14, 2007 RESIDENT PHYSICIAN:
|
|
|
- Alisha Butler
- 5 years ago
- Views:
Transcription
1 TITLE: Bell s Palsy SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: February 14, 2007 RESIDENT PHYSICIAN: Ki-Hong Kevin Ho, MD FACULTY PHYSICIAN: Shawn D. Newlands, MD, PhD, MBA SERIES EDITORS: Francis B. Quinn, Jr., MD and Matthew W. Ryan, MD "This material was prepared by resident physicians in partial fulfillment of educational requirements established for the Postgraduate Training Program of the UTMB Department of Otolaryngology/Head and Neck Surgery and was not intended for clinical use in its present form. It was prepared for the purpose of stimulating group discussion in a conference setting. No warranties, either express or implied, are made with respect to its accuracy, completeness, or timeliness. The material does not necessarily reflect the current or past opinions of members of the UTMB faculty and should not be used for purposes of diagnosis or treatment without consulting appropriate literature sources and informed professional opinion." Bell s palsy is the most common diagnosis given to patients with acute facial palsy. Despite substantial effort to study its disease process, the management of Bell s palsy remains controversial. This manuscript serves not as a treatment protocol for Bell s palsy, but a review of literature on the subject. Bell s palsy was named after Sir Charles Bell ( ). His most notable contribution is arguably his description of the facial nerve as the respiratory nerve of the face that controls our facial expression. The motor nucleus of the facial nerve lies deep within the reticular formation of the pons where it receives input from the precentral gyrus of the motor cortex, which innervates the ipsilateral and contralateral forehead. The cerebral cortical tracts also innervate the contralateral portion of the remaining face. This accounts for the sparing of the forehead motion in supranuclear lesions of the facial nerve. The parasympathetic secretory fibers of the nervous intermedius arise from the superior salivatory nucleus. These preganglionic fibers travel to the submandibular ganglion via the chorda tympani nerve to innervate the submandibular and sublingual glands, and to the sphenopalatine ganglion via the greater superficial petrosal nerve to innervate the lacrimal, nasal, and palatine glands. The secretory fibers of the lesser superficial petrosal nerve traverse the tympanic plexus, synapse in the otic ganglion, and travel via the auriculotemporal nerve to innervate the parotid gland. Taste fibers from the anterior 2/3 of the tongue reach the geniculate ganglion via the chorda tympani nerve and from there travel to the nucleus of the tractus solitarius. The facial nerve and nervus intermedius exit the brain stem at the pontomedullary junction and travel laterally mm with cranial nerve VIII to enter the internal acoustic meatus. The meatal segment of the nerve then travels 8-10 mm within the internal auditory canal (anterosuperior quadrant) to the meatal foramen where the canal narrows from 1.2 mm in diameter to 0.68 mm in diameter (the narrowest part of the canal). The labyrinthine segment then runs 2-4 mm to the geniculate ganglion. Here the greater superficial petrosal nerve exits to carry parasympathetic secretomotor fibers to the lacrimal gland. Just distal to this branch, the lesser superficial petrosal nerve exits to supply parasympathetic secretomotor fibers to the parotid. The
2 tympanic segment begins just distal to the geniculate ganglion where the nerve turns 40 to 80 degrees (first genu) and runs posteroinferiorly 11 mm across the tympanic cavity to the second genu. A branch leaves the segment near the pyramidal eminence to supply the stapedius muscle. The nerve then turns about 90 degrees at the second genu inferiorly where the mastoid segment travels for mm inferiorly in the anterior mastoid to exit the stylomastoid foramen. The terminal branch of the nervus intermedius, the chorda tympani, leaves the mastoid segment 5 mm proximal to the foramen and travels lateral to the incus, medial to the malleus to exit at the petrotympanic fissure. The extratympanic segment is composed entirely of motor fibers and enters the parotid gland after giving off the posterior auricular branch and a branch to the posterior belly of the digastric muscle. The pes anserus forms 20 mm from the stylomastoid foramen and further divides the nerve into the upper (temporal, and zygomatic) and lower (buccal, mandibular, and cervical) branches. Although Bell s palsy is a diagnosis of exclusion, it is the most common diagnosis given for acute facial palsy (> 60%). It causes peripheral facial neuropathy that tends to be unilateral and has a rapid onset. Its incidence is about 30 per 100,000. There is an equal male to female ration and a 3.3 times greater incidence in pregnant females. The left and right sides of the face are equally involved, and less than 1% of cases are bilateral. The recurrence rate is about 10% and can be ipsilateral or bilateral. Patients with diabetes have 4-5 times more risk of developing the disease. A family history is positive in about 10% of patients with Bell's palsy. In 1982, Peitersen et al. published an article on the natural history of Bell s palsy based on more than a thousand Danish patients. This study is unique in that it evaluates the spontaneous course of the disease without medical or surgical intervention. He found that Bell s palsy occurred in every decade of life, with a mean age of between 40 and 44 years. It was less common before the age of 15 and after the age of 60 years. Total unilateral facial paralysis occurred in 71%. Common symptoms included reduced stapedial reflex, postauricular pain, dysgeusia, reduced lacrimation, and phonophobia. The prognosis for Bell's palsy is generally good with 85 % of patients recovering completely within one month. The remaining 15% progress to complete degeneration and will not usually show signs of recovery for three to six months. The longer the time needed for recovery, the greater the probability of sequelae. Patients with incomplete paralysis will recover with no sequelae 95% of the time. Based on this study, poor outcome of Bell s palsy is associated with advanced age, late return of muscular function or beginning of remission, complete palsy, abnormal taste, stapedial reflex, and lacrimation. Although Bell s palsy has been described as idiopathic facial paralysis, there are increasing evidence suggesting a viral etiology. A study by Murakami et al. strongly suggests that herpes simplex virus type 1 (HSV-1) is active in idiopathic facial paralysis. DNA fragments of HSV-1 were exclusively found in the perineural fluid of Bell s palsy patients who underwent surgical decompression. An Iowa group has also identified HSV-1 DNA in a temporal bone section of a patient dying 6 days after developing Bell's palsy. These two independent pieces of evidence strongly support the concept that the facial paralysis associated with Bell's palsy is the result of a viral inflammatory response that induces edema within the facial nerve. The first step in evaluating any patient who presents with facial nerve paralysis involves taking a careful and thorough history. It is important to determine the onset of the paralysis (sudden vs delayed), the duration, and the rate of progression. It is especially important to
3 determine whether the paralysis is complete verses incomplete. Patients should be questioned regarding previous episodes, family history, associated symptoms (hearing loss, otorrhea, otalgia, vertigo, headaches, blurred vision, parasthesias), associated medical illnesses (diabetes, pregnancy, autoimmune disorders, cancer), history of trauma (recent or remote), and previous surgery (otologic, rhytidectomy, parotidectomy). A complete head and neck examination must be performed, including microscopic examination of the ears, careful palpation of the parotid glands and neck, ophthalmologic examination (r/o papilledema), auscultation of the neck ( r/o carotid bruits), and a thorough neurological examination. It is important to assess the degree of voluntary movement present in order to document the grade of facial paralysis as described in the House classification system: Grade Degree Description I Normal Normal facial movements; No synkinesis II Slight Mild deformity, mild synkinesis, good forehead function, slight asymmetry III Moderate Obvious facial weakness, forehead motion present, good eye closure, asymmetry, Bell's phenomenon present IV Moderately Obvious weakness, increasing synkinesis; no forehead motion V Severe Very obvious facial paralysis, some tone present, cannot close eye VI Total Complete facial paralysis, absent tone Any patient presenting with facial paralysis should undergo formal audiological testing, including pure tone, air and bone conduction, speech discrimination, reflexes, and tympanometry. If asymmetry is found on the audiogram, an ABR and/or MRI should be obtained. The most likely site of lesion in Bell's palsy is the meatal foramen (junction of the internal auditory canal portion of the nerve and the labyrinthine segment of the nerve), which is considered to be the narrowest portion of the fallopian canal. MRI with gadolinium will usually show enhancement of the labyrinthine portion of the nerve. As the edema within the nerve increases, axonal flow and circulation are inhibited resulting in varying degrees of nerve injury (first, second, and third degree). Patients who are most severely affected develop a high level of third degree injury that can result in the loss of endoneural tubules and misdirected axonal regeneration. Histological studies from patients with Bell's palsy who died of nonrelated causes reveal diffuse demyelination of the facial nerve with lymphocytic infiltrates. The principle behind topognostic testing is that lesions distal to the site of a particular branch of the facial nerve will spare the function of that branch. Moving distally from the brainstem, these tests include: the schirmer test for lacrimation (GSPN), the stapedial reflex test (stapedial branch), taste testing (chorda tympani nerve), salivary flow rates and ph (chorda tympani). Although these tests are of historical interest, they have not been found to be of much use clinically for determining the site of the lesion in facial paralysis or for predicting the outcome. Marked discrepancies are often seen. For example, patients may exhibit a marked decrease in lacrimation with a normal stapedial reflex and intact taste, or they may have absent lacrimation and an absent stapedial reflex with normal salivation. These discrepancies are easily explained in
4 Bell's palsy, where there can be multiple sites of inflammation and demyelinization from the brainstem to the peripheral branches of the nerve. Electrical tests are useful for patients with complete paralysis for determining prognosis for return of facial function and the endpoint of degeneration by serial testing. They are most useful when considering decompression surgery and are of no value in patients with incomplete paralysis. The nerve excitability test (NET), maximal stimulation test (MST), and electroneuronography (ENoG) are most useful in the degenerative phase. These tests will give normal results during the first 72 hours after injury due to the stimulating and recording electrodes both being distal to the site of the injury. After 3-4 days, the nerve degeneration reaches the site of stimulation and useful results will be obtained. These tests can only be used for unilateral paralysis because all three involve comparison to the contralateral side that must be normal for valid results. ENoG and electromyography (EMG) are employed more often than NET and MST as the latter two modalities rely on subjective evaluation of muscular response, whereas the former two quantitatively measure compound muscle action potential. For ENoG, the facial nerve is stimulated with an impulse transcutaneously at the stylomastoid foramen using bipolar electrodes. The muscular response is then recorded using bipolar electrodes placed near the nasolabial groove. The amplitude of the evoked compound action potential is considered proportional to the number of intact axons. The two sides are then compared with the response on the paralyzed side of the face expressed as a percentage of the response on the normal side of the face. A reduction in amplitude on the involved side to 10% or less of the normal side indicates a poor prognosis for spontaneous recovery. Fisch et al. notes that a maximal reduction of less than 90% within 3 weeks of onset gives an expected spontaneous rate of recovery of %. Disadvantages of ENoG include discomfort, cost, and test-retest variability owing to positioning of the electrodes and excitation of the muscles of mastication (V). EMG is of limited value early in the evaluation of facial paralysis because fibrillation potentials indicating axonal degeneration do not appear until 10 to 14 days post onset. However, EMG becomes important for assessing reinnervation potential of the muscle two weeks after onset. By using needle electrodes placed transcutaneously into the muscles of facial expression, muscle action potentials generated by voluntary activity can be recorded. Electrical silence can indicate normal muscle in a resting state, severe muscle wasting and fibrosis or acute facial paralysis in the early stages. During normal voluntary contraction organized diphasic or triphasic potentials are seen. Fibrillation potentials indicate degeneration of the neural supply to the muscle in question. Polyphasic potentials indicate reinnervation. These are important because they usually appear 6-12 weeks before clinical return of function. It is generally obtained if ENoG displays more than 95% degeneration. Sunderland's classification describes five degrees of nerve injury. The first degree (neuropraxia) involves a localized conduction block in the nerve with the nerve fibers responding
5 to electrical stimuli proximal and distal to the lesion, but not across the injured segment. Axonal continuity is preserved, wallerian degeneration does not occur, and recovery is usually complete. The second degree of nerve injury is called axonotmesis. This refers to disruption of the axon into proximal and distal portions with interrupted axoplasmic flow and Wallerian degeneration. The third, fourth, and fifth degree of nerve injury are grouped together as neurotmesis, and subdivided depending on the integrity of perineurium and epineurium. Wallerian degeneration occurs at the faster rate than axonotmesis and prognosis is the poorest. The rate of nerve degeneration in Bell s palsy falls in between axonotmesis and neurotmesis. However, there is no electrical test to-date that can quantitatively differentiate the two subclasses of injury. Treatment options of Bell s palsy range from observation, medical treatment, surgical decompression, to facial rehabilitation. The efficacies of oral prednisone and anti-viral agents have been studied extensively, yet there is no consensus among experts on ideal regimen and dosage. Cochrane review summarizes four trials (179 patients) that compare steroid to placebo, saline, and vitamin solutions. Its results show no significant benefit of giving steroid to Bell s palsy patients. A similar conclusion is reached by Turk Boru s randomized controlled trial (56 patients). Ramsey, however, points out in his meta-analysis that the rate of complete recovery (Grade VI I) is 17% higher in the steroid group, provided the total prednisone dose is at least 400 mg and that the treatment is initiated within a week of onset of paralysis (3 trials, 230 patients). The addition of anti-viral agent such as acyclovir is advocated by Adour, whose double-blind randomized controlled trial shows that the combined therapy of prednisone and acyclovir results in better return of muscle function and prevention of partial nerve degeneration. This result is challenged by another prospective trial by Kawaguchi who illustrates that valacyclovir plus prednisone have no advantage over prednisone alone. Regardless of medical regimen, early administration within 3 days of onset appear to have superior effect on outcome, as demonstrated in a study by Hato et al. Eye care is of utmost importance in facial nerve paralysis due to the risk of exposure keratitis. Artificial tears and lacrilube ointment should be prescribed. Taping of the eye lids during sleep may be helpful as well as the use of a moisture chamber. Patients should avoid contact lens, fans and dust, and should have eye protection when outside in the wind. Gold weight implant to the upper eyelid should be considered in patients with long-standing facial paralysis. Surgical decompression for Bell s palsy has evolved in many ways throughout the years. The emphasis has shifted from focusing on the stylomastoid foramen in the 1930s to decompressing the meatal foramen nowadays, the narrowest portion of the facial canal. Proponents of surgical decompression such as Gantz believe in early decompression within 2 weeks of onset of paralysis if ENoG demonstrates more than 90% degeneration and EMG shows no voluntary muscle potential. Those who are against decompression argue that the Bell s palsy is a result of viral demyelination and that increased intracanal pressure may not be the primary cause of Bell s palsy. Although the issue of surgical decompression remains highly controversial, factors such as age, medical comorbidities, endpoint and rate of progression of ENoG, days from onset of paralysis, and when muscle function begins to return likely influence the outcome and allow us to predict the success of surgery.
6 References: Peitersen E. Acta Otolaryngol 2002;549:4 30. Murakami: Ann Intern Med, Volume 124(1).January 1, Burgess RC et al. Ann Otol Rhinol Laryngol 1994;103(10): Gantz: Laryngoscope, Volume 109(8).August Kinoshita T et al. Clin. Radiology 2001; 56: Fisch U. Am J. Otology Turk-Boru U et al. Kulak Burun Bogaz Ihtis Derg. 2005;14(3-4):62-6. Ramsey MJ et al. Laryngoscope 2000; 110: Adour KK 1996 Ann Otol Rhinol Laryngol May;105(5):371-8 Kawaguchi: Laryngoscope, Volume 117(1).January Hato N. Otol & Neurotol: 24(6) 2003 Pensak ML. Assessment and Management of the Paralyzed face. Otol. & Neurotol. Update. Nov 2006 Adour KK Jan;259(1):40-7 Glasscock M, Shambaugh G: Facial nerve surgery. In Surgery of the ear, 1990:
Functional components
 Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Facial Nerve VII cranial nerve Emerges from Pons Two roots Functional components: 1. GSA (general somatic afferent) 2. SA (Somatic afferent) 3. GVE (general visceral efferent) 4. BE (Special visceral/branchial
Cranial Nerve VII - Facial Nerve. The facial nerve has 3 main components with distinct functions
 Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
Cranial Nerve VII - Facial Nerve The facial nerve has 3 main components with distinct functions Somatic motor efferent Supplies the muscles of facial expression; posterior belly of digastric muscle; stylohyoid,
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi
 By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
By : Prof Saeed Abuel Makarem & Dr.Sanaa Alshaarawi OBJECTIVES By the end of the lecture, students shouldbe able to: List the nuclei of the deep origin of the trigeminal and facial nerves in the brain
ASSESSMENT AND TREATMENT OF FACIAL PALSY. Michael J. LaRouere, M.D. Michigan Ear Institute Farmington Hills, Michigan
 ASSESSMENT AND TREATMENT OF FACIAL PALSY Michael J. LaRouere, M.D. Michigan Ear Institute Farmington Hills, Michigan FACIAL PARALYSIS - ETIOLOGY Bells Palsy Ramsay Hunt Syndrome Infection (Acute/Chronic)
ASSESSMENT AND TREATMENT OF FACIAL PALSY Michael J. LaRouere, M.D. Michigan Ear Institute Farmington Hills, Michigan FACIAL PARALYSIS - ETIOLOGY Bells Palsy Ramsay Hunt Syndrome Infection (Acute/Chronic)
4/30/2009 FN PARALYSIS HEMIFACIAL SPASM
 FN PARALYSIS HEMIFACIAL SPASM 1 Hemifacial spasm (Involuntary twitches) Etiology: Vascular loop compressing the FN at the root exit zone in the CPA = Neuro-vascular conflict Diagnosis: CT & MRI, Electrophysiology
FN PARALYSIS HEMIFACIAL SPASM 1 Hemifacial spasm (Involuntary twitches) Etiology: Vascular loop compressing the FN at the root exit zone in the CPA = Neuro-vascular conflict Diagnosis: CT & MRI, Electrophysiology
CHAPTER 13. FACIAL NERVE PARALYSIS
 CHAPTER 13. FACIAL NERVE PARALYSIS Introduction Facial nerve paralysis, whilst not a disease of the ear itself, commonly arises within the ear due to its anatomical course, and often as a result of ear
CHAPTER 13. FACIAL NERVE PARALYSIS Introduction Facial nerve paralysis, whilst not a disease of the ear itself, commonly arises within the ear due to its anatomical course, and often as a result of ear
Laith Sorour. Facial nerve (vii):
 Laith Sorour Cranial nerves 7 & 8 Hello, there are edited slides please go back to them to see pictures, they are not that much important in this lecture but still, and yes slides are included :p Let s
Laith Sorour Cranial nerves 7 & 8 Hello, there are edited slides please go back to them to see pictures, they are not that much important in this lecture but still, and yes slides are included :p Let s
Cranial Nerve VII & VIII
 Cranial Nerve VII & VIII Lecture Objectives Follow up the course of facial nerve from its point of central connections, exit and down to its target areas. Follow up the central connections of the facial
Cranial Nerve VII & VIII Lecture Objectives Follow up the course of facial nerve from its point of central connections, exit and down to its target areas. Follow up the central connections of the facial
Parotid Gland, Temporomandibular Joint and Infratemporal Fossa
 M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
M1 - Anatomy Parotid Gland, Temporomandibular Joint and Infratemporal Fossa Jeff Dupree Sanger 9-057 jldupree@vcu.edu Parotid gland: wraps around the mandible positioned between the mandible and the sphenoid
Evaluation and Management of Bell's Palsy January 2002
 TITLE: Evaluation and Management of Bell s Palsy SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 29, 2002 RESIDENT PHYSICIAN: Russell D. Briggs, MD FACULTY PHYSICIAN: Byron
TITLE: Evaluation and Management of Bell s Palsy SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 29, 2002 RESIDENT PHYSICIAN: Russell D. Briggs, MD FACULTY PHYSICIAN: Byron
Dr.Ban I.S. head & neck anatomy 2 nd y. جامعة تكريت كلية طب االسنان املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
جامعة تكريت كلية طب االسنان التشريح مادة املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Parotid region The part of the face in front of the ear and below the zygomatic arch is the parotid region. The
The Seventh Cranial Nerve The Facial By Prof. Dr. Muhammad Imran Qureshi
 The Seventh Cranial Nerve The Facial By Prof. Dr. Muhammad Imran Qureshi Functional Components: SVE: Fibers originate from nucleus of facial nerve, and supply facial muscles GVE: Fibers derived from superior
The Seventh Cranial Nerve The Facial By Prof. Dr. Muhammad Imran Qureshi Functional Components: SVE: Fibers originate from nucleus of facial nerve, and supply facial muscles GVE: Fibers derived from superior
Lec [8]: Mandibular nerve:
![Lec [8]: Mandibular nerve: Lec [8]: Mandibular nerve:](/thumbs/94/121295776.jpg) Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
Lec [8]: Mandibular nerve: The mandibular branch from the trigeminal ganglion lies in the middle cranial fossa lateral to the cavernous sinus. With the motor root of the trigeminal nerve [motor roots lies
POST TRAUMATIC FACIAL PARALYSIS - A REVIEW
 POST TRAUMATIC FACIAL PARALYSIS - A REVIEW Pages with reference to book, From 105 To 107 Naresh K. Panda, Y. N. Mehra, S.B.S. Mann, Satish K. Mehta ( Deptt. of Otolaryngology, Postgraduate Institute of
POST TRAUMATIC FACIAL PARALYSIS - A REVIEW Pages with reference to book, From 105 To 107 Naresh K. Panda, Y. N. Mehra, S.B.S. Mann, Satish K. Mehta ( Deptt. of Otolaryngology, Postgraduate Institute of
Imaging of facial paralysis
 Imaging of facial paralysis Poster No.: C-2151 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Martinez Molina, L. Aleman Romero, L. A. Sanchez Alonso, A. Puerta Sales, V. Garcia Medina; Murcia/ES
Imaging of facial paralysis Poster No.: C-2151 Congress: ECR 2013 Type: Educational Exhibit Authors: N. Martinez Molina, L. Aleman Romero, L. A. Sanchez Alonso, A. Puerta Sales, V. Garcia Medina; Murcia/ES
PTERYGOPALATINE FOSSA
 PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
PTERYGOPALATINE FOSSA Outline Anatomical Structure and Boundaries Foramina and Communications with other spaces and cavities Contents Pterygopalatine Ganglion Especial emphasis on certain arteries and
Temporal region. temporal & infratemporal fossae. Zhou Hong Ying Dept. of Anatomy
 Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Temporal region temporal & infratemporal fossae Zhou Hong Ying Dept. of Anatomy Temporal region is divided by zygomatic arch into temporal & infratemporal fossae. Temporal Fossa Infratemporal fossa Temporal
Unit VIII Problem 9 Anatomy of The Ear
 Unit VIII Problem 9 Anatomy of The Ear - The ear is an organ with 2 functions: Hearing. Maintenance of equilibrium/balance. - The ear is divided into 3 parts: External ear. Middle ear (which is also known
Unit VIII Problem 9 Anatomy of The Ear - The ear is an organ with 2 functions: Hearing. Maintenance of equilibrium/balance. - The ear is divided into 3 parts: External ear. Middle ear (which is also known
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR.
 The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
The Ear The ear consists of : 1-THE EXTERNAL EAR 2-THE MIDDLE EAR, OR TYMPANIC CAVITY 3-THE INTERNAL EAR, OR LABYRINTH 1-THE EXTERNAL EAR Made of A-AURICLE B-EXTERNAL AUDITORY MEATUS A-AURICLE It consists
Cranial nerves.
 Cranial nerves eaglezhyxzy@163.com Key Points of Learning Name Components Passing through Peripheral distribution Central connection Function Cranial nerves Ⅰ olfactory Ⅱ optic Ⅲ occulomotor Ⅳ trochlear
Cranial nerves eaglezhyxzy@163.com Key Points of Learning Name Components Passing through Peripheral distribution Central connection Function Cranial nerves Ⅰ olfactory Ⅱ optic Ⅲ occulomotor Ⅳ trochlear
K. J. Lee: Essential Otolaryngology and Head and Neck Surgery (IIIrd Ed) Chapter 10: Facial Nerve Paralysis. Evaluation
 K. J. Lee: Essential Otolaryngology and Head and Neck Surgery (IIIrd Ed) Chapter 10: Facial Nerve Paralysis Evaluation Evaluation of patients with facial nerve paralysis must be a careful process including
K. J. Lee: Essential Otolaryngology and Head and Neck Surgery (IIIrd Ed) Chapter 10: Facial Nerve Paralysis Evaluation Evaluation of patients with facial nerve paralysis must be a careful process including
Facial Paralysis: Objectives: Discuss the anatomy of the facial nerve. Look at common patterns of facial nerve palsy
 Facial Paralysis: Objectives: Discuss the anatomy of the facial nerve Look at common patterns of facial nerve palsy Discuss imaging appearance of lesions that lead to facial paralysis. Lindell R. Gentry,
Facial Paralysis: Objectives: Discuss the anatomy of the facial nerve Look at common patterns of facial nerve palsy Discuss imaging appearance of lesions that lead to facial paralysis. Lindell R. Gentry,
For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER
 GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
GROSS ANATOMY EXAMINATION May 15, 2000 For the following questions, indicate the letter that corresponds to the SINGLE MOST APPROPRIATE ANSWER 1. Pain associated with an infection limited to the middle
Dr. Sami Zaqout Faculty of Medicine IUG
 Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
Auricle External Ear External auditory meatus The Ear Middle Ear (Tympanic Cavity) Auditory ossicles Internal Ear (Labyrinth) Bony labyrinth Membranous labyrinth External Ear Auricle External auditory
Parotid Gland. Parotid Gland. Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible. Medial pterygoid.
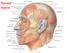 Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Parotid region Parotid Gland Largest of 3 paired salivary glands (submandibular; sublingual) Ramus of Mandible Medial pterygoid Cross section of mandible Masseter D S SCM Parotid Gland Mastoid Process
Major Anatomic Components of the Orbit
 Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Major Anatomic Components of the Orbit 1. Osseous Framework 2. Globe 3. Optic nerve and sheath 4. Extraocular muscles Bony Orbit Seven Bones Frontal bone Zygomatic bone Maxillary bone Ethmoid bone Sphenoid
Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus
 Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Outline of content Temporal fossa Infratemporal fossa Pterygopalatine fossa Terminal branches of external carotid artery Pterygoid venous plexus Boundary Content Communication Mandibular division of trigeminal
Omran Saeed. Luma Taweel. Mohammad Almohtaseb. 1 P a g e
 2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
2 Omran Saeed Luma Taweel Mohammad Almohtaseb 1 P a g e I didn t include all the photos in this sheet in order to keep it as small as possible so if you need more clarification please refer to slides In
Mohammad Hisham Al-Mohtaseb. Lina Mansour. Reyad Jabiri. 0 P a g e
 2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
2 Mohammad Hisham Al-Mohtaseb Lina Mansour Reyad Jabiri 0 P a g e This is only correction for the last year sheet according to our record. If you already studied this sheet just read the yellow notes which
Gross Anatomy of the. TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR
 Gross Anatomy of the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Professor of Anatomy and Neurobiology Assignment: Head
Gross Anatomy of the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Professor of Anatomy and Neurobiology Assignment: Head
Brain and spinal nerve. By: shirin Kashfi
 Brain and spinal nerve By: shirin Kashfi Nervous system: central nervous system (CNS) peripheral nervous system (PNS) Brain (cranial) nerves Spinal nerves Ganglions (dorsal root ganglions, sympathetic
Brain and spinal nerve By: shirin Kashfi Nervous system: central nervous system (CNS) peripheral nervous system (PNS) Brain (cranial) nerves Spinal nerves Ganglions (dorsal root ganglions, sympathetic
Bony orbit Roof The orbital plate of the frontal bone Lateral wall: the zygomatic bone and the greater wing of the sphenoid
 Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
Bony orbit Roof: Formed by: The orbital plate of the frontal bone, which separates the orbital cavity from the anterior cranial fossa and the frontal lobe of the cerebral hemisphere Lateral wall: Formed
General Sensory Pathways of the Face Area, Taste Pathways and Hearing Pathways
 General Sensory Pathways of the Face Area, Taste Pathways and Hearing Pathways Lecture Objectives Describe pathways for general sensations (pain, temperature, touch and proprioception) from the face area.
General Sensory Pathways of the Face Area, Taste Pathways and Hearing Pathways Lecture Objectives Describe pathways for general sensations (pain, temperature, touch and proprioception) from the face area.
Biology 323 Human Anatomy for Biology Majors Week 10; Lecture 1; Tuesday Dr. Stuart S. Sumida. Cranial Nerves and Soft Tissues of the Skull
 Biology 323 Human Anatomy for Biology Majors Week 10; Lecture 1; Tuesday Dr. Stuart S. Sumida Cranial Nerves and Soft Tissues of the Skull FOREBRAIN MIDBRAIN HINDBRAIN Forebrain: Cerebrum Perception,
Biology 323 Human Anatomy for Biology Majors Week 10; Lecture 1; Tuesday Dr. Stuart S. Sumida Cranial Nerves and Soft Tissues of the Skull FOREBRAIN MIDBRAIN HINDBRAIN Forebrain: Cerebrum Perception,
Brainstem and Cranial Nerves II. Nerves covered in other lectures. A reminder about embryology. Prof. Stuart Bunt
 Brainstem and Cranial Nerves II Prof. Stuart Bunt Nerves covered in other lectures 1 Olfactory 2 Optic 3,4,6 Extraocular eye muscles 8 Vestibulo-cochlear 5 Motor and Sensory to the face and muscles of
Brainstem and Cranial Nerves II Prof. Stuart Bunt Nerves covered in other lectures 1 Olfactory 2 Optic 3,4,6 Extraocular eye muscles 8 Vestibulo-cochlear 5 Motor and Sensory to the face and muscles of
Tracing the Cranial Nerves Osteologically
 CN I II III IV V 1 Supra-orbital ethmoidal nn. Ext. nasal V 2 Tracing the Cranial Nerves Osteologically Nucleus of Origin Olfactory tracts of frontal lobe of cerebrum Optic tracts from optic chiasma and
CN I II III IV V 1 Supra-orbital ethmoidal nn. Ext. nasal V 2 Tracing the Cranial Nerves Osteologically Nucleus of Origin Olfactory tracts of frontal lobe of cerebrum Optic tracts from optic chiasma and
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions. 4 May 2012
 SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
SCHOOL OF ANATOMICAL SCIENCES Mock Run Questions 4 May 2012 1. With regard to the muscles of the neck: a. the platysma muscle is supplied by the accessory nerve. b. the stylohyoid muscle is supplied by
Facial Paralysis Facial Nerve Subcommittee of the American Academy of Otolaryngology-Head & Neck Surgery
 Facial Paralysis Facial Nerve Subcommittee of the American Academy of Otolaryngology-Head & Neck Surgery Editor: Peter S Roland MD Contributors: Peter S Roland MD, Larry Lundy MD, Jacques Herzog MD, Fred
Facial Paralysis Facial Nerve Subcommittee of the American Academy of Otolaryngology-Head & Neck Surgery Editor: Peter S Roland MD Contributors: Peter S Roland MD, Larry Lundy MD, Jacques Herzog MD, Fred
Via Transmastoid Approach. Mitul Chaitan Bhatt. Maharashtra University Miraj India
 ISSN: 2250-0359 Volume 6 Issue 1 2016 Evaluation Of Patients Of Traumatic Facial Palsy Treated By Facial Nerve Decompression Via Transmastoid Approach Mitul Chaitan Bhatt Maharashtra University Miraj India
ISSN: 2250-0359 Volume 6 Issue 1 2016 Evaluation Of Patients Of Traumatic Facial Palsy Treated By Facial Nerve Decompression Via Transmastoid Approach Mitul Chaitan Bhatt Maharashtra University Miraj India
Gross Anatomy of the. TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR. Assignment: Head to Toe Temporomandibular Joint (TMJ)
 Gross Anatomy the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Pressor Anatomy and Neurobiology Assignment: Head to Toe
Gross Anatomy the TEMPORAL BONE, EXTERNAL EAR, and MIDDLE EAR M1 Gross and Developmental Anatomy 9:00 AM, December 11, 2008 Dr. Milton M. Sholley Pressor Anatomy and Neurobiology Assignment: Head to Toe
human anatomy 2016 lecture fifteen Dr meethak ali ahmed neurosurgeon
 Cranial Nerves Organization of the Cranial Nerves The cranial nerves are named as follows: I. Olfactory II. Optic III. Oculomotor IV. Trochlear V. Trigeminal VI. Abducent VII. Facial VIII. Vestibulocochlear
Cranial Nerves Organization of the Cranial Nerves The cranial nerves are named as follows: I. Olfactory II. Optic III. Oculomotor IV. Trochlear V. Trigeminal VI. Abducent VII. Facial VIII. Vestibulocochlear
Learning Outcomes. The Carotid 20/02/2013. Scalp, Face, Parotid. Layers of the Scalp. The Parotid Gland. The Scalp. The Carotid The Facial Artery
 Learning Outcomes The Scalp Layers of the Scalp Bleeding from the Scalp The Carotid The Facial Artery Major Muscles of the Face and Jaw(s) Muscles of Mastication Muscles of Facial Expression The Parotid
Learning Outcomes The Scalp Layers of the Scalp Bleeding from the Scalp The Carotid The Facial Artery Major Muscles of the Face and Jaw(s) Muscles of Mastication Muscles of Facial Expression The Parotid
The Evaluation and Management of Drooling
 The Evaluation and Management of Drooling Sarah Rodriguez, MD Faculty Advisor: Byron Bailey, MD, FACS The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January
The Evaluation and Management of Drooling Sarah Rodriguez, MD Faculty Advisor: Byron Bailey, MD, FACS The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation January
3-Deep fascia: is absent (except over the parotid gland & buccopharngeal fascia covering the buccinator muscle)
 The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
The Face 1-Skin of the Face The skin of the face is: Elastic Vascular (bleed profusely however heal rapidly) Rich in sweat and sebaceous glands (can cause acne in adults) It is connected to the underlying
Cranial Nerves. Steven McLoon Department of Neuroscience University of Minnesota
 Cranial Nerves Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Change in Lab Sequence Week of Oct 2 Lab 5 Week of Oct 9 Lab 4 2 Sensory and Motor Systems Sensory Systems:
Cranial Nerves Steven McLoon Department of Neuroscience University of Minnesota 1 Course News Change in Lab Sequence Week of Oct 2 Lab 5 Week of Oct 9 Lab 4 2 Sensory and Motor Systems Sensory Systems:
Ramsay Hunt syndrome a case report and review of literature
 From the SelectedWorks of Balasubramanian Thiagarajan January 1, 2013 Ramsay Hunt syndrome a case report and review of literature Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/27/
From the SelectedWorks of Balasubramanian Thiagarajan January 1, 2013 Ramsay Hunt syndrome a case report and review of literature Balasubramanian Thiagarajan Available at: https://works.bepress.com/drtbalu/27/
Infratemporal fossa: Tikrit University college of Dentistry Dr.Ban I.S. head & neck Anatomy 2 nd y.
 Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Infratemporal fossa: This is a space lying beneath the base of the skull between the lateral wall of the pharynx and the ramus of the mandible. It is also referred to as the parapharyngeal or lateral pharyngeal
Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :
![Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa : Tikrit University collage of dentistry Dr.Ban I.S. head & neck anatomy 2 nd y. Lec [5] / Temporal fossa :](/thumbs/88/115294566.jpg) Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Lec [5] / Temporal fossa : Borders of the Temporal Fossa: Superior: Superior temporal line. Inferior: gap between zygomatic arch and infratemporal crest of sphenoid bone. Anterior: Frontal process of the
Introduction to Head and Neck Anatomy
 Introduction to Head and Neck Anatomy Nervous Tissue Controls and integrates all body activities within limits that maintain life Three basic functions 1. sensing changes with sensory receptors 2. interpreting
Introduction to Head and Neck Anatomy Nervous Tissue Controls and integrates all body activities within limits that maintain life Three basic functions 1. sensing changes with sensory receptors 2. interpreting
A review of Bell's palsy
 University of North Dakota UND Scholarly Commons Physical Therapy Scholarly Projects Department of Physical Therapy 1996 A review of Bell's palsy Jodi Spicer University of North Dakota Follow this and
University of North Dakota UND Scholarly Commons Physical Therapy Scholarly Projects Department of Physical Therapy 1996 A review of Bell's palsy Jodi Spicer University of North Dakota Follow this and
INTRODUCTION: ANATOMY UNDERLYING CLINICAL TESTS OF CRANIAL NERVES
 INTRODUCTION: ANATOMY UNDERLYING CLINICAL TESTS OF CRANIAL NERVES CRANIAL NERVE I - OLFACTORY I - OLFACTORY NERVE - SMELL TEST: SMELL ODORS (note: not ammonia; pain in nasal cavity CN5 DAMAGE: LOSS OF
INTRODUCTION: ANATOMY UNDERLYING CLINICAL TESTS OF CRANIAL NERVES CRANIAL NERVE I - OLFACTORY I - OLFACTORY NERVE - SMELL TEST: SMELL ODORS (note: not ammonia; pain in nasal cavity CN5 DAMAGE: LOSS OF
04 Development of the Face and Neck. Development of the Face Development of the neck
 04 Development of the Face and Neck Development of the Face Development of the neck Development of the face Overview of facial development The fourth week ~ the twelfth week of prenatal development Between
04 Development of the Face and Neck Development of the Face Development of the neck Development of the face Overview of facial development The fourth week ~ the twelfth week of prenatal development Between
C h a p t e r PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas
 C h a p t e r 15 The Nervous System: The Brain and Cranial Nerves PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing
C h a p t e r 15 The Nervous System: The Brain and Cranial Nerves PowerPoint Lecture Slides prepared by Jason LaPres North Harris College Houston, Texas Copyright 2009 Pearson Education, Inc., publishing
Trigeminal Nerve (V)
 Trigeminal Nerve (V) Lecture Objectives Discuss briefly how the face is developed. Follow up the course of trigeminal nerve from its point of central connections, exit and down to its target areas. Describe
Trigeminal Nerve (V) Lecture Objectives Discuss briefly how the face is developed. Follow up the course of trigeminal nerve from its point of central connections, exit and down to its target areas. Describe
Facial nerve, more than any other cranial nerves, Intratemporal Facial Nerve Paralysis- A Three Year Study. Case Series
 Case Series Intratemporal Facial Nerve Paralysis- A Three Year Study Anirban Ghosh, 1 Sankar Prasad Bera, 2 Somnath Saha 3 ABSTRACT Introduction This study on intratemporal facial paralysis is an attempt
Case Series Intratemporal Facial Nerve Paralysis- A Three Year Study Anirban Ghosh, 1 Sankar Prasad Bera, 2 Somnath Saha 3 ABSTRACT Introduction This study on intratemporal facial paralysis is an attempt
Contents. Facial nerve re- animation techniques Conclusions. Microsurgical resection Radiosurgery
 Contents Introduction Anatomy of facial nerve Imaging Intra- op landmarks and intra- op nerve monitoring Grading of facial palsy Factors associated with preservation of facial nerve Microsurgical resection
Contents Introduction Anatomy of facial nerve Imaging Intra- op landmarks and intra- op nerve monitoring Grading of facial palsy Factors associated with preservation of facial nerve Microsurgical resection
PERIPHERAL NERVOUS SYSTEM
 CHAPTER 13 PERIPHERAL NERVOUS SYSTEM Functional division of nervous system = afferent info to the CNS ascending spinal cord = efferent info from CNS descending spinal cord somatic skin, muscles visceral
CHAPTER 13 PERIPHERAL NERVOUS SYSTEM Functional division of nervous system = afferent info to the CNS ascending spinal cord = efferent info from CNS descending spinal cord somatic skin, muscles visceral
function - sensory & postganglionic sympathetic [communication from the internal carotid plexus in the cavernous sinus] innervation of the mucosa of
![function - sensory & postganglionic sympathetic [communication from the internal carotid plexus in the cavernous sinus] innervation of the mucosa of function - sensory & postganglionic sympathetic [communication from the internal carotid plexus in the cavernous sinus] innervation of the mucosa of](/thumbs/74/71276096.jpg) Nerves I. Cranial nerves A. Olfactory (CN I) 1. Olfactory bulb 2. Olfactory tract B. Optic n. (CNII) function - carries visual sensory information from the neural retina to the diencephalon & midbrain
Nerves I. Cranial nerves A. Olfactory (CN I) 1. Olfactory bulb 2. Olfactory tract B. Optic n. (CNII) function - carries visual sensory information from the neural retina to the diencephalon & midbrain
Trigeminal Nerve Worksheets, Distributions Page 1
 Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
Trigeminal Nerve Worksheet #1 Distribution by Nerve Dr. Darren Hoffmann Dental Gross Anatomy, Spring 2013 We have drawn out each of the branches of CN V in lecture and you have an idea now for their basic
GUIDELINE FOR THE MANAGEMENT OF IDIOPATHIC FACIAL PALSY. All children under 16 presenting to UHW or CHfW with IFP. Dr P Jeffrey Morgan ST8
 GUIDELINE FOR THE MANAGEMENT OF IDIOPATHIC FACIAL PALSY Reference: IFP Version No: 1 Applicable to All children under 16 presenting to UHW or CHfW with IFP Classification of document: Area for Circulation:
GUIDELINE FOR THE MANAGEMENT OF IDIOPATHIC FACIAL PALSY Reference: IFP Version No: 1 Applicable to All children under 16 presenting to UHW or CHfW with IFP Classification of document: Area for Circulation:
Perineural Tumor Spread (PNS) Perineural Tumor Spread (PNS) PNS Anatomic Considerations. Perineural Tumor Spread-Imaging
 Imaging of Perineural Tumor Spread in Head and Neck Cancer Lawrence E. Ginsberg, MD Departments of Diagnostic Radiology and Head and Neck Surgery University of Texas M.D. Anderson Cancer Center Houston,
Imaging of Perineural Tumor Spread in Head and Neck Cancer Lawrence E. Ginsberg, MD Departments of Diagnostic Radiology and Head and Neck Surgery University of Texas M.D. Anderson Cancer Center Houston,
Unit VIII Problem 3 Neuroanatomy: Brain Stem, Cranial Nerves and Scalp
 Unit VIII Problem 3 Neuroanatomy: Brain Stem, Cranial Nerves and Scalp - Brain stem: It is connected to the cerebellum and cerebral hemispheres. Rostral end of brain stem: diencephalon is the area which
Unit VIII Problem 3 Neuroanatomy: Brain Stem, Cranial Nerves and Scalp - Brain stem: It is connected to the cerebellum and cerebral hemispheres. Rostral end of brain stem: diencephalon is the area which
Upper and Lower Motoneurons for the Head Objectives
 Upper and Lower Motoneurons for the Head Objectives Know the locations of cranial nerve motor nuclei Describe the effects of motor cranial nerve lesions Describe how the corticobulbar tract innervates
Upper and Lower Motoneurons for the Head Objectives Know the locations of cranial nerve motor nuclei Describe the effects of motor cranial nerve lesions Describe how the corticobulbar tract innervates
Motor tracts Both pyramidal tracts and extrapyramidal both starts from cortex: Area 4 Area 6 Area 312 Pyramidal: mainly from area 4 Extrapyramidal:
 Motor tracts Both pyramidal tracts and extrapyramidal both starts from cortex: Area 4 Area 6 Area 312 Pyramidal: mainly from area 4 Extrapyramidal: mainly from area 6 area 6 Premotorarea: uses external
Motor tracts Both pyramidal tracts and extrapyramidal both starts from cortex: Area 4 Area 6 Area 312 Pyramidal: mainly from area 4 Extrapyramidal: mainly from area 6 area 6 Premotorarea: uses external
ParasymPathetic Nervous system. Done by : Zaid Al-Ghnaneem
 ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
ParasymPathetic Nervous system Done by : Zaid Al-Ghnaneem In this lecture we are going to discuss Parasympathetic, in the last lecture we took sympathetic and one of the objectives of last lecture was
The sebaceous glands (glands of Zeis) open directly into the eyelash follicles, ciliary glands (glands of Moll) are modified sweat glands that open
 The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
The Orbital Region The orbits are a pair of bony cavities that contain the eyeballs; their associated muscles, nerves, vessels, and fat; and most of the lacrimal apparatus upper eyelid is larger and more
A Study of Etiopathology and Management of Facial Palsy at a Tertiary Care Institute
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 7 Ver.VII (July 2016), PP 71-75 www.iosrjournals.org A Study of Etiopathology and Management
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 7 Ver.VII (July 2016), PP 71-75 www.iosrjournals.org A Study of Etiopathology and Management
Trigeminal Nerve Anatomy. Dr. Mohamed Rahil Ali
 Trigeminal Nerve Anatomy Dr. Mohamed Rahil Ali Trigeminal nerve Largest cranial nerve Mixed nerve Small motor root and large sensory root Motor root Nucleus of motor root present in the pons and medulla
Trigeminal Nerve Anatomy Dr. Mohamed Rahil Ali Trigeminal nerve Largest cranial nerve Mixed nerve Small motor root and large sensory root Motor root Nucleus of motor root present in the pons and medulla
Anatomy of the ear: Lymphatics
 Anatomy of the ear: 1. External ear which consist of auricle and external auditory canal. The auricle has a framework of cartilage except the lobule, the skin is closely adherent to perichonderium at the
Anatomy of the ear: 1. External ear which consist of auricle and external auditory canal. The auricle has a framework of cartilage except the lobule, the skin is closely adherent to perichonderium at the
Face and Scalp 解剖學科鄭授德
 Face and Scalp 解剖學科鄭授德 本教材之圖片取自於 1 Gray s Anatomy for Students, 3rd ed, 2015, by Drake, Vogl, and Mitchell 2 Clinically Oriented Anatomy, 7th ed, 2014, by Moore, Dalley, and Agur 3 Clinically Oriented
Face and Scalp 解剖學科鄭授德 本教材之圖片取自於 1 Gray s Anatomy for Students, 3rd ed, 2015, by Drake, Vogl, and Mitchell 2 Clinically Oriented Anatomy, 7th ed, 2014, by Moore, Dalley, and Agur 3 Clinically Oriented
Drooling January 2003
 TITLE: Drooling SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 30, 2003 RESIDENT PHYSICIAN: Sarah Rodriguez, MD FACULTY ADVISOR: Byron J. Bailey, MD SERIES EDITORS: Francis
TITLE: Drooling SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: January 30, 2003 RESIDENT PHYSICIAN: Sarah Rodriguez, MD FACULTY ADVISOR: Byron J. Bailey, MD SERIES EDITORS: Francis
MRI ANATOMY OF THE CRANIAL NERVES. Alexandra Borges Radiology Dpt. Instituto Português de Oncologia de Lisboa
 MRI ANATOMY OF THE CRANIAL NERVES Alexandra Borges Radiology Dpt. Instituto Português de Oncologia de Lisboa SENR 2014 CRANIAL NERVES Olfactory: I Optic: II Oculomotor nerves: III, IV, VI Trigeminal nerve:
MRI ANATOMY OF THE CRANIAL NERVES Alexandra Borges Radiology Dpt. Instituto Português de Oncologia de Lisboa SENR 2014 CRANIAL NERVES Olfactory: I Optic: II Oculomotor nerves: III, IV, VI Trigeminal nerve:
VII NERVE PALSY EVALUATION AND MANAGEMENT
 VII NERVE PALSY EVALUATION AND MANAGEMENT The eye cannot close and constantly weeps. The mouth dribbles, the speech is interfered with and mastication impaired. The delicate shades of continence are lost.
VII NERVE PALSY EVALUATION AND MANAGEMENT The eye cannot close and constantly weeps. The mouth dribbles, the speech is interfered with and mastication impaired. The delicate shades of continence are lost.
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi. E. mail:
 The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
The Skull and Temporomandibular joint II Prof. Abdulameer Al-Nuaimi E-mail: a.al-nuaimi@sheffield.ac.uk E. mail: abdulameerh@yahoo.com Temporal fossa The temporal fossa is a depression on the temporal
Cranial nerve Dept. of Anatomy Zhou Hong Ying
 Cranial nerve Dept. of Anatomy Zhou Hong Ying Key Points of Learning Name Components Passing through Peripheral distribution Central connection Function Cranial nerve Ⅰ olfactory Ⅱ optic Ⅲ occulomotor
Cranial nerve Dept. of Anatomy Zhou Hong Ying Key Points of Learning Name Components Passing through Peripheral distribution Central connection Function Cranial nerve Ⅰ olfactory Ⅱ optic Ⅲ occulomotor
Bell s Palsy. clinical practice. clinical problem. Donald H. Gilden, M.D.
 clinical practice Bell s Palsy Donald H. Gilden, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented,
clinical practice Bell s Palsy Donald H. Gilden, M.D. This Journal feature begins with a case vignette highlighting a common clinical problem. Evidence supporting various strategies is then presented,
STUDY OF VARIOUS CAUSES OF FACIAL PALSY AND ITS MANAGEMENT PROTOCOL
 STUDY OF VARIOUS CAUSES OF FACIAL PALSY AND ITS MANAGEMENT PROTOCOL S. Venkataramana Rao 1, V. S. Sharma 2, M. V. Subba Rao 3, B. J. Prasad 4, Kalyan 5, Pravin Tez 6, Vijay Kumar 7, G. S. Keerthi 8 1Professor,
STUDY OF VARIOUS CAUSES OF FACIAL PALSY AND ITS MANAGEMENT PROTOCOL S. Venkataramana Rao 1, V. S. Sharma 2, M. V. Subba Rao 3, B. J. Prasad 4, Kalyan 5, Pravin Tez 6, Vijay Kumar 7, G. S. Keerthi 8 1Professor,
Cranial Nerves and Spinal Cord Flashcards
 1. Name the cranial nerves and their Roman numeral. 2. What is Cranial Nerve I called, and what does it 3. Scientists who are trying to find a way to make neurons divide to heal nerve injuries often study
1. Name the cranial nerves and their Roman numeral. 2. What is Cranial Nerve I called, and what does it 3. Scientists who are trying to find a way to make neurons divide to heal nerve injuries often study
b. The groove between the two crests is called 2. The neural folds move toward each other & the fuse to create a
 Chapter 13: Brain and Cranial Nerves I. Development of the CNS A. The CNS begins as a flat plate called the B. The process proceeds as: 1. The lateral sides of the become elevated as waves called a. The
Chapter 13: Brain and Cranial Nerves I. Development of the CNS A. The CNS begins as a flat plate called the B. The process proceeds as: 1. The lateral sides of the become elevated as waves called a. The
Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve
 Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve Muscle weakness or complete paralysis may be secondary to an interruption in the communication between the brain and nerve cells in the
Muscle Weakness Or Paralysis With Compromise Of Peripheral Nerve Muscle weakness or complete paralysis may be secondary to an interruption in the communication between the brain and nerve cells in the
ORIGINAL ARTICLE. Is Bell s palsy a component of polyneuropathy?
 ORIGINAL ARTICLE Is Bell s palsy a component of polyneuropathy? Tu ba Tunç MD, Erkan Tarhan MD,, Haldun O uz MD, Mustafa As m Þafak MD, Gülnihal Kutlu MD, Levent E. nan MD From Ministry of Health, Ankara
ORIGINAL ARTICLE Is Bell s palsy a component of polyneuropathy? Tu ba Tunç MD, Erkan Tarhan MD,, Haldun O uz MD, Mustafa As m Þafak MD, Gülnihal Kutlu MD, Levent E. nan MD From Ministry of Health, Ankara
Anatomy and Physiology. Bones, Sutures, Teeth, Processes and Foramina of the Human Skull
 Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
Anatomy and Physiology Chapter 6 DRO Bones, Sutures, Teeth, Processes and Foramina of the Human Skull Name: Period: Bones of the Human Skull Bones of the Cranium: Frontal bone: forms the forehead and the
12 Anatomy and Physiology of Peripheral Nerves
 12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
12 Anatomy and Physiology of Peripheral Nerves Introduction Anatomy Classification of Peripheral Nerves Sensory Nerves Motor Nerves Pathologies of Nerves Focal Injuries Regeneration of Injured Nerves Signs
Anatomy of the Trigeminal Nerve
 19 Anatomy of the Trigeminal Nerve.1 Introduction 0. The Central Part of the Trigeminal Nerve 1..1 Origin 1.. Trigeminal Nuclei.3 The Peripheral Part of the Trigeminal Nerve 4.3.1 Ophthalmic Nerve 4.3.
19 Anatomy of the Trigeminal Nerve.1 Introduction 0. The Central Part of the Trigeminal Nerve 1..1 Origin 1.. Trigeminal Nuclei.3 The Peripheral Part of the Trigeminal Nerve 4.3.1 Ophthalmic Nerve 4.3.
The Nervous System: Central Nervous System
 The Nervous System: Central Nervous System I. Anatomy of the nervous system A. The CNS & the body by: 1. monitoring of the body 2. & information between parts of the body 3. acting as a to gather, store,
The Nervous System: Central Nervous System I. Anatomy of the nervous system A. The CNS & the body by: 1. monitoring of the body 2. & information between parts of the body 3. acting as a to gather, store,
Taste buds Gustatory cells extend taste hairs through a narrow taste pore
 The Special Senses Objectives Describe the sensory organs of smell, and olfaction. Identify the accessory and internal structures of the eye, and explain their function. Explain how light stimulates the
The Special Senses Objectives Describe the sensory organs of smell, and olfaction. Identify the accessory and internal structures of the eye, and explain their function. Explain how light stimulates the
Cranial Nerve VII : The Facial Nerve and Taste
 62 Cranial Nerve VII : The Facial Nerve and Taste H. KENNETH WALKER Definition The motor portion, or the facial nerve proper, supplies all the facial musculature. The principal muscles are the frontalis,
62 Cranial Nerve VII : The Facial Nerve and Taste H. KENNETH WALKER Definition The motor portion, or the facial nerve proper, supplies all the facial musculature. The principal muscles are the frontalis,
SPECIAL SENSES PART I: OLFACTION & GUSTATION
 SPECIAL SENSES PART I: OLFACTION & GUSTATION 5 Special Senses Olfaction Gustation Vision Equilibrium Hearing Olfactory Nerves Extend through cribriform plate into nasal cavity on both sides of nasal septum
SPECIAL SENSES PART I: OLFACTION & GUSTATION 5 Special Senses Olfaction Gustation Vision Equilibrium Hearing Olfactory Nerves Extend through cribriform plate into nasal cavity on both sides of nasal septum
Maxilla, ORBIT and infratemporal fossa. Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine
 Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Maxilla, ORBIT and infratemporal fossa Neophytos C Demetriades MD, DDS, MSc Associate professor European University of Cyprus School of Medicine MAXILLA Superior, middle, and inferior meatus Frontal sinus
Rehabilitation of the Paralyzed Face
 Rehabilitation of the Paralyzed Face Elizabeth J. Rosen, MD Faculty Advisor: Karen H. Calhoun, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 30,
Rehabilitation of the Paralyzed Face Elizabeth J. Rosen, MD Faculty Advisor: Karen H. Calhoun, MD The University of Texas Medical Branch Department of Otolaryngology Grand Rounds Presentation October 30,
I: To describe the pyramidal and extrapyramidal tracts. II: To discuss the functions of the descending tracts.
 Descending Tracts I: To describe the pyramidal and extrapyramidal tracts. II: To discuss the functions of the descending tracts. III: To define the upper and the lower motor neurons. 1. The corticonuclear
Descending Tracts I: To describe the pyramidal and extrapyramidal tracts. II: To discuss the functions of the descending tracts. III: To define the upper and the lower motor neurons. 1. The corticonuclear
Dr.Ban I.S. head & neck anatomy 2 nd y جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102
 جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
جامعة تكريت كلية طب االسنان مادة التشريح املرحلة الثانية أ.م.د. بان امساعيل صديق 6102/6102 Pterygopalatine fossa: The pterygopalatine fossa is a cone-shaped depression, It is located between the maxilla,
Peripheral Nervous System Dr. Gary Mumaugh
 Peripheral Nervous System Dr. Gary Mumaugh Spinal Nerves Overview Thirty-one pairs of spinal nerves are connected to the spinal cord No special names; numbered by level of vertebral column at which they
Peripheral Nervous System Dr. Gary Mumaugh Spinal Nerves Overview Thirty-one pairs of spinal nerves are connected to the spinal cord No special names; numbered by level of vertebral column at which they
Intensity of MR Contrast Enhancement Does Not Correspond to Clinical and Electroneurographic Findings in Acute Inflammatory Facial Nerve Palsy
 Intensity of MR Contrast Enhancement Does Not Correspond to Clinical and Electroneurographic Findings in Acute Inflammatory Facial Nerve Palsy Sabine Sartoretti-Schefer, Peter Brändle, Werner Wichmann,
Intensity of MR Contrast Enhancement Does Not Correspond to Clinical and Electroneurographic Findings in Acute Inflammatory Facial Nerve Palsy Sabine Sartoretti-Schefer, Peter Brändle, Werner Wichmann,
Anatomic Relations Summary. Done by: Sohayyla Yasin Dababseh
 Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Anatomic Relations Summary Done by: Sohayyla Yasin Dababseh Anatomic Relations Lecture 1 Part-1 - The medial wall of the nose is the septum. - The vestibule lies directly inside the nostrils (Nares). -
Facial Nerve Palsy in Three HIV/AIDS Patients
 Facial Nerve Palsy in Three HIV/AIDS Patients By A.I. Shugaba, R.M. Mathew, C. B. Uzokwe, F.Shinku, Y.M. Usman B. M. Mohammed, A. M. Rabiu, I. M. Gambo and M.B.T. Umar ISSN 0970-4973 (Print) ISSN 2319-3077
Facial Nerve Palsy in Three HIV/AIDS Patients By A.I. Shugaba, R.M. Mathew, C. B. Uzokwe, F.Shinku, Y.M. Usman B. M. Mohammed, A. M. Rabiu, I. M. Gambo and M.B.T. Umar ISSN 0970-4973 (Print) ISSN 2319-3077
Viral Antibody Titer Changes in Acute and Convalescent Stage of Bell s Palsy
 Journal of the K. S. C. N. Vol. 3, No. 1 Viral Antibody Titer Changes in Acute and Convalescent Stage of Bell s Palsy Sang Il Suh, M.D., Joon Soek Bae, M.D., Sung Je Kim, M.D., Tae Il Kim M.D., Ji Eun
Journal of the K. S. C. N. Vol. 3, No. 1 Viral Antibody Titer Changes in Acute and Convalescent Stage of Bell s Palsy Sang Il Suh, M.D., Joon Soek Bae, M.D., Sung Je Kim, M.D., Tae Il Kim M.D., Ji Eun
1. What is the embryologic origin of the major salivary glands, and when do they develop? 2. What is the embryologic origin of minor salivary glands?
 Salivary Gland Chapters 37, 38, 39, 40 Shapiro 1. What is the embryologic origin of the major salivary glands, and when do they develop? Outpouchings of oral ectoderm in the 6th 8 th week 2. What is the
Salivary Gland Chapters 37, 38, 39, 40 Shapiro 1. What is the embryologic origin of the major salivary glands, and when do they develop? Outpouchings of oral ectoderm in the 6th 8 th week 2. What is the
