Aykan AKAR, Erdinc CİVELEK, Tufan CANSEVER, Fatih AYDEMİR, Mehmet Nur ALTINÖRS
|
|
|
- Thomas Crawford
- 6 years ago
- Views:
Transcription
1 DOI: / JTN Received: / Accepted: Published Online: Original Investigation The Relationship of the Vertebral Artery with Anatomical Landmarks in the Posterior Craniovertebral Junction of Fresh Human Cadavers in the Turkish Population Aykan AKAR, Erdinc CİVELEK, Tufan CANSEVER, Fatih AYDEMİR, Mehmet Nur ALTINÖRS Baskent University, School of Medicine, Department of Neurosurgery, Ankara, Turkey ABSTRACT AIm: Surgical anatomy concerning the posterior craniovertebral region in fresh human cadavers was studied to provide most accurate information for the surgical approach. MaterIal and Methods: In thirty-two fresh human cadavers, the distance from the posterior tubercle to the sulcus of vertebral artery (VA), the thickness and length of the third segment of VA (V3), the distance of C1/C2 facet to V3, the length, height and shape of the C2 ganglion to the neighboring structures, the distance from medial border of C1 lateral mass to dura mater, the distance of the transverse process of atlas to mastoid tip, the thickness of C1 posterior arcus were measured. Results: There were variations of sulcus of VA in 14 of 32 cadavers (43.7%), the right VA was larger in 23 cadavers (71.8%). The ganglion was found over the C1 lateral mass screw entry point in 45 of 64 ganglions (70.31%) and below the screw entry point in 19 of 64 ganglions (29.69%). The distance of the medial border of the C1 lateral mass to dural tube was 3.81±0.55 mm at the right side and 3.91±0.59 mm at the left. The thickness of C1 posterior arch was 3.73±0.75 mm at the right side and 3.75±0.77 mm at the left. The mean distance from the transverse process of C1 to the mastoid tip was 15.82±4.49 mm at the right side and 15.46±4.38 mm at the left. ConclusIon: This is the most comprehensive and only fresh cadaver study about this region in the literature. Keywords: Anatomical landmark, Craniovertebral junction, Vertebral artery INTRODUCTION The craniovertebral junction and upper cervical spine surgery requires a three-dimensional understanding of the anatomy. Instability in the upper cervical spine can occur when any part of the components are damaged by congenital defects, neoplasm, inflammation, or trauma including fractures of occipital condyle, atlas, axis and atlantooccipital and atlantoaxial dislocations. In 1910, the first description of surgical treatment with posterior approach for instability of upper cervical spine appeared in the literature. Mixter et al. reported securing the posterior arch of the atlas to the spinous process of the axis with a heavy silk thread (20). Since then, other techniques have been developed. These include wire fixation with a midline graft (Gallie-type), wire fixation with two laminar grafts (Brookstype), transarticular screw fixation (Magerl technique), and bilateral laminar clamps (Halifax technique) (4, 19, 20). The most recent technique involves screw fixation of the lateral mass of C1 with pedicle screws to C2 the so-called Goel technique as modified by Harms (29). The proximity of the VA, spinal cord, and C-2 ganglion and nerve root to the upper cervical spine has confirmed the difficulty of the surgery in this region. qr code Corresponding author: Aykan AKAR aykanakar@gmail.com Turk Neurosurg,
2 There are many important structures in this region. The current study which was performed in fresh human cadavers evaluates the morphometric characteristics of these important structures and landmarks. their anatomic position (Figure 4) and the measurements of C2 ganglion were performed (Figures 6, 7). After removing the posterior arch of C1, the distance of the medial part of lateral mass to the dural tube was measured (Figure 8). MATERIAL and METHODS This study was performed in the Center of Forensic Medicine. Thirty-two cadavers aged 18 to 65 years (mean age 43 years, 21 men and 11 women) were used. The cadavers were fresh cadavers chosen in postmortem 12 to 24 hours. Exclusion criteria in chosen cadavers were having neck trauma, gross evidence of congenital or acquired vertebral pathology and previous cervical operation. All dissections were performed by a single neurosurgeon in a private autopsy training room. A digital camera (Sony, 5.1 megapixels), and some necessary tools (tripod and light power) were placed to most proper place to take high-quality pictures during dissections. Surgical Dissection The cadavers were placed on the autopsy table in prone position. For each dissection, we approximated true intraoperative positioning by placing the head of the cadaver in flexed position. The chest was supported with 10 cm height of pad. Instead of a standard linear skin incision beginning at the level of the inion, the routine bicoronal skin incision used in autopsy procedure was lengthened over the mastoid region until the level of the prominence of C7 spinous process (Figure 1). All symmetric structures were measured bilaterally and were used electronic digital calipers and a standard rule accurate to 0.01 mm. Using microsurgical instruments, dissection was carried out from the skin up to the VA, dural tube and C2 ganglion, in layers. The most superficial muscle layer was composed of the trapezius, splenius capitis and semispinalis capitis muscles (Figure 2). We reflected the trapezius and splenius capitis medially, and identified the longissimus capitis and inferiorly the transverse process of Cl, one of the most important bony landmarks for VA identification (Figure 3). Muscle dissection proceeded with the goal of locating the suboccipital triangle composed of the superior and inferior oblique muscles, and the rectus capitis major muscle (Figure 3). Once it was found, we opened this triangle to reveal the VA between C1 and the occiput. Small tributaries from internal vertebral plexus and small muscular veins in the suboccipital triangle form a rich venous plexus around the VA (Figure 3). The spinous process of the 3 rd cervical vertebra, the axis and the posterior arch of the atlas were then visualized. The transverse process of C1 was identified along with the attachment of the superior and inferior oblique muscles (Figure 3). The suboccipital muscles were then removed and the entire posterior arch of the C1 was dissected subperiosteally up to the transverse processes on either side. The VA and suboccipital nerve was then dissected and VA was followed up to its dural entry point (Figures 4, 5). The bony landmarks were defined and digital photographs were taken. The course, relationships and the branches of the VA were studied and measurements were taken (Figure 6). The C2 ganglion and the spinal nerve were preserved in Figure 1: Skin incision used in dissections. Figure 2: The superficial muscle layer photograph of a cadaveric specimen (NL: Nuchal ligament, SCM: sternocleidomastoid muscle, SC: splenius capitus muscle, SSC: semispinalis capitus muscle). 2 Turk Neurosurg, 2016
3 Figure 3: A photograph of a cadaveric specimen (White-thick dashed line: midline, RCMi: Rectus capitis minor muscle, RCMa: Rectus capitis major muscle, pt: posterior tubercle, Sp: spinous process of C2, OCI: inferior oblique capitis muscle, OCS: superior oblique capitis muscle, white-dashed triangle: suboccipital triangle, single asterisks: Dorsal rami of C2 root, double asterisks: vertebral artery, tp: transverse process of C1, mp: mastoid process, l: distance from transverse process of C1 to mastoid process). Figure 4: A photograph of a cadaveric specimen (White-thick dashed line: midline, Oc: occipital bone, aom: atlantooccipital membrane, MS: medulla spinalis, C2g: C2 ganglion, single asterisks: Ventral rami of C2 root, double asterisks: Dorsal rami of C2 root, Va2: second segment of vertebral artery, Va3: third segment of vertebral artery, tp: transverse process of C1, k: the length of third segment of VA). Figure 5: A photograph of a cadaveric specimen (Whitethick dashed line: midline, va: vertebral artery, black arrow: suboccipital nerve, single asterisks: complete canal of vertebral artery sulcus). Figure 6: A photograph of a cadaveric specimen (White-thick dashed line: midline, Oc: occipital bone, va: vertebral artery, C2g: C2 ganglion, single asterisks: medial border of vertebral artery sulcus, double asterisks: C2/C3 facet joint, g: the distance of medial border of C2 ganglion to midpoint of the dural tube, h: the distance of posterior tubercle of atlas to medial border of sulcus of vertebral artery, i: thickness of third segment of vertebral artery, j: the distance of C2 ganglion to midpoint of C2-C3 facet joint). Turk Neurosurg,
4 Measured Landmarks and Structures For each dissection, we recorded the following measurements: 1) the distance of tubercule of atlas to medial border of VA navigating within sulcus, 2) the calibration of 3 rd segment of VA, 3) the length of 3 rd segment of VA, 4) the distance of C1-C2 facet joint to 3 rd segment of VA, 5) the height of C2 ganglion, 6) the length of C2 ganglion, 7) the distance of superior border of C2 ganglion to inferior border of posterior arcus of atlas, 8) the distance of inferior border of C2 ganglion to superior border of the lamina of axis, 9) the distance of superior border of C2 ganglion to 3 rd segment of VA, 10) the distance of C2 ganglion to midpoint of C2-C3 facet joint, 11) the distance of medial border of C2 ganglion to midpoint of the dural tube, 12) the distance from medial border of C1 lateral mass to dural tube, 13) the distance of the tip of the transverse process of Atlas to mastoid tip, 14) the thickness of C1 posterior arcus (so-called pedicle thickness). Figure 7: A photograph of a cadaveric specimen (White-thick dashed line: midline, Oc: occipital bone, va: vertebral artery, C2g: C2 ganglion, sp: spinous process of C2, single asterisks: C1/C2 facet, a: the distance of superior border of C2 ganglion to inferior border of posterior arcus of atlas b: the distance of superior border of C2 ganglion to 3 rd segment of vertebral artery, c: the distance of inferior border of C2 ganglion to superior border of the lamina of axis, d: the length of C2 ganglion, e: the height of C2 ganglion, f: the distance of C1-C2 facet joint to third segment of vertebral artery). Figure 8: A photograph of a cadaveric specimen (White-thick dashed line: midline, Oc: occipital bone, va: vertebral artery, MS: medulla spinalis, m: the distance from medial border of C1 lateral mass to dural tube, single asterisks: C1/C2 facet). The measurements in male and female specimens and the effect of the age on the measurements for each parameter were compared with linear regression test. The values of the right and the left sides were compared with paired sample tests. Statistical significance was set at P<0.05. RESULTS The details of the measurements were listed in the Table I. The sulcus of VA Variations In 14 cadavers (43.8%), a variation of VA sulcus in C1 vertebra was seen. In 9 cadavers (28.1 %) there was semi-canal, in 7 (21.9%) there was complete canal (Figure 9). In 2 (6.3%) cadavers bilateral semi-canal, right-sided semi-canal in 4 cadavers (12.5 %), left-sided semi-canal in 1 cadavers (3.1%), right-sided complete canal in 4 cadavers (12.5%), left-sided complete canal in 1 cadavers (3.1%) and in 2 cadavers (6.3%) both semi-canal and complete canal were present. There were variations of sulcus of VA in 10 of 21 male cadavers (47.6 %) and in 4 of 11 female cadavers (36.4%). Complete canal were present in 5 male (23.8%) and in 2 female cadavers (18.2 %). Localization of suboccipital nerve in VA sulcus Suboccipital nerve was observed at neighboring of posteroinferior part of the vertebral artery in 32 cadavers, and at posterior part of the VA in 2 cadavers (Figure 9). VA (third part) (V3) In all cases, the artery was located in the transverse foramen of C1 and traveled through the suboccipital triangle. The posterior-inferior cerebellar artery did not arise from the VA segment in any specimen. In 23 cadavers, the right VA was larger than the left one and in 9 cadavers the left side was larger (Table I). The larger side was accepted as the dominant side. In 18 cadavers, the right VA was longer than the left and in 14 cadavers the left side was longer (Table I). 4 Turk Neurosurg, 2016
5 The distance of inferior border of V3segment to midpoint of C1-C2 facet joint In 18 cadavers, the left side was longer than the right and in 14 cadavers the right side was longer (Table I). C2 Ganglion The first intervertebral space is not a real foramen as the other cervical levels because it is not limited by any bone structure posteriorly. The C2 ganglion lies with accompanying venous plexus in a large space formed posteriorly by ligamentum flavum. In our observation, at the atlantoaxial interspace the C-2 nerve exited and divided into anterior and posterior rami (Figure 4). The nerve then passed medially and inferiorly to the joint of the C-1 lateral mass. In all dissections the C-2 nerve root ganglion could be retracted downward or upward to expose the lateral mass screw entry zone (Figures 10,11). It was observed that extensive upward or downward moving of the ganglion may cause retraction of the spinal cord and this may cause spinal cord injury. Shapes Figure 9: A photograph of a cadaveric specimen (White-thick dashed line: midline, Oc: occipital bone, va: vertebral artery, C2g: C2 ganglion, ns: suboccipital nerve, single asterisks: semicanal for vertebral artery, noma: major occipital nerve, black arrow: dorsal rami of C3 spinal nerve, double asterisks: branch to C3 spinal nerve). The C2 ganglions were classified in three groups with respect to their shapes (3): 1. Spherical ganglion: The difference between height and the horizontal length of the ganglion was <1 mm. 2. Oval ganglion: The difference between height and the horizontal length of the ganglion was mm. Table I: The Measurements (mm) of the Parameters Male Female Mean Right Left Right Left Right Left C1 post. tubercle- VA sulcus MB 18.90± ± ± ± ± ±2.03 V3 calibration 4.63± ± ± ± ± ±0.88 V3 length 19.28± ± ± ± ± ±1.45 C1/C2 facet joint-v ± ± ± ± ± ±1.87 C2G height 4.88± ± ± ± ± ±0.67 C2G length 5.85± ± ± ± ± ±1.08 C2G SB - C1 post. arcus IB 2.18± ± ± ± ± ±1.29 C2G IB - C2 lamina SB 3.68± ± ± ± ± ±1.60 C2G SB - V3 7.58± ± ± ± ± ±1.57 C2G-C2/C3 facet joint MP 16.73± ± ± ± ± ±2.79 C2G- dural tube MP 13.20± ± ± ± ± ±3.49 C1 lateral mass-dural tube 3.77± ± ± ± ± ±0.59 C1 transverse process tipmastoid tip 15.92± ± ± ± ± ±4.38 C1 pedicle thickness 3.80± ± ± ± ± ±0.77 VA: vertebral artery, G: ganglion, V3: third segment of the vertebral artery, MB: medial border, SB: superior border, IB: inferior border, MP: midpoint. Turk Neurosurg,
6 3. Spindle-like ganglion: The difference between height and the horizontal length of the ganglion was 2.5 mm. There were 17 spherical, 12 oval and 3 spindle-like ganglion at the right side and 14 spherical, 14 oval and 4 spindle-like ganglion at the left side (Table II). According to this definition, 48.4% (31 of 64) of ganglions were spherical, 40.6% (26 of 64) of ganglions were oval, and 10.9% (7 of 64) of ganglions were spindle-like. The ganglions having oval or spherical shapes could be dissected easily but retraction and dissection of the spindle-like shape having ganglions were difficult. The localization of the ganglion according to the point of the lateral mass screwing (The midpoint of the inferior part of the lateral mass) The localization of the ganglion was evaluated by using the lateral mass screwing point which is midpoint of the inferior part of the lateral mass in both mediolateral and cranio-caudal directions. The localizations of the ganglia were described as on, over or below the point. Table II: Distribution of C2 Ganglion Types Right Left Total Spherical ganglion Oval ganglion Spindle-like ganglion The ganglion was found over the screw entry point in 45 of 64 ganglions (70.31%) and below the screw entry point in 19 of 64 ganglions (29.69%) (11 at the right and 8 at the left) (Figures 10,11). The ganglion was covering bilaterally the screw entry point in 19 cadavers, and it was located below the screw entry point bilaterally in 6 cadavers. C1 lateral mass screw trajectory The measurements of distance of the medial border of the C1 lateral mass to dural tube were listed in Table I. The C1 lateral mass screw trajectory is usually 17 degrees medially and 22 degrees cranially. C1 Posterior Arch Thickness (the thickness of so-called C1 pedicle) The part of the posterior arch on the vertical line passing through the entry point of the lateral mass screwing was bilaterally determined. The thickness of C1 posterior arch (the distance between superior and inferior borders was measured (Table I). This distance was measured as below 3 mm in 5 cadavers (15.6%), between 3 and 4 mm in 15 cadavers (46.8%), between 4 and 5 mm in 8 cadavers (25%) and above 5 mm in 4 cadavers (12.5%). The tip of the transverse process of C1 was located anterior, medial, and inferior to the mastoid process. The measurements of distance of the tip of C1 transverse process to the tip of the mastoid process were listed in the Table I. Figure 10: A photograph of a cadaveric specimen (White-thick dashed line: midline, Oc: occipital bone, va: vertebral artery, C2g: C2 ganglion, ns: suboccipital nerve, single asterisks: complete canal variation of vertebral artery sulcus, black arrow: semi-canal variation of vertebral artery sulcus, double asterisks: occipital condyle, triple asterisks: lateral mass). Figure 11: A photograph of a cadaveric specimen (White-thick dashed line: midline, Oc: occipital bone, black arrows: bilateral C2/C3 facet fusion anomaly, plus sign: lateral mass screw inserting point). 6 Turk Neurosurg, 2016
7 In all the quantitative measurements of different parameters, there was no statistically significant difference in the mean values between the right and the left side and no significant differences between the male and female cadavers. DISCUSSION The atlas has two thick lateral masses and these are connected behind by the long posterior arch (21). In up to 5% of the population, the posterior arch of the atlas is incomplete, and recognition of this condition before surgical exploration is important to avoid a damage of the spinal cord (9). In our study, we did not observe such a variation. Senoglu et al. concluded that most congenital anomalies of the arch of atlas are found incidentally in asymptomatic patients. They also concluded that congenital defects of the posterior arch are more common (3.35%) (28). The posterior arch of atlas has a groove which accommodates V3 and C1 spinal nerve. The V3 (suboccipital part) extends from the foramen transversarium of the atlas vertebra to its passage through the dura mater at the foramen magnum. Cacciola et al. concluded that the C1 roots course posteriorinferior in relationship to the artery (5). In our study, suboccipital nerve was observed at neighboring of posteroinferior part of the VA in 32 cadavers, and at posterior part of the VA in 2 cadavers. The arcuate foramen is an anatomical variant of the atlas vertebra: anterior and posterior osseous bridges or ponticles can arch over the VA, to a greater or lesser degree, transforming the arterial groove into a complete or semi-canal. Ponticles are said to occur in 3 to 15% of the population (14). A complete canal was found 1.2% in another study (8). Paraskevas et al. found the presence of a canal for the VA (CVA) in 10.23% and an incomplete CVA in 24.43% (23). The complete canal and semi-canal is more common in males (11.11% and 24.9 %) than in females (9.3% and 24.42%). In our study there were variations of sulcus of VA in 10 of 21 male cadavers (47.6%) and in 4 of 11 female cadavers (36.4%). Complete canal were present in 5 male (23.8%) and in 2 female cadavers (18.2%). Radojevic et al. saw the CVA in 3.4% of the cases and incomplete CVA in 1%, while Lamberty et al. saw the CVA in 7.58% of the cases and incomplete CVA in 6.06% (15, 25). Taitz et al. found in the Middle Eastern population an unusually high percentage of atlas bridging (57%) in comparison to other studies (31). If a posterior ponticulus is present, placing the screw too superiorly might cause VA injury. In a study performed in formalin-fixed cadavers by Tubbs et al., they found that the foramen arcuale may compress the V3. They identified a foramen arcuale in 5% of the cadavers (33). Avci et al. concluded that the artery was completely surrounded by bone at the posterior arch of C1 in 30% of cases (2). In our study, in 14 cadavers (43.8%), a variation of VA sulcus in C1 vertebra was seen. In 9 cadavers (28.1%) there was semi-canal, in 7 (21.9%) there was complete canal. Bilateral semi-canal was present in 2 (6.3%) cadavers, rightsided semi-canal in 4 cadavers (12.5%), left-sided semi-canal in 1 cadaver (3.1%), right-sided complete canal in 4 cadavers (12.5%), left-sided complete canal in 1 cadavers (3.1%) and both semi-canal and complete canal in 2 cadavers (6.3%). The VA, as it lies in the groove along the atlas vertebra, normally glides easily with neck movements. If this movement of the artery is restricted, intimal damage may occur leading to dissection. It was hypothesized that the presence of the arcuate foramen might cause tethering of the VA and lead to its dissection by repetitive trauma (6, 23). In the majority of cases VA occlusion does not cause ischemia, but tends to act as a source of recurrent embolism. A syndrome involving symptoms of headache, retroorbital pain, vasomotor disturbances of the face, and recurrent disturbances of vision, swallowing, and phonation was described and it was hypothesized that these symptoms were due to alternations of the blood flow within the VAs (17). Limousin et al. has reported good results in patients with this syndrome and identified cases in which the foramen arcuale was surgically fractured and a periarterial sympathectomy of the V3 performed. Although the suboccipital nerve also travels with the VA through the foramen arcuale no reported cases of symptomatic entrapment of this nerve at this site have been reported. This may be due to the fact that this nerve primarily innervates the small muscles that form the suboccipital triangle and rarely has a cutaneous branch. Ebraheim et al. suggested that dissection on the posterior aspect of the posterior ring should remain within 12 mm lateral to the midline, and dissection on the superior aspect of the posterior ring should remain within 8 mm of the midline (8). In other studies this distance was varied from 10 mm to 19.7 mm (1, 5, 26, 30). In our study, the mean distance of the VA groove from the midline on the outer cortex was found to be 18.60±2.44 mm. (right side) and 18.25±2.03 mm (left side). These results are greater than the results in the literature (1, 8, 26, 30). In the previous studies the diameter of VA was varying from 2.3 mm to 7.4 mm (2,5). In our study, the average right VA diameter was 4.38±0.77 mm whereas that for the left VA was 4.29±0.88 mm. The larger side was accepted as the dominant side. In 23 cadavers, the right VA was larger than the left one and in 9 cadavers the left side was larger. Cacciola et al. found the length between exit point of the VA from C1 transverse foramen to dural entry point as 32.3 mm to 43.5 mm (average 35.7 mm) (5). In our study, in 18 cadavers, the right VA was longer than the left and in 14 cadavers the left side was longer. Our results are smaller than the results presented in the study performed by Cacciola et al. Hong et al. found anatomical variations (fenestrated VA, anomalous origin of the PICA) of the V3 in 55 cases (5.4%) in CT angiography. In our study, we did not detect these types of abnormal courses of VA (12). The transverse process of the atlas is easily felt as the single bony prominence between the mastoid process and the angle of the jaw. Reports in the literature state that the transverse process of C1 is located approximately mm inferior and posteromedial to the mastoid tip similar to our results (2, 7). Turk Neurosurg,
8 The axis which has large spinous process plays a principal role in extending and stabilizing the head and neck. At C-2, there are five muscles: 1) the rectus capitis posterior major muscle; 2) the obliquus capitis inferior muscle; 3) the semispinalis cervicis muscle; 4) the multifidus muscle; and 5) the interspinalis muscle. Together, they act as a dynamic stabilizer for the cervical spine. Several authors have emphasized the importance of reattaching the removed muscles to the C-2 spinous process as a means of preventing postoperative cervical malalignment (13, 22). The C2 ganglion lies in the intervertebral space, which is bordered superiorly by the posterior arch of atlas, inferiorly by the lamina of axis, anteriorly by the lateral atlantoaxial joint and its fibrous capsule, and posteriorly by the anterior edge of the ligamentum flavum. The positions of the dorsal root ganglions, the shape and height of the C2 ganglion and its anatomic relations were described in previous studies (3, 18). However, they were not examined in fresh human cadavers previously. The exploration of the large C-2 ganglion provides a wide exposure of the region. Sectioning of the C-2 ganglion may result in anesthesia in the suboccipital region. Other authors studying this region also agree that sectioning of the C-2 ganglion does not result in any significant disability (10). The retraction of the ganglion for exposure of the region may be more dangerous to the spinal cord than its sectioning. Sectioning of the C2 nerve root does not result in any related symptoms (10, 24). During dissections and measurements, it was seen that the shape of the ganglions was not always the same. Although they differ individually, the same shaped ganglions were detected bilaterally in the same cadaver. Similar to our findings, Bilge concluded that the different shaped ganglions may be detected in the same cadaver in a study performed in human embalmed cadavers. In respect of its shapes, three types of ganglion (oval, spindle-like, and spherical) were defined as in the study performed by Bilge (3). The shapes of the ganglions were defined as in three types: 70% were oval, 20% were spindle-like, and 10% were spherical. In our study, 48.4% (31 of 64) of ganglions were spherical, 40.6% (26 of 64) of ganglions were oval, and 10.9% (7 of 64) of ganglions were spindle-like. Our observation showed that the ganglions having oval or spherical shapes could be dissected easily but retraction and dissection of the spindle-like shape having ganglions was difficult. In our study, observations confirmed that the C2 nerve root and ganglion exit from the cord and travel out of the foramen following an almost horizontal course. All C2 ganglia were confined within the C2 foramen between the posterior arch of atlas and the lamina of the axis (Figures 4, 6, 9). Our anatomical dissections showed that the venous plexus can cover the lateral mass and C2 nerve root and ganglion. Intraoperative bleeding from these veins can limit vision to the surgical field, leading to injury of the VA, dural tube and C-2 nerve. In our study, the localization of the ganglion was evaluated by using the lateral mass screwing point which is the midpoint of the inferior part of the lateral mass in both mediolateral and cranio-caudal directions. The localizations of the ganglia were described as on, over or below the point. The lateral mass screwing procedure commonly requires caudal retraction of the C2 dorsal root ganglion. Therefore, the localization of the ganglion is clinically important. The ganglion was found over the screw entry point in 45 of 64 ganglions (70.31%) and below the screw entry point in 19 of 64 ganglions (29.69%) (11 at the right and 8 at the left) (Figure 10). The ganglion was covering bilaterally the screw entry point in 19 cadavers, and it was located below the screw entry point bilaterally in 6 cadavers. Stabilization of the upper cervical spine may be required when treating traumatic instability, inflammatory arthropathy, degenerative disease, congenital malformation, and malignancy. Many techniques were developed by and several variations exist (4, 11, 19). Injury to the VA during placement of a posterior C-1 screw, especially when it occurs on the dominant side, may result in very serious complications. These types of injuries include the formation of an arteriovenous fistula, occlusion, dissection of the VA, and massive bleeding (26). The risk of injury to the VA during placement of screws for atlantoaxial fixation has been calculated to be 4.1% per patient or 2.2% per screw inserted (34). These are considered to be highly associated with screw malpositioning. The risk of neurologic deficit from VA injury was 0.2% per patient or 0.1% per screw, and the mortality rate was 0.1% (34). In C1 lateral mass screw placement, Goel et al. concluded that the preferred site of screw insertion is the center of the posterior surface of the lateral mass, just above the inferior articular facet of the atlas (10). Tan et al. described the screw fixation via posterior arch and lateral mass in atlas resembling pedicle screw fixation, so-called C1 pedicle screws. Screws inserted through the posterior arch of C1 into the lateral mass have a longer trajectory compared to lateral mass screws (32). Lee et al. concluded that the average minimal thickness of the posterior-lateral atlas was 3.95 mm. Overall, 85.2% of the 709 mature atlas specimens had a thickness greater than 3 mm, 654 (46.2%) greater than 4 mm, and 194 (13.7%) greater than 5 mm. They estimated that a minimum of 5 mm of bone thickness would be required to safely pass a 3.5-mm screw via the posterior lateral arch, without violating any of the cortical margins (16). Ebraheim et al. measured the thickness of the posterior arch at the thinnest part of groove as 4.1 ± 1.2 mm and Tan et al. measured this parameter as 4.58 ± 0.65 mm (8, 32). In our study, the thickness of C1 posterior arch was 3.73±0.75 mm at the right side and 3.75±0.77 mm at the left. This distance was measured below 3 mm in 5 cadavers (15.6%), between 3 and 4 mm in 15 cadavers (46.8%), between 4 and 5 mm in 8 cadavers (25%) and above 5 mm in 4 cadavers (12.5%). Seal et al. concluded that the average length of the C1 lateral mass was 16.82±1.00 mm, the average width was 16.06±0.91 mm, and the average height was 15.68±0.98 mm in a study performed in formalin-fixed specimens (27). In dry samples of atlas, Tan et al. found that the transverse diameter of lateral mass and the middle height of lateral mass were 17.52±2.97mm and ±1.18 mm (32). The distance of medial border of 8 Turk Neurosurg, 2016
9 lateral mass to the dura is clinically important. This measure was not mentioned before in a study in the literature. In our study, the mean value was 3.81±0.55 mm at the right side and 3.91±0.59 mm at the left. The anatomy of the osseous groove on the superior surface of posterior arch has been studied by various authors; however, the relation of the VA to the C1-C2 facet joint has not been addressed. This distance is important due to close proximity to the C1 lateral mass screw entry point. In our study, the mean distance was 11.04±1.84 mm at the right side and 11.35±1.87 mm at the left. In 18 cadavers, the left side was longer than the right and in 14 cadavers the right side was longer. In our opinion, the percutaneous ablation of the C2 ganglion in cervicogenic pain and occipital neuralgia may be useful. Therefore, the measurements related to distance of the C2 ganglion to the some landmarks given here are planned to be discussed in another study. In the posterior approach, detailed anatomical information related to important structures are essential to carry out the operation in more radical manner and in low risk. The current study revealed some surgical landmarks, measurements and, variations for the operations of posterior part of upper cervical spine. All studies in the literature performed about this subject were conducted upon formalin fixed cadavers or cervical spine that are processed with chemicals. Formalin-fixed techniques render the soft tissue structures, such as ligament, muscle and adipose tissue. Therefore, identification of the structures is more difficult. In contrast to other studies related to this subject, the current study was performed in fresh cadavers; therefore we believe that the data given here are more accurate and helpful for surgery. REFERENCES 1. An HS, Simpson JM: Spinal instrumentation of the cervical spine. In: An HS, Simpson JM (eds), Surgery of the Cervical Spine. London: Martin Dunitz, 1994: Avci E, Kocaogullar Y, Fossett D: Vertebral artery landmarks for the far-lateral transcondylar approach: An anatomic study. Turk Neurosurg 10: , Bilge O: An Anatomic and morphometric study of C2 nerve root ganglion and its corresponding foramen. Spine 29(5): , Brooks AL, Jenkins EB: Atlanto-axial arthrodesis by the wedge compression method. J Bone Joint Surg Am 60: , Cacciola F, Phalke U, Goel A: Vertebral artery in relationship to C1-C2 vertebrae: An anatomical study. Neurol India 52(2): , Cushing KE, Ramesh V, Gardner-Medwin D, Todd NV, Gholkar A, Baxter P, Griffiths PD: Tethering of the vertebral artery in the congenital arcuate foramen of the atlas vertebra: A possible cause of vertebral artery dissection in children. Developmental Medicine & Child Neurology 43: , Dowd GC, Zeiller S, Awasthi D: Far lateral transcondylar approach: Dimensional anatomy. Neurosurgery 45:95-99, Ebraheim NA, Rongming X, Muhammad A, Bruce H: The Quantitative anatomy of the vertebral artery groove of the atlas and its relation to the posterior atlantoaxial approach. Spine 23(3): , Gehweiler JA Jr, Daffner RH, Roberts L Jr: Malformations of the atlas vertebra simulating the Jefferson fracture. AJR Am J Roentgenol 140(6): , Goel A, Desai KI, Muzumdar DP: Atlantoaxial fixation using plate and screw method: A report of 160 treated patients. Neurosurgery 51: , Harms J, Mellcher RP: Posterior C1-2 fuson with polyaxial screw and rod fixation. Spine 26: , Hong JT, Lee SW, Son BC, Sung JH, Yang SH, Kim IS, Park CK: Analysis of anatomical variations of bone and vascular structures around the posterior atlantal arch using three dimensional computed tomography angiography. J Neurosurg Spine 8: , Iizuka H, Shimizu T, Tateno K, Toda N, Shimada H, Takagishi K: Extensor musculature of the cervical spine after laminoplasty: Morphologic evaluation by coronal view of the magnetic resonance image. Spine 26: , Köhler H, Zimmer F: Vertebral column. In: Schmidt and Schmidt (eds), Borderlands of normal and early pathological findings in skeletal radiography. New York: Thieme Medical Publishers, Lamberty B, Zivanovic S: The retroarticular vertebral artery ring of the atlas and its significance. Acta Anat (Basel) 85: , Lee MJ, Cassinelli E, Riew KD: The feasibility of inserting atlas lateral mass screws via the posterior arch. Spine 31(24): , Limousin CA: Foramen arcuale and syndrome of Barre-Lieou. Its surgical treatment. Int Orthop 4:19-23, Lu J, Ebraheim NA: Anatomic considerations of C2 nerve root ganglion. Spine 23(6): , Magerl F, Seeman PS: Stable posterior fusion of the atlas and axis by transarticular screw fixation. In: Kehr P, Weidner A, (eds), Cervical Spine. Berlin: Springer-Verlag, 1986: Mixter SJ, Osgood RB: Traumatic lesions of the atlas and axis. Ann Surg 51: , Naderi S, Cakmakcı H, Acar F, Arman C, Mertol T, Arda MN: Anatomical and computed tomographic analysis of C1 vertebra. Clin Neurol Neurosurg 105: , Nolan JP Jr, Sherk HH: Biomechanical evaluation of the extensor musculature of the cervical spine. Spine 13:9-11, Paraskevas G, Papaziogas B, Tsonidis C, Kapetanos G: Gross morphology of the bridges over the vertebral artery groove on the atlas. Surg Radiol Anat 27: , Payer M, Luzi M, Tessitore E: Posterior atlanto-axial fixation with polyaxial C1 lateral mass screws and C2 pars screws. Acta Neurochir 151: , 2009 Turk Neurosurg,
10 25. Radojevic S, Negovanovic B: La gouttiere et les anneaux osseux de l artere vertebrale de l atlas. Acta Anat (Basel) 55: , Rocha R, Safavi-Abbasi S, Reis C, Theodore N, Bambakidis N, De oliveira E, Sonntag VK, Crawford NR: Working area, safety zones, and angles of approach for posterior C-1 lateral mass screw placement: A quantitative anatomical and morphometric evaluation. J Neurosurg Spine 6: , Seal C, Zarro C, Gelb D,Ludwig S: C1 lateral mass anatomy proper placement of lateral mass screws. J Spinal Disord Tech 22: , Senoglu M, Safavi-Abbasi S, Theodore N, Bambakidis NC, Crawford NR, Sonntag VKH: The frequency and clinical significance of congenital defects of the posterior and anterior arch of the atlas. J Neurosurg Spine 7: , Sonntag VKH: Lateral mass screw fixation of the atlas: Importance of anatomy of C1 for lateral mass screw placement. World Neurosurg 74: , Stauffer ES: Posterior atlanto-axial arthrodesis: The Gallie and Brooks techniques and their modifications. Techniques in Orthopaedics 9:43-48, Taitz C, Nathan H: Some observations on the posterior and lateral bridge of the atlas. Acta Anat (Basel) 127: , Tan M, Wang H, Wang Y, Zhang G, Yi P, Li Z, Wei H, Yang F: Morphometric evaluation of screw fixation in atlas via posterior arch and lateral mass. Spine 28(9): , Tubbs RS, Johnson P, Shoja MM, Loukas M, Oakes WJ: Foramen arcuale: Anatomical study and review of the literature. J Neurosurg Spine 6:31-34, Wright NM, Lauryssen C: Vertebral artery injury in C1 2 transarticular screw fixation: Results of a survey of the AANS/ CNS section on disorders of the spine and peripheral nerves. J Neurosurg 88: , Turk Neurosurg, 2016
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Radiological Analysis of Ponticulus Posticus in Koreans
 Yonsei Med J 50(1):45-49, 2009 DOI 10.3349/ymj.2009.50.1.45 Radiological Analysis of Ponticulus Posticus in Koreans Department of Neurosurgery, Ewha Womans University School of Medicine, Seoul, Korea.
Yonsei Med J 50(1):45-49, 2009 DOI 10.3349/ymj.2009.50.1.45 Radiological Analysis of Ponticulus Posticus in Koreans Department of Neurosurgery, Ewha Womans University School of Medicine, Seoul, Korea.
Anatomy and Physiology II. Spine
 Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Anatomy and Physiology II Spine Bones and Other Structures Vertibrae Contains Cervical, Thoracic, Lumbar, Sacral and Coccygeal regions We use Capital letters to refer to these (C, T, L, S, and Co) and
Craniovertebral Junction Embryology and Anatomy. Presented by: Amandeep Moderators: S.S.Kale G.D.Satyarthi. CVJ-Embryology & Anatomy
 Craniovertebral Junction Embryology and Anatomy Presented by: Amandeep Moderators: S.S.Kale G.D.Satyarthi CVJ-Embryology & Anatomy CVJ-Embryology SOMITE-The building block of vertebrae, skeletal muscle
Craniovertebral Junction Embryology and Anatomy Presented by: Amandeep Moderators: S.S.Kale G.D.Satyarthi CVJ-Embryology & Anatomy CVJ-Embryology SOMITE-The building block of vertebrae, skeletal muscle
The Back OUTLINE. Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region
 The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
The Back OUTLINE Vertebral Column (review) Craniovertebral Joints Dorsal Scapular Region(review) Muscles of the Back Suboccipital Region Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com
Morphometric Anatomy of the Atlas and Axis Vertebrae
 Original Article Morphometric Anatomy of the Atlas and Axis Vertebrae Gökflin fiengül Hakan Hadi KADIO LU ABSTRACT OBJECTIVE: In this study, forty dried specimens of atlas and axis vertebrae were examined
Original Article Morphometric Anatomy of the Atlas and Axis Vertebrae Gökflin fiengül Hakan Hadi KADIO LU ABSTRACT OBJECTIVE: In this study, forty dried specimens of atlas and axis vertebrae were examined
Pichayen Duangthongpon MD*, Chaiwit Thanapaisal MD*, Amnat Kitkhuandee MD*, Kowit Chaiciwamongkol MD**, Vilaiwan Morthong MD**
 The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
The Relationships between Asterion, the Transverse-Sigmoid Junction, the Superior Nuchal Line and the Transverse Sinus in Thai Cadavers: Surgical Relevance Pichayen Duangthongpon MD*, Chaiwit Thanapaisal
_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]
![_CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come] _CH01redo.qxd 9/24/07 3:07 PM Page 1. [Half-Title to come]](/thumbs/81/84146690.jpg) 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 1 [Half-Title to come] 10752-01_CH01redo.qxd 9/24/07 3:07 PM Page 2 THE BACK Lippincott Williams & Wilkins atlas of ANATOMY CHAPTER 1 Plate 1-01 Palpable Structures
Cervical Spine Anatomy and Biomechanics. Typical Cervical Vertebra C3 6. Typical Cervical Vertebra Anterior 10/5/2017
 Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Cervical Spine Anatomy and Biomechanics Typical Cervical Vertebra C3 6 Small, relatively broad body Bifid SpinousProcess Long and narrow laminae Spinal Canal: large, triangular; remarkably consistent dimensions
Inferior view of the skull showing foramina (Atlas of Human Anatomy, 5th edition, Plate 12)
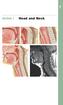 Section 1 Head and Neck Skull, Basal View Incisive foramen Choanae Foramen ovale Foramen lacerum Foramen spinosum Carotid canal Jugular fossa Mastoid process Inferior view of the skull showing foramina
Section 1 Head and Neck Skull, Basal View Incisive foramen Choanae Foramen ovale Foramen lacerum Foramen spinosum Carotid canal Jugular fossa Mastoid process Inferior view of the skull showing foramina
Ligaments of the vertebral column:
 In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
In the last lecture we started talking about the joints in the vertebral column, and we said that there are two types of joints between adjacent vertebrae: 1. Between the bodies of the vertebrae; which
The sacrum is a complex anatomical structure.
 A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
A Review Paper Rongming Xu, MD, Nabil A. Ebraheim, MD, and Nicholas K. Gove, MD Abstract Treatment in spinal disorders, sacroiliac joint disruption, and sacral fractures may involve instrumentation of
Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach
 J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
J Neurosurg 87:555 585, 1997 Microsurgical anatomy of the transcondylar, supracondylar, and paracondylar extensions of the far-lateral approach HUNG T. WEN, M.D., ALBERT L. RHOTON, JR., M.D., TOSHIRO KATSUTA,
Morphometric study of the Axis vertebra
 ORIGINAL ARTICLE Eur J Anat, 16 (2): 98-103 (2012) Morphometric study of the Axis vertebra Shilpa Gosavi 1, Vatsala Swamy 2 1- Dept. of Anatomy, Padmashree Dr.Vitthalrao Vikhe Patil Foundation s Medical
ORIGINAL ARTICLE Eur J Anat, 16 (2): 98-103 (2012) Morphometric study of the Axis vertebra Shilpa Gosavi 1, Vatsala Swamy 2 1- Dept. of Anatomy, Padmashree Dr.Vitthalrao Vikhe Patil Foundation s Medical
The Anatomy of the Atlantoaxial Complex
 The Anatomy of the Atlantoaxial Complex T. GLENN PAIT, M.D., KENAN 1. ARNAUTOVIC, M.D., and LUIS A.B. BORBA, M.D. Operating on the atlantoaxial complex has always posed a challenge to the surgeon because
The Anatomy of the Atlantoaxial Complex T. GLENN PAIT, M.D., KENAN 1. ARNAUTOVIC, M.D., and LUIS A.B. BORBA, M.D. Operating on the atlantoaxial complex has always posed a challenge to the surgeon because
Thoracic Cooled-RF Training Presentation
 Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
Thoracic Cooled-RF Training Presentation Patient Selection Anatomy Overview Neuroanatomy Lesion targets Technique Diagnostic Block Cooled-RF Precautions Summary Appendix AGENDA Patient Selection Thoracic
2. The vertebral arch is composed of pedicles (projecting from the body) and laminae (uniting arch posteriorly).
 VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
VERTEBRAL COLUMN 2018zillmusom I. VERTEBRAL COLUMN - functions to support weight of body and protect spinal cord while permitting movements of trunk and providing for muscle attachments. A. Typical vertebra
Thoracic and Lumbar Spine Anatomy.
 Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
Thoracic and Lumbar Spine Anatomy www.fisiokinesiterapia.biz Thoracic Vertebrae Bodies Pedicles Laminae Spinous Processes Transverse Processes Inferior & Superior Facets Distinguishing Feature Costal Fovea
Vertebral Artery Anomalies at the Craniovertebral Junction: A Case Report and Review of the Literature
 Case Report 121 Vertebral Artery Anomalies at the Craniovertebral Junction: A Case Report and Review of the Literature Amir M. Abtahi 1 Darrel S. Brodke 1 Brandon D. Lawrence 1 1 Department of Orthopaedics,
Case Report 121 Vertebral Artery Anomalies at the Craniovertebral Junction: A Case Report and Review of the Literature Amir M. Abtahi 1 Darrel S. Brodke 1 Brandon D. Lawrence 1 1 Department of Orthopaedics,
Table of contents. Introduction. Features and Benefits 2. AO Principles 4. Indications and Contraindiactions 5. Implants 6. Productinformation
 Technique Guide CerviFix. Modular tension band system for posterior fixation of the occipito - cervical spine, upper and lower cervical spine, and upper thoracic spine. Table of contents Introduction
Technique Guide CerviFix. Modular tension band system for posterior fixation of the occipito - cervical spine, upper and lower cervical spine, and upper thoracic spine. Table of contents Introduction
You have 24 vertebrae in your spinal column. Two are special enough to be individually named.
 You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
You have 24 vertebrae in your spinal column. Two are special enough to be individually named. Your atlas (C01) and axis (C02) are very important vertebrae. Without them, head and neck movement would be
A morphometric study of the Pedicles of dry human typical lumbar vertebrae
 Original article: A morphometric of the Pedicles of dry human typical lumbar vertebrae Dhaval K. Patil 1 *, Pritha S. Bhuiyan 2 1Resident, Department of Anatomy, Seth G S Medical College, Parel, Mumbai-400012,
Original article: A morphometric of the Pedicles of dry human typical lumbar vertebrae Dhaval K. Patil 1 *, Pritha S. Bhuiyan 2 1Resident, Department of Anatomy, Seth G S Medical College, Parel, Mumbai-400012,
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Cervical Cooled RF Training Presentation
 Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
Cervical Cooled RF Training Presentation Agenda Patient Selection Considerations Diagnostic Block General Considerations COOLIEF* Cooled RF Technique Posterior Lateral Precautions Summary Appendix 2 Disclaimer
The indications of upper cervical fusion include. Posterior fixation and fusion with atlas pedicle screw system for upper cervical diseases
 Chinese Journal of Traumatology 2008; 11(6):323-328.. Original articles Posterior fixation and fusion with atlas pedicle screw system for upper cervical diseases LI Lei *, ZHOU Feng-hua, WANG Huan, and
Chinese Journal of Traumatology 2008; 11(6):323-328.. Original articles Posterior fixation and fusion with atlas pedicle screw system for upper cervical diseases LI Lei *, ZHOU Feng-hua, WANG Huan, and
1 Normal Anatomy and Variants
 1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
1 Normal Anatomy and Variants 1.1 Normal Anatomy MR Technique. e standard MR protocol for a routine evaluation of the spine always comprises imaging in sagittal and axial planes, while coronal images are
THE THORACIC WALL. Boundaries Posteriorly by the thoracic part of the vertebral column. Anteriorly by the sternum and costal cartilages
 THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces Superiorly by the suprapleural
Copyright 2010 Pearson Education, Inc.
 E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
E. VERTEBRAL COLUMN 1. The vertebral column extends from the skull to the pelvis and forms the vertical axis of the skeleton. 2. The vertebral column is composed of vertebrae that are separated by intervertebral
Anatomy and Physiology II. Review Spine and Neck
 Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer
 Review article The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer 1Dr. Jaspreet Singh Badwal, 2 Dr. Upkardeep Singh, 3 Dr. Neha Bharti, 4 Dr.Shivani Garg, 5 Dr.Simarpreet Singh
Review article The Far Lateral Approach to Skull Base: in the Context of Head and Neck Cancer 1Dr. Jaspreet Singh Badwal, 2 Dr. Upkardeep Singh, 3 Dr. Neha Bharti, 4 Dr.Shivani Garg, 5 Dr.Simarpreet Singh
Posterior surgical procedures are those procedures
 9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
9 Cervical Posterior surgical procedures are those procedures that have been in use for a long time with established efficacy in the treatment of radiculopathy and myelopathy caused by pathologies including
Technique Guide. ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Technique Guide ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Table of Contents Introduction Overview 2 AO ASIF Principles 4 Indications and Contraindications 5 Product Information
Structure and Function of the Vertebral Column
 Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms.
 RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
RHEUMATOID SPINE Involvement of the spine is common in rheumatoid. Incidence been reported to be 85% radiologically but only 30% have neurological signs and symptoms. When neurology is present it may manifest
Occipital-Cervical-Thoracic Fixation Techniques
 Occipital-Cervical-Thoracic Fixation Techniques Neill M. Wright, M.D. Herbert Lourie Professor of Neurological Surgery Professor of Orthopaedic Surgery Washington University School of Medicine Disclosures
Occipital-Cervical-Thoracic Fixation Techniques Neill M. Wright, M.D. Herbert Lourie Professor of Neurological Surgery Professor of Orthopaedic Surgery Washington University School of Medicine Disclosures
The Back. Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa
 The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D.
 Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
Imaging of Cervical Spine Trauma Tudor H Hughes, M.D. General Considerations Most spinal fractures are due to a single episode of major trauma. Fatigue fractures of the spine are unusual except in the
The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine
 J Neurosurg (Spine 2) 98:188 194, 2003 The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine MASATOU KAWASHIMA, M.D., NECMETTIN TANRIOVER,
J Neurosurg (Spine 2) 98:188 194, 2003 The transverse process, intertransverse space, and vertebral artery in anterior approaches to the lower cervical spine MASATOU KAWASHIMA, M.D., NECMETTIN TANRIOVER,
CERVIFIX Modular tension band system for posterior fixation of the occipito cervical spine, upper and lower cervical spine, and upper thoracic spine
 CERVIFIX Modular tension band system for posterior fixation of the occipito cervical spine, upper and lower cervical spine, and upper thoracic spine PRODUCT OBSOLETED 30th June 2017 DSEM/SPN/1215/0387(1)
CERVIFIX Modular tension band system for posterior fixation of the occipito cervical spine, upper and lower cervical spine, and upper thoracic spine PRODUCT OBSOLETED 30th June 2017 DSEM/SPN/1215/0387(1)
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of th
 Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
Any of the vertebra in the cervical (neck) region of the spinal column. The cervical vertebra are the smallest vertebra in the spine, reflective of the fact that they support the least load. In humans,
Co-Innervation of Triceps Brachii Muscle with Variant Branch of Ulnar Nerve
 DOI: 10.5137/1019-5149.JTN.22126-17.2 Received: 23.11.2017 / Accepted: 07.02.2018 Published Online: 26.02.2018 Turk Neurosurg, 2018 Original Investigation Co-Innervation of Triceps Brachii Muscle with
DOI: 10.5137/1019-5149.JTN.22126-17.2 Received: 23.11.2017 / Accepted: 07.02.2018 Published Online: 26.02.2018 Turk Neurosurg, 2018 Original Investigation Co-Innervation of Triceps Brachii Muscle with
Module: #15 Lumbar Spine Fusion. Author(s): Jenni Buckley, PhD. Date Created: March 27 th, Last Updated:
 Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Module: #15 Lumbar Spine Fusion Author(s): Jenni Buckley, PhD Date Created: March 27 th, 2011 Last Updated: Summary: Students will perform a single level lumbar spine fusion to treat lumbar spinal stenosis.
Muscles of the Upper Limb that are dissected in the Back Region Muscle Origin Insertion Action Innervation Artery Notes
 Muscles of Upper Limb that are dissected in Back Region Muscle Origin Insertion Action Innervation Artery Notes floor of thoraco thoraco inserting spines from intertubercular arm nerve (C7,8) a. tendon
Muscles of Upper Limb that are dissected in Back Region Muscle Origin Insertion Action Innervation Artery Notes floor of thoraco thoraco inserting spines from intertubercular arm nerve (C7,8) a. tendon
Incidence of Ponticles in Human Atlas Vertebrae - A Study from South Gujarat Population
 Original Research Incidence of Ponticles in Human Atlas Vertebrae - A Study from South Gujarat Population Nitixa P. Patel 1,*, Deepa S.Gupta 2, Nisha D. Parmar 3 1 3 rd Year Resident, 2 Professor & Head,
Original Research Incidence of Ponticles in Human Atlas Vertebrae - A Study from South Gujarat Population Nitixa P. Patel 1,*, Deepa S.Gupta 2, Nisha D. Parmar 3 1 3 rd Year Resident, 2 Professor & Head,
VERTEBRAL COLUMN ANATOMY IN CNS COURSE
 VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
VERTEBRAL COLUMN ANATOMY IN CNS COURSE Vertebral body Sections of the spine Atlas (C1) Axis (C2) What type of joint is formed between atlas and axis? Pivot joint What name is given to a fracture of both
International J. of Healthcare & Biomedical Research, Volume: 1, Issue: 4, July 2013, Pages
 Original article: Morphometry of first pedicle of sacrum and its clinical relevance Sinha Manisha B, Rathore Mrithunjay, Trivedi Soumitra, Siddiqui A U Department of Anatomy, All India Institute of Medical
Original article: Morphometry of first pedicle of sacrum and its clinical relevance Sinha Manisha B, Rathore Mrithunjay, Trivedi Soumitra, Siddiqui A U Department of Anatomy, All India Institute of Medical
human anatomy 2015 lecture four Dr meethak ali ahmed neurosurgeon
 The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
The Vertebral Column the vertebral columnis central pillar of the body.it serve to protect the spinal cord and support the weight of the head trunk, which it transmits to the hip bones & the lower limbs.
An anatomic consideration of C2 vertebrae artery groove variation for individual screw implantation in axis
 Eur Spine J (2013) 22:1547 1552 DOI 10.1007/s00586-013-2779-4 ORIGINAL ARTICLE An anatomic consideration of C2 vertebrae artery groove variation for individual screw implantation in axis Janhua Wang Hong
Eur Spine J (2013) 22:1547 1552 DOI 10.1007/s00586-013-2779-4 ORIGINAL ARTICLE An anatomic consideration of C2 vertebrae artery groove variation for individual screw implantation in axis Janhua Wang Hong
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty.
 ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
ARCH Laminoplasty System. Dedicated System for Open-door Laminoplasty. Surgical Technique This publication is not intended for distribution in the USA. Instruments and implants approved by the AO Foundation.
Main Menu. Trunk and Spinal Column click here. The Power is in Your Hands
 1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
VERTEBRAL COLUMN VERTEBRAL COLUMN
 VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
VERTEBRAL COLUMN FUNCTIONS: 1) Support weight - transmits weight to pelvis and lower limbs 2) Houses and protects spinal cord - spinal nerves leave cord between vertebrae 3) Permits movements - *clinical
Axial Skeleton: Vertebrae and Thorax
 Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
Axial Skeleton: Vertebrae and Thorax Function of the vertebral column (spine or backbone): 1) 2) 3) Composition of Vertebral column The vertebral column is formed by 33 individual vertebrae (some of which
1TRUNK: BODY WALL AND SPINE
 TRUNK: BODY WALL AND SPINE SURFACE ANATOMY SKELETON JOINTS & LIGAMENTS MUSCLES VASCULATURE NERVES SPINAL CORD & VERTEBRAL CANAL ANTERIOR BODY WALL & MAMMARY GLAND LATERAL BODY WALL INGUINAL REGION SUPERFICIAL
TRUNK: BODY WALL AND SPINE SURFACE ANATOMY SKELETON JOINTS & LIGAMENTS MUSCLES VASCULATURE NERVES SPINAL CORD & VERTEBRAL CANAL ANTERIOR BODY WALL & MAMMARY GLAND LATERAL BODY WALL INGUINAL REGION SUPERFICIAL
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5. September 30, 2011
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 September 30, 2011 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) EXAM NUMBER A. Suprascapular nerve B. Axillary nerve
THE VERTEBRAL COLUMN. Average adult length: In male: about 70 cms. In female: about 65 cms.
 THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
THE VERTEBRAL COLUMN Average adult length: In male: about 70 cms. In female: about 65 cms. 1 Vertebral Column (Regions and Curvatures) Curvatures of the vertebral column: A. Primary curvature: C-shaped;
Posterior cervical fusion has gained wide acceptance. A comparison of open versus percutaneous cervical transfacet fixation
 laboratory investigation J Neurosurg Spine 25:43 435, 216 A comparison of open versus percutaneous cervical transfacet fixation Adeel Husain, MD, 1 Yusuf T. Akpolat, MD, 1 Daniel K. Palmer, BS, 2 David
laboratory investigation J Neurosurg Spine 25:43 435, 216 A comparison of open versus percutaneous cervical transfacet fixation Adeel Husain, MD, 1 Yusuf T. Akpolat, MD, 1 Daniel K. Palmer, BS, 2 David
Morphometric Characteristics of C1-C2 Vertebrae to Perform Anterior Transarticular Crossing Screw Fixation
 DOI: 10.5137/1019-5149.JTN.18971-16.1 Received: 01.09.2016 / Accepted: 21.11.2016 Published Online: 12.12.2016 Original Investigation Morphometric Characteristics of C1-C2 Vertebrae to Perform Anterior
DOI: 10.5137/1019-5149.JTN.18971-16.1 Received: 01.09.2016 / Accepted: 21.11.2016 Published Online: 12.12.2016 Original Investigation Morphometric Characteristics of C1-C2 Vertebrae to Perform Anterior
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D.
 Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
8/4/2012. Causes and Cures. Nucleus pulposus. Annulus fibrosis. Vertebral end plate % water. Deforms under pressure
 Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
Causes and Cures Intervertebral discs Facet (zygopophyseal) joints Inter body joints Spinal nerve roots Nerve compression Pathological conditions Video Causes of back pain Nucleus pulposus Annulus fibrosis
The Thoracic wall including the diaphragm. Prof Oluwadiya KS
 The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The Thoracic wall including the diaphragm Prof Oluwadiya KS www.oluwadiya.com Components of the thoracic wall Skin Superficial fascia Chest wall muscles (see upper limb slides) Skeletal framework Intercostal
The craniocervical junction
 Anver Jameel, MD The craniocervical junction A biomechanical and anatomical unit that extends from the skull base to C2 Includes the clivus, foramen magnum and contiguous occipital bone, the occipital
Anver Jameel, MD The craniocervical junction A biomechanical and anatomical unit that extends from the skull base to C2 Includes the clivus, foramen magnum and contiguous occipital bone, the occipital
Anatomy of the Thorax
 Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
Anatomy of the Thorax A) THE THORACIC WALL Boundaries Posteriorly by the thoracic part of the vertebral column Anteriorly by the sternum and costal cartilages Laterally by the ribs and intercostal spaces
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of direct C1 lateral mass screw procedure for cervical spine stabilisation Introduction
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedures overview of direct C1 lateral mass screw procedure for cervical spine stabilisation Introduction
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Technique Guide. C1/C2 Access System. Percutaneous transarticular screw fixation.
 Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
Technique Guide C1/C2 Access System. Percutaneous transarticular screw fixation. C1/C2 Access System Table of Contents General introduction 2 Indications/Contraindications 2 Image intensifier-assisted
Lauren M. Burke, Warren D. Yu, Anthony Ho, Timothy Wagner, Joseph R. O Brien. Department of Orthopaedic Surgery George Washington University
 Lauren M. Burke, Warren D. Yu, Anthony Ho, Timothy Wagner, Joseph R. O Brien Department of Orthopaedic Surgery George Washington University O Brien: Consultant for Globus, Relivant, Stryker. Royalties:
Lauren M. Burke, Warren D. Yu, Anthony Ho, Timothy Wagner, Joseph R. O Brien Department of Orthopaedic Surgery George Washington University O Brien: Consultant for Globus, Relivant, Stryker. Royalties:
Gross Morphology of Spinal Cord
 Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Gross Morphology of Spinal Cord Lecture Objectives Describe the gross anatomical features of the spinal cord. Describe the level of the different spinal segments compared to the level of their respective
Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach
 Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach Joseph Naiem.S Aziz 1 and Ahmed Khaled Al-Hrabi2 1 Deparment of Anatomy, Faculty
Morphological study of the foramen magnum and occipital condyle and its surgical implications in transcondylar approach Joseph Naiem.S Aziz 1 and Ahmed Khaled Al-Hrabi2 1 Deparment of Anatomy, Faculty
Dorsal Cervical Surgeries and Techniques
 Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
Dorsal Cervical Approaches Dorsal Cervical Surgeries and Techniques Gregory R. Trost, MD Professor and Vice Chair of Neurological Surgery University of Wisconsin-Madison Advantages Straightforward Easily
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW
 INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
INDEPENDENT LEARNING: DISC HERNIATION IN THE NATIONAL FOOTBALL LEAGUE: ANATOMICAL FACTORS TO CONSIDER IN REVIEW CDC REPORT - CAUSES OF DISABILITY, 2005 REVIEW QUESTIONS ABOUT DISC HERNIATION IN THE NATIONAL
Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives
 1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
Bony framework of the vertebral column Structure of the vertebral column
 5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
5.1: Vertebral column & back. Overview. Bones o vertebral column. o typical vertebra. o vertebral canal. o spinal nerves. Joints o Intervertebral disc. o Zygapophyseal (facet) joint. Muscles o 2 compartments:
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
2 Back and Spinal Cord
 2 Back and Spinal Cord Cards 2-1 to 2-24 Bones and Joints 2-1 Vertebral Column 2-2 Cervical Vertebrae 2-3 Thoracic Vertebrae 2-4 Lumbar Vertebra 2-5 Lumbar Vertebrae 2-6 Vertebral Ligaments: Lumbar Region
2 Back and Spinal Cord Cards 2-1 to 2-24 Bones and Joints 2-1 Vertebral Column 2-2 Cervical Vertebrae 2-3 Thoracic Vertebrae 2-4 Lumbar Vertebra 2-5 Lumbar Vertebrae 2-6 Vertebral Ligaments: Lumbar Region
It consist of two components: the outer, laminar fibrous container (or annulus), and the inner, semifluid mass (the nucleus pulposus).
 Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Lumbar Spine The lumbar vertebrae are the last five vertebrae of the vertebral column. They are particularly large and heavy when compared with the vertebrae of the cervical or thoracicc spine. Their bodies
Transitioning to the Suboccipital Triangle. Suboccipital Triangle
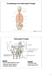 Transitioning to the Suboccipital Triangle Syllabus p. 14-15 Suboccipital Triangle Borders -Rectus capitis posterior major -Obliquus capitis superior -Obliquus capitis inferior Contents -Vertebral artery
Transitioning to the Suboccipital Triangle Syllabus p. 14-15 Suboccipital Triangle Borders -Rectus capitis posterior major -Obliquus capitis superior -Obliquus capitis inferior Contents -Vertebral artery
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 5 October 6, 2006 PART l. Answer in the space provided. (8 pts) 1. Identify the structures. (2 pts) B C A. _pisiform B. _ulnar artery A C. _flexor carpi
T.L.I.F. Surgical Technique. Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System.
 Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Surgical Technique T.L.I.F. Transforaminal Lumbar Interbody Fusion Featuring the T.L.I.F. SG Instruments, VG2 PLIF Allograft, and the MONARCH Spine System. CONSULTING SURGEON Todd Albert, M.D. Rothman
Why does sideflexion increase ipsilateral vertebral artery occlusion with contralateral atlanto-axial rotation? Thomas Langer
 Why does sideflexion increase ipsilateral vertebral artery occlusion with contralateral atlanto-axial rotation? Thomas Langer 1 Introduction When the head and neck are placed in the premanipulative position
Why does sideflexion increase ipsilateral vertebral artery occlusion with contralateral atlanto-axial rotation? Thomas Langer 1 Introduction When the head and neck are placed in the premanipulative position
Anatomy of the Nervous System. Brain Components
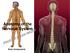 Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Anatomy of the Nervous System Brain Components NERVOUS SYSTEM INTRODUCTION Is the master system of human body, controlling the functions of rest of the body systems Nervous System CLASSIFICATION A. Anatomical
Copyright 2010 Pearson Education, Inc. Copyright 2010 Pearson Education, Inc. Figure Sectioned spinous process. Interspinous.
 PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 7 The Skeleton: Part B Vertebral Column Transmits weight of trunk to lower limbs Surrounds and protects spinal cord
PowerPoint Lecture Slides prepared by Janice Meeking, Mount Royal College C H A P T E R 7 The Skeleton: Part B Vertebral Column Transmits weight of trunk to lower limbs Surrounds and protects spinal cord
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography
 THIEME GLOBAL SPINE JOURNAL Original Article 383 Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography Moon Soo Park 1 Seong-Hwan Moon 2 Tae-Hwan Kim 1 Jae Keun
THIEME GLOBAL SPINE JOURNAL Original Article 383 Surgical Anatomy of the Uncinate Process and Transverse Foramen Determined by Computed Tomography Moon Soo Park 1 Seong-Hwan Moon 2 Tae-Hwan Kim 1 Jae Keun
Common fracture & dislocation of the cervical spine. Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University
 Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Common fracture & dislocation of the cervical spine Theerachai Apivatthakakul Department of Orthopaedic Chiangmai University Objective Anatomy Mechanism and type of injury PE.and radiographic evaluation
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Human Anatomy. Spinal Cord and Spinal Nerves
 Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
Human Anatomy Spinal Cord and Spinal Nerves 1 The Spinal Cord Link between the brain and the body. Exhibits some functional independence from the brain. The spinal cord and spinal nerves serve two functions:
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Chapter 7 Part B The Skeleton
 Chapter 7 Part B The Skeleton 7.2 The Vertebral Column General Characteristics Extends from skull to pelvis Also called spine or spinal column Functions to transmit weight of trunk to lower limbs, surround
Chapter 7 Part B The Skeleton 7.2 The Vertebral Column General Characteristics Extends from skull to pelvis Also called spine or spinal column Functions to transmit weight of trunk to lower limbs, surround
Posterior Cervical Arthrodesis by Lateral Mass Screws Fixation A Long term Follow-up Study
 Original Article Posterior Cervical Arthrodesis by Lateral Mass Screws Fixation A Long term Follow-up Study Bhaskar G 1, Sharath Kumar Maila 2, Lakshman Rao A 3, Mastan Reddy A 4 1 Professor I/C 2, 3 Assistant
Original Article Posterior Cervical Arthrodesis by Lateral Mass Screws Fixation A Long term Follow-up Study Bhaskar G 1, Sharath Kumar Maila 2, Lakshman Rao A 3, Mastan Reddy A 4 1 Professor I/C 2, 3 Assistant
Gross Anatomy Faculty: Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Melissa McGinn. Welcome to Gross and Developmental Anatomy
 Welcome to Gross and Developmental Anatomy M1 Anatomy Gross Anatomy Faculty: Dr. Richard Krieg Dr. Milton Sholley Dr. David Simpson 1 2 Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Steve Gudas Dr.
Welcome to Gross and Developmental Anatomy M1 Anatomy Gross Anatomy Faculty: Dr. Richard Krieg Dr. Milton Sholley Dr. David Simpson 1 2 Gross Anatomy Faculty: Gross Anatomy Faculty: Dr. Steve Gudas Dr.
ARCH Laminoplasty System
 Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Dedicated System for Open-door Laminoplasty ARCH Laminoplasty System Surgical Technique Image intensifier control This description alone does not provide sufficient background for direct use of DePuy Synthes
Unilateral extended suboccipital approach for a C1 dumbbell schwanoma
 38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
38 Gorgan et al Unilateral extended suboccipital approach for a C1 dumbbell schwanoma Unilateral extended suboccipital approach for a C1 dumbbell schwanoma R.M. Gorgan, Angela Neacşu, A. Giovani Clinical
Instrumentation and fixation of the C2 spinal segment. Evaluation of C2 pedicle screw placement via the freehand technique by neurosurgical trainees
 CLINICAL ARTICLE J Neurosurg Spine 29:235 240, 2018 Evaluation of C2 pedicle screw placement via the freehand technique by neurosurgical trainees Martin H. Pham, MD, Joshua Bakhsheshian, MD, Patrick C.
CLINICAL ARTICLE J Neurosurg Spine 29:235 240, 2018 Evaluation of C2 pedicle screw placement via the freehand technique by neurosurgical trainees Martin H. Pham, MD, Joshua Bakhsheshian, MD, Patrick C.
Demonstrate the bony features of Cl and C2 vertebrae evident on this Xray
 SUBJECT: ANATOMY 7 September 2007 am. TOPIC: X-ray: Lateral C spine NUMBER: JL Demonstrate the bony features of Cl and C2 vertebrae evident on this Xray 1 Odontoid peg (dens) 2 Bodies of Cl andc2 3 anterior
SUBJECT: ANATOMY 7 September 2007 am. TOPIC: X-ray: Lateral C spine NUMBER: JL Demonstrate the bony features of Cl and C2 vertebrae evident on this Xray 1 Odontoid peg (dens) 2 Bodies of Cl andc2 3 anterior
Vertebral Column. Backbone consists of 26 vertebrae. Five vertebral regions. Cervical
 Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
Vertebral Column Backbone consists of 26 vertebrae. Five vertebral regions Cervical vertebrae (7) in the neck. Thoracic vertebrae (12) in the thorax. Lumbar vertebrae (5) in the lower back. Sacrum (5,
AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM
 AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM APPENDICULAR SKELETON BONES OF THE FREE APPENDAGES & THEIR POINTS OF ATTACHMENTS
AXIAL SKELETON FORM THE VERTICAL AXIS OF THE BODY CONSISTS OF 80 BONES INCLUDES BONES OF HEAD, VERTEBRAL COLUMN, RIBS,STERNUM APPENDICULAR SKELETON BONES OF THE FREE APPENDAGES & THEIR POINTS OF ATTACHMENTS
Surgical management of combined fracture of atlas associated with fracture of axis vertebrae (CAAF): Case Series
 Romanian Neurosurgery (2015) XXIX 3: 335-341 335 Surgical management of combined fracture of atlas associated with fracture of axis vertebrae (CAAF): Case Series Guru Dutta Satyarthee, Gaurang Vaghani,
Romanian Neurosurgery (2015) XXIX 3: 335-341 335 Surgical management of combined fracture of atlas associated with fracture of axis vertebrae (CAAF): Case Series Guru Dutta Satyarthee, Gaurang Vaghani,
