Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich
|
|
|
- June Booker
- 6 years ago
- Views:
Transcription
1 Zurich Open Repository and Archive University of Zurich Main Library Strickhofstrasse 39 CH-8057 Zurich Year: 2013 Nitric oxide synthase 2 is required for conversion of pro-fibrogenic inflammatory CD133+ progenitors into F4/80+ macrophages in experimental autoimmune myocarditis Blyszczuk, Przemyslaw; Berthonneche, Corrine; Behnke, Silvia; Glönkler, Marcel; Moch, Holger; Pedrazzini, Thierry; Lüscher, Thomas F; Eriksson, Urs; Kania, Gabriela Abstract: AIMS: Experimental Autoimmune Myocarditis (EAM) model mirrors important mechanisms of inflammatory dilated cardiomyopathy (idcm). In EAM, inflammatory CD133(+) progenitors are a major cellular source of cardiac myofibroblasts in post-inflammatory myocardium. We hypothesized that exogenous delivery of Macrophage-Colony Stimulating Factor (M-CSF) can stimulate macrophage lineage differentiation of inflammatory progenitors and therefore prevent their naturally occurring myofibroblast fate in EAM.Methods and ResultsEAM was induced in wild-type (BALB/c) and Nitric oxide synthase 2 deficient (Nos2(-/-)) mice and CD133(+) progenitors were isolated from inflamed hearts. In vitro, M-CSF converted inflammatory CD133(+) progenitors into nitric oxide-producing F4/80(+) macrophages and prevented TGF--mediated myofibroblast differentiation. Importantly, only a subset of heart-infiltrating CD133(+) progenitors expresses macrophage-specific antigen F4/80 in EAM. These CD133(+)/F4/80(hi) cells show impaired myofibrogenic potential compared to CD133(+)/F4/80(-) cells. M-CSF treatment of wild-type mice with EAM at the peak of disease markedly increased CD133(+)/F4/80(hi) cells in the myocardium, and CD133(+) progenitors isolated from M-CSF-treated mice failed to differentiate into myofibroblasts. In contrast, M-CSF was not effective in converting CD133(+) progenitors from inflamed hearts of Nos2(-/-) mice into macrophages, and M-CSF treatment did not result in increased CD133(+)/F4/80(hi) cell population in hearts of Nos2(-/-) mice. Accordingly, M-CSF prevented postinflammatory fibrosis and left ventricular dysfunction in wild-type but not in Nos2(-/-) mice. CON- CLUSIONS: Active and NOS2-dependent induction of macrophage lineage differentiation abrogates the myofibrogenic potential of heart-infiltrating CD133(+) progenitors. Modulating the in vivo differentiation fate of specific progenitors might become a novel approach for the treatment of inflammatory heart diseases. DOI: Posted at the Zurich Open Repository and Archive, University of Zurich ZORA URL: Accepted Version Originally published at: Blyszczuk, Przemyslaw; Berthonneche, Corrine; Behnke, Silvia; Glönkler, Marcel; Moch, Holger; Pedrazzini, Thierry; Lüscher, Thomas F; Eriksson, Urs; Kania, Gabriela (2013). Nitric oxide synthase 2 is required for conversion of pro-fibrogenic inflammatory CD133+ progenitors into F4/80+ macrophages in experimental autoimmune myocarditis. Cardiovascular Research, 97(2): DOI:
2 Cardiovascular Research Advance Access published October 22, Nitric oxide synthase 2 is required for conversion of pro-fibrogenic inflammatory CD133 + progenitors into F4/80 + macrophages in experimental autoimmune myocarditis Przemyslaw Blyszczuk 1,2, Corrine Berthonneche 3, Silvia Behnke,4, Marcel Glönkler 5, Holger Moch 5, Thierry Pedrazzini 3, Thomas F. Lüscher 1,6, Urs Eriksson 1,2, Gabriela Kania 1,2 1 Cardiovascular Research and Zürich Center for Integrative Human Physiology; Institute of Physiology, University of Zürich, Winterthurerstr. 190, CH-8057 Zürich, Switzerland; 2 Department of Medicine, GZO - Zürich Regional Health Center, Spitalstr. 66, CH-8620 Wetzikon, Switzerland; 3 Experimental Cardiology Unit, Department of Medicine, University of Lausanne Medical School, CH-1011 Lausanne, Switzerland 4 Sophistolab AG, Bauelenzelgstrasse 20, 8193 Eglisau, Switzerland, 5 Institute for Surgical Pathology, Department of Pathology; 6 Department of Cardiology; University of Zurich, Switzerland; Winterthurerstr. 190, CH-8057 Zürich, and University Hospital Zürich, Rämistr. 100, CH-8001 Zürich, Switzerland Corresponding author: Gabriela Kania, PhD Cardioimmunology, Cardiovascular Research, Institute of Physiology, University of Zürich Winterthurerstrasse 190, CH-8057 Zürich, Switzerland phone: ; fax: gabriela.kania@uzh.ch Shared last authorship Published on behalf of the European Society of Cardiology. All rights reserved. The Author For permissions please journals.permissions@oup.com
3 2 Abstract Aims: Experimental Autoimmune Myocarditis (EAM) model mirrors important mechanisms of inflammatory dilated cardiomyopathy (idcm). In EAM, inflammatory CD133 + progenitors are a major cellular source of cardiac myofibroblasts in post-inflammatory myocardium. We hypothesized that exogenous delivery of Macrophage-Colony Stimulating Factor (M-CSF) can stimulate macrophage lineage differentiation of inflammatory progenitors and therefore prevent their naturally occurring myofibroblast fate in EAM. Methods and Results: EAM was induced in wild-type (BALB/c) and Nitric oxide synthase 2 deficient (Nos2 / ) mice and CD133 + progenitors were isolated from inflamed hearts. In vitro, M-CSF converted inflammatory CD133 + progenitors into nitric oxide-producing F4/80 + macrophages and prevented TGF-βmediated myofibroblast differentiation. Importantly, only a subset of heart-infiltrating CD133 + progenitors expresses macrophage-specific antigen F4/80 in EAM. These CD133 + /F4/80 hi cells show impaired myofibrogenic potential compared to CD133 + /F4/80 cells. M-CSF treatment of wild-type mice with EAM at the peak of disease markedly increased CD133 + /F4/80 hi cells in the myocardium, and CD133 + progenitors isolated from M-CSF-treated mice failed to differentiate into myofibroblasts. In contrast, M-CSF was not effective in converting CD133 + progenitors from inflamed hearts of Nos2 / mice into macrophages, and M- CSF treatment did not result in increased CD133 + /F4/80 hi cell population in hearts of Nos2 / mice. Accordingly, M-CSF prevented post-inflammatory fibrosis and left ventricular dysfunction in wild-type but not in Nos2 / mice. Conclusions: Active and NOS2-dependent induction of macrophage lineage differentiation abrogates the myofibrogenic potential of heart-infiltrating CD133 + progenitors. Modulating the in vivo differentiation fate of specific progenitors might become a novel approach for the treatment of inflammatory heart diseases. Key words: experimental autoimmune myocarditis, CD133 progenitor, M-CSF, myofibroblast, macrophage, nitric oxide synthase 2
4 Introduction Inflammatory dilated cardiomyopathy (idcm) is an important cause of heart failure and sudden death in children and young patients 1. Progressive cardiac dilation and fibrosis are hallmarks of idcm in humans. idcm refers to an end stage heart failure phenotype which often results from virus-triggered myocarditis 2. Both, clinical observations and animal experiments suggest that infection-triggered autoimmunity plays an important role in idcm 3. Heart-specific autoimmune responses are a consequence of the lack of T cell tolerance to heart-specific alpha-myosin heavy chain (αmyhc) in mice and in humans 4. Experimental autoimmune myocarditis (EAM) is a CD4 + T cell-mediated mouse model of idcm. In susceptible mouse strains, EAM is commonly induced after immunization with αmyhc peptide together with a strong adjuvant 4. In BALB/c mice, the extent of cardiac infiltrates peaks three weeks after immunization. Inflammatory infiltrates largely resolve thereafter, but the process of pathological remodelling continues and many mice develop an end stage heart failure phenotype, including ventricular dilation, myocardial fibrosis and heart failure on follow-up 5. At the peak of EAM, inflammatory cells, including granulocytes, monocytes, macrophages, T cells, B cells, and CD133 + progenitors infiltrate the myocardium 4, 6. CD133 (prominin-1) and its human orthologue, AC133, are often expressed on primitive cell populations including hematopoietic stem cells. In EAM, bone marrow-derived CD133 + progenitors represent the major cellular source of collagen-producing fibroblasts involved in the progressive Transforming Growth Factor-beta (TGF-β)-mediated cardiac remodelling 6, which reflects the transition from acute inflammation into the typical end stage heart failure phenotype. Macrophages represent another important heart-infiltrating cell subset in EAM 7. In mice, macrophages commonly express the F4/80 antigen. Their role in disease pathogenesis, however, remains controversial. So far, the nitric oxide synthase 2 (NOS2)-expressing M1 macrophage subset had been considered to contribute to disease progression 7, 8, On the other hand, nitric oxide also acts as a strong immunosuppressive molecule preventing EAM development via induction of T cell apoptosis 6. Alternatively activated M2 macrophages, are considered to promote resolution of inflammation and reduce disease severity 7-9.
5 4 Macrophage-colony stimulating factor (M-CSF) is one of the key cytokines regulating immune responses and reparative processes in many inflammatory and cardiovascular disorders 10, 11. M-CSF plays a pivotal role in differentiation and maturation of the macrophage myeloid lineage 12. Mice lacking functional M-CSF show macrophage deficiency, reduced phagocytosis and strongly impaired nitric oxide production 13. In animal models of ischemic heart failure and viral myocarditis, M-CSF treatment improves cardiac function 14, 15,16, but the mechanism is still unclear. We hypothesize that altering the in vivo fate of inflammatory progenitors by selectively promoting macrophage lineage differentiation, may protect from myofibroblast accumulation and cardiac fibrosis in EAM. In fact, M-CSF induced conversion of heart-infiltrating CD133 + progenitors into F4/80 + macrophages and prevented their myofibroblast differentiation in the post-inflammatory phase of EAM. Moreover, our data points to critical role of NOS2 and nitric oxide in M-CSF-dependent macrophage lineage differentiation of inflammatory CD133 + progenitors. Thus, we demonstrate how exogenous cytokine treatments may change the default differentiation fate of inflammatory progenitors and can prevent pathological tissue remodelling in idcm.
6 Methods Mice BALB/c (n=250) and Nos2 / (n=50) mice on BALB/c background were used in this study. Animal experiments were performed in accordance with the Swiss federal law and with the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH Publication, 8th Edition, 2011). All animal experiments were approved by the Cantonal Veterinary Office in Zürich. EAM induction and cytokine treatments Mice were injected subcutaneously with 150 µg of αmyhc (Ac-RSLKLMATLFSTYASADR-OH; Caslo) peptide emulsified 1:1 with Complete Freund's Adjuvant (CFA, Difco) on days 0 and µg/kg M-CSF (Peprotech) were intravenously injected 5x every second day between days or days of EAM. Control mice received solvent only. Histopathology and Immunocytochemistry Hearts were formalin-fixed and paraffin-embedded. Heart sections were stained with rat anti-mouse CD45 (BD Bioscience), rabbit anti-mouse CD3 (Neomarkers), rat anti-mouse F4/80 (BMA biomedicals) and rabbit anti-rat IgG (Abcam) antibodies, and with Bond Polymer Refine Detection kit using BOND-MAX system (both Leica). Masson s Trichrom staining was used to detect fibrosis. Immunopositive cells and fibrotic areas were quantified using analysis FIVE software (Olympus). Echocardiography Mice were lightly anesthetized with 1-1.5% isoflurane, maintaining heart rate at beats per minute. Transthoracic echocardiography was performed using a 30 MHz probe and the Vevo 770 Ultrasound system (VisualSonics) as described 17 and in Supplementary Material. Cell cultures Myocarditis-positive hearts were perfused, dissected and digested with Liberase Blendzyme (Roche) for 45
7 6 min at 37 C and tissue suspensions were passed sequentially through 70 µm and 40 µm cell strainers. Cardiomyocytes were separated by low speed centrifugation (50 g, 2 min). CD133 + cells were isolated by positive selection using anti-cd133-pe antibody (ebioscience) and magnetic anti-pe-microbeads (Miltenyi) or using FACS. Enriched CD133 + cells were plated onto gelatine-coated cell culture plates and cultured in the Iscove's Modified Dulbecco's Medium supplemented with 20% foetal bovine serum, 1:100 penicillin/streptomycin, 100 mm non-essential amino acids, 100 mm sodium pyruvate and 50mM β- mercaptoethanol (all Invitrogen). Macrophage differentiation was induced with 10 ng/ml M-CSF, and fibroblast differentiation with 10 ng/ml TGF-β (both PeproTech). Flow cytometry and cell sorting Single cell suspensions were prepared from digested hearts and cultured cells. Cells were incubated 30 min on ice with the appropriate combination of fluorochrome- or biotin-conjugated antibodies. The following antibodies were used: anti-cd45-fitc, anti-cd45-pe, anti-nos2-fitc (all BD Bioscience), anti-cd133- PE, anti-f4/80-pe (both ebioscience), biotin-conjugated anti-f4/80 (Cedarlane), anti-cd16/32 (Miltenyi), anti-cd206 (Biolegend), anti-cd301 (Serotec), anti-cd133 (ebioscience). Streptavidin-APC (BD Bioscience) was used to detect biotin-conjugated antibodies. Cells were analysed with the FACSCanto analyser (BD Bioscience) and FlowJo software (Tree Star). In some experiments, cells were sorted with FACSAria III (BD Bioscience). Quantitative RT-PCR Total RNA was isolated using RNeasy micro kit (Qiagen). cdnas were amplified using the Power SYBR Green PCR Master Mix (Applied Biosystems) and oligonucleotides complementary to transcripts of the analyzed genes using the 7500 Fast Real-Time PCR System (Applied Biosystems). The following oligonucleotides were used in this study: αsma (Acta2): 5 -cgctgtcaggaaccctgaga-3, 5 - cgaagccggccttacaga-3 ; collagen I (Col1a1): 5 -gatgacgtgcaatgcaatgaa-3, 5 -ccctcgactcctacatcttctga- 3 ; fibronectin (Fn1): 5 -taccaaggtcaatccacacccc-3, 5 -cagatggcaaaagaaagcagagg-3 ; gapdh (Gapdh): 5 - ctgcaccaccaactgcttagc-3, 5 -ggcatggactgtggtcatgag-3. Transcript levels of gapdh were used as endogenous reference, and relative gene expression was analyzed using the 2 - Ct method.
8 Immunohistochemistry and phagocytosis assays Cells were cultured on gelatine-coated cover slips and fixed with 4% paraformaldehyde or methanol:acetone (7:3). 1% bovine serum albumin was used as blocking solution. The following antibodies were used: mouse IgG anti-αsma (Sigma), rabbit IgG anti-fibronectin (Milipore), AlexaFluor488 anti-mouse IgG and AlexaFluor546 anti-rabbit IgG 1:600 (both Invitrogen). DAPI was used to label nuclei. Alexa Fluor 488- conjugated Escherichia coli BioParticles (Invitrogen) were used according to manufacturer s recommendations. Immunofluorescence was analysed using the Olympus BX51 fluorescence microscope. Statistics Normally distributed data were analysed by unpaired, two-tailed Student s t-test and by one-way ANOVA followed by Bonferroni post-hoc test. Severity scores were analysed by the one-way Kruskal-Wallis analysis. For correlation analysis, Pearson's correlation coefficient was calculated. All analyses were computed using GraphPad Prism 5 software. Differences were considered as statistically significant for p<0.05.
9 8 Results M-CSF converts heart-infiltrating CD133 + progenitors into functional F4/80 + macrophages, and prevents TGF-β-induced myofibroblast differentiation in vitro. BALB/c mice receiving two subcutaneous injections of αmyhc/cfa at days 0 and 7 develop severe myocarditis at day 21. At this stage, CD133 + progenitors represent about 30% of all CD45 + inflammatory cells in the heart 6. To assess the differentiation capacity of these cells at the peak of disease, CD133 + cells were isolated from diseased hearts at day 21 of EAM, plated and expanded for two weeks in vitro. Expanded cells were cultured in the presence or absence of M-CSF or TGF-β for additional 14 days. In the presence of TGF-β, CD133 + cells differentiated into myofibroblasts, positive for αsma and fibronectin (Fig. 1A-B). In contrast, addition of M-CSF failed to trigger myofibroblast differentiation (Fig. 1A-B) and pre-treatment of CD133 + cells with M-CSF for 3 days prevented TGF-β-triggered myofibroblast formation (Fig. 1C-D). In cytokine-free cultures, most expanded cells remained positive for CD133 and were mainly negative for macrophage marker F4/80 (Supplementary Figure 1A-B). In the presence of M-CSF, however, CD133 expression was reduced (Supplementary Figure 1A) and cells up-regulated F4/80, CD11b and CD16/32, suggesting macrophage lineage differentiation (Supplementary Figure 1B-D). Cells cultured with M-CSF developed into fully active macrophages producing NOS2, secreting nitric oxide and phagocyting E.coli bacteria (Supplementary Figure 1E,F,J). Of note, M-CSF treatment did not affect expression of markers characteristic for alternatively activated M2 macrophages (CD206, CD301, Supplementary Figure 1G-H) or markers characteristic for granulocytes or dendritic cells, i.e. Gr-1 (Ly6C, Supplementary Figure 1I), MHC class II and CD11c (not shown). To address the immunomodulating potential of CD133 + progenitors and CD derived M-CSFdifferentiated macrophages we co-cultured them with αmyhc-reactive Th17 cell lines in the presence of αmyhc-pulsed irradiated splenocytes as antigen presenting cells. On irradiated splenocytes, αmyhcreactive CD4 + T cells proliferated rapidly. In the presence of CD133 + progenitors or M-CSF-differentiated macrophages, however, proliferation was completely abolished (Supplementary Figure 2A). Further, we induced EAM in BALB/c mice and additionally administrated intravenously 2x10 6 of either in vitro
10 expanded CD133 + progenitors or CD derived mature macrophages at day 7 after EAM induction and analysed myocarditis severity at day 21. In animals treated with both, CD133 + progenitors and M-CSFdifferentiated macrophages practically no myocarditis was observed compared to sham treated mice (Supplementary Figure 2B). In contrast, administration of M-CSF-differentiated macrophages expanded from Nos2 / mice failed to protect from myocarditis (Supplementary Figure 2C). These latter findings confirm the protective and NOS2-dependent role of CD derived M-CSF-differentiated macrophages in EAM. M-CSF treatment promotes accumulation of F4/80 + macrophages in the post-inflammatory heart At day 21, inflamed hearts contained a substantial pool of CD133 + progenitors, but fibrosis was not evident at this time point. As illustrated above, M-CSF effectively directs CD133 + progenitors into functional macrophages and prevents their myofibroblast differentiation. We therefore analysed how systemic M-CSF treatment of αmyhc/cfa-immunized mice affects the pattern of heart-infiltrating cell subsets. Accordingly, αmyhc/cfa-immunized mice received M-CSF injections between days of EAM (Supplementary figure 3A). Three days after the first M-CSF injection, we observed significantly increased number of F4/80 + and CD133 + cells in the myocardium of M-CSF treated mice (day 24, Figure 2A-B). Immunopositive F4/80 + macrophages in the myocardium decreased over time and remained at low numbers at day 40 (Figure 2A; Supplementary Figure 4A-B). M-CSF treatments, however, did not affect the expression of CD16/32, CD206 and CD301 in inflammatory macrophages (Figure 2E-G). Instead, we observed significantly increased NOS2 on F4/80 + cells in the heart after M-CSF treatment of wild-type mice (Figure 2D). M-CSF inhibits formation of myofibroblasts from inflammatory CD133 + progenitors in EAM Heart-infiltrating CD133 + progenitors represent the major cellular source of myofibroblasts in postinflammatory EAM 6. At day 24 of EAM, we sorted inflammatory (CD45-positive) CD133 + /F4/80 and CD133 + /F4/80 hi cells from the inflamed myocardium of BALB/c mice and found elevated levels of myofibroblast-specific genes in CD133 + cells negative for F4/80 (Figure 3A-B). These findings suggest that CD133 + /F4/80 rather than CD133 + /F4/80 hi cells contribute to fibrogenesis in post-inflammatory EAM.
11 10 M-CSF-stimulated CD133 + progenitors acquired a functional macrophage phenotype within 3 days in vitro (Figure 2H). We therefore analysed F4/80 expression on heart-infiltrating CD133 + progenitors in M- CSF-treated mice. We found that heart-infiltrating CD133 + /CD45 + cells of M-CSF-treated mice had marked higher F4/80 at day 24 (i.e. 3 days after the cytokine treatment, Figure 3C-D). Next, we sorted heartinfiltrating CD133 + /CD45 + cells from PBS- and M-CSF-treated mice and found reduced mrna levels of myofibroblast-specific genes in the M-CSF-treated group (Figure 3E). Furthermore, sorted heart-infiltrating CD133 + /CD45 + cells from both groups were plated and cultured in the presence of TGF-β for 10 days. CD133 + /CD45 + cells isolated from the myocardium of M-CSF-treated mice failed to differentiate into αsma- and fibronectin-expressing myofibroblasts (Figure 3F). NOS2 controls M-CSF-dependent macrophage differentiation of heart-infiltrating CD133 + progenitors F4/80 hi macrophages derived from CD133 + progenitors up-regulate NOS2 and produce nitric oxide. We therefore addressed the role of NOS2 in the macrophage differentiation processes. Accordingly, CD133 + progenitors were isolated at day 21 after immunization from inflamed hearts of wild-type or Nos2 / mice and cultivated in the presence of M-CSF. Nos2 / CD133 + progenitors showed reduced F4/80 and CD14 expression and were functionally impaired as indicated by reduced E.coli phagocytosis (Figure 4A-E). To determine whether macrophage differentiation was mediated by NOS activity, CD133 + progenitors isolated from inflamed hearts of BALB/c mice were cultured for 3 days in the presence of M-CSF with or without L- NAME, a non-specific NOS inhibitor. Cells cultured with L-NAME showed significantly reduced E.coli phagocytosis (Figure 4F) and reduced nitric oxide levels (Figure 4G). M-CSF treatment prevents cardiac fibrosis and left ventricular dysfunction in EAM M-CSF prevents TGF-β-mediated myofibroblast differentiation and promotes formation of macrophages from inflammatory CD133 + progenitors. Given that CD133 + progenitors represent the major source for myofibroblasts in EAM, we addressed whether M-CSF treatment reduces fibrogenesis in the postinflammatory heart. Accordingly, we treated αmyhc/cfa-immunized mice with M-CSF between days or of EAM, and analysed the hearts at day 40 and 60 respectively (Supplementary figure 3A). As
12 illustrated in the Figure 5, M-CSF treatment completely prevented accumulation of fibroblasts in the postinflammatory heart (Figure 5A-C; Supplementary figure 4B). Of note, M-CSF treatment failed to attenuate fibrosis when delivered between days (Figure 5A). These findings suggest that M-CSF treatment prevented the fibrotic process, but did not revert already established cardiac fibrosis. Relapses of inflammatory cells are quite common in autoimmune diseases. In BALB/c mice, we observed spontaneous inflammatory relapses 40 days after the first immunization (Figure 5D-E). During relapses, CD45 + inflammatory cells were mainly detected in the pericardium and largely represented CD3 + T lymphocytes (Figure 5D-E, Supplementary figure 3C). Interestingly, M-CSF treatment between days inhibited relapses in αmyhc/cfa-immunized mice as reflected by reduced numbers of CD45 + and CD3 + T cells in the myocardium at day 40 (Figure 5D-E; Supplementary figure 3C). Cardiac fibrosis parallels both, diastolic dysfunction, and reduced cardiac contractility. Not all immunized mice develop severe myocarditis. Consequently the extent of post-inflammatory fibrosis varies in the EAM model. In our series, 11 out of 20 αmyhc/cfa-immunized BALB/c mice showed substantial fibrosis (>2% of total heart area) on day 40. At this time point, echocardiography revealed reduced ejection fraction and fractional shortening in mice with significant fibrosis (Figure 5F). In addition, the extent of fibrosis correlated with increased mass, systolic and diastolic volume and isovolumetric contraction time of the left ventricle (Supplementary Figure 5A). Echocardiography of αmyhc/cfa-immunized and M-CSFtreated mice showed unaffected cardiac function at day 40 (Figure 5F, Supplementary Figure 5E). Next, we immunized Nos2 / mice with αmyhc/cfa and treated with M-CSF or PBS between days αmyhc/cfa immunization resulted in myocarditis in Nos2 / mice (not shown), but M-CSF treatment failed to affect fibrosis and heart functions during the post-inflammatory phase of EAM in Nos2 / mice (Figure 6A, Supplementary figure 6). Similar results were observed if mice were M-CSF treated between days (not shown). M-CSF treatment of Nos2 / mice failed to increase the numbers of F4/80 + macrophages and CD133 + cells in the myocardium at day 24 and 40 of EAM (Figure 6A-C). We also observed no differences in F4/80 expression on inflammatory CD133 + /CD45 + progenitors (not shown) and in the expression of M1/M2 markers on heart infiltrating F4/80 + /CD45 + macrophages between M-CSF- and PBS-treated Nos2 / mice (Figure 6D).
13 12 Discussion We previously reported that in the EAM model post-inflammatory pathogenic myofibroblasts mainly originate from heart-infiltrating CD133 + progenitor cells 6. In line with our previous findings, herein we demonstrate that M-CSF controls the formation of anti-inflammatory macrophages from inflammatory CD133 + progenitors and prevents TGF-β-mediated differentiation into pathogenic myofibroblasts. Thus, our data suggest that in myocarditis, a significant pool of cells infiltrating the myocardium at the peak of disease represent non-committed progenitors. From a clinical perspective it is important that the differentiation fate of multipotent, noncommitted precursor cells infiltrating the myocardium, can be modulated via specific cytokine signalling in a controlled fashion. M-CSF is a key cytokine guiding macrophage differentiation in vitro 8 and in vivo 18. In EAM, M-CSF treatment up-regulated F4/80 expression on CD133 + inflammatory progenitors promoting macrophage differentiation. In untreated mice, however, heart-infiltrating CD133 + progenitors spontaneously differentiate into pathogenic myofibroblasts. To our knowledge, this is the first report describing the change of in vivo fate of inflammatory progenitors naturally present in the inflamed organ. So far, it has been described that M-CSF treatment improved cardiac function in a viral model of myocarditis 16, after myocardial infarction 14, 15, 19 and in the ischemia-reperfusion model 20. Similar to our findings, M-CSF treatment promoted monocyte/macrophage accumulation in the heart after myocardial infarction 14, 15 or virus inoculation 16. Myocardial fibrosis plays a dual role in remodelling after cardiac injury. On one hand, it is a prerequisite for wound healing, as in case of ischemic injuries, for example. On the other hand, it contributes to ventricular stiffening and typical pathological remodelling in heart failure. Our previous and current data clearly show that excessive cardiac fibrosis parallels impaired cardiac function in EAM 17. Thus, preserved left ventricular function in M-CSF-treated mice results primarily from reduced myofibroblast differentiation, rather than protective macrophage activity. We propose that the conversion of inflammatory progenitors into functional macrophages, instead of myofibroblasts, represent a key mechanism explaining reduced fibrogenesis upon M-CSF treatment. However, we cannot rule out that M-CSF also activates other pathways inhibiting myocardial fibrogenesis. For example, M-CSF may protect cardiomyocytes from H 2 O 2 -induced death 20. Moreover, M-CSF could affect extracellular matrix composition and levels of matrix
14 metalloproteinases and cytokines/chemokines, which drastically alter the myocardial microenvironment. Nevertheless, we can exclude direct M-CSF-mediated effects on cardiac fibroblasts, because upon M-CSF treatment during the late post-inflammatory phase of the EAM (days 40-48), the fibrosis was not reverted. It has been proposed that differential macrophage activation defines protective and pathogenic functions. Accordingly, adoptive transfer of M1 macrophages promoted histological disease scores, whereas injection of M2 macrophages was largely protective in Coxackievirus-induced myocarditis 9. Also most heart-infiltrating macrophages were classified as M2 macrophages expressing mannose receptor and Gr-1 in αmyhc/cfa- and Coxackievirus-induced myocarditis 7, 21. However, macrophages expressing M1 marker NOS2 have been identified in myocarditis as well 22. We critically analysed macrophages in the myocardium after the peak of disease, during the post-inflammatory phase of EAM, and detected both, M1- and M2- specific markers. We were, however, unable to clearly delineate two distinct activation states. We assume that during EAM, heart-infiltrating macrophages were activated classically (M1) and alternatively (M2) at the same time. In fact, it is well known that T cells and other heart-infiltrating cells massively produce both, M1-activating IFN-γ as well as M2-activating IL-4 and IL Importantly, M-CSF treatment did not affect the expression of M1 and M2 markers except of NOS2. M-CSF-induced macrophage accumulation in the post-inflammatory heart was not pathogenic in our model, because resolution of inflammation, defined by the extent of inflammatory cells was clearly M-CSF independent. Moreover, M-CSF-induced macrophages showed strong immunosuppressive activity in vitro and in vivo. We believe that accumulation of the immunosuppressive macrophages in M-CSF-treated mice protected from spontaneous T cell relapse. Nevertheless, we cannot, entirely rule out that M-CSF also mediates protective effects by acting on other target cells. We previously found that M-CSF-induced CD11b + monocytes prevented EAM development and suppressed CD4 + T cell proliferation in a nitric oxide-dependent manner 23. M-CSF treatment promoted inflammatory macrophages expressing NOS2 in EAM, We therefore hypothesized that macrophageproduced nitric oxide might control both; T cell mediated early inflammation as well as post-inflammatory fibrosis in EAM. Indeed, mice lacking NOS2 or treated with nitric oxide inhibitors showed enhanced cardiac inflammation and fibrotic lesions in a model of Coxackievirus-induced myocarditis 24, 25. Similarly, Nos2 / mice also develop more severe myocarditis in the EAM model (Kania, Blyszczuk & Eriksson- unpublished
15 14 observations). Nevertheless, we observed spontaneous resolution of inflammation in Nos2 / mice, suggesting that NOS2 is not critically involved in the resolution of inflammation in the EAM model. Surprisingly, treatment of Nos2 / mice with M-CSF failed to turn CD133 + progenitors into macrophages and to prevent fibrosis development. Furthermore, we showed that Nos2 / CD133 + progenitors stimulated with M-CSF failed to generate functional macrophages. These results suggested that NOS2 was required for M-CSF-induced macrophage differentiation and maturation. Accordingly, NOS2 has been reported to control differentiation of human monoblasts 26. Regulation of gene expressions by nitric oxide can explain requirement of NOS2 in this differentiation processes 27. At this stage, we cannot, however, exclude that in Nos2 / mice, heart-infiltrating CD133 + progenitors are committed toward fibroblast phenotype due to alerted cytokine expression profile in the myocardium. Based on our findings, we can assume that M-CSF stimulates nitric oxide production that, in turn, promotes macrophage differentiation of inflammatory progenitors. In summary, our data demonstrate that a single hematopoietic cytokine, such as M-CSF can modulate the in vivo fate of inflammatory CD133 + progenitors in a way to promote their differentiation into macrophages instead of myofibroblasts in the post-inflammatory phase of the EAM. Furthermore, our data suggest that mature inflammatory macrophages, in contrast to progenitor-derived fibroblasts, do not promote heart failure after acute myocarditis. These findings are in line with the clinical observation that fulminant myocarditis implies an excellent long-term prognosis whereas subacute myocarditis usually progresses to end stage heart failure 28. Acknowledgment We thank Marta Bachman for excellent technical assistance, Flow Cytometry Facility at University Zurich for excellent sorting service and Dr. Pavani Mocharla for critical reading. Funding U.E. acknowledges support from the Swiss Life Foundation, P.B. from the Swiss Heart Foundation and G.K. from the Olga Mayenfisch Foundation, Hartmann Müller Foundation, and Holcim Foundation. The study was supported by the Swiss National Science Foundation (U.E. and G.K.: Grant 32003B_130771) and Swiss
16 National Science Foundation MHV subsidy (G.K.: Grant PMPDP3_129013). Conflict of Interest None
17 16 References: 1. Aretz HT, Billingham ME, Edwards WD, Factor SM, Fallon JT, Fenoglio JJ, Jr. et al. Myocarditis. A histopathologic definition and classification. Am J Cardiovasc Pathol. 1987;1: Kishimoto C, Abelmann WH. In vivo significance of T cells in the development of Coxsackievirus B3 myocarditis in mice. Immature but antigen-specific T cells aggravate cardiac injury. Circ Res. 1990;67: Leuschner F, Katus HA, Kaya Z. Autoimmune myocarditis: past, present and future. J Autoimmun. 2009;33: Rose NR. Myocarditis: infection versus autoimmunity. J Clin Immunol. 2009;29: Kania G, Blyszczuk P, Eriksson U. Mechanisms of cardiac fibrosis in inflammatory heart disease. Trends Cardiovasc Med. 2009;19: Kania G, Blyszczuk P, Stein S, Valaperti A, Germano D, Dirnhofer S et al. Heart-infiltrating prominin-1+/cd133+ progenitor cells represent the cellular source of transforming growth factor beta-mediated cardiac fibrosis in experimental autoimmune myocarditis. Circ Res. 2009;105: Fairweather D, Cihakova D. Alternatively activated macrophages in infection and autoimmunity. J Autoimmun. 2009;33: Gordon S, Martinez FO. Alternative activation of macrophages: mechanism and functions. Immunity. 2010;32: Li K, Xu W, Guo Q, Jiang Z, Wang P, Yue Y et al. Differential macrophage polarization in male and female BALB/c mice infected with coxsackievirus B3 defines susceptibility to viral myocarditis. Circ Res. 2009;105: Parissis J, Filippatos G, Adamopoulos S, Li X, Kremastinos DT, Uhal BD. Hematopoietic colony stimulating factors in cardiovascular and pulmonary remodeling: promoters or inhibitors? Curr Pharm Des. 2006;12: Hamilton JA. Colony-stimulating factors in inflammation and autoimmunity. Nat Rev Immunol. 2008;8: Wiktor-Jedrzejczak W, Gordon S. Cytokine regulation of the macrophage (M phi) system studied
18 using the colony stimulating factor-1-deficient op/op mouse. Physiol Rev. 1996;76: Naito M, Hayashi S, Yoshida H, Nishikawa S, Shultz LD, Takahashi K. Abnormal differentiation of tissue macrophage populations in 'osteopetrosis' (op) mice defective in the production of macrophage colony-stimulating factor. Am J Pathol. 1991;139: Yano T, Miura T, Whittaker P, Miki T, Sakamoto J, Nakamura Y et al. Macrophage colonystimulating factor treatment after myocardial infarction attenuates left ventricular dysfunction by accelerating infarct repair. J Am Coll Cardiol. 2006;47: Morimoto H, Takahashi M, Shiba Y, Izawa A, Ise H, Hongo M et al. Bone marrow-derived CXCR4+ cells mobilized by macrophage colony-stimulating factor participate in the reduction of infarct area and improvement of cardiac remodeling after myocardial infarction in mice. Am J Pathol. 2007;171: Hiraoka Y, Kishimoto C, Takada H, Suzaki N, Shiraki K. Colony-stimulating factors and coxackievirus B3 myocarditis in mice: macrophage colony-stimulating factor suppresses acute myocarditis with increasing interferon-alpha. Am Heart J. 1995;130: Blyszczuk P, Kania G, Dieterle T, Marty RR, Valaperti A, Berthonneche C et al. Myeloid differentiation factor-88/interleukin-1 signaling controls cardiac fibrosis and heart failure progression in inflammatory dilated cardiomyopathy. Circ Res. 2009;105: Wiktor-Jedrzejczak W, Ratajczak MZ, Ptasznik A, Sell KW, Ahmed-Ansari A, Ostertag W. CSF-1 deficiency in the op/op mouse has differential effects on macrophage populations and differentiation stages. Exp Hematol. 1992;20: Miki T, Miura T, Nishino Y, Yano T, Sakamoto J, Nakamura Y et al. Granulocyte colony stimulating factor/macrophage colony stimulating factor improves postinfarct ventricular function by suppression of border zone remodelling in rats. Clin Exp Pharmacol Physiol. 2004;31: Okazaki T, Ebihara S, Asada M, Yamanda S, Saijo Y, Shiraishi Y et al. Macrophage colonystimulating factor improves cardiac function after ischemic injury by inducing vascular endothelial growth factor production and survival of cardiomyocytes. Am J Pathol. 2007;171: Cihakova D, Barin JG, Afanasyeva M, Kimura M, Fairweather D, Berg M et al. Interleukin-13 protects against experimental autoimmune myocarditis by regulating macrophage differentiation.
19 18 Am J Pathol. 2008;172: Lowenstein CJ, Hill SL, Lafond-Walker A, Wu J, Allen G, Landavere M et al. Nitric oxide inhibits viral replication in murine myocarditis. J Clin Invest. 1996;97: Valaperti A, Marty RR, Kania G, Germano D, Mauermann N, Dirnhofer S et al. CD11b+ monocytes abrogate Th17 CD4+ T cell-mediated experimental autoimmune myocarditis. J Immunol. 2008;180: Zaragoza C, Ocampo C, Saura M, Leppo M, Wei XQ, Quick R et al. The role of inducible nitric oxide synthase in the host response to Coxsackievirus myocarditis. Proc Natl Acad Sci U S A. 1998;95: Hiraoka Y, Kishimoto C, Takada H, Nakamura M, Kurokawa M, Ochiai H et al. Nitric oxide and murine coxsackievirus B3 myocarditis: aggravation of myocarditis by inhibition of nitric oxide synthase. J Am Coll Cardiol. 1996;28: Kim SJ, Bang OS, Lee YS, Kang SS. Production of inducible nitric oxide is required for monocytic differentiation of U937 cells induced by vitamin E-succinate. J Cell Sci. 1998;111 ( Pt 4): Wink DA, Hines HB, Cheng RY, Switzer CH, Flores-Santana W, Vitek MP et al. Nitric oxide and redox mechanisms in the immune response. J Leukoc Biol. 2011;89: McCarthy RE, 3rd, Boehmer JP, Hruban RH, Hutchins GM, Kasper EK, Hare JM et al. Long-term outcome of fulminant myocarditis as compared with acute (nonfulminant) myocarditis. N Engl J Med. 2000;342:
20 Figure legends Figure 1. M-CSF prevents differentiation of heart-infiltrating CD133 + progenitors into myofibroblasts. (A,B) Heart-infiltrating CD133 + cells were expanded from myocarditis-positive hearts at day 21 of EAM and stimulated without (control, white) or with 10 ng/ml M-CSF (gray), or 10 ng/ml TGF-β (black) for 14 days. Relative mrna expression of myofibroblast-specific fibronectin (Fn1), collagen I (Col1a1) and αsma (Acta2) (A, n=5). Representative immunofluorescence and quantification analysis of αsma (top) and fibronectin (bottom) in cultured cells (B, n=5). (C,D) Expanded heart-infiltrating CD133 + cells (EAM d21) pre-treated for 3 days without (control, black) or with 10 ng/ml M-CSF (+M-CSF d-3, hatch), washed and stimulated with 10 ng/ml TGF-β for 14 days. Relative mrna levels of myofibroblast-specific genes (C, n=5) and representative immunofluorescence and quantification analysis of αsma (D, top) and fibronectin (D, bottom) are shown (n=5). *** p<0.001 (two-tailed Student s t-test versus control), bar = 20µm. Figure 2. M-CSF treatment turns inflammatory CD133 + progenitors into F4/80 + macrophages in EAM. BALB/c mice were immunized with αmyhc/cfa at day 0 and 7, and treated with PBS or M-CSF between days (A) Quantification of F4/80 + macrophages in the myocardium of PBS- (black) and M-CSF-treated (white) mice at day 24 (n=6), 28 (n=5) and 40 (n=20). Immunopositive cells were quantified per mm 2 of heart tissue. (B) Flow cytometry analysis of CD133 and F4/80 on heart infiltrating CD45 + -gated cells (left) in EAM. Quantification of CD133 + (left graph) and F4/80 + (right graph) cells gated on CD45 + infiltrates of PBS- (black) and M-CSF-treated (white) mice at day 24 (n=5) and 28 (n=5) of EAM. (C-G) Flow cytometry analysis of M1 and M2 activation markers on heart infiltrating CD45 + /F4/80 + -gated macrophages (left) in EAM. Mean fluorescence intensity (MFI) of membrane markers (CD16/32, CD206, CD301) and intracellular NOS2 expression gated on inflammatory macrophages of PBS- (black) and M- CSF-treated (white) mice at day 24 (n=10) of EAM. ( ) isotype controls, (+) antigen-specific antibodies.
21 20 (H) Overlay of phase contrast (left and middle) or F4/80 expression (right, red) with E.coli bacteria (green) taken up in the phagocytosis assay of expanded heart-infiltrating CD133 + cells (isolated from heart at d21) stimulated with M-CSF for 1 (left) and 3 days (middle and right). Bar = 20µm. ns p>0.05, * p<0.05, ** p<0.01, *** p<0.001 (two-tailed Student s t-test). Figure 3. M-CSF inhibits myofibroblast lineage differentiation of inflammatory CD133 + in EAM. (A) Representative flow cytometry analysis of CD133 + and F4/80 (right) gated on heart infiltrating CD45 + cells (left) at day 24 of EAM. Numbers indicate percentage of positive cells in the adjacent gates. (B) Heart-infiltrating CD45 + /CD133 + /F4/80 (white) and CD45 + /CD133 + /F4/80 hi (black) cells were FACS sorted from myocarditis-positive hearts at day 24 of EAM. Relative mrna levels of myofibroblast-specific genes are shown for 1 out of 2 independent experiments (n=5). (C) Representative flow cytometry analysis of CD133 and F4/80 gated on heart infiltrating CD45 + /CD133 + progenitor cells (left) of PBS- (+PBS) and M-CSF-treated (+M-CSF) mice at day 24 of EAM. Staining with anti-cd45 and anit-cd133 and IgG control to anti-f4/80 antibodies (IgG control) was used to set the gates. Numbers indicate percentage of positive cells in the adjacent gates. (D) Quantification of F4/80 hi (left) and F4/80 (right) cells gated of CD45 + /CD133 + progenitor cells (gated as shown in C) of PBS- (black) and M-CSF-treated (white) mice at day 24 of EAM. (E,F) Heart-infiltrating CD45 + /CD133 + cells were FACSorted from myocarditis-positive hearts at day 24 of EAM from control PBS-treated (black, +PBS) or M-CSF-treated (white, +M-CSF). A relative mrna level of myofibroblast-specific genes of sorted cells is shown (E, n=5). In addition, sorted cells were plated and stimulated with 10 ng/ml TGF-β for 10 days. Representative immunofluorescence and quantification analysis of αsma (F, top) and fibronectin (F, bottom) are shown (n=5). Bar = 20µm, ns p>0.05, * p<0.05, ** p<0.01, *** p<0.001 (two-tailed Student s t-test). Figure 4. NOS2 is required for M-CSF-dependent macrophage lineage differentiation from CD133 + progenitors. (A-E) Expanded heart-infiltrating CD133 + cells (EAM d21) from wild-type BALB/c and Nos2 / mice were stimulated with 10 ng/ml M-CSF for 3 days. (A) Representative flow cytometry analysis of expanded cells
22 using anti-cd133 (right) and IgG control (left) antibodies. Numbers indicate percentage of positive cells in the adjacent gates. Representative histogram analysis of macrophage specific antigens F4/80 (B), CD11b (C), CD14 (D), and E.coli bacteria taken up in the phagocytosis assay (E) on CD133 + cells (gated as shown in A). Isotype controls are displayed in grey. Numbers in histograms indicate mean fluorescence intensity (MFI). Bar graphs show quantification of the respective analyses for wild-type (black) and Nos2 / (hatch) cells. n=5, ( ) isotype controls, (+) antigen-specific antibodies or E.coli. (F) Expanded heart-infiltrating CD133 + cells (EAM d21) from BALB/c (wild-type) mice were stimulated with 10 ng/ml M-CSF for 3 days in the absence (control) or presence of 2mM L-NAME (+L-NAME). Representative histogram analysis of E.coli bacteria uptake by CD133 + cells (gated as shown in A). Controls without E.coli are displayed in grey. Numbers in histograms indicate MFI. Bar graphs show quantification of the respective analyses in the absence (white) or presence of L-NAME (grey). n=5, ( ) control, (+) E.coli (G) Nitrite levels in supernatants of cultures stimulated with 0.1 µg/ml LPS for 24h. n = 4 ns p>0.05, * p<0.05, ** p<0.01, *** p<0.001 (two-tailed Student s t-test). Figure 5. M-CSF treatment attenuates myocardial fibrosis and prevents heart failure in EAM. BALB/c mice were immunized at day 0 and 7 with αmyhc/cfa and injected either with PBS (black) or M-CSF between days (white) or days (grey). (A) Fibrosis was evaluated in heart sections at day 24 (n=10), 28 (n=10), 40 (n=20) and 60 (n=6-8). The degree of fibrosis was analysed by Masson s trichrome staining and calculated as percentage of the fibrotic area in heart sections. (B,C) The representative microphotographs of the myocardial tissue (d60) following PBS (B) or M-CSF (C) treatment between days stained with Masson s trichrome. Bar = 100 µm. p values were computed using two-tailed Student s t-test (A, d24, d28 and d40), one-way ANOVA (A, d60). (D-E) Quantification of CD45 + cells (defining all inflammatory infiltrates, D) and CD3 + cells (defining T lymphocytes, E) within the myocardium during EAM at day 24 (n=10), 28 (n=10), 40 (n=20) and 60 (n=6-8) after the first immunization. Immunopositive cells were quantified per mm 2 of heart tissue. (F) Echocardiographic parameters of healthy, untreated BALB/c mice (white) in comparison to
23 22 αmyhc/cfa-immunised mice with <2% myocardial fibrosis (hatch, n=9), >2% myocardial fibrosis (black, n=11) and αmyhc/cfa-immunised mice treated with M-CSF at days (grey, n=20). p values were computed using correlation analysis (F) and the one-way ANOVA (A,D,E). * p<0.05, ** p<0.01, *** p<0.001 for the respective group versus healthy controls (white) calculated with Bonferroni post-hoc test. Figure 6. M-CSF treatment fails to reduce fibrosis in Nos2 / mice. Nos2 / mice were immunized at day 0 and 7 with αmyhc/cfa and treated with PBS or M-CSF between days (A,B) Quantification of fibrosis and F4/80 + macrophages in the myocardium of PBS- (black) and M-CSFtreated (white) Nos2 / mice at day 24 (A, n=5) and 40 (B, n=10) of EAM. F4/80 + cells were quantified per mm 2 of heart tissue, and the degree of fibrosis was analysed by Masson s trichrome staining. (C) Representative histograms of CD133 expression gated on heart infiltrating CD45 + inflammatory cells (left) of PBS- (+PBS) and M-CSF-treated (+M-CSF) Nos2 / mice at day 24 of EAM. Isotype controls are displayed in grey. Numbers indicate percentage of positive cells in the presented histograms. Bar graphs show quantification of CD133 + and F4/80 + gated on CD45 + cells of PBS- (black) and M-CSF-treated (white) Nos2 / mice (n=5). (D) Flow cytometry analysis of M1 and M2 activation markers in EAM. Quantification of mean fluorescence intensity (MFI) of membrane macrophage activation markers gated on heart infiltrating CD45 + /F4/80 + -gated macrophages (left) of PBS- (grey) and M-CSF-treated (hatch) Nos2 / mice at day 24 of EAM (n=5). ( ) isotype controls, (+) antigen-specific antibodies, ns p>0.05 (two-tailed Student s t-test).
24 A! relative expression! 4! 2! Fn1! Col1a1! Acta2! ***! 4! ***! 4! ***! 2! 2! ***! control! +M-CSF! +TGF-β! B! control! +M-CSF! +TGF-β! αsma! Fibronectin! Fibronectin (%)! αsma (%)! ***! ***! C! +TGF-β! relative expression! 1.2! 0.8! 0.4! Fn1! Col1a1! Acta2! ***! ***! 1.2! 1.2! ***! 0.8! 0.8! 0.4! 0.4! control! +M-CSF d-3! D! +TGF-β! αsma! Fibronectin! control! +M-CSF d-3! Fibronectin (%)! αsma (%)! ***! ***! Blyszczuk et al., Figure 1!
25 A! F4/80 + cells/mm 2! p=0.001! p=0.04! p=0.37! d24! d28! d40! +PBS! +M-CSF! C! CD45! B! CD45! F4/ FSC! H! + M-CSF! CD133 +! (% of CD45 + )! 6 3 **! d24! d28! d24! d28! MFI! **! **! F4/80 +! (% of CD45 + )! D! E! cell count! control! +M-CSF! NOS2! 26.9! 8 NOS2!! +! cell count! F! G! cell count! control! +M-CSF! CD206! 35.7! 30.9! MFI! control! +M-CSF! ***! 518! 442! CD16/32! +PBS!!+M-CSF! 30 5! +!! +! CD301! E.coli! E.coli! F4/80/E.coli! d1! d3! d3! MFI! CD16/32! 60! +! CD206! CD !! 10 cell count! control! +M-CSF! 54.6! MFI! Blyszczuk et al., Figure 2!
26 A! CD45! C! FSC! CD133! Fn1! Col1a1! Acta2! 33! 9! ***! 8! 4! 40 ***! F4/8 IgG control! B! relative expression! F4/80! - F4/80 hi! 4! 2! 20 +PBS! +M-CSF! CD45! D! +M-CSF! +PBS! F4/80 hi (%)! CD133! ***! F4/80 (%)! CD133! 97! **! E! relative expression! CD133! IgG control! 2! 1! ! 1 1 7! 76! F4/ CD133! 10 0 F4/ Fn1! Col1a1! Acta2! 2! 2! **! **! 1! 1! +TGF-β! F! αsma! Fibronectin! +PBS! CD133 + cells! +M-CSF! CD133 + cells! Fibronectin (%)! αsma (%)! ***! ***! Blyszczuk et al., Figure 3!
27 A! IgG! B! cell count! D! cell count! F! IgG! WT! Nos2 /! WT! Nos2 /! 0.4! 63.9! FSC! 362! F4/8 CD14! ! ! FSC! ! 92! MFI! CD133! MFI! CD133! FSC! FSC! F4/80! ***!! +! CD14! *!! +! C! E! cell count! cell count! cell count! control! +L-NAME! WT! Nos2 /! WT! Nos2 /! E.coli! - wild-type +M-CSF! - Nos2 / +M-CSF! CD11b! E.coli! 393! 292! 25.2! 149! 104! 32! MFI! MFI! MFI! CD11b!! +! E.coli! E.coli!! +! ***!! +! G! nitrite (μm)! 3 ***! ***! M-CSF! - M-CSF +L-NAME! Blyszczuk et al., Figure 4!
28 A D! E! Fibrosis (%)! CD45 + cells/mm 2! CD3 + cells/mm 2! 15! 1 5! p<0.0001! p=0.003! p=0.0005! p=0.005! p=0.0002! p=0.97! p=0.0004! p=0.79! p=0.27! d24! d28! d40! p<0.0001! p=0.38! p=0.89! d60! B! C! +PBS! +M-CSF, d21-29! +PBS! +M-CSF, d21-29! +M-CSF, d40-48! F! FS%! LV Vol ; d (µl)! ! 5 25! -healthy! -MyHC/CFA, fibrosis-negative! -MyHC/CFA, fibrosis-positive! -MyHC/CFA,+M-CSF!! p=0.001! p=0.0001! 8 p=0.0002! 4! **! 6 **! 6 3! **! 4 2! 4 2 1! 2 EF%! p=0.03! p=0.004! p<0.0001! p=0.009! *! 16 *! 12! ***! 2 **! 12 8! ! LV mass (mg)! LVID, s (mm)! HW/Tibial length! LV Vol ; s (µl)! IVCT (ms)! p=0.003! *! Blyszczuk et al., Figure 5!
Supporting Information
 Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Supporting Information Desnues et al. 10.1073/pnas.1314121111 SI Materials and Methods Mice. Toll-like receptor (TLR)8 / and TLR9 / mice were generated as described previously (1, 2). TLR9 / mice were
Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD-
 Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Supplementary Methods Blocking antibodies and peptides. Rat anti-mouse PD-1 (29F.1A12, rat IgG2a, k), PD- L1 (10F.9G2, rat IgG2b, k), and PD-L2 (3.2, mouse IgG1) have been described (24). Anti-CTLA-4 (clone
Alternatively Activated Macrophages Determine the Repair of the Infarcted
 Alternatively Activated Macrophages Determine the Repair of the Infarcted Adult Murine Heart (Shiraishi et al.) List of Supplemental Materials Supplemental Methods Supplemental Figure 1. Cardiac CD206
Alternatively Activated Macrophages Determine the Repair of the Infarcted Adult Murine Heart (Shiraishi et al.) List of Supplemental Materials Supplemental Methods Supplemental Figure 1. Cardiac CD206
The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells
 1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
1 SUPPLEMENTARY INFORMATION The toll-like receptor 4 ligands Mrp8 and Mrp14 play a critical role in the development of autoreactive CD8 + T cells Karin Loser 1,2,6, Thomas Vogl 2,3, Maik Voskort 1, Aloys
Interferon γ regulates idiopathic pneumonia syndrome, a. Th17 + CD4 + T-cell-mediated GvH disease
 Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
Interferon γ regulates idiopathic pneumonia syndrome, a Th17 + CD4 + T-cell-mediated GvH disease Nora Mauermann, Julia Burian, Christophe von Garnier, Stefan Dirnhofer, Davide Germano, Christine Schuett,
MATERIALS AND METHODS. Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All
 MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
MATERIALS AND METHODS Antibodies (Abs), flow cytometry analysis and cell lines Neutralizing antibodies specific to mouse Dll1, Dll4, J1 and J2 were prepared as described. 1,2 All other antibodies used
Supplemental Table 1. Primer sequences for transcript analysis
 Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Supplemental Table 1. Primer sequences for transcript analysis Primer Sequence (5 3 ) Primer Sequence (5 3 ) Mmp2 Forward CCCGTGTGGCCCTC Mmp15 Forward CGGGGCTGGCT Reverse GCTCTCCCGGTTTC Reverse CCTGGTGTGCCTGCTC
Supplementary Figures
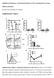 Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Inhibition of Pulmonary Anti Bacterial Defense by IFN γ During Recovery from Influenza Infection By Keer Sun and Dennis W. Metzger Supplementary Figures d a Ly6G Percentage survival f 1 75 5 1 25 1 5 1
Eosinophils are required. for the maintenance of plasma cells in the bone marrow
 Eosinophils are required for the maintenance of plasma cells in the bone marrow Van Trung Chu, Anja Fröhlich, Gudrun Steinhauser, Tobias Scheel, Toralf Roch, Simon Fillatreau, James J. Lee, Max Löhning
Eosinophils are required for the maintenance of plasma cells in the bone marrow Van Trung Chu, Anja Fröhlich, Gudrun Steinhauser, Tobias Scheel, Toralf Roch, Simon Fillatreau, James J. Lee, Max Löhning
c Ischemia (30 min) Reperfusion (8 w) Supplementary Figure bp 300 bp Ischemia (30 min) Reperfusion (4 h) Dox 20 mg/kg i.p.
 a Marker Ripk3 +/ 5 bp 3 bp b Ischemia (3 min) Reperfusion (4 h) d 2 mg/kg i.p. 1 w 5 w Sacrifice for IF size A subset for echocardiography and morphological analysis c Ischemia (3 min) Reperfusion (8
a Marker Ripk3 +/ 5 bp 3 bp b Ischemia (3 min) Reperfusion (4 h) d 2 mg/kg i.p. 1 w 5 w Sacrifice for IF size A subset for echocardiography and morphological analysis c Ischemia (3 min) Reperfusion (8
SUPPLEMENTARY METHODS
 SUPPLEMENTARY METHODS Histological analysis. Colonic tissues were collected from 5 parts of the middle colon on day 7 after the start of DSS treatment, and then were cut into segments, fixed with 4% paraformaldehyde,
SUPPLEMENTARY METHODS Histological analysis. Colonic tissues were collected from 5 parts of the middle colon on day 7 after the start of DSS treatment, and then were cut into segments, fixed with 4% paraformaldehyde,
Supplementary Figure 1. Characterization of basophils after reconstitution of SCID mice
 Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Supplementary figure legends Supplementary Figure 1. Characterization of after reconstitution of SCID mice with CD4 + CD62L + T cells. (A-C) SCID mice (n = 6 / group) were reconstituted with 2 x 1 6 CD4
Suppl Video: Tumor cells (green) and monocytes (white) are seeded on a confluent endothelial
 Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary Information Häuselmann et al. Monocyte induction of E-selectin-mediated endothelial activation releases VE-cadherin junctions to promote tumor cell extravasation in the metastasis cascade
Supplementary information. The proton-sensing G protein-coupled receptor T-cell death-associated gene 8
 1 Supplementary information 2 3 The proton-sensing G protein-coupled receptor T-cell death-associated gene 8 4 (TDAG8) shows cardioprotective effects against myocardial infarction 5 Akiomi Nagasaka 1+,
1 Supplementary information 2 3 The proton-sensing G protein-coupled receptor T-cell death-associated gene 8 4 (TDAG8) shows cardioprotective effects against myocardial infarction 5 Akiomi Nagasaka 1+,
Postn MCM Smad2 fl/fl Postn MCM Smad3 fl/fl Postn MCM Smad2/3 fl/fl. Postn MCM. Tgfbr1/2 fl/fl TAC
 A Smad2 fl/fl Smad3 fl/fl Smad2/3 fl/fl Tgfbr1/2 fl/fl 1. mm B Tcf21 MCM Tcf21 MCM Smad3 fl/fl Tcf21 MCM Smad2/3 fl/fl Tcf21 MCM Tgfbr1/2 fl/fl αmhc MCM C 1. mm 1. mm D Smad2 fl/fl Smad3 fl/fl Smad2/3
A Smad2 fl/fl Smad3 fl/fl Smad2/3 fl/fl Tgfbr1/2 fl/fl 1. mm B Tcf21 MCM Tcf21 MCM Smad3 fl/fl Tcf21 MCM Smad2/3 fl/fl Tcf21 MCM Tgfbr1/2 fl/fl αmhc MCM C 1. mm 1. mm D Smad2 fl/fl Smad3 fl/fl Smad2/3
Role of Tyk-2 in Th9 and Th17 cells in allergic asthma
 Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplementary File Role of Tyk-2 in Th9 and Th17 cells in allergic asthma Caroline Übel 1*, Anna Graser 1*, Sonja Koch 1, Ralf J. Rieker 2, Hans A. Lehr 3, Mathias Müller 4 and Susetta Finotto 1** 1 Laboratory
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured
 Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
Supplemental Figure 1. Signature gene expression in in vitro differentiated Th0, Th1, Th2, Th17 and Treg cells. (A) Naïve CD4 + T cells were cultured under Th0, Th1, Th2, Th17, and Treg conditions. mrna
Targeting tumour associated macrophages in anti-cancer therapies. Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018
 Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Targeting tumour associated macrophages in anti-cancer therapies Annamaria Gal Seminar Series on Drug Discovery Budapest 5 January 2018 Macrophages: Professional phagocytes of the myeloid lineage APC,
Pretargeting and Bioorthogonal Click Chemistry-Mediated Endogenous Stem Cell Homing for Heart Repair
 Pretargeting and Bioorthogonal Click Chemistry-Mediated Endogenous Stem Cell Homing for Heart Repair Mouse Model of Myocardial Infarction (MI) All animal work was compliant with the Institutional Animal
Pretargeting and Bioorthogonal Click Chemistry-Mediated Endogenous Stem Cell Homing for Heart Repair Mouse Model of Myocardial Infarction (MI) All animal work was compliant with the Institutional Animal
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
doi:10.1038/nature10134 Supplementary Figure 1. Anti-inflammatory activity of sfc. a, Autoantibody immune complexes crosslink activating Fc receptors, promoting activation of macrophages, and WWW.NATURE.COM/NATURE
Supplemental figure 1. PDGFRα is expressed dominantly by stromal cells surrounding mammary ducts and alveoli. A) IHC staining of PDGFRα in
 Supplemental figure 1. PDGFRα is expressed dominantly by stromal cells surrounding mammary ducts and alveoli. A) IHC staining of PDGFRα in nulliparous (left panel) and InvD6 mouse mammary glands (right
Supplemental figure 1. PDGFRα is expressed dominantly by stromal cells surrounding mammary ducts and alveoli. A) IHC staining of PDGFRα in nulliparous (left panel) and InvD6 mouse mammary glands (right
Supplementary Figure 1
 Supplementary Figure 1 a Percent of body weight! (%) 4! 3! 1! Epididymal fat Subcutaneous fat Liver SD Percent of body weight! (%) ** 3! 1! SD Percent of body weight! (%) 6! 4! SD ** b Blood glucose (mg/dl)!
Supplementary Figure 1 a Percent of body weight! (%) 4! 3! 1! Epididymal fat Subcutaneous fat Liver SD Percent of body weight! (%) ** 3! 1! SD Percent of body weight! (%) 6! 4! SD ** b Blood glucose (mg/dl)!
Cardiac myosin-th17 responses promote heart failure in human myocarditis
 Cardiac myosin-th17 responses promote heart failure in human myocarditis Jennifer M. Myers,, Carol J. Cox, Madeleine W. Cunningham JCI Insight. 2016;1(9):e85851. https://doi.org/10.1172/jci.insight.85851.
Cardiac myosin-th17 responses promote heart failure in human myocarditis Jennifer M. Myers,, Carol J. Cox, Madeleine W. Cunningham JCI Insight. 2016;1(9):e85851. https://doi.org/10.1172/jci.insight.85851.
Supplemental Information. T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism
 Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
Immunity, Volume 33 Supplemental Information T Cells Enhance Autoimmunity by Restraining Regulatory T Cell Responses via an Interleukin-23-Dependent Mechanism Franziska Petermann, Veit Rothhammer, Malte
Supplemental Materials for. Effects of sphingosine-1-phosphate receptor 1 phosphorylation in response to. FTY720 during neuroinflammation
 Supplemental Materials for Effects of sphingosine-1-phosphate receptor 1 phosphorylation in response to FTY7 during neuroinflammation This file includes: Supplemental Table 1. EAE clinical parameters of
Supplemental Materials for Effects of sphingosine-1-phosphate receptor 1 phosphorylation in response to FTY7 during neuroinflammation This file includes: Supplemental Table 1. EAE clinical parameters of
Supporting Information
 Supporting Information Idoyaga et al. 10.1073/pnas.0812247106 SSC a) Single cell suspension 99 Aqua b) Live cells 96 -W c) Singlets 92 -A CD19+ER119 d) CD19 ER119 cells 97 CD3 e) CD3 cells 27 f) DX5 cells
Supporting Information Idoyaga et al. 10.1073/pnas.0812247106 SSC a) Single cell suspension 99 Aqua b) Live cells 96 -W c) Singlets 92 -A CD19+ER119 d) CD19 ER119 cells 97 CD3 e) CD3 cells 27 f) DX5 cells
Supplemental Figure 1
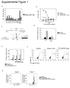 Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
Supplemental Figure 1 1a 1c PD-1 MFI fold change 6 5 4 3 2 1 IL-1α IL-2 IL-4 IL-6 IL-1 IL-12 IL-13 IL-15 IL-17 IL-18 IL-21 IL-23 IFN-α Mut Human PD-1 promoter SBE-D 5 -GTCTG- -1.2kb SBE-P -CAGAC- -1.kb
Supplementary Materials for
 www.sciencetranslationalmedicine.org/cgi/content/full/8/352/352ra110/dc1 Supplementary Materials for Spatially selective depletion of tumor-associated regulatory T cells with near-infrared photoimmunotherapy
www.sciencetranslationalmedicine.org/cgi/content/full/8/352/352ra110/dc1 Supplementary Materials for Spatially selective depletion of tumor-associated regulatory T cells with near-infrared photoimmunotherapy
Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer
 Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
Supplementary Information Combined Rho-kinase inhibition and immunogenic cell death triggers and propagates immunity against cancer Gi-Hoon Nam, Eun-Jung Lee, Yoon Kyoung Kim, Yeonsun Hong, Yoonjeong Choi,
Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice
 Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
Supplementary Methods: Cell isolation. Spleen and lymph nodes (axillary, inguinal) were removed from mice and gently meshed in DMEM containing 10% FBS to prepare for single cell suspensions. CD4 + CD25
SUPPLEMENTARY INFORMATION
 doi:10.1038/nature10188 Supplementary Figure 1. Embryonic epicardial genes are down-regulated from midgestation stages and barely detectable post-natally. Real time qrt-pcr revealed a significant down-regulation
doi:10.1038/nature10188 Supplementary Figure 1. Embryonic epicardial genes are down-regulated from midgestation stages and barely detectable post-natally. Real time qrt-pcr revealed a significant down-regulation
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs
 Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
Supplementary Fig. 1 p38 MAPK negatively regulates DC differentiation. (a) Western blot analysis of p38 isoform expression in BM cells, immature DCs (idcs) and mature DCs (mdcs). A myeloma cell line expressing
sequences of a styx mutant reveals a T to A transversion in the donor splice site of intron 5
 sfigure 1 Styx mutant mice recapitulate the phenotype of SHIP -/- mice. (A) Analysis of the genomic sequences of a styx mutant reveals a T to A transversion in the donor splice site of intron 5 (GTAAC
sfigure 1 Styx mutant mice recapitulate the phenotype of SHIP -/- mice. (A) Analysis of the genomic sequences of a styx mutant reveals a T to A transversion in the donor splice site of intron 5 (GTAAC
Supplementary Information. Tissue-wide immunity against Leishmania. through collective production of nitric oxide
 Supplementary Information Tissue-wide immunity against Leishmania through collective production of nitric oxide Romain Olekhnovitch, Bernhard Ryffel, Andreas J. Müller and Philippe Bousso Supplementary
Supplementary Information Tissue-wide immunity against Leishmania through collective production of nitric oxide Romain Olekhnovitch, Bernhard Ryffel, Andreas J. Müller and Philippe Bousso Supplementary
Cardiac myosin-th17 responses promote heart failure in human myocarditis
 Cardiac myosin-th17 responses promote heart failure in human myocarditis Jennifer M. Myers, 1 Leslie T. Cooper, 2 David C. Kem, 3 Stavros Stavrakis, 4 Stanley D. Kosanke, 5 Ethan M. Shevach, 6 DeLisa Fairweather,
Cardiac myosin-th17 responses promote heart failure in human myocarditis Jennifer M. Myers, 1 Leslie T. Cooper, 2 David C. Kem, 3 Stavros Stavrakis, 4 Stanley D. Kosanke, 5 Ethan M. Shevach, 6 DeLisa Fairweather,
Intracellular MHC class II molecules promote TLR-triggered innate. immune responses by maintaining Btk activation
 Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
Intracellular MHC class II molecules promote TLR-triggered innate immune responses by maintaining Btk activation Xingguang Liu, Zhenzhen Zhan, Dong Li, Li Xu, Feng Ma, Peng Zhang, Hangping Yao and Xuetao
hemodynamic stress. A. Echocardiographic quantification of cardiac dimensions and function in
 SUPPLEMENTAL FIGURE LEGENDS Supplemental Figure 1. Fbn1 C1039G/+ hearts display normal cardiac function in the absence of hemodynamic stress. A. Echocardiographic quantification of cardiac dimensions and
SUPPLEMENTAL FIGURE LEGENDS Supplemental Figure 1. Fbn1 C1039G/+ hearts display normal cardiac function in the absence of hemodynamic stress. A. Echocardiographic quantification of cardiac dimensions and
B6/COLODR/SPL/11C/83/LAP/#2.006 B6/COLODR/SPL/11C/86/LAP/#2.016 CD11C B6/COLODR/SPL/11C/80/LAP/#2.011 CD11C
 CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
CD3-specific antibody-induced immune tolerance and suppression of autoimmune encephalomyelitis involves TGF-β production through phagocytes digesting apoptotic T cells Sylvain Perruche 1,3, Pin Zhang 1,
effect on the upregulation of these cell surface markers. The mean peak fluorescence intensity
 SUPPLEMENTARY FIGURE 1 Supplementary Figure 1 ASIC1 disruption or blockade does not effect in vitro and in vivo antigen-presenting cell activation. (a) Flow cytometric analysis of cell surface molecules
SUPPLEMENTARY FIGURE 1 Supplementary Figure 1 ASIC1 disruption or blockade does not effect in vitro and in vivo antigen-presenting cell activation. (a) Flow cytometric analysis of cell surface molecules
Supporting Information. Calculation of the relative contributions of myocyte proliferation, stem cell. Supporting Information Fig 1 (page 9)
 Supporting Information Table of contents Calculation of the relative contributions of myocyte proliferation, stem cell differentiation and cardioprotection (page 2) Supporting Information Fig 1 (page 9)
Supporting Information Table of contents Calculation of the relative contributions of myocyte proliferation, stem cell differentiation and cardioprotection (page 2) Supporting Information Fig 1 (page 9)
Supporting Online Material for
 www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
www.sciencemag.org/cgi/content/full/1175194/dc1 Supporting Online Material for A Vital Role for Interleukin-21 in the Control of a Chronic Viral Infection John S. Yi, Ming Du, Allan J. Zajac* *To whom
Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice
 Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice (a) CD11c.DOG transgenic mice (tg) were treated with 8 ng/g body weight (b.w.) diphtheria toxin (DT) i.p. on day -1 and every
Supplementary Figure 1. Efficient DC depletion in CD11c.DOG transgenic mice (a) CD11c.DOG transgenic mice (tg) were treated with 8 ng/g body weight (b.w.) diphtheria toxin (DT) i.p. on day -1 and every
% of live splenocytes. STAT5 deletion. (open shapes) % ROSA + % floxed
 Supp. Figure 1. a 14 1 1 8 6 spleen cells (x1 6 ) 16 % of live splenocytes 5 4 3 1 % of live splenocytes 8 6 4 b 1 1 c % of CD11c + splenocytes (closed shapes) 8 6 4 8 6 4 % ROSA + (open shapes) % floxed
Supp. Figure 1. a 14 1 1 8 6 spleen cells (x1 6 ) 16 % of live splenocytes 5 4 3 1 % of live splenocytes 8 6 4 b 1 1 c % of CD11c + splenocytes (closed shapes) 8 6 4 8 6 4 % ROSA + (open shapes) % floxed
D CD8 T cell number (x10 6 )
 IFNγ Supplemental Figure 1. CD T cell number (x1 6 ) 18 15 1 9 6 3 CD CD T cells CD6L C CD5 CD T cells CD6L D CD8 T cell number (x1 6 ) 1 8 6 E CD CD8 T cells CD6L F Log(1)CFU/g Feces 1 8 6 p
IFNγ Supplemental Figure 1. CD T cell number (x1 6 ) 18 15 1 9 6 3 CD CD T cells CD6L C CD5 CD T cells CD6L D CD8 T cell number (x1 6 ) 1 8 6 E CD CD8 T cells CD6L F Log(1)CFU/g Feces 1 8 6 p
Trim29 gene-targeting strategy. (a) Genotyping of wildtype mice (+/+), Trim29 heterozygous mice (+/ ) and homozygous mice ( / ).
 Supplementary Figure 1 Trim29 gene-targeting strategy. (a) Genotyping of wildtype mice (+/+), Trim29 heterozygous mice (+/ ) and homozygous mice ( / ). (b) Immunoblot analysis of TRIM29 in lung primary
Supplementary Figure 1 Trim29 gene-targeting strategy. (a) Genotyping of wildtype mice (+/+), Trim29 heterozygous mice (+/ ) and homozygous mice ( / ). (b) Immunoblot analysis of TRIM29 in lung primary
SUPPLEMENTARY INFORMATION
 1. Supplementary Figures and Legends Supplementary Fig. 1. S1P-mediated transcriptional regulation of integrins expressed in OP/monocytoid cells. Real-time quantitative PCR analyses of mrna for two integrins,
1. Supplementary Figures and Legends Supplementary Fig. 1. S1P-mediated transcriptional regulation of integrins expressed in OP/monocytoid cells. Real-time quantitative PCR analyses of mrna for two integrins,
SUPPLEMENTARY MATERIALS. IL-4 as a Repurposed Biological Drug for Myocardial Infarction through. Augmentation of Reparative Cardiac Macrophages:
 1 SUPPLEMENTARY MATERIALS IL-4 as a Repurposed Biological Drug for Myocardial Infarction through Augmentation of Reparative Cardiac Macrophages: Proof-of-Concept Data in Mice Yusuke Shintani MD PhD, Tomoya
1 SUPPLEMENTARY MATERIALS IL-4 as a Repurposed Biological Drug for Myocardial Infarction through Augmentation of Reparative Cardiac Macrophages: Proof-of-Concept Data in Mice Yusuke Shintani MD PhD, Tomoya
Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained
 1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
1 2 3 4 5 6 7 8 9 10 11 Supplementary Figure 1. H-PGDS deficiency does not affect GI tract functions and anaphylactic reaction. (a) Representative pictures of H&E-stained jejunum sections ( 200 magnification;
Supplementary Materials for
 immunology.sciencemag.org/cgi/content/full/2/16/eaan6049/dc1 Supplementary Materials for Enzymatic synthesis of core 2 O-glycans governs the tissue-trafficking potential of memory CD8 + T cells Jossef
immunology.sciencemag.org/cgi/content/full/2/16/eaan6049/dc1 Supplementary Materials for Enzymatic synthesis of core 2 O-glycans governs the tissue-trafficking potential of memory CD8 + T cells Jossef
International Graduate Research Programme in Cardiovascular Science
 1 International Graduate Research Programme in Cardiovascular Science This work has been supported by the European Community s Sixth Framework Programme under grant agreement n LSHM-CT-2005-01883 EUGeneHeart.
1 International Graduate Research Programme in Cardiovascular Science This work has been supported by the European Community s Sixth Framework Programme under grant agreement n LSHM-CT-2005-01883 EUGeneHeart.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and
 Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Supplementary Figure S1. Flow cytometric analysis of the expression of Thy1 in NH cells. Flow cytometric analysis of the expression of T1/ST2 and Thy1 in NH cells derived from the lungs of naïve mice.
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Cover Page The handle http://hdl.handle.net/1887/23854 holds various files of this Leiden University dissertation. Author: Marel, Sander van der Title: Gene and cell therapy based treatment strategies
Nature Immunology: doi: /ni Supplementary Figure 1. Huwe1 has high expression in HSCs and is necessary for quiescence.
 Supplementary Figure 1 Huwe1 has high expression in HSCs and is necessary for quiescence. (a) Heat map visualizing expression of genes with a known function in ubiquitin-mediated proteolysis (KEGG: Ubiquitin
Supplementary Figure 1 Huwe1 has high expression in HSCs and is necessary for quiescence. (a) Heat map visualizing expression of genes with a known function in ubiquitin-mediated proteolysis (KEGG: Ubiquitin
Serum cytokine levels in control and tumor-bearing male and female mice at day 15.
 Supplementary Table 1. Serum cytokine levels in control and tumor-bearing male and female mice at day 15. Male Female Cytokine Control C-26 Control C-26 IL-1β 2.0 ± 0.8 9.6 ± 1.5* 1.8 ± 0.2 6.8 ± 1.4*
Supplementary Table 1. Serum cytokine levels in control and tumor-bearing male and female mice at day 15. Male Female Cytokine Control C-26 Control C-26 IL-1β 2.0 ± 0.8 9.6 ± 1.5* 1.8 ± 0.2 6.8 ± 1.4*
Role of Inflammatory and Progenitor Cells in Pulmonary Vascular Remodeling: Potential Role for Targeted Therapies. Traditional Hypothesis Stress
 3/1/212 Role of Inflammatory and Progenitor Cells in Pulmonary Vascular Remodeling: Potential Role for Targeted Therapies K.R. Stenmark University of Colorado Denver, CO 845 Prominent Fibroproliferative
3/1/212 Role of Inflammatory and Progenitor Cells in Pulmonary Vascular Remodeling: Potential Role for Targeted Therapies K.R. Stenmark University of Colorado Denver, CO 845 Prominent Fibroproliferative
Inflammatory dilated cardiomyopathy refers to an end-stage. Heart Failure
 Heart Failure Innate Signaling Promotes Formation of Regulatory Nitric Oxide Producing Dendritic Cells Limiting T-Cell Expansion in Experimental Autoimmune Myocarditis Gabriela Kania, PhD; Stefanie Siegert,
Heart Failure Innate Signaling Promotes Formation of Regulatory Nitric Oxide Producing Dendritic Cells Limiting T-Cell Expansion in Experimental Autoimmune Myocarditis Gabriela Kania, PhD; Stefanie Siegert,
The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF
 CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
CORRECTION NOTICE Nat.Immunol. 12, 568 575 (2011) The encephalitogenicity of TH17 cells is dependent on IL-1- and IL-23- induced production of the cytokine GM-CSF Mohamed El-Behi, Bogoljub Ciric, Hong
well for 2 h at rt. Each dot represents an individual mouse and bar is the mean ±
 Supplementary data: Control DC Blimp-1 ko DC 8 6 4 2-2 IL-1β p=.5 medium 8 6 4 2 IL-2 Medium p=.16 8 6 4 2 IL-6 medium p=.3 5 4 3 2 1-1 medium IL-1 n.s. 25 2 15 1 5 IL-12(p7) p=.15 5 IFNγ p=.65 4 3 2 1
Supplementary data: Control DC Blimp-1 ko DC 8 6 4 2-2 IL-1β p=.5 medium 8 6 4 2 IL-2 Medium p=.16 8 6 4 2 IL-6 medium p=.3 5 4 3 2 1-1 medium IL-1 n.s. 25 2 15 1 5 IL-12(p7) p=.15 5 IFNγ p=.65 4 3 2 1
VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization
 Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
Cell Reports, Volume 9 Supplemental Information VEGFR2-Mediated Vascular Dilation as a Mechanism of VEGF-Induced Anemia and Bone Marrow Cell Mobilization Sharon Lim, Yin Zhang, Danfang Zhang, Fang Chen,
Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder I Nakaya, Kousik
 SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
SUPPLEMENTARY FIGURES 1-19 T H 2 response to cysteine-proteases requires dendritic cell-basophil cooperation via ROS mediated signaling Hua Tang, Weiping Cao, Sudhir Pai Kasturi, Rajesh Ravindran, Helder
NK cell flow cytometric assay In vivo DC viability and migration assay
 NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
NK cell flow cytometric assay 6 NK cells were purified, by negative selection with the NK Cell Isolation Kit (Miltenyi iotec), from spleen and lymph nodes of 6 RAG1KO mice, injected the day before with
Supplementary Figure 1.
 Supplementary Figure 1. Female Pro-ins2 -/- mice at 5-6 weeks of age were either inoculated i.p. with a single dose of CVB4 (1x10 5 PFU/mouse) or PBS and treated with αgalcer or control vehicle. On day
Supplementary Figure 1. Female Pro-ins2 -/- mice at 5-6 weeks of age were either inoculated i.p. with a single dose of CVB4 (1x10 5 PFU/mouse) or PBS and treated with αgalcer or control vehicle. On day
Online supplement. Phenotypic, functional and plasticity features of classical and alternatively activated
 Online supplement Phenotypic, functional and plasticity features of classical and alternatively activated human macrophages Abdullah Al Tarique*, Jayden Logan *, Emma Thomas *, Patrick G Holt *, Peter
Online supplement Phenotypic, functional and plasticity features of classical and alternatively activated human macrophages Abdullah Al Tarique*, Jayden Logan *, Emma Thomas *, Patrick G Holt *, Peter
Supplemental Table I.
 Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
Supplemental Table I Male / Mean ± SEM n Mean ± SEM n Body weight, g 29.2±0.4 17 29.7±0.5 17 Total cholesterol, mg/dl 534.0±30.8 17 561.6±26.1 17 HDL-cholesterol, mg/dl 9.6±0.8 17 10.1±0.7 17 Triglycerides,
CD14 + S100A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer
 CD14 + S1A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer Po-Hao, Feng M.D., Kang-Yun, Lee, M.D. Ph.D., Ya-Ling Chang, Yao-Fei Chan, Lu- Wei, Kuo,Ting-Yu
CD14 + S1A9 + Monocytic Myeloid-Derived Suppressor Cells and Their Clinical Relevance in Non-Small Cell Lung Cancer Po-Hao, Feng M.D., Kang-Yun, Lee, M.D. Ph.D., Ya-Ling Chang, Yao-Fei Chan, Lu- Wei, Kuo,Ting-Yu
Supplemental Information. Tissue Myeloid Progenitors Differentiate. into Pericytes through TGF-b Signaling. in Developing Skin Vasculature
 Cell Reports, Volume 18 Supplemental Information Tissue Myeloid Progenitors Differentiate into Pericytes through TGF-b Signaling in Developing Skin Vasculature Tomoko Yamazaki, Ani Nalbandian, Yutaka Uchida,
Cell Reports, Volume 18 Supplemental Information Tissue Myeloid Progenitors Differentiate into Pericytes through TGF-b Signaling in Developing Skin Vasculature Tomoko Yamazaki, Ani Nalbandian, Yutaka Uchida,
Nature Medicine: doi: /nm.3922
 Title: Glucocorticoid-induced tumor necrosis factor receptor-related protein co-stimulation facilitates tumor regression by inducing IL-9-producing helper T cells Authors: Il-Kyu Kim, Byung-Seok Kim, Choong-Hyun
Title: Glucocorticoid-induced tumor necrosis factor receptor-related protein co-stimulation facilitates tumor regression by inducing IL-9-producing helper T cells Authors: Il-Kyu Kim, Byung-Seok Kim, Choong-Hyun
Canberra, Australia). CD11c-DTR-OVA-GFP (B6.CD11c-OVA), B6.luc + and. Cancer Research Center, Germany). B6 or BALB/c.FoxP3-DTR-GFP mice were
 Supplemental Materials and Methods Mice Female C57BL/6 (B6, I-E null, H-2 b ), BALB/c (H-2 d ) + ), FVB/N (H-2 q, I-E null, CD45.1 + ), and B6D2F1 (H-2 b/d ) mice were purchased from the Animal Resources
Supplemental Materials and Methods Mice Female C57BL/6 (B6, I-E null, H-2 b ), BALB/c (H-2 d ) + ), FVB/N (H-2 q, I-E null, CD45.1 + ), and B6D2F1 (H-2 b/d ) mice were purchased from the Animal Resources
FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH
 FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH ALETA A SOURCE OF 1,3-BETA GLUCANS Aleta is highly bioavailable, offering a concentration greater than 5% of 1,3-beta glucans. Aleta provides a consistent response
FOR OPTIMAL GUT HEALTH KEMIN.COM/GUTHEALTH ALETA A SOURCE OF 1,3-BETA GLUCANS Aleta is highly bioavailable, offering a concentration greater than 5% of 1,3-beta glucans. Aleta provides a consistent response
Fig 1 CD163. CD11b S100A9. Sirius Red. 100μm ** ** CD163. CD11b S100A9 ** Sirius Red (PL) Sirius Red SUM Mo.
 T47D T47D + o SU-59 Fig SU-59 + o IHC score (-3) IHC score (-2) CD63 3 2 IHC score (-3) CD63 3 ** 2 CDb CDb * * SA9 SA9 ** * 2 IHC score (-4) αsa αsa 4 ** ** 2 Sirius Red μm IHC score (%) Sirius Red 8
T47D T47D + o SU-59 Fig SU-59 + o IHC score (-3) IHC score (-2) CD63 3 2 IHC score (-3) CD63 3 ** 2 CDb CDb * * SA9 SA9 ** * 2 IHC score (-4) αsa αsa 4 ** ** 2 Sirius Red μm IHC score (%) Sirius Red 8
Chronic variable stress activates hematopoietic stem cells
 SUPPLEMENTARY INFORMATION Chronic variable stress activates hematopoietic stem cells Timo Heidt *, Hendrik B. Sager *, Gabriel Courties, Partha Dutta, Yoshiko Iwamoto, Alex Zaltsman, Constantin von zur
SUPPLEMENTARY INFORMATION Chronic variable stress activates hematopoietic stem cells Timo Heidt *, Hendrik B. Sager *, Gabriel Courties, Partha Dutta, Yoshiko Iwamoto, Alex Zaltsman, Constantin von zur
Supplementary Figure S1. PTPN2 levels are not altered in proliferating CD8+ T cells. Lymph node (LN) CD8+ T cells from C57BL/6 mice were stained with
 Supplementary Figure S1. PTPN2 levels are not altered in proliferating CD8+ T cells. Lymph node (LN) CD8+ T cells from C57BL/6 mice were stained with CFSE and stimulated with plate-bound α-cd3ε (10µg/ml)
Supplementary Figure S1. PTPN2 levels are not altered in proliferating CD8+ T cells. Lymph node (LN) CD8+ T cells from C57BL/6 mice were stained with CFSE and stimulated with plate-bound α-cd3ε (10µg/ml)
Supplementary Data Table of Contents:
 Supplementary Data Table of Contents: - Supplementary Methods - Supplementary Figures S1(A-B) - Supplementary Figures S2 (A-B) - Supplementary Figures S3 - Supplementary Figures S4(A-B) - Supplementary
Supplementary Data Table of Contents: - Supplementary Methods - Supplementary Figures S1(A-B) - Supplementary Figures S2 (A-B) - Supplementary Figures S3 - Supplementary Figures S4(A-B) - Supplementary
Supplementary Figure 1. mrna expression of chitinase and chitinase-like protein in splenic immune cells. Each splenic immune cell population was
 Supplementary Figure 1. mrna expression of chitinase and chitinase-like protein in splenic immune cells. Each splenic immune cell population was sorted by FACS. Surface markers for sorting were CD11c +
Supplementary Figure 1. mrna expression of chitinase and chitinase-like protein in splenic immune cells. Each splenic immune cell population was sorted by FACS. Surface markers for sorting were CD11c +
SUPPLEMENTARY INFORMATION
 doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
doi:1.138/nature1554 a TNF-α + in CD4 + cells [%] 1 GF SPF 6 b IL-1 + in CD4 + cells [%] 5 4 3 2 1 Supplementary Figure 1. Effect of microbiota on cytokine profiles of T cells in GALT. Frequencies of TNF-α
Supplementary Figure 1 Chemokine and chemokine receptor expression during muscle regeneration (a) Analysis of CR3CR1 mrna expression by real time-pcr
 Supplementary Figure 1 Chemokine and chemokine receptor expression during muscle regeneration (a) Analysis of CR3CR1 mrna expression by real time-pcr at day 0, 1, 4, 10 and 21 post- muscle injury. (b)
Supplementary Figure 1 Chemokine and chemokine receptor expression during muscle regeneration (a) Analysis of CR3CR1 mrna expression by real time-pcr at day 0, 1, 4, 10 and 21 post- muscle injury. (b)
Nature Medicine: doi: /nm.2109
 HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
HIV 1 Infects Multipotent Progenitor Cells Causing Cell Death and Establishing Latent Cellular Reservoirs Christoph C. Carter, Adewunmi Onafuwa Nuga, Lucy A. M c Namara, James Riddell IV, Dale Bixby, Michael
Uncovering the mechanisms of wound healing and fibrosis
 Any Questions??? Ask now or contact support support@sabiosciences.com 1-888-503-3187 International customers: SABio@Qiagen.com Uncovering the mechanisms of wound healing and fibrosis Webinar related questions:
Any Questions??? Ask now or contact support support@sabiosciences.com 1-888-503-3187 International customers: SABio@Qiagen.com Uncovering the mechanisms of wound healing and fibrosis Webinar related questions:
Gene expression was analyzed by real time PCR (SYBR GREEN PCR Master. Mix, Roche Applied Science) using specific oligonucleotides.
 1 SUPPLEMENTAL MATERIAL SUPPLEMENT METHODS Real Time PCR. Gene expression was analyzed by real time PCR (SYBR GREEN PCR Master Mix, Roche Applied Science) using specific oligonucleotides. Rat ST2L forward
1 SUPPLEMENTAL MATERIAL SUPPLEMENT METHODS Real Time PCR. Gene expression was analyzed by real time PCR (SYBR GREEN PCR Master Mix, Roche Applied Science) using specific oligonucleotides. Rat ST2L forward
BMDCs were generated in vitro from bone marrow cells cultured in 10 % RPMI supplemented
 Supplemental Materials Figure S1. Cultured BMDCs express CD11c BMDCs were generated in vitro from bone marrow cells cultured in 10 % RPMI supplemented with 15 ng/ml GM-CSF. Media was changed and fresh
Supplemental Materials Figure S1. Cultured BMDCs express CD11c BMDCs were generated in vitro from bone marrow cells cultured in 10 % RPMI supplemented with 15 ng/ml GM-CSF. Media was changed and fresh
An epithelial-to-mesenchymal transition-inducing potential of. granulocyte macrophage colony-stimulating factor in colon. cancer
 An epithelial-to-mesenchymal transition-inducing potential of granulocyte macrophage colony-stimulating factor in colon cancer Yaqiong Chen, Zhi Zhao, Yu Chen, Zhonglin Lv, Xin Ding, Renxi Wang, He Xiao,
An epithelial-to-mesenchymal transition-inducing potential of granulocyte macrophage colony-stimulating factor in colon cancer Yaqiong Chen, Zhi Zhao, Yu Chen, Zhonglin Lv, Xin Ding, Renxi Wang, He Xiao,
Evaluation of directed and random motility in microslides Assessment of leukocyte adhesion in flow chambers
 Evaluation of directed and random motility in microslides Motility experiments in IBIDI microslides, image acquisition and processing were performed as described. PMN, which ended up in an angle < 180
Evaluation of directed and random motility in microslides Motility experiments in IBIDI microslides, image acquisition and processing were performed as described. PMN, which ended up in an angle < 180
Detailed step-by-step operating procedures for NK cell and CTL degranulation assays
 Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Supplemental methods Detailed step-by-step operating procedures for NK cell and CTL degranulation assays Materials PBMC isolated from patients, relatives and healthy donors as control K562 cells (ATCC,
Supplementary Figure 1. HOPX is hypermethylated in NPC. (a) Methylation levels of HOPX in Normal (n = 24) and NPC (n = 24) tissues from the
 Supplementary Figure 1. HOPX is hypermethylated in NPC. (a) Methylation levels of HOPX in Normal (n = 24) and NPC (n = 24) tissues from the genome-wide methylation microarray data. Mean ± s.d.; Student
Supplementary Figure 1. HOPX is hypermethylated in NPC. (a) Methylation levels of HOPX in Normal (n = 24) and NPC (n = 24) tissues from the genome-wide methylation microarray data. Mean ± s.d.; Student
Role of Inflammation in Pulmonary Hypertension
 Role of Inflammation in Pulmonary Hypertension K. R. Stenmark University of Colorado Denver, USA Prominent Fibroproliferative Changes are Observed in the Lung Vasculature of Infants With Pulmonary Arterial
Role of Inflammation in Pulmonary Hypertension K. R. Stenmark University of Colorado Denver, USA Prominent Fibroproliferative Changes are Observed in the Lung Vasculature of Infants With Pulmonary Arterial
C57BL/6 Mice are More Appropriate. than BALB/C Mice in Inducing Dilated Cardiomyopathy with Short-Term Doxorubicin Treatment
 Original Article C57BL/6 Mice are More Appropriate Acta Cardiol Sin 2012;28:236 240 Heart Failure & Cardiomyopathy C57BL/6 Mice are More Appropriate than BALB/C Mice in Inducing Dilated Cardiomyopathy
Original Article C57BL/6 Mice are More Appropriate Acta Cardiol Sin 2012;28:236 240 Heart Failure & Cardiomyopathy C57BL/6 Mice are More Appropriate than BALB/C Mice in Inducing Dilated Cardiomyopathy
Supplementary Figure 1. Expression of CUGBP1 in non-parenchymal liver cells treated with TGF-β
 Supplementary Figures Supplementary Figure 1. Expression of CUGBP1 in non-parenchymal liver cells treated with TGF-β and LPS. Non-parenchymal liver cells were isolated and treated with or without TGF-β
Supplementary Figures Supplementary Figure 1. Expression of CUGBP1 in non-parenchymal liver cells treated with TGF-β and LPS. Non-parenchymal liver cells were isolated and treated with or without TGF-β
Liver-Resident Macrophage Necroptosis Orchestrates Type 1 Microbicidal Inflammation and Type-2- Mediated Tissue Repair during Bacterial Infection
 Liver-Resident Macrophage Necroptosis Orchestrates Type 1 Microbicidal Inflammation and Type-2- Mediated Tissue Repair during Bacterial Infection Camille Blériot, Théo Dupuis, Grégory Jouvion, Gérard Eberl,
Liver-Resident Macrophage Necroptosis Orchestrates Type 1 Microbicidal Inflammation and Type-2- Mediated Tissue Repair during Bacterial Infection Camille Blériot, Théo Dupuis, Grégory Jouvion, Gérard Eberl,
Supplementary Information:
 Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supplementary Information: Follicular regulatory T cells with Bcl6 expression suppress germinal center reactions by Yeonseok Chung, Shinya Tanaka, Fuliang Chu, Roza Nurieva, Gustavo J. Martinez, Seema
Supplemental Information. CD4 + CD25 + Foxp3 + Regulatory T Cells Promote. Th17 Cells In Vitro and Enhance Host Resistance
 Immunity, Volume 34 Supplemental Information D4 + D25 + + Regulatory T ells Promote Th17 ells In Vitro and Enhance Host Resistance in Mouse andida albicans Th17 ell Infection Model Pushpa Pandiyan, Heather
Immunity, Volume 34 Supplemental Information D4 + D25 + + Regulatory T ells Promote Th17 ells In Vitro and Enhance Host Resistance in Mouse andida albicans Th17 ell Infection Model Pushpa Pandiyan, Heather
CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads (Miltenyi Biotec) for depletion of CD25 +
 Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
Supplements Supplemental Materials and Methods Depletion of CD25 + T-cells from PBMC. Fresh or HD precultured PBMC were stained with the conjugate CD25-PE (BD Biosciences) and labeled with anti-pe-microbeads
CYTOKINES. Based on: Cellular and Molecular Immunology, 4 th ed.,abbas A.K., Lichtman A.H. and Pober J.S. Sounders company; Philadelphia, 2010.
 CYTOKINES Based on: Cellular and Molecular Immunology, 4 th ed.,abbas A.K., Lichtman A.H. and Pober J.S. Sounders company; Philadelphia, 2010. 1 What are cytokines? Glycoproteins (15 25 kda): Interleukins
CYTOKINES Based on: Cellular and Molecular Immunology, 4 th ed.,abbas A.K., Lichtman A.H. and Pober J.S. Sounders company; Philadelphia, 2010. 1 What are cytokines? Glycoproteins (15 25 kda): Interleukins
SUPPLEMENTARY FIGURES
 SUPPLEMENTARY FIGURES Supplementary Figure 1: Chemokine receptor expression profiles of CCR6 + and CCR6 - CD4 + IL-17A +/ex and Treg cells. Quantitative PCR analysis of chemokine receptor transcript abundance
SUPPLEMENTARY FIGURES Supplementary Figure 1: Chemokine receptor expression profiles of CCR6 + and CCR6 - CD4 + IL-17A +/ex and Treg cells. Quantitative PCR analysis of chemokine receptor transcript abundance
As outlined under External contributions (see appendix 7.1), the group of Prof. Gröne at the
 3 RESULTS As outlined under External contributions (see appendix 7.1), the group of Prof. Gröne at the DKFZ in Heidelberg (Dept. of Cellular and Molecular pathology) contributed to this work by performing
3 RESULTS As outlined under External contributions (see appendix 7.1), the group of Prof. Gröne at the DKFZ in Heidelberg (Dept. of Cellular and Molecular pathology) contributed to this work by performing
Supporting Information
 Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Supporting Information Valkenburg et al. 10.1073/pnas.1403684111 SI Materials and Methods ELISA and Microneutralization. Sera were treated with Receptor Destroying Enzyme II (RDE II, Accurate) before ELISA
Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow
 SUPPLEMENTARY DATA Supplementary Figure Legends Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow cytometry analysis of PMVs labelled with annexin-v-pe (Guava technologies)
SUPPLEMENTARY DATA Supplementary Figure Legends Figure S1. PMVs from THP-1 cells expose phosphatidylserine and carry actin. A) Flow cytometry analysis of PMVs labelled with annexin-v-pe (Guava technologies)
Pearson r = P (one-tailed) = n = 9
 8F4-Specific Lysis, % 1 UPN1 UPN3 8 UPN7 6 Pearson r =.69 UPN2 UPN5 P (one-tailed) =.192 4 UPN8 n = 9 2 UPN9 UPN4 UPN6 5 1 15 2 25 8 8F4, % Max MFI Supplementary Figure S1. AML samples UPN1-UPN9 show variable
8F4-Specific Lysis, % 1 UPN1 UPN3 8 UPN7 6 Pearson r =.69 UPN2 UPN5 P (one-tailed) =.192 4 UPN8 n = 9 2 UPN9 UPN4 UPN6 5 1 15 2 25 8 8F4, % Max MFI Supplementary Figure S1. AML samples UPN1-UPN9 show variable
Journal Club Semmler Lorenz
 Beer et al. 2015 - Analysis of the Secretome of Apoptotic Peripheral Blood Mononuclear Cells: Impact of Released Proteins and Exosomes for Tissue Regeneration Journal Club 13.11.2017 1 Introduction to
Beer et al. 2015 - Analysis of the Secretome of Apoptotic Peripheral Blood Mononuclear Cells: Impact of Released Proteins and Exosomes for Tissue Regeneration Journal Club 13.11.2017 1 Introduction to
Optimizing Intracellular Flow Cytometry:
 Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
Optimizing Intracellular Flow Cytometry: Simultaneous Detection of Cytokines and Transcription Factors An encore presentation by Jurg Rohrer, PhD, BD Biosciences 10.26.10 Outline Introduction Cytokines
SUPPLEMENTARY INFORMATION
 DOI: 1.138/ncb3355 a S1A8 + cells/ total.1.8.6.4.2 b S1A8/?-Actin c % T-cell proliferation 3 25 2 15 1 5 T cells Supplementary Figure 1 Inter-tumoral heterogeneity of MDSC accumulation in mammary tumor
DOI: 1.138/ncb3355 a S1A8 + cells/ total.1.8.6.4.2 b S1A8/?-Actin c % T-cell proliferation 3 25 2 15 1 5 T cells Supplementary Figure 1 Inter-tumoral heterogeneity of MDSC accumulation in mammary tumor
