIC SULPHATE EXCRETION BY THE HUMAN KIDNEY. BY CUTHBERT L. COPE. (From the Biochemistry Department, Oxford, and the Radcliffe Infirmary, Oxford.) IN putting forward his modern theory of
Question 1: Solution 1: Question 2: Question 3: Question 4: Class X The Excretory System Biology
 A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
A. MULTIPLE CHOICE TYPE: (select the most appropriate option in each case) Book Name: Selina Concise Question 1: Excretion primarily involves (a) removal of all byproducts during catabolism (b) removal
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
University College, London.)
 6I2.I2I:547.472*3 LACTIC ACID FORMATION AND REMOVAL WITH CHANGE OF BLOOD REACTION. BY M. GRACE EGGLETON1 AND C. LOVATT EVANS. (From the Department of Physiology and Biochemistry, University College, London.)
6I2.I2I:547.472*3 LACTIC ACID FORMATION AND REMOVAL WITH CHANGE OF BLOOD REACTION. BY M. GRACE EGGLETON1 AND C. LOVATT EVANS. (From the Department of Physiology and Biochemistry, University College, London.)
technique by Hemingway [1931] makes it possible to
![technique by Hemingway [1931] makes it possible to technique by Hemingway [1931] makes it possible to](/thumbs/90/101795941.jpg) 6I2.464 THE ACTION OF CYANIDE ON THE ISOLATED MAMMALIAN KIDNEY. BY L. E. BAYLISS' AND E. LUNDSGAARD2 (Copenhagen). (From the Department of Physiology and Biochemistry, University College, London.) THE
6I2.464 THE ACTION OF CYANIDE ON THE ISOLATED MAMMALIAN KIDNEY. BY L. E. BAYLISS' AND E. LUNDSGAARD2 (Copenhagen). (From the Department of Physiology and Biochemistry, University College, London.) THE
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
MOLECULAR SIZE, ELECTRICAL CHARGE, AND SHAPE DETERMINE THE FILTERABILITY OF SOLUTES ACROSS THE GLOMERULAR FILTRATION BARRIER
 MOLECULAR SIZE, ELECTRICAL CHARGE, AND SHAPE DETERMINE THE FILTERABILITY OF SOLUTES ACROSS THE GLOMERULAR FILTRATION BARRIER The glomerular filtration barrier consists of three elements: (1) endothelial
MOLECULAR SIZE, ELECTRICAL CHARGE, AND SHAPE DETERMINE THE FILTERABILITY OF SOLUTES ACROSS THE GLOMERULAR FILTRATION BARRIER The glomerular filtration barrier consists of three elements: (1) endothelial
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
UNIT 3 Conditions supporting life
 Biology Form 4 Page 32 Ms. R. Buttigieg UNIT 3 Conditions supporting life In this unit we shall be seeing how an important condition that supports life is the ability of the organism to maintain a constant
Biology Form 4 Page 32 Ms. R. Buttigieg UNIT 3 Conditions supporting life In this unit we shall be seeing how an important condition that supports life is the ability of the organism to maintain a constant
Na + Transport 1 and 2 Linda Costanzo, Ph.D.
 Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Na + Transport 1 and 2 Linda Costanzo, Ph.D. OBJECTIVES: After studying this lecture, the student should understand: 1. The terminology applied to single nephron function, including the meaning of TF/P
Pressure Diuresis 9 Sample Student Essays
 Pressure Diuresis 9 Sample Student Essays Below please find assembled consecutively in one document the brief analyses submitted by nine students in Mammalian Physiology 08 to the Teach Yourself Pressure
Pressure Diuresis 9 Sample Student Essays Below please find assembled consecutively in one document the brief analyses submitted by nine students in Mammalian Physiology 08 to the Teach Yourself Pressure
already been published [O'Connor, 1958 b]. emphasized that the most prominent action of adrenaline on the kidney is to
![already been published [O'Connor, 1958 b]. emphasized that the most prominent action of adrenaline on the kidney is to already been published [O'Connor, 1958 b]. emphasized that the most prominent action of adrenaline on the kidney is to](/thumbs/88/116101114.jpg) THE EFFECT ON THE VOLUME AND COMPOSITION OF THE URINE OF THE INFUSION OF ADRENALINE AND NORADRENALINE. By W. J. O'CoNNoR. From the Department of Physiology, School of Medicine, University of Leeds. (Received
THE EFFECT ON THE VOLUME AND COMPOSITION OF THE URINE OF THE INFUSION OF ADRENALINE AND NORADRENALINE. By W. J. O'CoNNoR. From the Department of Physiology, School of Medicine, University of Leeds. (Received
Chapter 25 The Urinary System
 Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Chapter 25 The Urinary System 10/30/2013 MDufilho 1 Kidney Functions Removal of toxins, metabolic wastes, and excess ions from the blood Regulation of blood volume, chemical composition, and ph Gluconeogenesis
Urinary System and Fluid Balance. Urine Production
 Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
Urinary System and Fluid Balance Name Pd Date Urine Production The three processes critical to the formation of urine are filtration, reabsorption, and secretion. Match these terms with the correct statement
General renal pathophysiology
 General renal pathophysiology 1 Relationship between plasma solute concentration and its excretion by kidneys General scheme of a feedback regulation (ig 1) 1 Relationship between plasma solute concentration
General renal pathophysiology 1 Relationship between plasma solute concentration and its excretion by kidneys General scheme of a feedback regulation (ig 1) 1 Relationship between plasma solute concentration
hold for the human kidney.2 Shannon and Smith (4) have rightfully stressed
 THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
THE RENAL EXCRETION OF INULIN AT LOW PLASMA CONCEN- TRATIONS OF THIS COMPOUND, AND ITS RELATIONSHIP TO THE GLOMERULAR FILTRATION RATE IN NORMAL, NEPHRITIC AND HYPERTENSIVE INDIVIDUALS' By BENJAMIN F. MILLER,
Visscher(6) that the oxygen consumption of the heart-lung preparation
 BY A. R. FEE1 AND A. HEMINGWAY. (From the Department of Physiology and Biochemistry, University College, London.) SEVERAL investigations of the metabolism of the kidney have been made to ascertain the
BY A. R. FEE1 AND A. HEMINGWAY. (From the Department of Physiology and Biochemistry, University College, London.) SEVERAL investigations of the metabolism of the kidney have been made to ascertain the
A. Correct! Flushing acids from the system will assist in re-establishing the acid-base equilibrium in the blood.
 OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
OAT Biology - Problem Drill 16: The Urinary System Question No. 1 of 10 1. Which of the following would solve a drop in blood ph? Question #01 (A) Decreased retention of acids. (B) Increased excretion
ansesthesia; an oncometer was used for measurement of the splenic Laboratory, Cambridge.)
 6I2.4I3:6I2.I43 CAUSE OF RHYTHMICAL. CONTRACTION OF THE SPLEEN. BY J. BARCROFT AN Y. NISIMARU' (Okayama). (From the Physiological Laboratory, Cambridge.) Roy [1881] was the first to discover the rhythmical
6I2.4I3:6I2.I43 CAUSE OF RHYTHMICAL. CONTRACTION OF THE SPLEEN. BY J. BARCROFT AN Y. NISIMARU' (Okayama). (From the Physiological Laboratory, Cambridge.) Roy [1881] was the first to discover the rhythmical
estimates were made of the normal rate of increase in plasma urea over periods in skin and in plasma, hypertonic sodium chloride solution was
 482 J. Physiol. (I95I) II5, 482-487 THE STTE OF BODY WTER IN THE CT BY M. GRCE EGGLETON From the Department of Physiology, University College, London (Received 5 July 1951) In the course of an investigation
482 J. Physiol. (I95I) II5, 482-487 THE STTE OF BODY WTER IN THE CT BY M. GRCE EGGLETON From the Department of Physiology, University College, London (Received 5 July 1951) In the course of an investigation
by Starling [1914] and Daly [1925].
![by Starling [1914] and Daly [1925]. by Starling [1914] and Daly [1925].](/thumbs/83/88889966.jpg) 612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
612.13 PROPERTIES OF THE PERIPHERAL VASCULAR SYSTEM AND THEIR RELATION TO THE SYSTEMIC OUTPUT. BY HENRY BARCROFT. Harmsworth Scholar, St Mary's Hospital, London. (Experiments performed in the Physiological
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Use the following diagram to answer the next question. 1. In the diagram above, pressure filtration occurs in a. W b. X c. Y d. Z
 Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
Part A: Multiple Choice Questions Value: 32 Marks Suggested time: 40 minutes Instructions: For each question select the best answer and record your choice on the Scantron card provided. Using an HB pencil,
WJEC. Kidney. Question
 WJEC Kidney Question 7 Examiner Arholwr yn unig (d) Humans can be affected by a condition known as multiple sclerosis (MS). In this condition T cells of the immune system attack and destroy the
WJEC Kidney Question 7 Examiner Arholwr yn unig (d) Humans can be affected by a condition known as multiple sclerosis (MS). In this condition T cells of the immune system attack and destroy the
Glomerular filtration rate (GFR)
 LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
LECTURE NO (2) Renal Physiology Glomerular filtration rate (GFR) Faculty Of Medicine Dept.Of Physiology The glomerulus Is a tuft of capillaries enclosed within a Bowman capsule. It is supplied by an afferent
excreted, in spite of its constant presence in the blood. Similarly, a salt-free diet will rapidly cause the practical disappearance of chlorides
 THE REGULATION OF EXCRETION OF WATER BY THE KIDNEYS. I. By J. S. HALDANE, M.D., F.R.S. AND J. G. PRIESTLEY, B.M., Captain R.A.M.C., Beit Memorial Research Fellow. NUMEROUS observations tend to show that
THE REGULATION OF EXCRETION OF WATER BY THE KIDNEYS. I. By J. S. HALDANE, M.D., F.R.S. AND J. G. PRIESTLEY, B.M., Captain R.A.M.C., Beit Memorial Research Fellow. NUMEROUS observations tend to show that
MAJOR FUNCTIONS OF THE KIDNEY
 MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
MAJOR FUNCTIONS OF THE KIDNEY REGULATION OF BODY FLUID VOLUME REGULATION OF OSMOTIC BALANCE REGULATION OF ELECTROLYTE COMPOSITION REGULATION OF ACID-BASE BALANCE REGULATION OF BLOOD PRESSURE ERYTHROPOIESIS
Anatomy/Physiology Study Guide: Unit 9 Excretory System
 Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
Anatomy/Physiology Study Guide: Unit 9 Excretory System 1) In the space below, list the primary structures (organs) and their corresponding functions. Structures: Functions: KIDNEY 1) URETER BLADDER URETHRA
University of Edinburgh.)
 THE ACTION OF DIURETICS. BY ARTHUR R. CUSHNY AND C. G. LAMBIE. (From the Pharmacological Laboratory, University of Edinburgh.) IN the study of the action of diuretics', the first question to determine
THE ACTION OF DIURETICS. BY ARTHUR R. CUSHNY AND C. G. LAMBIE. (From the Pharmacological Laboratory, University of Edinburgh.) IN the study of the action of diuretics', the first question to determine
The functions of the kidney:
 The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
The functions of the kidney: After reading this lecture you should be able to.. 1. List the main functions of the kidney. 2. Know the basic physiological anatomy of the kidney and the nephron 3. Describe
THE WATER AND ELECTROLYTE EXCHANGE OF NEREIS DIVERSICOLOR (MULLER)
 34 THE WATER AND ELECTROLYTE EXCHANGE OF NEREIS DIVERSICOLOR (MULLER) BY W. G. ELLIS Zoology Department, University College of North Wales, Bangor {Received g December 1936) (With Nine Text-figures) IT
34 THE WATER AND ELECTROLYTE EXCHANGE OF NEREIS DIVERSICOLOR (MULLER) BY W. G. ELLIS Zoology Department, University College of North Wales, Bangor {Received g December 1936) (With Nine Text-figures) IT
Chapter 23. Composition and Properties of Urine
 Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Osmotic Regulation and the Urinary System. Chapter 50
 Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
Osmotic Regulation and the Urinary System Chapter 50 Challenge Questions Indicate the areas of the nephron that the following hormones target, and describe when and how the hormones elicit their actions.
(Received 27 September 1937)
 222 J. Physiol. (I937) 9I, 222-23I 6I2.46I:6I2.392.6 THE SECRETION OF URINE IN MAN DURING EXPERIMENTAL SALT DEFICIENCY BY R. A. McCANCE AND E. M. WIDDOWSON From the Biochemical Laboratory, King's College
222 J. Physiol. (I937) 9I, 222-23I 6I2.46I:6I2.392.6 THE SECRETION OF URINE IN MAN DURING EXPERIMENTAL SALT DEFICIENCY BY R. A. McCANCE AND E. M. WIDDOWSON From the Biochemical Laboratory, King's College
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
H. M. Carleton, Lecturer in Histology, University of Oxford. (From the Department of Physiology.) INTRODUCTORY.
 Note on the Comparative Effects on Tissues of Isotonic Saline and Distilled Water when used as Solvents for Mercuric Chloride and Formol in Histological Fixation. By H. M. Carleton, Lecturer in Histology,
Note on the Comparative Effects on Tissues of Isotonic Saline and Distilled Water when used as Solvents for Mercuric Chloride and Formol in Histological Fixation. By H. M. Carleton, Lecturer in Histology,
Similarly, oliguria is commonly taken to reflect a uniform reduction of. oliguria. An analysis of such 'peaks' in clearance has been made in
 J. Physiol. (1966), 187, pp. 63-614 With 5 text-ftgures n C li 63 Printed in Great Britain CONCEALED GLO LA A TION BY E. G. BREWIN,* R. E NASHAT AND R. W.P From the Departments of Physiology and Nuclear
J. Physiol. (1966), 187, pp. 63-614 With 5 text-ftgures n C li 63 Printed in Great Britain CONCEALED GLO LA A TION BY E. G. BREWIN,* R. E NASHAT AND R. W.P From the Departments of Physiology and Nuclear
describe the location of the kidneys relative to the vertebral column:
 Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
Basic A & P II Dr. L. Bacha Chapter Outline (Martini & Nath 2010) list the three major functions of the urinary system: by examining Fig. 24-1, list the organs of the urinary system: describe the location
A&P 2 CANALE T H E U R I N A R Y S Y S T E M
 A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
A&P 2 CANALE T H E U R I N A R Y S Y S T E M URINARY SYSTEM CONTRIBUTION TO HOMEOSTASIS Regulates body water levels Excess water taken in is excreted Output varies from 2-1/2 liter/day to 1 liter/hour
The Urinary System. BIOLOGY OF HUMANS Concepts, Applications, and Issues. Judith Goodenough Betty McGuire
 BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
BIOLOGY OF HUMANS Concepts, Applications, and Issues Fifth Edition Judith Goodenough Betty McGuire 16 The Urinary System Lecture Presentation Anne Gasc Hawaii Pacific University and University of Hawaii
Homeostatic Regulation
 Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question.
 Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
Exam Name SHORT ANSWER. Write the word or phrase that best completes each statement or answers the question. Figure 25.1 Using Figure 25.1, match the following: 1) Glomerulus. 2) Afferent arteriole. 3)
** TMP mean page 340 in 12 th edition. Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2:
 QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
QUESTION Questions 1 and 2 Use the following clinical laboratory test results for questions 1 and 2: Urine flow rate = 1 ml/min Urine inulin concentration = 100 mg/ml Plasma inulin concentration = 2 mg/ml
CONTROLLING THE INTERNAL ENVIRONMENT
 AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
AP BIOLOGY ANIMAL FORM & FUNCTION ACTIVITY #5 NAME DATE HOUR CONTROLLING THE INTERNAL ENVIRONMENT KIDNEY AND NEPHRON NEPHRON FUNCTIONS Animal Form & Function Activity #5 page 1 NEPHRON STRUCTURE NEPHRON
Urinary System and Excretion. Bio105 Lecture 20 Chapter 16
 Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Urinary System and Excretion Bio105 Lecture 20 Chapter 16 1 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of the urinary system
Outline Urinary System. Urinary System and Excretion. Urine. Urinary System. I. Function II. Organs of the urinary system
 Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
Outline Urinary System Urinary System and Excretion Bio105 Chapter 16 Renal will be on the Final only. I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure III. Disorders of
ance of the sugar, until at plasma levels of 140 mgm. per cent the creatinine/sugar clearance ratio
 THE RENAL EXCRETION OF CREATININE IN MAN BY JAMES A. SHANNON 1 (From The Department of Physiology, New York University College of Medicine, New York City) In a previous paper the evidence on the excretion
THE RENAL EXCRETION OF CREATININE IN MAN BY JAMES A. SHANNON 1 (From The Department of Physiology, New York University College of Medicine, New York City) In a previous paper the evidence on the excretion
Chapter 13 The Urinary System
 Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
Biology 12 Name: Urinary System Per: Date: Chapter 13 The Urinary System Complete using BC Biology 12, page 408-435 13.1 The Urinary System pages 412-413 1. As the kidneys produce urine, they carry out
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Chapter 25: Urinary System
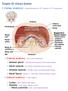 Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Chapter 25: Urinary System I. Kidney anatomy: retroperitoneal from 12 th thoracic to 3 rd lumbar area A. External anatomy: hilus is the indentation 1. Adrenal gland: in the fat at the superior end of each
Complete the table below to compare the processes of excretion and secretion.
 1. Excretion and secretion are two processes that take place in the body of a mammal. Complete the table below to compare the processes of excretion and secretion. excretion secretion one difference one
1. Excretion and secretion are two processes that take place in the body of a mammal. Complete the table below to compare the processes of excretion and secretion. excretion secretion one difference one
STUDIES ON KIDNEY FUNCTION. LX. I. THE RATE OF FILTRATION AND REABSORPTION IN THE HUMAN KIDNEY.
 LX. STUDIES ON KIDNEY FUNCTION. I. THE RATE OF FILTRATION AND REABSORPTION IN THE HUMAN KIDNEY. BY POUL BRANDT REHBERG. From the Laboratory of Zoophysiology, University of Copenhagen. (Received April 26th,
LX. STUDIES ON KIDNEY FUNCTION. I. THE RATE OF FILTRATION AND REABSORPTION IN THE HUMAN KIDNEY. BY POUL BRANDT REHBERG. From the Laboratory of Zoophysiology, University of Copenhagen. (Received April 26th,
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Outline Urinary System
 Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
Urinary System and Excretion Bio105 Lecture Packet 20 Chapter 16 Outline Urinary System I. Function II. Organs of the urinary system A. Kidneys 1. Function 2. Structure B. Urine formation 1. Hormonal regulation
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Physiology (4) 2/4/2018. Wael abu-anzeh
 Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
Physiology (4) 2/4/2018 Wael abu-anzeh In the previous lectures we have discussed the filtration and the reabsorption processes but in this lecture we will talk about the factor that will regulate or control
administration of adrenaline or in cases of increased perfusion pressure. approximately the same within fairly wide variations of the systemic
 6I2. I72. I THE DISTRIBUTION OF THE BLOOD IN THE CORONARY BLOOD VESSELS. BY G. V. ANREP, A. BLALOCK AND M. HAMMOUDA. (From the Physiological Laboratory, Cambridge.) As a result of experiments on perfused
6I2. I72. I THE DISTRIBUTION OF THE BLOOD IN THE CORONARY BLOOD VESSELS. BY G. V. ANREP, A. BLALOCK AND M. HAMMOUDA. (From the Physiological Laboratory, Cambridge.) As a result of experiments on perfused
Renal Excretion of Drugs
 Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Smith, Miller and Grab er(4) state that the maintenance of an efficient
 THE SIGNIFICANCE OF THE DIASTOLIC AND SYSTOLIC BLOOD-PRESSURES FOR THE MAINTENANCE OF THE CORONARY CIRCULATION. BY G. V. ANREP AND B. KING. (From the Physiological Laboratory, Cambridge.) IT is generally
THE SIGNIFICANCE OF THE DIASTOLIC AND SYSTOLIC BLOOD-PRESSURES FOR THE MAINTENANCE OF THE CORONARY CIRCULATION. BY G. V. ANREP AND B. KING. (From the Physiological Laboratory, Cambridge.) IT is generally
Dr.Nahid Osman Ahmed 1
 1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
1 ILOS By the end of the lecture you should be able to Identify : Functions of the kidney and nephrons Signs and symptoms of AKI Risk factors to AKI Treatment alternatives 2 Acute kidney injury (AKI),
Please remember that based on your personalized learning plan and your past experience you may not be required to complete all four modules.
 Course Overview Welcome to the Team PD pre-work participant guide. Team PD is a new education program offered by Baxter that utilizes individual learning maps so nurses receive a personalized approach
Course Overview Welcome to the Team PD pre-work participant guide. Team PD is a new education program offered by Baxter that utilizes individual learning maps so nurses receive a personalized approach
Kidneys and Homeostasis
 16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
16 The Urinary System The Urinary System OUTLINE: Eliminating Waste Components of the Urinary System Kidneys and Homeostasis Urination Urinary Tract Infections Eliminating Waste Excretion Elimination of
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
The technique of multiple clearance was chosen. because it supplied us with the filtration rate, the
 RENAL REABSORPTION OF CHLORIDE AND PHOSPHATE IN NORMAL SUBJECTS AND IN PATIENTS WITH ESSENTIAL ARTERIAL HYPERTENSION' By EDITH B. FARNSWORTH (From the Department of Medicine, Northwestern University Medical
RENAL REABSORPTION OF CHLORIDE AND PHOSPHATE IN NORMAL SUBJECTS AND IN PATIENTS WITH ESSENTIAL ARTERIAL HYPERTENSION' By EDITH B. FARNSWORTH (From the Department of Medicine, Northwestern University Medical
Renal Physiology Intro to CRRT Concepts. Catherine Jones September 2017
 Renal Physiology Intro to CRRT Concepts Catherine Jones September 2017 Learning Outcomes To revise anatomy & physiology of kidney in health: To understand basic principles of continuous renal replacement
Renal Physiology Intro to CRRT Concepts Catherine Jones September 2017 Learning Outcomes To revise anatomy & physiology of kidney in health: To understand basic principles of continuous renal replacement
THE CONTROL OF THE RENAL EXCRETION OF WATER* II. TB~ RATE OF LIBERATION OF THE POSTERIOR PITUITARY ANTIDIURETIC HORMONE IN THE DOG
 Published Online: 1 October, 1942 Supp Info: http://doi.org/10.1084/jem.76.4.387 Downloaded from jem.rupress.org on July 3, 2018 THE CONTROL OF THE RENAL EXCRETION OF WATER* II. TB~ RATE OF LIBERATION
Published Online: 1 October, 1942 Supp Info: http://doi.org/10.1084/jem.76.4.387 Downloaded from jem.rupress.org on July 3, 2018 THE CONTROL OF THE RENAL EXCRETION OF WATER* II. TB~ RATE OF LIBERATION
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
You should know the T max for any substance that you use and for PAH ; T max = mg / min
 Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
Urinary System Organization. Urinary System Organization. The Kidneys. The Components of the Urinary System
 Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
Urinary System Organization The Golden Rule: The Job of The Urinary System is to Maintain the Composition and Volume of ECF remember this & all else will fall in place! Functions of the Urinary System
5.Which part of the nephron removes water, ions and nutrients from the blood?
 Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Uro question 1.While reading a blood test I notice a high level of creatinine, I could assume from this that A) There is a possibility of a UTI B) There is a possibility of diabetes C) There is a possibility
Barsoum & Gaddum [1935a], working on dogs, found that the histamine. obtained a similar effect by severely restricting the arterial blood supply to
![Barsoum & Gaddum [1935a], working on dogs, found that the histamine. obtained a similar effect by severely restricting the arterial blood supply to Barsoum & Gaddum [1935a], working on dogs, found that the histamine. obtained a similar effect by severely restricting the arterial blood supply to](/thumbs/89/99230787.jpg) 297 J. Physiol. (I944) I03, 297-305 547*78iT5:6I6-005.2 LIBERATION OF HISTAMINE DURING REACTIVE HYPERAEMIA AND MUSCLE CONTRACTION IN MAN BY G. V. ANREP, G. S. BARSOUM, S. SALAMA AND Z. SOUIDAN From the
297 J. Physiol. (I944) I03, 297-305 547*78iT5:6I6-005.2 LIBERATION OF HISTAMINE DURING REACTIVE HYPERAEMIA AND MUSCLE CONTRACTION IN MAN BY G. V. ANREP, G. S. BARSOUM, S. SALAMA AND Z. SOUIDAN From the
WJEC. BY4 Kidney Questions
 NAME: OPTION GROUP WJEC BY4 Kidney Questions Question Book 2 (Legacy Qs from Jan 2000 to June 2014) Question Number(s) Due Date & Pass Mark Homework Mark Resist Question number(s) Resist Due Date & Pass
NAME: OPTION GROUP WJEC BY4 Kidney Questions Question Book 2 (Legacy Qs from Jan 2000 to June 2014) Question Number(s) Due Date & Pass Mark Homework Mark Resist Question number(s) Resist Due Date & Pass
November 30, 2016 & URINE FORMATION
 & URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
& URINE FORMATION REVIEW! Urinary/Renal System 200 litres of blood are filtered daily by the kidneys Usable material: reabsorbed back into blood Waste: drained into the bladder away from the heart to the
Acute Kidney Injury (AKI) Undergraduate nurse education
 Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
Acute Kidney Injury (AKI) Undergraduate nurse education Year One Developed Summer 2017 Overview Basic A & P of: Urinary system Kidneys Followed by: Introduction to Acute Kidney Injury Urinary System The
Copyright 2009 Pearson Education, Inc. Copyright 2009 Pearson Education, Inc. Figure 19-1c. Efferent arteriole. Juxtaglomerular apparatus
 /6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
/6/0 About this Chapter Functions of the Kidneys Anatomy of the urinary system Overview of kidney function Secretion Micturition Regulation of extracellular fluid volume and blood pressure Regulation of
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
1. Urinary System, General
 S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
S T U D Y G U I D E 16 1. Urinary System, General a. Label the figure by placing the numbers of the structures in the spaces by the correct labels. 7 Aorta 6 Kidney 8 Ureter 2 Inferior vena cava 4 Renal
Chapter 23. The Nephron. (functional unit of the kidney
 Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
Chapter 23 The Nephron (functional unit of the kidney Renal capsule The Nephron Renal cortex Nephron Collecting duct Efferent arteriole Afferent arteriole (a) Renal corpuscle: Glomerular capsule Glomerulus
