Guide to the Medical Evaluation in Suspected Physical Abuse
|
|
|
- Arline Newman
- 5 years ago
- Views:
Transcription
1 Guide to the Medical Evaluation in Suspected Physical Abuse Introduction Every year more than 3 million referrals are made to child protective services for concerns of child abuse and neglect with almost 700,000 children found to be victims of child maltreatment. While the majority of reports are due to neglect, almost 20% are due to physical abuse affecting almost 10 out of every 1,000 children. 1 Infants are disproportionately affected with rates of serious physical abuse 2 and abusive head trauma 3 more than twice the rate of children between 1 and 3 years of age 4. The diagnosis of physical abuse is still frequently missed resulting in additional injuries 5 and/or death 6, 7. Diagnostic testing for additional occult injuries in children with concerns for abuse may be based on clinician gestalt or on the presence of social risk factors such as a history of domestic violence, caregiver substance abuse, or previous involvement with social services. While the presence of risk factors is associated with child maltreatment, this approach may result in disproportionate child abuse evaluations according to race and/or socioeconomic status. 6, 8-12 Despite published recommendations by the American Academy of Pediatrics on screening for occult fractures in children under 2 years of age, fewer than 50% of physically abused children under 2 years of age received a skeletal survey for occult fractures with substantial variation between US hospitals. 13 An approach to child physical abuse that includes routine medical evaluations for additional serious injury may minimize this disparity while reducing the risk for additional serious injury. Red Flags While many children with abusive head trauma and inflicted skeletal trauma may not have visible cutaneous trauma 14, 15, bruising is still one of the most common manifestations of physical abuse and perhaps the easiest to recognize. Physicians have long recognized that bruises are rare in healthy infants who have not become mobile (e.g. crawling or cruising). 16, 17 Bruising, in an infant younger than 6 months of age, is therefore considered a red flag for abuse Red Flags also include patterned skin injuries and unusual locations of injury. These unusual locations are referred to as the TEN-FACES distribution; where TEN refers to bruising to the torso, ear or neck and FACES refers to frenulum, auricular (ear), cheek, eyelid or sclera. An easy mnemonic to remember is TEN-4 FACES where the number 4 refers to children under 4 years of age with bruising in the TEN distribution or any bruising in infants less than 4-6 months of age. 19 The importance of the bruise in an infant cannot be understated. One recent publication identified a history of prior bruising or oral injury in more than 25% of infants evaluated for serious physical abuse and abusive head trauma. 21 In a recent analysis of infants presenting with apparently isolated bruising, 50% had at least one additional serious injury identified on routine medical evaluation including physical examination, skeletal survey, neuroimaging and abdominal injury screening. 22 Other red flags may be found as part of the comprehensive medical evaluation. The comprehensive medical evaluation includes history of injury, developmental history, nutrition, past medical history (including pregnancy and birth), family medical history, social history, review of systems, physical examination and screening for additional serious injury through skeletal
2 survey, neuroimaging, and abdominal injury screening, or screening for medical conditions (e.g., bleeding disorders 23, 24, metabolic bone disease 25 ). The history of injury should include determining when the infant or child was last well as onset of symptoms such as crying, irritability, vomiting, and change in appetite or activity may represent symptoms of injury. Chief complaints such as unresponsiveness, seizure activity, colic or fussiness, or ALTE should be considered high risk necessitating a detailed skin examination. When the injury is known such as a long bone fracture, the history should assess injury plausibility. The child s developmental capabilities, timeline, and mechanism provided should be consistent with the fracture type (e.g., transverse, oblique, compression, buckle etc.). 26 Psychosocial assessments should review the child s caregivers and who lives in the home. Other children and respective ages should be identified as these contacts in the home are also at risk for additional injury and may require medical evaluation. 27 Psychosocial red flags to identify include: social service involvement, domestic/intimate partner violence, law enforcement involvement, substance abuse (drugs and/or alcohol), mental health issues, and negative attributions ascribed to the child by the caregiver. Current research utilizing these 6 psychosocial risk factors after a positive TEN-4-FACES skin screening examination has helped differentiate accidental from abusive head trauma. 28 However, additional research is still in progress at multiple institutions to determine whether clinical decision rules are needed 29 to predict abusive head trauma or to determine which children need additional serious injury screening 30. Screening for Additional Head Injury Abusive head trauma is the leading cause of serious intracranial injury in infants and death in children less than 4 years of age. 31 Intracranial injuries in young infants can be difficult to diagnosis as symptoms are non-specific (vomiting, irritability, fussiness, poor feeding) and can be attributed to benign illness (e.g. gastritis, colic, reflux). Although the presence of occult intracranial injury in approximately 30% of neurologically asymptomatic infants is supported by published studies 32, 33, recommendations on neuroimaging have not been as clearly defined as those for skeletal survey. In a recent multicenter study of infants under 6 months of age presenting with apparently isolated bruising, 90% of infants had neuroimaging obtained with new injury identified in 25%. Neuroimaging (CT or MRI, or both. 34, 35 ) should be performed even in neurologically asymptomatic infants with suspected child abuse. While the Center for Safe & Healthy Children s guidelines for physical abuse state that neuroimaging is mandatory for infants under 6 months (categorized as high-risk), occult injury still occurs in infants 6-12 months of age. 32, 33 Further study is needed to determine an appropriate age cut-off for mandatory neuroimaging. Screening for Additional Skeletal Trauma The skeletal survey (SS) is a series of radiographic images of the entire skeleton for the purpose of assessing a child for trauma as well as skeletal dysplasias and neoplasias. In a recent large population-based study, child abuse accounted for 12% of fractures in children less than 36 months of age. 36 The goal of the SS is to accurately identify fractures in children with suspected abuse as fractures may not be appreciated on examination (healing) and as associated bruising is uncommon. 14, 15 safechild@fairview.org 2
3 SSs are recommended by the American Academy of Pediatrics in all children younger than 2 years of age with concerns for child physical abuse, and in selected children between 2-5 years of age (e.g. developmental delay, non verbal, burns 37, 38, extensive trauma). 34, 35 SSs identify additional injury in as many as 25% of infants and children when obtained. 22, There is published literature to support obtaining SSs in older children as the yield of the SS in children 2-3 years of age is comparable to children 1-2 years of age (10% versus 12%). 43 It is also recommended to repeat the initial SS in 2 weeks, as acute fractures (e.g., rib fractures and classic metaphyseal lesions) may be occult. Large multisite studies have identified additional healing fractures on the follow-up skeletal survey or FUSS in 10-15% 41, 44 with overall additional clinical information (new fractures or reassuring findings) in more than 20% of children. 41 SSs should also be performed in children presenting with burns as the prevalence of fractures detected has been between 14-18%. 37, 38 Screening for Additional Abdominal Injury Abdominal injury is the second leading cause of death in children from physical abuse (second only to head injury). Overall, the estimate of the rate of missed diagnosis in child physical abuse is 30% or higher. 6, 45 The prevalence of inflicted abdominal injury is not sufficient to recommend universal screening with computed tomography of the abdomen. However, clinical examination remains insufficient to diagnose occult abdominal injury from child abuse. The prevalence of occult abdominal injury ranges from 3-6% depending upon the population studied In the highest risk age group (12-23 months), occult injury can be detected in 1 of every 20 toddlers with the use of liver transaminases. 48 The ULTRA study 47 (Utility of Liver Transaminases to Recognize Abuse in Children) prospectively studied 1676 children under the age of 5 years receiving child abuse consultation. Of these children, 1272 had liver transaminase screening with 54 (3.2%) having an identified abdominal injury (17 of those injuries were clinically occult). The rate of injury on CT of the abdomen was 16% (1 in 6 children). Sensitivity and specificity of an AST or ALT greater than 80 for the identification of abdominal injury was 77% and 82% respectively with a negative predictive value of 98%. If the physical examination is notable for abdominal bruising or tenderness or a GCS score < 15, the sensitivity and specificity of the CT for the identification of abdominal injury was 83% and 80%. NOTE: If transaminase screening were to be performed on 100 children with suspected child abuse 100 blood tests would be ordered, 18 CT scans of the abdomen (when AST or ALT is greater than 80) would be performed, and 3 additional injuries would be detected. The most sensitive and specific examination for the identification of abdominal trauma remains the abdominal/pelvis CT with contrast. While ultrasound has the benefit of speed, and is without radiation, it is insensitive and non-specific. In a study of the utility of liver enzymes to screen for abdominal trauma in children, 13% of abdominal injuries were missed including a grade 3 liver laceration. 50 safechild@fairview.org 3
4 MINNESOTA CHILD ABUSE NETWORK Assessment for Physical Abuse Tools in the Medical Evaluation (see Appendix A ASSESSMENT FOR PHYSICAL ABUSE CHART): 1. If the routine patient encounter identifies red flags on the history, physical examination or observation, a more comprehensive medical evaluation for suspected abuse and neglect is indicated: a. Red Flags on Chief Complaint: i. Vomiting ii. Fussiness iii. ALTE or unresponsiveness iv. Unwitnessed Fall or Fell off bed (most common history in accidental and abusive injuries) 51, A witnessed fall would include the presence of an additional person other than the primary caregiver b. Red Flags on History: i. Injury not consistent with child s age, development abilities, or injury morphology ii. History is vague or changes with time, repetition or caregiver iii. Delay in seeking medical care c. Red Flags on Psychosocial Assessment i. Negative attributions ascribed to the child by the caregiver (e.g., my baby is mean ) ii. Social service involvement iii. Law enforcement involvement iv. Domestic/intimate partner violence v. Substance abuse vi. Mental health issues d. Red Flags on Examination i. Full or bulging fontanelle in an infant ii. Rapidly increasing head circumference iii. Any bruising in an infant iv. Bruising in a child in the TEN or FACES distribution v. Patterned injury vi. Failure to thrive or weight loss e. Red Flags by Injury Type i. Rib Fracture ii. Metaphyseal Fracture iii. Long bone Fracture (non-ambulatory infant or child) iv. Oropharygngeal Injury (non-ambulatory infant or child) v. Abdominal Injury (non-mvc) vi. Head Injury (unwitnessed see above, unexplained) 2. Laboratory Evaluation: The goal of laboratory evaluation includes screening for additional serious abdominal injury: a. All children under age 5 years with concerns for physical abuse: i. CBC, Metabolic panel with liver enzymes, Lipase ii. Urine Drug Screening safechild@fairview.org 4
5 b. Additional testing to consider: i. Non-patterned bruising: PT-INR/PTT ii. Intracranial hemorrhage: PT-INR/PTT, Fibrinogen, D-Dimers iii. Extensive skin trauma: CPK iv. Suspected chest wall trauma: Troponin or CK-MB c. Child Abuse Physician Consultation: i. Intracranial Hemorrhage (no skeletal trauma or patterned injury): Bleeding disorder evaluation to include PT-INR/PTT, Fibrinogen, D-Dimers, Factors 8/9/13 (quantitative) 24 ii. Bruising (no skeletal trauma or patterned injury): Bleeding disorder evaluation to include PT-INR/PTT, von Willebrand s Panel and PFA iii. Skeletal Trauma (no additional ICH or patterned injury): Metabolic bone disease evaluation to include calcium, phosphorous, alkaline phosphatase, intact PTH, 25-hyroxy Vitamin D. Additional testing such as DNA for Osteogenesis Imperfecta should occur only in consultation with Genetics. 3. Skeletal Surveys: a. Initial SS recommended in all children under age 2 years and in selected children 2-5 years of age 53 i. Bruising: 19, SS should be completed in any infant under 6 months of age with a bruise except in cases of injury as a result of MVC, birth trauma, or witnessed fall in a public place. 2. SS should be completed in a child under 2-3 years of age with cutaneous injury in the TEN-FACES distribution, patterned injury (e.g. loop marks), injury occurring during domestic violence. ii. Fractures: SS is necessary in all children under 2 years of age with fractures thought secondary to domestic violence or attributed to minor trauma such as a toy or object. 2. SS is necessary in all children under 2 years of age with unusual or high specificity fractures such as rib fractures, metaphyseal fractures, complex or ping-pong skull fractures. 3. SS is necessary in children 0-11 months of age with ANY type of fracture with the exception of the following (as long as there are no additional concerns for injury): a. Linear unilateral skull fracture in a child over 6 months of age with a history of a fall or a caregiver landing on a child b. Distal radius/ulna buckle fracture or toddler s fracture of the tibia/fibula in a cruising child 9 months of age or older c. Clavicle fracture likely attributed to birth (e.g., acute fracture in an infant less than 2-3 weeks old or a healing fracture in an infant less than 1 month of age) b. Initial SS should be completed to ACR Standards 56 c. The literature supports the use of the SS in children 2-3 years of age with a similar yield (10%) as children 1-2 years of age (12%). 43 safechild@fairview.org 5
6 d. Follow-up SS or FUSS should be completed in approximately 2-3 weeks after the initial SS 53 e. Published literature supports the use of a more limited view FUSS as long as the child has been in protective placement and does not have prior concern for vertebral or pelvic fractures Abdominal Imaging: a. Abdominal/Pelvis CT with contrast is indicated: i. Abnormal abdominal examination e.g. bruising 47, 58, distention 58, tenderness 47 ii. AST or ALT greater than 8047, 49 b. Ultrasound is insensitive and non-specific for the identification of abdominal trauma Neuroimaging: a. CT head and/or MRI brain is indicated in all infants under 6 months of age with concerns for abuse regardless of symptoms or location of bruising22, 32, 33 b. CT head and/or MRI brain is indicated in children with concerns for abuse and i. Altered mental status ii. Skull fracture(s) iii. Bruising to the face, ear, scalp c. Child Abuse Consultation: i. MRI Brain is indicated in infants with abnormal mental status whose initial head CT is considered normal as hyperacute subdural hemorrhages may not be detected on initial CT59, 60 ii. When early head CT is complemented by MRI Brain, additional information is identified in 25% of children including intracranial hemorrhages, shearing injury, ischemia and infarction. 61 iii. MRI Brain & MRI C-Spine (with STIR) is indicated in children with concerns for abusive head trauma on initial CT head due to associated cervical injuries identified in infants. 62, 63 iv. NOTE: The literature also supports MR imaging of the whole spine due to associated cervical and thoracic injury. 63, Ophthalmology: Dilated fundoscopic examination should be performed: a. In infants and children with intracranial hemorrhage and concerns for abusive head trauma. b. In infants with negative neuroimaging, but who have abnormal mental status and concerns for physical abuse. c. Within 24 hours of presentation due to the transient nature of retinal hemorrhages, ideally no longer than 72 hours 65 d. NOTE: Dilated fundoscopic examination is not necessary if neuroimaging is negative with normal mental status and without facial bruising 66 ; OR the intracranial hemorrhage is small and in contact with a linear non-occipital skull fracture 67 in an infant or child with normal mental status and without facial bruising. safechild@fairview.org 6
7 MINNESOTA CHILD ABUSE NETWORK (MN CAN) Consultation by a Regional Child Abuse Program should be considered for the following: Bruising or oral injury in non-ambulatory infants Unexplained head injury (e.g., intracranial hemorrhages, skull fractures), especially in children < 3 years of age Unexplained fractures or fractures occurring in non-ambulatory children Unexplained (non-mvc) abdominal injury, especially in children < 3 years of age Unexplained burns including immersion, pattern and questionable burns in nonambulatory children Concerns for prolonged exposure or intentional starvation safechild@fairview.org 7
8 References: 1. U.S. Department of Health and Human Services, Administration for Children and Families, Administra- tion on Children, Youth and Families, Children s Bureau. (2012). Child maltreatment Available from 2. Leventhal JM, Martin KD, Gaither JR. Using US data to estimate the incidence of serious physical abuse in children. Pediatrics 2012;129: Niederkrotenthaler T, Xu L, Parks SE, et al. Descriptive factors of abusive head trauma in young children-united States, Child Abuse Negl Leventhal JM, Martin KD, Asnes AG. Fractures and traumatic brain injuries: abuse versus accidents in a US database of hospitalized children. Pediatrics 2010;126:e Ravichandiran N, Schuh S, Bejuk M, et al. Delayed identification of pediatric abuse-related fractures. Pediatrics 2010;125: Jenny C, Hymel KP, Ritzen A, et al. Analysis of missed cases of abusive head trauma. JAMA 1999;281: Oral R, Yagmur F, Nashelsky M, et al. Fatal abusive head trauma cases: consequence of medical staff missing milder forms of physical abuse. Pediatr Emerg Care 2008;24: Wood JN, Hall M, Schilling S, et al. Disparities in the evaluation and diagnosis of abuse among infants with traumatic brain injury. Pediatrics 2010;126: Wood JN, Christian CW, Adams CM, et al. Skeletal surveys in infants with isolated skull fractures. Pediatrics 2009;123:e Laskey AL, Stump TE, Perkins SM, et al. Influence of race and socioeconomic status on the diagnosis of child abuse: a randomized study. J Pediatr 2012;160: e Drug-Facilitated Sexual Assault Fast Facts: Questions and Answers. In: Center NDI, ed.: U.S. Department of Justice (vol 2008). 12. Lane WG, Rubin DM, Monteith R, et al. Racial differences in the evaluation of pediatric fractures for physical abuse. JAMA 2002;288: Wood JN, French B, Song L, et al. Evaluation for Occult Fractures in Injured Children. Pediatrics 2015;136: Mathew MO, Ramamohan N, Bennet GC. Importance of bruising associated with paediatric fractures: prospective observational study. Bmj 1998;317: Peters ML, Starling SP, Barnes-Eley ML, et al. The presence of bruising associated with fractures. Arch Pediatr Adolesc Med 2008;162: Labbe J, Caouette G. Recent skin injuries in normal children. Pediatrics 2001;108: Sugar NF, Taylor JA, Feldman KW. Bruises in infants and toddlers: those who don't cruise rarely bruise. Puget Sound Pediatric Research Network. Arch Pediatr Adolesc Med 1999;153: Feldman KW. The bruised premobile infant: should you evaluate further? Pediatr Emerg Care 2009;25: Pierce MC, Kaczor K, Aldridge S, et al. Bruising characteristics discriminating physical child abuse from accidental trauma. Pediatrics 2010;125: Pierce MC, Smith S, Kaczor K. Bruising in infants: those with a bruise may be abused. Pediatric emergency care 2009;25: Sheets LK, Leach ME, Koszewski IJ, et al. Sentinel injuries in infants evaluated for child physical abuse. Pediatrics 2013;131: Harper NS, Feldman KW, Sugar NF, et al. Additional injuries in young infants with concern for abuse and apparently isolated bruises. J Pediatr 2014;165: e Carpenter SL, Abshire TC, Anderst JD, et al. Evaluating for suspected child abuse: conditions that predispose to bleeding. Pediatrics 2013;131:e Anderst JD, Carpenter SL, Abshire TC, et al. Evaluation for bleeding disorders in suspected child abuse. Pediatrics 2013;131:e safechild@fairview.org 8
9 25. Flaherty EG, Perez-Rossello JM, Levine MA, et al. Evaluating children with fractures for child physical abuse. Pediatrics 2014;133:e Snyder KR, Currie ML, Stockhammer TF. Interviewing Caregivers of Suspected Child Abuse Victims. In: Jenny C, ed. Child Abuse and Neglect: Diagnosis, Treatment, and Evidence. St. Louis, MO: Elsevier Saunders, Lindberg DM, Blood EA, Campbell KA, et al. Predictors of Screening and Injury in Contacts of Physically Abused Children. J Pediatr Pierce MC, Kaczor K, Lorenz D, et al. Bruising Characteristics and Psychosocial Factors Help Discriminate Abusive from Accidental Head TraumaThe Ray E Helfer Society Annual Meeting. Annapolis, MD, Berger R, Mcginn T. Deciding whether to screen for abusive head trauma: do we need a clinical decision rule? Pediatr Crit Care Med 2013;14: Hymel KP, Willson DF, Boos SC, et al. Derivation of a clinical prediction rule for pediatric abusive head trauma. Pediatr Crit Care Med 2013;14: US Advisory Board on Child Abuse and Neglect. A nation's shame: fatal child abuse and neglect in the United States. In: Services UDoHaH, ed., Laskey AL, Holsti M, Runyan DK, et al. Occult head trauma in young suspected victims of physical abuse. J Pediatr 2004;144: Rubin DM, Christian CW, Bilaniuk LT, et al. Occult head injury in high-risk abused children. Pediatrics 2003;111: Diagnostic imaging of child abuse. Pediatrics 2009;123: Kellogg ND. Evaluation of suspected child physical abuse. Pediatrics 2007;119: Leventhal JM, Martin KD, Asnes AG. Incidence of fractures attributable to abuse in young hospitalized children: results from analysis of a United States database. Pediatrics 2008;122: Degraw M, Hicks RA, Lindberg D. Incidence of fractures among children with burns with concern regarding abuse. Pediatrics 2010;125:e Hicks RA, Stolfi A. Skeletal surveys in children with burns caused by child abuse. Pediatr Emerg Care 2007;23: Day F, Clegg S, Mcphillips M, et al. A retrospective case series of skeletal surveys in children with suspected non-accidental injury. J Clin Forensic Med 2006;13: Barber I, Perez-Rossello JM, Wilson CR, et al. Prevalence and relevance of pediatric spinal fractures in suspected child abuse. Pediatr Radiol 2013;43: Harper NS, Eddleman S, Lindberg DM, et al. The utility of follow-up skeletal surveys in child abuse. Pediatrics 2013;131:e Duffy SO, Squires J, Fromkin JB, et al. Use of skeletal surveys to evaluate for physical abuse: analysis of 703 consecutive skeletal surveys. Pediatrics 2011;127:e Lindberg DM, Berger RP, Reynolds MS, et al. Yield of skeletal survey by age in children referred to abuse specialists. J Pediatr 2014;164: e Singh R, Squires J, Fromkin JB, et al. Assessing the use of follow-up skeletal surveys in children with suspected physical abuse. J Trauma Acute Care Surg 2012;73: Theodore AD, Chang JJ, Runyan DK, et al. Epidemiologic features of the physical and sexual maltreatment of children in the Carolinas. Pediatrics 2005;115:e Coant PN, Kornberg AE, Brody AS, et al. Markers for occult liver injury in cases of physical abuse in children. Pediatrics 1992;89: Lindberg D, Makoroff K, Harper N, et al. Utility of hepatic transaminases to recognize abuse in children. Pediatrics 2009;124: Lane WG, Dubowitz H, Langenberg P. Screening for occult abdominal trauma in children with suspected physical abuse. Pediatrics 2009;124: safechild@fairview.org 9
10 49. Lindberg DM, Shapiro RA, Blood EA, et al. Utility of hepatic transaminases in children with concern for abuse. Pediatrics 2013;131: Karam O, La Scala G, Le Coultre C, et al. Liver function tests in children with blunt abdominal traumas. Eur J Pediatr Surg 2007;17: Adamsbaum C, Grabar S, Mejean N, et al. Abusive head trauma: judicial admissions highlight violent and repetitive shaking. Pediatrics 2010;126: Chadwick DL, Chin S, Salerno C, et al. Deaths from falls in children: how far is fatal? J Trauma 1991;31: Christian CW, Committee on Child A, Neglect AaOP. The evaluation of suspected child physical abuse. Pediatrics 2015;135:e Wood JN, Fakeye O, Mondestin V, et al. Development of hospital-based guidelines for skeletal survey in young children with bruises. Pediatrics 2015;135:e Wood JN, Fakeye O, Feudtner C, et al. Development of guidelines for skeletal survey in young children with fractures. Pediatrics 2014;134: American College of Radiology. ACR-SPR Practice Parameter for Skeletal Surveys in Children, 2014 (Resolution 39). 57. Hansen KK, Keeshin BR, Flaherty E, et al. Sensitivity of the limited view follow-up skeletal survey. Pediatrics 2014;134: Hilmes MA, Hernanz-Schulman M, Greeley CS, et al. CT identification of abdominal injuries in abused pre-school-age children. Pediatr Radiol 2011;41: Morad Y, Avni I, Benton SA, et al. Normal computerized tomography of brain in children with shaken baby syndrome. J AAPOS 2004;8: Sato Y, Yuh WT, Smith WL, et al. Head injury in child abuse: evaluation with MR imaging. Radiology 1989;173: Kemp AM, Rajaram S, Mann M, et al. What neuroimaging should be performed in children in whom inflicted brain injury (ibi) is suspected? A systematic review. Clin Radiol 2009;64: Kadom N, Khademian Z, Vezina G, et al. Usefulness of MRI detection of cervical spine and brain injuries in the evaluation of abusive head trauma. Pediatr Radiol 2014;44: Choudhary AK, Ishak R, Zacharia TT, et al. Imaging of spinal injury in abusive head trauma: a retrospective study. Pediatr Radiol 2014;44: Kemp AM, Joshi AH, Mann M, et al. What are the clinical and radiological characteristics of spinal injuries from physical abuse: a systematic review. Arch Dis Child 2010;95: Levin AV, Christian CW, Committee on Child A, et al. The eye examination in the evaluation of child abuse. Pediatrics 2010;126: Thackeray JD, Scribano PV, Lindberg DM. Yield of retinal examination in suspected physical abuse with normal neuroimaging. Pediatrics 2010;125:e Li S, Mitchell E, Fromkin J, et al. Retinal hemorrhages in low-risk children evaluated for physical abuse. Arch Pediatr Adolesc Med 2011;165: safechild@fairview.org 10
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines
 Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Trauma Center Practice Management Guideline Blank Children s Hospital (BCH) Des Moines Non-Accidental Trauma (NAT) PEDIATRIC Practice Management Guideline Contact: Trauma Center Medical Director/ Trauma
Suspected Physical Abuse Clinical Practice Guideline
 Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Suspected Physical Abuse Clinical Practice Guideline WHEN TO CONSIDER ABUSE Consider abuse on the differential Injuries to multiple organ systems Injuries in different stages of healing Patterned injuries
Bilateral rib fractures 2 on right and 1 on left In different stages of healing, with left fracture older than right fractures
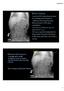 More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
More history: Seen by PCP yesterday because of vomiting and fussinesss. Called by ED today because Mom presents with same complaints. ED found nothing but got an abdominal x ray. ED now wants kid admitted
Radiological investigations
 Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
Nita Jain, MD, FRCPC The role of diagnostic imaging in the evaluation of child abuse Radiologists experienced in pediatric imaging can provide invaluable assistance to health care teams working to identify
2/13/13. Ann S. Botash, MD SUNY Upstate Medical University
 Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
Ann S. Botash, MD SUNY Upstate Medical University 3 month old, previously healthy infant, brought to the primary care physician due to a fall He was being carried by the father, who tripped over the family
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation **
 PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
PHYSICAL ABUSE: INITIAL EVALUATION AND MANAGEMENT **Child Protection MD is available by pager for questions or formal consultation ** I. RECOGNITION A. History 1. Unexplained or un-witnessed injury 2.
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May Leslie M. Quinn M.D.
 CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
CHILD MALTREATMENT- GUIDELINES FOR SUSPICION and INITIAL MEDICAL EVALUATION DRAFT May 2012 - Leslie M. Quinn M.D. PHYSICAL ABUSE: For any child presenting with signs and or symptoms of an injury consider
Evidence Base for Child Abuse Fractures
 Evidence Base for Child Abuse Fractures SPR Sunrise Session May 17, 2018 Megan B. Marine, MD, FAAP Assistant Professor of Clinical Radiology, Pediatric Division Co-Director, Pediatric Radiology Fellowship
Evidence Base for Child Abuse Fractures SPR Sunrise Session May 17, 2018 Megan B. Marine, MD, FAAP Assistant Professor of Clinical Radiology, Pediatric Division Co-Director, Pediatric Radiology Fellowship
Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics
 Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics Disclosure I have nothing to disclose Objectives Describe common accidental injuries which can be confused with child abuse Describe
Abuse or Accident? Suzanne B. Haney, MD, FAAP Child Abuse Pediatrics Disclosure I have nothing to disclose Objectives Describe common accidental injuries which can be confused with child abuse Describe
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast
 The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
The Medical Assessment of Fractures in Suspected Child Maltreatment: Infants and Young Children with Skeletal Injury CPS Podcast September 27, 2018 Introduction: Hello everyone, my name is Dominique Piché
OVERVIEW OF CHILD PHYSICAL ABUSE
 2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
2011 MFMER slide-1 OVERVIEW OF CHILD PHYSICAL ABUSE Mark S. Mannenbach, MD Mayo Medical Center Rochester, MN 2011 MFMER slide-2 Objectives At the conclusion of this session, the participant will be able
Overview of Abusive Head Trauma: What Everyone Needs to Know. 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012
 Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Overview of Abusive Head Trauma: What Everyone Needs to Know 11 th Annual Keeping Children Safe Conference Boise, ID October 17, 2012 Deborah Lowen, MD Associate Professor Pediatrics Director, Child Abuse
Evaluation of a Pediatric Patient
 September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
September 2005 Evaluation of a Pediatric Patient Percy Ballard, Harvard Medical School Year III Our Little Man: 6mo old male transferred to Children s from hospital in the Philippines 3mo history of meningitis,
Common Abusive Skeletal Injuries
 Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Common Abusive Skeletal Injuries Paul Kleinman, M.D. Children s Hospital Harvard Medical School Boston, Ma. Rib fractures, especially posteromedial Rib fractures, especially posteromedial Kemp AM et. Al.
Pediatric Abusive Head Trauma
 Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
Pediatric Abusive Head Trauma Rebecca Girardet Associate Professor of Pediatrics Director, Division of Child Protection Pediatrics McGovern Medical School at The University of Texas Health Science Center
ACR Appropriateness Criteria Suspected Physical Abuse Child EVIDENCE TABLE
 6. Merten DF, Carpenter BL. Radiologic imaging of inflicted injury in the child abuse syndrome. Pediatr Clin North Am. 1990;7():815-87. 7. Servaes S, Brown SD, Choudhary AK, et al. The etiology and significance
6. Merten DF, Carpenter BL. Radiologic imaging of inflicted injury in the child abuse syndrome. Pediatr Clin North Am. 1990;7():815-87. 7. Servaes S, Brown SD, Choudhary AK, et al. The etiology and significance
Pediatric head trauma: the evidence regarding indications for emergent neuroimaging
 DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
DOI 10.1007/s00247-008-0996-5 ALARA: BUILDING BRIDGES BETWEEN RADIOLOGY AND EMERGENCY MEDICINE Pediatric head trauma: the evidence regarding indications for emergent neuroimaging Nathan Kuppermann Received:
The Viewing Study Guide for Physical Abuse Slides
 The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
The Viewing Study Guide for Physical Abuse Slides Adapted From The Visual Diagnosis of Non-Accidental Trauma and Failure to Thrive A Study Guide By Barton D. Schmitt, M.D. in Cooperation with The American
Since the publication of The Battered-Child Syndrome in 1962,1
 The new england journal of medicine Clinical Practice Caren G. Solomon, M.D., M.P.H., Editor Physical Abuse of Children Carol D. Berkowitz, M.D. This Journal feature begins with a case vignette highlighting
The new england journal of medicine Clinical Practice Caren G. Solomon, M.D., M.P.H., Editor Physical Abuse of Children Carol D. Berkowitz, M.D. This Journal feature begins with a case vignette highlighting
Disclosure. Physical Abuse. Objectives. What is the Mechanism of the Injury?
 Disclosure Abuse or Not Abuse: What is the Answer? Natalie Kissoon, MD Assistant Professor Division of Child Abuse Pediatrics University of Texas Health Science Natalie Kissoon, MD has no relationships
Disclosure Abuse or Not Abuse: What is the Answer? Natalie Kissoon, MD Assistant Professor Division of Child Abuse Pediatrics University of Texas Health Science Natalie Kissoon, MD has no relationships
Analysis of pediatric head injury from falls
 Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Neurosurg Focus 8 (1):Article 3, 2000 Analysis of pediatric head injury from falls K. ANTHONY KIM, MICHAEL Y. WANG, M.D., PAMELA M. GRIFFITH, R.N.C., SUSAN SUMMERS, R.N., AND MICHAEL L. LEVY, M.D. Division
Medical Aspects of Child Physical Abuse the approach to physically abused kids. Objectives
 Center for Safe & Healthy Children Medical Aspects of Child Physical Abuse the approach to physically abused kids Nancy S. Harper, MD FAAP Child Abuse Pediatrics Associate Professor of Pediatrics, University
Center for Safe & Healthy Children Medical Aspects of Child Physical Abuse the approach to physically abused kids Nancy S. Harper, MD FAAP Child Abuse Pediatrics Associate Professor of Pediatrics, University
Imaging of non-accidental injury; what is clinical best practice?
 REVIEW ARTICLE Imaging of non-accidental injury; what is clinical best practice? Amy Nguyen, BRadMedImag (Hons), & Robin Hart, PhD Department of Medical Imaging and Radiation Sciences, Faculty of Medicine,
REVIEW ARTICLE Imaging of non-accidental injury; what is clinical best practice? Amy Nguyen, BRadMedImag (Hons), & Robin Hart, PhD Department of Medical Imaging and Radiation Sciences, Faculty of Medicine,
Reviewing the recent literature to answer clinical questions: Should I change my practice?
 Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
Reviewing the recent literature to answer clinical questions: Should I change my practice? JILL MILLER, MD PEM ATTENDING CHKD ASSISTANT PROFESSOR PEDIATRICS, EVMS Objectives Review the literature to answer
of Trauma Assembly 27 th Page 1
 Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Eastern Association for the Surgery of Trauma 27 th Annual Scientific Assembly Sunrise Session 08 To Scan or Not To Scan Thatt is the Question January 16, 2014 Waldorf Astoria Naples Naples, Floridaa Page
Index. Note: Page numbers of article titles are in bold face type.
 Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
Neurosurg Clin N Am 13 (2002) 259 264 Index Note: Page numbers of article titles are in bold face type. A Abdominal injuries, in child abuse, 150, 159 Abrasions, in child abuse, 157 Abuse, child. See Child
10/8/17. I have no disclosures. What are they? Upper extremity fractures Lower extremity fractures Non accidental trauma
 I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
I have no disclosures Upper extremity fractures Lower extremity fractures Non accidental trauma What are they? Fractures of the radius, ulna and/or humerus Who gets them? Active children usually after
Abuse Or Not? Interactive Visual Clues in Child Abuse
 Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
Abuse Or Not? Interactive Visual Clues in Child Abuse Amy Baxter MD FAAP FACEP Associate Clinical Professor Medical College of Georgia 4 month old sleepy vomiting Mom works nights Wouldn t feed well Shivering
Original Article. Emergency Department Evaluation of Ventricular Shunt Malfunction. Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH
 Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Original Article Emergency Department Evaluation of Ventricular Shunt Malfunction Is the Shunt Series Really Necessary? Raymond Pitetti, MD, MPH Objective: The malfunction of a ventricular shunt is one
Pattern of Fractures in Non-Accidental Injuries in the Pediatric Population in Singapore
 Original Article Clinics in Orthopedic Surgery 2014;6:432-438 http://dx.doi.org/10.4055/cios.2014.6.4.432 Pattern of Fractures in Non-Accidental Injuries in the Pediatric Population in Singapore Sumanth
Original Article Clinics in Orthopedic Surgery 2014;6:432-438 http://dx.doi.org/10.4055/cios.2014.6.4.432 Pattern of Fractures in Non-Accidental Injuries in the Pediatric Population in Singapore Sumanth
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains
 5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
5 B s of Child Physical Abuse: Bruises, Burns, Bones, Bellies, and Brains Kristen Reeder, MD Child Abuse Pediatrician, REACH Program Children s Health SM Children s Medical Center Dallas Assistant Professor
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age. DRAFT REVIEW May 2008
 Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
Child Protection Guidelines in Suspected Non-Accidental Head Injury (NAHI) in Children Under 2 years of age DRAFT REVIEW May 2008 Responsibility for monitoring Review and update CPU Dr. Jean Herbison Current
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C)
 Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Subtle Signs of Child Abuse Child s Protection Office MOH Presented by Dr.Fatoumah Alabdulrazzaq M.D,FRCPC,FAAP,PEM(C) Cutaneous Injuries Bruise : injury to soft tissues in which skin is not broken, characterized
Children diagnosed with skull fractures are often. Transfer of children with isolated linear skull fractures: is it worth the cost?
 clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
clinical article J Neurosurg Pediatr 17:602 606, 2016 Transfer of children with isolated linear skull fractures: is it worth the cost? Ian K. White, MD, 1 Ecaterina Pestereva, BS, 1 Kashif A. Shaikh, MD,
The Evaluation of Suspected Child Physical Abuse
 CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care The Evaluation of Suspected Child Physical Abuse Cindy W. Christian, MD, FAAP, COMMITTEE ON CHILD ABUSE AND NEGLECT Child physical
CLINICAL REPORT Guidance for the Clinician in Rendering Pediatric Care The Evaluation of Suspected Child Physical Abuse Cindy W. Christian, MD, FAAP, COMMITTEE ON CHILD ABUSE AND NEGLECT Child physical
Stair falls: caregiver s missed step as a source of childhood fractures
 J Child Orthop (2014) 8:77 81 DOI 10.1007/s11832-014-0551-x ORIGINAL CLINICAL ARTICLE Stair falls: caregiver s missed step as a source of childhood fractures Andrew T. Pennock George D. Gantsoudes Jennifer
J Child Orthop (2014) 8:77 81 DOI 10.1007/s11832-014-0551-x ORIGINAL CLINICAL ARTICLE Stair falls: caregiver s missed step as a source of childhood fractures Andrew T. Pennock George D. Gantsoudes Jennifer
I have no financial disclosures.
 In the Belly of the Whale: Surviving Thoracoabdominal Trauma Debra Esernio Jenssen, MD, FAAP I have no financial disclosures. Objectives Review epidemiology of abusive chest and abdominal trauma. Identify
In the Belly of the Whale: Surviving Thoracoabdominal Trauma Debra Esernio Jenssen, MD, FAAP I have no financial disclosures. Objectives Review epidemiology of abusive chest and abdominal trauma. Identify
Use of CT in minor traumatic brain injury. Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD
 Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
Use of CT in minor traumatic brain injury Lisa Ayoub-Rodriguez, MD Bert Johansson, MD Michael Lee, MD No financial or other conflicts of interest Epidemiology of traumatic brain injury (TBI) Risks associated
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services OBJECTIVES DEFINITION 11/8/2017. Identify SCIWORA.
 SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
SCIWORA Rozlyn McTeer BSN, RN, CEN Pediatric Trauma Coordinator Trauma Services Identify SCIWORA. OBJECTIVES Identify the population at risk. To identify anatomic and physiologic reasons for SCIWORA. To
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND
 Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
Thoracic aortic trauma A.T.O.ABDOOL-CARRIM ACADEMIC HEAD VASCULAR SURGERY DEPARTMENT OF SURGERY UNIVERSITY OF WITWATERSRAND Thoracic Aortic Trauma In USA and CANADA 7500-8000 die of blunt thoracic aortic
Injuries in Non Mobile Infants Protocol
 Injuries in Non Mobile Infants Protocol Contents 1. Introduction 2. Definition 3. Recommended Action 4. Specific considerations for disabled children 5. Accidental / non-accidental / inconclusive categories
Injuries in Non Mobile Infants Protocol Contents 1. Introduction 2. Definition 3. Recommended Action 4. Specific considerations for disabled children 5. Accidental / non-accidental / inconclusive categories
ORTHOPEDIC ASPECTS CHILD ABUSE. A summary of the physical, metaphysical, psychological, and sociological aspects of Non-
 ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
ORTHOPEDIC ASPECTS OF CHILD ABUSE A summary of the physical, metaphysical, psychological, and sociological aspects of Non- Accidental Injury with specific references to both the perpetrator and victim
PEM GUIDE CHILDHOOD FRACTURES
 PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
PEM GUIDE CHILDHOOD FRACTURES INTRODUCTION Skeletal injuries account for 10-15% of all injuries in children; 20% of those are fractures, 3 out of 4 fractures affect the physis or growth plate. Always consider
ARTICLE. Intracranial Hemorrhage in Children Younger Than 3 Years
 Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
Intracranial Hemorrhage in Children Younger Than 3 Years Prediction of Intent ARTICLE Robert G. Wells, MD; Christine Vetter, MD; Prakash Laud, PhD Objective: To determine whether certain computed tomographic
17. Imaging and interventional radiology
 17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
17. Imaging and interventional radiology These guidelines have been adapted from the Leeds Major Trauma Centre Imaging in Paediatric Major Trauma guidelines Written by Dr Annmarie Jeanes (Consultant Paediatric
Subdural haematoma and effusion in children aged < 2 years
 Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
Subdural haematoma and effusion in children aged < 2 years Zurynski YA 1,2, Marks S 3, Chaseling R 3 on behalf of the Subdural Haematoma study group 1. Australian Paediatric Surveillance Unit 2. The University
The Ray E. Helfer Society s 2013 Annual Meeting Schedule
 Sunday, 4/14 Scholar Pre Conference 8am 5pm Registration The Ray E. Helfer Society s 2013 Annual Meeting Schedule 8:30 am Welcome Mary Greiner, MD 8:30 8:55 am Raise Your Right Hand: Child Abuse Pediatricians
Sunday, 4/14 Scholar Pre Conference 8am 5pm Registration The Ray E. Helfer Society s 2013 Annual Meeting Schedule 8:30 am Welcome Mary Greiner, MD 8:30 8:55 am Raise Your Right Hand: Child Abuse Pediatricians
Brain and Cervico-Medullary Injury : Patterns and Mechanisms
 Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Brain and Cervico-Medullary Injury : Patterns and Mechanisms P. Ellen Grant MD Associate Professor of Radiology, HMS Director, Center for Fetal-Neonatal Neuroimaging & Developmental Science Children s
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
Surgical Care at the District Hospital 1 17 Orthopedic Techniques Key Points 2 17.1 Traction Use an appropriate method of traction to treat fractures of the extremities and cervical spine Apply extremity
6/23/2017. What do you see? skull fracture
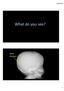 What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
What do you see? skull fracture 1 Head CT On soft tissue windows, posterior soft tissues swelling and hemorrhage, no definite evidence of fracture Head CT On bone windows, fracture now seen subjacent to
Recognizing and Responding to Child Abuse & Neglect
 Recognizing and Responding to Child Abuse & Neglect Maria D. McColgan, MD Associate Professor Drexel University College of Medicine Director, Child Protection Program St. Christopher s Hospital for Children
Recognizing and Responding to Child Abuse & Neglect Maria D. McColgan, MD Associate Professor Drexel University College of Medicine Director, Child Protection Program St. Christopher s Hospital for Children
Evaluation of Children with Blunt Abdominal Trauma. James F. Holmes, MD, MPH UC Davis School of Medicine
 Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Evaluation of Children with Blunt Abdominal Trauma James F. Holmes, MD, MPH UC Davis School of Medicine Objectives Epidemiology of intra-abdominal injury (IAI) Physical examination findings with IAI Laboratory
Disclosure Statement. Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk.
 Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Disclosure Statement Dr. Kadish has no relevant financial relationships with any commercial interests mentioned in this talk. Head Trauma Evaluation Primary and secondary injury Disposition Sports related
Imaging in the Trauma Patient
 Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
Imaging in the Trauma Patient David A. Spain, MD Department of Surgery Stanford University Pan Scan Instead of Clinical Exam? 1 Granted, some patients don t need CT scan Platinum Package Stanford Special
They re not little adults, but they are little humans. Pearls for your next pediatric trauma patient. Children are little humans
 They re not little adults, but they are little humans Pearls for your next pediatric trauma patient Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago Alisa McQueen
They re not little adults, but they are little humans Pearls for your next pediatric trauma patient Alisa McQueen MD, FAAP, FACEP Associate Professor of Pediatrics The University of Chicago Alisa McQueen
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes. Lisa Schwing, RN Trauma Program Manager Dayton Children s
 Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
Little Kids in Big Crashes The Bio-mechanics of Kids in Car Crashes Lisa Schwing, RN Trauma Program Manager Dayton Children s Very Little Research There has been very little research on the forces a crash
Non-Accidental Trauma (NAT) Protocol
 Non-Accidental Trauma (NAT) Protocol All children suspected of non-accidental trauma will have a complete work-up including a complete history and physical exam with a focus on injuries and explanation
Non-Accidental Trauma (NAT) Protocol All children suspected of non-accidental trauma will have a complete work-up including a complete history and physical exam with a focus on injuries and explanation
PEDIATRIC BLUNT TRAUMA WHAT S DIFFERENT? NORDIC TRAUMA COURSE 2016
 PEDIATRIC BLUNT TRAUMA WHAT S DIFFERENT? NORDIC TRAUMA COURSE 2016 Ken F. Linnau, MD, MS Emergency Radiology Harborview Medical Center University of Washington Seattle, WA Thanks to Nupur Verma, MD University
PEDIATRIC BLUNT TRAUMA WHAT S DIFFERENT? NORDIC TRAUMA COURSE 2016 Ken F. Linnau, MD, MS Emergency Radiology Harborview Medical Center University of Washington Seattle, WA Thanks to Nupur Verma, MD University
CORE-INFO: fractures in children
 CORE-INFO: fractures in children This leaflet summarises what is currently known about the relationship between fractures and physical abuse and will be of particular interest to paediatricians, general
CORE-INFO: fractures in children This leaflet summarises what is currently known about the relationship between fractures and physical abuse and will be of particular interest to paediatricians, general
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages.
 Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
Non-accidental Trauma: An unresponsive infant with bilateral retinal hemorrhages. Lucas J. A. Wendel, MD, Susannah Q. Longmuir, MD, and Nasreen A. Syed, MD February 12, 2009 Chief Complaint: 7 month old
Embargo Copy - Not for Distribution
 Page 1 of 8 Embargo Copy - Not for Distribution Using US Data to Estimate the Incidence of Serious Physical Abuse in Children John M. Leventhal, MD, Kimberly D. Martin, PhD, and Julie R. Gaither, RN, MPH
Page 1 of 8 Embargo Copy - Not for Distribution Using US Data to Estimate the Incidence of Serious Physical Abuse in Children John M. Leventhal, MD, Kimberly D. Martin, PhD, and Julie R. Gaither, RN, MPH
PEDIATRIC EMERGENCY DEPARTMENT CLINICAL GUIDELINE: GI SURGICAL EMERGENCIES: VOMITING
 GI SURGICAL EMERGENCIES: VOMITING PYLORIC STENOSIS Population: Infants: onset between 2-5 weeks of age 1 in 250 births Male: female ratio 4:1 Familial incidence History: No vomiting in the first few weeks
GI SURGICAL EMERGENCIES: VOMITING PYLORIC STENOSIS Population: Infants: onset between 2-5 weeks of age 1 in 250 births Male: female ratio 4:1 Familial incidence History: No vomiting in the first few weeks
Recognising and Managing Child Abuse in General Practice. Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital
 Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
Recognising and Managing Child Abuse in General Practice Dr Ceiridwen Davies Consultant Paediatrician Child Abuse Team Red Cross Children s Hospital Definition Outline Importance of Child Abuse Common
CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect
 CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect I. IDENTIFY THE CHILD WHO MAY BE A VICTIM OF ABUSE OR NEGLECT. A. Injuries
CLINICAL PRACTICE RESOURCE FOR HOSPITALS AND EMERGENCY DEPARTMENTS: Evaluation and Management of Suspected Child Abuse or Neglect I. IDENTIFY THE CHILD WHO MAY BE A VICTIM OF ABUSE OR NEGLECT. A. Injuries
Role of the Radiologist
 Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Diagnosis and Treatment of Blunt Cerebrovascular Injuries NORDTER Consensus Conference October 22-24, 2007 Clint W. Sliker, M.D. University of Maryland Medical Center R Adams Cowley Shock Trauma Center
Request Card Task ANSWERS
 Request Card Task ANSWERS Medical Student Workbook Author: Dr Sam Leach, SpR Case 1 What differential diagnoses are most likely? Which investigation is most appropriate? Case 1 The most likely diagnosis
Request Card Task ANSWERS Medical Student Workbook Author: Dr Sam Leach, SpR Case 1 What differential diagnoses are most likely? Which investigation is most appropriate? Case 1 The most likely diagnosis
The medical assessment of bruising in suspected child maltreatment cases: A clinical perspective
 The medical assessment of bruising in suspected child maltreatment cases: A clinical perspective Michelle GK Ward, Amy Ornstein, Anne Niec, C Louise Murray; Canadian Paediatric Society Child and Youth
The medical assessment of bruising in suspected child maltreatment cases: A clinical perspective Michelle GK Ward, Amy Ornstein, Anne Niec, C Louise Murray; Canadian Paediatric Society Child and Youth
Validity of Caregivers Reports on Head Trauma Due to Falls in Young Children Aged Less than 2 Years
 Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Clinical Medicine Insights: Pediatrics Original Research Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Validity of Caregivers Reports on Head Trauma Due
Pan Scan Instead of Clinical Exam? David A. Spain, MD
 Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Pan Scan Instead of Clinical Exam? David A. Spain, MD Granted, some patients don t t need CT scan Platinum Package Stanford Special CT Scan Head Neck Chest Abdomen Pelvis Takes about 20 minutes to do
Indications for cervical spine immobilisation: -
 Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Paediatric Trauma Cervical Spine Guidelines UHW Traumatic injuries of the cervical spine (C-spine) are uncommon in children. However, it is safer assume there is a cervical spine injury until examination
Kristin s Head Trauma Board Questions 11/07/14
 Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Kristin s Head Trauma Board Questions { 11/07/14 A healthy 15 y/o boy was playing football at a park near his home with a group of friends when he tripped over a friend s leg while trying to catch a pass.
Pediatric Abdomen Trauma
 Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
Pediatric Abdomen Trauma Susan D. John, MD, FACR Pediatric Trauma Trauma is leading cause of death and disability in children and adolescents Causes and effects vary between age groups Blunt trauma predominates
Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database
 TECHNICAL SPECIFICATIONS AND METHODS SUPPLEMENT Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database MAY 2017 Minnesota Department of Health Health Economics Program 85 E. 7th
TECHNICAL SPECIFICATIONS AND METHODS SUPPLEMENT Analysis of Low-Value Health Services in the Minnesota All Payer Claims Database MAY 2017 Minnesota Department of Health Health Economics Program 85 E. 7th
3/16/2018. Normal patterns of growth Definition and causes of FTT Medical evaluation and management Effects of FTT Early intervention
 WI CAN Educational Series Hillary W. Petska, MD, MPH, FAAP Child Advocacy and Protection Services Children s Hospital of Wisconsin Normal patterns of growth Definition and causes of FTT Medical evaluation
WI CAN Educational Series Hillary W. Petska, MD, MPH, FAAP Child Advocacy and Protection Services Children s Hospital of Wisconsin Normal patterns of growth Definition and causes of FTT Medical evaluation
Pediatric Trauma Karim Rafaat, MD
 Pediatric Trauma Karim Rafaat, MD Goals Time is short I m going to presume you know your basic ATLS (that s that whole ABCD thing, by the way) Discuss each general trauma susceptible region Focus on: Epidemiology
Pediatric Trauma Karim Rafaat, MD Goals Time is short I m going to presume you know your basic ATLS (that s that whole ABCD thing, by the way) Discuss each general trauma susceptible region Focus on: Epidemiology
Pediatric metabolic bone diseases
 Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
Pediatric metabolic bone diseases Classification and overview of clinical and radiological findings M. Mearadji International Foundation for Pediatric Imaging Aid www.ifpia.com Introduction Metabolic bone
EAST MULTICENTER STUDY DATA DICTIONARY
 EAST MULTICENTER STUDY DATA DICTIONARY Does the Addition of Daily Aspirin to Standard Deep Venous Thrombosis Prophylaxis Reduce the Rate of Venous Thromboembolic Events? Data Entry Points and appropriate
EAST MULTICENTER STUDY DATA DICTIONARY Does the Addition of Daily Aspirin to Standard Deep Venous Thrombosis Prophylaxis Reduce the Rate of Venous Thromboembolic Events? Data Entry Points and appropriate
Management of Severe Traumatic Brain Injury
 Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
Guideline for North Bristol Trust Management of Severe Traumatic Brain Injury This guideline describes the following: Initial assessment and management of the patient with head injury Indications for CT
CONTENT OUTLINE. Child Abuse Pediatrics
 THE AMERICAN BOARD OF PEDIATRICS CONTENT OUTLINE Child Abuse Pediatrics Subspecialty In-Training, Certification, and Maintenance of Certification (MOC) Examinations INTRODUCTION This document was prepared
THE AMERICAN BOARD OF PEDIATRICS CONTENT OUTLINE Child Abuse Pediatrics Subspecialty In-Training, Certification, and Maintenance of Certification (MOC) Examinations INTRODUCTION This document was prepared
2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: CLAIMS, REGISTRY
 Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Measure #416: Emergency Medicine: Emergency Department Utilization of CT for Minor Blunt Head Trauma for Patients Aged 2 through 17 Years - National Quality Strategy Domain: Efficiency and Cost Reduction
Screening and Management of Blunt Cereberovascular Injuries (BCVI)
 Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Grady Memorial Hospital Trauma Service Guidelines Screening and Management of Blunt Cereberovascular Injuries (BCVI) BACKGROUND Blunt injury to the carotid or vertebral vessels (blunt cerebrovascular injury
Child abuse has become widely recognized
 Cause and Clinical Characteristics of Rib Fractures in Infants Blake Bulloch, MD, FAAP, FRCPC*; Charles J. Schubert, MD, FAAP*; Patrick D. Brophy, MD, FRCPC ; Neil Johnson, MD ; Martin H. Reed, MD, FRCPC
Cause and Clinical Characteristics of Rib Fractures in Infants Blake Bulloch, MD, FAAP, FRCPC*; Charles J. Schubert, MD, FAAP*; Patrick D. Brophy, MD, FRCPC ; Neil Johnson, MD ; Martin H. Reed, MD, FRCPC
Paediatric Trauma. A/Prof Drew Richardson. The Canberra Hospital May MB BS (Hons) FACEM Grad CertHE MD
 Paediatric Trauma A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Identify unique anatomic and physiologic characteristics of injured children Describe
Paediatric Trauma A/Prof Drew Richardson MB BS (Hons) FACEM Grad CertHE MD The Canberra Hospital May 2013 Objectives Identify unique anatomic and physiologic characteristics of injured children Describe
Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff. Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012
 Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012 Objectives for Presentation At the end of this talk; the
Evaluation of Failure to Thrive in a Young Child: Case Example of Jeff Andrew Hsi, MD, MPH Family Medicine Pediatric Grand Rounds, 8 August 2012 Objectives for Presentation At the end of this talk; the
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Introduction to Emergency Medical Care 1 OBJECTIVES 31.1 Define key terms introduced in this chapter. Slides 13 15, 17, 19, 28 31.2 Describe the components and function of the nervous system and the anatomy
Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures
 July 2006 Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures Denise De Las Nueces, Harvard Medical School Year IV General Overview Introduction
July 2006 Radiologic Assessment of Child Abuse in Infants: A Focus on Plain Film Analysis of Highly Specific Fractures Denise De Las Nueces, Harvard Medical School Year IV General Overview Introduction
A N.S. Technologists Experiences
 A N.S. Technologists Experiences I have nothing to disclose What does appropriate imaging mean For radiologists? For technologists? How does this affect patients and technologists? Discuss ordering trends
A N.S. Technologists Experiences I have nothing to disclose What does appropriate imaging mean For radiologists? For technologists? How does this affect patients and technologists? Discuss ordering trends
R-SCAN: Engaging Clinicians in Value-based Care
 R-SCAN: Engaging Clinicians in Value-based Care Nancy Fredericks, MBA R-SCAN Director rscan.org What is R-SCAN? A collaborative between referring clinicians and radiologists to improve patient care R-SCAN
R-SCAN: Engaging Clinicians in Value-based Care Nancy Fredericks, MBA R-SCAN Director rscan.org What is R-SCAN? A collaborative between referring clinicians and radiologists to improve patient care R-SCAN
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
Objectives. Pediatric Mortality. Another belly pain. Gastroenteritis. Spewing & Pooing Child 4/18/16
 Gastro-tastrophies A Review of Pediatric GI Emergencies Objectives Discuss common presentations of Pediatric Abdominal Pain complaints Discuss work up and physical exam findings Discuss care, management
Gastro-tastrophies A Review of Pediatric GI Emergencies Objectives Discuss common presentations of Pediatric Abdominal Pain complaints Discuss work up and physical exam findings Discuss care, management
The radiological investigation of suspected physical abuse in children
 September 2017 Contents Foreword 3 1. Introduction 4 2. Recommendations 5 References 11 3. Evidence base 12 4. Working party members and other contributors 20 Appendix A. Skeletal survey: standard views,
September 2017 Contents Foreword 3 1. Introduction 4 2. Recommendations 5 References 11 3. Evidence base 12 4. Working party members and other contributors 20 Appendix A. Skeletal survey: standard views,
Child as a victim of injury. Maciej Dudkiewicz M.D. Ph.D. Dpt of Anaesthesia and Intensive Care Medical University of Lodz
 Child as a victim of injury Maciej Dudkiewicz M.D. Ph.D. Dpt of Anaesthesia and Intensive Care Medical University of Lodz Epidemiology Trauma is most common cause of mortality and morbidity in the US pediatric
Child as a victim of injury Maciej Dudkiewicz M.D. Ph.D. Dpt of Anaesthesia and Intensive Care Medical University of Lodz Epidemiology Trauma is most common cause of mortality and morbidity in the US pediatric
Sometimes we get it wrong. Sheila Weitzman MB BCh
 Sometimes we get it wrong Sheila Weitzman MB BCh Pediatric cancer Survival ~80% One in five children still die Second commonest cause of death in developed countries Delay in diagnosis in children with
Sometimes we get it wrong Sheila Weitzman MB BCh Pediatric cancer Survival ~80% One in five children still die Second commonest cause of death in developed countries Delay in diagnosis in children with
CHILD PHYSICAL ABUSE
 CHILD PHYSICAL ABUSE Kansas Association of Osteopathic Medicine April 13 th, 2018 Jami Jackson DO, FAAP, MPH Children s Mercy Hospitals and Clinics Department of Emergency Medicine Assistant Professor
CHILD PHYSICAL ABUSE Kansas Association of Osteopathic Medicine April 13 th, 2018 Jami Jackson DO, FAAP, MPH Children s Mercy Hospitals and Clinics Department of Emergency Medicine Assistant Professor
Shenandoah Co. Fire & Rescue. Injuries to. and Spine. December EMS Training Bill Streett Training Section Chief
 Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
Shenandoah Co. Fire & Rescue Injuries to the Head and Spine December EMS Training Bill Streett Training Section Chief C.E. Card Information BLS Providers 2 Cards / Provider Category 1 Course # Blank Topic#
LOSS OF CONSCIOUSNESS & ASSESSMENT. Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT
 LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
LOSS OF CONSCIOUSNESS & ASSESSMENT Sheba Medical Center Acute Medicine Department MATTHEW WRIGHT OUTLINE Causes Head Injury Clinical Features Complications Rapid Assessment Glasgow Coma Scale Classification
Contributors. Thanks to Peter Miller, MD; LCDR Kevin Preston, MD; and Keith Newbrough, MD for their generous contribution of images:
 Contributors Thanks to Peter Miller, MD; LCDR Kevin Preston, MD; and Keith Newbrough, MD for their generous contribution of images: Peter Miller, MD, Indiana University School of Medicine Chapter 1: Figure
Contributors Thanks to Peter Miller, MD; LCDR Kevin Preston, MD; and Keith Newbrough, MD for their generous contribution of images: Peter Miller, MD, Indiana University School of Medicine Chapter 1: Figure
BEHAVIORAL EMERGENCIES
 LESSON 21 BEHAVIORAL EMERGENCIES 21-1 Behavioral Emergencies Process of giving first aid may be complicated by victim s behavior Many injuries or illnesses can cause altered mental status or emotional
LESSON 21 BEHAVIORAL EMERGENCIES 21-1 Behavioral Emergencies Process of giving first aid may be complicated by victim s behavior Many injuries or illnesses can cause altered mental status or emotional
Spine MRI and Spine CT Test Request Tip Sheet
 Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of multimodality supervised
Spine MRI and Spine CT MRI is almost always preferred over CT scan; if ordering CT, CLEARLY document why MRI is not appropriate. In cases of back pain without red flags, six weeks of multimodality supervised
Date of Admission: [DATE]. Date of Discharge:
![Date of Admission: [DATE]. Date of Discharge: Date of Admission: [DATE]. Date of Discharge:](/thumbs/74/71277118.jpg) Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
Date of Admission: [DATE]. Date of Discharge: History of Present Illness: Mr. [NAME] AKA [NAME] is a 31-year-old male who presents to the [PLACE] Trauma Surgery Service as a moderate trauma on [DATE] following
