2018 RN.ORG, S.A., RN.ORG, LLC
|
|
|
- Alexandrina Farmer
- 5 years ago
- Views:
Transcription
1 Abdominal Trauma Reviewed October, 2018, Expires October, 2020 Provider Information and Specifics available on our Website Unauthorized Distribution Prohibited 2018 RN.ORG, S.A., RN.ORG, LLC By Wanda Lockwood, RN, BA, MA Purpose The purpose of this course is to outline the different types of abdominal injuries that may result from blunt or penetrating trauma, including diagnosis, symptoms, associated injuries, and treatment approaches. Goals Upon completion of this course, the healthcare provider should be able to: Describe 3 types of blunt injuries. Discuss penetrating injuries. Explain the 3 sections of the abdominal cavity and the organs in each. Discuss primary and secondary surveys. Describe physical signs of bleeding, including Cullen s sign and Grey Turner s sign. Describe the 4 classes of hemorrhagic shock. Explain the APVU and AMPLE methods of neurological assessment. Describe key information needed during history for motor vehicle accidents and penetrating trauma. Explain FAST and DPL. Discuss hepatic trauma, including grading. Discuss splenic trauma, including grading. Discuss gastric trauma, including grading. Discuss intestinal trauma, including at least 6 signs of peritonitis. Discuss pancreatic trauma, including grading. Discuss bladder trauma and at least 4 indications of bladder rupture. Describe the difference between intraperitoneal bladder rupture and extraperitoneal, including implications. Discuss renal trauma, including grading. Discuss adrenal trauma. Discuss aortic trauma.
2 Introduction Wikimedia Commons Abdominal trauma is responsible for about 10% of all deaths related to trama. Abdominal trauma may involve penetrating or blunt injuries. Penetrating injuries include gunshot and shrapnel injuries, impalements, and knifings. Penetrating injuries often result in injury to hollow organs, such as the intestines. The liver is the most commonly injured solid organ. Gunshot wounds are classified as high energy and may result in extensive damage, especially if the bullet ricochets off of bone. Patients are at increased risk for both hemorrhage and peritonitis, especially with intestinal injury. The most common injuries from gunshot wounds include: o Small intestines: 50%.
3 o Colon: 40%. o Liver: 30%. o Vascular structures: 25%. The most common injuries from stab wounds include: o Liver: 40%. o Small bowel: 30%. o Diaphragm: 20%. o Colon: 15%. Blunt trauma is more common than penetrating and may result from motor vehicle accidents, sports accidents, blows, falls, or explosions. Blunt trauma is more difficult to assess because injuries are less obvious, so massive blood loss may occur before injuries are detected. There are 3 types of blunt injuries: 1) crush, which results from compression, 2) shear, which involves tearing, and 3) burst, which relates to sudden increased pressure (such as from an explosion). Motor vehicle accidents, the most common cause of blunt abdominal injuries, often result in hepatic injury to the passenger if impact is on the passenger s side and splenic injury to the driver if impact is on the driver s side. A tremendous force is needed to fracture a pelvis, so any time a trauma patient presents with pelvic trauma, abdominal trauma should be suspected. Abdominal cavity Thoracic Liver, spleen, abdomen diaphragm, stomach Retroperitoneal abdomen True abdomen Kidneys, ureters, pancreas, duodenum Small intestines, colon, bladder The ribs provide some protection although the organs are vulnerable to both blunt and penetrating trauma. Organs are generally better protected than organs in the thoracic abdomen as they are behind other organs. The large and small intestines are vulnerable to rupture with blunt trauma. The bladder is somewhat protected behind the symphysis pubis, but a full bladder is especially vulnerable
4 to rupture. Common abdominal injuries include: Hepatic lacerations. Splenic rupture. Bladder rupture. Mesenteric artery tears. Great vessel tears. Diaphragmatic rupture. Gastric rupture. Renal injury. Pancreatic injury. Retroperitoneal hematoma. Multiple injuries are common, so any type of abdominal injury should raise suspicions of associated injuries. Initial assessment Primary survey: ABCs As with all trauma patients, assessment should begin with the primary survey, during which the patient is at least partially disrobed for examination, placed on monitors (BP, cardiac, pulse oximeter) as indicated, and two large-bore intravenous lines placed. It IV access cannot be achieved, then a large-bore central line may be placed in the femoral vein, subclavian, or internal jugular vein. In some cases, venous cutdown may be indicated. An interosseous line may also be placed, especially in children, if other access is not possible. Airway, breathing, and circulation (ABCs) are checked immediately, often while resuscitation efforts are occurring. The patient must be assessed for blood loss. With blunt trauma, severe bleeding may occur rapidly, so the patient must be observed for signs of bleeding and blood loss estimated. Any impaled items, such as a knife stuck into the abdomen, should be stabilized with bulky dressings until scans are completed and/or the patient is taken for surgical removal. Protruding organs or eviscerations should be covered with sterile saline dressings. Oxygen is usually administered with a non-rebreather mask, and NG tube inserted (if there is no facial trauma), and blood samples (type
5 and crossmatch and CBC) and urine specimen obtained per indwelling catheter. Physical signs of internal bleeding include: Abdominal pain. Guarding, rigidity. Bruising, crepitus, swelling (especially across chest and pelvis from seat belt and or shoulder harness). Abdominal distention, deformity. Tachycardia, hypotension. Pallor. Evisceration. Cullen s sign: Bruising about the umbilicus (may indicate hemoperitoneum or retroperitoneal bleeding but may take 12 hours to develop). Grey Turner s sign: Bruising over flank (may indicate retroperitoneal bleeding but may take 12 hours to develop). Hematuria. Blood or semen at urethral meatus (from injury to prostate). Inability to urinate. Hemorrhagic shock classification Class Blood loss Signs and symptoms I 15% Mild tachycardia ( bpm), localized swelling, and frank bleeding. II 15 to 25% Tachycardia, prolonged capillary refill and increased diastolic BP. III 25 to 50% Above signs (any) as well as hypotension, confusion, decreased urinary output, and acidosis. IV >50% Hypotension and acidosis unresponsive to resuscitation. Geriatric patients must be observed carefully as they may have less obvious signs of shock for a variety of reasons. Cardiac response to hypovolemia is often lessened because of myocardial pathology or medications, such as -blockers and calcium channel blockers. Metabolic acidosis (decreased serum bicarbonate and increased base deficit (> -6) or increased serum lactate) may result from hemorrhage and hypovolemia. Secondary survey: DE,
6 ABPU, and AMPLE The patient is examined more thoroughly to determine which diagnostic tests are indicated (often after initial standard x-rays of later cervical spine, supine chest, and pelvis). D: Neurological status (D for disability) is assessed. A quick assessment may be done using the AVPU method: A: Is the patient alert? V: Is the patient verbal? P: Is the patient responding only to verbal stimuli? U: Is the patient completely unresponsive. If the patient is alert (A) and verbal (V), then the AMPLE method may be used to ask a series of basic informational questions: A: Do you have any allergies? M: Are you taking any medications? P: What is your past medical history and (if applicable) are you pregnant? L: When did you last eat? E. What events led to the trauma, and when did you have your last tetanus vaccination? E (for exposure): The patient is completely disrobed, if possible. If there is any danger of cervical trauma or the patient cannot be moved, the clothing should be cut off. If forensics are involved (as in shootings and knifings), care must be used to avoid cutting through or damaging areas of clothing that may provide evidence, such as where a bullet has entered clothing. Protocols for collection of evidence should be carefully followed. NOTE: In reality, the Primary and secondary surveys may be done concurrently or overlap, depending on the patient s condition. Key information needed during history Motor vehicle Crash mechanism (what happened). accidents Use of seatbelt and chest restraints. Amount of external damage to the car. Airbag deployment. Integrity of windshield. Deformity of steering wheel Loss of consciousness. Ambulatory status. Other passenger injuries or fatalities. Ejection from vehicle. Penetrating Type of weapon involved
7 trauma Number of injuries (gunshots, stabbings). Victim s distance from weapon. Patient s position at the time of injury. Diagnostic procedures: If time is not a critical factor, the CT scan is the best tool for assessing all types of abdominal injuries, including bleeding. CT is usually done with contrast. Fast-scanning and image-reconstructing helical CT scanners have reduced the turnaround time for CTs to as little as 10 minutes, but older scanners may require more time. X-rays, while often done, provide little useful information as they may not identify free air and fluid collections must be large (>800 ml) to be detected by standard x-ray. Angiograms are indicated if injury to vessels is suspected in order to identify the site of bleeding. However, if the patient is unstable or severe bleeding is suspected, then focused abdominal sonography in trauma (FAST) examination should be done. FAST is able to identify intra-abdominal fluid in about 98% of cases. With multiple trauma patients, FAST may also be used if the CT scan is in use and wait time is extended. However, it s important to remember that while FAST will identify intra-abdominal fluid or bleeding, it is not sufficiently sensitive to show disruption of an internal organ. Additionally, a single negative finding by FAST does not preclude bleeding or other injury as it is sensitive to >300 ml of blood. For example, a bowel perforation may result in limited intraabdominal fluid in the initial period. Additionally, intracapsular bleeding or delayed organ rupture may not be captured at the time of FAST but may be identified on later examination or CT scan. Additionally, a positive FAST finding does not necessarily indicate a need for surgical intervention. Diagnostic peritoneal lavage (DPL) may also be used, but FAST is preferred and has generally replaced DPL, as it is relatively fast and
8 less invasive. DPL is especially insensitive to colonic wounds, which require early diagnosis and treatment. DPL is done by inserting an abdominal catheter under local anesthetic. Aspiration is done to determine if free blood is present. If aspirate contains <10 ml of blood and no evidence of intestinal contents, the aspirate is usually reinjected and 1 L of NS infused with the fluid recollected through gravity drainage. Positive findings for DPL Blunt trauma RBC/mL: 100,000 WBC/mL: 500 Amylase (IU/L): 30 Alkaline phosphatase (IU/L): 3 Intestinal contents: Any amount Penetrating trauma RBC/mL (Abdominal stab wound): 5000 RBC/mL (Gunshot wound): 5000 Note that a CBC and hemoglobin are not reliable to diagnose blood loss in the initial assessment although serial tests may indicate blood loss or hemodilution related to fluid resuscitation. White blood cell counts with left shift commonly occur after trauma, usually related to demargination. Usual indications for automatic surgical exploration/repair include: Hemodynamic instability. Evisceration. Peritonitis. Free air in abdomen. Gunshot wound.
9 Stab wounds that are superficial may require extending the wound opening and exploring to determine the extent of injury. Laparoscopy may be used to determine if the peritoneum has been violated. Hepatic trauma The liver is especially vulnerable to trauma because of its anterior position in the abdomen. It may be lacerated or avulsed by either blunt or penetrating injuries. Liver injury should be suspected if a patient has rib fractures on the right side or has abdominal pain, especially in the right upper quadrant. After the spleen, hepatic injury is the second most common abdominal injury, with injury to the posterior segment of the right lobe occurring most frequently. Because of this, bleeding may occur into the retroperitoneal area rather than the peritoneal. Injuries that are commonly associated with hepatic trauma include right lung contusion, right pneumothorax, right-sided rib fractures, right kidney and/or
10 adrenal gland injuries. About 45% of those with hepatic injuries also have injury to the spleen. Injury of the left lobe is less common and most often associated with direct blow to the epigastric area and is associated with injury to the duodenum, pancreas, and transverse colon. Mortality rates with hepatic injury are high (8% to 25%), and it is the most common cause of death related to abdominal trauma. With severe injuries, death can occur within minutes. Hepatic injuries can include lacerations, contusions, subcapsular hematoma, and intrahepatic hematoma. Hepatic injury grading scale Grade I Laceration(s) < 1cm deep. Subcapsular hematoma <1 cm diameter. Grade II Laceration(s) 1 to 3 cm deep. Subcapsular or central hematoma 1 to 3 cm diameter. Grade III Laceration(s) 3 to 10 cm deep. Subcapsular or central hematoma 3 to 10 cm deep. Grade IV Laceration(s) >10 cm deep. Subcapsular or central hematoma >10 cm diameter. Lobar maceration or devascularization. Grade V Bilobar tissue maceration or devascularization. While in the past, surgical management of liver injury was common, it was found that those undergoing surgery tended to have more complications and required more transfusions than those treated more conservatively, so presently only about 20% are treated surgically. In about 70% of cases, bleeding stops spontaneously. Even grade IV injuries may be treated non-surgically if there is no bleeding into the peritoneal or retroperitoneal cavities. However, patients must be carefully monitored as delayed complications, including hemorrhage, abscess, and biloma (encapsulated collection of bile in the peritoneal cavity), may occur. Additionally, patients may require replacement fluids and blood products, such as plasma and platelets for coagulopathy. Hepatic contusions usually heal within a week, but subcapsular hematomas may enlarge initially before slowly clearing. Lacerations may require weeks to heal, and small residual bilomas are common.
11 Splenic trauma The spleen lies posteriorly in the left upper quadrant, behind the 9 th, 10 th, and 11 th ribs with the convex surface under the left hemidiaphragm. The tail of the pancreas contacts the spleen in about 30% of people and is within 1 cm of the spleen in about 70%. The splenic artery provides the major blood supply to the spleen. The spleen filters approximately 10 to 15% of the total blood volume every minute and usually contains 40 to 50 ml of blood, but the spleen can expand to hold much more blood. Splenic injuries are the most common solid organ injuries, accounting for about a fourth of total injuries. Splenic injuries may occur along with injuries to other abdominal organs as well. Penetrating injuries are not common, but can occur, especially with gunshot wounds. Blunt trauma may occur from compression or deceleration injuries, including motor vehicle accidents, blows to the abdomen (kick injuries), and falls. The most common injury associated with splenic injury is fracture of the left lower rib as this indicates sufficient force to the LUQ to cause organ damage. The triad of symptoms associated with splenic rupture includes: Elevation of the left hemidiaphragm. Left lower lobe atelectasis. Pleural effusion. Patients may present with various clinical symptoms. Indications of splenic trauma can include left upper quadrant or left flank pain, Kehr sign (referred pain to the left shoulder). Some patients may be
12 essentially asymptomatic. Indications of shock may be present, including tachycardia, tachypnea, anxiety, and hypotension. If blood begins to pool in the intraperitoneal area, more diffuse abdominal pain and rebound tenderness may be evident. Hypotension occuring with splenic injury is cause for concern as it may indicate rupture of the spleen with profound hemorrhage. If shock cannot be compensated, immediate surgical exploration is indicated as the delay needed to confirm hemorrhage by CT scan may result in the patient bleeding out. Patients with compensated shock may be treated with angioembolization if this can be done quickly. Because of the spleen s importance to the immune system, splenic retention is the goal for those who are hemodynamically stable. Over 90% of children can be treated nonsurgically, regardless of the grade of injury and up to 65% of adults. Patients who are unstable with suspected injury to the spleen and intra-abdominal hemorrhage may require exploratory laparotomy and repair or removal of the spleen. Additionally, patients with blunt trauma and hemodynamic instability that does not respond to administration of intravenous fluids may be considered to have a lifethreatening splenic injury requiring surgery. Splenic injury grading scale Grade I Laceration(s) < 1cm deep. Subcapsular hematoma <1 cm diameter. Grade II Laceration(s) 1 to 3 cm deep. Subcapsular or central hematoma 1 to 3 cm diameter. Grade III Laceration(s) 3 to 10 cm deep. Subcapsular or central hematoma 3 to 10 cm deep. Grade IV Laceration(s) >10 cm deep. Subcapsular or central hematoma >10 cm diameter. Grade V Splenic tissue maceration or devascularization. The goal with splenic injury is to conserve the spleen whenever possible. Splenectomy increases the risk of postsplenectomy sepsis although it may be necessary with multiple injuries or severe hemodynamic instability. Postoperatively, recurrent bleeding may occur with splenorrhaphy, especially during the first 24 to 48 hours. Complications in the early
13 postoperative period for splenectomy or splenorrhaphy can include bleeding, gastric distention, gastric necrosis, pancreatitis, and subphrenic abscess. Later complications can include deep vein thrombosis and overwhelming post splenectomy infection (OPSI) (usually at 1 to 6 weeks). OPSI can occur within 2 years of splenectomy, especially in children, so prophylactic antibiotics may be given for 2 years. OPSI occurs in about 3% of splenectomy patients with about 50% developing pneumonia or meningitis. Symptoms are often rapid and about half die within 2 days of onset. Gastric Trauma Because the stomach has 3 muscle layers, blunt trauma perforations are rare although risk increases if a person suffers a severe blunt force trauma with a full stomach. Forceful blunt trauma may result in rupture of the left hemidiaphragm, causing the stomach to herniate into the left hemithorax. The areas most prone to rupture include: Anterior wall: 40%. Greater curvature: 23%. Lesser curvature: 15%. Posterior wall: 15%. Perforation may result from abdominal impact such as when a pedestrian is struck by a motor vehicle or during a motor vehicle accident in which a person is ejected from the car or the seat belt is improperly applied. Other injuries can include hematomas and contusions, but these injuries are often essentially asymptomatic and may resolve over time although large hematoma of the distal portion of the stomach may narrow the lumen and prevent emptying. Because the stomach has a rich supply of arteries, damage to the arteries may result in lifethreatening hemorrhage.
14 It s important to note that when blunt trauma is severe enough to cause perforation of the stomach, 95% of patients also have another serious injury. The most common injuries associated with gastric perforation include: Spleen: 27% to 43%. Left chest: 18% to 29% Liver: 18%. Small intestine: 18%. Penetrating trauma of the stomach, such as from a knife or gunshot wound, is more common and should be suspected when penetration is inferior to the nipples or 4 th intercostal space anteriorly or inferior to the tips of the scapulae posteriorly. Symptoms of perforation include severe abdominal pain, abdominal rigidity, hematemesis and bloody nasogastric drainage. While the stomach usually contains few bacteria, with perforation, stomach acids begin to pour into the peritoneal cavity, resulting in chemical peritonitis. Most patients present with shock and pain in the abdomen, but some patients may have no signs of an acute abdomen in the initial period. Gastric injury grading scale I Intramural hematoma OR superficial laceration II <2 cm laceration of pylorus or gastroesophageal junction OR <5 cm laceration of proximal third of stomach OR <10 cm laceration of distal two-thirds of stomach. May be observed or drain placed with Lembert, imbricated suturing. Similar to above. III >2 cm laceration of pylorus or Primary surgical repair,
15 IV V GE junction OR 5 cm laceration of proximal third of stomach OR 10 cm laceration of distal twothirds of stomach. Perforation or devascularization of <two-thirds of stomach. Perforation or devascularization of >two-thirds of stomach. pyloroplasty or total gastrectomy (usually for GE junction injury) as indicated. Subtotal or total gastrectomy with Roux-en Y or Billroth II reconstruction. Gastrectomy (Roux-en-Y reconstruction). Upright x-rays may show free air in the abdomen, but only about 50% to 66% develop enough free air in the abdomen to be detected by upright x-ray. DPL may show food particles or bilious fluids in the abdomen. However, if the patient is hemodynamically stable, CT with contrast provides a definitive diagnosis. Intestinal trauma Intestinal trauma may occur as the result of blunt or penetrating trauma, such as from gunshot wounds or knifings. Penetrating trauma may result in evisceration of the small intestines through the abdominal wall. Falls from great heights or crush injuries may result in evisceration through the rectum or perineum. The small intestines are especially vulnerable to penetrating wounds as they cover the
16 abdominal surface. Motor vehicle accidents also frequently result in injury to the small intestines. The location of the duodenum and its attachments make it one of the most commonly injured sites, especially with steering wheel injuries that force the duodenum against the spine. Patients often present with back pain when they have duodenal injuries. Blunt trauma can result from two different types of forces: Compression: Increases intraluminal pressure inside of the bowel and compresses the fluid-filled bowel against the vertebrae or other solid structures. Deceleration: Stretches and tears the bowel. Injuries of the small intestine occur about 4 times more frequently than injuries of the colon. Injury to the colon occurs in 2% to 15% of those with blunt abdominal injuries, often motor vehicle accidents. Intestinal trauma may also result from diagnostic or therapeutic procedures, such as colonoscopy, laparoscopy, and radiotherapy, as well as from ingestions, such as from swallowing a toothpick. Because injury to the colon requires considerable force, other abdominal injuries are frequently present, especially with injury to the transverse colon. Other injuries include: Hepatic: 64%. Spleen: 52%. Small intestinal mesentery: 48%. Intestinal injuries results in mortality rates of 10% to 30%, but death may be caused by other injuries rather than just the intestinal trauma. Delay in diagnosing and treating intestinal perforation results in mortality rates of 25% to 35%. As with other abdominal injuries, the CT is the best diagnostic tool and is about 97% accurate in providing evidence of bowel injury; however, CT findings may be compromised if a patient first has DPL, as this procedure may introduce intraperitoneal fluid and air. CT is not always effective in identifying the exact location of an injury to the bowel, and CT in general is less effective in identifying injuries to hollow organs than to solid organs. Typically, patients have non-specific symptoms or are asymptomatic initially but return with a few hours or a couple of days with signs of peritonitis, including: Abdominal distention, rigidity.
17 Guarding, rebound tenderness. Abdominal pain. Lack of bowel sounds, paralytic ileus. Elevated WBC counts. Fever. Tachycardia. Dyspnea. Nausea and vomiting. If gross blood is found with a rectal exam, this is usually indicative of severe intestinal injury. Intestinal perforation may progress to abscess, fistula, and/or sepsis. The site of perforation is an important risk determinant. Little bacteria are present in the proximal segments of the small intestines, but the distal segments contain both aerobic and anaerobic bacteria, which can rapidly result in severe infection. According to some studies, the most commonly perforated areas of the small intestine are the proximal jejunum and the distal ileum. Treatment of mild intestinal injury may be conservative, but with perforation, surgical intervention with peritoneal lavage is indicated as well as antibiotics. In some cases, primary closure is avoided and the wound left open to heal by secondary intention. Pancreatic trauma The pancreas is located in a fairly protected part of the abdomen, high in the retroperitoneum, so when it is injured as the result of blunt trauma, then 90% to 95% of the time, there are injuries to other organs as well. Because of this, injury to the pancreas may be overlooked. Common associated injuries include: Liver: 32% to 42%. Spleen: 25% to 40%. Stomach: 20% to 40%. Major vessel: 25% to 35%. Thorax: 22% to 31%. Intestines: 10% to 29%. Central Nervous System: 25%. Duodenum: 18%. While injury to the pancreas occurs in fewer than 10% of all cases of blunt abdominal trauma, the pancreas is injured in 20% to 30% of cases of penetrating trauma. Blunt trauma may result from motor vehicle or pedestrian accidents. Direct blows to the epigastrium may crush the pancreas against the spine.
18 Penetrating injuries most often are associated with gunshot wounds or stabbings to the back, flank, or abdomen. Because vascular structures, such as the aorta and the superior mesenteric artery lie close to the head of the pancreas, injury to that area may include adjacent vascular injury and life-threatening hemorrhage. Symptoms specific to pancreatic trauma are often missing or nonspecific but can include abdominal pain, flank pain, epigastric pain and nausea and vomiting (bile). Diagnosis is often delayed because patients are treated for other injuries and then further testing is done when the patients fail to improve or continue to deteriorate. As with other injuries, the CT scan provides the most definitive diagnosis as the scan may show lacerations or peripancreatic fluids. Blunt trauma may result in retroperitoneal hematoma and fluid, free abdominal fluid and pancreatic edema. In the early phases after injury, CT scans may not detect injury, so ongoing evaluation is necessary. If the CT scan is inconclusive, then magnetic resonance cholangiopancreatography may be indicated, as it more clearly outlines damage to the ducts. Standard x-rays are not effective for diagnosis of pancreatic injury but findings of fractures of the lower thoracic or upper lumbar vertebrae should raise suspicion of pancreatic or duodenal injury. FAST may show free abdominal fluid but the position of the pancreas and the overlying of the pancreas by the colonic gas make visualization difficult. DPL has not been found useful because of the retroperitoneal location.
19 Serum amylase levels have been used to help diagnose pancreatic injury, but studies show that levels don t elevate for about 3 hours, so serum amylase levels prior to 3 hours are not diagnostic. Additionally, patients with brain injuries also have elevations in serum amylase, so if a patient suffers both brain and abdominal trauma, elevation does not necessarily indicate pancreatic trauma. Pancreatic enzymes (amylase and lipase) may be abnormal because of shock rather than direct pancreatic injury, but they may remain normal even with severe pancreatic injury. There are 3 different grading scales used to classify pancreatic injury. Although they are similar, this can lead to some confusion. The following grading system is that of the Organ Injury Scaling Committee of the American Association for the Surgery of Trauma. Pancreatic injury grading scale I Simple contusion. II Major contusion or laceration without tissue loss or involvement of the main pancreatic duct. III Complete transection of the pancreas or a parenchymal injury with involvement of the major duct to the left of the superior mesenteric vein. IV Ductal transection or a major parenchymal injury to the right of the superior mesenteric vein. V Massive disruption of the head of the pancreas. Most injuries to the pancreas are relatively minor and can be treated by inserting external drains until healing occurs. Distal pancreatectomy may be necessary with traum to the body, neck and/or tail with duct disruption. Trauma to the head of the pancreas is usually treated with external drainage even in the presence of ductal damage. Pancreaticoduodenectomy is usually done only when the head of the pancreas has been severely damaged and devitalized. Post-operative complications can include pancreatic abscess, fistula, pseudocysts, and diabetes mellitus. The most common complication is development of a pancreatic fistula. These usually resolve spontaneously in 1 to 2 weeks with adequate drainage and nutrition. Octreotide is sometimes given perioperatively to prevent fistula development or when a pancreatic fistula occurs. Complications occur in 20% to 40% of those who are treated surgically for pancreatic trauma with 30% of deaths related to sepsis and multi-organ failure. About 10% to 25% develop abscesses. Pseudocysts may develop
20 weeks or months after trauma. About 18% of those with surgical repair of pancreatic trauma develop mild transient pancreatitis. Bladder trauma The urinary bladder is a muscular hollow distensible organ that lies at the floor of the pelvis, protected by the symphysis pubis. The bladder is most vulnerable in children because it is suspended above the symphysis pubis. By about age 20, the bladder descends into the pelvis. Older males are also more vulnerable because an enlarged prostate displaces the bladder upward. The most common injury is bladder contusion, an incomplete or partial tear of the bladder mucosa, causing localized injury and hematoma. Contusion usually presents as gross hematuria, but the condition usually resolves after a period of bedrest. Blunt trauma is more likely to result in rupture of the bladder if the bladder is distended, causing it to rise above the symphysis pubis. People who are inebriated at the time of injury in a motor vehicle injury should be carefully examined for possible bladder rupture as excessive drinking often results in a distended bladder. Most blunt trauma results from motor vehicle accidents (85%) with falls (7%) and assaults (6%) causing the rest of the injuries. Fractures of the pelvis (commonly the anterior pubic arch) or symphysis pubis may also result in rupture either from bone fragments or shear injury. Damage to the bladder may also result from orthopedic trauma when orthopedic pins or screws used to stabilize
21 pelvic fractures perforate the bladder. Up to a quarter of those with pelvic fractures also have urethral trauma. The bladder may also be ruptured through penetrating trauma, such as gunshot wounds (85%) and knifings (15%) usually resulting in multiple organ injuries. While non-traumatic bladder perforation can occur, about 82% of bladder rupture relates to external trauma with 60% to 85% from blunt trauma and 15% to 40% from penetrating. Approximately 50% to 71% of traumatic bladder perforations are extraperitoneal (usually related to pelvic fractures) while 25% to 43% are intraperitoneal (usually related to a direct blow to a distended bladder, such as with a seatbelt injury) and 7% to 14% are combined (often related to gunshot wounds), a much more serious situation with a 60% mortality rate. Intraperitoneal perforation may remain undiagnosed for extended periods because the urine continues to drain into the abdomen. In this case, the patient may be anuric and may develop electrolyte imbalances as urine is reabsorbed. Urinary ascites may occur with diagnosis per paracentesis. Associated injuries are common and include: Gunshot wounds: 83% have bowel injuries. Stab wounds: 33% have colon injuries. Penetrating trauma in general: 82% have vascular injuries. While symptoms of bladder injury may be non-specific, a common triad includes hematuria, suprapubic pain or discomfort, and difficulty urinating or anuria. Gross hematuria occurs in about 90% of those with bladder rupture with 88% having pelvic fractures. Other signs of rupture include abdominal distention, guarding, and rebound tenderness. With intraperitoneal rupture, bowel sounds may be absent. Blood in the urethral meatus may indicate trauma to the urethra, an indication for retrograde urethrography prior to insertion of a Foley catheter because passing a catheter may exacerbate a small tear. If a patient has a posterior urethral injury, a suprapubic catheter should be inserted. Urethral injuries are rare in females but may occur in males because of the longer length and positioning of the urethra. Ureters are rarely injured by blunt trauma but may be damaged by penetrating trauma.
22 The CT cystogram provides the most definitive diagnosis of bladder rupture. Once a catheter is in place, dilute water soluble contrast is instilled followed by an abdominal/pelvic CT. Note that water soluble contrast is less likely to result in peritonitis if the solution leaks into the abdomen. In some cases, standard cystography may also be indicated. Treatment depends on the type of rupture: Extraperitoneal ruptures: Foley catheter (SP or urethral) for 7 to 10 days with a cystogram to determine if laceration has healed. Almost all heal within 21 days. If extensive extravasation occurs, then surgical exploration may be indicated.
23 Intraperitoneal: Most require surgical repair as prolonged catheterization alone rarely brings about healing. However, some authorities recommend conservative treatment for small perforations, but there is no consensus regarding this approach. Note that gunshot wounds are almost always explored surgically, and in that case, even extraperitoneal ruptures may be sutured closed. After surgical exploration, a pelvic drain is usually left in place for 2 to 3 days, and IV antibiotics are administered. Post-surgical complications can include urinary extravasation (usually treated by extended catheter drainage), wound dehiscence, hemorrhage, infection, and impaired bladder function. Remember that while only 10% of pelvic fracture patients have a ruptured bladder, 90% of ruptured bladders relate to pelvic fractures, so bladder rupture should always be suspected with pelvic fractures. Renal trauma Generally, the kidneys are paired organs in the retroperitoneal space on the posterior abdominal wall extending from the 12 th thoracic vertebrae to the 3 rd lumbar vertebrae in the adult. The kidneys are well protected by the rib cage and the muscles of the back and abdomen; however, the lower portions of the kidneys extend below
24 the 12 th ribs. Fatty deposits that protect them against jarring surround the kidneys. An adrenal gland sits on top of each kidney. The kidneys receive 20% to 25% of the total cardiac output, and all of the body s blood circulates through the kidneys about 12 times each hour, so damage to the kidney s vasculature may result in hemorrhage. About 10% of those with abdominal trauma sustain renal injuries with blunt trauma injuries about 9 times more frequent than penetrating trauma injuries. Blunt injuries include renal contusion, renal laceration, and renal vascular injury. Blunt injuries usually result from motor vehicle accidents, falls, and pedestrian accidents or sport injury that result in a direct blow to the flank area. Symptoms may be very nonspecific but can include abdominal or flank pain and gross or microscopic blood in the urine. In the renal injury grading system, grades I and II are classified as minor injuries and grades III, IV, and V as major. Major renal trauma is usually caused by penetrating injuries (40%) rather than blunt (15%). Renal injury grading system I Contusion: Microscopic or gross hematuria. Urological studies normal. Hematoma: Subcapsular, nonexpanding without parenchymal laceration. II Hematoma: Nonexpanding perirenal hematoma confined to renal retroperitoneum. Laceration: <1cm parenchymal depth of renal cortex without urinary extravasation. III Laceration: >1 cm depth of rental cortex, without collecting system rupture or urinary extravasation. IV Laceration: Parenchymal laceration extending through the renal cortex, medulla, and collecting system. Vascular: Main renal artery or vein injury with contained hemorrhage. V Laceration: Completely shattered kidney. Vascular: Avulsion of renal hilum, which devascularizes kidneys. Diagnosis is based on a number of factors. Urinalysis is standard, but some types of renal injury (avulsion, renal artery laceration) may not result in hematuria, so the absence of blood does not rule out damage to the kidneys. In the past the intravenous pyelogram (IVP) was used
25 for diagnosis, but the CT scan with contrast is now the procedure of choice. While in the past surgical repair was the standard, with low-grade blunt trauma, the kidneys actually usually heal with bedrest and observation. Most injuries to the kidneys (grades I to IV) are managed non-surgically, but patients must be monitored carefully after treatment as late bleeding may occur, and some patients develop hypertension because of kidney damage. With high-grade trauma or penetrating injuries, surgical exploration may be indicated, especially if the patient has other abdominal injuries and is hemodynamically unstable. Only about 9% of renal injuries require surgical intervention and about 11% of these result in nephrectomy, usually because of hemorrhage or severe renovascular injury. Complications can also include perirenal abscess and or urinary leakage. Adrenal trauma Trauma to the adrenal glands is rare (<1% to 2%) because they are well protected under the rib cage, but injuries do occur, especially with multiple organ traumas. Adrenal gland trauma is associated with mortality rates about 5 times higher than if there is no adrenal gland trauma. Injury may result from blunt trauma (most commonly motor vehicle accidents), or penetrating trauma.
26 Adrenal trauma is associated with: Hepatic injury. Splenic injury. Renal injury. Rib fractures. Lumbar fractures. Pelvic fractures. In many cases, patients also have multiple other injuries, such as head injuries and injuries to the extremities. Hematoma or laceration of the adrenal gland often is found incidentally with CT scan to evaluate other abdominal injuries. One study found that left adrenal hematomas were most commonly associated with left rib fractures and splenic and left renal injuries while right adrenal hematomas were associated with right rib fracture and hepatic and right renal injuries. One study of pediatric patients with adrenal trauma showed that those with unilateral injury rarely showed evidence of adrenal insufficiency, but adrenal insufficiency should be suspected in bilateral injuries. About 78% of adrenal hematomas occur on the right, possibly because the area about the gland is more confined because of the mass of the liver on the right. Additionally, high deceleration pressures may be transmitted through the inferior vena cava and the short right adrenal gland. The right adrenal gland lies directly behind the inferior vena cava. Diagnosis is by CT but may be impacted by the presence of benign adenomas, which are common but can be misdiagnosed as hematomas. FAST may also be used as a screening tool. Treatment is usually conservative as hematomas usually resolve over time. In severe injuries, such as with gunshot wounds, adrenalectomy may be indicated. Hemorrhage may require transfusions. Acute adrenal insufficiency (usually related to bilateral injury and hemorrhage) must be quickly diagnosed and treated with glucocorticoids. Aortic trauma The aorta can be injured with both blunt and penetrating trauma. Tearing may occur from sudden deceleration, as in motor vehicle accidents, and impact with the steering wheel may result in
27 compression that ruptures the aorta. About 80% to 90% of great vessel trauma is fatal with 15% of deaths related to motor vehicle accidents caused by aortic trauma. Those with small tears or partial thickness tears may survive. A free rupture typically present with widened mediastinum, hemothorax and hemodynamic instability and is almost always fatal; however, a controlled rupture in which there is no hemothorax and the patient remains hemodynamically stable has about a 90% survival rate with prompt surgical intervention. The most common site of aortic trauma is distal to the
28 left subclavian at the level of the ligamentum arteriosum as this is the point of maximum stress and tearing from deceleration forces. Therefore, the aorta is at risk in frontal and side impacts as well as falls from heights. If aortic injury is not treated promptly the patient may develop hypoxia and hypovolemia with anoxic encephalopathy and ischemic damage to other viscera. Diagnosis of aortic injury is through CT scan. If the scan is not definitive, than an aortogram may be done to identify small tears. In some cases intravascular ultrasound (IVUS) or transesophageal echocardiography (TEE) may be done instead of aortogram, as these procedures are less invasive. CT scan may be preceded by chest x-ray (with head elevated) and insertion of an NG tube and/or chest tube. The CT may show a contained rupture, which is referred to as a traumatic pseudoaneurysm. Chest x-ray is not diagnostic but may show an abnormal mediastinum, distortion of the aorta, and depressed left main stem bronchus as well as deviation of a nasogastric tube. These finding are suggestive of aortic injury. Bleeding may result from tears of mediastinal veins, but this is an indirect indication of possible aortic injury. If patients with suspected aortic injury are hemodynamically unstable, priority is given to controlling hemorrhage while avoiding overresuscitation. FAST of DPL may be utilized to identify concealed areas of hemorrhage. Patients with aortic tear and impending rupture may develop a cyclical pattern of responding to fluid resuscitation and then
29 exhibiting hypotension. A cycle of repeated fluid resuscitations can lead to rupture, especially if other signs, such as widened mediastinum and left-sided hemothorax, are present. Aortic injury is associated with diaphragmatic rupture, so any patient with aortic injury should be assessed for injury to the diaphragm and vice versa. Aortic injuries are almost always repaired surgically. In some cases thoracic endovascular aortic repair (TEVAR) with insertion of stents may be used. Recent studies indicate that delaying surgery for up to 4 days in non-acute cases, allowing other injuries to be treated and the patient stabilized, has resulted in a lower overall mortality rate than rushing patients into surgery. If the patient must undergo a craniotomy or exploratory laparotomy because of other injuries and the aortic injury is not acute, -blockers may be administered to reduce heart rate and force of contractions. Nitroprusside may also be used to control blood pressure and prevent rupture. Conclusion Time is a critical factor with abdominal trauma. Patients must be assessed and evaluated immediately, and a finding of pelvic fracture or trauma to one abdominal organ should always raise suspicion of associated injuries. The diaphragm is the broad muscle that separates the thoracic cavity from the abdominal cavity. The diaphragm is rarely (<5%) injured with blunt trauma, and most of these injuries result from motor vehicle accidents with lateral impact 3 times more likely to cause tears than frontal impacts because of distortion of the chest wall and shearing. Diaphragm injuries may occur from either gunshot wounds or stabbings. Diaphragmatic injuries rarely occur in isolation so they may be overlooked when attention focuses on associated abdominal injuries, but diaphragmatic injury should be suspected in those with abdominal trauma presenting with ventilatory compromise. References
30 Abdominal trauma: Role of CT. (n.d.). The Radiology Assistant. Retrieved November 9, 2011, from American Academy of Orthopaedic Surgeons. (2009). Advanced Assessment and Treatment of Trauma. Sudbury, MA: AAOS. Bjerke, HS. (2009, August 6). Splenic rupture. Medscape Reference. Retrieved November 9, 2011, from Bjerke, HS. (2010, January 2). Pancreatic Trauma. Medscape Reference. Retrieved November 9, 2011, from Chest trauma: Traumatic aortic injury. (2004, April). Trauma.org. Retrieved November 9, 2011, from Degiannis, E, Glapa, M, Loukogeorgakis, SP, & Smith, MD. (2008). Management of pancreatic trauma. International Journal of the care of the Injured, 39: Retrieved November 9, 2011, from a.pdf Fotheringham, T. (2008). Pancreatic injuries. Nordic Trauma Society. Retrieved November 9, 2011, from Havens, J, & Lieberman, G. (2002, November 17). Blunt thoracic aortic trauma. Harvard Medical School. Retrieved November 9, 2011, from Hepatic trauma: Liver laceration. (2004). LearningRadiology.com. Retrieved November 9, 2011, from e.htm Kawashima, A, et al. (2001, May). Imaging of renal trauma: A comprehensive review. RadioGraphics. Retrieved November 9, 2011, from Kidney (renal) trauma. (2011, January). AUAFoundation. Retrieved November 9, 2011, from Lusaya, DG. (2011, October 20). Renal trauma. Medscape Reference. Retrieved November 9, 2011, from overview#showall McPhee, SM, & Papadakis, MA. (2009). Current Medical Diagnosis & Treatment. San Francisco: McGraw Hill Medical.
31 Mick, MW, Peter, JR, Egan, D, & Nadel, ES. (2006). Blueprints Emergency Medicine. 2 nd ed. Baltimore, MD: Lippincott Williams & Wilkins. Mitchell, EL, & Medson, R. (2005). Introduction to Emergency Medicine. Philadelphia: Lippincott Williams & Wilkins. Mukhopadhyay, M. (2009). Intestinal injury from blunt abdominal trauma: A study of 47 cases. OMJ, 24: Retrieved November 9, 2011, from ntestinalinjuryfromblunabdominaltraumaastudy.html Rackley, R. (2009, August 17). Bladder trauma. Medscape Reference. Retrieved November 9, 2011, from Rana, AI, et al. (2004, March). Adrenal gland hematomas in trauma patients. Radiology, 230: Retrieved November 9, 2011, from Seldman, C. (n.d.). Renal trauma. Trauma.org. Retrieved November 9, 2011, from Smeltzer, SC, Bare, BG, Hinkle, JL, & Cheever, KH. (2008). Brunner & Suddarth s Textbook of Medical-Surgical Nursing, 11 ed., Philadelphia: Wolters Kluwer/Lippincott, Williams, & Wilkins. Stanton-Maxey, KJ. (2011, August 9). Penetrating abdominal trauma. Medscape Reference. Retrieved November 9, 2011, from overview#a0104 Tritos, NA. (2011, July 13). Adrenal hemorrhage. Medscape Reference. Retrieved November 9, 2011, from
Muscle spasm Diminished bowel sounds Nausea/vomiting
 3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
3 4 5 6 7 8 9 0 Chapter 8: Abdomen and Genitalia Injuries Abdominal Injuries Abdomen is major body cavity extending from to pelvis. Contains organs that make up digestive, urinary, and genitourinary systems.
Abdomen and Genitalia Injuries. Chapter 28
 Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
Abdomen and Genitalia Injuries Chapter 28 Hollow Organs in the Abdominal Cavity Signs of Peritonitis Abdominal pain Tenderness Muscle spasm Diminished bowel sounds Nausea/vomiting Distention Solid Organs
PROTOCOLS. Lap-belt syndrome. Principal investigator. Background
 Lap-belt syndrome Principal investigator Claude Cyr, MD, Centre hospitalier universitaire de Sherbrooke, 3001 12 e Avenue Nord, Sherbrooke QC J1H 5N4; tel.: (819) 346-1110, ext. 14634; fax: (819) 564-5398;
Lap-belt syndrome Principal investigator Claude Cyr, MD, Centre hospitalier universitaire de Sherbrooke, 3001 12 e Avenue Nord, Sherbrooke QC J1H 5N4; tel.: (819) 346-1110, ext. 14634; fax: (819) 564-5398;
Pediatric Abdomen Trauma
 Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
2. Blunt abdominal Trauma
 Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Abdominal Trauma 1. Evaluation and management depends on: a. Mechanism (Blunt versus Penetrating) b. Injury complex in addition to abdomen c. Haemodynamic stability assessment: i. Classically patient s
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma. Last reviewed June 2014
 Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
Canadian Undergraduate Urology Curriculum (CanUUC): Genitourinary Trauma Last reviewed June 2014 Session Objectives 1. Recognize hematuria as the cardinal symptom of urinary tract trauma. 1. Outline the
A Z OF ABDOMINAL RADIOLOGY
 Z OF BDOMINL RDIOLOGY bdominal trauma to Z of bdominal Radiology Clinical characteristics general discussion, followed by organ-specific summaries, is given below. bdominal trauma is managed as part of
Z OF BDOMINL RDIOLOGY bdominal trauma to Z of bdominal Radiology Clinical characteristics general discussion, followed by organ-specific summaries, is given below. bdominal trauma is managed as part of
UBC Department of Urologic Sciences Lecture Series. Urological Trauma
 UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
UBC Department of Urologic Sciences Lecture Series Urological Trauma Disclaimer: This is a lot of information to cover and we are unlikely to cover it all today These slides are to be utilized for your
Role of imaging in evaluation of genitourinary i trauma Spectrum of GU injuries Relevance of imaging findings in determining management Focus on MDCT
 Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
Genitourinary Tract Injuries 6 th Nordic Course Scott D. Steenburg, MD Assistant Professor University of Maryland Department of Radiology Division of Trauma and Emergency Radiology R Adams Cowley Shock
LIVER INJURIES PROFF. S.FLORET
 LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
LIVER INJURIES PROFF. S.FLORET Abdominal injuries For anatomical consideration: Abdomen can be divided in four areas Intra thoracic abdomen True abdomen Pelvic abdomen Retroperitoneal abdomen ETIOLOGY
Diagnosis & Management of Kidney Trauma. LAU - Urology Residency Program LOP Urology Residents Meeting
 Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
Diagnosis & Management of Kidney Trauma LAU - Urology Residency Program LOP Urology Residents Meeting Outline Introduction Investigation Staging Treatment Introduction The kidneys are the most common genitourinary
PARA107 Summary. Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38:
 PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
PARA107 Summary Page 1-3: Page 4-6: Page 7-10: Page 11-13: Page 14-17: Page 18-21: Page 22-25: Page 26-28: Page 29-33: Page 34-36: Page 37-38: Injury, Mechanisms of Injury, Time Critical Guidelines Musculoskeletal
Genitourinary Trauma Introduction GU Trauma overlooked
 Genitourinary Trauma Introduction GU Trauma overlooked 10-20% of all injured patients Long term morbidity Impotence Incontinence Life-threatening injuries first Urethral Injury Plan Bladder Injury Kidney
Genitourinary Trauma Introduction GU Trauma overlooked 10-20% of all injured patients Long term morbidity Impotence Incontinence Life-threatening injuries first Urethral Injury Plan Bladder Injury Kidney
If your patient is stable, perform a complete assessment using inspection, auscultation, percussion, and pal- By Cynthia Blank-Reid, RN, CEN, MSN
 Abdominal trauma: Dealing with the damage Hidden in the abdomen, life-threatening injuries can elude detection. Find out how to evaluate your patient s condition and prevent further harm. By Cynthia Blank-Reid,
Abdominal trauma: Dealing with the damage Hidden in the abdomen, life-threatening injuries can elude detection. Find out how to evaluate your patient s condition and prevent further harm. By Cynthia Blank-Reid,
SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad
 SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad Trauma Emergency Room layout Ideally the trauma emergency room is centrally located to provide
SPECIAL DIAGNOSTIC STUDIES IN BLUNT TRAUMA OLEH : Prof.DR.Dr Abdul Rasyid SpRad (K),Ph.D Dr.Evo Elidar Sp.Rad Trauma Emergency Room layout Ideally the trauma emergency room is centrally located to provide
Which Blunt Trauma Patients Should Be Studied by Abdominal CT?
 MDCT of Bowel and Mesenteric Injury: How Findings Influence Management 4 th Nordic Trauma Radiology Course 2006 4 th Nordic Trauma Radiology Course 2006 Stuart E. Mirvis, M.D., FACR Department of Radiology
MDCT of Bowel and Mesenteric Injury: How Findings Influence Management 4 th Nordic Trauma Radiology Course 2006 4 th Nordic Trauma Radiology Course 2006 Stuart E. Mirvis, M.D., FACR Department of Radiology
ABDOMINAL TRAUMA Lecture Prof. Zbigniew Wlodarczyk
 ABDOMINAL TRAUMA Lecture Prof. Zbigniew Wlodarczyk Epidemiology 2% of all traumas (4% amongst hospitalized patients) 75% M 25% F Average age 35 years 80% close 20% penetrating 40% liver and spleen, 10%
ABDOMINAL TRAUMA Lecture Prof. Zbigniew Wlodarczyk Epidemiology 2% of all traumas (4% amongst hospitalized patients) 75% M 25% F Average age 35 years 80% close 20% penetrating 40% liver and spleen, 10%
Penetrating abdominal trauma clinical view. Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland
 Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Penetrating abdominal trauma clinical view Ari Leppäniemi, MD Department of Abdominal Surgery Meilahti hospital University of Helsinki Finland Meilahti hospital - one of Helsinki University hospitals -
Radiological Investigations of Abdominal Trauma
 76 77 Investigations of Abdominal Trauma Introduction: Trauma to abdominal organs is a common cause of patient morbidity and mortality among trauma patients. Causes of abdominal trauma include blunt injuries,
76 77 Investigations of Abdominal Trauma Introduction: Trauma to abdominal organs is a common cause of patient morbidity and mortality among trauma patients. Causes of abdominal trauma include blunt injuries,
Review. 1. Peritonitis would MOST likely result following injury to the: A. liver. B. spleen. C. kidney. D. stomach.
 Chapter 28 Review Review 1. Peritonitis would MOST likely result following injury to the: A. liver. B. spleen. C. kidney. D. stomach. Review Answer: D Rationale: In general, solid organs bleed when injured
Chapter 28 Review Review 1. Peritonitis would MOST likely result following injury to the: A. liver. B. spleen. C. kidney. D. stomach. Review Answer: D Rationale: In general, solid organs bleed when injured
Clinical aspects in urogenital injuries
 Clinical aspects in urogenital injuries Rolf Wahlqvist Oslo Urological University Clinic Aker University Hospital Nordic Rad.2008 1 Urogenital injuries in trauma patients Renal injury Ureteral injury (infrequent/iatrogenic)
Clinical aspects in urogenital injuries Rolf Wahlqvist Oslo Urological University Clinic Aker University Hospital Nordic Rad.2008 1 Urogenital injuries in trauma patients Renal injury Ureteral injury (infrequent/iatrogenic)
Bladder Trauma Data Collection Sheet
 Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
Bladder Trauma Data Collection Sheet If there was no traumatic injury with PENETRATION of the bladder DO NOT proceed Date of injury: / / Time of injury: Date of hospital arrival: / / Time of hospital arrival:
A Severely Injured Pediatric Trauma Patient: Case Presentation and Discussion
 A Severely Injured Pediatric Trauma Patient: Case Presentation and Discussion Christopher Butts PhD, DO Surgical Critical Care Fellow Cooper University Hospital H&P 10 year old female presents as a trauma
A Severely Injured Pediatric Trauma Patient: Case Presentation and Discussion Christopher Butts PhD, DO Surgical Critical Care Fellow Cooper University Hospital H&P 10 year old female presents as a trauma
Trauma. Neck trauma zones. Neck Injuries 1/3/2018. Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure
 Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
Trauma 45 minutes highest points Ahmed Mahmoud, MD Basic principles A ; Airway B ; Breathing C ; Circulation D ; Disability E ; Exposure Neck trauma zones Airway ;Rapid sequence intubation Breathing ;Needle
UROLOGIC TRAUMA. Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara
 UROLOGIC TRAUMA Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara UROLOGIC TRAUMA Renal trauma Ureteral injury Bladder injury Urethral injury Injury to external genitalia
UROLOGIC TRAUMA Urology Division, Surgery Department Medical Faculty, University of Sumatera Utara UROLOGIC TRAUMA Renal trauma Ureteral injury Bladder injury Urethral injury Injury to external genitalia
Urogenital Injuries The role of radiology
 Urogenital Injuries The role of radiology NORDTER 7 th Nordic Trauma Radiology Course Helsinki, Finland May 21-24, 2012 Johann Baptist Dormagen, MD, PhD Oslo University Hospital, Norway Kidney injuries
Urogenital Injuries The role of radiology NORDTER 7 th Nordic Trauma Radiology Course Helsinki, Finland May 21-24, 2012 Johann Baptist Dormagen, MD, PhD Oslo University Hospital, Norway Kidney injuries
ABDOMINAL TRAUMA. Aurora Health Care EMS Continuing Education 2 nd Quarter 2011 Packet
 Aurora Health Care EMS Continuing Education 2 nd Quarter 2011 Packet ABDOMINAL TRAUMA Blunt and penetrating abdominal trauma are major causes of morbidity and mortality in the United States, particularly
Aurora Health Care EMS Continuing Education 2 nd Quarter 2011 Packet ABDOMINAL TRAUMA Blunt and penetrating abdominal trauma are major causes of morbidity and mortality in the United States, particularly
Activity Three: Where s the Bleeding?
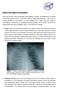 Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Activity Three: Where s the Bleeding? There are five main sites of potentially fatal bleeding in trauma, remembered by the phrase on the floor and four more. On the floor refers to losing blood externally
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System
 Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Lab Monitor Images Dissection of the Abdominal Vasculature + Lower Digestive System Stomach & Duodenum Frontal (AP) View Nasogastric tube 2 1 3 4 Stomach Pylorus Duodenum 1 Duodenum 2 Duodenum 3 Duodenum
Internal Injury Documentation Guidelines
 Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Internal Injury Documentation Guidelines General Open Wound of Thorax Injury to Heart Identify episode of care Initial Subsequent Sequela Laterality Sequela of injury Place of occurrence of injury Activity
Trauma Overview. Chapter 22
 Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Trauma Overview Chapter 22 Kinematics of Trauma Injuries are the leading cause of death among children and young adults. Kinematics introduces the basic physical concepts that dictate how injuries occur
Uroradiology For Medical Students
 Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
Uroradiology For Medical Students Lesson 4: Cystography & Urethrography - Part 2 American Urological Association Review Cystography is useful in evaluating the bladder, the urethra and the competence of
West Yorkshire Major Trauma Network Clinical Guidelines 2015
 WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
WYMTN: Pelvic fracture with urogenital trauma KEY RECOMMENDATIONS 1. During the initial exploratory survey / secondary survey, a. The external urethral meatus and the transurethral bladder catheter (if
TRAUMA SERIES: ABDOMINAL TRAUMA
 TRAUMA SERIES: ABDOMINAL TRAUMA Jassin M. Jouria, MD Dr. Jassin M. Jouria is a medical doctor, professor of academic medicine, and medical author. He graduated from Ross University School of Medicine and
TRAUMA SERIES: ABDOMINAL TRAUMA Jassin M. Jouria, MD Dr. Jassin M. Jouria is a medical doctor, professor of academic medicine, and medical author. He graduated from Ross University School of Medicine and
Algorithms for managing the common trauma patient
 ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
ALGORITHMS Algorithms for managing the common trauma patient J John, MB ChB Department of Urology, Frere Hospital, East London Hospital Complex, East London, South Africa Corresponding author: J John (jeffveenajohn@gmail.com)
George M Wadie, MD Director Division of Pediatric Surgery Sacred Heart Medical Center. Springfield, OR Adjunct Assistant Professor of Surgery Oregon
 George M Wadie, MD Director Division of Pediatric Surgery Sacred Heart Medical Center. Springfield, OR Adjunct Assistant Professor of Surgery Oregon Health and Sciences University. Portland, OR Outline
George M Wadie, MD Director Division of Pediatric Surgery Sacred Heart Medical Center. Springfield, OR Adjunct Assistant Professor of Surgery Oregon Health and Sciences University. Portland, OR Outline
Interventional Radiology in Trauma. Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital
 Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
Interventional Radiology in Trauma Vikash Prasad, MD, FRCPC Vascular and Interventional Radiology The Moncton Hospital Disclosures None relevant to this presentation Shareholder Johnson and Johnson Goal
A Review on the Role of Laparoscopy in Abdominal Trauma
 10.5005/jp-journals-10007-1109 ORIGINAL ARTICLE WJOLS A Review on the Role of Laparoscopy in Abdominal Trauma Aryan Ahmed Specialist General Surgeon, ATLS Instructor, Department of General Surgery, Hamad
10.5005/jp-journals-10007-1109 ORIGINAL ARTICLE WJOLS A Review on the Role of Laparoscopy in Abdominal Trauma Aryan Ahmed Specialist General Surgeon, ATLS Instructor, Department of General Surgery, Hamad
Gastrointestinal Emergencies CEN REVIEW 2017 MARY RALEY, BSN, RN, CEN, TCRN, TNSCC
 Gastrointestinal Emergencies CEN REVIEW 2017 MARY RALEY, BSN, RN, CEN, TCRN, TNSCC Gastrointestinal Emergencies is 7% of the CEN A. Acute abdomen B. Bleeding C. Cholecystitis D. Cirrhosis E. Diverticulitis
Gastrointestinal Emergencies CEN REVIEW 2017 MARY RALEY, BSN, RN, CEN, TCRN, TNSCC Gastrointestinal Emergencies is 7% of the CEN A. Acute abdomen B. Bleeding C. Cholecystitis D. Cirrhosis E. Diverticulitis
Renal Trauma: Management Options
 Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Renal Trauma: Management Options Immediate surgical repair Nephrectomy Conservative management Alonso RC et al. Kidney in Danger: CT Findings of Blunt and Penetrating Renal Trauma. RadioGraphics 2009;
Imaging of Thoracic Trauma: Tips and Traps. Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania
 Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
Imaging of Thoracic Trauma: Tips and Traps Arun C. Nachiappan, MD Associate Professor of Clinical Radiology University of Pennsylvania None Disclosures Objectives Describe blunt and penetrating traumatic
TRAUMA CARE: ABDOMINAL TRAUMA
 TRAUMA CARE: ABDOMINAL TRAUMA Jassin M. Jouria, MD Dr. Jassin M. Jouria is a medical doctor, professor of academic medicine, and medical author. He graduated from Ross University School of Medicine and
TRAUMA CARE: ABDOMINAL TRAUMA Jassin M. Jouria, MD Dr. Jassin M. Jouria is a medical doctor, professor of academic medicine, and medical author. He graduated from Ross University School of Medicine and
Lecture 2: Clinical anatomy of thoracic cage and cavity II
 Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Lecture 2: Clinical anatomy of thoracic cage and cavity II Dr. Rehan Asad At the end of this session, the student should be able to: Identify and discuss clinical anatomy of mediastinum such as its deflection,
Advances in MDCT of Thoracic Trauma
 Baltic Congress of Radiology, Riga 2010 Advances in MDCT of Thoracic Trauma Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General
Baltic Congress of Radiology, Riga 2010 Advances in MDCT of Thoracic Trauma Robert A. Novelline, MD Professor of Radiology, Harvard Medical School Director of Emergency Radiology, Massachusetts General
2 Blunt Abdominal Trauma
 2 Blunt Abdominal Trauma Ricardo Ferrada, Diego Rivera, and Paula Ferrada Pearls and Pitfalls Patients suffering a high-energy trauma have solid viscera rupture in the abdomen and/or aortic rupture in
2 Blunt Abdominal Trauma Ricardo Ferrada, Diego Rivera, and Paula Ferrada Pearls and Pitfalls Patients suffering a high-energy trauma have solid viscera rupture in the abdomen and/or aortic rupture in
Imaging in abdominal trauma
 Imaging in abdominal trauma Dilyana Baleva Medical University Varna Landesklinikum Mistelbach-Gänserndorf Learning objectives Definition, demographics and etiology Imaging modalities and protocols Common
Imaging in abdominal trauma Dilyana Baleva Medical University Varna Landesklinikum Mistelbach-Gänserndorf Learning objectives Definition, demographics and etiology Imaging modalities and protocols Common
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair BACKGROUND EPIDEMIOLOGY 9/11/2018
 Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Pancreatico-Duodenal Trauma: Drain, Debride, Divert, Despair Rochelle A. Dicker, M.D. Professor of Surgery and Anesthesia UCLA BACKGROUND Lancet 1827: Travers, B Rupture of the Pancreas British Journal
Case Discussion Splenic Abscess
 Case Discussion Splenic Abscess Personal Data Gender: male Birth Date: 1928/Mar/06th Allergy: Mefenamic Smoking: 0.5 PPD for 55 years Alcohol: negative (?) 4 Months Ago Abdominal pain: epigastric area
Case Discussion Splenic Abscess Personal Data Gender: male Birth Date: 1928/Mar/06th Allergy: Mefenamic Smoking: 0.5 PPD for 55 years Alcohol: negative (?) 4 Months Ago Abdominal pain: epigastric area
INJURIES CHEST, ABDOMEN, LIMBS. FN Brno November 2011
 INJURIES CHEST, ABDOMEN, LIMBS FN Brno November 2011 Injury Chest Abdomen Limbs Injury to the rib cage Fractured one or more ribs Sharp pain at the site of fracture Pain on taking a deep breath Shallow
INJURIES CHEST, ABDOMEN, LIMBS FN Brno November 2011 Injury Chest Abdomen Limbs Injury to the rib cage Fractured one or more ribs Sharp pain at the site of fracture Pain on taking a deep breath Shallow
Chapter 29 - Chest Injuries
 1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
1 2 3 4 5 6 7 8 9 National EMS Education Standard Competencies (1 of 5) Trauma Applies fundamental knowledge to provide basic emergency care and transportation based on assessment findings for an acutely
Chapter 24 - Abdominal_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 24.1 Define key terms introduced in this chapter. 13, 15, 18, 20 22 24.2 Describe the location, structure, and function of the organs in the abdominal
Introduction to Emergency Medical Care 1 OBJECTIVES 24.1 Define key terms introduced in this chapter. 13, 15, 18, 20 22 24.2 Describe the location, structure, and function of the organs in the abdominal
Lecture 56 Kidney and Urinary System
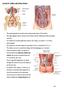 Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Lecture 56 Kidney and Urinary System The adrenal glands are located on the superomedial aspect of the kidney The right diagram shows a picture of the kidney with the abdominal walls and organs removed
Pelvic fractures. Dr Raymond Yean, MBBS Surgical SRMO
 Pelvic fractures Dr Raymond Yean, MBBS Surgical SRMO PELVIC FRACTURES Pelvic fracture account for 2-8% all skeletal injuries Associated with High energy trauma Soft tissue injuries and blood loss. Shock,
Pelvic fractures Dr Raymond Yean, MBBS Surgical SRMO PELVIC FRACTURES Pelvic fracture account for 2-8% all skeletal injuries Associated with High energy trauma Soft tissue injuries and blood loss. Shock,
Focused History and Physical Examination of the
 Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Henry: EMT Prehospital Care, Revised 3 rd Edition Lecture Notes Chapter 10: Focused History and Physical Examination of Trauma Patients Chapter 10 Focused History and Physical Examination of the Trauma
Imaging abdominal vascular emergencies. V.Stoynova
 Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Imaging abdominal vascular emergencies V.Stoynova Abdominal vessels V. Stoynova 2 Acute liver bleeding trauma anticoagulant therapy liver disease : HCC, adenoma, meta, FNH, Hemangioma Diagnosis :CT angiography
Chapter 29 - Chest_and_Abdominal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Introduction to Emergency Medical Care 1 OBJECTIVES 29.1 Define key terms introduced in this chapter. Slides 11, 15, 18, 27 29.2 Describe mechanisms of injury commonly associated with chest injuries. Slides
Penetrating Neck Injuries. Jason Levine MD Lutheran Medical Center July 22, 2010
 Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
Penetrating Neck Injuries Jason Levine MD Lutheran Medical Center July 22, 2010 CASE PRESENTATION 19 YO M 3 Stab Wounds Right zone I neck SW 2 SW anterior abdomen Left epigastrium anterior axillary line
ASSESSING THE PLAIN ABDOMINAL RADIOGRAPH M A A M E F O S U A A M P O F O
 ASSESSING THE PLAIN ABDOMINAL RADIOGRAPH M A A M E F O S U A A M P O F O Introduction The abdomen (less formally called the belly, stomach, is that part of the body between the thorax (chest) and pelvis,
ASSESSING THE PLAIN ABDOMINAL RADIOGRAPH M A A M E F O S U A A M P O F O Introduction The abdomen (less formally called the belly, stomach, is that part of the body between the thorax (chest) and pelvis,
Duodenum retroperitoneal
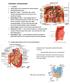 Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Duodenum retroperitoneal C shaped Initial region out of stomach into small intestine RETROperitoneal viscus Superior 1 st part duodenal cap ; moves upwards and backwards to lie on the R crura medial to
Exploring Anatomy: the Human Abdomen
 Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Exploring Anatomy: the Human Abdomen PERITONEUM AND PERITONEAL CAVITY PERITONEUM The peritoneum is a thin serous membrane that lines the abdominal cavity and covers, in variable amounts, the viscera within
Biology Human Anatomy Abdominal and Pelvic Cavities
 Biology 351 - Human Anatomy Abdominal and Pelvic Cavities You must answer all questions on this exam. Because statistics demonstrate that, on average, between 2-5 questions on every 100-point exam are
Biology 351 - Human Anatomy Abdominal and Pelvic Cavities You must answer all questions on this exam. Because statistics demonstrate that, on average, between 2-5 questions on every 100-point exam are
ABDOMINAL TRAUMA MODULE
 INTRODUCTION ABDOMINAL TRAUMA MODULE Blunt abdominal trauma most commonly occurs in the setting of motor vehicle accidents, pedestrian related trauma, direct blows and falls. 1 In these situations, blunt
INTRODUCTION ABDOMINAL TRAUMA MODULE Blunt abdominal trauma most commonly occurs in the setting of motor vehicle accidents, pedestrian related trauma, direct blows and falls. 1 In these situations, blunt
I have no financial disclosures.
 In the Belly of the Whale: Surviving Thoracoabdominal Trauma Debra Esernio Jenssen, MD, FAAP I have no financial disclosures. Objectives Review epidemiology of abusive chest and abdominal trauma. Identify
In the Belly of the Whale: Surviving Thoracoabdominal Trauma Debra Esernio Jenssen, MD, FAAP I have no financial disclosures. Objectives Review epidemiology of abusive chest and abdominal trauma. Identify
Chapter 13. Injuries to the Thorax and Abdomen
 Chapter 13 Injuries to the Thorax and Abdomen Anatomy Review Thoracic cage has 12 pairs of ribs. The first 7 pairs connect directly to sternum. Pairs 8 through 10 connect via common costal cartilage. Pairs
Chapter 13 Injuries to the Thorax and Abdomen Anatomy Review Thoracic cage has 12 pairs of ribs. The first 7 pairs connect directly to sternum. Pairs 8 through 10 connect via common costal cartilage. Pairs
IMAGING OF BLUNT ABDOMINAL TRAUMA, PART I
 IMAGING OF BLUNT ABDOMINAL TRAUMA, PART I QuickTime and a TIFF (Uncompressed) decompressor are needed to see this picture. Ruedi F. Thoeni, M. D. D University of California, San Francisco SCBT-MR Summer
IMAGING OF BLUNT ABDOMINAL TRAUMA, PART I QuickTime and a TIFF (Uncompressed) decompressor are needed to see this picture. Ruedi F. Thoeni, M. D. D University of California, San Francisco SCBT-MR Summer
Child as a victim of injury. Maciej Dudkiewicz M.D. Ph.D. Dpt of Anaesthesia and Intensive Care Medical University of Lodz
 Child as a victim of injury Maciej Dudkiewicz M.D. Ph.D. Dpt of Anaesthesia and Intensive Care Medical University of Lodz Epidemiology Trauma is most common cause of mortality and morbidity in the US pediatric
Child as a victim of injury Maciej Dudkiewicz M.D. Ph.D. Dpt of Anaesthesia and Intensive Care Medical University of Lodz Epidemiology Trauma is most common cause of mortality and morbidity in the US pediatric
PRACTICE GUIDELINE TITLE: NON-OPERATIVE MANAGEMENT OF LIVER / SPLENIC INJURIES
 PRACTICE GUIDELINE Effective Date: 6-18-04 Manual Reference: Deaconess Trauma Services TITLE: N-OPERATIVE MANAGEMENT OF LIVER / SPLENIC INJURIES PURPOSE: To define when non-operative management of liver
PRACTICE GUIDELINE Effective Date: 6-18-04 Manual Reference: Deaconess Trauma Services TITLE: N-OPERATIVE MANAGEMENT OF LIVER / SPLENIC INJURIES PURPOSE: To define when non-operative management of liver
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal injuries clinical presentation of, 23 24 Abdominal trauma evaluation for pediatric surgeon, 59 74 background of, 60 colon and
Index Note: Page numbers of article titles are in boldface type. A Abdominal injuries clinical presentation of, 23 24 Abdominal trauma evaluation for pediatric surgeon, 59 74 background of, 60 colon and
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS. December 19, 2012
 PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
PEDIATRIC TRAUMA I: ABDOMINAL TRAUMA BURNS Niel F. Miele,, M.D. December 19, 2012 EPIDEMIOLOGY Major Trauma responsible for
Urinary tract embolization
 Beograd, 14.10.2012 Urinary tract embolization asist. Peter Popovič, MD, MSc Head of abdominal radiology department, Institute of Radiology, UMC Ljubljana Embolization Who and when procedure: local/general
Beograd, 14.10.2012 Urinary tract embolization asist. Peter Popovič, MD, MSc Head of abdominal radiology department, Institute of Radiology, UMC Ljubljana Embolization Who and when procedure: local/general
Urinary 1 Checklist Gross Anatomy of the Urinary System
 Urinary 1 Checklist Gross Anatomy of the Urinary System Urinary system Kidneys Parietal peritoneum Retroperitoneal Renal fascia The urinary system consists of two kidneys, two ureters, the urinary bladder,
Urinary 1 Checklist Gross Anatomy of the Urinary System Urinary system Kidneys Parietal peritoneum Retroperitoneal Renal fascia The urinary system consists of two kidneys, two ureters, the urinary bladder,
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol
 Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
Focused Assessment Sonography of Trauma (FAST) Scanning Protocol Romolo Gaspari CHAPTER 3 GOAL OF THE FAST EXAM Demonstrate free fluid in abdomen, pleural space, or pericardial space. EMERGENCY ULTRASOUND
SAS Journal of Surgery ISSN SAS J. Surg., Volume-2; Issue-1 (Jan-Feb, 2016); p Available online at
 SAS Journal of Surgery ISSN 2454-5104 SAS J. Surg., Volume-2; Issue-1 (Jan-Feb, 2016); p-53-59 Available online at http://sassociety.com/sasjs/ Original Research Article Clinical Study, Evaluation and
SAS Journal of Surgery ISSN 2454-5104 SAS J. Surg., Volume-2; Issue-1 (Jan-Feb, 2016); p-53-59 Available online at http://sassociety.com/sasjs/ Original Research Article Clinical Study, Evaluation and
Thoracic Trauma: 5/19/2010. Keihan Golshani, MD, Assistant Professor of emergency Medicine, Isfahan Medical University,
 Thoracic Trauma: 1 Thoracic trauma: A significant cause of mortality. Many patients with thoracic trauma: die after reaching the hospital Many of them can be prevented by: Prompt diagnosis and treatment.
Thoracic Trauma: 1 Thoracic trauma: A significant cause of mortality. Many patients with thoracic trauma: die after reaching the hospital Many of them can be prevented by: Prompt diagnosis and treatment.
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN
 CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
CT Imaging of Blunt and Penetrating Vascular Trauma DENNIS FOLEY MEDICAL COLLEGE WISCONSIN THORACO ABDOMINAL TRAUMA 0 10 20 30 40 50 60 5 cc/sec 30 secs 1.25 mm/ 55 mm Z1.375 2.5 mm/ 55 mm Z 1.375 Grade
We have reviewed this material in accordance with U.S. Copyright Law and have tried to maximize your ability to
 Author(s): Patrick Carter, Daniel Wachter, Rockefeller Oteng, Carl Seger, 2009-2010. License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
Author(s): Patrick Carter, Daniel Wachter, Rockefeller Oteng, Carl Seger, 2009-2010. License: Unless otherwise noted, this material is made available under the terms of the Creative Commons Attribution
The abdominal Esophagus, Stomach and the Duodenum. Prof. Oluwadiya KS
 The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
The abdominal Esophagus, Stomach and the Duodenum Prof. Oluwadiya KS www.oluwadiya.com Viscera of the abdomen Abdominal esophagus: Terminal part of the esophagus The stomach Intestines: Small and Large
Kinetic Energy Energy in Motion KE = Mass (weight) X Velocity (speed)² 2 Double Weight = Energy Double Speed = Energy IS THE GREATEST DETERMINANT
 1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
1 Chapter 17 Blunt Trauma 2 Introduction to Blunt Trauma Most common cause of trauma death and disability exchange between an object and the human body, without intrusion through the skin 3 Blunt trauma
Genitourinary Tract Injuries
 Genitourinary Tract Injuries Chapter 18 Genitourinary Tract Injuries Introduction Genitourinary injuries constitute approximately 5% of the total injuries encountered in combat. Their treatment adheres
Genitourinary Tract Injuries Chapter 18 Genitourinary Tract Injuries Introduction Genitourinary injuries constitute approximately 5% of the total injuries encountered in combat. Their treatment adheres
MANAGEMENT OF SOLID ORGAN INJURIES
 MANAGEMENT OF SOLID ORGAN INJURIES Joseph Cuschieri, MD FACS Professor of Surgery, University of Washington Director of Surgical Critical Care, Harborview Medical Center Introduction Solid organ injury
MANAGEMENT OF SOLID ORGAN INJURIES Joseph Cuschieri, MD FACS Professor of Surgery, University of Washington Director of Surgical Critical Care, Harborview Medical Center Introduction Solid organ injury
Traumatic Renocaval Fistula With Pseudoaneurysm Leading To Renal Atrophy
 ISPUB.COM The Internet Journal of Radiology Volume 6 Number 2 Traumatic Renocaval Fistula With Pseudoaneurysm Leading To Renal Atrophy M Kukkady, A Deena, S Raj, Ramachandra Citation M Kukkady, A Deena,
ISPUB.COM The Internet Journal of Radiology Volume 6 Number 2 Traumatic Renocaval Fistula With Pseudoaneurysm Leading To Renal Atrophy M Kukkady, A Deena, S Raj, Ramachandra Citation M Kukkady, A Deena,
Damage Control in Abdominal and Pelvic Injuries
 Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
Damage Control in Abdominal and Pelvic Injuries Raul Coimbra, MD, PhD, FACS The Monroe E. Trout Professor of Surgery Surgeon-in Chief UCSD Medical Center Hillcrest Campus Executive Vice-Chairman Department
European Resuscitation Council
 European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
European Resuscitation Council Incidence of Trauma in Childhood Leading cause of death and disability in children older than one year all over the world Structured approach Primary survey and resuscitation
You Are the Emergency Medical Responder
 Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
Lesson 32: Injuries to the Chest, Abdomen and Genitalia You Are the Emergency Medical Responder Your police unit responds to a call in a part of town plagued by violence. When you arrive, you find the
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3. October 16, 2015
 STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 16, 2015 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
STRUCTURAL BASIS OF MEDICAL PRACTICE EXAMINATION 3 October 16, 2015 PART l. Answer in the space provided. (12 pts) 1. Identify the structures. (2 pts) A. B. A B C. D. C D 2. Identify the structures. (2
Guido Barbagli. Center for Reconstructive ti Urethral lsurgery
 Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Guido Barbagli Center for Reconstructive ti Urethral lsurgery Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it Dedicated to Ruggero Lenzi, teacher and friend. His passing was a great
Center for Reconstructive Urethral Surgery Guido Barbagli Center for Reconstructive Urethral Surgery Arezzo - Italy
 Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
Guido Barbagli Arezzo - Italy E-mail: guido@rdn.it Website: www.urethralcenter.it 23 rd ANNUAL EAU CONGRESS Sub-plenary Session on Male urinary incontinence 26 29 March 2008 Milan Italy Incontinence following
Penetrating Trauma in Pediatric Patients. Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017
 Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Penetrating Trauma in Pediatric Patients Heidi P. Cordi, MD, MPH, MS, EMTP, FACEP, FAADM EMS WEEK 2017 Introduction Trauma is the leading cause of death between ages of 1-18 years Penetrating injury accounts
Esophageal Perforation
 Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal Perforation Dr. Carmine Simone Thoracic Surgeon, Division of General Surgery Head, Division of Critical Care May 15, 2006 Overview Case presentation Radiology Pre-operative management Operative
Esophageal injuries. 新光急診張志華醫師 Facebook.com/jack119
 Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Esophageal injuries 新光急診張志華醫師 Facebook.com/jack119 Pre-test 1 What is the most common cause of esophageal injuries? A. Traffic accidents B. Gunshot wounds C. Iatrogenic Pre-test 2 Which contrast agent
Gastrointestinal & Genitourinary Emergencies. Lesson Goal. Learning Objectives 9/10/2012
 Gastrointestinal & Genitourinary Emergencies Lesson Goal Recognize, assess & provide care to patients with abdominal cavity injuries Learning Objectives Discuss different causes of nontraumatic abdominal
Gastrointestinal & Genitourinary Emergencies Lesson Goal Recognize, assess & provide care to patients with abdominal cavity injuries Learning Objectives Discuss different causes of nontraumatic abdominal
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines
 Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Blunt Abdominal Trauma Evaluation and Management Guideline PEDIATRIC Practice Management Guideline Contact: Trauma Center
Trauma Center Practice Management Guideline Iowa Methodist Medical Center Des Moines Blunt Abdominal Trauma Evaluation and Management Guideline PEDIATRIC Practice Management Guideline Contact: Trauma Center
9/10/2012. Chapter 49. Learning Objectives. Learning Objectives (Cont d) Thoracic Trauma
 Chapter 49 Thoracic Trauma 1 Learning Objectives Explain relevance of thoracic injuries as part of the overall mortality rate from major trauma List thoracic injuries that may result in early death if
Chapter 49 Thoracic Trauma 1 Learning Objectives Explain relevance of thoracic injuries as part of the overall mortality rate from major trauma List thoracic injuries that may result in early death if
Case Report Delayed Presentation of Traumatic Intraperitoneal Rupture of Urinary Bladder
 Case Reports in Urology Volume 2012, Article ID 430746, 4 pages doi:10.1155/2012/430746 Case Report Delayed Presentation of Traumatic Intraperitoneal Rupture of Urinary Bladder Hazim H. Alhamzawi, 1 Husham
Case Reports in Urology Volume 2012, Article ID 430746, 4 pages doi:10.1155/2012/430746 Case Report Delayed Presentation of Traumatic Intraperitoneal Rupture of Urinary Bladder Hazim H. Alhamzawi, 1 Husham
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Pancreas & Biliary System. Dr. Vohra & Dr. Jamila
 Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
Pancreas & Biliary System Dr. Vohra & Dr. Jamila 1 Objectives At the end of the lecture, the student should be able to describe the: Location, surface anatomy, parts, relations & peritoneal reflection
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES
 JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
JOHN M UECKER, MD, FACS COMPLEX PANCREATICODUODENAL INJURIES THE PROBLEM DUODENAL / PANCREATIC INJURIES Difficult to diagnose Not very common Anatomic and physiologic challenges 90% rate of associated
Biology Human Anatomy Abdominal and Pelvic Cavities
 Biology 351 - Human Anatomy Abdominal and Pelvic Cavities Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics
Biology 351 - Human Anatomy Abdominal and Pelvic Cavities Please place your name and I.D. number on the back of the last page of this exam. You must answer all questions on this exam. Because statistics
Professional Development & Training MM3. Firefighter Prehospital Care Program. Maintenance Module 3 Course Mill Version
 Professional Development & Training MM3 Firefighter Prehospital Care Program F T Maintenance Module 3 Course Mill Version S Objectives Upon successful completion of the Firefighter Prehospital Care Maintenance
Professional Development & Training MM3 Firefighter Prehospital Care Program F T Maintenance Module 3 Course Mill Version S Objectives Upon successful completion of the Firefighter Prehospital Care Maintenance
CHEST TRAUMA. Dr Naeem Zia FCPS,FACS,FRCS
 CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
CHEST TRAUMA Dr Naeem Zia FCPS,FACS,FRCS Learning objectives Anatomy of chest wall and thoracic viscera Physiology of respiration and nerve pathways for pain Enumerate different thoracic conditions requiring
