Bilateral superior ophthalmic vein enlargement associated with diffuse cerebral swelling
|
|
|
- Eustacia McDowell
- 5 years ago
- Views:
Transcription
1 J Neurosurg 86: , 1997 Bilateral superior ophthalmic vein enlargement associated with diffuse cerebral swelling Report of 11 cases ROHIT K. KHANNA, M.D., CHRISTOPHER J. PHAM, D.O., GHAUS M. MALIK, M.D., ERIC M. SPICKLER, M.D., BHARAT MEHTA, M.D., AND MARK L. ROSENBLUM, M.D. Departments of Neurosurgery and Radiology (Neuroradiology), Henry Ford Hospital, Detroit, Michigan Bilateral superior ophthalmic vein (SOV) enlargement has rarely been shown to occur in patients with septic and aseptic cavernous sinus thrombosis, Graves disease due to obstruction of the SOV by enlarged extraocular muscles, or carotid cavernous fistulas caused by retrograde flow. The authors describe 11 patients with bilateral SOV enlargement associated with cerebral swelling as detected by computerized tomography scanning. The bilaterally enlarged SOVs returned to a normal size following resolution of cerebral swelling and elevated intracranial pressure. To the authors knowledge, this is the first report of bilateral SOV enlargement associated with diffuse cerebral swelling that subsequently resolved after treatment of the cerebral edema. The authors believe that the bilateral SOV enlargement was caused by mechanical cavernous sinus venous stagnation due to cerebral swelling, a syndrome that occurs more commonly than currently appreciated. KEY WORDS cavernous sinus cerebral edema computerized tomography head injury intracranial aneurysm superior ophthalmic vein enlargement U NILATERAL superior ophthalmic vein (SOV) enlargement has been reported in patients with carotid cavernous fistulas, intraorbital pathology, and (infrequently) parasellar tumors. 3,7,10 12 The syndrome is associated with increased retrograde SOV flow, SOV obstruction, or cavernous sinus compression. Except for some patients with cavernous sinus thrombosis, 5 Graves disease, 10 or carotid cavernous fistulas, 1,9 SOV enlargement is almost always unilateral. We report on 11 patients with bilateral SOV enlargement associated with cerebral edema that resolved after treatment. Clinical Review A comprehensive review of over 500 computerized tomography (CT) scans obtained in patients admitted to the neurosurgical intensive care unit at Henry Ford Hospital in Detroit, Michigan, over a 2-year period was undertaken. The CT scans of the head included sections through the orbits, thus allowing for evaluation of the SOVs as well as any intracranial pathology. Patients whose bilateral SOV enlargement could be evaluated on serial CT scans were included. Patients with unilateral SOV enlargement, those in whom one scan showed SOV enlargement but in whom no other CT scans offered good orbital sections for evaluation of their SOVs, and those with a known cause for bilateral SOV enlargement were excluded from the study. Because variability exists in the size of SOVs among different patients, only patients with transient SOV enlargement were included and these patients served as their own controls. Generally, an SOV size of greater than 2 mm on axial CT scanning was considered to be a possible indication of enlargement, 3 mm or more a likely indication of enlargement, and 4 mm or more a definite indication of enlargement. A total of 55 patients met the inclusion criteria. Results Of the 55 patients meeting the inclusion criteria, intracranial pressure (ICP) was monitored in 40 and was found to be elevated ( 20 mm Hg) at some point in 21. Our review identified 11 patients with bilateral SOV enlargement associated with cerebral edema that returned to normal size after the cerebral edema resolved. Table 1 shows the clinical presentation, surgical treatment, hospital course, and outcome for each patient. Four patients were placed on a ventilator during initial CT scanning, but the positive end-expiratory pressure (PEEP) did not rise above 5 mm Hg during this time. The findings on initial and follow-up head CT scans are listed in Table 2. Of the 21 patients with intracranial hypertension, transient bilat- 893
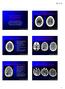
2 R. K. Khanna, et al. TABLE 1 Clinical characteristics, hospital course, and outcome in 11 patients with enlarged SOVs* Highest Case Age GCS ICP (mm No. (yrs) Diagnosis Score Hg) Complications Surgical Procedure Outcome 1 15 closed head injury 3 25 none subdural hematoma evacuation w/ severe deficits temporal craniectomy, ventriculostomy 2 54 ruptured middle cerebral artery aneurysm uncal herniation, aneurysm clipping, temporal lobec- moderate hydrocephalus tomy,vp shunt deficits 3 38 ruptured middle cerebral artery aneurysm 6 NM hydrocephalus aneurysm clipping, VP shunt severe deficits 4 29 ruptured posterior communicating artery severe symptomat- aneurysm clipping, VP shunt good recovery aneurysm ic vasospasm 5 19 ruptured basilar tip aneurysm hydrocephalus, aneurysm clipping, VP shunt mild deficits vasospasm 6 22 posterior fossa ependymoma hydrocephalus, ependymoma resection, VP shunt vegetative status epilepticus state 7 59 frontotemporal & subarachnoid 5 20 uncal herniation, intracerebral hematoma evacuation, death hemorrhage hydrocephalus temporal lobectomy, ventriculostomy 8 39 ruptured ACoA aneurysm hydrocephalus aneurysm clipping, VP shunt mild deficits 9 49 large basal ganglia hypertensive hemorrhage 6 38 seizure, hydro- intracerebral hematoma evacuation, severe deficits cephalus ventriculostomy closed head injury 11 NM seizure temporal lobectomy w/ intracerebral good recovery hematoma evacuation ruptured large frontal & basal ganglia AVM none AVM resection, ventriculostomy mild deficits * ACoA = anterior communicating artery; AVM = arteriovenous malformation; GCS = Glasgow Coma Scale; ICP = intracranial pressure; NM = not monitored; VP = ventriculoperitoneal. eral SOV enlargement was seen in eight (38.1%); of 19 patients with normal ICP, only one (5.3%) had transient bilateral SOV enlargement, and even this patient exhibited increased ICP (up to 16 mm Hg) during the period of bilateral SOV enlargement. Two (13.3%) of the 15 patients who did not undergo monitoring had transient bilateral SOV enlargement associated with cerebral swelling. The bilateral SOV enlargement usually followed ICP elevations, either immediately or up to several hours later. Case Report History. This 41-year-old man (Case 10) was brought to the emergency room by his family members 4 hours after receiving an injury to the head during an assault. The patient suffered a generalized seizure in the emergency room prior to evaluation. His medical history was significant for moderate-to-severe alcohol consumption. Examination. On examination the patient was combative, exhibited slurred speech, and moved all four extremities spontaneously. His left pupil was reactive; his right pupil could not be evaluated because of a ruptured globe sustained 7 years previously. The patient exhibited no chemosis, palpebral swelling, or cranial nerve deficits, and no intracranial bruits were heard. A CT scan of the head showed diffuse cerebral swelling of the brain and FIG. 1. Initial CT scans in a patient with bilateral SOV enlargement. Left: Note the enlarged right superior ophthalmic vein (arrow) as well as the right temporal hemorrhage. The ethmoid air cells, sphenoid sinus, and mastoid air cells are clear. Right: The left superior ophthalmic vein is also enlarged (arrow). FIG. 2. Higher sections from the initial CT in the same patient. Left: There is diffuse cerebral swelling with loss of cisternal space as well as right frontal and left temporal lobe hemorrhages. The frontal sinuses are clear. Right: Note the diffuse cerebral swelling with obliteration of the sulcal pattern. 894
3 Bilateral SOV enlargement with cerebral edema TABLE 2 Serial CT findings in 11 patients with enlarged SOVs* Case No. Initial Head CT Scan First Follow-Up CT Scan Second Follow-Up CT Scan 1 bilat SOV enlargement, acute rt frontotemporoparietal 8-mm- 2 days later: smaller SOVs, resolved subdural thick subdural hemorrhage, 5-mm midline shift, entrapped hemorrhage & hydrocephalus, moderate lt lat ventricle diffuse cerebral swelling, no midline shift 2 bilat SOV enlargement, diffuse cerebral swelling, SAH 18 hours later: smaller SOVs w/ mild cere- 2 days later: smaller SOVs w/ mild in rt sylvian fissure, acute rt temporoparietal lobe hemor- bral swelling, rt temporal lobectomy w/ cerebral swelling & resolving rt rhage w/ 1.5-cm midline shift to lt side, rt lat IVH hemorrhage evacuation, persistent rt lat IVH ventricle hemorrhage, no midline shift 3 bilat SOV enlargement, diffuse cerebral swelling, impinge- 12 hours later: same findings as initial CT 1 day later: smaller SOVs w/ rt ment of rt lat ventricle w/ no midline shift, SAH in rt basal ganglia infarct & resolving sylvian fissure & bilat ambient cisterns rt sylvian fissure hemorrhage 4 small SOVs; mild hydrocephalus; SAH in rt sylvian fissure; 3 days later: bilat SOV enlargement w/ 6 days later: small SOVs w/ no suprasellar, perimesencephalic & ambient cisterns; diffuse cerebral swelling cerebral swelling fourth ventricle hemorrhage 5 bilat SOV enlargement; moderate hydrocephalus; SAH in 12 days later: smaller SOVs w/ resolved prepontine, suprasellar, bilat ambient cisterns & sylvian hydrocephalus, SAH, & fourth ventricle fissures; fourth ventricle hemorrhage hemorrhage 6 bilat SOV enlargement, diffuse edema especially in cere- 1 day later: bilat SOV enlargement, im- 6 days later: smaller SOVs, rebellum, mild hydrocephalus, SAH along folia of cere- proving edema, moderate hydrocephalus, solving edema, SAH, & IVH bellum & ambient cisterns lt lat ventricle hemorrhage 7 bilat SOV enlargement; SAH in prepontine, suprasellar, 4 days later: smaller SOVs, resolving ICH, lt ambient cistern & sylvian fissure; lt frontotemporal IVH, & SAH, no hydrocephalus hemorrhage; lt lat ventricle; third & fourth ventricle hemorrhage; moderate hydrocephalus 8 bilat SOV enlargement, rt frontal hemorrhage, bilat lat 1 day later: smaller SOVs, resolved frontal ventricle hemorrhage, moderate hydrocephalus hemorrhage, persistent ventricular hemorrhage, & hydrocephalus 9 bilat SOV enlargement, large lt frontotemporoparietal hemor- 1 day later: bilat SOV enlargement, resolving 7 days later: smaller SOVs, lt rhage, lt lat ventricle hemorrhage, midline shift of 7 cerebral hemorrhage & hydrocephalus, frontotemporoparietal mm, moderate hydrocephalus persistent lt frontotemporal edema, & 5-mm encephalomalacia midline shift 10 bilat SOV enlargement, diffuse cerebral swelling, acute bilat 10 days later: smaller SOVs w/ mild cerebral temporal rt frontal & lt parietal lobe hemorrhages swelling & rt temporal lobectomy w/ hemorrhage evacuation 11 bilat SOV enlargement; resected rt frontal/basal ganglia rup- 11 days later: smaller SOVs, resolved IVH & tured arteriovenous malformation; diffuse IVH & hydro- SAH, no hydrocephalus cephalus; SAH in rt frontal sulci, perimesencephalic, prepontine, & rt ambient cistern * ICH = intracerebral hemorrhage; IVH = intraventricular hemorrhage; SAH = subarachnoid hemorrhage. acute intracerebral hemorrhages in the temporal lobes bilaterally (much more pronounced in the right side) and in the right frontal and high left parietal lobes (Figs. 1 and 2). The routine thin CT sections through the posterior fossa also included the orbits and showed bilaterally enlarged SOVs with no evidence of cavernous sinus thrombosis (Fig. 1). The paranasal sinuses and the mastoid air cells were not opacified, and there was no evidence of any other intraorbital pathology. Operation. The patient was immediately taken to the operating room where the right temporal hematoma was evacuated and a decompressive right temporal lobectomy was performed. The patient received mannitol for his cerebral edema both pre- and postoperatively but an effort was made to avoid dehydration. Postoperative Course. Ten days postsurgery a repeated CT scan showed a normal-sized SOV bilaterally (Fig. 3) with a significant decrease in diffuse cerebral swelling (Fig. 4). At this time the patient was neurologically intact except for some mild cognitive impairment. Discussion Enlargement of an SOV can be detected reliably by high-resolution CT scanning. 2,7,10,11 Unilateral SOV enlargement has been reported secondary to cavernous sinus thrombosis, carotid cavernous fistula, Graves orbitopathy, orbital pseudotumor (idiopathic orbital inflammation), orbital varices and arteriovenous malformations, and parasellar tumors. 3,7,10 12 The SOV provides major orbital venous drainage into the cavernous sinus via the superior orbital fissure. Because of the lack of valves in this vein, retrograde flow from a carotid cavernous fistula or impaired venous outflow caused by cavernous sinus compression or thrombosis can lead to its enlargement. Compression of the SOV by enlarged extraocular muscles secondary to Graves disease, as well as intraorbital inflammation, infection, or neoplasm, can also cause SOV enlargement. Although unilateral SOV enlargement is more common, bilateral SOV enlargement has been reported infrequently in patients with Graves orbitopathy, cavernous sinus thrombosis, and carotid cavernous fistulas. 1,6,9,10 895
4 R. K. Khanna, et al. FIG. 3. Follow-up CT scans in the same patient. Left: The right superior ophthalmic vein (arrow) has returned to its normal size. Note the right temporal lobectomy. Right: The left superior ophthalmic vein (arrow) has also returned to its normal size. FIG. 4. Follow-up CT scans in the same patient. Left: Section at the same level as shown as Fig. 2 left. Note the decreased cerebral swelling and the presence of the cisternal spaces. Right: Section at the same level as shown in Fig. 2 right illustrating the decreased cerebral swelling with the normal appearance of the sulci and gyral pattern. Unlike the dural venous sinuses, the cavernous sinus is not formed by splits in the dura and therefore is easily compressible. The cavernous sinus is a venous plexus located on each side of the sphenoid bone beginning at the superior orbital fissure and extending to the petrous apex of the temporal bone. The two cavernous sinuses communicate via the intercavernous sinuses, which pass anteriorly and posteriorly to the sella turcica and pituitary gland. Generalized cerebral edema can lead to intracranial hypertension with consequent compression of the cavernous sinuses. Because the cerebral veins and venous sinuses do not have valves, blood within them can flow in either direction depending on the pressure gradients. Yasargil and Damur 14 have previously documented the phenomenon of mechanical venous stagnation with thrombosis of pial veins in patients with cerebral edema following closed head injury. Early appearance of SOV on carotid angiography also has been shown to occur in patients with increased ICP from brain tumors. 5 The reversibility of bilateral SOV enlargement in our patients after resolution of cerebral edema indicates that mechanical venous stagnation rather than venous thrombosis in the cavernous sinus was the cause of their condition, although initial cavernous sinus thrombosis secondary to intracranial hypertension with subsequent recanalization is another possible cause that cannot be excluded. This phenomenon of thrombosed cerebral vein recanalization has been documented by magnetic resonance imaging. 8 Prolonged intracranial hypertension accompanied by dehydration could easily lead to cavernous sinus and pial vein thrombosis, further exacerbating the cerebral swelling. We initially considered posttraumatic carotid cavernous fistulas as the likely cause of the bilaterally enlarged SOVs in patients with closed head injury. However, we subsequently ruled out this possibility based on the clinical picture and because both SOVs returned to normal size after resolution of the cerebral swelling. Posttraumatic fistulas usually do not disappear spontaneously. 9 Septic cavernous sinus thrombosis was also excluded as a possible cause because these patients had no predisposing infections. 4 Increased cerebral blood volume secondary to hyperemia from a generalized seizure could have led to cerebral swelling and/or bilaterally enlarged SOVs, but this is unlikely because no CT scan was obtained either during or immediately after a seizure, and any hyperemia should have resolved by the time the CT scans were obtained. Arteriovenous shunt placement for treatment of cerebral arteriovenous malformations can cause bilateral SOV enlargement in some patients; however, this was not the case in our patient with an arteriovenous malformation because the bilateral SOV enlargement was seen after resection of the malformation, at which time no arteriovenous shunting was present. The effect of PEEP on central venous pressure elevations and venous engorgement with subsequent SOV enlargement in some of our intubated patients also seems unlikely because the PEEP in our intubated patients was 5 mm Hg or less, thus exerting a negligible effect on central venous pressure elevations and/or venous engorgement. Conclusions We believe that bilateral enlargement of the SOVs occurs more commonly in patients with cerebral edema than is currently appreciated. When corroborated by other clinical criteria and by CT scanning for increased ICP, this finding usually reflects significant intracranial hypertension and may call for early aggressive treatment. A prospective analysis with magnetic resonance imaging and venography should ultimately provide a better understanding of the pathophysiological mechanism(s) involved in this syndrome. References 1. Ahmadi J, Teal JS, Segall HD, et al: Computed tomography of carotid-cavernous fistula. AJNR 4: , Bacon KT, Duchesneau PM, Weinstein MA: Demonstration of the superior ophthalmic vein by high resolution computed tomography. Radiology 124: ,
5 Bilateral SOV enlargement with cerebral edema 3. Brismar G, Brismar J: Thrombosis of the intraorbital veins and cavernous sinus. Acta Radiol Diag 18: , DiNubile MJ: Septic thrombosis of the cavernous sinuses. Arch Neurol 45: , Hacker H, Porrero M: Demonstration and significance of the superior ophthalmic vein in carotid angiography. Radiology 94:717, 1970 (Abstract) 6. Hasso AN, Lasjaunias P, Thompson JR, et al: Venous occlusions of the cavernous area a complication of crushing fractures of the sphenoid bone. Radiology 132: , Howard GR, Nerad JA, Carter KD: Superior ophthalmic vein enlargement and proptosis caused by middle cranial fossa lipoma. Am J Ophthalmol 110: , 1990 (Letter) 8. Macchi PJ, Grossman RI, Gomori JM, et al: High field MR imaging of cerebral venous thrombosis. J Comput Assist Tomogr 10:10 15, Mullan S: Carotid-cavernous fistulas and intracavernous aneurysms, in Wilkins RH, Rengachary SS (eds): Neurosurgery. New York: McGraw-Hill, 1985, pp Nugent RA, Belkin RI, Neigel JM, et al: Graves orbitopathy: correlation of CT and clinical findings. Radiology 177: , Peyster RG, Savino PJ, Hoover ED, et al: Differential diagnosis of the enlarged superior ophthalmic vein. J Comput Assist Tomogr 8: , Scotti LN, Goldman RL, Hardman DR, et al: Venous thrombosis in infants and children. Radiology 112: , Teasdale G, Jennett B: Assessment of coma and impaired consciousness. A practical scale. Lancet 2:81 84, Yasargil MG, Damur M: Thrombosis of the cerebral veins and dural sinuses, in Newton TH, Potts DG (eds): Radiology of the Skull and Brain. St. Louis: Mosby, 1974, pp Manuscript received September 18, Accepted in final form December 19, Address reprint requests to: Ghaus M. Malik, M.D., c/o Editorial Office, Department of Neurosurgery, Henry Ford Hospital, 2799 West Grand Boulevard, Detroit, Michigan
Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins
 ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
ISPUB.COM The Internet Journal of Radiology Volume 18 Number 1 Cryptogenic Enlargement Of Bilateral Superior Ophthalmic Veins K Kragha Citation K Kragha. Cryptogenic Enlargement Of Bilateral Superior Ophthalmic
A Case of Carotid-Cavernous Fistula
 A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
A Case of Carotid-Cavernous Fistula By : Mohamed Elkhawaga 2 nd Year Resident of Ophthalmology Alexandria University A 19 year old male patient came to our outpatient clinic, complaining of : -Severe conjunctival
UPSTATE Comprehensive Stroke Center. Neurosurgical Interventions Satish Krishnamurthy MD, MCh
 UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
UPSTATE Comprehensive Stroke Center Neurosurgical Interventions Satish Krishnamurthy MD, MCh Regional cerebral blood flow is important Some essential facts Neurons are obligatory glucose users Under anerobic
NEURO IMAGING 2. Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity
 NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
NEURO IMAGING 2 Dr. Said Huwaijah Chairman of radiology Dep, Damascus Univercity I. EPIDURAL HEMATOMA (EDH) LOCATION Seventy to seventy-five percent occur in temporoparietal region. CAUSE Most likely caused
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD
 Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
Head CT Scan Interpretation: A Five-Step Approach to Seeing Inside the Head Lawrence B. Stack, MD Five Step Approach 1. Adequate study 2. Bone windows 3. Ventricles 4. Quadrigeminal cistern 5. Parenchyma
North Oaks Trauma Symposium Friday, November 3, 2017
 Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
Traumatic Intracranial Hemorrhage Aaron C. Sigler, DO, MS Neurosurgery Tulane Neurosciences None Disclosures Overview Anatomy Epidural hematoma Subdural hematoma Cerebral contusions Outline Traumatic ICH
For Emergency Doctors. Dr Suzanne Smallbane November 2011
 For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
For Emergency Doctors Dr Suzanne Smallbane November 2011 A: Orbit B: Sphenoid Sinus C: Temporal Lobe D: EAC E: Mastoid air cells F: Cerebellar hemisphere A: Frontal lobe B: Frontal bone C: Dorsum sellae
ISCHEMIC STROKE IMAGING
 ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
ISCHEMIC STROKE IMAGING ผศ.พญ พญ.จ ร ร ตน ธรรมโรจน ภาคว ชาร งส ว ทยา คณะแพทยศาสตร มหาว ทยาล ยขอนแก น A case of acute hemiplegia Which side is the abnormality, right or left? Early Right MCA infarction
INCREASED INTRACRANIAL PRESSURE
 INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
INCREASED INTRACRANIAL PRESSURE Sheba Medical Center, Acute Medicine Department Irene Frantzis P-Year student SGUL 2013 Normal Values Normal intracranial volume: 1700 ml Volume of brain: 1200-1400 ml CSF:
NEURORADIOLOGY DIL part 3
 NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
NEURORADIOLOGY DIL part 3 Bleeds and hemorrhages K. Agyem MD, G. Hall MD, D. Palathinkal MD, Alexandre Menard March/April 2015 OVERVIEW Introduction to Neuroimaging - DIL part 1 Basic Brain Anatomy - DIL
Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage
 Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Cronicon OPEN ACCESS EC PAEDIATRICS Case Report Brain AVM with Accompanying Venous Aneurysm with Intracerebral and Intraventricular Hemorrhage Dimitrios Panagopoulos* Neurosurgical Department, University
Perioperative Management Of Extra-Ventricular Drains (EVD)
 Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Perioperative Management Of Extra-Ventricular Drains (EVD) Dr. Vijay Tarnal MBBS, FRCA Clinical Assistant Professor Division of Neuroanesthesiology Division of Head & Neck Anesthesiology Michigan Medicine
Moron General Hospital Ciego de Avila Cuba. Department of Neurological Surgery
 Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
Moron General Hospital Ciego de Avila Cuba Department of Neurological Surgery Early decompressive craniectomy in severe head injury with intracranial hypertension Angel J. Lacerda MD PhD, Daisy Abreu MD,
HEAD AND NECK IMAGING. James Chen (MS IV)
 HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
HEAD AND NECK IMAGING James Chen (MS IV) Anatomy Course Johns Hopkins School of Medicine Sept. 27, 2011 OBJECTIVES Introduce cross sectional imaging of head and neck Computed tomography (CT) Review head
secondary effects and sequelae of head trauma.
 Neuroimaging of vascular/secondary secondary effects and sequelae of head trauma. Andrès Server Alonso Department of Neuroradiology Division of Radiology Ullevål University Hospital Oslo, Norway. Guidelines
Neuroimaging of vascular/secondary secondary effects and sequelae of head trauma. Andrès Server Alonso Department of Neuroradiology Division of Radiology Ullevål University Hospital Oslo, Norway. Guidelines
Intracranial spontaneous hemorrhage mechanisms, imaging and management
 Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Intracranial spontaneous hemorrhage mechanisms, imaging and management Dora Zlatareva Department of Diagnostic Imaging Medical University, Sofia, Bulgaria Intracranial hemorrhage (ICH) ICH 15% of strokes
Cerebro-vascular stroke
 Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Cerebro-vascular stroke CT Terminology Hypodense lesion = lesion of lower density than the normal brain tissue Hyperdense lesion = lesion of higher density than normal brain tissue Isodense lesion = lesion
Principles Arteries & Veins of the CNS LO14
 Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Principles Arteries & Veins of the CNS LO14 14. Identify (on cadaver specimens, models and diagrams) and name the principal arteries and veins of the CNS: Why is it important to understand blood supply
Non-Traumatic Neuro Emergencies
 Department of Radiology University of California San Diego Non-Traumatic Neuro Emergencies John R. Hesselink, M.D. Nontraumatic Neuroemergencies 1. Acute focal neurological deficit 2. Worst headache of
Department of Radiology University of California San Diego Non-Traumatic Neuro Emergencies John R. Hesselink, M.D. Nontraumatic Neuroemergencies 1. Acute focal neurological deficit 2. Worst headache of
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD.
 Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Angel J. Lacerda MD PhD, Daisy Abreu MD, Julio A. Díaz MD, Sandro Perez MD, Julio C Martin MD, Daiyan Martin MD. Introduction: Spontaneous intracerebral haemorrhage (SICH) represents one of the most severe
Cerebellar Hemorrhage due to a Direct Carotid Cavernous Fistula after Surgery for Maxillary Cancer
 Case Report J Korean Neurosurg Soc 60 (1) : 89-93, 2017 https://doi.org/10.3340/jkns.2015.1206.001 pissn 2005-3711 eissn 1598-7876 Cerebellar Hemorrhage due to a Direct Carotid Cavernous Fistula after
Case Report J Korean Neurosurg Soc 60 (1) : 89-93, 2017 https://doi.org/10.3340/jkns.2015.1206.001 pissn 2005-3711 eissn 1598-7876 Cerebellar Hemorrhage due to a Direct Carotid Cavernous Fistula after
Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D.
 J Neurosurg 48:355-359, 1978 Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D. Department of Radiology, University
J Neurosurg 48:355-359, 1978 Intracranial air on computerized tomography ANNE G. OSBORN, M.D., JONATHAN H. DAINES, M.D., S. DOUGLAS WING, M.D., AND ROBERT E. ANDERSON, M.D. Department of Radiology, University
Transient Bilateral Oculomotor Nerve. Palsy (TOP) Associated with Ruptured. Anterior Communicating Artery Aneurysm: A Case Report
 Case Report imedpub Journals http://www.imedpub.com Insights in Neurosurgery ISSN 2471-9633 DOI: 10.21767/2471-9633.100012 Abstract Transient Bilateral Oculomotor Nerve Palsy (TOP) Associated with Ruptured
Case Report imedpub Journals http://www.imedpub.com Insights in Neurosurgery ISSN 2471-9633 DOI: 10.21767/2471-9633.100012 Abstract Transient Bilateral Oculomotor Nerve Palsy (TOP) Associated with Ruptured
Ophthalmoplegia in carotid cavernous sinus fistula
 British Journal of Ophthalmology, 1984, 68, 128-134 Ophthalmoplegia in carotid cavernous sinus fistula T. J. K. LEONARD, I. F. MOSELEY, AND M. D. SANDERS From the Departments ofneuro-ophthalmology and
British Journal of Ophthalmology, 1984, 68, 128-134 Ophthalmoplegia in carotid cavernous sinus fistula T. J. K. LEONARD, I. F. MOSELEY, AND M. D. SANDERS From the Departments ofneuro-ophthalmology and
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN
 Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
Marshall Scale for Head Trauma Mark C. Oswood, MD PhD Department of Radiology Hennepin County Medical Center, Minneapolis, MN History of Marshall scale Proposed by Marshall, et al in 1991 to classify head
PRACTICE GUIDELINE. DEFINITIONS: Mild head injury: Glasgow Coma Scale* (GCS) score Moderate head injury: GCS 9-12 Severe head injury: GCS 3-8
 PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
PRACTICE GUIDELINE Effective Date: 9-1-2012 Manual Reference: Deaconess Trauma Services TITLE: TRAUMATIC BRAIN INJURY GUIDELINE OBJECTIVE: To provide practice management guidelines for traumatic brain
Transverse-Sigmoid Sinus Dural Arteriovenous Malformations
 Transverse-Sigmoid Sinus Dural Arteriovenous Malformations Kenan I. Amautovic, M.D., and Ali F. Krisht, M.D. '-...--- Learning Objectives: After reading this article, the participant should: 1. Have an
Transverse-Sigmoid Sinus Dural Arteriovenous Malformations Kenan I. Amautovic, M.D., and Ali F. Krisht, M.D. '-...--- Learning Objectives: After reading this article, the participant should: 1. Have an
The central nervous system
 Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Sectc.qxd 29/06/99 09:42 Page 81 Section C The central nervous system CNS haemorrhage Subarachnoid haemorrhage Cerebral infarction Brain atrophy Ring enhancing lesions MRI of the pituitary Multiple sclerosis
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case
 Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Dural Arteriovenous Fistula of the Cavernous Sinus Presenting with Progressive Venous Congestion of the Pons and Cerebrum: Report of one case Soo-Bin Yim, M.D., Jong-Sung Kim, M.D., Yang Kwon,M.D.*, Choong-Gon
Case Conference: Neuroradiology. Case 1: Tumor Case 1: 22yo F w/ HA and prior Seizures
 Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
Case Conference: Neuroradiology Case 1: 22yo F w/ HA and prior Seizures David E. Rex, MD, PhD Stanford University Hospital Department of Radiology Case 1: Tumor Most likely gangiloglioma, oligodendroglioma,
Vascular and Parameningeal Infections of the Head and Neck
 Vascular and Parameningeal Infections of the Head and Neck Kevin B. Laupland, MD, MSc, FRCPC Associate Professor Departments of Medicine, Critical Care Medicine, Pathology and Laboratory Medicine, and
Vascular and Parameningeal Infections of the Head and Neck Kevin B. Laupland, MD, MSc, FRCPC Associate Professor Departments of Medicine, Critical Care Medicine, Pathology and Laboratory Medicine, and
Dural Arteriovenous Malformations and Fistulae (DAVM S DAVF S)
 Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
Jorge Guedes Campos NEUROIMAGING DEPARTMENT HOSPITAL SANTA MARIA UNIVERSITY OF LISBON PORTUGAL DEFINITION region of arteriovenous shunting confined to a leaflet of packymeninges often adjacent to a major
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT. G. Tamburrini, Rome
 INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
INTRACRANIAL ARACHNOID CYSTS: CLASSIFICATION AND MANAGEMENT G. Tamburrini, Rome Incidence 2% of occasional neuroradiological findings From clinical studies (1960 s): 0.4-1% of intracranial space occupying
41 year old female with headache. Elena G. Violari MD and Leo Wolansky MD
 41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
41 year old female with headache Elena G. Violari MD and Leo Wolansky MD ? Dural Venous Sinus Thrombosis with Hemorrhagic Venous Infarct Acute intraparenchymal hematoma measuring ~3 cm in diameter centered
Papilledema. Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D.
 Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
Papilledema Golnaz Javey, M.D. and Jeffrey J. Zuravleff, M.D. Papilledema specifically refers to optic nerve head swelling secondary to increased intracranial pressure (IICP). Optic nerve swelling from
2. Subarachnoid Hemorrhage
 Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
Causes: 2. Subarachnoid Hemorrhage A. Saccular (berry) aneurysm - Is the most frequent cause of clinically significant subarachnoid hemorrhage is rupture of a saccular (berry) aneurysm. B. Vascular malformation
8/29/2011. Brain Injury Incidence: 200/100,000. Prehospital Brain Injury Mortality Incidence: 20/100,000
 Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Traumatic Brain Injury Almario G. Jabson MD Section Of Neurosurgery Asian Hospital And Medical Center Brain Injury Incidence: 200/100,000 Prehospital Brain Injury Mortality Incidence: 20/100,000 Hospital
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD
 Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Enhancement of Cranial US: Utility of Supplementary Acoustic Windows and Doppler Harriet J. Paltiel, MD Boston Children s Hospital Harvard Medical School None Disclosures Conventional US Anterior fontanelle
Spontaneous occlusion of a cerebral arteriovenous malformation after subtotal endovascular embolisation
 206 Chiriac et al Spontaneous occlusion of a cerebral arteriovenous malformation Spontaneous occlusion of a cerebral arteriovenous malformation after subtotal endovascular embolisation A. Chiriac, N. Dobrin*,
206 Chiriac et al Spontaneous occlusion of a cerebral arteriovenous malformation Spontaneous occlusion of a cerebral arteriovenous malformation after subtotal endovascular embolisation A. Chiriac, N. Dobrin*,
Traumatic brain Injury- An open eye approach
 Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Traumatic brain Injury- An open eye approach Dr. Sunit Dr Sunit, Apollo children's hospital Blah blah Lots of head injury Lot of ill children Various methods of injury Various mechanisms of brain damage
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes
 Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
Diagnosis of Subarachnoid Hemorrhage (SAH) and Non- Aneurysmal Causes By Sheila Smith, MD Swedish Medical Center 1 Disclosures I have no disclosures 2 Course Objectives Review significance and differential
A.J. Hauer Intracranial dural arteriovenous fistulae
 A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
A.J. Hauer 27-06-2018 Intracranial dural arteriovenous fistulae Dural arteriovenous fistulae (davfs) epidemiology Pathological anastomoses (within the dural leaflets) between meningeal arteries and dural
OBJECTIVES. At the end of the lecture, students should be able to: List the cerebral arteries.
 DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
DR JAMILA EL MEDANY OBJECTIVES At the end of the lecture, students should be able to: List the cerebral arteries. Describe the cerebral arterial supply regarding the origin, distribution and branches.
Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage
 Lehigh Valley Health Network LVHN Scholarly Works Department of Medicine Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage Hussam A. Yacoub MD Lehigh Valley Health
Lehigh Valley Health Network LVHN Scholarly Works Department of Medicine Isolated Cranial Nerve-III Palsy Secondary to Perimesencephalic Subarachnoid Hemorrhage Hussam A. Yacoub MD Lehigh Valley Health
Benign brain lesions
 Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Benign brain lesions Diagnostic and Interventional Radiology Hung-Wen Kao Department of Radiology, Tri-Service General Hospital, National Defense Medical Center Computed tomography Hounsfield unit (HU)
Classical CNS Disease Patterns
 Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
Classical CNS Disease Patterns Inflammatory Traumatic In response to the trauma of having his head bashed in GM would have experienced some of these features. NOT TWO LITTLE PEENY WEENY I CM LACERATIONS.
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER
 CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
CLEAR III TRIAL : UPDATE ON SURGICAL MATTERS THAT MATTER CLEAR Surgical Center Team July 2011 Trial Enrollment Status Updates Insert latest enrollment update chart from most recent CLEAR newsletter Imaging
Intracranial dural arteriovenous fistulas (DAVFs) with retrograde
 ORIGINAL RESEARCH W.J. van Rooij M. Sluzewski G.N. Beute Dural Arteriovenous Fistulas with Cortical Venous Drainage: Incidence, Clinical Presentation, and Treatment BACKGROUND AND PURPOSE: Our purpose
ORIGINAL RESEARCH W.J. van Rooij M. Sluzewski G.N. Beute Dural Arteriovenous Fistulas with Cortical Venous Drainage: Incidence, Clinical Presentation, and Treatment BACKGROUND AND PURPOSE: Our purpose
Rerupture of intracranial aneurysms: a clinicoanatomic study
 J Neurosurg 67:29-33, 1987 Rerupture of intracranial aneurysms: a clinicoanatomic study ALBERT HIJDRA, M.D., MARINUS VERMEULEN, M.D., JAN VAN GIJN, M.D., AND HANS VAN CREVEL, M.D. Departments ~[ Neurology.
J Neurosurg 67:29-33, 1987 Rerupture of intracranial aneurysms: a clinicoanatomic study ALBERT HIJDRA, M.D., MARINUS VERMEULEN, M.D., JAN VAN GIJN, M.D., AND HANS VAN CREVEL, M.D. Departments ~[ Neurology.
A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage
 July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
July 2013 A Guide to the Radiologic Evaluation of Extra-Axial Hemorrhage John Dickson, Harvard Medical School Year III Agenda 1. Define extra-axial hemorrhage and introduce its subtypes 2. Review coup
Brain Arteriovenous Malformations Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos
 Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
Endovascular Therapy and Associated Therapeutic Protocols Jorge Guedes Cabral de Campos Neuroradiology Department Hospital de Santa Maria University of Lisbon CEREBRAL AVM CLINICAL / EPIDEMIOLOGY Brain
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage. By: Shifaa AlQa qa
 CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
CENTRAL NERVOUS SYSTEM TRAUMA and Subarachnoid Hemorrhage By: Shifaa AlQa qa Subarachnoid Hemorrhage Causes: Rupture of a saccular (berry) aneurysm Vascular malformation Trauma Hematologic disturbances
Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report
 214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
214 Balasa et al - Acute cerebral MCA ischemia Acute cerebral MCA ischemia with secondary severe head injury and acute intracerebral and subdural haematoma. Case report D. Balasa 1, A. Tunas 1, I. Rusu
ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA. Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
 Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Malaysian Journal of Medical Sciences, Vol. 8, No. 2, July 2001 (47-51) CASE REPORT ARTERIOVENOUS MALFORMATION OR CONTUSION : A DIAGNOSTIC DILEMMA Yong Pei Yee, Ibrahim Lutfi Shuaib, Jafri Malin Abdullah*
Medical Review Guidelines Magnetic Resonance Angiography
 Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
Medical Review Guidelines Magnetic Resonance Angiography Medical Guideline Number: MRG2001-05 Effective Date: 2/13/01 Revised Date: 2/14/2006 OHCA Reference OAC 317:30-5-24. Radiology. (f) Magnetic Resonance
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital
 C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
C. Douglas Phillips MD FACR Director of Head and Neck Imaging Weill Cornell Medical College/NewYork-Presbyterian Hospital Disclosures Neither I nor any family members have any pertinent financial relations
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery
 Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Surgical Management of Stroke Brandon Evans, MD Department of Neurosurgery 2 Stroke Stroke kills almost 130,000 Americans each year. - Third cause of all deaths in Arkansas. - Death Rate is highest in
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT
 Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
Pearls and Pitfalls in Neuroradiology of Cerebrovascular Disease The Essentials with MR and CT Val M. Runge, MD Wendy R. K. Smoker, MD Anton Valavanis, MD Control # 823 Purpose The focus of this educational
MR imaging as predictor of delayed posttraumatic cerebral hemorrhage
 J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
J Neurosurg 69:203-209, 1988 MR imaging as predictor of delayed posttraumatic cerebral hemorrhage TOKUTARO TANAKA, M.D., TSUNEO SAKAI, M.D., KENICHI UEMURA, M.D., ATSUSHI TERAMURA, M.D., ICHIRO FUJISHIMA,
2/20/2019 BRAIN DISSECTION CODING AND DOCUMENTATION OBJECTIVES INTRODUCTION
 BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
BRAIN DISSECTION CODING AND DOCUMENTATION Diana R. Phelps, CPC, CPC-I, CEMC OBJECTIVES Identify general structure of the human brain Describe how the different parts work Recognized the two hemispheres
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth. Objectives 11/7/2017
 Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Pediatric Subdural Hematoma and Traumatic Brain Injury J. Charles Mace MD FACS Springfield Neurological Institute CoxHealth Objectives 1. Be able to discuss brain anatomy and physiology as it applies to
Head trauma - interpreting CT scans
 Head trauma - interpreting CT scans Poster No.: C-2075 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Rihtar; Zagreb/HR Keywords: Trauma, Hemorrhage, Edema, Diagnostic procedure, CT, Neuroradiology
Head trauma - interpreting CT scans Poster No.: C-2075 Congress: ECR 2014 Type: Educational Exhibit Authors: T. Rihtar; Zagreb/HR Keywords: Trauma, Hemorrhage, Edema, Diagnostic procedure, CT, Neuroradiology
Vascular Malformations
 Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Vascular Malformations LTC Robert Shih Chief of Neuroradiology Walter Reed Medical Center Special thanks to LTC Alice Smith (retired) Disclosures: None. This presentation reflects the personal views of
Residence of Discipline of Neurosurgery of Hospital da Santa Casa de Misericórdia of Sao Paulo Sao Paulo, Brazil
 Cronicon OPEN ACCESS NEUROLOGY Research Article Efficacy of the Lamina Terminalis Fenestration Associated With the Liliequist Membrane Fenestration in Reducing Shunt-Dependent Hydrocephalus Following Aneurysm
Cronicon OPEN ACCESS NEUROLOGY Research Article Efficacy of the Lamina Terminalis Fenestration Associated With the Liliequist Membrane Fenestration in Reducing Shunt-Dependent Hydrocephalus Following Aneurysm
Paul Gigante HMS IV Gillian Lieberman, MD. Sept Mr. T s T s Headache. Paul Gigante,, Harvard Medical School Year IV Gillian Lieberman, MD
 Sept 2005 Mr. T s T s Headache Paul Gigante,, Harvard Medical School Year IV Mr. T s T s Presentation 45 year-old welder complains of sudden severe headache and witnessed seizure with loss of consciousness
Sept 2005 Mr. T s T s Headache Paul Gigante,, Harvard Medical School Year IV Mr. T s T s Presentation 45 year-old welder complains of sudden severe headache and witnessed seizure with loss of consciousness
Mechanisms of presentation of caroticocavernous
 Brit.. Ophthal. (1970) 54, I86 Mechanisms of presentation of caroticocavernous fistulae EDWIN R. BICKERSTAFF The Midland CentreJor Neurosurgery and Neurology, Smethwick The clinical features of carotico-cavernous
Brit.. Ophthal. (1970) 54, I86 Mechanisms of presentation of caroticocavernous fistulae EDWIN R. BICKERSTAFF The Midland CentreJor Neurosurgery and Neurology, Smethwick The clinical features of carotico-cavernous
Distal anterior cerebral artery (DACA) aneurysms are. Case Report
 248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
248 Formos J Surg 2010;43:248-252 Distal Anterior Cerebral Artery Aneurysm: an Infrequent Cause of Transient Ischemic Attack Followed by Diffuse Subarachnoid Hemorrhage: Report of a Case Che-Chuan Wang
Spontaneous Intracranial Hypotension Diagnosis and Treatment
 Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
Spontaneous Intracranial Hypotension Diagnosis and Treatment John W. Engstrom MD, Philip R. Weinstein MD, and William P. Dillon M.D. University of California, San Francisco Spontaneous Intracranial Hypotension
What Are We Going to Do? Fourth Year Meds Clinical Neuroanatomy. Hydrocephalus and Effects of Interruption of CSF Flow. Tube Blockage Doctrine
 Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Fourth Year Meds Clinical Neuroanatomy Ventricles, CSF, Brain Swelling etc. David A. Ramsay, Neuropathologist, LHSC What Are We Going to Do? Hydrocephalus and some effects of the interruption of CSF flow
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Blow-in fracture of both orbital roofs caused by shear strain to the skull. Department of Neurosurgery, Kanto Teishin Hospital, Tokyo, Japan
 J Neurosurg 49:734-738, 1978 Blow-in fracture of both orbital roofs caused by shear strain to the skull Case report OSAMU SATO, M.D., HIROSHI KAMITANI, M.D., AND TAKASHI KOKUNAI, M.D. Department of Neurosurgery,
J Neurosurg 49:734-738, 1978 Blow-in fracture of both orbital roofs caused by shear strain to the skull Case report OSAMU SATO, M.D., HIROSHI KAMITANI, M.D., AND TAKASHI KOKUNAI, M.D. Department of Neurosurgery,
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution
 CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
CT and MR findings of systemic lupus erythematosus involving the brain: Differential diagnosis based on lesion distribution Poster No.: C-2723 Congress: ECR 2010 Type: Educational Exhibit Topic: Neuro
Treatment of Acute Hydrocephalus After Subarachnoid Hemorrhage With Serial Lumbar Puncture
 19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
19 Treatment of Acute After Subarachnoid Hemorrhage With Serial Lumbar Puncture Djo Hasan, MD; Kenneth W. Lindsay, PhD, FRCS; and Marinus Vermeulen, MD Downloaded from http://ahajournals.org by on vember,
Carotid Cavernous Fistula
 Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Chief Complaint: Double vision. Carotid Cavernous Fistula Alex W. Cohen, MD, PhD; Richard Allen, MD, PhD May 14, 2010 History of Present Illness: A 46 year old female patient presented to the Oculoplastics
Traumatic Brain Injuries
 Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
Traumatic Brain Injuries Scott P. Sherry, MS, PA-C, FCCM Assistant Professor Department of Surgery Division of Trauma, Critical Care and Acute Care Surgery DISCLOSURES Nothing to disclose Discussion of
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE
 THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
THE ROLE OF IMAGING IN DIAGNOSIS OF SUBDURAL HEMATOMA: REVIEW ARTICLE * Dr. Sumendra Raj Pandey, Prof. Dr. Liu Pei WU, Dr. Sohan Kumar Sah, Dr. Lalu Yadav, Md. Sadam Husen Haque and Rajan KR. Chaurasiya
Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions
 https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
https://doi.org/10.1007/s12028-017-0487-3 ORIGINAL ARTICLE Ventriculostomy and Risk of Upward Herniation in Patients with Obstructive Hydrocephalus from Posterior Fossa Mass Lesions Sherri A. Braksick
An Introduction to Imaging the Brain. Dr Amy Davis
 An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
An Introduction to Imaging the Brain Dr Amy Davis Common reasons for imaging: Clinical scenarios: - Trauma (NICE guidelines) - Stroke - Tumours - Seizure - Neurological degeneration memory, motor dysfunction,
Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report
 Neurosurg Focus 7 (4):Article 5, 1999 Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report Akira Watanabe, M.D.,
Neurosurg Focus 7 (4):Article 5, 1999 Endosaccular aneurysm occlusion with Guglielmi detachable coils for obstructive hydrocephalus caused by a large basilar tip aneurysm Case report Akira Watanabe, M.D.,
A Less Invasive Approach for Ruptured Aneurysm with Intracranial Hematoma: Coil Embolization Followed by Clot Evacuation
 A Less Invasive Approach for Ruptured Aneurysm with Intracranial Hematoma: Coil Embolization Followed by Clot Evacuation Je Hoon Jeong, MD 1 Jun Seok Koh, MD 1 Eui Jong Kim, MD 2 Index terms: Endovascular
A Less Invasive Approach for Ruptured Aneurysm with Intracranial Hematoma: Coil Embolization Followed by Clot Evacuation Je Hoon Jeong, MD 1 Jun Seok Koh, MD 1 Eui Jong Kim, MD 2 Index terms: Endovascular
Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/300 Clinical Outcome of Borderline Subdural Hematoma with 5-9 mm Thickness and/or Midline Shift 2-5 mm Raja S Vignesh
Applicable Neuroradiology
 For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
For the Clinical Neurology Clerkship LSU Medical School New Orleans Amy W Voigt, MD Clerkship Director Introduction The field of Radiology first developed following the discovery of X-Rays by Wilhelm Roentgen
Vascular Malformations of the Brain: A Review of Imaging Features and Risks
 Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Vascular Malformations of the Brain: A Review of Imaging Features and Risks Comprehensive Neuroradiology: Best Practices October 27-30, 2016 Sudhakar R. Satti, MD Associate Director Neurointerventional
Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving the Laterocavernous Sinus
 Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Journal of Neuroendovascular Therapy 2017; 11: 1 7 Online November 9, 2016 DOI: 10.5797/jnet.oa.2016-0062 Transvenous Embolization of Cavernous Sinus Dural Arteriovenous Fistulas with Shunts Involving
Meninges and Ventricles
 Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
Meninges and Ventricles Irene Yu, class of 2019 LEARNING OBJECTIVES Describe the meningeal layers, the dural infolds, and the spaces they create. Name the contents of the subarachnoid space. Describe the
PTA 106 Unit 1 Lecture 3
 PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
PTA 106 Unit 1 Lecture 3 The Basics Arteries: Carry blood away from the heart toward tissues. They typically have thicker vessels walls to handle increased pressure. Contain internal and external elastic
CT - Brain Examination
 CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
CT - Brain Examination Submitted by: Felemban 1 CT - Brain Examination The clinical indication of CT brain are: a) Chronic cases (e.g. headache - tumor - abscess) b) ER cases (e.g. trauma - RTA - child
V. CENTRAL NERVOUS SYSTEM TRAUMA
 V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
V. CENTRAL NERVOUS SYSTEM TRAUMA I. Concussion - Is a clinical syndrome of altered consiousness secondary to head injury - Brought by a change in the momentum of the head when a moving head suddenly arrested
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum
 Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal
 AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
AJNR Am J Neuroradiol 20:2016 2020, November/December 1999 Case Report Three Cases of Dural Arteriovenous Fistula of the Anterior Condylar Vein within the Hypoglossal Canal Robert Ernst, Robert Bulas,
Cerebral aneurysms A case study
 August 2001 Cerebral aneurysms A case study Heather L. Hinds, Harvard Medical School Year III Our Patient 57yr old woman History of migraines Presents with persistent headache several months duration different
August 2001 Cerebral aneurysms A case study Heather L. Hinds, Harvard Medical School Year III Our Patient 57yr old woman History of migraines Presents with persistent headache several months duration different
INTRACRANIAL PRESSURE -!!
 INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
INTRACRANIAL PRESSURE - Significance raised ICP main cause of death in severe head injury main cause of morbidity in moderate and mild head injury main target and prognostic indicator in the ITU setting
Cavernous sinus thrombosis: Departmental guidelines
 Michele Long Division of Otorhinolaryngology Faculty of Health Sciences Tygerberg Campus, University of Stellenbosch Cavernous sinus thrombosis: Departmental guidelines Anatomy- cavernous sinus 2cm in
Michele Long Division of Otorhinolaryngology Faculty of Health Sciences Tygerberg Campus, University of Stellenbosch Cavernous sinus thrombosis: Departmental guidelines Anatomy- cavernous sinus 2cm in
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum
 Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
Intracranial complications of sinusitis and mastoiditis in children: imaging spectrum Poster No.: R-0098 Congress: RANZCR ASM 2013 Type: Scientific Exhibit Authors: L. L. Wang, J. Leach; Cincinnati/US
Importance of Hematoma Removal Ratio in Ruptured Middle Cerebral Artery Aneurysm Surgery with Intrasylvian Hematoma
 Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.1.5 Original Article Importance of Hematoma Removal Ratio in Ruptured Middle
Journal of Cerebrovascular and Endovascular Neurosurgery pissn 2234-8565, eissn 2287-3139, http://dx.doi.org/10.7461/jcen.2017.19.1.5 Original Article Importance of Hematoma Removal Ratio in Ruptured Middle
Brain Injuries. Presented By Dr. Said Said Elshama
 Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Brain Injuries Presented By Dr. Said Said Elshama Types of head injuries 1- Scalp injuries 2- Skull injuries 3- Intra Cranial injuries ( Brain ) Anatomical structure of meninges Intra- Cranial Injuries
Neurosurgical decision making in structural lesions causing stroke. Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery)
 Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Neurosurgical decision making in structural lesions causing stroke Dr Rakesh Ranjan MS, MCh, Dip NB (Neurosurgery) Subarachnoid Hemorrhage Every year, an estimated 30,000 people in the United States experience
Cranial cavity. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Cranial cavity Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-DURA MATER 2-ARACHNOID MATER 3-PIA MATER
Cranial cavity Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology The Meninges The brain in the skull is surrounded by three membranes or meninges: 1-DURA MATER 2-ARACHNOID MATER 3-PIA MATER
