Department of Pharmacology & NIPER-Guwahati, Gauhati Medical College & Hospital, Guwahati , Assam, INDIA. 3
|
|
|
- Cory Sharp
- 6 years ago
- Views:
Transcription
1 J Young Pharm, 2016; 8(2): A multifaceted peer reviewed journal in the field of Pharmacy Short Communication A study on drug induced Stevens-Johnson Syndrome (SJS), Toxic Epidermal Necrolysis (TEN) and SJS-TEN overlap in a tertiary care hospital of Northeast India Ratan J. Lihite, 1 Mangala Lahkar, 2 Ajoy Borah, 3 Debeeka Hazarika, 4 Sukhjinder Singh 5 1 Department of Pharmacology, ADR Monitoring Centre (Pharmacovigilance Programme of India, IPC-NCC, Ministry of Health & Family welfare, GoI), Gauhati Medical College & Hospital, Guwahati , Assam, INDIA. 2 Department of Pharmacology & NIPER-Guwahati, Gauhati Medical College & Hospital, Guwahati , Assam, INDIA. 3 Department of Pharmacology, Gauhati Medical College & Hospital, Guwahati , Assam, INDIA. 4 Department of Dermatology & STD, Gauhati Medical College & Hospital, Guwahati , Assam, INDIA. 5 Department of Pharmacy Practice, National Institute of Pharmaceutical Education & Research (NIPER) (Department of Pharmaceuticals, Ministry of Chemicals and Fertilizers, GoI), Guwahati , Assam, INDIA. ABSTRACT Background: Stevens Johnson syndrome (SJS), toxic epidermal necrolysis (TEN) and SJS-TEN overlap are rare, but potentially life-threatening, reactions to medications. From Northeast India, limited epidemiological data is available on these cutaneous drug reactions. Aims: The purpose of this study was to assess the drug-induced SJS/TEN cases of a tertiary care hospital of Northeast India. Methods: This cross sectional study was conducted in Gauhati Medical College and Hospital of Guwahati city, Northeast India. WHO UMC probability assessment system and ALDEN were used for causality assessment of reported SJS/TEN cases. Results are presented in percentage; mean (standard deviation), and median (interquartile range difference). Results: Forty five cases of drug induced SJS (42.22%), TEN (55.55%) & SJS-TEN (2.22%) overlap were reported. Out of these, 25 patients were males and 20 patients were females. The mean age of the patients was (17.57) year. The median time duration between drug intake and onset of symptoms for SJS/TEN was 25(4) and the median duration of hospital stay by patients was 13(8). The most offending groups of drugs were antimicrobials (35.55%), followed by anticonvulsants (28.89%), antipyretics (17.78%), and nonsteroidal anti-inflammatory drugs (6.67%). In individual drug category, paracetamol (17.77%) and phenytoin (15.55%) were among the commonly reported offending drugs. Altered liver function test was commonly reported complication in SJS/TEN patients. As per ALDEN, drug causality was very probable in 16 cases whereas by WHO-UMC assessment system, 1 case was certain while 29 cases were probable. Limitations: Statistical significance among the variables was not shown and large study sample may be required for interpretation of results to arrive at a definite conclusion. Conclusions: Antimicrobials, anticonvulsants, and antipyretics were commonly reported group of offending drugs to cause SJS/TEN in patients. Paracetamol & phenytoin were commonly reported individual offending drugs. Key words: SJS, TEN, Northeast India, Paracetamol, Anticonvulsants. Correspondence : Ratan J. Lihite, Department of Pharmacology, ADR Monitoring Centre, Gauhati Medical College and Hospital, Guwahati , Assam, INDIA. Phone on: r.lihite@yahoo.com DOI: /jyp INTRODUCTION Adverse drug reactions (ADR) accounts 6% of the total hospital admission, increases economic burden on healthcare system, results into withdrawal of drugs from market and death. 1,2 Among various ADR, cutaneous drug reactions mainly Stevens-Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) are rare but potentially fatal reactions endangers patient s life. These reactions are characterized by mucocutaneous tenderness, typically hemorrhagic erosions, erythema with more or less severe epidermal detachment presenting as blisters and areas of denuded skin. 3 In addition to the severe skin symptoms, both diseases are often accompanied by complications in numerous organs, such as the liver, kidney, and lung. Patient may initially present with SJS, which subsequently evolves into TEN or SJS-TEN overlap. Diagnosis mainly relies on clinical signs and histopathology of skin lesions. The exact pathogenesis of SJS and TEN remains to be elucidated but apoptotic mechanisms, including involvement of cytotoxic T cells, tumor necrosis factor (TNF)-α, and Fas (CD95), Fas ligand (FasL) interaction are considered to be relevant to these diseases. 4 As reported, the rate of occurrence of SJS & TEN to medications is low. 2,5 However, drugs are most commonly implicated for SJS, TEN and SJS-TEN overlap and other possible causes are infections, immunizations, environment chemicals and radiation therapy. 2,5 The incidence of SJS ranges from 1.2 to 6 patients per million per year, while for TEN it ranges from 0.4 to 1.2 patients per million per year. 6 The mortality for SJS varies from 3% to 10% and for TEN from 20% to 40%. 7 It was observed that still there is lack of studies on these cutaneous disorders from Northeast region of India as compare to other part of country. 2 This cross sectional study was conducted to assess drug-induced SJS, TEN and SJS-TEN overlap cases reported from a tertiary care hospital situated at Guwahati, Northeast India. In our study, cases with widespread purpuric macules and epidermal detachment below 10% are called SJS. Those with cutaneous detachment between 10% and 30% are called transitional SJS-TEN, and those with more than 30% epidermal detachment are designed TEN. 8 METHODS The permission from institutional ethical committee of Gauhati Medical College & Hospital, Guwahati (Northeast India) was obtained to conduct this study. Patients admitted between January 2011 and December 2014, and diagnosed with SJS, SJS/TEN overlap or TEN were identified from the hospital. The diagnosis of SJS, TEN, and SJS-TEN overlap was done according to the criteria laid down by Bastuji-Garin et al. 8 These cases were reported from inpatient departments of dermatology, paediatrics, gynaecology, medicine, psychiatry, neurology, haematology and intensive treatment unit of hospital. Those patients were excluded who complained of only symptoms without visible skin lesions, those who Journal of Young Pharmacists, Vol 8, Issue 2, Apr-Jun,
2 could not recall the name of the consumed drug, and other whose lesions turned out to be disease related (e.g. viral exanthems, rash of rickettsial infections, and collagen vascular disease) on closer examination. The patients who reported to have consumed ayurvedic and homeopathic drugs were also excluded as the herbal ingredients could not be identified in their case. We have collected data of those patients who had following details in a predesigned suspected ADR reporting form of Pharmacovigilance Programme of India. 9 Collected data included patient s age & sex, duration of hospital stay, the time period between the drug component intake & onset of eruption, suspected drug (drug notoriety), dechallenge and prechallenge/rechallenge of suspected drug, indication, and other complications. Drug that has been taken within four weeks preceding the onset of symptoms was considered as culprit drug. In present study, WHO-UMC probability assessment system and algorithm for assessment of drug causality in Epidermal Necrolysis (ALDEN) 10 were followed for assessing the causality of reported ADR cases. WHO UMC probability assessment system is generally used for drug causality assessment under Pharmacovigilance Programme of India; proposed by the WHO collaborating centre for international drug monitoring, the Uppsala Monitoring Centre (UMC), Sweden. 9 While using ALDEN, the index day (time lag from initiation of drug intake to onset of reaction) for all the reported cases were suggestive (+3) except one whose index day was 29, which was categorized as compatible (+2). The probability that the drug was present in the body at the time of the onset of the reaction was considered definite (0) for all the reported SJS/TEN cases. The suspected drug was withdrawn (dechallenge) after the onset of eruptions in all the SJS/TEN cases and prechallenge/rechallenge was not performed in any reported cases. The drug notoriety was performed as per the Euro SCAR study as high risk drug, lower risk drug and the drug of no evidence of association. 11 Statistical analysis: Descriptive statistics were used for data analysis. Mean (standard deviation) was calculated for normally distributed continuous variable whereas for non-normally distributed continuous variable, results are presented in median (interquartile range difference). RESULTS During study period, 45 cases of drug induced SJS (19/45, 42.22%), TEN (25/45, 55.55%) & SJS-TEN (1/45, 2.22%) overlap were reported. Total 25 males and 20 females were reported. Of these, 11 males & 8 females had SJS while 12 males & 13 females had TEN. Only 1 male patient of SJS-TEN overlap was reported. The mean age of the patients was (17.57) year. The youngest patient was of 4 year old child while oldest was of 83 year old. The median time duration between drug intake and onset of symptoms for SJS/TEN was 25(4) and the median duration of hospital stay by patients was 13(8). The causality assessment was performed using probability assessment systems of WHO-UMC and ALDEN. Drug causality was very probable in 16 cases by ALDEN whereas as per WHO-UMC assessment system, 1 case was certain while 29 cases were probable (Figure 1). The major group of drugs causing SJS/TEN were antimicrobials (16/45, 35.55%), anticonvulsants (13/45, 28.89%), antipyretics (8/45, 17.78%), nonsteroidal anti-inflammatory drugs (NSAIDs) (3/45, 6.67%), and anticancer drugs (2/45, 4.4%) (Table 1). Besides these, there were cases due to methotrexate, lenalidomide, allopurinol and reboxetine (Table 1). Figure 1: Drug causality assessment using ALDEN and WHO-UMC 150 Journal of Young Pharmacists, Vol 8, Issue 2, Apr-Jun, 2016
3 Table 1: Offending drugs with respect to reactions Offending drugs No. of patients with SJS No. of patients with TEN No. of patients with SJS-TEN overlap Total no. of patients (%) Antimicrobial drugs [5] [11] - 16 (35.5%) levofloxacin (fluoroquinolones) ceftazidime (3 rd cephalosporins) sulfamethizole (sulfonamides) cefixime (3 rd cephalosporins) cefuroxime (2 nd cephalosporins) ceftriaxone (3 rd cephalosporins) ofloxacin (fluoroquinolones) norfloxacin (fluoroquinolones) sulfasalazine (sulfonamides) metronidazole (antiamoebic) clofazimine (antileprotic) isoniazid (antitubercular drug) artesunate (antimalarial) efavirenz (antiretroviral) Anticonvulsants [6] [7] - 13 (28.89%) phenytoin sodium valproate carbamazepine NSAIDs [1] [1] [1] 3 (6.67%) etoricoxid aspirin ibuprofen Antipyretics [4] [4] - 8 (17.78%) paracetamol Antihistaminics [1] (2.2%) Sinarest (chlorpheniramine maleate 2 mg, phenylephrine hydrochloride 10 mg, paracetamol 500 mg, anhydrous caffeine 30 mg) Antigout agent -- [1] - 1(2.2%) allopurinol Anticancer drugs [2] (4.4%) lenalidomide methotrexate Antidepressant - [1] - 1 (2.2%) reboxetine Total One case of SJS-TEN overlaps was reported due to aspirin. Sinarest tablet containing chlorpheniramine maleate 2 mg, phenylephrine hydrochloride 10 mg, paracetamol 500 mg, and anhydrous caffeine 30 mg was taken over-the-counter by a patient and induced SJS. While considering individual drugs, paracetamol (8/45, 17.77%) & phenytoin (7/45, 15.55%) were among the commonly reported offending drugs (Table 1). The conditions for which patients took these offending drugs were seizure, high-grade fever, arthralgia, cerebrovascular accident, multiple myeloma, chronic diarrhoea, ovarian tumour, HIV, pulmonary tuberculosis, hansen s disease, malaria, cystic kidney disease, cervical spondylosis, paranoid schizophrenia, gout and depression. Various complications were observed in SJS, TEN and SJS-TEN overlap patients. Liver function test (20/45, 44.44%) followed by leukocytosis (15/45, 33.33%), neutrophilia (10/45, 22.22%), leukocytopenia (5/45, 11.11%), eosinophilia (5/45, 11.11%), neutropenia (3/45, 6.66%), thrombocytopenia (3/45, 6.66%), hypokalemia (2/45, 4.44%), and hyperglycemia (1/45, 2.22%) were reported. Other complications were secondary infections, ocular, electrolytes imbalance, gastritis, oral candidiasis, pulmonary edema, respiratory distress, lung abscess, psychosis, septicaemia, and acute renal failure. In treatment, almost all patients have received systemic steroid comprised of dexamethasone (29/45, 64.44%), prednisolone (14/45, 31.11%), and prednisolone and dexamethasone pulse therapy (2/45, 8.88%). Journal of Young Pharmacists, Vol 8, Issue 2, Apr-Jun,
4 DISCUSSION In our study, male preponderance (55.6% male and 44.4% female) was observed, unlike female preponderance from previous studies The mean age in previous studies were varied from 22 to 50 year 5,15-18 whereas in our study, most of the patients (62.22%) were beyond 21 year of age and mean age was year. Duration between the drug intake and first onset of symptom in SJS/TEN ranges between few hours and 45 days, and the period of hospitalization ranges from 5 to 31 days. 19 In our study, the median time duration between drug intake and onset of symptoms (25), and the median duration of hospital stay (13) were within these ranges. In several studies, antimicrobials, anticonvulsants and NSAIDs were the most common group of drugs causing SJS, TEN and SJS-TEN overlap Similarly in our study, antimicrobials were commonly reported group of drugs followed by anticonvulsants, antipyretics, and NSAIDs. Sixteen patients (35.5%) had experienced SJS/TEN due to antimicrobials. The majority of TEN cases (44%) were due to antimicrobials which was in concordance with the studies from (42%) West Germany 13 & (44%) South India. 19 Penicillins and cephalosporins were the commonly reported causative drugs from Japan & Singapore. 17,18 In present study, among β-lactam antibiotics, cephalosporins were implicated in 4 cases. Fluoroquinolones were commonly reported from Indian state, Gujarat & Karnataka. 2,5 Antibacterial sulphonamides were the most common offending drugs reported from Lome, Togo. 15 In our study, 3 cases were reported due to fluoroquinolones (ofloxacin, norfloxacin, and levofloxacin) and 2 cases were reported due to sulphonamides (sulfamethizole and sulfasalazine). Anticonvulsants (28.89%) were second most commonly reported offending drugs for SJS/TEN. Among them, phenytoin was the commonly reported offending drug followed by carbamazepine and sodium valproate. Phenytoin and carbamazepine are most common anti epileptic drugs reported for SJS/TEN in Asian population. 20 As reported, the risk of developing SJS/TEN in patients who carries HLA-B*1502 allele is very high. 21 Therefore, drug controller authority of India has instructed manufacturers to include SJS in package inserts of the product containing carbamazepine and advised to screen the patients for HLA-B*1502 allele before initiating treatment with carbamazepine. 9 Sodium valproate is rarely reported as an offending drug in literature 2 whereas in present study, 3 cases were reported due to sodium valproate. Eight cases of SJS/TEN were reported due to paracetamol which was in concordance with the study from Gujarat, India. 2 NSAIDs were commonly reported offending drugs from France. 22 In present study, 3 cases of SJS/TEN were reported due to NSAIDs (etoricoxib, aspirin, and ibuprofen). It was observed that patients often took an analgesic or antipyretic agent to treat unspecific symptoms such as fever or pain, which might be early sign of SJS/TEN or indication for an infection. Therefore, there was always doubt for any causal relation for analgesics or antipyretics. HIV is a most common co-morbid condition in the patients of SJS/TEN 2 and mortality is also very high in these patients. 15 Among antiretrovirals, nevirapine is commonly reported causative drug 15,19 whereas in this study 1 case of efavirenz-induced TEN was reported. HLA-B*5801 allele is another genetic marker reported to have strong association with allopurinol-induced SJS/TEN. 21 In Europe & Asia, allopurinol is commonly reported offending drug for SJS & TEN 18 whereas in present study, only 1 case of allopurinol-induced TEN was reported. Few cases of SJS/TEN due to antituberculars (isoniazid), cytotoxic drugs (lenalidomide, methotrexate), antimalarials (artesunate), antileprotics (clofazimine), antiamoebic (metronidazole) and antidepressant (reboxetine) were also reported in our study. Considering their widespread use across India, risk seems minimal. The most common complications in SJS/TEN patients are septicemia, secondary infections, pneumonitis and acute renal failure. 2 In our study, secondary infection was the most common complication in SJS/TEN patients. Beside this, altered liver functions, hematological, electrolytes, hyperglycemia and renal functions were also the conditions reported in this study. It was observed that the use of ALDEN requires good data. This algorithm is specific to SJS and TEN because it includes some characteristic that are specific to these disease. A precise clinical history of the patient is needed to determine the index day and to document alteration in liver and kidney function because these are taken into account in determining the presence of the drug in the body at the time of onset of the adverse reaction. 10 In our study, as per ALDEN, drug causality was very probable in 16 cases and was probable in 14 cases. However, only 1 case was certain and 29 cases were probable by WHO-UMC system. CONCLUSION Antimicrobials, anticonvulsants and antipyretics were commonly reported offending group of drugs for SJS/TEN in patients. Paracetamol (8/45) & phenytoin (7/45) were commonly reported offending drugs in individual drug category. Most of the cases were categorized very probable as per ALDEN whereas by WHO-UMC causality assessment system most of the cases were probable. Since the number of cases studied is less, it warrants further research. ACKNOWLEDGEMENTS Authors would like to thank post graduate trainees of Department of Dermatology & STD, Gauhati Medical College & Hospital, Guwahati-32, Northeast India for reporting adverse drug reactions. Authors also like to acknowledge National Coordination Centre-Pharmacovigilance programme of India, Indian Pharmacopoeia Commission, Ministry of Health & Family Welfare, Govt. of India for permitting us to conduct this study. CONFLICT OF INTEREST The author declare no conflict of interest. ABBREVIATIONS USED SJS: Stevens Johnson syndrome; TEN: toxic epidermal necrolysis; ADR: adverse drug reactions; TNF: tumor necrosis factor; FasL: Fas ligand; ALDEN: assessment of drug causality in epidermal necrolysis; WHO: World Health Organization; UMC: uppsala monitoring centre; NSAIDs: nonsteroidal anti-inflammatory drugs. ABOUT AUTHOR Ratan J. Lihite: is a Technical Associate under Indian Pharmacopoeia Commission, Ministry of Health and Family Welfare, Govt. of India posted at ADR Monitoring Centre, Department of Pharmacology, Gauhati Medical College, Guwahati-32, Assam, Northeast India. He did his post graduation from Department of Pharmacy Practice, National Institute of Pharmaceutical Education and Research (NIPER)-Guwahati, Northeast India and has well experience in the area of pharmacovigilance and clinical pharmacology. Certificate of appreciation was bestowed by Drugs Controller General of India (DCGI), Hon ble Dr. G.N. Singh for his valuable contribution in the Pharmacovigilance Programme of India (PvPI) at Indian Pharmacopoeia Commission in Journal of Young Pharmacists, Vol 8, Issue 2, Apr-Jun, 2016
5 REFERENCES 1. Svensson CK, Cowen EW, Gaspari AA. Cutaneous Drug Reactions. Pharmacological Reviews. 2001;53(3): Patel TK, Barvaliya MJ, Sharma D, Tripathi C. A systematic review of the druginduced Stevens-Johnson syndrome and toxic epidermal necrolysis in Indian population. Indian J Dermatol Venereol Leprol. 2013;79(3): Harr T, French LE. Toxic epidermal necrolysis and Stevens-Johnson syndrome. Orphanet J Rare Dis. 2010;5(1): Saha K. Toxic epidermal necrolysis: Current concepts in pathogenesis and treatment. Indian Dermatol Venereol Leprol. 2000;66(1): Naveen KN, Pai VV, Rai V, Athanikar SB. Retrospective analysis of Steven Johnson syndrome and toxic epidermal necrolysis over a period of 5 years from northern Karnataka, India. Indian J Pharmacol. 2013;45(1): Wolkenstein P, Revuz J. Drug-induced severe skin reactions. Incidence, manage ment and prevention. Drug Saf. 1995;13(1): Mokenhaupt M, Schopf E. Epidemiology of drug-induced severe skin reactions. Semin Cutan Med Surg. 1996;15(4): Bastuji-Garin S, Rzany B, Stern RS, Shear NH, Naldi L, Raujeau JC. Clinical classi fication of cases of toxic epidermal necrolysis, Stevens Johnson Syndrome and erythema multiforme. Arch Dermatol. 1993;129(1): Lihite RJ, Lahkar M. An update on Pharmacovigilance Programme of India. Front Pharmacol. 2015;6: Ameen KH, Pinninti R, Jami S. Aceclofenac induced Stevens-Johnson/toxic epidermal necrolysis overlap syndrome. J Pharmacol Pharmacother. 2013;4(1): Mockenhaupt M, Viboud C, Dunant A, Naldi L, Halevy S, Bouwes BJN, et al. Steven-Johnson syndrome and toxic epidermal necrolysis: assessment of medication risks with emphasis on recently marketed drugs. The Euro SCARstudy. J Invest Dermatol. 2008;128(1); Devi K, George S, Criton S, Suja V, Sridevi PK. Carbamazepine The commonest cause of toxic epidermal necrolysis and Stevens-Johnson syndrome: A study of 7 years. Indian J Dermatol Venereol Leprol. 2005;71(5): Schopf E, Stuhmer A, Rzany B, Victor N, Zentgraf R, Kapp JF. Toxic epidermal necrolysis and Stevens-Johnson syndrome: An epidemiologic study from West Germany. Arch Dermatol.1991;127(6): Lihite RJ, Lahkar M. A Study on Cutaneous Adverse Drug Reactions in ADR Monitoring Centre of Tertiary Care Hospital, Guwahati. J App Pharm Sci. 2013;3(3): Saka B, Kombate K, Mouhari-Toure A, Akakpo S, Tchangai-Walla K, Pitche P. Stevens-Johnson syndrome and toxic epidermal necrolysis in a teaching hospital in Lome, Togo: retrospective study of 89 cases. Med Trop (Mars). 2010;70(3): Chen J, Wang B, Zeng Y, Xu H. High-dose intravenous immunoglobulins in the treatment of Stevens-Johnson syndrome and toxic epidermal necrolysis in Chinese patients: a retrospective study of 82 cases. Eur J Dermatol. 2010;20(6): Yamane Y, Aihara M, Ikezawa Z. Analysis of Stevens-Johnson syndrome and toxic epidermal necrolysis in Japan from 2000 to Allergol Int. 2007;56(4): Tan SK, Tay YK. Profile and pattern of Stevens-Johnson syndrome and toxic epidermal necrolysis in a general hospital in Singapore: treatment outcomes. Acta Derm Venereol. 2012;92(1): Sanmarkan AD, Sori T, Thappa DM, Jaisankar TJ. Retrospective Analysis of Stevens-Johnson syndrome and Toxic Epidermal Necrolysis over a Period of 10 Years. Indian J Dermatol. 201;56(1): Yang CY, Dao RL, Lee TJ, Lu CW, Yang CH, Hung SI, et al. Severe cutaneous adverse reactions to antiepileptic drugs in Asians. Neurology. 2011;77 (23): Chung WH, Hung SI. Genetic Markers and Danger Signals in Stevens-Johnson syndrome and Toxic Epidermal Necrolysis. Allergology International. 2010; 59(4): Roujeau JC, Guillaume JC, Fabre JP, Penso D, Fléchet ML, Girre JP. Toxic epidermal necrolysis (Lyell Syndrome): Incidence and drug etiology in France, Arch Dermatol. 1990;126(1): Journal of Young Pharmacists, Vol 8, Issue 2, Apr-Jun,
Prevalence and pattern of adverse cutaneous drug reactions presenting to a tertiary care hospital
 International Journal of Research in Dermatology Janardhan B et al. Int J Res Dermatol. 2017 Mar;3(1):74-78 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20164248
International Journal of Research in Dermatology Janardhan B et al. Int J Res Dermatol. 2017 Mar;3(1):74-78 http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20164248
Correspondence should be addressed to Wanjarus Roongpisuthipong; rr
 Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Dermatology Research and Practice, Article ID 237821, 5 pages http://dx.doi.org/10.1155/2014/237821 Research Article Retrospective Analysis of Corticosteroid Treatment in Stevens-Johnson Syndrome and/or
Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course
 Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Southern Adventist Univeristy KnowledgeExchange@Southern Graduate Research Projects Nursing 12-4-2015 Stevens Johnson Syndrome: How Diagnosis Impacts Disease Course Sharon K. Hart Southern Adventist University,
Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review
 Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review Yap FBB, MRCP; Wahiduzzaman M, MBBS; Pubalan M, MRCP. Egyptian Dermatology Online Journal 4 (1): 1,
Stevens - Johnson syndrome (SJS) and Toxic Epidermal Necrolysis (TEN) In Sarawak: A Four Years Review Yap FBB, MRCP; Wahiduzzaman M, MBBS; Pubalan M, MRCP. Egyptian Dermatology Online Journal 4 (1): 1,
allergy Asia Pacific Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from
 pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
pissn -876 eissn -868 Original Article Asia Pac Allergy 6;6:-7 Stevens-Johnson syndrome and toxic epidermal necrolysis in Dr. Hasan Sadikin General Hospital Bandung, Indonesia from 9 Oki Suwarsa *, Wulan
A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome
 Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
Open Journal of Clinical & Medical Case Reports Volume 2 (2016) Issue 11 A Case Report on Amoxicillin Induced Stevens- Johnson Syndrome Rajendra Singh Airee*; Aastha Rawal; Binu Mathew; H. Doddayya Abstract
1 Introduction. Kenneth Irungu 1 David Nyamu
 Drugs - Real World Outcomes (2017) 4:79 85 DOI 10.1007/s40801-017-0105-x ORIGINAL RESEARCH ARTICLE Characterization of Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Among Patients Admitted to
Drugs - Real World Outcomes (2017) 4:79 85 DOI 10.1007/s40801-017-0105-x ORIGINAL RESEARCH ARTICLE Characterization of Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Among Patients Admitted to
CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
 WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
WORLD JOURNAL OF PHARMACY AND PHARMACEUTICAL SCIENCES Ragesh SJIF Impact Factor 2.786 Volume 3, Issue 6, 1599-1604. Case Study ISSN 2278 4357 CARBAMAZEPINE INDUCED STEVENS JOHNSON SYNDROME- A CASE STUDY
Original Article. Barvaliya M, Sanmukhani J, Patel T, Paliwal N, Shah H 1, Tripathi C
 Original Article Drug-induced Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and SJS-TEN overlap: A multicentric retrospective study Barvaliya M, Sanmukhani J, Patel T, Paliwal N, Shah
Original Article Drug-induced Stevens-Johnson syndrome (SJS), toxic epidermal necrolysis (TEN), and SJS-TEN overlap: A multicentric retrospective study Barvaliya M, Sanmukhani J, Patel T, Paliwal N, Shah
PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS
 PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS M. Ghaffarpour *, S. S. Hejazie, M. H. Harirchian and H. Pourmahmoodian Department of Neurology, Imam Khomeini Hospital,
PHENYTION, CARBAMAZEPINE, SODIUM VALPROATE AND LAMOTRIGINE INDUCED CUTANEOUS REACTIONS M. Ghaffarpour *, S. S. Hejazie, M. H. Harirchian and H. Pourmahmoodian Department of Neurology, Imam Khomeini Hospital,
Address for correspondence: Dr. Patel Raksha M. R-3, Doctor s Quarters, Jail Road, Vadodara- 01, Gujarat, India.
 Clinical study of cutaneous drug eruptions in 200 patients Raksha M. Patel, Y. S. Marfatia Department of Skin and V.D, Medical College, Vadodara, Gujarat, India Address for correspondence: Dr. Patel Raksha
Clinical study of cutaneous drug eruptions in 200 patients Raksha M. Patel, Y. S. Marfatia Department of Skin and V.D, Medical College, Vadodara, Gujarat, India Address for correspondence: Dr. Patel Raksha
Profile and Pattern of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in a General Hospital in Singapore: Treatment Outcomes
 Acta Derm Venereol 2012; 92: 62 66 CLINICAL REPORT Profile and Pattern of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in a General Hospital in Singapore: Treatment Outcomes Siew-Kiang Tan and
Acta Derm Venereol 2012; 92: 62 66 CLINICAL REPORT Profile and Pattern of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in a General Hospital in Singapore: Treatment Outcomes Siew-Kiang Tan and
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT
 OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
OXCARBAZEPINE-INDUCED STEVENS-JOHNSON SYNDROME: A CASE REPORT Lung-Chang Lin, 1,2 Ping-Chin Lai, 3 Sheau-Fang Yang, 4 and Rei-Cheng Yang 1,5 Departments of 1 Pediatrics and 4 Pathology, Kaohsiung Medical
Dilantin (phenytoin) ROBERT A. SCHWARTZ
 Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Dilantin (phenytoin) ROBERT A. SCHWARTZ Bailey & Galyen Attorney in Charge, Mass Tort Litigation Managing Attorney, Houston 18333 Egret Bay Blvd., Suite 120 Houston, Texas 77058 Toll Free: (866) 715-1529
Emergency Dermatology Dr Melissa Barkham
 Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Emergency Dermatology Dr Melissa Barkham Spotlight Seminar 30 th September 2010 Why is this important? Urgent recognition and treatment of dermatologic emergencies can be life saving and prevent long term
Drug Allergy A Guide to Diagnosis and Management
 Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Drug Allergy A Guide to Diagnosis and Management (Version 1 April 2015 updated April 2018) Author: Jed Hewitt Chief Pharmacist, Governance & Professional Practice Date of Preparation: April 2015 Updated:
Analysis of Cutaneous Adverse Drug Reactions at a Tertiary Care Hospital a Prospective Study
 Tropical Journal of Pharmaceutical Research August 2011; 10 (4): 517-522 Pharmacotherapy Group, Faculty of Pharmacy, University of Benin, Benin City, 300001 Nigeria. All rights reserved. Available online
Tropical Journal of Pharmaceutical Research August 2011; 10 (4): 517-522 Pharmacotherapy Group, Faculty of Pharmacy, University of Benin, Benin City, 300001 Nigeria. All rights reserved. Available online
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW
 SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
SKIN REACTIONS WITH PSYCHOTROPICS: A SYSTEMATIC REVIEW *Anderson Isaac, PharmD Candidate, 2019 Pooja Patel, PharmD Candidate, 2019 Katelyn Thomasson, PharmD Candidate, 2019 Erika Tillery, PharmD, BCPP,
Adverse cutaneous drug reactions: Clinical pattern and causative agents in a tertiary care center in South India
 Study Adverse cutaneous drug reactions: Clinical pattern and causative agents in a tertiary care center in South India David Pudukadan, Devinder Mohan Thappa Department of Dermatology and STD, Jawaharlal
Study Adverse cutaneous drug reactions: Clinical pattern and causative agents in a tertiary care center in South India David Pudukadan, Devinder Mohan Thappa Department of Dermatology and STD, Jawaharlal
Adverse Drug Reactions pattern in a tertiary level teaching hospital: A Retrospective Study
 Original Article Adverse Drug Reactions pattern in a tertiary level teaching hospital: A Retrospective Study Anita Gupta, Anjleen Kaur, Prashant Shukla*, Hema Chhabra Department of Pharmacology, Government
Original Article Adverse Drug Reactions pattern in a tertiary level teaching hospital: A Retrospective Study Anita Gupta, Anjleen Kaur, Prashant Shukla*, Hema Chhabra Department of Pharmacology, Government
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review
 Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Title: Cutaneous Adverse Drug Reactions in Indian population: A systematic review Review question(s) To carry out a systematic review of the published evidence of the cutaneous adverse drug reactions in
Adverse Drug Reactions (ADRs) Outline
 Adverse Drug Reactions (ADRs) Outline 1. What are Adverse Drug Reactions (ADRs)? WHAT WHY HOW 2. How important are ADRs and are they preventable? 3. What are the classifications and mechanisms of ADRs?
Adverse Drug Reactions (ADRs) Outline 1. What are Adverse Drug Reactions (ADRs)? WHAT WHY HOW 2. How important are ADRs and are they preventable? 3. What are the classifications and mechanisms of ADRs?
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening
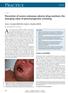 CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
CMAJ Cases Prevention of severe cutaneous adverse drug reactions: the emerging value of pharmacogenetic screening Suran L. Fernando MB BS PhD, Andrew J. Broadfoot MB BS Previously published at www.cmaj.ca
Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
 Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Case Reports in Immunology Volume 2012, Article ID 931528, 4 pages doi:10.1155/2012/931528 Case Report Cephazolin-Induced Toxic Epidermal Necrolysis Treated with Intravenous Immunoglobulin and N-Acetylcysteine
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update
 Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Stevens-Johnson s Syndrome / Toxic Epidermal Necrolysis: An update Robert G. Micheletti, MD Assistant Professor of Dermatology and Medicine Director, Cutaneous Vasculitis Clinic, Penn Vasculitis Center
Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection
 Case Report Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection J Med Assoc Thai 2015; 98 (Suppl. 7): S243-S247 Full text. e-journal:
Case Report Carbamazepine-Induced Incomplete Stevens-Johnson Syndrome: Report of a Case in Children without Mycoplasma pneumoniae Infection J Med Assoc Thai 2015; 98 (Suppl. 7): S243-S247 Full text. e-journal:
Stevens-Johnson syndrome (SJS) and toxic epidermal. necrolysis in Asian children
 Stevens-Johnson syndrome and toxic epidermal necrolysis in Asian children Mark Jean-Aan Koh, MD, and Yong-Kwang Tay, MD Singapore Background: Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis
Stevens-Johnson syndrome and toxic epidermal necrolysis in Asian children Mark Jean-Aan Koh, MD, and Yong-Kwang Tay, MD Singapore Background: Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis
Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review
 140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
140 Taiwanese Journal of Psychiatry (Taipei) Vol. 25 No. 3 2011 Overview Risk Factors and Management of Mood Stabilizer-associated Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis: A Mini-review Gen-Tang
Analysis of Individual Case Safety Reports of Severe Cutaneous Adverse Reactions in Korea
 Original Article Yonsei Med J 2019 Feb;60(2):208-215 pissn: 0513-5796 eissn: 1976-2437 Analysis of Individual Case Safety Reports of Severe Cutaneous Adverse Reactions in Korea Min-Gyu Kang 1,2,3, Kyung-Hee
Original Article Yonsei Med J 2019 Feb;60(2):208-215 pissn: 0513-5796 eissn: 1976-2437 Analysis of Individual Case Safety Reports of Severe Cutaneous Adverse Reactions in Korea Min-Gyu Kang 1,2,3, Kyung-Hee
A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive Patients
 Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Journal of US-China Medical Science 12 (2015) 85-89 doi: 10.17265/1548-6648/2015.02.008 D DAVID PUBLISHING A Retrospective Study of Spectrum of Nevirapine Induced Cutaneous Drug Reactions in HIV Positive
Analysis of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in Japan from 2000 to 2006 Yumiko Yamane 1, Michiko Aihara 1 and Zenro Ikezawa 1
 Allergology International. 7;:9- DOI:. allergolint.o-7- ORIGINAL ARTICLE Analysis of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in Japan from to Yumiko Yamane, Michiko Aihara and Zenro Ikezawa
Allergology International. 7;:9- DOI:. allergolint.o-7- ORIGINAL ARTICLE Analysis of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in Japan from to Yumiko Yamane, Michiko Aihara and Zenro Ikezawa
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME
 EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
EFAVIRENZ ASSOCIATED STEVENS-JOHNSON SYNDROME To the Editor: Persons with human immunodeficiency virus (HIV) infection are highly susceptible to adverse dermatological reactions to specific medications
Research Pattern of adverse drug reactions reported to the regional Pharmacovigilance center at Nepal Medical College and Teaching Hospital, Kathmandu
 Research Pattern of adverse drug reactions reported to the regional Pharmacovigilance center at Nepal Medical College and Teaching Hospital, Kathmandu Durga Bista 1*, Bal Ram Shrestha 2, Prakash Rai 1,
Research Pattern of adverse drug reactions reported to the regional Pharmacovigilance center at Nepal Medical College and Teaching Hospital, Kathmandu Durga Bista 1*, Bal Ram Shrestha 2, Prakash Rai 1,
Pediatric Dermatology
 Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Pediatric Dermatology --------- Emergencies & Urgencies Nicholas V. Nguyen, M.D. Director, Pediatric Dermatology Disclosures In the past 12 months, I have had the following financial relationships with
Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis: a case report
 Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
Kasahara et al. BMC Nephrology (2017) 18:237 DOI 10.1186/s12882-017-0648-9 CASE REPORT Open Access Warfarin-induced toxic epidermal necrolysis in combination therapy of Henoch- Schönlein purpura nephritis:
SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC
 SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC Shasha Khairullah, Rokiah Che Ismail Department of Medicine, Faculty
SEVERE CUTANEOUS ADVERSE DRUG REACTIONS: STEVENS-JOHNSON SYNDROME AND TOXIC EPIDERMAL NECROLYSISA, A REPORT OF 4 CASES SEEN AT UMMC Shasha Khairullah, Rokiah Che Ismail Department of Medicine, Faculty
Cutaneous Drug Reactions
 Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
Cutaneous Drug Reactions Andrei Metelitsa, MD, FRCPC, FAAD Co-Director, Institute for Skin Advancement Clinical Associate Professor, Dermatology University of Calgary, Canada Copyright 2017 by Sea Courses
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES. R e g i S C A R PATIENT'S DATA. Age country of birth
 REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
REGISTRY OF SEVERE CUTANEOUS ADVERSE REACTIONS TO DRUGS AND COLLECTION OF BIOLOGICAL SAMPLES R e g i S C A R PATIENT'S DATA Initials of the patient date of birth Age country of birth Gender male female
A Case Report on Paracetamol Induced Generalized Fixed Drug Eruptions
 Human Journals Case report November 2016 Vol.:7, Issue:4 All rights are reserved by Dr. C Sugunakar Raju et al. A Case Report on Paracetamol Induced Generalized Fixed Drug Eruptions Keywords: Skin Eruptions,
Human Journals Case report November 2016 Vol.:7, Issue:4 All rights are reserved by Dr. C Sugunakar Raju et al. A Case Report on Paracetamol Induced Generalized Fixed Drug Eruptions Keywords: Skin Eruptions,
The liver and skin are two of the commonest
 AMERICAN ASSOCIATION FOR THE STUDY OFLIVERD I S E ASES HEPATOLOGY, VOL. 63, NO. 3, 2016 LIVER INJURY/REGENERATION Drug-Induced Liver Injury Associated With Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis:
AMERICAN ASSOCIATION FOR THE STUDY OFLIVERD I S E ASES HEPATOLOGY, VOL. 63, NO. 3, 2016 LIVER INJURY/REGENERATION Drug-Induced Liver Injury Associated With Stevens-Johnson Syndrome/Toxic Epidermal Necrolysis:
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Drug Allergy. These podcasts are designed to give medical students an overview of key topics in pediatrics. The audio
IJBCP International Journal of Basic & Clinical Pharmacology
 Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20171661 Original Research Article A study of cutaneous
Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20171661 Original Research Article A study of cutaneous
Skin Manifestations of Drug Reactions
 Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Skin Manifestations of Drug Reactions Dr Carol Hlela, Division of Dermatology Department of Medicine, University of Cape Town and Red Cross Children s Hospital What are the Skin Manifestations of Drug
Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review
 Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
Case Report Toxic Epidermal Necrolysis and SJS : Case Reports & Brief Review Deepali P. Mohite*, Satyajitraje Tekade*, Amol Gadbail*, M. S. Chaudhary** Abstract : Toxic epidermal necrolysis (TEN) and Stevens
A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit
 J Korean Surg Soc 0;:133-139 DOI:.414/jkss.0..3.133 원 저 A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit Departments of Surgery
J Korean Surg Soc 0;:133-139 DOI:.414/jkss.0..3.133 원 저 A Clinical Study of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis: Efficacy of Treatment in Burn Intensive Care Unit Departments of Surgery
International Journal of Basic & Clinical Pharmacology. Profile of cutaneous adverse drug reactions of carbamazepine
 Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175211 Original Research Article Profile of cutaneous
Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20175211 Original Research Article Profile of cutaneous
Causes and Treatment Outcomes of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in 82 Adult Patients
 original article korean j intern med 2012;27:203-210 pissn 1226-3303 eissn 2005-6648 Causes and Treatment Outcomes of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in 82 Adult Patients Hye-In
original article korean j intern med 2012;27:203-210 pissn 1226-3303 eissn 2005-6648 Causes and Treatment Outcomes of Stevens-Johnson Syndrome and Toxic Epidermal Necrolysis in 82 Adult Patients Hye-In
PACKAGE LEAFLET: INFORMATION FOR THE USER
 PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg Tablets sodium fusidate Read all of this leaflet carefully before you start taking this medicine because it contains important information for you.
PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg Tablets sodium fusidate Read all of this leaflet carefully before you start taking this medicine because it contains important information for you.
Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
 BRIEF COMMUNICATION http://dx.doi.org/10.4110/in.2016.16.4.256 pissn 1598-2629 eissn 2092-6685 Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
BRIEF COMMUNICATION http://dx.doi.org/10.4110/in.2016.16.4.256 pissn 1598-2629 eissn 2092-6685 Stevens Johnson Syndrome and Toxic Epidermal Necrolysis Associated with Acetaminophen Use during Viral Infections
New product information wording Extracts from PRAC recommendations on signals
 20 July 2017 EMA/PRAC/406976/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 3-6 July 2017 PRAC The
20 July 2017 EMA/PRAC/406976/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 3-6 July 2017 PRAC The
University Journal of Pre and Para Clinical Sciences
 ISSN 2455 2879 Volume 2 Issue 4 2016 CASE REPORT- A RARE CASE OF DAPSONE HYPERSENSITIVITY SYNDROME VINOTH KUMAR CHITTARANJAN Department of Pharmacology, MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL
ISSN 2455 2879 Volume 2 Issue 4 2016 CASE REPORT- A RARE CASE OF DAPSONE HYPERSENSITIVITY SYNDROME VINOTH KUMAR CHITTARANJAN Department of Pharmacology, MADRAS MEDICAL COLLEGE AND GOVERNMENT GENERAL HOSPITAL
Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital
 Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
Original article: Drug-induced stevens-johnson syndrome : Experience from a tertiary care hospital *Arjun R 1,Mahalingeshwara Bhat K P 2, Sara C 1 1 PG student in General Medicine, KS Hegde Medical Acadamy,
PEER REVIEW HISTORY ARTICLE DETAILS VERSION 1 - REVIEW
 PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
PEER REVIEW HISTORY BMJ Paediatrics Open publishes all reviews undertaken for accepted manuscripts. Reviewers are asked to complete a checklist review form and are provided with free text boxes to elaborate
Risk of Stevens Johnson syndrome and toxic epidermal necrolysis in new users of antiepileptics
 Risk of Stevens Johnson syndrome and toxic epidermal necrolysis in new users of antiepileptics Maja Mockenhaupt, MD; John Messenheimer, MD; Pat Tennis, PhD; and Juergen Schlingmann Abstract Background:
Risk of Stevens Johnson syndrome and toxic epidermal necrolysis in new users of antiepileptics Maja Mockenhaupt, MD; John Messenheimer, MD; Pat Tennis, PhD; and Juergen Schlingmann Abstract Background:
Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate
 Original Research Article Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate Manab Nandy 1, Sangeeta De 2*, Mustafa Asad 2, Nirmal
Original Research Article Analysis of causation of Stevens Johnson Syndrome in a patient of rheumatoid arthritis with increased dose of methotrexate Manab Nandy 1, Sangeeta De 2*, Mustafa Asad 2, Nirmal
HIV-Associated Toxic Epidermal Necrolysis at San Francisco General Hospital: A 13-Year Retrospective Review
 HIV Clinical Management HIV-Associated Toxic Epidermal Necrolysis at San Francisco General Hospital: A 13-Year Retrospective Review Journal of the International Association of Providers of AIDS Care 2017,
HIV Clinical Management HIV-Associated Toxic Epidermal Necrolysis at San Francisco General Hospital: A 13-Year Retrospective Review Journal of the International Association of Providers of AIDS Care 2017,
Severe cutaneous reactions to drugs in the setting of a general hospital *
 758 INVESTIGATION s Severe cutaneous reactions to drugs in the setting of a general hospital * Luciana Rosa Grando 1 Tatiana Aline Berger Schmitt 1 Renato Marchiori Bakos 1 DOI: http://dx.doi.org/10.1590/abd1806-4841.20142997
758 INVESTIGATION s Severe cutaneous reactions to drugs in the setting of a general hospital * Luciana Rosa Grando 1 Tatiana Aline Berger Schmitt 1 Renato Marchiori Bakos 1 DOI: http://dx.doi.org/10.1590/abd1806-4841.20142997
Severe cutaneous adverse reactions due to isoniazid in a HIV Positive patient
 Indian J Lepr 202, 84 : 227-232 Hind Kusht Nivaran Sangh, New Delhi http://www.ijl.org.in Case Report Severe cutaneous adverse reactions due to isoniazid in a HIV Positive patient BK Viswanath, P Ranka,
Indian J Lepr 202, 84 : 227-232 Hind Kusht Nivaran Sangh, New Delhi http://www.ijl.org.in Case Report Severe cutaneous adverse reactions due to isoniazid in a HIV Positive patient BK Viswanath, P Ranka,
PHARMACOVIGILANCE CELL Government Medical College, Bhavnagar, Gujarat.
 PHARMACOVIGILANCE CELL Introduction Pharmacovigilance is the science and activities relating to the detection, assessment, understanding and prevention of adverse effects or any other drugrelated problems.
PHARMACOVIGILANCE CELL Introduction Pharmacovigilance is the science and activities relating to the detection, assessment, understanding and prevention of adverse effects or any other drugrelated problems.
Drug eruptions and hepatic involvement: a study
 International Journal of Research in Dermatology http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183819 Drug eruptions and hepatic involvement:
International Journal of Research in Dermatology http://www.ijord.com Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4529.intjresdermatol20183819 Drug eruptions and hepatic involvement:
Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin
 Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
Turkish Journal of Cancer Vol. 32/ No. 4/2002 Stevens-Johnson Syndrome in patients receiving cranial irradiation and concomitant diphenylhydantoin ERKAN TOPKAN, FARUK ZORLU, MURAT GÜRKAYNAK Hacettepe University
A 10-years retrospective study on Severe Cutaneous Adverse Reactions (SCARs) in a tertiary hospital in Penang, Malaysia
 ORIGINAL ARTICLE A 10-years retrospective study on Severe Cutaneous Adverse Reactions (SCARs) in a tertiary hospital in Penang, Malaysia Chai Har Loo, MRCP, Wooi Chiang Tan, AdvMDerm, Yek Huan Khor, AdvMDerm,
ORIGINAL ARTICLE A 10-years retrospective study on Severe Cutaneous Adverse Reactions (SCARs) in a tertiary hospital in Penang, Malaysia Chai Har Loo, MRCP, Wooi Chiang Tan, AdvMDerm, Yek Huan Khor, AdvMDerm,
Agenda* The 9th International Congress on Cutaneous Adverse Drug Reactions (iscar 2015)
 1 of 5 Agenda* The 9th International Congress on Cutaneous Adverse Drug Reactions (iscar 2015) Co-chairs: Dr. Neil H. Shear at the 23rd World Congress of Dermatology in Vancouver, Canada. Division of Dermatology,
1 of 5 Agenda* The 9th International Congress on Cutaneous Adverse Drug Reactions (iscar 2015) Co-chairs: Dr. Neil H. Shear at the 23rd World Congress of Dermatology in Vancouver, Canada. Division of Dermatology,
Cutaneous Conditions Associated with Systemic Disease
 Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Cutaneous Conditions Associated with Systemic Disease Johnnie M Woodson, M.D., F.A.A.D. Assistant Professor of Dermatology University of Nevada School of Medicine Director of J. Woodson Dermatology & Associates,
Lam0 trig he-induced Severe Cutaneous Adverse Reactions
 Epilepsia, 39(Suppl. 7):S22-S26, 1998 Lippincott Williams & Wilkins, Philadelphia 0 International League Against Epilepsy Lam0 trig he-induced Severe Cutaneous Adverse Reactions *Raymond G. Schlienger,
Epilepsia, 39(Suppl. 7):S22-S26, 1998 Lippincott Williams & Wilkins, Philadelphia 0 International League Against Epilepsy Lam0 trig he-induced Severe Cutaneous Adverse Reactions *Raymond G. Schlienger,
Your letter Your reference The Hague, Subject Request for change in the product information following the PhVWP/CMDh decision
 Registratiehouder ( t.a.v. registratieafdeling) Your letter Your reference The Hague, -- --.. Case number Our reference../../ Case manager Telephone number Subject Request for change in the product information
Registratiehouder ( t.a.v. registratieafdeling) Your letter Your reference The Hague, -- --.. Case number Our reference../../ Case manager Telephone number Subject Request for change in the product information
Severe cutaneous adverse reactions: an evidence based approach
 Original Article 21 Severe cutaneous adverse reactions: an evidence based approach D.P. Shrestha, D. Gurung, A. Kumar Department of Dermatology and Venereology, Maharagunj Campus, Institute of Medicine,
Original Article 21 Severe cutaneous adverse reactions: an evidence based approach D.P. Shrestha, D. Gurung, A. Kumar Department of Dermatology and Venereology, Maharagunj Campus, Institute of Medicine,
REVIEW ARTICLES ADVERSE DRUG REACTION: A COMMON DERMATOLOGICAL EMERGENCY
 REVIEW ARTICLES ADVERSE DRUG REACTION: A COMMON DERMATOLOGICAL EMERGENCY LUBNA KHONDKER 1, MD ABDUL WAHAB 2, MD SHIRAJUL ISLAM KHAN 3. Abstract In the evaluation of patients with a history of adverse cutaneous
REVIEW ARTICLES ADVERSE DRUG REACTION: A COMMON DERMATOLOGICAL EMERGENCY LUBNA KHONDKER 1, MD ABDUL WAHAB 2, MD SHIRAJUL ISLAM KHAN 3. Abstract In the evaluation of patients with a history of adverse cutaneous
Cutaneous adverse drug reactions in a tertiary care hospital
 Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 202, 4 (2):408-43 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-507 USA CODEN: DPLEB4 Cutaneous
Available online at www.scholarsresearchlibrary.com Scholars Research Library Der Pharmacia Lettre, 202, 4 (2):408-43 (http://scholarsresearchlibrary.com/archive.html) ISSN 0975-507 USA CODEN: DPLEB4 Cutaneous
An unpredictable, dose-independent adverse drug reaction which is immunologically or IgEmediated.
 R H E U M A T I S M D I S O R D E R S A N D A L L E R G I E S APPROACH TO DRUG ALLERGY Dr Bernard Thong DEFINITION OF DRUG ALLERGY An unpredictable, dose-independent adverse drug reaction which is immunologically
R H E U M A T I S M D I S O R D E R S A N D A L L E R G I E S APPROACH TO DRUG ALLERGY Dr Bernard Thong DEFINITION OF DRUG ALLERGY An unpredictable, dose-independent adverse drug reaction which is immunologically
Cutaneous drug eruptions are seen commonly
 REVIEW ARTICLE Cutaneous drug reactions in children Sandipan Dhar, Raghubir Banerjee, Rajib Malakar Department of Pediatric Dermatology, Institute of Child Health, Kolkata, West Bengal, India ABSTRACT
REVIEW ARTICLE Cutaneous drug reactions in children Sandipan Dhar, Raghubir Banerjee, Rajib Malakar Department of Pediatric Dermatology, Institute of Child Health, Kolkata, West Bengal, India ABSTRACT
cipro loxacin; stevens-johnson syndrome; urinary tract infection; adverse drug reaction
 Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 7 ISSN 2379-1039 Cipro loxacin induced Stevens Johnson syndrome: A case report on Dermatology department P Mohammed Sha i*; K Narotham
Open Journal of Clinical & Medical Case Reports Volume 3 (2017) Issue 7 ISSN 2379-1039 Cipro loxacin induced Stevens Johnson syndrome: A case report on Dermatology department P Mohammed Sha i*; K Narotham
Herbal and homeopathic products, often considered natural and non-toxic, can also cause adverse drug reactions.
 Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
Idiosyncratic and potentially serious cutaneous adverse drug reactions (CADRs), although relatively rare, account for significant morbidity and mortality. RANNAKOE J LEHLOENYA, BSc, MB ChB, FCDerm (SA)
Fluconazole erythema multiforme
 Fluconazole erythema multiforme Search 1. Eur J Dermatol. 2012 Sep-Oct;22(5):693-4. doi: 10.1684/ejd.2012.1806. Fluconazoleinduced fixed drug eruption imitating herpes labialis with erythema multiforme.
Fluconazole erythema multiforme Search 1. Eur J Dermatol. 2012 Sep-Oct;22(5):693-4. doi: 10.1684/ejd.2012.1806. Fluconazoleinduced fixed drug eruption imitating herpes labialis with erythema multiforme.
STEVEN JOHNSON S SYNDROME: A BRIEF REVIEW
 STEVEN JOHNSON S SYNDROME: A BRIEF REVIEW G. Ramya sree*, Sreeram Vandavasi Guru 1, E. Sam Jeeva Kumar 2 * Pharm D, Intern, P. Rami Reddy Memorial College of Pharmacy, Kadapa. 1 Pharm-D Intern, P. Rami
STEVEN JOHNSON S SYNDROME: A BRIEF REVIEW G. Ramya sree*, Sreeram Vandavasi Guru 1, E. Sam Jeeva Kumar 2 * Pharm D, Intern, P. Rami Reddy Memorial College of Pharmacy, Kadapa. 1 Pharm-D Intern, P. Rami
New product information wording Extracts from PRAC recommendations on signals
 12 October 2017 EMA/PRAC/610988/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 25-29 September 2017
12 October 2017 EMA/PRAC/610988/2017 Pharmacovigilance Risk Assessment Committee (PRAC) New product information wording Extracts from PRAC recommendations on signals Adopted at the 25-29 September 2017
Severe Cutaneous Adverse Reactions Related to Systemic Antibiotics
 MAJOR ARTICLE Severe Cutaneous Adverse Reactions Related to Systemic Antibiotics Ying-Fang Lin, 1 Chih-Hsun Yang, 2,3 Hu Sindy, 1,3 Jing-Yi Lin, 2,3 Chung-Yee Rosaline Hui, 2,3 Yun-Chen Tsai, 2 Ting-Shu
MAJOR ARTICLE Severe Cutaneous Adverse Reactions Related to Systemic Antibiotics Ying-Fang Lin, 1 Chih-Hsun Yang, 2,3 Hu Sindy, 1,3 Jing-Yi Lin, 2,3 Chung-Yee Rosaline Hui, 2,3 Yun-Chen Tsai, 2 Ting-Shu
Toxic epidermal necrolysis and Stevens Johnson syndrome in South Africa: a 3-year prospective study
 Q J Med 2012; 105:839 846 doi:10.1093/qjmed/hcs078 Advance Access Publication 28 April 2012 Toxic epidermal necrolysis and Stevens Johnson syndrome in South Africa: a 3-year prospective study S.M.H. KANNENBERG
Q J Med 2012; 105:839 846 doi:10.1093/qjmed/hcs078 Advance Access Publication 28 April 2012 Toxic epidermal necrolysis and Stevens Johnson syndrome in South Africa: a 3-year prospective study S.M.H. KANNENBERG
PACKAGE LEAFLET: INFORMATION FOR THE USER
 PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg/5 ml Oral Suspension fusidic acid Read all of this leaflet carefully before you start taking this medicine because it contains important information
PACKAGE LEAFLET: INFORMATION FOR THE USER Fucidin 250 mg/5 ml Oral Suspension fusidic acid Read all of this leaflet carefully before you start taking this medicine because it contains important information
IJBCP International Journal of Basic & Clinical Pharmacology. Pharmacovigilance study in medicine department in a tertiary care hospital
 Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20164133 Original Research Article Pharmacovigilance
Print ISSN: 2319-2003 Online ISSN: 2279-0780 IJBCP International Journal of Basic & Clinical Pharmacology DOI: http://dx.doi.org/10.18203/2319-2003.ijbcp20164133 Original Research Article Pharmacovigilance
A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash
 CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
CLINICAL CASE OF THE MONTH A Middle-Aged Man with Newly Diagnosed HIV Infection and Rash Patrick Njoku, MD; Temeka Tate, MD; Sousan Zadeh, MD; Erin Hauck, MD; Anila Chaudhry, MD; Betty Lo-Blais, MD; Lee
Chemotherapy Induced Adverse Drug Reactions in Cancer Patients in a Tertiary Care Hospital in South India
 J Young Pharm, 2017; 9(4): 593-597 A multifaceted peer reviewed journal in the field of Pharmacy www.jyoungpharm.org www.phcog.net Original Article Chemotherapy Induced Adverse Drug Reactions in Cancer
J Young Pharm, 2017; 9(4): 593-597 A multifaceted peer reviewed journal in the field of Pharmacy www.jyoungpharm.org www.phcog.net Original Article Chemotherapy Induced Adverse Drug Reactions in Cancer
PACKAGE LEAFLET: INFORMATION FOR THE USER. EASOFEN MAX STRENGTH 400mg FILM-COATED TABLETS. Ibuprofen
 PACKAGE LEAFLET: INFORMATION FOR THE USER EASOFEN MAX STRENGTH 400mg FILM-COATED TABLETS Ibuprofen Read all of this leaflet carefully before you start taking Easofen Max Strength Tablets because it contains
PACKAGE LEAFLET: INFORMATION FOR THE USER EASOFEN MAX STRENGTH 400mg FILM-COATED TABLETS Ibuprofen Read all of this leaflet carefully before you start taking Easofen Max Strength Tablets because it contains
Oral Acetazolamide after Boston Keratoprosthesis in Stevens Johnson Syndrome
 Oral Acetazolamide after Boston Keratoprosthesis in Stevens Johnson Syndrome The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Oral Acetazolamide after Boston Keratoprosthesis in Stevens Johnson Syndrome The Harvard community has made this article openly available. Please share how this access benefits you. Your story matters
Toxic epidermal necrolysis
 REVIEW Anaesthesiology Intensive Therapy 2015, vol. 47, no 3, 257 262 ISSN 0209 1712 10.5603/AIT.2015.0037 www.ait.viamedica.pl Toxic epidermal necrolysis Joanna Hinc-Kasprzyk, Agnieszka Polak-Krzemińska,
REVIEW Anaesthesiology Intensive Therapy 2015, vol. 47, no 3, 257 262 ISSN 0209 1712 10.5603/AIT.2015.0037 www.ait.viamedica.pl Toxic epidermal necrolysis Joanna Hinc-Kasprzyk, Agnieszka Polak-Krzemińska,
Scratching the Surface: A Review of SJS/TEN
 Scratching the Surface: A Review of SJS/TEN Sarah Smith, PharmD Pharmacy Grand Rounds 2018 November 27, 2018 2018 MFMER slide 1 Toxic Epidermal Necrolysis Cutaneous Anthrax Stevens Johnson Syndrome Necrotizing
Scratching the Surface: A Review of SJS/TEN Sarah Smith, PharmD Pharmacy Grand Rounds 2018 November 27, 2018 2018 MFMER slide 1 Toxic Epidermal Necrolysis Cutaneous Anthrax Stevens Johnson Syndrome Necrotizing
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving
 Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
Present : Dr Pham Thi Minh Rang Internal Department No2-Hospital for children No2 AIMS To update the use of IVIG and CORTICOIDS IN management of SJS/ TEN To remind Doctors being careful when giving To
STEVENS-JOHNSON SYNDROME: A CASE REPORT
 STEVENS-JOHNSON SYNDROME: A CASE REPORT Castana O., Rempelos G., Anagiotos G., Apostolopoulou C., Dimitrouli A., Alexakis D. Department of Plastic and Reconstructive Surgery, Evangelismos General Hospital,
STEVENS-JOHNSON SYNDROME: A CASE REPORT Castana O., Rempelos G., Anagiotos G., Apostolopoulou C., Dimitrouli A., Alexakis D. Department of Plastic and Reconstructive Surgery, Evangelismos General Hospital,
Comprehensive survival analysis of a cohort of patients with Stevens-Johnson syndrome and toxic epidermal necrolysis.
 Comprehensive survival analysis of a cohort of patients with Stevens-Johnson syndrome and toxic epidermal necrolysis. Supplementary online-material Supplementary Table S1: Detailed descriptive analysis
Comprehensive survival analysis of a cohort of patients with Stevens-Johnson syndrome and toxic epidermal necrolysis. Supplementary online-material Supplementary Table S1: Detailed descriptive analysis
International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: Vol.8, No.1, pp , 2015
 International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: 0974-4304 Vol.8, No.1, pp 101-105, 2015 To Study the Pattern of Adverse Drug Reaction of Antipsychotic Drugs in a Tertiary Care Hospital
International Journal of PharmTech Research CODEN (USA): IJPRIF, ISSN: 0974-4304 Vol.8, No.1, pp 101-105, 2015 To Study the Pattern of Adverse Drug Reaction of Antipsychotic Drugs in a Tertiary Care Hospital
TOXIC EPIDERMAL NECROLYSIS AND CLARITHROMYCIN
 TOXIC EPIDERMAL NECROLYSIS AND CLARITHROMYCIN Nadia Khaldi 1, Alain Miras 1, Sophie Gromb 1,2 1 Forensic Science Laboratory, Pellegrin Hospital, University Teaching Hospital Bordeaux, France, 2 Forensic
TOXIC EPIDERMAL NECROLYSIS AND CLARITHROMYCIN Nadia Khaldi 1, Alain Miras 1, Sophie Gromb 1,2 1 Forensic Science Laboratory, Pellegrin Hospital, University Teaching Hospital Bordeaux, France, 2 Forensic
1.1. Lenalidomide and (aggravation of) psoriasis
 20-4-2012 1.1. Lenalidomide and (aggravation of) psoriasis Introduction Lenalidomide (Revlimid ), was registered on the Dutch market in June 2007 and is indicated for the treatment of multiple myeloma
20-4-2012 1.1. Lenalidomide and (aggravation of) psoriasis Introduction Lenalidomide (Revlimid ), was registered on the Dutch market in June 2007 and is indicated for the treatment of multiple myeloma
פורמט עלון זה נקבע ע"י משרד הבריאות ותוכנו נבדק ואושר SUMMARY OF PRODUCT CHARACTERISTICS
 פורמט עלון זה נקבע ע"י משרד הבריאות ותוכנו נבדק ואושר SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT FELDENE GEL 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each gram contains 5mg
פורמט עלון זה נקבע ע"י משרד הבריאות ותוכנו נבדק ואושר SUMMARY OF PRODUCT CHARACTERISTICS 1. NAME OF THE MEDICINAL PRODUCT FELDENE GEL 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each gram contains 5mg
Nevirapine 200mg Tablet WHOPAR part 4 May 2005 Section 7 updated: May 2016 SUMMARY OF PRODUCT CHARACTERISTICS
 SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Nevirapine 200mg Tablet. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains nevirapine 200 mg. For excipients, see section
SUMMARY OF PRODUCT CHARACTERISTICS 1 1. NAME OF THE MEDICINAL PRODUCT Nevirapine 200mg Tablet. 2. QUALITATIVE AND QUANTITATIVE COMPOSITION Each tablet contains nevirapine 200 mg. For excipients, see section
Elements for a public summary
 VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Nevirapine is used for antiretroviral combination therapy of Human Immunodeficiency Virus (HIV) infection. Human immunodeficiency
VI.2 Elements for a public summary VI.2.1 Overview of disease epidemiology Nevirapine is used for antiretroviral combination therapy of Human Immunodeficiency Virus (HIV) infection. Human immunodeficiency
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Blum CA, Nigro N, Briel M, et al. Adjunct prednisone
Cutaneous drug reactions
 Maintenance of Certification clinical management series Series editor: James T. Li, MD, PhD Cutaneous drug reactions David A. Khan, MD Dallas, Tex INSTRUCTIONS Credit can now be obtained, free for a limited
Maintenance of Certification clinical management series Series editor: James T. Li, MD, PhD Cutaneous drug reactions David A. Khan, MD Dallas, Tex INSTRUCTIONS Credit can now be obtained, free for a limited
Toxic Epidermal Necrolysis - A Case Report
 The Journal of Critical Care Medicine 2017;3(1):29-33 CASE REPORT Toxic Epidermal Necrolysis - A Case Report Laura Stătescu¹, Magda Constantin², Horia Silviu Morariu³ *, Laura Gheucă Solovăstru¹ ¹ Dermatology
The Journal of Critical Care Medicine 2017;3(1):29-33 CASE REPORT Toxic Epidermal Necrolysis - A Case Report Laura Stătescu¹, Magda Constantin², Horia Silviu Morariu³ *, Laura Gheucă Solovăstru¹ ¹ Dermatology
