Regional anesthesia and invasive techniques to manage head and neck pain
|
|
|
- Cody West
- 5 years ago
- Views:
Transcription
1 Otolaryngol Clin N Am 36 (2003) Regional anesthesia and invasive techniques to manage head and neck pain Morton Rosenberg, DMD a, James C. Phero, DMD b, * a Department of Anesthesia and Oral and Maxillofacial Surgery, College of Dentistry, Tufts University Schools of Dental Medicine and Medicine, 1 Kneeland Street, Boston, MA 02111, USA b Anesthesia Department, College of Medicine, University of Cincinnati, 3558 MSB, 231 Albert Sabin Way, PO Box , Cincinnati, OH , USA Head and neck regional anesthesia provides the practitioner the option of managing acute and chronic pain situations. The dermatomes are well defined with good options for approaching and blocking the majority of peripheral nerves in this region of the body (Figs. 1 and 2). Local anesthesia considerations Carefully administered in select patients, nerve blocks can be effective in the management of acute or procedural pain as well as chronic head and neck pain. For surgery in shorter cases, 1% to 2% lidocaine or 2% to 3% mepivacaine are effective in producing rapid onset of regional anesthesia with short duration. With the addition of epinephrine 1:100,000 or 1:200,000, a degree of hemostasis can be obtained and anesthesia prolonged. Because of bupivacaine s longer onset time, this agent is often injected after the initial block has been assured to provide a sustained block. Reinforcement of the block using 0.5% bupivacaine can provide anesthesia for longer procedures and be used as an integral part of postoperative pain control strategies. Sympathetic blockade can be achieved by using concentrations of local anesthetic below that required for sensory and motor loss. Thus, the practitioner can produce a select block involving unmyelinated C fibers and A delta fibers without significant impairment of motor function. Typically, 0.25% bupivacaine is used for diagnostic and therapeutic blocks for pain that is sympathetically mediated. Sympathetic blockade significantly outlasts the pharmacologic action of the local anesthetic. Neurolytic blocks can be * Corresponding author. address: james.phero@uc.edu (J.C. Phero) /03/$ - see front matter Ó 2003 Elsevier Inc. All rights reserved. doi: /s (03)
2 1202 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 1. Dermatomes indicating innervation of the head and neck. produced by the use of alcohol, phenol, cryotherapy (ÿ70 centigrade), or thermocoagulation (70 centigrade). The practitioner must use caution with patients on anticoagulant therapy and infection at the site of the block. Local anesthesia toxicity is a concern where large volumes of concentrated local anesthetic are used. Clinicians must use care to avoid injecting more milligrams per kilogram than is recommended to avoid a toxic response, which could potentially lead to CNS, respiratory, and cardiac depression. When there is a need for a large volume of local anesthetic to be administered, the incidence of toxicity can be avoided by using the lowest concentration of local anesthetic that will produce the required block and calculating the maximum volume of this solution that each patient may receive in advance of starting the injection. This is especially true in the pediatric patient where drug toxicity can become a life-threatening complication if maximum doses are not strictly controlled. Additionally, neurolytic agents may produce significant complications related to development of neuritis and vascular compromise.
3 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 2. Anatomical location of peripheral cutaneous nerves of the head and neck. Cervical plexus The cervical plexus is formed by the first four cranial nerves. The dorsal and ventral roots join to form a spinal nerve as they exit through the intervertebral foramen. The cervical spinal nerves then divide into dorsal and ventral divisions. These dorsal branches innervate the muscles and skin of the back of the neck and head. The ventral branches of C1-4 form the cervical plexus. These nerves emerge from the intervertebral foramina and then lie on the transverse processes and scalenous medius muscle covered by the prevertebral fascia. Lateral to the transverse process, these cervical nerves are in a fascial space derived from the fascia of the muscles attached to the tubercles of the transverse processes. This space is continuous with the interscalene fascial plane and inferior to it, allowing for a single injection to anesthetize the plexus. The anterior primary rami of C2-4 form three loops, which are referred to as the cervical plexus. This plexus lies behind the sternomastoid muscle, giving off superficial and deep branches [1]. The superficial branches innervate skin and superficial tissues in the head, neck, and shoulder. The four branches of the superficial cervical plexus are the lesser occipital, the great auricular, the transverse cervical, and the supraclavicular nerves (Fig. 3) [2]. Cervical plexus block is useful for many surgical procedures of the anterior neck, lateral neck, and supraclavicular fossa (Box 1). Anatomical landmarks for accessing the cervical plexus include the tip of the mastoid process of the temporal bone and the anterior tubercle of C6 transverse process at the level of the cricoid arch. To achieve superficial cervical plexus block, the midpoint of the sternomastoid muscle at the posterior border is identified. The needle is inserted subcutaneously behind and deep to the sternomastoid muscle with 5 ml of local anesthetic injected.
4 1204 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 3. The cervical plexus with branches. Also, 5 ml of local anesthetic is injected from this point going superiorly, and 5 ml of local is directed inferiorly [3]. Deep cervical plexus block is most commonly accomplished by way of a lateral approach rather than a posterior one. Traditionally, three needles are inserted at the C2-4 levels [4]. However, a single injection technique has become more popular for producing blockade of the deep cervical plexus. A single needle is placed at the C4 level behind the sternomastoid muscle and directed slightly cephalad toward the C4 process. In the adult patient, the C4 transverse process is located approximately 3 cm below C2, which is 1 to 2 cm below the mastoid process. The volume of local anesthetic required to block C2-4 using this approach is 10 to 15 ml [5]. Cervical plexus block combined with laryngeal nerve block and subfascial infiltration produces good regional anesthesia for neck surgery (Fig. 4). The practitioner must use care to avoid local anesthetic injection into the subarachnoid space, epidural space, the vertebral artery, and the pleura of the lung. Aspiration before injection is always advocated. The development
5 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Box 1. Cervical plexus block indications Neck dissection Lymph node dissection Superficial neck surgery Thyroidectomy Thyroglossal and branchial cyst surgery Carotid endarterectomy Postoperative pain management after neck surgery Occipital pain management Metastatic pharyngeal pain management of brachial plexus anesthesia on the side opposite the block may indicate developing epidural or spinal anesthesia. Occipital nerve block The sensory innervation of the posterior head and neck comes from the second and third cervical nerves. The lateral section of the posterior scalp is supplied by the lesser occipital and great auricular nerves (Fig. 5). Once the mastoid process, the greater occipital protuberance, and the superior nuchal line have been identified, the practitioner can palpate the occipital arterial pulse which is located one third of the distance from the greater occipital protuberance toward the mastoid [6]. The needle is then placed medial to the artery along this plane and 3 to 5 ml of local anesthetic is injected to achieve the block. Trigeminal blocks The trigeminal nerve is the largest of the cranial nerves (Fig. 6), containing sensory and motor fibers. General somatic afferent nerve fibers carry sensory impulses from the face (Fig. 7). Somatic impulses, including thermal, touch, and pain, are transmitted from the skin of the face and forehead, mucous membranes of the nasal surfaces and oral cavity, the teeth, the anterior twothirds of the tongue, and anterior portions of the cranial dura. Proprioceptive impulses are carried from the teeth, periodontium, hard palate, and temporomandibular joint. The trigeminal nerve is involved in carrying afferent impulses from stretch receptors in the muscles of mastication. Additionally, visceral efferent fibers innervate the muscles of mastication, the tensor tympani and tensor veli palatine muscles, muscles of the eye, and facial muscles.
6 1206 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 4. Regional anesthesia for neck surgery. (Adapted from Labat G. Regional anesthesia its technique and clinical application. Philadelphia: WB Saunders; 1922.) First division trigeminal/orbital blocks Block of the supratrochlear and supraorbital nerves is useful for forehead surgical procedures. Additionally, these blocks may provide relief of neuralgias and headaches in the distribution of the ophthalmic nerve. The supraorbital nerve traverses through the supraorbital foramen, which lies approximately 2 to 3 cm lateral to the midline of the face at the inferior edge of the supraorbital ridge. The supratrochlear nerve exits the orbit between the trochlea and the supraorbital foramen to innervate the lower part of the forehead. To block the supraorbital nerve, a short, small-gauge needle is advanced perpendicular to the skin toward the supraorbital notch with injection of 1 to 2 ml of local anesthetic once paresthesia is obtained or the foramina encountered. Caution should be used not to auger the needle into the foramina to avoid potential nerve damage. To block the supratrochlear nerve, a short, small- gauge needle is advanced medial to the supraorbital notch. Again, the block is obtained with 1 to 2 ml of local anesthetic. Orbicularis oculi muscle block results in eyelid paresis. This block is common with intraocular surgery to prevent blepharospasm. Local anesthetic is infiltrated at the lower lateral angle of the inferior orbital
7 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 5. Occipital nerve anatomy. (Adapted from Tucker JH, Flynn JF. Head and neck regional blocks. In: Brown DL, editor. Regional anesthesia and analgesia. Philadelphia: WB Saunders; p. 240.) margin along the lateral margin of the orbit and along the inferior orbital margin. Retrobulbar block is performed by needle entry through the lower eyelid at the lower lateral angle of the orbit. The needle is advanced to enter at the lower lateral angle of the orbit and directed toward the apex of the orbit. As the ciliary ganglion is located deep in the orbit lateral to the optic nerve and lateral to the rectus muscle, the adult needle depth in the adult patient from the skin should not exceed 3.5 cm to avoid puncturing the blood vessels in the apex of the orbit [7]. A local anesthetic volume of 2 to 4 ml provides satisfactory regional anesthesia. Second and third division trigeminal blocks Extraoral maxillary and mandibular blockade Intraoral injections to achieve nerve blockade of the maxillary and mandibular branches are the trigeminal nerves are commonly performed by the dental profession. However, obtaining definitive regional anesthesia of these branches of the trigeminal nerve can be more easily obtained by using the lateral extraoral approach. The needle enters the skin at the point of intersection of the lower border of the zygoma and the anterior border of the mandibular ramus through the coronoid notch. For blockade of the maxillary nerve, the needle is directed slightly upward, forward, and
8 1208 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 6. Trigeminal nerve anatomy. (Adapted from Phero, JC, Robins G. Eye, ear, nose, and throat surgery. In: Raj PP, editor. Handbook of regional anesthesia. New York: Churchill Livingstone; p. 14.) medially until it meets the greater wing of the sphenoid. For blockade of the mandibular nerve, the needle starts at the same place on the skin as the maxillary extraoral block. After the needle contacts the lateral pterygoid plate, it is withdrawn and reinserted upward and slightly posterior until a paresthesia is noted or the needle has reached a depth of 5 cm. Though the anterolateral approach is a consideration for maxillary nerve blockade, the lateral approach appears to offer more consistent nerve blockade (Fig. 8). The maxillary, second division of the trigeminal nerve is a sensory nerve. It exits the skull through the foramen rotundum, enters the pterygopalatine fossa extending into the inferior orbital fissure and then to the oral cavity. It exits in the front of the maxilla by the infraorbital foramen. The posterior
9 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 7. Trigeminal nerve sensory dermatomes. superior alveolar and zygomatic nerves originate in the pterygopalatine fossa. The maxillary nerve branches into the infraorbital nerve at the infraorbital fissure. Infraorbital block The infraorbital foramen is approximately 2 to 3 cm lateral to the midline of the face. It emerges from the infraorbital foramen and dives into four branches: the inferior palpebral, the external nasal, the internal nasal, and the superior labial. These branches innervate the lower eyelid, lateral inferior portion of the nose and vestibule, and the upper lid and mucosa. The anterior superior alveolar nerve branches from the infraorbital nerve in the anterior part of the infraorbital canal and innervates the maxillary incisor and cuspid teeth. The extraoral approach to this nerve is the preferred access for nerve blockade. The infraorbital ridge of the maxillary bone is located and the infraorbital foramen palpated approximately 2 cm from the lateral surface of the nose. The anterior portion of the canal in the orbit is typically covered
10 1210 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 8. Lateral extraoral approach for maxillary and mandibular nerve regional anesthesia. (Adapted from Pai UT, Nayak R. Maxillary, mandibular, and glossopharyngeal nerve blocks. In: Benzon HT, Raja SN, Borsook D. Essentials of pain medicine and regional anesthesia. New York: Churchill Livingstone; p. 10.) with a thin plate of bone, so the needle should start 0.5 cm below and slightly medial to the foramen to allow for the backward and upward slant of the infraorbital canal. The needle must be advanced past the opening of the infraorbital canal so that the anterior superior alveolar nerve is not blocked. However, the needle should not be advanced more than 0.5 cm past the entry into the infraorbital foramen. A volume of 1 to 3 ml of local anesthetic is sufficient for nerve blockade. Nasopalatine block This injection provides soft tissue palatal anesthesia or to supplement anesthesia of the nasal passages (Fig. 9). The needle is advanced 0.5 cm intraorally into the incisor canal behind the maxillary incisors. As the palatal tissues are not highly elastic, the practitioner should slowly inject 0.25 to 0.5 ml of local anesthetic for the blockade. Sphenopalatine block The sphenopalatine ganglion (pterygopalatine, nasal, or Meckel s ganglion) is one of four autonomic ganglia in the head. The ganglion is a 5 mm triangular structure comprising the largest group of neurons in the head, except for the brain. Major branches of the trigeminal nerve, facial nerve, carotid plexus, and superior cervical ganglion arise from the sphenopalatine ganglion. Nerve blockade is obtained by application of topical anesthetic to the upper posterior wall of the nasal pharynx and the upper border of the middle turbinate at the sphenoid. Transnasal injection of 5 to 10 ml of local anesthetic to this region may also be performed for the blockade (Fig. 10).
11 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 9. Anatomy of nasopalatine nerve and anterior ethmoidal nerve. Anterior approach to trigeminal ganglion by way of the foramen ovale A more complex block to anesthetize any of the three trigeminal nerve divisions involves placing the needle through the foramen ovale into the gasserian ganglion (Fig. 11). The subzygomatic approach to the trigeminal nerve ganglion is optimized by use of fluoroscopy to guide the needle into the foramen ovale. A nerve stimulator is often used to differential the exact portion of the nerve the practitioner desires to block. This approach is often used for treatment of chronic trigeminal neuralgia and intractable cancer pain in patients that are refractory to aggressive pharmacological pain management. Longer nerve block duration may be obtained with use of radiofrequency or neurolytic gasserian ganglionotomy. The first division of the trigeminal nerve is most medial and deepest within the foramen. The second division is centrally located and intermediate in depth. The third division is most lateral and superficial. Trigeminal neuralgia therapy with gamma knife radiosurgery Because of the unique therapy offered by gamma knife surgery (GKS) and the contemporary nature of the device, the background and current considerations for the management of trigeminal neuralgia by GKS should be discussed. The revolution of sophisticated software and computer technology combined with advanced radiation physics has produced a new
12 1212 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 10. Anatomy of the sphenopalatine ganglion nerve. tool for the successful treatment of many neurologic conditions, including trigeminal neuralgia. The gamma knife is not a knife but a complex machine that uses cobalt-60 to provide the energy for cutting. It is able to focus a precise intersection of 201 beams of gamma rays to perform radiosurgery. The evolution of high-resolution CT and MRI scans coupled with computer technology permits targets to be clearly defined. Currently, there are 120 gamma knife surgery (GKS) centers around the world and 45 in North America. Arteriovenous malformations, brain metastases, acoustic nerve tumors, meningiomas, and other benign brain tumors can be managed with the gamma knife. Certain functional disorders, such as intractable pain, seizures, the tremors and rigidity of Parkinson s disease, and certain psychoneuroses, have responded to gamma knife radiosurgery. Of special interest to health professions treating patients with head and neck pain is the use of the gamma knife in the treatment of trigeminal neuralgia. Several options exist for the treatment of trigeminal neuralgia. Medical therapy with carbamazepine, phenytoin, and gabapentin has provided good first-line treatment [8 11]. Microvascular decompression, glycerol rhizotomy, radiofrequency rhizotomy, and nerve section have proven effective surgical options [12,13]. Currently, GKS has become a good option for patients unresponsive to medical therapy. Recent advances in imaging and increased experience with this procedure support the value of GKS as a treatment for trigeminal neuralgia.
13 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 11. Lateral skeletal view showing needle entry through the foramen ovale into the gasserian ganglion. In 1951, Lars Leksell, the inventor of the gamma knife, was the first to use radiosurgery for the treatment of functional disorders such as trigeminal neuralgia. Using a conventional stereotactic frame, he aimed the radiation beam produced by an orthovoltage x-ray tube at the trigeminal ganglion [14]. Over the next 40 years, poor imaging, poor target fixation, and the choice of the gasserian ganglion as the target brought less than satisfactory results [15,16]. In 1996 a multicenter study coordinated by the University of Pittsburgh rekindled interest in the radiosurgical treatment of trigeminal neuralgia [17]. In this study, the proximal trigeminal nerve near the pons, rather than the ganglion in Meckel s cavity, was chosen as the target. This permitted direct visualization of the nerve proper to be treated. Highresolution MRI permitted accurate targeting. With this modification, 94% of the patients in the study showed resolution or significant decrease of their pain. Many authors have since reported similar results [18 21]. Success rates are similar to other interventional procedures. Complications are primarily limited to facial numbness, which occurs at a frequency of less than 10%.
14 1214 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) GKS is now being used as a safe alternative to traditional surgery and as first-line therapy for trigeminal neuralgia. Procedure planning is performed by a multidisciplinary group. The expertise of a neuroradiologist, radiation oncologist, medical physicist, and neurosurgeon are combined to provide optimal treatment. GKS is a four-step procedure. The patients are first fitted with the Leksell stereotactic headframe. Because neurophysiologic feedback is not a component of the targeting procedure, high-quality and accurate imaging is necessary. Highresolution images of the target and the surrounding structures must be obtained. MRI is the neurodiagnostic modality of choice. Gadolinium enhanced T1-weighted MRI with magnetization-prepared rapid gradient echo, T2-weighted fast spin-echo sequences and other MRI algorithms are used. Long-Tr MR sequences can be used in adjunct to contrast the nerve against the high-signal CSF background. The trigeminal nerve is identified in coronal, axial, and sagittal planes on its course from the brainstem to Meckel s cavity. For patients with pacemakers, metallic foreign bodies, or other contraindications to MRI, high-resolution computerized topography with contrast cisternography can be used [22]. The ElectaLeksell gamma knife unit with cobalt-60 sources is used to irradiate the target. The trigeminal nerve is targeted at the location of an imaged vascular compression or at the site of the trigeminal nerve exit from the pons if no compressing vessel is identified. The effectiveness of treatment at this exit zone is thought to be due to the proximal nerve being covered by oligodendrocyte myelin, which is more radiosensitive than the distal swan-cell myelin, or because of concomitant irradiation to the dorsal root entry zone at the brainstem. Care is taken to protect the brainstem from radiation exposure, which presents minimal difficulty because of the precision of the gamma knife system. Target doses range from 65 to 100 Gy, with a mode of 70 to 90 Gy. Old age and multiple sclerosis are criteria for the lower doses. Higher doses are used for patients with a history of previous trigeminal surgeries. A dose of 80 Gy is effective in 90% of patients, with the risk of partial facial numbness at less than 10%, and a risk of anesthesia dolorosa under 1% [23]. The entire procedure is performed under local anesthesia with sedation. The exact mechanism of GKS pain relief is not known. The majority of patients report an immediate decrease in the intensity of the pain even if the attacks still occur. This is postulated to be the result of an immediate interruption of ephaptic transmission. Several weeks later there is classically complete cessation of the attacks. This is probably secondary to delayed demyelination injury to the nerve. Regis et al [24] have speculated that gamma knife irradiation has a differential effect on myelinated and unmyelinated fibers, allowing for control of pain without dysesthesia. This is not supported by the recent finding of Kodziolka et al [25]. They performed histologic analysis of two baboons treated with gamma knife. They targeted the trigeminal nerve just anterior to the pons and used doses in the 80 to 100 Gy range. All irradiated nerves exhibited axonal
15 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) degeneration with remnants of some myelinated axons. Myelinated and unmyelinated fibers were affected. Nerve necrosis was identified with the 100 Gy treatment. The pathohistologic changes of lower doses are not known, and further studies are needed. Young et al reported a 74.5% rate of complete relief, and a 95.5% response rate [26,27]. In their multicenter study published in 1996, 60% of the patients became pain-free and required no further medical therapy, 17% had a 50% to 90% reduction in pain, and 9% had slight pain improvement [19,21,28]. Of those that attained complete relief, only 10% developed a relapse of their pain. Similar high response rates and long-term pain relief have been found by several other authors. The effectiveness of the treatment is confounded by the type of neuralgia. Additional studies found that the highest response rate was for essential neuralgia (77%) followed by neuralgia with multiple sclerosis (43%), postherpetic neuralgia (38 44%), and atypical neuralgia (33%) [29,30]. Patients with atypical symptomatology or those with prior surgical procedures, have lower initial and long term response rates [27]. In a study of 172 patients, Brisman found that those treated with gamma knife as primary management had better outcomes than those treated as secondary treatment. Thus, GKS may be considered for first-line treatment in some patients. The overall response rate with gamma knife compares favorably with that of other surgical modalities. This gains support when the practitioner considers that most patients undergoing GKS present with having failed medical and surgical treatment and present a challenge. Side effects of GKS are limited primarily to facial paresthesias or sensory loss. In most reports the rate of such complications is less than 10%. In the 1996 Young et al multicenter trial, 6% of patients developed increased paresthesia after the procedure [26,27]. Nicol et al found that higher doses (90 Gy) might be associated with increased rates of paresthesia (16.7%) and dysgeusia (9.5%) [31]. The overall rate of facial paresthesia is slightly higher than MVD but substantially lower than the 60% to 80% quoted for percutaneous procedures [32,33]. Unlike traditional surgery, though, GKS does not carry the increased risk of infection, anesthesia complications, hematoma formation, CSF leak, facial weakness, hearing loss, and brainstem injury. Serious side effects are rare, no hospital stay is usually required, treatment is accomplished in one session, and patients may return in a short time to normal activities. Glossopharyngeal block The glossopharyngeal nerve is the ninth cranial nerve. It exits through the intermediate compartment of the jugular foramen. It then runs between the internal carotid artery and internal jugular vein and travels around the stylopharyngeus muscle deep to the styloid process and goes toward the pharynx and the tongue. The nerve supplies motor fibers to the pharyngeal muscles and sensory fibers to the middle ear, posterior third of the tongue, and
16 1216 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Fig. 12. Anatomy of the autonomic nerves in the head in relation to the sphenopalatine ganglion. the pharynx. It innervates the carotid sinus and carotid body. It is important to remember the close proximity of the glossopharyngeal nerve to the vagus nerve, accessory nerve, and the sympathetic trunk. In the adult patient, a 3- inch needle is required to perform this block. The practitioner must gently contact the styloid process with the needle entering the skin at a point midway between the angle of the mandible and the mastoid process. Once the styloid process has been identified, the needle is withdrawn and redirected anterior to the styloid process at a depth 0.5 cm further than when the styloid was identified. Then, 2 to 3 ml of local anesthetic is deposited for the blockade. Stellate ganglion/cervicothoracic ganglion sympathetic block The stellate ganglion is located between the anterolateral surface at the seventh cervical vertebral body and the neck of the first rib. The
17 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) Box 2. Stellate/cervicothoracic ganglion block indications Complex regional pain syndrome (CRPS) Type 1 (reflex sympathetic dystrophy) Complex regional pain syndrome (CRPS) Type 2 (causalgia) Neuropathic pain states (postherpetic neuralgia) Raynaud s disease Vascular occlusion or impaired circulation Scleroderma and arteriopathies Occlusive vascular disease cervicothoracic ganglion is a continuation of this autonomic chain and located at the sixth cervical vertebral body. The cervicothoracic ganglion is formed by the joining of the most inferior cervical and the first thoracic sympathetic ganglia (Fig. 12). This block has several indications for the diagnosis and management of chronic pain conditions (Box 2). Typically, this block is performed at the C6 level, which reduces needle entry to the vertebral artery and the lung. The cervicothoracic ganglion is Fig. 13. Cervicothoracic ganglion paratracheal approach block. Transverse section at the C6 level showing the needle medial to the finger, which is retracting the carotid artery laterally.
18 1218 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) formed by the joining of the most inferior cervical and the first thoracic sympathetic ganglia. This block has several indications for the diagnosis and management of chronic pain conditions (see Box 2). The anterior paratracheal technique is commonly used. Local anesthetic concentration can be reduced, as autonomic nerves (C-fibers) are small with no myelin. Lidocaine 0.5% or bupivacaine 0.25% is effective. Needle placement for the cervicothoracic ganglion block requires the patient to be supine with the needle inserted vertically at 90 degrees between the cricoid cartilage and the carotid artery to touch the anterior tubercle on the transverse process of C6 (Fig. 13). A 10-mL dose of local anesthetic is required for sympathetic blockade. Careful aspiration before injection is mandatory because injection of only a small volume of local anesthetic into the vertebral artery can lead to immediate convulsion, blindness, and loss of consciousness [34]. This block will interrupt sympathetic outflow to the face, head, neck, and upper extremity. Summary Regional anesthesia of the head and neck is an effective method of obtaining surgical anesthesia for various procedures. Diagnostic and therapeutic head and neck blocks can also assist with the diagnosis and management of many chronic pain conditions, including headache, postherpetic neuralgia, and cancer pain in this region. Gamma knife surgery offers a unique approach to the management of refractory trigeminal neuralgia. Because of the proximity of so many critical structures adjacent to these nerves, a solid understanding of the anatomical basis of these nerve blocks is necessary. Appropriate patient selection, monitoring, proper injection technique, knowledge of the pharmacokinetics and pharmacodynamics of local anesthetics and vasoconstrictors, possible drug interactions, and recommended doses will ensure safe and successful application of head and neck nerve blockade. References [1] Pappas JL, Warfield CAKCH. Cervical plexus blockade. In: Waldman SD, Winnie AP, editors. Interventional pain management. Philadelphia: WB Saunders; p [2] Tucker JH, Flynn JF. Head and neck regional blocks. In: Brown DL, editor. Regional anesthesia and analgesia. Philadelphia: WB Saunders; p [3] Raj PP, Pai U, Rawal N. Techniques of regional anesthesia in adults. Clinical practice of regional anesthesia. New York: Churchill Livingston; p [4] Murphy TM. Somatic blockade of head and neck. In: Cousins MJ, Bridenbaugh PO, editors. Neural blockade in clinical anesthesia and management of pain. Philadelphia: Lippincott-Raven; p [5] Winnie AP, Ramamurthy S, Durrani Z, Radonjic R. Interscalene cervical plexus block: a single injection technique. Anesth Analg 1975;54: [6] Tucker JH, Flynn JF. Head and neck regional blocks. In: Brown DL, editor. Regional anesthesia and analgesia. Philadelphia: WB Saunders; p [7] Allen ED, Elkington AR. Local anaesthesia and the eye. Br J Anaesth 1980;52:
19 M. Rosenberg, J.C. Phero / Otolaryngol Clin N Am 36 (2003) [8] Sidebottom A, Maxwell A. The medical and surgical management of trigeminal neuralgia. J Clin Pharm Ther 1995;20:31 5. [9] Green MW, Selman JE. Review article: the medical management of trigeminal neuralgia. Headache 1991;31: [10] Perkin GD. Trigeminal neuralgia. Curr Treat Options Neurol 1999;1: [11] Zakrewska JM, Patsalos PN. Drugs used in the management of trigeminal neuralgia. Oral Surg Oral Med Oral Pathol 1992;74: [12] Zakrewska JM. Trigeminal neuralgia. Prim Dent Care 1997;1997:17 9. [13] Zakrewska JM. Surgical management of trigeminal neuralgia. Br Dent J 1991;170:61 2. [14] Leksell L. The stereotaxic method and radiosurgery of the brain. Acta Chir Scand 1951;102: [15] Leksell L. Sterotaxic radiosurgery in trigeminal neuralgia. Acta Chir Scand 1971;137: [16] Lindquist C, Kihlstrom L, Hellstrand E. Functional neurosurgery a future for the gamma knife. Stereotact Funct Neurosurg 1991;57: [17] Kondziolka D, Lunsford LDFJC, Young RF, et al. Stereotactic radiosurgery for trigeminal neuralgia: a multiinstitutional study using the gamma unit. J Neurosurg 1996;84: [18] Chang JW, Chang JHPYG, Chung SS. Gamma knife radiosurgery for idiopathic and secondary trigeminal neuralgia. J Neurosurg 2000;93: [19] Han PP, Shetter AG, Smith KA, et al. Gamma knife radiosurgery for trigeminal neuralgia: experience at the Barrow Neurological Institute. Stereotact Funct Neurosurg 1999;73: [20] Rogers CL, Shetter AG, Fiedler JA, et al. Gamma knife radiosurgery for trigeminal neuralgia: the initial experience of The Barrow Neurological Institute. Int J Radiat Oncol Biol Phys 2000;47: [21] Rand RW. Leksell gamma knife treatment of tic douloureux. Neurosurg Clin N Am 1997;8:75 8. [22] Worthington C, Hutson K, Boulware R, et al. Computerized tomography cisternography of the trigeminal nerve for sterotactic radiosurgery. Case report. J Neurosurg 2000;93: [23] Brisman R, Mooij R. Gamma knife radiosurgery for trigeminal neuralgia: dose-volume histograms for the brainsteam and trigeminal nerve. J Neurosurg 2000;93: [24] Regis J, Bartolomei F, Metellus P, et al. Radiosurgery for trigeminal neuralgia and epilepsy. Neurosurg Clin N Am 1999;10: [25] Kondziolka D, Lacomis D, Niranjan A, et al. Histological effects of trigeminal nerve radiosurgery in a primate model: implications for trigeminal neuralgia radiosurgery. Neurosurgery 2000;46: [26] Young RF, Vermeulen SS, Grimm P, et al. Gamma knife radiosurgery for treatment of trigeminal neuralgia: idiopathic and tumor related. Neurology 1997;48: [27] Young RF, Vermulen S, Posewitz A. Gamma knife radiosurgery for the treatment of trigeminal neuralgia. Stereotact Funct Neurosurg 1998;70: [28] Kondziolka D, Perez B, Flickinger JC, et al. Gamma knife radiosurgery for trigeminal neuralgia: results and expectations. Arch Neurol 1998;55: [29] Urgosik D, Vymazal J, Vladyka V, Liscak R. Treatment of postherpetic trigeminal neuralgia with the gamma knife. J Neurosurg 2000;93: [30] Urgosik D, Vymazal J, Vladyka V, Liscak R. Gamma knife treatment of trigeminal neuralgia: clinical and electrophysiological study. Stereotact Funct Neurosurg 1998;70: [31] Nicol B, Regine WF, Courtney C, et al. Gamma knife radiosurgery using 90 Gy for trigeminal neuralgia. J Neurosurg 2000;93: [32] Brown JA, McDaniel MD, Weaver MT. Percutaneous trigminal nerve compression for treatment of trigeminal neuralgia: results in 50 patients. Neurosurgery 1993;32: [33] Taha JM, Tew JMJ, Buncher CR. A prospective 15-year follow-up of 154 consecutive patients with trigeminal neuralgia treated by percutaneous stereotactic radiofrequency rhizotomy. J Neurosurg 1995;83: [34] Szeinfeld M, Laurencio M, Pallares VS. Total reversible blindness following Stellate ganglion block. Anal Analg 1981;60:
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Anatomic Relations Summary. Done by: Sohayyla Yasin Dababseh
 Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Veins of the Face and the Neck
 Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Veins of the Face and the Neck Facial Vein The facial vein is formed at the medial angle of the eye by the union of the supraorbital and supratrochlear veins. connected through the ophthalmic veins with
Prevertebral Region, Pharynx and Soft Palate
 Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Unit 20: Prevertebral Region, Pharynx and Soft Palate Dissection Instructions: Step1 Step 2 Step 1: Insert your fingers posterior to the sternocleidomastoid muscle, vagus nerve, internal jugular vein,
Skull-2. Norma Basalis Interna Norma Basalis Externa. Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Skull-2 Norma Basalis Interna Norma Basalis Externa Dr. Heba Kalbouneh Associate Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
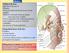 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Trigeminal Nerve Worksheets, Distributions Page 1
 Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Structure Location Function
 Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Frontal Bone Cranium forms the forehead and roof of the orbits Occipital Bone Cranium forms posterior and inferior portions of the cranium Temporal Bone Cranium inferior to the parietal bone forms the
Mohammad Hisham Al-Mohtaseb. Lina Mansour. Reyad Jabiri. 0 P a g e
 2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
THIEME. Scalp and Superficial Temporal Region
 CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
CHAPTER 2 Scalp and Superficial Temporal Region Scalp Learning Objectives At the end of the dissection of the scalp, you should be able to identify, understand and correlate the clinical aspects: Layers
Face. Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face
 Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
Face Definition: The area between the two ears and from the chin to the eye brows. The muscles of the face The muscle of facial expression (include the muscle of the face and the scalp). All are derived
The Neck the lower margin of the mandible above the suprasternal notch and the upper border of the clavicle
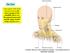 The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
The Neck is the region of the body that lies between the lower margin of the mandible above and the suprasternal notch and the upper border of the clavicle below Nerves of the neck Cervical Plexus Is formed
Introduction to Local Anesthesia and Review of Anatomy
 5-Sep Introduction and Anatomy Review 12-Sep Neurophysiology and Pain 19-Sep Physiology and Pharmacology part 1 26-Sep Physiology and Pharmacology part 2 Introduction to Local Anesthesia and Review of
5-Sep Introduction and Anatomy Review 12-Sep Neurophysiology and Pain 19-Sep Physiology and Pharmacology part 1 26-Sep Physiology and Pharmacology part 2 Introduction to Local Anesthesia and Review of
Mandibular and Maxillary Anesthesia
 Mandibular and Maxillary Anesthesia Uses of the Conduction Technique JACK H. SELTSAM, D.D.S., M.D., Los Angeles THE ARMAMENTARIUM of a surgeon who operates on the head and neck should include the ability
Mandibular and Maxillary Anesthesia Uses of the Conduction Technique JACK H. SELTSAM, D.D.S., M.D., Los Angeles THE ARMAMENTARIUM of a surgeon who operates on the head and neck should include the ability
Introduction to Head and Neck Anatomy
 Introduction to Head and Neck Anatomy Nervous Tissue Controls and integrates all body activities within limits that maintain life Three basic functions 1. sensing changes with sensory receptors 2. interpreting
Introduction to Head and Neck Anatomy Nervous Tissue Controls and integrates all body activities within limits that maintain life Three basic functions 1. sensing changes with sensory receptors 2. interpreting
Chapter 7 Part A The Skeleton
 Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Chapter 7 Part A The Skeleton Why This Matters Understanding the anatomy of the skeleton enables you to anticipate problems such as pelvic dimensions that may affect labor and delivery The Skeleton The
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi
 Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Posterior Triangle of the Neck By Prof. Dr. Muhammad Imran Qureshi For the purpose of anatomical description the neck is sub divided into two major triangles, the Anterior and the Posterior by muscle bellies
Omran Saeed. Luma Taweel. Mohammad Almohtaseb. 1 P a g e
 2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
Dr.Ban I.S. head & neck anatomy 2 nd y جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
Trigeminal Nerve (V)
 Trigeminal Nerve (V) Lecture Objectives Discuss briefly how the face is developed. Follow up the course of trigeminal nerve from its point of central connections, exit and down to its target areas. Describe
Trigeminal Nerve (V) Lecture Objectives Discuss briefly how the face is developed. Follow up the course of trigeminal nerve from its point of central connections, exit and down to its target areas. Describe
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
Trigeminal Nerve Anatomy. Dr. Mohamed Rahil Ali
 Trigeminal Nerve Anatomy Dr. Mohamed Rahil Ali Trigeminal nerve Largest cranial nerve Mixed nerve Small motor root and large sensory root Motor root Nucleus of motor root present in the pons and medulla
Trigeminal Nerve Anatomy Dr. Mohamed Rahil Ali Trigeminal nerve Largest cranial nerve Mixed nerve Small motor root and large sensory root Motor root Nucleus of motor root present in the pons and medulla
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
The orbit-1. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
The orbit-1 Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Orbital plate of frontal bone Orbital plate of ethmoid bone Lesser wing of sphenoid Greater wing of sphenoid Lacrimal bone Orbital
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
MAXILLA, ORBIT & PTERYGOPALATINE FOSSA Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine Maxilla MAXILLA Superior, middle, and inferior meatus Frontal
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
Cranial nerves.
 Cranial nerves eaglezhyxzy@163.com Key Points of Learning Name Components Passing through Peripheral distribution Central connection Function Cranial nerves Ⅰ olfactory Ⅱ optic Ⅲ occulomotor Ⅳ trochlear
Cranial nerves eaglezhyxzy@163.com Key Points of Learning Name Components Passing through Peripheral distribution Central connection Function Cranial nerves Ⅰ olfactory Ⅱ optic Ⅲ occulomotor Ⅳ trochlear
For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER
 GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
Dr. Sami Zaqout, IUG Medical School
 The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
The skull The skull is composed of several separate bones united at immobile joints called sutures. Exceptions? Frontal bone Occipital bone Vault Cranium Sphenoid bone Zygomatic bones Base Ethmoid bone
Biology 218 Human Anatomy. Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division
 Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Adapted from Martini Human Anatomy 7th ed. Chapter 6 The Skeletal System: Axial Division Introduction The axial skeleton: Composed of bones along the central axis of the body Divided into three regions:
Brain and spinal nerve. By: shirin Kashfi
 Brain and spinal nerve By: shirin Kashfi Nervous system: central nervous system (CNS) peripheral nervous system (PNS) Brain (cranial) nerves Spinal nerves Ganglions (dorsal root ganglions, sympathetic
Brain and spinal nerve By: shirin Kashfi Nervous system: central nervous system (CNS) peripheral nervous system (PNS) Brain (cranial) nerves Spinal nerves Ganglions (dorsal root ganglions, sympathetic
The Pharynx. Dr. Nabil Khouri MD. MSc, Ph.D
 The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
The Pharynx Dr. Nabil Khouri MD. MSc, Ph.D Introduction The pharynx is the Musculo-fascial halfcylinder that links the oral and nasal cavities in the head to the larynx and esophagus in the neck Common
Chapter 7: Head & Neck
 Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Chapter 7: Head & Neck Osteology I. Overview A. Skull The cranium is composed of irregularly shaped bones that are fused together at unique joints called sutures The skull provides durable protection from
Bones of the skull & face
 Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Bones of the skull & face Cranium= brain case or helmet Copyright The McGraw-Hill Companies, Inc. Permission required for reproduction or display. The cranium is composed of eight bones : frontal Occipital
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton
 Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
Human Anatomy and Physiology - Problem Drill 07: The Skeletal System Axial Skeleton Question No. 1 of 10 Which of the following statements about the axial skeleton is correct? Question #01 A. The axial
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi
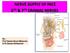 By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function
 The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
The root of the neck Jeff Dupree, Ph.D. e mail: jldupree@vcu.edu OBJECTIVE: To obtain a fundamental knowledge of the root of the neck with respect to structure and function READING ASSIGNMENT: Moore and
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E
 Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
Neural Blocks in Pain Medicine D R M A R G A R E T E B O N E M B C H B F R C A F F P M R C A C O N S U LTA N T I N PA I N M E D I C I N E Stellate Ganglion Block Lumbar Sympathetic Block Requirements Diagnosis
THE SKELETAL SYSTEM. Focus on the Skull
 THE SKELETAL SYSTEM Focus on the Skull Review Anatomical Terms Anterior/Posterior Dorsal/Ventral Medial/Lateral Superior/Inferior Bone Markings - Review Projections for attachment of muscles, ligaments
THE SKELETAL SYSTEM Focus on the Skull Review Anatomical Terms Anterior/Posterior Dorsal/Ventral Medial/Lateral Superior/Inferior Bone Markings - Review Projections for attachment of muscles, ligaments
Bisection of Head & Nasal Cavity 頭部對切以及鼻腔. 解剖學科馮琮涵副教授 分機
 Bisection of Head & Nasal Cavity 頭部對切以及鼻腔 解剖學科馮琮涵副教授 分機 3250 E-mail: thfong@tmu.edu.tw Outline: The structure of nose The concha and meatus in nasal cavity The openings of paranasal sinuses Canals, foramens
Bisection of Head & Nasal Cavity 頭部對切以及鼻腔 解剖學科馮琮涵副教授 分機 3250 E-mail: thfong@tmu.edu.tw Outline: The structure of nose The concha and meatus in nasal cavity The openings of paranasal sinuses Canals, foramens
APPENDICULAR SKELETON 126 AXIAL SKELETON SKELETAL SYSTEM. Cranium. Skull. Face. Skull and associated bones. Auditory ossicles. Associated bones.
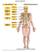 SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
SKELETAL SYSTEM 206 AXIAL SKELETON 80 APPENDICULAR SKELETON 26 Skull Skull and associated s 29 Cranium Face Auditory ossicles 8 4 6 Associated s Hyoid Thoracic cage 25 Sternum Ribs 24 Vertebrae 24 column
Anatomy of the Trigeminal Nerve
 19 Anatomy of the Trigeminal Nerve.1 Introduction 0. The Central Part of the Trigeminal Nerve 1..1 Origin 1.. Trigeminal Nuclei.3 The Peripheral Part of the Trigeminal Nerve 4.3.1 Ophthalmic Nerve 4.3.
19 Anatomy of the Trigeminal Nerve.1 Introduction 0. The Central Part of the Trigeminal Nerve 1..1 Origin 1.. Trigeminal Nuclei.3 The Peripheral Part of the Trigeminal Nerve 4.3.1 Ophthalmic Nerve 4.3.
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان املرحلة الثانية
 جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102-6102 1 The Palate The palate forms the roof of the mouth and the floor of the nasal cavity. It is divided into two
جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102-6102 1 The Palate The palate forms the roof of the mouth and the floor of the nasal cavity. It is divided into two
Tikrit University College of Dentistry Dr.Ban I.S. head & neck anatomy 2 nd y.
 Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
Lec [3]/The scalp The scalp extends from the supraorbital margins anteriorly to the nuchal lines at the back of the skull and down to the temporal lines at the sides. The forehead, from eyebrows to hairline,
University of Palestine. Midterm Exam 2013/2014 Total Grade:
 Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
Course No: DNTS2208 Course Title: Head and Neck Anatomy Date: 09/11/2013 No. of Questions: (50) Time: 1hour Using Calculator (No) University of Palestine Midterm Exam 2013/2014 Total Grade: Instructor
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
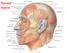 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Dr.Noor Hashem Mohammad Lecture (5)
 Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
Dr.Noor Hashem Mohammad Lecture (5) 2016-2017 If the mandible is discarded, the anterior part of this aspect of the skull is seen to be formed by the hard palate. The palatal processes of the maxillae
3. The Jaw and Related Structures
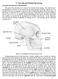 Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Overview and objectives of this dissection 3. The Jaw and Related Structures The goal of this dissection is to observe the muscles of jaw raising. You will also have the opportunity to observe several
Lec [8]: Mandibular nerve:
![Lec [8]: Mandibular nerve: Lec [8]: Mandibular nerve:](/thumbs/94/121295776.jpg) Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
PERIPHERAL NERVOUS SYSTEM
 CHAPTER 13 PERIPHERAL NERVOUS SYSTEM Functional division of nervous system = afferent info to the CNS ascending spinal cord = efferent info from CNS descending spinal cord somatic skin, muscles visceral
CHAPTER 13 PERIPHERAL NERVOUS SYSTEM Functional division of nervous system = afferent info to the CNS ascending spinal cord = efferent info from CNS descending spinal cord somatic skin, muscles visceral
Skull-2. Norma Basalis Interna. Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology
 Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Skull-2 Norma Basalis Interna Dr. Heba Kalbouneh Assistant Professor of Anatomy and Histology Norma basalis interna Base of the skull- superior view The interior of the base of the skull is divided into
Cranium Facial bones. Sternum Rib
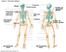 Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Figure 7.1 The human skeleton. Skull Thoracic cage (ribs and sternum) Cranium Facial bones Sternum Rib Bones of pectoral girdle Vertebral column Sacrum Vertebra Bones of pelvic girdle (a) Anterior view
Cranial Nerve VII - Facial Nerve. The facial nerve has 3 main components with distinct functions
 Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions. 4 May 2012
 SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
cardiac plexus is continuous with the coronary and no named branches pain from the heart and lungs
 Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Nerves of the Thoracic Region Nerve Source Branches Motor Sensory Notes cardiac plexus cardiac brs. of the vagus n. and cervical ; thoracic l nn. the heart and lungs cardiac, cervical cardiac, vagal vagus
Skeletal System -Axial System. Chapter 7 Part A
 Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
Skeletal System -Axial System Chapter 7 Part A Skeleton Learn: Names of the s. Identify specific landmarks that allow: Bones to fit into each other, Organs to fit into the cavities, Muscles to attach,
Stereotactic radiosurgery for idiopathic trigeminal neuralgia
 J Neurosurg 97:347 353, 2002 Stereotactic radiosurgery for idiopathic trigeminal neuralgia BRUCE E. POLLOCK, M.D., LOI K. PHUONG, M.D., DEBORAH A. GORMAN, R.N., ROBERT L. FOOTE, M.D., AND SCOTT L. STAFFORD,
J Neurosurg 97:347 353, 2002 Stereotactic radiosurgery for idiopathic trigeminal neuralgia BRUCE E. POLLOCK, M.D., LOI K. PHUONG, M.D., DEBORAH A. GORMAN, R.N., ROBERT L. FOOTE, M.D., AND SCOTT L. STAFFORD,
HBA THE BODY Head & Neck Written Examination October 23, 2014
 HBA 531 - THE BODY Head & Neck Written Examination October 23, 2014 Name: NOTE 2: When asked to trace nerve, artery, or vein pathways, do so by using arrows, e.g., structure a structure b structure c...
HBA 531 - THE BODY Head & Neck Written Examination October 23, 2014 Name: NOTE 2: When asked to trace nerve, artery, or vein pathways, do so by using arrows, e.g., structure a structure b structure c...
Chapter 7. Skeletal System
 Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
Chapter 7 Skeletal System 1 Skull A. The skull is made up of 22 bones: 8 cranial bones, 13 facial bones, and the mandible. B. The Cranium encloses and protects the brain, provides attachments for muscles,
AXIAL SKELETON SKULL
 AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
AXIAL SKELETON SKULL CRANIAL BONES (8 total flat bones w/ 2 paired) 1. Frontal forms forehead & upper portion of eyesocket (orbital) 2. Parietal paired bones; form superior & lateral walls of cranium 3.
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi. E mail: a.al E. mail:
 Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Spinal nerves and cervical plexus Prof. Abdulameer Al Nuaimi E mail: a.al nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Branches of ophthalmic artery Muscles of face A spinal nerve Spinal
Lecture 07. Lymphatic's of Head & Neck. By: Dr Farooq Amanullah Khan PMC
 Lecture 07 Lymphatic's of Head & Neck By: Dr Farooq Amanullah Khan PMC Dated: 28.11.2017 Lymphatic Vessels Of the 800 lymph nodes in the human body, 300 are in the Head & neck region. The lymphatic vessels
Lecture 07 Lymphatic's of Head & Neck By: Dr Farooq Amanullah Khan PMC Dated: 28.11.2017 Lymphatic Vessels Of the 800 lymph nodes in the human body, 300 are in the Head & neck region. The lymphatic vessels
Head and Face Anatomy
 Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Head and Face Anatomy Epicranial region The Scalp The soft tissue that covers the vault of skull. Extends from supraorbital margin to superior nuchal line. Layers of the scalp S C A L P = skin = connective
Tracing the Cranial Nerves Osteologically
 CN I II III IV V 1 Supra-orbital ethmoidal nn. Ext. nasal V 2 Tracing the Cranial Nerves Osteologically Nucleus of Origin Olfactory tracts of frontal lobe of cerebrum Optic tracts from optic chiasma and
CN I II III IV V 1 Supra-orbital ethmoidal nn. Ext. nasal V 2 Tracing the Cranial Nerves Osteologically Nucleus of Origin Olfactory tracts of frontal lobe of cerebrum Optic tracts from optic chiasma and
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli.
 Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
Anatomy: head and Neck (6 questions) 1. Prevertebral Flexor Musculature (lying in front of the vertebrae) include all, EXCEPT: Longus Colli. Rectus Capitis Anterior. Rectus Capitis Lateralis. Rectus Capitis
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper. Oral vestibule : is slit like space between.
 Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
Oral cavity Oral cavity : consist of two parts: the oral vestibule and the oral cavity proper Oral vestibule : is slit like space between the teeth, buccal gingiva, lips, and cheeks 1 Oral cavity Oral
NERVOUS SYSTEM ANATOMY
 INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
INTRODUCTION to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science
Maxillary LA: Techniques. Ra ed Salma BDS, MSc, JBOMFS, MFDRCSI
 Maxillary LA: Techniques Ra ed Salma BDS, MSc, JBOMFS, MFDRCSI dr.raedsalma@riyadh.edu.sa https://sites.google.com/a/riyadh.edu.sa/raed/ LA Options for the Maxilla Infiltration Submucosal Supraperiosteal
Maxillary LA: Techniques Ra ed Salma BDS, MSc, JBOMFS, MFDRCSI dr.raedsalma@riyadh.edu.sa https://sites.google.com/a/riyadh.edu.sa/raed/ LA Options for the Maxilla Infiltration Submucosal Supraperiosteal
Functional components
 Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
C h a p t e r PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas
 C h a p t e r 15 The Nervous System: The Brain and Cranial Nerves PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing
C h a p t e r 15 The Nervous System: The Brain and Cranial Nerves PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing
Major Anatomic Components of the Orbit
 Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Techniques of local anesthesia in the mandible
 Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Techniques of local anesthesia in the mandible The technique of choice for anesthesia of the mandible is the block injection and this is attributed to the absence of the advantages which are present in
Alexander C Vlantis. Selective Neck Dissection 33
 05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
05 Modified Radical Neck Dissection Type II Alexander C Vlantis Selective Neck Dissection 33 Modified Radical Neck Dissection Type II INCISION Various incisions can be used for a neck dissection. The incision
Bones Ethmoid bone Inferior nasal concha Lacrimal bone Maxilla Nasal bone Palatine bone Vomer Zygomatic bone Mandible
 splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
splanchnocranium - Consists of part of skull that is derived from branchial arches - The facial bones are the bones of the anterior and lower human skull Bones Ethmoid bone Inferior nasal concha Lacrimal
Biology 323 Human Anatomy for Biology Majors Week 10; Lecture 1; Tuesday Dr. Stuart S. Sumida. Cranial Nerves and Soft Tissues of the Skull
 Biology 323 Human Anatomy for Biology Majors Week 10; Lecture 1; Tuesday Dr. Stuart S. Sumida Cranial Nerves and Soft Tissues of the Skull FOREBRAIN MIDBRAIN HINDBRAIN Forebrain: Cerebrum Perception,
Biology 323 Human Anatomy for Biology Majors Week 10; Lecture 1; Tuesday Dr. Stuart S. Sumida Cranial Nerves and Soft Tissues of the Skull FOREBRAIN MIDBRAIN HINDBRAIN Forebrain: Cerebrum Perception,
Anatomy and Physiology II. Review Spine and Neck
 Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Anatomy and Physiology II Review Spine and Neck Spine regions How many cervical vertibrae are there? 7 The curvature is the cervical region posterior? Concave posterior How many thoracic? And curvature?
Organisation of the nervous system
 Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
Chapter1 Organisation of the nervous system 1. Subdivisions of the nervous system The nervous system is divided: i) Structurally The central nervous system (CNS) composed of the brain and spinal cord.
ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION COW BONE DISSECTION
 ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION Objectives: 1) How to get ready: Read Chapter 7, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. Learning the meanings
ACTIVITY 3: AXIAL SKELETON AND LONG BONE DISSECTION Objectives: 1) How to get ready: Read Chapter 7, McKinley et al., Human Anatomy, 4e. All text references are for this textbook. Learning the meanings
Subdivided into Vestibule & Oral cavity proper
 Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
Extends from the lips to the oropharyngeal isthmus The oropharyngeal isthmus: Is the junction of mouth and pharynx. Is bounded: Above by the soft palate and the palatoglossal folds Below by the dorsum
NERVOUS SYSTEM ANATOMY
 NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
NTRODUCTON to NERVOUS SYSTEM ANATOMY M1 - Gross and Developmental Anatomy Dr. Milton M. Sholley Professor of Anatomy and Neurobiology and Dr. Michael H. Peters Professor of Chemical and Life Science Engineering
Nose & Mouth OUTLINE. Nose. - Nasal Cavity & Its Walls. - Paranasal Sinuses. - Neurovascular Structures. Mouth. - Oral Cavity & Its Contents
 Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com Nose & Mouth OUTLINE Nose - Nasal Cavity & Its Walls - Paranasal Sinuses - Neurovascular Structures Mouth - Oral Cavity & Its
Dept. of Human Anatomy, Si Chuan University Zhou hongying eaglezhyxzy@163.com Nose & Mouth OUTLINE Nose - Nasal Cavity & Its Walls - Paranasal Sinuses - Neurovascular Structures Mouth - Oral Cavity & Its
*in general the blood supply of the nose comes from branches of the internal and external carotid arteries.
 In the previous lecture we talked about the anatomy of the nasal cavity, today we will talk about its blood supply, venous drainage, innervations, and finally about the paranasal sinuses. When we describe
In the previous lecture we talked about the anatomy of the nasal cavity, today we will talk about its blood supply, venous drainage, innervations, and finally about the paranasal sinuses. When we describe
Lab 16: PNS: Nerves and Autonomic NS Hamilton Answers to Pre- Lab Assignments
 Lab 16: PNS: Nerves and Autonomic NS Hamilton Answers to Pre- Lab Assignments Pre-Lab Activity 1: 1. a. olfactory nerve b. optic nerve c. oculomotor nerve d. abducens nerve e. trochlear nerve f. trigeminal
Lab 16: PNS: Nerves and Autonomic NS Hamilton Answers to Pre- Lab Assignments Pre-Lab Activity 1: 1. a. olfactory nerve b. optic nerve c. oculomotor nerve d. abducens nerve e. trochlear nerve f. trigeminal
REVIEW/PREVIEW OF HEAD AND NECK ANATOMY FOR ENT EXAM
 REVIEW/PREVIEW OF HEAD AND NECK ANATOMY FOR ENT EXAM - 2017 PALPATE CAROTID ARTERY: AT LEVEL OF CAROTID BIFURCATION VERTEBRAL LEVEL C4 Sternocleidomastoid Muscle INTERNAL CAROTID EXTERNAL CAROTID COMMON
REVIEW/PREVIEW OF HEAD AND NECK ANATOMY FOR ENT EXAM - 2017 PALPATE CAROTID ARTERY: AT LEVEL OF CAROTID BIFURCATION VERTEBRAL LEVEL C4 Sternocleidomastoid Muscle INTERNAL CAROTID EXTERNAL CAROTID COMMON
INDEX. Cancerpain alcohol neurolysis for, 5, 20, 53-54
 INDEX Alcohol advantages of, 54 celiac plexus block with, 19-20, 165 chemical hypophysectomy with, 20 complications and side effects of, 18, 19, 45-46, 54-55 contraindications for, 54 doses with, 52 drug
INDEX Alcohol advantages of, 54 celiac plexus block with, 19-20, 165 chemical hypophysectomy with, 20 complications and side effects of, 18, 19, 45-46, 54-55 contraindications for, 54 doses with, 52 drug
Surgery Under Regional Anesthesia
 Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Surgery Under Regional Anesthesia Jean Daniel Eloy, MD Assistant Professor Residency Program Director Rutgers-New Jersey Medical School Rutgers The State University of New Jersey Peripheral Nerve Block
Anatomy images for MSS practical exam- 2019
 Anatomy images for MSS practical exam- 2019 Ilium Ischium Pubis Acetabulaum Iliac crest Iliac tubercle ASIS (muscle and ligament attached) AIIS (muscle attached) PSIS PIIS Ischial spine Ischial tuberosity
Anatomy images for MSS practical exam- 2019 Ilium Ischium Pubis Acetabulaum Iliac crest Iliac tubercle ASIS (muscle and ligament attached) AIIS (muscle attached) PSIS PIIS Ischial spine Ischial tuberosity
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR.
 The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
Tympanic Bulla Temporal Bone. Digastric Muscle. Masseter Muscle
 Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
Superior view Hyoid Bone The hyoid bone does not articulate with any other bones. It is held in place by ligaments to the styloid process of the temporal bone and the thyroid cartilage of the larynx. It
