First described by Conn in 1955, primary aldosteronism is. Clinicopathologic Correlates of Primary Aldosteronism
|
|
|
- Herbert Wright
- 6 years ago
- Views:
Transcription
1 Clinicopathologic Correlates of Primary Aldosteronism Primary aldosteronism is the most common cause of secondary hypertension, incurring significant cardiovascular morbidity and mortality. Our understanding of this disease has evolved substantially during the past decade. Recently, the molecular basis of primary aldosteronism has begun to be unraveled, with the discovery of mutations in potassium channel (KCNJ5), ATPases (ATP1A1, ATP2B3), and calcium channel (CACNA1D), and aberrant Wnt/bcatenin signaling. The most recent data suggest that 95% of cases are sporadic, whereas 5% of cases are hereditary. Pathologic correlates of primary aldosteronism include adrenal cortical hyperplasia, adenoma, and carcinoma. Although the most common clinical presentation is bilateral adrenal cortical hyperplasia, this entity is usually treated medically. Therefore, in the setting of primary aldosteronism, surgical pathologists are most commonly exposed to adrenocortical adenomas and the odd occasional carcinoma. This review provides an update on the current knowledge of primary aldosteronism and discusses the clinicopathologic correlations of this important disease. (Arch Pathol Lab Med. 2015;139: ; doi: / arpa rs) First described by Conn in 1955, primary aldosteronism is defined as a group of disorders in which aldosterone production is inappropriately elevated, relatively independent from the renin-angiotensin system, and nonsuppressible by sodium loading. 1 4 Our understanding of this disease has evolved drastically in the last decade with the advent of biochemical screening using plasma aldosterone to renin ratio (ARR). 1 7 Previously thought to be a rare and relatively benign cause of hypertension, primary aldosteronism is currently recognized as the leading cause of secondary hypertension, with a prevalence of 5% to 13% among hypertensive adults. 1 5 Furthermore, it incurs significant cardiovascular morbidity and mortality, which are specific to aldosterone itself. 1 5 Pathologic correlates of primary aldosteronism include adrenal cortical hyperplasia, adenoma, and carcinoma. The Accepted for publication June 24, From the Department of Pathology, University Health Network, and the Department of Laboratory Medicine and Pathobiology, University of Toronto, Toronto, Ontario, Canada. The authors have no relevant financial interest in the products or companies described in this article. Reprints: Ozgur Mete, MD, Department of Pathology, University Health Network, 200 Elizabeth St, 11th Floor, Toronto, ON M5G 2C4, Canada ( ozgur.mete2@uhn.ca). Kai Duan, MD; Ozgur Mete, MD diagnostic features of these entities have been refined during the past decade with the advent of modern imaging, biochemical testing, and molecular pathology Primary aldosteronism is now known to comprise both sporadic (95%) and familial (5%) forms. 11 Bilateral adrenal hyperplasia (idiopathic hyperaldosteronism) accounts for 65% of sporadic cases of primary aldosteronism. 1 4 With the advent of adrenal vein sampling, these lesions are almost never encountered in surgical pathology, because virtually all of the cases are treated medically. 12,13 Rare cases of unilateral adrenal hyperplasia causing primary aldosteronism (2%) have been reported to benefit from surgical treatment 1 4,7 ; however, the spectrum of morphologic changes in this context has not been extensively described. Aldosteroneproducing adrenal cortical adenoma accounts for the remaining 30% of sporadic cases 1 7 and is the most commonly encountered aldosterone-producing lesion in surgical pathology practice. Adrenocortical carcinoma has also been reported in 1% of cases of sporadic primary aldosteronism. 1 7 CLINICAL AND LABORATORY FEATURES In clinical practice, primary aldosteronism is equally reported in both sexes, with a peak incidence between ages 30 and 60 years; it is rarely seen in children. 1 4 Normokalemic hypertension is the most common presentation, with hypokalemia present only in severe cases. 1 5 Unlike patients with Cushing syndrome or adrenogenital syndrome, most patients with primary aldosteronism are usually asymptomatic and do not harbor any specific physical findings. 1 5 Occasionally, some patients with marked hypokalemia may have symptoms such as muscle weakness and cramping, headaches, palpitations, polydipsia, polyuria, nocturia, or a combination of these. 1 4 Primary aldosteronism is a laboratory diagnosis. The vast majority of cases are detected during routine biochemical screening of population groups with higher reported rates of primary aldosteronism. 1 5 These include patients with refractory hypertension, hypokalemia, suggestive family history, or an incidentally detected adrenal mass. 1 5 The current gold standard screening test is the plasma ARR. 1 5 The most commonly adopted cutoff value of ARR is 30 ng/dl per ng/ ml per hour (or 750 pmol/l per ng/ml per hour). 1 When the ARR value is higher than the cutoff, the diagnosis of primary aldosteronism is confirmed or excluded by an aldosterone suppression test. The most widely used confirmatory tests are intravenous saline loading, oral sodium loading, fludrocortisone suppression, and captopril challenge test. 1 5 Occasionally, primary aldosteronism is diagnosed as part of the workup for an incidentaloma, in which case special attention should be given to the biochemical results of an overnight 948 Arch Pathol Lab Med Vol 139, July 2015 Primary Aldosteronism Duan & Mete
2 Overview of Familial Hyperaldosteronism (FH) a FH Type Inheritance Associated Gene Clinical Features Pathologic Features FH-I Autosomal dominant CYP11B1, CYP11B2 Early onset (often before age 20 y), resistant hypertension, mostly normokalemic, complete aldosterone response to dexamethasone FH-II Autosomal dominant; undetermined in some cases Unknown; linked to 7p22 Clinical features indistinguishable from sporadic primary aldosteronism: onset in adulthood, resistant hypertension, mostly normokalemic FH-III Autosomal dominant KCNJ5 Very early onset (childhood), severely resistant hypertension, hypokalemia, very high aldosterone concentrations (2 10 times normal concentrations) a Data derived from Bar-lev and Annes, 6 Zennaro et al, 8 Scholl and Lifton, 10 and Mulatero et al. 11 Normal adrenal glands; occasional adrenal cortical nodular disease or bilateral hyperplasia Adrenal cortical adenoma or bilateral hyperplasia Marked bilateral adrenal hyperplasia; occasional normal adrenal glands dexamethasone suppression test and 24-hour urinary measurement of fractionated metanephrines and catecholamines, to exclude Cushing or subclinical Cushing syndrome and pheochromocytoma. 14 In sporadic primary aldosteronism, some clinical and laboratory features are distinctive of hyperplasia (idiopathic hyperaldosteronism), adenoma, or carcinoma. 1 4,7 Primary aldosteronism caused by adrenal cortical hyperplasia usually presents in older individuals, has a predominance among males, is more often normokalemic, and has less severe hypertension. 1 4,7 By contrast, aldosterone-producing adenomas usually appear at an earlier age, occur more often in females, and are more often associated with hypokalemia and severe hypertension. 1 4,7 When primary aldosteronism is caused by an adrenocortical carcinoma, it usually presents with much more profound hypokalemia, very high aldosterone concentrations, and in some cases concurrent cortisol and/or sex-steroid production, leading to Cushing syndrome or virilization. 7,15,16 Three types of familial primary aldosteronism have also been identified all are inherited in an autosomaldominant manner (Table) Familial hyperaldosteronism type I, also known as glucocorticoid-remediable aldosteronism, has been attributed to less than 1% of cases of primary aldosteronism and is caused by a recombination between the CYP11B2 and CYP11B1 genes. 11 Familial hyperaldosteronism type II is responsible for 3% to 5% of cases of primary aldosteronism and has been linked to 7p22, although no specific gene has been identified to date Familial hyperaldosteronism type III is a more recent discovery and has been found in less than 1% of cases, involving mutations in a potassium channel (KCNJ5). 11 Hereditary forms of primary aldosteronism typically manifest more florid symptoms, with the exception of familial hyperaldosteronism type II, which is clinically and biochemically indistinguishable from sporadic cases. 6,11 Familial hyperaldosteronism type II is usually only diagnosed when at least two first-degree members of the same family have confirmed primary aldosteronism and after familial hyperaldosteronism types I and III have been excluded. 6,11 Most individuals with familial hyperaldosteronism type I develop severe hypertension early in life (before the age of 20 years) and display high rates of morbidity and mortality from cerebrovascular events, although milder clinical phenotypes have also been reported. 11 A defining feature of familial hyperaldosteronism type I is that administration of exogenous glucocorticoids reverses the state of mineralocorticoid excess. 1 5 Individuals with familial hyperaldosteronism type III typically develop an early-onset and particularly severe form of primary aldosteronism, with very high aldosterone concentrations (2 10 times normal concentrations), marked hypokalemia, and severe hypertension resistant to medical therapy. 11 RADIOLOGIC FEATURES Once primary aldosteronism is confirmed biochemically, radiologic investigations provide a preliminary method for localization and subtyping of aldosterone-producing lesions. Adrenal computed tomography (CT) scan is the initial modality of choice. 1 4,17,18 The findings on CT for adrenal hyperplasia are usually nonspecific, showing either enlarged or normal-size adrenal glands. 7 Adrenal adenomas usually appear homogeneous, round, and small, with smooth borders and well-delineated margins (Figure 1, A). 14,17,18 Radiologic features of tumors suspicious for adrenocortical carcinoma include larger size (.4 cm), irregular margins, inhomogeneous contents, and areas of necrosis, hemorrhage, and calcification. 1 4,14,17,18 Because of the fact that adenomas often have intracytoplasmic fat, resulting in lower attenuation, measurement of the attenuation value in Hounsfield units is helpful in distinguishing adenomas from nonadenomas 14,18 ; tumors with attenuation values of less than 10 Hounsfield units on an unenhanced CT are often diagnostic of adrenocortical adenomas (Figure 1, A). 14,18 It is important to note, however, that CT cannot reliably visualize microadenomas or hyperplasia, or determine the functional status of an adrenal cortical adenoma. 1 4,14,17,18 Given the limitations of adrenal CT scan, adrenal venous sampling has become the gold standard test to determine lateralization of the source of the excessive aldosterone secretion. 1 4,17 This method is also helpful in differentiating aldosterone-producing adenoma from bilateral adrenal hyperplasia. 17 After successful catheterization of both adrenal veins under interventional radiology, comparison of the aldosterone to cortisol ratio between both sides is the currently accepted criterion for determining unilateral versus bilateral disease. 17 This is also known as the lateralization index (aldosterone-to-cortisol ratio on the dominant side divided by the aldosterone-to-cortisol ratio on the nondominant side). Most investigators concur that a lateralization index of 4 or higher during cosyntropin stimulation (2 for unstimulated adrenal vein sampling) is indicative of unilateral aldosterone production and favors the diagnosis of aldosterone-producing adenoma, whereas a lateralization index lower than 4 is more suggestive of bilateral Arch Pathol Lab Med Vol 139, July 2015 Primary Aldosteronism Duan & Mete 949
3 Figure 1. Characteristics of aldosterone-producing adrenal cortical adenomas. Computed tomography (CT) scan identified a solitary, round, wellcircumscribed lesion with an attenuation value of less than 10 Hounsfield units on an unenhanced CT in a patient with primary aldosteronism (A). From a radiologic perspective, the findings were consistent with an adrenal cortical adenoma. Gross examination justified the presence of a welldefined mass showing a golden yellow appearance (B). The lesion did not show evidence of malignancy and consists of clear cells (C). The nontumorous adrenal cortex is not atrophic (B and C) but shows zona glomerulosa layer hyperplasia (arrows) characterized by a continuous and multilayered zona glomerulosa layer (D). The overall findings are diagnostic of an aldosterone-producing adrenal cortical adenoma (B through D). The presence of spironolactone bodies within an adrenal cortical adenoma provides another morphologic clue leading to recognition of aldosterone production if the patient is treated with spironolactone (E). The distinctive feature of spironolactone bodies is their concentric and lamellated patterns (E). Luxol fast blue stain can be used to distinguish these inclusions from other mimics because of their rich content of phospholipids (F) (hematoxylin-eosin, original magnifications [C], 310 [D], and 320 [E]; Luxol fast blue, original magnification 320 [F]). 950 Arch Pathol Lab Med Vol 139, July 2015 Primary Aldosteronism Duan & Mete
4 aldosterone production involving bilateral adrenal hyperplasia. 17 GROSS FEATURES The normal adult adrenal gland weighs 4 g at surgical excision, 12,15,16 with an average cortical thickness of almost 2 mm. 12 However, there may be variation from gland to gland or thicker areas in different parts of the same gland. 12 Grossly, adrenal gland with hyperplasia (idiopathic hyperaldosteronism) may appear unremarkable or show slight enlargement, with grossly visible micronodules or macronodules. 12,13 Aldosterone-producing adenomas often present with a round-to-ovoid unicentric neoplasm measuring a few centimeters in diameter. 12,13,15,16,19 Most adenomas are unilateral and solitary, but occasional bilateral adenomas have also been reported. 13,16,19 These tumors are often intraadrenal and unencapsulated, but some may also show a true capsule or a pseudocapsule. 12,15,16 The cut surface is classically described as homogenous, and golden yellow or canary yellow (Figure 1, B), and larger tumors may have areas of hemorrhage or cystic change. 12,13,15,16,19 Adrenocortical carcinomas usually weigh more than 100 g, and can measure from 3 to 40 cm 15,16 ; some are encapsulated, but many are adherent to or invade adjacent structures. 15,16 On slicing, they often show lobulation with fibrous bands and areas of necrosis and hemorrhage. 15,16 The gross features of familial hyperaldosteronism are scarcely reported in the literature. In type I, macroscopic examination usually reveals normal adrenal glands, although some cases showing adrenal cortical nodular disease and massive bilateral adrenal hyperplasia have been described. 11,20 In type II, gross examination can reveal either adrenal cortical adenoma or bilateral hyperplasia. 11 In type III, the adrenal glands show marked bilateral hyperplasia, which can be seen grossly, although normal adrenal glands have also been described in some families. 11 During the gross examination, particular attention should be given to the width of the cortex. 13,15,19,24 Even grossly, the identification of atrophy of the nontumorous adrenal cortex in a gland with a dominant cortical adenoma should prompt the attention of the surgical pathologist to determine whether the patient has been diagnosed with concurrent Cushing syndrome. If not, a timely call to the treating physician will prevent the unanticipated postoperative crisis of acute Addison disease. 21 HISTOPATHOLOGIC FEATURES The histopathologic correlates of primary aldosteronism include adrenal cortical hyperplasia, adenoma, and carcinoma. Although adrenal cortical hyperplasia is the most common clinical presentation, this entity rarely presents itself in surgical pathology, because most cases involve bilateral glands and are treated medically. 12,13 Although rare examples of unilateral adrenal cortical hyperplasia have been reported in patients with primary aldosteronism, the spectrum of morphologic changes has not been extensively defined in this setting. 1 7,12,13 Therefore, with the exception of paradoxic zona glomerulosa (ZG) hyperplasia, pathologists are most commonly exposed to adrenal cortical neoplasms, especially adenomas, from patients with primary aldosteronism. 12,13,15,16,19 On light microscopy, aldosterone-producing adrenal cortical adenomas appear partially or completely encapsulated, with a compressed fibrous rim or fibrous pseudocapsule at the expansile borders of the tumor (Figure 1, C). 12,15,16 Tumor cells often present in a nesting or alveolar pattern, as short cords, as blunt anastomosing trabeculae, or as mixtures of these architectural patterns. 12 The morphology of individual cells may be quite heterogeneous, with varying proportions of 4 different types of cells: clear cells resembling zona fasciculata cells, cells resembling ZG cells, compact cells indistinguishable from those of the zona reticularis, and a group of cells designated as hybrid cells with cytologic features of both zona fasciculata and ZG cells. 12,13,15,19 22 Lipid-rich clear cells usually predominate in these lesions, giving them a characteristic golden yellow color. 12,15,19,21,22 Similar to other endocrine lesions, oncocytic change has also been reported in the literature. 12,22 Some cases exhibit cytoplasmic eosinophilic globular inclusions, reflecting degenerated mitochondria. 22 Occasionally, the existence of a cortisol-producing adenoma may be missed by the clinician preoperatively. Although this may be due to an omission, a variant of aldosterone-producing adenoma with concurrent cortisol production has also been described. 23 The distinction between cortisol-producing adenoma and aldosteroneproducing adenoma can be made on hematoxylin-eosin stained slides by assessing the nontumorous adrenal cortex. 12,21,22 Cortisol-producing adrenal cortical adenomas are associated with atrophy of the nontumorous cortex due to the negative feedback suppression effect of the hypothalamic-pituitary axis. 12,13,21,22 Unlike glucocorticoid-producing adenomas, aldosteroneproducing cortical neoplasms are not associated with cortical atrophy, 12,13,15,19 22 and paradoxical ZG hyperplasia can be identified in the nontumorous adrenal cortex (Figure 1, D). 12,13,15,19 22 The ZG is composed of small angular cells with a high nuclear to cytoplasm ratio, dispersed focally below the capsule. In other words, the presence of a continuous ZG layer is a sign of hyperplasia. The presence of spironolactone bodies within an adrenal cortical adenoma provides another morphologic clue leading to recognition of aldosterone production. 12,15,19 22 These are described as intracytoplasmic eosinophilic inclusions following spironolactone treatment (Figure 1, E). 12,15,19 22 These inclusions are often small (2 12 lm), round to oval, and delineated from surrounding cytoplasm by a small, clear halo. 12 Red blood cells and other intracytoplasmic inclusions can sometimes mimic spironolactone bodies. Although a distinctive feature of spironolactone bodies is their concentric and lamellated pattern, Luxol fast blue stain can also be used to distinguish these inclusions from other mimickers because of their rich content of phospholipids (Figure 1, F). 12 Despite being a rare cause of primary aldosteronism, adrenocortical carcinoma must be excluded, particularly if a large tumor is found. 1 4,12,13,15,19 Histologic examination reveals a more disorganized architecture than in adenomas, with trabecular and diffuse patterns. 12,13,15,19,24 Nuclear pleomorphism and increased mitoses (.5 per 50 highpower fields), including atypical figures, are often present, along with capsular and/or vascular invasion in the vast majority of high-grade adrenocortical carcinomas. 12,13,15,19,24 However, making the distinction between a noninvasive low-grade adrenocortical carcinoma and adrenal cortical adenoma with atypical features can be challenging. Although many scoring schemes have been defined in this field, even the most commonly used Weiss scoring scheme carries significant interobserver variability, along with a gray zone when an adrenal cortical neoplasm receives a score of Arch Pathol Lab Med Vol 139, July 2015 Primary Aldosteronism Duan & Mete 951
5 Figure 2. Molecular biologic features of primary aldosteronism. In normal physiology, zona glomerulosa cells are typically hyperpolarized because of predominant potassium conductance, primarily mediated by K þ channels (A). Activation of the renin-angiotensin system leads to production of angiotensin II (AT2), which binds to type 1 angiotensin II receptor (AT2R) on the zona glomerulosa cells, inhibiting potassium currents and inducing cell membrane depolarization. This depolarization activates voltage-gated Ca 2þ channels: the influx of calcium and the activation of the calcium/calmodulin kinase pathway result in aldosterone synthesis (B). In primary aldosteronism, sporadic mutations arising in potassium channels (KCNJ5), calcium channels (CACNA1D), and ATPases (ATP1A1 and ATP2B3) account for approximately 60% of aldosterone-producing adenomas (C). Mutations in the KCNJ5 gene result in sodium permeability of the mutant K þ channel, causing cellular depolarization and subsequent calcium influx. In other cases, mutations in the ATP1A1 gene lead to loss of Na þ /K þ ATPase pump activity, resulting in cell membrane depolarization. Deletions in the ATP2B3 gene, encoding Ca 2þ ATPase, result in distortion of the Ca 2þ -binding site and affect intracellular calcium clearance. Somatic mutations in the CACNA1D gene, which encodes the voltage-gated Ca 2þ channel, cause channel activation at less depolarized potentials. 2 or 3. Recently, Volante et al 25 introduced a simplified approach by using the reticulin algorithm to define malignancy through an altered reticulin network associated with one of the following parameters: high mitotic rate (.5 mitoses per 50 high-power fields), vascular invasion, and necrosis. This method has subsequently been shown to have a high interobserver reproducibility. 26 Furthermore, insulinlike growth factor 2 and p53 overexpression, and a high amount of Ki-67 (.5%) have also been shown to be effective in differentiating carcinoma from adenoma. 15,16,24 ANCILLARY STUDIES The ultrastructural features of aldosterone-producing adenomas are unique. Aldosterone-producing cells contain mitochondria with lamella-type or platelike cristae, characteristic of ZG-type cells, whereas glucocorticoid-producing and nonfunctioning adenoma cells contain mitochondria with tubulovesicular cristae. 12,13,21,22 Furthermore, ultrastructural spironolactone bodies, consisting of a central core with amorphous, electron-dense material surrounded by multiple concentric membranes, are seen in aldosterone-producing adenoma. 12,13,21,22 Currently, immunohistochemical tests are not part of the routine histopathologic assessment of aldosterone-producing lesions, because most cases can be given a diagnosis using conventional histology in conjunction with biochemical evidence of primary aldosteronism. 12,13,15,19 22 In the past, some investigators have used positive P450(c17) and 3b-hydroxysteroid dehydrogenase immunostaining as evidence of steroid production in aldosterone-producing cells, although these also stain positive in cortisol-producing cells. 13,27,28 Recently, two studies concurrently described the use of a novel immunostain, CYP11B2, to confirm the production of aldosterone and the histopathologic diagnosis of primary aldosteronism. 27,28 CYP11B2 is a key enzyme for aldosterone synthesis, and positive staining for CYP11B2 is indicative of cells producing aldosterone in both tumor and in the ZG of adjacent tissue. 27,28 Occasionally, when there is a need to distinguish an adrenal cortical adenoma from another tumor, one can confirm the adrenal cortical origin by demonstrating positivity for universal markers of adrenal cortical cytodifferentiation, including steroidogenic factor-1, Melan-A (clone A103), calretinin, synaptophysin, and a- inhibin. PATHOGENESIS AND MOLECULAR BIOLOGIC FEATURES In normal physiology, aldosterone is secreted by the adrenal cortex in response to hyperkalemia and angiotensin II. 6,8 10 The responsive cells are typically hyperpolarized because of predominant K þ conductance, which is primarily mediated by K þ channels. 6,8 10 Activation of the reninangiotensin system leads to the production of angiotensin II, which binds to type 1 angiotensin II receptor, inhibiting potassium currents and inducing cell membrane depolarization (Figure 2, A and B). 6,8 10 Depolarization subsequently activates low-voltage activated calcium channels, leading to calcium influx. 6,8 10 The resulting activation of the calcium/ calmodulin kinase pathway leads to increased production of rate-limiting enzymes for aldosterone synthesis. In addition to this acute effect, chronic Ca 2þ signaling also stimulates ZG proliferation. 6,8 10 The molecular mechanism underlying autonomous aldosterone production from the adrenal cortex has only begun to be unraveled recently Primary aldosteronism occurs in a number of familial syndromes. The causal genes underlying two hereditary forms of primary aldosteronism have been identified. 5,6,8,10,11 These include rearrangement of CYP11B1/CYP11B2 genes in type I familial hyperaldosteronism, and germ line mutations in KCNJ5 (T158A and G151R) in type III familial hyperaldosteronism (Figure 2, C). 952 Arch Pathol Lab Med Vol 139, July 2015 Primary Aldosteronism Duan & Mete
6 Although the causal gene underlying type II familial hyperaldosteronism has not yet been identified, some reports have linked it to chromosome 7p22. 5,6,8,10,11 During the past 2 years, considerable interest has been generated by the discovery of sporadic mutations in potassium channels (KCNJ5), calcium channels (CACNA1D), and ATPases (ATP1A1 and ATP2B3; Figure 2, C). Together, these 4 mutations account for approximately 60% of aldosterone-producing adenomas KCNJ5 encodes Kir3.4, an inward rectifier potassium channel in ZG layer cells Two common somatic gain-of-function mutations (G151R and L168R) located in or close to the KCNJ5 selectivity filter have been reported in 40% of aldosteroneproducing adenomas The mechanism underlying aldosterone production and cell proliferation is the sodium permeability of the mutant KCNJ5 channel, causing cellular depolarization and calcium influx through voltage-gated calcium channels Recently, a lower expression of the KCNK5 gene encoding Twik-related Acid-sensitive K þ channels 2 (TASK2) has also been described in aldosterone-producing adenomas and was shown to increase production of aldosterone in vitro. 33 Some investigators suggested that KCNJ5 mutations are more prevalent in aldosterone-producing adenomas resembling clear cells of the zona fasciculata but are absent in a subset of aldosterone-producing adenomas resembling small angular cells of the ZG cells. 30 Exon sequencing of the latter group identified somatic mutations in either ATP1A1 or CAC- NA1D, which could suggest a common subtype of aldosterone-producing adenoma. 30 Many adenomas harboring these mutations were less than 1 cm in diameter and had been overlooked on conventional adrenal imaging. 30 ATP1A1 (encoding Na þ /K þ ATPase a subunit) and ATP2B3 (encoding Ca 2þ ATPase) play an important role in the regulation of aldosterone production by maintaining cell membrane potential. 30,31 Mutations in the Na þ /K þ ATPase a subunit lead to a loss of pump activity and reduced affinity for K þ (Figure 2, C). 30,31 Deletions in ATP2B3 are inferred to cause distortion of the Ca 2þ -binding site and to affect intracellular calcium clearance (Figure 2, C). 30,31 Another study identified somatic mutations (Gly403 and Ile770) in the CACNA1D gene, which encodes a voltage-gated calcium channel (Ca v 1.3; Figure 2, C). 30,32 The altered residues cause channel activation at less depolarized potentials. Gl403 alterations also impair channel inactivation. 30,32 These effects are inferred to cause increased Ca 2þ influx, which in turn stimulates aldosterone production and cell proliferation. 30,32 In the adrenal gland, dysregulation of the Wnt/b-catenin signaling pathways has already been reported in the development of micronodular and macronodular hyperplasia and adrenocortical neoplasms. 24,30,34 Recently, a study has shown that Wnt/b-catenin signaling is aberrantly activated in 70% of aldosterone-producing adenomas in a series of 47 patients. 34 This study also provides further evidence that decreased expression of the Wnt inhibitor SFRP2 may be contributing to dysregulated Wnt signaling and aldosterone-producing adenoma development in some patients. 34 TREATMENT AND PROGNOSIS Unilateral laparoscopic adrenalectomy is currently the gold standard for treatment of aldosterone-producing adenomas and often results in improved blood pressure and serum concentrations postoperatively. 1 5 In bilateral adrenal hyperplasia (idiopathic hyperaldosteronism), the preferred treatment is usually pharmacologic, using mineralocorticoid antagonists. 1 4 Although spironolactone is still recommended as the primary agent, eplerenone has been described as an alternative option. 1 In rare cases of unilateral adrenal hyperplasia, unilateral adrenalectomy has been shown to be beneficial, although the long-term outcome of surgery has not been extensively reported. 1 5 Aldosterone-producing adrenocortical carcinoma is treated similarly to other adrenocortical carcinomas, with surgical resection and adjuvant mitotane treatment. 4,35 The guidelines for the testing of familial hyperaldosteronism have not been firmly established. 1 7,11 Currently, only screening for familial hyperaldosteronism type I has been recommended in patients with early onset of primary aldosteronism and those with a family history of primary aldosteronism or stroke at a young age. 1 The initial treatment for familial hyperaldosteronism type I consists of low-dose dexamethasone; spironolactone or amiloride may also be considered if treatment with glucocorticoid does not normalize blood pressure. 1 4 CONCLUSION Despite emerging evidence using genomic sequencing, there is still much debate regarding the molecular mechanisms leading to hyperaldosteronism, cell proliferation, and tumor formation. Pathologic correlates of primary aldosteronism include adrenal cortical hyperplasia, adenoma, and carcinoma. Although each aldosterone-producing lesion possesses particular clinical, laboratory, and radiologic findings, preoperative subtyping may be difficult in some cases. Therefore, it is important for the practicing pathologist to recognize the spectrum of primary aldosteronism and differentiate aldosterone-producing adrenal cortical adenoma from hyperplasia and carcinoma, because it is of tremendous importance for management. References 1. Funder J, Carey R, Fardella C, et al. Case detection, diagnosis, and treatment of patients with primary aldosteronism: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab. 2008;93: Young WF. Primary aldosteronism: renaissance of a syndrome. Clin Endocrinol (Oxf). 2007;66(5): Mattsson C, Young WF. Primary aldosteronism: diagnostic and treatment strategies. Nat Clin Pract Nephrol. 2006;2(4): Schirpenbach C, Reincke M. Primary aldosteronism: current knowledge and controversies in Conn s syndrome. Nat Clin Pract Endocrinol Metab. 2007; 3(3): Funder JW. The genetic basis of primary aldosteronism. Curr Hypertens Rep. 2012;14(2): Bar-lev A, Annes JP. Genetics of adrenocortical disease: an update. Curr Opin Endocrinol Diabetes Obes. 2012;19(3): Ganguly A. Primary aldosteronism. N Engl J Med. 1998;339(25): Zennaro MC, Rickard AJ, Boulkroun S. Genetics of mineralocorticoid excess: an update for clinicians. Eur J Endocrinol. 2013;169(1):R15 R Gomez-Sanchez CE, Oki K. Minireview: potassium channels and aldosterone dysregulation: is primary aldosteronism a potassium channelopathy? Endocrinology. 2014;155(1): Scholl UI, Lifton RP. New insights into aldosterone-producing adenomas and hereditary aldosteronism: mutations in the K þ channel KCNJ5. Curr Opin Nephrol Hypertens. 2013;22(2): Mulatero P, Monticone S, Rainey WE, Veglio F, Williams TA. Role of KCNJ5 in familial and sporadic primary aldosteronism. Nat Rev Endocrinol. 2013;9(2): Lack EE. Tumors of the Adrenal Glands and Extraadrenal Paraganglia. Washington, DC: ARP Press; Atlas of Tumor Pathology; 4th series, fascicle Sasano H. The adrenal cortex. In Stefaneanu L, Sasano H, Kovacs K, eds. Molecular and Cellular Endocrine Pathology. London, England: Arnold; 2000: Young WF. Clinical practice: the incidentally discovered adrenal mass. N Engl J Med. 2007;356(6): Arch Pathol Lab Med Vol 139, July 2015 Primary Aldosteronism Duan & Mete 953
7 15. McNicol AM. Update on tumours of the adrenal cortex, phaeochromocytoma and extra-adrenal paraganglioma. Histopathology. 2011;58(2): McNicol AM. Lesions of the adrenal cortex. Arch Pathol Lab Med. 2008; 132(8): Sacks BA, Brook OR, Brennan IM. Adrenal venous sampling: promises and pitfalls. Curr Opin Endocrinol Diabetes Obes. 2013;20(3): Ilias I, Sahdev A, Reznek RH, Grossman AB, Pacak K. The optimal imaging of adrenal tumours: a comparison of different methods. Endocr Relat Cancer. 2007;14(3): DeLellis RA, ed. Pathology & Genetics: Tumours of Endocrine Organs. Vol 8. Lyon, France: IARC Press; Velarde-Miranda C, Gomez-Sanchez EP, Gomez-Sanchez CE. Regulation of aldosterone biosynthesis by the Kir3.4 (KCNJ5) potassium channel. Clin Exp Pharmacol Physiol. 2013;40: Mete O, Asa SL. Morphological distinction of cortisol-producing and aldosterone-producing adrenal cortical adenomas: not only possible but a critical clinical responsibility. Histopathology. 2012;60(6): Mete O, Asa SL. Aldosterone-producing adrenal cortical adenoma with oncocytic change and cytoplasmic eosinophilic globular inclusions. Endocr Pathol. 2009;20(3): Späth M, Korovkin S, Antke C, Anlauf M, Willenberg HS. Aldosterone- and cortisol-co-secreting adrenal tumors: the lost subtype of primary aldosteronism. Eur J Endocrinol. 2011;164(4): McNicol AM. Diagnostic and molecular aspects of adrenal cortical tumors. Semin Diagn Pathol. 2013;30(3): Volante M, Bollito E, Sperone P, et al. Clinicopathological study of a series of 92 adrenocortical carcinomas: from a proposal of simplified diagnostic algorithm to prognostic stratification. Histopathology. 2009;55(5): Duregon E, Fassina A, Volante M, et al. The reticulin algorithm for adrenocortical tumor diagnosis: a multicentric validation study on 245 unpublished cases. Am J Surg Pathol. 2013;37(9): Nanba K, Tsuiki M, Sawai K, et al. Histopathological diagnosis of primary aldosteronism using CYP11B2 immunohistochemistry. J Clin Endocrinol Metab. 2013;98(4): Volpe C, Höög A, Ogishima T, et al. Immunohistochemistry improves histopathologic diagnosis in primary aldosteronism. J Clin Pathol. 2013;66(4): Young DMJ, Fuller PJ, Stowasser M, Mihailidou AS. Introduction. Clin Exp Pharmacol Physiol. 2013;40: Azizan EA, Poulsen H, Tuluc P, et al. Somatic mutations in ATP1A1 and CACNA1D underlie a common subtype of adrenal hypertension. Nat Genet. 2013;45(9): Beuschlein F, Boulkroun S, Osswald A, et al. Somatic mutations in ATP1A1 and ATP2B3 lead to aldosterone-producing adenomas and secondary hypertension. Nat Genet. 2013;45(4): Scholl UI, Goh G, Stölting G, et al. Somatic and germline CACNA1D calcium channel mutations in aldosterone-producing adenomas and primary aldosteronism. Nat Genet. 2013;45(9): Lenzini L, Caroccia B, Campos AG, et al. Lower expression of the TWIKrelated acid-sensitive Kþ channel 2 (TASK-2) gene is a hallmark of aldosteroneproducing adenoma causing human primary aldosteronism. J Clin Endocrinol Metab. 2014;99(4):e674 e Berthon A, Drelon C, Ragazzon B, et al. WNT/b-catenin signalling is activated in aldosterone-producing adenomas and controls aldosterone production. Hum Mol Genet. 2014;23(4): Fassnacht M, Kroiss M, Allolio B. Update in adrenocortical carcinoma. J Clin Endocrinol Metab. 2013;98(12): Arch Pathol Lab Med Vol 139, July 2015 Primary Aldosteronism Duan & Mete
The Adrenal Glands. I. Normal adrenal gland A. Gross & microscopic B. Hormone synthesis, regulation & measurement. II.
 The Adrenal Glands Thomas Jacobs, M.D. Diane Hamele-Bena, M.D. I. Normal adrenal gland A. Gross & microscopic B. Hormone synthesis, regulation & measurement II. Hypoadrenalism III. Hyperadrenalism; Adrenal
The Adrenal Glands Thomas Jacobs, M.D. Diane Hamele-Bena, M.D. I. Normal adrenal gland A. Gross & microscopic B. Hormone synthesis, regulation & measurement II. Hypoadrenalism III. Hyperadrenalism; Adrenal
Endocrine MR. Jan 30, 2015 Michael LaFata, MD
 Endocrine MR Jan 30, 2015 Michael LaFata, MD Brief case 55-year-old female in ED PMH: HTN, DM2, HLD, GERD CC: Epigastric/LUQ abdominal pain, N/V x2 days AF, HR 103, BP 155/85, room air CMP: Na 133, K 3.6,
Endocrine MR Jan 30, 2015 Michael LaFata, MD Brief case 55-year-old female in ED PMH: HTN, DM2, HLD, GERD CC: Epigastric/LUQ abdominal pain, N/V x2 days AF, HR 103, BP 155/85, room air CMP: Na 133, K 3.6,
G3.02 The malignant potential of the neoplasm should be recorded. CG3.02a
 G3.02 The malignant potential of the neoplasm should be recorded. CG3.02a Conventional adrenocortical neoplasm. Each of the below parameters is scored 0 when absent and 1 when present. 3 or more of these
G3.02 The malignant potential of the neoplasm should be recorded. CG3.02a Conventional adrenocortical neoplasm. Each of the below parameters is scored 0 when absent and 1 when present. 3 or more of these
Endocrine hypertensionmolecules. Marie Freel Caledonian Endocrine Society Meeting 29 th November 2015
 Endocrine hypertensionmolecules and genes Marie Freel Caledonian Endocrine Society Meeting 29 th November 2015 Plan Mineralocorticoid hypertension Myths surrounding Primary Aldosteronism (PA) New developments
Endocrine hypertensionmolecules and genes Marie Freel Caledonian Endocrine Society Meeting 29 th November 2015 Plan Mineralocorticoid hypertension Myths surrounding Primary Aldosteronism (PA) New developments
What s New in Adrenal Gland Pathology. Marina Scarpelli
 What s New in Adrenal Gland Pathology Marina Scarpelli Background Histological criteria for adrenocortical proliferative lesions Immunohistochemical markers Molecular markers Histological Criteria for
What s New in Adrenal Gland Pathology Marina Scarpelli Background Histological criteria for adrenocortical proliferative lesions Immunohistochemical markers Molecular markers Histological Criteria for
Primary Aldosteronism
 Primary Aldosteronism Odelia Cooper, MD Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism Cedars-Sinai Medical Center HYPERTENSION CENTER Barriers to diagnosing primary
Primary Aldosteronism Odelia Cooper, MD Assistant Professor of Medicine Division of Endocrinology, Diabetes, and Metabolism Cedars-Sinai Medical Center HYPERTENSION CENTER Barriers to diagnosing primary
Upon completion, participants should be able to:
 Learning Objectives Upon completion, participants should be able to: Describe the causes of secondary hypertension and the prevalence of primary aldosteronism Discuss the diagnostic approach to primary
Learning Objectives Upon completion, participants should be able to: Describe the causes of secondary hypertension and the prevalence of primary aldosteronism Discuss the diagnostic approach to primary
The Work-up and Treatment of Adrenal Nodules
 The Work-up and Treatment of Adrenal Nodules Lawrence Andrew Drew Shirley, MD, MS, FACS Assistant Professor of Surgical-Clinical Department of Surgery Division of Surgical Oncology The Ohio State University
The Work-up and Treatment of Adrenal Nodules Lawrence Andrew Drew Shirley, MD, MS, FACS Assistant Professor of Surgical-Clinical Department of Surgery Division of Surgical Oncology The Ohio State University
Mineralocorticoids: aldosterone Angiotensin II/renin regulation by sympathetic tone; High potassium will stimulate and ACTH Increase in aldosterone
 Disease of the Adrenals 1 Zona Glomerulosa Mineralocorticoids: aldosterone Angiotensin II/renin regulation by sympathetic tone; High potassium will stimulate and ACTH Increase in aldosterone leads to salt
Disease of the Adrenals 1 Zona Glomerulosa Mineralocorticoids: aldosterone Angiotensin II/renin regulation by sympathetic tone; High potassium will stimulate and ACTH Increase in aldosterone leads to salt
THE HIGHS AND LOWS OF ADRENAL GLAND PATHOLOGY
 THE HIGHS AND LOWS OF ADRENAL GLAND PATHOLOGY Symptoms of Adrenal Gland Disorders 2 Depends on whether it is making too much or too little hormone And on what you Google! Symptoms include obesity, skin
THE HIGHS AND LOWS OF ADRENAL GLAND PATHOLOGY Symptoms of Adrenal Gland Disorders 2 Depends on whether it is making too much or too little hormone And on what you Google! Symptoms include obesity, skin
Adrenal incidentaloma
 Adrenal incidentaloma Prevalence 5% post-mortem series 4% CT series 6-20% CT series in patients with Hx extra-adrenal malignancy Commoner with increasing age Associated with adrenal hyperfunction in 15%
Adrenal incidentaloma Prevalence 5% post-mortem series 4% CT series 6-20% CT series in patients with Hx extra-adrenal malignancy Commoner with increasing age Associated with adrenal hyperfunction in 15%
ADRENAL MEDULLARY DISORDERS: PHAEOCHROMOCYTOMAS AND MORE
 ADRENAL MEDULLARY DISORDERS: PHAEOCHROMOCYTOMAS AND MORE DR ANJU SAHDEV READER AND CONSULTANT RADIOLOGIST QUEEN MARY UNIVERSITY AND ST BARTHOLOMEW S HOSPITAL BARTS HEALTH, LONDON, UK DISCLOSURE OF CONFLICT
ADRENAL MEDULLARY DISORDERS: PHAEOCHROMOCYTOMAS AND MORE DR ANJU SAHDEV READER AND CONSULTANT RADIOLOGIST QUEEN MARY UNIVERSITY AND ST BARTHOLOMEW S HOSPITAL BARTS HEALTH, LONDON, UK DISCLOSURE OF CONFLICT
Primary aldosteronism clinical practice guidelines: a re-appraisal The Management of Primary Aldosteronism
 Primary aldosteronism clinical practice guidelines: a re-appraisal The Management of Primary Aldosteronism Prof. FRANCO MANTERO Division of Endocrinology University of Padua Italy Case Detection, Diagnosis
Primary aldosteronism clinical practice guidelines: a re-appraisal The Management of Primary Aldosteronism Prof. FRANCO MANTERO Division of Endocrinology University of Padua Italy Case Detection, Diagnosis
Odise Cenaj, Harvard Medical School Year III. Gillian Lieberman, MD
 February 2012 Radiologic evaluation of adrenal masses and an atypical radiologic presentation of adrenocortical carcinoma in a patient with primary aldosteronism Odise Cenaj, Harvard Medical School Year
February 2012 Radiologic evaluation of adrenal masses and an atypical radiologic presentation of adrenocortical carcinoma in a patient with primary aldosteronism Odise Cenaj, Harvard Medical School Year
Clarification of hypertension Diagnosis of primary hyperaldosteronism
 Nr. 1/2010 Clarification of hypertension Diagnosis of primary hyperaldosteronism Marc Beineke The significance of the /renin ratio (ARR) in the diagnosis of normoalaemic and hypokalaemic primary hyperaldosteronism,
Nr. 1/2010 Clarification of hypertension Diagnosis of primary hyperaldosteronism Marc Beineke The significance of the /renin ratio (ARR) in the diagnosis of normoalaemic and hypokalaemic primary hyperaldosteronism,
ADRENAL LESIONS 10/09/2012. Adrenal + lesion. Introduction. Common causes. Anatomy. Financial disclosure. Dr. Boraiah Sreeharsha. Nothing to declare
 ADRENAL LESIONS Financial disclosure Nothing to declare Dr. Boraiah Sreeharsha MBBS;FRCR;FRCPSC Introduction Adrenal + lesion Adrenal lesions are common 9% of the population Increase in the detection rate
ADRENAL LESIONS Financial disclosure Nothing to declare Dr. Boraiah Sreeharsha MBBS;FRCR;FRCPSC Introduction Adrenal + lesion Adrenal lesions are common 9% of the population Increase in the detection rate
Year 2004 Paper two: Questions supplied by Megan 1
 Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 96 A 32yo woman if found to have high blood pressure (180/105mmHg) at an insurance medical examination. She is asymptomatic. Clinical examination
Year 2004 Paper two: Questions supplied by Megan 1 QUESTION 96 A 32yo woman if found to have high blood pressure (180/105mmHg) at an insurance medical examination. She is asymptomatic. Clinical examination
Endocrine. Endocrine as it relates to the kidney. Sarah Elfering, MD University of Minnesota
 Endocrine Sarah Elfering, MD University of Minnesota Endocrine as it relates to the kidney Parathyroid gland Vitamin D Endocrine causes of HTN Adrenal adenoma PTH Bone Kidney Intestine 1, 25 OH Vitamin
Endocrine Sarah Elfering, MD University of Minnesota Endocrine as it relates to the kidney Parathyroid gland Vitamin D Endocrine causes of HTN Adrenal adenoma PTH Bone Kidney Intestine 1, 25 OH Vitamin
Evaluation of Thyroid Nodules
 Evaluation of Thyroid Nodules Stephan Kowalyk, MD January 25 28, 2018 1 Primary goal Exclude malignancy Incidental thyroid nodules If found on CT, MRI, PET scan, carotid Doppler ULTRASOUND!! January 25
Evaluation of Thyroid Nodules Stephan Kowalyk, MD January 25 28, 2018 1 Primary goal Exclude malignancy Incidental thyroid nodules If found on CT, MRI, PET scan, carotid Doppler ULTRASOUND!! January 25
Adrenal Incidentaloma Management
 Adrenal Incidentaloma Management Full Title of Guideline: Author Management of Incidentally-discovered Adrenal Lesions ( Incidentalomas ) Mr David Chadwick Consultant Endocrine Surgeon david.chadwick2@nuh.nhs.uk
Adrenal Incidentaloma Management Full Title of Guideline: Author Management of Incidentally-discovered Adrenal Lesions ( Incidentalomas ) Mr David Chadwick Consultant Endocrine Surgeon david.chadwick2@nuh.nhs.uk
Case Scenario 1: Thyroid
 Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Case Scenario 1: Thyroid History and Physical Patient is an otherwise healthy 80 year old female with the complaint of a neck mass first noticed two weeks ago. The mass has increased in size and is palpable.
Approach to Adrenal Incidentaloma. Alice Y.Y. Cheng, MD, FRCP
 Approach to Adrenal Incidentaloma Alice Y.Y. Cheng, MD, FRCP Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form
Approach to Adrenal Incidentaloma Alice Y.Y. Cheng, MD, FRCP Copyright 2017 by Sea Courses Inc. All rights reserved. No part of this document may be reproduced, copied, stored, or transmitted in any form
ADRENAL INCIDENTALOMA. Jamii St. Julien
 ADRENAL INCIDENTALOMA Jamii St. Julien Outline Definition Differential Evaluation Treatment Follow up Questions Case Definition The phenomenon of detecting an otherwise unsuspected adrenal mass on radiologic
ADRENAL INCIDENTALOMA Jamii St. Julien Outline Definition Differential Evaluation Treatment Follow up Questions Case Definition The phenomenon of detecting an otherwise unsuspected adrenal mass on radiologic
My personal experience at University of Toronto and recent updates of
 My personal experience at University of Toronto and recent updates of Endocrine Pathology Toshitetsu Hayashi M.D. Ph.D. ¹Department of Diagnostic Pathology, Takamatsu Red Cross Hospital, Japan ²Laboratory
My personal experience at University of Toronto and recent updates of Endocrine Pathology Toshitetsu Hayashi M.D. Ph.D. ¹Department of Diagnostic Pathology, Takamatsu Red Cross Hospital, Japan ²Laboratory
Spectrum of Hypertension & Hypokalemia
 Spectrum of Hypertension & Hypokalemia Farheen K. Dojki, PGY-6 Hypertension Fellow, ASH Hypertension Center Dr. Dojki does not have any relevant financial relationships with any commercial interests. OBJECTIVES:
Spectrum of Hypertension & Hypokalemia Farheen K. Dojki, PGY-6 Hypertension Fellow, ASH Hypertension Center Dr. Dojki does not have any relevant financial relationships with any commercial interests. OBJECTIVES:
Primary Aldosteronism: screening, diagnosis and therapy
 Primary Aldosteronism: screening, diagnosis and therapy Jacques W.M. Lenders, internist DEPT. OF INTERNAL MEDICINE, RADBOUD UNIVERSITY NIJMEGEN MEDICAL CENTER, NIJMEGEN,THE NETHERLANDS DEPT. OF INTERNAL
Primary Aldosteronism: screening, diagnosis and therapy Jacques W.M. Lenders, internist DEPT. OF INTERNAL MEDICINE, RADBOUD UNIVERSITY NIJMEGEN MEDICAL CENTER, NIJMEGEN,THE NETHERLANDS DEPT. OF INTERNAL
Management of adrenal incidentalomas
 31 Management of adrenal incidentalomas KEVIN MURTAGH, NANA MUHAMMAD AND MAREK MILLER The return of a scan result with reference to an incidental finding of an adrenal mass is a common scenario. 1 The
31 Management of adrenal incidentalomas KEVIN MURTAGH, NANA MUHAMMAD AND MAREK MILLER The return of a scan result with reference to an incidental finding of an adrenal mass is a common scenario. 1 The
Aldosterone-Producing Adrenocortical Carcinoma with Co-Secretion of Cortisol and Estradiol: A Case Report* Karen Lazaro and Perie Adorable-Wagan
 Case RePort Journal of the ASEAN Federation of Endocrine Societies with Co-Secretion of Cortisol and Estradiol: A Case Report* Karen Lazaro and Perie Adorable-Wagan Section of Endocrinology, Diabetes and
Case RePort Journal of the ASEAN Federation of Endocrine Societies with Co-Secretion of Cortisol and Estradiol: A Case Report* Karen Lazaro and Perie Adorable-Wagan Section of Endocrinology, Diabetes and
Resistant hypertension is defined as blood. Primary Hyperaldosteronism Decoded: A Case of Curable Resistant Hypertension.
 Case Review Primary Hyperaldosteronism Decoded: A Case of Curable Resistant Hypertension Timothy R. Larsen, DO, Wadie David, Susan Steigerwalt, MD, Shukri David, MD Department of Internal Medicine, Section
Case Review Primary Hyperaldosteronism Decoded: A Case of Curable Resistant Hypertension Timothy R. Larsen, DO, Wadie David, Susan Steigerwalt, MD, Shukri David, MD Department of Internal Medicine, Section
Case Based Urology Learning Program
 Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 4 CBULP 2010 004 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Case Based Urology Learning Program Resident s Corner: UROLOGY Case Number 4 CBULP 2010 004 Case Based Urology Learning Program Editor: Associate Editors: Manager: Case Contributors: Steven C. Campbell,
Kidney Case 1 SURGICAL PATHOLOGY REPORT
 Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Kidney Case 1 Surgical Pathology Report February 9, 2007 Clinical History: This 45 year old woman was found to have a left renal mass. CT urography with reconstruction revealed a 2 cm medial mass which
Dimitrios Linos, M.D., Ph.D. Professor of Surgery National & Kapodistrian University of Athens
 Dimitrios Linos, M.D., Ph.D. Professor of Surgery National & Kapodistrian University of Athens What is an adrenal incidentaloma? An adrenal incidentaloma is defined as an adrenal tumor initially diagnosed
Dimitrios Linos, M.D., Ph.D. Professor of Surgery National & Kapodistrian University of Athens What is an adrenal incidentaloma? An adrenal incidentaloma is defined as an adrenal tumor initially diagnosed
Incidental adrenal masses A primary care approach
 CLINICAL Incidental adrenal masses A primary care approach Rasha Gendy, Prem Rashid Background The common use of cross-sectional imaging for the investigation of abdominal and thoracic illness has resulted
CLINICAL Incidental adrenal masses A primary care approach Rasha Gendy, Prem Rashid Background The common use of cross-sectional imaging for the investigation of abdominal and thoracic illness has resulted
Primary Aldosteronism & Implications for Primary Hypertension
 & Implications for Primary Hypertension Richard J. Auchus, MD, PhD, FACE Professor and Fellowship Program Director Depts of Internal Medicine/MEND & Pharmacology University of Michigan Disclosures Contracted
& Implications for Primary Hypertension Richard J. Auchus, MD, PhD, FACE Professor and Fellowship Program Director Depts of Internal Medicine/MEND & Pharmacology University of Michigan Disclosures Contracted
Adrenal Mass. Cynthia Kwong SUNY Downstate Medical Center Grand Rounds October 13, 2016
 Adrenal Mass Cynthia Kwong SUNY Downstate Medical Center Grand Rounds October 13, 2016 Case Presentation 65F found to have a 4cm left adrenal mass in 2012 now presents with 6.7cm left adrenal mass PMHx:
Adrenal Mass Cynthia Kwong SUNY Downstate Medical Center Grand Rounds October 13, 2016 Case Presentation 65F found to have a 4cm left adrenal mass in 2012 now presents with 6.7cm left adrenal mass PMHx:
Updates in primary hyperaldosteronism and the rule
 Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. Professor of Medicine and Physiology and Functional Genomics University of Florida College of Medicine and NF/SGVHS The 20-50
Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. Professor of Medicine and Physiology and Functional Genomics University of Florida College of Medicine and NF/SGVHS The 20-50
Papillary Lesions of the Breast A Practical Approach to Diagnosis. (Arch Pathol Lab Med. 2016;140: ; doi: /arpa.
 Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
Papillary Lesions of the Breast A Practical Approach to Diagnosis (Arch Pathol Lab Med. 2016;140:1052 1059; doi: 10.5858/arpa.2016-0219-RA) Papillary lesions of the breast Span the spectrum of benign,
COPYRIGHTED MATERIAL. Adrenal Imaging. 1.1 Introduction. Khaled M. Elsayes 1, Isaac R. Francis 1, Melvyn Korobkin 1 and Gerard M.
 1 Adrenal Imaging Khaled M. Elsayes 1, Isaac R. Francis 1, Melvyn Korobkin 1 and Gerard M. Doherty 2 1 Department of Radiology, University of Michigan 2 Department of Radiology and Surgery, University
1 Adrenal Imaging Khaled M. Elsayes 1, Isaac R. Francis 1, Melvyn Korobkin 1 and Gerard M. Doherty 2 1 Department of Radiology, University of Michigan 2 Department of Radiology and Surgery, University
Patel et al. Patel et al. Diagnostic Pathology 2014, 9:147
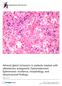 Adrenal gland inclusions in patients treated with aldosterone antagonists (Spironolactone/ Eplerenone): incidence, morphology, and ultrastructural findings Patel et al. Patel et al. Diagnostic Pathology
Adrenal gland inclusions in patients treated with aldosterone antagonists (Spironolactone/ Eplerenone): incidence, morphology, and ultrastructural findings Patel et al. Patel et al. Diagnostic Pathology
Disclosure. Relevant Financial Relationship(s) None. Off Label Usage None MFMER slide-1
 Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Disclosure Relevant Financial Relationship(s) None Off Label Usage None 2013 MFMER slide-1 Case Presentation A 43 year old male, with partial nephrectomy for a right kidney mass 2013 MFMER slide-2 2013
Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation
 Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Acta Radiológica Portuguesa, Vol.XVIII, nº 70, pág. 61-70, Abr.-Jun., 2006 Pediatric Retroperitoneal Masses Radiologic-Pathologic Correlation Marilyn J. Siegel Mallinckrodt Institute of Radiology, Washington
Adrenocortical Oncocytoma
 The Korean Journal of Pathology 2007; 41: 329-33 Adrenocortical Oncocytoma - A Case Report - Hun-Soo Kim Dae-Young Kang 1 Department of Pathology, Wonkwang University School of Medicine, Iksan; 1 Department
The Korean Journal of Pathology 2007; 41: 329-33 Adrenocortical Oncocytoma - A Case Report - Hun-Soo Kim Dae-Young Kang 1 Department of Pathology, Wonkwang University School of Medicine, Iksan; 1 Department
Adrenal incidentaloma guideline for Northern Endocrine Network
 Adrenal incidentaloma guideline for Northern Endocrine Network Definition of adrenal incidentaloma Adrenal mass detected on an imaging study done for indications that are not related to an adrenal problem
Adrenal incidentaloma guideline for Northern Endocrine Network Definition of adrenal incidentaloma Adrenal mass detected on an imaging study done for indications that are not related to an adrenal problem
Prevalence and characterization of somatic mutations in Chinese aldosterone-producing adenoma. patients. Supplemental data. First author: Baojun Wang
 Prevalence and characterization of somatic mutations in Chinese aldosterone-producing adenoma patients Supplemental data First author: Baojun Wang Patients and tumor samples A total of 87 patients with
Prevalence and characterization of somatic mutations in Chinese aldosterone-producing adenoma patients Supplemental data First author: Baojun Wang Patients and tumor samples A total of 87 patients with
Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation
 246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
246) Prague Medical Report / Vol. 113 (2012) No. 3, p. 246 250 Solitary Fibrous Tumor of the Kidney with Massive Retroperitoneal Recurrence. A Case Presentation Sfoungaristos S., Papatheodorou M., Kavouras
Update in Salivary Gland Pathology. Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016
 Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
Update in Salivary Gland Pathology Benjamin L. Witt University of Utah/ARUP Laboratories February 9, 2016 Objectives Review the different appearances of a selection of salivary gland tumor types Establish
Diplomate of the American Board of Pathology in Anatomic and Clinical Pathology
 A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
A 33-year-old male with a left lower leg mass. Contributed by Shaoxiong Chen, MD, PhD Assistant Professor Indiana University School of Medicine/ IU Health Partners Department of Pathology and Laboratory
Normal thyroid tissue
 Thyroid Pathology Overview Normal thyroid tissue Normal thyroid tissue with follicles filled with colloid. Thyroid cells form follicles, spheres of epithelial cells (always single layered in health, usually
Thyroid Pathology Overview Normal thyroid tissue Normal thyroid tissue with follicles filled with colloid. Thyroid cells form follicles, spheres of epithelial cells (always single layered in health, usually
Disclosures. Parathyroid Pathology. Objectives. The normal parathyroid 11/10/2012
 Disclosures Parathyroid Pathology I have nothing to disclose Annemieke van Zante MD/PhD Assistant Professor of Clinical Pathology Associate Chief of Cytopathology Objectives 1. Review the pathologic features
Disclosures Parathyroid Pathology I have nothing to disclose Annemieke van Zante MD/PhD Assistant Professor of Clinical Pathology Associate Chief of Cytopathology Objectives 1. Review the pathologic features
The Management of adrenal incidentaloma
 The Management of adrenal incidentaloma Dimitrios Linos, MD Director of Surgery, Hygeia Hospital, Athens, Greece Consultant in Surgery, Massachusetts General Hospital, Boston, USA 8 th Postgraduate Course
The Management of adrenal incidentaloma Dimitrios Linos, MD Director of Surgery, Hygeia Hospital, Athens, Greece Consultant in Surgery, Massachusetts General Hospital, Boston, USA 8 th Postgraduate Course
Indications for Surgical Removal of Adrenal Glands
 The adrenal glands are orange-colored endocrine glands which are located on the top of both kidneys. The adrenal glands are triangular shaped and measure about one-half inch in height and 3 inches in length.
The adrenal glands are orange-colored endocrine glands which are located on the top of both kidneys. The adrenal glands are triangular shaped and measure about one-half inch in height and 3 inches in length.
The endocrine system is made up of a complex group of glands that secrete hormones.
 1 10. Endocrinology I MEDCHEM 535 Diagnostic Medicinal Chemistry Endocrinology The endocrine system is made up of a complex group of glands that secrete hormones. These hormones control reproduction, metabolism,
1 10. Endocrinology I MEDCHEM 535 Diagnostic Medicinal Chemistry Endocrinology The endocrine system is made up of a complex group of glands that secrete hormones. These hormones control reproduction, metabolism,
CPY 605 ADVANCED ENDOCRINOLOGY
 CPY 605 ADVANCED ENDOCRINOLOGY THE ADRENAL CORTEX PRESENTED BY WAINDIM NYIAMBAM YVONNE HS09A187 INTRODUCTION Two adrenal glands lie on top of each kidney. Each gland between 6 and 8g in weight is composed
CPY 605 ADVANCED ENDOCRINOLOGY THE ADRENAL CORTEX PRESENTED BY WAINDIM NYIAMBAM YVONNE HS09A187 INTRODUCTION Two adrenal glands lie on top of each kidney. Each gland between 6 and 8g in weight is composed
Adrenal gland Incidentaloma
 Adrenal gland Incidentaloma Topic review 17 sep 2008 Anatomy 1 Anatomical consideration Blood supply Artery: small branches from Inf. phrenic, renal artery and aorta Vein: Rt : medial aspect to IVC Lt
Adrenal gland Incidentaloma Topic review 17 sep 2008 Anatomy 1 Anatomical consideration Blood supply Artery: small branches from Inf. phrenic, renal artery and aorta Vein: Rt : medial aspect to IVC Lt
Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy
 ISPUB.COM The Internet Journal of Urology Volume 9 Number 1 Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy S Bontha, N Sanalkumar, M Istarabadi, G Lepsien,
ISPUB.COM The Internet Journal of Urology Volume 9 Number 1 Adrenal Ganglioneuroma Presenting With Adrenal Insufficiency After Unilateral Adrenalectomy S Bontha, N Sanalkumar, M Istarabadi, G Lepsien,
How to Recognize Adrenal Disease
 How to Recognize Adrenal Disease CME Away India & Sri Lanka March 23 - April 7, 2018 Richard A. Bebb MD, ABIM, FRCPC Consultant Endocrinologist Medical Subspecialty Institute Cleveland Clinic Abu Dhabi
How to Recognize Adrenal Disease CME Away India & Sri Lanka March 23 - April 7, 2018 Richard A. Bebb MD, ABIM, FRCPC Consultant Endocrinologist Medical Subspecialty Institute Cleveland Clinic Abu Dhabi
Clinicopathological correlates of adrenal Cushing s syndrome
 1 Department of Pathology, University Health Network, Toronto, Ontario, Canada 2 Department of Laboratory Medicine and Pathobiology, University of Toronto, Ontario, Canada 3 Department of Medicine, University
1 Department of Pathology, University Health Network, Toronto, Ontario, Canada 2 Department of Laboratory Medicine and Pathobiology, University of Toronto, Ontario, Canada 3 Department of Medicine, University
ENDOCRINOLOGY 3. R. A. Benacka, MD, PhD, prof. Department of Pathophysiology Medical faculty, Safarik University, Košice
 Academic lectures for general medicine 3rd year 2005/2006, 2013/2014 ENDOCRINOLOGY 3 R. A. Benacka, MD, PhD, prof. Department of Pathophysiology Medical faculty, Safarik University, Košice Figures and
Academic lectures for general medicine 3rd year 2005/2006, 2013/2014 ENDOCRINOLOGY 3 R. A. Benacka, MD, PhD, prof. Department of Pathophysiology Medical faculty, Safarik University, Košice Figures and
Updates in primary hyperaldosteronism and the rule
 Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of
Updates in primary hyperaldosteronism and the 20-50 rule I. David Weiner, M.D. C. Craig and Audrae Tisher Chair in Nephrology Professor of Medicine and Physiology and Functional Genomics University of
A Rare Case of ACTH-independent Macronodular Adrenal Hyperplasia Associated with Aldosterone-producing Adenoma
 CASE REPORT A Rare Case of ACTHindependent Macronodular Adrenal Hyperplasia Associated with Aldosteroneproducing Adenoma Eri Hayakawa 1, Takanobu Yoshimoto 1, Kiichiro Hiraishi 1, Masako Kato 1, Hajime
CASE REPORT A Rare Case of ACTHindependent Macronodular Adrenal Hyperplasia Associated with Aldosteroneproducing Adenoma Eri Hayakawa 1, Takanobu Yoshimoto 1, Kiichiro Hiraishi 1, Masako Kato 1, Hajime
ظظظ/ Omar Sami. Hussam Twaissi. Mousa Abbadi
 ظظظ/ 5 Omar Sami Hussam Twaissi Mousa Abbadi The doctor started this lecture by revising what we have taken in lecture number four, I won t re-write these stuff as it becomes boring so often. This sheet
ظظظ/ 5 Omar Sami Hussam Twaissi Mousa Abbadi The doctor started this lecture by revising what we have taken in lecture number four, I won t re-write these stuff as it becomes boring so often. This sheet
I. Adrerenocortical Hyperfunction (Hyperadrenalism) 1. Hypercortisolism (Cushing Syndrome) - In clinical practice, most cases are caused by the
 The Adrenal gland I. Adrerenocortical Hyperfunction (Hyperadrenalism) 1. Hypercortisolism (Cushing Syndrome) - In clinical practice, most cases are caused by the administration of exogenous glucocorticoids
The Adrenal gland I. Adrerenocortical Hyperfunction (Hyperadrenalism) 1. Hypercortisolism (Cushing Syndrome) - In clinical practice, most cases are caused by the administration of exogenous glucocorticoids
ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain
 ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain OUR APPROACH Incidental adrenal nodule/mass Isaac R Francis, M.B;B.S University of Michigan, Ann Arbor, Michigan Disclosures None (in memory) M Korobkin,
ESUR 2018, Sept. 13 th.-16 th., 2018 Barcelona, Spain OUR APPROACH Incidental adrenal nodule/mass Isaac R Francis, M.B;B.S University of Michigan, Ann Arbor, Michigan Disclosures None (in memory) M Korobkin,
Personal data. Age : 63 Gender : male
 Personal data Age : 63 Gender : male Chief complain No specific symptom or discomfort A hepatic mass, found by abdominal sonography of routine health exam on 88-12-08 Past history 1984-3-3 Old CVA with
Personal data Age : 63 Gender : male Chief complain No specific symptom or discomfort A hepatic mass, found by abdominal sonography of routine health exam on 88-12-08 Past history 1984-3-3 Old CVA with
Essentials of Clinical MR, 2 nd edition. 73. Urinary Bladder and Male Pelvis
 73. Urinary Bladder and Male Pelvis Urinary bladder carcinoma is best locally staged with MRI. It is important however to note that a thickened wall (> 5 mm) is a non-specific finding seen in an underfilled
73. Urinary Bladder and Male Pelvis Urinary bladder carcinoma is best locally staged with MRI. It is important however to note that a thickened wall (> 5 mm) is a non-specific finding seen in an underfilled
ORIGINAL ARTICLE. Pathologic Features of Prognostic Significance for Adrenocortical Carcinoma After Curative Resection. with adrenocortical carcinoma
 ORIGINAL ARTICLE Pathologic Features of Prognostic Significance for Adrenocortical Carcinoma After Curative Resection Lawrence E. Harrison, MD; Paul B. Gaudin, MD; Murray F. Brennan, MD Objective: To identify
ORIGINAL ARTICLE Pathologic Features of Prognostic Significance for Adrenocortical Carcinoma After Curative Resection Lawrence E. Harrison, MD; Paul B. Gaudin, MD; Murray F. Brennan, MD Objective: To identify
Proliferative Epithelial lesions of the Breast. Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London
 Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Proliferative Epithelial lesions of the Breast Sami Shousha, MD, FRCPath Charing Cross Hospital & Imperial College, London Amman, November2013 Proliferative Epithelial Lesions of the Breast Usual type
Pathology of the endocrine system
 Pathology of the endocrine system Endocrine system A. Endocrine organs 1. Pituitary gland 2. Pineal gland 3. Thyroid gland 4. Adrenal glands 5. Parathyroid glands B. Organs with partial endocrine functions
Pathology of the endocrine system Endocrine system A. Endocrine organs 1. Pituitary gland 2. Pineal gland 3. Thyroid gland 4. Adrenal glands 5. Parathyroid glands B. Organs with partial endocrine functions
Pitfalls in the diagnosis of well-differentiated hepatocellular lesions
 2013 Colorado Society of Pathology Pitfalls in the diagnosis of well-differentiated hepatocellular lesions Sanjay Kakar, MD University of California, San Francisco Outline Hepatocellular adenoma: new WHO
2013 Colorado Society of Pathology Pitfalls in the diagnosis of well-differentiated hepatocellular lesions Sanjay Kakar, MD University of California, San Francisco Outline Hepatocellular adenoma: new WHO
Protocol for the Examination of Specimens From Patients With Carcinoma of the Adrenal Gland
 Protocol for the Examination of Specimens From Patients With Carcinoma of the Adrenal Gland Version: Adrenal Gland 4.0.2.0 Protocol Posting Date: February 2019 CAP Laboratory Accreditation Program Protocol
Protocol for the Examination of Specimens From Patients With Carcinoma of the Adrenal Gland Version: Adrenal Gland 4.0.2.0 Protocol Posting Date: February 2019 CAP Laboratory Accreditation Program Protocol
ADRENAL GLAND. Introduction 4/21/2009. Among most important and vital endocrine organ. Small bilateral yellowish retroperitoneal organ
 Introduction Among most important and vital endocrine organ ADRENAL GLAND D.Hammoudi.MD Small bilateral yellowish retroperitoneal organ Lies just above kidney in gerota s fascia 2 1 The Adrenal Gland Anatomy
Introduction Among most important and vital endocrine organ ADRENAL GLAND D.Hammoudi.MD Small bilateral yellowish retroperitoneal organ Lies just above kidney in gerota s fascia 2 1 The Adrenal Gland Anatomy
ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY. Jonathan I. Epstein.
 1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
1 ARTHUR PURDY STOUT SOCIETY COMPANION MEETING: DIFFICULT NEW DIFFERENTIAL DIAGNOSES IN PROSTATE PATHOLOGY Jonathan I. Epstein Professor Pathology, Urology, Oncology The Reinhard Professor of Urological
Adrenal Gland. Zona Glomerulosa (mineralcorticoids) Zona Fasciculata (glucocorticoids) Zona Reticularis (sexual hormones) Adrenaline and noradrenaline
 n Cortex Zona Glomerulosa (mineralcorticoids) Zona Fasciculata (glucocorticoids) Zona Reticularis (sexual hormones) n Medulla Adrenaline and noradrenaline n Adrenocortical Hyperfunction Hyperaldosteronism
n Cortex Zona Glomerulosa (mineralcorticoids) Zona Fasciculata (glucocorticoids) Zona Reticularis (sexual hormones) n Medulla Adrenaline and noradrenaline n Adrenocortical Hyperfunction Hyperaldosteronism
PATHOLOGY OF LIVER TUMORS
 PATHOLOGY OF LIVER TUMORS Pathobasic, 31.05.2016 WHO Classification Approach to a Liver Mass Lesion in a patient with chronic liver disease? Lesion in a patient without chronic liver disease? Malignant
PATHOLOGY OF LIVER TUMORS Pathobasic, 31.05.2016 WHO Classification Approach to a Liver Mass Lesion in a patient with chronic liver disease? Lesion in a patient without chronic liver disease? Malignant
Papillary Lesions of the breast
 Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Papillary Lesions of the breast Emad Rakha Professor of Breast Pathology The University of Nottingham Papillary lesions of the breast are a heterogeneous group of disease, which are characterised by neoplastic
Cracking the diagnostic puzzle of tumours of adrenal cortex: a histopathological study
 International Journal of Research in Medical Sciences Madabhushi V et al. Int J Res Med Sci. 2016 Apr;4(4):1242-1247 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20160817
International Journal of Research in Medical Sciences Madabhushi V et al. Int J Res Med Sci. 2016 Apr;4(4):1242-1247 www.msjonline.org pissn 2320-6071 eissn 2320-6012 Research Article DOI: http://dx.doi.org/10.18203/2320-6012.ijrms20160817
CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. CYSTIC NEPHROMA
 Page 1 CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. Department of Pathology & Laboratory Medicine Phone (317) 274-4806 Medical Science A-128 FAX: (317) 278-2018 635 Barnhill Drive jeble @iupui.edu Indianapolis,
Page 1 CYSTIC TUMORS OF THE KIDNEY JOHN N. EBLE, M.D. Department of Pathology & Laboratory Medicine Phone (317) 274-4806 Medical Science A-128 FAX: (317) 278-2018 635 Barnhill Drive jeble @iupui.edu Indianapolis,
Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events
 Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events Sandrine Rorive, M.D., PhD. Erasme Hospital - Université Libre de Bruxelles (ULB) INTRODUCTION The assessment of thyroid nodules
Ultrasound-Guided Fine-Needle Aspiration of Thyroid Nodules: New events Sandrine Rorive, M.D., PhD. Erasme Hospital - Université Libre de Bruxelles (ULB) INTRODUCTION The assessment of thyroid nodules
How to approach resistant hypertension. Teh-Li Huo, M.D., Ph.D.
 How to approach resistant hypertension Teh-Li Huo, M.D., Ph.D. BP goals No risk factors:
How to approach resistant hypertension Teh-Li Huo, M.D., Ph.D. BP goals No risk factors:
Complementary somatic mutations of KCNJ5, ATP1A1, and ATP2B3 in sporadic aldosterone producing adrenal adenomas
 Complementary somatic mutations of KCNJ5, ATP1A1, and ATP2B3 in sporadic aldosterone producing adrenal adenomas Ravi Kumar Dutta, Jenny Welander, Michael Brauckhoff, Martin Walz, Piero Alesina, Thomas
Complementary somatic mutations of KCNJ5, ATP1A1, and ATP2B3 in sporadic aldosterone producing adrenal adenomas Ravi Kumar Dutta, Jenny Welander, Michael Brauckhoff, Martin Walz, Piero Alesina, Thomas
AN AUTOPSY CASE OF PARATHYROID CARC. Matsumoto, Koji; Ito, Masahiro; Sek. Citation Acta medica Nagasakiensia. 1989, 34
 NAOSITE: Nagasaki University's Ac Title Author(s) AN AUTOPSY CASE OF PARATHYROID CARC Hsu, Chao-Tien; Naito, Shinji; Shik Matsumoto, Koji; Ito, Masahiro; Sek Citation Acta medica Nagasakiensia. 1989, 34
NAOSITE: Nagasaki University's Ac Title Author(s) AN AUTOPSY CASE OF PARATHYROID CARC Hsu, Chao-Tien; Naito, Shinji; Shik Matsumoto, Koji; Ito, Masahiro; Sek Citation Acta medica Nagasakiensia. 1989, 34
Diseases of the Adrenal gland
 Diseases of the Adrenal gland Adrenal insufficiency Cushing disease vs syndrome Pheochromocytoma Hyperaldostronism What are the layers of the adrenal gland?? And what does each layer produce?? What are
Diseases of the Adrenal gland Adrenal insufficiency Cushing disease vs syndrome Pheochromocytoma Hyperaldostronism What are the layers of the adrenal gland?? And what does each layer produce?? What are
Recommendations for Reporting of Tumors of the Adrenal Cortex and Medulla
 A J C P / REPORTING OF TUMORS OF THE ADRENAL CORTEX AND MEDULLA Recommendations for Reporting of Tumors of the Adrenal Cortex and Medulla Association of Directors of Anatomic and Surgical Pathology" Key
A J C P / REPORTING OF TUMORS OF THE ADRENAL CORTEX AND MEDULLA Recommendations for Reporting of Tumors of the Adrenal Cortex and Medulla Association of Directors of Anatomic and Surgical Pathology" Key
Pituitary Gland Disorders
 Pituitary Gland Disorders 1 2 (GH-RH) (CRH) (TRH) (TRH) (GTRH) (GTRH) 3 Classification of pituitary disorders: 1. Hypersecretory diseases: a. Acromegaly and gigantism: Usually caused by (GH)-secreting
Pituitary Gland Disorders 1 2 (GH-RH) (CRH) (TRH) (TRH) (GTRH) (GTRH) 3 Classification of pituitary disorders: 1. Hypersecretory diseases: a. Acromegaly and gigantism: Usually caused by (GH)-secreting
Diseases of the breast (1 of 2)
 Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
Diseases of the breast (1 of 2) Introduction A histology introduction Normal ducts and lobules of the breast are lined by two layers of cells a layer of luminal cells overlying a second layer of myoepithelial
RECURRENT ADRENAL DISEASE. Megan Applewhite Endorama 2/19/2015 SR , SC
 RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
RECURRENT ADRENAL DISEASE Megan Applewhite Endorama 2/19/2015 SR 2412318, SC 3421561 Category: Adrenal Attendings: Angelos & Grogan PATIENT #1 36yo woman with a hx of Cushing s Syndrome and right adrenalectomy
18F-FDG PET for the Identification of Adrenocortical Carcinomas among Indeterminate Adrenal Tumors at Computed Tomography Scanning
 World J Surg (2010) 34:1506 1510 DOI 10.1007/s00268-010-0576-3 18F-FDG PET for the Identification of Adrenocortical Carcinomas among Indeterminate Adrenal Tumors at Computed Tomography Scanning Marie Laure
World J Surg (2010) 34:1506 1510 DOI 10.1007/s00268-010-0576-3 18F-FDG PET for the Identification of Adrenocortical Carcinomas among Indeterminate Adrenal Tumors at Computed Tomography Scanning Marie Laure
!! 2 to 3% of All New Visceral Cancers.!! Peak Incidence is 6th Decade!! M:F = 2:1
 !! Kathleen M. O Toole, M.D.!! 2 to 3% of All New Visceral Cancers!! Peak Incidence is 6th Decade!! M:F = 2:1!! Grossly is a Bright Yellow, Necrotic Mass with a Pseudocapsule 1 !!Conventional RCC! Clear
!! Kathleen M. O Toole, M.D.!! 2 to 3% of All New Visceral Cancers!! Peak Incidence is 6th Decade!! M:F = 2:1!! Grossly is a Bright Yellow, Necrotic Mass with a Pseudocapsule 1 !!Conventional RCC! Clear
Disorders of Cell Growth & Neoplasia. Histopathology Lab
 Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
Disorders of Cell Growth & Neoplasia Histopathology Lab Paul Hanna April 2010 Case #84 Clinical History: 5 yr-old, West Highland White terrier. skin mass from axillary region. has been present for the
hyperplastic parathyroid glands
 Journal of Clinical Pathology, 1978, 31, 626-632 A histological comparison of adenomatous and hyperplastic parathyroid glands D. A. S. LAWRENCE From the Department of Histopathology, Royal Free Hospital,
Journal of Clinical Pathology, 1978, 31, 626-632 A histological comparison of adenomatous and hyperplastic parathyroid glands D. A. S. LAWRENCE From the Department of Histopathology, Royal Free Hospital,
Impact of aldosterone-producing cell clusters on diagnostic discrepancies in primary aldosteronism
 , 2018, Vol. 9, (No. 40), pp: 26007-26018 Impact of aldosterone-producing cell clusters on diagnostic discrepancies in primary aldosteronism Mitsuhiro Kometani 1, Takashi Yoneda 1,2, Daisuke Aono 1, Shigehiro
, 2018, Vol. 9, (No. 40), pp: 26007-26018 Impact of aldosterone-producing cell clusters on diagnostic discrepancies in primary aldosteronism Mitsuhiro Kometani 1, Takashi Yoneda 1,2, Daisuke Aono 1, Shigehiro
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Medical Expert
 Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
Health Sciences Centre, Team A, Dr. L. Bohacek (Endocrine Surgery) Introduction Medical Expert This is a three month PGY 1-5 rotation in which residents gain exposure in the care and management of patients
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017
 Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
Prostate cancer ~ diagnosis and impact of pathology on prognosis ESMO 2017 Dr Puay Hoon Tan Division of Pathology Singapore General Hospital Prostate cancer (acinar adenocarcinoma) Invasive carcinoma composed
EDUCATIONAL CASES E1 & E2. Natasha Inglis 20/03/15
 EDUCATIONAL CASES E1 & E2 Natasha Inglis 20/03/15 CASE E1 79 year old female Rectum. Altemeier operation Histology Superficial erosions and mucosal congestion volcano lesion and pseudomembrane formation
EDUCATIONAL CASES E1 & E2 Natasha Inglis 20/03/15 CASE E1 79 year old female Rectum. Altemeier operation Histology Superficial erosions and mucosal congestion volcano lesion and pseudomembrane formation
Endocrine Hypertension
 Endocrine Hypertension 1 No Disclosures Endocrine Hypertension Objectives: 1. Understand Endocrine disorders causing hypertension 2. Understand clinical presentation of Pheochromocytoma and Hyperaldosteronism
Endocrine Hypertension 1 No Disclosures Endocrine Hypertension Objectives: 1. Understand Endocrine disorders causing hypertension 2. Understand clinical presentation of Pheochromocytoma and Hyperaldosteronism
Traumatic and Non Traumatic Adrenal Emergencies
 Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
Traumatic and Non Traumatic Adrenal Emergencies Michael N. Patlas, MD, FRCPC (1), Christine O. Menias, MD (2), Douglas S. Katz, MD, FACR (3), Ania Z. Kielar, MD, FRCPC (4), Alla M. Rozenblit, MD (5), Jorge
ENDOCRINE FORMS OF HYPERTENSION. Michael Stowasser
 ENDOCRINE FORMS OF HYPERTENSION Michael Stowasser Hypertension Unit, University Department of Medicine, Princess Alexandra Hospital, Brisbane 4102, Australia. ENDOCRINE FORMS OF HYPERTENSION Mineralocorticoid
ENDOCRINE FORMS OF HYPERTENSION Michael Stowasser Hypertension Unit, University Department of Medicine, Princess Alexandra Hospital, Brisbane 4102, Australia. ENDOCRINE FORMS OF HYPERTENSION Mineralocorticoid
27 F with new onset hypertension and weight gain. Rajesh Jain Endorama 10/01/2015
 27 F with new onset hypertension and weight gain Rajesh Jain Endorama 10/01/2015 HPI 27 F with hypertension x 1 year BP 130-140/90 while on amlodipine 5 mg daily She also reports weight gain, 7 LB, mainly
27 F with new onset hypertension and weight gain Rajesh Jain Endorama 10/01/2015 HPI 27 F with hypertension x 1 year BP 130-140/90 while on amlodipine 5 mg daily She also reports weight gain, 7 LB, mainly
Thyroid follicular neoplasms in cytology. Ulrika Klopčič Institute of Oncology, Department of Cytopathology, Ljubljana, Slovenia
 Thyroid follicular neoplasms in cytology Ulrika Klopčič Institute of Oncology, Department of Cytopathology, Ljubljana, Slovenia Lecture overview importance of FNAB in assessing thyroid lesions follicular
Thyroid follicular neoplasms in cytology Ulrika Klopčič Institute of Oncology, Department of Cytopathology, Ljubljana, Slovenia Lecture overview importance of FNAB in assessing thyroid lesions follicular
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life.
 B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
B. Environmental Factors. a. The major risk factor to papillary thyroid cancer is exposure to ionizing radiation, during the first 2 decades of life. b. Deficiency of dietary iodine: - Is linked with a
